|
BOX 5.1 Suzanne is a divorced mother, with three children under the age of 12.1 She experiences severe pain from rheumatoid arthritis and fibromyalgia that intermittently limits her ability to walk. Since she cannot sit for long periods or drive on a regular basis, she has not been able to hold a steady job. Her ex-husband pays a reasonable level of child support, but he has no health insurance either. Ironically, the child support puts her just over the income level that would make her eligible for Medicaid in her state. She recently enrolled her children in the State Children’s Health Insurance Program (SCHIP), but she finds it difficult to drive them to their regular appointments, either for preventive services or to deal with the mild scoliosis (spinal curvature) of her oldest child. Suzanne, a smoker since she was 15, has tried to quit on her own but, like most heavy smokers, has failed repeatedly. As a caring mother however, she is very good about not smoking around her children. Suzanne’s health would be a lot better if she could get to the doctor regularly, get regular medications for her pain, and get medications and support to help her quit smoking completely. Now that her youngest child is in school every day, she really wants to go to work. She is aware that if her pain were controlled she could likely get some kind of job (maybe even one with health care coverage!) that would help her and her family both financially and emotionally. She thinks she might be eligible for at least partial disability benefits and with this Medicaid coverage for people with disabilities, if only she could afford the full diagnostic work-up needed to document her condition. Suzanne lives in a state that is currently considering expanding the SCHIP program to parents of eligible children. This would be a solution that would help Suzanne and her children a great deal. |
5
Family Well-Being and Health Insurance Coverage
Family members’ health insurance status, use of health care, and health itself are interrelated. This chapter documents the relationship between parents’ health insurance coverage, access to, and use of health services and their children’s coverage and use of health care. Second, it explores the mechanisms by which the health and attitudes of parents can affect the well-being of other family members, specifically their children’s health and life chances. The Committee’s previous report, Care Without Coverage, demonstrates that uninsured parents are likely to have poorer health than they would if insured. Research presented in the second section of this chapter demonstrates the interrelatedness of the health of family members and the effects of stress on the family as a whole.
PARENTS’ INFLUENCE ON CHILDREN’S ACCESS TO AND USE OF HEALTH SERVICES
Parent’s Role in Obtaining Insurance Coverage for the Family
Finding: Many uninsured children are eligible for, but not enrolled in public programs. More than half of the 8 million children who remain uninsured are eligible for Medicaid or State Children’s Health Insurance Program (SCHIP) coverage.
Finding: Extension of publicly supported health insurance to low-income uninsured parents is associated with increased enrollment among children.
Growth in the enrollment of children in Medicaid and SCHIP accounts for most of the increase in the general population insurance coverage rate that occurred between 1999 and 2000 (Hoffman and Pohl, 2002). By December 2001, 3.46 million children were enrolled in SCHIP (Smith and Rousseau, 2002). An estimated 8 million children remained uninsured in 2000 (Urban Institute, 2002a). More than half of those uninsured children, nearly 5 million, were eligible for Medicaid or SCHIP. The potential of these public insurance programs to eliminate much of the problem of uninsurance among children, despite the fact that SCHIP is not an entitlement, has not yet been fully realized.
Overall, if parents are insured, the likelihood is greater that the children will be insured as well (see Chapter 2, Figure 2.7). This pattern holds for lower-income families: if parents are insured children are more likely to be insured (Lambrew, 2001b). Medicaid and SCHIP are more likely to provide coverage for children than for their parents. Thus, lower-income parents have an uninsured rate one and a half times as high (33 percent) as that of lower-income children (Lambrew, 2001b).
Although the simple descriptive information presented in Chapter 2 demonstrates a strong association between parental and child insurance coverage, it does not address whether more low-income children would be insured if coverage were extended to their parents. Very recent studies show that this is likely to be the case. Two studies have examined the coverage rates of children in states that expanded Medicaid coverage to parents. While using different methodologies and different data sets, both studies found that states that had implemented broad coverage expansions to low-income parents had higher child participation rates compared to states that had not expanded coverage to parents (Ku and Broaddus, 2000; Dubay and Kenney, 2002).
One study, based on Current Population Survey (CPS) data examined the coverage of children under age 6 with family income below 133 percent of the federal poverty level (FPL) in three states (Hawaii, Oregon, and Tennessee) that expanded Medicaid eligibility to parents beginning in 1994 (Ku and Broaddus, 2000). The authors report a gain in children’s enrollment of 16 percentage points in the expansion states compared to a 3-point gain in the states that did not expand coverage prior to 1998.
The second study found that in states without coverage expansion to parents, 57 percent of the lower-income children who were eligible enrolled in the Medicaid program, compared to 81 percent in states that expanded coverage to parents (Dubay and Kenney, 2002). When differences among states in the characteristics of the eligible population were taken into account in the analysis (using a multivariable model that controlled for age, race, and health status of the child; work status, education, and nativity of the parent; income and welfare history of the family; and number of children in the family), Medicaid participation rates among eligible children in states with family coverage expansions remained more than 20 percentage points higher than in states with no family coverage.
An examination of Medicaid coverage rates for children in Massachusetts
before and after expansion to their parents confirms these findings (Dubay and Kenney, 2002). In July 1997, Massachusetts introduced expanded coverage for parents up to 133 percent FPL, and found that not only did adult enrollment increase, but enrollment of children also increased, primarily among those already eligible (Dubay and Kenney, 2002). Researchers contrasted changes in the Medicaid coverage for children in Massachusetts before and after implementation of the family coverage with changes in Medicaid coverage for children over this period in the rest of the nation. They also contrasted changes in private coverage and in the uninsured rate in Massachusetts with comparable changes in the rest of the nation in order to assess whether the observed increases in coverage are due to reductions in the uninsured rate or to substitution of public for private coverage.
The studies to date do not explain how these program expansions to parents led to increased enrollment of children. Studies of why so many eligible children remain uninsured, however, demonstrate that parents’ lack of information about the programs, confusion about eligibility, and problems associated with the enrollment process limit children’s participation (Cohen and Wolfe, 2001; Kaiser Commission, 2000). When parents themselves have an opportunity to enroll, they may be more likely to learn about and more motivated to pursue coverage for both themselves and their children. The application process for publicly sponsored health insurance is often fraught with delays and barriers that may be particularly burdensome for lower-income parents. Although the process is being simplified in many states, it can still be cumbersome and humiliating (see Box 5.2).
After initial enrollment, public insurance coverage typically lasts for only one year and parents must recertify themselves and their children annually (and sometimes more frequently) to maintain coverage.1 A survey of more than 3,700 parents in seven states shows that 34 percent of parents of current SCHIP enrollees and 44 percent of families who did not re-enroll thought that too much background paperwork, such as pay stubs or income documentation, was required for renewal (National Academy for State Health Policy et al., 2002).
Care-Seeking Behavior Within Families with Children
Finding: If parents use health care, their children are more likely to use health care as well.
Parents bring their own experiences to bear when making decisions about care for their children, and children’s use of health care is highly correlated with their parents’ utilization. For example, mothers with high physician use are nearly four times as likely to have children with high physician use, compared to children of mothers with low use (Newacheck, 1992). Parents who have experienced
|
BOX 5.2 Enrolling in Medicaid and SCHIP1 Applying for Medicaid or SCHIP is more difficult than enrolling in a workplace health plan, and enrollment periods are shorter. To qualify for either Medicaid or SCHIP, a child must be in a family with income below a specified level (the level may vary with the age of the child), reside in the state, and in some cases, be a citizen or have resided in the United States before a given date. As part of the application process, families need to fill out an application form and supply proof of family income, child’s age, child’s residence, and for some children, immigration status. Federal law requires only one document—proof of qualified alien status for individuals applying who are not citizens of the United States.2 States determine what constitutes proof of meeting the other eligibility requirements and the information that is requested on the application form. States establish the period of enrollment and thus determine how frequently families must document eligibility. They also determine whether applicants must have a face-to-face interview or can apply by mail. Each of these administrative choices affects how burdensome the application process is for enrollees. Most of the states have simplified enrollment in Medicaid and SCHIP: For example,
Most states no longer require documentary proof of age (e.g., birth certificate) or residence (e.g., lease). To a lesser extent (a quarter of the Medicaid programs and a third of the separate SCHIP), states are moving away from the requirement for documentary proof of income (e.g., pay stubs) if evidence of income is available elsewhere in the state’s records. |
access problems or negative encounters with health care may have less confidence not only in obtaining care for themselves, but also for their children. Further, a parent who does not have a regular source of care or who has problems with access may also have difficulty negotiating the health care system on behalf of their children. This section looks first at studies that relate parental use of care to their children’s use and then at subjective experiences with health care.
The Relationship Between Parent’s Use and Children’s Use
Studies conducted over the past two decades suggest that insuring children without insuring parents may not be enough to ensure that children fully benefit from their coverage. A parent’s lack of connection to the health care system may be a more important barrier to care for the child than lack of insurance, as demonstrated by several large studies.
One of the early studies (Newacheck and Halfon, 1986) examined the association between mothers’ and children’s use of physician services using the 1978 National Health Interview Survey (NHIS) and found that mothers’ use of health care was the single best predictor of children’s use or nonuse and second only to the child’s health status in predicting number of visits.
More recently, other studies have reexamined the link between parents’ and children’s health care utilization and have reached similar conclusions (Hanson, 1998; Minkovitz et al., 2002). Hanson (1998) analyzed the impact of maternal utilization separately for children with private insurance and children with no insurance, using the 1990 NHIS and found that a primary parent’s use of physician services remains the most potent predictor of children’s use for both uninsured and privately insured children, when other individual and family attributes are controlled. No other independent variables approached the magnitude of this effect, with the exception of measures of age and health status of the child. Both groups of children are more likely to have a physician visit if their parents do and to have more physician visits if their primary parent also has more visits. Minkovitz and colleagues (2002) used the 1996–1997 Community Tracking Study Household Survey to examine the relationship between maternal use of services and children’s use and found a strong relationship for a variety of services, including physician visits, emergency department use, hospitalizations and mental health visits. These authors concluded that the strong associations suggest that patterns of maternal use are important for understanding and improving children’s health care utilization.
The association between parental and children’s use of care is more substantial in the privately insured group. Uninsured children whose primary parent had a physician visit were twice as likely to have had a visit themselves, whereas privately insured children were three times as likely, compared with children whose parent had no visit. This finding demonstrates that the combination of parental experience within the health care delivery system (measured here as at least one physician visit) and financial access for the child (measured here as private health insurance coverage) increases a child’s likelihood of having a physician visit over
the effect of insurance alone. Hanson (1998) concludes that even if all children were insured, parents’ health care utilization would remain a key determinant in children’s use of services.
Most recently, the relationship between parental insurance status and children’s access to care has been evaluated. Davidoff and colleagues (2002) analyzed the NSAF 1999 data set and found that having an uninsured parent decreased the likelihood that a child would have any medical provider visit by 6.5 percentage points and the likelihood of a well-child visit by 6.7 percentage points, compared with having an insured parent. In addition, this analysis found that a parent without health insurance is less likely to have confidence in the family’s ability to get medical care when needed. As would be expected, the effects of having uninsured parents are smaller than the effects of the children themselves being uninsured. Still, they add to the mounting body of evidence that links parents’ well-being to that of their children.
The link between parental use of health care and the use of such care for their children possibly is established even before birth. For example, mothers receiving less-than-adequate prenatal care also take their children for well-child visits less often than do women with adequate prenatal care. Also, children of mothers with less-than-adequate prenatal care are less likely to be immunized, even after controlling for a number of important factors, including income and insurance status (Bates et al., 1994; Kogan et al., 1998a; Freed et al., 1999). Further evidence of parental attitudes affecting the care children receive is provided by a study of influenza vaccination rates for children with asthma. It found parental concern to be an important factor in whether or not such children were vaccinated (Szilagyi et al., 1992).
Experiences with the Health Care System
The experiences that parents have when seeking care can affect their decisions about health care for their children. Uninsured adults are more likely to have negative reactions to their encounters with health care institutions and providers than are insured adults. They are more likely than insured adults to rate physician care experiences more negatively and to express dissatisfaction with waiting time and time spent with physicians (Schoen and Puleo, 1998). Finally, uninsured adults are more likely to have negative experiences with the health care system related to bill paying (Duchon et al., 2001).
Racial and ethnic minority families are more likely to be dissatisfied with their experiences seeking health care and they are more likely to be uninsured than are white, non-Hispanic families. Proportionally more Hispanics, African Americans, and Asian Americans than non-Hispanic whites report that they had been treated with disrespect by the health care system. Furthermore, they report that they think they would have received better care or would have been treated with more respect were it not for their race or ethnicity, their language skills, or their ability to pay for their care. They report negative experiences with the health system
more frequently than do whites (Collins et al., 2002; Doty and Ives, 2002; Hughes, 2002).2
Insurance coverage is an important factor contributing to improved satisfaction with care received:
-
Insured Hispanic adults more often report being very satisfied with their care than do uninsured Hispanic adults (62 percent and 42 percent, respectively).
-
Uninsured respondents in all racial and ethnic categories are less likely to have confidence in their ability to receive quality care than are insured respondents (35 percent compared to 51 percent) (Collins et al., 2002).
These negative experiences of minority adults may affect their attitudes and behavior in seeking care for their children.
Uninsured adults in poor health are especially likely to encounter access problems in obtaining care for themselves; they are two to three times as likely to go without needed care and are twice as likely to lack a regular source of care as healthier uninsured adults (Schoen and Puleo, 1998; Duchon et al., 2001). Uninsured adults in fair or poor health are more likely to have experienced a time without needed care than are continuously insured adults of comparable health status. Schoen and Puleo (1998) find that the worse the health status, the greater is the likelihood of access problems when insurance status is controlled in the analysis. At the same time, they found that being currently or recently uninsured at least doubles the likelihood of experiencing access problems compared to those with insurance at every level of health (Schoen and Puleo, 1998).
Conclusion
The Committee has previously shown that insured adults are more likely to have a physician visit and use other health services than are uninsured adults (IOM, 2001, 2002a). The weight of the studies just discussed suggest that neglecting financial access to care for adults may have the unintended effect of diminishing the impact of targeted health insurance programs for children. While providing health insurance to parents would not guarantee appropriate health care visits for their children, it is one potential intervention that might help.
EFFECT OF FAMILY HEALTH ON CHILD HEALTH AND WELL-BEING
The previous section demonstrates that parental insurance and use of health care may be important determinants of children’s coverage and use of health care,
which suggests that providing health insurance for children is a necessary, but not sufficient, condition for ensuring appropriate health care for children.
In this section, the Committee extends the discussion of interdependencies within families beyond health insurance and health care use to health itself. Specifically, this section explores the interactions between parental health and family environment and children’s health and well-being. Research in this area, too, suggests that parents are critical to the well-being of their children.
Studies to date have not addressed the role of health insurance in these larger complex family health interactions. Nonetheless, family health interdependencies should serve as a backdrop when considering health insurance policy issues. Debates around current policies, which target individuals, often lose sight of the larger family context in which the consequences of policies are actually experienced.
Parents’ Health and Children’s Well-Being
Finding: The health of one family member can affect the health and well-being of other family members. In particular, the health of parents can play an important role in the well-being of their children.
Finding: Parents in low-income families and families with children have higher rates of poor mental and physical health than do parents in higher-income families. There is substantial overlap between poor parental physical and mental health.
Parents in poor health may have greater difficulty attending to their children’s health needs. It is easy to imagine that getting children to a doctor, getting immunizations on schedule, and coping with children’s illnesses are likely to be more difficult for parents in poor health, particularly those with impaired mobility or certain mental health conditions. Parents with health insurance are more likely to receive appropriate care for their health conditions and would be expected to experience better health than they would if they lacked coverage (IOM, 2002a).
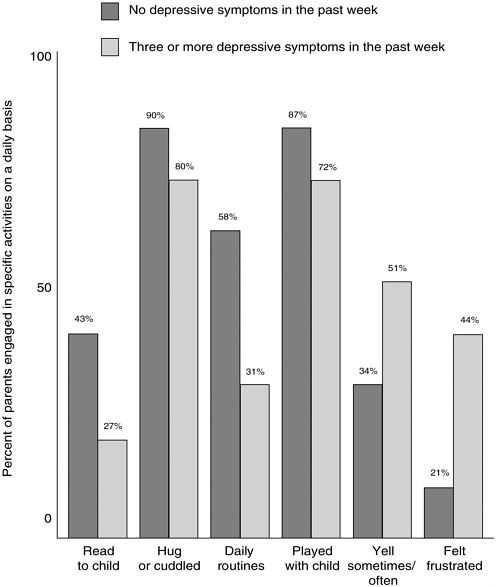
Much of the research on parental health and its effect on children addresses mental health, particularly depression in mothers. There is a growing body of evidence that parents’ mental health strongly affects childrearing practices (Shonkoff and Phillips, 2000). Those parents reporting poor mental health are more likely to yell and feel frustrated with their children and less likely to read, play with, or hug their children or to establish orderly daily routines for meals, naps, and bedtime (Young et al., 1998), as shown in Figure 5.1.
Research also shows that children of depressed mothers display greater social, behavioral, and academic impairment from infancy through adolescence than do children of non-depressed mothers (Hammen et al., 1987; Downey and Coyne, 1990; Nolen-Hoeksema et al., 1995). Studies find that parental depression is reflected in the child, increasing the probability of significantly decreased social
competence, impaired academic performance, poor school behavior, and relatively chronic, clinically significant problems in psychosocial functioning (Anderson and Hammen, 1993), as well as significantly higher rates of affective disorder (Beardslee et al., 1993; Boyle and Pickles, 1997). In addition, parental depression increases the likelihood of negative maternal behavior and disengagement from the child.
While most research has examined the impact of poor parental health on children’s health and well-being, recent studies have investigated the relationship in the other direction. These studies use poor child health as a risk factor for poor parental health (Lyons-Ruth et al., 2000). A very recent study (Bethell et al., 2002) showed this association for a group of Medicaid-insured parents. Specifically, parents of children who are in poor physical health or have special health needs are more likely to be in poor mental health themselves than are parents whose children are not in poor physical or mental health. Of parents who have a child with a special health need or in poor health, 30 percent show symptoms of depression in contrast to 18.6 percent of parents who do not have such children. Because all parents in this study were enrolled in Medicaid, it does not provide comparative information about uninsured and insured parents. Rather, it suggests that the demands on parents of caring for sick children can be severe and place parents’ health at risk.
Other studies also find that when children are in poor health, their parents may be adversely affected. For example, the well-being of parents may be affected by having a child with asthma, but other family characteristics such as “coherence” and “hardiness” also play important roles (Svavarsdottir et al., 2000). Stress and negative health outcomes in parents have been found to be associated with the presence of specific chronic conditions in children (Bouma and Schweitzer, 1990; Walker et al., 1992). In low-income households with other stressors in the home, the presence of children in the home may be a contributor to poor parental mental health (Lyons-Ruth et al., 2000). Having an unhealthy child is associated with a greater likelihood that a mother will be single and thus that she and her child will face additional social and economic challenges and obstacles (Corman and Kaestner, 1992).
Studies find that the rates of poor parental health vary by income groups, with the lowest-income groups at greatest risk (Lovejoy et al., 2000). A study of firsttime welfare recipients reported that 52 percent were at risk for clinical depression (Kalil et al., 2001). A number of studies and surveys have found that women with young children, those who are low income, and single mothers report high numbers of depressive symptoms (Belle, 1990; Jackson, 1992; Kahn et al., 2000; Siefert et al., 2000; Reading and Reynolds, 2001). It is unclear the extent to which poverty and its related economic effects might contribute to clinical depression in parents, the extent to which depression in parents might limit their earnings, and the impact of health insurance on these circumstances.
The National Survey of American Families also shows high levels of poor physical and mental health, particularly among parents of children at the lowest income levels.3 One-third of parents with family incomes below 100 percent
TABLE 5.1 Percentage of Parents in Poor Physical and Mental Health Across Income Ranges
|
Parents |
<100% FPL n = 4,889 |
100-200% FPL n = 7,692 |
>200% FPL n = 21,651 |
|
Fair or poor physical health |
27.2 |
14.6a |
5.9a |
|
Poor mental health |
33.1 |
16.8a |
10.1 |
|
Very poor mental health |
22.3 |
10.8a |
5.5a |
|
ap <.001. SOURCE: Analysis of 1999 National Survey of American Families data conducted by Gerry Fairbrother. |
|||
FPL report symptoms of poor mental health and more than one-quarter (27 percent) describe their physical health as fair or poor (see Table 5.1). In fact, only 37 percent of parents below 100 percent FPL say that their physical health is either “excellent” or “very good.” (This is the income band at which most of the Medicaid expansions that include parents are targeted.) Parents with family incomes between 100 and 200 percent FPL and proportionally more of those with incomes above 200 percent FPL report better physical and mental health than do those in families with incomes below 100 percent FPL. Only 10 percent of parents in the highest-income group and 17 percent of those from 100 to 200 percent FPL report symptoms of poor mental health compared with 33 percent of those in families with incomes below 100 percent FPL.
The physical and mental health of parents serving as the primary child caregiver is related. Forty-three (43) percent of caregivers with poor physical health reported poor mental health as well. Adding together the percentage of caregivers with either poor physical or poor mental health yields 42 percent of caregivers in families with incomes below 100 percent FPL, compared to 23 percent within families with incomes at 100–200 percent FPL and 10 percent in families with incomes above 200 percent FPL.
The impact of health insurance for either parent or child on the psychological well-being of the other has not been studied. Thus, conclusions about the degree to which health insurance coverage could improve family members’ psychological well-being cannot be drawn based on the research conducted so far. However, the Committee’s previous report, Care Without Coverage, concluded that health insurance was associated with better physical and mental health outcomes for working-age Americans and that adults who do not have health insurance suffer diminished health and experience reduced life expectancy. In addition, the Committee found that having any health insurance, even if it does not specifically cover
mental health services, increases the likelihood that an adult with a condition such as depression or anxiety will receive some care for that condition (IOM, 2002a). The separate strands of research regarding health interactions among family members and the potential of health insurance to ameliorate these are promising and warrant further investigation.
The Family Environment
Finding: Family stress may adversely affect the health of its members and is associated with higher levels of behavioral and emotional problems in children. Lower-income families tend to have higher levels of stress than higher-income families.
Finding: There is some very limited evidence that having health insurance for children may reduce the amount of family stress, enable children to get the care they need, and ease some family burdens.
Some researchers have moved beyond the health of the parents to examine the health of the family environment and its impact on child well-being (Shonkoff and Phillips, 2000). These researchers have identified linkages between stress in families and adverse physical and psychological effects on children and adolescents (Garmezy, 1983; Johnson, 1986; Compas, 1987).4 Moore and Vandivere (2000) show that family stress affects the level of children’s engagement in their school-work and that it is also associated with higher levels of behavioral and emotional problems for both children and youth. Although Moore and Vandivere do not address the possibility of children’s behavior or school problems causing family stress, their findings are consistent with other research indicating that maternal psychological distress and high family stress are associated with greater behavioral problems among children (Myers et al., 1992; Resnick et al., 1993). Yager (1982) describes the possible role of family stress patterns in the development of anorexia nervosa in adolescents, and other studies show an association between family stress and the use of mental health services among children (Verhulst and van der Ende 1997). It would be reasonable to expect that families with children suffering the ill effects of stress and in need of mental health services would have easier access to them if their children were insured. This has not been directly examined in empirical studies, however.
Families with incomes below 200 percent FPL experience more stress than do
higher-income families.5 Forty percent of children in families with incomes below 200 percent FPL live in stressful environments, in contrast to 22 percent of all children (Moore and Vandivere, 2000). Echoing the link between parental health and child well-being, other studies show the effect of family stress on the physical health and well-being of children. Specifically, studies show that high levels of family stress are associated with the poor metabolic control of diabetes in children and adolescents (Viner et al., 1996) and that family stress may play an important role in the development of coronary risk in children (Weidner et al., 1992). The connections between family stress and difficulties for parents in providing good home environments for their children are evident (Straus et al., 1980; Cole and Cole, 1993).
Family stress has many varied dimensions, and health policies may have at least the potential for ameliorating some of them. For example, parents report that having health insurance for their children reduces the amount of family stress, enables children to get the care they need, and eases family burdens (Lave et al., 1998a). Dubay and Kenney (2001) report that parental confidence that family members can obtain needed care is strongest when all family members are insured. There are still too few studies examining the relationship between family stress and health insurance coverage to support definitive conclusions. Nevertheless, the recent studies provide good reason to assess a broader array of phenomena and indicators of personal and familial well-being in considering the effects of the lack of health insurance than has been customary in health services research.
SUMMARY
A family encompasses an array of social, economic, and emotional relationships that are not well studied by health services and health policy researchers. Research that addresses discrete aspects of health, care-seeking behavior, and well-being within families suggests, however, that having the whole family covered by health insurance is important. Because parents are the key decision makers and seekers of care for their children, their own connections to the health care system are important for their children as well as for themselves.
If parents are insured they are more likely to have insured children than are uninsured parents. Medicaid and SCHIP have not yet fulfilled their considerable potential for reducing uninsurance among American children. Some states have found that expanding eligibility for parents is an effective way to promote enrollment of eligible children in Medicaid and SCHIP.
Insured adults have better access to the health care system and are more likely to use services than are uninsured adults. In addition, insured adults are less likely to have unmet health needs, have their health deteriorate, and die prematurely
than are uninsured adults. Studies show that a mother’s use of health services is a strong predictor of her child’s use of care. Being uninsured can affect one’s attitudes toward and use of the health care system, and for parents this has implications for their children.
Healthier parents are better able to care for their children and have better child rearing practices. The illness of a parent, particularly depression, is associated with poorer psychosocial functioning of the child. The Committee previously found that health insurance is associated with more appropriate care for conditions such as depression.
Stress in the family environment, particularly at higher levels, is associated with physical and behavioral health problems for the children. Lower-income parents are more likely to report higher levels of stress than are parents with higher incomes. Parents also report that having health insurance for their children reduces stress.
Many factors contribute to the health and stability of families. Health insurance is one important factor. Recent studies examining the relationship between family stress and health insurance coverage are suggestive and argue for a more systematic assessment of the impact of health insurance on a broad array of indicators of personal and familial well-being. Providing health insurance to all members of a family is one intervention that could improve the health not only of those who gain coverage but also, through the interdependence of the health and activities of family members, of others in the family as well.
|
BOX 5.3 Summary of Findings
|