Executive Summary
BACKGROUND
The establishment of sanitary practices in the late nineteenth century for the disposal of sewage and the increasing use of filtration and chlorination of drinking water throughout the twentieth century resulted in a dramatic decrease in waterborne diseases such as cholera and typhoid fever in the United States. Despite these historical efforts, ongoing advances in water and wastewater treatment, and several layers of federal, state, and local government laws, regulations, and guidance designed to protect public water supplies from contamination, waterborne disease outbreaks still occur every year in the United States. Furthermore, epidemiologists generally agree that these documented outbreaks represent only a fraction of the total that actually occur because many go undetected or unreported.
In order to protect public health, and as mandated in the Clean Water Act and the Safe Drinking Water Act (SDWA), it is important to have accurate, reliable, and scientifically defensible methods for determining whether source waters for drinking water and recreational waters are contaminated by pathogens and to what extent. For more than 100 years, U.S. public health personnel have relied extensively on an indicator organism approach to assess the microbiological quality of drinking water. More specifically, these enteric bacterial indicator microorganisms (predominantly “coliforms”1) are typically used to detect the possible
|
1 |
Coliforms include several genera of bacteria belonging to the family Enterobacteriaceae, of which Escherichia coli is the most important member. The historical definition of this group is based on the method (lactose fermentation) used for its detection (see Chapter 1 for further information). |
presence of microbial contamination of drinking water from human waste. The use of coliforms was later expanded and adopted for ambient, recreational, and shellfish waters and continues to focus on identification of fecal contamination.
Over the long history of their development and use, the current bacterial indicator approaches have become standardized, are relatively easy and inexpensive to use, and constitute a cornerstone of local, state, and federal monitoring and regulatory programs. An increased understanding of the diversity of waterborne pathogens, their sources, physiology, and ecology, however, has resulted in a growing understanding that the use of bacterial indicators may not be as universally protective as was once thought. For example, the superior environmental survival of pathogenic viruses and protozoa raised serious questions about the suitability of relying on relatively short-lived coliforms as an indicator of the microbiological quality of water. That is, while the presence of coliforms could still be taken as a sign of fecal contamination, the absence of coliforms could no longer be taken as assurance that the water was uncontaminated. Thus, existing bacterial indicators and indicator approaches do not in all circumstances identify all potential waterborne pathogens. Furthermore, recent and forecasted advances in microbiology, molecular biology, and analytical chemistry make it timely to reassess the current paradigm of relying predominantly or exclusively on traditional bacterial indicators for waterborne pathogens. Nonetheless, indicator approaches will still be required for the foreseeable future because it is not practical or feasible to monitor for the complete spectrum of microorganisms that may occur in source waters for drinking water and recreational waters, and many known pathogens are difficult to detect directly and reliably in water samples.
This report was written by the National Research Council (NRC) Committee on Indicators for Waterborne Pathogens—jointly overseen by the NRC’s Board on Life Sciences and Water Science and Technology Board—and comprised of 12 volunteer experts in microbiology, waterborne pathogens (bacteriology, virology, parasitology), aquatic microbial ecology, microbial risk assessment, water quality standards and regulations, environmental engineering, biochemistry and molecular biology, detection methods, and epidemiology and public health. This report’s contents, conclusions, and recommendations are based on a review of relevant technical literature, information gathered at four committee meetings, a public workshop on indicators for waterborne pathogens (held on September 4, 2002), and the collective expertise of committee members. Furthermore, because of space limitations, this Executive Summary includes only the major conclusions and related recommendations of the committee in the general order of their appearance in the report. More detailed conclusions and recommendations can be found within individual chapters and are summarized at the end of each chapter.
The committee was formed in early 2002 at the request of the U.S. Environmental Protection Agency (EPA) Office of Water and originally charged to report on candidate indicators and/or indicator approaches (including detection technologies) for microbial pathogen contamination in U.S. recreational waters
(excluding coastal marine water and marine-estuarine water) and source water (including groundwater) for drinking water. It is important to note that the committee’s original charge was slightly but substantively altered after its first meeting and subsequent discussions with EPA, most notably to include coastal and marine-estuarine recreational waters that were originally excluded (see Box ES-1). The consequences of this important change regarding the emphasis and content of this report are summarized in Chapter 1. For example, it was agreed that the report would give less space and emphasis to defining currently known waterborne pathogen classes and anticipating those emerging waterborne patho-
|
BOX ES-1 The NRC will convene a committee to report on candidate indicators and/or indicator approaches (including detection technologies) for microbial pathogen contamination in U.S. recreational waters (including coastal marine water and marine/estuarine water) and source water (including groundwater). Specifically, the committee will:
|
gens that are likely to be of public health concern (although Appendix A provides a brief summary discussion and table of new and [re]emerging waterborne pathogens).
While this is the first NRC study to focus specifically on indicators for waterborne pathogens, issues surrounding their use have been discussed in several recent and historical NRC reports, as summarized in chronological order in Appendix B. In addition, many federal, state, and local government and nongovernmental organizations, including the water industry and academia, have addressed the issue of the microbiological quality of drinking water and recreational water and its association with various adverse human health effects. Thus, Appendix B also includes summaries of some major reports that have been published addressing these concerns.
HEALTH EFFECTS ASSESSMENT: EPIDEMIOLOGY OF WATERBORNE HUMAN DISEASE
The ultimate objective for determining the microbiological quality of water is to identify and then minimize the public health risk from consuming water intended for drinking and from exposure to recreational water. Health effects assessments for waterborne pathogens can be based on a number of approaches. Each approach has strengths and weaknesses (see Chapter 2 for further information), and all have been or are being used to document and quantify the health risks from microbes in water. Many of these approaches involve the use of epidemiology, which is a well-established, essential tool for determining the linkage between the presence of identified waterborne pathogens and their indicators and human disease. However, the significant cost and methodological difficulty of designing, conducting, and interpreting epidemiologic studies have limited their use.
One health effects assessment approach that is being used increasingly for waterborne pathogens is quantitative microbiological risk assessment (QMRA). Developed in the 1980s following the traditional framework for chemical risk assessment, QMRA has several substantive differences, and most applications to date have focused on its use to predict primary infections or illnesses resulting from exposure to a contaminated medium such as water. QMRA is a useful tool for identifying the potentially most influential parameters in the waterborne disease transmission process for which there are data gaps, especially models that include infectious disease parameters such as immunity. However, some of the key needs for QMRA include dose-response and exposure information (e.g., intensity and duration of contagion), which are often lacking. In some cases, impacts from such population level phenomena may dramatically alter projected estimates of human risk.
The comprehensiveness of investigations of waterborne disease outbreaks in the United States varies by the type of outbreak and by state, and results are
compiled in the Centers for Disease Control and Prevention’s (CDC’s) surveillance system. However, this system has low sensitivity and does not consistently provide information that links indicator and pathogen data with adverse health outcomes. This gap occurs because most outbreak investigations include primarily the epidemiologic component which concentrates on linking illness to water (e.g., through determination of the agent in clinical specimens), and tend to neglect the environmental component (e.g., determination of water quality through measurement of indicator and pathogen occurrence in the water). This gap occurs more frequently with outbreaks associated with drinking water than with those associated with recreational water. In addition, 40-50 percent of the identified waterborne disease outbreaks remain of unknown etiology.
A substantial effort to determine the potential health risks associated with consumption of drinking water has been going on since the late 1990s. As required by the SDWA Amendments of 1996, epidemiologic studies of drinking water and endemic disease have focused on establishing associations between water consumption and gastrointestinal illness. Thus far, these studies have not established a good correlation between indicators of waterborne pathogens, the pathogens themselves, and adverse human health effects, although some earlier studies have shown an association between tap water and endemic gastrointestinal illness. To have adequate statistical power to address the epidemiologic association of health outcomes with specific indicators and specific waterborne pathogens, the study sample has to be large, which leads to significant costs. In addition, methodologic complexities as well as difficulty in interpretation of results have limited the use of some of the studies.
In contrast, epidemiologic studies involving recreational bathing waters have shown predictive associations between several swimming-associated health effects and various microbial indicators or pathogens. A recent systematic review and meta-analysis of recreational waterborne studies (both freshwater and marine) undertaken at the specific request of the committee confirmed that indicators can provide reliable estimates of water quality that are predictive of human health risks under some but not all water quality conditions (see Chapter 2 for further information).
Building on these conclusions, the committee provides several recommendations regarding future directions for epidemiologic and microbiological research as related to health effect assessment for waterborne pathogens and their indicators. In this regard, the committee first recommends that EPA and CDC take a greater leadership role in such efforts, and fund and work with stakeholders and academic researchers in the following areas:
-
CDC should actively work with state and local health departments to encourage testing for pathogens (especially viruses and parasites) in clinical specimens during waterborne outbreak investigations.
-
CDC and EPA should actively work with state and local health depart-
-
ments to encourage collection and testing of environmental data (i.e., water quality data for source, finished, and distribution system waters that include indicators and pathogens) during waterborne outbreak investigations.
-
Standardized protocols and definitions are needed for outbreak investigations and epidemiologic studies, especially to help ensure a comprehensive investigation or study that includes the collection of clinical, laboratory, and environmental data (including co-occurrence of pathogens and indicators).
-
Fewer but more comprehensive epidemiologic studies should be conducted rather than multiple small-scale studies that do not adequately address multiple risk factors and health outcomes when working within a fixed or constrained budget. More specifically, the link between pathogens and their potential indicators, and among pathogens, indicators, and adverse health outcomes, would be strengthened by including in comprehensive and adequately funded studies, epidemiologic measurements of health outcomes, measurements of pathogens in clinical specimens, as well as measurements of pathogens and their potential indicators in relevant water samples.
-
Additional epidemiologic studies are needed to look at the association between water consumption and gastrointestinal illness in groundwater systems, and to correlate water quality data (pathogens and indicators) with health outcomes. Furthermore, these studies should include the collection of epidemiologic, clinical, laboratory, and environmental data whenever feasible.
-
Health outcomes studied in association with drinking water exposure should not be limited to gastrointestinal illness (e.g., should consider including respiratory and dermatological illnesses).
-
Additional epidemiologic studies should be conducted to determine the occurrence of chronic/recurrent disease attributable to waterborne pathogens in habitual users of recreational waters (e.g., surfers) from point and nonpoint sources of contamination.
-
Studies on recreational waters should be carried out on a broader range of geographical and ecological sites, including tropical and sub-tropical waters, and ocean beaches.
ECOLOGY AND EVOLUTION OF WATERBORNE PATHOGENS AND INDICATOR ORGANISMS
The nature and abundance of waterborne microbial assemblages and communities varies widely from location to location and over time, according to various environmental and anthropogenic factors. In general, most waterborne pathogens of public health concern discussed in this report (see also Appendix A) are not native to the types of waterbodies addressed here, but are introduced from either point sources (e.g., sewage discharge) or nonpoint sources (e.g., agriculture, rainfall).
Past efforts to develop and implement indicators of microbial contamination
have often given little or no consideration to the role of evolution in the ecology and natural history of such waterborne pathogens. Their ecology and evolution, however, have important implications for their emergence and reemergence in the aquatic environment and for subsequent public health concerns. Furthermore, the concept of using indicators for waterborne pathogens implies that certain characteristics of microorganisms such as genes and gene products remain constant under varying environmental conditions. However, this assumption does not always hold because the effectiveness of indicator technologies that are based on the detection of some aspect of the biology or chemistry of a living organism (whether a pathogen or an indicator microorganism) may decrease over time due to evolutionary changes in the target organism. Therefore, it is important to understand the effects of the environment on these targets and organisms. For these reasons, existing and candidate indicator organisms should have ecologies and responses to environmental variations that are similar to those of the pathogenic organisms whose presence they are supposed to be indicating.
The committee provides the following recommendations to improve understanding of the ecology and evolution of waterborne pathogens, as related to the development of new and effective indicators of microbial contamination:
-
Bacteria, viruses, and protozoa have evolved mechanisms that facilitate their rapid response to environmental changes and may influence their infectivity and pathogenicity. Therefore, additional research is needed on microbial evolutionary ecology to address long-term public health issues.
-
Genetic and phenotypic characterizations of pathogenic viral, bacterial, and protozoan parasites are needed to elucidate zoonotic relationships with their animal hosts and the factors influencing waterborne transmission to humans.
-
The ecology of waterborne pathogens should be assessed in relation to modern agricultural practices and other anthropogenic activities, such as urbanization. Animal wastes from agriculture and urban sewage, runoff and storm water are major contributors of both human pathogenic and non-pathogenic strains of microbes and the wide use of antibiotics in animal agriculture and in human and veterinary therapy leads to selection for antibiotic-resistant phenotypes.
-
Advanced analytical methods should be used to help discriminate between introduced pathogenic and naturally occurring non-pathogenic strains of waterborne microorganisms and to characterize the emergence of new strains of pathogens as a result of genetic change.
-
Natural background density of waterborne pathogens should be established to differentiate between native opportunistic pathogens and introduced pathogens. Efforts should be made to differentiate between indicators and pathogens that are native to the environment and those that are introduced from external sources, such as human and animal wastes.
-
Research is need to develop a better understanding of the ecology and natural history of both the environmental and infectious stages of pathogens and
-
the parallel stages of indicator organisms to grasp how the organisms are distributed in nature; how they persist and accumulate in water, other environmental media, and animal reservoirs; and how dissemination of the environmental form occurs, especially human exposure.
ATTRIBUTES AND APPLICATION OF INDICATORS
Microbial water quality indicators are used in a variety of ways within public health risk assessment frameworks, including assessment of potential hazard, exposure assessment, contaminant source identification, and evaluating effectiveness of risk reduction actions. As noted previously, however, no single indicator or analytical method (or even a small set of indicators or analytical methods) is appropriate to all applications. A suite of indicators and indicator approaches is required for different applications and different geographies.
For almost 40 years, Bonde’s attributes of an ideal indicator have served as an effective model of how a fecal contamination index of public health risk and treatment efficiency should function (see Box 4-1). However, Bonde’s attributes must be refined to continue their relevance to public health protection because the development and increasing availability of new measurement methods necessitates the separation of criteria for evaluating indicators and detection methods. Historic definitions of microbial indicators, such as coliforms, have been tied to the methods used to measure them. Newly available methods (particularly molecular methods) allow more specificity in the taxonomic grouping of microorganisms that are measured. More importantly, a variety of new methods are becoming increasingly available, providing several options for measuring each indicator group. Thus, separate criteria allow one to choose the indicator with the most desirable biological attribute for a given application and then match this with a measurement method that best meets the need of the application. Box ES-2 provides a summary listing of desirable biological attributes of indicators and desirable attributes of indicator methods (see Boxes 4-2 and 4-3 for further information).
The most important biological attribute is a strong quantitative relationship between indicator concentration and the degree of public health risk. One of the most important method attributes is its specificity, or ability to measure the target indicator organism in an unbiased manner. The speed of the method (processing time and rapidity of results) is also an important characteristic in many applications.
Several factors limit the effectiveness of current recreational water warning systems, the most prominent of which is the delay in warnings caused by long laboratory sample processing time. One approach that is increasingly being used to address this problem is predictive models intended to prevent exposure. Another shortcoming of present warning systems is the poorly established relationship between presently used indicators and health risk. Present studies do not
|
BOX ES-2 Biological Attributes of Indicators
Attributes of Methods
|
address all sources of contamination, have not been conducted in enough geographic locations, and do not address chronic exposure. Many reported failures of beach water quality standards are associated with nonpoint source contamination, but the epidemiologic studies used to establish recreational bathing water standards have been based primarily on exposure to point source contamination dominated by human fecal material. A final problem with present water contact warning systems is that bacterial indicator concentrations are spatiotemporally variable and most sampling is too infrequent to transcend this granularity. There are many promising source identification techniques that can help in deciding whether a health warning should be issued or in identifying the best approach for fixing the problem. However, these techniques have not yet been standardized or fully tested.
Groundwater quality monitoring is rare, despite data that show the majority of waterborne outbreaks of disease in the United States result from groundwater systems. Viral contamination of groundwater is a particular concern because the small size and considerable environmental persistence of viruses makes it more likely they will reach and contaminate groundwater. The known risks from viruses in fecally contaminated groundwater, and evidence that human enteric viruses are detectable in fecally contaminated groundwater, suggest that coliphage or direct virus monitoring would enhance the assessment of groundwater microbiological quality and would make a better indicator of human health risk.
The committee makes the following recommendations related to the consideration and use of indicator attributes for different applications:
-
The link between potential indicators and pathogens, and among indicators, pathogens, and adverse health outcomes, would be strengthened by including measurements of both indicators and pathogens in comprehensive epidemiologic studies. In particular, studies should be conducted to better assess the role of nonpoint sources in occurrence of human pathogens and indicator organisms, disease outbreaks, and endemic health risks in recreational waters. Use of alternative indicators need to be included in these studies.
-
Improved indicators for viruses in groundwater sources of drinking water need to be developed.
-
New paradigms for reporting water contact health risk, such as “letter grades” for public beaches, need to be developed. The present all-or-none closure decisions can misinform the public because of large spatiotemporal heterogeneity in indicator concentrations. Letter grades are one option that would effectively address the granularity issue by integrating data over a longer time period and are readily understandable.
-
Investment should be made in developing rapid analytical methods because the most commonly used warning systems involve laboratory methods that are too time consuming to achieve the best possible public health protection.
-
There are several promising source identification (i.e., microbial source tracking) techniques on the horizon that should be incorporated into monitoring systems when they have been adequately validated. Public health risk from exposure to fecally contaminated water is likely to vary depending on whether high indicator concentrations resulted from animal or human sources, and microbial source tracking tools will allow public health managers to incorporate that distinction into their decision making.
-
Models that predict future water quality conditions, based on factors such as rainfall, are potentially valuable tools for warning the public before exposure occurs, but the scientific foundation for these models has to be enhanced before they can be widely used.
NEW BIOLOGICAL MEASUREMENT OPPORTUNITIES
Although classic microbiological culture methods for detection of pathogens and indicator microorganisms have proved effective over many decades, the advent of increasingly sophisticated and powerful molecular biology techniques provides new opportunities to improve upon present indicators and pathogens by both culture and non-culture methods. Regardless of the indicator or detection method or approach used, it is essential that collection, sample processing or preprocessing, measurement, and data processing all be considered for accurate analysis of microbial water quality (i.e., not merely the measurement itself).
The collection of representative samples requires careful consideration of the objectives or purpose of sampling in the context of the need to obtain a reliable estimate of microbial exposure in a timely fashion. At present, most water quality measurement methods are single-parameter based. Ongoing research in the micro/nano-technology field, combined with efforts in array sensing and intelligent processing, should provide the tools for creating inexpensive, ubiquitous universal sensing and detection systems now and over the next several decades. This development is essential because the committee recognizes the lack of technical, infrastructure, and financial resources required to implement advanced water quality monitoring methods in many parts of the United States. The microbiological community needs to develop and implement multiparameter approaches in which many technologies and methods are integrated to provide the best possible information regarding the microbial quality of water.
The funding of methods development in the United States has been relatively poor to date for many pathogens, for new and emerging methods, and for new and innovative indicators. Development of new and improved methods has been funded substantially for only a few pathogens, specifically those targeted for regulation in drinking water. Greater and more consistent efforts should be made to support methods development for new and emerging microbial detection technologies, for many more pathogens, and for new and improved candidate indicators of waterborne pathogens.
Newer methods involving immunofluorescence techniques and nucleic acid analysis are proving their value, and novel microtechnologies are evolving rapidly, spurred partly by recent concerns about bioterrorism. However, problems associated with sample concentration, purification, and efficient (quantitative) recovery remain and will require significant effort to be resolved. One technology area that will enable significant reductions in sample preparation and separation time is the field of microfluidics and microelectromechanical systems. Thus, the introduction of molecular techniques for nucleic acid analysis is viewed by the committee as a growth opportunity for waterborne pathogen detection.
With the prospect for such an enormous amount of data to be collected from the many sensors disposed on arrays, the potentially large numbers of sensor arrays deployed for water monitoring, and the continuous data streams coming from these sensor networks, greater attention must be paid to the fields of data analysis, intelligent decision making, and archiving. There is a need for a database that compiles and serves as a clearinghouse for all microbiological methods that have been utilized and published for studying water quality. Research methods, in particular those that have great potential for becoming accepted as conventional methods, will have to be documented.
Recent developments in molecular and microbiology methods and their application to public health-related water microbiology have necessitated a new approach for the rapid assessment, standardization, and validation of such methods. It is clear that a major effort is needed for accessible methods to examine
microbial water quality for health decisions. To move new methods into the main-stream, a process is required that not only allows for standardization and validation, but also facilitates widespread acceptance and implementation. In this regard, the committee concludes that the Association of Analytical Communities (AOAC International) Peer-Verified approach or its equivalent may be the best way forward.
Based on these conclusions, the committee provides the following recommendations regarding the development of new biological measurement opportunities in the field of microbial water quality assessment:
-
A specific program on promising research methodologies for waterborne microorganisms of public health concern should be supported by EPA and other organizations concerned with microbial water quality. Such methodologies need not be microorganism specific, but should be application specific, focusing on the desirable attributes of the method.
-
Ongoing research should be supported and expanded to develop and validate rapid, ultimately inexpensive, sensitive, and robust methods for detection and measurement of all classes of waterborne pathogens and their indicators. Such expanded research should go beyond pathogenic bacteria and indicators to include improved methods for the detection of pathogenic viruses and protozoa.
-
Additional research is needed to develop improved methods for rapid sample concentration and effective, reproducible microbial recovery.
-
The adoption of new molecular techniques should be accelerated for waterborne pathogen detection. New methods undergoing validation should be tested using whole microorganisms, rather than just extracted DNA or RNA targets.
-
Research should be funded to develop approaches to the detection of infectious or viable microbes by nucleic acid detection methods.
-
Focused efforts should be made to support the development of inexpensive and rapid fieldable methods for testing microbial water quality. This will require the concurrent development of reagents, methods, and the attendant portable instruments that can survive repeated transport and use in the field.
-
Issues of sensitivity, reproducibility, and representativeness of miniaturized detection methods should be addressed as one of the most important technological challenges to analysis of waterborne pathogens and indicators.
-
EPA should reinvigorate its role with standard-setting organizations, including the American Society for Testing and Materials International (ASTM), AOAC, and the International Organization for Standardization (ISO), that focus on new and innovative methods. Regular input by professional organizations such as the American Society for Microbiology should also be encouraged.
-
EPA should support the design, development, and maintenance of a nationwide database that compiles and serves as a clearinghouse for all microbiological methods used and published for studying water quality. Guidance on ap-
-
propriate data needed for methods studies and a process for on-line iterative development of consensus methods should be included in this database.
EVALUATION OF RISK: A PHASED APPROACH TO MONITORING MICROBIAL WATER QUALITY
Many factors, including differences in the purpose for which indicator data will be used, environmental conditions, and the availability of technology to detect the microorganism(s), profoundly affect the choice of appropriate indicators and approaches to assessing microbial water quality. The selection of a suitable indicator or indicator strategy may also differ significantly depending on the water type or waterbody under consideration and the intended use of the information. Often, indicators are used to provide an early warning of potential microbial contamination, an application for which a rapid, simple, broadly applicable technique is appropriate. Indicators are used for confirmation of health risk, where resulting actions can be costly and time consuming. They are also used to identify and ameliorate the source of a microbial contamination problem. In both of the latter applications, the time frame and investment in indicators, indicator approaches, and methods must be greater than those typically used in routine monitoring.
Because a single, unique indicator or even a small set of microbial water quality indicators cannot meet this diversity of needs and applications, what is required is development and use of a “tool box” in which the indicator(s) and method(s) are matched to the requirements of a particular microbial water quality application. In this regard, the committee recommends the use of a phased, three-level monitoring framework, as illustrated in Figure ES-1, for selecting indicators and indicator approaches for waterborne pathogens. Chapter 6 describes the potential application of this framework to three typical monitoring situations in the near-term future (including the proposed Ground Water Rule and Interim Enhanced Surface Water Rule provisions) and in the long-term future at each level of investigation.
The first phase of this framework is screening or routine monitoring (Level A). The objective of this phase is early warning of a health risk or of a change from background condition that could lead to a health risk. This is the most frequent type of monitoring and is conducted routinely throughout the country. In general, the most important indicator attributes at this level are speed, low cost (logistical feasibility), broad applicability, and sensitivity.
Once screening has identified a potential problem, the second phase involves more detailed studies to confirm a health risk (Level B). The aim of such investigations is to assess the need for further management actions and/or expanded specific data gathering efforts. The confirmation phase often involves measurement of new indicators, including direct measurement of pathogens. Such studies
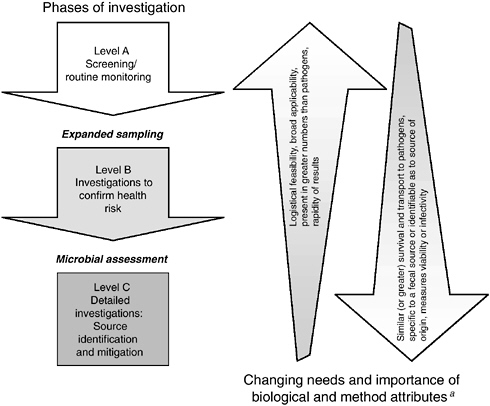
FIGURE ES-1 Recommended three-level phased monitoring framework for selection and use of indicators and indicator approaches for waterborne pathogens.
aNot all biological and method attributes summarized in Box ES-2 are included in this figure, nor are they listed in order of importance.
are not initiated on a routine basis, but would typically be undertaken when screening indicators persist at high levels without a clearly identifiable contamination source. Many of the new and emerging biological measurement methods and detection technologies described in Chapter 5 and Appendix C will be useful at this stage of investigation. Since confirmation studies focus on assessing health risk, the most important indicator biological attributes during this phase are correlation with contamination sources and transport or survival behavior similar to pathogens.
The third phase (Level C) involves studies to determine the sources of microbial contamination so that the health risk can be abated through a variety of engineering and policy solutions. However, this report focuses on the identification of sources of microbial contamination rather than their mitigation. In some cases, source identification is accomplished through expanded spatial sampling to look for gradients in indicator organisms or pathogens. Where recreational waters are
concerned, new indicator strategies based on molecular signatures are increasingly used in place of screening indicators. For these detailed investigations, essential indicator attributes include specificity to a fecal source and quantifiability. Level C studies often overlap in goal with Level B health risk confirmation studies, since identifying the source helps to identify health risk. Depending on the overlap, the ability to measure infectiousness may also be important.
The preceding discussion is focused on microbial water quality monitoring to support risk management, not the risk management actions themselves which are largely beyond the scope of this report. Appropriate risk management decisions depend not only on the results of monitoring but on the application the monitoring is designed to address. For example, when Level A monitoring identifies a potential risk in a drinking water supply that already receives complete treatment before use, management actions might be limited until Level B and/or C investigations enable the solidification of that risk assessment, at which time a significant upgrade in treatment might be in order. On the other hand, if the Level A monitoring outcomes are on water to which the public is directly exposed such as at recreational beaches, significant and immediate management action may be called for in parallel with Level B and C monitoring activities, depending on the risks implied by the Level A results. Under any circumstances, time is of the essence in all three levels of microbial water quality monitoring whenever there exists a possibility that the public may be at risk.
In general, the standardization and regulation of monitoring methodology decrease as indicator use moves through the three phases. Methods used in the screening phase are typically “standard” and can be accomplished by almost all county health department laboratories. This also holds true for many Level B studies. However, the techniques used during the latter phases may be more specialized and require the expertise of a research laboratory—this is especially true for Level C studies. The responsibility for study costs may also shift through the three phases, with parties potentially responsible for contamination sources typically more involved with the latter two levels of studies.
Microbial measurement technology is evolving rapidly and there is an opportunity to leverage these advances toward water quality needs. If sufficient investment is made in the coming decade, indicator systems will undergo a comprehensive evolution, and the correct and rapid identification of waters that are contaminated with pathogenic microorganisms will be substantially enhanced. Historically, EPA has focused much of its investment on indicators and indicator systems that are used at the screening level (A), but there is an increasing need for national leadership and guidance for the subsequent phases of microbial investigation that follow screening. Within the limited context of screening, EPA’s guidance has been of mixed value, and in this regard, the committee concludes that (1) the selection of enterococci for screening at marine recreational beaches is appropriate because enterococci have shown to have the best relationship to health risk; (2) existing and proposed monitoring requirements for surface water sources
of drinking water are irregular and are not supported by adequate research; and (3) proposed monitoring requirements for groundwater are not adequately protective for viral pathogens.
Based on these conclusions, the committee provides the following recommendations regarding the development of a phased approach to monitoring microbial water quality:
-
EPA should invest in a long-term research and development program to build a flexible tool box of indicators and methods that will serve as a resource for all three phases of investigation identified in this report.
-
This tool box should include the following: (1) the development of new indicators, particularly direct measures of pathogens that will enhance health risk confirmation and source identification; (2) the use of coliphages, as suggested by EPA’s Science Advisory Board, in conjunction with bacterial indicators as indicators of groundwater vulnerability to fecal contamination; and (3) the use of routine microbiological monitoring of surface water supplies of drinking water before as well as after treatment.
-
A significant portion of that investment should be directed toward concentration methods because existing technology is inadequate to measure pathogens of concern at low concentrations.
-
Consistent with previous related recommendations, EPA should invest in comprehensive epidemiologic studies to (1) assess the effectiveness and validity of newly developed indicators or indicator approaches for determining poor microbial water quality and (2) assess the effectiveness of the indicators or indicator approaches at preventing and reducing human disease.
-
EPA should develop a more proactive and systematic process for addressing microorganisms on the Drinking Water Contaminant Candidate List (CCL). The EPA should (1) prepare a review of published methods for each CCL microorganism and groups of related microorganisms, (2) publish those reviews on the Internet so researchers and practitioners can use them and comment on how to improve them, and (3) promote their use in special studies and monitoring efforts.
These conclusions and recommendations should not be taken as an excuse to either cling to or abandon current indicator systems until research develops new approaches. On the contrary, the committee recommends a phased approach to monitoring, as both a means to make existing indicator systems more effective, and to encourage the successive adoption of new, more promising indicator systems as they become available.
















