Chapter 1
Introduction
During the last decade, there has been growing recognition among organizations, experts, health professionals, and more recently the American public that serious, widespread, and unacceptable quality problems exist in the nation’s health care system (Blendon et al., 2001, 2002; Davis et al., 2002). Numerous studies have documented the scope of this problem and its many facets, including disparities based on race and ethnicity (Chassin, 1998; IOM, 2000, 2001, 2003a; Leatherman and McCarthy, 2002; McGlynn et al., 2003). The 1st Annual Crossing the Quality Chasm Summit was part of a series of efforts undertaken by the Institute of Medicine (IOM) to address this pervasive problem.
BACKGROUND
The IOM report To Err Is Human: Building a Safer Health System (IOM, 2000) is credited with helping to raise the public’s consciousness about the nation’s broken health care system. Its troubling bottom-line finding—that tens of thousands of Americans die each year and hundreds of thousands more suffer not because of their illnesses, but because of the care they are receiving in our nation’s hospitals—elevated the quality problem from scientific journals to the evening news and the policy arena. Both To Err Is Human and the subsequent IOM report Crossing the Quality Chasm: A New Health System for the 21st Century (IOM, 2001) emphasize that placing the blame on physicians, nurses, pharmacists, and others or asking them to just try harder will not solve this critical problem. Patients are needlessly suffering and dying as a result of a faulty system that undermines clinicians’ best efforts or does not help them succeed.
To address this urgent national issue, the Quality Chasm report challenges the country to undertake a comprehensive reform of the health care delivery system and the policy environment that shapes and
influences it. To this end, the report provides overall guidance for the systemic reforms it proposes, setting forth six quality aims for the health care system: it should be safe, effective, patient-centered, timely, efficient, and equitable (see Box 1-1).
Numerous private-sector organizations, the federal and local governments, and communities across the country have launched efforts to redesign the nation’s health care system, guided by the vision laid out in the Quality Chasm report (AHRQ, 2004; CMS, 2004; JCAHO, 2004; NCQA, 2004; The Leapfrog Group, 2004). These efforts are not always coordinated to the extent they might be for maximum leverage. And despite what they have accomplished, the system’s level of performance remains inadequate, some would say even unjust, given the resources our country expends on health care (Millenson, 2003).
The 1st Annual Crossing the Quality Chasm Summit: A Focus on Communities was an effort by the IOM to bring together and catalyze the various committed and innovative leaders across the country toward a highly targeted purpose: improving care for a selected set of clinical conditions within the Quality Chasm framework. This report serves as a summary of that 2-day event, held January 6–7, 2004. The committee that planned the summit (see Appendix A for biographical sketches) hopes this report will serve to further activate, coordinate, and integrate the quality efforts of the leaders who attended, as well as other reform-minded individuals from around the nation. While the committee is responsible for the overall quality and accuracy of the report as a record of what transpired at the summit, the views contained herein are not necessarily those of the committee. It is also hoped that this summit will be the first of many such annual events bringing together diverse leaders from across the country to further their work in implementing the vision set forth in the Quality Chasm for a 21st-century health care system.
|
Box 1-1.
SOURCE: IOM, 2001:39–40. |
THE QUALITY CHASM SUMMIT
Since Crossing the Quality Chasm was released in 2001, the IOM has issued six reports focused on implementing various facets of that report’s vision for a 21st-century health system (IOM, 2002a,b, 2003a,b,c, 2004). Each of these reports helped lay the foundation for the summit, with two of them being particularly germane: Priority Areas for National Action: Transforming Health Care Quality (IOM, 2003c) and Fostering Rapid Advances in Health Care: Learning from System Demonstrations (IOM, 2002a). (See Appendix B for a list of references and websites related to the Quality Chasm series.)
At the behest of the Agency for Healthcare Research and Quality (AHRQ), the Priority Areas report identifies 20 areas—which account for the majority of the nation’s health care burden and expenditures—to be the focus of national and local efforts to redesign health care. Five of these 20 areas were selected to be the focus of the summit: asthma, diabetes, heart failure, major depression, and pain control in advanced cancer. These five areas were chosen at the advice of many experts in the field because collectively they touch on all age groups from children to the elderly, are important to a diverse set of payers, and encompass the full spectrum of care delivery; moreover, many existing community efforts addressing these areas can be shared, supported, and disseminated. The committee anticipates that subsequent summits will focus on additional priority areas. Finally, in addition to selecting the priority areas on which to focus at the summit, the committee identified six crosscutting topics applicable to all of these areas: measurement, information and communications technology, care coordination, patient self-management support, finance, and community coalition building.
Fostering Rapid Advances, written in response to a request from Health and Human Services Secretary Thompson, lays out ideas for health system reform in the form of demonstrations that draw on many of the ideas developed in the Quality Chasm series. One of the central premises of that report is that we must support innovations at the local level, which can inform and guide comprehensive national policy. This was also a central premise behind the design of the summit, and one that informed many of its deliberations.
Goal and Objectives
At the start of the summit, Reed Tuckson, chair of the IOM organizing committee, asked participants to “envision this summit as a practical and tangible next step in the process of crossing the quality chasm.” Harvey Fineberg, president of the IOM, described the summit as “an effort to bring together agents of change who can work in their communities and with their colleagues to (re)make the health system.” Tuckson delineated what the committee hoped the summit would engender: an active dialogue—and even alliances—between local leaders involved in shaping community health systems and national leaders who influence the quality of the nation’s health care infrastructure, which he described as a “two-way street.” Tuckson expressed what the committee hoped would result from such a dialogue: articulation of on-the-ground experiences to inform and influence national-level policies, and the fostering of national action and policy directed at the local level to sustain and encourage innovators or early adopters (Berwick, 2003). Box 1-2 presents the objectives of the summit.
|
We are motivated by the reality of what is at stake…whether people shall live or whether they shall prematurely die…. And we have all been learning as we go, learning as we lay the tracks and run the trains over the chasms in our health care system. But much more progress is needed, and much more quickly.” —Reed Tuckson, committee chair |
|
Box 1-2.
|
The summit participants included approximately 45 leaders from 15 communities across the country, selected from a pool of 90 communities identified as innovative in improving quality of care in at least one of the five targeted clinical areas (see Appendix C for a description of the communities and Appendix D for selection criteria). The 15 communities selected (see Box 1-3) are quite diverse, and while largely anchored in a geographic region, they are not solely defined by geography but rather by a “community of interest.” For example, they include coalitions that encompass all of the stakeholders in a local market and others that comprise a more selective group; a state-level initiative involving providers, schools, and others focused almost entirely on patient and clinician education; and an integrated delivery system that has established links to community resources, including the public health department and community health centers.
Participants also included leaders from national organizations referred to as “national champions” (see Box 1-4), which through their influence could expedite progress at the local level.2 These national leaders and other experts who attended the summit (see Appendix E) represented a broad range of organizations, including health plans, hospitals, physician groups, federal agencies, employer coalitions, consumer advocacy groups, quality groups, and disease-specific organizations, among others.
The participants worked together to identify key strategies for enhancing care in the five clinical areas that were the focus of the summit. These strategies had many common themes, the most prevalent being focused on information and communications technology, finance, and measurement. The strategies also addressed comorbidities or, as one summit participant, Bruce Bagley from the American Academy of Family Physicians, noted, “the necessity of taking care of the patient as a whole patient and not as a segment of disease.”
|
Box 1-3.
|
|
Box 1-4.
|
John Lumpkin of The Robert Wood Johnson Foundation, which funded the summit, characterized the larger environment in which the event was taking place in the spirit of Dickens’ A Tale of Two Cities—as the best and worst of times. Among his characterization of what was the worst, he cited a recent New England Journal of Medicine article revealing that Americans receive only about 50 percent of the care that the evidence suggests they should get (McGlynn et al., 2003). He characterized the best as including the many more tools the field has to improve quality and the varied, committed, and talented stakeholders represented by the summit participants, who are developing community-based approaches to improving quality that hold promise for making a real difference.
Patients at the Center, with Community as a Focus
Reed Tuckson opened the 2-day summit by emphasizing that the patient must be at the center of all reform efforts. In this vein, he introduced the consumer panel, which began with a patient’s story, relayed by a family member who is also a nurse. Martha Whitecotton told of her son’s struggle with major depression, highlighting the gaps and dysfunctions that prevented him from receiving the best possible care. She touched on themes that are endemic to care not just for depression, but for all chronic conditions and across the entire health care system. In particular, Whitecotton stated, drawing from the Quality Chasm report, “patients’ experiences should be the fundamental source of the definition of quality…[but] we have a long way to go.” Patient-centered care has different meanings for each patient. For some patients it may mean care only for themselves; for others it includes both patients and their families; while for others it comprises non–professionally trained caregivers who serve as a safety net. When the “patient” is referred to in this report, the term implicitly represents this range of circumstances.
Don Berwick, president of the Institute for Healthcare Improvement and the summit’s keynote speaker, echoed the notion that the patient must serve as the compass for the system. He asked the participants to develop a “fundamentally new view of the patient, not as the object of our care, not as a guest in our house, but as the host of our work and as the person who ultimately has the say in what we do or do not do.” Berwick further challenged the group by saying that “we must learn to honor individual choices, respecting the variability in need, the variability in ethnicity and diversity, and the need for structures [that respect] the habits and spirits of the people we serve.”
Henry Gaines of the Greater Flint Health Coalition in Genesee County, Michigan, provided an example of how one community put a program in place to change the culture for the delivery of maternal and child health care services. Friendly Access—developed to increase access, satisfaction, and utilization—is based in part on the well-regarded customer service model developed by the Disney Institute. Gaines described the model as making it possible to better understand the wants, needs, and emotions of the patients being served, and to translate those needs into policies and procedures, while motivating clinicians to provide care that exceeds patient expectations.
The Community Focus
With the patient as the central guiding force, the Quality Chasm report calls for systemic, simultaneous changes at four levels of the health system—the patient/family and other key non–professionally trained caregivers who may be involved with the patient; small-practice settings or microsystems; health care organizations; and the broader environment (e.g., payment, education, regulatory). These levels are nested within each other and interact in many complex ways (Berwick, 2002).
As Don Berwick noted, the community focus for the summit was particularly exciting because
it encompasses each of these four levels, including the environment. Thus, he said, “You have a chance to actually raise issues which normally can’t be raised because there aren’t enough payers in the room.” A community focus allows for a multiple-stakeholder approach to the complex set of issues posed by comprehensive redesign of the American health care system. John Lumpkin concurred, “If we’re going to fix this system, we have to focus on quality. And if we’re going to fix our system, communities are where we have to do the work.”
|
“Each of the communities that are participating is a building block. Each is an experimental center. Each is a place of innovation. And if we take advantage of our mutual learning in the course of this day to renew our own sense of possibility and direction, then the objectives of our meeting will have been accomplished.” —Harvey Fineberg, President, IOM |
Working at the community level also provides an opportunity for greater interaction between the personal health system and the public or population-based health system. Given that health care outcomes are determined by both health- and non-health-related factors—with behavioral patterns, social circumstances, environmental exposures and genetics playing substantial roles (McGinnis et al., 2002)—this interaction can maximize health for all by allowing individuals to obtain needed care and support for addressing broader health-related behaviors. This benefit is particularly relevant for children. For example, an approach to diabetes care that spans the personal and population-based systems might include individualized diabetic care, as well as programs in local schools and worksites designed to promote changes in diet and exercise, with the goal of reducing obesity and better managing or preventing the disease. Many summit participants echoed the need for such integration and for inclusion of a focus on primary prevention. Box 1-5 describes the Steps to a HealthierUS initiative, which is taking such an approach.
|
Box 1-5. The Department of Health and Human Services (DHHS) is currently supporting 12 communities in their efforts to promote better health and prevent disease through the newly launched Steps to a HealthierUS program. These DHHS awards, which totaled $13.7 million in fiscal year 2003, are focused on helping communities reduce the burden associated with diabetes, obesity, and asthma while addressing three related risk factors—physical inactivity, poor nutrition, and tobacco use. The overall goal of the effort is to help Americans live longer, better, and healthier lives. The grants are being used by leaders in small and large cities, rural communities, and one tribal consortium to implement community action plans that target racial and ethnic minorities, low-income populations, uninsured and underinsured persons, and others at high risk. Funded programs include those that focus on health care organizations, schools, workplaces, and other organizations, and are tailored to meet the needs of the particular community. In 2004, DHHS expects to award grants to additional communities and to continue funding existing efforts (Steps to a HealthierUS Initiative, 2004). |
|
“In the case of asthma, it seems to me that if you are not dealing with the environmental determinants of health, you are then involved in a very Sisyphean task of rolling and rolling the rock up the hill, and then having it roll right back down on top of you.” —Shoshanna Sofaer, summit participant |
Finally, there is value in working across communities as leaders share information about what does and does not work in their local health systems. Communities that collaborate may be able to learn from each other about transferable approaches and share strategies for delivering high-quality care.
Sustaining Community Innovators
Throughout the course of the summit, IOM committee members, speakers, participants, and others offered ideas about the best ways to catalyze and sustain systemic reform at the community level. National champions offered specific kinds of support (see Chapter 9). In addition, two of the five condition-specific plans that emerged from the summit deliberations included strategies for educating and activating communities. These strategies ranged from holding community-wide dialogues about issues associated with heart failure care, to supporting asthma coalitions, to developing innovative finance solutions that encompass both traditional and nontraditional methods of paying for services and span the personal and public health systems.
Don Berwick noted that communities must begin with a shared vision for reform that he described as a “change in purpose,” and must focus the system on the experience of the people that it serves. He stated further that there must be an acceptance of responsibility that is beyond guilt, beyond blame, and beyond denial and is coupled with intense commitment. He noted that without this commitment, failure is more likely than success given the myths, belief systems, and habits, as well as system fragmentation, that undermine efforts at transformation.
Advance Work with the Communities and National Champions
To make the summit as action-oriented as possible, the IOM organizing committee worked in advance with leaders from the selected communities to summarize what they had accomplished and identify gaps in their current efforts. Committee members also contacted key national champions to inform them about the summit’s objectives and ask them to consider in advance what they might commit to at the summit to further the vision of the Quality Chasm at both the community and national levels. Armed with the results of this substantial advance work, summit participants were able to minimize the time spent reviewing past accomplishments and focus more on shared learning and cooperative strategizing about future opportunities for improving care.
The community representatives shared the results of their considerable amount of advance work in one of five groups focused on the priority conditions cited above. Their efforts included the completion of two matrices, led by a clinical expert on the IOM committee. Sample matrices may be found in Appendix F. These two tools afforded the community leaders an evidence-based approach to self-evaluation and the chance to learn from others engaged in improving care for the same condition.
The first matrix aligned each component of the process of “ideal” care against the six aims of high-quality health care set forth in the Quality Chasm report and outlined above. The community representatives ranked where they thought they stood with regard to consistently providing the recommended care, and these scores were used to identify the areas most in need of improvement. The second matrix was adapted from the Chronic Care Model (CCM),
developed by staff at the Improving Chronic Illness Care program of The Robert Wood Johnson Foundation (Improving Chronic Illness Care, 2004; Wagner, 2002). The CCM (see Figure 1-1) provides a scientific framework for organizing and delivering care at the level of the small-practice setting or microsystem. Under this model, patients are expected to participate actively in their care and play an integral role in both directing and managing their chronic condition. They are supported in their self-management efforts by their families and other key non–professionally trained caregivers who may be involved with the patient, as well as a proactive and well-prepared team of clinicians who provide regular follow-up.
The centerpiece of the CCM is facilitation of “productive interactions” between patients and their providers. To allow for greater specificity in the participants’ advance work with respect to what infrastructure had been developed within their communities to support such interactions, the components of these interactions were explicitly compartmentalized. Team members from the 15 communities assessed what system elements they had in place to support evidence-based care for the chronic condition they were addressing (asthma, diabetes, depression, heart failure, or pain control in advanced cancer) consistent with the five elements of the CCM—clinical information systems, delivery system design, decision support, self-management support, and community resources and policies. This approach also provided a way to consider the interface between the health system and community resources so that, in the words of Reed Tuckson, public health is considered “not a competitive but a synergistic activity.”
During the summit, Don Berwick described such evidence-based approaches to quality improvement as the way to be optimistic in the face of all that is wrong with our current system. He noted, “The optimism we have is science. It’s the scientific understanding of what makes quality happen in the first place. The qualities
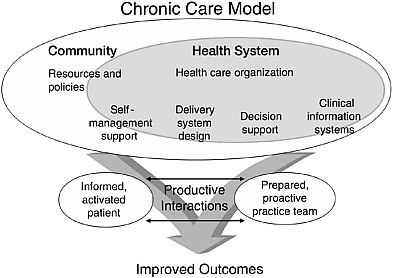
Figure 1-1 Chronic Care Model
SOURCE: Reprinted with permission from Effective Clinical Practice. Copyright 1998 by Effective Clinical Practice. (Wagner, 1998)
we care about…these are qualities of design.” He further challenged the summit participants: “Every system is perfectly designed to achieve the results it gets…. If you don’t like your results, change your system.”
Intensive planning by IOM committee members and input from the sponsor, liaisons, and others greatly contributed to the smooth execution and overall success of the summit. Appendix G details this extensive preparation.
The morning of the first day of the summit set the context for the event. It shone a spotlight on our broken health system from the patient’s perspective, highlighted ways in which communities are working to overhaul the dysfunctional design of local health systems, and challenged participants—both local and national—to reach further and stretch higher in their efforts to remake American health care.
The summit welcome and introductions were shared by Reed Tuckson, IOM committee chair and senior vice president, UnitedHealth Group; Harvey Fineberg, president of the IOM; and John Lumpkin, senior vice president, The Robert Wood Johnson Foundation. (See Appendix H for the full summit agenda.) The consumer panel was chaired by Allen Daniels, an IOM committee member and CEO of Alliance Behavioral Care, and included Martha Whitecotton, R.N., Carolinas Medical Center; William Bruning, J.D., Mid-America Coalition on Health Care Community Initiative on Depression; Henry Gaines, Greater Flint Health Coalition; and Jay Portnoy, M.D., Children’s Mercy Hospital/Kansas City Asthma Coalition. The keynote speaker was Don Berwick, President of the Institute for Healthcare Improvement.
In the afternoon, summit participants attended strategy sessions addressing the six crosscutting topics. These sessions were intended to further prepare participants in the relevance of particular interventions to their ongoing quality improvement efforts so that the subsequent working groups focused on the priority areas could be maximally productive. For those with experience in such interventions, these sessions afforded an opportunity to share what they have learned with a larger group. The sessions were facilitated by subject experts and included short presentations from community representatives whose programs had focused on the particular interventions. The sessions and cofacilitators were as follows:
-
Measurement, with facilitators Judith Hibbard, University of Oregon, and Arnold Milstein, Pacific Business Group on Health
-
Information and Communications Technology, with facilitators David Kibbe, American Academy of Family Physicians, and David Brailer, Health Technology Center
-
Care Coordination, with facilitators Gerard Anderson, the Johns Hopkins Bloomberg School of Public Health, and Christine Cassel, American Board of Internal Medicine
-
Patient Self-Management, with facilitators Kate Lorig, Stanford University, and Russell Glasgow, Kaiser Permanente Colorado
-
Finance, with facilitators Peter Lee, Pacific Business Group on Health, and Steve Udvarhelyi, Independence Blue Cross
-
Community Coalition Building, with facilitators Shoshanna Sofaer, Baruch College, and David Stevens, Agency for Healthcare Research and Quality
The working groups addressing the priority areas met at the end of day one of the summit and for the first half of day two. The groups—which included community representatives, national champions, and other experts––used facilitation tools (see Appendix I) to develop plans incorporating key strategies at both the local and national levels for improving care for the targeted conditions. These plans describe who might spearhead such efforts, include time lines for implementation, and in most cases call
for measures to gauge the effectiveness of the proposed strategies. These plans were presented at the plenary session, where initial feedback was received from summit participants. A diverse reactor panel—including moderator Bruce Bradley, an IOM committee member and Director of Health Plan Strategy and Policy, General Motors Corporation; Al Charbonneau, Rochester Health Commission; Helen Darling, National Business Group on Health; Sylvia Drew Ivie, The Help Everyone Clinic; and George J. Isham, HealthPartners, Inc.—provided further reflection on the plans and a candid reality check.
The final session of the summit, chaired by Reed Tuckson and described by many as a revival session, focused on commitments articulated by national champions for furthering the vision of the Quality Chasm report. These commitments targeted both the community and national levels, and included many that were announced for the first time at the summit, as well as others aimed at strengthening existing relevant efforts.
SCOPE AND ORGANIZATION OF THE REPORT
This report provides a synthesis of the outcomes of the summit, and is not intended to contain an exhaustive review of the literature for all of the topics discussed. Its content reflects the committee’s commitment to carrying out its charge, which was to plan and execute a national summit focused on the vision of the Quality Chasm report for improving quality of care for a targeted set of conditions at both the community and national levels. A number of additional issues beyond this charge were discussed by the committee during its deliberations and by some summit participants, but are not captured in this follow-up report. Among others, these include how to enhance public health infrastructure and integrate it effectively into the personal health care system; how clinical education must be transformed so that health care professionals are best prepared to practice in a transformed system; and how clinicians, particularly physicians, can be engaged in quality improvement efforts.
In summarizing the summit outcomes, this report offers a vision, emerging from the summit deliberations, for how care for a targeted set of conditions can be improved by leveraging and integrating both community- and national-level strategies focused on key crosscutting interventions:
-
Chapters 2 through 7 focus on the crosscutting strategies for improving care identified in the Quality Chasm report and by community leaders at the summit. These chapters highlight barriers and related solutions, based on discussions during the cross-cutting sessions and among the condition-specific working groups. They include examples from the participating communities illustrating how particular interventions can enhance care for one or more conditions.
-
Chapter 8 provides a synopsis of the key strategies for change at the local and national levels proposed by the condition-specific working groups.
-
Chapter 9 delineates next steps, calling for action on the part of both national and local leadership. It identifies the major commitments of the national champions and describes how they dovetail with the key strategies identified both in the cross-cutting sessions and by the five condition-specific working groups. It also includes comments from the reactor panel and summit participants.
-
A series of appendices provides key summit documents, including the agenda, participant list, descriptions of participating communities, and other related materials.
REFERENCES
AHRQ (Agency for Healthcare Research and Quality). 2004. Quality Research for Quality Healthcare. [Online]. Available: http://www.ahrq.gov/ [accessed April 5, 2004].
Berwick DM. 2002. A User’s Guide for the IOM’s Quality Chasm Report. Health Affairs (Millwood, VA) 21(3):80–90.
Berwick DM. 2003. Disseminating innovations in health care. The Journal of the American Medical Association 289(15):1969–1975.
Blendon RJ, DesRoches CM, Brodie M, Benson JM, Rosen AB, Schneider E, Altman DE, Zapert K, Herrmann MJ, Steffenson AE. 2002. Views of practicing physicians and the public on medical errors. New England Journal of Medicine 347 (24):1933–1940.
Blendon RJ, Schoen C, Donelan K, Osborn R, DesRoches CM, Scoles K, Davis K, Binns K, Zapert K. 2001. Physicians’ views on quality of care: A five-country comparison. Health Affairs (Millwood, VA) 20(3):233–243.
Chassin MR. 1998. Is health care ready for six sigma quality? Milbank Quarterly 76(4):510, 565–591.
CMMS (Centers for Medicare and Medicaid Services). 2004. Centers for Medicare and Medicaid Services. [Online]. Available: http://www.cms.hhs.gov/ [accessed April 5, 2004].
Davis K, Schoenbaum SC, Collins KS, Tenney K, Hughes DL, Audet AJ. 2002. Room for Improvement: Patients Report on the Quality of Their Health Care. Report 534. New York, NY: The Commonwealth Fund.
Improving Chronic Illness Care. 2004. ICIC: Fostering Improvement: Learning Session #1. [Online]. Available: http://www.improvingchroniccare.org/improvement/ls1.html#lstools8 [accessed April 6, 2004].
IOM (Institute of Medicine). 2000. To Err Is Human: Building a Safer Health System. Kohn LT, Corrigan JM, Donaldson MS, eds. Washington, DC: National Academy Press.
IOM. 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
IOM. 2002a. Fostering Rapid Advances in Health Care: Learning from System Demonstrations. Corrigan JM, Greiner AC, Erickson SM, eds. Washington, DC: National Academy Press.
IOM. 2002b. Leadership by Example: Coordinating Government Roles in Improving Health Care Quality . Corrigan JM, Eden J, Smith BM, eds. Washington, DC: National Academy Press.
IOM. 2003a. Patient Safety: Achieving a New Standard for Care. Aspden P, Corrigan JM, Wolcott J, Erickson SM, eds. Washington, DC: National Academy Press.
IOM. 2003b. Health Professions Education: A Bridge to Quality. Greiner AC, Knebel E, eds. Washington, DC: National Academy Press.
IOM. 2003c. Priority Areas for National Action: Transforming Health Care Quality. Adams K, Corrigan JM, eds. Washington, DC: National Academy Press.
IOM. 2004. Keeping Patients Safe: Transforming the Work Environment of Nurses. Page A, ed. Washington, DC: National Academy Press.
JCAHO (Joint Commission on Accreditation of Healthcare Organizations). 2004. JCAHO Welcome Page. [Online]. Available: http://www.jcaho.org/ [accessed April 5, 2004].
Leatherman S, McCarthy D. 2002. Quality of Health Care in the United States: A Chartbook. New York, NY: The Commonwealth Fund.
McGinnis MJ, Williams-Russo P, Knickman JR. 2002. The case for more active policy attention to health promotion: To succeed, we need leadership that informs and motivates, economic incentives that encourage change, and science that moves the frontiers. Health Affairs (Millwood, VA) 21(2):78–93.
McGlynn EA, Asch SM, Adams J, Keesey J, Hicks J, DeCristofaro A, Kerr EA. 2003. The quality of health care delivered to adults in the United States. New England Journal of Medicine 348 (26):2635–2645.
Millenson ML. 2003. The silence. Health Affairs (Millwood, VA) 22(2):103–112.
NCQA (National Committee for Quality Assurance). 2004. NCQA: National Committee for Quality Assurance. [Online]. Available: http://www.ncqa.org/index.asp [accessed April 5, 2004].
Steps to a HealthierUS Initiative. 2004. Grantees, Steps to a HealthierUS Initiative. [Online]. Available: http://www.healthierus.gov/steps/grantees.html [accessed March 24, 2004].
The Leapfrog Group. 2004. The Leapfrog Group. [Online]. Available: http://www.leapfroggroup.org [accessed April 5, 2004].
Wagner EH. 1998. Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice 1(1):2–4.
Wagner EH. 2002. IOM Health Professions Education Summit. Powerpoint Presentation. Washington, DC:














