4
Lighting: Research and Findings
Mark Rea
Lighting is often forgotten in discussions of indoor environmental quality and building occupants’ health, yet it has been shown to affect both health and productivity. There are two biological systems by which light can affect human performance and health: the visual and the circadian (see Figure 4.1). The circadian system involves biological rhythms that repeat at approximate 24-hour intervals.
To understand the impact of light on the human condition, one has to break it down into its components: intensity, spectrum, distribution, timing (when it is received), and duration. One then needs to understand where and how these light components are processed in the brain.
We understand the visual system well in terms of the effects of light on both appearance (what things look like) and visual performance (how well visual information is processed). The visual system is a very quick remote-sensing mechanism that alerts us to changes in the environment and enables us to identify friend or foe.
The circadian system is one that has been long known in plants and animals. However, it is only in the past 20 years that we have begun to take a serious look at the impact that light has on the daily patterns or daily rhythms of people, with the sleep/wake cycle being the most notable. Unlike the visual system, the circadian system is slow and has a very different tuning curve for electromagnetic radiation, and its sensitivity to light intensity is dependent on the time of day.
Humans are inherently a daytime species, born to be awake during the day and asleep at night. Eighty percent of the working population in North America works during the day, while 20 percent works on night shifts.
For a large majority of the population working in buildings, lighting for vision during the day is adequate. In part, this is because people have very flexible visual systems. If we examine the range of light levels that illuminate buildings, we see that of the 16 log unit range in sensitivity only 4 log units are used with electric lighting (see Figure 4.2).
Out in the real world, people can often adjust to their environments. Consider, for instance, that most of us adjust our computer displays more for how we want people to meet us when they enter our office than for lighting conditions. We may, for example, have our monitor up against a bright window or have it turned so that the window image is actually reflecting off the screen.
Figure 4.3 shows how people adjust their posture in response to the available light. The farther they are from the light, the closer they hold the reading materials to maintain a constant ability to read. Experiments in the laboratory similarly show that under dim conditions people will adjust the eye-to-task distance, that is, move closer to the task. The visual system combined with a flexible body provides us with the ability to adapt to the lighting environment.
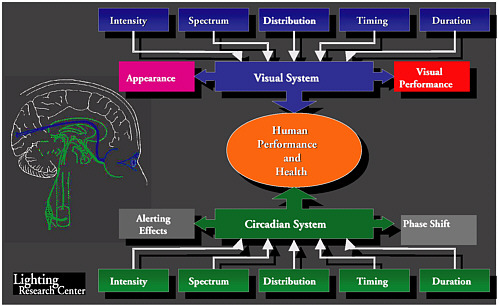
FIGURE 4.1 Light as it affects human performance and health through the visual and circadian systems. SOURCE: Produced by Lighting Research Center.
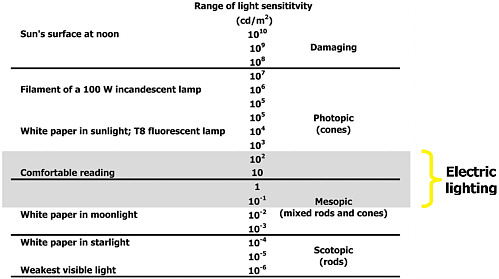

FIGURE 4.2 Range of human sensitivity to light together with the range of luminances provided by electric lighting.
SOURCE: Robert Sekuler and Randolph Blake. Perception. New York, McGraw-Hill, third edition, 1994.
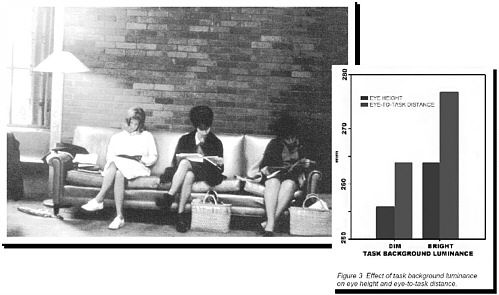
FIGURE 4.3 Lighting levels and their impact on posture. SOURCE: Photo by Murray Milne, University of California, Los Angeles. Provided by Hayden McKay, Hayden McKay Lighting Design, New York, N.Y. Chart reprinted courtesy of the Illuminating Engineering Society of North America, Journal of the Illuminating Engineering Society 15(1):235.
There is an important caveat to the statement that lighting is adequate for the majority of the working population. It is related to the fact that the second leading cause of death on the job in the United States is homicide. Research has shown that bright exterior lighting is associated with a significant reduction in the risk of being killed on the job, which is certainly a health-related impact. So we should think about more than just office workers when discussing lighting and health. There are other lighting applications to consider, including security and egress. Stair lighting is one example; trips and falls resulting from inadequate lighting result in many injuries in the workplace.
Normal aging is another factor to consider in studying lighting, indoor environmental quality, and workers’ health and productivity. Over the past 100 years there has been a significant improvement in the life expectancy of people, from 47.3 years for those born in 1900 to 77.2 years for those born in 2003, depending on race and gender. Health care and life expectancy are improving, and the number of older people in the workforce is increasing.
Normal aging involves optical changes before age 65 and neural changes after age 65. One optical change, presbyopia, is the inability to focus on near objects. People over age 45 usually show symptoms of presbyopia. Many use optical aids to focus near objects. This situation implies that without eyeglasses their ability to lean closer to tasks is compromised, so good lighting becomes more important.
The second optical change is loss of retinal illuminance and reduced retinal contrast. As a person ages, the crystalline lens of the eyes yellow and have less optical fidelity. Figure 4.4 simulates the difference in visual clarity of a 30-year-old person and someone who is 75. To the older person, a medicine cabinet, room, or other objects would appear darker and hazier.
After age 65, vision deteriorates as a result of neural as opposed to optical changes. Some people develop photophobia, a painful sensitivity to strong light. For others neurological changes result in a reduced visual field (see Figure 4.5).
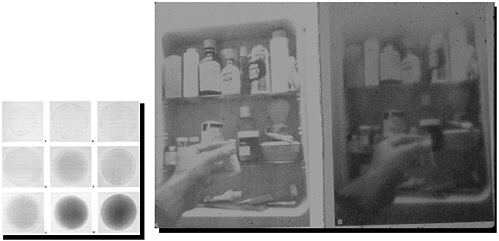
FIGURE 4.4 Simulated age-related loss of retinal illuminance and reduced retinal contrast together with age-related changes in the crystalline lens. SOURCE: Reprinted and adapted with permission of Leon A. Pastalan. Classification system for yellowing of the lens. © Lighthouse International.
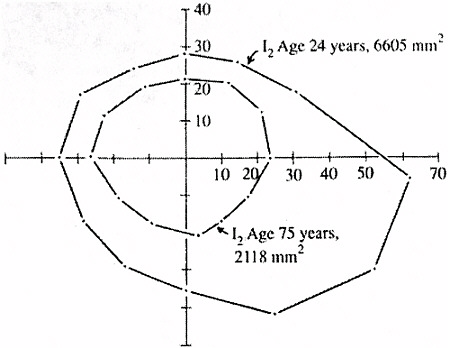
FIGURE 4.5 Aging and central visual field area. SOURCE: Reprinted with permission from D.T. Williams, 1983, Aging and central visual field area, American Journal of Optometry and Physiological Optics 60:888-891. American Academy of Optometry.
Loss of peripheral vision affects seniors both indoors and in office environments, where a slight ramp or an uneven surface can result in trips and falls. Senior drivers are also more likely to have an accident at an intersection because they cannot readily detect objects in their peripheral field of vision. More serious age-related diseases of the eyes include glaucoma, macular degeneration, and diabetic retinopathy.
Circadian rhythms comprise a new area of study that is profound in its implications for building practices. Light is the primary synchronizer of circadian rhythms. We actually have a circadian pattern that is about 24 hours and 20 minutes. Every morning when we awake, we reset our biological clock through light. This system requires a very high sustained light level to tell the body it is really daytime. If someone works in a mine, for example, that person’s body will go out of synchrony with daily solar light and dark phases.
Current office lighting levels tend to be at the low end with regard to regulation of circadian rhythms. During the winter months, people sitting in an interior office are potentially in biological darkness all day. Those sitting next to a window, in contrast, probably receive enough light to activate their circadian system. We are not necessarily looking at a crisis, but we are observing some interesting implications.
We do know that circadian regulation in some populations is disrupted by inadequate light. One of the best-documented symptoms is seasonal affective disorder. Seasonal depression (also known as winter depression) is prevalent in northern latitudes, and the medical profession recognizes bright lights as a treatment.
Perhaps the impact of low light levels in buildings can have long-term effects that are not so obvious. Older people, for example, commonly have what is called phase advance syndrome. They tend to go to bed at 8:00 p.m. and rise at 4:00 a.m., roaming around before anyone else is awake. Bright light exposure in the evening will delay their sleep, allowing them to sleep later in the morning and rise at a more appropriate time.
On the other hand, about 15 to 20 percent of young adults miss significant portions of school because they do not go to sleep until 2:00 a.m. and consequently cannot get up in the morning. This condition is known as phase delay syndrome. Providing bright light in the morning and limiting light exposure in the evening can get these young adults back to more normal sleep/wake schedules.
People with Alzheimer’s disease are just as likely to be asleep as they are to be awake any time during the day or night. We have used the knowledge gained about spectral sensitivity to the circadian system to provide Alzheimer’s sufferers with blue light treatment early in the evening. After blue light treatment, they not only slept longer but also consolidated their sleep and were more likely to be asleep at night and awake during the day.
Lighting does matter. However, it is usually at the extremes of the population (night-shift workers, seniors, and young people) where lighting demonstrably affects the well-being and performance of workers. We do not yet understand how important light regulation is for the well-being of the majority of the population, but we are beginning to find health-related problems in segments of the population that may be harbingers to problems in the general population.
ABOUT THE PRESENTER
Mark Rea, Ph.D., is a professor of Cognitive Science at Rensselaer Polytechnic Institute’s (RPI) Lighting Research Center (http://www.lrc.rpi.edu). His research interests include vision, lighting engineering, and human factors. Prior to joining the RPI faculty, Dr. Rea was a senior research officer and manager of the Indoor Environment Program of the Building Performance Section at the National Research Council of Canada. He is a fellow of the Society of Light and Lighting of the United Kingdom, and is a member of the Commission Internationale de L’Eclairage, the Illuminating Society of North America, the Optical Society of America, and the American Association for the Advancement of Science. During his career Dr. Rea has received the Illuminating Engineering Society of North America’s Medal and the William H. Wiley Distinguished Faculty Award from RPI. He holds a Master of Science and a Ph.D. in biophysics from Ohio State University.





