2
Pillar One: Improving Surveillance and Response
Successful disease control measures are based on effective integration of human and animal disease surveillance and response programs. Examples of essential routine surveillance and response activities are: (1) identifying and tracing contaminated food and issuing warnings and recalls; (2) diagnosing prevalent influenza virus strains to guide vaccine development and use; (3) monitoring the blood supply to ensure its safety; and (4) tracking the spread of antibiotic-resistant infections and instituting controls as necessary. To heighten the likelihood of containing infectious diseases through effective surveillance and response, whether the diseases are common infections or newly emerging threats, a nation needs support from all levels of government and cooperation among health care and veterinary networks throughout the country (CDC, 1998a, 1998b).
In brief, surveillance begins with systematic collection, analysis, and dissemination of data related to the health of the population, including animal diseases that could be transmitted to people. Important data include information on clinical diagnoses, laboratory-based test results, specific syndromes, health-related behaviors, and those related to the use of products to combat diseases such as the sales of antimicrobial drugs. These data provide the basis for detecting outbreaks, characterizing disease transmission patterns, developing prevention and control alternatives, and conducting evaluations.
Enhancing surveillance capabilities to provide better, timelier, and more informative data is a never-ending process. Many countries are currently concentrating on: (1) integrating public health information banks and surveillance data systems, and more effectively utilizing data available in the broader health community; (2) applying molecular fingerprinting, ranging from the identification of
strains of E. coli and Salmonella to tracking the spread of HIV/AIDS and brucellosis, for example; and (3) identifying the presence of those microbes and viruses of particular bioterrorism concern (CDC, 1998a, 1998b).
Responding to warning signals from surveillance activities is also essential for protecting the population. The response may be limited to confirming initial reports and then ensuring that authorities are taking appropriate control measures, or it may entail a broad international response to threats that cross national borders. A response may require special localized surveillance and control efforts or wider-scale efforts as the likelihood of disease proliferation becomes clear. Additionally, it may depend on a country’s surge capacity to quickly deploy resources without interrupting routine activities. Finally, surveillance responses will probably generate considerable scientific information that may be useful for addressing similar problems in the future.
IMPORTANCE OF SURVEILLANCE AND RESPONSE IN RUSSIA
The Russian Ministry of Health and Social Development devotes much of its attention to socially significant diseases (see Appendix E). It receives frequent reminders of their importance, such as the nationwide outbreak of diphtheria in 1993-1996; the emergence of polio in Chechnya in 1995; the surging incidence nationwide of tuberculosis, syphilis, and hepatitis B; and even continuing malaria infections in some localities. At the top of the list of the newer diseases of concern are HIV, followed by hemorrhagic fever, Lyme disease, and 25 other potentially dangerous infections (Onishchenko, 2002). These realities force health authorities to improve preventive measures to combat common infectious diseases, generally within the framework of national immunization strategies and policies (see Appendix I).
The Russian government has not hesitated to respond promptly and vigorously, within the constraints of available specialists and funds, to disease threats once they have been identified. As an example of Russian capabilities, the government response to the severe acute respiratory syndrome (SARS) outbreak in China was impressive. Attendants on Russian passenger trains leaving China and personnel at Russia’s international airports were important components of this response. These personnel, who had been routinely trained to cope with sick travelers, were quickly given supplemental information to enable them to identify travelers who might be infected with SARS. Those travelers then had immediate access to public health personnel for professional health examinations when needed. Despite the long Russia-China border, SARS did not infect the Russian population with the possible exception of one questionable case in the Far East.
The government is also organized to respond to an incident of bioterrorism, particularly in Moscow, which is considered by many Russians the most likely target of such an attack. Special medical manuals have been prepared. Special organizations have been designated to provide the needed health-related tech-
nical support to the Ministry for Emergency Situations, which coordinates all responses in cooperation with city authorities. Emergency assignments have been made to units of the Ministry of Health and Social Development. However, Russian officials readily admit that in recent years there has been a considerable degradation in their ability to detect or respond to disease outbreaks, including bioterrorism incidents outside Moscow and St. Petersburg.1
Unfortunately, in Russia the initial detection and assessment of a naturally occurring or human induced outbreak is hampered by several factors. They include inadequate diagnostic capabilities, outmoded communication networks across vast geographic areas that might be part of infected zones, and the reluctance of ill people to turn to a Russian health system that had previously provided services free of charge but now may require payment for services of adequate quality. Any degradation of capabilities is of concern to the Ministry of Health and Social Development and related agencies. Therefore efforts are under way to correct deficiencies that have arisen since 1991.
The Russian Ministry of Agriculture has long been concerned about the prevalence of common diseases, such as foot-and-mouth disease, rabies, brucellosis, and wheat rust. It devotes considerable effort to monitoring for these and other diseases. More than 200 research institutes associated with the ministry and the Academy of Agricultural Sciences are located throughout the country (see Appendix J). Many have a role in monitoring and reporting animal and plant diseases. The ministry and the academy justify the need for the large number of research institutes by pointing to the country’s size and its many different agroecological regions and diseases. The Veterinary Service of the Ministry of Agriculture also monitors the condition of a limited number of animals, particularly if there are reports of outbreaks from farmers or other sources. Finally, the anti-plague institutes, discussed later in this chapter, provide a front line for surveillance. Specialists at these institutes routinely collect and analyze rodents and other potential reservoirs of animal and human diseases.
Much like the decline in capabilities in human health surveillance and response, Russia’s capability to detect and diagnose agricultural problems has eroded in recent years. The incentives to expend resources on animal or plant protection are not great, and the lack of priority they command obviously has implications for human health.
Another area of concern to public health and agricultural officials is the integration of the systems for detecting food-borne diseases with food monitoring systems. A useful step suggested by a Western expert would be to use Salmonella
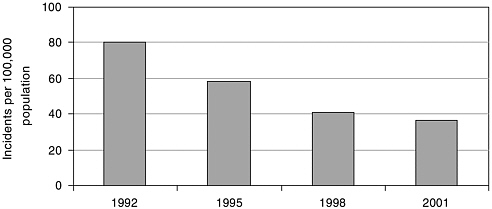
FIGURE 2.1 Salmonella incidence in Russia, selected years, 1992-2001. SOURCE: Onishchenko, 2002:26.
as a case study.2 Through applying lessons learned from investigations of outbreaks of Salmonella, the two types of monitoring systems might be brought closer together. Since the World Health Organization (WHO) has established a collaborating center on Salmonella at the Central Research Institute of Epidemiology in Moscow, such an initiative would probably be easy to implement. As indicated in Figure 2.1, Salmonella outbreaks are on the decline in Russia, but they remain a public health concern and provide a good topic for detailed examination.
SURVEILLANCE AND MONITORING SYSTEMS
System of State Sanitary Epidemiological Surveillance Centers (SSESCs)
A system for combating and controlling infectious human diseases, unique in both size and standardization of approach, has been functioning in Russia for many years. The State Sanitary Epidemiological Service has 89 regional centers and 1,700 district-level centers. Overall, the system covers the entire country with about 2,300 centers, and employs over 6,000 medical doctors and many other specialists. In addition to carrying out critical surveillance and response functions, these centers are important in developing research priorities such as the following recent examples (Onishchenko et al., 2003):
-
new rapid pathogen detection diagnostics and tools based on cutting-edge research in the field of biotechnology and nanotechnology
-
next generation vaccines and live recombinant vaccines based on viral vectors developed through genetic engineering methods
-
new chemical substances and formulations for disinfectant agents
Unfortunately, since the disintegration of the Soviet Union, the system has lost some of its capabilities, despite the ever-increasing variety of infectious diseases in Russia. The sanitary epidemiological center that serves the city of Moscow has state-of-the-art capabilities to identify, diagnose, report, and analyze data. However, many SSESCs in the outlying areas of the country have had difficulty paying employees, let alone replacing outmoded analytical equipment and installing modern communications equipment. Although the health sector receives generally favorable consideration in the federal budget process in Russia, the competing internal demands for increased government resources are severe. The continued economic recovery should improve prospects for increases in government funding for health and agriculture surveillance, but many of the facilities are currently facing financial difficulties.
The Anti-plague Surveillance and Research Network
The Russian anti-plague network includes 5 institutes and 12 stations that operate throughout Russia (see Appendix J). The institutes address a number of diseases in addition to plague, including, for example, anthrax and tularemia. These institutes have regional orientations, concentrating on infectious agents of particular concern to those regions. The stations similarly concentrate on local problems as would be expected.
During the Soviet era, this network of facilities was important in addressing disease outbreaks not only in Russia but also in other Soviet republics. Although the Russian components of the former network now concentrate primarily on problems in Russia, they still play a role as a technical resource for supporting activities organized by the governments of neighboring countries in Central Asia and the Caucasus. One institute, the Stavropol Scientific Research Anti-plague Institute, has served as a WHO collaborating center since 1973, and has sent teams to China and Mongolia; but it has had only limited interactions with Western institutions (Stavropol Scientific Research Anti-plague Institute, 2003).
IMPROVING SURVEILLANCE AND RESPONSE
Set forth below are two structural and organizational recommendations that could contribute to the improvement of Russia’s surveillance capabilities. These initiatives are intended to help: (1) determine the incidence and prevalence of endemic and emerging infectious agents in humans and animals; and (2) improve the detection, diagnosis, and identification of infectious agents within a national reference laboratory system that is connected to the global system of the WHO. If
Russia builds on its long history of successful epidemiology and disease surveillance, it will be in a position to develop strong state-of-the-art abilities to investigate disease outbreaks. The following suggestions are modest in scope, but nevertheless can spotlight important practical steps that should be taken on a broader basis.
A realistic approach to strengthening Russian capabilities for disease surveillance and response over the next ten years is to make incremental improvements throughout the SSESC system. To guide this effort, the committee recommends prompt establishment of two model SSESCs for surveillance, diagnosis, analysis, and communication of information concerning infectious disease episodes.
One center would be at the regional (oblast) level and a related center would be at the local level within the same region. Geographical integration of the two centers would provide many opportunities to demonstrate how communications and cooperation within and between regions throughout the national system can be upgraded. The centers might be closely linked to research institutes that are in the same geographical areas. Preferably, the selected region should be distant from Moscow and St. Petersburg, which traditionally have attracted more financial resources than other areas of the country. Such outreach beyond the two principal cities of Russia would certainly command attention throughout the country.
The two centers would be an important step in establishing standards for upgrading the entire SSESC network over the long term. Further, because SSESCs are the primary organizations for reporting disease trends and outbreaks, particularly at the local level, they are an essential resource for supporting the surveillance oversight at the excellent facilities in Moscow. Their interactions with the highly experienced Moscow center should also benefit the model centers.
The model centers should be internally linked via electronic communications with SSESCs throughout the country. The entire system should be externally linked with the WHO and other nodes of the international disease surveillance community. The model centers should have surge capacity to address outbreaks and other crisis situations not only in their own geographical areas but also in nearby regions of the country while providing up-to-date information to Moscow. Also, the centers could become regional and local training centers.
Regardless of their locations, significant investments will be required to establish the centers, either through upgrading existing facilities or constructing new facilities. Still larger investments will be required to upgrade additional centers based on lessons learned at the model centers. Important capabilities of the proposed regional model center are set forth in Box 2.1.
The center at the local level would have more modest capabilities building on those that may already be available in the area. Modern diagnostic capabilities and communication facilities would be key components at both centers. New
|
BOX 2.1
|
personnel needs would depend on the capabilities currently existing at the selected locations.
Special allocations of funds, either from the Russian government or from a combination of government and international sources, will be needed to establish the model centers since the investment costs for the two centers will be significant, perhaps totaling in the tens of millions of dollars or more each. However, this level of funding is very small in comparison with the funds required to upgrade the entire SSESC system of 2,300 facilities. As the Russian economy continues to improve, new funds for much wider improvements throughout the system will likely become available from the government budget. The experiences with the model centers can provide important and persuasive long-term guidance on how other facilities can best use resources they now receive or will receive in the future. Such guidance is important to ensure consistency within the system.
In developing the recommendation to upgrade the SSESC system through the establishment of two model centers, the committee considered three other options as targets for initial investments that may become available. All of the other options were considered less promising means of launching a large-scale upgrade of the entire system of 2,300 centers. The three alternatives considered were as follows:
-
Additional funding directed toward upgrading communication networks throughout the entire system. While improved communication is important and needed, more complete and authoritative information sent over the existing networks is an even more critical need, particularly in the long term. Experts at many of the centers know what is required to improve communication and are taking steps to help remedy the situation. However, upgrading their other activities is stymied not only by the lack of funding but also the inability to determine which improvements are needed and which are of highest priority.
-
Additional funding spread across the 89 regional centers, enabling them to focus on the most pressing needs in their particular regions. Determining how best to divide funds and then account for their use would be difficult and might well destroy the program before it started. Also, it is highly unlikely that the performance of many SSESCs would be significantly improved in the absence of an unrealistically massive influx of funding. Finally, there would be little likelihood that an attractive standard for nationwide emulation would be achieved.
-
Additional funding spread across six to eight SSESCs, which would become “partial” model facilities. This approach is less likely to have nationwide impact than the chosen alternative. As has been demonstrated at the center in Moscow, government officials at the national and local levels and the general public are more impressed by a “complete package” of modern technology as a goal than by partial measures. Unfortunately, because Moscow is widely considered a special case with nearly unlimited funding support, that center cannot effectively serve as a model. However, two modern centers in distant cities would attract considerable attention as realistic models for the rest of the country.
Turning to a second recommendation, despite the strong field capabilities of Russia’s anti-plague system, it has remained organizationally distinct from the system of SSESCs and somewhat detached from Western efforts to improve surveillance and response capabilities in Russia. Further, there has been little progress in efforts to harness the resources of the anti-plague system to serve broader global interests. Still, the system continues to be an essential component of Russian efforts to counter infectious diseases. Therefore these facilities are in a unique position to lead investigations of outbreaks under a variety of environmental conditions that would be of interest to the broader international community.
Thus, the second recommended initiative is directed toward fully integrating Russia’s anti-plague network into the national public health surveillance system and then into global systems. Even though the Russian anti-plague monitoring facilities have remained largely isolated from the international community, perhaps due to security sensitivities dating from the Soviet era, they continue to be an essential component of Russian efforts to prevent and control infectious diseases of local, national, and global interest. Their data banks and their strain collections are valuable resources and should be fully utilized in
building modern disease prevention and control programs that include geographic monitoring, laboratory diagnosis, reference identification, and intervention.
Transformation from an internal to an external orientation could begin with modest investments to update disease surveillance within Russia by improving the equipment and communication capabilities of the five anti-plague institutes and then moving toward international cooperation. It is likely that, if asked, the international community would contribute some of the necessary funds, given the worldwide benefits of such a transformation. The initiation of joint U.S.-Russian epidemiological systems would be a logical early step in this direction.
Upgrading the SSESC system and bringing the anti-plague network more directly into national and international surveillance systems are only two possible initiatives to strengthen Russia’s surveillance and response capabilities. Certainly greater support of agriculture disease surveillance networks with special attention to zoonotic diseases would be highly beneficial as well.
The next chapter addresses the role of research organizations which support surveillance and control activities described in this chapter. Together, these two chapters should provide useful guidance for further Russian efforts to improve the scientific base for combating infectious diseases.









