Summary and Assessment
The cold war era has passed. The fall of the Berlin Wallin 1989 marked the beginning of the disappearance of old borders and a new global era of unparalleled human movement and interaction. Although the new global arena has created economic opportunities and growth, the benefits have not been equally distributed, and the risks—especially the health risks—of this increasingly interconnected and fast-paced world continue to grow. As people, products, food, and capital travel the world in unprecedented numbers and at historic speeds, so, too, do the myriad of disease-causing microorganisms. The worldwide resurgence of dengue fever, the introduction of West Nile virus into New York City in 1999, the rapid spread of human immunodeficiency virus (HIV) infection in Russia, and the global spread of multidrug-resistant tuberculosis (TB) are but a few examples of the profound effects of globalizing forces on the emergence, distribution, and spread of infectious diseases. No nation is immune to the growing global threat that can be posed by an isolated outbreak of infectious disease in a seemingly remote part of the world. Today, whether carried by an unknowing traveler or an opportunistic vector, human pathogens can rapidly arrive anywhere in the world.
At the same time, the very interdependency and connectedness that create such opportunities for the global spread of pathogens also offer mechanisms for innovative, multinational efforts to address the threat. A growing network of such efforts, combined with the global proliferation of technology and information, continues to strengthen the global public health capacity to prevent and control the spread of emerging and reemerging
infectious diseases. One participant in the Workshop on the Impact of Globalization on Infectious Disease Emergence and Control described the situation thus: just as the globalization of infectious diseases is characterized by a transformation of separate entities into a unified epidemiological system, disease control capacity in one part of the globe can readily be deployed to fight diseases in other parts of the world.
Workshop participants discussed the impacts of increasingly integrated trade, economic development, human movement, and cultural exchange on patterns of disease emergence and reemergence; identified opportunities for countering those impacts; examined the scientific evidence supporting current and potential global strategies; and considered new response methods and tools available for use by private industry, public health agencies, regulatory agencies, policy makers, and academic researchers. Participants included experts from the international community, industry, academia, the public health community, and government; invited international participants included key representatives from the Americas, the European Union, and Russia. Detailed summaries of the workshop’s formal presentations and roundtable discussions are presented in Chapters 1 through 4 of this report.
At one point during the workshop, a call was made to heed the danger of equating globalization with Americanization, as an international point of view is crucial to a true understanding of the issues. Participants were also asked to strike a balance between what could be perceived as the negative aspects of globalization and its humanizing and empowering potential. As one participant explained, to examine the globalization of emerging infectious disease, one must address a more general tension that characterizes any globalization phenomenon: that between globalization as opportunity, the view taken by Friedman (2000) in The Lexus and the Olive Tree, and as something that is frightening and potentially dangerous, the perspective taken in the more radical social scientific literature (see Appendix A). As another participant put it, while examining the responses needed to meet this Malthusian challenge, one concludes that the solutions may be unearthed from the problem.
THE PAST, PRESENT, AND FUTURE OF THE GLOBALIZATION OF INFECTIOUS DISEASE
Globalization is by no means a new phenomenon; transcontinental trade and the movement of people date back at least 2,000 years, to the era of the ancient Silk Road trade route. The global spread of infectious disease has followed a parallel course. Indeed, the emergence and spread of infectious disease are, in a sense, the epitome of globalization. By Roman times, world trade routes had effectively joined Europe, Asia, and North America
into one giant breeding ground for microbes. Millions of Roman citizens were killed between 165 and 180 AD when smallpox finally reached Rome during the Plague of Antoninus. Three centuries later, the bubonic plague hit Europe for the first time (542–543 AD) as the Plague of Justinian. It returned in full force as the Black Death in the fourteenth century, when a new route for overland trade with China provided rapid transit for fleainfested furs from plague-ridden Central Asia.
Even before the development of world trade routes, however, human pathogens had experienced two major bonanzas. First, when people lived as hunter-gatherers, they were constantly on the move, making it difficult for microbes to keep up with their human hosts. Once people started living as farmers, they began residing in larger numbers in the same place—and were in daily contact with their accumulating feces—for extended periods of time. Second, the advent of cities brought even larger numbers of people together under even worse sanitary conditions. In the Middle Ages, when people threw human waste out their windows in England, they were said to be “blessing the passerby.”
Now, two millennia later, human pathogens are experiencing yet another bonanza from a new era of globalization characterized by faster travel over greater distances and worldwide trade. Although some experts mark the fall of the Berlin Wall as the beginning of this new era, others argue that it is not so new. Even a hundred years ago, at the turn of the nineteenth century, the tremendous impact of increased trade and travel on infectious disease was evident in the emergence of plague epidemics in numerous port cities around the world. As Echenberg (2002) notes, plague epidemics in colonial African cities were closely tied to the increased communication, travel, and trade that accompanied the advent of the steamship. The economic and social impacts of these epidemics were profound. In Johannesburg, in what is now South Africa, the occurrence of plague led to the relocation of black residents in an effort to remove what the white colonists believed was the source of the disease. At about the same time, the influenza pandemic killed many millions of people worldwide.
Thus the current era of globalization is more properly viewed as an intensification of trends that have occurred throughout history. Never before have so many people moved so quickly throughout the world, whether by choice or force. Never before has the population density been higher, with more people living in urban areas. Never before have food, animals, commodities, and capital been transported so freely and quickly across political boundaries. And never before have pathogens had such ample opportunity to hitch global rides on airplanes, people, and products.
The future of globalization is still in the making. Despite the successful attempts of the developed world during the course of the last century to control many infectious diseases and even to eradicate some deadly afflic-

FIGURE S-1 Leading causes of mortality from infectious disease, 2000 estimates.
SOURCE: Klaucke (2002).
tions, 13 million people worldwide still die from such diseases every year (see Figure S-1).
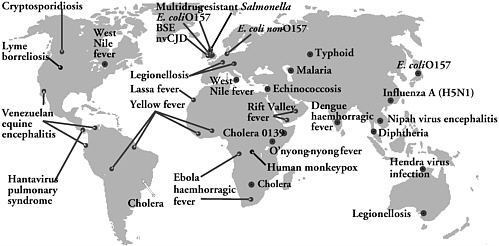
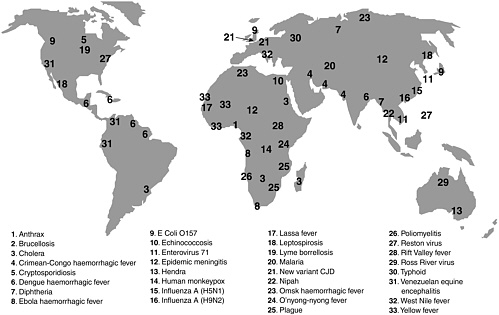
Although the burden is greatest for the developing world, infectious diseases are a growing threat to all nations. The problem is compounded by the emergence of new diseases, such as severe acute respiratory syndrome (SARS),1 that occur unexpectedly and require urgent interventions (see Figures S-2a and S-2b).
The uncertainties of what can and will happen posed challenges to the workshop participants as they discussed the issues. At the same time, their collective wisdom presented opportunities to establish a framework for progress. The growing threat of the emergence, reemergence, and rapid global spread of infectious disease calls for a new, global paradigm of participation by the public health community. The need for collaboration has never been greater. Long-term, multinational training and partnerships among government, health care, financial, and other institutions are vital to building the global public health capacity necessary to address the threat posed worldwide by even an isolated incident of an infectious disease. The
full and equal participation of partners in the developing world will be critical to this effort.
What exactly does such a collaborative, international framework entail? What opportunities does globalization afford to support the effort? How can these new global tools be used to their maximum advantage? What obstacles must be overcome? These are some of the many questions deliberated by the workshop participants, as summarized in this report.
Chapters 1 and 2 describe how globalizing forces have affected the prevention and control of infectious disease. The topics discussed range from the impact of the international flow of capital on emerging infectious diseases to the opportunities provided by the new, unprecedented influx of spending on defense against bioterrorism. Chapter 3 describes a variety of new opportunities for enhancing infectious disease control, such as global surveillance capabilities and the changing nature of transnational public health training programs. Chapter 4 summarizes some key components of the new global public health framework: the role of public–private partnerships, the role of international law, and the importance of a social science perspective for understanding and studying emerging infectious diseases. Finally, the appendices to this report consist of the workshop agenda and papers contributed by David Fidler, Jonathan Mayer, and Andrey Demin.
A WORLD IN MOTION
As the human immunodeficiency virus (HIV) disease pandemic surely should have taught us, in the context of infectious diseases, there is nowhere in the world from which we are remote and no one from whom we are disconnected.
—IOM, 1992
Over the past two centuries, the average distance and speed of human travel have increased a thousand-fold, but incubation times for infectious diseases have remained the same. What historically may have been only a small, localized outbreak can now develop in a matter of days into a large, worldwide epidemic. Not only have the speed and distance of human travel accelerated and expanded, but unprecedented numbers of people are also on the move. Thirty years ago there were only about 200 million international tourist arrivals annually, compared with an expected 900 million or more by 2010. The global spread of HIV/AIDS is only one, albeit the most devastating, example of the impact of this tremendous human mobility on infectious disease.
Tourists are not the only people taking advantage of open borders and international travel opportunities. Each year millions of people leave their homes, either temporarily or permanently, in search of work or an im-
proved quality of life, and millions more are forcibly displaced by war. These migrant populations, especially refugees, are among the most vulnerable to emerging infectious diseases. In many developed countries, the emergence and reemergence of infectious diseases, such as multidrug-resistant TB, are frequently linked to the massive influx of immigrants from poor countries with a higher prevalence of such diseases. The situation is expected to worsen in the future as the world population grows, demographic and economic gaps between the developed and developing worlds deepen, and greater numbers of people either are forcibly displaced or leave their homes by choice in search of a better life.
Although increased human mobility may be the most obvious manifestation of globalization, it is by no means the most important. As several workshop participants noted, the global spread of capitalism and the free market is the main driving force behind the current era of globalization. Much discussion at the workshop thus focused on the rapidly changing nature of the global marketplace; the ease with which food, commodities, capital, and economic and political decision-making powers are being passed around the world; and the important implications of these changes for infectious disease emergence and control.
The same advances in transportation technology that facilitate global travel by humans also allow the rapid transcontinental movement of infectious disease vectors. It has been hypothesized, for example, that the vehicle for the introduction of West Nile virus into the United States in 1999, the first occurrence of this disease in the western hemisphere, was an airplane carrying an infected mosquito vector (Cetron, 2002). That mosquito vectors can hitch rides in the wheel wells of airplanes is well known. Controversial evidence also suggests that global warming, much of which is generated by human trade-related activities, may be leading to an increase in the geographic expansion and distribution of vectors.
Historically, most food has been produced and consumed locally. Over the last two decades, however, as consumer demand and expectations have increased and as food production and processing activities have become more geographically fragmented (e.g., foods produced in one locale being processed elsewhere), the epidemiology of foodborne disease has changed significantly. More recently, changes in international trade law, including the establishment of the World Trade Organization (WTO) in 1995, have altered even more dramatically the ways in which all products, food and others, are bought and sold. For example, before the establishment of WTO in 1995, trade in animals and animal products was conducted according to a policy of zero risk. Now, imported products are treated no less favorably than domestic products, at least with regard to animal health restrictions. The experience of bovine spongiform encephalopathy in the United Kingdom and Europe illustrates the tremendous risk that accompanies the seem-
ingly unlimited growth and opportunity offered by new international trade regulations enforced by WTO.
It is cause for alarm that many countries do not have comprehensive food safety programs integrated into their public health strategies. The problem is not limited to the developing world or to food products imported from those nations. Outbreaks of foodborne illness have revealed several inadequacies in food safety regulation capabilities even in the United States. The free flow of food also raises serious concerns about the global spread of antibiotic resistance associated with the consumption of antibiotic-fed food animals.
Finally, although the use of the term “globalization” in the health sciences literature generally refers to growing global interdependency, particularly as manifested by increased international travel, the phenomenon of globalization encompasses much more. It also refers to the changing nature of the world’s global political economy, the development of a truly global marketplace, and the power relationships embedded within this new economy. In fact, given that the spread of capitalism and the free market is the main driving force behind globalization, the health sciences community might benefit from examining the ways in which this movement of capital affects emerging infectious diseases. An excellent demonstration of this point is the use of foreign capital to fund dam construction and other similar environmental modification projects, which almost always alter, either directly or indirectly, local vector ecologies and human–pathogen interactions. For example, not only is construction of the Three Gorges Dam on the Yangtze River in China altering the potential for the transmission of schistosomiasis and other diseases by disrupting local vector ecologies, but it is also increasing the risk of transmission even further by forcing people to leave their homes and live in highly concentrated areas. In light of the damaging effects of many projects on their local and regional environments and public health, workshop participants suggested that perhaps current economic models need to be reexamined, and that the potential (and costly) public health ramifications of investment decisions need some-how to be incorporated into those models.
EXAMINING THE CONSEQUENCES
As the public health ramifications of dam construction and other environmental modification projects illustrate, the growing international market and the increased mobility of the global population have already and will continue to play a central role in shaping the global infectious disease landscape, both literally and figuratively. Other global developments discussed at the workshop have important public health implications as well, including globally fueled armed conflicts and the massive displacement of
people, the inability to monitor and provide adequate health care to the continually growing numbers of mobile people displaced because of war or other reasons, the incapacity to monitor foodborne and trade-related infectious disease risks worldwide, and the growing actual and perceived threats of bioterrorism. These developments have at least one thing in common: if left unchecked, they could have profound and potentially devastating consequences for global public health.
Some argue that as the global economy improves, the living conditions of poor populations will also improve. As one participant suggested, however, this is not necessarily true. Poor countries of the world are still poor, violence is increasing, and the same diseases still exist. As information becomes easier to access in even the remotest corners of the world, everyone will know how everyone else is living and under what circumstances. Greater numbers of people will leave their homes in search of work and an improved quality of life, and greater numbers of people will be forcibly displaced. As the world population continues to grow, as urban areas in the developing world continue to expand and further strain their already resource-limited governments, and as the global marketplace continues to hone the already sharp demarcation in wealth—and health—that exists between rich and poor countries, the ensuing social unrest and loss of state control will likely fuel even more communal conflict, forced migration, and terrorism.
Unless the public health infrastructure is modified to accommodate the health care needs of mobile populations and unless the capacity to monitor mobile populations is strengthened, both pre- and postarrival, the United States and other developed countries will be unable to handle the massive influx of immigrant and refugee populations. One participant described the surveillance of mobile populations as a “new but necessary idea.” The global spread of TB, particularly multidrug-resistant TB, illustrates what can result from the failure to monitor and provide health care for mobile populations. The gap in the prevalence of TB between U.S.-born and foreign-born U.S. residents is already huge; according to the Centers for Disease Control and Prevention, foreign-born residents accounted for 46 percent of new cases of TB in the United States in 2000 (CDC, 2002). Other developed countries are experiencing the same phenomenon; for example, according to a 1998 study, 92 percent of all multidrug-resistant TB cases in Canada were imported (Grondin, 2002). Not only are migrants and refugees more likely than the general population to become infected, but they also put others at risk.
Standards are therefore needed for monitoring the health of mobile populations. While such standards are necessary, however, they will not be sufficient. Unless their underlying causes are addressed, armed conflict and the threat of terrorism will continue to plague the world, drive mass migra-
|
Box S-1 In a retrospective study, Mohle-Boetani and colleagues (2000) analyzed a number of factors that contributed to the recognition of cyclosporiasis during eight months of outbreaks in California in the spring of 1997. The authors interviewed index patients with the disease and reviewed the proportion of cases detected because of enhanced laboratory surveillance. Diagnosis of cyclosporiasis requires special testing not done with standard ova and parasite methods. Six of the eight index cases were diagnosed more than two weeks after onset of symptoms. In six of the eight cases, stool testing was done after patients brought information to their physicians and requested the tests. The information came from Internet searches and from newspapers and other media coverage. In one instance, a physician was prompted by a television report to test for cyclosporiasis. Multiple communication channels link physicians and patients and educate both. This study shows how knowledge derived from websites and the media led to the diagnosis of a disease previously unknown to many clinicians. Enhanced laboratory surveillance also contributed to detection of the parasite. SOURCE: Mohle–Boetani et al. (2000). |
tion, and increase the risk of the emergence and spread of infectious disease. In the case of wars, almost all of which involve the use of small arms, workshop participants cited limiting the availability of such arms as an example of a tangible step that could be taken, given that the legal small arms trade is amenable to modification through U.S. policy (Leaning, 2002).
As with the monitoring of mobile populations, unless the capacity to monitor the global transport of foodborne and trade-related vectorborne infectious diseases is improved, such diseases will continue to pose serious public health risks. Although some argue that the risk of imported foodborne disease is relatively low—at least in the United States and in comparison with the risk of domestically derived foodborne disease—others argue that the surprisingly low incidence of the former reflects more a lack of surveillance than a lack of disease. The 1996–1998 outbreaks of cyclosporiasis in North America, caused by contaminated raspberries imported from Guatemala (see Box S-1), may not be as isolated an incident as one might think. One of the reasons this outbreak received so much attention was the scientific excitement surrounding the relatively newly discovered pathogenic culprit. Yet even if foodborne outbreaks caused by imported products are uncommon, the potential for such outbreaks is increasing. Although WTO, the World Health Organization (WHO), the Asia-Pacific Economic Cooperation (APEC), and a handful of other re-
gional organizations have recently attempted to improve surveillance for foodborne and trade-related infectious diseases, this is still a somewhat underappreciated need.
Finally, one of the most prominent features of the new global landscape is the increased threat of bioterrorism. As one participant put it, today we are standing at the crossroads of two historical trajectories: one stemming from a day in 1453 when Constantinople fell to the Turks after centuries of conflict between the Christian West and the Muslim East, an event that signified the end of the Middle Ages and the beginning of the Renaissance; the other stemming from an event that occurred nearly 500 years later, when the British scientific journal Nature published an article by two young scientists, James Watson and Frances Crick, reporting the discovery of the DNA double helix. Thus, as the world enters the twenty-first century, society is simultaneously witnessing the reemergence of conflict between western and eastern cultures, the denouement of the age of physics, and the ascendance of the age of biology. The result is the convergence of global terrorism and the widespread availability of molecular biology techniques. At the heart of this collision is the use of infectious disease as a weapon.
The threat of increased bioterrorism was made real by the terrorist attacks of September 11, 2001, and the subsequent mailing of letters laden with anthrax spores in October 2001. The challenges faced by international health programs have increased as a result. The current Bush Administration has responded with a 319 percent increase in spending on defense against bioterrorism—to $5.9billion for fiscal year 2003. The funds will be used to improve detection and surveillance systems, strengthen medical capabilities, improve planning and coordination, foster research, expand training exercises and communication strategies, and address policies that create bureaucratic barriers to strengthening the U.S. capacity to address bioterrorism. The promised funding will potentially provide many new opportunities to strengthen the U.S. public health capacity to address multiple emerging infectious disease threats, both domestically and worldwide. This unprecedented level of funding offers a rare chance to make a difference in the surveillance and prevention of infectious diseases, although workshop participants expressed several concerns regarding the use and the sustainability of this funding.
OPPORTUNITIES AND OBSTACLES
The recent funding for biodefense initiatives is but one example of the many benefits of the globalization of efforts to combat microbial threats. Other benefits and advances include the growth and changing nature of training and research partnerships between developed and developing coun-
tries, the development of new treatments and vaccines that could potentially save millions of lives, and advances in information technology.
Despite a century of European involvement and decades of U.S. involvement in tropical medicine and infectious disease research and training programs, only recently have partnerships between developed and developing countries (also termed North–South partnerships) evolved into the type of egalitarian, bidirectional arrangement required for the global control of infectious disease. Most such programs, such as that of the Liverpool School of Tropical Medicine, founded in Liverpool, England, in 1898, were originally designed to develop Northern capacity and expertise in tropical medicine. However, to develop the global public health capacity needed to respond rapidly and effectively to an unexpected pandemic, whether introduced naturally or intentionally, more resources and focus must be directed toward strengthening the public health capacity of the developing world.
Several participants cited the Peru-based Gorgas Course in Clinical Tropical Medicine, a collaborative effort between the University of Alabama and the Instituto de Medicina Tropical “Alexander von Humboldt,” as an example of the kind of program that is needed. This collaboration empowers its Southern participants in a way that lays the groundwork for building a sustainable intellectual and public health capacity in that developing nation. The Fogarty International Center of the National Institutes of Health is undertaking similar efforts by planning and implementing a range of training programs overseas.
The need to strengthen the public health capacity in the developing world should not, however, detract from the still urgent need to incorporate public health education and training into the curricula of U.S. medical and veterinary schools. A number of recent microbial threats have been zoonotic. To address these and other future threats effectively, links need to be established between medical and veterinary schools. Human and animal health issues must be addressed in a coordinated manner if the public health workforce is to be trained to combat zoonotic diseases. Moreover, many practicing physicians in developed nations have never seen a case of measles, let alone malaria. Thus, transnational programs should continue to serve the original goal of strengthening the public health capacity in the North as well. After all, there is much to be learned in and from the developing world.
Peru has a long and rich history of experience with infectious diseases. For example, Peruvian mummies have yielded evidence that the first known TB epidemic occurred in that country nearly 2,000 years ago. Several hundred years ago, Spaniards introduced smallpox into Peru when they first landed on the shores of the Americas (Peru, in turn, sent syphilis back to sixteenth-century Europe, where Spanish troops spread the epidemic throughout the continent). In the last 25 years, one-third of all new infec-
tious diseases described in the published literature have been discovered in Latin America. And the upwelling of the cold deep water off the coast of Peru, a decidedly local phenomenon, has become a worldwide problem in the form of the El Niño2 Southern Oscillation, which in turn has had a significant effect on the ecology and public health–related consequences of infectious diseases worldwide.
North-south training partnerships are but one example of the type of multinational collaboration that the increasing interconnectedness of the world not only allows but demands. Workshop participants also cited the vital source of expertise and knowledge of infectious diseases represented by scientists from the former Soviet Union and the potential role Russia could play in transnational public health education and training.
Russia has been participating in other international efforts to prevent and control the emergence and reemergence of infectious diseases. Leading the way is the State Research Center of Virology and Biotechnology Vector (SRC VB Vector) in Koltsovo. Despite the achievements of SCR VB Vector, however, an enormous amount of work remains to be done to strengthen Russia’s public health capacity. The country is experiencing the emergence and reemergence of multiple infectious disease agents, from hepatitis A virus to HIV and is on the verge of experiencing major epidemics. This crisis has been attributed to the tremendous economic, social, and public health fallout from the dissolution of the former Soviet Union. The pieces have yet to come back together again, and Russian leaders are urgently in need of a new public health paradigm.
As the situation in Russia demonstrates, taking full advantage of new global opportunities does not necessarily come easily. Antiretroviral agents, for example, have more than proven their public health worth in the United States and other developed countries for the treatment of HIV and other infections. However, sub-Saharan Africa—the region of the world worst affected by HIV/AIDS—and other resource-constrained settings are in urgent need of a way to scale up the delivery of antiretroviral therapy. It would be neither prudent nor practical to apply the U.S. model of the introduction and dissemination of antiretroviral agents. HIV infections resistant to antiretroviral agents have already become a serious problem in the United States, in part because of premature introduction of the drugs; if
resistance to these agents emerges in Africa, it is likely that no amount of money or political will be able to stem the resulting crisis.
In addition, although vaccines have more than earned their reputation as one of the greatest public health tools in history, their utility in many developing countries is limited by weak or nonexistent public health infrastructures and a lack of resources. Despite the early successes of the Global Alliance for Vaccines and Immunization—formed in 2000 in response to the growing gap in levels of vaccine usage between developed and developing countries—numerous impediments to accelerating the global deployment of the available vaccines remain. For example, the limitations imposed by local conditions must be accounted for if new public health measures are to be implemented and new technologies transferred. Also, in the rush to achieve desirable short-term outcomes, local programs tend to be scaled up rapidly. The sudden infusion of billions of dollars into these systems, however, raises the question of how quickly this money can be spent wisely. Too often, hasty decisions have detrimental long-term consequences, and the cure ends up being worse than the problem.
Drug and vaccine delivery is only half of the problem. Equally urgent is the need to redress the imbalance between drug research and development efforts directed toward developed and developing nations. As one participant noted, although pharmaceutical companies have produced more than 2,000 new compounds over the last decade, only six of these are for the treatment of tropical diseases. As the global economy becomes even more interconnected, this will likely become an extremely difficult challenge to overcome.
Global surveillance is another example of a tool that holds tremendous promise but still faces many difficult political, scientific, and coordination challenges. Many countries fail to report local outbreaks in an effort to avoid potentially huge negative economic and political repercussions, such as trade sanctions and travel advisories. For several reasons, international reactions to public reports of infectious disease outbreaks typically far exceed what is warranted by the actual situation and public health risks. Even regional surveillance can be difficult to achieve, as the efforts in the Caribbean demonstrate (Corber, 2002).
A novel but for the most part untested idea introduced during the workshop was the establishment of a global public health bank for the storage and distribution of limited resources that might otherwise not be used to their maximum advantage. It was suggested that this program could be managed by a global health broker and would enable resources to be shared across borders (Timpieri, 2002).
Finally, most would agree that the Internet offers obvious and tremendous potential for infectious disease surveillance, prevention, and control. Never before have information and data been so easy to access and share.
The Global Outbreak Alert and Response Network (http://www.who.int/csr/outbreaknetwork/en/) and the Global Atlas of Infectious Diseases (http://www.whqathena.who.int/globalatlas/) are but two examples of how the Internet and other advances in information technology are being exploited in the fight against infectious diseases.
FRAMEWORK FOR PROGRESS
Recent large increases in spending on international health—for example, through the Global Fund to Fight AIDS, Tuberculosis, and Malaria and President Bush’s recently proposed Millennium Challenge Account—reflect growing awareness and appreciation of the importance of global health. A number of factors account for these changing perceptions. First and foremost, support for international health efforts is no longer perceived as a costly charity endeavor; rather, it has become a cost-effective way of doing business. Even a century ago, millionaire ship owner Sir Alfred Lewis Jones founded the Liverpool School of Tropical Medicine, which sponsored 32 expeditions to the tropics between 1989 and 1913. Jones and other members of the Liverpool, England, business community recognized the wisdom of investing in the study of tropical diseases given that employee illnesses and deaths from malaria abroad led to reduced productivity and increased health expenditures at home.
Not only is poor public health bad for business, but it also threatens international political stability and U.S. national security. For example, at the same time that high HIV infection rates in sub-Saharan Africa limit the potential for international trade partnerships, they threaten the political and social stability of the entire region, thus posing a significant national security risk to the United States. The situation is exacerbated when armed forces are hit by high HIV infection rates, weakening military and peacekeeping capacities.
Despite increased funding and dramatic changes in the general perception of international health, several participants agreed that strengthening the global capacity to prevent and control the emergence and spread of infectious diseases will require even more money and newer approaches. Others emphasized the importance of recognizing the difference between the need for more money and the need to spend the available money more wisely. Without a strong infrastructure and knowledge base in place, large influxes of money are often wasted. It is crucial, therefore, that international systems and local agencies have the capacity to program significant amounts of money effectively. On the other hand, the tremendous amount of resources needed to address the most pressing global health problems, such as the HIV/AIDS pandemic and the global spread of drug-resistant malaria, cannot and should not be underestimated.
Participants identified four key components of a newer approach to infectious disease control:
-
A global mind-set,
-
Long-term collaborations, particularly public–private partnerships, among states, interstate and regional organizations, nongovernmental organizations, multinational corporations, and various other nonstate actors,
-
Larger, more flexible financial consortiums, such as the Global Fund to Fight AIDS, Tuberculosis, and Malaria, and
-
The concept of public goods, especially with regard to product development and the dissemination of knowledge.
With regard to the need for a global mind-set, the colors of the geopolitical map in no way reflect what is going on epidemiologically. A rational approach to infectious disease control must be based on science, not political boundaries. At the same time, however, public health agencies are generally constrained by the reality that they operate according to politically defined organizational structures. India, for example, has more than 50 different zones, each with its unique epidemiological conditions, yet the country is treated by WHO as a single unit or member state (Miller, 2002).
Since 1994, the Centers for Disease Control and Prevention (CDC) has attempted to define its mission in a more global context by taking a global approach to infectious diseases. CDC’s strategy focuses on strengthening global capacity in six priority areas: international outbreak assistance, disease surveillance, applied research on diseases of global importance, application of proven public health tools, initiatives for disease control, and public health training for capacity building. This strategy can serve as a point of reference for the development of national, regional, and global strategies for addressing the globalization of infectious diseases.
Public–private partnerships serve as a vital conduit for providing public health care supplies and services to populations, particularly in the developing world, that would otherwise not receive them. Examples include a multitude of recently developed innovative, achievement-oriented joint venture collaborations and partnerships involving the privatization of health care delivery services, with the public sector setting the rules and monitoring the quality of service. These arrangements are characterized by their mutually beneficial nature and shared decision making, among other attributes. Yet despite the clear and growing demand for the participation of multinational corporations in these partnerships and in global health efforts in general, engaging their full interest still poses a considerable challenge. This situation is very worrisome. The Global Fund to Fight AIDS, Tuberculosis, and Malaria, for example, may not be sustainable without
the commitment of nongovernmental entities, in terms of not only financing, but also technical and intellectual support.
Beyond a newer approach to infectious disease control on the part of the public health sector, globalization demands a new legal framework. The changing nature of the sovereignty and territorial basis of governments has tremendous implications for public health legislation and the role of international law in the prevention and control of emerging infectious diseases. International health regulations are being revised accordingly, but this may not be enough. Governance and the rule of law may have changed in such a way that even the revised regulations may not meet the legal needs of a new, internationally coordinated approach to the management of public health.
Finally, globalization demands a new social scientific framework for studying and understanding the emergence of infectious diseases. This is not a new realization. Five of the six factors related to the emergence of infectious diseases identified in a 1992 Institute of Medicine report on microbial threats (IOM, 1992) were social in nature, and the sixth, microbial adaptation and change, is partly the result of social behavior and social change. Yet the study of emerging infectious diseases is still conducted almost entirely within the realm of the biological sciences. The political ecology of disease might serve as new conceptual approach to studying and understanding the emergence of infectious diseases.
REFERENCES
CDC (Centers for Disease Control and Prevention). 2002. Tuberculosis morbidity among U.S.-born and foreign-born populations: United States, 2000. MMWR 51(05):101–104.
Cetron M. 2002 (April 16). The World and Its Moving Parts. Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
Corber S. 2002 (April 16). Invited Discussion: A Response to the Shifting Trends. Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
Echenberg M. 2002. Black Death, White Medicine: Bubonic Plague and the Politics of Public Health in Colonial Senegal, 1914–1945. Portsmouth, NH: Heinemann.
Friedman TL. 2000. The Lexus and the Olive Tree: Understanding Globalization. New York: Anchor Books.
Grondin D. 2002 (April 16). Global Migration and Infectious Diseases. Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and the Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
IOM (Institute of Medicine). 1992. Emerging Infections: Microbial Threats to Health in the United States. Washington, D.C.: National Academy Press.
Klaucke D. 2002 (April 17). Globalization and Health: A Framework for Analysis and Action. Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and the Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
Leaning J. 2002 (April 16). Health, Human Rights, and Humanitarian Assistance: The Medical and Public Health Response to Crises and Disasters. Presentation at the Institute of Medicine Workshop on The Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
Miller M. 2002 (April 17). Invited Discussion: Considerations for Shaping the Agenda. Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and the Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
Mohle-Boetani JC, Werner SB, Waterman SH, Vugia DJ. 2000. The impact of health communication and enhanced laboratory-based surveillance on detection of cyclosporiasis outbreaks in California. Emerging Infectious Diseases 6(2):200–203.
Timpieri R. 2002 (April 17). Invited Discussion: Considerations for Shaping the Agenda. Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities, Washington, D.C. Institute of Medicine Forum on Emerging Infections.
WHO (World Health Organization). 1999. Infectious diseases are the biggest killer of the young. In: Removing Obstacles to Healthy Development. Geneva, Switzerland: WHO.