1
Introduction
Memorial Hospital Emergency Department
Tuesday, 3:00 PM
Memorial Hospital, a large, urban medical center and level I trauma center, has an emergency department (ED) designed to hold 40 acute patients. It is operating well over capacity, with more than 80 patients actively undergoing care, 30 of whom lie on wheeled stretchers in hallways. Of these 80 patients, 24 are waiting to be admitted to inpatient beds; 4 have been waiting 7–10 hours, 1 for 20 hours, and 1 for over 24 hours. The hospital has been on EMS diversion for 5 hours, but with other nearby hospitals also on diversion, it is still receiving a steady stream of patients. Doctors and nurses used to the high stress of emergency care are maintaining relative order, although they have been operating at full tilt for most of the shift. The risk of errors from fatigue, stress, and hurry grows steadily higher. An EMS crew that has been waiting to offload a patient into the busy ED for more than 35 minutes stands by impatiently. The waiting room is crowded with more than 50 people—34 patients, family, and friends—including children, adults, and elderly. Some are in pain, at least one is bleeding, while others appear to have cold or flu symptoms.
A call from the dispatch center notifies the ED that five patients will soon arrive from a car crash on the nearby interstate, with injuries of varying severity. One is coming by helicopter, and the trauma team is mobilized. The ED director does her best to clear
additional space in the ED. More nursing staff are requested, but none are available; the evening supervisor has been trying to call in personnel for the past 4 hours. The level of activity in the ED is growing visibly, and the amount of attention being provided to each patient is minimal. Several patients in the waiting room give up and leave before being seen by a physician, and two patients who are undergoing treatment in the ED sign out against the medical advice of staff.
To make matters worse, a nearby hospital requests transfer of a complex neurological and orthopedic case to Memorial. The patient is stable, but his condition may deteriorate without immediate intervention. Memorial is normally well equipped to handle such patients, but the neurological and orthopedic specialists on call to the hospital are already busy with other cases in the operating room.
As the night wears on, the volume of patients gradually declines. Although the ED has been pushed to the limit at times, a meltdown has been averted by the efforts of the staff. Nonetheless, despite the best efforts of the emergency care professionals—from emergency medical technicians to emergency doctors and nurses and on-call specialists—the quality of health care delivered by the emergency care system on this night was less than it could and should have been.
Hospital-based emergency and trauma care is critically important to the health and well-being of Americans. In 2003, nearly 114 million visits were made to hospital EDs, more than one for every three people in the United States. About one-quarter of those visits were due to unintentional injuries, the leading cause of death for people aged 1 through 44; indeed, traumatic injury has surpassed heart disease as the most expensive category of medical treatment, resulting in $71.6 billion dollars in expenditures per year (AHRQ, 2006). While most Americans encounter the ED only rarely, they count on it to be there when they need it.
Over the last several decades, the role of hospital-based emergency and trauma care has evolved substantially. EDs continue to focus on their traditional mission of providing urgent and lifesaving care, but have taken on additional responsibilities to meet the needs of communities, providers, and patients. EDs have become a key component of the health care safety net, providing a considerable volume of care to uninsured patients and Medicaid beneficiaries who often cannot access health services elsewhere. EDs are also
an important public health partner, responsible for alerting public health agencies to possible threats in the community and sometimes counseling patients on prevention or self-care. Moreover, EDs play a central role in preparing their communities for disasters, and have become an important adjunct to community physicians’ practices. While the demands on emergency and trauma care have grown dramatically, however, the capacity of the system has not kept pace. Balancing these roles in the face of increasing patient volume and limited resources has become increasingly challenging.
A GROWING NATIONAL CRISIS
Hospital EDs have become frequently crowded environments, with patients sometimes lining hallways and waiting hours and even days to be admitted to inpatient beds (Asplin et al., 2003). Ambulance diversion, once rare, is now a common if not daily event in many major cities, and can lead to catastrophic consequences for patients (GAO, 2001; Schafermeyer and Asplin, 2003). Specialists needed to treat emergency and trauma patients are increasingly difficult to find; the result is longer waits and at times, distant transport of critically ill or injured patients for specialty care. The emergency system itself appears to be crumbling in major cities. In Los Angeles, for example, 8 hospital EDs have closed since 2003, bringing the total closed countywide to over 60 in the last decade (see Box 1-1) (Robes, 2005).
These trends are symptomatic of a growing national crisis in emergency care. This crisis is multifaceted and impacts every aspect of emergency care—from prehospital EMS to hospital-based emergency and trauma care. Of the many challenges confronting hospital-based emergency and trauma care today, the following stand out for their complexity, gravity, and urgency:
-
Demand outpacing capacity—Between 1993 and 2003, ED visits increased from 90.3 to 113.9 million, a 26 percent increase. During this same period, the United States experienced a net loss of 425 hospital EDs. The problem of excess demand is exacerbated by the above-noted role of the ED as one of the nation’s principal sources of care for patients with limited access to other providers, including the 45 million uninsured Americans. The result of this growing imbalance between demand and capacity is a nationwide epidemic of ED overcrowding, boarding, and ambulance diversion.
-
ED crowding—Crowding is the most obvious manifestation of the imbalance between ED demand and capacity. It occurs when patient volume backs up in the ED: many patients come in the front door, but not enough can be admitted to the hospital in a timely manner to make room for more incoming patients. As admitted patients back up in the ED, crowding be-
|
BOX 1-1 Meltdown of Emergency Care: Emergency Department Closures in Los Angeles County Los Angeles (L.A.) County, the largest county in the nation, is home to more than 10 million people (L.A. County Online, 2005). It also leads the nation in shuttered EDs. Between 1980 and 2000, 20 percent of the county’s EDs closed (Sussman, 2000); since 2003, eight more hospital EDs and one trauma center have closed. At the same time, the number of patients seeking care at EDs has soared, so the facilities that remain are being forced to absorb an overwhelmingly large patient load. These hospitals are in an increasingly tenuous financial position (Robes, 2005). While some ED closures may be justified by the changing needs of communities, the ED closures in L.A. County have led to serious consequences for patient care. The demand for emergency care at the EDs that remain is so high that waiting times can reach 8 to 12 hours (South Bay’s ERs are in a State of Emergency, 2005). Additionally, L.A. County hospitals went on diversion an average of 23 percent of the time in 2004, meaning they closed their doors to patients arriving by ambulance almost one-quarter of the time. Paramedics in L.A. County report that the closure of EDs, coupled with frequent ED diversion, is forcing them to drive farther and farther to find a hospital that is able to care for a sick or injured patient. Longer transport times translate into delays in patients’ receiving definitive care. But even once paramedics arrive at an open ED with a patient, one in eight trips involves an additional delay (Hymon, 2003). Because EDs are so crowded with patients, paramedics often must wait hours for the transported patient to be admitted to the ED. While the paramedics wait with the transported patient, they are unable to respond to other emergency calls. |
-
comes severe. ED overcrowding blocks access to emergency care, induces stress in providers and patients alike, and can lead to errors and impaired quality of care.
-
Boarding—A consequence of crowded EDs is the practice of boarding—holding a patient who needs to be admitted in the ED until an inpatient bed becomes available. In a nationwide survey of nearly 90 EDs across the country, conducted on a typical Monday evening, 73 percent of hospitals reported boarding two or more admitted patients. Boarding not only is frustrating and at times hazardous for the patient, but also adds to an already stressful work environment for physicians and nurses and enhances the potential for errors, delays in treatment, and diminished quality of care.
-
Ambulance diversion—When EDs become saturated to the point that
|
Even the most severely injured patients are affected by problems within the system. The L.A. Fire Department, which oversees EMS, has a departmentwide mandate that requires a maximum transport time of 30 minutes for trauma patients. However, it is difficult for paramedics to find an open trauma center within a 30-minute radius, so at times they deliver patients to non–trauma centers (regular EDs that are less well equipped to handle serious injuries). These types of situations occur almost every weekend in L.A. (California Healthline, 2004). The closure of L.A. County EDs and trauma centers can be attributed to financial pressures on hospitals, due particularly to the large volume of care they provide to uninsured patients. In fact, one in three ED patients in L.A. County is uninsured (Felch, 2004). Historically, about two-thirds of uninsured patients were served by the four county-run hospitals, while private hospitals cared for the remaining third. In 2003, however, because of cost concerns, the county changed its policies to limit the ability of private hospitals to transfer patients to the county hospitals. In the 14 months following the policy change, the number of uninsured doubled at some private hospitals and tripled at others (Felch, 2004). In 2002, L.A. County voters overwhelmingly approved (73 to 27 percent) a modest tax on building improvements to fund emergency services, trauma care, and bioterrorism preparedness efforts countywide. This was the first voter-approved increase in the property tax since the 1970s. The measure passed after a $1.5 million media campaign that warned voters of a system collapse unless the tax was approved. Advertisements for the measure showing feverish paramedics driving around the city looking for a hospital with available beds struck a cord with voters (L.A. County Online, 2005). The measure, although a step in the right direction, has been described as “a $170-million answer to a $700 million problem” (Trauma Tax Falls Short, 2004). More ED closures are expected in the county. |
-
patient safety is compromised, inbound ambulances may be diverted to alternative hospitals. Once a safety valve to be used in extreme situations, ambulance diversion has now become a commonplace event. A recent federal study reported that 501,000 ambulances were diverted in 2003, an average of 1 per minute. According to the American Hospital Association, nearly half of all hospitals, and close to 70 percent of urban hospitals, reported time on diversion in 2004. Ambulance diversions can lead to catastrophic delays in treatment for seriously ill or injured patients.
-
Uncompensated care—Hospital EDs are required by federal law to provide emergency care to all in need without regard for the patient’s ability to pay. No federal funding is allocated to offset the costs of this care. Uncompensated emergency and trauma care services can impose an extreme
-
financial burden on hospitals that see large numbers of uninsured patients. Substantial financial losses and ED and trauma center closures have been attributed to uncompensated emergency and trauma care.
-
Inefficient use of resources—Innovations in industrial engineering that have swept through other sectors of the economy, from banking to airlines to manufacturing, have failed to take hold in health care delivery. Tools and information technologies adapted from other industries could be used effectively to address the bottlenecks that occur in the flow of patients throughout the hospital and result in ED crowding. But hospitals have been slow to adopt these measures.
-
Inadequate surge capacity—Many hospitals are already operating at or over capacity. Because major hospital EDs are already crowded with patients and may even be boarding large numbers of inpatients, there is little or no surge capacity to absorb a large influx of patients from a significant mass casualty event. Furthermore, supplies of specialized equipment, such as personal protective equipment, negative pressure rooms, and ventilators, are inadequate to meet the demands of a major disaster or an epidemic.
-
Inadequate protection for staff—Hospital workers confront a host of daily hazards, from bloodborne and airborne pathogens to violent patients. Inadequate steps have been taken to protect hospital assets and staff in routine situations, let alone in the event of an infectious disease outbreak or a chemical or biological attack.
-
Inadequate supply of on-call specialists—One of the most troubling aspects of the current emergency and trauma care system is the lack of available specialists to provide on-call services to hospital EDs and trauma centers. This is particularly true for highly skilled specialties such as neurosurgery, interventional cardiology, and orthopedic surgery.
-
Medical liability—Emergency and trauma care providers, including hospitals, emergency and trauma physicians, and on-call specialists, face extraordinary liability exposure, leading many to limit the scope of their practice or stop assuming ED call.
-
Fragmented systems—Emergency care systems are highly fragmented. Emergency medical services (EMS) agencies, hospitals, trauma centers, public safety services (e.g., police and fire), and public health agencies often lack effective communications and fail to coordinate well across the continuum of emergency care. Coordinating the regional flow of patients is critical to ensuring that each patient is directed to the most appropriate setting for care, yet few systems nationwide have effective coordination between EMS and hospital EDs and trauma centers.
-
Lack of performance measurement and accountability—There is no standardized measurement or reporting of the performance of emergency and trauma care providers and systems. As a result, few people have any
-
real understanding of the quality of care they can expect to receive from their local emergency providers.
-
Inadequate research funding and infrastructure—Because emergency care is a relatively young field, it lacks a strong and stable research base within the National Institutes of Health and other agencies. Despite the importance of emergency and trauma care, research funding in the field lags well behind that in other fields.
IMPACT ON QUALITY AND PATIENT SAFETY
Quality and safety have been driving concerns of emergency care leaders for decades, and notable achievements in quality have been made. Improved care of patients with acute myocardial infarction, stroke, pneumonia, and sepsis are notable examples (Barron et al., 1999; Adams et al., 2002; Dellinger et al., 2004). Nonetheless, the numerous problems identified in this chapter have an impact on the quality and safety of the care provided by the system. The depth of this impact is difficult to determine. One way to assess the overall quality of the emergency care system is to consider the six quality aims defined by the Institute of Medicine (IOM) in Crossing the Quality Chasm: A New Health System for the 21st Century (IOM, 2001): care should be safe, effective, patient-centered, timely, efficient, and equitable (see Box 1-2). While the evidence base is limited, there are strong indications that the current emergency care system fails the American public in significant ways.
Safe
EDs are often high-risk, high-stress environments fraught with opportunities for error (Leape et al., 1991; Chisholm et al., 2000; Goldberg et al., 2002; Cosby, 2003; Weiss et al., 2004; Chamberlain et al., 2004; Selbst et al., 2004). A landmark study of hospitalized patients found that although the ED was the site of only 3 percent of adverse events, it was the site of 70 percent of those events attributed to negligence (Leape et al., 1991). Additional studies looking at hospital admissions and malpractice claims have also found the ED to be the site of a significant number of errors resulting in adverse events (Thomas et al., 2000). Two of the most common types of errors in the ED are failure to diagnose a patient properly (Leape et al., 1991; Weingart et al., 2000; Cosby, 2003; Thomas et al., 2004; White et al., 2004) and medication errors (IOM, 2006; Leape et al., 1991).
Errors in the ED are caused by multiple factors. ED staff are frequently interrupted in the course of their duties to attend to other patients or issues (Chisholm et al., 2001); are required to see a broad case mix of patients;
|
BOX 1-2 The Six Quality Aims of the Institute of Medicine’s Quality Chasm Report Health care should be: Safe—avoiding injuries to patients from the care that is intended to help them. Effective—providing services based on scientific knowledge to all who could benefit and refraining from providing services to those not likely to benefit. Patient-centered—providing care that is respectful of and responsive to individual patient preferences, needs, and values and ensuring that patient values guide all clinical decisions. Timely—reducing waits and sometimes harmful delays for both those who receive and those who give care. Efficient—avoiding waste, including waste of equipment, supplies, ideas, and energy. Equitable—providing care that does not vary in quality because of personal characteristics such as gender, ethnicity, geographic location, and socioeconomic status. SOURCE: IOM, 2001, Pp. 5–6. |
and must often make rapid clinical decisions, frequently without the benefit of medical histories or diagnostic tests (Selbst et al., 2004). Failures of communication or teamwork are significant problems in the ED, and in some cases have been shown to be direct contributors to adverse medical outcomes (Risser et al., 1999; White et al., 2004). The routine distractions of an ED are dramatically compounded when conditions are crowded. Problems include patients boarded in hallways for long periods; long waiting times; patients who decide to leave without being seen; others who demand to sign out against medical advice; and delays in diagnostic imaging, laboratory results, drug administration, and consultative support by on-call specialists.
Effective
In contrast to the surprisingly limited evidence base for a number of clinical practices that are widely used in the prehospital arena, hospital-based emergency care is substantially evidence based. In major tertiary hospitals, emergency and trauma care brings together the best of American medicine—highly trained, interdisciplinary teams of dedicated special-
ists armed with advanced medical technology. Beyond these large tertiary centers, however, the effectiveness of the system is less certain. Many community hospitals, especially in rural areas, do not have board-certified emergency physicians on staff. Many lack key specialists to back up their ED physicians. Furthermore, as discussed earlier, hospital EDs are often required to provide an enormous amount of primary care that would likely be provided better in other settings. Because ED physicians may not have access to the patient’s medical record, they cannot easily address primary care issues that go beyond the patient’s chief complaint. They have little or no opportunity for follow-up contact with patients, chronic care management, assurance of patient adherence to treatment, and coordination of care across providers and patient care settings.
Patient-Centered
EDs are designed to maximize visibility rather than to preserve patient privacy. At best they can hardly be considered patient-centered. A crowded ED, with its packed waiting rooms, long waiting times, and patients boarding in hallways, is even less so. Physicians and nurses find it nearly impossible to have a private conversation with a patient in such conditions. Injured or highly contagious patients may be placed in close proximity to children and individuals with only minor health problems who are using the ED for primary care.
Hospitals have begun to address these issues in a variety of ways. Some have established fast-track areas to deal with patients who are not truly emergency cases. Hospitals have also set up specialized areas, such as psychiatric and pediatric EDs within or adjacent to the main ED. Other approaches to making ED care more patient-centered include using bedside registration rather than making patients register first; sending physicians to the waiting room to see patients with simple problems, thus averting the need for long waits for an ED exam room; expediting inpatient admissions to clear crowded ED hallways; and treating pain more aggressively.
Timely
EDs are designed to provide timely care for unscheduled emergencies; nevertheless, timeliness of care in the ED is a growing concern. As noted, many patients experience long wait times before being seen, especially if they have a problem that is not immediately life-threatening, and the boarding of admitted patients who are waiting for an available inpatient bed has become commonplace. Long ED wait times can result in protracted pain and suffering and delays in diagnosis and treatment (Derlet et al., 2001; Derlet, 2002; James et al., 2005), and can lead some patients to leave without being seen
(Quinn et al., 2003) or to sign out against medical advice. Cognizant of these problems, ED staff and hospital administrators are attempting a variety of strategies to address them. Nevertheless, the problems persist.
Efficient
The health sector in general and emergency and trauma care services in particular lag behind other industries in adopting engineering principles and information technologies that can improve process management, lower costs, and enhance quality. Although EDs are quite efficient in some respects (they have diagnostic testing readily available and can complete in hours an in-depth evaluation that might otherwise require several days), they are highly dependent on hospital operations for efficient operation. When a hospital is full or its ancillary services are slow, ED crowding, inpatient board-ing, and ambulance diversion are almost inevitable. These are system failures that could be addressed through better overall management of hospital operations. There are other dimensions of inefficiency in emergency care as well. For example, the increasing amount of primary care delivered in EDs has important cost and quality implications, and may detract from the ED’s primary mission of providing emergency and lifesaving care. Further, the high degree of liability exposure in emergency and trauma care can lead to defensive medicine—the use of diagnostic tests and treatment measures primarily for the purpose of averting malpractice lawsuits (Lawthers et al., 1992; Berenson et al., 2003; Katz et al., 2005; Studdert et al., 2005).
Equitable
Disparities in the health care received by Americans on the basis of race and ethnicity were thoroughly documented in the IOM report Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care (IOM, 2003). Results of a small number of studies suggest that disparities may exist in access to emergency care and the treatment received. For example, there is evidence of variability in treatment, wait times, and insurance authorizations based on patients’ race and ethnicity (Lowe and Bindman, 1994; Todd et al., 2000; Bazarian et al., 2003; Richardson et al., 2003; James et al., 2005), although other researchers have reported that for a given level of severity of illness, the decision to admit an ED patient to the hospital does not appear to be influenced by the patient’s race, ethnicity, or payer status (Kellermann and Haley, 2003; Oster and Bindman, 2003). ED crowding, patient boarding, and ambulance diversion tend to be associated with large, urban medical centers, and thus have a disproportionate effect on racial and ethnic minorities that tend to dwell in the inner cities. Nonetheless, emergency care is arguably one of the more equitable settings in medicine, largely
because of the Emergency Medical Treatment and Active Labor Act, which has created a broad mandate to serve all, regardless of ability to pay.
PURPOSE OF THIS STUDY
While the problems discussed in this report are not new, they have largely been overlooked until now. Within the last several years, the complex problems facing the emergency care system have erupted into public view. Negative stories have increasingly appeared in the media regarding slow EMS response, ambulance diversions, trauma center closures, the medical malpractice crisis, ground and air crashes occurring during patient transport, and the frequent lack of on-call specialist coverage. The events of September 11, 2001, and more recent disasters, such as the train bombings in Madrid and Hurricane Katrina, have sharpened the public’s awareness of these issues.
The sponsors of this study—the Health Resources and Services Administration (HRSA), Emergency Medical Services for Children (EMS-C) program; the National Highway Traffic Safety Administration; the Agency for Healthcare Research and Quality; the Centers for Disease Control and Prevention, Center for Injury Prevention and Control; and the Josiah Macy, Jr. Foundation—requested that the IOM undertake a study aimed at assessing the current emergency care system, identifying its strengths and weaknesses, developing a comprehensive vision for the future of emergency care, and providing a blueprint for achieving that vision. The study was designed to encompass all of the key components of emergency care—prehospital EMS, hospital-based emergency care, trauma care, and injury prevention and control—in an integrated effort. The complete statement of task for the study committee is shown in Box 1-3.
This study builds on a large body of previous work, some conducted by the National Academies and some by other organizations. The landmark report Accidental Death and Disability: The Neglected Disease of Modern Society (NAS and NRC, 1966) first focused attention on the inadequacy of emergency and trauma care in the United States. This was followed by Injury in America: A Continuing Public Health Problem (NRC and IOM, 1985), which called for expanded research into the epidemiology and treatment of injury, and Reducing the Burden of Injury (IOM, 1999), which called for the development of a broad program for injury research, prevention, and control. The report Emergency Medical Services for Children (IOM, 1993) described the limited capacity of the developing emergency care system to address the special needs of children, and called for strong state and federal support for enhancements to emergency care education and training, infrastructure, research, and funding targeting the needs of children.
Other reports have touched on important specific aspects of emergency
|
BOX 1-3 Statement of Task for This Study The objectives of this study are to: (1) examine the emergency care system in the United States; (2) explore its strengths, limitations, and future challenges; (3) describe a desired vision of the emergency care system; and (4) recommend strategies required to achieve that vision. In this context, the Subcommittee on Hospital-Based Emergency Care will identify and address a wide range of issues, including:
|
care. A report of the Josiah Macy, Jr. Foundation, The Role of Emergency Medicine in the Future of American Medical Care (Josiah Macy, Jr. Foundation, 1995) examined the young specialty of emergency medicine and explored a vision for the future development of emergency medical practice, research, and care delivery. The IOM report A Shared Destiny: Community Effects of Uninsurance described the importance of the emergency care system to the national public health safety net and the enormous burden placed on hospitals by the growing uninsured population (IOM, 2004). To Err Is Human: Building a Safer Health System (IOM, 2000) and Crossing the Quality Chasm: A New Health System for the 21st Century (IOM, 2001) drew attention to the critical quality problems in health care, to which emergency care contributes significantly, and provided an important framework for assessing the performance of the emergency care system—the six quality aims reviewed above. Building a Better Delivery System: A New
Engineering/Health Care Partnership identified engineering and operations management tools from other industries that could be adapted to health care settings, assessed barriers to their adoption, and highlighted research opportunities for engineering applications to improve the health care delivery system (IOM, 2005).
In addition, a series of Emergency Medical Services Agenda for the Future reports sponsored by major federal agencies has addressed key issues. The original Emergency Medical Services Agenda for the Future (NHTSA, 1996), published in 1996, described a vision for an integrated emergency care system of the future, while a companion report, Emergency Medical Services Agenda for the Future: Implementation Guide (NHTSA, 1998) outlined specific steps for achieving that vision. Detailed assessments were then provided in Emergency Medical Services Education Agenda for the Future: A Systems Approach (NHTSA, 2000), National EMS Research Agenda (NHTSA, 2001a), Rural and Frontier Emergency Medical Services Agenda for the Future (NHTSA, 2003), Trauma System Agenda for the Future (NHTSA, 2001b), and CDC Acute Injury Care Research Agenda: Guiding Research for the Future (CDC National Center for Injury Control and Prevention, 2005).
As important as these preceding efforts have been, progress in implementing needed reforms has been slow, and much work remains to be done. Deeply entrenched parochial interests have impeded progress, and today the field is as fragmented as ever. Accountability remains dispersed, and there is little public understanding of either the importance or the profound limitations of emergency and trauma care.
STUDY SCOPE
The scope of this study is broad, like the field of emergency care itself. It encompasses the full range of activities associated with emergency care, including first aid and cardiopulmonary resuscitation (CPR) rendered by bystanders; 9-1-1 and dispatch; emergency medical response and treatment at the scene; transport of patients via ambulance or air medical service; emergency assessment and treatment at the hospital ED or trauma center; critical care services in the operating room, the intensive care unit, or other inpatient departments; interfacility transport of patients; treatment in specialized facilities such as burn, stroke, and cardiac centers, as well as children’s hospitals; and access to follow-up in community-based referral sites, such as primary care practices, skilled nursing facilities, psychiatric hospitals, and substance abuse clinics.
Emergency care is unique in the health field because it operates at the intersection of medical care, public health, and public safety. Consequently, the study views emergency care from all three perspectives. In addition to
exploring the traditional role of the emergency care system as provider of urgent and lifesaving care, the study considers the system’s roles in public health—including surveillance to detect injury trends and disease outbreaks—and as a critical component of the public safety net. Also addressed are the multiple interactions between emergency care and community providers: urgent care that can substitute for ED services, use of the emergency care system as an adjunct to physician practices, and the role of preventive services and chronic care management that can reduce the need for emergency services. The study further considers emergency care’s public safety role and its intersection with police, fire, and emergency management services. Finally, emergency care is examined within a systems framework: how the many components of the system, such as EDs, EMS, community providers, and on-call specialists, work together—or frequently fail to work together—to achieve a level of performance for the system as a whole.
STUDY APPROACH
The committee was structured to balance the desire for an integrated, systems approach to the study with an interest in placing focused attention on hospital-based, EMS, and pediatric emergency care issues. The result was a main committee and three subcommittees representing the latter three focus areas (see Figure 1-1).
The main committee guided the overall study process and separately addressed a set of overarching systemwide issues. The three subcommittees examined the unique challenges associated with hospital-based emergency and trauma care, prehospital EMS, and the provision of emergency services to children. The membership of the main committee and subcommittees overlapped—the 11-member pediatric subcommittee, for example, included
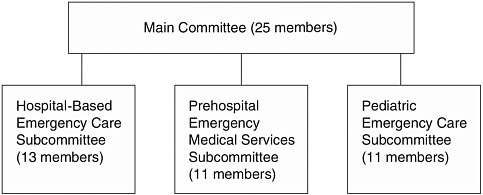
FIGURE 1-1 Committee and subcommittee structure.
5 members from the main committee. Subcommittees met both separately— reporting their discussions and findings to the main committee—and in a combined session with the main committee. A total of 40 individuals1 served across all four committees (see Appendix A). Biographical information on each committee member is contained in Appendix B.
The committee and subcommittees held 17 meetings from February 2004 through October 2005, heard testimony from a wide range of experts (see Appendix C), and commissioned 11 technical papers (see Appendix D). Staff and committee members met with a variety of stakeholders and interested individuals, conducted study visits, and participated in public meetings sponsored by stakeholder groups and the study sponsors.
A NOTE ABOUT TERMINOLOGY
There is substantial confusion about terminology in emergency care. To ensure clarity and consistency, this study uses the following terminology throughout. Emergency medical services, or EMS, denotes prehospital emergency medical services, such as 9-1-1 and dispatch, emergency medical response, field triage and stabilization, and transport by ambulance or helicopter to a hospital and between facilities. EMS system refers to the organized delivery system for EMS within a specified geographic area—local, regional, state, or national—as indicated by the context.
Emergency care is defined more broadly than EMS and encompasses the full continuum of services involved in emergency medical care, including EMS, hospital-based emergency and trauma care, on-call specialty care, bystander care, and injury prevention and control. Emergency care system refers to the organized delivery system for emergency care within a specified geographic area. It is important to note that the committee’s definitions of emergency care and emergency care system may be narrower than other definitions, such as those used by the federal Emergency Medical Services for Children program, which also encompass injury prevention and rehabilitation services.
Trauma care is the care received by a victim of trauma in any setting, while a trauma center is a hospital specifically designated to provide trauma care. Some trauma care is provided in settings other than a trauma center. Trauma system refers to the organized delivery system for trauma care at the local, regional, state, or national level. Trauma care is an essential component of emergency care. Primary care and ambulatory care are often mentioned in the context of the expanding role of the ED. Such care is usually described as the first point of care for patients except in emergencies.
It is typically office- or clinic-based medical care that includes diagnosis, treatment, prevention, and ongoing care management, and can include the establishment of patient–physician relationships and continuity of care over time. Ambulatory care is all care that is provided outside the hospital. Primary care is a subset of ambulatory care; however, the two are used somewhat interchangeably throughout the report to indicate the type of care that is typically given outside of the hospital but is increasingly being delivered in EDs.
For the purposes of this report, the terms children and pediatric denote infants, children, and adolescents through age 18. To avoid confusion, the terms emergency medical services for children and EMS-C denote the HRSA program itself.
ORGANIZATION OF THE REPORT
This report—one of a series of three—summarizes the committee’s findings and recommendations regarding hospital-based emergency care:
-
Chapter 2 describes the evolution of emergency and trauma care and the multiple roles currently served by the emergency care system—from care for those in urgent need to primary care for the uninsured, public health surveillance, and preparation for disasters.
-
Chapter 3 defines the committee’s broad vision for an emergency care system that is coordinated, regionalized, and accountable.
-
Chapter 4 considers the efficiency of emergency and trauma care in the context of other industries, and explores applications of engineering techniques that could be used to improve the efficiency and quality of emergency services.
-
Chapter 5 takes a focused look at the array of new information and clinical technologies that have the potential to transform medicine and emergency care over the next two decades, and offers guidance on how to prioritize these technologies to enhance emergency care most cost-effectively.
-
Chapter 6 addresses workforce issues and focuses on one of the most serious problems confronting emergency and trauma care today—the shortage of specialists available to take emergency call. It also addresses the neglected problem of provider safety and the need for better protection from the day-to-day hazards encountered in emergency care, a theme echoed in the next chapter in the context of biological and chemical threats.
-
Chapter 7 deals with disaster preparedness and the current lack of hospital capacity to address normal surges in ED visits, much less a major mass casualty event.
-
Chapter 8 describes the significant achievements of emergency and trauma care research and the vast range of opportunities for expanding
-
the evidence base in basic, clinical, and health systems–oriented research. It also considers the meager funding that supports this critically important enterprise.
-
Appendix A contains a chart of all committee and subcommittee members.
-
Appendix B contains biographical information for members of the main committee and the Subcommittee on Hospital-Based Emergency Care.
-
Appendix C lists the presentations that were made during public sessions of the committee meetings.
-
Appendix D lists the research papers commissioned by the committee.
-
Appendix E provides additional statistical information about ED utilization, supplementing that in Chapter 2.
-
Appendix F also supplements Chapter 2 by providing a description of the historical development of the emergency and trauma care fields.
-
Appendix G summarizes the recommendations from all three reports in the Future of Emergency Care series in a table that indicates the entity with primary responsibility for implementing each recommendation.
REFERENCES
Adams R, Acker J, Alberts M, Andrews L, Atkinson R, Fenelon K, Furlan A, Girgus M, Horton K, Hughes R, Koroshetz W, Latchaw R, Magnis E, Mayberg M, Pancioli A, Robertson RM, Shephard T, Smith R, Smith SC Jr, Smith S, Stranne SK, Kenton EJ III, Bashe G, Chavez A, Goldstein L, Hodosh R, Keitel C, Kelly-Hayes M, Leonard A, Morgenstern L, Wood JO. 2002. Recommendations for improving the quality of care through stroke centers and systems: An examination of stroke center identification options. Multidisciplinary consensus recommendations from the Advisory Working Group on Stroke Center Identification Options of the American Stroke Association. Stroke 33(1):e1–e7.
AHRQ (Agency for Healthcare Research and Quality). 2006. Costs of Treating Trauma Disorders Now Comparable to Medical Expenses for Heart Disease. [Online]. Available: http://www.ahrq.gov/news/nn/nn012506.htm [accessed May 16, 2006].
Asplin BR, Magid DJ, Rhodes KV, Solberg LI, Lurie N, Camargo CA Jr. 2003. A conceptual model of emergency department crowding. Annals of Emergency Medicine 42(2):173–180.
Barron HV, Rundle A, Gurwitz J, Tiefenbrunn A. 1999. Reperfusion therapy for acute myocardial infarction: Observations from the national registry of myocardial infarction 2. Cardiology in Review 7(3):156–160.
Bazarian JJ, Pope C, McClung J, Cheng YT, Flesher W. 2003. Ethnic and racial disparities in emergency department care for mild traumatic brain injury. Academic Emergency Medicine 10(11):1209–1217.
Berenson RA, Kuo S, May JH. 2003. Medical malpractice liability crisis meets markets: Stress in unexpected places. Issue Brief (Center for Studying Health System Change) (68):1–7.
California Healthline. 2004. Emergency Department, Trauma Unit Closures Increasing Patient Wait Times in Los Angeles County. [Online]. Available: http://www.californiahealthline.org/index.cfm?action=dspItem&itemid=107158 [accessed January 5, 2006].
CDC (Centers for Disease Control and Prevention) National Center for Injury Control and Prevention. 2005. CDC Acute Injury Care Research Agenda: Guiding Research for the Future. Atlanta, GA: CDC.
Chamberlain J, Slonim A, Joseph J. 2004. Reducing errors and promoting safety in pediatric emergency care. Ambulatory Pediatrics 4(1):55–63.
Chisholm CD, Collison EK, Nelson DR, Cordell WH. 2000. Emergency department workplace interruptions: Are emergency physicians “interrupt-driven” and “multitasking”? Academic Emergency Medicine 7(11):1239–1243.
Chisholm CD, Dornfeld AM, Nelson DR, Cordell WH. 2001. Work interrupted: A comparison of workplace interruptions in emergency departments and primary care offices. Annals of Emergency Medicine 38(2):146–151.
Cosby KS. 2003. A framework for classifying factors that contribute to error in the emergency department. Annals of Emergency Medicine 42(6):815–823.
Dellinger RP, Carlet JM, Masur H, Gerlach H, Calandra T, Cohen J, Gea-Banacloche J, Keh D, Marshall JC, Parker MM, Ramsay G, Zimmerman JL, Vincent JL, Levy MM, Surviving Sepsis Campaign Management Guidelines Committee. 2004. Surviving sepsis campaign guidelines for management of severe sepsis and septic shock. Critical Care Medicine 32(3):858–873.
Derlet RW. 2002. Overcrowding in emergency departments: Increased demand and decreased capacity. Annals of Emergency Medicine 39(4):430–432.
Derlet R, Richards J, Kravitz R. 2001. Frequent overcrowding in U.S. emergency departments. Academic Emergency Medicine 8(2):151–155.
Felch J. 2004, August 24. Domino effect feared from closures of emergency rooms. Los Angeles Times. P. A1.
GAO (U.S. Government Accountability Office). 2001. Emergency Care: EMTALA Implementation and Enforcement Issues. Washington, DC: U.S. Government Printing Office.
Goldberg R, Kuhn G, Andrew L, Thomas H. 2002. Coping with medical mistakes and errors in judgment. Annals of Emergency Medicine 39(3):287–292.
Hymon S. 2003, December 19. Study cites paramedic response delay crews are often unable to take urgent calls because they are waiting for patients to be admitted to an ER. Los Angeles Times. P. B3.
IOM (Institute of Medicine). 1993. Emergency Medical Services for Children. Washington, DC: National Academy Press.
IOM. 1999. Reducing the Burden of Injury. Washington, DC: National Academy Press.
IOM. 2000. To Err Is Human: Building a Safer Health System. Washington, DC: National Academy Press.
IOM. 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
IOM. 2003. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: The National Academies Press.
IOM. 2004. A Shared Destiny: Community Effects of Uninsurance. Washington, DC: The National Academies Press.
IOM. 2005. Building a Better Delivery System: A New Engineering/Health Care Partnership. Washington, DC: The National Academies Press.
IOM. 2006. Preventing Medication Errors. Washington, DC: The National Academies Press.
James CA, Bourgeois FT, Shannon MW. 2005. Association of race/ethnicity with emergency department wait times. Pediatrics 115(3):e310–e315.
Josiah Macy, Jr. Foundation. 1995. The Role of Emergency Medicine in the Future of American Medical Care. New York, NY: Josiah Macy, Jr. Foundation.
Katz DA, Williams GC, Brown RL, Aufderheide TP, Bogner M, Rahko PS, Selker HP. 2005. Emergency physicians’ fear of malpractice in evaluating patients with possible acute cardiac ischemia. Annals of Emergency Medicine 46(6):525–533.
Kellermann AL, Haley LH. 2003. Hospital emergency departments: Where the doctor is always “in.” Medical Care 41(2):195–197.
L.A. County Online. 2005. General Info: Overview. [Online]. Available: http://lacounty.info/ overview.htm [accessed February 1, 2006].
Lawthers AG, Localio AR, Laird NM, Lipsitz S, Hebert L, Brennan TA. 1992. Physicians’ perceptions of the risk of being sued. Journal of Health Politics, Policy and Law 17(3):463–482.
Leape L, Brennan TA, Laird N, Lawthers AG, Localio AR, Barnes BA, Hebert L, Newhouse JP, Weiler PC, Hiatt H. 1991. The nature of adverse events in hospitalized patients: Results of the Harvard medical practice study. New England Journal of Medicine 324:377–384.
Lowe RA, Bindman AB. 1994. The ED and triage of nonurgent patients. Annals of Emergency Medicine 24(5):990–992.
NAS, NRC (National Academy of Sciences, National Research Council). 1966. Accidental Death and Disability: The Neglected Disease of Modern Society. Washington, DC: National Academy of Sciences.
NHTSA (National Highway Traffic Safety Administration). 1996. Emergency Medical Services Agenda for the Future (U.S. Department of Transportation, HS 808441). Washington, DC: U.S. Government Printing Office.
NHTSA. 1998. Emergency Medical Services Agenda for the Future: Implementation Guide. Washington, DC: U.S. Department of Transportation.
NHTSA. 2000. Emergency Medical Services Education Agenda for the Future: A Systems Approach. Washington, DC: U.S. Department of Transportation.
NHTSA. 2001a. National EMS Research Agenda. Washington, DC: U.S. Department of Transportation.
NHTSA. 2001b. Trauma System Agenda for the Future. Washington, DC: U.S. Department of Transportation.
NHTSA. 2003. Rural and Frontier Emergency Medical Services Agenda for the Future. Washington, DC: NHTSA.
NRC, IOM (National Research Council, Institute of Medicine). 1985. Injury in America: A Continuing Public Health Problem. Washington, DC: National Academy Press.
Oster A, Bindman AB. 2003. Emergency department visits for ambulatory care sensitive conditions: Insights into preventable hospitalizations. Medical Care 41(2):198–207.
Quinn JV, Polevoi SK, Kramer NR, Callaham ML. 2003. Factors associated with patients who leave without being seen. Academic Emergency Medicine 10(5):523–524.
Richardson LD, Babcock Irvin C, Tamayo-Sarver JH. 2003. Racial and ethnic disparities in the clinical practice of emergency medicine. Academic Emergency Medicine 10(11):1184–1188.
Risser DT, Rice MM, Salisbury ML, Simon R, Jay GD, Berns SD. 1999. The potential for improved teamwork to reduce medical errors in the emergency department. The MedTeams Research Consortium. Annals of Emergency Medicine 34(3):373–383.
Robes K. 2005. Medical center may close ER: Rising cost of uninsured patient care part of the problem. Long Beach Press Telegram.
Schafermeyer RW, Asplin BR. 2003. Hospital and emergency department crowding in the United States. Emergency Medicine (Fremantle, W.A.) 15(1):22–27.
Selbst SM, Levine S, Mull C, Bradford K, Friedman M. 2004. Preventing medical errors in pediatric emergency medicine. Pediatric Emergency Care 20(10):702–709.
South Bay’s ERs Are in a State of Emergency. 2005, February 6. South Bay Daily Breeze.
Studdert DM, Mello MM, Sage WM, DesRoches CM, Peugh J, Zapert K, Brennan TA. 2005. Defensive medicine among high-risk specialist physicians in a volatile malpractice environment. Journal of the American Medical Association 293(21):2609–2617.
Sussman D. 2000, May 25. Emergency shutdown: ER closures place patient care in jeopardy. Nurse Week.com. [Online]. Available: http://www.nurseweek.com/features/00-05/er.html [accessed January 16, 2006].
Thomas EJ, Studdert DM, Burstin HR, Orav EJ, Zeena T, Williams EJ, Howard KM, Weiler PC, Brennan TA. 2000. Incidence and types of adverse events and negligent care in Utah and Colorado. Medical Care 38(3):261–271.
Thomas M, Morton R, Mackway-Jones K. 2004. Identifying and comparing risks in emergency medicine. Emergency Medicine Journal 21(4):469–472.
Todd K, Deaton C, D’Adamo A, Goe L. 2000. Ethnicity and analgesic practice. Annals of Emergency Medicine 35(1):11–16.
Trauma Tax Falls Short. 2004, August 27. Los Angeles Times. P. B12.
Weingart SN, Wilson RM, Gibberd RW, Harrison B. 2000. Epidemiology of medical error. British Medical Journal 320(7237):774–777.
Weiss SJ, Derlet R, Arndahl J, Ernst AA, Richards J, Fernandez-Frackelton M, Schwab R, Stair TO, Vicellio P, Levy D, Brautigan M, Johnson A, Nick TG. 2004. Estimating the degree of emergency department overcrowding in academic medical centers: Results of the national ED overcrowding study (NEDOCs). Academic Emergency Medicine 11(1):38–50.
White AA, Wright SW, Blanco R, Lemonds B, Sisco J, Bledsoe S, Irwin C, Isenhour J, Pichert JW. 2004. Cause-and-effect analysis of risk management files to assess patient care in the emergency department. Academic Emergency Medicine 11(10):1035–1041.




















