8
Home
Families can play an essential role in preventing childhood obesity. The Institute of Medicine (IOM) Health in the Balance report proposed a set of recommended actions for families and the home environment (Box 8-1) (IOM, 2005). The central recommendation is that parents should promote healthful eating behaviors and regular physical activity for their children. In addition, as noted throughout that report, actions need to be taken by government, industry, communities, and schools that will provide an environment that supports and reinforces the healthy behaviors promoted at home.
Parents and other household caregivers are influential role models, policy makers, and change agents in the home. They can control the home environment, monitor their children’s and adolescents’ behaviors, set goals for the family or household, reward successful behavioral changes, address problems to overcome barriers to change, and apply their parenting skills to maintain in their households attitudes and actions that are consistent with healthy behaviors (Dietz and Robinson, 2005). For example, if toddlers and young children are given multiple opportunities to try new foods without being coerced to eat them, many of the foods, including fruits and vegetables, will become a part of their diet even if they initially reject them (Birch and Marlin, 1982; Wardle et al., 2003).
Because parents and other caregivers are often strong influences in their children’s lives, many of the policies and programs implemented in other settings (e.g., schools, communities, and the marketplace) target behaviors that manifest in the family and home context. Thus, the home environment
|
BOX 8-1 Recommendations for the Home from Preventing Childhood Obesity: Health in the Balance Parents should promote healthful eating behaviors and regular physical activity for their children. To implement this recommendation parents can
SOURCE: IOM (2005). |
represents a setting that is particularly relevant to the prevention of childhood obesity. Parents and families can respond to policy changes and initiatives implemented in other settings. For example, if communities develop safe walkways and bikeways or initiate neighborhood farmers markets, parents can encourage family involvement in physical activity or purchasing fresh produce in these settings. If industry creates healthier calorie-controlled packaged foods and beverages, then adults and adolescents can purchase these products and work to ensure that nutrition is a priority when they plan meals for their families.
Parents can serve as advocates to promote changes that encourage and support healthy choices in their children’s schools and communities as well as in their homes. Parents’ Action for Children, a nonprofit organization dedicated to advancing the interests of families and children, suggests that parents get involved in their children’s school wellness programs (Mansukhani, 2005).
Other useful resources that provide guidance to parents are the Parents as Teachers National Center (2005), which works to expand parents’ knowledge of early childhood development and to improve parenting practices, as well as the resources and support provided by the national Parent
Teacher Association to promote health and wellness and prevent obesity (PTA, 2006). Parents can make the school environment healthier by advocating for the greater availability of low-calorie and nutrient-dense food and beverage products in vending machines and expanding opportunities for their children to be physically active throughout the school day. The Child Nutrition and WIC (Special Supplemental Nutrition Program for Women, Infants, and Children) Reauthorization Act of 2004 (Public Law 108-265) required school districts to involve parents in the process of establishing a local school wellness policy by the 2006–2007 school year (CNWICRA, 2004) (Chapters 4 and 7).
State-level efforts are also actively engaging parents. Recent legislation proposed or passed in many states requires parental representation on state and school advisory committees or task forces established to prevent childhood obesity (CDC, 2005; NCSL, 2006). For example, elementary, middle, and junior high schools in Texas are required to adopt by 2007 a state-approved coordinated school health program that includes a strong parental involvement component (Texas Department of State Health Services, 2006). Additionally, Oklahoma enacted legislation that requires each public school to establish a Healthy and Fit School Advisory Committee comprised of teachers, administrators, parents, health care professionals, and business community representatives to examine and make recommendations to the school principal regarding health education, physical education and physical activity, and nutrition and health services (NCSL, 2006).
OPPORTUNITIES AND CHALLENGES
Families in the United States face many potential opportunities and challenges that influence the efforts of household members to engage in healthy behaviors. The challenges include the stresses and pressures of daily living, along with economic and time constraints that make healthful eating and daily physical activity difficult for many families to achieve (Devine et al., 2003). The Health in the Balance report acknowledged that since the early 1970s expanded job opportunities as well as economic necessities have led to the entry of more women into the work force (IOM, 2005). In an estimated 62.4 percent of two-parent households, both parents are working; and in single-parent households, more than three-quarters of mothers (77.1 percent) and fathers (88.7 percent) are working (Fields, 2003). In 2004, both parents of 59 percent of children under 6 years of age were in the labor force and neither parent of 10 percent of children under 6 years of age was in the work force (Annie E. Casey Foundation, 2006). In addition to long work and commute hours, many families have busy schedules, with both parents and their children participating in activities outside the home, all of which can lead to reduced time for free play or for families to engage
in physical activity together. Family meals may also be more irregular, and family members with busy schedules may rely more on take-out meals and fast food (Devine et al., 2003).
McIntosh and colleagues (2006) conducted an analysis of more than 300 household telephone interviews and self-administered questionnaires and examined the effects of parental work experiences on selected aspects of children’s diet and health. Children’s and youths’ percentage of total calories from fat and saturated fat were examined in relation to their waist circumference and body mass index (BMI). The findings showed that household income, the quality and amount of parental time spent with their children, and parents’ work experiences are associated with the total calorie and fat intake and obesity-related outcomes for children and youth ages 9 to 15 years. Mothers’ behaviors tended to be more closely associated with their children’s dietary intake than fathers’ behaviors. Additionally, the characteristics and behaviors of both parents were strongly related to the behaviors of younger children ages 9 to 11 years than youth ages 13 to 15 years (McIntosh et al., 2006).
Family meals may have an important role in promoting positive dietary intakes in adolescents. Teens who consume meals with their families more frequently or who assist with the preparation of dinner for their families report higher intakes of fruits, vegetables, grains, and essential nutrients and lower intakes of low-nutrient foods, such as sweetened soft drinks and dietary fat, and are at lower risk for developing eating disorders (Larson et al., 2006; Neumark-Sztainer, 2006; Neumark-Sztainer et al., 2003). Adolescents living in families that prioritize eating meals together, provide structure around meals, and maintain an enjoyable meal-time atmosphere are less likely to engage in less healthful dietary practices and dieting behaviors. However, it has been suggested that a challenge for families, given current work and other life pressures, is the establishment of broader social networks to support healthful family meals (Neumark-Sztainer, 2006).
Another formidable challenge that parents face is the conflicted relationship that they have with television in their families. Although some parents have guidelines for the content of what their children view, especially in entertainment media, few parents appear to have rules restricting the amount of time that their children spend watching television (Hersey and Jordan, 2006). Moreover, the vast majority of families have multiple televisions in their homes, with children and teens often having televisions in their bedrooms (Rideout, 2004; Roberts et al., 2005).
Parents have identified several barriers to reducing television viewing to two hours or less per day, as recommended by the Health in the Balance report (IOM, 2005), the American Academy of Pediatrics (AAP, 2001), and Healthy People 2010 (DHHS, 2000). These barriers include their own heavy television viewing habits, the use of television as a safe and afford-
able distraction for their children, the central role that television plays in family routines (e.g., relaxing, eating, and falling asleep), and the perspective that children should choose how to spend their leisure time (Hersey and Jordan, 2006; Rideout and Hamel, 2006). Parents often use electronic media such as television to manage busy family schedules, maintain peace in the household, facilitate family routines with their children, and teach their children things that parents do not have the time to teach themselves (Rideout and Hamel, 2006).
Several promising strategies can facilitate bringing about reductions in children’s television viewing time, although they have not yet been fully evaluated. These strategies include encouraging parents to refrain from placing a television in their child’s bedroom, establishing family rules about television viewing when children are young and consistently enforcing the rules, limiting the amount of time that children can watch television and use other electronic media on school days, not placing a television in household eating areas, disconnecting television viewing with eating meals or snacks, being attentive to how much time children spend with electronic media during their leisure time, and role modeling by limiting parental television viewing (Hersey and Jordan, 2006). School-based curricula promoting some of these behaviors have proven effective in reducing the sedentary television viewing habits of children (Robinson, 1999), adolescents (Gortmaker et al., 1999), and other family members (Robinson and Borzekowski, 2006).
Life experiences and opportunities are associated with the knowledge and behaviors of parents and caregivers. Demographic factors and personal perceptions about obesity are associated with parents’ readiness to help their children who are obese or who are at risk for obesity to lose weight (Rhee et al., 2005). A review of barriers and facilitating factors for healthful eating among 11- to 16-year-olds found that family support, the broad availability of foods and beverages that contribute to a healthful diet, and a desire to take care of one’s appearance were important factors in promoting healthy choices (Shepherd et al., 2006). Other barriers to changing adolescents’ behaviors include adolescents’ perceptions of low levels of caring by their parents, the difficulty that adolescents have with talking to their parents about problems, and the fact that adolescents value their friends’ opinions over their parents’ opinions for serious decisions. The feelings accompanying these barriers were associated with body dissatisfaction, depression, and low self-esteem (Ackard et al., 2006). If parents are unwilling or unable to change family behaviors, then interventions to promote positive lifestyle behaviors for the family are unlikely to be effective.
An additional challenge is a belief held by some that obesity is primarily an issue of personal or family responsibility and that government should not intervene in the home environment. This perspective makes it difficult to directly influence family behaviors and leads to a situation in
difficult to directly influence family behaviors and leads to a situation in which parents face even greater obstacles to providing a healthy home environment.
Parents and caregivers are often unaware that their child is obese or at risk for obesity. A study conducted by the Centers for Disease Control and Prevention (CDC) showed that one-third of mothers of obese 2- to 11-year-old children thought that their child’s weight was in the normal range (Maynard et al., 2003). In another study, parents involved in the Fit WIC pilot program of the U.S. Department of Agriculture (USDA), which was designed to evaluate social and environmental approaches to the prevention of obesity, showed that many parents of obese preschoolers neither viewed their children as being obese, nor were they concerned about their children’s weight (USDA, 2005b). Thus, it is important for health care providers to discuss with parents and caregivers their child’s weight and BMI, and the important roles of nutrition and physical activity in the promotion of normal growth and development and a healthy weight in their child.
Health care providers face several challenges when they address childhood obesity (Chapter 6). They report that they are often reluctant to discuss obesity with families because of the associated stigma, concern that parents will feel blamed, and apprehension that a discussion of weight may lead to unintended consequences, such as further stigmatization or an eating disorder. A neutral, nonjudgmental approach to weight management and obesity prevention may help parents and caregivers take responsibility for helping their children and teens reach a healthy weight and also assess the family’s readiness to change (Dietz and Robinson, 2005). Ongoing efforts are focused on assisting individual health care providers with becoming more informed and comfortable with counseling children and their parents about obesity. Professional health care organizations such as the American Academy of Family Physicians, the American Academy of Pediatrics (AAP), and the American Dietetic Association provide evidence-based position statements, online patient and provider tool kits, and websites to help them manage obesity in children and adolescents (AAFP, 2004; AAP, 2006b; Ritchie et al., 2006).
The use of a combination of family-based and school-based multicomponent programs may more likely be effective at preventing obesity in children and youth if they address both the physical environment (e.g., food availability and portion size or access to opportunities for physical activity) and the social environment (e.g., socioeconomic and sociocultural factors and the mealtime structure) (Patrick and Nicklas, 2005). It has been suggested that multifaceted interventions should include the promotion of physical activity, parent training and modeling, behavioral counseling, and nutrition education for children and youth (Ritchie et al., 2006). Additionally, an integrated approach that promotes both healthy eating and physical
activity choices and the acceptance of diverse body shapes and sizes among children and youth may have a greater likelihood of preventing both obesity and eating disorders and the health consequences of these weight-related eating disorders (Neumark-Sztainer, 2005a).
Although childhood obesity treatment research has demonstrated the importance of involving parents in interventions to change obese children’s and adolescents’ dietary and physical activity behaviors (Epstein et al., 1990), the challenges identified have contributed to the modest efficacies of parent and family interventions in obesity prevention studies. Challenges that remain in the home setting are motivating parents and families to participate in obesity prevention programs (Perry et al., 1989) and designing and implementing evaluations to assess changes in the home environment. Even when the level of parent participation is high, family-based interventions that have been evaluated have generally only produced relatively modest short-term effects on behavioral outcomes with limited effects on children’s BMI levels and other anthropometric and health outcomes (Hearn et al., 1992; Nader et al., 1983; Perry et al., 1987, 1989; Vega et al., 1988).
For example, in a study of a home correspondence intervention for families of third grade students in Minnesota and North Dakota, a parent participation rate of 86 percent was achieved and the home-only and home-plus-school curriculum groups reported significant improvements in targeted dietary behaviors compared with the improvements for the school-curriculum-only and untreated control groups. There were no significant changes in anthropometric measures, however, and the dietary behavior differences were not maintained at a one-year follow-up (Perry et al., 1989).
Similarly, the large National Heart, Lung, and Blood Institute’s (NHLBI’s) Child and Adolescent Trial for Cardiovascular Health found only modest added benefits of the family intervention when it was combined with a school intervention in a comparison with the school intervention alone (Luepker et al., 1996). Parent-child interventions implemented independently of school programs have also had limited effects. A 12-week culturally tailored obesity prevention program for African-American mothers and daughters in households of low socioeconomic status resulted in statistically significant improvements in mothers’ self-reported diets; but only minimal behavioral changes were observed for their daughters, and there were no significant changes in the daughters’ BMI levels (Stolley and Fitzgibbon, 1997).
To intervene earlier in childhood, parents and families of preschool-aged children have recently been targeted by prevention programs. For example, a 16-week controlled trial that involved 43 American-Indian mothers of preschool-aged children used peer educators to deliver a home-based childhood obesity prevention program that included encouraging parental
role modeling of healthy eating behaviors and establishing household rules about food and beverage choices. The trial produced nonstatistically significant differences between groups, although there was a trend toward lower weight for height and lower calorie intakes for children in the intervention group compared with those for the group receiving standard home-based parenting sessions (Harvey-Berino and Rourke, 2003). No differences between groups in the percentage of preschool children who were obese or at risk for obesity or in the children’s physical activity levels emerged. There also were no differences in the mothers’ BMIs, dietary intakes, or activity levels.
In 1999, the USDA began funding Fit WIC, an initiative to support and evaluate social and environmental approaches to the prevention and reduction of the levels of obesity in preschool children ages 2 to 4 years. Four state WIC programs (California, Kentucky, Vermont, Virginia) and the Inter-Tribal Council of Arizona were funded for a 3-year period to identify ways in which WIC could respond to the childhood obesity epidemic for program participants (USDA, 2005b) (Chapter 4).
Evaluation results of the Fit WIC pilot program in Virginia compared participating parents’ behaviors in the intervention WIC clinic with those of parents at a non-randomly selected control WIC site. Parents who participated in the program were encouraged to perform six behaviors that affect their children. These included increasing their physical activity, monitoring mealtime behaviors, limiting household television, offering water instead of sweetened beverages, consuming five fruits and vegetables per day, and increasing family activities to promote physical fitness. WIC staff was asked to model these behaviors for parents, and complementary educational materials were sent to community agencies serving WIC clients. After one year of the intervention, Fit WIC program participants reported that they more frequently offered water to their children and more frequently engaged in more active play with their children than the participants at the comparison site (McGarvey et al., 2004). However, in the evaluation, limited and differential follow-up response rates and ethnic differences between the intervention and control sites complicated the attribution of differences between the groups to the Fit WIC intervention.
A promising preschool intervention that has been evaluated is Hip-Hop to Health Jr., a two-year randomized controlled trial with 420 low-income, predominantly African-American children enrolled in the Head Start program at 12 sites (Fitzgibbon et al., 2005). A 14-week intervention included 20-minute healthy eating or physical activity educational lessons and 20 minutes of aerobic activity three times per week. Control group participants received general health education on a weekly basis. The parents of the children received newsletters and homework assignments on a weekly basis and a $5.00 gift certificate for each completed assignment. After the
intervention there were no differences in BMI levels between the groups. After one year of follow-up, the change in BMI levels (adjusted for age and baseline BMI) was significantly less for the treatment group. Smaller but statistically significant effects were maintained after two years (Fitzgibbon et al., 2005).
A systematic evidence-based review of obesity interventions for children and youth showed that multicomponent family-based programs are the most likely to be effective for children ages 5 to 12 years. However, there is limited evidence regarding effective obesity interventions for adolescents ages 13 years and older (Ritchie et al., 2006). Although there is the potential for a range of childhood obesity prevention interventions that involve parents and families, much more remains to be learned about effective strategies and how these strategies can be widely disseminated across various contexts.
CURRENT EFFORTS
Many different ongoing efforts are focused on improving dietary patterns, increasing physical activity, and preventing childhood obesity in the home environment. However, evaluations of the interventions are generally not performed; therefore there is limited evidence of whether and how these efforts may assist families, whether they have effects on family lifestyles, or even whether they produce unintended adverse effects and outcomes. Federal, state, and local government programs, as well as industry, community, and school-based efforts, often focus on reaching parents and their children at home or include a family-based component.
We Can! (Ways to Enhance Children’s Activity and Nutrition) is a collaborative effort of four institutes of the National Institutes of Health (NIH)1 and is one of many government-funded obesity prevention interventions focused on families. We Can! is designed to prevent obesity in children and tweens (tweens refer to young people from the ages of 9 to 13 years) by providing practical advice, resources, and community-based programs to parents, caregivers, children, and youth to adopt healthy lifestyles. The handbook developed for parents focuses on three critical behaviors: improve food choices, increase physical activity, and reduce leisure screen time. An evaluation of this effort is in progress (NIH, 2005) (Appendix D).
USDA’s Food and Nutrition Service developed Eat Smart. Play Hard. as a national nutrition education and promotion campaign to convey
evidence-based, behavior-focused, and motivational messages about healthy eating and physical activity (USDA, 2005a). The campaign uses an animated cartoon character, the Power Panther™, to deliver messages to children and their caregivers. A formative evaluation of this campaign has been conducted (Appendix C). However, a long-term evaluation examining the campaign’s influence on children’s behavioral outcomes is needed.
Some food companies have developed programs and tools to assist families and parents in planning healthy meals or engaging in regular physical activity. For example, parents and a group of several food companies and food retailers, including Annie’s Homegrown, Applegate Farms, Horizon Organic, Newman’s Own, Newman’s Own Organics, and Whole Foods Market, initiated the Eat Smart, Grow StrongSM campaign in 2005. The campaign is focused on encouraging families to consume more healthful foods and promoting healthy eating habits at home (Public Interest Media Group, 2005). The campaign’s interactive website offers parents a range of ideas for healthy recipes and includes games to teach children about healthy eating habits.
In August 2002, Gerber Products Company launched the Start Healthy, Stay Healthy™ campaign that was designed to provide parents and consumers with educational materials on raising healthy infants and toddlers and preventing childhood obesity (Gerber Products Company, 2006). A recent addition to the campaign is the Start Healthy, Stay Healthy Promise, a program aimed at mobilizing parents across the country to pledge to give their children a healthy start. Parents who enroll in the program receive advice on healthy feeding practices (Gerber Products Company, 2005). In some states, such as Arkansas, Gerber has entered into a public-private partnership with Wal-Mart and state government agencies, under the leadership of Governor Michael Huckabee, to reach parents through state programs. The Arkansas program has established the goal of increasing the number of healthier preschoolers by 50 percent by 2010 (Gerber Products Company, 2005). The committee recommends comprehensive and independent evaluations of industry-supported programs to assess the programs and to examine the direct and indirect effects of industry sponsorship (Chapter 5).
As noted above, health care professionals and health care-related organizations have frequent interactions with families. These interactions provide opportunities for obesity prevention information to be conveyed to parents. A recent policy statement by AAP recommends that physicians regularly assess a child’s weight, diet, and level of physical activity; work with families to identify possible barriers to healthy living; encourage parents to serve as role models for healthy living through their own diet and exercise regimens; and encourage parents to support their children’s regular participation in sports and other physical activities (AAP, 2006a).
A number of ongoing school-based interventions include a family-based component that may involve activities or work sheets that families may complete together or logs of family meals, television viewing, and physical activity. For example, the Stanford SMART (Student Media Awareness to Reduce Television) classroom curriculum, which was intended to reduce third and fourth graders’ leisure screen time, included periodic newsletters for parents to teach parenting skills about television use and distributed electronic television time managers to families to help children budget their television time in the home. The intervention statistically significantly slowed the gain in BMI, triceps skinfold thickness, waist circumference, and waist-to-hip ratio in children receiving the curriculum compared with the values for the controls (Robinson, 1999) and also significantly reduced the television viewing times of the mothers, fathers, older siblings, and other children in the household (Robinson and Borzekowski, 2006).
Many parents can improve their modeling of healthy behaviors for their children. It is clear that much progress is needed, given that two-thirds of the American adult population is either overweight or obese (Ogden et al., 2006), only 22.2 percent of adults regularly engage in leisure-time physical activity for at least 30 minutes per day five or more times per week, and less than a quarter (23.3 percent) of adults consume five or more fruits and vegetables per day (Reeves and Rafferty, 2005). Families have an important role to play in reinforcing positive behaviors as well as protecting their children from negative influences or unintended consequences. Parents can assist their children with engaging in more healthful eating and physical activity behaviors by modeling the behaviors themselves, providing a supportive environment that facilitates the selection of healthier choices by their children, emphasizing healthy lifestyles and behaviors rather than weight or BMI, and engaging in supportive communication with their children (Neumark-Sztainer, 2005b).
EVALUATING PROGRESS AND NEXT STEPS
Coordinated public health interventions may successfully shape parental behaviors in the home, and lessons can be learned from other public health efforts. A frequently cited example is the Back to Sleep campaign to reduce the risk of sudden infant death syndrome (SIDS). In 1994, AAP, in partnership with the National Institute of Child Health and Human Development, the SIDS Alliance (now First Candle/SIDS Alliance), the Association of SIDS and Infant Mortality Programs, and the Maternal and Child Health Bureau of the Health Resources and Services Administration, launched the Back to Sleep campaign to inform all parents, infant caregivers, and health care professionals about the importance of placing healthy infants on their backs instead of their stomachs when they go to sleep. This
required behavioral changes among parents and caregivers. Since the Back to Sleep campaign was introduced, the percentage of infants placed on their backs has increased substantially, and the rates of SIDS have declined by more than 50 percent (NICHD, 2005). Through the examination of multiple sources of data, these changes have generally been attributed to the campaign (Moon et al., 2004).
Limited efficacy and effectiveness data hinder the development of best practices for childhood obesity prevention in the home environment. However, several promising practices have been published in the literature. The Stanford GEMS (Girls Health Enrichment Multisite Studies) pilot study confirmed the feasibility and efficacy of using after-school dance classes and a family-based intervention to decrease television viewing time and videogame use to reduce weight gain in African-American girls (Robinson et al., 2003). Reducing television viewing time and videogame use (Robinson, 1999), closely monitoring children’s eating behaviors (Brann and Skinner, 2005), emphasizing regular breakfast consumption (Fiore et al., 2006), and substituting noncaloric beverages for sugar-sweetened beverages at home (Ebbeling et al., 2006) are all promising approaches to preventing childhood obesity. However, these interventions require continued evaluations and research to confirm the findings. A recent Cochrane systematic review of childhood obesity prevention interventions concluded that the appropriateness of the development, design, intensity, and duration of interventions must be considered along with the comprehensive reporting of the scope of the intervention and the process (Summerbell et al., 2006). It has also been confirmed that sufficient data from randomized clinical trials to support any particular obesity prevention strategy are currently lacking (Summerbell et al., 2006). Thus, an integrated approach to using the best available evidence is recommended and reinforced by a systematic evaluation of the interventions (IOM, 2005).
APPLYING THE EVALUATION FRAMEWORK TO THE HOME ENVIRONMENT
What Constitutes Progress for Families and at Home?
Progress in preventing childhood obesity through family- and home-based interventions can be categorized as progress in providing environments that facilitate obesity prevention; progress in changing parental, familial, and caregiver behaviors and practices; and progress in research, evaluation, and surveillance. As noted earlier in this chapter, numerous external stresses, pressures, and challenges make it difficult for parents and caregivers to provide guidance and care for their children. Changes in some of these external conditions may facilitate desirable parental behavior. For
example, the more widespread availability of convenient and private rooms for pumping breastmilk at worksites could potentially facilitate mothers’ continued breastfeeding of their infants for the recommended 4 to 6 months. Modifications to the built environment to reduce work-related travel time or to provide common outdoor play areas for children are other examples of changes that may facilitate parents’ and caregivers’ efforts to prevent childhood obesity.
The recommendations for parents and caregivers from the Health in the Balance report (Box 8-1), can be used as a guide for parents to assess their own progress. These recommendations were based on the IOM committee’s consensus of the best available evidence for changing physical activity and eating behaviors to prevent childhood obesity and represent promising practices that require further and ongoing evaluation. The majority of the available evidence was derived from small-scale behavioral research and population-based surveys and, by extension, from research on other types of behaviors (IOM, 2005).
Many of the policies and programs implemented in other settings influence the behaviors of parents, caregivers, families, and households. Therefore, the present IOM committee’s recommendations and next steps for assessing progress focus on actions for parents, caregivers, families, and households (detailed below) and also on the actions needed by industry, government, communities, and schools (Chapters 4, 5, 6, and 7).
One of the challenges in assessing progress and evaluating the childhood obesity prevention initiatives implemented by families is the difficulty in collecting data at the individual parent-caregiver or family-household level. Sampling to determine overall national-level estimates may be feasible, but doing so at a meaningful level for each local area and every state is likely to be costly in terms of human and financial resources. Therefore, evaluations may need to rely on a combination of national data sources, as well as many different types of state and local data sources (Appendix C). A range of evaluation designs and research on families is needed in order to build a sufficient evidence base of promising obesity prevention strategies that can be widely disseminated. Some of the most useful data for planners and policy makers will come from evaluations of local programs that can be translated and adapted to other communities and populations (Chapters 3 and 6).
Another challenge to evaluating progress is a lack of reliable and valid measures with demonstrated sensitivities to changes in many of the outcomes that should be measured and that are recommended in Chapter 2. New methods and measures will need to be developed to monitor progress in reaching a variety of outcomes in the home setting. Additionally, there is a need to account for the possibility that obesity prevention interventions
may have adverse or unanticipated outcomes, such as the stigmatization of children or the development of eating disorders (Doak et al., 2006).
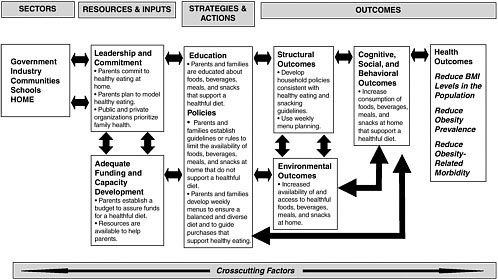
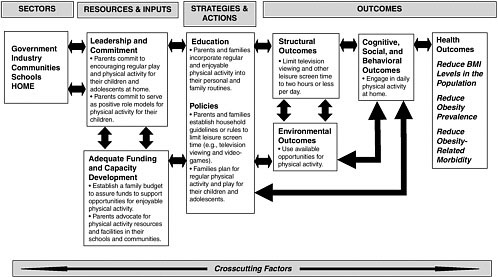
As is the case for government, industry, communities, and schools, the efforts of families and caregivers at home to prevent childhood obesity involve all aspects of the evaluation framework. For example, if promoting the consumption of healthful foods, beverages, and snacks at home is the desired outcome (Figure 8-1), the following events might be expected to occur. In terms of resources and inputs, parents commit to healthful eating at home, develop a plan to model and encourage healthful eating, and modify the household budget, as necessary. Relevant strategies and actions include educating parents about the nutritional value of foods and beverages; encouraging parents and families to establish household guidelines or rules limiting the availability and consumption of less healthful foods, beverages, meals, and snacks at home and limiting leisure screen time; and assisting parents and families with the development of weekly menus to ensure a balanced and diverse diet. Outcomes that could be examined include the increased availability of and access to healthful foods, beverages, meals, and snacks in the home; the use of weekly menu planning; and the extent to which family members adhere to healthful diets that are consistent with the Dietary Guidelines for Americans 2005. Figure 8-1 assesses efforts to promote the consumption of fruits, vegetables, and other low-calorie and high nutrient foods, beverages, meals, and snacks at home; and Figure 8-2 applies the framework to assess how parents may promote regular physical activity at home.
Box 8-2 provides a checklist that parents, families, and caregivers can use to assess their ongoing progress in adopting a healthy lifestyle for their families.
NEEDS AND NEXT STEPS IN ASSESSING PROGRESS
Promote Leadership, Commitment, and Collaboration
The Health in the Balance report emphasized that “a child’s health and well-being are fostered by a home environment with engaged and skillful parenting that models, values, and encourages sensible eating habits and a physically active lifestyle. By promoting certain values and attitudes, by rewarding or reinforcing specific behaviors, and by serving as role models, parents can have a profound influence on their children” (IOM, 2005, p. 285). Parents should provide leadership in the home and act as positive role models for healthy lifestyles. They can also act as community change agents and advocates to create healthy communities for their families by getting involved in school and community wellness programs and other activities at their children’s schools and in the community. Collaboration among all
|
BOX 8-2 Checklist for Parents, Families, and Caregivers
SOURCE: Adapted from IOM (2005). |
sectors is needed to create healthy environments for children both at home and away from home.
Develop, Sustain, and Support Evaluation Capacity and Implementation
Evaluation capacity refers to assisting families with developing or strengthening their ability to meet specific goals or objectives, as well as monitoring and evaluating their strategies and actions to promote healthier lifestyles in the home setting. Families need to recognize that even small incremental advances are valuable in improving dietary quality, decreasing sedentary time, and increasing physical activity.
Just as families may periodically evaluate their household budgets and financial well-being and their children’s academic progress, it is important
for parents, caregivers, children, and adolescents to periodically assess their health-related family practices and home environment. They can use such informal evaluation strategies as keeping regular food and physical activity diaries or use MyPyramid and MyPyramid for Kids, which have online tracking tools that can be used to monitor the lifestyle changes made in the home. Checklists of strategies for behavioral change can also be helpful (Box 8-2).
Enhance Surveillance, Monitoring, and Research
Further research on family interventions, as well as more family-targeted interventions, is needed to prevent childhood obesity (Jackson et al., 2005; Lindsay et al., 2006). Few rigorous evaluations on the effectiveness of these programs have been performed. However, current evidence suggests that parent interventions may work most effectively as a component of comprehensive interventions across a variety of settings, including schools, health care services, communities, and federal food and nutrition programs such as the WIC program.
Appendix C contains data sources and evaluation tools that can be used to measure obesity prevention-related outcomes, several of which are related to the home environment. Among these are the Behavioral Risk Factor Surveillance System, which assesses fruit and vegetable consumption and physical activity levels reported by parents and caregivers. The National Survey of Children’s Health and the National Survey of Early Childhood Health collect information from families on a variety of relevant behaviors, including breastfeeding, family mealtime, physical activity, and family rules concerning television viewing. The Youth Risk Behavior Surveillance System assesses the physical activity levels, television viewing times, leisure-time computer use, and fruit and vegetable consumption of middle school and high school students.
Disseminate and Use Evaluation Results
Although families play a central role in childhood obesity prevention, parents and families have only a limited number of information sources on obesity prevention. These include television and other media; materials brought home from preschool, school, child-care, and after-school care; and interactions with teachers, health care professionals, social workers, and coaches. Innovative approaches are needed to provide families with relevant obesity prevention information, particularly information that is practical, that is easily implemented, and that does not judge or lecture parents, who are often overwhelmed with multiple health-related messages and competing priorities. The federal government, state governments, local
governments, communities, and the media should find ways to disseminate promising interventions and initiatives such as Small Steps and Small Step Kids!; the Dietary Guidelines for Americans; MyPyramid and MyPyramid for Kids; the Eat Smart. Play Hard. campaign; the Food Stamp Nutrition Education Program; the WIC program; 5 a Day for Better Health; the Fresh Fruit and Vegetable Program; and We Can!. Consideration should be given to the development of channels that provide parents with information at multiple points through the child’s development, from prenatal and baby care to adolescence.
SUMMARY AND RECOMMENDATIONS
Each of the committee’s four recommendations is directly relevant to improving the implementation and evaluation of family-based interventions, policies, and initiatives.
Recommendation 1: Government, industry, communities, schools, and families should demonstrate leadership and commitment by mobilizing the resources required to identify, implement, evaluate, and disseminate effective policies and interventions that support childhood obesity prevention goals.
Implementation Actions for Home
Families, parents, and caregivers should commit to promoting healthful eating and regular physical activity to create a healthy home environment.
To accomplish this:
-
Parents and caregivers should make physical activity and healthful eating priorities at home. They should provide food and beverage choices for their children that contribute to a healthful diet, encourage and support physical activity, limit children’s television viewing and other leisure screen time, and serve as positive role models. Parents can also serve as advocates to promote changes that encourage and support healthy behaviors in their local schools and communities.
Recommendation 2: Policy makers, program planners, program implementers, and other interested stakeholders—within and across relevant sectors—should evaluate all childhood obesity prevention efforts, strengthen the evaluation capacity, and develop quality interventions that take into account diverse perspectives, that use culturally relevant approaches, and that meet the needs of diverse populations and contexts.
Implementation Actions for Home
Parents and caregivers, as the policy makers in the household, should assess their family’s progress in achieving positive lifestyle changes.
To accomplish this,
-
Families should regularly assess their progress in adopting and maintaining healthful behaviors at home and achieving positive lifestyle changes.
Recommendation 3: Government, industry, communities, and schools should expand or develop relevant surveillance and monitoring systems and, as applicable, should engage in research to examine the impact of childhood obesity prevention policies, interventions, and actions on relevant outcomes, paying particular attention to the unique needs of diverse groups and high-risk populations. Additionally, parents and caregivers should monitor changes in their family’s food, beverage, and physical activity choices and their progress toward healthier lifestyles.
Implementation Actions for Home
Parents and caregivers should monitor their families’ lifestyle changes; and government, foundations, and industry should support applied research that examines family interventions in real-world settings.
To accomplish this:
-
Parents and caregivers should monitor their families’ lifestyle changes on an ongoing basis, including their capabilities as role models, the family’s dietary intake and levels of physical activity, and their children’s weight status.
-
Parents should work with their child’s physician to track body mass indices and healthy growth.
-
The federal government should create and make available simple tools for parents and families to track their children’s dietary intake and physical activity behaviors.
-
Relevant federal agencies (e.g., CDC, NIH, USDA, and U.S. Department of Education), foundations, and other organizations should fund and support applied research that examines family interventions focused on specific ways that families can improve diets, reduce sedentary behaviors, and increase levels of physical activity in the home setting.
-
Relevant federal and state agencies, foundations, and academic institutions should develop and enhance surveillance systems
-
and other data sources and assessment tools to expand knowledge about the relationship between changes in the home environment and a variety of outcomes for children and youth.
Recommendation 4: Government, industry, communities, schools, and families should foster information-sharing activities and disseminate evaluation and research findings through diverse communication channels and media to actively promote the use and scaling up of effective childhood obesity prevention policies and interventions.
Implementation Actions for Home
Government (federal, state, and local), communities, families, and the media should disseminate and widely promote the evaluation results of effective family- and home-based childhood obesity prevention efforts.
To accomplish this:
-
Government agencies (federal, state, and local), communities, and the media should promote the results of evaluations and specific practical guidance related to promising family-based obesity prevention interventions such as approaches for reducing children’s television viewing, promoting leisure-time physical activity, and promoting healthier food and beverage choices at home.
-
Parents, children, and youth should share information about promising obesity-prevention strategies and activities with other families through parenting groups and school meetings and in family, social, faith-based, and other venues.
REFERENCES
AAFP (American Academy of Family Physicians). 2004. Obesity and Children: Helping Your Child Keep a Healthy Weight. [Online]. Available: http://www.aafp.org/afp/20040215/928ph.html [accessed June 2, 2006].
AAP (American Academy of Pediatrics). 2001. Children, adolescents, and television. Pediatrics 107(2):423–426.
AAP. 2006a. Active healthy living: Prevention of childhood obesity through increased physical activity. Pediatrics 117(5):1834–1842.
AAP. 2006b. Overweight and Obesity. [Online]. Available: http://www.aap.org/healthtopics/overweight.cfm [accessed June 2, 2006].
Ackard DM, Neumark-Sztainer D, Story M, Perry C. 2006. Parent-child connectedness and behavioral and emotional health among adolescents. Am J Prev Med 30(1):59–66.
Annie E. Casey Foundation. 2006. 2006 Kids Count Data Book. [Online]. Available: http://www.aecf.org/kidscount/sld/databook.jsp [accessed July 10, 2006].
Birch LL, Marlin DW. 1982. I don’t like it; I never tried it: Effects of exposure on two-year-old children’s food preferences. Appetite 3(4):353–360.
Brann LS, Skinner JD. 2005. More controlling child-feeding practices are found among parents of boys with an average body mass index compared with parents of boys with a high body mass index. J Am Diet Assoc 105(9):1411–1416.
CDC (Centers for Disease Control and Prevention). 2005. State Legislative Information: Search for Bills. [Online]. Available: http://apps.nccd.cdc.gov/DNPALeg/ [accessed April 24, 2006].
CNWICRA (Child Nutrition and WIC Reauthorization Act). 2004. Child Nutrition and WIC Reauthorization Act of 2004. Public Law 108-265 108th Congress. June 30, 2004. [Online]. Available: http://www.fns.usda.gov/cnd/Governance/Legislation/PL_108-265.pdf [accessed March 22, 2006].
Devine CM, Connors MM, Sobal J, Bisogni CA. 2003. Sandwiching it in: Spillover of work onto food choices and family roles in low- and moderate-income urban households. Soc Sci Med 56(3):617–630.
DHHS (U.S. Department of Health and Human Services). 2000. Healthy People 2010: Understanding and Improving Health. Washington, DC: DHHS. [Online]. Available: http://www.healthypeople.gov/Document/ [accessed July 17, 2006].
Dietz WH, Robinson TN. 2005. Overweight children and adolescents. N Engl J Med 352(20): 2100–2109.
Doak CM, Visscher TL, Renders CM, Seidell JC. 2006. The prevention of overweight and obesity in children and adolescents: A review of interventions and programmes. Obes Rev 7(1):111–136.
Ebbeling CB, Feldman HA, Osganian SK, Chomitz VR, Ellenbogen SJ, Ludwig DS. 2006. Effects of decreasing sugar-sweetened beverage consumption on body weight in adolescents: A randomized, controlled pilot study. Pediatrics 117(3):673–680.
Epstein LH, Valoski A, Wing RR, McCurley J. 1990. Ten-year follow-up of behavioral, family-based treatment for obese children. J Am Med Assoc 264(19):2519–2523.
Fields J. 2003. Children’s Living Arrangements and Characteristics: March 2002. Current Population Reports. Washington, DC: U.S. Bureau of the Census.
Fiore H, Travis S, Whalen A, Auinger P, Ryan S. 2006. Potentially protective factors associated with healthful body mass index in adolescents with obese and nonobese parents: A secondary data analysis of the third National Health and Nutrition Examination Survey, 1988–1994. J Am Diet Assoc 106(1):55–64.
Fitzgibbon ML, Stolley MR, Schiffer L, Van Horn L, KauferChristoffel K, Dyer A. 2005. Two-year follow-up results for Hip-Hop to Health Jr.: A randomized controlled trial for overweight prevention in preschool minority children. J Pediatr 146(5):618–625.
Gerber Products Company. 2005. Gerber Aims to Increase Number of Healthier Preschoolers by 50 Percent by 2010. News release. September 20. [Online]. Available: http://www.gerber.com/content/usa/bin/pdf/press/Arkansas_Start_Healthy_Press_Event_20Sep05.pdf [accessed June 17, 2006].
Gerber Products Company. 2006. Start Healthy, Stay Healthy™ Fact Sheet. [Online]. Available: http://www.gerber.com/content/usa/bin/pdf/press/Start_Healthy_Fact_Sheet.pdf [accessed June 11, 2006].
Gortmaker SL, Peterson K, Wiecha J, Sobol AM, Dixit S, Fox MK, Laird N. 1999. Reducing obesity via a school-based interdisciplinary intervention among youth: Planet Health. Arch Pediatr Adolesc Med 153(4):409–418.
Harvey-Berino J, Rourke J. 2003. Obesity prevention in preschool Native-American children: A pilot study using home visiting. Obes Res 11(5):606–611.
Hearn MD, Bigelow C, Nader PR, Stone E, Johnson C, Parcel G, Perry CL, Luepker RV. 1992. Involving families in cardiovascular health promotion: The CATCH feasibility study. J Health Educ 23(1):22–31.
Hersey JC, Jordan A. 2006. Reducing Children’s TV Time to Reduce the Risk of Childhood Overweight: The Children’s Media Use Study. Final report. Prepared for the Centers for Disease Control and Prevention and The Association of Preventive Medicine Teaching and Research. Washington, DC: Research Triangle Institute International.
IOM (Institute of Medicine). 2005. Preventing Childhood Obesity: Health in the Balance. Washington, DC: The National Academies Press.
Jackson D, Mannix J, Faga P, McDonald G. 2005. Overweight and obese children: Mother’s strategies. J Adv Nurs 52(1):6–13.
Larson NI, Story M, Eisenberg ME, Neumark-Sztainer D. 2006. Food preparation and purchasing roles among adolescents: Associations with sociodemographic characteristics and diet quality. J Am Diet Assoc 106(2):211–218.
Lindsay AC, Sussner KM, Kim J, Gortmaker S. 2006. The role of parents in preventing childhood obesity. In: Paxon C, ed. Future Child 16(1):169–186.
Luepker RV, Perry CL, McKinlay SM, Nader PR, Parcel GS, Stone EJ, Webber LS, Elder JP, Feldman HA, Johnson CC. 1996. Outcomes of a field trial to improve children’s dietary patterns and physical activity. The Child and Adolescent Trial for Cardiovascular Health (CATCH). J Am Med Assoc 275(10):768–776.
Mansukhani R. 2005. Why Are So Many Kids Today Overweight? What Every Parent Needs to Know. [Online]. Available: http://www.parentsaction.org/news/parenting-info/nutrition/why-are-so-many-kids-today-overweight/ [accessed May 8, 2006].
Maynard LM, Galuska DA, Blanck HM, Serdula MK. 2003. Maternal perceptions of weight status of children. Pediatrics 111(5 Pt 2):1226–1231.
McGarvey E, Keller A, Forrester M, Williams E, Seward D, Suttle D. 2004. Feasibility and benefits of a parent-focused preschool child obesity intervention. Am J Public Health 94(9):1490–1495.
McIntosh A, Davis G, Nayga R Jr, Anding J, Torres C, Kubena K, Perusquia E, Yeley G, You W. 2006. Parental Time, Role Strain, and Children’s Fat Intake and Obesity-Related Outcomes. Economic Research Service, U.S. Department of Agriculture. [Online]. Available: http://www.ers.usda.gov/Publications/CCR19/ccr19.pdf [accessed June 17, 2006].
Moon RY, Oden RP, Grady KC. 2004. Back to Sleep: An educational intervention with Women, Infants, and Children program clients. Pediatrics 113(3 Pt 1):542–547.
Nader PR, Baranowski T, Vanderpool NA, Dunn K, Dworkin R, Ray L. 1983. The family health project: Cardiovascular risk reduction education for children and parents. J Dev Behav Pediatr 4(1):3–10.
NCSL (National Conference of State Legislatures). 2006. Childhood Obesity—2005 Update and Overview of Policy Options. [Online]. Available: http://www.ncsl.org/programs/health/ChildhoodObesity-2005.htm [accessed July 17, 2006].
Neumark-Sztainer D. 2005a. Can we simultaneously work toward the prevention of obesity and eating disorders in children and adolescents? Int J Eat Disord 38(3):220–227.
Neumark-Sztainer D. 2005b. Preventing the broad spectrum of weight-related problems: Working with parents to help teens achieve a healthy weight and a positive body image. J Nutr Educ Behav 37(Suppl 2):S133–S140.
Neumark-Sztainer D. 2006. Eating among teens: Do family mealtimes make a difference for adolescents’ nutrition? New Dir Child Adolesc Dev Spring(111):91–105.
Neumark-Sztainer D, Hannan PJ, Story M, Croll J, Perry C. 2003. Family meal patterns: Associations with sociodemographic characteristics and improved dietary intake among adolescents. J Am Diet Assoc 103(3):317–322.
NICHD (National Institute of Child Health and Human Development). 2005. SIDS: “Back to Sleep” Campaign. [Online]. Available: http://www.nichd.nih.gov/sids/sids.cfm [accessed May 9, 2006].
NIH (National Institutes of Health). 2005. Welcome to We Can! [Online]. Available: http://www.nhlbi.nih.gov/health/public/heart/obesity/wecan/index.htm [accessed May 9, 2006].
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM. 2006. Prevalence of overweight and obesity in the United States, 1999–2004. J Am Med Assoc 295(13): 1549–1555.
Parents as Teachers National Center. 2005. Parents as Teachers. [Online]. Available: http://www.parentsasteachers.org/site/pp.asp?c=ekIRLcMZJxE&b=272091 [accessed July 17, 2006].
Patrick H, Nicklas TA. 2005. A review of family and social determinants of children’s eating patterns and diet quality. J Am Coll Nutr 24(2):83–92.
Perry CL, Crockett SJ, Pirie P. 1987. Influencing parental health behavior: Implications of community assessments. Health Educ 18(5):68–77.
Perry CL, Luepker RV, Murray DM, Hearn MD. 1989. Parent involvement with children’s health promotion: A one-year follow-up of the Minnesota Home Team. Health Educ Q 16(2):171–180.
PTA (Parent Teacher Association). 2006. Health and Wellness. [Online]. Available: http://www.pta.org/pr_category_details_1117232379734.html [accessed July 17, 2006].
Public Interest Media Group. 2005. Eat Smart, Grow Strong. [Online]. Available: http://www.eatsmartgrowstrong.com/ [accessed May 9, 2006].
Reeves MJ, Rafferty AP. 2005. Healthy lifestyle characteristics among adults in the United States, 2000. Arch Intern Med 165(8):854–857.
Rhee KE, DeLago CW, Arscott-Mills T, Mehta SD, Davis RK. 2005. Factors associated with parental readiness to make changes for overweight children. Pediatrics 116(1):94–101.
Rideout V. 2004. Parents, Media and Public Policy: A Kaiser Family Foundation Survey. Menlo Park, CA: Henry J. Kaiser Family Foundation.
Rideout V, Hamel E. 2006. The Media Family: Electronic Media in the Lives of Infants, Toddlers, Preschoolers and Their Parents. Menlo Park, CA: Henry J. Kaiser Family Foundation.
Ritchie LD, Crawford PB, Hoelscher DM, Sothern MS. 2006. Position of the American Dietetic Association: Individual-, family-, school-, and community-based interventions for pediatric overweight. J Am Diet Assoc 106(6):925–945.
Roberts DF, Foehr UG, Rideout V. 2005. Generation M: Media in the Lives of 8–18 Year Olds. Menlo Park, CA: Henry J. Kaiser Family Foundation. [Online]. Available: http://www.kff.org/entmedia/upload/Generation-M-Media-in-the-Lives-of-8-18-Year-olds-Report.pdf [accessed July 22, 2006].
Robinson TN. 1999. Reducing children’s television viewing to prevent obesity. A randomized controlled trial. J Am Med Assoc 282(16):1561–1567.
Robinson TN, Borzekowski DLG. 2006. Effects of the SMART classroom curriculum to reduce child and family screen time. J Communic 56(1):1–26.
Robinson TN, Killen JD, Kraemer HC, Wilson DM, Matheson DM, Haskell WL, Pruitt LA, Powell TM, Owens AS, Thompson NS, Flint-Moore NM, Davis GJ, Emig KA, Brown RT, Rochon J, Green S, Varady A. 2003. Dance and reducing television viewing to prevent weight gain in African-American girls: The Stanford GEMS pilot study. Ethn Dis 13(1 Suppl 1):S1.65–S1.77.
Shepherd J, Harden A, Rees R, Brunton G, Garcia J, Oliver S, Oakley A. 2006. Young people and healthy eating: A systematic review of research on barriers and facilitators. Health Educ Res 21(2):239–257.
Stolley MR, Fitzgibbon ML. 1997. Effects of an obesity prevention program on the eating behavior of African American mothers and daughters. Health Educ Behav 24(2):152– 164.
Summerbell CD, Waters E, Edmunds LD, Kelly S, Brown T, Campbell KJ. 2006. The Cochrane Database of Systematic Reviews. Interventions for Preventing Obesity in Children. The Cochrane Collaboration. John Wiley & Sons, Ltd. [Online]. Available: http://www.cochrane.org/reviews/en/ab001871.html [accessed November 28, 2006].
Texas Department of State Health Services. 2006. A Guide to School Health Advisory Councils (SHACs): A Basic Primer for Texas. [Online]. Available: www.dshs.state.tx.us/schoolhealth/ [accessed June 2, 2006].
USDA (U.S. Department of Agriculture). 2005a. Eat Smart. Play Hard.™ Campaign Overview. [Online]. Available: http://www.fns.usda.gov/eatsmartplayhard/Original/default.htm [accessed August 19, 2006].
USDA. 2005b. Fit WIC: Programs to Prevent Childhood Overweight in Your Community. Special Nutrition Program Report Series, No. WIC-05-FW. Food and Nutrition Service, USDA. Alexandria, VA: Office of Analysis, Nutrition, and Evaluation. [Online]. Available: http://www.fns.usda.gov/oane/MENU/Published/WIC/FILES/fitwic.pdf [accessed February 28, 2006].
Vega WA, Sallis JF, Patterson TL, Rupp JW, Morris JA, Nader PR. 1988. Predictors of dietary change in Mexican-American families participating in a health behavior change program. Am J Prev Med 4(4):194–199.
Wardle J, Cooke LJ, Gibson EL, Sapochnik M, Sheiham A, Lawson M. 2003. Increasing children’s acceptance of vegetables: A randomized trial of parent-led exposure. Appetite 40(2):155–162.