7
Building Characteristics and the Spread of Infectious Diseases
Transmission of infectious diseases among school children is frequent and probably inevitable. Although most such cross-infections are transient and not serious, they may have concentric circles of repercussions for other students, teachers, parents, and educational achievement. Actions that can help control the spread of such infections are, therefore, important to the health of students, teachers, and other adults.
Outbreaks of acute infections caused by viruses, bacteria, parasites, and protozoa have been documented among both students and staff in schools (Harley et al., 2001; Brennan et al., 2000; Khetsuriani et al., 2001; Davison et al., 2004; Lee et al., 2004; Otsu, 1998; AAP, 2003a,b). The majority of infections causing absenteeism in schools are respiratory and gastrointestinal illnesses. These types of illnesses occur continuously throughout the year. Although they are less obvious than outbreaks of infections, they nonetheless have an impact (Hammond et al., 2000; Brady, 2005; AAP, 2003a,b). Respiratory infections acquired in schools, especially rhinovirus infections, play a major role in exacerbating asthma and causing hospitalization for it (Johnston et al., 1995, 1996). Such illnesses result in increased health care costs, lost public funding for schools, added administrative expenses, and absences from work on the part of parents.
For children attending public schools, the transmission of common infectious diseases is estimated to result in more than 164 million lost school days each year (Vital Health and Statistics, 1998). On average, students are absent from school 4.5 days per year, and teachers miss work 5.3 days each year because of acute illness (Middleton, 1993). When surveyed, more than 80 percent of teachers cited school absenteeism as their main
problem (Carnegie Foundation, 1990). This finding is complemented by research showing the detrimental effect of absenteeism due to illness on student achievement (Ohlund and Ericsson, 1994).
Infectious agents can be transmitted by person-to-person contact, by droplets or large particles spread by coughing, sneezing, or wheezing, or by fomites (self-innoculation after touching contaminated surfaces). Distinguishing the various transmission modes is difficult, and the role of airborne transmission in respiratory infections is not yet completely understood. It is clear that many factors affect infection transmission, including the number of students in a school, their ages, the degree of crowding in classrooms, teacher-to-student ratios, geographic location, seasonal variation in the activity of common infectious agents, the number of recent immigrants, the proportion of children with chronic health conditions, and the number of young children: Young children have relatively less immunity to common infections and tend to pay less attention to personal hygiene (Hall, 2001; Marchisio et al., 2001; Goldmann, 2001; Brady, 2005; Musher, 2003).
School building factors that influence the transmission of specific infectious agents include the ventilation rate, humidity, filtration effectiveness, the cleanliness of surfaces, and the number, accessibility, and functional state of sinks and toilets (Bloomfield, 2001; Vernon et al., 2003) (Figure 7.1).
Current green school guidelines typically contain few measures related to these building characteristics, although they may address filter efficiencies. Additional measures could be included in future guidelines that might interrupt the transmission of infectious diseases, thereby improving the health of students, teachers, and others.
MODES OF TRANSMISSION FOR RESPIRATORY VIRUSES
The main agents of respiratory infections in schoolchildren, their families, and caretakers are respiratory syncytial virus,1 picornaviruses (especially the three genera enteroviruses, rhinoviruses,2 and parechoviruses3), influenza, adenoviruses,4 parainfluenza viruses,5 measles, and
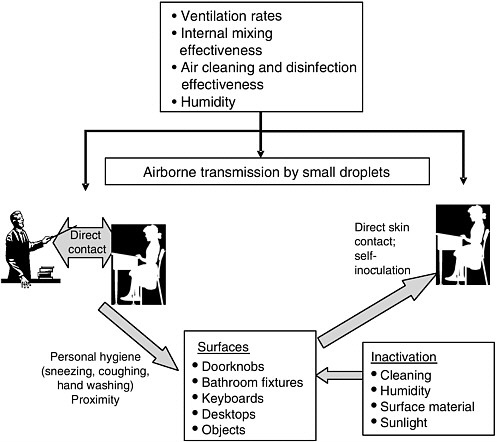
FIGURE 7.1 Transmission modes for spread of infectious diseases.
human respiratory coronaviruses6 (McIntosh, 2005). Respiratory viruses are shed primarily as nasal or oral secretions (runny nose) or projected into the air by sneezing, coughing, spitting, or speaking. Most are transmitted from the infected person to others by any of three possible mechanisms mentioned above. Specific viruses may be spread by more than one of these mechanisms.
Small-particle aerosols (<10 µm mass median diameter) are usually generated by coughing or sneezing and may traverse distances ≥1.8 m, can occur without close or direct contact with the infected person or the
infectious secretions. Evidence is emerging that quiet breathing can also generate small particles. Aerosolized respiratory fluids (small droplets, sometimes less than 1 µm in size) evaporate quickly when discharged into room air, resulting in droplet nuclei (Riley and O’Grady, 1961). Such small particles do not settle on surfaces and clothes to any appreciable extent, are inefficiently removed by conventional filtration, and are easily dispersed by air movement indoors. Viruses that can be spread by small-particle aerosols, such as the measles, chicken pox, and, sometimes, influenza, can cause rapid outbreaks of infection in susceptible populations.
Transmission by large droplets or large particles, in contrast, requires close person-to-person contact, usually at a distance of ≤0.9 m, for infection to occur directly: Large droplets (>10 to 100 µm diameter) expectorated during a sneeze or cough may be released with sufficient momentum to contact directly the mucosa of another person’s eyes, nose, or mouth. However, large droplets have appreciable settling velocities and infectious material might also land on clothing or the surfaces of nearby objects. Some viruses are able to remain infectious on environmental surfaces, are transferable to skin, and can remain infectious for a long enough time to allow self-inoculation into the respiratory tract (Hall, 1981, 2000).
The third transmission mechanism is self-inoculation by touching contaminated surfaces. Clinical studies, especially those using infection control interventions, have indicated that the primary mode of transmission for the most common respiratory and gastrointestinal viruses acquired by children and adults within schools is close contact with infected individuals or touching infectious secretions that contaminate inanimate objects (Hall, 1981; Hall and Douglas, 1981; Hall et al., 1981; Ansari et al., 1991; Mbithi et al., 1992). These articles suggest that fomites are a primary mode and that large droplet spread (across distances of less than 3 feet) is also important.
Fabian et al. (2006) point out that discrimination between the various modes of transmission has been difficult for several reasons. One is that the concentration of infectious particles in air required to transmit infection is very low—thus it can be very difficult to detect them and prove that the particles exist. A second reason is the nature of human source aerosols and their dissemination has not been well understood or widely appreciated.
Understanding the role of airborne transmission is further complicated by the fact that the human infectious dose will vary substantially among viruses. Dilution in the indoor air supply may make concentrations far too low for transmission to occur. However, there is no reason to believe that airborne viruses are uniformly dispersed in indoor spaces. The mixing of air within a classroom and certainly within spaces having cubicles, partitions, files, and bookshelves is far from homogeneous. Areas
of high concentrations might persist for longer than would be predicted by the calculated air exchange rate for the room. Reports on the transmission of respiratory infections, including SARS, in places like airplanes, office buildings, and hospitals also suggest the potential importance of an airborne component (Moser et al., 1979; Roy and Milton, 2004; Reichert et al., 2001; McLean, 1961; Riley et al., 1978).
New insight into the generation of respiratory aerosols and the role of airborne transmission in respiratory infections is being gained with more sophisticated aerosol measurement equipment (Fabian et al., 2006). Earlier work focused on larger droplets produced from the upper respiratory mucosa (Riley and O’Grady, 1961) and used techniques generally insensitive to particles less than 1.0 µm in diameter. Those early studies found that as many as 40,000 droplets are generated during a sneeze, about one order of magnitude more than by coughing and two to four orders more than by talking loudly (Cox, 1987). Most of the particles detected were less than 4 µm (Duguid, 1946; Gerone et al., 1966). Very few particles were thought to be liberated during quiet breathing (Riley and O’Grady, 1961), and there were few data to suggest interindividual differences in the generation of aerosols during coughing, sneezing, or talking.
More recent studies conducted by Edwards et al. (2004) show it is possible to generate large numbers of particles from the human respiratory system during quiet mouth breathing. They used a laser light-scattering instrument (not available to earlier researchers) to detect particles in the submicron range down to 150 nm. Although the number of subjects was small (11), they demonstrated a clear bimodal phenomenon with respect to respiratory particle generation during quiet breathing. Over the 6 hours of monitoring, five volunteers produced an average of only 14 to 71 particles per liter of exhaled air. However, the other six volunteers consistently exhaled 10 times that number of particles per liter (an average of more than 500 particles per liter over 6 hours), with one subject generating up to 3,230 particles per liter during quiet breathing. This translates to 5,000 to 32,000 particles liberated per minute for those “high producers.” The mechanism by which these submicron droplet nuclei are generated is not known. Microdroplets formed by bursting films of respiratory fluid or the fragmentation of specula during breathing are suspected of producing submicron droplets. Obviously these intriguing observations need further research to determine if they might explain the existence of “super shedders” in outbreaks of SARS, measles, and influenza.
Roy and Milton (2004) characterized the potential aerosolized transmission as “obligate” (TB), “preferential” (measles), or “opportunistic” (most respiratory viruses). This classification is based on an agent’s capacity to be transmitted and to induce disease through fine-particle aerosols and other routes. The authors noted that probably all viruses have different
likelihoods of being spread by aerosols or droplets but the likelihood of spreading is highly variable and the concentration of virus is often too low to cause human infection, despite its being detectable by advanced techniques (Roy and Milton, 2004). A number of clinical studies suggest that the primary or “preferential” mode of spread is not airborne. For example, it seems that rhinoviruses can be airborne, although the preponderance of real-world studies suggested that this was not the preferential mode of spread (Hendley et al., 1973; Winther et al., 1998; Gwaltney and Hendley, 1982; Gwaltney et al., 1978). A well-designed experiment by Jennings and Dick (1987) provided evidence that the airborne route was more important for the transmission of rhinovirus than contact and fomites. Myatt et al. (2004) reexamined earlier studies of the Gwaltney group and found them to be underpowered to detect airborne transmission.
The importance of this evidence to schools administrators, teachers, and other decision makers is that they need to recognize multiple routes for the transmission of infectious diseases. As discussed in the following sections, control strategies range from the mundane and inexpensive— control via hand cleansing and decontamination of surfaces—to improved ventilation systems, including displacement ventilation.
MEASURES FOR CONTROLLING THE SPREAD OF INFECTIONS IN SCHOOLS
Two of the most effective measures for controlling the spread of infection in schools are immunization and the exclusion of children and adults with infectious cases. Because these are policy measures unrelated to school buildings, they are not discussed further in this report.
Design-related control measures have generally focused on hand cleansing, along with personal hygiene and decontamination of surfaces. Most studies evaluating methods of infection control have been in recognized high-risk populations, such as hospitalized and compromised patients and children in out-of-home care who are less than 3 years old. Whether the findings of these studies can be applied to the general population of K-12 students and staff in schools is unclear. The exception is the benefit of effective hand cleansing. Some studies suggest that effective and routine hand washing can diminish common infections and could cut down on absenteeism among school children (Kimel, 1996; Master et al., 1997; Early et al., 1998). Evident also, however, is the difficulty of maintaining compliance in a school population (Guinan et al., 1997, 2002), especially among younger children.
Hand and Personal Hygiene
The use of hand sanitizers or hand rubs for infection control has been evaluated in health care facilities, at home, and in day care centers and schools (Meadows and Le Saux, 2004; Lee et al., 2005; Girou et al., 2002; CDC, 2002; Rochon-Edouard et al., 2004; Master et al., 1997; Early et al., 1998; Zaragoza et al., 1999; Turner et al., 2004; Sandora et al., 2005). Most of these studies showed a significant reduction in the occurrence of infections in general. However, effectiveness of the sanitizers may vary depending on the individual agents, especially viruses (IFH, 2002b). Hand sanitizer products containing alcohol tend to have greater activity against nonenveloped viruses (e.g., respiratory syncytial virus, influenza, parainfluenza viruses, HIV, and herpes simplex virus) than against enveloped viruses (e.g., rhinovirus, parechoviruses, enterovirus, adenovirus, rotavirus,7 and caliciviruses).8 Washing one’s hands for an extended time, however, can enhance the antiviral activity of hand sanitizers toward enveloped viruses. Picornaviruses (e.g., enteroviruses, rhinoviruses, and hepatitis A virus) are particularly difficult to eradicate from hands or environmental surfaces but may be inactivated by high concentrations of alcohol and extended hand-washing time. Nevertheless, for all of these viruses, hand sanitizers have been shown to be more effective than routine hand washing (IFH, 2002a,c).
A number of studies have examined the efficacy of hand sanitizers over traditional hand-washing methods in reducing the incidence of acute illnesses and absenteeism. A systematic review of five published studies on the effectiveness of hand sanitizers in preventing absenteeism due to illness in elementary school children revealed a significant advantage for hand sanitizer use over baseline conditions, which may have included soap and water or no structured hand washing. However, the quality and heterogeneity of the reports prevented the calculation of pooled estimates (Meadows and Le Saux, 2004).
Recently the Centers for Disease Control and Prevention (CDC) revised its guidelines for hand hygiene in health care settings to recommend hand washing to remove visible soiling. Otherwise the use of hand sanitizers is recommended based on their efficacy, the propensity of health care workers to use them, and the low incidence of adverse effects (CDC, 2002).9
The CDC’s recommendations also emphasized that for health care facilities the items necessary for hygiene and cough etiquette must be
readily available, including disposable tissues, no-touch waste receptacles, conveniently located dispensers of alcohol-based hand rub solutions, and, wherever sinks are available, supplies for hand washing. Similar measures could be implemented in green schools; ongoing maintenance would be required if such measures are to be effective.
The efficacy of the measures contained in these recommendations in reducing respiratory illness and absenteeism has not been proved. The recommendations are based, instead, on the assumption that the measures will disrupt the primary modes of transmission of the agents most frequently causing respiratory and gastrointestinal illnesses. Assuring compliance with these measures is problematic for any age and probably impossible for young children. However, for older children and staff, constant reminders to follow these measures and ensuring that hand sanitizers and other items are routinely available seem reasonable considering the ways in which infectious agents spread, the low cost of these items, and the absence of significant adverse effects.
DECONTAMINATION OF ENVIRONMENTAL SURFACES
Many of the common agents causing infections in schools have been found to survive on hands and environmental surfaces long enough to allow the transfer of infectious organisms from the environment to the hands. The duration of viability and the inoculating dose required are highly variable according to the organism. A number of studies, mostly under experimental conditions, have evaluated the survival of common organisms on inanimate objects in order to ascertain their potential for being spread by fomites (Hall et al., 1980; Brady et al., 1990; Butz et al., 1993; Dettenkofer et al., 2004; Dowell et al., 2004; Neely and Orloff, 2001; Rogers et al., 2000; IFH, 2002b). Few of these studies, however, went so far as to determine the survival of the transferred organisms on the skin or under different environmental conditions (Hall et al., 1980).
Surface decontamination procedures include cleaning using a liquid or soap detergent and hot water. In general this method has been found to produce a surface clean enough that the organisms that remain are not transferable or are too few in number to cause human illness. Rinsing well after cleaning is a critical step. This method of cleaning may be less effective if the surface is damaged or in poor condition. In addition, for this or any other method, results will be compromised by using a drying cloth or other material that is not initially clean and that is used continually without itself being repeatedly decontaminated.
Surfaces are also cleaned using a soap or detergent followed by an application of a chemical disinfectant product. The disinfecting product should achieve a hygienic surface sufficient to interrupt the spread of
organisms to cause infection. Furthermore, the agent should have a broad and rapid inactivating action against a variety of bacterial, viral, and fungal pathogens.
Use of a combined detergent and disinfectant product allows for a one-step procedure. The characteristics of disinfectants in the combined products, such as their recommended concentrations, whether they are static or cidal toward the microbes, and the recommended methods of use, are published or available on the Web, along with guidelines for the selection and use of disinfectant products (IFH, 2002a; Rutala et al., 2000; Rutala and Weber, 2004).
Literature comparing the effect on cross-infection rates of disinfecting environmental surfaces as opposed to cleaning them without using disinfectants was systematically reviewed (Dettenkofer et al., 2004). Of the 236 identified published articles, none was a randomized controlled trial and only four were cohort studies with matching inclusion criteria. None of these studies showed diminished rates of infection associated with the routine practice of disinfecting surfaces in comparison to cleaning them with detergent only. The authors concluded that disinfectants could adversely affect individuals in the area and also the environment and that if they were used, special safety precautions should be taken. The authors also concluded that more well-designed studies would need to be performed to assess the role of surface disinfection in preventing the transmission of infection.
One alternative to conventional methods of disinfection of environmental surfaces would be the development of hands-free designs for those surfaces most often touched—doors, faucets, flushers, soap and towel dispensers, and entrances to restrooms. While these solutions are becoming more frequent in airports for their ease of cleaning, they are less common in schools. Research on the effect of hands-free design on infection rates in schools would be valuable.
Choosing surfaces and components such as faucets, door handles, and so forth, that can be easily cleaned may help to interrupt the transmission of infectious diseases through fomites. One precedent of note is the involvement of “cleaning engineers” (a discipline in Holland) in the review of design/engineering drawings. Their signature certifies that the building as designed can be effectively cleaned and will not create undue health and degradation risks.
VENTILATION AND AIR CLEANING
Three building characteristics are relevant to the survival, dispersal, and removal of airborne pathogens—the relative humidity of the room air,
the dispersion path and dilution provided by the ventilation system, and the return air mixing and filtration provided in the fresh air supply.
Exhaled particles will readily evaporate in typical indoor humidities, and disperse or slowly settle on surfaces and people. Aerosols even 5 µm in size have slow settling velocities, taking about 44 minutes to settle from a height of 2 meters. A 1 µm particle would take 18 hours to settle in still air. Since settling is negligible for particles less than 5 µm in size, they will disperse with the air currents created by mechanical ventilation systems, movement of people, buoyant convections by people and equipment, and pressure-driven flows (natural and mechanical) within a room, throughout a structure, and even into the outdoor air.
Humidifiers are not routinely installed in schools. Although humidification carries its own health concerns, a lack of it in school buildings can result in low relative humidity (RH) (<30 percent) in the winter (heating months), although the RH would be more moderate (30-70 percent) during periods when the outside air must be cooled. At lower relative humidities common to schools, exhaled drops would quickly evaporate and be suspended for long periods before finally settling onto surfaces or being carried out of the room or building by the exhaust air. Furthermore, low humidity has been associated with increased viability for some viruses. Harper (1961) showed that vaccinia and influenza viruses survived longer at RHs in the low 20 percent range. Other viruses have optimal survival at different RH values. Remington et al. (1985), in a study that followed up on a measles outbreak in a doctor’s office, suggested that low humidity was a contributing factor. Given low RHs and hard surfaces, viruses might survive as suspended droplets or on fomites for many hours in schools. On the other hand, the rhinovirus (common cold) survives longer at moderate to high relative humidities.
A second factor affecting the spread of infections in schools is the dispersion path and dilution provided by the ventilation system. The conventional design for HVAC systems is to forcefully introduce conditioned air into a room at the ceiling level to ensure effective mixing of “fresh” air with the existing room air. The mixing within a room (or zone), however, will in turn cause the dispersion of indoor-generated viral material present as small droplets. In office environments, Myatt et al. (2004) collected nasal swabs and air samples to look for viruses in nearby colleagues using the polymerase chain reaction. They confirmed that an office worker was responsible for a virus strain isolated in an air sample taken in the same general work area.
Although conventional ceiling-based ventilation systems can cause dispersion of viral material, increasing ventilation rates can speed the dilution and removal of viral material. Milton et al. (2000) tracked sick leave as a function of CO2 levels and building ventilation. Across 42 build-
ings grouped according to ventilation rates, employees in buildings with higher ventilation rates (approximately 48 cfm/person diluting outside air) reported using 1.6 fewer days of sick leave than employees working in the buildings at lower ventilation rates (4 cfm/person the current ASHRAE 62.1 2004 standard).
While increasing the ventilation rate may cause more rapid mixing, it also causes more rapid dilution and removal. However, there may be practical limitations to this effect, since not all the air is completely replaced with each air exchange. Typically only two-thirds of the air is removed per air exchange because of the size and location of supply and exhaust ducts, short circuiting, and obstructions (blocked unit ventilators). Also, dilution with increased ventilation air can cost more for larger ducts, fans, and heating and cooling. The potential for increased mechanical noise in classrooms would also be a concern (see Chapter 6).
An alternative to this typical mechanical mixing of conditioned air from the ceiling is the use of floor-based or side-wall-based displacement ventilation. Theoretically, ventilation effectiveness is maximized by displacement flow. By bringing in fresh air near the floor and returning it at the ceiling, infectious droplets and contaminants are not forced toward neighboring occupants. As demonstrated in chamber studies, exposures to occupants can be reduced substantially and ventilation efficiency can be increased.
A third ventilation-related factor affecting the spread of infections within schools is the percent of the return air mixed into the supply air and the filtration provided in the air stream. Most schools are conditioned with a combination of recirculated air and outside air that has either been cooled, with some ambient moisture removed, and/or heated to meet thermal requirements.
To reduce the potential for exchanging infectious substances, schools could be designed to use 100 percent outside air, as hospitals have done. To ensure energy efficiency, however, it would be critical to introduce heat recovery or to separate the ventilation from the thermal conditioning system. Thoughtful attention to thermal heat loads, sensible and latent heat recovery, and possibly the use of thermal elements such as chilled beams and radiant heating might make affordable the use of 100 percent outside air to meet ventilation requirements, exhausting all breathing air that might contain infectious aerosols. Research on the costs and benefits of eliminating recirculated air in schools should be undertaken for different climate conditions.
At the same time, it is imperative to assess the effects of filtration on reducing airborne pathogens and pollutants from both outside and return air sources. Airborne pathogens that have evaporated to submicron size will not settle out nor will they be effectively removed by filtration.
Indeed, in a recirculated air system, viable airborne pathogens could be distributed to other classrooms by the mechanical ventilation system. Riley et al. (1978) present the case of a measles outbreak in an elementary school consistent with airborne transmission. Riley and Nardell, in their 1989 review, cite cases where tuberculosis was transmitted through the air to infect people who had no direct contact with the infected person.
Germicidal UV Radiation
Viruses can be readily inactivated with ultraviolet (UV) light (Nuanualsuwan et al., 2002; Nuanualsuwan and Cliver, 2003), and the use of UV light to control the airborne transmission of infectious respiratory agents has been documented (Riley and O’Grady, 1961; Riley and Nardell, 1989). Germicidal UV radiation in the short wavelengths (100 to 280 nm) is referred to as UVC radiation or UVGI. The Centers for Disease Control and Prevention’s (CDC) Web site (www.cdc.gov) cites numerous instances of UVC use to kill or inactivate tuberculosis and other infectious agents in hospitals, military housing, and classrooms. UVC fixtures have been used to clean the air in areas where undiagnosed tuberculosis patients might be present, such as emergency room waiting areas, shelters, and correctional facilities.
More than 40 years ago, Jensen (1963) demonstrated the germicidal effectiveness of UV radiation at 254 nm wave length (UVC) on vaccinia and other viruses. The work of McClean (1961) is often cited as evidence that UV irradiation has germicidal efficacy for airborne viruses. During the late 1950s, a Veterans Administration hospital in Livermore, California, was operating upper room UV lights in one of its wings. Two outbreaks of acute febrile respiratory illness (ARI) occurred in two wings of the hospital during the fall and winter of 1957/58, one of them in the wing with the UV lights. Baseline serology was obtained in July 1957 before the first outbreak. Follow-up serology was taken in November 1957 and again in March 1958 after the first and second ARI outbreaks. Only staff or visitors could have been the source of infection since the patients were in long-term care and restricted to the hospital. Since the source of the first infection was not known, it was also not known whether patients in both wings were similarly exposed. Nevertheless, there were four times as many influenza titers10 in the wing without the upper room UV lights. Over the two outbreaks, 18 percent of the staff and 19 percent of the patients in the wing without the UV lights became ill, whereas only 2 percent in the wing with the upper room UV lights were ill. McClean reports that the
first wave of ARI was not influenza but that influenza clearly dominated (not exclusively) the second outbreak. Nevertheless, the UV lights in one of the wings were protective against both viral agents. There have not been any additional epidemiologic studies on infection control with UVC in hospitals, offices, or schools.
Today’s increased focus on technologies that offer protection against biological threats has renewed interest in the germicidal effectiveness of UVC. This, in turn, has led to recent chamber studies in which UV lamp placement or configuration, room air exchange, supplemental air mixing, wattage (UV fluence rates in µmW/scm2), and relative humidity have been looked at to determine the rates at which they inactivate several types of spores, cells, and viruses. The CDC Web site (www.cdc.gov) summarizes the findings in its 2005 TB guidelines published in Morbidity and Mortality Weekly Report, December 30, 2005. The salient facts are described below.
In a well-mixed room, UVGI fixtures properly located to irradiate the upper space of a room (>8 feet) and having the appropriate wattage can significantly enhance the inactivation rate of test organisms. A substantially higher “effective” air exchange rate (ACH) can be achieved with a combination of upper room UV and mechanical air change rates. Effective ACHs with upper room UVC can greatly exceed what is practically possible with other combinations of air filtration and mechanical ventilation (Nardell et al., 1991). However, inactivation effectiveness diminishes as UV fluence decreases and as RH increases above 60 percent. Servicing of UV lamps to maintain performance specifications is important, particularly in settings when the lamp surfaces can become soiled. Guidelines for application of upper room UVC are contained in several ASHRAE publications (First et al., 1999a,b).
The long-term exposure of occupants to UVC radiation is a concern because it could cause skin and eye damage. The CDC and the National Institute for Occupational Safety and Health (NIOSH) have published recommended exposure limits to protect health care workers from the acute effects of UV light exposure. The potential carcinogenic effects of UVA and UVB, but not UVC, are reviewed by Parrish (2005). The exposure of building occupants to UVC used in upper room installations is very low. A recent report on UVC dose monitoring showed that even when some areas of the lower room exceeded 0.2 µW/cm2, the 8-hour dose was a small fraction of the 6 mJ/cm2 recommended exposure limit (First et al., 2005). There is a risk of acute photokeratitis, a self-limiting condition. This is the basis of the 6 mJ/cm2 8-hour maximum dose standard. There is no literature demonstrating a long-term risk to the eye from the extremely low exposures to UVC in the lower room. Even if one assumed that an installation in a school classroom gave an average exposure of 0.2 µW/cm2 for a 6-hour school day, every day for a 180-day school year, the total UVC
dose to the skin from the UVC lights would be <0.8 J/cm2. By comparison, the average adult receives 33 J/cm2 of UVA and UVB from sunlight each year. Given that 50 percent of UVA and UVB penetrate to the basal cell layer while only 5 percent of UVC penetrates to expose the dividing cells, the maximum conceivable annual dose to the basal cells of the epidermis from use of upper room UVC in classrooms would be 0.24 percent of the annual dose of UVA plus UVB from sunlight.
When UVC lamps have been placed in ventilation ducts or in the air-conditioning systems of air-handling units (cooling coil and drip pans) or have been configured into portable room air cleaners, the UVC exposure to occupants has essentially been eliminated. A chamber study of portable UVGI systems demonstrated their effectiveness in inactivating or killing airborne vegetative bacteria (Green and Scarpino, 2002). The efficiency of UVGI in air-handling units was tested in an office building and reported by Menzies et al. (2003), who examined microbial contamination including endotoxins but not airborne pathogens (see Chapter 4). The application of supplemental air cleaning with UVGI for classrooms, while promising, should first be researched and evaluated more thoroughly. Although enclosing UVC in air ducts or portable air cleaners might reassure parents, its effectiveness will be limited by the amount of supply air that can be treated. Upper room UVC still has a comparative advantage because more effective air exchange rates can be achieved (Nardell et al., 1991).
FINDINGS AND RECOMMENDATIONS
Finding 7a: Common viruses and infectious diseases can be transmitted by multiple routes: through the air, by person-to-person contact, and by touching contaminated surfaces (fomites). Certain characteristics of buildings, including the cleanliness of surfaces, relative humidity, and ventilation effectiveness, influence the transmission of common viruses. Evidence from studies in nonschool environments suggests that interventions which interrupt the known modes of transmission of common infectious agents may decrease the occurrence of such illnesses in schoolchildren and staff.
Finding 7b: The best way to control infections, especially gastroenteritis, appears to be instituting procedures that promote good hand cleansing. Available but limited information indicates that hand sanitizers are superior to the routine washing of hands.
Finding 7c: Cleaning of surfaces that are commonly touched (e.g., doors, faucets, desktops) is effective for interrupting the transmission of infec-
tious agents. Disinfecting surfaces with water and detergents is apparently as effective as applying germicidal agents.
Finding 7d: The use of no-touch faucets, doorways, receptacles, and equipment seems to be a reasonable, though unproven, method for infection control.
Finding 7e: The survival, dispersal, and removal of airborne pathogens are affected by relative humidity, ventilation rate, and the percentage of recirculated air in the air supply. Increased ventilation rates have been shown to speed the dilution and removal of viral material. The use of displacement ventilation and the reduction of the percentage of recirculated air in the air supply have the potential to reduce building occupants’ exposures to airborne pathogens.
Finding 7f: Ultraviolet germicidal irradiation (UVGI) may be effective for inactivating and killing some infectious organisms, but its use in schoolroom applications has not been systematically studied.
Recommendation 7a: Future green school guidelines should include measures for the regular cleaning of commonly touched surfaces and the availability of hand sanitizers at sinks. The use of “no-touch” faucets, receptacles, equipment, and egress from bathrooms should be considered, taking into account the age of the children in the school.
Recommendation 7b: Full-scale classroom and school studies should be conducted to quantify the efficacy of a variety of ventilation strategies, including displacement ventilation and the elimination of recirculated air, for the dispersion and removal of airborne infectious agents. Studies should also quantify the potential costs and benefits of such ventilation strategies.
Recommendation 7c: Additional research should be conducted to determine the optimal infection-control interventions in terms of measurable outcomes such as absenteeism and academic achievement. One line of research is the use of ultraviolet germicidal irradiation in supplemental or portable air-cleaning devices in schoolroom applications and its effects on human health.















