11
Dietary Reference Intakes: Applications in Dietary Assessment and Planning1
In this session on the Dietary Reference Intakes (DRIs) application reports, five individuals addressed research recommendations related to dietary assessment and planning. Suzanne P. Murphy of the University of Hawaii (the first chair of the Subcommittee on Interpretation and Uses of Dietary Reference Intakes) covered research recommendations in the DRI Dietary Assessment Report (IOM, 2000a). Susan I. Barr of the University of British Columbia (the second subcommittee chair) covered research recommendations in the DRI Dietary Planning Report (IOM, 2003a). Jay Hirschman of the Food and Nutrition Service, Patricia M. Guenther of the Center for Nutrition Policy and Promotion, and Rena Mendelson of Ryerson University, Toronto, presented perspectives of users of the reports.
DIETARY REFERENCE INTAKES: APPLICATIONS IN DIETARY ASSESSMENT
Presenter: Suzanne P. Murphy
Dietary Reference Intakes: Applications in Dietary Assessment (IOM, 2000a) has been available for 6 years. This presentation summa-
rized the progress on the research recommendations. For convenience, the report’s 29 research recommendations are grouped into four broad categories:
-
Improvements to the DRIs themselves
-
Improvements in dietary assessment methods
-
Better statistical methods
-
Tools to help professionals use the DRIs correctly
A brief discussion of each category follows, along with highlights of 12 of the general recommendations (the recommendations are italicized).
Recommendations That Were Related to the DRIs Themselves
Most of the recommendations have been covered by previous speakers, but they are summarized below along with Dr. Murphy’s assessment of the progress made in reducing the research gap.
-
Obtain better data on the distribution of requirements. To determine the Recommended Dietary Allowance (RDA), one needs some information on the variability of requirements. Many assumptions were necessary, and there is still a need to improve those estimates. Little progress has been made.
-
Replace Adequate Intakes (AIs) with Estimated Average Requirements (EARs) and RDAs. Figure 11-1 depicts the possible placement of a “mythical” AI on a graph showing the frequency distribution of individual requirements. When the DRI nutrient panels did not have enough information to set an EAR and an RDA, they set this single number—the AI. Because one doesn’t know anything about the distribution of requirements, one cannot use the paradigm that was developed for estimating the probability of adequacy or the prevalence of inadequacy. One only can look at whether mean intakes are at the AI. In most cases, the AI probably is larger than the RDA. Therefore, the AI is not a very satisfactory DRI value in terms of dietary assessment. Based on previous presentations during this workshop, some good progress is anticipated on replacing some of the AIs with EARs as time goes by.
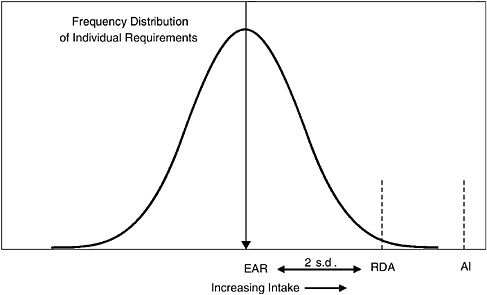
FIGURE 11-1 Position of selected DRI values on a frequency distribution of individual requirements.
NOTE: EAR = Estimated Average Requirement, RDA = Recommended Dietary Allowance, AI = Adequate Intake, s.d. = standard deviation. RDA = EAR + 2 s.d.
-
Set Tolerable Upper Intake Levels (ULs) for all nutrients and provide information on the distribution of adverse effects. This type of distribution was not specified for any nutrient. If someone has an intake above the UL, one does not know if the risk of an adverse effect is very low or if there is great reason for concern. Little progress has been made.
-
Better specify factors that can alter requirements. It could be useful to know if there were some way to determine approximately where on the requirement distribution a person’s individual requirement falls. For example, Dr. Dawson-Hughes mentioned that the calcium requirement for children or for adolescents may be related to their height. Knowledge of such factors could be very helpful in estimating the probability of inadequacy for a specific person. Some progress is anticipated.
Recommendations Related to Improvement in Dietary Assessment Methods
Much work is being done in this area, as highlighted below.
-
Improve food composition tables to use the same units and forms as the DRIs. This essentially has been accomplished, largely because of work by the Nutrient Composition Laboratory at the U.S. Department of Agriculture (USDA). For example, the food composition tables now list micrograms of dietary folate equivalents (µg of DFE). Alpha-tocopherol equivalents had to be changed to alpha-tocopherol, and in many databases the different tocopherols had not been separated out. Retinol equivalents had to be changed to retinol activity equivalents to adjust for the lower availability of some of the carotenoids. Also, the databases needed to include different forms of some nutrients for the EAR and the UL. For example, the UL for folate applies only to folic acid (the synthetic form of folate), whereas the EAR is for total folate and DFEs.
-
Improve dietary data collection instruments to remove the bias of underreporting. This bias has long been recognized as one of the most serious problems with dietary assessment methods. Progress is being made. For example, the automated multiple pass method that is being used for U.S. national surveys seems to reduce underreporting and appears to be capturing much better data. Additionally, a group at the National Cancer Institute (NCI) is looking at a combination of recalls and a propensity questionnaire, a type of food frequency questionnaire to estimate the distribution of intakes for groups Additionally, the Observing Protein and Energy Nutrition (OPEN) Study that NCI conducted provided a much better understanding of the errors that are inherent in some dietary data.
-
Find better ways to quantify intakes from dietary supplements. Considerable work is in progress on this topic. For example, 2 days of supplement intake data are being collected in U.S. national surveys, and this will provide some information on day-to-day variation in supplement intake. The USDA Nutrient Data Laboratory is building an analytic database so that it will become unnecessary to rely on label data. At the University of Hawaii, Dr. Murphy is conducting a study to try to quantify the errors in
-
reporting across multiple instruments used for collecting data on dietary supplements. It is hoped the findings will provide useful information about the accuracy of the data being collected.
Recommendations for Better Statistical Methods
Little progress has been made with regard to any of the research recommendations in this category, as described below.
-
Improve methods of assessing individuals. Dr. Murphy noted that the use of the DRIs to assess an individual’s intake is a highly contentious issue. Because a practical and valid process for determining an individual’s usual intake is not yet available, reliance must be placed on estimates from reported intake or observed intake; and the resulting confidence in the assessment of adequacy may be low. Adjustment for the confidence of adequacy has been problematic; methods are not complete for all nutrients (that is, for nutrients with a high coefficient of variation of daily intakes), and the process is subject to misinterpretation (consumers and professionals may assume that a low confidence means that intake needs to be increased, but often it just means that intake needs to be observed over a longer period).
Figure 11-2 presents a hypothetical example in which the EAR is 6.8, the RDA is 9, and the person’s usual intake (based on the 3 days of intake data) is 10 units of this nutrient. If one simply calculates the straight probability of adequacy, the result would be about 100 percent; that is, if true usual intake were 10 units a day, one would be virtually certain that the individual met his or her requirement. However, the method used in the DRI Assessment Report also considers the uncertainty in basing the estimate of usual intake on only 3 days of reported intake. “True” usual intake could be either higher or lower than 10 units. In this situation, one would have much less confidence that the individual’s true usual intake actually had 100 percent probability of adequacy. By using statistical equations and looking at the day-to-day variation in intake of the specific nutrient, the estimated confidence might be only 80 percent. Although the methods are quite good if one knows usual long-term diet, little
-
progress has been made in improving the assessment methods for individuals for whom just a few days’ data are available.
-
Assess the performance of the main methods of assessing groups, namely the full probability approach versus the cut-point method. The cut-point method is much easier to apply than is the full probability approach, and it provides a very good approximation of the prevalence of inadequacy if the assumptions made are correct. The recommendation to conduct a systematic investigation of those assumptions has not yet been acted upon.
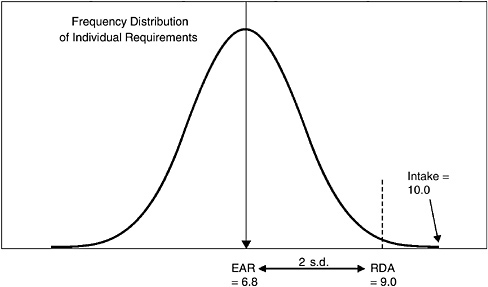
FIGURE 11-2 A usual long-term intake of 10.0 units would be above the RDA for this hypothetical nutrient and thus would have a high probability of adequacy. However, if intake data were available for only 3 days, then 10.0 might be higher or lower than the true usual intake, and the confidence that usual long-term intake was adequate would be reduced to approximately 80 percent.
NOTE: EAR = Estimated Average Requirement, RDA = Recommended Dietary Allowance, s.d. = standard deviation.
-
Develop methods to test for differences in the prevalence of adequacy between groups, controlling for other factors. Suppose, for example, that one wanted to compare the prevalence of adequacy of nutrient intakes of two groups: (1) food stamp participants and (2) food stamp-eligible persons who were not participating in the program. To determine whether the results were statistically different, one would first have to adjust each distribution of intakes to obtain the usual intake distribution. Because the two groups may differ in other ways (e.g., income, education), multivariate analyses would be needed to adjust for the covariates. The DRI Assessment Report (IOM, 2000a) contains a proposed methodology to adjust for day-to-day variation and for these covariates, but it appears that the method has not been tested yet.2
Recommendations to Develop Tools to Help Professionals Use the DRIs Correctly
Some progress has been made with regard to extending software to assist users with new methods, but more and better tools are needed. The C-SIDE3 program from Iowa State University is very helpful in assessing groups, but it is a rather complex program. A few of the software developers that have programs for assessing the diets of individuals have incorporated probability calculations into their programs rather than reporting intake as a percentage of the RDA.
APPLICATIONS IN DIETARY PLANNING
Presenter: Susan I. Barr
The report Dietary Reference Intakes: Applications in Dietary Planning (IOM, 2003a) has been available for only 3 years. This presentation included an overview of the DRIs in planning and a summary of relevant research recommendations and progress to date.
Framework for Planning
The planning framework that was outlined in the DRI Planning Report provides some context for considering the research recommendations and the progress that has occurred. Figure 11-3 presents the conceptual framework for the uses of DRIs. It illustrates that to plan or assess diets, one needs valid estimates of nutrient requirements and of nutrient intakes. That is, planning and assessing are iterative processes: assessment is necessary for the planning, and planning needs be evaluated by assessment. The procedures used differ somewhat.
The goal stated for dietary planning is to optimize the prevalence of diets that are nutritionally adequate without being excessive. For an individual, the goal would be (1) a low risk that the person does not meet his or her individual requirement and (2) a low risk that the person’s intake is excessive. For a group, this translates to a low prevalence of inadequacy and of potential risk of excess. Within this framework, planning goals are for intakes. Traditionally, however, planning has been for foods offered or served. In the DRI planning framework, what matters is not that the nutrient is available but whether or not it is consumed by the individual or group.
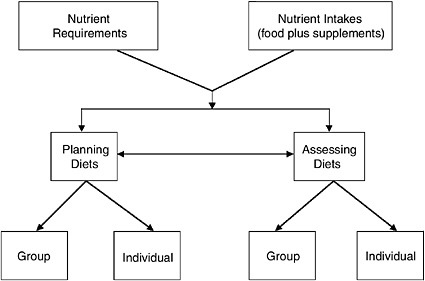
FIGURE 11-3 Conceptual framework: uses of Dietary Reference Intakes.
SOURCE: IOM (2000a), adapted from Beaton (1994).
An outline of the planning processes that the DRI Applications Subcommittee developed will help illuminate the research recommendations. Figure 11-4 illustrates the process used in planning for individuals. In this case, the relevant question is whether the individual has special considerations. If there were special considerations that would affect requirements (for example, smoking cigarettes increases the vitamin C needs of a smoker), then planning for that nutrient would be based on the special consideration. Planning for the other nutrients involves planning to meet the RDA or AI while keeping intake below the UL, meeting energy needs, and staying within the Acceptable Macronutrient Distribution Ranges (AMDRs).
Figure 11-5 shows the planning paradigm for groups. If the group is homogeneous (for example, a group of adult men), then one considers whether the requirement distribution is symmetrical or skewed. If it is not skewed, the plan can be based on the EAR cut-point method in such a way that the distribution of intake would have a low prevalence of persons with intakes below the EAR. If the requirement distribution were skewed, the full probability method would be used to achieve a low prevalence of inadequacy.
In the case of a heterogeneous group, the term vulnerable subgroup refers to a group that has a high nutrient requirement relative to energy needs. An example would be 6- to 12-month-old infants: they have high iron needs relative to their energy needs and could be a target for intervention.
A nutrient density approach to planning was proposed for heterogeneous groups for which vulnerable subgroups cannot be identified. This approach considers the joint distributions of energy and nutrient requirements to plan for the nutrient density that will lead to a low prevalence of inadequacy.
Figure 11-6 depicts the difference between the baseline usual intake distribution (dashed line) and the target usual intake distribution (solid line). The planning approach was used to attempt to shift the distribution to the right to lower the prevalence of inadequacy. Thus, in this target distribution, the prevalence of inadequacy (area to the left of the EAR) is now low, and usual intakes remain below the UL.
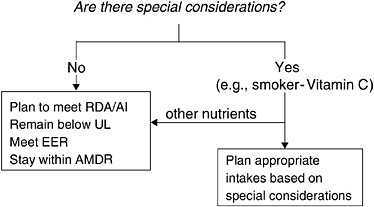
FIGURE 11-4 Decision tree for use when planning intakes for individuals.
NOTE: RDA = Recommended Dietary Allowance, AI = Adequate Intake, EER = Estimated Energy Requirement, AMDR = Acceptable Macronutrient Distribution Range.
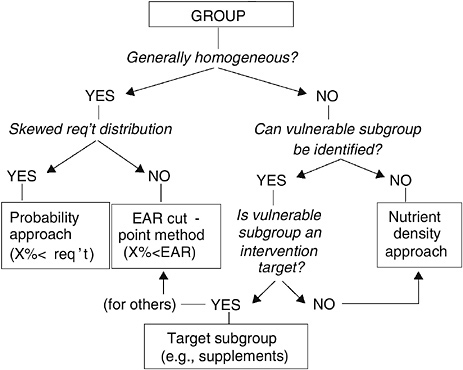
FIGURE 11-5 Decision tree for use when planning intakes for groups.
NOTE: EAR = Estimated Average Requirement.
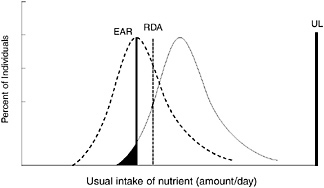
FIGURE 11-6 A comparison between the baseline and target usual intake distribution.
NOTE: dashed line = baseline usual intake distribution and solid line = the target usual intake distribution.
Research Recommendations and Progress
Because this fairly complex paradigm is largely theoretical, a number of research recommendations arose in different categories.
Recommendations Related to Intake Distributions
Determine usual intake distributions of specific population groups. At the time the subcommittee was preparing the report, it was necessary to commission special analyses to obtain data about usual intake distributions (i.e., intake distributions from which within-person variability had been removed). Considerable progress has been made toward conducting such analyses. For example, the most recent publication of What We Eat in America (Moshfegh et al., 2005) presents data on usual intake distributions by age and sex. In addition, several of the Canadian provincial surveys present their data in this way, and Dr. Barr anticipates that the 2004 Canadian National Survey will also present data on adjusted usual intake distributions (Health Canada, 2006).
Recommendations Related to the Planning Process Itself
A number of recommendations were related to the goal of shifting nutrient intake distributions to achieve a low prevalence of inadequacy and a low prevalence of excessive intake.
-
Pilot test the proposed approach to planning for a low group prevalence of inadequacy. Progress towards this goal has been limited. Can the intake goals be achieved while meeting other important goals such as avoiding excess energy intakes, maintaining nutrient intakes below the upper level, and avoiding unnecessary food waste? The Institute of Medicine (IOM) Committee to Revise the WIC4 Food Packages attempted to use the model in preparing recommendations for its report and found the approach to be quite challenging to implement for that purpose (IOM, 2006c).
-
Determine the relationship between foods offered and the nutrient intake in the context of group planning. If one offered more vitamin A-rich foods to a group that had a high prevalence of inadequate vitamin A intakes, for example, would the prevalence of inadequacy decrease? Such a decrease would only occur if the vitamin-A rich foods were actually consumed by those with inadequate intakes. Little progress has been made in systematically examining this relationship. Although some insight might be gained from the impact of food fortification programs such as the mandatory fortification of enriched cereal products with folic acid, that example does not really address what happens when the specific foods offered to groups are changed.
-
Determine how different nutrition interventions affect nutrient intake distributions. For example, will the distribution simply shift and otherwise retain the same shape? Compared with changes in education, supplementation, or food availability, would changes in fortification have a different impact on the shape of the distribution? Other than the example of folic acid fortification, data are not available regarding the effect of different types of nutrition interventions on intake distributions. It is possible, however, that future implementation of a new WIC food package may provide some insight on what happens when food availability is changed.
-
Develop and evaluate dietary planning strategies for heterogeneous groups. The DRI Planning Subcommittee proposed a nutrient density approach to plan for heterogeneous groups. Although one can envision how such an approach could be used to formulate a standard emergency relief ration that would meet the nutrient requirements, even of those with low energy needs, it is much more difficult to envision how this could be accomplished when a variety of foods differing in energy and nutrient content is available. No progress appears to have been made in this area.
Recommendations Related to Implementation of the Planning Process
Several recommendations address how one takes the information on nutrient requirement distributions and translates it to food-based patterns that would achieve the desired nutrient intake patterns.
-
Review and, where necessary, revise existing food guides. The USDA has released a revised food guide called MyPyramid (USDA, 2005). It incorporates recommended intakes from the DRI reports. In general, persons who follow MyPyramid would be expected to meet the RDA or AI for most or all nutrients.
-
Develop food guides for group planning. Canada is using an innovative modeling approach to develop a food guide that (if followed) would result in a low prevalence of diets with inadequate nutrient intakes. It could thus be used to plan diets both for groups and for individuals.
-
Assess the application of the DRIs for food and supplement labeling. Points to consider are the updating of values, synthetic sources of nutrients, and information on the UL. Dietary Reference Intakes: Guiding Principles for Nutrition Labeling and Fortification (IOM, 2003b) addressed these topics. That report contains a recommendation to use a weighted EAR as the Daily Value, and this recommendation has engendered considerable debate. The Food and Drug Administration has not yet published a proposed rule on the topic.
-
Communicate with and educate nutritional professionals about correct uses of the DRIs. Although much remains to be done to meet this goal, some progress has been made. For example, an online course on DRIs developed in Canada5 is available, and several articles have been published in scientific journals addressing how to use the DRIs in assessment and planning. Notably, Dietary Reference Intakes: The Essential Guide to Nutrient Requirements (IOM, 2006a), a single-volume summary of the DRI series is likely to be a widely read and useful resource.
In conclusion, some real progress has occurred, but many critical knowledge gaps need to be bridged to be able to plan confidently for low prevalences of inadequacy and excess using the DRIs.
|
5 |
The website is www.dieteticsatwork.com. A fee is charged. |
DISCUSSION OF RESEARCH RECOMMENDATIONS FROM THE APPLICATION REPORTS
Presenter: Jay Hirschman
This presentation was from the position of one who works with the U.S. federal food assistance programs—food stamps; school lunch; the Supplemental Nutrition Program for Women, Infants, and Children (WIC); and many others—and thus focuses mainly on the DRI Planning Report (IOM, 2003a). Points covered included a planning conundrum, the use of end points, statistical adjustment, testing the group planning methodology, and the shape of the target intake distribution.
The Planning Conundrum
Federal food programs work mainly with heterogeneous groups. The DRI Planning Report suggests using a target usual nutrient distribution by selecting a target percent inadequate. An example given is 2.5 percent inadequate—the estimated percentage of individuals who would not be covered by meeting the RDA.
Because most of the EARs and AIs for children are determined indirectly, they involve a higher degree of uncertainty than the values for adults. Notably, approximately 50 million children in the United States attend schools that participate in the National School Lunch Program, and one should never expect the U.S. federal government to say that it is satisfactory for 2.5 percent of schoolchildren to be inadequate in a nutrient. That would translate to 1.25 million children. These factors make application of the recommended DRI planning methodology difficult in practice.
End Points
The methods of determining end points differ across the different nutrients, and the science varies enormously across the range of nutrients. However, the DRI Planning Report provides no guidance on the relative importance of reducing the percent inadequate across the different nutrients. That is, would it be better to use the same target percent inade-
quate for all the nutrients or, for example, to target 1 percent inadequate for one nutrient and 10 percent inadequate for another? Would the result be satisfactory if using a specific target pushed a portion of the distribution into the UL range? Those responsible for applying the methodology are left with considerable uncertainty as they make decisions about program operation on a day-to-day basis.
Statistical Adjustment Question
Mr. Hirschman raised the statistical question, Does the statistical correction based on 2 days’ data correct for the intraindividual variation equally across nutrients? Basiotis and coworkers (1987) demonstrated that the number of days required for a true group average estimate of nutrient intake varies considerably across the nutrients. If the correction is not equal, this could have important implications for planning. During the discussion period, Dr. Kevin W. Dodd, a statistician at NCI, explained that the adjustment applies equally across the nutrients.
Testing the Group Planning Methodology
Mr. Hirschman has used a number of different data sets and the nutrients vitamin C and zinc to test the nutrient density approach to planning for heterogeneous groups—adolescents in particular. Figure 11-7 illustrates some of Mr. Hirschman’s findings. Nutrient density per 1,000 kcals was calculated using the following formula:
The first two bars in the figure used the 1989 RDAs for vitamin C and the average energy allowance at median height and weight rather than intake. The next two bars, which used the 2000 RDA and the estimated energy expenditure for sedentary adolescents, show a considerably larger target nutrient density. (The RDA for vitamin C had increased and the energy value, which is in the denominator, had decreased). The School Nutrition Dietary Assessment (SNDA) Studies are nationally representative studies of U.S. children attending schools offering the National School Lunch Program.
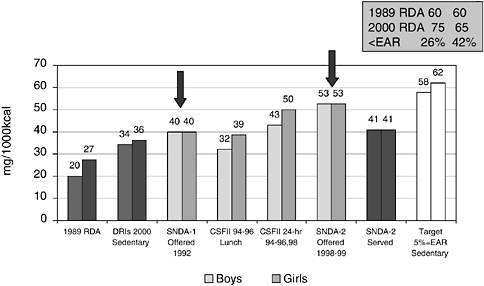
FIGURE 11-7 Vitamin C nutrient density: a comparison of survey results for adolescents. All values include vitamin pill supplements.
NOTE: RDA = Recommended Dietary Allowance, DRI = Dietary Reference Intake, EAR = Estimated Average Requirement, SNDA = School Nutrition Dietary Assessment Study, CSFII = Continuing Survey of Food Intake by Individuals. The 2000 DRI value shown is an RDA. Median values are not readily available. These are approximations based on [(mean intake/mean energy) × 1,000]
The first arrow shows vitamin C density—approximately 40 mg of vitamin C/1,000 kcal—of the food offered to the children in 1992. The estimated vitamin C density of food reported to be consumed at lunch, which is from an analysis of data from the 1994–1996 Continuing Survey of Food Intake by Individuals, is somewhat lower. Data from SNDA-2, 1998–1999, (see the second arrow in Figure 11-7) indicates that the nutrient density for vitamin C in foods offered was considerably higher than that reported by SNDA-1. In the interim, the USDA had implemented the School Meals Initiative for Healthy Children—a national effort to try to improve the quality of school meals.
These data show that it is functionally possible to increase nutrient density in the meals that are offered to children. However, the figure also shows that the vitamin C density of the meals served is substantially lower than that offered, meaning that the students did not take all the offerings, and they selected foods with lower than average vitamin C per
1,000 kcal. The last two bars in the figure show what the vitamin C density targets would be. For a heterogeneous population, one would use the higher nutrient density—namely 62 mg of vitamin C/1,000 kcal.
More information will become available from the analysis of SNDA-3 data from school year 2004–2005, which included (in addition to data on foods offered and foods served), data on what the children ate—both at the meals at school and over 24 hours.
Shape of the Target Intake Distribution
Government programs frequently aim to shift the shape of the distribution, as by providing larger benefits to families with lower income. This raises the research question, What assumptions should be made in planning regarding changes in the shape of the intake distribution?
Concluding Remarks
In his concluding remarks, Mr. Hirschman made the following points regarding research needs:
-
Consider a coordinated research effort to review the existing mammalian animal studies, and then design and complete new mammalian studies that will improve the estimate of the variation, being sure to select species with natural variation. Also these studies should be used to improve the methods for extrapolating from adult values to other groups, especially children.
-
Given that it is difficult to select the target percent inadequate, the shape of the distribution is intended to change, the end points are variable, and there is uncertainty in the intake estimates, consider the need for a new study and publication with a title that might be along the lines of Applications of the DRIs in Planning: Health and Statistical Considerations in Selecting Targets for the Percent Inadequate Across Nutrients.
RESEARCH RECOMMENDATIONS FOR DRI APPLICATIONS
Presenter: Patricia M. Guenther
This presentation highlighted applications of the DRIs at the USDA Center for Nutrition Policy and Promotion (CNPP), especially related to the following:
-
Dietary Guidelines for Americans 2005 (DHHS/USDA, 2005), the nutrition policy of the U.S. federal government, the development of which considered assessment of the proportion of the population with inadequate intakes of nutrients
-
MyPyramid, the USDA’s major consumer education tool, which uses the RDAs and AIs as the nutrient adequacy goals
-
The USDA food plans, including the Thrifty Food Plan (which provides the basis of the Food Stamp Program allotments)
The purposes of the presentation were to report on the progress made regarding the research recommendations in the two DRI applications reports and to identify the research needs that remain unmet.
Progress Made Related to Assessment
A summary of progress related to assessment is presented below.
-
Reporting estimates of usual or long-run average daily intakes when assessing nutrient adequacy. A major milestone was reached when the USDA's Agricultural Research Service used the method and software developed at Iowa State University (ISU) to estimate the proportions of the population having usual intakes below their EARs and the standard errors of these estimates (Moshfegh et al., 2005).
-
Estimating usual intake—developing more applications and greater efficiency. NCI has developed a method for estimating usual intake that builds on previous work. It was developed for estimating population distributions of usual intakes of episodically consumed foods. Papers describing the method—by Dodd
-
et al., Subar et al., and Tooze et al.—are scheduled to appear in the October 2006 issue of The Journal of the American Dietetic Association. The NCI method is expected to work for nutrients as well as for foods. It could be used to determine whether the prevalence of inadequacy differs between two groups and whether it would be more efficient than the ISU method for that purpose.
Using models that relate intake to a health outcome within the context of the 2003–2004 National Health and Nutrition Examination Survey (NHANES), the NCI method also can predict an individual's usual intake and its standard error using appropriate covariates. The National Center for Health Statistics (NCHS) Data Users’ conference in July 2006 had a session about this; and further information, SAS macros, and a web tutorial will be forthcoming through the NCHS website.
-
Developing estimates of an individual's usual intake in a clinical setting for the purposes of determining the probability of inadequate intakes. This remains a research need. The NCI group believes that this can be done and that a confidence interval for the predicted usual intake could be estimated. This approach may prove to be more useful than the confidence-of-adequacy approach described in the DRI Assessment Report. The CNPP has found that that the confidence-of-adequacy approach is impractical for use with consumers.
-
Understanding the underreporting of food intake. Tooze and colleagues (2004) describe results of a multivariate exploration of the underreporting of food intake and a review of earlier work done to address this topic.
-
Biomarkers. Progress has been made in the use of recovery biomarkers such as doubly labeled water and urinary nitrogen to estimate bias in dietary assessments. Progress has also occurred in the use of concentration biomarkers (e.g., serum carotenoids, which are correlated with nutrient intake). However, consensus has not yet been reached regarding the usefulness of concentration biomarkers.
-
Measuring the intake of supplements. The plans for the NHANES 2007–2008 include collecting 2 days of supplement and dietary intake data, which will facilitate the estimation of
-
day-to-day variability in nutrient intake from supplements and total nutrient intake.
-
Qualitative consumer-oriented research on how to communicate concepts related to assessing dietary adequacy, the most important one being probability of adequacy. This remains a research need. The CNPP needs some exploratory research to find out what consumers want to know about dietary adequacy and what will be meaningful to them. Dietitians need consumer research-based advice about how to explain dietary adequacy information to their clients.
Progress Made Related to Planning
The CNPP uses the RDAs and AIs in the development of its food guidance system, (MyPyramid), which provides plans for use by individuals. Dr. Guenther concurred with previous speakers that a well-conceived and tested nutrient density approach to the DRIs could facilitate the planning of diets for families whose members have heterogeneous nutrient needs. The CNPP will be using a nutrient density approach in its dietary assessment tool. The revised Healthy Eating Index will assess food intakes per 1,000 calories of energy intake.
Potential New Research Questions
The following two topics of interest to the CNPP might be considered for future research:
-
Noting that the AMDRs are density standards, the CNPP would find it very helpful if more of the DRIs could be expressed on a density basis, such as per 1,000 calories of energy intake or per kilogram of body weight.
-
A recommended ratio of sodium to potassium intake could also be useful. The protective effect of potassium-rich diets in blunting the adverse effects of sodium intake has not yet been quantified to the extent that it could be used in dietary guidance and assessment. Given the difficulty of planning higher calorie diets that do not exceed the AI for sodium, a research-based rec-
-
ommendation that simultaneously considers both sodium and potassium intake would be most welcome.
Summary
Progress in applying the DRIs has been demonstrated by the use of the ISU method and software to estimate the prevalence of inadequacy, the development of the NCI method for further applications of usual intake, advances in biomarkers, and plans for improved collection of information on supplement use. The remaining research needs are methods for estimating individual usual intake, consumer communication research, and expanding the research base for the development of DRIs that can be expressed as densities or ratios.
EDUCATING PROFESSIONALS ON THE USE OF DIETARY REFERENCE INTAKES
Presenter: Rena Mendelson
This presentation briefly covered topics related to communicating about the DRIs from the perspective of an individual who teaches undergraduate dietetic students and who needs to explain the DRIs to young college students. Then, very brief mention was made concerning application of the DRIs from the perspective of work with the Ontario Food Survey in Canada.
Students, other professionals, consumers, and others basically want to know if they are deficient in any nutrients and, if they are deficient, what they should do to make up for the deficiency. Dr. Mendelson finds that textbooks pose a problem. The most popular textbooks tend to include the RDAs but not the EARs. Textbooks come with nutritional analysis software, but students have difficulty determining whether they have made a mistake or not. Two major reasons for this difficulty are the students’ lack of knowledge of food composition data and lack of experience with hand analyses of nutrient intake. Moreover, the target to which intake is compared varies in different software packages and may not be clearly identified.
Explaining the probability of inadequacy to a student who is looking for a deficiency poses a challenge. Having them do the analysis for their intake by hand is a tedious process, but doing one’s own analysis helps with comprehension.
Dr. Mendelson considers it important to examine how dietitians are using the DRIs in conjunction with dietary data. Pertinent questions include, How are they analyzing and interpreting the information? and How are the many other providers of nutrition advice using the information? She concurred with Dr. Guenther’s recommendation concerning research on communicating with consumers.
Using the DRIs in conjunction with survey data may pose other challenges. After applying the cut-point method to look at the estimated prevalence of inadequacy in the population, interpreting and acting on the findings requires careful consideration. For example, what action is needed, if any, in view of the finding that 35 percent of the population has an estimated prevalence of inadequacy of magnesium?
DISCUSSION
Topics covered during the discussion included supplements, nutrient density, software, and the DRI paradigm. For comments on the DRI paradigm, see the “Discussion” section in Chapter 13.
Vitamin-Mineral Supplements
Dr. Dwyer commented that supplements and fortified foods are sometimes overlooked in dietary planning. Several discussants responded, giving examples pertaining to dietary assessment. Food surveys provide data about fortified foods but not necessarily about supplements. Dr. Hirschman pointed out that targets for children are based on nutrients from foods and that the conservative approach is to examine intake from foods only unless there is a concern with exceeding the UL. Drs. Mendelson and Barr commented that the estimated prevalence of inadequacy with supplement use was essentially the same as that without supplement use in one Canadian survey, but it was lower in another one. Method of data collection, region of the country, and year all may have contributed to the difference in the findings.
Nutrient Density
Dr. Bier noted that there is no standard definition of nutrient density and that we lack a way to compare the nutrient density if, for example, one food is rich in vitamin E and another in vitamin C. Is it correct to use calories as the denominator? Dr. Barr clarified that, in the DRI Planning Report, nutrient density was considered nutrient by nutrient. One examines the distribution of the nutrient requirement in relation to the distribution of the energy requirement. She noted that no method was developed to combine the densities for different nutrients.
Software
In response to Dr. Dwyer’s question regarding availability of quality software, Dr. Mendelson suggested that software companies link up with publishers of widely distributed textbooks and that the two parties synchronize their approach to computerized dietary assessments.
























