7
Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids1
During this session, Joanne Lupton of Texas A&M University, former chair of the panel on macronutrients, discussed selected research recommendations covering the five types of nutrients in the Dietary Reference Intakes (DRI) Macronutrients Report (IOM, 2002/2005). Harold Kohl of the Centers for Disease Control and Prevention (CDC) addressed research recommendations pertaining to physical activity, and Joanne Slavin of the University of Minnesota, St. Paul, provided perspectives on research recommendations pertaining to fiber.
DISCUSSION OF RESEARCH RECOMMENDATIONS
Presenter: Joanne R. Lupton
This presentation on the knowledge gaps and research gaps from the DRI Macronutrients Report (IOM, 2002/2005) covered specific research recommendations if they met one or more of the following criteria:
-
The research has a direct effect on either changing a current DRI value or the criteria upon which that value is established. This could include providing sufficient data to move from an Adequate Intake (AI) to a Recommended Dietary Allowance (RDA), for example.
-
The research results could be used in establishing a new DRI value.
-
The handling of the topic in the DRI Macronutrients Report generated much discussion within the professional community.
-
The research is related to DRI values that were difficult to meet as a part of eating plans that are consistent with the Dietary Guidelines for Americans 2005 (DHHS/USDA, 2005).
Background information of the derivation of specific Estimated Average Requirements (EARs), RDAs, or AIs is provided to help clarify the continuing research needs.
Carbohydrates
Recommended Dietary Allowance
With regard to carbohydrates, there is much controversy over the RDA of 130 grams of carbohydrate per day and over the recommendation that intake of added sugars be less than 25 percent of calories. In addition, a recommendation to revisit the difference between high-glycemic and low-glycemic diets on diabetes and coronary heart disease needs attention.
The RDA of 130 grams of carbohydrate per day is based on the amount of glucose needed by the brain in a day. That amount of carbohydrate, however, is less than the amount that would be the lower limit of the Acceptable Macronutrient Distribution Range (AMDR). Thus, there is reason to consider basing the RDA for carbohydrate on the overall diet. Notably, the carbohydrate RDA was not used in developing the Dietary Guidelines for Americans 2005 (DHHS/USDA, 2004, 2005). In this example, the research question might be, What level of carbohydrate intake is commensurate with a healthy diet?
Added Sugars
The recommendation to limit added sugars to no more than 25 percent of calories was derived from a review of all the studies that examined the intake of added sugars and its relationship to micronutrient
intake. The cutoff point at which decreased intake of micronutrients appears to become statistically significant is approximately 25 percent of calories coming from added sugars.
Three longitudinal studies that show an increase in weight gain with added sugars from certain sources have been released since 2002 (Berkey et al., 2004; Mrdjenovic and Levitsky, 2003; Phillips et al., 2004). Other studies are in progress. These new data show that over time, in the same group of individuals, weight gain occurs if one consumes added sugars, especially if the sugars are obtained from soft drinks (sodas). Importantly, to develop food patterns that follow the 2005 Dietary Guidelines and meet nutrient needs and energy, most of one’s energy must be obtained from the food groups, and very few calories are available to use in the form of added sugars.
Discretionary calories was the name given by the Dietary Guidelines Advisory Committee (DHHS/USDA, 2004) for the difference between energy needs and the energy provided by servings from the food groups to meet nutrient needs. Added sugars fit into the discretionary calories category. Thus, Dr. Lupton suggested considering the new literature and the ongoing studies on added sugars and weight gain, and how many discretionary calories can be consumed without gaining weight.
Glycemic Response
The research on the glycemic response to the diet is advancing to the point where a panel might make specific recommendations. The need now is for clinical intervention trials that compare diets with high glycemic index or load to diets with low glycemic index or load, using appropriate end points, including diabetes, hemoglobin A1c, blood glucose, and blood insulin.
Fiber
An AI was set for total fiber, which includes the fiber from foods (dietary fiber) and the fiber that is synthesized or extracted and added to foods (functional fiber). Decreased risk of coronary heart disease was the end point used. Although the recommendation was based on the totality of fiber and coronary heart disease (CHD) research, the specific numbers for the DRI value were generated from three prospective trials. Dr. Lup-
ton stated that a randomized clinical trial, preferably with three levels of fiber intake and surrogate markers for CHD, would be necessary to move from an AI to an EAR for fiber. Alternatively, a panel might consider changing the clinical end point from decreased risk of CHD to improved bowel health or healthy laxation, for example. Many studies with relevant data have been published, but agreement on the definition of healthy laxation or bowel health would be required.
Considerable concern has been expressed that the AI of 14 grams of fiber per 1,000 calories is too high for children. Thus, a research need is to study the effect of fiber intake, specifically in children.
A pertinent research question is whether a difference in overall health occurs if the fiber in a high-fiber diet is derived mainly from dietary fiber versus functional fiber. Would the end point be the same? To date, nearly all the research papers cover dietary fiber.
Dr. Lupton indicated that each fiber source that is promoted or suggested as a functional fiber needs to be tested for efficacy before it is added to the food supply. In addition, she raised a question about the potential for adverse effects from consuming too high a fiber intake from foods to which functional fiber has been added and whether there is a need for a Tolerable Upper Intake Level (UL) for functional fiber.
Fatty Acids, Fat, and Cholesterol
The report includes AIs for linoleic acid and for alpha-linolenic acid, the two essential fatty acids. Because the research literature was scant, the AI values were based on median intakes in the United States. It probably is important to revisit DRIs for fatty acids, particularly for n-3 fatty acids, to consider health promotion rather than deficiency symptoms. Also, considerable research published since 2002 concerning docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) merits consideration with regard to setting DRI values for these two fatty acids.
See the DRI Macronutrients Report (IOM, 2002/2005) for reasons why there is currently no UL for saturated fat, trans fat, or cholesterol. According to Dr. Lupton, this lack presents a conundrum that needs to be addressed. She proposed a research recommendation to determine the lowest levels of saturated fat, trans fat, and cholesterol that are consistent with a healthy diet and that may cause a low but acceptable amount of harm.
Amino Acids
Because insufficient data were available on dose–response relationships, no ULs were set for amino acids even though some of them are known to result in toxic effects at high doses. This research gap continues to merit attention.
Energy and Physical Activity
With regard to energy and physical activity, it is notable that the single-most contentious issue in this report is the recommendation for one hour of moderate intensity physical activity per day to maintain normal body mass index. Three major research needs include the following:
-
Expand the doubly labeled water database.
-
Determine the effect of physical activity on overall health and wellness rather than solely on body weight and/or risk of disease.
-
Decide on the place and significance of physical activity in the overall arsenal of efforts to promote public health. These efforts include the DRI process, the Dietary Guidelines for Americans, and food intake surveys.
RESEARCH PRIORITIES: ENERGY AND PHYSICAL ACTIVITY FRESH PERSPECTIVES
Presenter: Harold W. Kohl
This presentation provided background information on physical activity as related to Dietary Guidelines for Americans and then focused on a selection of the many specific research recommendations contained in the DRI Macronutrients Report.
Physical Activity and Dietary Guidelines for Americans
Physical activity was incorporated in the Dietary Guidelines for Americans in 1990 when the role of physical activity for energy balance
was first acknowledged. Over the ensuing years, physical activity gained increasing recognition in the guidelines. Most recently, in 2005, a specific recommendation was made that both adults and children should accumulate 60 minutes of daily moderate intensity physical activity in addition to the activities required to maintain a sedentary lifestyle to prevent weight gain and to promote additional health benefits.
Status of Research Recommendations Pertaining to Energy and Physical Activity
The DRI Macronutrients Report (IOM, 2002/2005) contains 30 specific recommendations for energy (13 labeled as major knowledge gaps, 13 as knowledge gaps, and 4 as research methods), and an additional 18 specific recommendations for physical activity (only 4 of which are labeled as major knowledge gaps, 13 as knowledge gaps, and 1 as a research method).
Energy Expenditure and Weight Gain or Loss
Dr. Kohl focused on a few of the research recommendations, with his selections influenced by recent research findings. In particular, he took the position that emerging data now suggest that recommendations for patterns of energy expenditure and physical activity differ for the prevention of weight gain, for weight loss, and for the prevention of weight gain after a substantial weight loss. This information is relevant to children, adults, older adults, and pregnant and lactating women.
Regarding the prevention of weight gain, a key question is, What physical activity and energy expenditure patterns will prevent weight gain and for whom, and how would this interact with dietary intake (including diet composition)? Dr. Kohl considers research recommendation number 271-E2 (regarding energy requirements of overweight and obese individuals and their relationship to physical activity patterns) to be extremely critical in helping to answer this question. Some data suggest that the patterns for energy requirements for overweight and obese people may be different than those for people who never gain weight or who maintain their weight over time.
|
2 |
To find the exact wording of each research recommendation to which an identification code corresponds, see Appendix C. |
An understanding is needed of some of the longitudinal aspects of physical activity in preventing weight gain. Dr. Kohl repeatedly emphasized investigation of the form, frequency, intensity, and duration of exercise and physical activity in relation to the successful management of body weight.
With regard to weight loss strategies, why do existing data not support an additional benefit of physical activity (above dietary restriction)?
Methods
Some of the disparate results seen in studies of weight loss and of the prevention of weight gain or weight regain may be methodologically driven. Thus, there is a need for reliable, noninvasive, and clinically appropriate measurements of body composition, cardiovascular function, and fitness. Much more thorough assessments are needed regarding the form, frequency, and intensity and duration of exercise, and on their interactions as related to long-term risk for weight gain. Dr. Kohl considers it absolutely essential to expand the doubly labeled water studies of total energy expenditure, giving attention to the need for prospective data, adequate representation of age groups and ethnic groups, and a randomly selected set of study subjects.
Exercise and Substrate Utilization
Research on the effects of exercise on substrate utilization remains an important recommendation. Moderate intensity physical activity—namely, less than about six metabolic equivalents—preferentially oxidizes lipids and lipoproteins. Once the physical activity becomes vigorous, carbohydrates oxidize. Information is needed, however, on the effect of having the same dose of physical activity in terms of kilocalories but under different conditions. For example, two groups could burn the same number of kilocalories if individuals in one group have moderate intensity physical activity for a specific duration, and those in the other group are vigorously active for a shorter period. How would such an interaction help in understanding the process of weight loss?
Possible New Research Questions
Possible new research questions include the following:
-
By what mechanisms does it appear that formerly obese persons may need 60 to 90 minutes of physical activity daily to maintain weight loss? Some of the strongest data from randomized trials show that people who have lost a substantial amount of weight (which might be 30, 40, or 50 pounds or some significant percentage of their body weight) have a different energy requirement than do people who have not lost weight or who have lost weight and then regained.
-
What behavioral, environmental, policy, and other factors help people adhere to a physical activity and exercise strategy to help maximize their potential for maintenance of weight loss? Some data indicate that the people who exercise more frequently and who adhere to their physical activity regimens are more likely to maintain their weight loss. In the physical activity literature, evidence-based strategies have been identified that promote physical activity, both on the individual and on the environmental level. Thus, Dr. Kohl recommended that more attention be given to understanding factors influencing these behaviors.
-
To what extent do differences in body composition and fat-free mass need to be considered in studies—rather than just considering differences in body mass index?
Figure 7-1 illustrates several different conceptual relationships between physical activity and risk of selected diseases. Notably, consistent inverse associations exist between physical activity and the disease outcomes presented. Moreover, higher amounts of physical activity are associated with a continuing lower risk of disease outcome, but at an increasingly diminishing level. The major exception may be musculoskeletal injury. All these relationships together suggest that there are different kinds of associations of physical activity that go beyond weight, body fat, and obesity. In fact, it may be advisable to consider developing a process for physical activity recommendations that would parallel the process for the Dietary Guidelines, with updating of the recommendations perhaps every 5 years.
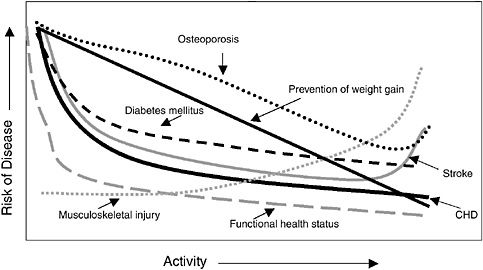
FIGURE 7-1 Risk curves with increasing physical activity, by disease or condition.
NOTE: CHD = coronary heart disease.
FIBER RESEARCH UPDATE
Presenter: Joanne L. Slavin
This presentation began with a very brief history of the evolution of dietary fiber, as illustrated by Figure 7-2, and the periodic “rediscovery” of fiber—culminating with the issuance of fiber definitions and AIs for fiber by the Institute of Medicine (IOM, 2002/2005). Additional topics included considerations for setting DRI values for fiber, research progress, and research questions that merit more attention.
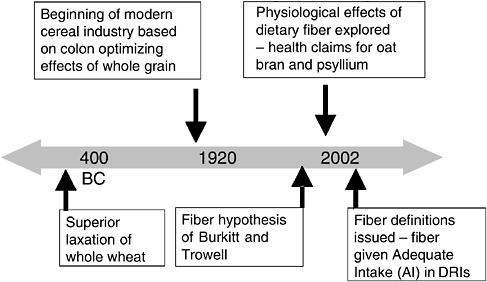
FIGURE 7-2 Highlights of the evolution of attention to dietary fiber, 400 BC–AD 2002.
Considerations for Setting DRI Values for Fiber
Unlike the case for most other nutrients, the recommended intake of fiber was based on protection against disease, not another functional end point. Dr. Slavin agreed with Dr. Lupton that applying the adult AI for fiber (14 g/1,000 kcal) to set the AI for children leads to a higher AI than needed. The AIs for children are much higher than earlier recommendations (e.g., the recommended number of grams of fiber per day equals five plus the child’s age); such recommendations were made by other expert groups and were based mainly on intakes. Applying the same ratio (14 g of fiber/1,000 kcal) to elderly adults results in a lower absolute AI than for younger adults. This appears inconsistent considering older persons’ concerns about getting enough fiber. The AIs for children and the elderly are based on a calorie conversion factor, not on empirical data. In fact, since fiber was just designated as a nutrient, less relevant human research has been conducted than is the case for some of the other nutrients. In contrast, much useful research related to pet animals and pigs may be available.
Because fiber is nondigestible, it seems obvious that information about fecal material could be used as an indicator in setting DRIs for fi-
ber, and the DRI macronutrients panel investigated that possibility. However, inconsistencies arise when relating fiber intake to either stool output or to a marker in the stool. In part, this is due to the many factors in addition to fiber intake that affect laxation including
-
stress,
-
exercise (Oettle, 1991),
-
smoking,
-
coffee drinking,
-
drugs (Lembo and Camilleri, 2003),
-
personality (Tucker et al., 1981), and
-
type of fiber (per gram of fiber fed, wheat produces a greater weight of stool than do oats, and oats produce a greater weight of stool than does pectin [Cummings, 1993]; most types of fiber have not been studied).
The definition of normal laxation—from three or more stools per week to three or fewer stools per day—covers a wide range. Moreover, definitions related to laxation have some inconsistencies. For example, stool weight greater than 200 g/day has been clinically defined as diarrhea (Fine and Schiller, 1999), but many vegetarians have stool weights of 300 g/day or more.
Research on laxation presents some obvious problems. Collecting fecal samples is not practical in epidemiological studies. Moreover, there is no accepted standard with regard to stool weight, stool chemistry, microflora (preferred methods and desirability of different organisms), stool frequency (promising because it is easy data to collect), or quality of life (a measure used in irritable bowel syndrome trials).
Research Progress
The DRI Macronutrients Report contains 12 research recommendations pertaining to fiber—all of which Dr. Slavin rated as highly important, and most of which involved some collection of fecal samples. Because essentially no investigators are collecting fecal samples, little progress has occurred.
Research progress has been made, however, with regard to the relationship of dietary fiber and C-reactive protein (CRP) concentrations. Ajani et al. (2004), using data from the 1999–2000 National Health and
Nutrition Examination Survey, reported that dietary fiber intake is inversely associated with serum CRP. The odds ratio for increased CRP was 0.49 for the highest quintile of fiber intake compared with the lowest. In addition, Ma and colleagues (2006) conducted a longitudinal study of 529 subjects and reported that dietary fiber intake is protective against high CRP.
Despite the strong and consistent evidence that higher levels of fiber intake are protective against CHD, it remains unclear why the data are so strong. It may be in part because of serum cholesterol lowering, but also perhaps because of lower CRP.
Research Questions That Merit More Attention
Some big questions regarding dietary fiber and functional fiber merit more attention. What measurements should be recommended for investigating effects of feeding functional fibers? Are the most important parameters effects on blood cholesterol, CRP, microflora, stool weight, or other? What studies would provide a sound basis for setting fiber recommendations for children, adolescents, and older people? Dr. Slavin considers it important to revise the AI for children and adolescents.
Most of the 12 research recommendations call for basic information, such as feeding dose amounts of fibers and measuring stool weight. Dr. Slavin pointed out that accomplishing these studies will take dedicated research funding because such research would not be funded in the competitive research arena. If food or fiber companies want to know that the fiber has a specific health effect, they might be interested in conducting research that provides information that a regulatory agency will request in the future.
DISCUSSION
Questions and comments during the discussion period focused mainly on (1) the relationship of discretionary calories to the RDA and to energy expenditure, and (2) carbohydrate recommendations.
Discretionary Calories
Discussants disagreed about the value of the concept of discretionary calories and noted that the concept is difficult to communicate effectively. Dr. Murphy clarified that the RDA is about 120 percent of the EAR, not the much higher amounts stated during the discussion. Several discussants pointed out that physical activity is the factor that has the biggest impact on discretionary calories. Dr. Kohl mentioned Jean Meyer’s studies in the 1950s that suggested a physical activity threshold below which energy regulation may be impaired, and Dr. Dwyer encouraged replication of those studies.
Carbohydrate Recommendations
Dr. Bier noted the essentiality of glucose for the brain and suggested that the problem is not the carbohydrate RDA but a communication issue. Dr. Lupton agreed that carbohydrate recommendations led to misunderstandings, especially with regard to the recommendation not to exceed an added sugars intake of 25 percent of energy intake.














