2
Background
HEALTH IN THE BALANCE: RECOMMENDATIONS FOR THE U.S. POPULATION
The childhood obesity epidemic was recognized in the United States as well as in other places around the world; it is an alarming trend in children of all ages. Figure 2-1 shows that the percentages of obese children have doubled in the early teen years and tripled for children in the 6–11 years of age range. The epidemic affects millions of children in the United States, and its persistence is clear. The reasons for the concern over the obesity prevalence increase stems largely from its very serious comorbidities (see Box 2-1), including a predisposition toward diabetes—a new form of the disease that formerly occurred only in adults. The onset of child diabetes used to be a more genetically determined disease, however, there now is a need to shift strategies because of the change in disease patterns.
Jeffrey Koplan, chair of the Committee on Prevention of Obesity in Children and Youth, summarized highlights from the IOM report Preventing Childhood Obesity: Health in the Balance (2005). The report was published after two years of deliberations by the committee and support from the CDC, the National Institutes of Health, the Office of Disease Prevention and Health Promotion of the Department of Health and Human Services, and the Robert Wood Johnson Foundation. The study was a collaboration between the IOM’s Food and Nutrition Board and the Board on Population Health and Public Health Practice. The final report was produced by a diverse committee of 19 people and in accordance with IOM procedures.
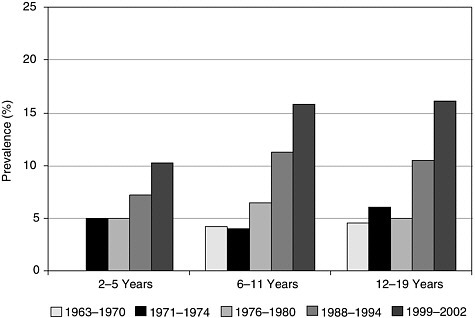
FIGURE 2-1 Childhood obesity prevalence, 1963–2002.
SOURCE: Hedley et al. (2004).
|
BOX 2-1 Implications for Children and Society: Physical, Social, and Emotional Health Consequences of Obesity Physical Health Glucose intolerance Insulin resistance Type 2 diabetes Hypertension Dyslipidemia Hepatic Steatosis Cholelithiasis Sleep apnea Orthopedic problems Emotional Health Low self-esteem Negative body image Depression Social Health Stigma Negative stereotyping Discrimination Teasing and bullying SOURCE: IOM (2005). |
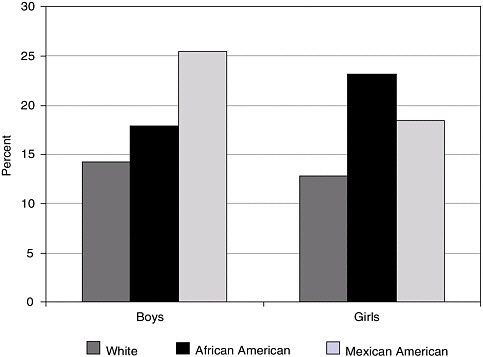
FIGURE 2-2 Childhood obesity prevalence in children 6–19 years old in 1999–2002.
SOURCE: Hedley et al. (2004).
In their search for interventions to prevent obesity, committee members and members of the public offered many single solutions—for example, eliminating vending machines from schools, increasing physical activity levels, and eliminating sweetened carbonated beverages or fast foods. However, although these elements might be contributory and important in childhood obesity prevention, the committee shared the view that a comprehensive study of the entire environment and all the sub-populations in the United States would be important in recognizing and understanding the elements’ interrelations and how they impacted childhood obesity. To show the severity of the problem, Koplan presented Figure 2-2 with trend data for obesity prevalence from 1963 to 2002 among some U.S. ethnic populations.
The committee decided early in the study that although more research is needed before there is unequivocal scientific evidence to take definitive, specific actions, waiting for the evidence before taking action would be irresponsible. Because the problem is so urgent and widespread, the com-
mittee recommended that actions be taken based on the best available evidence, rather than waiting for the best possible evidence. The committee was careful, though, to emphasize the need for further evaluation and measurement of the recommended actions since many have not been validated. This need to measure the effectiveness of the applied interventions within and across different sectors is the focus of an ongoing IOM study on the progress in preventing childhood obesity (IOM, 2007).The study emphasizes the importance of evaluating programs and interventions in government, industry, schools, communities, and at home.
The committee concluded that childhood obesity is a serious nationwide health problem with multi-factorial causes requiring a population-based prevention approach and a comprehensive response. The committee also concluded that it is important to maintain energy balance for children and youth through the promotion of healthy eating behaviors and regular physical activity. Achieving energy balance is a process that relies on equalizing calories consumed versus calories expended. The goal, therefore, is to create energy balance in which physical activity and a healthful diet merge to improve the long-term health of future adults. Since preventing childhood obesity is a collective responsibility, this goal will be realized only by actively engaging many players and sectors, including parents, schools, governments, the food and beverage industry, the advertising industry, the physical activity industry, community groups, volunteer groups, and professional organizations such as medical and health groups (see Box 2-2). During the workshop, Koplan suggested that this concept of collective responsibility also might apply to Mexico.
|
BOX 2-2 Key Stakeholders Involved in Preventing Childhood Obesity
SOURCE: IOM (2005). |
Unfortunately, society is typically crisis-driven; that is, only when faced with an acute public health issue does society respond with sufficient leadership and resources to mitigate it. Childhood obesity prevention is a long-term goal, and just as it took years for obesity to develop into an epidemic, the timeframe to begin reversing the problem might take years of coordinated multidisciplinary interventions. Because the rise in obesity prevalence has occurred over a long period of time and because it brings a complicated picture of contributors and solutions, the response has been inadequate.
Koplan emphasized that it is important not to undermine the interesting activities evolving in the communities, schools and school systems, and YMCAs, activities helping to change social norms (e.g., driving instead of walking, paying less money but receiving larger food servings, and using the elevator instead of the stairs) and encourage a reversal of the obesity problem. Also, Koplan noted that societal norm changes in countries such as Australia or Western Europe could serve as positive models for change. Although changing societal norms may seem like an insurmountable task, there are examples of successful health programs that have effected changes in social norms in the United States, for example, highway safety, tobacco control, and attitudes toward drinking and driving.
The IOM report’s action plan includes a series of specific recommendations. For example, when targeting families and home life, the action plan recommends breastfeeding over other means, and for governments it recommends ensuring that all school meals meet the Dietary Guidelines for Americans. The report engages the whole society, including parents and healthcare providers, as part of the solution. There is undoubtedly an element of individual responsibility associated with making food choices; however, children cannot differentiate between health messages and pure product marketing, so individual responsibility becomes a less significant factor in the case of childhood obesity. Koplan stated that even though individuals need to make the right choices, society (e.g., industry, schools, government, and parents) needs to help.
OBESITY IN CHILDREN AND YOUTH OF MEXICAN ORIGIN: A SILENT BUT ALARMING EPIDEMIC
As mentioned by Rivera, obesity is undoubtedly one of the major public health problems in Mexico, and the devastating effects of obesity on health threaten to raise the burden of health services and affect not only the health but also the productivity of the population.
Sepúlveda highlighted indicators of the obesity epidemic in Mexico. He pointed out that according to the Organization of American States (http://www.oas.org), among its 30-country membership, Mexico sits in second place as far as having the highest rates of prevalence for obesity and risk for
obesity. In Mexico, an anthropometric review of survey household data revealed that almost 29 percent of the country’s preschool children are obese or at-risk of becoming obese (based on the U.S. reference population and definitions). In Mexican schools, one of every five children is obese. In the adult population, two-thirds of all men and women have tendencies toward obesity or are obese, and one of every five Mexicans is obese. Moreover, according to the last National Health Survey (Olaiz et al., 2003) 8 percent of the Mexican population is diabetic, and 30 percent of Mexican adults have hypertension. The metabolic syndrome that accompanies obesity— which includes hypertension, hypercholesterolemia, and cardiovascular disease—is burdening Mexican public health, to a magnitude not yet realized. To add to the complexity of the obesity epidemic, there is still a serious problem of malnutrition and micronutrients deficiency in Mexico.
Despite the alarming trends and existence of survey systems (e.g., the National Health and Nutritional Surveys) and national programs (e.g., Progresa and Oportunidades), Sepúlveda acknowledged these findings have not yet been translated into government decisions and public policies. Mexican authorities and society in general have not initiated preventative strategies.
The information in this section summarizes presentations by the authors of the two background papers—“Preventing Obesity in Mexican Children and Adolescents” and “Preventing Obesity in Mexican–American Children and Adolescents.” For more details on the data available on obesity prevalence among Mexican and Mexican–American children and youth see Appendixes B and C, respectively.
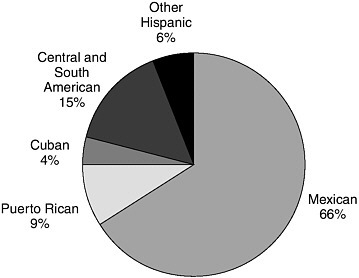
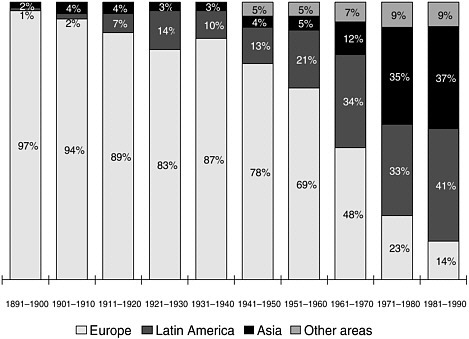
Fernando Mendoza, Stanford University School of Medicine, introduced the workshop audience to the cultural factors that define the Latino family and to the acculturation process they experience as they integrate into U.S. society. These factors are key to understanding the causes of obesity and proposing solutions. For example, a traditional Latino family holds strong Mexican cultural and religious traditions; when the acculturation process begins their traditional lifestyles change. The nature of these changes as they relate to factors that contribute to obesity is not fully understood, but it appears that U.S. social norms with respect to diet and exercise are adopted by Mexican Americans as they acculturate into mainstream society. Latinos, the largest minority population in the United States, represent 14 percent of the U.S. population and are predicted to represent about 25 percent by 2030 (NRC, 2006). From that Latino population, almost two-thirds are Mexican American, so Mexican Americans are the most prominent Latino group in the United States (see Figure 2-3). Because of the continued influx of Mexicans and other Latinos into the United States, there is a range of acculturation levels among them. Figure 2-4 shows the dramatic changes in the U.S. population throughout the century due to immigration
from Europe, Latin America (principally Mexico), and Asia. Vivid examples of states where the majority of the population is no longer white but people of color (primarily Latinos) include New Mexico, Texas, California, and Arizona. Approximately one third of California’s population is Latino (primarily Mexican American); half of the babies born in California are either Mexican Americans or of other Latino heritage. This increase in the Latino population has spurred a great interest among policy makers and public-life leaders.
Mendoza pointed to the fact that for many years the health and social concerns among Mexicans in the United States went unnoticed because the Mexican population was not large enough to be considered for surveys. Today Mexican Americans have problems with obesity, homicide, poverty, and accidents. The third National Health and Nutrition Examination Survey (NHANES) (Burgos et al., 2005) shows that in the early 1990s 75 percent of the first generation of Mexican Americans was in poverty, two-thirds were uninsured, and approximately 80 percent possessed less than a ninth-grade education. The higher poverty rate of Mexican Americans compared with other non-Latino whites appears to continue into the second and even third generations. Thus, poverty is an issue both for Mexican and Mexican Americans, and as such its environmental correlates are important factors to examine in the evaluation of obesity among Mexican and Mexican Americans. Even though genetic factors might provide a predisposition to obesity, the environment is really what makes the biggest difference between being obese and non-obese and, in general, having good and poor health. The hope is that with the increase in the Mexican–American population greater attention will be given to this population, and public policy will address obesity and other health disparities affecting them. With new leaders such as Antonio Villaraigosa in public policy, the mayor in Los Angeles, the city with the largest population of Mexicans outside Mexico, positive changes may happen.
Robert Valdez, Univision Communication Corporation’s “Salud es Vida: ¡Enterate!,” added that a complex cultural transition process is happening not only in the United States but also in Mexico and is reflected in the differences between northern and southern Mexico that developed over the last several years. In addition, there is a third emergent culture along the U.S.–Mexican border where the cities on both sides are becoming more similar. Understanding the basic principles; causes; and social, psychological, and economic consequences of this cultural adaptation process will allow researchers and players in other sectors to better understand and prevent the obesity problem.
For the purposes of this workshop and background papers, children at-risk for obesity were defined as those with a BMI in the 85–95th percentile, and obese children were defined as those with a BMI in percentiles higher
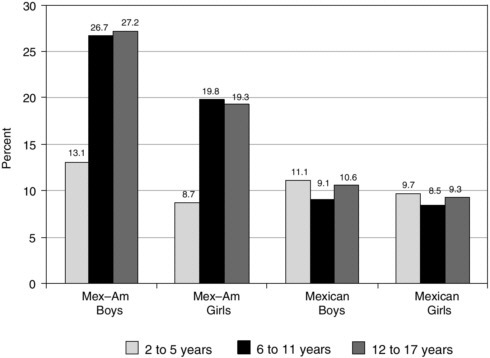
FIGURE 2-5 Obesity prevalence in Mexican–American and Mexican Children, 1999– 2000.
SOURCE: Rivera et al. (2002) and del Rio-Navarro et al. (2004).
than the 95th. BMI, rather than waist circumference, was used as an obesity indicator because not only is it currently the parameter most commonly used but also it is standardized and easy to measure. Whether measured by BMI or waist circumference, the obesity issue in the United States is most urgent among the Mexican–American community (see Figure 2-5). In fact, the summary of epidemiological data in Appendix C indicates that among various ethnic groups (i.e., White, African American, and Mexican American), Mexican Americans show the highest obesity prevalence in both the 2–5- and 6–11-year-old boys. A similar conclusion is drawn from obesity prevalence data in girls. Clearly, preventing obesity in Mexican–American children presents an important public health challenge; the problem is also severe among other ethnic groups.
Comparing only the U.S. and Mexican–American populations in Figure 2-5, Mexican–American boys and girls are more obese in the older-age groups and somewhat more obese in the younger-age groups. The problem affects the entire U.S. population, with an increase in obesity in boys from 14 percent to 18 percent, a 30 percent increase from the 1980s to the 1990s.
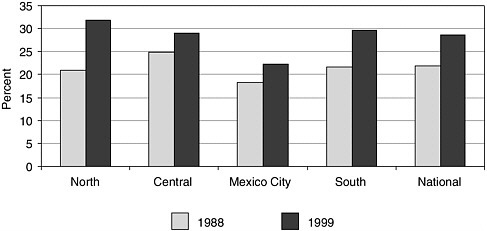
FIGURE 2-6 Prevalence of obesity or at risk for obesity by region and year of survey (children ages 2–4 years).
SOURCE: Rivera et al. (2001).
Mendoza reminded the audience that the obesity epidemic for Mexican Americans is nothing new and was recognized from all the NHANES surveys; for the first time, however, it has been recognized publicly not only as a national issue but also as an issue that greatly affects Mexican Americans.
Ruy López, INSP, presented a summary of the data on obesity prevalence in Mexico, where the nature of the obesity epidemic in children 2 to 4 years of age can be appreciated from the National Nutrition Surveys conducted in 1988 and 1999 (see Appendix B and Figure 2-6). Although it can be argued that the parameters used here and in Appendix B might not constitute ideal indicators of obesity or risk of obesity in the Mexican population because the reference is the U.S. population, the authors argued that those indicators should be used until a more appropriate reference population database is developed.
Martorell commented that the prevalence levels underestimate the obesity problem because of the reference curves used; he compared the reference curves to the World Health Organization’s (WHO’s) new growth curves for children under 5 years of age, based on studies done in Brazil, India, Ghana, Oman, Norway, and the United States with breastfed children of a high socioeconomic level. Martorell believes that these new curves should be used in the future because they reflect optimal growth as compared with the growth curves currently used (see also Appendix C). It is critical that the public be informed about the value of their use and that researchers coordinate and compare data across countries. Rivera suggested
that data currently being collected on malnutrition, overweight issues, obesity, and risk of chronic disease from the third National Survey on Health and Nutrition could be analyzed using the WHO’s new reference curves so that consensus on interpretation could be reached. Regardless, a preliminary assessment of the data indicates that several prevalences, including those for low weight for size, low size for age, and obesity, will increase.
Lopez noted that despite these questions a study by Villalpando (Villalpando el al., in press), which analyzed data from a national survey, demonstrates that children 10–19 years old showed a significantly higher glucose level before breakfast; higher levels of insulin, cholesterol, and triglycerides; and lower levels of high-density lipoproteins for obese or at-risk of obesity children than for normal weight children. These measurements are indicators of cardiovascular disease and demonstrate the severity of this problem in Mexico among obese or at-risk for obesity children.
Lopez concluded that it is clear from the survey data that the epidemic is real; however, information available at this time provides only suggestions for the possible risk factors associated with the epidemic. Based on the current epidemiological data, participants acknowledged that an obesity epidemic similar to the U.S. epidemic is also occurring in Mexico. Despite the limited information on potential risk factors associated with childhood obesity in Mexico, participants emphasized the urgency for key players to initiate preventative interventions for reversing the epidemic.
RISK FACTORS ASSOCIATED WITH CHILDHOOD OBESITY
This section summarizes the limited data on potential risk factors associated with childhood obesity in children and youth of Mexican heritage. For a more detailed description see Appendixes B and C. A discussion of the factors associated with this growing epidemic shows few controversies: authors of both background papers concluded that the lack of energy balance is the fundamental issue underlying the epidemic. However, when attempting to understand all the interrelated factors that make up the concept of energy balance they agreed that the picture is less clear. Intuitively, dietary factors and physical activity are the key factors but what are the environmental, genetic, physiological, or cultural factors that contribute to an energy balance? Lopez used Figure 2-7 (adapted from the 2005 IOM report Preventing Childhood Obesity: Health in the Balance) to represent an ecologic model that embraces interrelated factors affecting obesity.
Data for children 2–4 years old, the only age group for which data on trends exist in Mexico, suggest a similar increase in the prevalence of obesity as that seen in the United States (see Figure 2-6). Moreover, this figure shows that the prevalence of obesity is evident in all regions of the country. Lopez discussed the influence of socioeconomic status; in general, the preva-
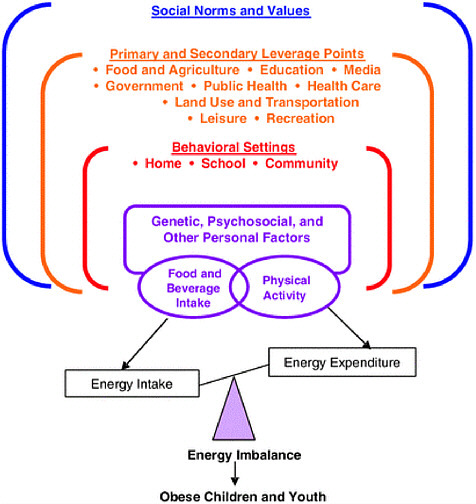
FIGURE 2-7 Factors influencing childhood obesity: ecological model.
SOURCE: IOM (2005).
lence of obesity in children increases as the socioeconomic level of the family increases. However, this is not the case in adults, where in the last two surveys associations among socioeconomic levels and obesity are the reverse. That is, the higher socioeconomic level of the family is associated with a lower prevalence of obesity. During the discussion, Rivera commented that the positive relationship between obesity and socioeconomic level in children implies that any program that improves wages in the population might also result in increases in the prevalence of childhood obesity.
In this sense he recommends that in programs like Mexico’s Oportunidades, for example, improvements in income should happen in parallel with interventions to prevent obesity. The association between obesity and socioeconomic level seems to be different in the United States, where, in general, the more deprived sectors of society appear to have children with the highest rate of obesity (this association seems also to be the case for Mexican Americans). According to Rivera, an association between socioeconomic status and obesity similar to Mexico’s also has been seen in Brazil; one explanation could be that this obesity trend is related to industrial development.
Several Mexican participants highlighted one factor that distinctly sets apart the obesity epidemic in Mexico, that is, the coexistence of obesity and malnutrition, sometimes within the same family. This dual burden of disease should be considered when identifying solutions, especially when the prevalence of malnutrition in Mexico is higher than in other Latin American countries. Wasting rate, a parameter that measures malnutrition in terms of weight for age, has decreased but low size for age continues to exist in Mexico and is associated with low socioeconomic status. Micronutrient deficiencies, including anemia in obese children, is also observed in Mexican populations.
The following sections underscore information on various factors, their interrelations, and their potential association with the obesity epidemic. Also, differences and similarities highlighted among the Mexican– American and Mexican populations are presented.
Diet-Related Factors
Frederick Trowbridge, Trowbridge and Associates, Inc., addressed the importance of psychosocial factors contributing to the high prevalence of obesity. He noted that these factors affect dietary habits and physical activity participation among Mexican immigrants as they integrate into U.S. culture. For example, U.S.-born Hispanics and long-term immigrants are much more likely to be obese than their foreign-born counterparts. U.S.-born Hispanics eat more fat and less fiber, as reported in dietary studies. Adolescents from more acculturated families eat more fat, protein, and calories. These findings point to changing dietary habits favoring obesity-prone diets. These changes in dietary habits also might originate from poverty and associated inaccessibility to affordable healthy foods.
Lopez described a different kind of nutritional transition occurring on the other side of the border, the one experienced by Mexicans in both urban and rural environments. Data from the 1988 and 1999 National Nutritional surveys (Barquera et al., in press) show an increase in fat intake and a decrease in carbohydrates intake. Income and Spending National Surveys report that spending for carbonated beverages, sodas, and refined carbohy-
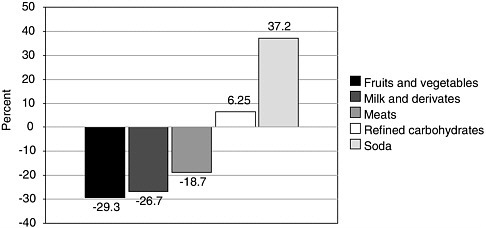
FIGURE 2-8 Changes in mean food purchases in 1996 (relative to 1994) by food group.
SOURCE: Rivera et al. (2004).
drates increased from 1994 to 1996; in contrast, spending for fruits and vegetables decreased, possibly because of high prices (see Figure 2-8). Additionally, data show that 60 percent of school children consume less than 100 grams of fruits and that only 8 percent of the school population follows the recommendation of five fruits or vegetables a day. Other food consumption data show that almost 40 percent of preschool-age children’s energy comes from processed food; this appears to happen not only in urban areas but also in the rural environment.
Rivera and colleagues have collected research data that provides invaluable information about the situation in the school environment. The data suggest that childhood obesity is favored by a lack of water in schools (i.e., children substitute carbonated, high-calorie drinks for water), a lack of regulations or guidances appropriate for school food choices, and greater access to high-energy food than to nutritious food such as fruit.
Lopez stressed that although the evidence supporting the hypothesis that these foods contribute to obesity is unclear, there is enough information to believe that the transition in dietary habits might be contributing to obesity in the Mexican population. Concomitant with this dietary transition period, the fast food industry has grown, and street food in Mexico is being made with less healthy options such as cheaper, less healthy cooking oils.
Physical Activity-Related Factors
Trowbridge summarized the data regarding physical activity among Mexican Americans (see Appendix B). A literature review on physical activity revealed that free time physical activity self-reported by 9–13-year-old children and teenagers is similar in all the ethnic groups, but White, Non-Hispanics report much more participation in organized physical activity than African Americans or Hispanics; this finding may be related to unique barriers such as availability and expense to join an organized activity (i.e., entrance fees are required to join leagues), lack of transportation, availability of organized programs, and personal safety in the Mexican–American population as reported in the surveys.
Lopez presented Figure 2-9 to illustrate the results of a study by Bernardo Hernández in Mexico City that examined levels of physical activities in children 9–16 years old by income level. Regardless of the income level, the time spent viewing television and other videos is higher than the time spent on physical activity. The data from Mexico City showed that children who watch television for more than three hours daily have a 1.69-times higher risk of being obese than those who watch just one hour. (The
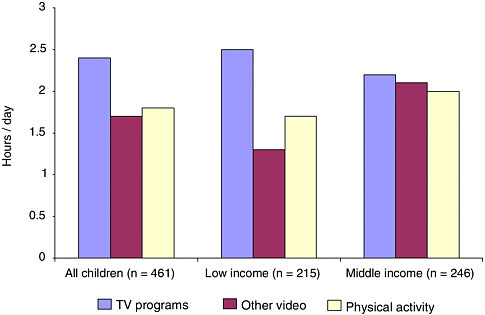
FIGURE 2-9 Levels of physical activity or inactivity. Mean time dedicated to video viewing and physical activity in children 9–16 years old in Mexico City.
SOURCE: Hernández et al. (1999).
recommendation by international experts is for children to engage in no more than two hours of screen viewing per day). Although there are no published national data on physical activity or its association with obesity, similar associations as in Mexico City have been found in other Mexican urban settings. Although no related survey data were found, personal safety could be an important barrier to Mexican children and youth engaging in physical activity, just as it is a barrier for the U.S. Hispanic population. In addition, a worrisome fact is that the school policies regarding physical activity are generally not followed, and 30 percent of the children do not enjoy physical activity at school, as observed in a small sample where physical activity constituted an average of only 10 minutes per day. In addition, extracurricular programs, which could add some physical exercise to children’s daily activities, are very difficult to implement in Mexico.
Culture-Related Factors
As mentioned previously, sociopsychological and cultural factors play an important role in defining diet and physical activity habits of a population. Among them, culturally-based perceptions of body weight cannot be overlooked; for example, Trowbridge said that Hispanic mothers might be more likely to equate plumpness with healthy weight. Also, the strength of the idea of family is very powerful in Hispanic families and may have some unintended consequences on attitudes toward physical activity. For example, the CDC Youth Media Campaign Longitudinal Survey found that Hispanic youth were taught to put family needs above their own needs and that physical activity for their own benefit may be discouraged (see also Appendixes B and C and IOM, 2006). The lack of health insurance and access to healthcare might also constitute barriers to obesity prevention.
Several social and family factors seem to be unique in affecting Mexican dietary habits and some may remain as part of the Mexican heritage of the Mexican–American community in the United States. For instance, similar to the Mexican–American community, Lopez noted that although there is no scientific basis to confirm the idea that “chubby children are healthy children,” it is very much engrained in low-income populations. Also, enjoying comforts and appliances such as television provides a certain desirable social status. The data about television access and Internet usage (see Appendix B) point to a higher use by children and youth over time, which could be seen as an opportunity (e.g., to communicate messages about health via television and the Internet) as well as a threat (e.g., supports the evidence of increased physical inactivity) for Mexican children. Nevertheless, increased car sales, television watching, and time spent on computers and the Internet suggest that Mexico is moving towards an obesogenic environment.
Regardless of the strength of the association between risk factors and the prevalence of obesity, the following are some critical elements that, according to Lopez, speak about the urgency of the matter:
-
The prevalence of obesity among children is growing.
-
The severity of the impact of obesity in both long-term health and economy could increase.
-
Today’s child and youth obesity epidemic will be observed in the future as children grow into adults.
This sense of urgency to take action against the obesity epidemic was transparent during the course of workshop discussions and was expressed in reference to both the United States and Mexico.
REFERENCES
Barquera S, Hotz C , Rivera J, Tolentino L, Espinoza J, Campos I, Shamah T. In press. Food consumption, food expenditure, anthropometric status, and nutrition-related diseases in Mexico. In: Kennedy et al., eds. The Double-Burden of Diseases in Developing Countries. Rome, Italy: Food and Agricultural Organization.
Burgos A, Schetzina K, Dixon B, Mendoza F. 2005. Importance of generational status in examining access to and utilization of health care services by Mexican American children. Pediatrics 115(3):322–330.
del Rio-Navarro BE, Velazquez-Monroy O, Sanchez-Castillo CP, Lara-Esqueda A, Berber A, Fanghanel G, Violante R, Tapia-Conyer R, James W. 2004. The high prevalence of overweight and obesity in Mexican children. Obesity Research 12:215–223.
Hedley AA, Ogden CL, Johnson CL, Carroll MD, Flegal KM. 2004. Prevalence of overweight and obesity among U.S. children, adolescents, and adults. Journal of the American Medical Association 91(23):2847–2850.
Hernández B, Gortmaker SL, Colditz GA, Peterson KE, Laird NM, Parra-Cabrera S. 1999. Association of obesity with physical activity, television programs and other forms of video viewing among children in Mexico City. International Journal of Obesity 23: 845–854.
IOM (Institute of Medicine). 2005. Preventing Childhood Obesity: Health in the Balance. Washington, DC: The National Academies Press.
IOM. 2007. Progress in Preventing Childhood Obesity: How Do We Measure Up? Washington, DC: The National Academies Press.
NRC (National Research Council). 2006. Multiple Origins, Uncertain Destinies: Hispanics and the American Future. Washington, DC: The National Academies Press.
Olaiz G, Rojas R, Barquera S, Shamah T, Aguilar C, Cravioto P, Lopez P, Hernandez M, Tapia R, Sepúlveda J. 2003. Encuesta Nacional de Salud 2000, Tomo II. La salud de los adultos. Cuernavaca, Morelos, México: Instituto Nacional de Salud Pública.
Rivera JA, Shamah-Levy T, Villalpando-Hernández S, González de Cossio T, Hernández-Prado B, Sepúlveda J. 2001. Encuesta Nacional de Nutrición 1999. Estado Nutricional en Niños y Mujeres en México, ed. Oropeza. Cuernavaca, Morelos, México: Instituto Nacional de Salud Pública.
Rivera JA, Barquera S, Campirano F, Campos I, Safdie M, Tovar V. 2002. Epidemiological and nutritional transition in Mexico: Rapid increase of non-communicable chronic diseases and obesity. Public Health Nutrition 5(1A):113–122.
Rivera JA, Barquera S, González-Cossio T, Olaiz G, Sepúlveda J. 2004. Nutrition transition in Mexico and in other Latin American countries. Nutrition Reviews 62(7):S149–S157.
Villalpando S, Carrión C, Barquera S. In press. The body mass index is associated with hyperglycemia and alterations of some components of the metabolic syndrome in Mexican adolescents aged 10–19 years. Salud Pública de México.