Below is the uncorrected machine-read text of this chapter, intended to provide our own search engines and external engines with highly rich, chapter-representative searchable text of each book. Because it is UNCORRECTED material, please consider the following text as a useful but insufficient proxy for the authoritative book pages.
6 DEPARTMENT OF VETERANS AFFAIRS TOBACCO- CONTROL ACTIVITIES The Department of Veterans Affairs (VA) is responsible for providing health care and benefits to veterans and their dependents. Given the growing number of veterans leaving active military service and the recent rise in the proportion of these veterans who use tobacco, tobacco-cessation services will be an increasingly important element of VA programs. This chapter describes the services offered by VA, its structure and resources, and the population it serves with a view to identifying opportunities for improving and coordinating tobacco-control programs. VA estimates that there are about 24 million living veterans, many of whom have served in a US military conflict. Living veterans, their spouses and dependent children, and survivors of deceased veterans make up about 20% of the US population (VA, 2008a). VA provides health care, disability compensation, pensions, assistance with education and training, home-loan assistance, life insurance, vocational rehabilitation, and burial benefits to eligible veterans. In 2007, about 7.8 million veterans were enrolled in the VA health-care system (see Chapter 2 for a description of eligibility requirements for enrollment in the system), and 5.5 million individual veterans were treated (VA, 2008b). VAâs fiscal year (FY) 2009 spending is projected to be about $93.4 billion, including $40 billion for health care, $46.9 billion for benefits, and $230 million for the national cemetery system (VA, 2009a). VA employs almost 280,000 people, the overwhelming majority of them in the Veterans Health Administration (VHA). VAâs other two service organizations are the Veterans Benefits Administration and the National Cemetery Administration. ORGANIZATIONAL OVERVIEW In this section, the committee briefly describes the organizational structure of VA with an emphasis on identifying where responsibilities 263
264 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS and activities related to tobacco control reside. The relevant structure includes VHA, which provides health care for veterans; the National Leadership Board (NLB, a senior advisory group); the Public Health Strategic Health Care Group (PHSHCG) in VA headquarters, which develops policies and programs related to several major public-health concerns, including tobacco; and the Veterans Integrated Service Networks (VISNs, the regional units that administer VA health facilities). Veterans Health Administration VHA is charged with providing medical and rehabilitation services to veterans, medical research, graduate medical education, and emergency management. The VHA mission has shifted since the 1990s from a focus on inpatient care toward outpatient care. The changing focus has been reflected in the growth of outpatient clinics in the VA medical centers (VAMCs) and community-based outpatient clinics (CBOCs) to serve veterans who do not live near VA medical centers. VHA continues to provide long-term care for veterans in VA nursing homes and state-owned and -operated veteransâ homes, and contract care in private nursing homes, home health services, and adult day care. VHA does not provide health-care services for dependents or survivors of veterans, with a few exceptions. VHA is directed by the VA under secretary for health, who reports to the secretary for veterans affairs, a member of the Cabinet. Headquarters staff report to the principal deputy under secretary for health, as does the deputy under secretary for health for operations and management (see Figure 6-1). The VA health-care system provides direct health care, including outpatient and inpatient services. Veterans who enroll in the VA health system are assigned to one of eight priority groups (see Chapter 2, Box 2-8, for a description of the priority groups) on the basis of whether they have service-connected disabilities and on the basis of their income. Veterans who have medical conditions related directly to military service, those with lower incomes, and those who are uninsured are given higher priority than those with higher incomes or nonâservice- connected disabilities. Reservists and National Guard members who are called to active duty by a federal executive order may qualify for VA health-care benefits. Returning service members, including reservists and National Guard members who served on active duty in a theater of combat operations (for example, Iraq and Afghanistan), have special eligibility for hospital care, medical services, and nursing-home care for 5 years after discharge from active duty.
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 265 Secretary -------------------- Deputy Secretary Under Secretary for Health Veterans Health Administration Principal Deputy Under Secretary for Health -------------------- Assistant Deputy Under Secretary for Health for Clinical and Organizational Support Chief Public Health and Deputy Under Secretary for Health Environmental Hazards Officer for Operations and Management 21 VISN Directors FIGURE 6-1 VA organizational chart for tobacco-control responsibilities. SOURCE: Adapted from VA (2008c). VHA is a discretionary program and thus relies on annual budget appropriations from Congress. The number of veterans enrolled in VA health care grew from 4.18 million in 1999 to 7.42 million in 2004, and VAâs medical budget grew from about $20 billion in 1999 to about $28 billion in 2004 (Congressional Budget Office, 2005). If, in a given year, VA does not have sufficient funds to care for all enrollees, care is allocated to higher-priority groups first; when necessary, VA can freeze enrollment of veterans in lower-priority groups. The Congressional Budget Office notes that only a small fraction of eligible veterans are enrolled in the VA health-care system; about 20% of veterans in priority groups 7 and 8 were enrolled in 2004 (Congressional Budget Office, 2005). Many veterans are enrolled in private health-insurance programs through their employers or receive Medicare or Medicaid; some veterans have no insurance but have not enrolled in the VA system. Over 78% of
266 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS enrollees have some type of public or private health insurance: 40.7% are covered by Medicare B, 25.9% by Medigap, 16.2% by a health- maintenance organization (HMO) or managed care, 11.6% by non-HMO or nonâmanaged-care insurance, and 9.4% by Medicaid (VA, 2006a). Of veterans eligible for VHA medical care as of 2004, including enrolled and nonenrolled veterans, priority groups P1, P2, P3, and P4 together made up only 13% of the total veteran population. Most veterans are in priority groups P8, P7, and P5â37%, 22%, and 24%, respectively (Congressional Budget Office, 2005). National Leadership Board The VHA NLB was established by VA Directive 2008-035 to serve as a forum to advise the under secretary for health regarding the departmentâs mission, goals, and priorities. According to the directive, the NLB has âan active and extensive role in determining VHA policy, strategy, and oversight of organizational performance [and in] determining standards and measures for organizational performance, including financial performance, and ensuring that those standards and measures are metâ (VA, Directive 2008-035, 2008). The NLB comprises the under secretary for health, all directors of VISNs, all chief officers, and other senior leaders. It has provided support for several VA tobacco- control initiatives, such as the elimination of copays for tobacco- cessation counseling, the need for smoke-free VAMC facilities, and activities to increase tobacco cessation among VA employees. Finding: The NLB has the authority and expertise to develop and encourage the implementation of a VA-wide tobacco-control strategic plan and to ensure that VA leadership is engaged in the success of the plan. Public Health Strategic Health Care Group National oversight of tobacco-use cessation and tobacco-control policy and advocacy for tobacco control resides in the PHSHCG in the Office of the Chief Public Health and Environmental Hazards Officer (see Figure 6-1). The Public Health National Prevention Program, directed by the PHSHCG, is responsible for developing and overseeing public-health policy and clinical programs in VHA related to smoking and tobacco-use cessation. In headquarters, the director of the National Prevention Program is the primary staff member working on tobacco issues. The director administers a budget that includes policy development, dissemination, and training and is also responsible for
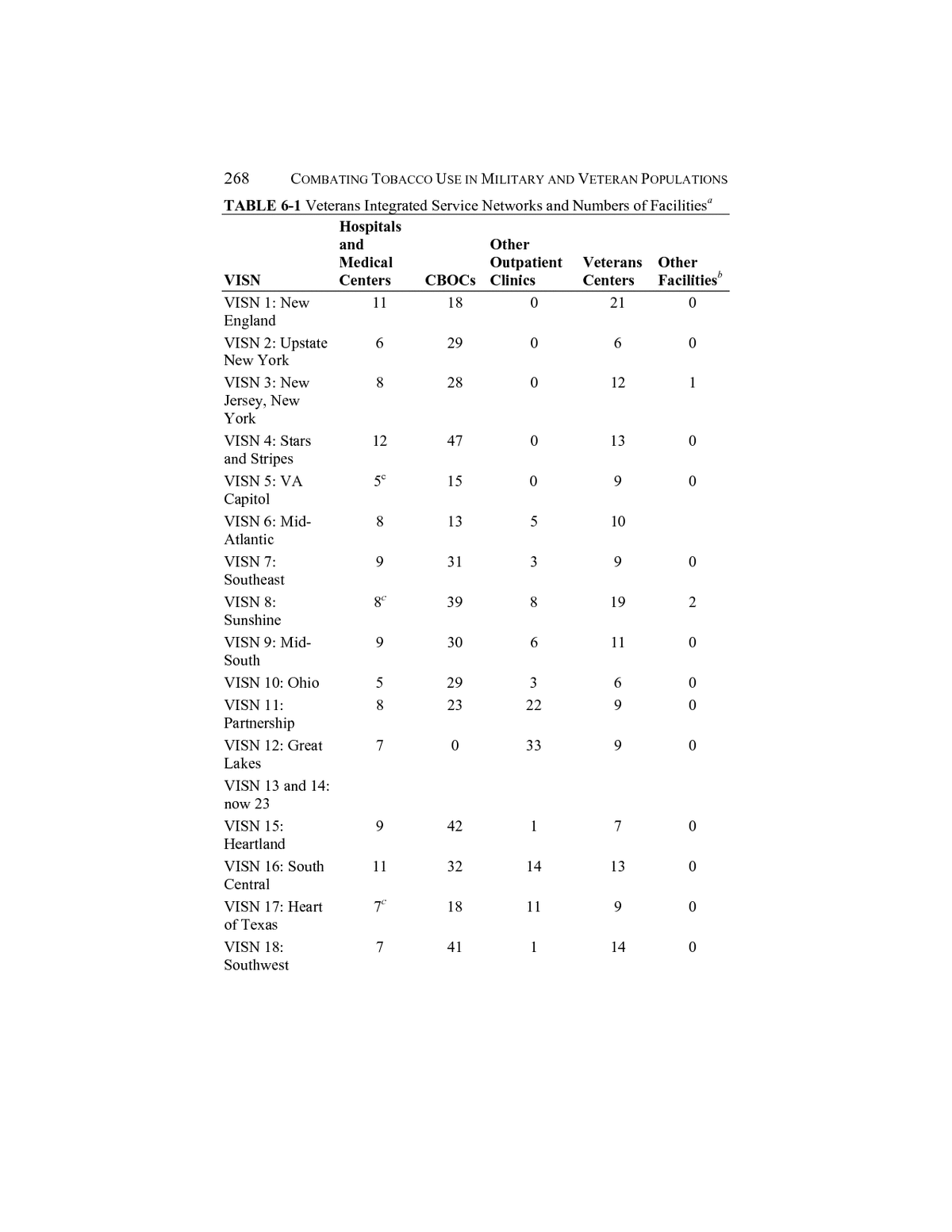
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 267 nonâtobacco-related programs, such as human immunodeficiency virus prevention. The director of the National Prevention Program is assisted by a technical advisory group (TAG) of VA health-care practitioners from the VISNs that provides consultation and expert advice on best practices in tobacco-use cessation for veteran populations, on the health effects of tobacco use and related illness, and on new treatment services. Those practitioners represent pulmonary and critical care, primary care, preventive medicine, mental health, and substance-use treatment and are administrators, researchers, and educators, including a representative of the Pharmacy Benefits Management Strategic Health Care Group. The TAG has monthly conference calls to discuss tobacco-related issues and meets twice a year; it also can arrange emergency calls to deal with special issues, such as VA use of varenicline for patients who have mental-health disorders (Kim Hamlett-Berry, VA, personal communication, December 3, 2008). The committee notes that the TAG does not include representatives of all 21 VISNs or every VAMC, nor are there formal mechanisms for disseminating information from the TAG to the lead clinicians in VAMCs or for the lead clinicians and other health providers to request advice from the TAG. The PHSHCG also participates in the Interagency Committee on Smoking and Health (ICSH), sponsored by the Department of Health and Human Services (HHS) and convened by the US Surgeon General. The ICSH coordinates research, educational programs, and other smoking and health efforts for HHS, in addition to similar activities of other federal, state, local, and private agencies. Other federal agencies engaged in health careâsuch as the several institutes of the National Institutes of Health, the Department of Education, and the Centers for Disease Control and Prevention (CDC)âare also members of the ICSH. Veterans Integrated Service Networks In addition to VHA headquarters staff, 21 VISNs provide health care to veterans (see Table 6-1). The VISNs include hospitals and medical centers, residential rehabilitation centers, outpatient clinics (including CBOCs), and Veterans Centers for treating posttraumatic stress disorder (PTSD) and other mental-health disorders. The VISN directors report to the deputy under secretary for health for operations and management. All outpatient clinics and CBOCs are affiliated with a VAMC.
268 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS TABLE 6-1 Veterans Integrated Service Networks and Numbers of Facilitiesa Hospitals and Other Medical Outpatient Veterans Other VISN Centers CBOCs Clinics Centers Facilitiesb VISN 1: New 11 18 0 21 0 England VISN 2: Upstate 6 29 0 6 0 New York VISN 3: New 8 28 0 12 1 Jersey, New York VISN 4: Stars 12 47 0 13 0 and Stripes VISN 5: VA 5c 15 0 9 0 Capitol VISN 6: Mid- 8 13 5 10 Atlantic VISN 7: 9 31 3 9 0 Southeast VISN 8: 8c 39 8 19 2 Sunshine VISN 9: Mid- 9 30 6 11 0 South VISN 10: Ohio 5 29 3 6 0 VISN 11: 8 23 22 9 0 Partnership VISN 12: Great 7 0 33 9 0 Lakes VISN 13 and 14: now 23 VISN 15: 9 42 1 7 0 Heartland VISN 16: South 11 32 14 13 0 Central VISN 17: Heart 7c 18 11 9 0 of Texas VISN 18: 7 41 1 14 0 Southwest
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 269 Hospitals and Other Medical Outpatient Veterans Other VISN Centers CBOCs Clinics Centers Facilitiesb VISN 19: Rocky 6c 37 2 14 0 Mountain VISN 20: 9c 26 1 15 2 Northwest VISN 21: Sierra 8 9 26 20 0 Pacific VISN 22: Desert 5 29 5 11 1 Pacific VISN 23: 12 40 3 14 0 Midwest Total 170 576 144 251 6 a As of April 10, 2009. b Includes domiciliaries, federal hospitals, rehabilitation facilities, PTSD clinics, and care facilities. c Includes at least one VA health-care system in addition to the medical centers. SOURCE: Adapted from VA (2009b). The VISN administrators are responsible for implementing the many policies and programs for health-care services in the hospitals and clinics in each VISN, including tobacco-use cessation. Although the VISN administrators report to the deputy under secretary for health for operations and management, they have substantial autonomy and authority for the medical services offered within their own VISNs, including tobacco control. They can be instrumental in emphasizing tobacco-cessation activities at all of their medical facilities. Virtually all of the VAMCs have some form of tobacco-control program although the programs are not standardized or uniform (VA, 2006b). The agencyâs 2005 report Smoking and Tobacco Use Cessation indicated that although 99% of the facilities included in a survey had tobacco-control programs, they varied in who managed the programs, who was responsible for documenting patientsâ smoking status in the electronic medical records, who could prescribe medications, and whether they accommodated special populations, such as women, inpatient psychiatric patients, and hospitalized patients (VA, 2006b). There is even greater variation among the CBOCsâ tobacco- control services, although each one is affiliated with a specific VAMC. CBOCs were established in the 1990s to provide access to, and continuity of care for, underserved veteran populations, many of them in
270 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS rural areas. They provide primary health care, and a growing number also provide primary mental-health services. CBOCs are staffed by VA employees or independent contractors engaged through an outside care provider. The quality of care provided by CBOCs, whether through VA or contract staff, has been studied extensively since their growth in the early 1990s (Borowsky et al., 2002a, 2002b; Chapko et al., 2002; Fortney et al., 2002; Kirchner et al., 2008; Liu et al., 2008; Maciejewski et al., 2007). Most of the studies have either compared the level of care provided by CBOCs with that provided by medical-center clinics or determined the types of care that CBOCs provide and the veteran populations served by them. Kirchner et al. (2008) looked at mental- health services offered at 13 VAMCs and 12 CBOCs that integrated mental-health care with primary care at a VISN in the south central United States. Tobacco-cessation services were offered in the integrated clinics at 17% of the VAMCs and 67% of the CBOCs (Kirchner et al., 2008). TOBACCO-CONTROL PROGRAMS IN THE DEPARTMENT OF VETERANS AFFAIRS VA has been a leader in addressing tobacco use as a health priority for veterans. For example, in 2004, it held the national conference âVA in the Vanguard: Building on Success in Smoking Cessation,â which brought together about 80 tobacco experts to identify successful approaches to smoking-cessation treatment and possible obstacles to their implementation. This conference helped provide a roadmap for VA policies and best practices on tobacco use with an emphasis on special veteran populations such as those with psychiatric disorders. (VA, 2004). VHA has translated a number of evidence-based initiatives into its health-care system, including policy revisions to expand access to tobacco-cessation medications, particularly nicotine- replacement therapy (NRT); elimination of copayments for smoking- cessation counseling; and integration of smoking cessation into care for the growing veteran mental-health population. The VA has developed training programs to educate mental-health providers on integrating tobacco cessation in the treatment of mental-health disorders (Hamlett- Berry et al., 2009; VA, 2006c), has identified clinicians at each VAMC as a resource for tobacco-cessation information, and discontinued the sale of tobacco products at its facilities. The VA has in place many elements that would enable it to implement a comprehensive tobacco- control program, including communication networks, restrictions on tobacco use, and effective tobacco-cessation interventions. In Chapter 4, the committee identified the key elements that are required of any organization that wants to establish a comprehensive
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 271 tobacco-control program: a strategic plan, dynamic leadership, essential intervention components (enforceable and enforced policies, communication interventions, and evidence-based treatments), adequate resources, surveillance and evaluation of the programâs effectiveness, and management capability to adjust the program in response to that evaluation. In this section, the committee describes VAâs tobacco-control efforts and highlights the policies and programs that are in place and working well. This section also provides guidance on where important activities are lacking or where existing ones could be enhanced to improve tobacco cessation in the VA patient population and in VA employees. The key components already in placeâincluding many effective and enforceable policies, communication mechanisms, surveillance activities in the form of performance measures, and periodic evaluation of tobacco-control practices throughout the VISNsâcan be leveraged to expand and coordinate tobacco-control activities throughout VA. The agency lacks a strategic plan, senior leadership that believes that tobacco cessation should have high public-health priority for VA, a dedicated funding source for tobacco-control activities, and innovative approaches for raising veteransâ awareness of available tobacco-cessation services. VA is ideally structured to ensure adequate capacity and collaboration at all program levels while each VISN tailors tobacco- cessation activities to local circumstances and the needs of veterans and health-care providers. VA has an advantage over private-sector health- care systems in that it is able to make institutional changes at the highest administrative levels without worrying about profits or stockholders. This does not mean that the secretary of veterans affairs or the under secretary for health can make changes without consulting their staff, the NLB, or the veterans; but they do have the ability to change policy, procedures, and the institutional culture in VA quickly and uniformly. If tobacco cessation has high priority for the secretary and the under secretary, it will have high priority for the VISNs and all of the VA heath-care providers. As noted earlier, the responsibility for developing VA tobacco- control programs resides in the PHSHCG at VA headquarters, and the programs are implemented as part of the National Prevention Program. VHA Directive 2008-081,1 dated November 26, 2008, outlines VAâs National Smoking and Tobacco Use Cessation Program and lists all of the necessary resources for program implementation. The directive requires that VA continue its commitment to prevention with a âstrong 1 VHA Directive 2008-081, issued November 26, 2008, rescinded VHA Directive 2003-042.
272 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS public health educational effort on the health benefits of quitting tobacco use . . . with a strong emphasis on outreach and an increasing awareness of the availability of the full range of evidence-based smoking and tobacco-use cessation treatment options in VA.â The specific components of the public-health education effort are not listed, but the directive identifies the VA/DoD Clinical Practice Guideline for the Management of Tobacco Use as a key resource. The directive advocates the tobacco-use screening and cessation counseling program given in the guideline. In accordance with the guideline, the directive requires that smoking-cessation medication be made available to all smokers interested in quitting regardless of whether they attend a smoking- cessation program. The directive does not elaborate on how the guidelines are to be implemented, by whom, or how outcomes are to be evaluated. Nor does it encompass policy aspects of tobacco-use control, such as smoke-free policies at VA facilities, funding for the programs, or reporting requirements (VHA, Directive 2008-081, 2008). Leadership is necessary for the medical facilities in a VISN to develop and maintain comprehensive tobacco-use cessation programs (VA, 2007a). Lead staff members necessary to support tobacco-cessation programs reside in both Headquarters and VAMCs as evidenced by the National Prevention Program; at least one part-time employee assigned to the smoking-cessation program at each VISN is also necessary (VA, 2007a). VHA Directive 2008-081 mandates that the director of each VAMC designate a smoking and tobacco-use cessation lead clinician to be the point of contact for all clinical and other communication on tobacco cessation. According to the 2005 Smoking and Tobacco Use Cessation Report, some type of smoking-cessation program was offered at 96% of the 158 VAMCs surveyed. Although virtually all VAMCs have a lead clinician of the smoking cessation program, this position is not full-time. A 2005 survey of lead clinicians at each of 151 VAMCs that had tobacco-cessation programs found that the equivalent of only 61 full- time employees were allocated to the programs (VA, 2006b). About one- third of the 423 full- and part-time employees of the programs had tobacco-cessation care as part of their job description; in most of the facilities, 2 or more part-time staff provided tobacco-cessation services. Most of the services were provided by psychologists (22%) or registered nurses (12%), but other health-care professionals also provided tobacco- cessation services, including social workers, physicians, nurse practitioners, and pharmacists. The number of staff at medical-center outpatient clinics or CBOCs who provided tobacco-use cessation services was not determined. The availability of staff at CBOCs for tobacco-useâcessation services, other than prescribing medications and
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 273 brief counseling, was highly variable; some CBOCs had trained staff who offered group or individual counseling on site, and others only referred patients to outside tobacco-counseling services (Timothy Carmody, VA, personal communication, July 15, 2008; Clint McSherry, VA, personal communication, July 29, 2008). VA funds tobacco-control programs from its general public- health budget rather than as a separate budget item. Funding for tobacco control varies by VAMC, personnel available, and interest on the part of staff and patients. It is difficult for VAMC directors to justify having a staff member dedicated to tobacco-control services without a dedicated funding mechanism for a smoking-cessation lead clinician. VA health- care providers who conduct tobacco-cessation programs indicated that lack of dedicated staff and resources makes it difficult to provide services and to obtain educational materials (VA, 2007a). The National Prevention Program does have a budget for tobacco-control activities and can leverage funding from other sources, including the Employee Education System, for training (Kim Hamlett-Berry, VA, personal communication, December 3, 2008). VISNs and their medical facilities are required to provide many health services, such as suicide prevention and treatment for PTSD, and tobacco use is only one high-priority concern among many. Although the PHSHCG is the VA organizational lead for tobacco-use cessation programs, unless the secretary of veterans affairs and the Executive Office of the administration are actively concerned with the issue, individual VISNs are unlikely to be completely engaged in tobacco- control programs. Finding: VA has adopted several tobacco-control policies and programs, including its National Smoking and Tobacco Use Cessation Program, but they are not comprehensive, and implementation varies among VISNs, VAMCs, and CBOCs as a result of organizational discrepancies, lack of accountability, and inadequate funding. Finding: The infrastructure to support VA tobacco-control programs varies among VISNs and VAMCs, especially with respect to staffing and funding, and is inadequate in some geographic areas. Recommendation: VA can develop a comprehensive tobacco-control program by expanding and coordinating its
274 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS current programs under engaged leadership and clear direction. COMMUNICATION INTERVENTIONS VA can play a valuable role in motivating veterans to quit tobacco use by offering relevant information and treatment options. Increasing veteransâ interest in and willingness to quit tobacco use requires that veterans and their families be educated about the harmful effects of tobacco and about the treatment options available to them. It also requires that health-care providers be available to provide services when veterans seek assistance. This section summarizes methods of communicating that information. Tobacco advertising and promotions are not allowed at any VA facility or in any VA newsletter or Web site, but veterans live in the civilian population and as part of the general public are exposed to tobacco advertising. VA can counter such advertising by providing educational materials to veterans enrolled in VA health services. The committee was unable to identify any antitobacco mass-media campaigns in the VHA health-care system. It has, however, occasionally run articles about veterans who have stopped smoking or about VA tobacco- cessation programs in its online and print versions of veterans-health newsletters. For example, the summer 2008 edition of Veteransâ Health: The Wellness Magazine for Ohio Veterans, from the VA Healthcare System of Ohio, featured a 71-year-old veteran who had graduated from the Ohio VAâs tobacco-cessation program. The article profiled his tobacco-cessation attempts and success. It emphasized that although quitting tobacco is not easy, it is beneficial to oneâs health at any age, and professional help is available for all veterans who want to quit. Many VISNs have online newsletters that contain information and stories that promote VA tobacco-cessation programs. VA has several Web sites that assist veterans in obtaining health information, such as My HealtheVet (www.myhealth.va.gov), which includes smoking and tobacco cessation as one of the featured programs under the healthy living centers section; however, it does not include tobacco use as a vital sign. Highlighting tobacco cessation on VA Web sites could motivate veterans to consider quitting and to help those who are already interested in quitting get information more easily. There are also Web sites for specific VA health-care facilities with information on tobacco cessation, but the pages are not easily accessed through the VA home page and require the user to search for individual medical facilities. For example, the Web site for the Overton Brooks VA Medical Center in Shreveport, Louisiana, outlines how its smoking-cessation program
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 275 2 works. It might be helpful to include links to such programs on the VA My HealtheVet Web site. No formally organized group in or outside VA is actively promoting tobacco-use cessation programs on behalf of veterans. At the VA Provider Feedback Forum on Smoking and Tobacco Use Cessation (VA, 2007a), participants thought that VA should explore ways to promote tobacco cessation for veterans at VA medical facilities, including use of the My HealtheVet Web site. Suggestions for increasing participation in the programs included motivational videos in waiting rooms, audio messages for people holding on the telephone, and informational kiosks with computers that could show patients how the cessation programs work. Participants at the forum also noted that many cessation resources, including online resources, are available at little or no cost from the CDC Office on Smoking and Health. Participants agreed that state and local health departments were important partners for referrals for quitlines and other support. In states with active tobacco- control programs for the general population, VA may be able to leverage its resources by connecting veterans with free cessation services in their communities. VA engages veteran service organizations (VSOs) at many levels, but it is not apparent whether VSOs have been included in discussion about tobacco use by their members. The PHSHCG and individual VAMCs may want to assess whether VSO members are interested in receiving tobacco-cessation services at their local VA health-care facilities and to broadcast information about the availability of such services to the VSO members. Finding: VHA has many options for increasing the effective use of tobacco-cessation programs among its patients, but it has not been aggressive or uniform in developing and delivering antitobacco messages to its patients via newsletters, mailings, Web sites, or other media outlets, or providing information on how to access tobacco-cessation treatments. 2 Accessible at http://www.shreveport.va.gov/PatientEducation/ QuitSmart_Main.asp. Accessed on April 9, 2009.
276 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS TOBACCO-USE RESTRICTIONS Department of Veterans Affairs Tobacco-Free Policies VA has worked toward a tobacco-free policy that is applicable to all its health-care facilities since 1991. However, the Veterans Health Care Act of 1992 (Public Law 102-585, Section 526) required VA to establish and maintain either indoor smoking areas in VAMCs, nursing homes, and domiciliary-care facilities for veterans or detached smoking areas that are accessible to patients and have heating and air- conditioning. Several VA circulars and directives specify who may use the smoking areas, but they vary to some degree by facility. VHA Directive 2008-052, Smoke-Free Policy for VA Health Care Facilities, issued in August 2008, states that all VA health-care facilities are to be smoke-free and restricts required smoking areas to detached buildings that must be accessible, heated, and air-conditioned and meet the Joint Commission (formerly the Joint Commission on the Accreditation of Healthcare Organizations) requirements for ventilation. All acute-care patients, ambulatory-care patients, outpatients, and domiciliary patients must use the detached smoking areas. Smoking may be allowed on the grounds of a facility, but smoking areas may not be situated within 35 feet of any facility entrance that is routinely used by staff or patients. Smoking areas for VA employees should be separate from those for patients. Specifically designated indoor smoking areas are still maintained at some long-term care and mental-health program facilities, and they must have a ventilation system that meets American Society of Heating, Refrigerating and Air-Conditioning Engineers Standard 62- 2001. All remaining indoor smoking areas in long-term-care, spinal-care injury, and inpatient psychiatric facilities were to be phased out by February 2009, provided that appropriate outdoor areas were made available. The directive also prohibits the sale or distribution of tobacco products to long-term-care patients, inpatients, residents, employees, staff, and volunteers on VHA grounds. Finally, the VHA directive states that NRTs should be used by inpatients to prevent nicotine withdrawal unless medically contraindicated (VHA, Directive 2008-052, 2008). According to the 2005 Smoking and Tobacco Use Cessation Report on tobacco-use practices at 158 VA hospital facilities (VA, 2006b), 51 VA facilities provide 134 smoking shelters for patients only, 41 facilities provide 76 shelters for employees only, and 137 facilities provide 573 shelters for use by both patients and employees, with some facilities providing up to 32 shelters for combined use by patients and employees. Almost all (91%) of the VHA facilities indicated that patients and employees smoke in the same designated smoking areas. Of the 158 facilities surveyed, 77% are smoke-free indoors; 23% (36) permit some
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 277 indoor smoking in areas such as long-term-care inpatient, locked psychiatry wards, resident rooms, and nursing-home units; and 94% have separate ventilation systems. Almost half of the facilities allow smoking only in designated areas; the rest allow smoking outside a specified distance from buildings. VHA Circular 10-90-141 (November 23, 1990) prohibits employees from using indoor smoking areas intended for patients, so they must smoke outside. Finding: VA has worked to develop and implement tobacco-free medical facilities; however, it has been hampered in its efforts by congressional mandates that require each VAMC to maintain a smoking area for veterans. The language of the Veterans Health Care Act of 1992 prevents VA from eliminating tobacco use at its medical facilities and thus prevents VA from following the national trend toward tobacco-free facilities, in which it was initially a leader. VA does not sell tobacco products at its medical facilities. Tobacco Use by Department of Veterans Affairs Employees The committee was unable to determine how many VA employees use tobacco. However, more health providers at a primarily psychiatric VA hospital were smokers (30%) (Essenmacher et al., 2009) than at a general VA hospital (11%) (Duffy et al., 2008). This suggests that VA tobacco-cessation programs should include both employees and veterans. In keeping with general VHA policy favoring tobacco abstinence, VHA facilities have taken steps to help their employees who want to quit tobacco use. The majority of VAMCs provide outdoor smoking areas for employees; many of them have 3 to 10 employee shelters. However, at 91% of the VAMCs, patients and staff use the same smoking shelters (VA, 2006b). The 2008 VHA Directive 2008-052 requires that, whenever possible, patients and staff have separate smoking areas and that VAMC directors work toward a goal of having a single smoking area for patients and a single one for staff. Most VAMCs (65%) offer tobacco-cessation services for employees who are not veterans, and 85% of VAMCs refer employees to VA tobacco-cessation programs. Of facilities that offer employee tobacco-cessation programs, 84% allow staff to participate in them during work hours (VA, 2006b). Staff members who are not veterans cannot receive NRTs from the VA pharmacy, but some facilities offer NRTs to employees at reduced cost. It has been suggested that VA
278 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS facilities provide a break room for nonsmoking employees to counteract the perception that smokers are permitted more breaks (VA, 2007a). VA employees and contracted professionals perform ordinary functions that do not require the unique standard of physical fitness needed for military action. Therefore, it would be difficult to justify a policy that requires abstinence from tobacco use for VA personnel beyond the requirement not to smoke on VA premises or in the same areas as patients. Although there are few legal restrictions on adopting such a policy, it has the disadvantage of necessarily applying to many personal traits and behaviors beyond tobacco use, such as weight management. If VA were to require its employees to be nonsmokers, several principles might be available for justifying the use of smoking as a disqualification for employment: anything that adversely affects a personâs health also adversely affects the personâs ability to work, employers have the right to refuse to hire anyone who might increase costs to the employer regardless of the probability or amount of such cost increases, employers have the right to require their employees to behave in their private lives so as to promote the interests of the employer, and employers have the right to refuse to hire anyone for any reason or no reason regardless of ability. If VA adopts any of those principles, it could encourage similar policies by other public agencies and private organizations that are seeking to exclude employees for reasons other than tobacco use. Finding: Many VAMC facilities have multiple smoking areas for both veterans and employees although this may change in response to a new VHA directive. Most VAMCs have taken steps to offer tobacco-useâcessation services to interested employees, but such services are not available in all VA facilities. Recommendation: VA patients and staff should have barrier-free access to tobacco-cessation services if they use tobacco. TOBACCO-CONTROL INTERVENTIONS The VHA is a full-service health-care system that provides treatment for medical and mental-health conditions in inpatient and outpatient facilities. Tobacco-use cessation is one of the services offered to both inpatients and outpatients. After leaving active duty, veterans who participated in tobacco-cessation programs while on active duty in the military and want to continue in such programs must find new ones
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 279 when they enter the VHA health-care system. DoD and VHA health services are distinct, both jurisdictionally and geographically, so there is a lack of continuity between military and VA services that may interrupt or end a new veteranâs efforts to quit tobacco use. Evidence-based treatments can be offered by DoD and VA to help to bridge the gap in health-care service. In this section, the committee discusses the treatments currently offered by VA and identifies treatments that VA could add to develop a more comprehensive program. Evidence-Based Interventions The gold standard in VA for tobacco-cessation treatment is the VA/DoD Clinical Practice Guideline for the Management of Tobacco Use. The guideline, published in 2004, is modeled on the 2000 Treating Tobacco Use and Dependence: Clinical Practice Guideline (Fiore et al. 2000) sponsored by the Public Health Service (PHS); the PHS guideline was updated in 2008 (Fiore et al., 2008). In VAâs 2005 Smoking and Tobacco Use Cessation report, 51% of the 158 VAMCs in the survey used the VA/DoD clinical-practice guideline often (76â99% of the time), 24% used them always, and only 1% never used them; 1% of the VAMCs reported not knowing about them. Most often, a nurse is responsible for assessing a patientâs tobacco use, and a primary-care provider is able to provide smoking-cessation treatment, whether it be brief counseling, telephone counseling, or medications. The VA/DoD guideline presents evidence-based recommendations for assessment and treatment of veterans and prevention of tobacco use, and it includes several appendixes that provide specific information on counseling strategies and techniques, medications, and relapse prevention. Behavioral Interventions VA appears to offer a broad array of tobacco-cessationâ counseling interventions to patients, but there is little information on their effectiveness in veterans as a separate population. In 2006, VA eliminated the copay for smoking-cessation counseling (individual and group sessions) to reduce one barrier to access to care (38 Code of Federal Regulations 17). As with tobacco users in the Military Health System (see Chapter 5), for veterans who are tobacco users the VA/DoD guideline advocates the 5 Aâs and recommends intensive counseling of at least 4 sessions of 10 minutes each (VA/DoD, 2004). A variety of counseling formats are effective, including group and individual counseling in person and individual counseling over the telephone. Self- help materials may also be appropriate for patients who receive brief
280 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS counseling, might be motivated to quit, or as a supplement to other interventions. Participants in the 2007 Provider Feedback Forum on Smoking and Tobacco Cessation report stated that in addition to providing pharmacotherapeutic interventions for veterans who use tobacco, it would be advantageous to provide more behavioral counseling to improve long-term outcomes, particularly therapy that would address stress management and other coping skills to prevent relapse. Motivational interviewing and the use of incentives were also suggested as adjunct interventions. Some participants suggested that behavioral interventions should be incorporated into other behavioral programs, such as those for weight loss, stress management, and substance-abuse treatment (VA, 2007a). Tobacco-Cessation Medications The use of tobacco-cessation medications among VA patients has more than doubled in the last several years (Michael Valentino, VA, presentation to the committee, June 2, 2008). The VA National Formulary provides many of the tobacco-cessation medications approved by the Food and Drug Administration (FDA), including varenicline; however, it does not include nicotine nasal spray or nicotine inhaler, because these are rarely used by the VA population (Michael Valentino, VA, presentation to committee, June 2, 2008). Nevertheless, participants in the 2007 Provider Feedback Forum cited a lack of uniformity among and within VISNs with regard to policies related to access to NRTs. Although NRTs are available as over-the-counter medications in non-VA pharmacies, for a veteran to receive them free of charge from VA, the medications must be prescribed by a VA health-care provider and the prescriptions must be filled at a VA pharmacy. Forum participants noted that it could take considerable effort for health-care providers without prescribing privileges to obtain an NRT prescription for a patient (VA, 2007a). Although the 2003 National Smoking and Tobacco Use Cessation Program stated that tobacco-cessation medications must be available for all patients regardless of whether they attend a tobacco- cessation program, the 2005 Smoking and Tobacco Use Cessation Report suggested that some VAMCs were still restricting patientsâ access to NRTs and bupropion (VA, 2006b). Of the 104 VAMCs responding, 23% indicated that a patient must be in a tobacco-cessation program to receive NRTs or bupropion, in spite of a VA policy that tobacco-cessation medications must be available to all patients regardless of whether they participate in a tobacco-cessation program. Lack of adherence to the VA
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 281 policy is a barrier to ensuring that veterans have easy access to tobacco- cessation medications. Virtually all of the VAMCs have the nicotine patch on their centerâs formulary, and over 73% of them have the nicotine patch, bupropion, and sustained-release bupropion available at their pharmacies; fewer than 10% of the pharmacies had other NRTs available (VA, 2006b). Participants in the Provider Feedback Forum indicated that special drug requests are required for NRTs at some VISNs and obtaining combination therapies, such as multiple NRTs or NRTs with another tobacco-cessation medication, is challenging (VA, 2007a). The use of varenicline is of concern to VA because of recent adverse reactions to it in veterans. The PHSHCG Web site has a posting for the latest FDA public-health advisory on varenicline,3 and VA follows the FDA recommendations on its use. It is not a first-line medication in the VA National Formulary, and its use is restricted until a patient has failed to quit tobacco by using NRTs and bupropion. The Provider Feedback Forum found that most patients were receptive to using varenicline, but a nonformulary request was required to prescribe it, although this practice may have changed. It was also noted that many VA pharmacies were not following National Formulary guidelines for varenicline, and this was preventing patients from receiving it. Another concern was that the VA National Formulary does not include the varenicline starter pack, thus ensuring that the patient is receiving the correct dosage is problematic (VA, 2007a). The committee considers the requirement that veterans have a prescription for over-the-counter NRTs and that these prescriptions be filled at VA pharmacies to be a barrier to access for veterans. Another barrier is that all VA pharmacies do not have all tobacco-cessation medications available that are listed on the VA National Formulary. Combined Behavioral Interventions and Medication The VA/DoD guideline echoes the 2000 PHS guideline by advocating a combination of behavioral interventions with tobacco- cessation medications to achieve long-term abstinence. Combinations of medications, such as NRTs and bupropion, may also be used (VA/DoD, 2004). Most VAMCs that offer tobacco-cessation programs provide both behavioral therapy (group or individual) and medications. Almost every VAMC in the 2005 Smoking and Tobacco Use Cessation Survey 3 Food and Drug Administration. 2008. Public Health Advisory: Important Information on Chantix (Varenicline). http://www.fda.gov/CDER/ Drug/advisory/varenicline.htm. Accessed April 9, 2009.
282 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS indicated that medications are a part of treatment, and 82% of 151 VAMCs indicated that even if a patient chooses not to attend a tobacco- cessation program, he or she can still obtain tobacco-cessation medications. Of the VAMCs in the survey, 39% limit the number of tobacco-cessation treatmentsâbehavioral or medicationâthat a patient may receive each year to 2 (VA, 2006b). Other Individual Interventions The VA/DoD guideline finds that there is insufficient evidence to advocate the use of other tobacco-cessation interventions, such as acupuncture and hypnosis, although VA has conducted studies of hypnosis (Carmody et al., 2008) and the use of financial incentives (Volpp et al., 2006) for tobacco cessation. However, as noted in Chapter 4, the evidence base on the effectiveness of those treatments for long- term tobacco cessation in the general population and in veteran populations is unclear. Finding: VA has a long history of attempting to reduce smoking by veterans and has been responsible for numerous scientific advances regarding the health effects of smoking. Finding: VA offers a wide array of tobacco-cessation treatments, including all medications approved by FDA and behavioral counseling. However, the availability of treatments is not uniform among facilities and lack of availability may discourage or prevent patients from seeking or obtaining treatment and health-care providers from prescribing them or referring patients to a tobacco- cessation program. Recommendation: With the release of the updated 2008 PHS Clinical Practice Guideline for Treating Tobacco Use and Dependence in 2008, VA and DoD should revise their current guideline or adopt the 2008 PHS guideline. DELIVERY OF INTERVENTIONS There is no requirement that all VISNs use a standard tobacco- cessation program, such as that of the American Cancer Society or the American Lung Association or the commercially available QuitSmartâ¢, although many of them do so, in addition to following the VA/DoD guideline. See Box 6-1 for some examples of tobacco-cessation programs
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 283 used by VA. The committee was unable to determine which standardized tobacco-cessation programs are used by VA medical facilities and whether there is any mechanism for determining which are most effective for veteran populations. All VA medical facilities must offer some type of tobacco-cessation program even if it is only a brief counseling session with a clinician during an office visit and a prescription for medications. The VA has made progress in reducing some barrier to access to tobacco-cessation interventions such as eliminating the copay for tobacco-cessation counseling at VA facilties. Many of the smaller outpatient clinics and CBOCs that do not have staff available or trained to run tobacco-cessation programs cannot offer more than brief counseling and prescriptions and refer veterans to local health departments or state quitlines for more intensive counseling (Jean Beckham, VA, personal communication, July 18, 2008; Timothy Carmody, VA, personal communication, July 15, 2008; Clint McSherry, VA, personal communication, July 29, 2008). The disconnect between receiving tobacco-cessation counseling outside VA and for receiving tobacco-cessation medications from VA makes it difficult for clinicians to follow up and assist patients, and it may pose a barrier for veterans seeking treatment for tobacco use. BOX 6-1 Tobacco-Cessation Programs Used by VA ⢠Forever Free⢠was designed to help prevent relapse so that former smokers remain smoke-free for life. Booklets are written at an easy-to-read level (5thâ6th grade). The new Forever Free for Baby and Me⢠program was written for pregnant women and new mothers. (From the Tobacco Research and Intervention Program at the H. Lee Moffitt Cancer Center and Research Institute at the University of South Florida; accessed at http://www.smokefree.gov/pdf.html.) ⢠QuitSmart⢠Quit Smoking Program is a commercial four- session program that complements behavior-modification techniques with the latest nicotine-replacement strategies. Counselors can be certified to teach the program. (Accessed at http://www.quitsmart.com/.) ⢠American Cancer Societyâs FreshStart Program: see Chapter 4 for brief program description. ⢠American Lung Associationâs Freedom from Smoking Program: see Chapter 4 for a brief program description.
284 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS Clinical Settings Of the VAMC tobacco-cessation programs, 53% are in the mental-health divisions, 22% in primary care, 9% in psychology, and 16% in other medical services (VA, 2006b). The 2006 VA survey found that over half the programs offered individual counseling, with 60% of the patients receiving three or more sessions. Only about 20% of the programs offered more than three individual sessions. Most sessions were 10â30 minutes long. The overwhelming majority (93%) of the programs offered group counseling, most being four or more sessions of 30â60 minutes, although many of the programs (46%) had sessions longer than an hour (VA, 2006b). Although the committee has no information on how often such counseling programs are offered, it notes that should veterans not be able to attend a program once they have decided to quit, the lack of access to a program may prove to be a barrier to their quit attempts. The Guideline Implementation for Tobacco (GIFT) study (Joseph et al., 2004) and the Quality Improvement Trial for Smoking Cessation (QUITS) study (Sherman et al., 2006a) reported that for many veterans referred to a specialty smoking-cessation clinic, the wait for an appointment is a month or longer at most of the facilities. In their chapter in VA in the Vanguard: Building on Success in Smoking Cessation, Sherman and Farmer (2004) note that many patients may forgo using tobacco-cessation medications because of long waits to have the VA pharmacy fill their prescriptions. Again, the committee notes that a lengthy wait for a counseling session may pose a barrier to veteransâ accessing a tobacco-cessation program. Not all cessation programs require that the veteran be referred to it by a health-care provider; veterans may self-refer (VA, 2006b). The 2005 Smoking and Tobacco Use Cessation Survey found that 13% of the VAMCs in the survey use telemedicine to deliver tobacco-cessation services to their patients (VA, 2006b). VA is working to expand its use of telemedicine for this and other health programs, but most clinics are not yet able to provide such services (Timothy Carmody, VA, personal communication, July 15, 2008); and the effectiveness of this approach is unknown. Primary-Care Providers In most VAMC primary-care clinics, nurses or physicians are responsible for assessing a patientâs tobacco-use status (Sherman et al., 2006b; VA, 2006b). According to the 2005 Smoking and Tobacco Use
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 285 Cessation Report, 96% of primary-care providers are able to provide tobacco-cessation counseling to patients, and 89% are authorized to prescribe tobacco-cessation medications. Similar results were seen in 2 studies of 40 VHA medical facilitiesâincluding VAMCs, ambulatory- care clinics, and CBOCsâaround the country: the GIFT study (Joseph et al., 2004), and the QUITS study (Sherman et al., 2006a). Both GIFT and QUITS found that most facilities referred tobacco-using patients to specialty tobacco-cessation clinics; only 9 of the 151 facilities allowed primary-care providers to prescribe tobacco-cessation medications without restrictions, and 6 required clinicians to have specific training before they could prescribe the medications. The inability of all VA primary-care providers to provide tobacco-cessation medications may dissuade veterans from obtaining such medications, possibly reducing their incentive to quit tobacco and forming a barrier to their receiving treatment. Many VAMCs have policies on who may prescribe tobacco- cessation medications. A few require a physicianâs prescription, but most permit physician assistants and nurse practitioners to prescribe the medications (VA, 2006b). Participants in the Provider Feedback Forum suggested that a variety of health-care providers, not only primary-care providers, should be able to write prescriptions for tobacco-cessation medications, particularly NRTs, which are available over the counter outside VA. Removing this barrier to treatment could increase patient use of the medications (VA, 2007a). Primary-care providersâ attitudes about tobacco cessation are strongly associated with the likelihood that they will counsel patients to quit tobacco use or refer them to a tobacco-cessation program; VA providers who perceived barriers to such counseling and referrals were less likely to use them (Meredith et al., 2005). The availability of an on- call tobacco-cessation counselor who can provide immediate counseling, referral to a smoking-cessation clinic, medication management, and telephone follow-up for 2 months was effective in increasing the number of patients who were referred to and attended the clinics and who received tobacco-cessation medications (Sherman et al., 2007). Nurses Nurses play a key role in managing and encouraging tobacco cessation in VA patients. In VA primary-care clinics, nurses are responsible for assessing patientsâ tobacco-use status 91% of the time. Duffy et al. (2008) assessed the attitudes and effectiveness of hospital nurses in delivering tobacco-cessation interventions to inpatients at a VAMC. Although most of the patients indicated that they were interested
286 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS in quitting and were already limited in their access to tobaccoâand in many cases had already quit temporarily and thus may have already experienced the worst of their withdrawal symptomsâonly about 17% of them received tobacco-cessation interventions during their hospital stays. Fewer than half the nurses surveyed said that they provided such services, primarily because of a lack of confidence, a lack of training in tobacco-cessation counseling, and a perception that such advice might upset the patient (Duffy et al., 2008). Essenmacher et al. (2009) found similar results in 150 clinical and nonclinical staff surveyed at a primarily psychiatric VA hospital. Lack of time to provide such services was also an important disincentive. Nurses were less likely than other health providers to feel that it was important to provide smoking- cessation services regardless of their own tobacco-use status. More of the health providers smoked at this psychiatric hospital (30%) than at a general VA hospital surveyed by Duffy et al. (11%). Over half the nurses at the psychiatric hospital felt comfortable in providing smoking- cessation services regardless of their smoking status (Essenmacher et al., 2009). Other Health-Care Providers VA has assessed the effectiveness of a pharmacist-managed tobacco-cessation program known as âVets Without Cigarettes,â at a VA CBOC in Montana. Patients are referred to the program by their health- care providers, at which point they are added to the program roster. When the next class is offered, pharmacists invite up to 15 veterans to attend 3 sessions, 1 every 2 weeks. Participants receive medications from the pharmacy through the mail. Quit dates are typically set for shortly after the second session. The counseling sessions include behavioral strategies, cognitive techniques, stress management, and relapse prevention. In a follow-up survey of 87.8% of the program participants 6 months to 4 years after they attended the program, 41.5% of participants self-reported that they were abstinent; abstinence rates decreased with longer follow-up (Dent et al., 2004). Finding: Many VA health-care providers are in a position to counsel patients about tobacco cessation, but many of them do not take the opportunity to do so because of lack of time and training. Restrictions on who is able to prescribe tobacco-cessation medications in a primary-care clinic may also limit patientsâ access to the medications. Several VA studies suggest that health-care providers, such as hospital nurses and pharmacists, might be good resources for
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 287 tobacco-cessation counseling in the context of a well- managed program. Finding: Services available to veterans appear to be limited by VA resources rather than by veteransâ needs or wishes. Recommendation: All VA primary-care health providers should be able to provide brief counseling and prescribe tobacco-cessation medications. NRTs should be available without a prescription. Quitlines Telephone quitlines are widely used by VA because they are cost-effective and convenient mechanisms for engaging veterans in tobacco-use cessation programs (Joseph and An, 2004). Although some VA facilities have their own quitlines, most refer veterans interested in quitting tobacco either to the federal service offered by the National Cancer Institute (NCI, 1-800-QUIT-NOW) that serves as a portal to state quitlines or directly to their statesâ quitlines. Veterans can also be referred to the NCI toll-free quitline (1-877-44U-QUIT) to speak with a smoking-cessation counselor. VA does not have a national tobacco quitline dedicated to assisting veterans. In 2005, over half of the 158 VAMCs offered smoking-cessation treatment by telephone (VA, 2006b). Of those that did, 50% provided telephone care as part of their tobacco-cessation programs, 75% provided it for those unable to attend the regular programs, 13% had their own formal telephone-counseling programs, and 49% used telephone counseling for follow-up calls. Referral to an external telephone- counseling program was used by 29% of the VAMCs that had telephone care. For veterans that received only telephone counseling, 66% of the VAMCs provided smoking-cessation medications. VA has conducted several demonstration programs for telephone counseling for tobacco-use and smoking cessation for veterans with trained VA counselors or external quitlines. The first program was TELESTOP, conducted at five VAMCs in the upper Midwest, which compared telephone care with usual care (mailed self-help materials and access to referral-based tobacco-cessation programs and medications). Telephone care consisted of 7 calls by trained VA counselors over 2 months for up to 3 quit attempts in a year; counselors encouraged the use of tobacco-cessation medications, initially the nicotine patch. Telephone care resulted in higher participation in the counseling program, greater
288 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS use of smoking-cessation medications, and higher 12-month abstinence rates than usual care (13% vs. 4%) (An et al., 2006). In the later TeleQuit study, two California VISNs participated in a randomized trial to determine the efficacy of proactive quitlines and computerized referrals (Sherman et al., 2008). Intervention sites had a two-click computerized referral, care coordination, medications, and five follow-up telephone calls. Control sites provided standard care. Health- care providers (physicians, physicianâs assistants, or nurse practitioners) at the intervention sites had only to click on two boxes in a patientâs electronic medical record to refer him or her to the program. Of the 2,965 referred, 1,345 were connected to the proactive California Smokersâ Helpline. At the 6-month follow-up, 11% of all the referred and 25% of the helpline veterans were abstinent. Providers at the sites with computerized referral were more likely to refer patients to telephone counseling than those at the control sites (15.6 vs. 0.7 referrals in the prior month). Further assessment of the program at 35 VA facilities compared proactive and reactive quitlines. All veteran smokers received brief counseling and referral to a tobacco-cessation program; medications and self-help materials were also available (Sherman et al., 2008). Patients also received multisession counseling from the California Smokersâ Helpline or self-help materials (Joseph and An, 2004). Patients contacted proactively and those receiving only self-help materials were more likely to enroll in the proactive program than those who were referred to the reactive quitline or who were Helpline patients. At the 6-month follow-up, abstinence rates did not vary substantially among the 4 groups: reactive self-help, 15%; proactive quitline, 20%; reactive quitline, 22%; and proactive quitline, 25%. However, because of the greater reach of proactive quitlines and self-help materials, their potential impact is larger. It was estimated that the veterans using the California Smokersâ Helpline as part of TeleQuit made up 8% of the total quitline volume (Joseph and An, 2004). Quitlines are effective in increasing tobacco cessation in veterans. When VA refers veterans to state quitlines, it avoids the costs of providing such a service itself. However, the state quitlines are not tailored specifically to veterans, particularly those who may be suffering from comorbid mental-health disorders, such as PTSD. Furthermore, veterans must be registered with and attend a VA medical facility to receive a prescription for tobacco-cessation medication. Most state quitlines do not provide tobacco-cessation medications, thus requiring veterans to seek assistance from the VA for medications. Whether the quitlines would be more effective if staffed by counselors specifically trained to deal with veterans and offering tobacco-cessation medication is unknown (Joseph and An, 2004), but the committee considers that
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 289 such a quitline could be tested in a pilot program to determine if veterans found it helpful and if it increased tobacco abstinence. The committee is concerned that veterans receiving health care through VA may prefer to receive tobacco-cessation services from VA rather than from a state quitline or a counseling service that puts them outside the VA health-care system. Moreover, if state quitlines determine eligibility for their services on the basis of income (such as a means test), veterans may not be able to obtain state services. VA is beginning a study to look at the effectiveness of a quitline designed specifically for veterans with mental- health disorders (Scott Sherman, VA, personal communication, January 7, 2009). In an example of leveraging resources to address tobacco use in veterans, the Massachusetts Department of Public Health and the Massachusetts Department of Veteransâ Services jointly launched a free 8-month program in November 2008 to encourage veterans to quit smoking. Veterans and their families are asked to call the state 1-800- TRY-TO-QUIT line. After a simple medical screening over the telephone, eligible veterans receive tailored counseling over the telephone, a free 4-week supply of nicotine patches, and a Quit Kit with tips on quitting and informational resources. The goal is to combine nicotine-patch therapy with counseling and support from trained specialists in order to maximize the chances of quitting for this high-risk population. Because the program is new, outcomes are not yet available (Massachussetts Department of Veteransâ Services, 2008). Finding: VA has conducted several short-term quitline demonstration projects that have shown that referring veterans to quitlines, particularly proactive ones with multiple counseling sessions, is more effective than usual care in promoting tobacco cessation. Some VA facilities rely on external quitlines that disconnect veterans from the VHA for tobacco-cessation treatment and may not be available to all veterans who seek treatment. VA has not established a national quitline that is dedicated to veterans, nor has it worked with state quitlines to train counselors to meet the specific needs of veterans. Recommendation: The VA should develop and test a national quitline for veterans and their dependents. Quitline counselors should be able to provide free tobacco- cessation medications, at the very least NRTs, to callers.
290 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS Computer-Based Interventions VA has experimented with the use of computer-based tobacco- cessation programs. Lenert et al. (2003) conducted a pilot study of an 8- week online course for tobacco cessation that combined tools for self- monitoring behaviors with computer-tailored e-mails timed for each veteranâs quit stage. Results showed that most participants completed only two of the eight education modules, but there appeared to be some success in reducing tobacco use. VA has established a computer-based program for weight management, Managing Obesity/Overweight for Veterans Everywhere (MOVE!), that might be used as a prototype for a tobacco-cessation program. MOVE! is part of the HealthierUS Veterans program sponsored by VA and HHS to reduce obesity and diabetes by helping veterans to lose weight and keep it off. Those goals are similar to the goals of a tobacco-cessation program. The VA secretary and under secretary for health have promoted the weight-management program. The MOVE! Web site is easily accessed from the VA home page4 and contains information for veterans and health professionals. The program can be individualized to each veteran: on the basis of their responses to a questionnaire, the program produces a report with a list of downloadable MOVE! handouts (containing information on nutrition, physical activity, and healthy behavior); health professionals can also access the veteransâ questionnaires to discuss weight loss with them during a clinic visit. A short video, viewable on the site, explains and motivates veterans to join the free program. The My HealtheVet Web site is also a resource for information on smoking and tobacco-use cessation (accessible at www.myhealth.va. gov). The site provides information on self-management for tobacco cessation, but VA does not include tobacco use as one of its vital signs for veterans who may use the site to track their health. Finding: VA runs a computer-based intervention for weight management that could be used as a model for developing an online tobacco-cessation program for veterans who cannot attend programs at VA clinics, who prefer to work at their own pace, or who may need long- term support with quitting. The effectiveness of the MOVE! program, however, has not been evaluated. 4 Accessible at: http://www.move.va.gov/Default.asp.
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 291 Recommendation: VA should explore developing its own computer-based program, similar to the MOVE! program if that program is found to be effective, that is tailored to veteransâ particular concerns. Alternatively, the VA could contract with a commercial vendor to develop and implement such a program. Provider Education and Awareness Many veterans who are interested in quitting tobacco may not do so without motivation and help from a health-care provider. To provide such motivation and assistance, a veteranâs health-care provider must be both knowledgeable about how to help patients quit tobacco and be consistent and comfortable in providing advice and referrals. Each VAMC has a smoking-cessation lead clinician trained in tobacco- cessation services, but, as was shown in the 2005 Smoking and Tobacco Use Cessation Survey, no VAMC has a full-time staff member dedicated solely to tobacco cessation (VA, 2006b). The VA conducts provider training on an ongoing basis, including holding national training sessions in 2009 to provide health-care professionals with a clinical update on tobacco cessation based on the 2008 PHS guideline. Some VAMCs have modified their electronic-medical-record system to include reminders to assist clinicians in approaching patients and identifying available treatment options. The computer screens include premade order sets that a clinician can use to generate a prescription for nicotine patches, nicotine gum, or bupropion; they also have reminders that automatically schedule telephone follow-up at 2 weeks and 3 months and that print out patient-education materials. The reminders include a hyperlink to the VA/DoD clinical-practice guideline for additional information (Scott Sherman, VA, personal communication, September 25, 2008). Responses to the electronic prompts can provide a useful metric to determine compliance with performance measures. However, although the VA/DoD clinical-practice guideline describes evidence-based treatments and the electronic medical record prompts health-care providers to ask patients about their tobacco-use status, providers will not necessarily follow the guideline or respond to the prompts. As in any health-care organization, there are many reasons for that; the most important is lack of time to provide patients with advice. As a result of the broad array of training materials that can be used by VA for tobacco cessation, it was suggested by participants in the Provider Feedback Forum that the PHSHCG review the materials for quality and inform VISN staff about the best resources. Participants also suggested that tobacco-cessation providers be certified and that the
292 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS PHSHCG take the lead in identifying a certification program, such as that offered by the Mayo Clinic or the University of Pittsburgh School of Pharmacy, or designing one of its own (VA, 2007a). The QuitSmart program used by some VAMCs requires certification of its program counselors. Interventions that include VA provider education have mixed results. A 90-minute education session for primary-care providers resulted in increases in advising smokers to quit, in assisting them in quitting (with treatment or referral), and in arranging follow-up (Andrews et al., 2001). Having an on-call counselor perform monthly educational visits to VA primary-care providers and adding small financial incentives for the providers increased patient referrals for brief counseling, medications, and referral to a smoking-cessation program, but the rate of referrals was not sustained at 6 months (Sherman et al., 2007). Yano et al. (2008) found that quality-improvement plans for primary-care providers resulted in improved patient attendance at cessation clinics but no increase in cessation rates (Yano et al., 2008). The GIFT study of a multicomponent intervention (Joseph et al., 2004) showed that train-the-trainer education for two staff members at each VAMC and removal of restrictions on prescribing of tobacco- cessation medications resulted in a slight increase in the number of patients being asked their tobacco-use status and an increase in documentation of that status; however, it had no effect on the number of patients being counseled to quit or receiving medications. VA has also conducted train-the-trainer programs, such as its Preceptor Training Program, that have been effective in increasing tobacco-cessation awareness among VA mental health-care providers. The Preceptor Training Program trained over 160 preceptors representing all 21 VISNs in an integrated-care approach to incorporate tobacco-cessation treatments into mental-health treatment. Trainers monitored preceptorsâ progress at their medical facilities; preceptors were assisted in overcoming barriers to change through âbest practicesâ information, site progress reports, consultations with peers and mentors during regular conference calls, and dissemination of patient-health promotion materials and provider-education videos, print materials, and Web-based materials (VA, 2006c). Staff members are needed to obtain and disseminate educational materials for other staff and patients. Moreover, all staff should be knowledgeable about discussing tobacco use with their patients and making any necessary referrals for additional services; this may include referrals to community resources for veteransâ dependents who use tobacco. Lack of dedicated staff to conduct those tobacco-cessation
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 293 activities is a barrier to improved tobacco-cessation treatment (VA, 2007a). Finding: VA has instituted many provider-education programs that have been effective in raising awareness of the need for tobacco-cessation services for veterans. However, the programs may not be reaching all primary- care providers or other health professionals serving veterans. The use of reminders and prompts in patient medical records for tobacco-cessation counseling, referrals, and prescribing is one way in which VA has made innovative and effective advances. Recommendation: The committee recommends that all VA health-care providers receive training in tobacco-cessation interventions. SPECIAL POPULATIONS The VA health system provides care for a number of populations that may require special attention for tobacco-cessation treatment, including veterans with mental-health disorders, those with medical comorbidities, smokeless-tobacco users, female veterans (whose numbers are increasing), and veterans who are inpatients in hospitals, nursing homes, and psychiatric residences. As described in Chapter 2, VA serves a veteran population that tends to be older, less healthy, and of lower socioeconomic status than the general population. Reducing tobacco use in those populations poses a challenge to VA. The VA/DoD Clinical Practice Guideline for the Management of Tobacco Use addresses tobacco cessation in several special populations that are treated by VA, including pregnant women, hospitalized patients, older patients, and psychiatric and mental-health patients. The guideline encourages health-care providers to advise all of these patients to quit and to offer tobacco-cessation treatment. Additional recommendations on treating those patients refer to the population as a whole (including the general population, the military, and veterans); there are no modified recommendations for dealing with veterans in particular (VA/DoD, 2004). Veterans with Mental-Health Disorders VA provided mental-health care to an estimated 800,000 veterans in 2003 at a cost of more than $2 billion (Ziedonis et al., 2004). It is estimated that 25â40% of veterans in the VA health-care system
294 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS have a mental illness; diagnoses range from mild depression to severe forms of psychiatric illnesses. These veterans smoke at nearly twice the rate of people without mental-health disorders, and they smoke more heavily (VA, 2006c). VA is situated to care for veterans returning from the conflicts in Iraq and Afghanistan, one-third of whom are estimated to have a mental-health disorder; smoking is reported to have increased by 50% in those deployed veterans (Smith et al. 2008). Many of them also have diagnoses of more than one psychiatric disorder. VA is an acknowledged leader in research in the diagnosis and treatment of mental-health disorders, such as PTSD (Beckham et al., 2005, 2007, 2008; Dennis et al., 2007; Fu et al., 2007; Kirby et al., 2008). It has worked to improve tobacco-cessation services for those with mental illness. As described above, VA established a Preceptor Training Program to integrate tobacco-cessation treatment into mental health care. That program had 3 training sessions over 3 years and trained more than 160 preceptors representing all 21 VISNs; however, it has been discontinued. VA continues to hold train-the-trainer national conferences on such topics as the PHS Clinical Practice Guideline for Treating Tobacco Use and Dependence: 2008 Update. In 2004, VA sponsored a conference titled âVA in the Vanguard: Building on Success in Smoking Cessationâ on best practices in tobacco cessation in veteran populations served by VA; it included a session on mental health and PTSD (VA, 2004). Pharmacotherapy for treating nicotine dependence has been shown to be effective in people who have mental illness. This population faces additional challengesâstudies have indicated that those with comorbid conditions, particularly mental illness, are more likely to smoke and have a lower quit rate (see Chapter 4). The committee notes some important points regarding the use of smoking-cessation medications to treat tobacco dependence in people who have mental illness: this treatment requires a tailored approach to meet individual needs, it can be enhanced through a combination of pharmacotherapy and psychosocial therapy, and tobacco use can alter the effectiveness of a variety of medications used to treat mental illness, particularly antipsychotics, and should be monitored closely. The VA National Formulary contains all the FDA-approved tobacco-cessation medications that can be used by veterans with and without a mental illness. The formulary also has medications prescribed for psychiatric disorders. Mental-health professionals, primary-care physicians, and medical specialists need to be aware of all medications that their patients are taking, including such over-the-counter medications as NRTs.
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 295 The cost of medications for comorbid disorders in both DoD and VA is likely to decrease substantially if military personnel and veterans quit smoking. Patients with serious mental illnesses, such as schizophrenia and bipolar disorder, are commonly prescribed antipsychotic medications, such as olanzapine or clozapine. Those medications are expensive, and smokers who use them tend to need about twice the dose that nonsmokers need, because smoking increases their metabolism. VA uses several approaches to provide tobacco-use interventions to patients who have mental-health disorders and use tobacco. For many VA patients, the VA mental health-care provider is the de facto source of primary care. VA advocated an integrative approach to tobacco cessation for patients who have mental-health disorders in which mental health- care providers address both the mental illness and tobacco use rather than referring patients to a separate tobacco-cessation program (VA, 2006c). Specifics of how and why tobacco cessation should be integrated into mental health care in VA are given in the VA conference proceedings Integrating Tobacco Cessation Treatment into Mental Health Care: A Preceptor Training Program to Improve Delivery of Tobacco Cessation Treatment for Veterans with Mental Disorders (VA, 2006c). As described in Chapter 4, an integrative approach to tobacco cessation and mental health care has several advantages: ⢠Tobacco cessation works best when counseling is frequent and long-term; given the long-term nature of mental-health counseling, there is an opportunity for the therapist to provide continuing tobacco-cessation counseling. ⢠Patients may be more receptive to a combination of treatments at an appointment, inasmuch as many patients have substantial commutes or must take time out of their workday to attend a session, thus, the notion of a âone-stopâ session may be appealing. ⢠Given the potential for drug interactions, both favorable and adverse, between tobacco-cessation medications and medications for psychiatric disorders, the mental-health therapist can more effectively monitor side effects or psychologic changes that the patient experiences when taking multiple medications. The committee finds that the patient, provider, and programmatic barriers identified in the VA report are accurate, but believes that the evidence indicates that many of the barriers, particularly those related to providers and programs, can be overcome by establishing a more comprehensive program and emphasizing that the population in question
296 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS requires the same considerations and appropriate treatment as any other veteran population. Some VA researchers have advocated a stepped-care harm- reduction approach for VA tobacco users who have schizophrenia, particularly if they lack the motivation to quit (McChargue et al., 2002). This approach combines setting simple and progressive smoking- reduction goals with the use of atypical antipsychotics that reduce smoking spontaneously and eventually with the use of standard NRTs and bupropion. The approach steps up treatment once smoking reduction is maintained for a long period, but its effectiveness has not been evaluated. The VA National Cooperative Studies Program is supporting a study to include a targeted brief smoking-cessation component in the standard mental-health sessions received by veterans who have psychiatric disorders (McFall et al., 2007). The goal of this large, randomized, multisite effectiveness trial of integration of smoking- cessation treatment into mental health care is to have selected mental health-care providers who are trained in smoking-cessation techniques educate other mental-health professionals at their own facilities (Sherman and Farmer, 2004). All mental health-care providers would ask their patients about tobacco-use status, abstinence history, and reasons for smoking. The providers would also educate those who use tobacco about how it affects their psychologic and physical health, what improvements they might expect if they stopped using tobacco, and healthier strategies for managing emotional distress (Ziedonis, 2004). Ambivalent smokers receive motivational interventions. McFall et al. (2006) reported on the results of an earlier observational study of the above techniques in 107 veterans who had PTSD and smoked cigarettes. The study participants received psychotropic medications for PTSD and supportive psychotherapy in the form of five weekly sessions of smoking-cessation behavior counseling (and one follow-up session), self-help reading materials, intrasession support and assistance in identifying extrasession social support, self- directed behavioral methods for reducing anxiety (a relaxation training tape and stress-management materials), and pharmacologic interventions (bupropion and NRTs) from their mental health-care providers, including their case managers. The individual sessions were conducted during visits for PTSD or comorbid mental disorders. The integrated care was modeled on that given in the 2000 PHS clinical-practice guideline. Staff received 3 hours of training in smoking-cessation treatment. Results indicated that the integrated approach resulted in smoking quit rates comparable with those seen in studies involving smokers who had current mental disorders, such as schizophrenia and alcohol abuse. Those
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 297 who continued to smoke reduced their tobacco consumption. Furthermore, stopping smoking did not exacerbate the PTSD or comorbid depression (McFall et al., 2006). Beckham et al. (2008) found that smokers with PTSD were more likely to smoke when experiencing PTSD symptoms, anxiety, and stress. Finding: Veterans who have mental-health conditions may rely on the VHA for all of their health-care needs and may be unable to get access to tobacco-cessation treatment programs outside of VA. VA programs that integrate mental-health and tobacco-cessation treatment may increase cessation in veterans who have mental-health disorders. Recommendation: The VA should use an integrated approach for treating mental-health disorders and tobacco use. Mental-health providers should receive training in tobacco-cessation treatments and provide them to any patients who are willing to quit. Other Populations Smoking by veterans who have multiple sclerosis is common (28.5%). Many of them have attempted to quit, but most of those interested in quitting report that they do not receive smoking-cessation services (Turner et al., 2007). Veterans make up about one-third of the homeless population, and virtually all those veterans are male. Most homeless veterans are single, have poor and disadvantaged backgrounds, and are older and better educated than homeless nonveterans. About 45% of homeless veterans suffer from mental illness, and slightly more than 70% suffer from problems of alcohol or other drug abuse with substantial overlap in morbidities (VA, 2009c). There is virtually no information on tobacco use or tobacco-cessation services for homeless veterans. VA does not have a formal policy regarding tobacco-cessation services for spouses of veterans and nonveteran VA employees. Spouses of veterans and nonveteran VA employees are not eligible for VA pharmacy benefits that might cover the costs of tobacco-cessation medications or of formal counseling. Some VA cessation counselors, however, allow and even encourage veteran smokers to bring another person for support and to participate in cessation counseling sessions, but this practice is at the discretion of each counselor. The evidence shows that it is more difficult for a person to quit smoking if his or her spouse
298 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS continues to smoke (Monden et al., 2003; Murray et al., 1995; Osier and Prescott, 1998). VA employees, including union employees, may not have health-insurance coverage for prescription tobacco-cessation medications and may have to pay for both over-the-counter NRTs and prescription medications themselves whereas veterans can receive both types of medications as a covered benefit. Recommendation: The VA should assess the costs and benefits that might result from providing tobacco-cessation medications to partners of veterans and to nonveteran VA employees. Medications might be offered free of charge or at cost to the VA. SURVEILLANCE AND EVALUATION Ensuring the quality of all VA health programs is a continuing task and one that requires constant surveillance to determine what programs and policies are working and what should be done to correct the ones that are not. VA has used quality measurements and performance standards for many years but has not integrated them into an evaluation process that helps it to meet its goal of providing veterans with high-quality health care (Rosenheck, 2006). An assessment of performance does not necessarily result in improvement unless problems are addressed (Fink, 2005). VA conducts periodic internal surveys of veteransâ health, for example, the 2005 Survey of Veteran Enrolleesâ Health and Reliance upon VA with Selected Comparisons to the 1999â2003 Surveys. The surveys provide information on how many veterans use tobacco and how tobacco use varies by socioeconomic status, public and private insurance, health status, enrollee priority group, and VISN. That information is designed to assist VA decision-makers in policy development and strategic planning. The most recent survey shows that about 22% of veterans enrolled in the VA health service use tobacco (VA, 2006a). Evaluation programs can help VA in determining which of its programs have been most effective in helping various populations of veterans to cease tobacco use. VA has also conducted surveys of tobacco use and control throughout its health-care system. In particular, the 2005 Smoking and Tobacco Use Cessation Report (VA, 2006b), conducted for the Office of the Assistant Deputy Under Secretary for Health for Policy and Planning, provides a quantitative snapshot of smoking and tobacco-use cessation activities and smoke-free policies in VA. This survey of 158 VAMCs assessed facility resources to improve outcomes, identify best practices,
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 299 and promote collaborations among facilities. The smoking-cessation lead clinician at each VA facility completed the survey. The VA PHSHCG also held a Provider Feedback Forum on smoking- and tobacco-use cessation (VA, 2007a) to ask VA front-line health-care providers about their experiences in conducting smoking- and tobacco-cessation programs for VA patients. The forum addressed the implementation of evidence-based tobacco-use cessation interventions, special populations, pharmacy issues, tobacco-free policies, and current resources and future opportunities. However, beyond the data on required brief counseling and offer of medications, VA does not appear to have any data on whether its outpatient clinics and CBOCs offer tobacco-cessation programs, what types of services or referrals are offered and to whom, or how many veterans avail themselves of these services. The VA/DoD guideline and the 2008 PHS guideline for tobacco cessation recommend that VA health-care providers use the 5 Aâs for each patient. Before 2007, performance measures for VA health-care providers were based on whether patients were asked about tobacco use and whether they were advised to quit if they were users. Over 90% of providers were in compliance with these measures. The VA Office of Quality and Performance (OQP) is responsible for implementing and monitoring performance measures for VHA health-care providers, including adherence to the use of clinical reminders to ask about tobacco use and follow-up. In 2006, VA developed new performance measures that are used by the OQP to increase the provision of tobacco-cessation treatment to outpatients. The three performance measures are: (1) how many patients were provided with brief counseling in the preceding year, (2) how many patients who used tobacco were offered medication to assist in cessation, and (3) how many patients who used tobacco were offered referral to a smoking-cessation clinic to assist in cessation. Compliance with the performance measures for FY 2008 ranged from 75% to 99% among the VISNs (VA, 2007b). VA compliance with smoking-cessation care metrics exceeds that of the commercial sector or Medicaid for smoking-cessation counseling (89% vs. 76% vs. 70%, respectively), the offer of smoking- cessation medications (84% vs. 51% vs. 39%), and referral or use of smoking-cessation strategies (92% vs. 48% vs. 39%) (Kim Hamlett- Berry, VA, personal communication, November 10, 2008). Although VA is one of the health-care leaders in asking patients about tobacco use and has instituted electronic prompts in the patientsâ medical records to ensure that patients can receive tobacco-cessation medications and referrals if they want them, there is an almost total lack of information on whether the performance measures have had an effect on tobacco-use rates, although they have improved health-provider practices.
300 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS Furthermore, data on performance measures, the number of veterans who smoke, types of tobacco-cessation treatments available and their use, and costs and benefits of the programs are maintained in a variety of VA offices and facilities. Such scattering of the dataset makes evaluation of tobacco-control efforts difficult and opaque. The cost of treating veterans for tobacco use is comparatively small compared with the cost of treating veterans for tobacco-related diseases (Jonk et al., 2005), but the efficacy of the tobacco-cessation treatments is unclear. Without systematic and periodic evaluation of the outcomes of VAâs tobacco-cessation efforts, it is impossible for it to modify programs for maximum effectiveness or to introduce new and perhaps more successful approaches. The committee notes that VA does prepare an annual Performance and Accountability Report that includes a Clinical Practice Guidelines Index measure. This composite measure comprises âthe evidence and outcomes-based measures for high-prevalence and high-risk diseases that have significant impact on overall health status. The indicators within the Index are comprised of several clinical practice guidelines in the areas of ischemic heart disease, hypertension, diabetes mellitus, major depressive disorder, schizophrenia, and tobacco use cessation. . . . The measure demonstrates the degree to which VA provides evidence-based clinical interventions to veterans seeking care in VA. The measure targets elements of care that are known to have a positive impact on the health of our patients who suffer from commonly occurring acute and chronic illnessesâ (VA, 2008d). The measure, however, does not specifically report annual compliance with the VA/DoD Clinical Practice Guideline for the Management of Tobacco Use. Finding: The VA does conduct periodic surveys of its tobacco-cessation programs, but it has no central repository of information about the nature and implementation of tobacco-cessation activities. There is a lack of information about which treatment methods have been most sought by veterans and which have been most effective in enabling veterans to cease tobacco use. Recommendation: The VA should assess the reach and effectiveness of its tobacco-cessation programs.
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 301 REFERENCES An, L. C., S. H. Zhu, D. B. Nelson, N. J. Arikian, S. Nugent, M. R. Partin, and A. M. Joseph. 2006. Benefits of telephone care over primary care for smoking cessation: A randomized trial. Archives of Internal Medicine 166(5):536-542. Andrews, J. O., M. S. Tingen, J. L. Waller, and R. J. Harper. 2001. Provider feedback improves adherence with AHCPR Smoking Cessation Guideline. Preventive Medicine 33(5):415-421. Beckham, J. C., M. E. Feldman, S. R. Vrana, S. L. Mozley, A. Erkanli, C. P. Clancy, and J. E. Rose. 2005. Immediate antecedents of cigarette smoking in smokers with and without posttraumatic stress disorder: A preliminary study. Experimental and Clinical Psychopharmacology 13(3):219-228. Beckham, J. C., M. F. Dennis, F. J. McClernon, S. L. Mozley, C. F. Collie, and S. R. Vrana. 2007. The effects of cigarette smoking on script-driven imagery in smokers with and without posttraumatic stress disorder. Addictive Behaviors 32(12):2900-2915. Beckham, J. C., M. T. Wiley, S. C. Miller, M. F. Dennis, S. M. Wilson, F. J. McClernon, and P. S. Calhoun. 2008. Ad lib smoking in post- traumatic stress disorder: an electronic diary study. Nicotine and Tobacco Research 10(7):1149-1157. Borowsky, S. J., D. B. Nelson, J. C. Fortney, A. N. Hedeen, J. L. Bradley, and M. K. Chapko. 2002a. VA community-based outpatient clinics: Performance measures based on patient perceptions of care. Medical Care 40(7):578-586. Borowsky, S. J., D. B. Nelson, S. M. Nugent, J. L. Bradley, P. R. Hamann, C. J. Stolee, and H. B. Rubins. 2002b. Characteristics of veterans using Veterans Affairs community-based outpatient clinics. Journal of Health Care for the Poor and Underserved 13(3):334-346. Carmody, T. P., C. Duncan, J. A. Simon, S. Solkowitz, J. Huggins, S. Lee, and K. Delucchi. 2008. Hypnosis for smoking cessation: A randomized trial. Nicotine and Tobacco Research 10(5):811-818. Chapko, M. K., S. J. Borowsky, J. C. Fortney, A. N. Hedeen, M. Hoegle, M. L. Maciejewski, and C. VanDeusen Lukas. 2002. Evaluation of the Department of Veterans Affairs community-based outpatient clinics. Medical Care 40(7):555-560. Congressional Budget Office. 2005. The Potential Cost of Meeting Demand for Veteransâ Health Care. Washington, DC: Congress of the United States.
302 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS Dennis, M. F., C. P. Clancy, and J. C. Beckham. 2007. Gender differences in immediate antecedents of ad lib cigarette smoking in smokers with and without posttraumatic stress disorder: A preliminary report. Journal of Psychoactive Drugs 39(4):479-485. Dent, L. A., J. G. Scott, and E. Lewis. 2004. Pharmacist-managed tobacco cessation program in Veterans Health Administration community-based outpatient clinic. Journal of the American Pharmacists Association (2003) 44(6):700-714. Duffy, S. A., P. Reeves, C. Hermann, C. Karvonen, and P. Smith. 2008. In-hospital smoking cessation programs: What do VA patients and staff want and need? Applied Nursing Research 21(4):199-206. Essenmacher, C., C. Karvonen-Gutierrez, J. Lynch-Sauer, and S. A. Duffy. 2009. Staffâs attitudes toward the delivery of tobacco cessation services in a primarily psychiatric Veterans Affairs hospital. Archives of Psychiatric Nursing 23(3):231-242. Fink, A. 2005. Evaluation Fundamentals: Insights into the Outcomes, Effectiveness, and Quality of Health Programs. 2nd edition. London, UK: Sage Publications. Fiore, M. C., W. C. Bailey, and S. J. Cohen, et al. 2000. Treating Tobacco Use and Dependence. Clinical Practice Guideline. Rockville, MD: Department of Health and Human Services. Public Health Service. Fiore, M. C., C. R. Jaen, T. B. Baker, et al. 2008. Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guideline. Washington, DC: Department of Health and Human Services, Public Health Service. Fortney, J. C., S. J. Borowsky, A. N. Hedeen, M. L. Maciejewski, and M. K. Chapko. 2002. VA community-based outpatient clinics: Access and utilization performance measures. Medical Care 40(7):561-569. Fu, S. S., M. McFall, A. J. Saxon, J. C. Beckham, T. P. Carmody, D. G. Baker, and A. M. Joseph. 2007. Post-traumatic stress disorder and smoking: A systematic review. Nicotine and Tobacco Research 9(11):1071-1084. Hamlett-Berry, K., J. Davison, D. R. Kivlahan, M. H. Matthews, J. E. Hendrickson, and P. L. Almenoff. 2009. Evidence-based national initiatives to address tobacco use as a public health priority in the Veterans Health Administration. Military Medicine 174(1):29-34.
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 303 Jonk, Y. C., S. E. Sherman, S. S. Fu, K. W. Hamlett-Berry, M. C. Geraci, and A. M. Joseph. 2005. National trends in the provision of smoking cessation aids within the Veterans Health Administration. American Journal of Managed Care 11(2):77-85. Joseph, A. M., and L. C. An. 2004. Telephone care for smoking cessation in the Department of Veterans Affairs. In VA in the Vanguard: Building on Success in Smoking Cessation, edited by S. Isaacs, S. Schroeder and J. Simon. San Francisco, CA: Department of Veterans Affairs. Joseph, A. M., N. J. Arikian, L. C. An, S. M. Nugent, R. J. Sloan, and C. F. Pieper. 2004. Results of a randomized controlled trial of intervention to implement smoking guidelines in Veterans Affairs medical centers: Increased use of medications without cessation benefit. Medical Care 42(11):1100-1110. Kirby, A. C., B. P., Hertzberg, C. F. Collie, B. Yeatts, M. F. Dennis, S. D. McDonald, P. S. Calhoun, and J. C. Beckham. 2008. Smoking in help-seeking veterans with PTSD returning from Afghanistan and Iraq. Addictive Behaviors 33(11):1448-1453. Kirchner, J. E., R. R. Owen, N. Dockter, T. L. Kramer, K. Henderson, T. Armitage, and E. Allee. 2008. Equity in veteransâ mental health care: Veterans Affairs medical center clinics versus community-based outpatient clinics. American Journal of Medical Quality 23(2): 128-135. Lenert, L., R. F. Muñoz, J. Stoddard, K. Delucchi, A. Bansod, S. Skoczen, and E. J. Pérez-Stable. 2003. Design and pilot evaluation of an internet smoking cessation program. Journal of the American Medical Informatics Association 10(1):16-20. Liu, C. F., M. K. Chapko, M. W. Perkins, J. Fortney, and M. L. Maciejewski. 2008. The impact of contract primary care on health care expenditures and quality of care. Medical Care Research and Review 65(3):300-314. Maciejewski, M. L., M. Perkins, Y. F. Li, M. Chapko, J. C. Fortney, and C. F. Liu. 2007. Utilization and expenditures of veterans obtaining primary care in community clinics and VA medical centers: An observational cohort study. BMC Health Service Research 7:56. Massachussetts Department of Veteransâ Services. 2008. Free Nicotine Patches Now Available to Massachusetts Veterans and Their Families. Medical News Today. November 17. http://www.medicalnewstoday.com/articles/130034.php (accessed December 17, 2008).
304 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS McChargue, D. E., S. B. Gulliver, and B. Hitsman. 2002. Would smokers with schizophrenia benefit from a more flexible approach to smoking treatment? Addiction 97(7):785-793. McFall, M., D. C. Atkins, D. Yoshimoto, C. E. Thompson, E. Kanter, C. A. Malte, and A. J. Saxon. 2006. Integrating tobacco cessation treatment into mental health care for patients with posttraumatic stress disorder. American Journal of Addiction 15(5):336-344. McFall, M., A. J. Saxon, S. Thaneemit-Chen, M. W. Smith, A. M. Joseph, T. P. Carmody, J. C. Beckham, C. A. Malte, J. E. Vertrees, K. D. Boardman, and P. W. Lavori. 2007. Integrating smoking cessation into mental health care for post-traumatic stress disorder. Clinical Trials 4(2):178-189. Meredith, L. S., E. M. Yano, S. C. Hickey, and S. E. Sherman. 2005. Primary care provider attitudes are associated with smoking cessation counseling and referral. Medical Care 43(9):929-934. Monden, C. W. S., N. D. De Graaf, and G. Kraaykamp. 2003. How important are parents and partners for smoking cessation in adulthood? An event history analysis. Preventive Medicine 36(2): 197-203. Murray, R. P., J. J. Johnston, J. J. Dolce, W. W. Lee, and P. OâHara. 1995. Social support for smoking cessation and abstinence: The lung health study. Addictive Behaviors 20(2):159-170. Osier, M., and E. Prescott. 1998. Psychosocial, behavioural, and health determinants of successful smoking cessation: A longitudinal study of Danish adults. Tobacco Control 7(3):262-267. Rosenheck, R. 2006. Mental and substance-use health services for veterans: Experience with performance evaluation in the Department of Veterans Affairs. Appendix C, in Improving the Quality of Health Care for Mental and Substance-Use Conditions. Institute of Medicine. Washington, DC: The The National Academies Press. Pp. 423-482. Sherman, S. E., and M. M. Farmer. 2004. Best practices in tobacco control: Identifying effective strategies for improving quality within the Veterans Health Administration. In VA in the Vanguard: Building on Success in Smoking Cessation, edited by S. Isaacs, S. Schroeder and J. Simon. San Francisco, CA: Department of Veterans Affairs. Sherman, S. E., E. M. Yano, L. S. York, A. B. Lanto, B. A. Chernof, and B. S. Mittman. 2006a. Assessing the structure of smoking cessation care in the Veterans Health Administration. American Journal of Health Promotion 20(5):313-318.
DEPARTMENT OF VETERANS AFFAIRS TOBACCO-CONTROL ACTIVITIES 305 Sherman, S. E., A. M. Joseph, E. M. Yano, B. F. Simon, N. Arikian, L. V. Rubenstein, P. Parkerton, and B. S. Mittman. 2006b. Assessing the institutional approach to implementing smoking cessation practice guidelines in Veterans Health Administration facilities. Military Medicine 171(1):80-87. Sherman, S. E., M. Estrada, A. B. Lanto, M. M. Farmer, and I. Aldana. 2007. Effectiveness of an on-call counselor at increasing smoking treatment. Journal of General Internal Medicine 22(8):1125-1131. Sherman, S. E., N. Takahashi, P. Kalra, E. Gifford, J. W. Finney, J. Canfield, J. F. Kelly, G. J. Joseph, and W. Kuschner. 2008. Care coordination to increase referrals to smoking cessation telephone counseling: A demonstration project. American Journal of Managed Care 14(3):141-148. Smith, B., M. A. Ryan, D. L. Wingard, T. L. Patterson, D. J. Slymen, and C. A. Macera. 2008. Cigarette smoking and military deployment a prospective evaluation. American Journal Preventive Medicine 35(6): 539-546. Turner, A. P., D. R. Kivlahan, L. E. Kazis, and J. K. Haselkorn. 2007. Smoking among veterans with multiple sclerosis: Prevalence correlates, quit attempts, and unmet need for services. Archives of Physical Medicine and Rehabilitation 88(11):1394-1399. VA (Department of Veterans Affairs). 2004. VA in the Vanguard: Building on Success in Smoking Cessation. Edited by S. Isaacs, S. Schroeder and J. Simon. San Francisco, CA: VA. VA. 2006a. 2005 Survey of Veteran Enrolleesâ Health and Reliance upon VA with Selected Comparisons to the 1999â2003 Surveys. Washington, DC: Veterans Health Administration. VA. 2006b. Smoking and Tobacco Use Cessation Reportâ2005. Washington, DC: Veterans Health Administration, Office of the Assistant Deputy Under Secretary for Health for Policy Planning. VA. 2006c. Integrating Tobacco Cessation Treatment into Mental Health Care. Washington, DC: Veterans Health Administration. VA. 2007a. Provider Feedback Forum on Smoking and Tobacco Use Cessation. Atlanta, GA: Veterans Health Administration, Public Health Strategic Health Care Group. VA. 2007b. Q1 Technical Manual for the VHA Performance Measurement System. Washington, DC: Department of Veterans Affairs, Office of Quality and Performance. VA. 2008a. FY07 Annual VA Information Pamplet. http://www1.va.gov /vetdata /docs/Pamphlet_2-1-08.pdf (accessed February 2, 2009).
306 COMBATING TOBACCO USE IN MILITARY AND VETERAN POPULATIONS VA. 2008b. VA Benefits and Health Care Utilization. Washington, DC: National Center for Veterans Analysis and Statistics. VA. 2008c. 2008 Organizational Briefing Book. Washington, DC: VA, Office of Human Resources and Administration. VA. 2008d. FY 2008 Performance and Accountability Report. Washington, DC: VA, Office of the Secretary. VA. 2009a. Fact Sheet: VA Benefits & Health Care Utilization. http://www1.va.gov/vetdata/docs/ 4X6_spring09_sharepoint.pdf (accessed February 3, 2009). VA. 2009b. Locations: Veterans Health Administration. http://www2.va. gov/directory/guide/division.asp?dnum=1 (accessed April 9, 2009). VA. 2009c. Overview of Homelessness. http://www1.va.gov/homeless/ page.cfm?pg=1 (accessed April 10, 2009). VA/DoD (Department of Defense). 2004. VA/DoD Clinical Practice Guideline for the Management of Tobacco Use. Washington, DC: VA/DoD. Volpp, K. G., A. Gurmankin Levy, D. A. Asch, J. A. Berlin, J. J. Murphy, A. Gomez, H. Sox, J. Zhu, and C. Lerman. 2006. A randomized controlled trial of financial incentives for smoking cessation. Cancer Epidemiology Biomarkers and Prevention 15(1):12-18. Yano, E. M., L. V. Rubenstein, M. M. Farmer, B. A. Chernof, B. S. Mittman, A. B. Lanto, B. F. Simon, M. L. Lee, and S. E. Sherman. 2008. Targeting primary care referrals to smoking cessation clinics does not improve quit rates: Implementing evidence-based interventions into practice. Health Service Research 43(5):1637-1661. Ziedonis, D. M. 2004. Integrated treatment of co-occurring mental illness and addiction: Clinical invervention, program, and system perspectives. CNS Spectrums 9(12):892-904. Ziedonis, D. M., J. M. Williams, M. L. Steinberg, D. Smelson, J. Krejci, B. D. Sussner, N. Violette, and J. Foulds. 2004. Addressing tobacco dependence among veterans with a psychiatric disorder: A neglected epidemic of major clinical and public health concern. In VA in the Vanguard: Building on Success in Smoking Cessation, edited by S. Isaacs, S. Schroeder and J. Simon. San Francisco, CA: Department of Veterans Affairs.