1
Introduction and Background
Surveillance for, detection of, and response to natural or unintentional disease outbreaks are traditional responsibilities of public health authorities, who rely heavily on health care providers and laboratories to provide timely reports on diagnoses and test results. The national security community also has a long history of biosurveillance and response for defense against threats from biological weapons used as agents of warfare or terrorism. Since the 1990s, growing concerns about bioterrorism and potential epidemics of emerging infectious diseases have spurred interest in developing new and better ways to detect biological threats as quickly as possible so that preventive measures or treatment can be started in time to reduce illnesses and deaths.
After the 9/11 attacks and the anthrax letters in 2001, one response to the threat of bioterrorism was the initiation in 2003 of an environmental air monitoring program called BioWatch. Under this program, the Department of Homeland Security (DHS) has deployed hundreds of air samplers in more than 30 major cities, primarily in outdoor locations, to detect the presence of certain pathogens of concern, should any of them be released in aerosolized form. The aim of the BioWatch program is to speed the detection of aerosolized pathogens to help local health officials respond swiftly to a potential bioterrorism emergency.
Implementing the BioWatch program within a few weeks after it was announced in January 2003 required identifying an air sampling device that could be quickly adapted for field use and deployed. It also required determining how many devices would be used, where they would be placed, where and how the samples would be analyzed, and what the daily operat-
ing procedures would be. Since 2003, DHS has modified several aspects of the BioWatch system by enhancing the air samplers; deploying additional monitoring devices; relocating devices; and revising protocols for routine operations, analyses, and actions following a positive laboratory result. DHS has also been pursuing alternative approaches to sample collection and analysis to respond to a recognized need to produce results more quickly, more frequently, and from more varied locations than is possible with the current system.
The BioWatch system is a civilian environmental monitoring component of a much broader domestic biodefense effort that encompasses a variety of activities. These include information gathering and analysis to identify potential threats and the risk they pose, various monitoring and detection activities, public health and law enforcement responses, and programs leading to restoration and recovery (The White House, 2004; FEMA, 2008).
Among these activities are efforts being made to strengthen the ability at the local, state, and national levels to detect and respond to infectious disease emergencies of all types.1 The Department of Health and Human Services (HHS) is leading the federal activities with funding and other resources to support the development of a more robust capacity within the public health and the health care sectors to recognize unfamiliar illnesses or unusual clusters of cases, effectively assemble essential information to guide decision making, and speed deployment of an appropriate response.
Despite improvements since 2001 in the nation’s preparedness to detect and respond to bioterrorism or emerging infectious disease threats, some concerns remain. For example, the Government Accountability Office (GAO, 2009) highlighted continuing needs to clarify federal leadership roles and close known gaps in pandemic influenza preparedness plans. Particular concerns about BioWatch include the timeliness, probability, and accuracy of detection using the current system and the maturity of plans for the introduction of a new generation of devices for automated collection, preparation, and analysis of air samples (e.g., O’Toole, 2007a,b; Price, 2008). Another concern is whether the BioWatch system is appropriately integrated with other health-related surveillance and response efforts that must be available to act on a BioWatch alert (e.g., O’Toole, 2007b; Downes, 2008; Price, 2008; Lindley, 2009).
Because of such concerns, Congress, through the Subcommittee on Homeland Security of the House Appropriations Committee, directed the Office of Health Affairs (OHA) in DHS to engage the National Academies to evaluate the effectiveness of BioWatch, to compare the benefits and costs of the current version of BioWatch with a planned modification, and to
compare BioWatch with an enhanced national surveillance system that relies on the health care and public health systems.
STUDY CHARGE AND COMMITTEE MEMBERSHIP
To carry out this congressionally mandated study, the National Academies convened the Committee on Effectiveness of National Biosurveillance Systems: BioWatch and the Public Health System. The charge from DHS calls for the committee (1) to evaluate the effectiveness of BioWatch, including a comparison of benefits and costs for the existing program (referred to here as Generation 2) and for a planned “next generation” program that uses new, automated field devices deployed in greater numbers (Generation 3); (2) to assess the costs and benefits of enhanced national surveillance that relies on U.S. hospitals and the U.S. public health sector; and (3) to compare the effectiveness of surveillance activities and tools used by the public health and health care systems to that of the current BioWatch approach. The complete statement of task appears in Box 1-1.
Committee members were selected to contribute expertise in areas that include biological threat assessments, evaluation of biological detection systems, environmental monitoring technologies, biological assays, microbiology, virology, epidemiology, syndromic surveillance, health information technology, the U.S. public health sector, hospital systems, emergency medicine, laboratory operations, statistical methods, systems engineering, operations research, and economic analysis.
The committee met in person five times from July 2008 through January 2009 and conferred by conference call several times during the study. The group gathered information from presentations by invited participants at its first three meetings, responses to written requests for information submitted to DHS and the Centers for Disease Control and Prevention (CDC) in HHS, commissioned analyses, and examination of published literature. An interim report, which described the state of the committee’s review but contained no findings or recommendations, was released in February 2009.2 Additional information about the committee’s activities appears in Appendix A.
Invited participants at the committee’s meetings included Congressman David Price; representatives of DHS, HHS, and other federal agencies; representatives of state and local health departments; physicians in clinical practice; and researchers from academia and commercial firms who are developing laboratory testing tools. At the committee’s request, the firm Industrial Economics, Incorporated, prepared information on the costs of
|
2 |
The interim report is available from the National Academies Press at http://www.nap.edu/catalog.php?record_id=12599. |
the BioWatch program and of biosurveillance activities in the public health and health care systems. The committee also commissioned Dr. David Buckeridge of McGill University to perform a simulation analysis to compare the effect of detection methods on the time from release of aerosolized anthrax spores to initiation of treatment.
SCOPE OF THE STUDY
The committee interpreted its task as assessing current and proposed approaches for detecting serious human disease threats, especially those resulting from bioterrorism. These approaches include (1) aerosol monitoring by the BioWatch system, (2) public health case reporting from clinical and laboratory settings, and (3) “syndromic” surveillance programs that aggregate and analyze various types of data that might be available before the diagnosis of the first case (e.g., chief complaints at emergency department visits, pharmacy sales, absenteeism) to identify unusual patterns that may signal a disease outbreak.
National policy emphasizes the importance of surveillance for detection, as quickly as possible, of potentially catastrophic biological threats to the civilian population of the United States in order to have an opportunity to maximize the decisiveness, timeliness, and effectiveness of public health actions to control disease. The National Response Framework (FEMA, 2008, p. 42) defines a catastrophic incident as “any natural or manmade incident, including terrorism, that results in extraordinary levels of mass casualties, damage, or disruption severely affecting the population, infrastructure, environment, economy, national morale, and/or government functions.”
The study considered detection of both deliberately introduced and naturally occurring infectious diseases—that is, agents of bioterrorism and significant emerging infectious diseases such as pandemic influenza and SARS. Detection of bioterrorism received greater attention because it is the purpose of the BioWatch program. The committee recognized that the national security community maintains an active information acquisition and analysis system that focuses on a subset of the infectious disease threat that is related to bioterrorism and biowarfare. The committee also recognized, and emphasizes in this report, that the health care and public health systems together are intrinsically a funnel through which information about all forms of disease flow, whether related to bioterrorism or not.
Tasks the committee considered to be beyond the scope of the study include an evaluation of underlying assumptions about and estimates of the magnitude of (1) the risk of bioterrorism; (2) the risk of bioterrorism relative to other terrorism threats; (3) the risk posed by any one potential bioterrorism agent compared with another; and (4) relative risks from natural versus bioterrorist threats. Also beyond the study’s scope is an examination of the capability at
|
BOX 1-1 Statement of Task The Institute of Medicine (IOM) and National Research Council (NRC) will evaluate the effectiveness of BioWatch, including a comparison of benefits and costs for Generations 2 and 3; the costs and benefits of an enhanced national surveillance system that relies on U.S. hospitals and the U.S. public health system will also be assessed, and its effectiveness compared to that of the current BioWatch approach. The evaluation will include examination of the reliability of BioWatch monitoring data and the ability of hospitals and public health officials to respond based on information received from that system. Services under this contract will encompass the evaluation of the effectiveness of both current and enhanced biosurveillance systems to detect biological terrorism or other biothreats to human health, including (1) differing technological generations of BioWatch, (2) current human health-related surveillance systems, including those for zoonotic disease, and (3) describing necessary enhancements to hospital and public health systems based on measures of effectiveness in detecting attacks of bioterrorism or other biothreats. Measures of effectiveness will include the ability of surveillance systems to warn sufficiently to provide effective post-exposure prophylaxis and effective post-infection treatment to affected populations following a bioterrorist attack or other biothreat event. The IOM and the NRC shall provide expert advisors that reflect expertise in relevant fields, such as biological threat assessments, biological detection systems evaluation, environmental monitoring technologies, biological assays, microbiology, virology, epidemiology, health information technology, the U.S. public health system, hospital operations, local emergency management, public health response, statistical methods, infectious disease modeling, syndromic surveillance, systems engineering, operations research, complex database management and analysis; and economic analysis. The following are specific requirements under this requirement. The IOM/NRC shall provide sufficient staff support to organize meetings, generate reports and manage the contract. The IOM/NRC will: |
the federal, state, and local levels to mount a timely and effective response to the detection of a serious disease threat. Even so, the committee understands that these matters of risk and response capability are critically important to assessing the value of BioWatch and returns to them later in this chapter.
The study’s focus on the civilian population in the United States means that the committee, while recognizing the need to monitor and poten-
|
tially respond to international disease activity, did not examine disease surveillance systems in other countries or ones operated by international organizations. Disease threats to animals and plants per se are also excluded, although these disease threats are very much a part of the broader perspective on bioterrorism (e.g., NRC, 2002; GAO, 2004; The White House, 2004, 2007). Many known infectious disease agents and potential
bioterrorism agents are zoonotic; that is, they are animal diseases that can be transmitted to humans. New zoonotic disease threats may also arise as changes occur in the ability of animal diseases to adversely affect human health. As a result, surveillance tools that monitor animal health and the presence of zoonotic pathogens are an important component of surveillance systems that focus on human health.
CURRENT FEDERAL FUNDING FOR CIVILIAN ACTIVITIES FOR DEFENSE AGAINST BIOLOGICAL THREATS
No consolidated summary of federal funding for civilian activities to defend against bioterrorism and other significant biological threats is directly available from federal budget documents. Past estimates have been compiled from an examination of programs distributed across several departments, including DHS, HHS, the Department of Defense (DoD), the Department of Agriculture, and the Environmental Protection Agency (e.g., Franco, 2008). Although the President’s budget for fiscal year (FY) 2010 became available as this report was being completed, aggregated estimates were available only through FY 2009. The estimated FY 2009 total for federal funding for civilian activities to defend against bioterrorism and other significant biological threats was approximately $8.0 billion (Franco, 2008). Of this, $4.2 billion was for activities in HHS and $2.5 billion for DHS. Approximately $2.2 billion of the FY 2009 budget proposal for DHS was for a multiyear allocation for Project BioShield.3 The remaining $1.3 billion of the $8 billion total was to support activities in other agencies.
The HHS funding supports activities that range from basic research to operational support for states and communities in national emergencies. This includes the federal funding through CDC for public health surveillance activities, the cooperative agreement program to build state and local emergency preparedness capacity, and the Strategic National Stockpile.4 Excluding Project BioShield, the DHS funding includes the BioWatch program in OHA, the National Biosurveillance Integration Center, and research and development activities in the Science and Technology Directorate. Table 1-1 shows appropriated or proposed federal funding from FY 2007 through FY 2010 for specific activities in HHS and DHS.
TABLE 1-1 Federal Funding for Selected Civilian Activities to Defend Against Bioterrorism and Other Significant Biological Threats, Fiscal Years 2007–2010 (in millions $)
State and local funds also support related activities. The amount of state and local support for disease surveillance and other activities related to bioterrorism is difficult to estimate because these activities are generally carried out as part of a system aimed at detecting and responding to naturally occurring diseases.
BIOLOGICAL THREATS TO HUMAN HEALTH
Potential Bioterrorism Agents
Biological agents that might be deliberately introduced in an act of war or bioterrorism include a variety of bacteria, viruses, protozoa, multicellular parasites, and biological toxins. These may be naturally occurring pathogens or pathogens enhanced to increase their usefulness as bioterrorism agents. Biological agents that are publicly recognized as potentially useful for bioterrorism have been categorized by CDC on the basis of characteristics such as their lethality and potential for dissemination (see Box 1-2). The “Category A” agents are a high priority. The agents included in categories B and C are ones that appear to pose serious but more limited risks.
Further analysis and delineation of current and future potential bioterrorism and biowarfare threats is an ongoing activity performed by the
|
BOX 1-2 CDC Categories of Potential Bioterrorism Agents and Their Related Diseases Category A Agents that include organisms that pose a risk to national security because they can be easily disseminated or transmitted from person to person; result in high mortality rates and have the potential for major public health impact; might cause public panic and social disruption; and require special action for public health preparedness. Bacillus anthracis (anthrax) Clostridium botulinum toxin (botulism) Yersinia pestis (plague) Variola major (smallpox) Francisella tularensis (tularemia) Viruses causing hemorrhagic fevers, including Filoviruses (e.g., Ebola, Marburg)Filoviruses (e.g., Ebola, Marburg) Arenaviruses (e.g., Lassa, Machupo)Arenaviruses (e.g., Lassa, Machupo) Category B Agents that are moderately easy to disseminate; result in moderate morbidity rates and low mortality rates; and require specific enhancements of CDC’s diagnostic capacity and enhanced disease surveillance. Brucella species (brucellosis) Epsilon toxin of Clostridium perfringens Food safety threats, including |
national security community. In its work, the committee focused on surveillance for currently acknowledged bioterrorism threats, especially those addressed by the BioWatch program, but it recognizes the potential for other bioterrorism agents that may pose new surveillance challenges.
Because biological agents vary in their physical characteristics and impact on human health, no single strategy to defend against bioterrorism is likely to suffice. Inhalation anthrax and botulism, for example, are highly lethal if untreated, but these are not contagious illnesses (i.e., not transmissible from person to person). Smallpox, caused by the variola major virus, is contagious, but the mortality rate for untreated illness is likely to be much lower than that for inhalation anthrax. Medical options for prevention and treatment also vary. Vaccines are available to protect against anthrax and smallpox. Infections with some of these agents are susceptible to antibacterial or antiviral medications, and an antitoxin is available to treat some forms of botulism. However, other illnesses can only be treated
|
Salmonella species Escherichia coli O157:H7 Shigella species Burkholderia mallei (glanders) Burkholderia pseudomallei (melioidosis) Chlamydia psittaci (psittacosis) Coxiella burnetii (Q fever) Ricin toxin from Ricinus communis (castor beans) Staphylococcal enterotoxin B Rickettsia prowazekii (typhus fever) Viruses causing encephalitis, including Alphaviruses (e.g., Venezuelan equine encephalitis, eastern equine encephalitis, western equine encephalitis) Water safety threats, including Vibrio cholerae (cholera) Cryptosporidium parvum (cryptosporidiosis) Category C Agents that include emerging pathogens that could be engineered for mass dissemination in the future because of availability, ease of production and dissemination, and potential for high morbidity and mortality rates and major health impact. Emerging infectious agents such as Nipah virus and hantavirus SOURCE: Adapted from CDC (2008a). |
with supportive therapies (e.g., mechanical ventilation, hydration) that may reduce mortality.
In their naturally occurring forms, many of the Category A, B, and C agents are probably poorly suited to the aerosol dispersal that the BioWatch system is designed to detect, but some are naturally stable in the environment (e.g., the spores of Bacillus anthracis) (Sinclair et al., 2008). It is also possible to stabilize aerosolized agents to enhance retention of their infectivity. However, aerosol dispersal is not the only way biological agents might be used. Detection of an alternative dispersal mode would require a means other than BioWatch. For example, BioWatch is not designed to detect dissemination of biological agents through foodstuffs or deployed to detect them through postal delivery.
Modern medical and public health experience with many of these biological agents is limited, as is experience with bioterrorism. In 1984, there were 751 known cases of salmonellosis from deliberate contamination of a
salad bar but no deaths (Török et al., 1997). The 2001 anthrax letters produced infections in 22 patients, and 5 of these patients died (Jernigan et al., 2002). About 32,000 people who may have been exposed to the anthrax spores received antimicrobial prophylaxis (CDC, 2001a). The committee also noted that the impacts of bioterrorist activities can go far beyond morbidity and mortality statistics, as witnessed by the impacts of the anthrax letter attacks. The potential for impacts similar to other national security threats provides the basis for the classification of bioterrorism agents as weapons of mass destruction.
Naturally Occurring Infectious Disease Threats
Among the potential emerging disease threats, a highly virulent, pandemic influenza is a leading concern. The appearance of the novel influenza A (H1N1) virus in spring 2009 (as this report was being completed) gave an indication of the serious challenges that are anticipated, not only in managing the delivery of medications and medical care but also in implementing quarantines or other disease containment measures and minimizing the disruption of essential public and private services. The past decade has also seen the emergence of diseases caused by previously unrecognized threats (e.g., the SARS coronavirus) or the sudden appearance in a new environment of unfamiliar pathogens (e.g., West Nile virus or the monkeypox virus). These experiences point to several challenges for timely public health science and practice: distinguishing novel outbreaks from endemic disease, defining diagnostic criteria, identifying the causal agent and its route of transmission, tracking the spread of the disease, and identifying and deploying methods for prevention and treatment. Unusual disease outbreaks may also involve both the national security and public health communities until the origin of the outbreak is determined.
While the United States is preparing against the possibility of major infectious disease outbreaks from natural or intentional causes, infectious diseases are routinely responsible for tens of thousands of deaths each year. CDC estimated the infectious disease toll in 2000 at 75,000 deaths, plus approximately 15,000 additional deaths related to HIV/AIDS (Mokdad et al., 2004). In a typical year in the 1990s, as many as 36,000 deaths were related to influenza (Thompson et al., 2003). However, the influenza pandemic of 1918–1919 resulted in an estimated 675,000 deaths in the United States and perhaps as many as 50 million deaths worldwide (HHS, no date). The 2003 SARS epidemic was responsible for 774 reported deaths and 8,098 cases worldwide (WHO, 2004). The United States had 29 reported cases, 8 of which were confirmed by laboratory testing, but no deaths (CDC, 2003). The 2009 novel influenza A (H1N1) epidemic is still under way at the time this report is being finished. As of July 1, 2009, the World Health
Organization (WHO, 2009) had received reports of 77,201 cases and 332 deaths. CDC (2009b) was reporting 27,717 confirmed or probable cases and 127 deaths in the United States as of June 25, 2009.
DETECTING BIOLOGICAL THREATS
Routinely, health care providers, laboratories, and health departments work together to diagnose disease and recognize outbreaks that require a broader response than standard treatment provided for individual, unrelated cases. The BioWatch system is intended to provide an earlier warning to health departments of the aerosolized release of certain bioterrorism agents so that a rapid response can limit morbidity and mortality. While the use of this sort of “environmental monitoring” is intuitively appealing (assuming detection is likely and likely to be accurate), many questions arise from the premise that earlier awareness of the presence of a pathogen will result in a faster and more effective response and fewer deaths or illnesses. Recognizing the complexities around detection of and response to biological threats can help policy makers evaluate the scope, capability, and effectiveness of various biosurveillance approaches.
What Does “Early” Detection Mean?
One set of questions concerns the definition of “early” and the amount of time (hours? days?) that using BioWatch might save over clinical case finding or other surveillance approaches in delivering an appropriate response. As BioWatch currently operates, the air samplers typically have a 24-hour collection cycle, and their dry filters are manually collected and transported to laboratories for processing and analysis. The analysis of these samples can provide evidence that segments of the DNA of certain organisms were present some time during the 24-hour period before the filter was collected. Although the presence in the environment of segments of DNA associated with a pathogenic organism is a signal of possible danger, the committee saw that this information alone is not necessarily sufficient to determine the appropriate next steps and that it may be necessary to assess other important information to determine if an effective bioterrorism attack has occurred. Such information may include whether infectious organisms are present, whether these organisms are naturally occurring in the local environment, or perhaps whether hospitals are seeing patients with symptoms consistent with infection by the detected agent.
Alternatively, an epidemic arising from a bioterrorist attack or other source may be recognized by health care providers who notice an unusual pattern of disease among their patients or who diagnose an unusual infection that is recognized as a potential “index case” for an epidemic that is
yet to become fully manifest. Syndromic surveillance systems seek to automate and expand the recognition of unusual disease trends by capturing data related to the onset of illness, such as visits to emergency departments, clusters of patients with certain symptoms, increases in absenteeism, or purchase of over-the-counter medications. The resulting time line, which may run to days or weeks after an attack, will depend on multiple factors, such as the number of people exposed, the amount of the pathogen exposed people take in (i.e., the dose received), the incubation period of the disease, when and where infected people decide to seek care, and, for clinical case reporting, the astuteness of clinicians seeing those patients.
Figure 1-1 illustrates the general temporal relationship among different means of detecting the presence of a pathogen or illness or death resulting from exposure to the pathogen in jurisdictions where BioWatch operates. Depending on the nature of specific events, the relative sequence or overlap of events may vary from what is depicted here. For example, clinicians may recognize and report an increase in nonspecific manifestations of disease before syndromic surveillance systems yield statistical alarms. If laboratory testing of BioWatch samples were delayed, unusual trends in illness may be recognized before BioWatch yields an alert. Similarly if there is significant time between collection of clinical specimens and the availability of pre-
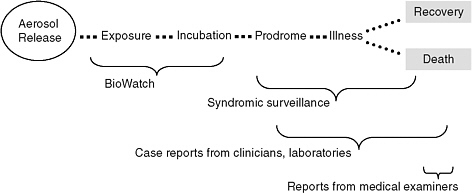
FIGURE 1-1 Schematic illustration of the temporal relation among potential mechanisms for detecting an aerosolized biological threat. The brackets span the interval over which a particular mechanism would have the potential to detect the presence of a pathogen (e.g., via BioWatch) or illness or death caused by the pathogen. This illustration represents the initial detection of a bioterrorism event. The time line for detection of subsequent events that are part of the same attack may be compressed because an initial detection is likely to increase attention to the potential threat.
SOURCE: Adapted from Sosin (2008).
liminary or definitive laboratory assessments, a signal from the BioWatch system may speed awareness of the attack.
For inhalation anthrax, considered by many to be the bioterrorism threat of greatest concern, the incubation period may be as little as 24 to 48 hours for susceptible individuals who receive a large dose, but cases may also occur as long as 1 to 2 months after exposure. The prodrome (a period of nonspecific signs and symptoms) may last 1 to 5 days before the onset of severe illness. Death may follow severe illness within 24 to 36 hours (CDC, 2002; Inglesby et al., 2002). Vaccination or antibiotics given soon after exposure may prevent many infections, and aggressive treatment before the onset of severe illness may prevent some deaths.
Does Early Detection Help?
A second set of questions concerns whether earlier detection by itself will make a difference. It is not a foregone conclusion that the systems of decision making and response in any particular location are able to use the advantage of earlier detection to prevent or limit exposure to a detected pathogen or effectively distribute medical countermeasures. As noted, effective medical countermeasures (e.g., antibacterials, antivirals, and vaccines) are available for some pathogens but not all. Even if such countermeasures exist, they will be most effective if they can be distributed and administered before most of the people who have been exposed develop illness. In the event of a massive airborne bioterrorist attack in an urban area, this may require delivering medications to hundreds of thousands, if not several million, people. For inhalation anthrax, the window between exposure and effective prophylaxis may be as short as 48 hours. However, the value of early detection may be less important or of unknown value for exposure to other agents, depending on the incubation period or the potential effectiveness of post-exposure prophylaxis. Furthermore, while failure to respond quickly in the face of a significant biological threat may have dire consequences, initiating an unnecessary response on the basis of misleading or erroneous information may have its own adverse results. For example, people may become ill from taking unnecessary medications, and mistakenly alarming the public may reduce the credibility and impact of justified warnings in the future.
A follow-on consideration is whether surveillance systems that detect a biological threat in one locality can contribute to improved “situational awareness” during the course of a prolonged or multisite attack or outbreak. With heightened awareness, it may be possible to intensify environmental sampling or disease surveillance activities in ways that will increase the chances of earlier detection of subsequent attacks or related outbreaks. This is similar to what may occur in a natural outbreak, such as the recent H1N1 pandemic.
What Should Be the Focus of Early Detection?
A third set of questions concerns the focus of any environmental monitoring system such as BioWatch. At present, BioWatch is designed to detect a limited number of potential bioterrorism agents, and DHS has proposed increasing this number (DHS, 2009a). Although this expansion may prove feasible, the rationale for selecting additional agents will have to be considered carefully in terms of the bioterrorism risk that any given agent represents, the reduction in poor health outcomes that would be possible with a BioWatch detection, and the potential costs of including additional agents in the monitoring program. An expanded panel of agents may add marginal improvements in bioterrorism detection capacity, but it may also increase the possibility of detecting closely related but nonpathogenic organisms, or even a target agent if it is naturally present in the environment. Unless the technology used to signal the presence of a targeted pathogen is highly selective, an expanded panel may increase the number of questionable alerts that must be investigated by local and state health department personnel and potentially reduce confidence in detection signals. To date, positive test results from BioWatch samples have not been related to bioterrorism. Instead, they have been attributed to the natural presence of microbiologic agents in the environment and have not been associated with recognized increases in human disease.
A somewhat similar set of questions can be asked about where BioWatch should be used. Will it be most valuable in major cities and administrative centers where population or high-risk targets are concentrated? Do national security concerns and intelligence information support its use in a limited number of specific localities or in specific sites in a locality? The plans for wider use of BioWatch in high-throughput indoor facilities are likely to result in risk-management and cost-effectiveness assessments that are distinctly different from those for the current outdoor deployment.
What Are the Trade-Offs Among Detection Approaches?
A fourth set of questions might concern trade-offs related to the costs, workforce requirements, and active attention required by a system like BioWatch. With limited financial and personnel resources in state and local health departments to meet day-to-day responsibilities, it may prove challenging to maintain a specialized monitoring system for a low-probability, albeit potentially catastrophic, event. At the federal level as well, there are trade-offs to be made in allocating available resources for the full range of needed biosurveillance activities.
TERMINOLOGY
Biosurveillance
Homeland Security Presidential Directive (HSPD) 21 (The White House, 2007) defines biosurveillance as “the process of active data-gathering with appropriate analysis and interpretation of biosphere data that might relate to disease activity and threats to human or animal health—whether infectious, toxic, metabolic, or otherwise, and regardless of intentional or natural origin—in order to achieve early warning of health threats, early detection of health events, and overall situational awareness of disease activity.” The full scope of biosurveillance as defined in HSPD-21 was beyond the scope of this report, which focuses on activities intended to detect threats to human health specifically from pathogens and biological toxins that might be used in bioterrorism or that might be associated with infectious diseases of public health significance. Detection may occur via means including environmental monitoring, clinical case finding, laboratory testing, or syndromic surveillance. Many of these activities are consistent with the long-standing use of the term “surveillance” to describe the process that public health and national security agencies use to monitor trends in diseases or other conditions as part of public health and national security programs (CDC, 2001b; Buehler, 2008).
The BioWatch Program and BioWatch System
Throughout this report the term “BioWatch program” describes the programmatic activity managed and funded by DHS. In managing the program, DHS works with other federal agencies and state and local partners. The “BioWatch system” refers to the collection of operational components (which are themselves systems) that produce information from air sampling and feed it into a public health decision-making process to determine the appropriate response to a BioWatch Actionable Result (BAR). Thus, the BioWatch system includes the technology to collect and test air samples, the associated laboratory assays, the additional information gathering needed to confirm and characterize an incident, operational guidance, interagency and risk communication, response planning and exercises, and the personnel to support these operations, whether or not these activities at federal, state, or local levels are directly funded by DHS.
For its goal of minimizing casualties in the event of a bioterrorist attack—the focus of this report—the BioWatch system should be seen as part of a public health approach to identifying disease hazards and making decisions regarding action to limit the impact of these hazards. Other perspectives are appropriate to assess the contributions that the BioWatch
system is intended to make in support of national security, law enforcement, and forensic aspects of detecting and responding to a bioterrorist attack.
In addition to DHS’s BioWatch program, the U.S. Postal Service (USPS) and DoD operate their own aerosol monitoring systems. The USPS has deployed the automated Biohazard Detection System (BDS) at more than 200 mail processing centers. The BDS collects air samples from mail sorting equipment and uses genomic testing specifically for the presence of DNA segments associated with B. anthracis (National Association of Letter Carriers, 2008). DoD has installed outdoor air samplers similar to those used in the BioWatch system at selected military bases in the United States. DoD also uses other technologies, such as lidar and the Joint Biological Standoff Detection System, for outdoor monitoring and has installed indoor monitoring systems at certain facilities (DoD, 2007; Mayor et al., 2008). DoD also has worked for many years to develop biodetection technologies to protect against biowarfare threats on the battlefield and in military facilities. The committee received briefings on these systems but does not review them in this report.
Other biodetection tools are being developed and offered in the private sector. For example, commercial vendors are offering a variety of handheld biological detection devices intended for use by first responders. Information about these devices has been compiled for DHS (2007), but systematic testing has not yet been done to establish the reliability and effectiveness of the devices (GAO, 2008b).
The Public Health and Health Care “Systems”
It is common to refer to the public health “system” or the health care “system,” but in the United States these systems are highly decentralized and only very loosely linked. Neither in public health nor in health care is there an overarching national mechanism for unifying or coordinating the disparate, and often competing, entities involved.
Health care is provided by an amalgam of clinicians in individual practice and group settings such as clinics and hospitals. These activities operate as a mix of public, private nonprofit, and for-profit enterprises and are funded by a variety of public and private payers. “Public health” is largely a governmental responsibility, with primary legal responsibility resting with the states, which sometimes delegate this responsibility to local governments. The federal government’s role in public health is extensive, including (but not limited to) leadership in policy development and financial and operational support for research, data collection, and certain services (e.g., vaccine purchase). The organization and operation of public health services is implemented through various configurations of state and local health departments, working with federal agencies, health care providers and organizations, contractors, entities they regulate, and public–private
partnerships. The boundaries between health care and public health services vary and are often vague, with many health departments providing some clinical services and clinicians and health care institutions playing a role in public health functions. In addition, both the health care and public health systems rely on an array of private- and public-sector laboratory services to detect, confirm, and report evidence of infectious disease.
CONSIDERATIONS GUIDING THE COMMITTEE’S WORK
This report focuses on the committee’s assessment of BioWatch and its relation to infectious disease surveillance through the public health and health care systems for detection of bioterrorist attacks. The effectiveness of each of these approaches is considered on its own merits, without an attempt to assess the merits of other aspects of the preparedness efforts of which each is a part. Even though the full range of preparedness concerns is beyond the scope of this study, three observations require specific note because they are inextricably linked to the committee’s assessments:
-
Systems for surveillance and detection of disease threats need to be accompanied by the capability to respond with appropriate public health or medical measures to minimize illness and death.
-
The BioWatch system is designed to detect certain biological agents that could be intentionally released in aerosolized form, and it operates in a limited number of localities. Detecting a bioterrorism event that relies on other routes of exposure or that involves aerosols released in places where BioWatch detectors are not deployed requires other approaches.
-
There is considerable uncertainty about the likelihood and magnitude of a biological attack and, as a result, uncertainty about the risk of an aerosolized release of a pathogen. There is also uncertainty about how this risk compares with risks from other potential forms of bioterrorism or from natural diseases.
Linking Surveillance and Response
Without an effective response capability, good surveillance and detection alone can contribute very little to limiting morbidity and mortality. Therefore, the committee emphasizes, as a fundamental premise, that the capability to effectively deliver public health and health care services, as well as law enforcement and other public services, in response to detected threats is essential. While early warning of an incipient epidemic may have some inherent value, achieving the full benefits of early detection depends on other factors, such as whether exposed people can be provided counter-
measures in time to prevent severe illness and whether additional exposure can be prevented by evacuation, limiting the movement of people into contaminated areas, or sheltering in place. It also depends upon whether the agent causes a communicable illness. Meeting the challenges posed by bioterrorism attacks or other large-scale disease outbreaks requires attention to a range of needs, of which effective surveillance and detection systems are only a limited portion. Indeed, there are serious questions about the current capabilities of the U.S. preparedness architecture and how to measure the effectiveness of current preparations (e.g., Nelson et al., 2007; TFAH, 2008, 2009; WMD Commission, 2008).
BioWatch Is Not Designed to Be Comprehensive
The BioWatch system, as the committee was informed by DHS officials, is specifically designed to detect the presence of certain aerosolized pathogens that have been released in a quantity that has the potential to infect substantial numbers of people in localities where air samplers have been deployed. Although this capacity addresses some high-priority concerns, the committee also recognizes that these concerns account for a circumscribed set of possible high-consequence terrorist scenarios. Because of the nature of the study charge, the committee has not addressed technologies analogous to BioWatch that would be needed to detect other forms of biological terrorism, such as contamination of food or water or environmental exposure to infectious agents distributed by means that BioWatch is not designed or deployed to detect (e.g., the 2001 anthrax letters). Nor is BioWatch designed to accomplish the necessary epidemiologic characterization of disease outbreaks. The health care and public health systems, however, need the capacity to detect and respond both to the health threats posed by the aerosolized pathogens that BioWatch is designed to detect and to the full range of other infectious disease threats. Regardless of how a significant biological threat is detected, the response is likely to require an array of resources, including not only public health and health care but also emergency response and law enforcement.
Given these fundamental differences in scope among different surveillance systems, the committee sought an approach to make comparative assessments. In some cases, the committee made head-to-head comparisons between BioWatch and other modes of surveillance specifically for an aerosol attack, such as with anthrax spores. In other cases, the committee accepted that no direct comparison was appropriate.
Uncertainty About Risk
Both bioterrorism agents and emerging infectious diseases are considered health threats for the United States; that is, they have the potential to
cause harm (IOM, 2003; Blair, 2009). The existence of the BioWatch program bears witness to a perceived threat to the nation from the intentional release of aerosolized biological agents. However, knowledge of the existence of a threat is different from an understanding of the likelihood that specific threat events will occur and the consequences they will produce.
DHS is charged with conducting biennial risk assessments to “provide the basis for risk-informed investments for national strategic biodefense planning while identifying key knowledge gaps and defining critical vulnerabilities” (DHS, 2009c). It has produced Bioterrorism Risk Assessment (BTRA) reports in 2006 and 2008. However, a National Academies report presented several concerns about the approach and methodology used in the 2006 DHS risk assessment (NRC, 2008).
For this report on BioWatch and biosurveillance through the public health and health care systems, the committee was not tasked to evaluate threat or risk information. For this reason, many of the conclusions of this report are couched in terms of a strongly conditioning assumption, such as, “Given that a particular biological agent, in a given quantity, is released at a specific location, how well would various surveillance systems perform?” The probabilities of such assumptions and the associated consequences are combined in the BTRAs to estimate the “risks.” Although risk assessments are not incorporated in the conclusions reached in this report, the committee is very conscious of the importance of understanding risk in evaluating the decisions to actually implement risk-mitigating strategies such as BioWatch and disease surveillance.
RELATED ACTIVITIES
Because of the salience and evolving nature of the nation’s civilian efforts to defend against bioterrorism and other biological threats, other related activities were under way during the course of this study. Two in particular—one by GAO and another by CDC—proceeded largely in parallel with the work of this committee. The concurrent nature of these activities limited the opportunity for the committee to benefit from their findings.
GAO, under Public Law 110-53, Implementing Recommendations of the 9/11 Commission Act of 2007, was charged with preparing a report for Congress on “the state of [f]ederal, [s]tate, local, and tribal government biosurveillance efforts” and making recommendations on integration of biosurveillance systems and the effective use of biosurveillance resources (P.L. 110-53, Sec. 1102). As described to the committee at its first meeting, the GAO has interpreted its task as encompassing all aspects of biosurveillance, including activities related to threats to plant and animal health (Jenkins, 2008). In congressional testimony in July 2008, GAO described the DHS plans to introduce new air sampling technology but provided no
evaluation of those plans or the program as a whole (GAO, 2008a). GAO plans to issue four reports from its review of biosurveillance, with the first two reports expected in summer 2009 (Tapia-Videla, 2009).
In mid-2008, CDC was given responsibility for leading the HHS planning and implementation of “an operational national epidemiologic surveillance system for human health …,” which was called for under HSPD-21, “Public Health and Medical Preparedness” (The White House, 2007). During much of the time the committee was studying the issues and preparing this report, CDC staff were engaged with numerous contributors from other federal agencies, state and local governments, and the private sector to develop a document laying out a national strategy for biosurveillance, including identifying potential enhancements of current systems and capabilities (Sosin, 2008, 2009a). A working document, distributed for comment in December 2008 (CDC, 2008b), identified six strategic priorities: (1) electronic health information exchange, (2) electronic laboratory information exchange, (3) unstructured data, (4) integrated biosurveillance information, (5) global disease detection and collaboration, and (6) the biosurveillance workforce of the future. Guidance for continuing development of the strategy is being provided by CDC’s National Biosurveillance Advisory Subcommittee, which will issue its initial report late in 2009 (Sosin, 2009b).
Also ongoing are local, regional, and national efforts to advance the development and adoption of health information technology, including electronic medical records and health information exchanges. The February 2009 federal economic stimulus package (P.L. 111-5)5 included $2 billion to promote wide deployment of health information technologies. Two HHS advisory committees are to guide the development of information system standards and information technology policy. A health care perspective appears to predominate in much of the work on health information technology, but the need to establish better information linkages between health care and the public health system has been recognized (AHIC, 2008; HITSP, 2008). These information system activities, although not driven by biosurveillance priorities, are clearly crucial in shaping the environment for improving information systems for biosurveillance.
Within the National Academies, two committees are at work on related topics. The Committee to Review the Department of Homeland Security’s Approach to Risk Analysis is to issue a report at the end of 2009 or in early 2010. Its charge is to review how DHS is building capabilities in risk analysis to inform decision making. The study includes an evaluation of the
quality of the current DHS approach to estimating risk for terrorist threats and for natural disasters and to applying those estimates in its management, planning, and resource-allocation activities.
The Committee on Achieving Sustainable Global Capacity for Surveillance and Response to Emerging Diseases of Zoonotic Origin is expected to issue its final report in late 2009. The issues being examined include the causes of and trends in the emergence and spread over the past several decades of agents of zoonotic origin; the risks of animal and human interactions, especially for diseases of international significance such as H5N1 influenza; lessons from previous human and animal health responses to emergent zoonotic diseases; the current state of and gaps in global systems for surveillance of zoonotic infections in human and animal populations; and the appropriate balance between emergency response to threats and sustainable global surveillance capacity.
THE COMMITTEE’S REPORT
This report provides a review and assessment of the effectiveness and costs of surveillance for and detection of disease threats through the BioWatch program and through the U.S. public health and health care systems. The committee presents its findings on the comparative merits of these approaches, examines costs, and describes promising enhancements to strengthen the nation’s capacity to conduct surveillance for major natural and man-made disease threats. As a result of its review, the committee identified various opportunities to further these enhancements, and it recommends actions that DHS, HHS, and others should undertake to help realize them.
REFERENCES
AHIC (American Health Information Community Workgroup). 2008. Population health and clinical care connection: Transition report. September 23. http://www.hhs.gov/healthit/ahic/materials/09_08/pop/transition_report.html (accessed March 6, 2009).
Blair, D.C. 2009. Annual threat assessment of the Intelligence Community for the Senate Select Committee on Intelligence. Unclassified statement for the record, February. Washington, DC: Office of the Director of National Intelligence. http://intelligence.senate.gov/090212/blair.pdf (accessed February 25, 2009).
Buehler, J.W. 2008. Surveillance. In Modern Epidemiology, 3rd ed. Edited by K.J. Rothman, S. Greenland, and T. L. Lash. Philadelphia, PA: Lippincott Williams & Wilkins. Pp. 459–480.
CDC (Centers for Disease Control and Prevention). 2001a. Update: Investigation of bioterrorism-related anthrax and adverse events from antimicrobial prophylaxis. Morbidity and Mortality Weekly Report 50(44):973–976.
CDC. 2001b. Updated guidelines for evaluating public health surveillance systems: Recommendations from the guidelines working group. Morbidity and Mortality Weekly Report 50(RR-13):1–35.
CDC. 2002. Factsheet: Anthrax information for health care providers. http://emergency.cdc.gov/agent/anthrax/anthrax-hcp-factsheet.asp#inhalation (accessed April 7, 2009).
CDC. 2003. Revised U.S. surveillance case definition for severe acute respiratory syndrome (SARS) and update on SARS cases—United States and worldwide, December 2003. Morbidity and Mortality Weekly Report 52(49):1202–1206.
CDC. 2008a. Bioterrorism agents and diseases. http://www.bt.cdc.gov/agent/agentlist-category.asp (accessed December 19, 2008).
CDC. 2008b. National biosurveillance strategy for human health, 2008–2013. Version 1.0. Atlanta, GA: CDC. http://sites.google.com/site/nbshh10/Welcome (accessed April 27, 2009).
CDC. 2009a. Justification of estimates for appropriation committees: FY 2010. http://www.cdc.gov/fmo/topic/Budget%20Information/appropriations_budget_form_pdf/FY2010_CDC_CJ_Final.pdf (accessed July 21, 2009).
CDC. 2009b. Novel H1N1 situation update, June 26, 2009. http://www.cdc.gov/h1n1flu/update.htm (accessed July 1, 2009)
DHS (Department of Homeland Security). 2007. Guide for the selection of biological agent detection equipment for emergency first responders, 2nd ed. Guide 101-06. Washington, DC: DHS. http://www.eeel.nist.gov/oles/Publications/dhs101-06.pdf (accessed August 4, 2009).
DHS. 2009a. BioWatch Gen-3 request for proposal: HSHQDC-09-R-00045. https://www.fbo.gov/download/54e/54e9ae25a4a9d2d39a9e9e836955001f/HSHQDC-09-R-00045_(5-27-2009).pdf (accessed August 5, 2009).
DHS. 2009b. Department of Homeland Security FY 2010 congressional justification budget, http://www.dhs.gov/xlibrary/assets/dhs_congressional_budget_justification_fy2010.pdf (accessed July 28, 2009).
DHS. 2009c. Selected chemical and biological projects. http://www.dhs.gov/xres/programs/gc_1228845015753.shtm (accessed March 6, 2009).
DoD (Department of Defense). 2007. Department of Defense Chemical and Biological Program annual report to Congress. Washington, DC: DoD. http://www.acq.osd.mil/cp/cbdreports/cbdpreporttocongress2007.pdf (accessed April 13, 2009).
Downes, F.P. 2008. One year later––Implementing the biosurveillance requirements of the ‘9/11 Act.’ Testimony before the Subcommittee on Emerging Threats, Cybersecurity, and Science and Technology of the Committee on Homeland Security, U.S. House of Representatives, July 16. Washington, DC. http://homeland.house.gov/SiteDocuments/20080716143630-34598.pdf (accessed August 4, 2009).
FEMA (Federal Emergency Management Agency). 2008. National response framework. http://www.fema.gov/NRF (accessed February 12, 2009).
Franco, C. 2008. Billions for biodefense: Federal agency biodefense funding, FY2008–FY2009. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 6(2):131–146.
GAO (Government Accountability Office). 2004. Emerging infectious diseases: Review of state and federal disease surveillance efforts. GAO-04-877. Washington, DC: GAO. http://www.gao.gov/new.items/d04877.pdf (accessed July 1, 2009).
GAO. 2008a. Biosurveillance: Preliminary observations on Department of Homeland Security’s biosurveillance initiatives. GAO-08-960T. Washington, DC: GAO. http://www.gao.gov/new.items/d08960t.pdf (accessed August 3, 2009).
GAO. 2008b. Homeland security: First responders’ ability to detect and model hazardous releases in urban areas is significantly limited. GAO-08-180. Washington, DC: GAO. http://www.gao.gov/new.items/d08180.pdf (accessed August 3, 2009).
GAO. 2009. Influenza pandemic: Sustaining focus on the nation’s planning and preparedness efforts. GAO-09-334. Washington, DC: GAO. http://www.gao.gov/new.items/d09334.pdf (accessed April 6, 2009).
HHS (Department of Health and Human Services). No date. Pandemics and pandemic threats since 1900. http://www.pandemicflu.gov/general/historicaloverview.html (accessed June 9, 2009).
HHS. 2008. Project Bioshield: Annual report to Congress, August 2006–July 2007. Washington, DC: Office of the Assistant Secretary for Preparedness and Response.
HITSP (Healthcare Information Technology Standards Panel). 2008. HITSP biosurveillance interoperability specification. HITSP/IS02. Version 3.2. http://www.hitsp.org/InteroperabilitySet_Details.aspx?MasterIS=false&PrefixAlpha=1&APrefix=IS&PrefixNumeric=2&ShowISId=452 (accessed April 27, 2009).
Inglesby, T.V., T. O’Toole, D.A. Henderson, J.G. Bartlett, M.S. Ascher, E. Eitzen, A.M. Friedlander, J. Gerberding, J. Hauer, J. Hughes, J. McDade, M.T. Osterholm, G. Parker, T.M. Perl, P.K. Russell, K. Tonat, and the Working Group on Biodefense. 2002. Anthrax as a biological weapon, 2002: Updated recommendations for management. Journal of the American Medical Association 287(17):2236–2252.
IOM (Institute of Medicine). 2003. Microbial threats to health: Emergence, detection, and response. Washington, DC: The National Academies Press.
Jenkins, W.O. 2008. Public comments to the Committee on Effectiveness of National Biosurveillance Systems: BioWatch and the Public Health System, Meeting 1, July 30–31, Washington, DC.
Jernigan, D.B., P.L. Raghunathan, B.P. Bell, R. Brechner, E.A. Bresnitz, J.C. Butler, M. Cetron, M. Cohen, T. Doyle, M. Fischer, C. Greene, K.S. Griffith, J. Guarner, J.L. Hadler, J.A. Hayslett, R. Meyer, L.R. Petersen, M. Phillips, R. Pinner, T. Popovic, C.P. Quinn, J. Reefhuis, D. Reissman, N. Rosenstein, A. Schuchat, W.J. Shieh, L. Siegal, D.L. Swerdlow, F.C. Tenover, M. Traeger, J.W. Ward, I. Weisfuse, S. Wiersma, K. Yeskey, S. Zaki, D.A. Ashford, B.A. Perkins, S. Ostroff, J. Hughes, D. Fleming, J.P. Koplan, J.L. Gerberding, and the National Anthrax Epidemiologic Investigation Team. 2002. Investigation of bioterrorism-related anthrax, United States, 2001: Epidemiologic findings. Emerging Infectious Diseases 8(10):1019–1028.
Lindley, C. 2009. BioWatch actionable result response: 2008 Democratic National Convention, August 28, 2008. Document submitted to the Committee on Effectiveness of National Biosurveillance Systems: BioWatch and the Public Health System, February 19.
Mayor, S.D., P. Benda, C. Murata, and R.J. Danzig. 2008. Lidars: A key component of urban biodefense. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 6(1):45–56.
Mokdad, A.H., J.S. Marks, D.F. Stroup, and J.L. Gerberding. 2004. Actual causes of death in the United States, 2000. Journal of the American Medical Association 291(10):1238–1245.
National Association of Letter Carriers, AFL-CIO. 2008. Safety and Health: USPS Biohazard Detection System (BDS). http://www.nalc.org/depart/safety/USPSBDS.html (accessed July 8, 2009).
Nelson C., N. Lurie, and J. Wasserman. 2007. Assessing public health emergency preparedness: Concepts, tools, and challenges. Annual Review of Public Health 28:1–18.
NRC (National Research Council). 2002. Countering agricultural bioterrorism. Washington, DC: The National Academies Press.
NRC. 2008. Department of Homeland Security bioterrorism risk assessment: A call for change. Washington, DC: The National Academies Press.
O’Toole, T. 2007a. Hearing on bioterrorism preparedness and the role of DHS Chief Medical Officer. Testimony before the U.S. House of Representatives Committee on Appropriations, Subcommittee on Homeland Security, March 29. Washington, DC.
O’Toole, T. 2007b. Six years after anthrax: Are we better prepared to respond to bioterrorism? Testimony before the U.S. Senate Committee on Homeland Security and Governmental Affairs, October 23. Washington, DC.
Price, D. 2008. Opening statement by David Price, Chairman, Subcommittee on Homeland Security, U.S. House of Representatives Committee on Appropriations, April 1, at the Hearing on the Office of Health Affairs, Department of Homeland Security. Washington, DC. http://appropriations.house.gov/pdf/PriceHealthAffairs04-01-08.pdf (accessed April 7, 2008).
Sinclair, R., S.A. Boone, D. Greenberg, P. Keim, and C.P. Gerba. 2008. Persistence of category A select agents in the environment. Applied and Environmental Microbiology 74(3):555–563.
Sosin, D. 2008. National biosurveillance for human health. Presentation to the Committee on Effectiveness of National Biosurveillance Systems: BioWatch and the Public Health System, Meeting 1, July 30–31, Washington, DC.
Sosin, D. 2009a. Enhancing nationwide biosurveillance for human health: Biosurveillance Coordination Unit. Presentation at the Integrated Surveillance Seminar, CDC, Atlanta, GA. http://www2.cdc.gov/ncphi/disss/seminars/archive.asp (accessed March 4, 2009).
Sosin, D. 2009b. RE: two questions for NAS/IOM study. Email to L. Joellenbeck, Committee on Effectiveness of National Biosurveillance Systems: BioWatch and the Public Health System, by D. Sosin, CDC, July 10.
Tapia-Videla, J. 2009. GAO’s Biosurveillance work: Scoping and reporting strategy. Email to L. Joellenbeck, Committee on Effectiveness of National Biosurveillance Systems: BioWatch and the Public Health System, by J. Tapia-Videla, GAO, February 11.
TFAH (Trust for America’s Health). 2008. Ready or not? Protecting the public’s health from diseases, disasters, and bioterrorism. Washington, DC: TFAH. http://healthyamericans. org/assets/files/bioterror-report-2008.pdf (accessed July 17, 2009).
TFAH. 2009. Pandemic flu preparedness: Lessons from the frontlines. Washington, DC: TFAH. http://healthyamericans.org/report/64/pandemic-flu-frontlines (accessed June 4, 2009).
Thompson, W.W., D.K. Shay, E. Weintraub, L. Brammer, N. Cox, L.J. Anderson, and K. Fukuda. 2003. Mortality associated with influenza and respiratory syncytial virus in the United States. Journal of the American Medical Association 289(2):179–186.
Török, T.J., R.V. Tauxe, R.P. Wise, J.R. Livengood, R. Sokolow, S. Mauvais, K.A. Birkness, M.R. Skeels, J.M. Horan, and L.R. Foster. 1997. A large community outbreak of salmonellosis caused by intentional contamination of restaurant salad bars. Journal of the American Medical Association 278(5):389–395.
The White House. 2004. Homeland Security Presidential Directive 10 (HSPD-10): Biodefense for the 21st Century. April 28. Washington, DC. http://www.dhs.gov/xabout/laws/gc_1217605824325.shtm (accessed March 6, 2009).
The White House. 2007. Public health and medical preparedness. Homeland Security Presidential Directive (HSPD) 21, October 18. Washington, DC. http://www.dhs.gov/xabout/laws/gc_1219263961449.shtm (accessed March 6, 2009).
WHO (World Health Organization). 2004. WHO SARS risk assessment and preparedness framework. WHO/CDS/CSR/ARO/2004.2. http://www.who.int/csr/resources/publications/CDS_CSR_ARO_2004_2.pdf (accessed June 8, 2009).
WHO. 2009. Pandemic H1N1 2009–update 56. http://www.who.int/csr/don/2009_07_01a/en/index.html (accessed July 1, 2009).
WMD Commission. 2008. World at risk: The report of the Commission on the Prevention of WMD Proliferation and Terrorism. New York: Vintage Books. http://www.preventwmd.gov/report/ (accessed December 5, 2008).

























