3
Development and Cardiovascular Disease
Chapter 2 reviewed the extent and nature of the burden of cardiovascular disease (CVD) and focused primarily on classically defined individual risk factors that contribute to the global burden of disease. To build on this epidemiological information, it is equally important to understand the relationship of CVD to economic growth and development, including related systemic drivers that contribute to the global burden of CVD, such as demographic change, urbanization, globalization, technological development, and social and cultural norms. This chapter presents conclusions from available evidence and analysis to help further understand the nature and consequences of the problem in low and middle income countries from this broad perspective.
This chapter first offers a discussion of the available evidence on the relationship between stage of economic development and CVD across countries. This is then expanded to a general overview of broad systemic drivers of health that affect trends in CVD and are closely related to economic growth and development—Chapter 5 will describe the drivers with the strongest rationale and evidence for targeted intervention approaches in more detail. The chapter then concludes with a review of the evidence documenting economic impacts of CVD in low and middle income countries, both for countries and for households, highlighting the finding that the burden falls disproportionately on the poor.
ECONOMIC DEVELOPMENT AND CARDIOVASCULAR DISEASE
Unfortunately, the economics of CVD in low and middle income countries is not heavily studied and methods and data are not uniform; as a
result, there is a scattering of estimates that are not comparable. Although more work is needed to truly understand the economics of this pressing global health issue, the totality of the existing evidence makes it clear that now, and increasingly over time, the economic consequences of CVD are significant.
It is widely accepted that health and income are interdependent, but the magnitude of the interaction is more difficult to discern. This is probably because each country has its own unique circumstances that determine how much health it can buy for a given expenditure. The point at which poor health slows economic growth sufficiently to impede development depends on the specific economic conditions. It is therefore difficult to derive general rules. In theory, the health–wealth relationship should be improved if health promotion and disease prevention policies and programs are able to start earlier in a country’s development trajectory. The relationship between health and economic development was carefully reexamined by the Commission on Growth and Development (World Bank Commission on Growth and Development, 2008), which concluded that despite considerable efforts through historical research, cross-sectional analysis, and innovative ways of integrating household factors into cross-country studies that have pushed the methodological envelope, the effects of health investments on economic performance remain inconclusive. The commission also concluded that chronic illness undermines current productivity and is likely to lead to future losses in economic output; however, it did not indicate the magnitude of that economic loss. Thus, not only will economic development alone be insufficient to improve chronic disease outcomes in developing countries, but also the widespread appearance of chronic disease also threatens to deter the economic growth needed in many low income countries.
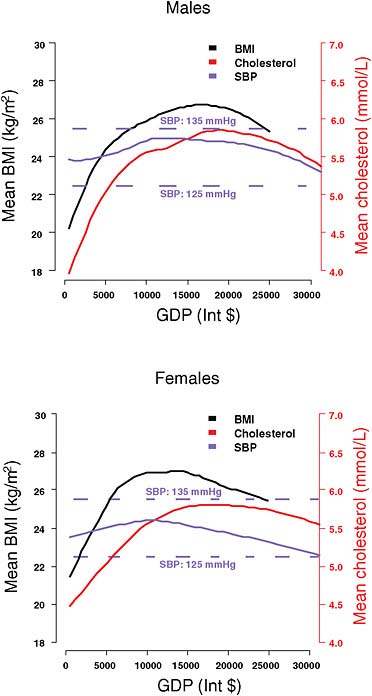
Historical experience in and across countries illustrates how increased wealth and development can be expected to affect cardiovascular health. Two conclusions emerge from the empirical analysis. First, there is no single pattern that characterizes the relationship between economic development and CVD. Indeed, as described in Chapter 2, there is wide variation in age-standardized mortality rates from CVD even among countries in the same income category (WHOSIS, 2009). Second, despite the variability, a general pattern does emerge in which the prevalence of CVD and its risk factors appear to increase and then to decline as countries progress through phases of development. Cross-country evidence suggests that CVD and other chronic disease incidence rises as countries move from lowest income to low-middle income, driven by exposure to lifestyle risks and low access to health services. As countries move further up the income scale to upper-middle and high income status, risks and prevalence decline (Ezzati et al., 2005). As described in Chapter 2, these declines stem from both behavioral changes and better health care. Figure 3.1 shows that with increasing gross
domestic product (GDP) there is an increase and then a decline in the major biological risks for CVD for both men and women.
Economic development is a major factor driving the epidemiological transition. For example, differences in GDP per capita explain almost two-thirds of the differences in female obesity among 37 developing countries (Monteiro et al., 2004). Within countries, CVD is also closely related to income level. CVD and its risks are concentrated among the lowest socioeconomic groups of the more developed (upper-middle and high income) countries, and among middle and high income populations of low-middle income countries (McLaren, 2007; Monteiro et al., 2004). However, even in some countries that have seen little economic progress, a transition to chronic disease can be observed. In part of rural Bangladesh, for example, estimated chronic disease-related mortality went from 8 to 68 percent, while estimated communicable disease mortality dropped from 52 to 11 percent (Ahsan Karar et al., 2009). Because CVD is rising in low and middle income countries and among the lowest socioeconomic groups in high income countries while falling among the wealthy, CVD is one of the few diseases that increases global health inequalities (Becker et al., 2005). Indeed, CVD and its related risks are gradually becoming diseases of the poor, and these divergences are pushing life expectancy in opposite directions in high income and low and middle income countries.
Not only can economic development influence trends in CVD risk, but also CVD can affect economic development. High CVD prevalence has likely depressed economic growth in high income countries in the past. This effect has lessened with recent declines in CVD in high income countries (Becker et al., 2005). CVD and other chronic diseases already have an economic impact in low and middle income countries, as described later in this chapter. The potential to result in a brake on economic growth may emerge as CVD risk rises (Suhrcke and Urban, 2006). Therefore, serious economic concerns remain for developing countries; however, the diminishing negative economic effects of CVD with decreasing prevalence in high income countries suggests that there is potential for risk and disease prevention to protect those countries from more serious economic ramifications.
Conclusion 3.1: In general, CVD risks are rising among low income countries, are highest for middle income developing countries, and then fall off for countries at a more advanced stage of development. This pattern reflects a complex interaction among average per capita income in a country, trends in lifestyle, and other risk factors, and health systems capacity to control CVD. Thus, the challenge facing low income developing countries is to continue to bring down prevalence of infectious diseases while avoiding an overwhelming rise in CVD, especially under conditions of resource limitations. This will require balancing
competing population-level health demands while maintaining relatively low overall health expenditures. Investments in health will also need to be balanced with pressing needs to invest in other social needs and industrial development to produce a positive health–wealth trajectory. The challenge facing middle income developing countries is to reverse or slow the rise in CVD in an affordable and cost-effective manner.
DEVELOPMENT AND SYSTEMIC DRIVERS OF HEALTH
Most of the countries that are now considered developed went through an economic transformation in the early to mid-20th century that was accompanied by major advances in health and longer life expectancy. The catalysts for advances in economic production included the expansion of public sanitation systems, new medical technology, and improved nutrition. Today, however, the relationship between health and economic development is more complex. Key historic indicators of development progress—a relative decline in agrarian society and rise in urban lifestyles, a dominance of manufacturing and service-sector employment, and greater diversity in food and agriculture—also pose risks that threaten to undermine or thwart economic development and negatively affect health, including shifts that increase chronic disease risk.
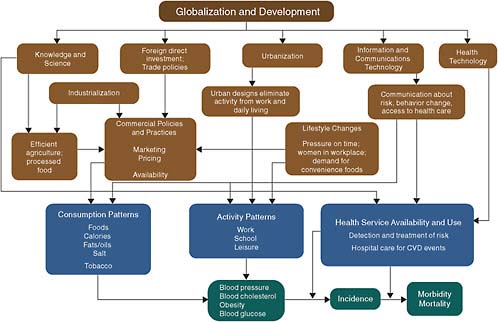
Therefore, related to the strong role that economic development and economic conditions exert on CVD, key systemic drivers—both distal and proximate—have emerged. Systemic drivers here refer to broad processes that ultimately have an effect on classically defined individual risk factors. Distal drivers have long-term impacts across many populations and can be thought of as underlying causes; while proximate drivers are closely tied to specific conditions and periods. Both are influenced by country-specific social, political, and economic factors; yet they may present opportunities to modify the factors leading to increased CVD incidence. These opportunities are discussed in Chapter 5. The broad distal drivers that influence CVD include dynamic demographic conditions such as population aging and urbanization; shifts in agriculture; technology development and adoption; education; cultural and social norms; and the multifarious influences of globalization and increasingly open world markets. These are accompanied by more proximate drivers such as health financing structures, the built environment, and ideology diffusion. This section briefly describes the expected relationship between these drivers and CVD, summarized in Figure 3.2. The drivers with the strongest rationale and evidence for targeted intervention approaches are described in more detail in Chapter 5. The relationships between CVD and other economic conditions—such as inequality and poverty—are described in greater detail later in this chapter.
Dynamic Demographic Conditions
Population Aging
A younger population is generally at lower risk of CVD, and most developing countries have younger populations than developed countries. However, the population median age in developing countries is catching up to that of developed countries. The number of persons worldwide aged 65 years or older is projected to reach more than 690 million by 2012, with 460 million in developing countries (Reddy, 2009). The decline in infectious diseases and nutritional disorders contributes to this transition and enhances the proportional burden of CVD (Reddy and Yusuf, 1998).
Although it is often assumed that age is a risk factor for CVD, in reality, this may be overstated. As discussed in Chapter 2, with age comes cumulative exposure to specific CVD risks as well as to the impact of negative social, educational, and economic factors. For example, the relationship between increasing risk and age with respect to blood pressure has been well described in various populations as they move from low-salt and low-stress environments to cities (Danaei et al., 2009; He and MacGregor, 2009; Iqbal et al., 2008). It may be the accumulation of these risks over time that contributes to increases in CVD rather than age per se (Darnton-Hill et al., 2004).This suggests that aging need not necessarily lead to a greater burden of ill health in the future but rather that by preventing and removing the risks, a significant part of the relationship between CVD and aging may be reduced. In fact, work done by Fries (2005) shows convincingly that in the United States there is evidence that lifelong prevention can yield lower age-specific disease and disability rates.
Urbanization
While many countries still lack those basic amenities that contribute to a large proportion of the infectious disease burden, such as clean water and sanitation, many more people also inhabit urban environments that inhibit human-propelled movement or punish it with soaring rates of road traffic accidents, expose people to highly polluted air, and introduce severe limitations on access to healthy food choices, especially for the poor. The nature of economic production has also changed with the rise of technology-based and other forms of employment that accelerate the transition from rural lifestyles. Occupational health risks—including sedentariness—add to a shift toward chronic disease risk exposures.
Urbanization is perhaps the second most powerful demographic change underway worldwide, second only to population aging in terms of its impact on CVD. The world has recently passed the point where there are more people living in the urban environment than in rural areas
(UNFPA, 2007). The pace of urbanization in the developing world will not slow for decades, and will be concentrated in the poorest—currently the most rural—regions (UNDESA, 2008; Yusuf et al., 2001a). Indeed, it is estimated that developing country populations will be largely urban by 2050 (UNDESA, 2008). In China, for example, the pace of urbanization has been staggering, with more than 170 cities with a population greater than 1 million people and more than 920 million people expected to be living in cities by 2025 (Agence-France Presse, 2008). The consequences of urban living for health in general and CVD more specifically demand far greater attention.
A very simplistic summary of the trends shows that urbanization is generally associated with an increase in tobacco use, obesity, some aspects of an unhealthy diet, and a decline in physical activity (Gajalakshmi et al., 2003; Goyal and Yusuf, 2006; Steyn, 2006; Yang et al., 2008; Yusuf et al., 2001a). These relationships have profound implications for CVD risk. However, concomitant with increased risks come greater access to health care and education—both factors that are associated with reduced CVD risk. On the whole, urban populations are both healthier and wealthier than rural populations. Latin America may be the best example of these dual trends as it has almost completed the journey through the demographic and epidemiological transitions as a consequence of economic growth and urbanization, but displays increasing inequalities in both income and level of education, with adverse impacts on lifestyle and nutritional risks (PAHO, 2007).
As will be discussed in Chapter 5, there are potential opportunities to avoid the negative impacts of urbanization, and possibly to use the growing investment in new city development for health gains, including gains for CVD. However, these opportunities need to be fully grasped, which requires urban designers to be more aware of the need to consider and incorporate CVD prevention and to be more willing to plan accordingly. In this context, recent proposals by Collins and Koplan (2009) about the value of health impact assessments prior to urban development initiatives being undertaken deserves attention. There are examples in the United States and Europe where this approach has been done successfully.
Immigration and Acculturation
Part of demographic change is population migration and acculturation into new social and cultural contexts. Since the 1970s evidence has grown that immigrants to western countries have higher rates of coronary heart disease (CHD) than the rates found in their country of origin. Early studies found that Japanese immigrants to the United States had higher rates of CHD and higher prevalence of several risk factors including dyslipidemia
and hypertension (Kato et al., 1973; Marmot et al., 1975). Subsequent research has found similar increases in CHD compared to that of the population of origin among immigrants from China and South Asia to western countries as well as among migrants who move from rural to urban settings within countries and adopt more “western” lifestyles (Yusuf et al., 2001a, 2001b). Research on indigenous populations within western countries has also found significant increases in rates of CVD and its associated risk factors when they abandon their traditional diets and ways of life (Yusuf et al., 2001b).
When compared to the general population in their new country, research has found that some immigrant groups exhibit higher rates of CVD, while other groups experience lower rates. For example, South Asian immigrants in the United Kingdom and Canada have higher rates of CHD compared to other ethnic groups; however, Chinese immigrants in Canada have markedly lower rates (Yusuf et al., 2001b). In general, research on immigration and acculturation supports the conclusion that the same risk factors are the main drivers of CVD across populations and countries and that it is differences in the exposure to these risks factors that influence rates of CVD in immigrant groups.
Shifts in Agriculture
In the past century, people were just beginning to move off the farms and away from small-scale food production. People were cognizant of what they were eating: if they hadn’t grown it themselves, they knew where it came from. Now, food is a globalized commodity—food exports accounted for 7.1 percent of all merchandise exports globally in 2008 (World Trade Organization, 2009). Food production and consumption have become separated, and governments exert greater influence over what is produced and what it costs, driven in part by a strong agricultural lobby. Consumers in developing as well as developed countries have far greater food choices along some dimensions, but far fewer along others. Food is more often prepared and eaten outside the home. As discussed in Chapter 2, high income country patterns of eating are increasingly available everywhere in the world to those who can afford it. However, developing country populations experience these dietary patterns without the educational levels, medical care, and public health systems that, in developed countries, can somewhat mitigate the risks they pose.
Technology Development and Adoption
Sparked by the discovery of penicillin, which quickly and cheaply cured many of the infectious diseases that formerly led to death at a young age,
a new era in health care and medicine since the past century has focused on devising new treatments and technologies to reduce disease. Indeed, developed countries have benefited relatively more than developing countries from reductions in mortality that required new technological developments, relatively costly change of habits, and expensive surgical interventions. In developing countries, it is transfers of previously available and less expensive health technology and knowledge from developed to developing countries that have reduced mortality from infectious, respiratory, and digestive diseases, congenital anomalies, and perinatal period conditions and helped bring life expectancy closer to the developed country average (Becker et al., 2005). It is not clear to what extent new technologies and expensive interventions of the kind that have been responsible for declines in CVD mortality in rich countries will provide feasible solutions in developing countries. Despite the technological advances being made and the market potential seen in many middle income countries, in many developing country settings there are cost-prohibitive challenges across all types of treatment options, from diagnostic technologies to provision of medication to advanced surgical interventions. It will be necessary to address the obstacles and opportunities associated with each aspect in order to ensure the continued development of affordable, sustainable solutions in low and middle income countries.
Cultural and Social Norms
Health is universally affected by cultural and social norms and behaviors, with wide variation across countries. Cultural food preferences, societal norms for body shape, cultural practices around use of leisure time and physical activity, and gender norms can interact with other risk factors to contribute to high rates of obesity and CVD risk. In Mexico, for example, high levels of consumption of traditional fruit-based sugary drinks contribute to obesity as the population has shifted from rural to urban lifestyles (Barquera et al., 2008). Cultural and social norms are embedded in society but not immutable. Greater globalization of the food supply, from agricultural production techniques to marketing, have altered consumer preferences and behaviors over a relatively brief period. Fiscal and other policies have also been used to rapidly change consumer choices for fats (Zatonski et al., 1998) and tobacco (Jha et al., 2006). Therefore, although CVD risk must be considered in view of cultural and social norms, it is not predetermined by them.
Globalization and CVD
Globalization has been associated with the spread of knowledge and science, telecommunications and other information technologies, and cul-
tural and behavioral adaptations. Globalization is a broad term that sometimes encompasses less regulated domestic and international markets; themselves associated with increased foreign direct investment, expansion of marketing, and wider and more homogeneous consumer choices. Although still a topic that arouses vigorous debate, globalization is generally accepted as having led to substantial improvement in quality of life for millions of people by advancing social and economic modernization. Yet, at the same time, there is legitimate concern and circumstantial evidence that globalization’s unintended consequences can fuel unhealthy consumption and lifestyle behaviors. Striking examples are presented by the spreading ubiquity of a “western” diet (Iqbal et al., 2008) and greater use of tobacco (Shafey et al., 2009), both of which are closely related to higher disposable incomes. While the latter phenomenon unambiguously contributes to CVD and should be addressed by aggressive public policies across agriculture, industrial, and consumer sectors, the former is more complicated. Globalization of food not only provides greater consumer choice, but also it has improved diets for large numbers of previously undernourished people. Thus, in these and other ways, globalization and its related impacts both reduce and create CVD risks. Policy action is required at the global level and through international channels such as trade discussions to, for example, address the expansion of transnational tobacco companies into low and middle income countries. Policy recommendations in international trade are generally beyond the Committee’s technical expertise and therefore, although acknowledged for their potential role in addressing the global epidemic of CVD, are not fully explored in the section on intersectoral policies in this report.
In conclusion, the “healthy growth” of the past in which development was synonymous with better health is now not as easily achieved. Development brings the benefits of higher incomes including, in most countries, higher life expectancy as childhood infectious disease deaths fall. But the modern development process also confronts populations with serious and long-lasting health risks, challenging societies to find alternative organizational, technological, and policy choices. Still-developing countries have the advantage that they have not fully adopted the behaviors and conditions that raise CVD risks, and countries all along the development spectrum have opportunities to use policy tools to create strong economic incentives to reverse the course that was established only very recently, and thereby implement healthier growth. Chapter 5 enumerates a wide range of policy actions that could lead to reduced CVD risks across multiple sectors and spells out health interventions that can achieve better CVD outcomes. However, the effectiveness and cost-effectiveness evidence about the broader steps societies can take to achieve a health-promoting environment remains patchy.
Conclusion 3.2: The drivers of CVD extend beyond the realm of the health sector, and a coordinated approach is required so that policies in non-health sectors of government, especially those involved in agriculture, urban development, transportation, education, and in the private sector can be developed synergistically to promote, or at least not adversely affect, cardiovascular health.
ECONOMIC IMPACTS FROM CVD
Evidence from historical experience in already-developed countries and cross-country analysis of aggregate trends such as that presented earlier in this chapter can be highly informative. However, it is far from predictive, and the rapidity and variability of the emergence of CVD in developing countries discourages excess reliance on general historical patterns. This section synthesizes evidence from a different source of analysis to better understand the relationship between CVD and economics, namely country studies that demonstrate the economic consequences of CVD and CVD risk factors for individuals, households, and countries.
Due to methodological and data disparities, these estimates from country studies are not comparable across studies, but those that include multiple countries do allow differences to be noted in the degree to which CVD affects entire economies. CVD also affects the economic well-being of households and individuals in ways that vary by socioeconomic status, occupation, and other individual characteristics. Households incur several types of economic costs from CVD. Direct costs are both tangible (expenses due to health care costs) and intangible (foregone productivity and earnings). Indirect losses derive from lower savings, less investment in assets, and reduced educational attainment, all due to financial adjustments forced on families from the burden of chronic diseases.
This section begins with a discussion of estimates of macroeconomic effects based on country studies, which will be followed by a synthesis of the available evidence of the microeconomic impacts of CVD. As a guide, Box 3.1 provides a short summary of terms and data conventions from the economics literature as well as issues regarding comparisons across studies and countries.
Macroeconomic Measures of CVD Impacts
Cost-of-Illness Measures of Macroeconomic Impacts
Cost-of-illness analysis considers the loss of national income due to medical expenditures and decreased productivity, otherwise called direct economic costs. In developing countries, a large proportion (more than
half) of direct costs stems from lost productivity. However, as explained in Box 3.1, estimates of lost productivity or earnings may be exaggerated depending on the underlying assumptions about economic conditions (Abegunde et al., 2007).
Estimates of macroeconomic losses due to CVD and other chronic diseases are listed in Table 3.1, with details of the key assumptions. These cost-of-illness studies indicate that CVD and other chronic diseases impose substantial economic costs, even on relatively poor countries in Africa (Kirigia et al., 2009).
Economic Growth Estimates of Macroeconomic Effects
The economic growth method incorporates a broader set of impacts of CVD on the economy compared to the cost-of-illness measures (Abegunde et al., 2007). It models the impact of reduced productivity and earnings due to death and disability on channels of economic activity that create growth, such as savings and investment. Reduced investment shifts the economy to a lower growth path over the long term, resulting in an accumulation of lost economic output. In economic terms, these studies attempt to measure general equilibrium impacts of CVD.
Estimates of macroeconomic losses from the effects of chronic diseases in developing countries range from 0.02 to 6.77 percent of a country’s GDP on an annual basis (Suhrcke et al., 2006). The wide range of estimates is due to both different CVD burdens and different economic conditions. Recently, Abegunde et al. (2007) estimated the effects of four chronic diseases on the economies of 23 countries using an economic growth model. These 23 countries account for approximately 80 percent of the total burden of chronic disease mortality in developing countries. They concluded that $84 billion of economic production will be lost due to heart disease, stroke, and diabetes in 23 high-burden developing countries between 2006 and 2015. Estimates of cumulative GDP loss over 10 years range from $0.15 billion in the Democratic Republic of Congo to $16.68 billion in India. A recent World Bank study of chronic disease in Russia using a dynamic model estimates “massive and growing” economic gains could be achieved if current trends in ill health from chronic diseases and injury are stemmed. The study shows relatively small economic gains from reduced chronic diseases and injuries in 2005 of $105-$324 in GDP per capita; however the economic toll rises to between $2856 and $9243 per capita by 2025 (World Bank Europe and Central Asia Human Development Department, 2005). This starkly illustrates the significant cumulative burden that CVD can have on a country’s development prospects.
|
BOX 3.1 Interpreting Economic Data
|
Social Welfare Measures of Macroeconomic Impacts
Going beyond the effects of CVD on economic flows, the social welfare (or “full-income”) method includes an economic valuation for lives lost due to CVD. Studies using this method typically use a rule of thumb that values human life equivalent to 100 to 200 times average annual wages (Abegunde et al., 2007). This figure is intended to account for a person’s full worth, beyond simply one’s role as a worker. This method arrives at an economic cost of CVD of a larger magnitude than the studies described previously. One recent example (WHO, 2005) estimated 10-year cumulative GDP losses of $2.5 billion for Tanzania and $7.6 billion for Nigeria from major chronic diseases.
|
Conclusion 3.3: The economic impacts of CVD are detrimental at national levels. Foregone economic output stemming from lower productivity and savings can reach several percent of GDP each year, with a significant cumulative effect. The toll is most severely felt in low and low-middle income countries, which can ill afford the lost economic output in light of already insufficient health resources.
Microeconomic Measures of CVD Impacts
The immediate impacts of CVD on households could derive both from expenditures incurred in preventing or treating disease and from lost earnings when work is reduced because of illness or premature mortality. The
TABLE 3.1 Macroeconomic Impacts from CVD and Chronic Diseases, Various Cost-of-Illness Studies
fact that CVD affects people in developing countries at a younger age than in developed countries implies the potential not only for a more widespread national effect on productivity and earnings in developing countries, but also for potentially more dire effects on the long-term welfare of households. Longer-term economic effects on households and individuals can occur when savings are reduced or less is invested in building the earnings potential of adults or children in the family.
Unfortunately, there is little information that measures how CVD affects household-level economic output in developing countries. Based on a review of studies primarily in high income countries, barriers to employment for people with chronic diseases and risk factors are likely to arise from productivity limitations, costs of disability, and in some cases, stigma (Suhrcke et al., 2006). In addition, Suhrcke et al. (2007) reviewed the available literature for Central and Eastern Europe and the Commonwealth of Independent states and found that, generally speaking, the presence of
chronic illness had a negative impact on individual labor productivity (as measured by the wage rate), the likelihood of labor force participation, and in some cases contributed to a significant loss of household income. Chronic illnesses also increased the likelihood that individuals would retire early.
A growing body of evidence from the employer side also demonstrates that productivity is strongly and adversely affected by chronic diseases. Global corporations monitoring the bottom line impacts of worker illhealth, particularly from chronic diseases, are showing dramatic returns on investment of up to $6 in greater productivity for every $1 spent on health promotion for their employees. Their results also show the indirect losses from absenteeism and “presenteeism” far outweigh the direct costs of health care (WEF, 2009). However, all these estimates are derived from particular labor market and economic conditions in different countries and cannot be generalized.
There is more information about how households are affected by and cope with health care expenses in developing countries, although very little is specific to chronic disease. Because poor households are rarely covered by insurance, there are often severe consequences for the entire household when sudden and significant health expenditures, or “health shocks,” occur. Surveys covering 89 percent of the world’s population suggest that 150 million people experience financial disaster due to health care expenses, and 100 million are pushed into poverty (Xu et al., 2007). Much of the burden imparted by these “health shocks” is from the suddenness of payment requirements (McIntyre et al., 2006).
It is less clear how households are affected specifically by CVD health care expenses, which is largely comprised of the long-term costs of drugs, routine doctors’ visits, and preplanned procedures rather than acute, short-term spending. In Vietnam, where out-of-pocket expenditures constituted 84 percent of all health care spending in 1998, catastrophic spending (defined as an expenditure that exceeds 10 to 40 percent of a household’s capacity to pay) was dominated by communicable disease needs. One reason may be that high costs of chronic disease care prevent lower-income groups from accessing treatment (Thuan et al., 2006). However, CVD events can also result in “catastrophic” health costs. Seventy-one percent of hospitalized Chinese stroke survivors experienced catastrophic financial impacts (defined as out-of-pocket health expenses in the 3 months after stroke that meet or exceed 30 percent of reported household income). Those without health insurance were hit particularly hard. Out-of-pocket expenses from stroke pushed 37 percent of patients and their families below the poverty line; 62 percent of those without insurance were pushed into poverty (Heeley et al., 2009).
Households employ a variety of methods to cope with these expenses, from dipping into savings accounts, to increasing the number of earners in
the family, to selling assets. In general, however, poor families have little flexibility to draw on savings to finance health needs. More often, they reduce basic consumption, sell assets that form the basis of their livelihood, and go into debt (McIntyre et al., 2006). Across 15 countries in Africa, 50 percent of households that had a hospitalized family member turned to borrowing and selling assets to pay for health expenditures. In most of the countries, inpatient expenses were more likely to cause distress selling of assets and borrowing than outpatient and routine health care by both rich and poor households, although the behavior was more predominant among the poor (Leive et al., 2008). In India, the risk of distress borrowing and distress selling increases significantly for hospitalized patients if they are smokers or even just belong to households with a member who smokes or drinks (Bonu et al., 2005; Suhrcke et al., 2006). In Burkina Faso, when a household member has a chronic illness, the probability of catastrophic consequences increased by 3.3- to 7.8-fold (Su et al., 2006; Suhrcke et al., 2006).
A further household burden is the direct expense of harmful lifestyle behaviors related to CVD risk. Many households experience dramatic shifts in spending and forgo other expenditures in order to buy tobacco and alcohol, two major risk factors for CVD. In India, for example, households that consumed tobacco had lower consumption of milk, education, clean fuel, and entertainment. These households also had lower per capita nutritional intake compared to tobacco-free households (Bump et al., 2009; John, 2008). In a sample of low income workers in Eastern China, smokers spent an average 11 percent of personal monthly income on tobacco and reported foregone savings and foregone consumption of health care and major household goods compared to non-smokers (Bump et al., 2009; Hesketh et al., 2007). In another study in rural China, tobacco spending negatively affected spending on health, education, farming equipment, seeds, savings, and insurance. For every 100 yuan spent on tobacco there was an associated decline in spending on education by 30 yuan, medical care by 15 yuan, farming by 14 yuan, and food by 10 yuan (Suhrcke et al., 2006; Wang et al., 2006). Frequently, alcohol expenditures increase hand-in-hand with tobacco expenditures. Families in Delhi, India, that had at least one member that consumed three or more drinks per week spent almost 14 times more on alcohol each month (resulting in fewer financial resources for food, education, and daily consumables) and more were in debt, when compared to families with no member consuming more than one drink (Saxena et al., 2003; Suhrcke et al., 2006).
In conclusion, the economic burden of CVD in developing countries is currently borne most directly by patients and their families, either through out-of-pocket expenses that reduce their provision of basic needs, or through reduced productivity and earnings. By contrast, in middle income
and high income countries where social and private insurance is available to finance health expenses, the financial costs of CVD are spread more widely.
Social Inequalities and CVD
In addition to the effects of CVD on household-level economic status, there is strong evidence that social inequalities contribute to CVD mortality and incidence. Thus, poverty plays a role both as a risk factor and as a consequence of CVD. Poverty, as a contributing factor to CVD, is related to the lack of access to health care and health information among the poor as well as exposure to multiple risk factors that increase CVD risk. Further, several studies have highlighted the effects of social and economic factors on health even when those factors are not directly related to major risks and specific treatments (CSDH, 2008).
In Brazil, for instance, the prevalence of hypertension was consistently and dramatically higher (30 to 130 percent higher) among the less educated, those with lowest income, and Afro-Brazilians. The poor had a 1.2 relative risk of dying from CVD compared to the wealthy (World Bank, 2005a). Demographic and Health Surveys from seven African countries show a 35 percent average increase in overweight and obesity between the early 1990s and 2000s, with the largest increase among the poor. The almost 50 percent rise in overweight and obesity among poor women is attributed to changing nutritional habits and urban lifestyles (Ziraba et al., 2009).
The income gradient of CVD in low and middle income countries mirrors that which has already taken place in developed countries. For example, in Scotland, a six-fold differential in CHD mortality is seen between the poorest and most affluent groups aged 35 to 44 years (O’Flaherty et al., 2009). The major causes for the social class differentials were related to unfavorable trends in risk factors, mainly related to tobacco use and poor diet. Similar findings have been reported for the United States, United Kingdom, Australia, and across Western Europe, where racial and ethnic differences in prevalence are also apparent (Mackenbach et al., 2003; Wang and Beydoun, 2007).
These factors of tobacco use, poor diet, and unequal access to care can explain the tendency for CVD to become more concentrated among the poor and near-poor within low and middle income countries. One reason worth highlighting is the transition to a more energy-dense diet. In addition to the trends in production and consumption related to the nutrition transition that were described in Chapter 2, global prices of edible oils, animal-based products, and sweeteners have declined for the past 20 years. But even while improving overall caloric and protein intake, the poor are now more likely to consume diets heavy in fats, salt, and sugar. In middle income
countries, the poor are also reducing physical activity while consuming additional calories (Drewnowski and Darmon, 2005; Popkin, 2003). Government policies often play a role, directly and indirectly, in subsidizing overconsumption of energy-dense foods. In Egypt, where more than two-thirds of women and half of men are overweight or obese, food subsidies encourage consumption of energy-dense foods (Asfaw, 2006). However, both government food policies and nutrition conditions among the poor are highly country-specific and should be examined on that basis.
Conclusion 3.4: There is growing evidence that CVD and its risk factors affect the poor within and across countries, both as a cause and as a consequence of poverty. In most countries, CVD hits hardest among the poor, who have greater risk-factor exposure, tend to be uninsured, and have less financial resilience to cope with the costs of disease management.
One promising way to stem this increasing burden on the poor in low and middle income countries may be through programs that are specifically tailored and targeted to reach the poor (Gwatkin et al., 2005). Programs already targeted to the lowest income population, such as those to reduce undernutrition in children and for the chronic management of infectious diseases, offer opportunities to ensure an early healthy nutritional start for children and to integrate cardiovascular health promotion and disease prevention.
CONCLUSION
CVD risks arise on the path to an advanced stage of economic development, driven in part by a range of development-related factors such as population aging and urbanization; shifts in agriculture; and the multifarious influences of globalization. CVD can affect the entire economy of a developing nation. Disability, early mortality, and direct health expenditures can divert resources from savings, investment, and other productive uses, affecting economic well-being at the household level and growth potential at the national level. Therefore, developing countries need to maneuver diligently and carefully to avoid cementing in place long-term roadblocks to healthy economic progress.
The pattern of rising CVD risks with development reflects a complex interaction among average per capita income in a country, trends in lifestyle and other risk factors, and health systems capacity to control CVD. Developing countries at different stages of development face different challenges in choosing public health strategies to reduce the burden of CVD. The challenge facing low income developing countries is to continue to bring down
prevalence of infectious diseases while avoiding an overwhelming rise in CVD, especially under conditions of resource limitations. This will require balancing competing population-level health demands while maintaining relatively low overall health expenditures. Investments in health will also need to be balanced with pressing needs to invest in other social needs and industrial development. The challenge facing middle income developing countries is to reverse or slow the rise in CVD in an affordable and cost-effective manner.
Although still not fully understood, the complex interrelationships in which economic development can contribute to and also be affected by the accelerating rates of inadequately addressed CVD and related chronic diseases in low and middle income countries supports the need for both urgent and carefully planned actions.
REFERENCES
Abegunde, D. O., C. D. Mathers, T. Adam, M. Ortegon, and K. Strong. 2007. The burden and costs of chronic diseases in low-income and middle-income countries. Lancet 370(9603):1929-1938.
Agence-France Presse. 2008. China’s urban problem. http://news.asiaone.com/News/Latest%2BNews/Asia/Story/A1Story20081218-108758.html (accessed December 9, 2009).
Ahsan Karar, Z., N. Alam, and P. Kim Streatfield. 2009. Epidemiological transition in rural Bangladesh, 1986-2006. Global Health Action June 2009(2).
Asfaw, A. 2006. Do government food prices affect the prevalence of obesity? Empirical evidence from Egypt. World Development 35(4):687-701.
Barquera, S., L. Hernandez-Barrera, M. L. Tolentino, J. Espinosa, S. W. Ng, J. A. Rivera, and B. M. Popkin. 2008. Energy intake from beverages is increasing among Mexican adolescents and adults. Journal of Nutrition 138(12):2454-2461.
Becker, G. S., T. J. Philipson, and R. R. Soares. 2005. The quantity and quality of life and the evolution of world inequality. American Economic Review 95(1):277-291.
Bonu, S., M. Rani, D. H. Peters, P. Jha, and S. N. Nguyen. 2005. Does use of tobacco or alcohol contribute to impoverishment from hospitalization costs in India? Health Policy and Planning 20(1):41-49.
Bump, J. B., M. R. Reich, O. Adeyi, and S. Khetrapal. 2009. Towards a political economy of tobacco control in low- and middle-income countries. Washington, DC: World Bank.
Collins, J., and J. P. Koplan. 2009. Health impact assessment: A step toward health in all policies. Journal of the American Medical Association 302(3):315-317.
CSDH (WHO Commission on Social Determinants of Health). 2008. Closing the gap in a generation: Health equity through action on the social determinants of health. Final report of the commission on social determinants of health. Geneva: World Health Organization.
Danaei, G., E. L. Ding, D. Mozaffarian, B. Taylor, J. R. Rehm, C. J. L. Murray, and M. Ezzati. 2009. The preventable causes of death in the United States: Comparative risk assessment of dietary, lifestyle, and metabolic risk factors. PLoS Med 6(4):e1000058.
Darnton-Hill, I., C. Nishida, and W. P. T. James. 2004. A life course approach to diet, nutrition and the prevention of chronic diseases. Public Health Nutrition 7(1 A):101-121.
Drewnowski, A., and N. Darmon. 2005. Food choices and diet costs: An economic analysis. Journal of Nutrition 135(4):900-904.
Ezzati, M., S. Vander Hoorn, C. M. Lawes, R. Leach, W. P. James, A. D. Lopez, A. Rodgers, and C. J. Murray. 2005. Rethinking the “Diseases of affluence” paradigm: Global patterns of nutritional risks in relation to economic development. PLoS Medicine 2(5): e133.
Finkelstein, E. A., C. J. Ruhm, and K. M. Kosa. 2005. Economic causes and consequences of obesity. Annual Review of Public Health 26:239-257.
Fries, J. F. 2005. Frailty, heart disease, and stroke: The compression of morbidity paradigm. American Journal of Preventive Medicine 29(5 Suppl 1):164-168.
Gajalakshmi, V., R. Peto, T. S. Kanaka, P. Jha. 2003. Smoking and mortality from tuberculosis and other diseases in India: Retrospective study of 43000 adult male deaths and 35000 controls. Lancet 362(9383):507-515.
Goyal, A., and S. Yusuf. 2006. The burden of cardiovascular disease in the Indian subcontinent. Indian Journal of Medical Research 124(3):235-244.
Gwatkin, D. R., A. Wagstaff, A. Yazbeck, J. Qamruddin, H. Waters, M. Grabowsky, N. Farrell, J. Chimumbwa, T. Nobiya, A. Wolkon, J. Selanikio, D. Montagu, N. Prata, M. Campbell, J. Walsh, S. Orero, M. Thiede, N. Palmer, S. Mbatsha, A. T. M. I. Anwar, J. Killewo, M. Chowdhury, S. Dasgupta, J. B. Schwartz, I. Bhushan, M. K. Ranson, P. Joshi, M. Shah, Y. Shaikh, D. Peters, K. Rao, G. N. V. Ramana, A. Malhotra, S. Mathur, R. Pande, E. Roca, L. Gasparini, M. Panadeiros, A. Barros, C. Victora, J. Cesar, N. Neumann, A. Bertoldi, and M. Valdivia. 2005. Reaching the poor with health, nutrition, and population services: What works, what doesn’t, and why. Washington, DC: World Bank.
He, F. J., and G. A. MacGregor. 2009. A comprehensive review on salt and health and current experience of worldwide salt reduction programmes. Journal of Human Hypertension 23(6):363-384.
Heeley, E., C. S. Anderson, Y. Huang, S. Jan, Y. Li, M. Liu, J. Sun, E. Xu, Y. Wu, Q. Yang, J. Zhang, S. Zhang, and J. Wang. 2009. Role of health insurance in averting economic hardship in families after acute stroke in China. Stroke 40(6):2149-256.
Hesketh, T., L. Lu, Y. X. Jun, and W. H. Mei. 2007. Smoking, cessation and expenditure in low income Chinese: Cross sectional survey. BMC Public Health 7:29.
IOM (Institute of Medicine). 2010. Mitigating the nutritional impacts of the global food price crisis. Washington, DC: The National Academies Press.
Iqbal, R., S. Anand, S. Ounpuu, S. Islam, X. Zhang, S. Rangarajan, J. Chifamba, A. Al-Hinai, M. Keltai, and S. Yusuf. 2008. Dietary patterns and the risk of acute myocardial infarction in 52 countries: Results of the INTERHEART study. Circulation 118(19):1929-1937.
Jha, P., F. J. Chaloupka, M. Corrao, and B. Jacob. 2006. Reducing the burden of smoking world-wide: Effectiveness of interventions and their coverage. Drug and Alcohol Review 25(6):597-609.
John, R. M. 2008. Crowding out effect of tobacco expenditure and its implications on household resource allocation in India. Social Science and Medicine 66(6):1356-1367.
Kato, H., J. Tillotson, and M. Z. Nichaman. 1973. Epidemiologic studies of coronary heart disease and stroke in Japanese men living in Japan, Hawaii and California: Serum lipids and diet. American Journal of Epidemiology 97(6):372-385.
Kirigia, J. M., H. B. Sambo, L. G. Sambo, and S. P. Barry. 2009. Economic burden of diabetes mellitus in the WHO African region. BMC International Health and Human Rights 9(1):6.
Leive, A., K. Xu, A. Leive, and K. Xu. 2008. Coping with out-of-pocket health payments: Empirical evidence from 15 African countries. Bulletin of the World Health Organization 86(11):849-856.
Mackenbach, J. P., V. Bos, O. Andersen, M. Cardano, G. Costa, S. Harding, A. Reid, O. Hemstrom, T. Valkonen, and A. E. Kunst. 2003. Widening socioeconomic inequalities in mortality in six Western European countries. International Journal of Epidemiology 32:830-837.
Marmot, M. G., S. L. Syme, and A. Kagan. 1975. Epidemiologic studies of coronary heart disease and stroke in Japanese men living in Japan, Hawaii and California: Prevalence of coronary and hypertensive heart disease and associated risk factors. American Journal of Epidemiology 102(6):514-525.
McIntyre, D., M. Thiede, G. Dahlgren, M. Whitehead, 2006. What are the economic consequences for households of illness and of paying for health care in low- and middle-income country contexts? Social Science and Medicine 62(4):858-865.
McLaren, L. 2007. Socioeconomic status and obesity. Epidemiologic Reviews 29:29-48.
Monteiro, C. A., W. L. Conde, B. Lu, and B. M. Popkin. 2004. Obesity and inequities in health in the developing world. International Journal of Obesity 28(9):1181-1186.
O’Flaherty, M., J. Bishop, A. Redpath, T. McLaughlin, D. Murphy, J. Chalmers, S. Capewell. 2009. Coronary heart disease mortality among young adults in Scotland in relation to social inequalities: Time trend study. British Medical Journal 339:b2613.
PAHO (Pan American Health Organization). 2007. Regional strategy and plan of action on an integrated approach to the prevention and control of chronic diseases. Washington, DC: Pan American Health Organization.
Popkin, B. M. 2003. Dynamics of the nutrition transition and its implications for the developing world. Forum Nutrition 56:262-264.
Reddy, K. S. 2009. Global perspectives on cardiovascular diseases. In Evidence based cardiology. 2nd ed. Edited by S. Yusuf, J. A. Caitns, A. J. Camm, E. L. Fallen and B. J. Gersh. London: BMJ Books.
Reddy, K. S., and S. Yusuf. 1998. Emerging epidemic of cardiovascular disease in developing countries. Circulation 97(6):596-601.
Saxena, S., R. Sharma, and P. K. Maulik. 2003. Impact of alcohol use on poor families: A study from north India. Journal of Substance Use 8:78-84.
Shafey, O., M. Eriksen, H. Ross, and J. Mackay. 2009. The tobacco atlas. 3rd ed. Atlanta: American Cancer Society.
Steyn, N. P., D. Bradshaw, R. Norman, J. Joubert, M. Schneider, K. Steyn. 2006. Dietary changes and the health transition in South Africa: Implications for health policy. Cape Town: South African Medical Research Council.
Su, T. T., B. Kouyate, and S. Flessa. 2006. Catastrophic household expenditure for health care in a low-income society: A study from Nouna district, Burkina Faso. Bulletin of the World Health Organization 84(1):21-27.
Suhrcke, M., and D. M. Urban. 2006. Are cardiovascular diseases bad for economic growth? http:/ssrn.com/paper=949412 (accessed February 5, 2010).
Suhrcke, M., and L. Rocco. 2008 (unpublished). Macroeconomics consequences of noncommunicable diseases at the individual or household level, with a focus on labor market outcomes.
Suhrcke, M., R. A. Nugent, D. Stuckler, and L. Rocco. 2006. Chronic disease: An economic perspective. London: Oxford Health Alliance.
Suhrcke, M., L. Rocco, M. McKee, WHO Regional Office for Europe, and European Observatory on Health Systems and Policies. 2007. Health: A vital investment for economic development in Eastern Europe and central Asia. Copenhagen: WHO Regional Office for Europe.
Thuan, N. T., C. Lofgren, N. T. Chuc, U. Janlert, L. Lindholm. 2006. Household out-of-pocket payments for illness: Evidence from Vietnam. BMC Public Health 6:283.
UNDESA (United Nations Department of Economic and Social Affairs). 2008. World urbanization prospects: The 2007 update. Geneva: United Nations.
UNFPA (United Nations Fund for Population Activities). 2007. State of world population 2007. New York: UNFPA.
Wang, H., J. L. Sindelar, and S. H. Busch. 2006. The impact of tobacco expenditure on household consumption patterns in rural China. Social Science and Medicine 62(6):1414-1426.
Wang, Y., and M. A. Beydoun. 2007. The obesity epidemic in the United States—gender, age, socioeconomic, racial/ethnic, and geographic characteristics: A systematic review and meta-regression analysis. Epidemiologic Reviews 29:6-28.
WEF (World Economic Forum). 2009. Employee health as a strategic imperative: Report of the governors meeting of the consumer industries. Geneva: World Economic Forum.
WHO (World Health Organization). 2005. Preventing chronic diseases: A vital investment. Geneva: World Health Organization.
WHOSIS (World Health Organization Statistical Information System). World Health Statistics. 2009. Geneva: World Health Organization.
World Bank. 2005a. Brazil: Addressing the challenge of non-communicable diseases in Brazil. Washington, DC: World Bank.
World Bank. 2005b. World development report overview 2006: Equity and development. Washington, DC: World Bank.
World Bank Commission on Growth and Development. 2008. The growth report: Strategies for sustained growth and inclusive development. Washington, DC: World Bank.
World Bank Europe and Central Asia Human Development Department. 2005. Dying too young: Addressing premature mortality and ill health due to non-communicable diseases and injuries in the Russian Federation. Washington, DC: World Bank.
World Trade Organization. 2009. International trade statistics 2009. Geneva: World Trade Organization.
Xu, K., D. B. Evans, G. Carrin, A. M. Aguilar-Rivera, P. Musgrove, T. Evans. 2007. Protecting households from catastrophic health spending. Health Affairs 26(4):972-983.
Yang, G., L. Kong, W. Zhao, X. Wan, Y. Zhai, L. C. Chen, and J. P. Koplan. 2008. Emergence of chronic non-communicable diseases in China. Lancet 372(9650):1697-1705.
Yusuf, S., S. Reddy, S. Ounpuu, and S. Anand. 2001a. Global burden of cardiovascular diseases: Part I: General considerations, the epidemiologic transition, risk factors, and impact of urbanization. Circulation 104(22):2746-2753.
Yusuf, S., S. Reddy, S. Ounpuu, and S. Anand. 2001b. Global burden of cardiovascular diseases: Part II: Variations in cardiovascular disease by specific ethnic groups and geographic regions and prevention strategies. Circulation 104(23):2855-2864.
Zatonski, W. A., A. J. McMichael, and J. W. Powles. 1998. Ecological study of reasons for sharp decline in mortality from ischaemic heart disease in Poland since 1991. British Medical Journal 316(7137):1047-1051.
Zhao, W., Y. Zhai, J. Hu, J. Wang, Z. Yang, L. Kong, and C. Chen. 2008. Economic burdenEconomic burden of obesity-related chronic diseases in mainland China. Obesity Reviews 9(1):62-67.
Ziraba, A. K., J. C. Fotso, and R. Ochako. 2009. Overweight and obesity in urban Africa: A problem of the rich or the poor? BMC Public Health 9:465.