3
The Burden of HIV/AIDS: Implications for U.S. Interests
|
Key Findings
|
The HIV/AIDS epidemic, first identified in 1981, remains among the greatest threats to global health, with an epicenter in the acutely affected countries of east and southern Africa (Independent Task Force Report No. 56, 2006; UNAIDS and WHO, 2009). Life-saving antiretroviral therapy (ART) was, until 2000, not accessible to those most in need because they were poor and lived in developing countries. With the turn of the 21st century, global attitudes on this morally intolerable situation began to shift, and the International AIDS Conference in Durban in July 2000 marked a turning point with a powerful call to the international community to take responsibility for mounting an urgent response.
The United States responded and, with the launch of the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) in 2003, established itself as a global leader in the fight against HIV/AIDS. Through PEPFAR and support for the Global Fund to Fight AIDS, Tuberculosis and Malaria, the United States helped galvanize an extraordinary global response to a single disease and mobilize donor and private-sector resources on an unprecedented scale to respond to the costly but critical task of addressing the HIV/AIDS crisis. Perhaps most important, this response demonstrated, in the face of considerable skepticism at the time, that dramatically expanding access to HIV/AIDS treatment was possible even in the world’s most resource-constrained settings (IOM, 2007). The U.S. campaign against HIV/AIDS has had a historic impact and is considered among the most significant and enduring achievements of the George W. Bush administration (Stolberg, 2008).
Yet despite its substantial immediate impact, this emergency response has failed to halt or reverse the HIV/AIDS epidemic in Africa. Indeed, as outlined in the previous chapter and Appendix A, the burden of HIV/AIDS in Africa will continue to grow. As a result of continued high HIV incidence rates, the need for lifelong HIV/AIDS treatment has grown more rapidly than the ability to initiate new patients on ART. This growing burden will place ever higher demands on health care services, including an increasing number of ambulatory and hospitalized patients requiring HIV/AIDS care, an increasing number of patients requiring ART, a substantial need for additional health care workers, and a continued rise in financial and other resource requirements.
In the context of this growing burden, the United States and the global community will face significant challenges in sustaining and expanding commitments to combating HIV/AIDS in Africa. In the United States, the effects of a historic global financial crisis and a domestic deficit approaching $2 trillion will likely drive greater congressional scrutiny of spending on foreign assistance (Garrett, 2010). Moreover, the success of the U.S. HIV/AIDS effort has, ironically, increased attention to other African health challenges, which may drive competition in resource allocation among disease and health priorities. Beyond health, U.S. interests in Africa have expanded dramatically in the last decade, resulting in growing recognition of new challenges that confront development in such areas as food security, climate change, and unemployment and creating
increased competition for scarce development assistance. And as the United States vies for influence in an increasingly competitive international context, it will seek new forms of engagement in Africa that provide greater political and economic leverage than traditional development and humanitarian assistance (Independent Task Force Report No. 56, 2006).
As new HIV infections continue to outstrip the world’s willingness to provide ART to those in need, the costs of treatment alone will consume ever larger proportions of available resources. The combination of competing health and development demands, the rising cost burden of HIV/AIDS treatment, and continued resource constraints will force difficult choices and trade-offs for U.S. policy makers, made more politically sensitive by heightened expectations around U.S. commitments. As the largest single contributor to global HIV/AIDS resource flows to date, the United States will need to manage these choices and trade-offs in a way that does not compromise the global achievements in HIV/AIDS; advances U.S. interests; and strengthens current and future global capacities to respond to HIV/AIDS, as well as other global health challenges.
One way for the United States to accomplish these goals while addressing its own fiscal concerns is to transition to a model for long-term sustainability. This model would be one of shared responsibility with African partner states and the broader international community. By looking to African partner states to assume increasing responsibility for leadership, management, and investment of resources in HIV/AIDS, the United States would be promoting a future of self-reliance and self-sustainability. Under this shared-responsibility model, the United States would assist African partner states in developing the leadership, academic, medical, research, and other capacities necessary to assume that responsibility effectively. Implementation of this model would necessitate greater accountability and transparency in the investments being made by each African partner state. Similarly, the United States would need to take an approach grounded in realism, setting ambitious but realistic objectives for the next 10 to 15 years and placing an urgent and consistent focus on prevention of new HIV infections.
This chapter begins by describing the U.S. contributions to the global HIV/AIDS response. It next details the implications of the African HIV/AIDS burden for a variety of U.S. interests, including diplomacy, the private sector, research and academia, and foundations. The chapter then assesses the policy challenges that lie ahead for the United States in addressing these impacts and offers recommendations for moving forward in the fight against HIV/AIDS in Africa.
U.S. CONTRIBUTIONS TO THE GLOBAL HIV/AIDS RESPONSE
While it is important to be cognizant of the policy challenges that lie ahead, it is also important to acknowledge the significant accomplishments that have resulted from U.S. leadership in the global response to HIV/AIDS. In less than a
decade, U.S. engagement in combating the pandemic has had a dramatic impact, particularly in Africa, the predominant focus of PEPFAR’s initial phase (Independent Task Force Report No. 56, 2006; UNAIDS and WHO, 2009). Beyond the immediate human impacts, U.S. leadership has stimulated the global community and created new awareness of and support for global health among U.S. domestic actors and institutions. Finally, the U.S. response has built new partnerships in Africa and in the broader international community that ultimately strengthen the nation’s standing in an increasingly competitive, multipolar global political environment (Pew Research Center, 2008; Ray, 2008).
The human impact of U.S. investments in HIV/AIDS has been profound. At the end of 2003, the year President Bush announced the PEPFAR initiative, an estimated 100,000 people, or 2 percent of those in need, were receiving ART in Africa (WHO et al., 2009). As of September 2009, more than 2.4 million people, approximately 20 percent of those in need, had access to life-saving ART because of direct bilateral PEPFAR support (PEPFAR, 2009b). Figure 3-1 shows the cumulative years of life gained through 2009 as a result of PEPFAR support for ART.
An additional 1.9 million individuals in Africa receive treatment through programs supported by the Global Fund to Fight AIDS, Tuberculosis and Malaria (Global Fund, 2010a), to which the United States is the largest national contributor. Figure 3-2 shows that 3.7 million people in low- and middle-income countries had been supported by PEPFAR and the Global Fund as of September
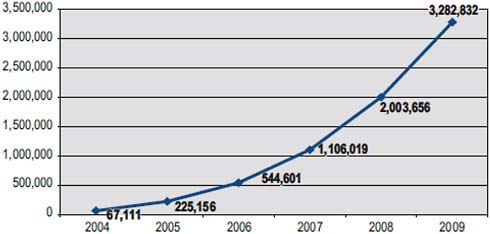
FIGURE 3-1 Cumulative years of life gained through 2009 as a result of PEPFAR support for antiretroviral therapy.
SOURCE: PEPFAR, 2009a.
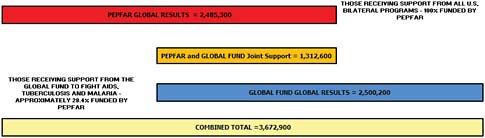
FIGURE 3-2 People receiving treatment with U.S. bilateral and multilateral support as of September 2009.
SOURCE: PEPFAR, 2010.
2009. In 2009, 6.4 million pregnant women in Africa received antenatal HIV counseling and testing because of PEPFAR, and 504,800 received antiretroviral (ARV) prophylaxis (PEPFAR, 2010). In 2009, PEPFAR gave direct HIV/AIDS and tuberculosis care and support to 6.9 million people living with HIV/AIDS and supported 3.5 million orphans and vulnerable children in Africa (PEPFAR, 2010).
At the same time, U.S. investments in responding to HIV/AIDS have advanced U.S. interests well beyond the pandemic and laid the foundation for a more comprehensive approach to public health and broader global support. U.S. leadership contributed directly to the formation of new international initiatives such as the Global Fund, with the United States providing an early $200 million in seed money, investing considerable attention in the early formation and structure of the fund (Summers, 2002) and remaining the largest single contributor to the fund since its inception. U.S. leadership has challenged other international donors to expand their investments in HIV/AIDS (see Figure 3-3) and led to the creation of numerous new public–private partnerships in the global HIV/AIDS response.
Within the United States, the PEPFAR initiative created greater public awareness of global HIV/AIDS and support for foreign aid. Beginning with the January 2002 State of the Union Address in which he first outlined the PEPFAR initiative, President Bush made combating HIV/AIDS a signature element of his foreign assistance strategy, brought home to the public through multiple trips by the President and the First Lady to African and non-African PEPFAR countries and numerous public statements and White House ceremonies highlighting the accomplishments of the initiative. Congressional travel, public speeches, and hearings on the initiative further raised the profile of global HIV/AIDS, and the focus within the U.S. government on HIV/AIDS helped fuel greater media coverage of the pandemic and the U.S. response. PEPFAR, which was the largest component of a near tripling of foreign assistance to Africa during the Bush administration (Fletcher, 2006), also garnered a robust bipartisan consensus within Congress in support of U.S. leadership; instigated a growing interest and activism among U.S.
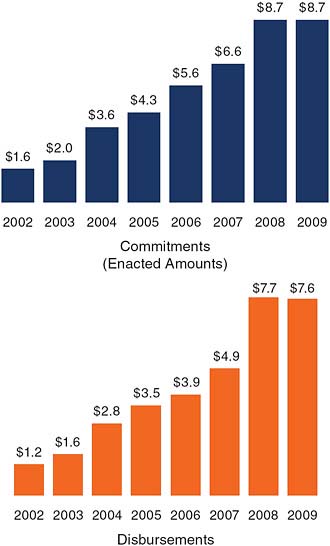
FIGURE 3-3 Steady increase in international funding for HIV/AIDS from Group of Eight (G8), European Community (EC), and other donor governments, 2002–2009 (in billions of U.S. dollars).
SOURCE: Kaiser Family Foundation, 2010.
faith-based communities with respect to development and poverty relief in Africa by opening up new areas of potential funding; and inspired new efforts by, among others, private foundations, public health researchers, political scientists, and development economists. Many of these groups brought to the forefront of U.S. leadership’s attention such potentially contentious issues as how the United States plans to deal with the human, health, security, and economic implications of the
projected international trends in HIV/AIDS. These new constituencies could be valuable sources of information for building a long-term strategy to combat HIV/AIDS, as well as influential bases of support for future efforts in global health.
Although the PEPFAR initiative has maintained a singular focus on HIV/AIDS, it has helped raise the profile of global health more broadly and catalyzed greater interest in the complexities of development and public health. As evidenced by adjustments to PEPFAR, new emphases in successive congressional authorizations, and the Obama administration’s Global Health Initiative, U.S. interventions in HIV/AIDS through PEPFAR quickly revealed the enduring challenges of gender inequity; health infrastructure deficits; shortages of health professionals; multiple disease threats; and the intersection of public health with education, economic development, and food security. PEPFAR’s early lessons have helped inform U.S. efforts going forward and have piqued the interest and commitment of a younger generation increasingly attracted to international service. Research and university partnerships have expanded, as have innovative public–private partnerships in health service delivery, training, and capacity building. These achievements will ultimately strengthen a long-term, comprehensive approach to HIV/AIDS, but also bring greater focus to the broader disease burden and structural development challenges faced by African countries.
IMPLICATIONS FOR U.S. INTERESTS
Implications for Diplomacy
PEPFAR funding and programming have engaged U.S. researchers, public health experts, technical experts, military personnel, and others with counterparts in African governments and communities in ways that simply would not have happened absent the PEPFAR platform. These interactions have impacts beyond HIV/AIDS: they build trust, strengthen a sense of shared purpose and responsibility, and foster abiding relationships that ultimately redound to U.S. interests in greater global engagement and understanding. African opinion of the United States has remained overwhelmingly positive in the last decade (Pew Research Center, 2008; Ray, 2008). Many observers attribute this goodwill to U.S. leadership and engagement in combating HIV/AIDS. While U.S. funding for HIV/AIDS treatment, which is, of necessity, a substantial long-term commitment, does not necessarily give U.S. policy makers greater leverage over recalcitrant authoritarian states in Africa (Lyman and Wittels, 2010), the linkages to individuals and communities built today may offer a basis for stronger partnerships in the future.
Finally, a less tangible but equally important outcome of U.S. global HIV/AIDS efforts has been to help rebuild the positive stature and constructive role of the United States in the world—a role that draws on international partnerships, such as those with European governments, United Nations agency heads, and African leaders, to tackle the world’s most vexing transnational problems and is
based on a core belief in the value of human dignity. Such leadership is all the more strategically important in a global context that is vastly different from that of 10 or 15 years ago, one in which the United States must compete with emerging powers and ideologies for alliance and influence. There is growing consensus, reiterated in the Obama administration’s 2010 National Security Strategy,1 on the need to rebuild and strengthen the elements of U.S. soft power2 and build a “whole of government” approach—integrating the military, diplomacy, development, intelligence, and security arenas—to U.S. engagement in the world (The White House, 2010). By sustaining its commitment to the fight against HIV/AIDS and bringing the multiple elements of U.S. soft power to bear—including capacities in research, education, technology, public health, private enterprise, and philanthropic institutions—the United States has at once had an impact on the pandemic and begun to burnish its credentials as a global force for positive change.
Implications for the Private Sector
The last decade has seen a dramatic rise in private-sector engagement on HIV/AIDS, involving advocacy, philanthropic contributions, in-country programming, in-kind donations, and an array of innovative public–private partnerships (IOM, 2009a). Many companies have recognized the reputational benefits of engagement and advocacy on HIV/AIDS and have found resonance with a U.S. consumer base that is socially conscious and better informed on the scope of the pandemic.
Corporations with operations in Africa, particularly those with large employee bases, have recognized the potential impact of HIV/AIDS on their workforce—in absenteeism, productivity declines, health care expenditures, and workforce turnover—and on the broader communities in which they operate. Provision of HIV/AIDS services to employees, their families, and the communities in which they live thus serves the purposes of both corporate social responsibility and good business sense.
Through the Global Business Coalition on HIV/AIDS, Tuberculosis and Malaria (GBC), for example, corporate-sector members (such as Chevron from the United States, South Africa’s Standard Bank, and nearly 200 others) align with a network built for action and achievement in the fight against infectious disease. GBC also manages the private-sector delegation to the Global Fund (GBC, 2010). Similarly, the South African Business Coalition on HIV & AIDS
(SABCOHA) coordinates a private-sector response to HIV/AIDS by empowering its members to plan for and effectively manage the impact of the epidemic in that nation. Its major projects include BizAIDS—a series of workshops with supportive materials to help micro and small companies reduce their operational risk and make them aware of the burden of HIV/AIDS—and supply chain management projects that aim to broaden the reach of private-sector HIV/AIDS initiatives (SABCOHA, 2010).
Corporate social responsibility and corporate philanthropy have brought significant resources to the global effort on HIV/AIDS, but equally important has been the rise in private–public partnerships that bring a company’s core competence to bear. Companies engage in public–private partnerships for a variety of reasons, including not only corporate philanthropic objectives but also more business-driven motivations. Such partnerships can improve market access and foster partnerships and goodwill with host country governments. They can also build capacities that, while benefiting partner organizations, may serve corporate interests as well, for example, in research and development; procurement, supply chain, and other logistics management; manufacturing of pharmaceuticals; adaptation of specific technologies; laboratory building; and development of a trained and knowledgeable workforce. Ultimately, these kinds of partnerships with direct relevance to a company’s business will be the most durable and sustainable, since philanthropic giving alone will be vulnerable to financial and economic fluctuations (IFC, 2008).
Pharmaceutical companies are vital to the fight against HIV/AIDS in developing new technologies, providing an adequate supply of drugs and technologies, and conducting critically needed research and development. In the early 2000s, pharmaceutical companies were a target of global HIV/AIDS activism, ultimately acquiescing to dramatic price reductions for first-line ARV drugs for the developing world. That experience may better prepare companies for future demands, but may also lead some to disinvest in research and development for products that are perceived as ultimately not serving bottom-line business interests. Already there are signs of a troubling decline in commercial investments in research and development for HIV/AIDS vaccines, microbicides, and prevention (AVAC, 2010).
As demand for affordable access to treatment increases in the future, companies will face strong downward pressure on prices for second-line therapies; new, more effective drugs; and other medical technologies. The World Trade Organization’s (WTO’s) Agreement on Trade Related Aspects of Intellectual Property Rights (TRIPS) includes a number of limitations and exceptions for developing countries that enable the import and manufacture of generic versions of needed drugs, although both the United States and some pharmaceutical companies have been accused at various times of retaliating against countries that choose to exercise these flexibilities (American University Washington College of Law Program on Information Justice and Intellectual Property, 2010). Moreover,
as some of these exemptions for developing countries expire in 2016, tensions around intellectual property rights may increase. A number of companies have negotiated creative licensing agreements with partner states—for example, Gilead Science’s arrangements with Indian and South African manufacturers to assist them in producing tenofovir while retaining patent rights—arrangements that offer hope of expanded and more sustainable access to drugs in Africa and the rest of the developing world (Bate, 2010).
Pharmaceutical companies have been strong proponents of patent protection in their attempts to protect their markets and profit margins. The result has been the perception that they place profit ahead of human welfare, a criticism that the sector has vigorously been trying to shed. Approaches to addressing this challenge include dual pricing (substantially lower prices in developing than in developed countries), voluntary licensing to developing-country generic drug manufacturers, and the creation of low-priced “generic equivalents” for low-income countries. While these approaches have increased access to affordable drugs, they have also enabled pharmaceutical companies to protect their lucrative developed-country markets and their patent provisions. In addition, pressure and support for voluntary patent pooling are rising. UNITAID, for example, announced its intention to launch a patent pool for HIV/AIDS drugs in mid-2010, an arrangement in which branded pharmaceutical companies will voluntarily waive patent rights in low-income countries in exchange for royalty fees, allowing production by local generic manufacturers while maintaining patent rights in higher-income countries. Some companies have embraced the model, although for others, questions around eligibility persist (UNITAID, 2010).
For the global effort against HIV/AIDS, it will be important that private-sector involvement and investment in new drugs and technologies be maintained (see the case example in Box 3-1). But are there adequate market signals and incentives for the development and manufacture of critically important drugs and technologies? Pharmaceutical and health technology manufacturers could help define and advocate for adequate, realistic incentive structures and advance purchasing mechanisms that would ensure investment in those drugs and technologies most relevant to the developing world. Organizations such as the Clinton Foundation and mechanisms such as UNITAID can serve as important interlocutors in these discussions.
Implications for Research and Academia
As noted, the HIV/AIDS pandemic and U.S. global efforts have attracted the attention of a younger generation increasingly interested in international service (Drain et al., 2007; IOM, 2009a,b). The last decade has seen an explosion of public and global health degree programs and multidisciplinary global health institutes at U.S. universities. A recent survey of 37 universities by the Coalition of Universities in Global Health revealed more than a doubling of the numbers
|
BOX 3-1 Building Drug Manufacturing Capacity: A Case Example Public–private partnerships can lend themselves to building not only human resource capacity but also drug manufacturing capacity. In 1989, Merck Pharmaceuticals, Inc. signed an agreement with the Chinese Ministry of Public Health to share Merck’s recombinant hepatitis B vaccine technology with two Chinese vaccine manufacturers. At the time, China had one of the highest hepatitis B rates in the world and limited production of plasma-derived hepatitis B vaccines. Through this partnership, Merck provided China with the process design knowledge needed to produce the hepatitis B vaccine and the training needed to operate the new technology. The Chinese ministry constructed the manufacturing facility, purchased the equipment, and managed the production of the vaccine in the newly built facilities. Over a 3-year period, Chinese engineers, quality control scientists, and production supervisors trained at Merck facilities in the United States, learning the design process, assembly, and testing for the manufacturing equipment. The equipment was then shipped and installed in China, with Merck employees assisting in the reassembly. Sixty-five percent of China’s hepatitis B vaccines are now produced in these facilities, preventing more than 30 million chronic hepatitis B infections and related sequelae (Feinberg, 2010). This example of a pharmaceutical company building capacity for drug manufacturing can be applied to Africa and ART for HIV/AIDS. |
of undergraduate, graduate, and doctoral students in global health studies in just 3 years, from 2006 to 2009. In addition, these 37 universities have a combined 302 long-term training and education projects in 97 countries around the world. Beyond the dramatic enrollment figures, the survey found that students had formed 105 global health groups—nearly three per campus (CUGH, 2009). Universities can capitalize on this burgeoning interest and broaden the interdisciplinary focus on global health and HIV/AIDS, encouraging inter- and intrauniversity collaborations and joint degree programs in public health, nursing, business, management, policy, and international affairs. Collaborations with African academic institutions, through faculty and student exchanges, distance learning, and shared curricula, can enrich both U.S. universities and African counterparts (IOM, 2005, 2009b).
U.S. academic institutions have played a key role in supporting and collaborating with African researchers to make substantial contributions to the generation of new knowledge, especially in the areas of clinical and public health research on HIV/AIDS. U.S.–African research partnerships are well established and have a long track record of building local capacity to conduct research. Most notable among these initiatives is the Fogarty AIDS International Training and
Research Program, which provides funds for both U.S. partner institutions and in-country institutions with a view to long-term capacity building and increased South–South collaboration.3 Such programs need to be expanded to more African countries as they help address, and in some instances reverse, the brain drain because of their high in-country retention rates.
At another level, strengthening of research capacity needs to extend beyond the training of individual researchers to create academically vibrant and sustainable research institutions in Africa. There are many examples of U.S. institutions creating world-class research institutes in Africa, most of which are self-sustaining with strong in-country leadership. Most notable among these are the Infectious Diseases Institute (IDI) in Uganda; the University of California, San Francisco–University of Zimbabwe (UCSF-UZ) collaboration in Zimbabwe; and the Centre for the AIDS Programme of Research in South Africa (CAPRISA). In addition, philanthropies such as the Doris Duke Charitable Foundation and the Howard Hughes Medical Institute have made substantial investments in creating major new basic science and clinical research institutes with long-term secure funding. Such long-term investments take the role of the United States in research capacity building one step further; they are strengthening institutional capacity and core resources such as libraries and access to scientific journals, building critical mass, helping to alleviate the brain drain, and creating capacity for high-quality in-country research training.
Since Africa is the region of the world most affected by HIV/AIDS, it is also the region with the greatest potential to make significant contributions to new breakthroughs in HIV/AIDS prevention and treatment. For example, Africa has contributed critically important HIV prevention strategies, such as the use of nevirapine and exclusive breastfeeding to reduce mother-to-child transmission of HIV, circumcision for the prevention of HIV in men, and topical ARV agents for HIV prevention in women. The development of these strategies was made possible by the long-term investments of the U.S. government in building clinical trial capacity in Africa. This capacity-building process occurred over decades, largely through clinical trial networks sponsored by the National Institutes of Health (NIH), which evolved from initial partnership arrangements led almost solely by U.S. investigators to the current model of partnerships of equals involving joint U.S.–African leadership. Chapter 5 provides a thorough discussion of capacity-building partnerships, including twinning, and offers recommendations for the academic sectors in the United States and Africa.
Implications for Foundations
Addressing the HIV/AIDS epidemic in Africa speaks to the core interest and mission of a large number of U.S. philanthropies—that is, contributing to a global public good and improving the lives of those most in need. U.S. foundations have been a major force in mobilizing responses and resources for the fight against HIV/AIDS. In 2008 they provided $618 million for programming related specifically to global HIV/AIDS, 36 percent of which targeted east and southern Africa (Funders Concerned About AIDS, 2009). The Bill & Melinda Gates Foundation accounted for about 59 percent of philanthropic funding in 2008, and such funding is increasingly concentrated among a relatively small number of organizations (Funders Concerned About AIDS, 2009). Large foundations that bring significant financial resources to bear can play an important role in protecting core commitments in uncertain political or financial times.
Beyond resource mobilization, foundations have a unique role to play in complementing the efforts of governments and multilateral institutions. Political independence gives them flexibility and the ability to innovate and take risks and to support interventions and programming in areas less likely than others to generate broad-based political support. There is tremendous variety across U.S. philanthropic organizations in objectives, time frames, and strategies, and this diversity is an additional asset in building a long-term, sustainable response to HIV/AIDS. Relatively new foundations, such as the Bill & Melinda Gates Foundation, have emphasized innovation (The Bill & Melinda Gates Foundation, 2010), pioneering efforts that may entail higher risk than most government programming is willing or able to bear. The Gates Foundation has played a vital role in sustaining commitment to HIV/AIDS vaccine and prevention research (AVAC, 2010) and has been the largest private contributor to the Global Fund (Global Fund, 2010c). It has had a strong political voice and helped catalyze efforts of a host of nongovernmental organizations in advocacy, prevention, and research. The Clinton Foundation, through the Clinton Health Access Initiative, has undertaken an innovative business-oriented approach, working with generic pharmaceutical companies in international efforts to reduce the price of drugs and medical technologies for low-income countries, as well as engaging in service delivery, training, and health policy assistance (Clinton Foundation, 2010). These and similar foundations have generated new knowledge and lessons learned; they have the ability to be nimble and adaptive and to reach communities and address issues that are politically marginalized or controversial.
On the other hand, long-standing U.S. foundations—such as the Ford Foundation, the Carnegie Corporation of New York, the John D. and Catherine T. MacArthur Foundation, the Rockefeller Foundation, the William and Flora Hewlett Foundation, and the Africa America Institute—have remarkable track records in building research, academic, and leadership capacity through sustained, long-term engagement. The mechanisms they have used include fellow-
ships, partnerships, and scholarships, the kinds of investments that do not yield quick returns but are critical in building the longer-term capacities that will be needed to address HIV/AIDS in coming generations.
Collaboration and communication among diverse U.S.-based foundations will be valuable in harnessing the strengths of each, sharing best practices and lessons learned, and identifying potential areas of need or neglect. Funders Concerned About AIDS (FCAA), which comprises some 1,500 private philanthropic organizations focused on HIV/AIDS, has helped play this role, providing information and technical advice to foundations and tracking trend lines in funding and programming for HIV/AIDS across U.S. philanthropies (Funders Concerned About AIDS, 2010).
The ability of philanthropic organizations to operate outside the control of donor and recipient governments is a benefit, although this independence does come with potential risks, particularly when significant resource flows are involved. Bringing disproportionate resources and innovation to bear on a problem of interest to a particular philanthropy but outside a national government’s strategic plan can potentially have distorting effects by drawing essential personnel and resources away from the host country’s priority challenges. Further, as efficiency of programming and rationalizing of multiple resource flows become increasingly important, foundations working in country will want to ensure that their efforts are aligned with or complementary to national strategies.
ADDRESSING THE IMPACTS ON U.S. INTERESTS
PEPFAR was born of an exceptional moment of international consensus around HIV/AIDS, propelled by a sense of urgency and opportunity. Today, 29 years into the pandemic and a decade after significant mobilization of the international community began, U.S. leadership in combating HIV/AIDS remains essential. In fact, such leadership is needed now more than ever, as the response to the pandemic needs to be transformed to meet the long-term challenge.
Building a Long-Term Approach to a Chronic Emergency
Among the greatest challenges will be the difficulty of maintaining a sense of urgency and focus on HIV/AIDS while responding to critics eager to move the U.S. global commitment away from such a strong emphasis on a single disease. As suggested earlier, as the initial impetus and sense of urgency for U.S. engagement on HIV/AIDS subside, U.S. policy makers will likely seek to take on new global and development challenges, and domestic constituencies and African partners will similarly press for attention and funding for competing health and development priorities. Yet HIV/AIDS remains a grave and immediate threat that puts millions of lives in jeopardy and will be an ongoing emergency for many decades to come, especially in Africa (see Chapter 2 and Appendix A).
The epidemic in the region is thus a crisis that requires an emergency response but at the same time the forethought, planning, and sustained commitment of a long-term development intervention (Whiteside and Whalley, 2007). If incidence rates do not slow significantly in the next decade, the ever-increasing demand for access to ART will threaten to overwhelm the human, institutional, and resource capacities currently available to African states and their partners. Accordingly, the international community must focus now on preventive measures and invest far greater effort in strategically building the human and institutional capacities needed to manage the epidemic in a sustainable way.
Moving beyond short-term strategies on HIV/AIDS will challenge U.S. policy makers, legislators (appropriators in particular), and the U.S. public, all of whom are eager to see quick, tangible returns on investments made (Feingold, 2007; Oomman et al., 2007; Ward, 2007). PEPFAR garnered strong bipartisan domestic support largely because it was presented as an emergency intervention and set hard targets for prevention, treatment, and care on which future funding would be predicated. Among the PEPFAR targets, expanding access to treatment has been the least difficult to measure and has had the most dramatic, immediate, and visible impact. Some have termed this rejuvenation of a community through the infusion of ART the “Lazarus” effect. This achievement has served as a powerful incentive for U.S. policy makers, who are able to see dramatic proof of the impacts of U.S. investments. More diffuse efforts in prevention, care, health system strengthening, and capacity building—critical areas for future success—have proven more difficult to measure and less immediately visible (Accordia Global Health Foundation, 2010), and thus they are potentially less likely to generate continued congressional enthusiasm. The full dividends from investments in education, training, and institution building likely will not be felt for 10 to 15 years, a considerably longer time horizon than that which typically preoccupies U.S. policy makers. In the fight against HIV/AIDS, as in development assistance more broadly, the U.S. Congress must be convinced to look beyond annual targets and undertake the longer-term commitments required for a sustained impact. To this end, the U.S. administration must forge a longer-term vision on HIV/AIDS, one that sets ambitious but realistic objectives over the next 15 years and that gives Congress and the U.S. public a sustained sense of purpose and direction for long-term U.S. investments in HIV/AIDS, as well as greater appreciation of how these investments will shape future outcomes.
Moving Toward Shared Responsibility
As noted earlier, a central feature of a long-term, sustainable approach is shared responsibility, with African partner governments assuming increasing responsibility for the mustering and management of resources for national HIV/AIDS strategies. If the United States is to sustain a long-term financial commitment to combating HIV/AIDS during a fiscal crisis, Congress and U.S. taxpayers
will likely demand greater assurance that the recipients of the funding are equally engaged both in mobilizing domestic resources and in ensuring efficiency and accountability in their use. At the same time, however, managing this transition to shared responsibility and striking the appropriate balance may prove politically sensitive.
U.S. leadership to date has created an expectation of continued rapid expansion of HIV/AIDS funding among recipient governments, the international community, and domestic constituencies focused on HIV/AIDS. These expectations may prove politically damaging if the United States is perceived as reneging on commitments or unilaterally disengaging through a strategy of “country ownership.” Domestic and international activists were quick to criticize the Obama administration’s slowdown in funding increases for HIV/AIDS, even in the aftermath of the worst domestic economic recession in a century (AHF, 2010; Tutu, 2010; Voice of America, 2010).
The burden of expectation will be particularly acute with respect to U.S. support for treatment. Today, the United States supports the provision of ART to some 2.4 million people in need globally, and the Obama administration has promised to extend that commitment to 4 million people by 2014 (Office of the Global AIDS Coordinator, 2009). This commitment, as well as the 2005 Group of Eight (G8) commitment to achieving “as close as possible” universal access to HIV treatment by 2010 (International AIDS Society, 2010), has created a general expectation on the part of recipients and partner governments that U.S. support for treatment can continue and expand as the number of those in need of ART increases. This expectation puts U.S. policy makers in a precarious position. They cannot in good conscience withdraw support from individuals who have accessed ART through U.S. intervention. As a result, support for ART has taken on attributes of an entitlement program, which cannot, for ethical and political reasons, easily be scaled down (Over, 2008). If the rate of expanded access to ART decreases, the United States may face popular resentment and diplomatic repercussions from partner governments. Recent shortages of ARV drugs in Uganda in early 2010, attributed to the United States withholding resources, generated headlines highly critical of the U.S. administration and linking U.S. budget decisions to heartbreaking stories of patients turned away from ART clinics (McNeil, 2010; Zakumumpa, 2010).
If the gap between treatment needs and available resources increases, difficult questions will inevitably arise about how to prioritize access to ART, with individual lives hanging in the balance. Already, the Office of the Global AIDS Coordinator has indicated that preference will be given to pregnant women, tuberculosis patients, and individuals with extremely low CD4 cell counts (Goosby, 2010). The merits of this or any particular approach aside, the larger question will inevitably arise of how these decisions are made and who has the authority to make them. The United States will not serve its interests by entangling itself in complex ethical questions that are more legitimately answered within recipient
states (see Chapter 6 for a more thorough discussion of the need for ethical decision-making capacity in African communities).
Although a shift to greater shared responsibility with African partner governments in the next decade is most desirable, it will not easily be accomplished in all countries. First, the question arises of whether partner states will be ready and willing to assume this role. To date, little scrutiny and expectation have been focused on African governments themselves in prioritizing or mobilizing resources for HIV/AIDS. Few African countries have come close to meeting commitments made at the Abuja summit in 2002, at which heads of state pledged to allocate 15 percent of their national budgets to the health sector. On a continental level, average general government expenditures on health as a percentage of total government expenditures rose marginally from 8.8 percent in 2001 to 9.0 percent in 2007 (the last full year for which data are available), although three countries—Djibouti, Botswana, and Rwanda—attained the target in 2007 (Global Fund, 2010d).
For most countries, external resources constitute a significant proportion of total health expenditures (the continental average in Africa rose from 15.3 percent in 2002 to 20.1 percent in 2006, with 14 countries at more than 30 percent). Many African countries remain highly dependent on external assistance for health resources (Global Fund, 2010d). In some countries, in fact, there is troubling evidence that donor assistance for health has had a negative effect on domestic government spending on health (Lu et al., 2010). Further, African partner countries vary widely with respect to the political will to assume a stronger leadership role and to develop strategic and planning capacity, management and implementation capacity, and institutional infrastructure and resources.
The question also arises of whether U.S. policy makers will be prepared to cede significant control over funding flows and allow for flexibility in meeting partner-driven, rather than U.S.-driven, priorities. The dominant role of U.S. funding in individual countries’ HIV/AIDS budgets has meant that in many cases, congressional earmarks and U.S. priorities drive national responses in recipient countries. And while the Office of the Global AIDS Coordinator has placed increasing emphasis on the notion of “country ownership,” it is not yet clear whether the United States, and in particular the Congress, will be prepared to act on this notion with respect to resource management and allocation.
In 2008, PEPFAR established the concept of “Partnership Frameworks”—nonbinding agreements intended as “joint strategic planning documents that outline the goals and objectives to be achieved and the commitments and contributions expected of all participating Framework members” (Office of the Global AIDS Coordinator, 2008). This approach is a strong and positive step toward clarifying the respective roles of the United States and its partners within a model of increasingly shared responsibility. Nonetheless, as resource requirements, the need for efficiency, and expectations for greater partner country investment mount, a more binding form of written agreement or contract would provide
strong incentives for effective and accountable partner-country governance and investment. It would also spell out U.S. obligations and commitments in a more reliable and predictable way that would facilitate future planning by host country governments. This model would resemble the compact model of the U.S. Millennium Challenge Account (MCA), which, based on strong positive indicators in the areas of good governance, economic freedom, and investments in their citizens, gives partner countries far greater control over planning, allocation, and management for large-scale, 5-year grants (MCC, 2010).
Because African countries fall along a broad continuum in terms of their capacity to take on “full ownership,” the shared-responsibility paradigm is intended to provide incentives to move toward greater ownership and help give African nations the capacities to do so. As with the MCA, countries with demonstrated political will, an emphasis on prevention, and efficient, transparent health management would receive stronger financial commitments with less control, oversight, or intervention from the United States. This approach would move the United States more in the direction of providing direct budget support. If African countries did not maintain their commitment to the binding aspects of the contract, the agreement would require a renegotiation. For the lowest-income, less-capable countries in Africa with weak leadership around HIV/AIDS, the contract model should incorporate incentives to improve their performance in order to receive increased financial support. In their relationship with these less equipped countries, the United States and other donors should play a larger role in the capacity-building aspects of the shared-responsibility paradigm, including leadership and infrastructure development, and should maintain strict oversight of budgetary support. Given the projected burden of HIV/AIDS in the coming decades, support from international donors today can help build the infrastructure, political will, and institutional and human resource capacity that African nations will need to address their own country-specific HIV/AIDS needs and priorities in 2020 and beyond.
The following are examples of what the United States and other partner governments might include as essential or “nonnegotiable” elements of such a contract relating to African government responsibilities:
-
sustained political leadership on HIV/AIDS;
-
commitment to human rights and an evidence-based national response to the epidemic;
-
a strong focus and voice on HIV/AIDS prevention; and
-
transparent, efficient, and accountable procedures for the use of both country-level and donor resources.
Those countries deemed as lacking these essential elements would not qualify for elevated levels of financing or a contract model ceding greater control to the African partner government.
The committee acknowledges that the achievement of these contract responsibilities may take time. Nevertheless, the United States should immediately make clear that it will become more selective with respect to its development partners. As less restrictive approaches to these types of institutional relationships have not succeeded in the past, it is the committee’s best judgment that binding contracts—in which the United States would cut back on funding in those countries that lagged in taking the path toward shared responsibility—are worth trying in the future.
Making Prevention a Priority
The greatest challenge to U.S. policy is the continued expansion of the epidemic in Africa. Today, incidence rates remain at alarmingly high levels, outstripping expanded access to treatment by a ratio of 5 to 2—for every two people accessing ART for the first time, an estimated five people are newly infected (see Chapter 2 for a discussion of the treatment gap and associated resource requirements).
The many achievements of the U.S. global HIV/AIDS response—and indeed the global community’s remarkable mobilization around the disease—are profoundly at risk if this trajectory persists. Yet despite these alarming statistics, support for prevention has been among the more politically divisive issues within the Congress, with ideological sensitivities focusing on condom promotion, sex education, outreach to commercial sex workers, and injecting drug use. Should new infections in Africa continue to outstrip access to treatment, by 2020 the costs of providing treatment will far exceed the international community’s capacity and will to mobilize adequate resources. This reality must be the central driver of any future strategy on HIV/AIDS. Failure to reduce incidence rates will make the goal of universal access to treatment impossible and will result in increasingly difficult decisions about complex trade-offs and political choices in the coming decade and beyond (see Chapter 2).
Chapter 2 underscores the importance of acting now to shape outcomes that will be apparent only in the long term. Failure to act decisively on HIV/AIDS prevention now will result in an even bleaker situation in 2020 in terms of the evergrowing need and demand for treatment resources. Prevention works best when interventions are selected on the basis of knowledge of the risks and drivers of the epidemic and when they are implemented appropriately and to scale. To this end, a better balance must be struck in the allocation of effort and resources to prevention and treatment (Independent Task Force Report No. 56, 2006; UNAIDS and WHO, 2009). The overlap between the two is significant (see Chapter 2) but not absolute, and in a context of finite resources and the present fiscal situation in the United States, trade-offs in resource allocation will most certainly be necessary. However, attaining the optimum balance between treatment and prevention will
likely be a politically complex issue, as saving lives through expansion of ART is the highly visible and pressing need.
Given this difficult challenge, it is important not to lose sight of the value of treatment efforts already under way while strengthening prevention messages and activities. Evidence of successes in HIV/AIDS prevention is growing; for example, the drop in new HIV infections among children between 2001 and 2009 suggests that the increase in coverage for services to prevent mother-to-child transmission of HIV is saving lives (UNAIDS, 2010).
Engaging the World: Leveraging Multilateral Assets
In today’s global political context, in which the United States must increase its reliance on global alliances and partnerships, strengthening and working through multilateral mechanisms are of increasing strategic importance, a point underscored in President Obama’s 2010 National Security Strategy (The White House, 2010). Accordingly, the United States will want to ensure continued international engagement on HIV/AIDS and leverage the full range of capabilities and resources that the broader global community can bring to bear.
Multilateral forums and institutions have been an important component of U.S. engagement on HIV/AIDS. They have been a strong asset for U.S. leadership in building international consensus, mobilizing resources and attention, coordinating global efforts, and creating and strengthening international institutions dedicated to global health and the fight against infectious disease. The Clinton administration’s engagement in the 2000 United Nations (UN) Security Council Session on HIV/AIDS in Africa, which declared HIV in Africa a threat to security (Gore, 2000), and participation in the UN General Assembly Special Session on HIV/AIDS in 2001 (UNGASS, 2001), for example, are considered watershed events in bringing greater international attention and urgency to the HIV/AIDS pandemic. Support for UNAIDS has allowed that organization to aggregate and communicate data on the pandemic effectively and to help ensure coordination and complementarity of international efforts at the country level.
The U.S. voice at successive G8 summit meetings has helped generate significant resource commitments from G8 members in support of HIV/AIDS endeavors. Mechanisms such as UNITAID, which pursues price reductions for drugs and medical technologies, offer models for innovative financing and market incentives that complement U.S. bilateral funding flows. Today, as the Group of Twenty (G20) gains global traction, the United States should seek to broaden discussions on global health and encourage continued attention to HIV/AIDS. It should make a particular effort to engage emerging economic powers, including China, India, Russia, and Brazil, both in formulating multilateral strategies on HIV/AIDS and in strengthening human resource–and capacity-building collaborations within South–South partnerships.
Perhaps most important in the multilateral arena, early U.S. support for the Global Fund helped initiate and sustain a new model of international financial support that is driven by country-level plans, priorities, and decision making (Global Fund, 2010b). How best to strike an appropriate balance between U.S. bilateral commitments and commitments channeled through multilateral mechanisms such as the Global Fund has been the source of ongoing domestic debate. Both approaches have their merits and shortcomings.
Bilateral programming has allowed the United States to channel resources quickly to recipient countries; realize quick returns on short-term investments; and retain close control, oversight, and accountability in U.S. funding flows. The pressure to see quick results led to an early tendency by PEPFAR implementers to seek to bypass weak, inefficient systems in recipient countries. PEPFAR’s decision to initially operate independently of existing mechanisms was key to making things happen quickly in partner organizations (as centralizing and coordinating slows down operations). In this sense, the approach was pragmatic and timely, but it did undermine host countries’ abilities to attain greater coordination. For this reason, bilateral programs have been criticized for creating parallel procurement and service delivery systems, for failing to integrate fully with recipient country priorities, and for tending toward short-term strategies that do not necessarily give priority to capacity building or sustainability.
The Global Fund model, on the other hand, ensures that funding flows are more clearly aligned with country priorities as determined by a multisectoral Country Coordinating Mechanism; that recipients enjoy greater flexibility in using resources for long-term approaches and system strengthening; and that more responsibility is placed with host countries for planning, management, and institutional capacity to oversee and account for health resources. This model also has been criticized, however, for such reasons as slow disbursements of funding, reliance on in-country capacities that are overly weak or politicized, and laborious bureaucratic processes.
No doubt both U.S. bilateral efforts and the Global Fund will require adjustments as the HIV/AIDS pandemic and country capacities evolve. By analyzing these efforts over the coming decade, the United States could capitalize on the positive aspects of both models; the committee calls for drawing on the best of both approaches. For example, as a recipient country’s capacity for delivery, management, and oversight of interventions becomes more robust, the United States may want to shift away from bilateral interventions to multilateral funding mechanisms. The committee does not expect this shift to occur overnight, but sees its progressive realization as a potentially important long-term goal of the proposed shared-responsibility model. The U.S. effort can help remedy inadequate infrastructure and systems only if the host country itself has the will to do so.
Striving for Integration and Efficiency
U.S. commitments to combating HIV/AIDS, and in particular the growing costs associated with expanded provision of treatment, may ultimately limit U.S. flexibility and ability to address the health and development priorities articulated by African partner states. Since 2001, HIV/AIDS has dominated U.S. global health funding. Critical investments in family planning, in maternal-child health, and in early childhood diseases have not seen increases commensurate with those in HIV/AIDS services, although they face devastating challenges in virtually every African state. The Obama administration’s expanded Global Health Initiative budget for 2010 includes significant increases in family planning and maternal-child health, but PEPFAR programming is expected to make up some 77 percent of overall funding flows (Kaiser Family Foundation, 2009).
Accusations of “AIDS exceptionalism” may intensify, especially if expenditures on ARV drugs consume an ever larger proportion of U.S. global health spending. Policy makers may face increasing pressure from U.S domestic interests, donor partners, and African partner governments to address more directly health priorities beyond HIV/AIDS and to support multipurpose investments in health system strengthening.4 In a world of finite financial resources, policy makers must confront difficult trade-offs, including that between focusing on life-prolonging ARV drug purchases and envisioning HIV/AIDS in a broader context of pressing and equally devastating disease challenges.
Just as striking the right balance between prevention and treatment efforts will be difficult for governments, striking the appropriate balance between funding for HIV/AIDS and other diseases will be an ongoing and sensitive political challenge. Identifying and strengthening synergies between HIV/AIDS interventions and other health objectives may alleviate some of this difficulty. To this end, implementers on the ground might proactively seek opportunities for integration of HIV/AIDS services and capacities with other disease and development interventions. Funders could help as well by identifying and developing approaches that better integrate HIV/AIDS interventions with other critical health priorities. For the U.S. government, this might mean better integration of global health efforts and improved alignment with host country priorities. By giving greater priority to those interventions that build enduring health care capacity, the United States can enable African partners to manage the multiple challenges their citizens confront.
An even broader challenge will be balancing HIV/AIDS and other health interventions with other forms of U.S. development assistance. In the course of the last decade, Africa has moved more firmly into the mainstream of U.S. policy with an expansion of U.S. interests and investments; a changing notion of what
|
4 |
An assessment of positive, negative, or neutral spillover effects of HIV/AIDS-targeted programs on health systems is discussed in Chapter 4. |
constitutes security; and greater competition for influence and alliance in an increasingly globalized, multipolar international context. Engagement on HIV/AIDS has been an important component of expanded U.S. relations with Africa, but only one of many strands of additional attention and concern. Support for HIV/AIDS programming represents a growing proportion of U.S. development assistance to Africa overall. In many African countries, HIV/AIDS and other health funding is by far the largest component of U.S. assistance. In Nigeria, HIV/AIDS constitutes 77 percent of U.S. State Department/U.S. Agency for International Development (USAID) assistance, and overall health programming constitutes 89 percent of assistance (USAID, 2009b); in Rwanda, the corresponding proportions are 60 percent and 79 percent (USAID, 2009c); in Kenya, 77 percent and 88 percent (USAID, 2009a); and in Uganda, 64 percent and 83 percent (USAID, 2009d).5 Investments in agriculture, in education, and in democracy and governance are dwarfed by HIV/AIDS funding, although each of those areas intersects in significant ways with public health and is viewed by many African governments as an important development priority in its own right. Further, expanded investments in HIV/AIDS and health will ultimately yield diminishing marginal returns if other critical developmental priorities—employment, food security, economic growth, education, and water and sanitation—remain unaddressed. Domestic critics may argue that U.S. efforts in international development are too heavily skewed toward HIV/AIDS and that areas of pressing international and foreign policy concern are being neglected.
HIV/AIDS interventions, some observers argue, may be popular among African partner countries, but they do not necessarily lead to greater leverage or influence (Lyman and Wittels, 2010). U.S. policy makers are understandably reluctant to use support for HIV/AIDS services or other forms of humanitarian assistance as a political bargaining chip. But the domination of HIV/AIDS within U.S. foreign assistance flows means there is little room for other forms of engagement that might provide that leverage. The 2010 National Security Strategy promises that “the United States will work to remain an attractive and influential partner by ensuring that African priorities such as infrastructure development, improving reliable access to power, and increased trade and investment remain high on our agenda” (The White House, 2010). Similarly, the administration has announced global food security as a top priority, with President Obama promising $3.5 billion to strengthen food security and enlisting the G8 to give greater priority to assisting poor farmers (Baker and Dugger, 2009; Council on Foreign Relations, 2009). A renewed focus on agricultural development through the Feed the Future initiative was welcomed by development experts and African leaders alike, who have seen investment in agricultural development fall from a high of 18 percent of official development assistance in 1979 to 3.5 percent in 2004 (World Bank, 2008). But unless the overall flow of U.S. assistance increases dra-
matically, there will be little room for these new initiatives—or for other major initiatives not yet envisioned—given current commitments to PEPFAR and global health. U.S. support for HIV/AIDS assistance to Africa is authorized primarily by the 1961 Foreign Assistance Act as well as the PEPFAR legislation, which was reauthorized in 2008 for an additional 5 years.6 The 1961 Foreign Assistance Act was last reauthorized in 2002, and the Congress is currently designing new legislation to update the act. This overhaul offers an opportunity to incorporate some of the steps toward shared responsibility that are described in this report.
RECOMMENDATIONS
Recommendation 3-17: Emphasize a new contract approach that incentivizes shared responsibility. The Office of the Global AIDS Coordinator should emphasize, develop, and implement a more binding, negotiated contract approach at the country level. The contract should incentivize shared responsibility whereby additive donor resources are provided to a large extent as matching funds for partner countries’ investments of their own domestic resources in health. Such matching funds should not be a uniform ratio; rather, the ratio should vary based on each African partner’s ability to contribute.
Recommendation 3-2: Develop a U.S. roadmap for HIV/AIDS in 2020. The White House and the Office of the Global AIDS Coordinator should develop a U.S. roadmap for HIV/AIDS in 2020 incorporating a model of U.S.–African shared responsibility that makes prevention a priority and balances bilateral and multilateral funding. The roadmap should:
-
Give priority to prevention as a central tenet of a sustainable long-term response to the HIV/AIDS epidemic. To this end, steps should be taken to:
-
strengthen country-level surveillance and monitoring of the epidemic to ensure adequate and reliable data with which to estimate incidence rates (see Recommendation 2-1);
-
encourage the UNAIDS-recommended approach of targeted prevention strategies tailored to in-country priority populations, applying evidence-based public health approaches;
-
increase access to and coverage of synergistic combinations of known effective prevention technologies; and
-
expand research and investments in new prevention technologies.
-
|
6 |
Tom Lantos and Henry J. Hyde United States Global Leadership against HIV/AIDS, Tuberculosis, and Malaria Reauthorization Act of 2008, Public Law 110-293 (July 30, 2008). |
|
7 |
See counterpart Recommendation 4-3 directed to African countries (Chapter 4). |
-
Strike an optimal balance between bilateral and multilateral mechanisms for HIV/AIDS funding. The United States should seek to capitalize on the strategic complementarity of bilateral and multilateral funding flows and engagement and work to strengthen multilateral institutions toward that end. U.S. policy makers should encourage greater involvement of emerging economic powers, including Brazil, China, Russia, and India, in international forums and activities on HIV/AIDS and in strengthening of South–South collaborations addressing the epidemic.
Recommendation 3-3: Integrate health and development. Congress should support greater integration of U.S.-funded HIV/AIDS interventions with broader U.S. global health initiatives and African countries’ comprehensive development plans. As Congress contemplates an overhaul of the U.S. Foreign Assistance Act, it should seek to encourage greater flexibility in development funding to ensure that assistance for both health and development meets recipient country priorities.
REFERENCES
Accordia Global Health Foundation. 2010. Return on investment: The long-term impact of building healthcare capacity in Africa. Washington, DC: Accordia Global Health Foundation.
AHF (AIDS Healthcare Foundation). 2010. AHF to roll out “Who’s better on AIDS?” Obama/Bush comparison ad campaign in DC. http://www.aidshealth.org/news/press-releases/ahf-president-obama-fails.html (accessed May 20, 2010).
AIHA (American International Health Alliance). 2005. HIV/AIDS twinning center frequently asked questions. http://www.twinningagainstaids.org/faq.html (accessed November 2, 2009).
American University Washington College of Law Program on Information Justice and Intellectual Property. 2010. Complaint to UN special rapporteur on the right to health, July 19, 2010.
AVAC: Global Advocacy for HIV Prevention. 2010. AVAC report 2010: Turning the page. New York: AVAC.
Baker, B., and C. Dugger. 2009. Obama enlists major powers to aid poor farmers with $15 billion. The New York Times.
Bate, R. 2010. Solving an innovator’s dilemma. The American: Journal of the American Enterprise Institute. http://www.american.com/archive/2010/may/solving-an-innovators-dilemma (accessed May 20, 2010).
The Bill & Melinda Gates Foundation. 2010. Overview: The Gates Foundation’s HIV strategy. http://www.gatesfoundation.org/hivaids/Documents/hiv-strategy-overview.pdf (accessed September 7, 2010).
Clinton Foundation. 2010. Why global health? Our approach. http://www.clintonfoundation.org/what-we-do/clinton-health-access-initiative/our-approach (accessed September 7, 2010).
CUGH (Consortium of Universities for Global Health). 2009. Saving lives: Universities transforming global health. San Francisco, CA: CUGH.
Council on Foreign Relations. 2009. Obama’s food security initiative in Africa. http://www.cfr.org/publication/20020/obamas_food_security_initiative_in_africa.html (accessed October 6, 2010).
Drain, P. K., A. Primack, D. D. Hunt, W. W. Fawzi, K. K. Holmes, and P. Gardner. 2007. Global health in medical education: A call for more training and opportunities. Academic Medicine 82(3):226-230.
Feinberg, M. 2010 (unpublished). Public-private partnerships addressing diseases of the developing world: Lessons learned; current challenges; future opportunities. Merck & Co. Inc.
Feingold, R. 2007. Remarks of U.S. Senator Russ Feingold on priorities for PEPFAR reauthorization.
Fletcher, M. 2006. Bush has quietly tripled aid to Africa. The Washington Post.
Funders Concerned About AIDS. 2009. U.S. philanthropic support to address HIV/AIDS in 2008. Brooklyn, NY: Funders Concerned About AIDS.
———. 2010. Mission & vision. http://www.fcaaids.org/AboutFCAA/MissionVision/tabid/171/De-fault.aspx (accessed August 26, 2010).
Garrett, L. 2010. The debate over foreign aid. Washington, DC: Council on Foreign Relations.
GBC (Global Business Coalition on HIV/AIDS Tuberculosis and Malaria). 2010. Collaboration, coordination and collective action that will end disease faster. http://www.gbcimpact.org/about-gbc (accessed September 24, 2010).
Global Fund. 2010a. The Global Fund 2010: Innovation and impact. Geneva: Global Fund.
———. 2010b. How the Global Fund works. http://www.theglobalfund.org/en/how/?lang=en (accessed September 7, 2010).
———. 2010c. Partnering for global health: The Global Fund and the private sector. Geneva: Global Fund.
———. 2010d. Trends in development assistance and domestic financing for health in implementing countries. Geneva: Global Fund.
Goosby, E. 2010. Presentation to IOM committee on envisioning a strategy to prepare for the long-term burden of HIV/AIDS: African needs and U.S. interests, Pretoria, South Africa, April 12, 2010.
Gore, A. 2000. Remarks as prepared for delivery by Vice President Al Gore: UN security council session on AIDS in Africa. Paper read at UN Security Council Session on HIV/AIDS in Africa.
IFC (International Finance Corporation). 2008. Business of health in Africa: Partnering with the private sector to improve people’s lives. Washington, DC: IFC.
Independent Task Force Report No. 56. 2006. More than humanitarianism: A strategic U.S. approach toward Africa. New York: Council on Foreign Relations, Inc.
International AIDS Society. 2010. IAS urges G8 to follow through on prior commitment to universal access to HIV prevention, treatment and care by 2010 as part of new maternal and child health initiative. http://www.iasociety.org/Default.aspx?pageId=393 (accessed October 21, 2010).
IOM (Institute of Medicine). 2005. Healers abroad: Americans responding to the human resource crisis in HIV/AIDS. Washington, DC: The National Academies Press.
———. 2007. PEPFAR implementation: Progress and promise. Washington, DC: The National Academies Press.
———. 2009a. The U.S. commitment to global health: Recommendations for the new administration. Washington, DC: The National Academies Press.
———. 2009b. The U.S. commitment to global health: Recommendations for the public and private sectors. Edited by P. Subramanian. Washington, DC: The National Academies Press.
Kaiser Family Foundation. 2009. Fact sheet: The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR). Washington, DC: Kaiser Family Foundation.
———. 2010. International AIDS assistance: Trends in G8/EC and other donor government assistance, 2002-2009. Washington, DC: Kaiser Family Foundation.
Lu, C., M. T. Schneider, P. O. Gubbins, K. Leach-Kemon, D. T. Jamison, and C. J. Murray. 2010. Public financing of health in developing countries: A cross-national systematic analysis. The Lancet 375(9723):1375-1387.
Lyman, P. N., and S. B. Wittels. 2010. No good deed goes unpunished. Foreign Affairs 89(4):74-84.
MCC (Millennium Challenge Corporation). 2010. About the MCC. http://www.mcc.gov/pages/about (accessed September 23, 2010).
McNeil, D. 2010. At front lines, AIDS war is falling apart. The New York Times.
Nye, J. S. 2006 (unpublished). Soft power, hard power and leadership. Harvard University.
Office of the Global AIDS Coordinator. 2008. Guidance for PEPFAR partnership frameworks and partnership framework implementation plans (version 2.0). Washington, DC: PEPFAR.
———. 2009. The U.S. President’s Emergency Plan for AIDS Relief: Five-year strategy. Washington, DC: PEPFAR.
Oomman, N., M. Bernstein, and S. Rosenzweig. 2007. Following the funding for HIV/AIDS: A comparative analysis of the funding practices of PEPFAR, the Global Fund and World Bank MAP in Mozambique, Uganda and Zambia. Washington, DC: Center for Global Development.
Over, M. 2008. Prevention failure: The ballooning entitlement burden of U.S. global AIDS treatment spending and what to do about it. Washington, DC: Center for Global Development.
PEPFAR (U.S. President’s Emergency Plan for AIDS Relief). 2009a. Celebrating life: Fifth annual report to Congress on PEPFAR (2009). Washington, DC: PEPFAR.
———. 2009b. World AIDS day 2009: Latest PEPFAR results (December 2009). Washington, DC: PEPFAR.
———. 2010. Sixth annual report to Congress on PEPFAR program results. Washington, DC: PEPFAR.
Pew Research Center. 2008. Global public opinion in the Bush years (2001-2008). Washington, DC: Pew Research Center.
Ray, J. 2008. U.S. Leadership approval highest in sub-Saharan Africa. Gallup. http://www.gallup.65com/poll/106306/us-leadership-approval-highest-subsaharan-africa.aspx (accessed June 8, 2010).
SABCOHA (South African Business Coalition on HIV/AIDS). 2010. Who we are. http://www.sabcoha.org/who-we-are/who-we-are.html (accessed September 24, 2010).
Stolberg, S. G. 2008. In global battle on AIDS, Bush creates a legacy. The New York Times.
Summers, T. 2002. The Global Fund to fight AIDS, TB, and malaria: Challenges and opportunities. Washington, DC: CSIS.
The White House. 2010. National security strategy. Washington, DC: The White House. http://www.whitehouse.gov/sites/default/files/rss_viewer/national_security_strategy.pdf (accessed July 12, 2010).
Tutu, D. 2010. Obama’s overdue AIDS bill. The New York Times.
UNAIDS (The Joint United Nations Programme on HIV/AIDS). 2010. Global report: UNAIDS report on the global AIDS epidemic 2010. Geneva: UNAIDS.
UNAIDS and WHO (The Joint United Nations Programme on HIV/AIDS and World Health Organization). 2009. AIDS epidemic update: December 2009. Geneva: UNAIDS.
UNGASS (United Nations General Assembly Special Session). 2001. Declaration of commitment on HIV/AIDS, 27 June 2001. http://data.unaids.org/publications/irc-pub03/aidsdeclaration_en.pdf (accessed September 7, 2010).
UNITAID. 2010. UNITAID approves patent pool. http://www.unitaid.eu/en/20091215237/News/UNITAID-APPROVES-PATENT-POOL.html (accessed October 19, 2010).
USAID (United States Agency for International Development). 2009a. Kenya fact sheet: FY 2008-11 USAID-state foreign assistance appropriations. Washington, DC: USAID.
———. 2009b. Nigeria fact sheet: FY 2008-11 USAID-state foreign assistance appropriations. Washington, DC: USAID.
———. 2009c. Rwanda fact sheet: FY 2008-11 USAID-state foreign assistance appropriations. Washington, DC: USAID.
———. 2009d. Uganda fact sheet: FY 2008-11 USAID-state foreign assistance appropriations. Washington, DC: USAID.
Voice of America. 2010. Obama criticized over AIDS funding. National Public Radio.
Ward, J. 2007. Bush to visit Africa to see fruit of U.S. AIDS funding. The Washington Times, December 1.
Whiteside, A., and A. Whalley. 2007. Reviewing “emergencies” for Swaziland: Shifting the paradigm in a new era. Mbabane and Durban: National Emergency Response Council on HIV/AIDS (NERCHA) and Health Economics & HIV/AIDS Research Division (HEARD).
WHO, UNAIDS, and UNICEF. 2009. Towards universal access: Scaling up priority HIV/AIDS interventions in the health sector, progress report 2009. Geneva: WHO.
World Bank. 2008. World development report: Agriculture for development. Washington, DC: World Bank.
Zakumumpa, H. 2010. Thousands risk early death as AIDS care centres turn away new patients. The Independent.




























