1
Introduction
The national dialogue leading to the passage of the Affordable Care Act of 2010 (ACA)1 vetted the failure of world-class clinical care to deliver world-class population health outcomes and health equity. The opportunities for change facilitated by the new law can come to fruition only if accompanied by a strong and comprehensive national effort to implement a population-level approach to health across the spectrum of medical, social, and environmental determinants of health.
The United States spent 17.3 percent ($2.5 trillion) of its gross domestic product (GDP) on clinical care in 2009, a proportion exceeding that of any other industrialized nation (Truffer et al., 2010). Organisation for Economic Co-operation and Development (OECD) comparisons show a persisting US per capita cost for clinical care more than twice that of the next-highest-spending country in the world (OECD, 2009). For the most recent year reported, 2008, the United States spent $7,290 per capita (16 percent of GDP) on clinical care compared with an average of $2,934 (9 percent of GDP) in OECD countries (OECD, 2009). More detailed information about clinical care costs to employers and workers for those who receive medical insurance through their employer is provided in Box 1-1.
The outlook for American spending on clinical care in the next decade is sobering. Expenditures are projected to rise sharply to 19.3 percent ($4.5 trillion) of GDP by 2019 (Truffer et al., 2010) and to 34 percent of GDP
|
1 |
“The comprehensive health care reform law was enacted in two parts: The Patient Protection and Affordable Care Act was signed into law in March 23, 2010[,] and was amended by the Healthcare and Education Reconciliation Act on March 30, 2010. The name ‘Affordable Care Act’ is used to refer to the final amended version of the law” (HealthCare.gov, 2010). |
|
BOX 1-1 Clinical Care Costs for Employers and Workers At the employee and employer levels, US clinical care system costs are exceedingly high and increasing at unsustainable rates relative to wages. In the 9-year period 1999–2007, average annual percentage increases in private health expenditures exceeded average annual percentage increases in wages by nearly a factor of 3 (Kaiser Family Foundation and Health Research and Educational Trust, 2007). From 1999 to 2009, the average premium for family health insurance and worker contributions rose by 131%, from $5,790 to $13,375 (Kaiser Family Foundation and Health Research and Eductional Trust, 2009). The individual portion of the premium rose from $1,543 to $3,515, and the employer portion rose from $4,247 to $9,860. In addition, workers saw a 47% cumulative increase in their out-of-pocket expenses for covered services during almost the same period, 2000–2008 (Commonwealth Fund, 2009). Employers, like workers, are staggering under the weight of health care costs. Coupled with projected spending increases in excess of 6% over the succeeding decade (Truffer et al., 2010), US corporations face enormous global competitive pressures in labor cost, particularly from lower-wage rapid-growth countries. In 2009, the Business Roundtable, an organization composed of the chief executive officers of leading US corporations, projected a 166% increase on a per-employee basis over the next decade if existing annual rates of increases in health care costs persist during this period (Hewitt Associates, 2009). |
by 2040 (Executive Office of the President, Council of Economic Advisers, 2009). From 2009 to 2019, individual costs for health-insurance coverage are projected to rise an average of 5.1 percent per year and out-of-pocket expenses 4.8 percent per year (Truffer et al., 2010).
The individual and population health return on those substantial clinical care expenditures is inadequate. In its 2008 National Scorecard on U.S. Health System Performance, the Commonwealth Fund reported on 37 indicators of performance spanning access, quality, efficiency, equity, and healthy lives (Davis et al., 2008). The report uses benchmarks from top-performing countries, U.S. states, regions, and health plans. In 2008, the US health system achieved an overall score of 65 compared with a possible 100. It ranked unfavorably on numerous indicators, including measures of mortality (such as infant mortality), effective and coordinated care (such as screening rates and hospital readmissions), patient-centered and timely care, access problems due to cost, and efficiency (for example, Medicare costs for chronic disease and emergency-room use for nonurgent conditions). US clinical care system performance on equity demonstrated numerous outcome disparities in risk ratios for selected measures, comparing those
with high and low incomes, comparing whites with Hispanics or blacks, and comparing insured with uninsured persons (Doty and Holmgren, 2006; Schoen et al., 2008). In a 2010 update of the scorecard, US clinical care system performance was compared with that of Australia, Canada, Germany, the Netherlands, New Zealand, and the United Kingdom. The US clinical care system ranked last or next-to-last in all five dimensions of high-performance examined (access, quality, cost, equity, and healthy lives) (Davis et al., 2010).
The national preoccupation with the cost of clinical care is well founded, and the need for change is urgent. However, improving the clinical care delivery system’s efficiency and effectiveness will probably have only a modest effect on the overall health of the population (see McGinnis and Foege, 1993; Woolf et al., 2010). Some effort has been made to estimate the preventable mortality (the rate of death due to all preventable causes, such as behaviors and environmental exposures, excluding largely unavoidable factors, such as genetics) that could be attributed to “shortfalls in medical care” (McGinnis et al., 2002). Although more work is needed to estimate the contributions of this and the other determinants of health, clinical care appears to explain only a portion of preventable mortality (see, for example, Nolte and McKee, 2008; Woolf et al., 2007).2 For example, McGinnis and colleagues (2002) estimated that 10–15 percent of preventable mortality could be reduced by improvements in the availability or quality of clinical care. A complementary way to measure the effect of various factors on population outcomes is to consider changes in life expectancy (for example, departures from the baseline provided by annual US statistics on life expectancy at birth). A Department of Health and Human Services report found that about 5 of the 30 years of increased life expectancy realized by Americans in the 20th century could be attributable to better clinical care (HHS et al., 1994). Cutler and colleagues (2006) estimated that as much as 50 percent of life-expectancy gains could be ascribed to advances in clinical care. Even if the 50 percent gains were validated, substantial gains are to be found outside the clinical care system.3
The ACA put into motion processes for comprehensive reform of the clinical care system in the United States (HHS, 2010a). Major reform objectives in the act dealt with broadening clinical-insurance coverage, reforming insurance practices, and improving aspects of the delivery of clinical care. The act also offers an opportunity to integrate parts of clinical care and public health efforts better to improve population health in
|
BOX 1-2 Provisions of the Patient Protection and Affordable Care Act and the Health Care and Education Affordability Reconciliation Act (Jointly, the Affordable Care Act [ACA]) Several ACA provisions are focused on prevention and wellness, including
|
the United States—actions ranging from improved delivery of effective clinical preventive services to population-based interventions that include broad changes in the many dimensions (social, physical, and economic) of the environment for health (see Box 1-2 for a list of the law’s provisions of greatest relevance to public health and to this committee’s work). Provisions pertaining to prevention and wellness offered in the act include the requirements for an absence of cost-sharing for recommended preventive services, for linking health-insurance premiums to participation in health-promotion programs, for public health workforce development (authorizes new training and placement programs for public health workers), and for community-based prevention activities. New community-based, prevention-focused grant programs have been created to target common modifiable risk factors rather than specific diseases. For example, community transformation grants will help local communities to address “policy, environmental, programmatic, and infrastructure changes needed to promote healthy living
|
and reduce health disparities” (Public Law 111-148). The act also provides for community-based prevention activities through new regulatory and revenue authorities (for example, restaurant menu and vending-machine labeling requirements, mandatory break time for nursing mothers, and a 10 percent tax on indoor tanning services). In another provision of particular relevance to the present report (described more fully in Chapter 2), the act calls for a key national indicator system that will include health and is to be constructed with guidance from the National Academies.
CHARGE TO THE COMMITEEE
Recognizing the potential of systems-oriented public health approaches to achieve greater improvement in population health outcomes than changes in clinical care alone, the Robert Wood Johnson Foundation asked the Institute of Medicine (IOM) to convene a committee to review population health
|
BOX 1-3 Charge to the Committee on Public Health Strategies to Improve Health The committee will review population health strategies, associated metrics, and interventions in the context of a reformed health care system. The committee will review the role of score cards and other measures or assessments in summarizing the impact of the public health system, and how these can be used by policy-makers and the community to hold both government and other stakeholders accountable and to inform advocacy for public health policies and practices. |
strategies, associated metrics, and interventions in the context of a reformed health care system. The Committee on Public Health Strategies to Improve Health was also asked (in the words of the charge given by the Robert Wood Johnson Foundation) to “review the role of score cards and other measures or assessments in summarizing the impact of the public health system, and how these can be used by policy-makers and the community to hold both government and other stakeholders accountable and to inform advocacy for public health policies and practices” (see Box 1-3).
The committee used two evidence-based notions as the starting point for its report. First, the committee believes that health strategies, interventions, and policies applied at the population level can advance current approaches to our nation’s most pressing health concerns (such as obesity, infant mortality, injuries, cardiovascular disease, and health inequities) more efficiently and effectively than can isolated, intensive individual-level actions within the clinical care sector (see, for example, Woolf et al., 2007, estimating the effect on mortality of changes in one of the determinants of health, education). The Task Force on Community Preventive Services, which regularly reviews and evaluates research, has shown that strong evidence supports recommending some population-based interventions, such as reductions in blood alcohol concentration for their effectiveness in decreasing motor-vehicle injuries and deaths, and increases in prices of tobacco products for their effect on smoking initiation (Shults et al., 2001). The task force also recommends multicomponent interventions of several kinds: strong evidence was found to support mass-media campaigns in combination with other multisectoral strategies, including tobacco-price increases, school-based education, and other community education programs (Hopkins et al., 2001; Task Force on Community Preventive Services, 2001). The evidence base will grow as the task force’s work expands with funding under the ACA and as the Cochrane Public Health Group (which published its first systematic
review in February 2010, linking flexible work conditions with improved health) and other evidence-review bodies continue their work.
Second, the committee believes that measuring health outcomes and their determinants at both the individual level and the community level and in multiple sectors is an essential ingredient, with policy and resources, in motivating change, mobilizing action, measuring progress, and improving performance. As the clinical care community learned first, data can help to drive important improvements in performance (Berwick et al., 2003; Galvin and McGlynn, 2003). For the purposes of the more broadly conceived health system, data can also inform advocacy, public policy, and allocation of resources and can lead to better population health outcomes. High quality of data and measures is a prerequisite for good results—for example, how well does the evidence link indicators to the outcomes being measured (see, for example, Chassin et al., 2010)? The committee will address other “ingredients for change” in two future reports, on the law and on funding in the context of public health.
An important consideration in the ability to manage intersectoral collaboration among parts of the government and partnerships among government agencies and the private sector is the quality of governance—the ability to align potentially divergent interests toward a shared goal at local (city and county), state, and national levels. Because a public health agency is only one actor among many, there is increasing emphasis on engaging the highest-level elected officials, whether mayors, governors, or the president, to promote Health-in-All Policies—an approach that considers the implications on population health of policies in other sectors of government (e.g., transportation, land use, agriculture) and that uses such tools as health impact assessments, described elsewhere in this report (Kickbusch and Buckett, 2010; Stahl et al., 2006). The topic of governance is discussed briefly in Chapter 4 and will be addressed in more detail in the later report on the law and population health.
KEY TERMS
In its deliberations and in this report, the committee used the definition of the public health system provided in the 2003 IOM report The Future of the Public’s Health in the 21st Century—an intersectoral, multistakeholder system whose core is the government public health infrastructure but also includes business, the clinical care delivery system, communities, schools, and nonprofit organizations (IOM, 2003). The 2003 figure (see Figure 1-1) did not explicitly refer to other components of government, but the current committee’s report refers directly to the contributions of other government agencies or sectors that influence population health (such as those in trans-
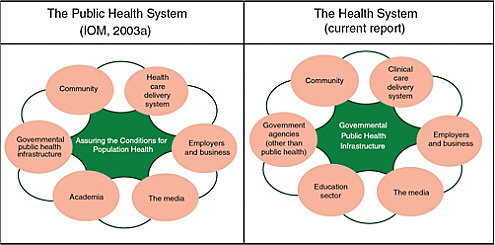
FIGURE 1-1 The health system.
NOTE: The present committee used the 2003 IOM committee’s figure of the circle of system partners and description of the system (IOM, 2003) but renamed the system and made three revisions in the figure. They include placing the government public health infrastructure at the center, making it clear that other government agencies (non–public health agencies, including transportation, education, and others) are also key actors in the circle, and replacing health care with clinical care. The government public health agencies are in the center not because they are the most important in the population health system but because they are specifically tasked with ensuring the health of the public through their actions and by working with and through others. An additional change (Academia is now referred to as Education sector) acknowledges the considerable current and potential contributions of schools of all types to health.
portation, environment, economic development and land use planning, and education).
The overall public health system represented in Figure 1-1 is renamed simply the health system, with the health care delivery oval described more specifically as the clinical care delivery system. The modifiers public and population are poorly understood by persons other than public health professionals; use of them has made it both harder to understand that public health is about the population as a whole and easier to misinterpret or overlook the collective influence and responsibility that all sectors have for creating and sustaining the conditions necessary for health. In describing the system that comprises public health agencies, the clinical care delivery system, communities, and other partners as the health system, the committee seeks to reclaim the proper and evidence-based understanding of health not merely as clinical care but as the entirety of what we do as a society to create the conditions in which people can be healthy (IOM, 1988). The committee viewed as critical the need to focus policy-makers and the public
on the complex interactions of multiple sectors that contribute to the production and maintenance of the health of Americans and the need to place contributions of the clinical care delivery system in perspective, including helping the public to understand the performance of the clinical care delivery system and its effects on population health.
In the present report, the committee uses the term indicator to refer to quantitative information that represents or is derived from statistics or measures (terms used interchangeably in the statistics community) that are developed by federal statistical agencies and other producers of data. Indicators are designed to be communicated to policy-makers or to the public. They may be simple (such as a disease-specific death rate in a particular age group) or complex (such as a composite figure that incorporates several types of data, for example, the Human Development Index4). Indicators are available for most steps in the process to health improvement—that is, indicators of resources; of capacities; of interventions, processes, and policies; of health outcomes; and performance. The term information is used, as in the 2003 IOM report, to refer generally to three distinct terms in information science: data, information (data put into context through analysis), and knowledge (Lumpkin, 2001).
TWO PARADIGMS
The committee contrasted two health paradigms and two corresponding approaches: the biomedical (or clinical) paradigm and the broader ecologic (or determinants-of-health) paradigm. Into the early part of the 20th century, changes in the means of production and in sanitation led to vast decreases in infectious disease and improvements in quality of life. In the latter half of the 20th century, biomedical science and greater understanding of the biologic basis of disease strongly shaped expert and popular understanding of the causes of poor health (CDC, 1999). The results were a proliferation of diagnostic and therapeutic technologies designed for individuals and, in time, the emergence of the biomedical model as the dominant paradigm for viewing health and its improvement (Fielding et al., 2010). The biomedical model is also associated with the emergence of insurance mechanisms to pay for new technologies and interventions and with the large increases in costs. The two paradigms are complementary, and a balanced investment in both would create health policy that produces improved health.
The World Health Organization has defined health as “a state of physical, mental and social well-being and not merely the absence of dis-
ease or infirmity” (WHO, 1948).5 Public health has been defined as “what we, as a society, do collectively to assure the conditions for people to be healthy” (IOM, 1988, 2003). The ecologic (or determinants-of-health and population-based) health model encompasses but is much broader than the clinical model, which is focused on pathophysiologic causes of individual risk factors for disease and injury. The perspective that informs the ecologic model is rooted in an examination of the “relationship between the innate biologic characteristics of individuals and their interactions with their peer groups, families, communities, schools and workplaces, as well as the broad economic, cultural, social, and physical environmental conditions at the local, national, and global levels” (Fielding et al., 2010, p. 176).
The committee reiterates an illustration of the determinants of health provided in the 2003 IOM report The Future of the Public’s Health in the 21st Century (IOM, 2003; see Figure 1-2). The clinical care model focuses largely on the two innermost circles (individual genes and biology, features of a disease, and behavior). In contrast with the highly specialized and individualized approaches of clinical medicine, health-improvement strategies that stem from the ecologic model are developed to address social and physical environments that influence patterns of disease and injury and human responses to them over the life cycle (Kindig and Stoddart, 2003). Interventions reflecting the latter (ecologic) model—from policies on air quality and living wages to health-promotion programs that target nutrition and physical activity—may have wide-ranging effects on multiple disease states (see Table 2-1 for examples). A healthy community has been described in various ways: for example, one where all sectors contribute to create social and physical environments that foster health. In practice, such a community meets basic needs: access to affordable, healthy foods; affordable housing and transportation; and such essential services as medical care and education. It offers a sustainable, healthful environment with clean air and water, open space and parks, low levels of toxic exposures and low emissions, and affordable, sustainable energy (Fielding et al., 2010). The present report argues that data can help communities to assess their status in those respects and to take steps to improve conditions for health with the ultimate goal of improving population health outcomes.
Human behavior of individuals (the second circle from the center in Figure 1-2) is strongly conditioned by people’s social frame of reference and relationships; such social institutions as school, religious congregations, and workplaces; income and economic conditions; and physical environments (see, for example, Evans et al., 1990). It is also influenced by
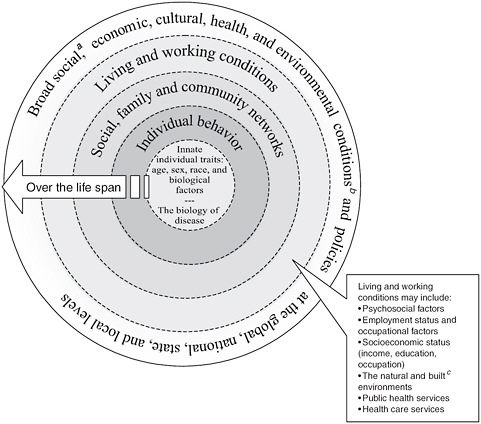
FIGURE 1-2 A guide to thinking about the determinants of population health.
a Social conditions include economic inequality, urbanization, mobility, cultural values, and attitudes and policies related to discrimination and intolerance on the basis of race, sex, and other differences.
b Other conditions at [the] national level might include major sociopolitical shifts, such as recession, war, and government collapse. The built environment includes transportation, water and sanitation, housing, and other dimensions under [the] auspices of urban planning.
c The built environment includes transportation, water and sanitation, housing, and other dimensions of urban planning.
SOURCE: Adapted from Dahlgren and Whitehead (1991). Dotted lines between levels of model denote interaction effects between and among various levels of health determinants (Worthman, 1999).
genetic constitution (the innermost circle), whose expression is in turn affected by interactions with environmental conditions. Inputs from multiple sectors correspond to determinants of health in diverse ways. For example, the social environment—which includes social capital, safety, and school policies—can be addressed through interventions for access to healthy food,
agricultural policy, cultural programming, and physical activities. Economic determinants, such as income and employment, can be addressed through living-wage policies, unemployment support, and retraining. Measures of those domains may assess social well-being or fresh-food availability, policy effectiveness, and program use.
The Evidence on Determinants of Health
Recognition of the determinants of health is well documented, but several milestones warrant highlighting, including Geoffrey Rose’s Strategy of Preventive Medicine (1992), which examined patterns of disease in populations; Evans and Stoddart’s article “Producing Health, Consuming Health Care” (1990); and the 2008 report of the World Health Organization Commission on Social Determinants of Health, Closing the Gap in a Generation: Health Equity Through Action on the Social Determinants of Health (Commission on Social Determinants of Health, 2008).
A robust and expanding peer-reviewed literature addresses the associations between the upstream determinants of health—social, economic, and environmental—and poor health outcomes and between socioeconomic inequality and poor health. Researchers have found that poverty, low levels of education, lower social status, and income inequality are linked with higher mortality and higher rates of poor health, with more or stronger evidence regarding some conditions (see, for example, Berkman and Kawachi, 2000; Carstairs and Morris, 1989; Daniels et al., 2000; Kaplan, 1996; Kennedy et al., 1998; Kogevinas et al., 1991; Marmot and Wilkinson, 1999). The Whitehall I and II studies of British civil servants, which controlled for an array of variables but still found a steep difference in mortality between the highest and lowest grades of civil-service employment, remain classics of the literature on determinants of health (Marmot et al., 1991). Neighborhood conditions (including deprivation, poor housing, violence, and other stressors) are also associated with worse health status (Ellen et al., 2001; Kawachi and Berkman, 2003; Yen and Kaplan, 1999).
Epidemiologists studying the relationships between health and the social environment generally describe three dimensions: the role of socioeconomics (for example, income, employment, and education); the role of social structure (for example, social institutions and phenomena, including discrimination and income inequality); and the quality of the social, built, and natural environment (for example, social cohesion, social capital, and civic engagement). The peer-reviewed literature contains evidence on the social environment and its relationship to asthma (Cagney and Browning, 2004; Williams et al., 2009; Wright, 2006) and to health risk behaviors, such as smoking (Kleinschmidt et al., 1995; Shohaimi et al., 2003); evidence on its relationship to birth weight shows the transgenerational effect of neighbor-
hood poverty during pregnancy (Collins et al., 2003, 2009; O’Campo et al., 1997; Schempf et al., 2009). And an increasing body of evidence sheds light on the relationship between access to healthy food and obesity (California Center for Public Health Advocacy et al., 2008; Larson et al., 2009; Morland et al., 2006). The mechanisms by which socioeconomic conditions can influence health outcomes, such as asthma, include chronic exposure to social stressors that can lead to changes in the brain and the immune system (Lantz and Pritchard, 2010).
The built environment (land use patterns, the transportation system, and design features) has seen increased research attention in recent years. Although there are still gaps in the evidence base and conceptual complexities (given the many mediators at work, including social and cultural variables and such psychosocial factors as feelings of safety and security), the influence of the built environment in constraining or facilitating physical activity is increasingly clear (TRB and IOM, 2005).
The Evidence on Interventions to Address Determinants of Health
Altering root causes (the determinants of health) to create healthy communities is challenging because they form or are woven into the very fabric of family, community, and societal structures. Strong, supportive families and communities foster safe, secure environments and build social capital. Public-sector and private-sector structures and systems, through policies and norms, provide social infrastructure and shape lives. Linear6 approaches involving one or two sectors to solve such complex health challenges will necessarily be modest in effect (Leischow and Milstein, 2006). Broad action on multiple determinants involving multiple sectors is needed to achieve greater effects on population health.
Unlike clinical interventions that focus on downstream factors (for example, individual-level factors), such as using prescription medication to lower blood sugar concentrations or blood pressure, population health interventions by public health agencies and their partners can address a broader spectrum of causation ranging from proximal conditions that lead to unhealthy behaviors and exposures in communities to sick people’s need for services in the medical care delivery system. Upstream strategies (aiming to affect root causes or underlying issues before they lead to poor individual health outcomes downstream) include policies and interventions that affect the social and physical environments, as illustrated in Table 2-1. These strategies demonstrate the versatility of population health interventions in reducing the burden of illness and injury and in advancing wellness by altering conditions that affect what people eat, drink, breathe, inhabit, work and
play with, and use (CDC, 1999; Frieden, 2010). There is also evidence that interventions in two components of the built environment—land use (for example, accessibility of public recreational venues) and transportation—can affect community health (Bauman and Bull, 2007; Davison and Lawson, 2006; Ewing et al., 2002; Handy et al., 2002) in areas that relate to physical activity, healthy eating, and obesity (Brownson et al., 2006).
Bold changes in clean air laws and tobacco taxes helped to transform social norms and led to reductions in cigarette-smoking. Box 1-4 shows how interventions at the population level can offer greater returns on investment than can clinical care alone.
Evidence on the effectiveness of interventions is more substantive when one considers the intermediate determinants and outcomes, such as behaviors that are risk factors for chronic disease (as described above). As one moves further upstream, to the outermost ring of the illustration in Figure 1-2, although strong evidence links health outcomes to various dimensions of the socioeconomic environment (such as education, income, housing and neighborhood quality, social cohesion, and social capital) and suggests some potential loci for interventions, there is still a dearth of evidence on the most effective interventions on many topics (see Bambra et al.,
|
BOX 1-4 Value of Population-Level Interventions Interventions at the population level (such as smoking laws, school programs, and motor-vehicle safety laws) can have greater cost savings than those at the individual level. For example, medical care accounts for the largest proportion of the direct costs of smoking. “Men who smoke incur $15,800 (in 2002 dollars) more in lifetime medical expenses than non-smokers, and women who smoke incur $17,500 more than non-smokers.” In 1999, the state [CA] “spent $8,564,623 in total health care costs directly attributable to smoking, including $4,016,568 in hospital care, $2,060,234 in outpatient care, and $1,133,432 for prescriptions” (California Benefits Review Program, 2006). A 2009 RAND study shows that reducing Americans’ average intake of sodium to the amount recommended by health officials could save the nation billions of dollars annually in avoided medical care costs and improve the quality of life of millions of people (RAND, 2009). The study estimates that meeting national sodium guidelines could eliminate 11 million cases of high blood pressure nationally. In just one calendar year, that would save 312,000 quality-adjusted life years with a monetary value of an estimated $32 billion (Palar and Sturm, 2009). Population-based strategies (such as redesigning food-labeling information and manufacturers’ voluntarily lowering of sodium concentrations in their products) would have multiple health effects (such as avoiding hypertension and the resulting cardiovascular disease and treatment) (Bibbins-Domingo et al., 2010). |
2010). Several examples—the US Head Start Program (Administration for Children and Families, 2010) and other early child-development programs, such as the Nurse-Family Partnership (Olds, 2002; Olds et al., 2007), or early academic-enrichment programs (Reynolds et al., 2007)—suggest that addressing the more upstream determinants of health can be effective. The remaining conceptual and methodologic challenges and gaps include defining socioeconomic environments and elucidating the complex and interrelated pathways between many determinants and health outcomes of interest. For example, higher levels of educational attainment are strongly linked with better health outcomes, but there are multiple confounding influences, including neighborhood conditions, early life experiences, and race and ethnicity (Woolf et al., 2007). And there are challenges in linking specific determinants of health to specific outcomes and, in cases in which the evidence of an association is strong, in establishing what interventions are most effective in addressing the determinants of health.
A primary challenge in research on population-based interventions is that the traditional gold standard technique of randomized controlled trials is not always feasible or appropriate in the public health context (for example, given the complexity of causal factors and the levels on which interventions function). However, other statistical techniques (such as observational studies and quasi-experimental study designs) may be used (Rosenbaum, 2002, 2010), as may tools offered by other disciplines (such as economics and the social sciences), to demonstrate the effectiveness of public health approaches. Such tools as health impact assessments can lead to syntheses of the best available evidence, and predictive modeling can supplement the evidence base (see, for example, Thomson et al., 2008). An additional contributor to the dearth of evidence about what works to address specific determinants of health are deficiencies in the reporting of public health intervention research (Armstrong et al., 2008).
MEETING THE CHARGE
To meet its charge, the committee reflected on the implications of the Affordable Care Act and the case for moving toward a population health approach as seen through the lens of measurement of health outcomes and system performance. The committee held three information-gathering meetings on public health measurement and reviewed the relevant literature (peer-reviewed journals and reports and white papers). Each meeting involved an array of stakeholders (see the agendas in Appendix C). After each information-gathering meeting, the committee met in closed session (and held two additional meetings that were closed to the public) to allow committee deliberation and discussion. In this report’s remaining three chapters (and seven recommendations), the committee discusses measurement-based
system improvements to support all partners in the health system, from the public health agencies and their clinical care counterparts to various community and private-sector organizations, in becoming more knowledgeable about population health outcomes and their determinants and in developing, implementing, and evaluating programs, policies, and interventions to improve health.
WHAT THIS REPORT DOES NOT ADDRESS
As discussed in this chapter and throughout the report, a population’s health is influenced by a multitude of factors that overlap and span many disciplines and topics. The committee aims to cover many of the topics through its three reports—the present one and two later ones. Each is intended to view population health improvement through a different lens (measurement, the law, and funding). The preface of this report describes the areas of overlap among the three overarching topics and explains that although each has unique characteristics and effects on health, none can be looked at exclusively without discussing the others. In the present report, on measurement and health, the committee uses the scope of measurement as a tool to improve population health. This report focuses on measurement and on the US population health statistics and information system (which collects, analyzes, and reports population health data, clinical care data, and health-relevant information from other sectors). However, it is important to note that the committee did not attempt to prepare a comprehensive and systematic catalog or evaluation of all activities (national, state, and local) to put forth health indicators or indicators of well-being. The committee referred to two overviews of indicator efforts in the health field (Public Health Institute, 2010; Wold, 2008) and a more general summary of key indicators (on multiple topics beyond health, including the economy, society, and the environment) contained in the Government Accountability Office’s report Informing Our Nation: Improving How to Understand and Assess the USA’s Position and Progress (GAO, 2004).
This IOM report notes topics for later reports of the committee, but it does not examine them in any depth. For example, many of the committee’s recommendations (in Chapters 3 and 4) call for increases or changes in resources, staffing, or allocations of funds. Other subjects related to measurement that the committee will review in more detail in its later reports on the law and funding include
-
accountability,
-
governance (and governing bodies),
-
innovative ways to use the law on the basis of what is learned though measurement,
-
inadequacy of resources available to government statistical agencies,
-
allocation of funding for public health agencies,
-
the mismatch between the targets of public health funding and the leading causes of preventable deaths and illnesses,
-
the public health role in monitoring clinical care quality and outcomes through the use of personal health information, and
-
the effects of health care reform on the structure of public health agencies.
The committee continues to hold information-gathering meetings and to research public health law and funding, and the issues noted above and other issues identified during that process will be raised in its two forthcoming reports.
REFERENCES
Administration for Children and Families. 2010. About the Office of Head Start. http://www.acf.hhs.gov/programs/ohs/about/index.html#factsheet (November 3, 2010).
Armstrong, R., E. Waters, L. Moore, E. Riggs, L. G. Cuervo, P. Lumbiganon, and P. Hawe. 2008. Improving the reporting of public health intervention research: Advancing trend and consort. Journal of Public Health 30(1):103-109.
Bambra, C., M. Gibson, A. Sowden, K. Wright, M. Whitehead, and M. Petticrew. 2010. Tackling the wider social determinants of health and health inequalities: Evidence from systematic reviews. Journal of Epidemiology and Community Health 64(4):284-291.
Bauman, A. E., and F. C. Bull. 2007. Environmental Correlates of Physical Activity and Walking in Adults and Children. London, England: National Institute of Health and Clinical Excellence.
Berkman, L. F., and I. Kawachi, eds. 2000. Social Epidemiology. New York: Oxford University Press.
Berwick, D. M., N. A. DeParle, D. M. Eddy, P. M. Ellwood, A. C. Enthoven, G. C. Halvorson, K. W. Kizer, E. A. McGlynn, U. E. Reinhardt, R. D. Reischauer, W. L. Roper, J. W. Rowe, L. D. Schaeffer, J. E. Wennberg, and G. R. Wilensky. 2003. Paying for performance: Medicare should lead. Health Affairs 22(6):8-10.
Bibbins-Domingo, K., G. M. Chertow, P. G. Coxson, A. Moran, J. M. Lightwood, M. J. Pletcher, and L. Goldman. 2010. Projected effect of dietary salt reductions on future cardiovascular disease. New England Journal of Medicine 362:590-599.
Booske, B. C., J. K. Athens, D. A. Kindig, H. Park, and P. L. Remington. 2009. Different Perspectives for Assigning Weights to Determinants of Health: County Health Rankings Working Paper. Madison: University of Wisconsin Population Health Institute.
Brownson, R. C., D. Haire-Joshu, and D. A. Luke. 2006. Shaping the context of health: A review of environmental and policy approaches in the prevention of chronic diseases. Annual Review of Public Health 27(1):341-370.
Cagney, K. A., and C. R. Browning. 2004. Exploring neighborhood-level variation in asthma and other respiratory diseases—the contribution of neighborhood social context. Journal of General Internal Medicine 19(3):229-236.
California Benefits Review Program. 2006. Criteria and Guidelines for the Analysis of Long-Term Impacts on Healthcare Costs and Public Health: California Health Benefits Review Program. Oakland, CA: University of California, Office of the President.
California Center for Public Health Advocacy, PolicyLink, and UCLA Center for Health Policy Research. 2008. Designed for Disease: The Link Between Local Food Environments and Obesity and Diabetes. Los Angeles, CA: UCLA Center for Health Policy Research.
Carstairs, V., and R. Morris. 1989. Deprivation and health. British Medical Journal 299(6713): 1462-1462.
CDC (Centers for Disease Control and Prevention). 1999. Ten Great Public Health Achievements—United States, 1900-1999. http://www.cdc.gov/mmwr/preview/mmwrhtml/00056796.htm (September 8, 2010).
Chassin, M. R., J. Loeb, and S. P. Schmaltz. 2010. Accountability measures—using measurement to promote quality improvement. New England Journal of Medicine 363:683-688.
Collins, J. W., Jr., R. J. David, N. G. Prachand, and M. L. Pierce. 2003. Low birth weight across generations. Maternal and Child Health Journal 7(4):229-237.
Collins, J. W., Jr., J. Wambach, R. J. David, and K. M. Rankin. 2009. Women’s lifelong exposure to neighborhood poverty and low birth weight: A population-based study. Maternal and Child Health Journal 13(3):326-333.
Commission on Social Determinants of Health. 2008. Closing the Gap in a Generation. Geneva, Switzerland: World Health Organization.
Commonwealth Fund. 2009. The Path to a High Performance US Health System: A 2020 vision and the policies to pave the way. New York: Commonwealth Fund.
Cutler, D. M., A. B. Rosen, and S. Vijan. 2006. The value of medical spending in the United States, 1960–2000. New England Journal of Medicine 355(9):920-927.
Dahlgren, G., and M. Whitehead. 1991. Policies and strategies to promote social equity in health. Stockholm, Sweden: Institute for Future Studies.
Daniels, M. J., F. Dominici, J. M. Samet, and S. L. Zeger. 2000. Estimating particulate matter-mortality dose-response curves and threshold levels: An analysis of daily time-series for the 20 largest U.S. cities. American Journal of Epidemiology 152(5):397-406.
Davis, K., C. Schoen, K. Shea, and C. Haran. 2008. Aiming high for the U.S. health system: A context for health reform. The Journal of Law, Medicine & Ethics 36(4):629-643.
Davis, K., C. Schoen, and K. Stremikis. 2010. Mirror, Mirror on the Wall: How the Performance of the U.S. Health Care System Compares Internationally—2010 update. Washington, DC: Commonwealth Fund.
Davison, K., and C. Lawson. 2006. Do attributes in the physical environment influence children’s physical activity? A review of the literature. International Journal of Behavioral Nutrition and Physical Activity 3(1):19.
Doty, M. M., and A. L. Holmgren. 2006. HealthCare Disconnect: Gaps in Coverage and Care for Minority Adults. Findings from the Commonwealth Fund Biennial Health Insurance Survey (2005). New York: The Commonwealth Fund.
Ellen, I. G., T. Mijanovich, and K. N. Dillman. 2001. Neighborhood effects on health: Exploring the links and assessing the evidence. Journal of Urban Affairs 23(3-4):391-408.
Evans, R. G., M. L. Barer, and T. R. Marmor, eds. 1990. Why are Some People Healthy and Others Not?: The Determinants of Health of Populations. New York: Walter de Gruyter.
Evans, R. G., and G. L. Stoddart. 1990. Producing health, consuming health-care. Social Science & Medicine 31(12):1347-1363.
Ewing, R., R. Pendall, and D. Chen. 2002. Measuring Sprawl and its Impact: Volume 1. Washington, DC: Smart Growth America.
Executive Office of the President, Council of Economic Advisers. 2009. The Economic Case for Health Care Reform. Washington, DC: Government Printing Office.
Fielding, J. E., S. M. Teutch, and L. Breslow. 2010. A framework for public health in the United States. Public Health Reviews 32(1):174-189.
Frieden, T. R. 2010. A framework for public health action: The health impact pyramid. American Journal of Public Health 100(4):590-595.
Galvin, R. S., and E. A. McGlynn. 2003. Using performance measurement to drive improvement—a road map for change. Medical Care 41(1):I48-I60.
GAO (Government Accountability Office). 2004. Informing Our Nation: Improving How to Understand and Assess the USA’s Position and Progress—Report to the Chairman, Subcommittee on Science, Technology, and Space, Committee on Commerce, Science, and Transportation, U.S. Senate. Washington, DC: GAO.
Handy, S. L., M. G. Boarnet, R. Ewing, and R. E. Killingsworth. 2002. How the built environment affects physical activity: Views from urban planning. American Journal of Preventive Medicine 23(2S):64-73.
HealthCare.gov. 2010. Understanding the Affordable Care Act: Introduction. http://www.healthcare.gov/law/introduction (November 12, 2010).
Hewitt Associates. 2009. Health Care Reform: The Perils of Inaction and the Promise of Effective Action. Lincolnshire, IL: Hewitt Associates.
HHS (Department of Health and Human Services). 2010a. Affordable Care Act: Laying the Foundation for Prevention. http://www.healthreform.gov/about/index.html (June 22, 2010).
HHS. 2010b. HHS Awards $16.8 Million to Train Public Health Workforce: Grants Awarded to 27 Public Health Training Centers. http://www.hhs.gov/news/press/2010pres/09/20100913a.html (November 12, 2010).
HHS, Public Health Services, and CDC. 1994. For the Health of a Nation: Returns on Investment in Public Health. Washington, DC: HHS.
Hopkins, D. P., P. A. Briss, C. J. Ricard, C. G. Husten, V. G. Carande-Kulis, J. E. Fielding, M. O. Alao, J. W. McKenna, D. J. Sharp, J. R. Harris, T. A. Woollery, and K. W. Harris. 2001. Reviews of evidence regarding interventions to reduce tobacco use and exposure to environmental tobacco smoke. American Journal of Preventive Medicine 20(2, Suppl 1):16-66.
IOM (Institute of Medicine). 1988. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 2003. The Future of the Public’s Health in the 21st Century. Washington, DC: The National Academies Press.
Kaiser Family Foundation and Health Research and Educational Trust. 2007. Employer Health Benefits 2007 Annual Survey. Menlo Park, CA: Kaiser Family Foundation and Health Research and Educational Trust.
Kaiser Family Foundation and Health Research and Educational Trust. 2009. Employer Health Benefits: 2009 Annual Survey. Menlo Park, CA: Kaiser Family Foundation and Health Research and Educational Trust.
Kaplan, G. A. 1996. People and places: Contrasting perspectives on the association between social class and health. International Journal of Health Services 26(3):507-519.
Kawachi, I., and L. F. Berkman, eds. 2003. Neighborhoods and Health. New York: Oxford University Press.
Kennedy, B. P., I. Kawachi, D. Prothrow-Stith, K. Lochner, and V. Gupta. 1998. Social capital, income inequality, and firearm violent crime. Social Science & Medicine 47(1):7-17.
Kickbusch, I., and K. Buckett. 2010. Implementing Health in All Policies: Adelaide 2010. Adelaide, South Australia: Department of Health, Government of South Australia.
Kindig, D., and G. Stoddart. 2003. What is population health? American Journal of Public Health 93(3):380-383.
Kleinschmidt, I., M. Hills, and P. Elliott. 1995. Smoking behaviour can be predicted by neighbourhood deprivation measures. Journal of Epidemiology and Community Health 49(Suppl 2):S72-S77.
Kogevinas, M., M. G. Marmot, and A. J. Fox. 1991. Socioeconomic differences in cancer survival. Journal of Epidemiology and Community Health 45:216-219.
Lantz, P. M., and A. Pritchard. 2010. Socioeconomic indicators that matter for population health. Preventing Chronic Disease Public Health Research, Practice and Policy 7(4). http://www.cdc.gov/pcd/issues/2010/jul/09_0246.htm (July 9, 2010).
Larson, N. I., M. T. Story, and M. C. Nelson. 2009. Neighborhood environments: Disparities in access to healthy foods in the U.S. American Journal of Preventive Medicine 36(1):74-81.
Leischow, S. J., and B. Milstein. 2006. Systems thinking and modeling for public health practice. American Journal of Public Health 96(3):403-405.
Lumpkin, J. R. 2001. Air, water, places, and data—public health in the information age. Journal of Public Health Management & Practice 7(6):22-30.
Marmot, M., and R. G. Wilkinson, eds. 1999. Social Determinants of Health. New York: Oxford Press.
Marmot, M. G., S. Stansfeld, C. Patel, F. North, J. Head, I. White, E. Brunner, A. Feeney, and G. D. Smith. 1991. Health inequalities among british civil servants: The Whitehall II study. The Lancet 337(8754):1387-1393.
McGinnis, J. M., and W. H. Foege. 1993. Actual causes of death in the United States. Journal of the American Medical Association 270(18):2007-2012.
McGinnis, J. M., P. Williams-Russo, and J. R. Knickman. 2002. The case for more active policy attention to health promotion. Health Affairs 21(2):78-93.
Morland, K., A. V. Diez Roux, and S. Wing. 2006. Supermarkets, other food stores, and obesity: The atherosclerosis risk in communities study. American Journal of Preventive Medicine 30(4):333-339.
National Prevention Health Promotion and Public Health Council. 2010. 2010 Annual Status Report. Washington, DC: HHS.
Nolte, E., and C. M. McKee. 2008. Measuring the health of nations: Updating an earlier analysis. Health Affairs 27(1):58-71.
O’Campo, P., X. Xue, M. C. Wang, and M. Caughy. 1997. Neighborhood risk factors for low birth weight in Baltimore: A multilevel analysis. American Journal of Public Health 87(7):1113-1118.
OECD (Organisation for Economic Co-operation and Development). 2009. OECD Health Data 2009: Statistics and Indicators for 30 Countries. Paris, France: OECD.
Olds, D. L. 2002. Prenatal and infancy home visiting by nurses: From randomized trials to community replication. Prevention Science 3(3):153-172.
Olds, D. L., H. Kitzman, C. Hanks, R. Cole, E. Anson, K. Sidora-Arcoleo, D. W. Luckey, C. R. Henderson, Jr., J. Holmberg, R. A. Tutt, A. J. Stevenson, and J. Bondy. 2007. Effects of nurse home visiting on maternal and child functioning: Age-9 follow-up of a randomized trial. Pediatrics 120(4):e832-e845.
Palar, K., and R. Sturm. 2009. Potential societal savings from reduced sodium consumption in the US adult population. American Journal of Health Promotion 24(1):49-57.
Public Health Institute. 2010. Data Sets, Data Platforms, Data Utility: Resource Compendium. Oakland, CA: Public Health Institute.
RAND. 2009. Lowering Sodium Consumption Could Save US $18 Billion Annually in Health Costs. Santa Monica, CA: RAND Corporation.
Reynolds, A. J., J. A. Temple, S.-R. Ou, D. L. Robertson, J. P. Mersky, J. W. Topitzes, and M. D. Niles. 2007. Effects of a school-based, early childhood intervention on adult health and well-being: A 19-year follow-up of low-income families. Archives of Pediatrics and Adolescent Medicine 161(8):730-739.
Rose, G. 1992. The Strategy of Preventive Medicine. New York: Oxford University Press.
Rosenbaum, P. R. 2002. Observational Studies. 2nd ed., Springer Series in Statistics. New York: Springer.
Rosenbaum, P. R. 2010. A matched observational study. In Design of Observational Studies, Springer series in statistics. New York: Springer. Pp. 153-161.
Schempf, A., D. Strobino, and P. O’Campo. 2009. Neighborhood effects on birthweight: An exploration of psychosocial and behavioral pathways in Baltimore, 1995-1996. Social Science & Medicine 68(1):100-110.
Schoen, C., S. R. Collins, J. L. Kriss, and M. M. Doty. 2008. How many are underinsured? Trends among U.S. Adults, 2003 and 2007. Health Affairs 27(4):w298-w309.
Shohaimi, S., R. Luben, N. Wareham, N. Day, S. Bingham, A. Welch, S. Oakes, and K. T. Khaw. 2003. Residential area deprivation predicts smoking habit independently of individual educational level and occupational social class. A cross sectional study in the norfolk cohort of the european investigation into cancer (EPIC-Norfolk). Journal of Epidemiology and Community Health 57(4):270-276.
Shults, R. A., R. W. Elder, D. A. Sleet, J. L. Nichols, M. O. Alao, V. G. Carande-Kulis, S. Zaza, D. M. Sosin, and R. S. Thompson. 2001. Reviews of evidence regarding interventions to reduce alcohol-impaired driving. American Journal of Preventive Medicine 21(4, Suppl 1):66-88.
Social Science Research Council. 2009. Methodology: The American Human Development Index. Brooklyn, NY: Social Science Research Council.
Stahl, T., M. Wismar, E. Ollila, E. Lahtinen, and K. Leppo, eds. 2006. Health in All Policies, Prospects and Potentials. Finland: Finnish Ministry of Social Affairs and Health.
Task Force on Community Preventive Services. 2001. Recommendations regarding interventions to reduce tobacco use and exposure to environmental tobacco smoke. American Journal of Preventive Medicine 20(2S):10-15.
Thomson, H., R. Jepson, F. Hurley, and M. Douglas. 2008. Assessing the unintended health impacts of road transport policies and interventions: Translating research evidence for use in policy and practice. Biomedical Central Public Health 8:339.
TRB (Transportation Research Board), and IOM. 2005. Does the Built Environment Influence Physical Activity? Examining the Evidence: Special Report 282. Washington, DC: National Academies Press.
Truffer, C. J., S. Keehan, S. Smith, J. Cylus, A. Sisko, and J. A. Poisal. 2010. Health spending projections through 2019. The recession’s impact continues. Health Affairs 29(3):522-529.
WHO (World Health Organization). 1948. WHO definition of health. http://www.who.int/about/definition/en/print.html (September 8, 2010).
Williams, D. R., M. Sternthal, and R. J. Wright. 2009. Social determinants: Taking the social context of asthma seriously. Pediatrics 123 (Suppl 3):S174-184.
Wold, C. 2008. Health Indicators: A Review of Reports Currently in Use. Conducted for The State of the USA. Wold and Associates.
Woolf, S. H., R. E. Johnson, R. L. Phillips, Jr., and M. Philipsen. 2007. Giving everyone the health of the educated: An examination of whether social change would save more lives than medical advances. American Journal of Public Health 97(4):679-683.
Woolf, S. H., R. M. Jones, R. E. Johnson, R. L. Phillips, Jr., M. N. Oliver, A. Bazemore, and A. Vichare. 2010. Avertable deaths associated with household income in Virginia. American Journal of Public Health 100(4):750-755.
Worthman, C. M. 1999. Epidemiology of human development. In Hormones, Health, and Behaviors: A Socio-Ecological and Lifespan Perspective, edited by C. Panter-Brick and C. M. Worthman. Cambridge: Cambridge University Press. Pp. 47-104.
Wright, R. J. 2006. Health effects of socially toxic neighborhoods: The violence and urban asthma paradigm. Clinics in Chest Medicine 27(3):413-421.
Yen, I. H., and G. A. Kaplan. 1999. Poverty area residence and changes in depression and perceived health status: Evidence from the Alameda County study. International Journal of Epidemiology 28(1):90-94.






















