4
Opportunities and Challenges for Those Implementing the ACA
In addition to the impact of the ACA on individuals discussed in Chapter 3, the new law presents a variety of challenges and opportunities for those organizations involved in implementing the different provisions of the Act. Perspectives on health literacy and the law in the context of the commissioned paper were provided by representatives of the federal government health insurer, Centers for Medicare and Medicaid Services (CMS); the private health insurance industry; a voluntary quality accreditation organization; and health system pharmacists.
CENTER FOR MEDICARE AND MEDICAID SERVICES
Frank Funderburk Center for Medicare and Medicaid Services
There are a number of provisions of the ACA that are particularly relevant to the CMS, including:
- Supporting informed consumer decision making;
- Standardizing prescription drug information and insurance plan information;
- Improving communications with diverse, low literacy patients;
- Improving beneficiary-provider communication;
- Encouraging use of new preventive care benefits; and
- Promoting health care system innovation, which is the charge of the new Center for Medicare and Medicaid Innovation.
Funderburk’s team at CMS focuses on using social marketing techniques supported by rigorous consumer testing, an approach that is applicable to both health literacy and to the ACA implementation goals.
Social Marketing
Vulnerable populations within Medicare, Medicaid, and CHIP include patients who are disabled (dual eligible) or have chronic diseases, seniors, low-income individuals and families, and people with low English proficiency. By taking a social marketing perspective in trying to reach these diverse audiences, CMS takes into account health literacy, culture, language, attitudes, perceptions, and “consumer reality,” that is, consumer needs, values, beliefs, motivations, and behaviors. The goal is to identify barriers to individuals taking a more active role in their personal health care. CMS is using plain language and consumer-centered design in its products and materials, and conducting extensive testing of materials and messages. Funderburk referred participants to a recently developed and disseminated CMS toolkit for making written materials more user friendly (http://www.cms.gov/WrittenMaterialsToolkit). A campaign team then helps to develop outreach activities for both general audiences and targeted audiences. An important part of the process is evaluating the behavioral impact of the marketing campaigns, and then refining and repeating the process.
CMS is using social marketing to improve communication activities that are particularly relevant to implementation of the ACA, including communications related to discharge planning, CHIP enrollment, and understanding Medicare choices. One of the specific audiences CMS has been trying to reach is the 2-3 million people who are eligible for, but have not enrolled in, low-income subsidy. This provides them with Medicare Part D prescription drug coverage at no, or very low cost, depending on their income level. CMS has conducted extensive focus groups and individual interviews with a variety of audiences, as well as an experimental field test of direct marketing techniques, to see if the agency could achieve a measurable impact in the number of people in this target audience applying for the subsidy benefit. The data suggest that a carefully constructed CMS letter can increase the application rate for the low-income subsidy if it is written in plain language, provides very simple steps to follow, and includes the phone number of a local contact person. More labor intensive approaches, including one-on-one assistance, were not substantially more effective than the letter, and are much more expensive.
Another area of focus is the Medicare Home Health Compare website (for beneficiaries to compare Medicare-certified home health agencies). The homepage was redesigned based on the results of consumer testing and is now more interesting, understandable, and simpler to use.
Fundeburk also described a discharge planning checklist that is currently being evaluated by several quality improvement organizations. CMS has taken the specific elements of discharge planning and broken them into simple steps so patients and caregivers can read and refer to them when they are being discharged. For example, the checklist reminds them of important questions to ask, gives details about the kind of help they will be needing at home, and provides a place for notes. Preliminary tests with patients, caregivers, and practitioners indicates that this is an effective way to impart important discharge information.
As mentioned in an earlier presentation, the Medicare handbook is a very lengthy and complex document. Unfortunately, Funderburk said, most of the content is legislatively mandated, so CMS is somewhat limited in the ways in which the handbook can be changed. One way the agency is trying to improve it is by making the decision tree a little simpler. A new flow chart takes beneficiaries through a series of choices, for example: Do you want original Medicare or full Medicare Advantage Plan? If you are choosing original Medicare, do you want drug coverage? If yes, consider if you need a Medigap Plan. Testing has indicated that people are finding this flow chart to be helpful (Figure 4-1).
Next Steps
CMS is expanding into alternative communications channels and techniques, such as “edutainment,” creating photo and radio novellas to engage certain populations. The agency is also looking at ways to expand communications to new audiences, working with staff and partners to help them communicate more effectively, and exploring ways to measure population health literacy. The main goal is to not leave people behind, and that means the agency needs to continue to provide materials in a written format, as well as in alternative formats.
The Center for Medicare and Medicaid Innovation, funded under the ACA, is designed to help realize the vision of an ideal health care system through high quality, reduced avoidable costs, and patient- and community-centered care. The approach looks at the health care system as a whole, with the health care consumer as an active part of the system. Health literacy will play an important role in achieving this vision. Funderburk said that the center provides a tremendous opportunity to look at how improvements in health literacy can help build an accountable health care system, and ways in which improvements in health literacy can be
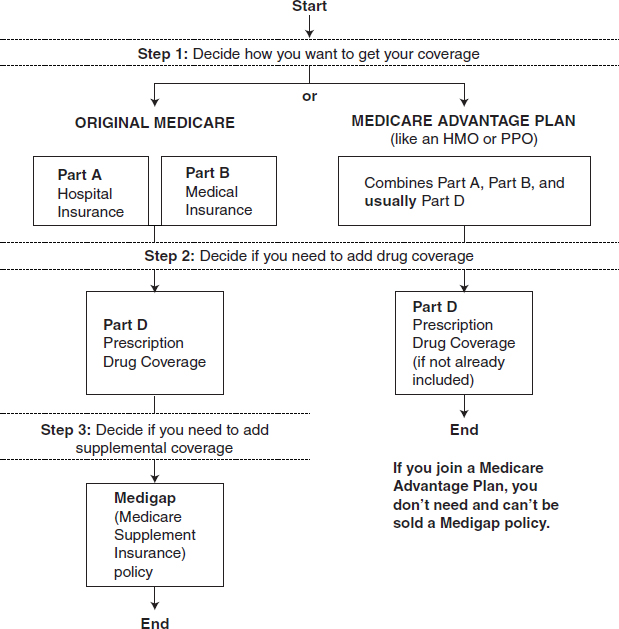
FIGURE 4-1 Flow chart simplifying Medicare choices.
SOURCE: Funderbunk, 2010.
linked to specific behaviors and patient-centered outcomes in environments like the patient-centered primary care environment. (Funderburk noted that in testing, the term medical home was not well received by individuals.) Accountability for improving health literacy could also support more general health care system improvements.
In conclusion, Funderburk said that improved health literacy can help build an accountable health care system; support better consumer decision-making; help reduce avoidable costs; produce better health outcomes; and improve the quality of life of CMS beneficiary populations and the people who care for them.
Susan Pisano, M.A. America’s Health Insurance Plans
The ACA affects every aspect of what insurance companies do, and all of the people they serve and partner with, Pisano began. The major challenges relative to health literacy are also the major challenges relative to implementation of the ACA in general. The specific challenges relative to the health literacy-related provisions in the law are the same challenges that affect efforts to advance health literacy in general. America’s Health Insurance Plans (AHIP) is a national association that represents nearly 1,300 member companies that provide health insurance coverage to more than 200 million Americans. A challenge for many of the member companies is that they are working to build and advance heath literacy programs at the same time that they are trying to implement health care reforms.
While the ACA does not specify that all patient tools, programs, and approaches should be developed using principles of clear health communication, it offers enormous potential to develop tools that are clear, easy to use, and relevant, and for the industry to learn as it goes along. For example, Section 2715 of the ACA calls for standard definitions and uniform explanation of coverage documents. Through focus groups, AHIP learned that consumers like to have a clear, easy-to-use summary, but they also want to know where they can get more detailed information. Providing that link to more information serves two purposes. One is obviously so patients can get the information they need. The other is that the availability of the information signals a level of transparency that engenders trust in the source.
One of the biggest challenges in implementing the ACA, Pisano said, is that health literacy was not a guiding principle in the drafting. What this means is that every coalition that is built and every program that is developed will require somebody to look for the opportunities and step up and take initiative. This is played out in various ways at AHIP, Pisano said. For example, AHIP incorporates health literacy into its comment letters. This may seem like a simple step, but Pisano advises her colleagues to look for every opportunity to incorporate health literacy and cultural competence into the work they are doing. AHIP is also providing tools and resources to member companies as they are developing new programs; encouraging them to take a few initial steps, bring a team together, assess their organizations, develop policies and procedures, make a plan, and train their people. AHIP worked with Emory University on the development of an assessment tool that enables health plans to evaluate if they have the infrastructure that supports good, clear communication. The tool was tested at 18 member companies, including national organizations,
regional companies, and local companies (many of whom serve primarily Medicaid beneficiaries) and is now in general use. Member companies are also using different media approaches to begin to educate the populations they serve about what health care reform is, and what it means for them.
One of the challenges for AHIP is determining where to set the priorities. There are opportunities everywhere, Pisano said, such as in the direct reference to health literacy in drug labeling (Section 3507). Even though insurers are not the locus of information on prescription drugs, AHIP has an opportunity because many of its member companies use personal health records that include beneficiaries’ prescription drug information.
With respect to workforce training, a number of member companies are working with their provider network, using AHIP toolkits, to encourage cross-cultural training of physicians, nurses, case managers, and health plan staff. This is an example of an area that can be built on as reform is being implemented. The primary area that member companies have been working on is how best to engage consumers and make it clear to them what their health benefits allow them to do. Companies have been developing plain language versions of benefits toolkits to support enrollment decisions, and summarizing lengthy documents in clear, one-page charts. With respect to Medicaid expansion, a number of member companies have been developing messaging and materials that incorporate an individual’s cultural beliefs and attitudes about the health care system, including preferred language.
The ACA touches everything that insurers do, Pisano concluded, and these examples show just a few areas in which AHIP member companies are active. A concerted, multistakeholder coordinated strategy to infuse health literacy into the implementation of the law is necessary if we are to achieve the full benefit of health care reform.
Sarah Hudson Scholle, Dr.P.H. National Committee on Quality Assurance
Health reform provides many new opportunities to focus on individuals and choice, equitable care, enrollment, delivery innovations, performance measurement, and engaging patients in shared decision making. But from the perspective of individuals with low health literacy, the ACA actually sets some relatively high expectations and new roles for consumers. It will be important to consider not just whether materials and tools are addressing health literacy needs, Scholle said, but how to get patients, families, and communities activated and engaged in this transformation.
Activated Consumers
Research has shown that activated patients are better consumers (Hibbard, 2009). The more people are participants in their own health care, the more likely they will be taking actions such as researching the qualifications of doctors, recognizing reliable health websites, using health resource books, finding comparative information about hospital quality, or comparing available health plans. These are demanding activities and low health literacy, alone or combined with difficulty understanding the language, makes it very challenging for consumers to get involved to the extent that the legislation expects or requires. People that have the lowest activation are also those with the lowest health literacy.
Scholle noted that the National Committee on Quality Assurance (NCQA) collects and reports data on quality and publishes health care report cards. Most people, however, would not know how to use them. The first step is to present information in a way that consumers can use. At the same time, it is necessary to get consumers to think that the information is, in fact, something that is useful to them. Research suggests that health literacy and activation are independent but related concepts. Scholle suggested that working on this concept of activation or engagement could help to compensate for some of the problems associated with low health literacy.
Opportunities to Engage Consumers
New delivery system approaches, such as the patient-centered medical home and accountable care organizations, have opportunities to support both literacy and patient engagement. These systems provide a locus of accountability and a place where individuals feel like they have a relationship with a trusted partner in their health care. Advances in literacy and engagement can be achieved using aspects of these systems such as health information technology, systematic approaches to care, connections to the community, and care coordination.
The NCQA has built the concept of health literacy into its patient-centered medical home program. It is expected, for example, that patients will receive information about how the practice works (e.g., how to make appointments, request medication refills). Practices should be identifying and documenting cultural and linguistic needs, and assessing family social and cultural resources and characteristics. In the process of care, tools such as medication reconciliation can be used to track patient medications. Practices should also be developing individualized self-management plans and providing clinical summaries that are meaningful to patients and their families. This also involves assessing patient
readiness and connecting patients with self-management support. Practices should always be measuring and improving patient experiences. To achieve this, Scholle noted, there may be a need for new skills development for practitioners.
The Challenge of Choice
The ACA presents the Medicaid and uninsured populations with the huge responsibility of choosing a health plan. These populations in general have less experience with and knowledge of insurance. Will people know how to enroll? Will they understand what cost sharing, benefits, and networks they should select? Will they know how to choose what is best for them based on both cost and quality?
One approach to helping consumers is the concept of “choice architecture.” Offer consumers an opportunity to have the exchanges picked for them. Offer high-quality, low-cost plan options and identify important plan features by person. Information could be enhanced with some sort of “seal of approval” for low-cost, high-quality plans. Quality measures should be used in setting payments.
The ACA also has requirements or expectations for new quality measures. The NCQA is very interested in patient reported measures of both their experiences of care, and their outcomes over time. The NCQA is looking at cross-cutting measures, and structural and process measures, as well as how best to collect the data, including reaching out to disadvantaged or vulnerable populations.
Research Needs
With the new Center for Medicare and Medicaid Innovation, the NCQA envisions opportunities to address issues around activating patients, providing them with simple information, and giving them the support they need to be involved in self-care decision making. The NCQA also hopes to gather evidence on what tools work, and practical methods for applying them in routine settings. Other areas for research include how to reach out to communities, and how to provide training so that staff can become more involved and engaged in working with patients with similar cultural backgrounds. Throughout all of these efforts, there needs to be a focus on activities that reduce costs and have the most impact on population health.
Gerald McEvoy, Pharm.D. American Society of Health-Systems Pharmacists
Most patients leave a physician’s office with a medication as part of an overall therapy regimen. Effective communication about medications is a key component of effective and safe use of therapy by patients, and is a core competency that will be required of pharmacists as they engage patients more directly in terms of care management. The information that patients encounter ranges from the label on the prescription container, to risk-benefit information, to participating in the decision with their physician as to whether or not they even want to receive a particular treatment. Patients must understand why it is that they are receiving a medicine, and why it is important to their overall health that they take it properly and regularly.
The American Society of Health-System Pharmacists (ASHP) represents pharmacists practicing in hospitals and organized health systems (e.g., acute care, ambulatory care clinics, hospital outpatient pharmacies, home care, long-term care). Pharmacists play a key role in managing medication therapy and reducing preventable harm.
The ACA and Pharmacy
The ASHP has, for many decades, fostered best practices that deal with quality issues for patient care, as well as the provision of information to patients. Historically, providing that information has been a core professional responsibility of pharmacists. Up to this point, much of those efforts involved communicating with other health care professionals, such as providing information to physicians to help them make a decision about a drug. Moving forward under the ACA, a key responsibility of pharmacists will be communicating effectively with patients to help them manage their health care with the medications that they have been prescribed. In this regard, there are a variety of tools that are available to help pharmacies assess their health literacy and training tools.
Disease prevention is another area in which pharmacists have established effective practices, covering areas such as diabetes, hypertension, cardiovascular disease, and tobacco cessation. Patient-centeredness is clearly an element of medication counseling, medication therapy management, and the U.S. Pharmacopeia (USP) prescription container labeling standards. As the key profession with expertise in medication therapy, pharmacists are integral to the collaborative-practice model that is at the core of medical homes. With regard to cultural competency and equity, there are a number of standards that apply to pharmacies (e.g., ASHP best
practice on disparities in health care, Pharm.D. accreditation standards, ASHP residency standards).
Coverage expansion under the ACA will result in increased drug benefit coverage. Pharmacy workforce development is not addressed specifically in the ACA, and McEvoy said that the ASPH will be advocating for the need to include pharmacists as a profession in workforce development programs. With regard to patient information, the FDA is expected to issue new standards for the provision of written information to patients in 2012.
McEvoy highlighted several sections of the ACA that are key areas for pharmacy stakeholders (Box 4-1). Section 3503, addressing medication therapy management services, is the cornerstone of the ACA in terms of pharmacy practice, he said. The goal is to optimize medication use for improved patient outcomes, and to improve communication between patients and the health care team regarding their therapeutic regimen. Section 3507 addresses patient information on risks and benefits, which is most useful when provided at the point of prescribing as opposed to the point of dispensing.
Collaborative Opportunities with Pharmacy
Communication is at the core of all of the opportunities for pharmacies under health care reform. Communicating benefits and risks to both patients and prescribers to facilitate informed decisions about therapy is paramount.
There are special medication risk management issues for the elderly, including concerns about health literacy; polypharmacy and simplifying regimens; adjusted dosing and explaining to patients the importance of taking the prescribed dosage and not altering it on their own; and the use of drugs that may contribute to risks that the elderly face (such as falls). Adherence to drug therapy, risk evaluation and mitigation strategies for high-risk drugs, and medication therapy management are other areas where there are opportunities for pharmacy.
With regard to the patient-centered medical home, most medications require assessment of effectiveness. About one-third of all adverse effects leading to hospitalization are attributable to medication. Only about 30 to 50 percent of patients with chronic conditions adhere to their prescribed medication therapies, and medication cost is an important cause of low adherence. Pharmacists can play an important role in managing therapies by reviewing the therapy that the patient is receiving; identifying cost-effective therapies and optimizing outcomes; resolving medication-related problems; optimizing complex regimens; designing and managing adherence programs; and finally, educating patients about the safe and effective use of their medications.
BOX 4-1
Key ACA Provisions for Pharmacy Stakeholders
- Sec. 3503 Medication therapy management (MTM) services
- Focus on patient-centered rather than product-centered process of care
- Optimize medication use for improved patient outcomes
- Improve communication between patients and the healthcare team
- Sec. 3507 Prescription drug benefit and risk information
- Present patient with benefit-risk information at point of prescribing (i.e., decision point); too late at dispensing point
- Sec. 10328 improve Part D MTM programs
- Support access to MTM by all Medicare Part D beneficiaries
- Sec. 6301 Patient-centered outcomes research
- Submitted nominations to the Patient Centered Outcomes Research Institute
- Pharmacy members of AHRQ’s pharmacy stakeholder advisory committee will recommend comparative effectiveness research and other activities
- Sec. 5307 Cultural competency, prevention, and public health
- Included in education, residency training, and professional practice standards
- Sec. 3021 Center for Medicare and Medicaid Innovation
- Advocate adoption of elements of MTM as part of development and testing of new care models
- Sec. 5305 Geriatric education and training
- Chronic disease testing and treatment, medication reconciliation, cognitive impairment assessment, and wellness guidance for elderly
- Meaningful use of electronic health records
- Patient-centered care models such as medical home
- Pharmacist collaboration for medication therapy services
________________
SOURCE: McEvoy, 2010
Health literacy opportunities include effective communication through the prescription container label, comprehensible patient-centered supplemental materials, and clear counseling, education, and training. One of the elements in the ACA, for example, is testing of a “drug facts box” that came out of research at Dartmouth about patient understanding of risk-benefit information.
Challenges
Among the principal challenges moving forward is the fact that medication therapy is becoming increasingly complex. The more complex therapy becomes, the more difficult it is to explain to the patient the importance of how to take the medication properly, any associated risks with that medication, and what the potential benefits to them as a patient might be. Medications are also becoming increasingly specialized and individualized, pushing the limits of the expertise of the health care professional to effectively explain the therapy. The cost of medications is also increasing. In addition to the communication challenges related to the therapies themselves, the consumer population is aging and becoming increasingly more diverse.
Pharmacy is currently engaged in addressing these challenges. The ASHP Pharmacy Practice Model Initiative, for example, is focused on direct patient care as opposed to delivery of product. The Center for Health Transformation’s 21st Century Intelligent Pharmacy Project is conducting similar pilot work looking at the transformation of pharmacy practice as a key component in providing affordable health care. Other projects are focused on specific diseases, such as the Asheville Project, where pharmacists managed four diseases for the city of Asheville, North Carolina, and the Diabetes Ten City Challenge.
These various programs and pilot projects show how pharmacist involvement in managing therapy with patients can be highly cost-effective, and highly effective in terms of patient outcomes in managing their disease.
Eligibility
A participant shared a hypothetical example of how people who qualify for Medicaid are not necessarily a steady population. Based on changing personal health, employment, and financial circumstances, they can migrate from Medicaid to the health insurance exchange to subsidized coverage by the federal government, and back again. Many are immigrants who have limited English-speaking capability and will be even more challenged to understand when they are eligible to be covered under what program. Funderburk recommended referring people to HealthCare.gov as a starting place, although currently the available languages are limited to English and Spanish. CMS is developing the health insurance portal such that it will ask individuals questions about their current situation and then show them the options that are available to them, allowing them to contrast and compare those options.
Another factor that comes into play for patients on the cusp of eligibility is whether they are being treated for an acute or chronic condition, McEvoy added. A patient with a chronic condition would, it is hoped, be in a managed setting or be engaged in medication therapy management, and would have an advocate, an established, trusted relationship with a provider or practice who can help him or her navigate the coverage process.
Scholle said that under the new standards for medical homes, practices are expected to be asking these kinds of questions and helping patients to determine what coverage they are eligible for. Even better would be a practice that is connected to a community center that can help with language and cultural needs.
Choosing Quality Care
An important market driver of quality is consumer demand. But when considering health care, most people do not know what quality is and as a result, there is no consumer demand for quality health care. Health literacy can help make quality more understandable to consumers. Scholle noted that the NCQA conducted focus groups of people who are treated in medical home practices and others from the same community who are in other practices. People in the medical home model were very happy with their care and understood and appreciated the concept of coordinated care, while the other group was skeptical of the whole idea (although neither was familiar with the term medical home). This supports the idea that there is no consumer demand because consumers often do not know what to demand until they have experienced it. We need to get people to think that managing their health is important, and give them experience with quality health systems that support that care, she said. The choice architecture concept supports this as well, by building decision frameworks that make it easy for people to choose what is good for them, even though they might not understand all of the elements.
Funderburk concurred that choice architecture is critical. The term medical home leads some to believe that they are losing control over their care. Better coordination could be achieved by being transparent and building on existing trusted relationships (e.g., a primary provider gives out his email or mail address and says, “If you go to another doctor, let me know because I think we could work together and make your care better for you”). The patient does not have to be an activated consumer, he or she just has to think that it sounds like a good idea.
Strategies and Interventions
Participants discussed further the concept of a multistakeholder coordinated strategy raised by Pisano. A coordinated effort gives the issue a louder voice, Pisano said. Such a strategy would likely involve some elements of the regulatory process, as well as involvement of consumer organizations. Consumer research would be needed to determine where to focus to achieve the greatest impact, and what should be the priorities. It is not possible to design major programs around every element of the ACA, she noted.
While accountable care organizations are potentially the best way of implementing health literacy practices, the incentives for establishment of ACOs are not yet clearly defined. Scholle said that the goal is to define a care structure that will incentivize provider organizations to work together to achieve the best results for the population with regard to health, reduced costs, and improved patient experiences. This involves motivating patients to become involved in improving their health and avoiding the need for hospitalization. The incentives will likely be financial, and there are opportunities to be involved in helping to define them as various agencies (e.g., the NCQA, CMS) are currently developing standards and calling for comments.
A question was raised about what actually constitutes a health literacy intervention. A participant said that when AHRQ conducted a review of the literature in 2004, they defined a health literacy intervention study as one that assessed the impact of an intervention on those with known limited health literacy. In other words, studies that measured the impact of a program on the overall population were not included, as they could actually be increasing disparities (people with higher health literacy reap most of the benefit while those with lower health literacy are left behind). This is a relatively narrow definition, and there are many relevant interventions that would not necessarily be called health literacy interventions.
Advice for Implementers
A participant asked panelists what their advice would be to those that are now charged with implementing the ACA, in terms of inserting health literacy into program design now, as opposed to having to retrofit it later. Scholle noted that there is no requirement for the reading level of informational materials in the medical home standards, in part because of the burden it would place on small physician practices. There needs to be an easy way to provide plain language materials at the appropriate reading level to practices. Second, workforce training is not just for physicians. A
workforce strategy needs to encompass all health care providers and staff. Funderburk said that providers also need well-designed, simple, step-by-step information and systems so they are not wasting their limited time trying to figure out how to be in compliance. Pisano added that it is critical to engage patients in the implementation process.
This page intentionally left blank.
















