4
Settings of Oral Health Care
The oral health care system is bifurcated with its two parts functioning in almost complete separation; in general, they use different financing systems, serve different population groups, and provide care in different settings. In the private delivery system, care is typically provided in small, private dental offices and financed primarily through employer-based or privately purchased dental coverage and out-of-pocket payments. The safety net, in contrast, is made up of a diverse and fragmented group of providers in various settings. It is financed primarily through Medicaid and the Children’s Health Insurance Program (CHIP), other government programs, private grants, and out-of-pocket payments. (Financing will be discussed more specifically in Chapter 5.) The safety net has an important role providing care to the underserved, but it is limited in its capacity. As discussed in Chapter 3, the nondental health care workforce is becoming increasingly involved in the provision of oral health care. While primary care settings (including private medical offices) should also be seen as settings of care for oral health, this chapter will focus primarily on settings for care provided by dental professionals.
This chapter gives an overview to the delivery of care in both private practices and safety net settings, including descriptions of their patients, staffing, challenges, and successes. The capacity of the system to care for vulnerable and underserved populations will be addressed, as well as particular non-financial challenges. Finally, the chapter concludes with descriptions of innovations occurring across the country to change how and where oral health services are provided in order to meet the needs of vulnerable and underserved populations.
Most dental services are provided in private dental practices owned and staffed by a single dentist. Approximately 92 percent of professionally active dentists work in this private practice model (ADA, 2009a). (See Box 3-1 in Chapter 3 for a description of types of dentists.) About 60 percent of private practice dentists are solo dentists (Wendling, 2010). Thirteen percent of private practice dentists are employees, and 3 percent function as independent contractors (ADA, 2009d). Private practices tend to be located in areas that have the population to support them; thus, there are more practices located in urban areas than rural areas, and more practices are located in high-income than low-income areas (ADA, 2009a; Solomon, 2007; Wall and Brown, 2007).
Staffing
Independent dentists usually employ one or more individuals in the private practice setting, with an average of 4.8 total staff members per dentist (ADA, 2009b). On average, the independent dentist employs 1.3 dental hygienists per dentist and 1.8 chairside assistants per dentist. Nearly 90 percent of independent dentists employ at least one full-time person, and 68 percent employ at least one person who only works part-time. The majority of these dentists employ chairside assistants (94 percent of dentists), secretaries/receptionists (91 percent), and dental hygienists (68 percent). Some independent dentists employ office managers (31 percent), financial coordinators (16 percent), and other personnel such as sterilization assistants and laboratory technicians. However, dental assistants often perform many of these duties.
Workload
Independent dentists work about 47.5 weeks annually and 35.9 hours per week. These dentists spend about 90 percent of their work hours treating patients (ADA, 2009a). In a survey by the American Dental Association (ADA) of the perceived workload of independent dentists, about 20 percent stated they were “not busy enough, could have treated more patients” (ADA, 2009a). Independent general practitioners have an average of 1,871 active patients1 (for single dentist practices) (ADA, 2009a). Independent general practitioners spend about 51 minutes per patient, and their patients have about 3.3 visits per year. Independent specialists spend slightly less time per patient (42 minutes), and the typical patient visits
______________
1 Active patients are commonly defined as those treated within the previous 2 years.
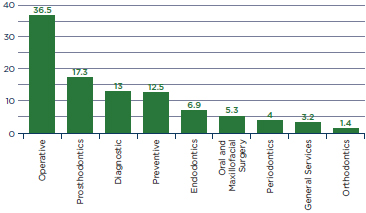
FIGURE 4-1
Percentage distribution of time spent by independent general practitioners in private practice, 2007.
SOURCE: ADA, 2009a.
more frequently (five times per year). Independent general practitioners only spend about one-quarter of their time on diagnosis or prevention (see Figure 4-1). Both new and existing patients wait about a week for a new appointment (a decrease of one full day from 2003). Independent dentists see a little over five walk-in or emergency patients each week. In 2007, independent dentists had about 81 weekly scheduled visits (including dental hygiene appointments).
In the private practices of independent dentists, dental hygienists work, on average, almost 47 weeks per year and 24 hours per week (ADA, 2009b). Dental hygienists see about 25 patients per week. Chairside assistants work almost 48 weeks per year and 32 hours per week.
Patient Population
The patients of independent general practitioners are spread relatively evenly across the age spectrum (see Figure 4-2). Specialists see a significantly greater proportion of patients aged 17 years or less, likely due to the practice profiles of orthodontists and pediatric dentists (ADA, 2009a).
Slightly more than half (55 percent) of independent dentists’ patients are female, and nearly two-thirds (63 percent) have private insurance (ADA, 2009a). Only 7 percent of the patients of independent dentists re-
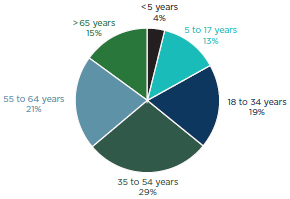
FIGURE 4-2
Age breakdown for patients of independent general practitioners in private practice, 2007.
NOTE: Does not total 100 percent due to rounding.
SOURCE: ADA, 2009a.
ceive public assistance for their dental coverage; the remaining 30 percent of patients are not covered by any dental insurance. Nearly two-thirds of all independent dentists (63.3 percent) and slightly more than half of all new independent dentists (57.5 percent) do not have any patients covered by public sources.
Expenses and Income
In 2007, the average gross billings per owner from the primary private practice for all independent dentists was approximately $774,000 (or about $656,000 per dentist in the practice and $500 per active patient), of which approximately 94 percent was collected2 (ADA, 2009c). Independent dentists in incorporated practices tend to have higher gross billings per owner than those in unincorporated practices. Independent dentists primarily receive payment from private insurance and direct patient payment (see Figure 4-3). Specialists tend to receive less payment from private insurance and more from direct patient payment.
______________
2 Gross billings are the total amount of fees charged. Calculations are made on a per owner basis assuming equal contribution by all partners. Gross billings are only reported for independent dentists who own their private practice.
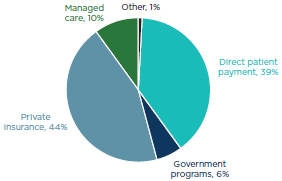
FIGURE 4-3
Sources of gross billings, all independent dentists, 2007.
SOURCE: ADA, 2009c.
In 2007, practice expenses (excluding the salaries of owners, but including the salaries of other employees) accounted for 59 percent of gross billings from the primary private practice of all independent dentists (ADA, 2009c). As discussed in Chapter 3, the salaries of private practice dentists vary depending on employment situation and type of practice. For all independent practitioners, net income does not vary greatly by number of years since graduation. However, this does not take the number of hours worked into account. Between 2003 and 2007, the net income of independent dentists increased about 1 percent annually (when adjusted for inflation) (ADA, 2009c). Between 1982 and 2000, dentists’ real income grew without change to their workload (essentially, the number of patients seen per day and the number of weeks worked per year remained relatively constant) (Guay, 2005). This increase in productivity is, in part, due to the increased use of dental hygienists and dental assistants (Brown, 2005; Guay, 2005). (The capacity and efficiency of the oral health care system is discussed further later in this chapter.)
Demand for dental care may vary with the economic climate of the country (Guay, 2005; Wendling, 2010). For example, the recent recession was identified as a key factor contributing to 2009 having the slowest rate of growth in health spending (4 percent) in the last 50 years (Martin et al., 2011). Notably, expenditures on dental services had a negative rate of growth (-0.1 percent) in 2009, down from a positive rate of growth of 5.1 percent in 2008.
Underserved and vulnerable populations often cannot access the private dental system due to geographic, monetary, or other barriers, and so they rely on the safety net. While the term safety net may give the impression of an organized group of providers available to serve anyone who cannot access the private system, the dental safety net is composed of unrelated entities that both individually and collectively have very limited capacity.
Generally, the safety net is composed of an array of providers, including (but not limited to) Federally Qualified Health Centers (FQHCs), FQHC look-alikes, non-FQHC community health centers, dental schools, school-based clinics, state and local health departments, and not-for-profit and public hospitals. Each type of provider offers some type of dental care, but the extent of the services provided and the number of patients served varies widely. Even with this variety of options, the safety net still does not meet the needs of all who are left out of the private system, often because of a lack of capacity of these providers or a perceived lack of affordable options by individuals (Bailit et al., 2006; Haley et al., 2008; Kenney et al., 2009; Mertz and O’Neil, 2002). The following sections give brief overviews of several types of providers and programs typically considered as part of the safety net.
Federally Qualified Health Centers
An FQHC is any health center that receives a grant established by section 330 of the Public Health Service Act.3 FQHCs must be located in or serve a medically underserved area or medically underserved population, provide both primary health care services as well as supportive services (e.g., education, transportation, translation services), and see patients regardless of their ability to pay for those services. FQHCs are governed by community boards that have a fiduciary responsibility for the center, and more than half of the board members must be patients of the health center and represent the population served. The statute that established FQHCs specifically identifies migratory and seasonal agricultural workers, the homeless, and residents of public housing as underserved populations. Thus, some FQHCs are referred to as Migrant Health Centers, Health Care for the Homeless Programs, and Public Housing Primary Health Care Centers. All of these programs fall under the umbrella term FQHC. FQHCs receive a number of additional benefits in addition to section 330 grants, including higher Medicare and Medicaid reimbursement rates, access to
______________
3 42 U.S.C. §254b.
providers funded by the National Health Service Corps, and drug pricing discounts (HRSA, 2010).
FQHCs primarily provide care to underserved and vulnerable individuals. In 2009, 71 percent of patients served by FQHCs had income at or below 100 percent of the federal poverty level, 93 percent had income at or below 200 percent of the federal poverty level, 38 percent were uninsured, and 37 percent were insured by Medicaid. Table 4-1 illustrates the proportion of FQHC patients who come from vulnerable and underserved populations, as compared to their representation in the U.S. population as a whole.
The FQHC program is growing steadily. In 2009, the Health Resources and Services Administration (HRSA) funded 1,131 FQHCs, which are located in all 50 states, the District of Columbia, and Puerto Rico (HRSA, 2011b). That number is up from 914 FQHCs in 2004. Funding for FQHCs is also increasing. The American Recovery and Rehabilitation Act includes $2 billion for FQHCs (HHS, 2010a), and the health care reform bills includes $11 billion for a Community Health Centers Trust Fund that will allow FQHCs to expand access and make capital improvements, and $1.5 billion for a new National Health Service Corps Trust Fund.4
FQHCs are required to provide certain services—including preventive, but not comprehensive, dental services—either in the clinic or by referral. In 2008, 80 percent of the 1,080 FQHCs provided on-site dental services, and 88 percent provided dental services on site or by referral (Anderson, 2010; Cottam, 2010). This reflects significant progress towards the Healthy People 2020 goal of 83 percent of health centers including an oral health component (HHS, 2010b). In 2009, FQHCs provided dental care to 3.4 million patients, in 8.4 million dental visits, which is nearly a three-fold increase over the number of patients and visits in 2000 (HRSA, 2011c; Ruddy, 2007). This care is not exclusively preventive; although FQHCs are not required to provide comprehensive oral health services, over 75 percent do so, and millions of patients received restorative and rehabilitative care through FQHCs in 2009 (Anderson, 2010; HRSA, 2011b). The expansion of dental services in FQHCs reflects a concerted commitment from HRSA. Since 2001, HRSA has invested $55 million in oral health service expansion grants (Anderson, 2010). In addition, a statutory change in the Children’s Health Insurance Program Reauthorization Act allows FQHCs to expand their reach outside of their physical facilities.5 FQHCs may now contract with private practice dentists to provide oral health services to FQHC
______________
4Patient Protection and Affordable Care Act, Public Law 148, 111th Cong., 2nd sess. (March 23, 2010); Health Care and Education Reconciliation Act of 2010, Public Law 152, 111th Cong. 2nd sess. (March 30, 2010).
5Children’s Health Insurance Program Reauthorization Act of 2009, Public Law 3, 111th Cong., 1st sess. (February 4, 2009), §501.
TABLE 4-1
Underserved and Vulnerable Populations Served in FQHCs as Compared to Their Representation in the U.S. Population, 2009
| Percentage of FQHC Population |
Percentage of U.S. Population |
|
| Poverty | ||
| At or below 100% of poverty | 71 | 14 |
| Medical insurance status | ||
| Uninsured | 38 | 17 |
| Medicaid (Title XIX) | 36 | 16 |
| Private insurance | 15 | 64 |
| Race | ||
| Asian/Pacific Islander | 5 | 5 |
| American Indian/Alaska Native | 2 | 1 |
| African American | 27 | 13 |
| White | 62 | 72 |
| Ethnicity | ||
| Hispanic/Latino | 35 | 16 |
NOTES: Percentages are of the FQHC population reporting a certain characteristic.
SOURCES: DeNavas-Walt et al., 2010; HRSA, 2011c; U.S. Census Bureau, 2010.
patients in the dentist’s office. Previously, some states required the dentist to individually enroll in Medicaid before providing services for the FQHC (CMS, 2011b).
FQHCs employ over 8,000 full-time equivalent dental staff, including over 2,500 dentists and over 1,000 dental hygienists (HRSA, 2011e). FQHC executive directors report that they most commonly recruit dentists through the National Health Service Corps, although only 10.2 percent of FQHC dentists report receiving a NHSC scholarship, and an additional 19.4 percent report receiving NHSC loan repayment (Bolin, 2010). Even fewer dental hygienists report receiving funding from the NHSC. A large number of FQHC dentists previously worked in the private sector; 31.9 percent reported previously working as a private practice owner, partner, or associate, and 18.5 percent reported previously working as an employee dentist in a private practice (Bolin, 2010). Dentists and dental hygienists working at FQHCs report being generally satisfied with their work: 80.2
percent of dentists and 93.3 percent of dental hygienists intend to remain employed in a health center practice (Bolin, 2010). But more than 39 percent of health centers reported at least one dentist vacancy, and over 50 percent of those positions were vacant for more than 6 months (Bolin, 2010; Cottam, 2010).
With the rapid expansion of dental programs in FQHCs, there appears to be a lack of training and guidance for FQHC dentists. FQHC dental programs are unique within dentistry because they generally function within a general health clinic, may not be ultimately overseen by a dental professional, and charge per encounter, rather than per procedure. Therefore, specialized guidance may be necessary for the dental programs to thrive (Geiermann, 2010). Previously, HRSA offered training and technical assistance to FQHC dentists through its regional dental consultant program. That program has essentially been eliminated, with the retirement of the last consultant in 2009 (Geiermann, 2010). The number of dental public health professionals employed by HRSA has dwindled from a high of over 100 to under 20, most of whom are not able to provide technical assistance to FQHCs. Anecdotal reports indicate that current FQHC dentists do not have a reliable source of assistance (Geiermann, 2010). Indeed, the last oral health guidance to FQHCs was issued in March 1987 (Geiermann, 2010).
FQHC Look-Alikes
FQHC look-alikes were established by Congress to extend the concept of FQHCs (HRSA, 2003). Look-alikes must meet all of the statutory requirements of FQHCs—for example, they provide services to the medically underserved, operate as nonprofits, and be governed by a community board—but they do not receive grant funding under section 330 (HRSA, 2003). FQHCs look-alikes are eligible for many, but not all, of the benefits extended to FQHCs, such as increased Medicaid and Medicare payments and drug pricing discounts (HRSA, 2003). Very little data are available about the dental care provided at FQHC look-alikes because they are not required to submit detailed information to the Department of Health and Human Services about visits.
Community Health Centers
Many community health centers (CHCs) do not receive federal funding or subsidies and operate completely outside of the FQHC system. Some of those health centers are nonprofits, while some are supported or operated by state and local governments. There is no national database of CHCs, so very little information is available about the types of services they provide or the numbers of patients they serve. One study roughly estimated that
they serve about 2.2 million dental patients each year (Bailit et al., 2006). CHCs generally have very limited funding. In 2001, for example, Illinois CHCs had an average annual budget of $182,000 (Byck et al., 2005).
Dental Schools and Residency Programs
Dental students gain experience treating patients in dental school-based clinics. The patients served in those clinics are generally low-income, so dental school clinics are considered part of the dental safety net (Bailit et al., 2006). Dental students provided about 2.9 million patient visits in 2001-2002, with an average of 13 visits per patient, meaning that dental students treated about 224,000 patients during the year (Bailit et al., 2006). The number of patient visits has remained relatively constant; in 2009, dental students had 2.9 million patient visits in dental school clinics and in community-based rotations (ADA, 2010).
The care provided in dental school clinics is affordable but time consuming for patients because clinics are organized as student teaching laboratories rather than patient-centered delivery systems (Bailit et al., 2007). Dental Education at the Crossroads recognized that the mixed missions of educating students and caring for patients lead to trade-offs in both efficiency and quality of care:
Dental students must gain sufficient clinical experience in a variety of technical procedures to become competent entry-level practitioners, qualified to graduate and become licensed. A procedure-driven learning process does not necessarily translate into efficient, high-quality patient care, particularly when student care is further constrained by low budgets for clinical and administrative support. (IOM, 1995)
Some progress has been made toward increasing the efficiency and patient-centeredness of dental school clinics, but more can be done (Formicola et al., 2008).
In addition to on-site clinics at dental schools, dental students also provide care through community rotations in FQHCs and community health centers (ADA, 2010). Of the 2.9 million dental visits provided by dental students in 2009, approximately 450,000 were provided in the community (ADA, 2010), and a large proportion of those visits were in underserved communities (Atchison et al., 2009).
Residencies in dentistry, as in medicine, are an important source of care for underserved populations, including economically and socially disadvantaged populations and medically compromised patients (Mito et al., 2002). One recent study concluded that requiring 1 year of residency training would significantly expand the capacity of community hospitals (or dental schools) to care for the underserved (Bailit et al., 2006). By their estimates,
approximately 1,800 additional dental school graduates would participate in a 1-year general dentistry residency program and an additional 887,000 patients would receive care each year.
School-Based Dental Clinics
School-based health centers (SBHCs) were developed to provide basic health care services, including dental care, in elementary and secondary schools. SBHCs are perhaps the most convenient care location for both children and parents because they eliminate the need for transportation, parent time off, and missed school. Children with access to a SBHC are more likely to have seen a dentist in the past year than similar students without access to a SBHC (Kaplan et al., 1999). In addition, children at high risk for dental caries who have access to a school-based dental sealant program are more than twice as likely to have sealants than children without access (Siegal and Detty, 2010). SBHCs are also associated with improved academic performance, increased use of primary care, reduced use of emergency rooms, and increased use of vaccines (Allison et al., 2007; Walker et al., 2010; Young et al., 2001).
While SBHCs offer significant potential to increase access to oral health care, only a small number of schools have SBHCs, and only a small percentage of those SBHCs offer dental services. Approximately 1,900 school-based health centers operate throughout the country (NASBHC, 2010). Table 4-2 summarizes the oral health services provided by SBHCs during the 2007-2008 school year. Many SBHCs offer simple preventive oral health care, such as oral health education and dental screenings, both on site and by referral, but fewer clinics offer more complex procedures. For example, 84 percent of SBHCs provide oral health education both on site and by referral, but that number drops to 57 percent for dental screenings, 20 percent for dental examinations by a dentist, and the ability of an SBHC to provide oral health services is limited by the number staff qualified to provide oral health services. Only 12.4 percent of SBHCs have a dental provider on staff (NASBHC, 2010). The dental capacity could potentially be expanded by using the new and emerging providers discussed in Chapter 3, as is now done with nurse practitioners and physician assistants in providing medical care in SBHCs. SBHCs have successfully worked in collaboration with public health departments (discussed below) to provide both screening and treatment services. Recognizing the potential for SBHCs to expand access to oral health care to underserved populations, HRSA recently announced a grant program to fund comprehensive oral health care services in SBHCs (HRSA, 2011d).
Although some concern has been raised about whether SBHCs have an adequate funding source (Silberberg and Cantor, 2008), the Patient
TABLE 4-2
Percentage of SBHCs Offering Selected Oral Health Services by Mode of Delivery 2007-2008 School Year
| Onsite and referral (%) |
By referral only (%) |
Not provided or referred (%) |
|
| Oral health education | 83.7 | 11.3 | 5.0 |
| Dental screenings | 56.7 | 37.0 | 6.3 |
| Dental examination (by a dentist) |
19.5 | 68.3 | 12.1 |
| Dental sealants | 25.1 | 61.2 | 13.7 |
| Fluoride mouth rinse | 21.3 | 57.6 | 21.1 |
| Fluoride varnish | 20.1 | 58.3 | 21.6 |
| Fluoride supplements | 14.9 | 61.2 | 24.0 |
| Dental cleaning | 22.6 | 65.4 | 12.1 |
| General dental care (fillings, extractions) |
10.3 | 75.8 | 13.9 |
| Specialty dental care (orthodontics, root canal) |
4.8 | 79.1 | 16.0 |
SOURCE: NASBHC, 2010.
Protection and Affordable Care Act established federal grant programs for the establishment and operation of SBHCs.6 While the legislation does not require SBHCs to offer oral health care, it does require any SBHC that receives federal funding to offer referrals to, and follow-up for, oral health services.
Mobile Dental Clinics
Mobile dental clinics (e.g., mobile vans) have also been used to bring oral health services to underserved populations. A mobile dental clinic can be set up in a retrofitted recreational vehicle or bus using portable dental equipment (ASTDD, 2011c). A range of dental services can be provided in a mobile dental clinic, from preventive care including oral exams, radiographs, and sealant placement, to restorative and specialty care (Carr et al., 2008). Mobile dental clinics are often operated by other safety net provid-
______________
6Patient Protection and Affordable Care Act, Public Law 148, 111th Cong., 2nd sess. (March 23, 2010).
ers, such as FQHCs, state and local health departments, and dental schools, in an effort to extend their reach. They are generally funded through a combination of grants, insurance payments, state and local agency funds, out-of-pocket payments, and volunteers (ASTDD, 2011b). Comprehensive data are not available on the number of mobile dental clinics in operation or on the number of patients they serve (ASTDD, 2011b).
Increasingly, mobile equipment is being used to provide care in settings such as nursing homes. Rather than requiring individuals to travel to a specific site of care (as may be difficult for older adults with physical limitations), this option allows oral health care professionals to provide care to patients where they live, work, and learn. The use of mobile equipment (apart from mobile vans) in alternative settings is discussed later in this chapter in the section on innovations.
Health Departments
Most states have established an oral health plan, whether as a part of the state’s direct dental public health activities or as a part of a larger health plan (CDC, 2011c). Such plans are usually developed and overseen by oral health directors or dental directors under the umbrella of state departments of (public) health. The Association of State and Territorial Dental Directors lists membership in all 50 states (ASTDD, 2011a). The range of services and activities provided under the auspices of state public health dentistry, however, vary considerably, and range from assessment (e.g., gathering oral health data through surveillance activities), to policy development (e.g., related to access), to assurance (e.g., providing clinical preventive and treatment services, supporting community-level water fluoridation) (ASTDD, 2011d).
Oral health data gathered through state public health dental programs allow state and federal agencies to identify trends in oral diseases, oral health professional shortage areas, and to provide the basis for future planning. Examples of policy development through state-level dental public activities include mandating that all children in kindergarten, second, and sixth grades receive an annual dental examination in Illinois (Conis, 2009); requiring Medicaid recipients in Iowa to have a dental home and receive preventive dental care (Rodgers et al., 2010); and developing statewide oral health coalitions.
State-level dental public health programs provide both population and individual-level preventive, promotive, and restorative care. State public health dental programs, through county and city health departments, also provide fluoride varnish, mouth rinse, and fluoride tablets (ASTDD, 2011d). School-based dental sealant programs are available in at least a dozen states and often target high-poverty areas where there is little avail-
ability of oral health care. For example, in 2009-2010, under the auspices of the Tennessee Department of Health, school-based dental sealant programs targeted schools with 50 percent or higher rate of free and reduced lunch, reaching over 300 schools and providing sealants to almost 50,000 children (Tennessee Department of Health, 2010).
Through a combination of both state and local support (including Title V funds), local health departments (LHDs) also provide a variety of oral health services. In 2008-2009, 394 LHDs in 28 states had a dental program that provided restorative services (ASTDD, 2010). Overall, a survey of states found more than 2,700 community-based dental clinics for low-income populations (ASTDD, 2010). The level and intensity of such services, though, varies considerably by the size of the community served by the LHD; for example, only 20 percent of LHDs that serve populations of less than 25,000 offer oral health services, while 57 percent of LHDs serving populations of 500,000 or more offer oral health services (NACCHO, 2009). The provision of oral health care at the LHD level, however, is decreasing: in 1992-1993, 44 percent of LHDs provided some level of oral health services; this decreased to 31 percent in 2005 and 29 percent in 2008 (NACCHO, 2006, 2009) and is likely to decrease further with state and local budget deficits.
Funding for state and local dental public health services continues to be challenging. In 2011, the Centers for Disease Control and Prevention (CDC) provided $6.8 million to just 20 state oral health programs to support evidence-based prevention programs (e.g., community water fluoridation and school-based sealant programs), to provide surveillance of the oral disease burden, and to develop plans to improve oral health and address disparities (CDC, 2011a). This is an increase from $2.3 million in 2003 to support 12 programs (CDC, 2011b). These funds are used to
• Ensure program leadership and staff support.
• Monitor oral diseases and their risk factors.
• Develop a state oral health plan.
• Develop and work with state oral health coalitions and other partnerships.
• Develop and evaluate disease prevention programs, such as community water fluoridation and school-based dental sealant programs (CDC, 2010).
HRSA also supports states through grants (e.g., Title V) for innovative programs to address the needs of designated dental health professional shortage areas. In the past, states have used these funds to increase the availability of school, community, and mobile-based oral health care; to develop cultural competence curriculum for allied health professionals;
and to implement school-based sealant programs, among many others (HRSA, 2011a). In the past, HRSA has also supported local public health infrastructure by training state dental directors and other dental public health professionals and offering technical assistance to state and local health departments through the regional dental consultant program described above (Geiermann, 2010). As mentioned previously, as of 2009, all of the regional dental consultants had retired, and the program had ended (Geiermann, 2010).
Hospital Emergency Departments
People have increasingly turned to hospital emergency departments (EDs) for dental care (Ladrillo et al., 2006; Maiuro, 2009; Shesser, 2010). One hospital reported a 121 percent increase in ED visits for dental complaints between 1997 and 2001, compared to a 28 percent increase for nondental complaints (Ladrillo et al., 2006). In many counties in California, the rate of ED visits for preventable dental complaints exceeds the rate of visits for both asthma and diabetes (Maiuro, 2009). In a presentation to this committee, Dr. Robert Shesser shared data from The George Washington University ED showing that they had 1,700 ED visits related to oral health between 2006 and 2009, accounting for 0.66 percent of all ED visits (Shesser, 2010). The most common diagnoses included dental caries (683 visits), dental pain (452 cases), and dental abscesses (321 cases).
Patients may seek dental care in EDs because they do not have access to traditional dental care. For example, residents of dental health professional shortage areas are more likely to visit an ED for dental care than people who do not live in shortage areas (Okunseri et al., 2008). A study of five Minneapolis hospital systems showed that most ED dental visits were made during normal business hours, when patients might visit a dental office or clinic if they had access to one (Davis et al., 2010). In Wisconsin, African Americans, Native Americans, and Asian Americans, who are more likely than the general population to have unmet dental needs, were also more likely to seek dental treatment in an ED (Okunseri et al., 2008).
Dental coverage appears to be a predictor of use of EDs for dental care (Cohen et al., 2002; Davis et al., 2010). In the Minneapolis study, most ED dental visits were paid by Medicaid or out-of-pocket (Davis et al., 2010). And when Maryland eliminated Medicaid dental coverage for adults, the rate of Medicaid ED claims for dental visits increased 12 percent (Cohen et al., 2002). In Washington state, dental disorders are the most common diagnosis in the ED for uninsured patients and the sixth most common for patients insured by Medicaid, but it is not in the top 25 diagnoses for patients with private insurance (Washington State Hospital Association, 2010).
EDs are not well suited to treat oral health problems; few have the equipment or staff necessary to diagnose and treat dental disease. Likely as a result, ED dental visits are more likely than nondental ED visits to result in a prescription for antibiotics or pain medication, and a referral to a another provider (Lewis et al., 2003). This method of care increases costs, because insurance must pay for both an unnecessary ED visit in addition to a follow-up dental appointment (Okunseri et al., 2008).
Volunteer Efforts
Private-sector efforts to supplement the safety net include the organization of volunteer events to provide free oral health care. These efforts are typically single-day events and provide temporary relief for some people, but they do not provide a regular source of care. As mentioned in Chapter 1, these include the Missions of Mercy (MOM) projects. MOM projects are often organized by state dental societies or private foundations and staffed by volunteer dental professionals to provide care on a first-come, firstserved basis. At these events, thousands of individuals often wait in lines for many hours (Dickinson, 2010). As of March 2010, 44 MOM projects served approximately 35,000 patients in 20 states (Dickinson, 2010). This included over $17 million in dental services, including 60,255 extractions and 31,018 restorations.
In 2003, the ADA established the annual Give Kids a Smile Day, an annual program that includes regional 1-day events to provide educational, screening, preventive, and clinical (e.g., restorative) services to underserved children. In 2010, over 2,100 single-day events served 317,319 children and were staffed by 10,455 dentists and 37,724 other volunteers. Overall, 30 percent of children received educational services; 27 percent received screening services; 23 percent received clinical services; and 20 percent received preventive services (Warren, 2010).
Remote Area Medical, founded in 1985, is a nonprofit, charitable organization that provides free health care, dental care, eye care, veterinary services, and technical and educational assistance to remote populations around the world, but most typically in Appalachia (www.ramusa.org). Volunteers offer a range of health care services (often concurrently) at events which typically last 2 or 3 days at a single location. The extent of dental services offered expanded from emergency extractions only to the provision of restorative care, cleanings, and fluoride treatments. Since its inception, Remote Area Medical has hosted over 600 events (Remote Area Medical, 2011).
CAPACITY AND EFFICIENCY OF THE CURRENT SYSTEM
Several factors contribute to the capacity and efficiency of the oral health care system. In large part, assessments of the oral health care system have focused on the adequacy of the dental workforce. These assessments are usually based either on unmet need or demand for dental services (Guthrie et al., 2009). In 2005, Brown did a comprehensive assessment of the adequacy of the dental workforce (Brown, 2005). He noted a combination of “demand-generating and demand-reducing” forces contribute to such an assessment, including the growth of the population, the retirement rate of dentists, the proportion of the population that seeks care, the types of services needed, the state of the economy, and the development of new treatment modalities. For example, wider recognition of the impact of oral diseases, especially by nondental professionals, could cause a shift toward preventive care and then potentially decrease the need for restorative care. Tough economic times may lead to decreased utilization, especially when services are not covered, or when job loss leads to the loss of dental benefits. Wider adoption of health information technology could help streamline practices and improve efficiency.
Capacity also relates to the typical characteristics of a dental practice. Very few dentists work in large practices, and often are in solo practice. Most of the expansion in the capacity of the private practice has been due to increased use of other personnel, such as dental hygienists and dental assistants, which allows them to delegate some responsibilities (Beazoglou et al., 2009; Brown, 2005). The use of these professionals, changes in office hours, and the design of office space have been attributed to the near doubling of dentist productivity between 1960 and 2002 (Brown et al., 2005). Another consideration is the interval of recall for routine dental examinations and cleanings. While the standard of biannual visits to the dentist is commonly accepted, there is no evidentiary basis to support this interval (Bader, 2005; Beirne et al., 2007). In fact, research suggests that the interval might be better determined for each individual patient based on a combination of factors including risk for oral diseases and clinical judgment and expertise of the dental team (Anthonappa and King, 2008; Bader, 2005; Gibson and Moosajee, 2008; National Institute for Clinical Excellence, 2004; Patel et al., 2010). Reassessment of recall intervals for low-risk populations might improve the capacity of the oral health care system to provide more care for those at higher risk for oral disease.
Estimating Workforce Adequacy
Historically, estimating the adequacy of the workforce itself has been difficult. Similar to the findings of Brown in 2005, in 2009, Guthrie et al. (2009) noted that
considering only unmet need without factoring in the role of economic, social, and cultural factors can lead to large miscalculations of the amount of dental care that will actually be used, which, in turn, can result in large miscalculations on workforce.
Between 1983 and 2001, estimates of the need for dentists fluctuated several times from predicting oversupply to undersupply (Brown, 2005). For example, between 1986 and 2001, seven dental schools closed, exacerbating concerns for future shortages (Guthrie et. al., 2009). Instead of simply estimating the number of individual dental professionals needed to deliver care to every American, more consideration is needed for the influences of supply and demand. Through several modeling exercises, Brown concluded that expanding the number of dentists would be costly and that a better approach to improving productivity would be for dentists to use more allied personnel (Brown, 2005). Brown did not consider expanding the scope of practice in his models. A recent economic modeling exercise to gauge the impact of the addition of several types of dental professionals (including dental therapists) to a private practitioner’s office showed that
By raising the number of patients served each day, allied providers can make it possible for most existing private practices to care for Medicaid-enrolled patients without sacrificing profitability. (Pew Center on the States, 2010)
Estimating the Capacity of the Safety Net
In 2006, Bailit and colleagues (2006) examined the capacity of the safety net to expand in order to care for, in their estimate, 33.3 million underserved individuals. (They assumed these expansions would occur within the current structure of the oral health care system.) Specifically, they looked to FQHCs, health centers, community hospitals, school-based clinics, and dental schools. Overall, they estimated that 7.4 million individuals were already being served in those sites of care, and that there was only capacity to add another 2.6 million patients. The authors, however, did note a lack of data for some of their assumptions. They did conclude that the three most important strategies for increasing the capacity of the safety net are to improve the productivity of FQHCs, require dental residency programs, and require dental student rotations in community-based care of underserved populations. They also concluded
Even with an expanded safety net, the majority of underserved patients would continue to receive care in private practices. Thus, a long-term reduction in access-to-care and oral health disparities requires greater participation by the private practice community. (Bailit et al., 2006)
The safety net system has an important role providing care to the underserved, but it is very limited in size. Compared with other safety net providers, only FQHC dental clinics have a definable source of long-term funding. While the number and size of FQHCs are likely to expand, they do not have the capacity to care for all the unmet needs of vulnerable and underserved populations. While safety net providers are essential to the care of vulnerable and underserved populations, access disparities cannot be reduced unless more private-sector dentists provide care to these populations.
Future Trends
Several trends may influence the future capacity and efficiency of the oral health care system in the future, although the extent of these influences, especially on access to care for vulnerable and underserved populations, remains to be seen.
The Changing Gender Profile in Dentistry
As noted in Chapter 3, entering classes of dental students are approaching an even split between male and female students. Some data show that up to the age of 45, female dentists are more likely to work part time than male dentists (with not enough data existing for female dentists after age 45) (Brown, 2005). However, in a 2009 IOM workshop, Valachovic stated that male dentists tend to work many hours early in their careers and then start to diminish the number of hours they work later in their careers, while women tend to take time off early in their careers for family-related issues, but then increase their number of hours later in their careers (IOM, 2009). Further research and data will be needed in order to fully understand the impact of the changing gender profile of dentists both on the productivity of dentists in general as well as on access to care.
Retirement Rates
In 2008, the IOM noted that a challenge to the health care workforce in general is the aging of its members (IOM, 2008). As noted in Chapter 3, the demographic profiles of dentists and dental hygienists raise concerns about the proportions of those workforces that will reach retirement ages over the next decade. However, retirement rates will depend on many factors
including the better health of older adults today which might lead to longer careers on either a full-time or part-time basis (Guthrie et al., 2009). As the IOM suggested in 2008, older workers might be retained by the development of less physically demanding roles or more flexible work schedules (IOM, 2008). In addition, the economic downturn of recent years might lead to delays in planned retirement (Guthrie et al., 2009). Again, however, these changes in practice patterns have unknown effects on access to care for vulnerable and underserved populations.
New Dental Schools
Another factor to consider is the impact of the several new dental schools that are in various stages of planning and development. An assessment by Guthrie et al. (2009) estimated more than 8,000 additional graduates by 2022, but ultimately concluded that “the increase in dentists will not noticeably improve access to care for low-income and rural populations absent additional public funding to support demand for these populations and concurrent measures to effect even distribution of dentists throughout the country” (Guthrie et al., 2009).
While the number of dental schools is expanding, existing schools are having difficulty with attracting and retaining faculty (Chmar et al., 2008; Haden et al., 2000; McAndrew, 2010; Vanchit et al., 2011). Common reasons for being unable to fill faculty positions include lack of response to position announcements, unqualified candidates, and budgetary limits (Chmar et al., 2008). Among faculty who leave academics, approximately one-third do so for more lucrative careers in private practice (Chmar et al., 2008). The Patient Protection and Affordable Care Act7 of 2010 (ACA) includes financial assistance to dentists who plan to teach or are teaching in general; pediatric or public health dentistry; and faculty loan repayment programs for general, pediatric, and public health dentists who agree to serve as full-time faculty. In addition, under Title VII, individuals from disadvantaged backgrounds who agree to serve as faculty for at least two years at dental and dental hygiene schools are eligible for the Faculty Loan Repayment Program.8
Overcoming Barriers in the System
The current oral health care system is not well designed to overcome barriers to caring for vulnerable and underserved populations. As was
______________
7Patient Protection and Affordable Care Act, Public Law 148, 111th Cong., 2nd sess. (March 23, 2010).
8 42 U.S.C. §293b.
discussed in Chapter 2, literacy issues have a profound effect on the appreciation of oral health care and subsequent utilization of oral health services, and the current system is not well designed to promote education and literacy improvement efforts. Patient behaviors—missed appointments in particular—are frequently cited as barriers to provider participation in Medicaid and as obstacles to providing care to Medicaid patients, especially in the private system (Borchgrevink et al., 2008; CMS, 2011a; GAO, 2000). It is important to note, however, that there may be significant challenges to keeping scheduled appointments for many lower-income patients, aside from health literacy issues. For example, many lower-income individuals may experience difficulty taking time off from work for dental appointments (by design of office hours that are inconvenient for working adults and parents), arranging transportation to the dentist, or finding child care (GAO, 2000; Greenberg et al., 2008; Mofidi et al., 2002; Shirk, 2010). Because providers are prohibited from charging Medicaid for missed appointments, they are financially disadvantaged when patients miss appointments. Therefore, reducing the number of missed appointments can be an important part of efforts to improve provider participation in Medicaid. (Provider participation in Medicaid is discussed further in Chapter 5.)
Well-designed case management programs can address many of dentists’ issues with Medicaid (ADA, 2004; Binkley et al., 2010; Greenberg et al., 2008). For example, a case management program in New York state took a multipronged approach to increasing Medicaid dental utilization in a rural county (Greenberg et al., 2008). The case manager recruited dentists through presentations, letters, phone calls, and mailings. To assist with billing concerns, the case manger arranged billing training for dental office support staff, tracked billing problems until they were resolved, and informed dental offices when patients lost or gained Medicaid coverage. The case manager addressed dentists’ concerns about missed appointments by educating patients about the importance of oral health and the appropriate use of oral health care, helping patients select the dentist that was most convenient to their work or home, making appointments, and following up with patients when the dental office could not reach them or when they had missed appointments. During the course of the case management program, the number of dentists participating in the program went from 2 to 28, and the percentage of Medicaid-eligible patients receiving dental care increased from 9 percent to over 40 percent. Other, comparable case management programs (some of which also included a reimbursement rate increase) have had similar results (ADA, 2004; Binkley et al., 2010).
INNOVATIONS IN SETTINGS OF CARE
The following sections provide descriptions of an array of innovations being used to improve access to oral health care by delivering care in alternative settings or through the use of new modalities. In some cases, these innovations are too new to have robust outcomes data for impact on access to care or oral health status, especially in the long term, and therefore the committee does not intend to imply that it is recommending these approaches. In addition, these examples are not exhaustive of all of the strategies being used across the nation. Instead, the following section serves to illustrate the wide variety of ideas and opportunities for providing care in a variety of settings, partnering with existing programs, or developing new sites of care in order to improve access to care for vulnerable and underserved populations.
Virtual Care
The use of telehealth technologies is emerging as a strategy to provide dental services in underserved communities where significant barriers to receiving care in a traditional dental office setting exist (Glassman and Subar, 2010; Kopycka-Kedzierawski et al., 2007; Sanchez Dils et al., 2004). The University of the Pacific Arthur A. Dugoni School of Dentistry has initiated a 4-year demonstration program for providing basic oral health care services to disadvantaged populations in remote locations. Dental professionals (including registered dental hygienists, registered dental hygienists in alternative practice, and registered dental assistants) provide screening, preventive services, temporary restorations, and case management services to low-income and disabled patients in nursing homes, public schools, and residential homes for developmentally disabled individuals under the supervision of dentists linked to the remote locations electronically (e.g., via portable video camera). The professionals in the field electronically send diagnostic information (e.g., physical examination, history, photographs, X-rays) to dentists who review the materials, make diagnoses, and develop treatment plans. Then, the field-based professionals provide preventive services such as oral hygiene instruction, prophylaxes and fluoride varnish, temporary restorations, and refer patients needing dental services to dental clinics or private practices. In some cases, dentists come to the remote sites with portable equipment and provide services. At this time the project is operating in nine remote sites (University of the Pacific, 2011).
While telehealth-enabled delivery systems have the potential to expand the reach of dentists and allied dental personnel into community sites, there are a number of barriers that currently limit their spread. These include the fact that most state laws do not allow general supervision of allied
dental personnel using telehealth technology (Center for Connected Health Policy, 2011). In addition, many private payers do not recognize the use of telehealth-delivered care (Whitten and Buis, 2007), although Medicare and many state Medicaid programs now pay for telehealth services (CMS, 2011c; Youngblade et al., 2005).
Extending the Reach of FQHCs
School-Based Care
In addition to formal SBHCs, school-based care systems have the potential to reduce access disparities and improve the oral health of children from low-income families. For example, in 2003, in response to low utilization rates of Medicaid and SCHIP-eligible children, an FQHC in central Connecticut initiated a school dental program in which dental hygienists provide screening and basic preventive services in schools using mobile equipment and temporary space (Bailit et al., 2010). The dental hygienists also identify children in need of more advanced care. As part of the hygienist’s examination, children are placed into risk groups that determine the frequency and types of preventive services they receive. Another program feature is organized as educational modules for teachers, caregivers, and students.
Since 2003, several other state FQHCs have established similar programs that currently provide oral health care to low-income children in over 200 public schools and Head Start programs. The estimated number of children treated each year is over 10,000 and growing rapidly (Bailit et al., 2010). The FQHCs target schools with large numbers of Medicaid- and CHIP-eligible children, aged 3 to 18 years, but all low-income children are eligible to receive care. FQHCs consider these children FQHC patients and are reimbursed at their usual visit rate. While most children are enrolled in the Medicaid or CHIP programs, those without insurance are also eligible to receive care at a low fee.
A major challenge is making sure that children receive needed restorative care. The Connecticut program began using case managers to arrange for caregivers to bring children to FQHC clinics, where they were given priority in obtaining timely appointments. Only 40 percent of referred children actually received care with this approach (Bailit et al., 2010). To increase the completion of restorative care, FQHC dentists now follow the hygienists and provide restorative and other services in schools using portable equipment. Only a relatively small percentage of these students have behavioral, medical, and dental problems that cannot be treated by dentists using portable equipment. In these cases, a case manager works with caregivers to make sure that these children receive treatment.
The program has the full support of organized dentistry in Connecticut, and it is highly regarded by public school administrators and teachers. In time, Connecticut FQHCs are expected to develop the capacity to meet the needs of all interested schools (Bailit et al., 2010). This plan has many advantages including
• Minimal need, if any, for special grant funding, since in most states FQHC per-visit Medicaid reimbursement rates should be adequate to cover program costs;
• Effective use of dental professionals;
• Limited startup capital; elimination of caregiver transportation, time, and scheduling barriers to taking children to dental offices and clinics;
• Availability of FQHCs to patients who require a more advanced level of care; and
• Dental education to teachers, caregivers, and patients.
Multisite FQHCs
The Marshfield Clinic has been successful at reducing oral health disparities in rural Wisconsin through a targeted, multisite FQHC approach (Nycz, 2010). As of July 2010, Marshfield clinic operated seven dental clinics in rural Wisconsin; at that time, the number was projected to increase to nine by 2011, and they planned to operate 16 dental clinics throughout the state by 2016 (Nycz, 2010). At that time, Marshfield dental clinics will have the capacity to provide over 400,000 visits per year to 158,000 patients in nearly 400 operatories staffed by 91 dentists and 69 hygienists (Nycz, 2010).
Marshfield has a four-part strategy for reducing oral health disparities in their community: regionalizing care, integrating dentistry with medicine, treating all populations, and training its own workforce (Nycz, 2010). To efficiently reach a dispersed, rural population, Marshfield opened clinics in regional centers, often county seats. This strategy also allowed them to place multiple dentists in each center, which they suspected might improve dentist recruitment and retention. Marshfield integrated dental records into their medical records and vice versa, which prompts physicians to educate their patients about oral health and refer them to the dental clinics, and gives dentists full access to patients’ medical records. In addition, each clinic is accessible to people with special health care needs, including wheelchair accessible operatories. Finally, Marshfield is in the process of establishing a dental school to train dentists specifically to work with underserved and vulnerable populations in rural areas (Kilsdonk, 2010; Nycz, 2010).
Three years after Marshfield opened its first dental clinic, the publicly
insured population in the county where it is located accessed care at the same rates as those who have private coverage (Nycz, 2010). In addition, cost per visit has decreased over time because the burden of disease has decreased in the population (Nycz, 2010).
Building on Existing Community Services
Another strategy to increase access is for dental professionals to partner with existing community partners, as a delivery point for providing oral health care. Below, two such examples are given in which oral health care has been incorporated into larger programs.
Women, Infants, and Children Agencies
The primary mission of the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) is to promote healthy diets and feeding practices for women, infants, and children. To participate, caregivers are required to go to WIC offices for food vouchers and education on a quarterly or monthly basis. As an example, California has the nation’s largest WIC program and serves 60 percent of all children born in California (Center for Oral Health, 2010). The WIC Early Intervention for Oral Health project builds on the existing nutrition program and adds a dental education, screening, prevention, and referral component. Partnerships between dental providers and California WIC programs are required to develop protocols for providing oral health care directly on site, in a mobile van, or an adjacent dental clinic; develop plans for parental education; track numbers seen; and provide case management for follow-up care (Center for Oral Health, 2010).
Head Start
In another example, the Head Start program, administered by the Office of Head Start of the Administration for Children and Families, is “a national program that promotes school readiness by enhancing the social and cognitive development of children through the provision of educational, health, nutritional, social and other services to enrolled children and families” (OHS, 2011). Head Start programs are required to determine whether a child has received age-appropriate preventive dental care within 90 days of the child entering the Head Start program.9 If a child has not received appropriate care, the Head Start program must help the parents
______________
9 Code of Federal Regulations, Office of Human Development Services, Department of Health and Human Services, title 45, sec. 1304.20 (2009).
make arrangements for the child to receive it.10 Appropriate care is determined by the state’s Early and Periodic Screening, Diagnosis, and Treatment program and periodicity schedule. Head Start programs must also obtain or arrange for testing, examination, and treatment for children with known or suspected dental problems, and develop and implement a follow-up plan for any problems identified.
To foster access to oral health for children enrolled in Head Start, in 2006, the Office of Head Start invested $2 million in grants to 52 Head Start, Early Head Start, and Migrant/Seasonal Head Start programs for the Head Start Oral Health Initiative; grantees received supplemental funding for 4 additional years. While grantees reported successfully developing partnerships with community organizations and providers who would serve Head Start children, educating staff about the importance of oral health, and incorporating oral health education into the curriculum, they reported that they likely could not sustain much of the oral health programming when the grant funding ended (Del Grosso et al., 2008).
Requirements Tied to Public Education
Several states have introduced programs requiring a dental examination or oral health assessment prior to school entry, though the provisions of these programs differ across states. Even though the requirements have been legislated, many of the plans do not have enforcement or follow-up mechanisms in place. In addition, little data exist on the impact of these types of requirements. Examples include the following:
• Illinois will withhold student report cards if the requirement is unfulfilled (Conis, 2009).
• In 2008, Kentucky passed a law effective in the 2010-2011 school year requiring children to have a dental examination prior to enrolling in public school (Conis, 2009).
• New York requests parents to provide a dental certificate documenting an oral health exam at certain points during a child’s school career (Conis, 2009).
Alternative Sites of Care
Portable Equipment
Patient-centered approaches to caring for vulnerable and underserved populations may require consideration for bringing oral health care to the
______________
10 Ibid.
sites that are more convenient for those populations. In particular, older adults and disabled individuals may be unable to travel to travel to dentists’ offices. In these cases, portable equipment is increasingly being used to provide on-site, community-based care in settings such as nursing homes, group homes, schools, and Head Start centers.
For example, Apple Tree Dental (Apple Tree) is a private, nonprofit organization in Minnesota that has provided care to individuals with special health care needs across the life span in a variety of settings for over 25 years (Silow-Carroll and Alteras, 2004). The program has two dental clinic “hubs,” but it provides most of its care through community-based mobile programs. Apple Tree contends advantages to mobile care include reduced anxiety for patients (due to the familiar environment), interdisciplinary care, and improved efficiency (e.g., reduction in transportation costs for each patient) (Silow-Carroll and Alteras, 2004). Apple Tree has been a source of community-based educational experiences for dental hygienists and dental assistants through partnerships with dental hygiene and dental assisting programs. Apple Tree also collects data on its patient population, which facilitates research on special care populations. In 2008, Apple Tree reported almost 60,000 patient encounters (Helgeson, 2009).
In another example, Dr. Greg Folse made a presentation to this committee regarding his work providing mobile oral health services for residents in 23 nursing facilities (Folse, 2010). Dr. Folse estimated that 61 percent of the dentate nursing home residents (or 45 percent of the total resident population) needed surgical interventions due to abscesses and/or severe gum disease. He further estimated that this meant that 1,062 existing patients were in need of surgical interventions and that an additional 371 new residents would need such care each year. In 2009, working part-time in these nursing homes and using portable equipment, Dr. Folse reported being able to treat 392 surgical cases, manage 3 cases of oral cancer, direct between 1 and 5 dental emergencies weekly (many of which were life threatening), and treat 262 denture patients. He also noted one death occurring as a result of oral disease. Dr. Folse also noted using portable dental equipment to care for children in Louisiana schools. He reported using 15 dentists and 18 expanded duty dental assistants to provide care in 275 schools. He stated that the benefits of using portable equipment included decrease in “no-show” patients, no late appointments, and no loss of time from work for parents. Disadvantages include difficulty with scheduling time during the school hours and obtaining parental consent. Dr. Folse noted that since 2001, his Louisiana school-based model had treated over 20,000 children in the school setting and included over 30,000 patient visits.
Retail Health Clinics
Retail health clinics have been rapidly developing as a new site of care for general health care (Hunter et al., 2009; Laws and Scott, 2008; Mullin, 2009; Pollack and Armstrong, 2009; Pollack et al., 2010; Rudavsky et al., 2009; Thygeson et al., 2008; Wang et al., 2010). Recently, retail dental clinics have been proposed as an alternative site of dental care (Scott, 2009, 2010). Much like retail health clinics, retail dental clinics would be located in pharmacies, grocery stores, and large retailers. The clinics would offer a limited menu of services at set prices, focus primarily on preventive and diagnostic care, and refer patients with more complex needs to dentists. Although no retail dental clinics currently exist, an economic model suggests that they could be viable if dental professionals could provide care without the presence of a dentist (Scott, 2009).
Dental Homes
While not a physical site of care, the dental home is an emerging strategy to increase access to consistent oral health care. A dental home is an ongoing relationship between a patient and a dentist (AAPD, 2010a). The dentist provides, among other things, regular comprehensive oral health assessment and care, individualized preventive care based on caries- and periodontal-risk assessments, education on proper nutrition and home care, and referrals to specialists when necessary (AAPD, 2010b). To date, dental homes have centered on providing care to children. However, the medical home model, on which dental homes are based, has been used with all populations to provide acute, chronic, and preventive medical services (Martin et al., 2004). Thus, there may be an opportunity to expand the dental home beyond the pediatric population.
One example of a dental home program is the Access to Baby and Child Dentistry (ABCD) program, operated across Washington state through a variety of public-private partnerships (ABCD, 2011; Donahue et al., 2005). Partners include local health departments, the Washington State Dental Society, local dental societies, the Washington Department of Health (WDOH), the Washington Department of Social and Health Services (WDSHS), the University of Washington School of Dentistry, the Washington Dental Service Foundation, private dentists, and other community partners. Local health departments typically manage the daily functions of ABCD programs. They work with the state and local dental professional organizations to encourage dentist participation. Dentists who participate in the program receive training and are paid an enhanced reimbursement rate. The health departments also actively recruit Medicaid-eligible children to the program through partnerships with community organizations such as WIC, Head
Start, and Early Head Start. In addition, the health departments provide case management services to ABCD families. The WDSHS, WDOH, University of Washington School of Dentistry, and Washington Dental Service Foundation oversee the program at the state level. The WDSHS oversees Medicaid financing in the state, and thus provides reimbursement to ABCDcertified dentists, and provides billing assistance, among other things. The WDSHS also contracts with the University of Washington Dental School to provide training and ongoing education to ABCD providers. The WDOH provides technical assistance and grants to local health departments. The Washington Dental Service Foundation provides start-up grants and ongoing technical assistance to local ABCD programs.
ABCD programs have significantly increased the rate of dental visits among children enrolled in Medicaid (Grembowski and Milgrom, 2000; Lewis et al., 2009; Milgrom et al., 1999), particularly among the youngest children (Kaakko et al., 2002). However, the evidence indicates that the programs may be more successful at encouraging parents to make a single dental appointment than develop an ongoing relationship with a dentist, which is a key component of a dental home (Kaakko et al., 2002; Milgrom et al., 1999). More long-term evaluations of the program need to be done to assess the program’s ability to establish dental homes.
The committee noted the following findings and conclusions:
• Most oral health care in the United States is provided in the private practice setting by dentists, who employ dental hygienists and dental assistants.
• Most patients seen in the private practice setting either have dental insurance or pay out of pocket.
• Only a small portion of private-sector oral health care is supported by publicly funded programs such as Medicaid.
• An array of programs provides oral health care to underserved and vulnerable populations, including FQHCs, dental schools, and health departments.
• An oral health safety net exists in concept, but the components of this safety net are not necessarily connected or coordinated.
• No single setting of care will meet the various needs or overcome the multitude of barriers for vulnerable and underserved populations.
• More research is needed on the impact of individual site of care models in improving access to care.
• More research is needed on best practices for individual sites of care.
• There is room for building the capacity of the safety net to care for vulnerable and underserved populations, but it will not be enough to care for all patients in need. Strategies to improve access to care for these populations will require the participation of dentists in the private practice setting.
AAPD (American Academy of Pediatric Dentistry). 2010a. Definition of dental home. http://www.aapd.org/media/Policies_Guidelines/D_DentalHome.pdf (accessed May 23, 2011).
AAPD. 2010b. Policy on the dental home. http://www.aapd.org/media/Policies_Guidelines/P_DentalHome.pdf (accessed May 23, 2011).
ABCD (Access to Baby and Child Dentistry). 2011. Partners & roles. http://www.abcd-dental.org/part.html (accessed May 24, 2011).
ADA (American Dental Association). 2004. State and community models for improving access to dental care for the underserved—a white paper. Chicago, IL.
ADA. 2009a. 2008 survey of dental practice: Characteristics of dentists in private practice and their patients. Chicago, IL: American Dental Association.
ADA. 2009b. 2008 survey of dental practice: Employment of dental practice personnel. Chicago, IL: American Dental Association.
ADA. 2009c. 2008 survey of dental practice: Income from the private practice of dentistry. Chicago, IL: American Dental Association.
ADA. 2009d. Distribution of dentists in the United States by region and state, 2007. Chicago, IL: American Dental Association.
ADA. 2010. 2008-09 survey of dental education: Academic programs, enrollment, and graduates—volume 1. Chicago, IL: American Dental Association.
Allison, M. A., L. A. Crane, B. L. Beaty, A. J. Davidson, P. Melinkovich, and A. Kempe. 2007. School-based health centers: Improving access and quality of care for low-income adolescents. Pediatrics 120(4):e887-e894.
Anderson, J. R. 2010. HRSA oral health programs. Paper presented at 2010 Dental Management Coalition, June 27, Annapolis, MD.
Anthonappa, R., and N. King. 2008. Six-month recall dental appointments, for all children, are (un)justifiable. Journal of Clinical Pediatric Dentistry 33(1):1-8.
ASTDD (Association of State and Territorial Dental Directors). 2010. Synopses of state dental public health programs: Data for FY 2008-2009. Sparks, NV: Association of State and Territorial Dental Directors.
ASTDD. 2011a. Membership roster. http://www.astdd.org/membership-roster/ (accessed January 25, 2011).
ASTDD. 2011b. Mobile and portable dental services in preschool and school settings: Complex issues. Sparks, NV: Association of State and Territorial Dental Directors.
ASTDD. 2011c. Mobile portable dental manual. http://mobile-portabledentalmanual.com/index.html (accessed March 10, 2011).
ASTDD. 2011d. State & territorial dental public health activities: A collection of descriptive summaries. http://www.astdd.org/state-activities/ (accessed January 25, 2011).
Atchison, K., A. Thind, T. Nakazono, D. Wong, J. Gutierrez, D. Carreon, and R. Andersen. 2009. Community-based clinical dental education: Effects of the pipeline program. Journal of Dental Education 73(2):S269-S282.
Bader, J. 2005. Risk-based recall intervals recommended. Evidence-based Dentistry 6(1):2-4.
Bailit, H., T. Beazoglou, N. Demby, J. McFarland, P. Robinson, and R. Weaver. 2006. Dental safety net: Current capacity and potential for expansion. Journal of the American Dental Association 137(6):807-815.
Bailit, H. L., T. J. Beazoglou, A. J. Formicola, and L. Tedesco. 2007. Financing clinical dental education. Journal of Dental Education 71(3):322-330.
Bailit, H., J. D’Adamo, and T. Beazoglou. 2010 (unpublished). Report to the Oral Health Access Committee: State case studies: Improving access to dental care for the underserved.
Beazoglou, T., L. J. Brown, S. Ray, L. Chen, and V. Lazar. 2009. An economic study of expanded duties of dental auxiliaries in Colorado. Chicago, IL: American Dental Association.
Beirne, P. V., J. E. Clarkson, and H. V. Worthington. 2007. Recall intervals for oral health in primary care patients. Cochrane Database of Systematic Reviews (4):CD004346.
Binkley, C. J., B. Garrett, and K. W. Johnson. 2010. Increasing dental care utilization by Medicaid-eligible children: A dental care coordinator intervention. Journal of Public Health Dentistry 70(1):76-84.
Bolin, K. A. 2010. Survey of health center oral health providers: Dental salaries, provider satisfaction, and recruitment and retention strategies. Denver, CO: National Network for Oral Health Access.
Borchgrevink, A., A. Snyder, and S. Gehshan. 2008. The effects of Medicaid reimbursement rates on access to dental care. Washington, DC: National Academy for State Health Policy.
Brown, L. J. 2005. Adequacy of current and future dental workforce: Theory and analysis. Chicago, IL: American Dental Association.
Brown, L. J., D. R. House, and K. D. Nash. 2005. The economic aspects of unsupervised private hygiene practice and its impact on access to care. Chicago, IL: American Dental Association.
Byck, G. R., J. A. Cooksey, and H. Russinof. 2005. Safety-net dental clinics: A viable model for access to dental care. Journal of the American Dental Association 136(7):1013-1021.
Carr, B. R., U. Isong, and J. A. Weintraub. 2008. Identification and description of mobile dental programs—a brief communication. Journal of Public Health Dentistry 68(4):234-237.
CDC (Centers for Disease Control and Prevention). 2010. Division of oral health: About us. http://www.cdc.gov/oralhealth/about.htm (accessed November 24, 2010).
CDC. 2011a. CDC-funded states. http://www.cdc.gov/oralhealth/state_programs/cooperative_agreements/index.htm (accessed October 7, 2011).
CDC. 2011b. CDC-previously funded states. http://www.cdc.gov/OralHealth/state_programs/cooperative_agreements/previously_funded.htm (accessed October 7, 2011).
CDC. 2011c. State health plans. http://www.cdc.gov/OralHealth/state_programs/OH_plans/index.htm (accessed January 25, 2011).
Center for Connected Health Policy. 2011. Advancing California’s leadership in telehealth policy: A telehealth model statute & other policy recommendations. Sacramento, CA: Center for Connected Health Policy.
Center for Oral Health. 2010. WIC programs. http://www.centerfororalhealth.org/programs/wic-programs (accessed January 31, 2011).
Chmar, J. E., R. G. Weaver, and R. W. Valachovic. 2008. Dental school vacant budgeted faculty positions, academic years 2005-06 and 2006-07. Journal of Dental Education 72(3):370-385.
CMS (Centers for Medicare and Medicaid Services). 2011a. Innovative state practices for improving the provision of Medicaid dental services. Baltimore, MD.
CMS. 2011b. Recent developments in Medicaid and CHIP policy. http://www.cms.gov/CMCSBulletins/downloads/CMCS-Info-Bulletin-March-2011-Final.pdf (accessed May 31, 2011).
CMS. 2011c. Telehealth services: Rural health fact sheet series. https://www.cms.gov/MLNProducts/downloads/TelehealthSrvcsfctsht.pdf (accessed May 27, 2011).
Cohen, L. A., R. J. Manski, L. S. Magder, and C. D. Mullins. 2002. Dental visits to hospital emergency departments by adults receiving Medicaid: Assessing their use. Journal of the American Dental Association 133(6):715-724.
Conis, E. 2009. Steps to improve oral health in Kentucky. Health Policy Monitor.
Cottam, W. W. 2010. The NNOHA survey of health center dental salaries: Trends and analysis. http://www.cdnetwork.org/NewCDN/LibraryView.aspx?ID=cdn565 (accessed March 8, 2011).
Davis, E. E., A. S. Deinard, and E. W. H. Maïga. 2010. Doctor, my tooth hurts: The costs of incomplete dental care in the emergency room. Journal of Public Health Dentistry 70(3):205-210.
Del Grosso, P., A. Brown, S. Silva, J. Henderson, N. Tein, and D. Paulsell. 2008. Strategies for promoting prevention and improving oral health care delivery in Head Start: Findings from the oral health initiative evaluation. Princeton, NJ: Mathematica Policy Research, Inc.
DeNavas-Walt, C., B. D. Proctor, and J. C. Smith. 2010. Income, poverty, and health insurance coverage in the United States: 2009. Washington, DC: U.S. Census Bureau.
Dickinson, T. D. 2010. The MOM experience: Pathways to collaboration and conversation. Paper presented at meeting of the Committee on Oral Health Access to Services, Washington, DC.
Donahue, G. J., N. Waddell, A. L. Plough, M. A. del Aguila, and T. E. Garland. 2005. The ABCDs of treating the most prevalent childhood disease. American Journal of Public Health 95(8):1322-1324.
Folse, G. 2010. Outreach dentistry. Paper presented at meeting of the Committee on Oral Health Access to Services, San Francisco, CA.
Formicola, A. J., R. Myers, J. F. Hasler, M. Peterson, W. Dodge, H. L. Bailit, T. J. Beazoglou, and L. A. Tedesco. 2008. Evolution of dental school clinics as patient care delivery centers. Journal of Dental Education 72(2 Supp.):110-127.
GAO (Government Accountability Office). 2000. Factors contributing to low use of dental services by low-income populations. Washington, DC: U.S. General Accounting Office.
Geiermann, S. L. 2010. Expertise and technical assistance in health centers. Presentation at meeting of the Committee on Oral Health Access to Services, San Francisco. July 27, 2010.
Gibson, C., and A. Moosajee. 2008. Selecting appropriate recall intervals for patients in general dental practice—an audit project to categorize patients according to risk. Dental Update 35(3):188-190, 193-194.
Glassman, P., and P. Subar. 2010. Creating and maintaining oral health for dependent people in institutional settings. Journal of Public Health Dentistry 70(Supp. 1):S40-S48.
Greenberg, B. J. S., J. V. Kumar, and H. Stevenson. 2008. Dental case management: Increasing access to oral health care for families and children with low incomes. Journal of the American Dental Association 139(8):1114-1121.
Grembowski, D., and P. M. Milgrom. 2000. Increasing access to dental care for Medicaid preschool children: The Access to Baby and Child Dentistry (ABCD) program. Public Health Reports 115(5):448-459.
Guay, A. H. 2005. Dental practice: Prices, production and profits. Journal of the American Dental Association 136(3):357-361.
Guthrie, D., R. W. Valachovic, and L. J. Brown. 2009. The impact of new dental schools on the dental workforce through 2022. Journal of Dental Education 73(12):1353-1360.
Haden, N. K., P. L. Beemsterboer, R. G. Weaver, and R. W. Valachovic. 2000. Dental school faculty shortages increase: An update on future dental school faculty. Journal of Dental Education 64(9):657-673.
Haley, J., G. Kenney, and J. Pelletier. 2008. Access to affordable dental care: Gaps for lowincome adults. http://www.kff.org/medicaid/upload/7798.pdf (accessed May 18, 2011).
Helgeson, M. 2009. Older adults and people with disabilities. Paper presented at IOM workshop on the U.S. Oral Health Workforce in the Coming Decade, Washington, DC.
HHS (Department of Health and Human Services). 2010a. Recovery Act (ARRA): Community health centers. http://www.hhs.gov/recovery/hrsa/healthcentergrants.html (accessed February 3, 2010).
HHS. 2010b. Healthy People 2020: Oral health objectives. http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicid=32 (accessed December 27, 2010).
HRSA (Health Resources and Services Administration). 2003. Program information notice 2003-21: Federally qualified health center look-alike guidelines and application. Rockville, MD: U.S. Department of Health and Human Services.
HRSA. 2010. The health center program: Benefits. http://bphc.hrsa.gov/about/benefits.htm (accessed February 3, 2010).
HRSA. 2011a. BHPR grants: Oral health workforce activities FY 2010 grantee abstracts. http://bhpr.hrsa.gov/grants/10oralhealthabstracts.htm (accessed January 10, 2011).
HRSA. 2011b. Health centers: 2009 at-a-glance. http://www.hrsa.gov/data-statistics/health-center-data/NationalData/2009/2009datasnapshot.html (accessed March 1, 2011).
HRSA. 2011c. Health centers: 2009 national total summary data. http://bphc.hrsa.gov/healthcenterdatastatistics/nationaldata/2009/2009nattotsumdata.html (accessed August 9, 2011).
HRSA. 2011d. School-based comprehensive oral health services grant program. https://grants.hrsa.gov/webExternal/SFO.asp?ID=513FD7F0-C025-48E0-B6EC-AAFEFD528AA7 (accessed June 1, 2011).
HRSA. 2011e. Staffing & utilization: National summary for 2009. http://www.hrsa.gov/data-statistics/health-center-data/NationalData/2009/2009_national_staffing.html (accessed March 10, 2011).
Hunter, L. P., C. E. Weber, A. P. Morreale, and J. H. Wall. 2009. Patient satisfaction with retail health clinic care. Journal of the American Academy of Nurse Practitioners 21(10): 565-570.
IOM (Institute of Medicine). 1995. Dental education at the crossroads: Challenges and change. Washington, DC: National Academy Press.
IOM. 2008. Retooling for an aging America: Building the health care workforce. Washington, DC: The National Academies Press.
IOM. 2009. The U.S. oral health workforce in the coming decade: Workshop summary. Washington, DC: The National Academies Press.
Kaakko, T., E. Skaret, T. Getz, P. Hujoel, D. Grembowski, C. S. Moore, and P. Mllgrom. 2002. An ABCD program to increase access to dental care for children enrolled in Medicaid in a rural county. Journal of Public Health Dentistry 62(1):45-50.
Kaplan, D. W., C. D. Brindis, S. L. Phibbs, P. Melinkovich, K. Naylor, and K. Ahlstrand. 1999. A comparison study of an elementary school-based health center. Archives of Pediatrics and Adolescent Medicine 153(3):235-243.
Kenney, G. M., J. M. Haley, and J. E. Pelletier. 2009. Covering Kids & Families evaluation. Washington, DC: Urban Institute.
Kilsdonk, G. J. 2010. Family health center of Marshfield & Marshfield clinic’s response to the surgeon general’s report: Oral health in America. Paper presented at the National Health Policy Forum, Washington, DC.
Kopycka-Kedzierawski, D. T., R. J. Billings, and K. M. McConnochie. 2007. Dental screening of preschool children using teledentistry: A feasibility study. Pediatric Dentistry 29:209-213.
Ladrillo, T. E., M. H. Hobdell, and A. C. Caviness. 2006. Increasing prevalence of emergency department visits for pediatric dental care, 1997-2001. Journal of the American Dental Association 137(3):379-385.
Laws, M., and M. K. Scott. 2008. The emergence of retail-based clinics in the United States: Early observations. Health Affairs 27(5):1293-1298.
Lewis, C., H. Lynch, and B. Johnston. 2003. Dental complaints in emergency departments: A national perspective. Annals of Emergency Medicine 42(1):93-99.
Lewis, C., E. Teeple, A. Robertson, and A. Williams. 2009. Preventive dental care for young, Medicaid-insured children in Washington State. Pediatrics 124(1):e120-e127.
Maiuro, L. S. 2009. Emergency department visits for preventable dental conditions in California. Oakland, CA: California HealthCare Foundation.
Martin, A., D. Lassman, L. Whittle, A. Catlin, J. Benson, C. Cowan, B. Dickensheets, M. Hartman, P. McDonnell, O. Nuccio, and B. Washington. 2011. Recession contributes to slowest annual rate of increase in health spending in five decades. Health Affairs 30(1):11-22.
Martin, J. C., R. F. Avant, M. A. Bowman, J. R. Bucholtz, J. R. Dickinson, K. L. Evans, L. A. Green, D. E. Henley, W. A. Jones, and S. C. Matheny. 2004. The future of family medicine: A collaborative project of the family medicine community. Annals of Family Medicine 2(Supp. 1):S3-S32.
McAndrew, M. 2010. Community-based dental education and the importance of faculty development. Journal of Dental Education 74(9):980-985.
Mertz, E., and E. O’Neil. 2002. The growing challenge of providing oral health care services to all Americans. Health Affairs 21(5):65-77.
Milgrom, P., P. Hujoel, D. Grembowski, and R. Fong. 1999. A community strategy for Medicaid child dental services. Public Health Reports 114(6):528-532.
Mito, R. S., K. A. Atchison, K. H. Lefever, S. Lin, and R. Engelhardt. 2002. Characteristics of civilian postdoctoral general dentistry programs. Journal of Dental Education 66(6):757-765.
Mofidi, M., R. G. Rozier, and R. S. King. 2002. Problems with access to dental care for Medicaid-insured children: What caregivers think. American Journal of Public Health 92(1):53-58.
Mullin, K. 2009. Considering retail health clinics. Journal of Nursing Administration 39(12): 531-536.
NACCHO (National Association of County & City Health Officials). 2006. 2005 national profile of local health departments. Washington, DC: National Association of County & City Health Officials.
NACCHO. 2009. 2008 national profile of local health departments. Washington, DC: National Association of County & City Health Officials.
NASBHC (National Assembly on School-Based Health Care). 2010. Census 2007-08: School-Based, school-linked and mobile health care survey. Washington, DC: National Assembly on School-Based Health Care.
National Institute for Clinical Excellence. 2004. Dental recall: Recall interval between routine dental examinations. London, UK: National Institute for Clinical Excellence.
Nycz, G. 2010. Solving oral health access: A regionalized, integrated, and rural dental system. Paper presented at meeting of the Committee on Oral Health Access to Services, San Francisco, CA.
OHS (Office of Head Start). 2011. About the Office of Head Start. http://www.acf.hhs.gov/programs/ohs/about/index.html (accessed May 22, 2011).
Okunseri, C., N. M. Pajewski, D. C. Brousseau, S. Tomany-Korman, A. Snyder, and G. Flores. 2008. Racial and ethnic disparities in nontraumatic dental-condition visits to emergency departments and physician offices: A study of the Wisconsin Medicaid program. Journal of the American Dental Association 139(12):1657-1666.
Patel, S., R. C. Bay, and M. Glick. 2010. A systematic review of dental recall intervals and incidence of dental caries. Journal of the American Dental Association 141(5):527-539.
Pew Center on the States. 2010. It takes a team: How new dental providers can benefit patients and practices. Washington, DC: The Pew Charitable Trusts.
Pollack, C. E., and K. Armstrong. 2009. The geographic accessibility of retail clinics for underserved populations. Archives of Internal Medicine 169(10):945-949.
Pollack, C. E., C. Gidengil, and A. Mehrotra. 2010. The growth of retail clinics and the medical home: Two trends in concert or in conflict? Health Affairs 29(5):999-1003.
Remote Area Medical. 2011. RAM expeditions. http://www.ramusa.org/expeditions/expeditions.htm (accessed October 6, 2011).
Rodgers, T., B. Russell, and S. Meister. 2010. Inside I-Smile 2009: An update on Iowa’s dental home initiative for children. Des Moines, IA: Iowa Department of Public Health, Oral Health Bureau.
Rudavsky, R., C. E. Pollack, and A. Mehrotra. 2009. The geographic distribution, ownership, prices, and scope of practice at retail clinics. Annals of Internal Medicine 151(5):315-320.
Ruddy, G. 2007. Health centers’ role in addressing the oral health needs of the medically underserved. Washington, DC: National Association of Community Health Centers.
Sanchez Dils, E., C. Lefebvre, and K. Abeyta. 2004. Teledentistry in the United States: A new horizon of dental care. International Journal of Dental Hygiene 2:161-164.
Scott, M. K. 2009. Retail dental clinics: A viable model for the underserved? Oakland, CA: California HealthCare Foundation.
Scott, M. K. 2010. Dental care in the express lane. Paper presented at meeting of the Committee on Oral Health Access to Services, San Francisco, CA.
Shesser, R. 2010. Oral health emergencies. Paper presented at meeting of the Committee on Oral Health Access to Services, Washington, DC.
Shirk, C. 2010. Oral health checkup: Progress in tough fiscal times? Washington, DC: National Health Policy Forum.
Siegal, M. D., and A. M. R. Detty. 2010. Do school-based dental sealant programs reach higher risk children? Journal of Public Health Dentistry 70(3):181-187.
Silberberg, M., and J. C. Cantor. 2008. Making the case for school-based health: Where do we stand? Journal of Health Politics Policy and Law 33(1):3-37.
Silow-Carroll, S., and T. Alteras. 2004. Community-based oral health programs: Lessons from three innovative models. Battle Creek, MI: W. K. Kellogg Foundation.
Solomon, E. S. 2007. Demographic characteristics of general dental practice sites. General Dentistry 55(6):552-558.
Tennessee Department of Health. 2010. School based dental prevention project. http://health.state.tn.us/oralhealth/school-based.html (accessed January 25, 2011).
Thygeson, M., K. A. Van Vorst, M. V. Maciosek, and L. Solberg. 2008. Use and costs of care in retail clinics versus traditional care sites. Health Affairs 27(5):1283-1292.
University of the Pacific. 2011. Virtual dental home demonstration project. http://dental.pacific.edu/Community_Involvement/Pacific_Center_for_Special_Care_(PCSC)/Projects/Virtual_Dental_Home_Demonstration_Project.html (accessed January 31, 2011).
U.S. Census Bureau. 2010. USA quickfacts from the U.S. Census Bureau. http://quickfacts.census.gov/qfd/states/00000.html (accessed March 9, 2011).
Vanchit, J., M. Papageorge, L. Jahangiri, M. Wheater, D. Cappelli, R. Frazer, and W. Sohn. 2011. Recruitment, development, and retention of dental faculty in a changing environment. Journal of Dental Education 75(1):82-89.
Walker, S. C., S. E. U. Kerns, A. R. Lyon, E. J. Bruns, and T. J. Cosgrove. 2010. Impact of school-based health center use on academic outcomes. Journal of Adolescent Health 46(3):251-257.
Wall, T. P., and L. J. Brown. 2007. The urban and rural distribution of dentists, 2000. Journal of the American Dental Association 138(7):1003-1011.
Wang, M. C., G. Ryan, E. A. McGlynn, and A. Mehrotra. 2010. Why do patients seek care at retail clinics, and what alternatives did they consider? American Journal of Medical Quality 25(2):128-134.
Warren, M. 2010. Statistical analysis and overview of the 2010 GKAS day data. http://www.ada.org/sections/newsAndEvents/pdfs/gkas_statisticalanalysis.pdf (accessed March 16, 2011).
Washington State Hospital Association. 2010. Emergency room use. http://www.wsha.org/files/127/ERreport.pdf (accessed April 11, 2011).
Wendling, W. R. 2010. Private sector approaches to workforce enhancement. Journal of Public Health Dentistry 70(Supp. 1):S24-S31.
Whitten, P., and L. Buis. 2007. Private payer reimbursement for telemedicine services in the United States. Telemedicine and e-Health 13(1):15-24.
Young, T. L., S. L. D’Angelo, and J. Davis. 2001. Impact of a school-based health center on emergency department use by elementary school students. Journal of School Health 71(5):196-198.
Youngblade, L., T. Malasanos, E. Shenkman, S. Aydede, J. Nackashi, S. Tuli, B. Vogel, L. Curry, D. Wegenre, K. Lustig, and P. Sloyer. 2005. Telemedicine for CSHCN: A stateby-state comparison of Medicaid reimbursement policies and Title V activities. Institute for Child Health Policy, University of Florida, Telehealth Connections for Children and Youth.




































