1
Introduction
Recognizing the role of nutrition in maintaining optimal mental and physical condition, the military has long been devoted to ensuring adequate nutrition for its personnel. Service members experience a wide range of environmental and physiological circumstances associated with a variety of situations, including training for or performing combat operations. The current combat operations in Afghanistan (referred to as Operation Enduring Freedom [OEF]) and Iraq (referred to as Operation Iraqi Freedom [OIF]) have also presented new wartime challenges. Since 2001, the OEF and OIF conflicts have been characterized by extended and repeated deployments of a smaller, all-volunteer force, new tactics and weapons (such as improvised explosive devices [IEDs]), and higher rates of injury to the head and neck region than in past conflicts (Owens et al., 2008; Tanielian et al., 2008). Although estimates of incidence and prevalence are elusive, the available data indicate that traumatic brain injury (TBI) is a significant cause of mortality and morbidity in the OEF and OIF conflicts (Elder and Cristian, 2009).
Contributing to nearly one-third of all injury-related deaths in the United States, TBI is also a major health concern for the civilian population, especially because the complications of this injury are not always readily apparent (Faul et al., 2010). The Centers for Disease Control and Prevention (CDC) estimates that 1.7 million people in the United States sustain a TBI each year (Faul et al., 2010). In addition, an estimated 207,830 patients with sports-related TBIs were treated in U.S. emergency departments annually between 2001 and 2005 (Schroeder et al., 2007). Because the CDC surveillance system only draws data from hospitalizations and emergency department visits, the actual burden in the United States is underrepresented in this estimate. In fact, when the data on sports-related brain injuries are extrapolated based on cases involving loss of consciousness, they suggest that on an annual basis, only 5.5–13 percent of patients visit hospital emergency departments. It is therefore estimated that 1.6–3.8 million sports-related TBIs actually occur in the United States annually, including those not treated by a health care provider (Langlois et al., 2006; Schroeder et al., 2007).
The increased attention that the issue of head injuries is receiving from sports leagues
and the military is generating greater overall awareness about this significant public health problem. However, TBI’s mechanisms and its damaging effects on the brain are still not fully understood. The multifactorial injury process of blast injuries—the most frequent cause of TBI in current combat operations—adds to the complexity of TBI. Similarly, multiple clinical trials on the acute treatment of TBI in civilian populations using pharmacological agents targeted at a single aspect of the injury cascade that follows TBI have been largely unsuccessful. Combat-related brain injury and stress disorders (such as posttraumatic stress disorder [PTSD]) as well as sports-related brain injuries have been the topic of several National Academies studies since 2000, including Returning Home from Iraq and Afghanistan: Preliminary Assessment of Readjustment Needs of Veterans, Service Members, and Their Families (IOM, 2010); Gulf War and Health: Volume 7: Long-Term Consequences of Traumatic Brain Injury (IOM, 2009); Opportunities in Neuroscience for Future Army Applications (NRC, 2009); Systems Engineering to Improve Traumatic Brain Injury Care in the Military Health System Workshop Summary (NAE/IOM, 2009); Treatment of Posttraumatic Stress Disorder: An Assessment of the Evidence (IOM, 2008); Evaluating the HRSA Traumatic Brain Injury Program (IOM, 2006a); Posttraumatic Stress Disorder: Diagnosis and Assessment (IOM, 2006b); and Is Soccer Bad for Children’s Heads?: Summary of the IOM Workshop on Neuropsychological Consequences of Head Impact in Youth Soccer (IOM, 2002).
Despite the paucity of evidence on effective treatments for TBI, new information is advancing the understanding of the relationship between nutrition status and brain func-
|
BOX 1-1 Statement of Task An expert committee will review the existing evidence that supports the potential role for nutrition in providing resilience (i.e., protecting), mitigating, or treating of primary (i.e., within minutes of insult) and secondary (i.e., within 24 hours of insult) associated effects of neurotrauma, with a focus on traumatic brain injury. As a background, it will include an overview of types of central nervous system–related neurotrauma (primary and secondary effects) that are most commonly associated with combat operations. Research in promising areas will also be identified. Specifically the committee will respond to the following questions:
|
tion, and increasingly indicates that nutritional interventions could possibly help with the prevention, resilience, or treatment of the acute events of TBI. Because the literature on the pathophysiology and treatment of TBI still contains significant information gaps, this study effectively raises more research questions than it provides specific recommendations for preventive interventions or acute treatments to mitigate an injury.
PURPOSE AND SCOPE OF THE STUDY
For these reasons, the Institute of Medicine (IOM) was requested to convene an ad hoc expert committee under the oversight of the Committee on Military Nutrition Research to review the potential role of nutrients and dietary supplements in the prevention and treatment of TBI. As requested in the statement of task presented in Box 1-1, this study reviews only the potential nutritional implications for primary and secondary physiological sequelae of neurotrauma. Although the effects of TBI (primary, secondary, and long-term effects) are conceptually expressed according to the amount of time elapsed after the initial insult, the boundaries of these definitions are actually ambiguous, and extrapolating the timing of effects from animal models to humans is not always feasible. That is, some of the early pathogenic events related to cell death may extend into the more chronically injured brain, while other pathogenic events typically associated with wound healing are also initiated—and perhaps resolved—within the more acutely injured brain. Given these challenges, this
|
report includes a select number of studies that also evaluate outcomes that are seemingly long term but that might be initiated in the acute phase of the disease. In general, however, long-term health disorders associated with neurotrauma, such as PTSD, neurodegenerative diseases (Alzheimer’s disease or parkinsonism), neurocognitive deficits, psychosocial health problems (e.g., major depression, impairment of social functioning and ability to work, suicide), epilepsy, pain, and other alterations in personality or behavior that might be affected by the nutritional status of the individual are not reviewed in this study.
It also should be noted that descriptions of diagnostics tools, such as imaging techniques or neuropsychological tests, are not included in this report because such descriptions are beyond the scope of the task. Although genetic factors may be identified as increasing risk of TBI effects in the acute and subacute phases in the future, this report does not include discussion of this consideration because the committee is unaware of research identifying genetics as a risk factor of TBI, and it would therefore be premature to make conclusions or recommendations concerning this possibility.
TRAUMATIC BRAIN INJURY
CDC defines TBI as being caused by a bump, blow, or jolt to the head or a penetrating head injury that disrupts the normal function of the brain.1 A penetrating brain injury is the result of an object, such as a bullet, shrapnel, or debris, piercing the skull. A closed head injury is caused by blunt-force trauma that does not break through the skull, as in a fall or hitting a car dashboard. Closed head injuries are commonly categorized by the severity of the symptoms, i.e., as mild, moderate, or severe. The definitions of severity are based on the clinical signs listed in Table 1-1. Mild TBI (mTBI), also referred to as concussion, accounts for over 75 percent of TBIs that occur annually in both civilian and military populations. Concussion and mTBI are often used interchangeably in clinical practice guidelines covering the management of TBI and by military and civilian health-care providers. For the purposes of this report, the two terms frequently appear together to recognize their consistent definitions. Much more is known about the effects of moderate to severe brain injuries, however, than those of mild or concussion injuries.
The cellular- and molecular-level events initiated by injury can be roughly characterized according to their sequence during and following injury (as described in Margulies et al., 2009). The complexity of TBI markedly restricts the precision of such characterization because the emergence and duration of pathogenic events are variable, and can even overlap. Primary effects refer to those effects that arise within minutes. The effects that emerge over the next 24 hours are considered secondary, and are believed to exacerbate the primary neurological damage. In this report, primary and secondary effects are also referred to as acute and subacute effects. Finally, long-term or chronic effects are those that are associated with the injury, but that occur weeks to years later. This characterization, described in greater detail in Chapter 3, served as the basis for the committee’s review of the effectiveness of select nutrients in treating the complex cascade of events initiated during the acute and subacute phases of TBI.
TBI in the Military
The definition of TBI currently used by the military, which has been modified to include combat-related mechanisms, appears in Box 1-2. Between 2000 and 2010, 195,547 service
|
1 |
Available online: http://www.cdc.gov/traumaticbraininjury/ (accessed December 1, 2010). |
TABLE 1-1 Severity Ratings of TBI Based on Clinical Signs
members were diagnosed with TBI.2 This number includes injuries sustained in both combat operations and in garrison. The leading causes of TBI in the military are blasts, fragments, bullets, motor vehicle crashes, and falls (DoD, 2010). Figure 1-1 breaks down the incidence of TBI for 2000 through 2010 by severity, according to the clinical classifications listed in Table 1-1.
The epidemiological data for combat-related TBI, especially blast-induced and mild TBI, are still evolving, with some researchers finding that 10–20 percent of returning veterans have sustained a TBI (Hoge et al., 2008; Tanielian et al., 2008; Terrio et al., 2009), while others estimate that TBI accounts for up to one-third of combat-related injuries in Iraq and Afghanistan (Meyer et al., 2008). About 78 percent of the TBIs occurring in 2009 across all military services were classified as mild,3 which has generated great concern for the military because of their high incidence, persistent health outcomes, and the often unnoticeable effects at the time of injury. The 2009 IOM report on long-term consequences of TBI identified several outcomes that can persist even after mTBI, including unprovoked seizures, depression, aggression, and postconcussion symptoms. These symptoms include headache; dizziness; fatigue; irritability; subjective concentration difficulty; memory impairment; insomnia; and reduced tolerance to stress, emotional excitement, or alcohol. The report also highlighted the research finding of a dose-response relationship with regard to severity of injury and outcome; that is, the more severe the TBI, the more severe the outcome (IOM, 2009).
Concurrent disorders have been found common among TBI patients, particularly post-traumatic stress disorder and other mental health disorders, substance abuse, and risk of suicide (Tanielian et al., 2008; Warden, 2006). The 2010 IOM report on readjustment needs indicated a greater prevalence of many of these health outcomes than in previous conflicts. Furthermore, in a study of more than 2,000 U.S. Army infantry soldiers three to four months after their return from Iraq, Hoge et al. (2008) found the highest prevalence of PTSD occurred among soldiers who had lost consciousness, suggesting a stronger association between TBI and PTSD than other types of injury and PTSD. This relationship is complicated and still not completely understood because of the overlap of symptoms between PTSD, TBI, and postconcussion syndrome.
The increased use of IEDs in the current conflicts has produced more blast-related injuries than previous combat operations. Approximately two-thirds of medical evacuations are blast-induced injuries, and these can often involve concurrent injuries resulting in cognitive, physical, or psychological impairments (commonly referred to as polytrauma), necessitating
|
2 |
Available online: http://www.dvbic.org/TBI-Numbers.aspx (accessed February 25, 2011). |
|
3 |
Available online: http://www.dvbic.org/TBI-Numbers.aspx (accessed December 1, 2010). |
|
BOX 1-2 Department of Defense Definition of Traumatic Brain Injury (2007) A traumatically induced structural injury and/or physiological disruption of brain function as a result of an external force that is indicated by new onset or worsening of at least one of the following clinical signs immediately following the event:
External forces may include any of the following events:
|
multiple health-care services (IOM, 2010; Warden, 2006). Of 433 TBI patients from OEF and OIF being treated at Walter Reed Army Medical Center between 2003 and 2005, 19 percent also required an amputation (Warden, 2006; Warden et al., 2005). TBI outcomes can be affected by some of these associated injuries. Significant blood loss and dehydration can produce hypotension, which has been associated with more adverse outcomes. A single
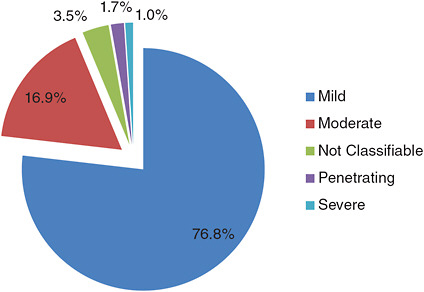
FIGURE 1-1 TBI Categories, 2000-2010Q3.
NOTE: Numbers for the current year are updated on a quarterly basis. 2009-2010Q3 numbers updated as of November 15, 2010.
SOURCE: See http://www.dvbic.org/TBI-Numbers.aspx (accessed December 1, 2010).
hypotensive episode during the prehospital phase of severe TBI has been associated with doubling of mortality and increased morbidity (Fearnside et al., 1993). In polytrauma situations where the other injuries require more immediate medical attention, it can be especially difficult to identify cases of mild or concussion injuries. Similar to the evidence on the detrimental long-term effects of repetitive sports-related concussion injuries and second impact syndrome, exposure to multiple blasts has been linked to increased probability of further injury that can result in long-term physical and psychological impairments (Lew et al., 2006, 2007; Tanielian et al., 2008). The understanding of blast as a contributing mechanism to TBI—and its clinical similarities to and differences from other forms of TBI—continues to evolve. A summary of some recent findings is included in the discussion on pathobiology found in Chapter 3.
The reader is referred to the workshop papers by Col. Michael Jaffee, Dr. Mårten Risling, and Col. Geoffrey Ling in Appendix C for greater detail on the epidemiology of TBI in the military.
Sports-Related Brain Injuries
With nearly half of Americans of all ages participating in non-work-related sports activities annually, there are ample opportunities for sports-related injuries, despite the health benefits of being physically active (Schroeder et al., 2007). Almost 16 percent of all cases of injury in the United States between 2004 and 2005 occurred during sports or exercise (Bergen et al., 2008). Among people under the age of 25, sports injuries are most prevalent, accounting for about 30 percent of all injury episodes (Bergen et al., 2008). The risk for sports-related TBI is likewise particularly high for children and adolescents, who had the highest rates among those treated in hospital emergency departments (Schroeder et al., 2007). Overall, an estimated 1.6–3.8 million sports-related TBIs occur in the United States each year (Langlois et al., 2006).
A review of the literature indicates that the blast-induced brain injuries most commonly seen in the military population have pathological characteristics that differ from other TBIs, despite their similar secondary effects (Cernak and Noble-Haeusslein, 2010). Although more research is needed to differentiate and draw parallels between the various injury mechanisms, much is being shared between the military and sports communities, particularly on the assessment and management of concussions. Because of the parallels between the acute pathological effects of blast-induced brain injuries and other injury mechanisms, the nutrients considered in this report can similarly be considered for sports-related and other civilian brain injuries.
STUDY APPROACH AND ORGANIZATION OF THE REPORT
From patient to patient, brain injuries are remarkably diverse. Apart from differences in the cause and severity of the injury, the insult initiates a complex cascade of mechanistic events, making it impossible for any therapeutic intervention to target a single event. The ability of nutrients to interact with a variety of physiological and metabolic injury responses suggests the advantage of nutritional approaches to the treatment of TBI. The committee believes that nutritional approaches, or interventions, should not been seen as singular therapies but rather as complementary or supportive of other therapies. The committee considers nutritional interventions to range from the clinical support provision of essential nutrients and energy for recovery from major trauma, to individual nutrients or dietary supplements that may uniquely alter the repair process. It is from this perspective that the committee approached its charge.
Initial work for this study began at a June 2008 meeting of the IOM Committee of Military Nutrition Research, with various researchers and neurosurgeons attending. Potential mechanistic targets, such as inflammation or mitochondrial dysfunction, were identified as relevant to the consideration of nutritional interventions for TBI. A preliminary exploration of the published literature was conducted, and several nutrients were selected for further exploration of their effectiveness in alleviating or mitigating various components of the injury process.
In spring of 2010, the IOM appointed a committee of 11 experts with extensive knowledge across both military and civilian populations in the areas of neurology; nutritional sciences, clinical nutrition, and dietetics; physiology; physical medicine and rehabilitation; psychiatry and behavior; biochemical and molecular neuroscience; epidemiology/methodology; and the pathobiology of traumatic brain injury. The committee gathered further information during two public workshops in June and October 2010 that featured presentations by civilian and military subject matter experts on TBI in the military, the pathophysiology of TBI, nutritional considerations in the clinical management of TBI, and various nutritional interventions studied in animal and human models of brain injury or other brain disorders.
The committee conducted a review of the scientific literature to examine physiological sequelae and metabolic responses to TBI. After identifying neuroprotective targets possibly responsive to nutritional interventions, the committee established a search plan to investigate the effect of promising nutrients on outcomes of brain injury, stroke, hypoxia, epilepsy, and subarachnoid hemorrhage. These additional conditions were selected for the literature review because of their pathophysiological similarities to the secondary events associated with TBI. Based on expert consultation, discussions, and their review of the literature, the committee focused on nutritional approaches that have demonstrated some level of efficacy in relevant physiological processes. The details of the committee’s approach to identifying the most promising nutrients that may be of benefit for the treatment of or resilience to TBI are described in Chapter 4. As with other ad hoc study reports prepared by The National Academies, the recommendations in the following chapters were reached by consensus.
In their comprehensive examination of the literature, the committee addressed the question of which specific nutritional approaches have been shown to enhance efficacy of treatment for patients experiencing neurotrauma, as well as which nutritional strategies might help with resilience to brain injury. The committee’s approach to reviewing the literature for the selected nutritional interventions targeted brain injuries with physiological effects similar to those of TBI (subarachnoid hemorrhage, hypoxia-ischemia, stroke, and epilepsy) because there was not enough evidence solely from TBI models for a thorough evaluation. The review did not include the preventive literature on other areas such as brain health and cognitive function of healthy individuals. The committee also reviewed current practice guidelines for specific nutritional approaches to the clinical treatment of TBI on the battlefield, in garrison, or in hospital intensive care units.
This report has been organized into three major sections based on the breakdown of the committee’s charge. Part I provides a background on the acute effects of neurotrauma most commonly associated with combat operations. Chapter 2 reviews the current clinical practice guidelines across all levels of severity of TBI, highlighting those practices that specify nutritional approaches for treatment and recovery. Chapter 3 provides background on the pathophysiological changes that accompany TBI. This review of the physiological mechanisms of TBI serves as the committee’s framework for the selection of nutrients, based on functions and mechanisms of action that suggest they might promote resilience and/or be efficacious when provided after TBI. Part II outlines the preliminary selection of nutritional interventions for TBI (Chapter 4), the importance of nutrition in resilience to TBI (Chapter
5), and energy and protein needs during early feeding following TBI (Chapter 6). Chapters 7 through 16 discuss the evidence on the nutrients and dietary supplements reviewed by the committee. Part III presents a summary of the committee’s findings and conclusions, and highlights its recommendations on promising areas for future research. Chapter 17 includes a breakdown of research, organized by topic, needed to overcome gaps in information, including assessing nutrition status of military personnel and TBI patients, improving animal models and identifying biomarkers of TBI, and prioritizing research that would address questions of TBI treatment efficacy for the most promising nutrients. Appendixes provide the workshop agenda, relevant nutrition advice in current clinical guidelines, workshop presentations, biographical sketches of committee members and speakers, a glossary of terms, and a list of acronyms and abbreviations.
REFERENCES
Bergen, G., L. H. Chen, M. Warner, and L. A. Fingerhut. 2008. Injury in the United States: 2007 chartbook. Hyattsville, MD: National Center for Health Statistics.
Cernak, I., and L. J. Noble-Haeusslein. 2010. Traumatic brain injury: An overview of pathobiology with emphasis on military populations. Journal of Cerebral Blood Flow and Metabolism 30(2):255–266.
DoD (Department of Defense). 2010. Mild traumatic brain injury pocket guide (conus). Washington, DC.
Faul, M., L. Xu, M. M. Wald, and V. G. Coronado. 2010. Traumatic brain injury in the United States: Emergency department visits, hospitalizations and deaths 2002–2006. Atlanta, GA: Centers for Disease Control and Prevention.
Fearnside, M. R., R. J. Cook, P. McDougall, and R. J. McNeil. 1993. The Westmead head-injury project outcome in severe head-injury—A comparative-analysis of prehospital, clinical and CT variables. British Journal of Neurosurgery 7(3):267–279.
Hoge, C. W., D. McGurk, J. L. Thomas, A. L. Cox, C. C. Engel, and C. A. Castro. 2008. Mild traumatic brain injury in U.S. soldiers returning from Iraq. The New England Journal of Medicine 358(5):453–463.
IOM (Institute of Medicine). 2002. Is soccer bad for children’s heads? Summary of the IOM workshop on neuropsychological consequences of head impact in youth soccer. Washington, DC: National Academy Press.
IOM. 2006a. Evaluating the HRSA Traumatic Brain Injury Program. Washington, DC: The National Academies Press.
IOM. 2006b. Posttraumatic stress disorder: Diagnosis and assessment. Washington, DC: The National Academies Press.
IOM. 2008. Treatment of posttraumatic stress disorder: An assessment of the evidence. Washington, DC: The National Academies Press.
IOM. 2009. Gulf War and health: Long-term consequences of traumatic brain injury. Vol. 7. Washington, DC: The National Academies Press.
IOM. 2010. Returning home from Iraq and Afghanistan: Preliminary assessment of readjustment needs of veterans, service members, and their families. Washington, DC: The National Academies Press.
Langlois, J. A., W. Rutland-Brown, and M. M. Wald. 2006. The epidemiology and impact of traumatic brain injury: A brief overview. Journal of Head Trauma Rehabilitation 21(5):375–378.
Lew, H. L., J. H. Poole, S. B. Guillory, R. M. Salerno, G. Leskin, and B. Sigford. 2006. Persistent problems after traumatic brain injury: The need for long-term follow-up and coordinated care. Journal of Rehabilitation Research and Development 43(2):vii–x.
Lew, H. L., D. Thomander, K. T. L. Chew, and J. Bleiberg. 2007. Review of sports-related concussion: Potential for application in military settings. Journal of Rehabilitation Research and Development 44(7):963–973.
Margulies, S., R. Hicks, and Combination Therapies for Traumatic Brain Injury Workshop Leaders. 2009. Combination therapies for traumatic brain injury: Prospective considerations. Journal of Neurotrauma 26(6):925–939.
Meyer, K., K. Helmick, S. Doncevic, and R. Park. 2008. Severe and penetrating traumatic brain injury in the context of war. Journal of Trauma Nursing 15(4):185–189; quiz 190–181.
NAE/IOM (National Academy of Engineering/Institute of Medicine). 2009. Systems engineering to improve traumatic brain injury care in the military health system workshop summary. Washington, DC: The National Academies Press.
NRC (National Research Council). 2009. Opportunities in neuroscience for future army application. Washington, DC: The National Academies Press.
Owens, B. D., J. F. Kragh, J. C. Wenke, J. Macaitis, C. E. Wade, and J. B. Holcomb. 2008. Combat wounds in Operation Iraqi Freedom and Operation Enduring Freedom. Journal of Trauma-Injury Infection and Critical Care 64(2):295–299.
Schroeder, T., C. Irish, J. L. Annest, T. Haileyesus, K. Sarmiento, and J. Mitchko. 2007. Nonfatal traumatic brain injuries from sports and recreation activities—United States, 2001–2005 Morbidity and Mortality Weekly Report 56(29):733–737.
Tanielian, T. L., and L. Jaycox. 2008. Invisible wounds of war psychological and cognitive injuries, their consequences, and services to assist recovery. http://site.ebrary.com/lib/natacademies/Doc?id=10246315 (accessed October 26, 2010).
Terrio, H., L. A. Brenner, B. J. Ivins, J. M. Cho, K. Helmick, K. Schwab, K. Scally, R. Bretthauer, and D. Warden. 2009. Traumatic brain injury screening: Preliminary findings in a U.S. Army Brigade Combat Team. Journal of Head Trauma Rehabilitation 24(1):14–23.
Warden, D. 2006. Military TBI during the Iraq and Afghanistan wars. Journal of Head Trauma Rehabilitation 21(5):398–402.
Warden, D. L., L. M. Ryan, K. M. Helmick, K. Schwab, L. French, W. Lu, W. Lux, G. Ling, and J. Ecklund. 2005. War neurotrauma: The Defense and Veterans Brain Injury Center (DVBIC) experience at Walter Reed Army Medical Center (WRAMC). Journal of Neurotrauma 22(10):1163–1258.










