Summary
Lesbian, gay, bisexual, and transgender (LGBT) individuals experience unique health disparities. Although the acronym LGBT is used as an umbrella term, and the health needs of this community are often grouped together, each of these letters represents a distinct population with its own health concerns. Furthermore, among lesbians, gay men, bisexual men and women, and transgender people, there are subpopulations based on race, ethnicity, socioeconomic status, geographic location, age, and other factors. Although a modest body of knowledge on LGBT health has been developed, these populations, stigmatized as sexual and gender minorities, have been the subject of relatively little health research. As a result, a number of questions arise: What is currently known about the health status of LGBT populations? Where do gaps in the research exist? What are the priorities for a research agenda to address these gaps?
At the request of the National Institutes of Health (NIH), the Institute of Medicine convened a consensus committee to answer these questions. The 17-member Committee on Lesbian, Gay, Bisexual, and Transgender Health Issues and Research Gaps and Opportunities comprised experts in the fields of mental health, biostatistics, clinical medicine, adolescent health and development, aging, parenting, behavioral sciences, HIV research, demography, racial and ethnic disparities, and health services. The committee was asked to
-
conduct a review and prepare a report assessing the state of the science on the health status of lesbian, gay, bisexual, and transgender populations; identify research gaps and opportunities; and outline a research agenda that will assist NIH in enhancing its research efforts in this area.
STUDY APPROACH
In conducting this study, the committee used a variety of sources: five formal committee meetings, including four public meetings with presentations from researchers, individuals, advocacy groups, and service providers; a literature review; commissioned papers; and consultants. The committee’s work was guided by four conceptual frameworks:
-
The life-course framework acknowledges that events at each stage of life influence subsequent stages and recognizes that experiences are shaped by one’s age cohort and historical context.
-
The minority stress model posits that sexual and gender minorities experience chronic stress as a result of their stigmatization.
-
Intersectionality examines an individual’s multiple identities and the ways in which they interact.
-
The social ecology perspective emphasizes that individuals are surrounded by spheres of influence, including families, communities, and society.
These frameworks complement each other and structured and informed the committee’s deliberations.
CONTEXT FOR UNDERSTANDING LGBT HEALTH
The committee believed that to examine the health of LGBT people, it was important to understand the contextual factors that influence their lives. Some of those factors include the history of LGBT people in the United States, the effects of stigma, laws and policies, demographic factors, and barriers to care. These factors are interrelated. For example, many historical events have contributed to the stigmatization of nonheterosexual and gender-variant individuals. The inclusion of homosexuality in the Diagnostic and Statistical Manual of Mental Disorders until 1973 shaped sexual-minority patients’ interactions with the health care system. Likewise, the legal landscape affects aspects of people’s lives that influence health. For instance, laws prohibiting marriage between same-sex individuals often affect the access of lesbians, gay men, and bisexual people to employer-sponsored health insurance. Other barriers to care include the limited availability of providers with adequate training to treat transgender patients in a culturally competent manner and LGBT patients’ previous negative experiences with the health care system.
The HIV/AIDS epidemic resulted in the deaths of thousands of gay and bisexual men; at the same time, it created a resilient and more unified LGBT community. HIV/AIDS remains one of the most critical health issues faced by some subgroups within LGBT populations in the United States—
particularly gay and bisexual men, as well as transgender women. The epidemic serves as an example of some of this report’s key themes: not only resilience, but also stigma, racial and ethnic disparities, and the importance of research funding.
CHALLENGES TO CONDUCTING RESEARCH ON LGBT POPULATIONS
A number of challenges are associated with conducting health research on LGBT populations. These include the following:
-
Sexual orientation and gender nonconformity are multifaceted concepts, and defining them operationally can be challenging.
-
Individuals may be reluctant to answer research questions about their same-sex sexual behavior or gender nonconformity.
-
Because LGBT populations represent a relatively small proportion of the U.S. population, it is labor-intensive and costly to recruit a large enough sample in general population surveys for meaningful analysis of these populations and their subgroups.
Despite these challenges, many researchers currently conduct health research on LGBT populations. In so doing, as with research on any populations, researchers must choose a sampling strategy and a data collection method. While probability samples allow findings to be generalized to the study’s target population, they are expensive and difficult to implement with LGBT populations given the research challenges listed above. However, the use of established statistical techniques makes it possible to improve the precision of estimates for small populations by combining two or more data sets.
Research on the health status of LGBT populations more commonly uses nonprobability samples. Even though the extent to which findings based on such samples accurately characterize these populations is unknown, these samples have yielded valuable information for expanding the field of LGBT research and identifying possible gaps in health services. In addition to providing general descriptive data for LGBT populations and their subgroups, nonprobability samples have served to reveal the existence of certain phenomena, to suggest relationships among variables, to identify possible differences among groups, and to generate hypotheses and formulate ideas that can be advanced for systematic study in the future. A variety of methods are used to generate nonprobability samples, including purposive, quota, and snowball sampling. While much of what is currently known about the health of LGBT populations comes from studies with nonprobability samples, the field of LGBT health would benefit if more data came from probability samples.
Best practices for research on the health status of LGBT populations include scientific rigor and respectful involvement of individuals who represent the target population. Scientific rigor includes incorporating and monitoring culturally competent study designs, such as the use of appropriate measures to identify participants and implementation processes adapted to the unique characteristics of the target population. Respectful involvement refers to the involvement of LGBT individuals and those who represent the larger LGBT community in the research process, from design through data collection to dissemination.
HEALTH STATUS OVER THE LIFE COURSE
Drawing on the life-course framework, the committee examined the health status of LGBT populations in three life stages: childhood and adolescence, early/middle adulthood, and later adulthood. Within these age blocks, the committee looked at mental health, physical health, risk and protective factors, health services, and contextual influences. Research on sexual- and gender-minority populations has been uneven. More research has focused on gay men and lesbians than on bisexual and transgender people. Research has not adequately examined subpopulations, particularly racial and ethnic groups. Most research has been conducted among adults; very few studies have focused on children, more on adolescents and young adults, and few again on LGBT elders. Some of the key findings of this study across the life course are summarized below.
Childhood/Adolescence
-
The burden of HIV falls disproportionately on young men, particularly young black men, who have sex with men.
-
LGB youth are at increased risk for suicidal ideation and attempts as well as depression. Small studies suggest the same may be true for transgender youth.
-
Rates of smoking, alcohol consumption, and substance use may be higher among LGB than heterosexual youth. Almost no research has examined substance use among transgender youth.
-
The homeless youth population comprises a disproportionate number of LGB youth. Some research suggests that young transgender women are also at significant risk for homelessness.
-
LGBT youth report experiencing elevated levels of violence, victimization, and harassment compared with heterosexual and non-gender-variant youth.
-
Families and schools appear to be two possible focal points for intervention research.
Early/Middle Adulthood
-
As a group, LGB adults appear to experience more mood and anxiety disorders, more depression, and an elevated risk for suicidal ideation and attempts compared with heterosexual adults. Research based on smaller convenience samples suggests that elevated rates of suicidal ideation and attempts as well as depression exist among transgender adults; however, little research has examined the prevalence of mood and anxiety disorders in this population.
-
Lesbians and bisexual women may use preventive health services less frequently than heterosexual women.
-
Lesbians and bisexual women may be at greater risk of obesity and have higher rates of breast cancer than heterosexual women.
-
HIV/AIDS continues to exact a severe toll on men who have sex with men, with black and Latino men being disproportionately affected.
-
LGBT people are frequently the targets of stigma, discrimination, and violence because of their sexual- and gender-minority status.
-
LGB adults may have higher rates of smoking, alcohol use, and substance use than heterosexual adults. Most research in this area has been conducted among women, with much less being known about gay and bisexual men. Limited research among transgender adults indicates that substance use is a concern for this population.
-
Gay men and lesbians are less likely to be parents than their heterosexual peers, although children of gay and lesbian parents are well adjusted and developmentally similar to children of heterosexual parents.
Later Adulthood
-
Limited research suggests that transgender elders may experience negative health outcomes as a result of long-term hormone use.
-
HIV/AIDS impacts not only younger but also older LGBT individuals. However, few HIV prevention programs target older adults, a cohort that also has been deeply affected by the losses inflicted by AIDS.
-
There is some evidence that LGBT elders exhibit crisis competence (a concept reflecting resilience and perceived hardiness within older LGBT populations).
-
LGBT elders experience stigma, discrimination, and violence across the life course.
-
LGBT elders are less likely to have children than heterosexual elders and are less likely to receive care from adult children.
RECOMMENDATIONS
The committee’s primary recommendation is the implementation of a research agenda that will assist NIH in enhancing its research efforts in the area of LGBT health. The committee also recommends six additional actions to advance understanding of LGBT health.
Research Agenda
Recommendation 1. NIH should implement a research agenda designed to advance knowledge and understanding of LGBT health.
The committee believes that building the evidence base on LGBT health issues will not only benefit LGBT individuals but also provide new research on topics that affect heterosexual and non-gender-variant individuals as well. Given the large number of areas in LGBT health in which research is needed, the committee formulated a research agenda that reflects those areas of highest priority. Within each of those areas, the conceptual frameworks identified above are evident as cross-cutting perspectives that should be considered. Figure S-1 illustrates the interactions between the priority research areas identified by the committee and these cross-cutting perspectives.
As noted above, although lesbians, gay men, bisexual men and women, and transgender people each are separate populations, they frequently are considered as a group. The primary driving force behind combining these populations is that they are nonheterosexual or gender nonconforming
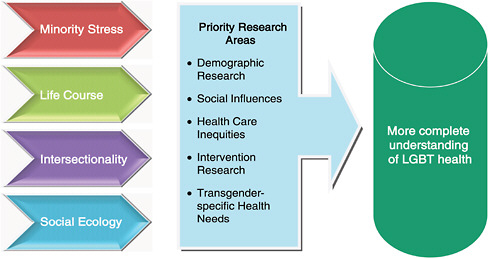
FIGURE S-1 Research agenda. A number of different conceptual perspectives can be applied to priority areas of research in order to further the evidence base for LGBT health issues.
and are frequently stigmatized as a consequence. These populations also are often combined in some way for research purposes. For example, researchers frequently merge lesbians, gay men, and bisexual people into a group labeled “nonheterosexual.” Similarly, in some HIV research, study participants are combined in a single category that may include gay men, bisexual men, transgender women, and men who do not identify as any of the above but still have sex with other men. Combining these populations in this way obscures differences among them.
Given that lesbians, gay men, bisexual women and men, and trans-gender people are in fact separate populations, it is important to note that most of the research on these populations has focused on lesbians and gay men. Much less research has been conducted on bisexual and transgender people. The committee therefore recommends research that focuses on all of these populations.
Cross-Cutting Perspectives
The following perspectives should inform research on LGBT health:
-
A minority stress perspective—Experiences of stigma shared by sexual and gender minorities and the impact of minority stress should be considered.
-
A life-course perspective—Cohort and age differences influence health needs. Longitudinal studies and studies that analyze data with respect to different age groups are needed to gain a better understanding of LGBT health.
-
An intersectional perspective—Sexual- or gender-minority status is only one of many factors that influence the lives and health of individuals. An examination of the health status of LGBT people in the context of racial, ethnic, socioeconomic, and geographic diversity will provide a more complete understanding.
-
A social ecological perspective—An individual’s health is affected by community and social circumstances. LGBT health research should consider both the individual and the various contexts, including interpersonal relationships, in which the individual lives.
Research Areas
Research in the following areas is essential for building a solid evidence base in LGBT health:
-
Demographic research—More demographic data on lesbian, gay, bisexual, and transgender people across the life course are needed, as are data on LGBT subpopulations.
-
Social influences on the lives of LGBT people—Social support plays an important part in mental health. The role of social structures— such as families, schools, workplaces, religious institutions, and community organizations—in the lives of LGBT people should be understood more fully.
-
Inequities in health care—LGBT people face barriers to equitable health care that profoundly affect their overall well-being. Understanding outcome disparities, provider attitudes and education, ways in which the care environment can be improved, and the experiences of LGBT individuals seeking care would provide a base from which to address these inequities.
-
Intervention research—Research is needed to develop and test the effectiveness of interventions designed to address health inequities and negative health outcomes experienced by LGBT people. Interventions that increase access to care or address the mental or physical conditions that lead to impaired health would assist in reducing these disparities. Interventions focused on subgroups are especially needed.
-
Transgender-specific health needs—An evidence base for providing transgender-specific health care to address gender dysphoria should be created. Most such research is based on small, non-probability samples. A more rigorous research program is needed to understand the health implications of hormone use and other transgender-specific issues.
Research Gaps and Opportunities
In its statement of task, the committee was asked to identify research gaps and opportunities related to LGBT health. In the committee’s view, one sets out to identify research gaps by reviewing a body of evidence that needs additional work in selected areas. However, this was not the committee’s experience in reviewing the literature on LGBT health. Instead, the committee found that the existing body of evidence is sparse and that substantial research is needed. The positive view of this situation is that there are many research opportunities related to LGBT health.
The research agenda proposed by the committee was drawn from the many research opportunities that currently exist. All of the topics on this agenda represent multiple opportunities for research that extends across the life course. In some cases, the focus is on specific subpopulations or fields, while in others it is on types of research or particular contexts. While not representing an exhaustive list, some specific research opportunities are noted at the end of Chapters 2 through 6 and in Chapter 7 in Table 7-1.
Data Collection
Recommendation 2. Data on sexual orientation and gender identity should be collected in federally funded surveys administered by the Department of Health and Human Services and in other relevant federally funded surveys.
Similar to race and ethnicity data, data on sexual and gender minorities should be included in the battery of demographic information that is collected in federally funded surveys. These data would help those seeking to undertake the demographic research recommended as part of the research agenda proposed by the committee. For example, given the interactions between social and economic circumstances and health, data from social and economic surveys could provide valuable information on the context for health disparities experienced by LGBT people. Similarly, surveys on crime and victimization, housing, and families would provide data on variables that relate to the health of sexual and gender minorities. This data collection would be aided by the development of standardized measures for sexual orientation and gender identity (see Recommendation 4 below).
Recommendation 3. Data on sexual orientation and gender identity should be collected in electronic health records.
The Office of the National Coordinator for Health Information Technology within the Department of Health and Human Services should include the collection of data on sexual orientation and gender identity as part of its meaningful-use objectives for electronic health records. Collecting these detailed patient-level data, with adequate privacy and security protection as is needed for all data collected in electronic health records, could assist in identifying and addressing LGBT health disparities. At present, possible discomfort on the part of health care workers with asking questions about sexual orientation and gender identity, a lack of knowledge by providers of how to elicit this information, and some hesitancy on the part of patients to disclose this information may be barriers to the collection of meaningful data on sexual orientation and gender identity. Nonetheless, the committee encourages the Office of the National Coordinator to begin planning for the collection of these data as part of the required set of demographic data for electronic health records. Detailed patient-level data such as those found in electronic health records could provide a rich source of information about LGBT populations and subpopulations.
Methodological Research
Recommendation 4. NIH should support the development and standardization of sexual orientation and gender identity measures.
NIH should support the rigorous development of valid, reliable measures focused on sexual orientation and gender identity. The development
and adoption of standardized measures in federally funded surveys would assist in synthesizing scientific knowledge about the health of sexual and gender minorities.
Recommendation 5. NIH should support methodological research that relates to LGBT health.
NIH should support research that will assist in addressing the methodological challenges associated with conducting research on LGBT health. Particularly helpful would be studies aimed at developing innovative ways to conduct research with small populations and determining the best ways to collect information on sexual and gender minorities in research, health care, and other settings.
Research Training
Recommendation 6. A comprehensive research training approach should be created to strengthen LGBT health research at NIH.
To encourage more research on LGBT health issues, NIH should expand its intramural and extramural training programs, focusing on three audiences: researchers who are working with or considering working with LGBT populations, researchers who may not be aware of LGBT health issues, and NIH staff. Training opportunities should be provided to postbaccalaureate, postdoctoral, graduate student, and career researchers.
Policy on Research Participation
Recommendation 7. NIH should encourage grant applicants to address explicitly the inclusion or exclusion of sexual and gender minorities in their samples.
Using the NIH policy on the inclusion of women and minorities in clinical research as a model, NIH should encourage grant applicants to address explicitly the extent to which their proposed sample includes or excludes sexual and gender minorities. Researchers would thereby be prompted to consider the scientific implications of including or excluding sexual and gender minorities and whether these groups will be included in sufficient numbers to permit meaningful analyses.










