INTERNATIONAL APPROACHES AND PRINCIPLES FOR DISTRESS, PAIN, AND EUTHANASIA
David Morton
Mental distress is arguably the biggest single enduring adverse effect on laboratory animals during their lives, and with the greatest impact on the science. It is not pain but fear and poor housing and poor husbandry systems that inflict most animal suffering during their lifetimes.
Although pain and distress are addressed in guidance and legislation, distress is still overlooked as a source of poor animal welfare and also poor science. In my view, pain has been overemphasized, mainly because it is of greater public concern and a more obvious target for nongovernmental organizations. However, this is now changing with current public concern about the welfare of animals in zoos, breeding of companion animals, and particularly farm animal husbandry and rearing systems.
The debate has moved away from pain to one about the quality of an animal’s life and how we can measure that. Even though there may be events that cause temporary pain, it is the suffering over a lifetime that probably matters most. Captive animals, including those kept for research, are held in impoverished conditions compared with the ecological niches into which they have evolved. In other words, we do not really meet their physiological and mental needs in terms of their evolutionary background. But of course we meet their vital needs; we have to.
Many laboratory animals have well-developed senses like smell, sound, sight, touch, and taste to survive in the world, and husbandry systems do not normally fulfill many of these evolutionary needs. Neither has domestication removed them, as, when domesticated animals are released into the wild, they soon adopt the ways of their progenitors. So there is still a need to meet these needs.
Imagine what you would miss if you were kept in a cell in solitary confinement. The same diet day in day out, without any sun, wind, rain and other forms of precipitation, with little sensory changes in sound, textures other than metal bars, bedding, or plastic, concrete, metal floors and walls, no choice of mates, without space to run, being unable to go where you want to go, and so on. This is why I say that keeping animals in captivity is impoverished for them. So keeping animals in such life-sustaining but otherwise inadequate housing conditions for the whole of their lives may cause considerable long-term suffering. That is one reason for my statement that fear, poor housing, and poor husbandry systems inflict most animal suffering during their lifetimes. Even best practice still compromises animal welfare considerably.
Of course there is no easy answer to this conundrum, as we have to confine animals to carry out research on them. But I believe we can do more to improve the quality of their shortened lives.
Furthermore, the evidence for what is acceptable or at least unacceptable for the animals is often not there. Only when animals die prematurely is there concern. In the meantime, how does one decide what to do, what to provide? Who gets the benefit of the doubt when the science can provide no answers—is it the human or the animal?
In science, the traditional surgical and physiological procedures that were once carried out are gradually being replaced by investigations using transgenic and genetically modified animals and this makes the issues of meeting their mental needs even more of an imperative. For instance, in the UK in 2007, genetically modified and mutant animals and their breeding accounted for nearly 50% of all animal experiments. Only 39% underwent “traditional” procedures of such severity that they required an anesthetic, and the number used for human clinical research was less than 1%. However, there will be more animals undergoing surgical interventions for purposes other than clinical research and all animals in laboratories will suffer the chronic distress of poor living conditions.
While pain is a well-defined and relatively well-understood area of animal physiology and pathology, it is treatable, and so it is often not necessary to keep animals in pain or to cause pain to animals unless there is an overriding scientific reason—for example, research on pain. This is yet another reason why poor mental health (i.e., distress) is so important: it is often unavoidable. I’m not saying that pain is unimportant—it is (Matt Leach will address pain in his talk); but distress is a neglected source of animal suffering.
The annual reports on animal suffering show some interesting differences between countries and the way they handle distress. Most do not separate distress but combine it with pain. Others do not separate intensity and duration of either pain or distress in any meaningful way. Most countries record only predicted adverse effects, while others estimate the adverse effects that actually occurred (i.e., a retrospective recording). The important point is that all countries recognize the term distress as well as pain. So how do we go about measuring pain and distress?
To understand animal suffering it is important to appreciate that animals cannot just be reduced to their component parts, which is the traditional scientific reductionist approach. Pain and distress are more than the sum of their component parts.
Mental distress (which I see as part of mental health) is reflected in several emotional states and is a more complex experience than pain. It embraces feelings like fear, boredom, frustration, malaise, inappetence, thirst. Animals are conscious beings; they respond to adverse external and internal stimuli as a whole, that is, they show an integrated multimodal response to a negative stimulus. Thus animals in pain have raised corticosteroid levels together with a range of physiological and behavioral changes from normal. They are likely also to experience distress states such as fear when they associate their condition with environmental factors such as a particular room or a particular person and an unpleasant experimental intervention, such as an injection. Memory is an important component in mammalian (and probably in all the other classes of the phylum Chordata) pain and distress.
Several of these adverse mental states can occur in the same animal at the same time. An animal is unlikely to experience just one state at a time, especially pain. However, a reductionist approach in science induces us to concentrate on just one aspect at a time. It is very important that a more holistic approach be taken. For example, an animal with a painful broken leg will be in some form of mental distress as well as pain. When the veterinarian who examined the leg reappears the animal may be fearful that she will cause it to feel pain again.
Mental distress causes a mixture of feelings or emotions that can influence bodily responses that increase the possibility for confounding scientific observations. Several years ago, a disturbance index was used to assess how animals behaved after they had had an injection. That was a rather interesting approach, but it has never been followed up. Animals became hyperactive or hypoactive after they had been subjected to a procedure such as an injection of cold saline, or an injection with a large needle size, or large volume. Differences in their responses were observed, and it might be possible to interpret these differences but the work was never completed.
However, there are other indirect and nonspecific physiological measures of distress including blood hormones such as cortisol, organ responses to hormonal changes, neurochemical binding patterns in the brain and spinal cord, and responses to known pharmacological agents. We are aware of many of these responses that potentially will confound the data being collected such as the impact of catecholamines on heart rate and blood pressure, [or] the effects of cortisol on the immune system. We may also be able to use such known actions to make a diagnosis of an animal’s emotional state. For example, if animals change their behavior after they have been given an analgesic, then that is some evidence that they were in pain. Increased heart rate, body temperature, and blood pressure as a result of catecholamine release could be a measure of fear
and anxiety. However, measuring hormonal levels is impractical; observing animals for changes in their behavior is more feasible.
Stress physiologists look at hormone levels and use the term “distress” for animals that are not coping with their environment and in which the whole endocrine system can eventually become unresponsive. I call this syndrome dys-stress, spelled with a y after the Greek dus, having a connotation of “badness,” as in dyspepsia (bad digestion). It may persist to a point where an animal cannot cope. In Europe, distress is interpreted more broadly than a physiological state of not coping and incorporates mental states rather than physiological states. That is when animals experience adverse feelings such as fear, anxiety, boredom, malaise, frustration, and the like.
There is a continuing debate about whether physiological levels (e.g., of hormones) are “harder” and more reliable scientific measures than measures of behavior. Some people think that signs are objective only if you can measure them and can assign a number on some sort of continuum. However, other signs (parametric) based on clinical signs or an animal’s behavior cannot easily be measured on a continuum (e.g., lameness, difficulty in breathing, stereotypic behavior) but are just as valid and just as objective, in the sense that we can observe them accurately and reproducibly. It is quite important that both sorts of signs be used depending on the circumstances and the adverse effects we are measuring.
Whether metric or parametric measures are used it is still necessary to interpret them in terms of understanding an animal’s mental state. It is this interpretation of an increased heart rate or increased blood pressure or a behavior that is the subjective step. The observation of the behavior and the measurement of a hormone level are both objective, but both have to be interpreted into [a gauge of the] intensity of mental distress.
In my opinion, in the measurement of animal well-being, behavior normally trumps physiology [in the] final integrated outcome of how an animal is feeling, it “votes with its feet.” We could invoke an analogy with people’s experience in hospitals today when they are in pain and do not get the treatment they feel they need. A scenario might occur where the nurse/doctor takes a blood sample and says, “No, you cannot be in pain, your blood hormones aren’t high enough.” What would you say? You know you are in pain and your behavior will most likely show that you are in pain (you may not want to move, feel nauseous, don’t feel like getting out of bed, look grey). All these physiological and behavioral signs are the outward integrated response but how you feel is mostly evidenced by your behavior and that is why I think behavior trumps physiological measurements for those that cannot speak and communicate.
In the ILAR working group on distress there were physiologists from the US who took the view that distress was the result of exposure to long-term stressors (I have referred to this as “dystress” above), and those from Europe who considered that (mental) distress could also result from a short-term exposure to stressors and cause mental states such as fear. Of course, it is very important from an evolutionary standpoint to be able to adapt to external stressors for
survival, sometimes referred to as “eu-stress” (Greek eu having a connotation of “good”). I recommend you read the ILAR report on distress; it is an extremely comprehensive document and it describes these tensions.1
I tried to find out for this conference something about the use of the word distress and what was happening in guidance and legislation in various countries. I emailed several colleagues in various countries with the following questions:
How does your country define distress and what emotional states would it cover? Would it for example cover the mental health of animals held for experiment as well as being in an experiment? (Animals are kept in their housing for possibly 100% of their time, but they are not on experiment for all that time.) Some countries provided a definition of distress whereas others preferred a descriptive approach to distress. That was very similar to what we decided in the ILAR group.
How does your country help users recognize distress? Some countries provided a list of signs and a guide to their assessment based on changes from normality—the more the observation deviated from normality, the greater the impact on the animal and the greater the distress.
How does your country help users treat distress? The emphasis here was on withdrawal—withdrawal of the animal from the stressful situation or avoiding it in the first place. Nobody really answered the question, although I was interested to see the Australian guidelines have started to follow the European Food Safety Authority (EFSA) model of welfare risk assessment. That is quite complicated, and I can give you some references to it. It is a rather tedious approach that looks at the intensity of an adverse state, its duration, the numbers of animals likely to be affected, and the likelihood that they will be affected if exposed to a stressor (or hazard in RA terms), but it does present some very interesting observations and challenging data sets to create. The [NRC report] had a section on treatment of distress, but I really don’t think it is going to be practical, because scientists are not going to want to give drugs that are neurologically active in their experiment.
Does your country have any formal guidelines for users? Canada and Australia had some formal guidelines, although I’m not quite sure how practically useful they are. When I looked through the [1996] US Guide for the Care and Use of Laboratory Animals, distress was mentioned only in conjunction with pain (i.e., “pain and distress”); there was no separate guidance on distress. But hopefully the ILAR report on distress will change that.
I received only three or four replies to my e-mail. There was resounding silence from the competent authorities in most countries. However, I received a good response from Australia and New Zealand with some really interesting observations. I would argue that is because they are the ones that have been at the forefront in developing broad-based local animal care and use ethics com-
_______________________
1Recognition and Alleviation of Distress in Laboratory Animals (2008). Washington: National Academies Press.
mittees and distress would have been an issue for many lay members. The US was very much ahead in setting up ethics committees in the first place, but the formal composition and skill base of these committees was very narrow and different from those in other countries; for example, they excluded animal protection members and did not mandate those with training in ethics.
I had a detailed response for farm animals from Italy, but unfortunately it was all in Italian. Many of the other countries either gave very general guidelines or simply did not address distress as a separate issue, although they often dealt with pain separately.
In the US, the major emphasis has been on pain but ignores its duration and intensity, and that is common to many other countries. However, that is historical, and maybe the revision of the Guide will include more information about intensity and duration of both pain and distress, in the same way that EFSA’s risk assessment does.
One of the major differences is that the US, in general, is far less willing to give animals the benefit of the doubt in the absence of scientific evidence. This raises interesting and productive tensions, with a more rigorous requirement for validation of welfare measures in the US than in the EU or elsewhere. Validation of welfare measures is becoming a key issue in other areas of animal use—for example, welfare assurance schemes for farmed animals such as the Welfare Quality project in the EU. This is a massive project—17 million euros have been invested in this activity, which includes 44 institutions and 13 member states, plus four in South America. They are trying to develop key welfare indicators that can reflect the quality of life of farmed animals before they are killed—did they have a good quality of life, did they have a life worth living, if you like? The Farm Animal Welfare Council in the UK is also looking into this.
The issues are the same for research animals. How do we assess their quality of life, which will include validation of the measures and how we determine whether a particular measure reflects pain or distress? We need more research on validation of the measures, their robustness, reliability, and how feasible they are to measure, and can they be scored with good observer reproducibility?
The advantage of measuring deviation from normality—measuring the impact of an experiment or system of husbandry on an animal—is that you don’t have to label it with a particular mental emotional state. The only reason one might want to label something as pain or distress is for implementing therapy: if an animal is in pain, it should receive an analgesic. However, distress is far more varied and complex and the cause is very important. Fear (e.g., of humans, rooms), anxiety (a raised awareness in general), frustration and boredom (e.g., because of housing and husbandry), malaise (e.g., because of infection) all have different causes and these have to be identified. Treatment will then be based more on causation as opposed to pain, which is generally easier to predict and diagnose and treat. It is also quite important not to label things too restrictively as various mental states often run together.
Most international guidelines emphasize that one should take steps to avoid any adverse effects for scientific reasons. This can be done through better
training of personnel, better techniques carried out competently, closer observations of animals, and early detection of adverse states and their causes.
In conclusion, mental ill health—i.e., distress—is the most common cause of suffering in laboratory animals. It is multifactorial and difficult to treat. There is little guidance in most countries on its recognition, assessment, avoidance, and alleviation. It can be recognized and assessed by measuring the impact of the procedures in animals, but research is needed to identify key validated and robust measures.
Pain: International Differences Across Guidelines and Approaches
Matt Leach
Introduction
Most of the work reported here is the work of the members of the pain systems group at Newcastle University, UK; in particular, the work of Claire Richardson, Claire Coulter, and Paul Flecknell will be referred to.
Before looking at guidelines and approaches a definition of animal pain is required. The most widely accepted definition of pain and the most appropriate in this case is that of the International Association for the Study of Pain (IASP 1994): “An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage.”
Guidelines and Codes of Practice
The vast majority of countries that carry out animal-based research have guidelines, almost all of which state that “Pain should be ‘minimized and/or alleviated…’” or have statements to a similar effect (e.g., ILAR, NIH, Australia’s National Health and Medical Research Council [NHMRC], the UK Home Office, the European Convention for the Protection of Vertebrate Animals Used for Experimental and Other Scientific Purposes [ETS 123], JCS, and CCAC). Pain can be minimized and/or alleviated using the principles of the 3Rs. The use of analgesia is critical. As a consequence of the guidelines that exist we should expect analgesia to be commonplace and extensive guidance on when and how to use analgesics to be in existence. So how widespread is analgesic use?
Analgesic Use in Rodents
A 2005 literature-based survey (Richardson and Flecknell 2005) looked at analgesic use in laboratory rodents undergoing painful procedures. It included papers published in bioscience journals in 1990-1992 (100 papers) and 2000-
2002 (100 papers). The proportion of papers reporting no analgesic use, analgesia via anesthesia, and analgesic use is shown in Figure 1.1
The high percentage of rodents that were reported not to receive analgesia is not surprising when we consider analgesic use in veterinary clinical practice in general. The work of Lascelles and colleagues (1999) in cats and Capner and colleagues (1999) in dogs demonstrates this (see Figure 2). The problem of low analgesic use is not a new problem as a similar situation was seen in human medical practice around 20 years ago. The lack of analgesic use in medical and veterinary clinical practice could be due to failure either to appreciate the significance of pain or to recognize signs of pain.
However, is this true for laboratory animals? The literature survey by Richardson and Flecknell (2005) carried a follow-up in which they emailed authors who reported no analgesic use in their papers (67% of papers) and asked whether they had simply not reported analgesia use (underreporting) or had not administered analgesics (underuse). The change in the proportions of papers reporting no analgesic use, analgesic use, and analgesia via anesthesia is shown in Figure 3.
Analgesic Use in Other Species and across Continents
Two literature surveys in 2007 looked at analgesic use after surgery in rodents (Stokes et al. 2009) and in larger species (rabbits, pigs, sheep, dogs, and primates; Coulter et al. 2009). The surveys covered studies that were carried out in a number of countries around the world and published between 2005 and 2006; for rodents these involved 86 papers in 10 journals and for larger species 75 papers in 61 journals. The results of these surveys are shown in Figure 4.
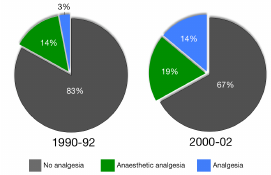
FIGURE 1 Reported analgesic use in rats and mice in bioscience journals in 1990-1992 (100 papers) and 2000-2002 (100 papers). Source: Richardson and Flecknell (2005).
_______________________
1The figures in this article appear in color in the online posting of this report at www.nap.edu.
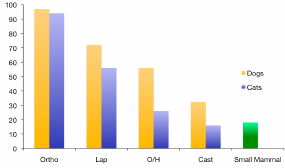
FIGURE 2 Percentage of dogs, cats, and small mammals receiving analgesia after different types of surgery in the United Kingdom. Source: Richardson and Flecknell (2005).
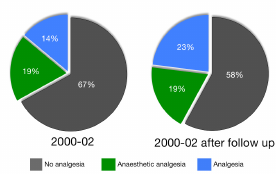
FIGURE 3 Changes in reported analgesic use in rats and mice in 2000-2002 after email follow-up of authors who reported no analgesic use. Source: Richardson and Flecknell (2005).
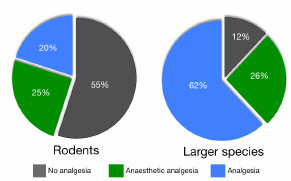
FIGURE 4 Reported analgesic use in 2005-2006 after surgery in rodents (Stokes et al. 2009) and larger species (rabbits, pigs, sheep, dogs, and primates) (Coulter et al. 2009).
These data can also be tentatively used to assess analgesic use by the continent on which the work was completed (see Figure 5). These are the only data of their kind as far as we know, and although they are indicative they should be interpreted with extreme care. The surveys were not designed to differentiate between countries, there was an unequal distribution of papers across countries, cultural differences were not taken into account, and the proportion of animal-based research carried out in each country was not taken into account, [any of which] could bias results.
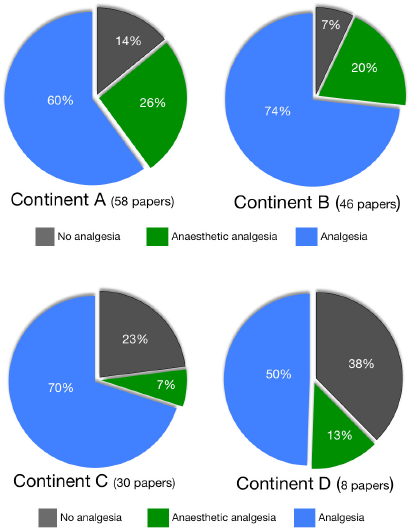
FIGURE 5 Reported analgesic use by continent in 2005-2006 after surgery in rodents and larger species. Sources: Coulter et al. (2009); Stokes et al. (2009).
Why Is There Such a Low and Varied Use of Analgesia in Animals?
There are a number of possible reasons for such low and varied use of analgesia in animals despite the prevalence of guidelines:
• Some consider that animals don’t feel pain and this is dependent on attitudes to pain in animals, which vary among countries and professions.
• There is no perceived need to give analgesics; however, this is often due to a failure to recognize indicators of pain in animals.
• Concern over interactions between the analgesics we can administer and the experimental protocol being carried out on animals.
• Concern over the extent of potential side effects associated with the analgesics we administer.
• Tradition or historical data showing that a potentially painful procedure has been carried out without analgesics before, used as evidence that it can be again.
In many cases unalleviated pain can cause as much if not more variation in the data as either interactions between the analgesics and experimental protocols or potential side effects associated with analgesics. If there is concern about the effect of analgesic administration on experimental validity then this can be considered with other sources of potential variation in a study (e.g., environmental, surgical) through well-designed and appropriate statistical analysis. In addition, the other effects of unalleviated pain on animal-based research should be appreciated, such as causing the death of animals, which can require the use of additional animals to maintain the study design. Increasing the number of animals used does not fulfill the spirit of the 3Rs.
In Summary
It seems that in many cases the apparent rationales for withholding analgesia do not withstand close scrutiny, which can easily be seen in the peer-reviewed literature, as for a given procedure analgesia will be administered in one case but withheld in another when carried out on different species, or even the same species, both between and within countries. Therefore, despite the prevalence of guidelines there remains considerable variation in the administration of analgesia in animal-based studies.
The final point of this presentation was to ask those who attended this meeting why they think there is such considerable variation in the administration of analgesia in animal-based studies.
References
Capner CA, Lascelles BDX, Waterman-Pearson AE. 1999. Current British veterinary attitudes to perioperative analgesia for dogs. Vet Rec 145:95-99.
Coulter CA, Flecknell PA, Richardson CA. 2009. Reported analgesic administration to rabbits, pigs, sheep, dogs and non-human primates undergoing experimental surgical procedures. Lab Anim 43:232-238.
IASP [International Association for the Study of Pain]. 1994. Classification of Chronic Pain: Descriptions of Chronic Pain Syndromes and Definitions of Pain Terms, 2nd ed. Available online (www.iasp-pain.org/AM/Template.cfm?Section=Pain_Definitions&Template=/CM/HTMLDisplay.cfm&ContentID=1728#Pain).
Lascelles BDX, Capner CA, Waterman-Pearson AE. 1999. Current British veterinary attitudes to perioperative analgesia for cats and small mammals. Vet Rec 145:601-604.
Richardson CA, Flecknell PA. 2005. Anaesthesia and post-operative analgesia following experimental surgery in laboratory rodents: Are we making progress? ATLA 33:119-127.
Stokes EL, Flecknell PA, Richardson CA. 2009. Reported analgesic and anaesthetic administration to rodents undergoing experimental surgical procedures. Lab Anim 43:149-154.
Gilly Griffin
Introduction
Various organizations around the world have developed guidance on euthanasia. Some have developed guidelines that are specific for animals used for scientific purposes, others have a broader mandate. Some of the organizations are also involved in overseeing animal use in science and therefore have tailored their documents to fit their particular national systems. A comparison of recommendations made in recent guidelines drawn from a variety of jurisdictions is provided. Differences in recommendations can be the result of difference in interpretation of scientific evidence, but may also reflect difference in expert opinion, national systems, and societal values.
Guideline Documents
As national authorities overseeing animals used for scientific purposes have evolved, they have either developed or adopted guidelines as a means of holding animal users accountable to prevailing societal values. Guidelines for the ethical use and care of experimental animals provide the basis for acceptable practices relating to animal-based research, testing, and teaching. Guidelines may address particular procedures, conditions of housing and care, and the behavior of individuals carrying out procedures or caring for animals.
The guidelines themselves are usually implemented at the local institutional level, with local and/or national assurance, depending on the country. In some places, the national authority may be the organization that both develops the guidelines and provides assurance that they are implemented at the institutional level (for example, the Canadian Council on Animal Care, CCAC). In other places, guidelines may be developed by one organization (for example, the American Veterinary Medical Association, AVMA) and implemented by another (for example, the Office for Laboratory Animal Welfare, OLAW). To illustrate this point, OLAW interprets and oversees compliance with the US Pub-
lic Health Service (PHS) Policy on Humane Care and Treatment of Animals, which states that a method of euthanasia used in the United States must be endorsed by the AVMA (OLAW 2002). The organization or authority responsible for overseeing the implementation of the guidelines may itself be operating according to particular legislation or a policy framework that has an impact on the manner in which the guidelines are viewed and implemented as well as on the manner in which they were drafted in the first place.
Development of Guidelines
The development of guidelines involves the translation of scientific evidence into recommendations that can be implemented in practice. Although best attempts are made to ground guidelines in current scientific evidence, there are at least two factors that make straight translation of science into guidelines or policy almost impossible to achieve. First, guideline development happens at a discrete point in time, whereas science is continually evolving. Guidelines therefore need to be sufficiently flexible to accommodate shifts in thinking that may improve the welfare of animals, particularly as guideline documents take a considerable amount of time to produce.
Second, however much one might strive to base guidelines on hard science, in reality that science is subject to expert opinion, the regulatory framework within which the animal-based research is carried out, and current societal values, as most oversight systems are either an arm of government or established to act on behalf of the broader public. These additional factors do not dilute the scientific basis for guidelines; rather, they translate hard science into guidance, and in doing so add value to the guidelines. This ensures that the guidelines can be readily implemented and can be defended both to the scientific community and the public at large.
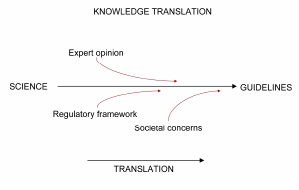
FIGURE 1 International harmonization.
International harmonization of guidelines is becoming increasingly important due to the evolving globalization of science. For this reason, the International Council for Laboratory Animal Science (ICLAS), an international scientific organization dedicated to advancing human and animal health by promoting the ethical care and use of laboratory animals in research worldwide, has been working on harmonization of guideline documents. At the ILAR symposium on science-based guidelines held in 2003, it was recognized that, due to differences in national systems of oversight, guidelines can only ever be harmonized and that standardization of guidelines is neither possible nor desirable (Demers 2004a).
Harmonization exercises conducted by ICLAS involve setting up international working groups in various subject areas to establish relevant guiding principles and to formally recognize guidelines that are suitable as international references. This has been achieved for exercises in each of the following areas: euthanasia, humane endpoints, ethical review, and animal user training programs (Demers 2004b; Demers et al. 2006; www.iclas.org/harmonization.htm). The principles are extremely useful as they do not impede a nation’s ability to formulate its own guidance appropriate to the oversight system in place. Rather, they provide keystones upon which guidelines can be built. For example, the 10 principles generated by the ICLAS working group on harmonization of euthanasia guidelines (listed below) formed the starting point for the development of the CCAC guidelines on euthanasia of animals used in science (in preparation; since published, 2010). The principles were interpreted to address the particular Canadian situation and formed the basis for guidelines that adopt guidance that is already well established as well as providing additional information and details where new scientific evidence has become available. This approach would be useful for any guideline development exercise.
ICLAS Principles on Euthanasia
The following ten principles on euthanasia prepared by ICLAS provide a means of evaluating euthanasia techniques (Demers et al. 2006):
1. Whenever an animal’s life is to be taken, it should be treated with the highest respect.
2. Euthanasia should place emphasis on making the animal’s death painless and distress-free. The method likely to cause the least pain and distress to the animals should be used whenever possible.
3. Euthanasia techniques should result in rapid loss of consciousness, followed by cardiac or respiratory arrest and ultimate loss of brain function.
4. Techniques should require minimum restraint of the animal and minimize distress and anxiety experienced by the animal before loss of consciousness.
5. Techniques should be appropriate for the species, age, and health of the animal.
to be used with Directive 86/609/EEC of 24 November 1986, on the approximation of laws, regulations, and administrative provisions of the member states regarding the protection of animals used for experimental and other scientific purposes (No L 358, ISSN 0378-6978). They refer especially to Article 2(1), published by the European Commission in October 1995, which defines “humane method of killing” as “the killing of an animal with a minimum of physical and mental suffering, depending on the species.” These documents are intended to be used in conjunction with the opinion of the Scientific Panel on Animal Health and Welfare (AHAW) of the European Food Safety Authority (EFSA 2005a).
• Aspects of the Biology and Welfare of Animals Used for Experimental and Other Scientific Purposes (EFSA 2005b). This report summarizes the position of the animal welfare panel of the European Food Safety Authority (EFSA), which was asked to consider the scientific evidence for the sentience and capacity of all invertebrate species used for experimental purposes and of fetal and embryonic forms to “experience pain, suffering, distress, or lasting harm.” The panel also considered and made recommendations concerning humane methods of killing animals. This report updates recommendations made by Close and colleagues (1996, 1997).
• Review of Schedule 1 of the Animals (Scientific Procedures) Act 1986: Appropriate Methods of Humane Killing (APC 2006). The UK Animal Procedures Committee (APC) was asked in June 2001 to review Schedule 1. Recommendations in the report include advice on humane killing of neonatal rodents; use of argon, nitrogen, or other inert gases; use of CO2; and weight thresholds for cervical dislocation of rodents. The Parliamentary Under Secretary of State for the Home Office responded to the APC’s review in August 2007 (Hillier 2007), requesting further consultation on several of the committee’s recommendations, while accepting the recommendation to provide advice on humane killing of neonatal rodents. These recommendations have not been implemented to date.
• Public Statement: Report of the ACLAM Task Force on Rodent Euthanasia (Artwohl et al. 2006). This report of the American College of Laboratory Animal Medicine is a response to growing concerns and controversy regarding techniques that were commonly used for rodent euthanasia. Three issues were targeted in the report: euthanasia of fetal and neonatal rodents, the use of CO2 for rodent euthanasia, and the impact of euthanasia techniques on data.
• Euthanasia of Animals Used for Scientific Purposes (ANZCCART 2001; under revision). The aim of the publication is to provide investigators and members of Australian and New Zealand animal ethics committees with detailed information on methods of euthanasia relevant for animals used for scientific purposes, including species not generally used elsewhere (e.g., dingos and marsupials).
• Canadian Council on Animal Care Guidelines on Euthanasia of Animals Used in Science (CCAC 2010, updating Chapter XII on euthanasia in
6. Death must be verified before disposal of the animal.
7. Personnel responsible for carrying out the euthanasia techniques should be trained: (i) to carry out euthanasia in the most effective and humane manner; (ii) to recognize signs of pain, fear, and distress in relevant species; and (iii) to recognize and confirm death in the species.
8. Human psychological responses to euthanasia should be taken into account when selecting the method of euthanasia, but should not take precedence over animal welfare considerations.
9. Ethics committees should be responsible for approval of the method of euthanasia (in line with any relevant legislation). This should include euthanasia as part of the experimental protocol as well as euthanasia for animals experiencing unanticipated pain and distress.
10. A veterinarian experienced with the species in question should be consulted when selecting the method of euthanasia, particularly when little species-specific euthanasia research has been done.
Euthanasia Guidelines
The guideline documents analyzed for this paper (listed below) have been developed by nationally recognized organizations. They were determined to be the most frequently used guidelines in this area, although other guidelines on euthanasia are also available.
• AVMA Guidelines on Euthanasia (2007, updating the 2000 Report of the AVMA Panel on Euthanasia). This document was prepared at the request of the AVMA Council on Research by the Panel on Euthanasia that convened in 1999 to review and make necessary revisions to the fifth Panel Report, published in 1993. In the 2000 Report, the panel updated information on euthanasia of animals in research and animal care and control facilities; expanded information on ectothermic, aquatic, and fur-bearing animals; added information on horses and wildlife; and deleted methods or agents considered unacceptable. In 2006, the AVMA Executive Board approved a recommendation that AVMA convene a panel of scientists at least once every 10 years to review all the literature that scientifically evaluates methods and potential methods of euthanasia for the purpose of producing AVMA guidelines on euthanasia. During the interim years, requests for inclusion of new or altered euthanasia procedures or agents in the AVMA Guidelines on Euthanasia will be directed to the AVMA Animal Welfare Committee. Revisions are based on a thorough evaluation of the available science and require Executive Board approval. The first interim revision, approved in 2006, added guidance on the use of maceration for chicks, poults, and pipped eggs (AVMA 2007).
• Recommendations for Euthanasia of Experimental Animals (Close et al. 1996, 1997). These two documents (Parts 1 and 2) were prepared for the EU Directorate-General of the Environment, Nuclear Safety, and Protection (DGXI)
CCAC 1993) is based on recommendations made by the International Council for Laboratory Animal Science (ICLAS) Working Group on Harmonization and the two international reference documents on euthanasia recommended by ICLAS: the AVMA Guidelines on Euthanasia (AVMA 2007) and the Recommendations for Euthanasia of Experimental Animals, Parts 1 and 2 (Close et al. 1996, 1997). This information has been adapted to suit the Canadian research environment.
Differences in Approach
The foregoing descriptions of each guideline document underline the fact that there are differences in the intent for each. The AVMA (2007) Guidelines on Euthanasia are primarily to assist veterinarians in exercising professional judgment in the application of euthanasia. The document covers not only animals used for scientific purposes but also those used as companions and for food, animals in the wild, and exotic species. Close and colleagues (1996, 1997) provide guidelines that are specific to animals used for experimental purposes. Euthanasia of these animals would not necessarily be carried out by a veterinarian. The EFSA recommendations are to be used in conjunction with those of Close and colleagues (1996, 1997) and will be legally binding once the new European Directive comes into force. Schedule 1 to the UK Animals (Scientific Procedures) Act 1986 provides a list of methods considered exempt from the requirement for a UK Home Office personal or project license. The CCAC guidelines and the ANZCCART guidelines are specific for animals used for scientific purposes and are targeted to investigators and animal care committees to provide them with the relevant information on which to base their decisions regarding methods of euthanasia.
Irrespective of the framework within which these guideline documents are implemented, there is considerable similarity of intent. In the United States, animals used for scientific purposes essentially fall under the PHS Policy, which requires “avoidance or minimization of discomfort, distress, and pain when consistent with sound scientific practices” and requires investigators to “consider that procedures that cause pain or distress in human beings may cause pain or distress in other animals” (OLAW 2002b). The Australian Code of Practice for the Care and Use of Animals for Scientific Purposes “assume(s) animals experience pain in a similar manner to humans” (NHMRC 2004). The CCAC policy states that animals must not be subjected to unnecessary pain or distress, and that cost and convenience must not take precedence when deciding on procedures and matters relating to the care of the animals (CCAC 1989). Similarly, European Directive 86/609/EEC requires that “all experiments shall be designed to avoid distress and unnecessary pain and suffering to the experimental animal” (EEC 1986). Last, the UK Animals (Scientific Procedures) Act 1986 regulates
procedures that may have the effect of causing the animal pain, suffering, distress, or lasting harm (the inference being that procedures not covered under the Act [methods of euthanasia listed in Schedule1] should not cause more than momentary pain or distress to the animal) (Home Office 1986).
Comparison of Provisions in the Guidelines
A comparison of euthanasia methods across documents is challenging because of the different approaches in the documents. The AVMA Guidelines on Euthanasia (2007) provide a table of methods considered by the panel of veterinarians responsible for drafting the guidelines to be acceptable, as well as tables of methods that they considered conditionally acceptable or unacceptable. Close and colleagues (1996, 1997) and the revised table developed by EFSA provide information based on species groups using a 1-5 rating system. The criteria used to assess the acceptability of euthanasia methods are similar between the AVMA and the EFSA documents, as illustrated in Table 1 below.
TABLE 1 Criteria Used to Evaluate Level of Acceptability of Euthanasia Methods
| Criteria used by EFSA | Criteria used by AVMA | |
| Rapidity | ||
| Efficacy | ||
| Ease of use | ||
| Operator safety | ||
| Species suitability | ||
| Aesthetic value (acceptability of method by operator) | ||
Table 2 shows a comparison of methods of euthanasia for rodent species, which are of particular interest because of the large numbers of mice and rats used for research and testing. This table has been prepared using a 5-star ranking, where 1 star indicates that the method is unacceptable under most circumstances; 3 stars indicate that the method is acceptable under some conditions; and 5 stars indicate that the method is acceptable. As the Australian and Canadian guidelines are currently both under revision, they have not been included.
TABLE 2 Comparison of Rodent Euthanasia Methods
| Method of euthanasia | European guidelines (Close et al. 1996, 1997) as amended by EFSA (2005b) | AVMA Guidelines (2007, amending the 2000 Report of the AVMA Panel on Euthanasia) |
| Inhalation anesthetics | ***** | ***** |
| Pentobarbitol | ***** | ***** |
| T-61 | *** | *** |
| (i.v. only) | (not available in the US) | |
| Inert as | *** | *** |
| Conc ssion | *** | * |
| (rodents under 1 kg) | ||
| Microwave irradiation | *** | ***** |
| (experienced personnel only) | ||
| Cervical dislocation | *** | *** |
| (rodents <150 g) | (rodents <200 g) | |
| Decapitation | ** | *** |
| CO2 | ***** | ***** |
| (unconscious) | ||
| * | ||
| (conscious) | ||
| CO | * | ***** |
| (danger to operator) | ||
| Ether | * | *** |
| Rapid freezing | * | *** |
| (only if anesthetized) | ||
| Potassium chloride | *** | ***** |
| (only on unconscious rodents) | (acceptable if anesthetized) | |
Carbon Dioxide
The use of carbon dioxide as a euthanizing agent has been increasingly challenged since the AVMA 2000 Panel Report. The principles espoused by all of the various international systems overseeing animal use in science are based on the premise that pain and distress must be minimized. In addition, the ICLAS principles of euthanasia point not only to minimization of pain and distress but also to immediate loss of consciousness as important in euthanasia. A review of the scientific literature provides substantial evidence that animals euthanized with carbon dioxide experience considerable pain and/or distress (depending on the manner in which CO2 is administered) (Conlee et al. 2005; Leach et al. 2002; Liotti et al. 2001; Niel and Weary 2007; Raj et al. 2004). To try to address these concerns, the following recent publications have made recommendations concerning the euthanasia of rodents by carbon dioxide:
• Report of the ACLAM Task Force on Rodent Euthanasia (Artwohl et al. 2006)
• CCAC Guidelines on Euthanasia of Animals Used in Science (CCAC 2010)
• Guidelines to Promote the Well-being of Animals Used for Scientific Purposes: The Assessment and Alleviation of Pain and Distress in Research Animals (NHMRC 2008)
• Opinion of the Scientific Panel on Animal Health and Welfare (AHAW) on a request from the Commission related to the aspects of the biology and welfare of animals used for experimental and other scientific purposes (EFSA 2005a)
• Review of Schedule 1 of the Animals (Scientific Procedures) Act 1986 (APC 2006).
In light of this concern, an international consensus meeting was held at the University of Newcastle upon Tyne in February 2006. The organizers recognized that there was no definitive guidance on whether and how CO2 can be administered humanely, and therefore brought together scientists with research experience in CO2 euthanasia, regulators, and members of the animal care community. The goals of the meeting were to try to reach consensus on the use of CO2, identify further research needed, meet the immediate need for practical guidance, and consider whether any preferable alternatives were currently available. The meeting concluded that there was no “ideal” way of killing rodents with CO2. Both methods currently used—prefill (placing the animals in a chamber already charged with carbon dioxide) or gradual fill (placing the animals in a chamber and then gradually filling it with carbon dioxide)—can cause welfare problems. It was decided that it is not yet possible to recommend the use of other gases (such as argon or nitrogen) that cause death by hypoxia, and that more research is needed into the physiological and affective responses to a range of gaseous agents in order to identify good practice and potential alternatives to CO2 (Hawkins et al. 2006).
In the interim, there are recommendations in guidelines that seek to establish good practice, in line with authors’ interpretation of the current scientific evidence. According to AVMA (2007), CO2 is acceptable for euthanasia in appropriate species; ACLAM (2006) states that the current peer-reviewed literature does not establish consistent requirements for CO2 euthanasia and/or even provide a clear definition of what constitutes a humane death; and EFSA (2005a) recommends that CO2 not be used as a sole agent in any euthanasia procedure unless the animal has first been rendered unconscious, and that its use be phased out as soon as possible. Table 3 provides a comparison of recommendations on the use of CO2 as a method of euthanasia in the guidelines studied.
TABLE 3 Comparison of Recommendations Concerning the Use of Carbon Dioxide as a Euthanasia Agent for Rodents
| AVMA (2007, amending the 2000 Report of the AVMA Panel on Euthanasia) | Acceptable method – gradual fill 33% of cage volume per minute | |
| ACLAM (2006) | Acceptable method – gradual fill 20% of chamber volume per minute | |
| CCAC (2010) | Conditionally acceptable – use 2-step method where possible (i.e., inhalant anesthetic followed by CO2); otherwise use gradual fill >15% and <30% of the chamber volume per minute | |
| Australia | Acceptable method – gradual fill 20% of chamber volume per minute | |
| EFSA (2005a) | Conditionally acceptable – only on unconscious animal | |
| APC (2006) – Schedule 1 Review | Conditionally acceptable – rising concentration (gradual fill) | |
Conclusion
Organizations responsible for the development of guidelines all work to ground their recommendations in sound scientific evidence. Nonetheless, translation of science into policy necessarily includes a variety of factors, such as the particular regulatory framework in which the guidelines will be implemented and the current opinion of experts in the area, as well as current societal values. It has been stated that there is insufficient scientific evidence to be able to harmonize guidelines worldwide (Kastello 2004, 201), and even if this were overcome, these other factors would present obstacles. However, the harmonization exercises organized by ICLAS, which have resulted in sets of internationally agreed principles, can form the basis for the preparation of guidelines tailored to fit particular national systems for overseeing animal use.
References
APC [Animal Procedures Committee]. 2006. Review of Schedule 1 of the Animals (Scientific Procedures) Act 1986 - appropriate methods of humane killing. London.
AVMA [American Veterinary Medical Association]. 2007. AVMA Guidelines on Euthanasia. Available at www.avma.org/issues/animal_welfare/euthanasia.pdf.
Artwohl J, Brown P, Corning B, Stein S, ACLAM Task Force. 2006. Report of the ACLAM Task Force on rodent euthanasia. JAALAS 45:98-105.
ANZCCART [Australian and New Zealand Council for the Care of Animals in Research and Teaching]. 2001. Euthanasia of Animals Used for Scientific Purposes, 2nd ed. J Reilly, ed. Adelaide, Australia.
CCAC [Canadian Council on Animal Care]. 1989. CCAC policy statement on ethics of animal experimentation. Ottawa.
CCAC. 1993. Euthanasia. In: Guide to the Care and Use of Experimental Animals, vol 1, 2nd ed. Ottawa.
CCAC. 2010. CCAC Guidelines on Euthanasia of Animals Used in Science. Ottawa.
Close B, Banister K, Baumans V, Bernoth EM, Bromage N, Bunyan J, Erhardt W, Flecknell P, Gregory N, Hackbarth H, Morton D, Warwick C. 1996. Re-commendations for euthanasia of experimental animals: Part 1. Lab Anim 30:293-316.
Close B, Banister K, Baumans V, Bernoth EM, Bromage N, Bunyan J, Erhardt W, Flecknell P, Gregory N, Hackbarth H, Morton D, Warwick C. 1997. Recommendations for euthanasia of experimental animals: Part 2. Lab Anim 31:1-31.
Conlee KM, Stephens ML, Rowan AN, King LA. 2005. Carbon dioxide for euthanasia: Concerns regarding pain and distress, with special reference to mice and rats. Lab Anim 39:137-161.
Demers G. 2004a. Current status: Identifying the issues. In: The Development of Science-Based Guidelines for Laboratory Animal Care: Proceedings of the November 2003 International Workshop. Washington: National Academies Press. p 30-35.
Demers G. 2004b. First ICLAS meeting for the harmonization of guidelines on the use of animals in science. In: Proceedings of the Ninth FELASA Symposium (Nantes, France, June), section 2. Federation of European Laboratory Animal Science Associations (FELASA). Available at www.lal.org.uk/pdffiles/FELASA/Section2.pdf.
Demers G, Griffin G, De Vroey G, Haywood JR, Zurlo J, Bédard M. 2006. Harmonization of animal care and use guidance. Science 312:700-701. Available at www.iclas.org/harmonization.htm.
EEC [European Economic Community]. 1986. Council Directive 86/609/EEC of 24 November 1986 on the approximation of laws, regulations and administrative provisions of the Member States regarding the protection of animals used for experimental and other scientific purposes. Official Journal L 358: 1-28. Available at http://ec.europa.eu/food/animal/welfare/references_en.htm.
EFSA [European Food Safety Authority]. 2005a. Opinion of the Scientific Panel on Animal Health and Welfare (AHAW) on a request from the Commission related to the aspects of the biology and welfare of animals used for experimental and other scientific purposes (EFSA-Q-2004-105). EFSA J 292:1-46. Available at www.efsa.europa.eu/en/science/ahaw/ahaw_opinions/1286.html (accessed October 23, 2008).
EFSA. 2005b. Aspects of the biology and welfare of animals used for experimental and other scientific purposes (EFSA-Q-2004-105). Annex to EFSA J 292:1-136. Available at www.efsa.europa.eu/en/science/ahaw/ahaw_opinions/1286.html.
Hawkins P, Playle L, Golledge H, Leach M, Banzett R, Coenen A, Cooper J, Danneman P, Flecknell P, Kirkden R, Niel L, Raj M. 2006. Newcastle consensus meeting on carbon dioxide euthanasia of laboratory animals. February 27-28, University of Newcastle upon Tyne, UK. Laboratory Animals (www.lal.org.uk/pdffiles/CO2%20Final%20Report.pdf).
Hillier M. 2007. Government response by Meg Hillier, MP, Parliamentary Under Secretary of State for the Home Department. Available at www.apc.gov.uk/reference/2007%2010%2010%20Schedule%201%20Report.pdf.
Home Office. 1986. Animals (Scientific Procedures) Act 1986. London: HMSO. Available at www.archive.official-documents.co.uk/document/hoc/321/321-xa.htm.
Kastello MD. 2004. Point/counterpoint: The cases for and against harmonization. In: The Development of Science-Based Guidelines for Laboratory Animal Care: Proceedings of the November 2003 International Workshop. Washington: National Academies Press.
Leach MC, Bowell VA, Allan TF, Morton DB. 2002. Aversion to gaseous euthanasia agents in rats and mice. Comp Med 52:249-257.
Liotti M, Brannan S, Egan G, Shade R, Madden L, Abplanalp B, Robillard R, Lancaster J, Zamarripa FE, Fox PT, Denton D. 2001. Brain responses associated with consciousness of breathlessness (air hunger). PNAS 98:2035-2040.
NHMRC [National Health and Medical Research Council], Australian Government. 2004. Australian Code of Practice for the Care and Use of Animals for Scientific Purposes, 7th ed. Canberra. Available at www.nhmrc.gov.au/publications/synopses/ea16syn.htm.
NHMRC. 2008. Guidelines to Promote the Wellbeing of Animals Used for Scientific Purposes: The Assessment and Alleviation of Pain and Distress in Research Animals. Canberra.
Niel L, Weary DM. 2007. Rats avoid exposure to carbon dioxide and argon. Appl Anim Behav Sci 107:100-109.
OLAW [Office of Laboratory Animal Welfare]. 2002a. ARENA/OLAW Institutional Animal Care and Use Committee Guidebook, 2nd ed. Section C.2.b. Bethesda, MD: NIH. Available at ftp://ftp.grants.nih.gov/IACUC/GuideBook.pdf.
OLAW. 2002b. Public Health Service Policy on Humane Care and Use of Laboratory Animals. Bethesda, MD: NIH. Available at http://grants1.nih.gov/grants/olaw/.
Raj ABM, Leach MC, Morton DB. 2004. Carbon dioxide for euthanasia of laboratory animals. Comp Med 54:470-471.

























