Assessing Affordability and the Potential for Underinsurance
Not only uninsured but also underinsured families have high out-of-pocket health care costs and often forego needed care. Jessica Banthin, an economist with the Agency for Healthcare Research and Quality’s (AHRQ’s) Center for Financing, Access and Cost Trends, and Cathy Schoen, Senior Vice President for Policy, Research, and Evaluation at The Commonwealth Fund, discussed consideration of affordability and underinsurance when designing benefits.
PRESENTATION BY DR. JESSICA BANTHIN, AGENCY FOR HEALTHCARE RESEARCH AND QUALITY (AHRQ)
Dr. Banthin outlined how AHRQ defines high financial burden and used data from the Medical Expenditure Panel Survey (MEPS) to provide information about the population characterized as uninsured. Total out-of-pocket (OOP) financial burden is the sum of a family’s OOP expenditures for health care services (e.g., OOP premiums, deductibles, co-pays, and payments for uncovered services) divided by the family’s income. Health care service burden is similar except that that the numerator excludes OOP premiums. For privately insured individuals, this latter measure is used to determine underinsurance or “lack of generosity of coverage.” In her analysis, Dr. Banthin defines the family as the health insurance eligibility unit (i.e., members of the family who are eligible for family coverage) (Banthin and Bernard, 2006).
Committee member Dr. Chernew asked for further details about how, or if, these measures account for uncovered expenses incurred by individuals. Dr. Banthin clarified that the measures incorporate what “the household chooses to report” and most often capture uncovered expenses. If an individual gets acupuncture that is not covered by his insurance, for instance, he would likely report the expenses he incurred. Similarly, individuals report out-of-pocket expenses for prescription drugs not included in their plan’s formulary.
MEPS
MEPS, which is conducted by AHRQ, surveyed a nationally representative sample of approximately 12,000 households and 31,000 people in 2008. The Household Component, in particular, collected detailed information on family income, demographics, health status, chronic conditions, use of and expenditures for health care services,
insurance and employment status, and OOP premiums, among other topics. A separate employer survey collected information on employer premium contributions.
To analyze these data, AHRQ groups services into broad categories: hospital inpatient stays, emergency room visits, outpatient services (i.e., physician and non-physician office-based provider visits), prescribed medicine fills and refills, dental visits, home health care, and supplies and equipment. Dr. Banthin recognized these categories as less detailed than the categories used to analyze claims data, but said the level of detail is a function of the information collected. For instance, MEPS collects information on the reason for a visit, but it does not collect data on the type of provider.
Relevant Findings from MEPS
Next, Dr. Banthin described relevant trends in the 2001 through 2005 MEPS data. For these analyses, she considered individuals who live in families with high total OOP financial burden (i.e., spending 10 percent or more of their income on health care):
- From 2001 through 2005, the percent of individuals in the U. S. nonelderly population who live in families with high financial burden rose from 15.9 percent to 19.1 percent.
- While poor families (under 100 percent of the FPL) are the most likely to have high financial burdens (29 percent of poor families have a high financial burden), one in five low-income (families between 100 and 200 percent of the FPL) and low-middle-income families (families between 200 and 300 percent of the FPL) also reach this level of spending.
- A greater proportion of women ages 50-64 (30 percent) live in a family with a high financial burden than females 18-50 years or males 18-64 years (Banthin, 2011).
In addition to these findings, Dr. Banthin described the financial burden of individuals both with and without employer-sponsored insurance (ESI). Compared with the uninsured and individuals with ESI or public insurance, individuals with private non-group coverage spend significantly more of their income on total OOP expenses (see Figure 14-1). This result, Dr. Banthin said, is because the total OOP spending includes premiums. Comparatively, she said, the uninsured have a lower financial burden because they do not pay premiums and because “they may restrict their health care services in order to avoid having to pay out-of-pocket.” However, when Dr. Banthin separated the uninsured into those with a chronic condition and the uninsured without a chronic condition, the uninsured with a chronic condition had a much higher level of burden (27 percent vs. 9 percent, respectively).
Committee member Mr. Michael Abroe noted that Figure 14-1 provides an apt opportunity to compare the private non-group insurance group with the uninsured group; both groups, he pointed out, are likely comprised of families without access to the ESI market. In 2005, 53 percent of families with private non-group insurance had a high financial burden, whereas in this same year, only 15 percent of uninsured families had a high financial burden. Mr. Abroe asked whether this 38 percent difference results from income differences between these two groups, because the uninsured individuals forego care, or because having insurance “induces” increased use of medical care. Dr. Banthin said all of his hypotheses likely factor into the 38 percent difference and cited research that explored the incomes and assets of people who did not have access to the ESI market (Bernard et al., 2009). People who purchased private non-group insurance “tend to have considerably higher wealth, even holding income constant,” she said. “But ignoring wealth for a minute, the uninsured definitely have lower incomes on average than the private non-group [individual],” and they use much less care (Bernard et al., 2009).
Committee member Mr. Schaeffer noted that the graph depicted in Figure 14-1 shows a distinct trend: the percent of families with a high financial burden increased from 2001 through 2003 and then decreased or remained steady from 2003 to 2005 (Banthin, 2011). Dr. Banthin commented that these trends are likely the result of trends in the MEPS data, which reflects activity in the economy.
Next, Dr. Banthin explored the distribution of OOP expenses for individuals with a “very high financial burden,” which she defined as spending more than 20 percent of family income on OOP health care expenses. In 2003, these individuals spent, on average, $1,528 in OOP expenses; approximately 50 percent was spent on
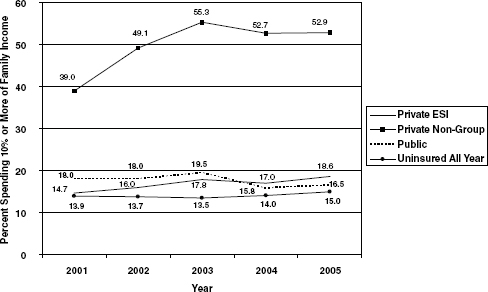
FIGURE 14-1 Percent of families spending 10 percent or more of family income by insurance status.
NOTE: Families with non-group insurance spend more of their family income on health care than uninsured families or families with employer-sponsored insurance (ESI).
SOURCE: Banthin, 2011.
prescription drugs, with the remainder spent on hospital care (8 percent), ambulatory care (23 percent), and all other expenses (18 percent). For families without a very high financial burden (i.e., spending less than 20 percent of family income on OOP health care spending), a smaller percentage of OOP expenses went toward prescription drugs (37 percent). These families spent, on average, $394 OOP—3 percent of which was spent on hospital care, 29 percent on ambulatory care, and 31 percent on other expenditures (Banthin and Bernard, 2006).
PRESENTATION BY MS. CATHY SCHOEN, THE COMMONWEALTH FUND
Ms. Schoen built on Dr. Banthin’s comments, describing how The Commonwealth Fund defines underinsurance and suggesting ways the U.S. Department of Health and Human Services (HHS) could design the essential health benefits (EHB) package to protect individuals and families against financial risk. Reiterating a point made by Mr. Wright in a previous panel (see Chapter 12), she described the goal of the Patient Protection and Affordable Care Act (ACA) as being to ensure access to care “with financial protections so that you do not go broke if you are sick.” To achieve this goal, one of the challenges that policy makers will face when “moving the uninsured into an insurance category,” she said, “is avoiding turning the uninsured into the underinsured.”
Defining the Underinsured
The Commonwealth Fund defines the underinsured as families who spend 10 percent or more of their income on medical expenses (very-low-income families are considered underinsured if they spend 5 percent or more of their income on medical expenses). This definition of underinsured is similar to AHRQ’s measure of health care service
burden in that it considers OOP medical expenses; however, it does not include premiums. These OOP expenses, Ms. Schoen said, are principally from deductibles, cost sharing for medications, and benefit gaps or limits.
High OOP Costs Affect the Underinsured
An analysis published by Ms. Schoen draws on responses to national surveys sponsored by The Commonwealth Fund. These surveys have tracked the experiences of those identified as “underinsured” since 2003. To accurately reflect OOP expenses that individuals incur while insured, Ms. Schoen and coauthors restricted the analysis to people who have had insurance all year. Consequently, her findings related to the underinsured do not “pick up the millions of people that churn in and out of coverage. Their out-of-pocket expenses might well have come during the three months they were uninsured rather than reflect something about their insurance policy.” All of these are classified as uninsured during the year. The analysis reveals that the underinsured are similar to the uninsured in that they often go without care because of costs and have problems paying medical bills.
After publishing an article about the underinsured in Health Affairs (Schoen et al., 2008), Ms. Schoen received numerous emails from people describing themselves as underinsured and sharing their stories. Many of these people, she said, told her that they had foregone care because they already had debt from medical expenses. In other work supported by the Fund, patients said, they could not afford additional care and they knew they would be “less than warmly received when they showed up at a physician’s office or hospital with unpaid bills.” In the analysis, a high proportion of the underinsured and uninsured said they had medical debt and that they used savings and took out loans against their homes to pay medical bills. A high proportion of those reporting medical debt (i.e., they had to pay off medical bills over time) said the expenses occurred while they were insured. These survey findings are supported by other studies on medical debt and bankruptcy, as well as by frequent media accounts (Himmelstein et al., 2005; O’Toole et al., 2004).
As shown in Figure 14-2, both uninsured and underinsured individuals are at high risk of foregoing needed care and of having financial stress related to outstanding medical bills or medical debt (Schoen et al., 2008). These results, she said, have been adjusted for health status and income and show that the “underinsured are much more
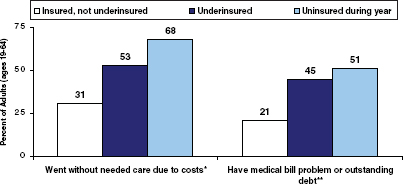
FIGURE 14-2 Underinsured and uninsured adults are at high risk of going without needed care and having financial stress due to medical debt.
*Did not fill prescription; skipped recommended medical test, treatment, or follow-up; had a medical problem but did not visit the doctor or did not get needed specialist care because of cost.
**Had problems paying medical bill; changed way of life to pay medical bills; or contacted by a collection agency for inability to pay medical bills.
SOURCE: Schoen, 2011. Based on analysis published in Schoen et al., 2010.
____________________
1 For related studies see Beeuwkes Buntin et al., 2011.
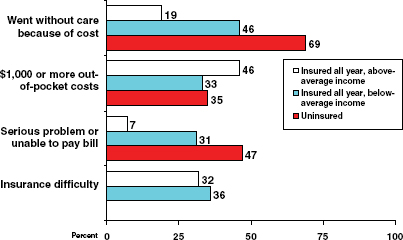
FIGURE 14-3 U.S. adults (under age 65) with below-average income have high out-of-pocket health care costs even when insured.
SOURCE: Schoen, 2011. Based on analysis published in Schoen et al., 2010.
similar to the uninsured than they are to the insured.” Dr. Ho, a committee member, noted that the results shown in Figure 14-2 are also “striking” because a significant amount of individuals with insurance forego care (31 percent) and have financial stress due to medical bills (21 percent). Ms. Schoen concurred with this observation and credited some of this foregone care to the burden created by high deductibles.1 This observation, she said, provides additional reason to be “cognizant” about “where the cost sharing is” in the bronze, silver, gold, and platinum levels mandated by the ACA.
Additionally, how insurers set limits on benefits can seriously impact utilization of necessary care, she said. For example, insured people with capped drug benefits have lower drug utilization and worse control of chronic conditions than insured people without a cap. However, even when benefits are not capped, many individuals still underutilize medications and have less desirable use of medical services (e.g., higher emergency department visits and hospitalizations) (Hsu et al., 2006). Ms. Schoen said research has revealed that when low- or modest-income people face even nominal out-of-pocket costs for essential prescriptions (e.g., insulin for diabetes, statins for hypertension), they often skip refills, which results in higher emergency room use, higher hospital use, and poorer health status (Chernew et al., 2008b; Hsu et al., 2006; Tamblyn et al., 2001). Ms. Schoen used the drug benefit example to reiterate that the aim of the ACA should not only be about providing insurance to the uninsured, but also providing “good insurance” to the underinsured. Fortunately, a lot of employers, she said, have begun thinking about the total cost of care (as opposed to thinking narrowly only about pharmaceutical costs) by moving toward value-based benefits.
Ms. Schoen described the United States as “an outlier on out-of-pocket costs.” The country has “much higher cost sharing and deductibles, and many more benefit limits than are typical in other countries” (Schoen et al., 2010). These high OOP costs have a particularly potent impact on when individuals seek care, particularly for families with below-average income, even when the family has insurance (Figure 14-3). In general, studies find
that those with low or modest incomes are particularly sensitive to OOP costs for essential and less essential care (Chernew et al., 2008a; Tamblyn et al., 2001).
Cost-Sharing Provisions in the ACA
The ACA requires a “sliding scale set of premium protections” for families up to 400 percent of the federal poverty level (FPL). Table 14-1 shows The Commonwealth Fund’s analysis of cost sharing requirements for the ACA’s silver level plan; the amount of the subsidy available in an exchange is tied to the second lowest silver level plan. Ms. Schoen pointed out that the OOP maximum is “substantial,” particularly for families under 150 percent of the federal poverty level (FPL), or under 200 percent of poverty. A family making $30,000 per year, for example, would have an OOP maximum of $3,967, which amounts to over 13 percent of their total income. In addition to medical expenses, families could be paying up to 4 percent of their income on health insurance premiums. Families making $35,000 a year would face OOP costs up to 11 percent of their incomes and premiums up to 6 percent of their incomes ($3,967/$35,000). "We don’t typically expose people who earn $100,000 or more to spend such high levels of their income,” Ms. Schoen said, “but we will for some in the low- and modest-income range.”
Considerations in Defining the EHB and Cost Sharing
Ms. Schoen concluded by sharing with the committee some of The Commonwealth Fund’s findings gleaned from researching insurance plans both domestically and internationally. First, the EHB, she said, should “be fairly broad in scope without arbitrary limits on the number of physical therapy visits or doctors’ visits.” If plans are allowed to variably impose such limits, she said, “it is a subtle way of doing risk selection” because the limits could “target people with particular health conditions.”
Second, cost sharing should be non-discriminatory by health condition, age, and sex. “Fine print” exclusions, Ms. Schoen said, can “be pretty subtle” and can have the effect of excluding all enrollees with diabetes, for instance, if the plan does not cover insulin.
Third, value-based insurance design offers the opportunity to use cost-sharing requirements to encourage use of valuable services while discouraging use of “discretionary” services. But these benefit decisions, she cautioned, must be evidence-based and transparent (e.g., through public disclosure in a standardized format) so that benefit design is not done with the goal of creating “niche markets for carriers.” To lower OOP pharmaceutical costs, for example, Ms. Schoen suggested exploring the exclusion of pharmaceuticals from the general deductible. This way, she said, plans could use a value-based design that encourages use of maintenance drugs.
|
|
||||
Poverty Threshold 2011 |
Income Single or Family | Premiumas%income, Silver level | Out of pocket maximum | Actuarial value |
|
|
||||
| <133% | S:<$14,484 F:<$29,726 |
2% | $1,983 $3,967 |
94% |
| 133to150% | S:<$16,335 F:<$33,525 |
3to4% | $1,983 $3,967 |
94% |
| 150to200% | S:<$21,780 F:<$44,700 |
4.0to6.3% | $1,983 $3,967 |
87% |
| 200to250% | S:<$27,225 F:<$55,875 |
6.3to8.05% | $2,975 $5,950 |
73% |
| 250to300% | S:<$32,670 F:<$67,050 |
8.05to9.5% | $2,975 $5,950 |
70%ifsilver |
| 300to400% | S:<$43,560 F:<$88,200 |
9.5% | $3,967 $7,933 |
70%ifsilver |
|
|
||||
| SOURCE: Schoen, 2011. Based on Collins et al., 2011. | ||||
Fourth, Ms. Schoen encouraged standardization of plans and formularies. Now, she said, “there does not seem to be any reason” why one plan has one formulary and another plan has a different formulary. “The more we can get formularies to be rational and more similar to each other, the less we’ll drive physicians crazy,” she said. One research study found that a physician and her staff spent $68,000 worth of time interacting with plans (Casalino et al., 2009); streamlined billing could save $7 billion annually (Blanchfield et al., 2010). Standardization could have a positive impact on physicians’ time and costs; it could also positively affect consumers by allowing them to more easily compare plans.
Finally, Ms. Schoen said that benefits should be designed to encourage “long-term attachment to a primary care provider” by exempting primary care visits from the deductible. Such incentives could encourage patients to have a medical home, visit a primary care provider, and enroll in chronic disease programs.
Banthin, J. S. 2011. High out of pocket financial burdens for health care. PowerPoint Presentation to the IOM Committee on the Determination of Essential Health Benefits by Jessica Banthin, Economist, Center for Financing, Access and Cost Trends, AHRQ, Costa Mesa, CA, March 2.
Banthin, J. S., and D. M. Bernard. 2006. Changes in financial burdens for health care: National estimates for the population younger than 65 years, 1996 to 2003. Journal of the American Medical Association 296(22):2712-2719.
Beeuwkes Buntin, M., A. M. Haviland, R. McDevitt, and N. Sood. 2011. Healthcare spending and preventive care in high-deductible and consumer-directed health plans. American Journal of Managed Care 17(3):222-230.
Bernard, D. M., J. S. Banthin, and W. E. Encinosa. 2009. Wealth, income, and the affordability of health insurance. Health Affairs 28(3):887-896.
Blanchfield, B. B., J. L. Heffernan, B. Osgood, R. R. Sheehan, and G. S. Meyer. 2010. Saving billions of dollars—and physicians’ time—by streamlining billing practices. Health Affairs 29(6):1248-1254.
Casalino, L. P., S. Nicholson, D. N. Gans, T. Hammons, D. Morra, T. Karrison, and W. Levinson. 2009. What does it cost physician practices to interact with health insurance plans? Health Affairs 28(4):w533-w543.
Chernew, M. E., T. B. Gibson, K. Yu-Isenberg, M. C. Sokol, A. B. Rosen, and A. M. Fendrick. 2008a. Effects of increased patient cost sharing on socioeconomic disparities in health care. Journal of General Internal Medicine 23(8):1131-1136.
Chernew, M. E., M. R. Shah, A. Wegh, S. N. Rosenberg, I. A. Juster, A. B. Rosen, M. C. Sokol, K. Yu-Isenberg, and A. M. Fendrick. 2008b. Impact of decreasing copayments on medication adherence within a disease management environment. Health Affairs 27(1):103-112.
Collins, S. R., M. M. Doty, R. H. Robertson, and T. Garber. 2011. Help on the horizon: How the recession has left millions of workers without health insurance and how health reform will bring relief. New York: The Commonwealth Fund.
Himmelstein, D. U., E. Warren, D. Thorne, and S. Woolhandler. 2005. Illness and injury as contributors to bankruptcy. Health Affairs W(5):63-73.
Hsu, J., M. Price, J. Huang, R. Brand, V. Fung, R. Hui, B. Fireman, J. P. Newhouse, and J. V. Selby. 2006. Unintended consequences of caps on Medicare drug benefits. New England Journal of Medicine 354(22):2349-2359.
O’Toole, T., J. Arbelaez, and R. Lawrence. 2004. Medical debt and aggressive debt restitution practices. Journal of General Internal Medicine 19(7):772-778.
Schoen, C. 2011. Essential benefits and “underinsured”: Ensuring access and protecting against financial risk. PowerPoint Presentation to the IOM Committee on the Determination of Essential Health Benefits by Cathy Schoen, Senior Vice President for Policy, Research, and Evaluation, The Commonwealth Fund, Costa Mesa, CA, March 2.
Schoen, C, S. R. Collins, J. L. Kriss, and M. M. Doty. 2008. How many are underinsured? Trends among U.S. adults, 2003 and 2007. Health Affairs 27(4):w298-w309.
Schoen, C, R. Osborn, D. Squires, M. M. Doty, R. Pierson, and S. Applebaum. 2010. How health insurance design affects access to care and costs, by income, in eleven countries. Health Affairs 29(12):2323-2334.
Tamblyn, R., R. Laprise, J. A. Hanley, M. Abrahamowicz, S. Scott, N. Mayo, J. Hurley, R. Grad, E. Latimer, R. Perreault, P. McLeod, A. Huang, P. Larochelle, and L. Mallet. 2001. Adverse events associated with prescription drug cost-sharing among poor and elderly persons. Journal of the American Medical Association 285(4):421-429.








