Good information about the allied health workforce is critical to good decision making, and three speakers at the workshop looked specifically at data issues as they relate to the supply and demand for allied health workers. Harold Jones, dean of the School of Health Professions at the University of Alabama at Birmingham, examined federal data sources and some of the limitations of those data in projecting supply and demand. Erin Fraher, director of the Health Professions Data System at the University of North Carolina at Chapel Hill, described the data collection and analysis system in North Carolina, which serves as an example for health care workforce planning. Finally, Jennifer Nooney, management analyst within the Health Resources and Services Administration’s (HRSA’s) National Center for Health Workforce Analysis, outlined the effort being undertaken by HRSA to develop a minimum dataset that can help harmonize data collection and analysis.
DATA FROM THE BUREAU OF LABOR STATISTICS
High-quality data are needed for policy makers at the federal, state, and local levels and for leaders in the education sector to make informed decisions. However, the allied health disciplines have a dearth of systematic data collection and integration of that data, said Jones. Some data are available, but they have significant limitations.
Every 2 years the Bureau of Labor Statistics (BLS) issues 10-year workforce projections. Data collection and analysis occur about 6 months before the report comes out, and the last publication was in November 2009, with
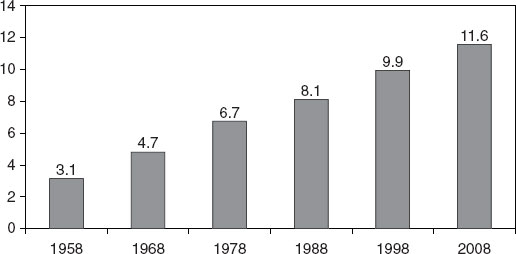
FIGURE 4-1 Percentage of total private-sector employment in private-sector health care industries: 1958–2008.
SOURCE: BLS, 2009b.
a new publication planned for November 2011. The report provides anticipated job openings based on the creation of new jobs and projected retirements and attrition. These projections are most useful for career guidance and some long-term planning exercises, said Jones. They identify industries expected to undergo growth, so that an individual can consider a career in those industries or policy makers can invest in workforce development. For example, as seen in Figure 4-1, the BLS data show health care occupations have grown rapidly as a percentage of total employment in the past: from about 3 percent in 1958 to almost 12 percent today. Further, Table 4-1 shows that BLS projections also forecast strong growth in the future for health care professionals.
Projections are also available for individual occupations (see Table 4-2), but the data become less reliable at smaller scales for several reasons. First, the model assumes full employment, but that assumption has not held for the past several years and is unlikely to do so for the next few years at least. According to a report from the Center on Education and the Workforce at Georgetown University,
The recession that began in December of 2007 is already 30 months old, but the U.S. economy will not recover its prerecession employment levels for at least another 2 years. From there, it will take an additional 3 years to make up for lost growth and create a job market strong enough to employ both the casualties of the recession and the millions of new workers who will stream into the workforce from schools across the country. (Carnevale et al., 2010)
For example, even though the profession of nursing is projected to undergo strong growth as the U.S. population ages, newly admitted resident nurses have had a hard time finding jobs as the economy has struggled.
Also, the BLS data generally do not anticipate trends well within an industry. For example, with the Patient Protection and Affordable Care Act slated to provide insurance for millions of additional people, several major questions arise: Will those people receive the majority of their care from primary care physicians, nurse practitioners, physician assistants, or others? What kinds of diagnostic testing will grow most strongly? Will accountable care organizations or other kinds of institutions have increased control over health care spending? Will projected growth in the number of physicians increase the demand for people in allied health, as it has in the past? These questions do not yet have answers, but those answers will have a powerful effect on workforce trends within allied health.
The biggest problem with the BLS data, said Jones, is that they only address demand, not supply. Matching demand to supply requires knowing the capacity for production in any given discipline. A cautionary tale from pharmacy is a good example. The BLS data (see Table 4-2) show the
|
TABLE 4-1 U.S. Workforce Employment, 2008 and Projected 2018 |
||||
| Occupation | Employment numbers (in thousands) | Change (percentage) | Total job openings due to growth and net replacements, 2008–2018 (in thousands) | |
| 2008 | 2018 | |||
| Community and social services occupations | 2,724 | 3,172 | 16.5 | 1,033 |
| Education, training, and library occupations | 9,210 | 10,534 | 14.4 | 3,332 |
| Health care practitioners and technical occupations | 7,491 | 9,091 | 21.4 | 3,139 |
| Health care support occupations | 3,982 | 5,130 | 28.8 | 1,595 |
| Sales and related occupations | 15,903 | 16,883 | 6.2 | 5,713 |
| Office and administrative support occupations | 24,101 | 25,943 | 7.6 | 7,255 |
| Installation, maintenance, and repair occupations | 5,798 | 6,238 | 7.6 | 1,586 |
| Production occupations | 10,083 | 9,734 | –3.5 | 2,156 |
SOURCE: BLS, 2009a.
|
TABLE 4-2 U.S. Workforce Employment, 2008 and Projected 2018 by Detailed Occupation |
||||
| Occupation | Employment numbers (in thousands) | Change (percentage) | Total job openings due to growth and net replacements, 2008–2018 (in thousands) | |
| 2008 | 2018 | |||
| Physicians and surgeons | 661 | 806 | 21.8 | 261 |
| Pharmacists | 270 | 316 | 17.0 | 106 |
| Registered nurses | 2,619 | 3,200 | 22.2 | 1,039 |
| Occupational therapists | 105 | 131 | 25.6 | 46 |
| Physical therapists | 186 | 242 | 30.3 | 79 |
| Physician assistants | 75 | 104 | 39.0 | 43 |
| Speech-language pathologists | 119 | 141 | 18.5 | 44 |
| Athletic trainers | 16 | 22 | 37.0 | 12 |
| Medical and clinical lab technologists | 172 | 193 | 11.9 | 53 |
| Medical and clinical lab technicians | 156 | 181 | 16.1 | 55 |
| Dental hygienists | 174 | 237 | 36.1 | 98 |
| Radiologic technologists and technicians | 215 | 252 | 17.2 | 68 |
| Respiratory therapists | 106 | 128 | 20.9 | 41 |
| Home health aides | 922 | 1,383 | 50.0 | 553 |
| Medical assistants | 484 | 648 | 33.9 | 218 |
SOURCE: BLS, 2009a.
demand for pharmacists growing by 17 percent from 2008 to 2018, with 106,000 new jobs over that period. For the past decade, pharmacy schools have responded to these projections by increasing enrollments and opening new programs. Now there is great concern about an overproduction of pharmacists. Similar mismatches are occurring in other fields.
Data Needs
Jones cited several factors that need to be taken into account in establishing workforce development policies. First, many important data are unavailable. What percentage of people trained in an area actually enter
that area, how long they stay in a profession, and how many people reenter a profession after time away from it are all uncertain. The geographic distribution of workers is another issue, particularly as it affects care in underserved areas. Finally, unforeseen policy or economic shifts can dramatically and quickly affect both workforce supply and demand.
Workforce projections in allied health face particular challenges. Allied health education is offered in almost every type of postsecondary educational institution. The professions that fall under the label of allied health have different sizes and structures, different education requirements, and different infrastructures for data collection. No one group has the responsibility to provide the needed data, said Jones. “The federal government does play a pivotal role in helping us to devise common ways to define the data and then serves as a nonbiased source to integrate that data that we collect, but this is something that we all have to share.”
ALLIED HEALTH WORKFORCE PLANNING IN NORTH CAROLINA
In 1979 the North Carolina Health Professions Data System (HPDS) began maintaining data files containing complete licensure data for a variety of health professions (HPDS, 2011). A collaboration between the University of North Carolina and the health professions licensing boards, the HPDS seeks to provide timely, objective, and evidence-based analyses to inform health workforce decisions. Data are provided voluntarily by the boards—no legislation requires them to do so. “They do it because they know it helps them and it helps the state,” said Fraher.
These data make it possible to do longitudinal and interprofessional comparisons that can greatly improve statewide planning. For example, in examining the data, Fraher found that the per capita population of physical therapists in North Carolina grew almost fivefold from 1979 to 2009. The population of physical therapy assistants has grown even faster, and both grew faster than the supply of physicians, nurses, and pharmacists. However, the population of physical therapists grew most dramatically in the areas of the state that do not have shortages of health care professionals. Programs exist to get physicians and nurses into shortage areas, said Fraher, but far less attention has been directed toward allied health professions.
The data also reveal that many allied health professions are less diverse than the North Carolina population. “What are we doing to get underrepresented minorities into the allied health professions and build career ladders?” Fraher asked.
The HPDS also collects demand-side data by tracking the number of vacancies in online sources and newspapers. For example, data from 2010 (Kimball et al., 2011) show that occupational therapy assistants are in the
highest demand relative to the size of the workforce. With 121 advertisements and a workforce of about 900, about 13.4 vacancies exist for every 100 people in the workforce. Educators can use this information to set enrollments in state programs, and workforce development boards can use them to allocate efforts, Fraher said. Demand varies by location in the state. About 30 percent of the allied health job vacancies in North Carolina in 2010 were for physical therapists, but this number varies from almost half in the southern portions of the state to about a quarter in the western parts of the state.
The data collected by the HPDS reveal that allied health is “a job machine,” according to Fraher. As seen in Figure 4-2, employment in health care and social assistance has steadily risen while manufacturing employment has fallen. “This is the graph that made the governor sit up straight and say we need to be concentrating on health jobs.” Even in the recent recession, Figure 4-3 shows that health care employment stayed fairly constant, while employment in areas other than health care plummeted. Health care has the potential to sustain local economies, particularly rural ones, and is less vulnerable to outsourcing, Fraher said. Job growth in these fields is also likely to continue given demographic changes, population growth, and the expansion of insurance coverage.
The workforce development commission in North Carolina has created an allied health regional skills partnership that includes community colleges, local government, health care employers, and other regional stake-
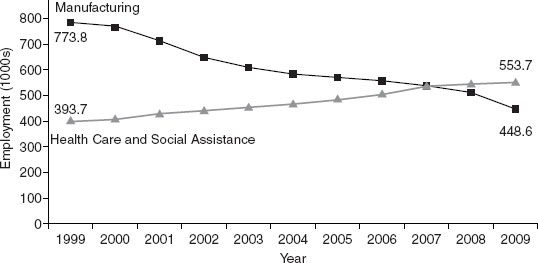
FIGURE 4-2 Health care and social assistance employment vs. manufacturing employment, North Carolina, 1999–2009.
SOURCE: Reprinted with permission from Erin Fraher, North Carolina Health Professions Data System.
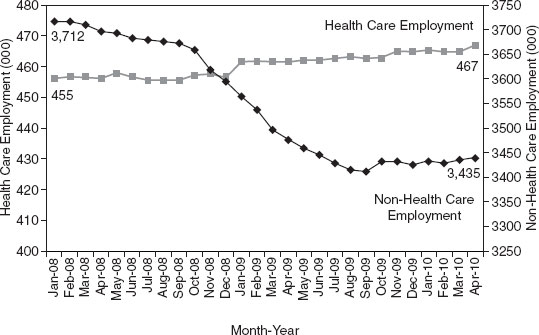
FIGURE 4-3 Health care and non-health care employment during recession, North Carolina.
SOURCE: Reprinted with permission from Erin Fraher, North Carolina Health Professions Data System.
holders. The partnership addresses allied health workforce issues in the region with a special focus on the sectors’ competitiveness and creating employment and career advancement opportunities for unemployed and dislocated workers. This is a great story, said Fraher, of “how you use data to implement change.”
Data and Health Care Reform
As health care reform progresses, workforce planning will become even more important, according to Fraher. Economic trends are of course influential, but large-scale policy change is needed for the next generation of workforce planning. In a new world of patient-centered medical homes (PCMHs) and accountable care organizations (ACOs), the emphasis will be on how care is delivered, not who delivers care.
Full implementation of the PCMH and ACO models will require shifting workforce planning away from specific professional groups or employment sectors toward planning for the health service needs of defined populations. Different models of care and configurations of skills will
need to be evaluated for cost and quality. For example, one practice might rely more heavily on medical assistants, while another uses more physical therapy assistants than physical therapists. Much better and more data will be needed on the effects of these differences on outcomes.
North Carolina has received a state health care workforce planning grant from HRSA and has used it to assess the key health care services provided by PCMHs, the number and types of professionals needed in PCMHs, and how well supply matches the needs of the population. It also is using the grant to identify the need for new programs, mechanisms to retool the existing workforce, and the need for new professionals to meet the needs of PCMHs.
Care in medical homes can be distinctive because of its reliance on coordination, case management, and linking the health care system with the community. But who does care coordination, Fraher asked. It could be a nurse, a social worker, a medical assistant, or another health care professional. Similarly, patient education can be done by medical assistants, registered nurses, primary care physicians, or others. “Let’s open the patient-centered medical home box and understand who is in there and what they’re doing… and then think about what that means for new programs,” Fraher said. Change will often require retooling the existing workforce rather than relying on new graduates and being open to new health professions that emerge as a result of change.
Lessons Learned in North Carolina
Fraher pointed to several lessons learned from experiences in North Carolina. First, we plan, she said. Having better information enables employers, educators, practitioners, and students to make better decisions. For example, Fraher noted that workforce planning saved the state $80 million when it decided not to open a pharmacy school because data showed that it did not need another pharmacy school. Instead, the data pointed to serious oral health disparities in the eastern part of the state, and eastern North Carolina now has an innovative model of dental education. “We actively engage in using our data for workforce planning.” An inventory of existing datasets could show what data are not collected that need to be, what the strengths and limitations of existing data are, and what the barriers to getting data are. Also, if a minimum dataset is defined, it should expand to cover all valid health professions, said Fraher.
Another lesson learned is to cultivate a role for professional associations and licensure bodies. The licensure bodies in North Carolina have been “fantastic,” said Fraher. “They are as actively involved in understanding health workforce planning in the state as we are.”
The balance between the state and federal roles is still in flux. What is
the national role in health workforce planning, what is the state role, and how can the two best work together?
National data comparable to the North Carolina data are not yet available. National data would benefit North Carolina as well as other states, because then state data could be compared with numbers in other states and with data for the nation as a whole. One impediment is that different states and the federal government have different ways of collecting and analyzing data. “Let’s get together and learn how to speak the same language,” Fraher stated.
Finally, continued investments are needed to build and maintain these datasets, and states will need technical assistance to get them up and running. “Be inventive,” said Fraher. “It’s not just federal resources; there is foundation funding and other funding.”
A UNIFORM HEALTH PROFESSIONS DATASET
Health workforce data serve several important uses, said Nooney. First, they make it possible to understand trends in workforce supply, demand, distribution, and shortage. “You have to know where you’ve been and what types of conditions occur alongside shortages to be able to predict when this is going to occur again,” Nooney said. Second, workforce data collected across time, place, and profession enable benchmarking against other professions, geographic areas, and baseline levels. “We have lots of workforce data, but one of the problems is it is all a little bit different from place to place and profession to profession. That hampers our ability to make these comparisons.” Third, data are a needed input for projections of supply and demand. Good projections provide detailed information about, for example, career transitions, the aging of the workforce, and when workers tend to retire. Without this information, it is difficult or impossible to project workforce supply in a particular area. Fourth, workforce data guide the development and evaluation of policies and programs to enhance the health workforce. Good policies are data driven. When something is going wrong, the data indicate ways to fix the problem and monitor progress toward a solution. “They allow course corrections through policies and programs,” said Nooney.
Sources and Limitations of Workforce Data
Many different entities collect workforce data in the health professions, and data are plentiful, but the quality of the data ranges widely. Many professional associations collect supply-side information on their workforce during membership renewal and at conferences. Many professional associations also attempt to survey all licensed professionals within an
area, but because they generally do not have the ability to mandate completion of the surveys, the data are incomplete. Regulatory and certification organizations, including state licensure boards and national certification and credentialing organizations, collect data during the registration and licensing processes. In this case, they are able to reach all of the licensed professionals in an area every several years. “That’s a great opportunity to collect information,” said Nooney. State workforce planning agencies, such as the HPDS in North Carolina, collect workforce data. Many researchers also collect workforce data, though their samples are often small and their topics narrow. However, these data can be useful for digging deeply into some of the complex questions that surround the workforce. Finally, the federal government collects data, both through federal-state collaboratives and through primary data collection. For example, HRSA has supported the National Sample Survey of Registered Nurses quadrennially since 1977 (HRSA, 2011b).
Despite all these sources of data, the information available is not sufficient to meet many policy objectives, Nooney said. As Fraher observed, the wide variation in approach is a major problem. The items in surveys, the wording or response options, the populations being sampled, and other factors vary from source to source. “This is problematic because we can’t put all of this together and make the comparisons that we need,” said Nooney. “Differences in data collection hamper comparisons across professions, area, and time.”
A Minimum Dataset
The purpose of the minimum dataset project at HRSA is to standardize data collection to improve workforce planning and policy development. As a first step, HRSA is focusing on supply data, with plans to apply lessons learned in that area to demand data and education program capacity and output. It also is collecting data initially for a limited number of health professions: physicians, nurses (including advanced practice nurses), physician assistants, dentists and dental hygienists, pharmacists, and physical therapists. These professions are some of the largest in health care and also reflect the priorities of HRSA, which is focused on primary care and health profession shortage areas.
Datasets will be harmonized through standardized questionnaires or instruments. A meeting of researchers was convened to discuss which items are essential, which are not essential, and the purposes of data collection. Items for a minimum dataset have been drafted, and at the time of the workshop they were being circulated for internal review and revision. The next step is to convene stakeholder meetings to gather feedback from the community about the items and about implementation. Documentation and
guidelines will be drafted to help in the collection of data, and outreach and technical assistance will promote implementation.
The broad areas in the minimum dataset include education and training (e.g., degrees earned and types of training and certification); basic demographic data (e.g., age, gender, and race); and practice, activity, and employment information (e.g., numbers of hours worked, activities conducted, and where those activities are conducted).
Nooney emphasized the word minimum. HRSA is not trying to collect detailed data for each profession. It is seeking to develop a core set of essential items that can be implemented with limited resources. “We are trying to keep it small and focus on standardizing a small subset of items that we can’t live without.” HRSA also will be building on the many entities that have well-developed data collection infrastructures. For example, professional associations and state licensure boards are in a unique position to support this endeavor because they collect data every time a licensed professional reregisters. Licensed professions such as medicine and nursing have available sources of data, but allied health is a bigger challenge since it is populated with many unlicensed professions. Also, some allied health professions have a lower rate of professional identity or membership in professional associations, which reduces the potential for data collection. And allied health professionals tend to practice in a wide variety of settings, so trying to reach them at their place of employment or through employers is a challenge. HRSA hopes to work out some of these problems before expanding to many of the allied health professions.
The benefits of a minimum dataset in the allied health professions will be similar to the benefits for medicine, nursing, and other professions, said Nooney. It will support the ability to assess trends in supply, distribution, and practice patterns; enable more accurate projections; guide the development of programs and policies; and improve understanding of workforce aging and retirement patterns. In fact, concluded Nooney, data for the allied health professions will be even more useful than in other areas because so little data are available today.
During the discussion period, the moderator of the session on data needs, Edward Salsberg, director of the National Center for Health Workforce Analysis, said that HRSA was open to talking with other allied health professions, in addition to physical therapy, about the minimum dataset. “One of the challenges, as you’ve seen from this morning’s discussion, is who we should sit with if we want to talk about allied health professions as a group.”
He also discussed possible ways to motivate organizations and states to
collect data. One approach is simply to emphasize that it is in an organization’s or state’s interest to do so. Another argument is that better data can help with the credentialing process.
He mentioned that HRSA is working with the BLS on demand-side issues. One complication is that the Standard Occupational Classification (SOC) is only changed once every 10 years, and the most recent change was in 2010. Because of the lead time involved in making changes, people who want to add an allied health profession to the next release of the SOC should start working with HRSA and BLS now.
Jones emphasized that the allied health professions cannot expect HRSA to collect all of the data that are needed. States, professional organizations, and educational institutions all need to collect data in a useful format and combine their efforts. These organizations also have much to gain from participating in this effort.
A workshop participant observed that standards, licensing, and credentialing requirements (e.g., requirements for higher educational levels) are often used to control the number of people in a workforce, and Jones agreed, saying that economic realities are inevitably a factor. But he also noted that health care reform is seeking to change some of these forces. Some activities carried out only by physicians in the past may move into the allied health professions. Activities such as coordinating chronic disease management could be handled in many different ways, and health care reform will influence the decisions that are made.
Fraher brought up the divide between advanced educational requirements and the activities actually performed in some allied health fields. For example, physical therapy contains two groups of practitioners: a more advanced group for whom higher educational levels are appropriate, and a more assistive group. Also, high educational levels can contribute to a lack of diversity and geographic disparities, she said. For example, community colleges tend to pull from their local communities and produce graduates who go to work in their local communities, which results in a more diverse and distributed workforce. Nursing deals with many of the same kinds of issues as allied health and could provide a model for allied health fields, she said.
Nooney observed that demand projections depend heavily on the age, size, and shape of the population. Also, surveying employers is a way to get demand-side information not available in other ways. “Employers see what’s happening on the ground,” she said. “They have vacancies or they don’t. They have trouble recruiting or they don’t. They have plans to expand their practice or their facility or they don’t.”
In response to a question about whether the professionals delivering care have the body of knowledge, accreditation, or certification needed to do so, Fraher said that much better data are needed on the outcomes of
using assistive personnel. “What are the implications for cost and quality of substituting an assistive person for someone else—we don’t know.” Certification limits supply, but better evidence is needed on skill mix configurations and what they mean for cost and quality.
Salsberg responded that a challenge in the workforce planning community is to understand both short- and long-term trends. In the recent recession, the job market was soft even for nurses and allied health professionals, but that does not say much about what the job market will be like 10 years from now. “It is critical that we do the analysis… so we can advise the community.” A focus on the short term can lead to overproduction and temporary surpluses followed by underproduction and shortages. “Getting better data and looking at the long-term needs is going to be critical for the future.”














