Methodology: Development of the Committee’s Recommendations
To develop recommendations1 for accelerating progress in obesity prevention, the committee undertook a series of steps. The process was informed primarily by the development of a set of guiding principles (detailed in Chapter 4). As described in Chapter 1, the committee was charged as a first step with reviewing obesity-related recommendations from previous Institute of Medicine (IOM) reports and other relevant sources. To this end, the committee identified recommendations to review, organized and grouped these recommendations, and developed a process for reviewing and filtering them. Complementary (and parallel) to the set of filtering criteria, an approach was used to help identify relationships and synergies among the recommendations with the most promise to accelerate progress in obesity prevention. Throughout the process, gaps were identified and considered in developing the final set of recommendations. From these efforts, a comprehensive approach to this study emerged that includes five critical areas, linked as an interrelated system. The committee’s recommendations and strategies and potential actions for implementation are presented in Chapters 5-9 (and again in Appendix C). The following sections provide additional detail on how the committee developed its recommendations.
![]()
1 As described in Box 4-1, the term “recommendations” as used in this report refers in general to a group of terms unless otherwise specified. Thus the committee’s “recommendations” include the recommendations and their associated goals, strategies, and potential actions, and the review of prior “recommendations” includes what others have identified as recommendations, interventions, actions, and strategies.
IDENTIFICATION, ORGANIZATION, REVIEW, AND FILTERING OF PRIOR RECOMMENDATIONS
Identification and Organization
The committee began by compiling all previous obesity-related recommendations from the IOM and other relevant sources. It should be noted that the IOM and National Research Council (NRC) reports all were developed to fulfill a specific task that defines the scope of each report and consequently may limit the scope of its recommendations.
The general criterion used in deciding which recommendations to review was that they were relevant to population-based obesity prevention approaches; that is, they were intended to lower the mean body mass index (BMI) level and decrease the rate at which people enter the upper end of the BMI distribution. Although searches were not limited by the date of publication, the year 2005 marked the beginning of the National Academies’ issuance of obesity prevention-related recommendations. The 2005 IOM report Preventing Childhood Obesity: Health in the Balance and the 2005 Transportation Research Board report Does the Built Environment Influence Physical Activity? demonstrated increasing recognition of the complex, multifaceted nature of the many factors that influence energy balance (IOM, 2005; TRB/IOM, 2005). This recognition led to the examination of obesity prevention strategies that moved beyond a biomedical model and an individual behavior change approach to encompass multilevel, multisector policy and environmental approaches. National Academies reports and reports outside of the National Academies that include recommendations emerging from this conceptualization were published mainly in 2005 and beyond (with some exceptions).
The criteria for including a report and consequently its recommendations in the committee’s review were as follows:
• included only population-based obesity prevention strategies;
• used established procedures for making recommendations (e.g., evidence-based, transparency in decisions made);
• included only environmental and policy strategies (as opposed to strategies focused on individual behavior or biomedical approaches); and
• was derived from some type of expert task force or committee consensus.
The quest for relevant publications included an online search of several databases and publication lists of relevant organizations and a review of references
in reports that were identified. Committee members, public workshop presenters and attendees, interested stakeholders, and the public also provided suggested sources for review (see the end of this appendix for a list of reports included in the review).
Approximately 800 obesity-prevention related recommendations were identified from these reports. To manage this large number of recommendations, the committee organized them into 10 broad topics (school foods; health care; food marketing; agriculture policy; physical activity, physical inactivity, transportation, and the built environment; pregnancy, early childhood, and child care; nutrition education and information; research, monitoring, and evaluation; food access and pricing; other). Within each broad topic, similar recommendations were grouped to help identify themes and continue to identify gaps.
Review and Filtering
Each recommendation that met the above inclusion criteria was reviewed and coded on several dimensions based on the committee’s guiding principles (see Chapter 4) so the committee could assess its promise for accelerating progress in obesity prevention over the next decade. A textual description of each filter was provided to the coder to ensure consistency in judgments. The filters used were
• policy or funding dependent;
• reach/scope;
• potential magnitude of impact;
• evidence base;
• reduction of disparities;
• geographic implementation to date;
• degree to which recommendation is actionable;
• measurability;
• unintended consequences;
• timeline to implementation; and
• feasibility, practicality, and cost if known.
At least two coders were assigned to each recommendation or group of related recommendations. Each coder worked independently, and disagreements were resolved through discussion. If consensus was not readily obtained by the pair of coders, additional committee members were consulted. Once agreement had been reached, both coders’ comments on the promise of the strategy were compiled,
and a list of strategies based on the results of the coding exercise was developed. These recommendations were shared with the full committee, revised, updated, and consolidated as a result of further committee deliberations. The recommendations were judged against these filters using the information or evidence provided in the reports in which the recommendations were offered. Additionally, related information and evidence made available since the issuance of the original recommendations, as well as information on the progress of their implementation, was identified and considered to inform the coding process.
The search for and interpretation of relevant evidence for each recommendation was guided by a framework that was developed to inform decisions on obesity prevention, integrating research evidence into a broader policy context (IOM, 2010a). This framework with which to locate, evaluate, and assemble evidence to inform decisions on obesity prevention decision making (the L.E.A.D. framework) was used to identify, locate, and evaluate the type of evidence appropriate for the task of prioritizing the recommendations based on the best available scientific evidence. Being concerned with locating evidence to help in assessing the effects of the recommended interventions, the committee sought effectiveness studies, as well as studies examining the presumed mechanism of the intervention effects. Guided by the L.E.A.D. framework, the committee broadened its search to include empirical comparative studies and evaluations commonly referred to as impact assessments or outcome evaluations. Additionally, the committee considered implementation evidence to determine whether an intervention is still needed, whether it had the intended effects with the expected impact, and whether changes to the intervention might be necessary in the future. Finally, the committee took into consideration political and practical concerns such as the cost, feasibility, and practicality of implementing the interventions. To identify research related to an intervention’s effectiveness, implementation, and relevance, the committee searched a wide variety of data sources, including the scientific literature; grey and unpublished literature; surveys, polls, and rankings; and government policies and programs. The committee focused its searches by first seeking and using literature syntheses and updates, and if no recent syntheses were found, searched for evidence on the particular recommendation of interest and also reached out to states, communities, and localities that have implemented an intervention for implementation-related research.
IDENTIFICATION OF LINKAGES AMONG FILTERED RECOMMENDATIONS
As described in Chapter 4 and recommended by the L.E.A.D. framework, mapping the determinants of a problem can elucidate potential mechanisms and dynamic pathways on which a more comprehensive approach should focus. Accordingly, the committee mapped the pathways through which the most promising recommendations (as identified through the above process) relate, thus taking a comprehensive systems approach that links the committee’s recommendations.
As the committee gathered and reviewed prior recommendations, it became increasingly clear that to identify which recommendations were most likely to accelerate progress in obesity prevention, the committee needed to understand and map how the various recommendations would interact and reinforce or perhaps inhibit progress. To this end, it was necessary to understand that for each recommendation under consideration, there was a primary mechanism by which change would be effected and that each had a set of prerequisites, accelerants, and inhibitors that could potentially come into play during its implementation. The primary mechanism describes the pathway, or how and why a recommendation would help prevent obesity. Prerequisites are elements necessary for a recommendation to be implemented or to be successful. Examples include public acceptance and willingness and adherence to or enforcement of existing policies and regulations. Accelerants are factors that will speed up the effectiveness or leverage the impact of a recommendation. Examples include appropriate resources and well-organized coalitions and partnerships, as well as tools and templates to offer guidance. Inhibitors are elements that will slow the effectiveness of a recommendation or impede its implementation. Examples include existing legislation, regulations, or policies that prohibit action; a lack of guidance for implementation; a lack of pilot programs implementing the recommendation; and a lack of public, private, or political will and leadership.
The committee undertook a process of participatory model building to create a systems map that would illustrate how the recommendations were interrelated. As discussed in further detail in Chapters 2 and 3, the committee discussed the determinants of obesity and what changes have occurred in the United States over the past several decades as the obesity epidemic emerged. The committee analyzed how past decisions influenced the current landscape, and considered why so many private, public, individual, and societal decisions have been ineffective in achieving intended objectives. Deliberations and discussions led the committee to accept that answers to such questions might lie in the dynamic behavior of social, personal,
environmental, political, and physical systems (Forrester, 1991), and that using system mapping as a tool (i.e., a systems map) would enable the committee to organize and make sense of the task at hand.
The result of these deliberations was the emergence of a comprehensive strategy to link actions in five critical areas that served as the basis for the committee’s recommendations. The next section provides a detailed discussion of the map of the committee’s recommendations as an interrelated system of interventions.
DEVELOPMENT OF THE SYSTEMS MAP
The systems map in this report is a visual tool designed to aid in identifying linkages among and between the committee’s recommendations and implementing strategies. It allows visual communication of the latent potential effects of the recommendations and strategies both individually and synergistically, as well as how they fit within the broader societal context. This map makes it possible to identify strategies that may serve as prerequisites for other actions or may help reinforce their impact. It also allows the discovery of “long chain” effects of strategies that go beyond their immediate focus and impact. Finally, the map facilitated the design of a cohesive set of strategies that support each other as a system, increasing the effectiveness of the committee’s recommendations by approaching them from multiple directions (see Figure B-1).
How to Read the Map
The map contains three shapes: squares, circles, and arrows. Squares are labeled with letters (A through E) and represent the committee’s five recommendations, as listed in the accompanying legend. Circles are labeled with numbers (1 through 20) and represent the strategies suggested for implementing the recommendations. The coloring of the strategies reflects the sector(s) of action they represent: the business community/private sector, the public sector, citizens and civic/ community organizations, health care, and worksites/employers. The recommendations and strategies shown on the map and listed on the legend are described in detail in Chapters 5 through 9.
An arrow indicates a connection between one strategy and another, between a strategy and a recommendation, or between two recommendations. The arrows are directional, indicating the flow of influence from one shape to another. An
arrow pointing from a circle to a square can be read as “this strategy influences or affects this recommendation.” Arrows may also be bidirectional, indicating positive feedback between the two shapes at its endpoints.
Construction of the Map
The systems map was constructed using an iterative process. Early in this process, the entire committee was given a background presentation on systems approaches and their use in other policy arenas. Working groups within the committee also participated in a thought exercise in which they were asked to identify key systems links between strategies and recommendations that met the inclusion criteria outlined above. Based on this exercise, discussions with the committee, and input and assistance from IOM staff, an initial systems map was developed and used to help frame the committee’s discussion of strategies and recommendations. As the committee’s deliberations proceeded, key systems connections were identified by committee members and staff. These connections, along with feedback on the map’s design and a finalized set of recommendations and strategies, were used to generate the final systems map. It is also important to note that as individuals take a systems perspective when implementing these recommendations and strategies, additional connections may be identified.
Each connection (arrow), whether between two strategies (circles), two recommendations (squares), or one strategy and one recommendation, represents a carefully considered relationship of influence or impact identified by the committee and/or staff that is based on the best available evidence or conceptual support. In all cases, a clear mechanism for the flow of influence can be identified.
For example, Figure B-2 shows that the strategy of a nutrition labeling system (a circle labeled 3 in the upper lefthand portion of the map) impacts the strategy of food literacy in schools (a circle labeled 5 at the left and lower in the map) because a simplified nutrition labeling system makes it easier for students to act on the nutrition guidelines taught in schools. Thus an arrow points from circle 13 to circle 15 on the map.
Elsewhere on the map, the strategy of a social marketing program (a circle labeled 11 in the upper center of the map) both impacts and is impacted by the strategy of physical activity-related community programs (a circle labeled 2 nearby) (see Figure B-3). The two are mutually reinforcing. Thus arrows connect the two circles in both directions.
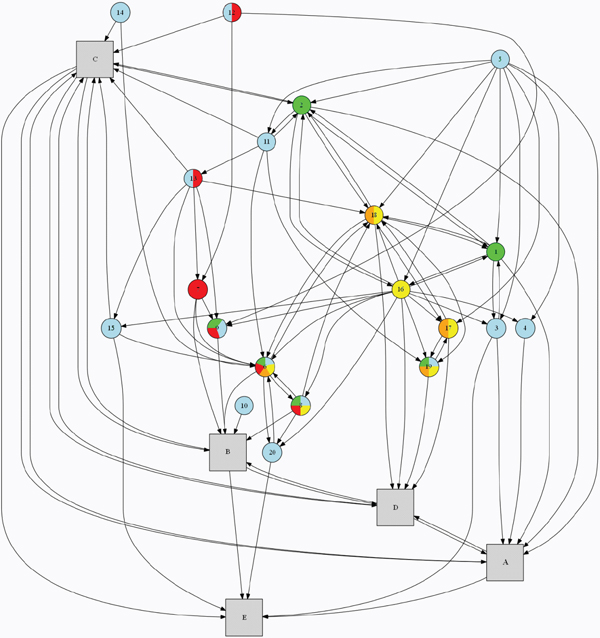
FIGURE B-1 Committee’s systems map for understanding and visualizing the interconnectedness of its recommendations and strategies.
|
Legend for Figure B-1 Strategies* (Circles) (1) Physical and built environment (2) Physical activity-related community programs (3) Physical education and physical activity in schools (4) Physical activity in child care centers (5) Science and practice of physical activity (6) Sugar-sweetened beverages (7) Food and beverage options for children in restaurants (8) Nutritional standards for all food and beverages (9) Food and beverage retailing and distribution policies (10) U.S. agriculture policy and research (11) Social marketing program (12) Food and beverage marketing standards for children (13) Nutrition labeling system (14) Nutrition education policies (15) Food literacy in schools (16) Health care and advocacy (17) Coverage of and access to and incentives for obesity prevention, screening, diagnosis, and treatment (18) Healthy eating and active living at work (19) Weight gain and breastfeeding (20) School food and beverage standards |
[A] Prioritize promotion of physical activity by increasing access and opportunities for such activity. [B] Reduce unhealthy food and beverage options and increase healthier options. [C] Transform the message environment. [D] Increase the support provided by health care providers, insurers, and employers. [E] Make schools a national focal point for obesity prevention. Sector of action (Color) • Business community/private sector (Red) • Public sector (Blue) • Citizens and civic community organizations (Green) • Health care (Yellow) • Worksites/employers (Orange) |
*The strategies and recommendations as seen in the legend have been abbreviated. Appendix C provides the complete content of each strategy and recommendation.
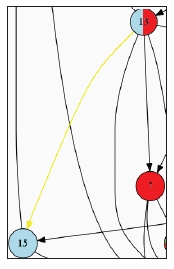
FIGURE B-2 A directional connection arrow on the map. A small section of the map is magnified here, and the arrow is highlighted in yellow.
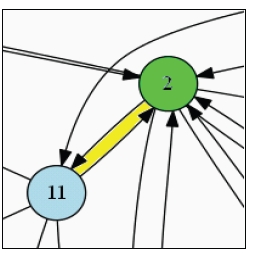
FIGURE B-3 A bidirectional connection on the map. A small section of the map is magnified here, and the two directional arrows are highlighted in yellow.
Use of the Map
The map represents a visual systems organization of the recommendations and strategies presented in the report. This systems view can be used to identify several kinds of patterns in the content of the report, many of which would be less evident in a linear or categorical textual organization of the concepts.
One important type of pattern is that of synergy between strategies that extends their influence to a greater number of recommendations. For example, strategy 14 (nutrition education policies) directly affects only recommendation C (transform the message environment). A categorical mapping of recommendations and strategies would show only this connection. However, the systems map also shows that through its connection to strategy 6 (sugar-sweetened beverages), strategy 14 also indirectly influences recommendation B (reduce unhealthy food and beverage options and increase healthier options) (Figure B-4). This type of
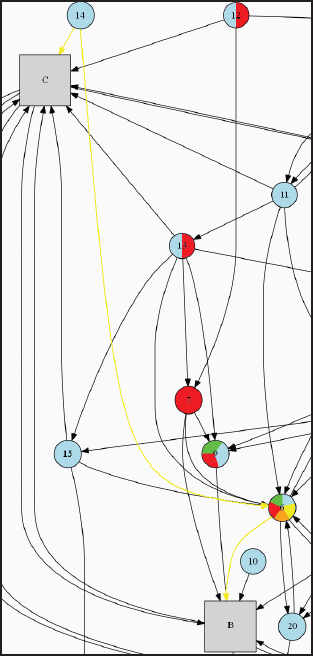
FIGURE B-4 An example of synergy. A subset of the map is magnified here. Direct influence of strategy 14 on recommendation C is shown, as well as indirect influence of strategy 14 via strategy 6 on recommendation B. Arrow tips of key connections are highlighted in yellow.
synergy between strategies helps define a systems approach to obesity prevention and demonstrates the potential for acceleration; the overall set of interventions may add up to more than simply the sum of its parts.
A related structural pattern is a positive feedback or “reinforcing” loop. A good example can be found in the center-right portion of the map, linking strategies 1 (physical and built environment), 16 (health care and advocacy), and 18 (healthy eating and active living at work). Bidirectional links connect strategies 18 and 1; another set of bidirectional links connects strategies 1 and 16; and strategy 16 connects back to strategy 18. Figure B-5 shows how these three strategies are mutually reinforcing and together may be more successful than any one on its own. The connections in this feedback cycle also link actions across three different sectors: citizens and civic/community organizations (strategy 1), health care (strategies 16/18), and worksites/employers (strategy 18). The positive feedback reinforcement between the three ultimately directly benefits recommendation D (increase the support provided by health care providers, insurers, and employers), as both strategy 16 and 18 flow into that recommendation.
A third type of pattern that can be identified using the map are “long chain” effects of strategies that go well beyond their immediate focus or impact. For example, strategy 15 (food literacy in schools) is linked directly only to recom-
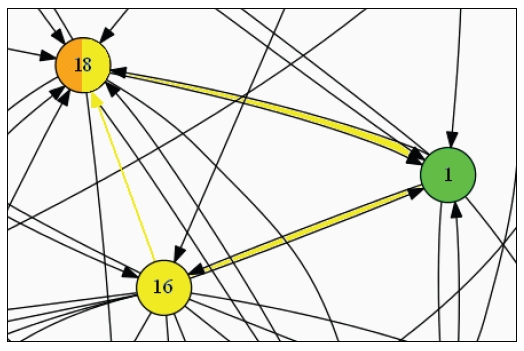
FIGURE B-5 An example of positive feedback. A subset of the map is magnified here. Key directional and bidirectional arrows are highlighted in yellow.
mendations C (transform the message environment) and E (make schools a national focal point for obesity prevention). Using the systems map, however, it can be seen that the impact of strategy 15 flows through to all the other recommendations (Figure B-6). It affects recommendation B via strategy 6 (sugar-sweetened beverages), a two-step connection. It affects recommendation D by a slightly longer chain, from strategy 15→6→18 (healthy eating and active living at work). Finally, it reaches recommendation A by a long chain from strategy 15→6→18→1 (physical and built environment). Thus the systems map shows that
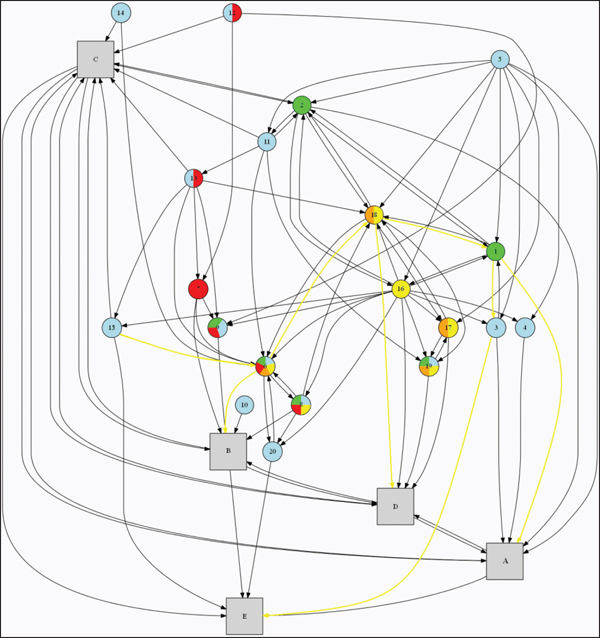
FIGURE B-6 An example of long-chain connections. Key directional arrows are highlighted in yellow.
nutrition education in schools can play a role directly or indirectly in all of the recommendations in the report and is a systemically important strategy.
The map also can be used to assess the package of recommendations and strategies in the report as a whole from a systems perspective and can serve as a national roadmap for action to accelerate progress in obesity prevention that is based on research evidence and the current level of progress in each area considered. The simultaneous implementation of the package of recommendations and strategies would create combined impacts that could further accelerate progress in preventing obesity. Indeed, a straightforward analysis of the map shows multiple connections and multiple pathways leading to each of the five recommendations— suggesting powerful overall systemic synergy as the strategies work together to achieve the recommendations. Similarly, relationship patterns such as those identified in the examples above are numerous, suggesting that the strategies themselves have important reinforcement potential. Finally, and also important from a systems perspective, the map shows many connections between strategies that focus on different recommendations or that involve different sectors of action. For example, strategies 13 and 15 (highlighted in Figure B-2) are connected to each other—even though strategy 13 feeds directly only to recommendation B and partially involves the business community/private sector, while strategy 15 feeds directly only to recommendation E and involves only the public sector. This coordination across sectors and recommendations is a key feature of the overall coordinated approach presented in this report.
Aside from the insight it provides into the system as a whole, the map is arranged to permit different audiences to quickly identify areas of individual interest. For example, the color coding of the strategies permits sectoral actors to identify those strategies in which they may be directly involved. Similarly, readers with an interest in a particular recommendation can quickly trace all of the strategies that feed directly or indirectly into that recommendation, as well as synergy with other recommendations (arrows between squares).
BASIS FOR PHYSICAL ACTIVITY AND DIETARY RECOMMENDATIONS
The committee looked to the 2008 Physical Activity Guidelines for Americans and the 2010 Dietary Guidelines for Americans to serve as the basis for defining adequate physical activity, healthy eating, and healthy foods (HHS/USDA, 2010; Physical Activity Guidelines Advisory Committee, 2008). In 2011, the release of MyPlate (http://www.choosemyplate.gov) provided additional guidance on healthy eating for the committee. These guidelines are based on the latest scientific evi-
dence and provide information on achieving adequate activity levels, choosing a nutritious diet, and maintaining a healthy weight to reduce the risk of many adverse health outcomes. The key physical activity guidelines and overarching concepts of the dietary guidelines are outlined in Box B-1.
The Physical Activity and Dietary Guidelines for Americans support the prevention of overweight and obesity through the overarching concept of maintaining calorie balance over time to achieve and sustain a healthy weight. To maintain calorie balance, the guidelines highlight that individuals should improve physical activity and eating behaviors, increase physical activity and reduce sedentary behavior, control total calorie intake, and maintain appropriate calorie balance over the life span. More specifically, the guidelines provide information on key physical activity goals over the life span, as well as foods to avoid and foods with which to replace them.
REPORTS INCLUDED IN THE COMMITTEE’S REVIEW (as of September 2010)
Institute of Medicine and National Research Council (by year)
Does the built environment influence physical activity? (TRB/IOM, 2005)
Preventing childhood obesity: Health in the balance (IOM, 2005)
Food marketing to children and youth: Threat or opportunity? (IOM, 2006a)
WIC food packages: Time for a change (IOM, 2006b)
Nutrition standards for foods in schools: Leading the way toward healthier youth (IOM, 2007a)
Progress in preventing childhood obesity: How do we measure up? (IOM, 2007b)
Adolescent health services: Missing opportunities (NRC/IOM, 2009)
Local government actions to prevent childhood obesity (IOM, 2009a)
Weight gain during pregnancy: Reexamining the guidelines (IOM, 2009b)
Bridging the evidence gap in obesity prevention: A framework to inform decision making (IOM, 2010a)
Review of the nutrition guidelines for the Child and Adult Care Food Program (IOM, 2011b)
School meals: Building blocks for healthy children (IOM, 2010b)
Early childhood obesity prevention policies (IOM, 2011a)
BOX B-1
Physical Activity and Dietary Guidelines for Americans
The Physical Activity and Dietary Guidelines for Americans promote energy balance and support prevention of obesity. The Physical Activity Guidelines are for Americans 6 years of age and older, and the Dietary Guidelines are for Americans 2 years of age and older. These guidelines provide a strong evidence base on how proper physical activity levels and a healthy diet help individuals maintain a healthy body weight and contribute to progress in obesity prevention. Key Physical Activity Guidelines and overarching concepts in the Dietary Guidelines include the following:
1. Focus on increasing physical activity levels.a
• Children and adolescents should participate in a minimum of 60 minutes of moderate-intensity physical activity each day.
• Adults and older adults should participate each week in a minimum of 150 minutes of moderate-intensity physical activity, 75 minutes of vigorous physical activity, or an equivalent combination of both.
• When older adults cannot engage in 150 minutes of moderate-intensity physical activity because of physical limitations, they should be as physically active as their abilities will allow.
Non-Academies Reports (by year)
Recommendations to increase physical activity in communities (Task Force on Community Preventive Services, 2002)
Public health strategies for preventing and controlling overweight and obesity in school and worksite settings: A report on recommendations of the Task Force on Community Preventive Services (Katz et al., 2005)
The Keystone Forum on away-from home foods: Opportunities for preventing weight gain and obesity (Keystone Forum, 2006)
2. Maintain calorie balance over time to achieve and sustain a healthy weight.b
• Increase physical activity and reduce sedentary behavior, improve physical activity and eating behaviors, control total calorie intake, and maintain appropriate calorie balance during each stage of life.
3. Focus on consuming nutrient-dense foods and beveragesb
• Establish a healthy eating pattern by reducing intake of sodium and calories from solid fats, added sugars, and refined grains and replacing them with nutrient-dense foods and beverages, including fruits and vegetables, whole grains, fat-free or low-fat milk or milk products, seafood, lean meats and poultry, eggs, beans and peas, and nuts and seeds.
Individuals can visit http://www.ChooseMyPlate.gov and http://www.cdc.gov/physicalactivity/everyone/guidelines for advice on how to follow these guidelines.
![]()
aPhysical Activity Guidelines for Americans (http://www.health.gov/paguidelines/).
bDietary Guidelines for Americans (http://www.health.gov/dietaryguidelines/).
Expert committee recommendations on the assessment, prevention and treatment of child and adolescent overweight and obesity (Childhood Obesity Action Network, 2007)
Recommendations for prevention of childhood obesity (Davis et al., 2007)
Promising strategies for creating healthy eating and active living environments (Lee et al., 2008a)
Strategies for enhancing the built environment to support healthy eating and active living environments (Lee et al., 2008b)
Physical Activity Guidelines for Americans (HHS, 2008)
Recommended community strategies and measurements to prevent obesity in the United States (Khan et al., 2009)
Action strategies toolkit: A guide for local and state leaders working to create healthy communities and prevent childhood obesity (RWJF, 2009)
Shaping a healthier generation: Successful state strategies to prevent childhood obesity (Mulheron and Vonasek, 2009)
Legislative task force on diabetes and obesity: Report to the California legislature (Greenwood et al., 2009)
F as in fat: How obesity threatens America’s future (Trust for America’s Health, 2010)
Solving the problem of childhood obesity within a generation: White House Task Force on Childhood Obesity report to the President (White House Task Force on Childhood Obesity, 2010)
National physical activity plan for the United States (National Physical Activity Plan, 2010)
Statement of policy, comprehensive obesity prevention (NACCHO, 2010)
The Surgeon General’s vision for a healthy and fit nation (HHS, 2010)
School-based obesity prevention strategies for state policymakers (CDC, date unknown)
REFERENCES
CDC (Centers for Disease Control and Prevention). Date unknown. School-based obesity prevention strategies for state policymakers. http://www.cdc.gov/healthyyouth/policy/pdf/obesity_prevention_strategies.pdf (accessed December 1, 2011).
Childhood Obesity Action Network. 2007. Expert committee recommendations on the assessment, prevention and treatment of child and adolescent overweight and obesity. Boston, MA: National Initiative for Children’s Healthcare Quality.
Davis, M. M., B. Gance-Cleveland, S. Hassink, R. Johnson, G. Paradis, and K. Resnicow. 2007. Recommendations for prevention of childhood obesity. Pediatrics 120(Suppl. 4):S229-S253.
Forrester, J. W. 1991. System dynamics and the lessons of 35 years. In The systemic basis of policy making in the 1990s, edited by K. B. De Greene. Cambridge, MA: MIT Press.
Greenwood, M. R. C., P. B. Crawford, and R. M. Ortiz. 2009. Legislative task force on diabetes and obesity: Report to the California legislature. Santa Clara, CA: Offices of Santa Clara County Supervisors.
HHS (U.S. Department of Health and Human Services). 2008. Physical activity guidelines for Americans. Washington, DC: HHS.
HHS. 2010. The Surgeon General’s vision for a healthy and fit nation. Rockville, MD: Office of the Surgeon General.
HHS/USDA (U.S. Department of Agriculture). 2010. Dietary guidelines for Americans. Washington, DC: U.S. Government Printing Office.
IOM (Institute of Medicine). 2005. Preventing childhood obesity: Health in the balance. Washington, DC: The National Academies Press.
IOM. 2006a. Food marketing to children and youth: Threat or opportunity? Edited by J. M. McGinnis, J. Gootman, and V. I. Kraak. Washington, DC: The National Academies Press.
IOM. 2006b. WIC food packages: Time for a change. Washington, DC: The National Academies Press.
IOM. 2007a. Nutrition standards for foods in schools: Leading the way toward healthier youth. Washington, DC: The National Academies Press.
IOM. 2007b. Progress in preventing childhood obesity: How do we measure up? Washington, DC: The National Academies Press.
IOM. 2009a. Local government actions to prevent childhood obesity. Washington, DC: The National Academies Press.
IOM. 2009b. Weight gain during pregnancy: Reexamining the guidelines. Washington, DC: The National Academies Press.
IOM. 2010a. Bridging the evidence gap in obesity prevention: A framework to inform decision making. Washington, DC: The National Academies Press.
IOM. 2010b. School meals: Building blocks for healthy children. Washington, DC: The National Academies Press.
IOM. 2011a. Early childhood obesity prevention policies. Washington, DC: The National Academies Press.
IOM. 2011b. Review of the nutrition guidelines for the Child and Adult Care Food Program. Washington, DC: The National Academies Press.
Katz, D. L., M. O’Connell, M. C. Yeh, H. Nawaz, V. Njike, L. M. Anderson, S. Cory, and W. Dietz. 2005. Public health strategies for preventing and controlling and obesity in school and worksite settings: A report on recommendations of the Task Force on Community Preventive Services. Morbidity and Mortality Weekly Report 54(RR-10):1-12.
Keystone Forum. 2006. The Keystone Forum on away-from home foods: Opportunities for preventing weight gain and obesity. Washington, DC: The Keystone Center.
Khan, L. K., K. Sobush, D. Keener, K. Goodman, A. Lowry, J. Kakietek, and S. Zaro. 2009. Recommended community strategies and measurements to prevent obesity in the United States. Morbidity and Mortality Weekly Report 58(RR-7):1-26.
Lee, V., L. Mikkelsen, J. Srikantharajah, and L. Cohen. 2008a. Promising strategies for creating healthy eating and active living environments. Oakland, CA: Prevention Institute, Healthy Eating Active Living Convergence Partnership, and PolicyLink.
Lee, V., L. Mikkelsen, J. Srikantharajah, and L. Cohen. 2008b. Strategies for enhancing the built environment to support healthy eating and active living environments. Oakland, CA: Prevention Institute, Healthy Eating Active Living Convergence Partnership, and PolicyLink.
Mulheron, J., and K. Vonasek. 2009. Shaping a healthier generation: Successful state strategies to prevent childhood obesity. Washington, DC: National Governors Association, Center for Best Practices.
NACCHO (National Association of County and City Health Officials). 2010. Statement of policy, comprehensive obesity prevention. Washington, DC: NACCHO.
National Physical Activity Plan. 2010. National physical activity plan for the United States. http://www.physicalactivityplan.org/index.php (accessed December 1, 2011).
NRC (National Research Council)/IOM. 2009. Adolescent health services: Missing opportunities. Washington, DC: The National Academies Press.
Physical Activity Guidelines Advisory Committee. 2008. Physical Activity Guidelines Advisory Committee report. Washington, DC: HHS.
RWJF (Robert Wood Johnson Foundation). 2009. Action strategies toolkit: A guide for local and state leaders working to create healthy communities and prevent childhood obesity. Princeton, NJ: RWJF.
Task Force on Community Preventive Services. 2002. Recommendations to increase physical activity in communities. American Journal of Preventive Medicine 22(4, Suppl. 1):67-72.
TRB (Transportation Research Board)/IOM. 2005. Does the built environment influence physical activity? Washington, DC: The National Academies Press.
Trust for America’s Health. 2010. F as in fat: How obesity threatens America’s future. Washington, DC: Trust for America’s Health.
White House Task Force on Childhood Obesity. 2010. Solving the problem of childhood obesity within a generation: White House Task Force on Childhood Obesity report to the President. Washington, DC: Executive Office of the President of the United States.




















