Goals, Targets, and Strategies for Change
Key Messages
• Now that obesity prevention efforts have some momentum, clarification of goals and targets for change going forward is essential.
• Goals for children, adolescents, and adults focus on prevention, with identification of specific behavioral targets and key outcomes for individuals and populations.
• An ecological model can be used to identify behavioral settings and sectors of influence in which and by which actions can be taken to improve environments for physical activity and healthful eating. Strategies for taking action are multifaceted and interrelated and include policy and legislative approaches, approaches that change organizational policies and practices and environments in communities and neighborhoods, health communication and social marketing approaches, and interventions in health care settings.
• Although there is not yet agreement on the set of specific strategies that will be effective, existing frameworks and successful models of social change can offer guidance on how to tackle the obesity epidemic utilizing a systems approach.
• Several major practical and policy considerations require close attention during the planning of strategies to accelerate obesity prevention, including the realities of the way Americans live, issues related to freedom of choice, food marketing to children and adolescents, potential adverse effects for
people who are obese, and effects on high-risk racial/ethnic minority and low-income populations.
• Measures with which to track progress are critical. Progress in achieving obesity prevention can be assessed in the short term by indicators of change in the environments that influence physical activity and eating.
It is clear from the preceding chapters that tremendous strides have been made in addressing the obesity epidemic, given the sheer amount of attention to the problem and the number and coherence of efforts to address the epidemic and bolster the scientific underpinnings and policy basis for taking action. Evidence of the stabilization of obesity prevalence in at least some demographic groups suggests that these deliberate initiatives to address the epidemic are on track, perhaps in concert with other, spontaneous countering forces. Given the scope and scale of what is needed and the inevitability of a time lag before true progress can be estimated, however, the developments to date create a unique opportunity to restate goals and refine targets and approaches in order to accelerate progress. As reviewed in this chapter, the goals themselves are clear with respect to the desired outcomes, as well as the types of behavioral changes that are relevant. There is not yet agreement on what specific set of strategies and actions will best curb and ultimately reverse the trends of increasing obesity prevalence. However, existing frameworks and successful models of social change can offer guidance on how to tackle the obesity epidemic and strongly indicate the need to take a systems approach, as described in Chapter 4.
The overall goal of obesity prevention is to create, through directed societal change, an environmental-behavioral synergy to foster the achievement and maintenance of healthy weight among individuals and in the population at large (IOM, 2005). This goal reflects a focus on prevention of obesity development, that is, primary prevention. Primary prevention emphasizes strategies that increase the
likelihood of shifting physical activity, eating, and weight management toward energy balance in the population as a whole, including those groups and individuals at high risk of becoming obese. In this report, primary prevention is viewed as relevant to the continuum of excess weight—prevention of the progression from normal weight to overweight, from overweight to obesity, and from mild or moderate to more severe obesity.
The logic of beginning obesity prevention during childhood is self-evident. At every life stage, from infancy onward, sustained excess weight and obesity increase the risk of longer-term obesity. In adults, obesity prevention targets those who enter adulthood with weight in the normal range, as well as those who may already be somewhat overweight or obese, to limit the severity of obesity and obesity-related health and social consequences. The need for effective preventive strategies is heightened by the seemingly intractable nature of established obesity, making the reduction of incidence—new cases of obesity—a priority. Effective treatments for established obesity continue to be elusive despite decades of research on treatment strategies, an active commercial weight loss industry, and a majority of U.S. adults trying to lose or maintain their weight at any given time. However, the need for prevention would persist even if effective treatments were available. In the absence of prevention, there would be a continual influx of people needing treatment (i.e., a majority of the population) such that the demand for treatment would exceed the supply.
Goals for Children and Adolescents
Goals for children and adolescents outlined in the Institute of Medicine (IOM) report Preventing Childhood Obesity: Health in the Balance (IOM, 2005) continue to inform actions at the national and community levels (see Box 3-1). For children and adolescents, obesity prevention means maintaining a healthy weight trajectory and preventing excess weight gain while growing, developing, and maturing (IOM, 2010). Goals include prevention of obesity and its adverse consequences during childhood, as well as longer-term prevention of obesity in adulthood, because children who are obese may remain so throughout life. Given the general increase in media attention to obesity as a result of the epidemic (see Chapter 2, Figures 2-7 and 2-8) and the potential for an increased focus on body size to foster inappropriate weight concern or dieting (Davison et al., 2003; Ikeda et al., 2006), an explicit goal has been added to those originally stated by the IOM (2005) to highlight the importance of maintaining a positive body image and avoiding excessive weight concern.
BOX 3-1
Goals of Obesity Prevention in Children and Adolescents
Individual Children and Adolescents
• A healthy weight trajectory, as defined by the Centers for Disease Control and Prevention body mass index (BMI) charts
• A healthful diet (quality and quantity)
• Appropriate amounts and types of physical activity
• Achievement of physical, psychosocial, and cognitive growth and developmental goals
• A healthy body image and the absence of potentially adverse weight concern or restrictive eating behaviors
Population of Children and Adolescents
• Reduction in the incidence of childhood and adolescent obesity
• Reduction in the prevalence of childhood and adolescent obesity
• Reduction of mean population BMI levels
• Improvement in the proportion of children and adolescents with dietary quality meeting the Dietary Guidelines for Americans
• Improvement in the proportion of children and adolescents meeting physical activity guidelines
• Achievement of physical, psychological, and cognitive growth and developmental goals
Examples of Possible Intermediate Indexes of Progress Toward Obesity Prevention in Children and Adolescents
• Increased number of children and adolescents who walk and bike to school safely
• Improved access to and affordability of fruits and vegetables for low-income populations
• Increased availability and use of community recreational facilities
• Increased play and physical activity opportunities
• Increased number of new industry products and advertising messages that promote energy balance at a healthy weight
• Increased availability and affordability of healthful foods and beverages at supermarkets, grocery stores, and farmers’ markets located within walking distance of the communities they serve
• Changes in institutional and environmental policies that promote energy balance
SOURCE: Adapted from IOM, 2005, 2007.
Goals for Adults
As noted in Chapter 2, the major human and societal consequences of obesity culminate during the adult years, and these consequences can be mitigated by stabilization of weight in the adult population. The payoff for intervening during adulthood is immediate in reducing both human and societal costs by limiting the development or exacerbation of obesity-related diseases during adulthood. There is a payoff as well in the direct and indirect effects on the familial context for the development of childhood obesity (Seidell et al., 2005).
Gradual weight gain during adulthood is typical and is commonly, although erroneously, viewed as a part of normal aging (Lewis et al., 2000; Williamson et al., 1990). A gradual weight gain of 1 or 2 pounds per year means a gain of 10 or 20 pounds in 10 years and twice that in a 20-year period. For example, adults recruited from four geographic areas in the United States for the longitudinal Coronary Artery Risk Development in Young Adults (CARDIA) study at ages 18 to 30 gained an estimated average of 1 to 2 pounds annually during the 10-year period from 1985-1986 to 1995-1996 (Lewis et al., 2000). This weight gain shifted many people from the healthy weight range into the overweight range, from the overweight range into the obese range, or from a moderate to an extreme level of obesity. As shown in Figure 3-1, this weight gain was associated with substantial increases in the prevalence of overweight and obesity (body mass index [BMI] of 25 or greater) in both blacks and whites and both men and women: 52 percent to 76 percent of adults in these race/sex subgroups were in the healthy weight range (BMI 18.5 to 24.9) at the start of this period, but only 28 percent to 58 percent were in this range 10 years later; the prevalence of extreme obesity (BMI of 40 or more) at least doubled in all subgroups (Lewis et al., 2000).
Goals of obesity prevention in adults are shown in Box 3-2. They are similar in concept to those for children and adolescents but focus on the weight trajectories and related behaviors associated with aging and, in women, reproduction. Weight levels of adults and of children and adolescents are interrelated in that parents and other adults are role models for children and adolescents. Moreover, maternal obesity may have direct effects on the risk of obesity in children and adolescents through gestational factors (IOM, 2009; Norman and Reynolds, 2011).
TARGETS FOR BEHAVIORAL AND ENVIRONMENTAL CHANGE
The available evidence points to a specific set of widely agreed-upon behavioral changes that are likely to promote energy balance. These behaviors are identified
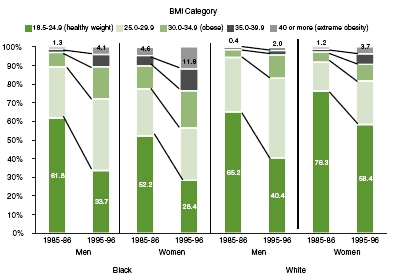
FIGURE 3-1 Ten-year changes in the distribution of body mass index in the Coronary Artery Risk Development in Young Adults (CARDIA) study.
SOURCE: Lewis et al., 2000.
as essential elements in obesity prevention for children, adolescents, and adults, as appropriate to life stage (Box 3-3). For physical activity, targeted behaviors relate to specified amounts of physical activity following guidelines for children, adolescents, and adults and decreases in television viewing—a major form of physical inactivity. For eating behaviors, the focus is on overall dietary quality as well as appropriate caloric consumption, achieved by increasing plant-based dietary components; reducing the consumption of sugar-sweetened beverages and of high-calorie, energy-dense foods; increasing breastfeeding and responsive child feeding; and ensuring the intake of nutrients needed to promote optimal linear growth.
In general terms, the types of environmental changes needed to motivate and support the indicated changes in individual behavior are directly related to the types of changes identified in the preceding chapters as having led to populationwide increases in weight gain and obesity and listed in Boxes 3-1 and 3-2 as
BOX 3-2
Goals of Obesity Prevention in Adults
Individual Adults
• Maintenance of weight during adult years, i.e., avoiding gradual incremental weight gain with increasing age
• Maintenance of waist size during adult years, i.e., avoiding gradual accumulation of fat around the abdomen
• Avoidance of weight regain after voluntary weight loss
• A high-quality diet with appropriate caloric intake (quality and quantity)
• Appropriate amounts and types of physical activity
• Appropriate prepregnancy weight, pregnancy weight gain, and subsequent postpartum weight loss
• A healthy body image and the absence of potentially adverse weight concern or restrictive eating behaviors
Population of Adults
• Reduction in the incidence of adult obesity
• Reduction in the prevalence of adult obesity
• Reduction of mean population body mass index (BMI) levels
• Improvement in the proportion of adults with dietary quality meeting the Dietary Guidelines for Americans
• Improvement in the proportion of adults meeting physical activity guidelines
• A population with weight and fitness levels conducive to a productive society
Examples of Possible Intermediate Indexes of Progress Toward Obesity Prevention in Adults
• Increased number of adults who routinely use active means of transportation, e.g., walking or cycling
• Improved access to and affordability of fruits and vegetables for low-income populations
• Increased availability, affordability, and use of community recreational facilities
• Increased opportunities to be physically active at work
• Increased number of new industry products and advertising messages that promote energy balance at a healthy weight
• Increased availability and affordability of healthful foods and beverages at supermarkets, grocery stores, and farmers’ markets located within walking distance of the communities they serve
• Community designs and social characteristics that encourage being physically active outdoors
• Changes in institutional and environmental policies that promote energy balance
SOURCES: IOM, 1995; USDA/HHS, 2010.
BOX 3-3
Target Individual Behaviors for Obesity Prevention
Activity-related
• Increase physical activity/promote an active lifestyle.
• Children and adolescents get at least 60 minutes of physical activity per day.
• Adults aim for 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity physical activity per week.
• Decrease television viewing.
Diet-related
• Increase the consumption of fruits and vegetables and legumes, whole grains, and nuts.
• Limit calories from added sugars, solid fats, and alcohol.
• Decrease the consumption of sugar-sweetened beverages/soft drinks.
• Increase breastfeeding initiation, duration, and exclusivity.
• Reduce the consumption of high-calorie, energy-dense foods.
• Parents accept their child’s ability to regulate energy intake instead of eating until the plate is empty.
• Ensure appropriate micronutrient intake to promote optimal linear growth.
SOURCE: IOM, 2010.
potential intermediate indicators of progress. Thus, the needed changes relate to options for physical activity, factors that predispose to sedentary behavior, the food supply, and food availability and promotion. Potential strategies for effecting such changes are the focus of the remainder of this chapter.
A COMPREHENSIVE AND INTEGRATED APPROACH TO PREVENTING AND ADDRESSING OBESITY
Identification of the behavioral and environmental variables that contribute to the populationwide obesity epidemic and how they influence and interact with each other is needed to determine which prevention efforts are the most promising. Both the 2005 IOM report and the follow-up report, Progress in Preventing Childhood Obesity: How Do We Measure Up? (IOM, 2007) use an ecological approach to identify leverage points for developing effective intervention strategies to promote energy balance, and specifically address individual factors, behavioral settings, sectors of society, and social norms and values that may constrain or reinforce regular physical activity and healthful eating as the accepted and encouraged standard. Using the model shown in Figure 3-2, pathways can be drawn to identify specific influences on the weight-related behaviors of individuals in demographically diverse population groups, within and among the levels shown. Each type of setting shown (top left) and each of the several sectors that can be focal points for intervention (at right) are complex, and these settings and sectors are interrelated. The different levels at which interventions may be undertaken demonstrate how, if taken together, a set of actions across levels might interrelate. Therefore, this figure illustrates the overall complexity of influences on obesity, and shows that preventive actions must be comprehensive and can vary according to the diversity and interrelationships that apply. Homes and families are often listed under “behavioral settings,” which would be appropriate. As explained in Chapter 1, however, the committee’s approach emphasizes changes in settings and sectors that can accelerate obesity prevention by improving physical activity options and healthful eating, as well as facilitators at both the family or household and individual levels, taking into account their interdependence.
The influence of obesity on the economy, productivity, and population fitness was highlighted in Chapter 2, emphasizing the importance of addressing the epidemic not only for governments but also for businesses and the private sector. The “sectors of influence” on obesity in Figure 3-2 have, therefore, been updated from prior versions to highlight the potential contributions of businesses other than those directly involved in the manufacturing of products related to physical
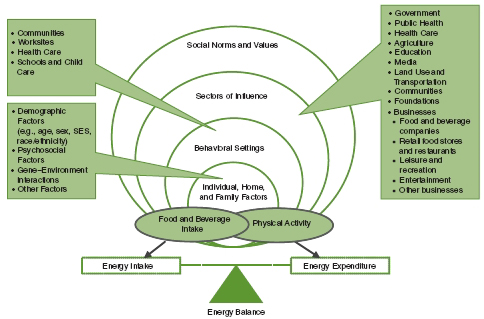
FIGURE 3-2 Various levels and sectors of influence on obesity in populations.
NOTE: SES = socioeconomic status.
SOURCE: Adapted from IOM, 2007.
activity and food. For example, businesses that provide catering or venues where the public eats—such as movie theaters, sporting event venues, and shopping malls—have a role to play in changing the availability of foods and norms about food consumption. Moreover, all employers, both public and private, increasingly are expected to foster work environments—including physical work settings, schedules, and health insurance coverage—that promote weight management and are conducive to good health for both employees and their families (Heinen and Darling, 2009). The Guide to Community Preventive Services, which represents the work of the Task Force on Community Preventive Services, recommends worksite programs for obesity control based on strong evidence of their effectiveness (Anderson et al., 2009). Results of a survey by Edelman (2011) indicate that the public expects businesses to contribute to health in a variety of ways in addition to providing health insurance coverage or worksite wellness programs, such as by educating people about the health risks of products or services, creating products and services that are conducive to good health, fostering a dialogue about public priorities related to health, and contributing funds or in-kind services to improve the health of the public. And the Partnership to Build a Healthier America, part of the First Lady’s Let’s Move campaign, works with food and beverage companies, as well as other companies, to generate meaningful sponsorship commitments that will increase physical activity and improve access to healthy, affordable foods (www.ahealthieramerica.org).
Thus, as emphasized throughout this report, obesity prevention in communities and populations requires social change. The strategies to be employed are similar to those applicable to other situations in which broad actions are needed to affect environments and the rules that apply to them. The Spectrum of Prevention, developed by Cohen and Swift (1999), is a framework for developing multifaceted approaches to address complex health problems and is commonly used in public health and health promotion. It identifies levels of increasing scope and emphasizes that effectiveness in addressing an issue requires integration across those levels: policy and legislative approaches; approaches involving changes in organizational policies, environments, and practices; approaches designed to foster changes in communities and neighborhoods; health communication and social marketing approaches; interventions in health care settings; and finally, multilevel, multisector approaches (IOM, 2010). The relevance of the Spectrum of Prevention as a typology for categorizing strategies relevant to obesity prevention is discussed in detail in the report Bridging the Evidence Gap in Obesity Prevention: A Framework to Inform Decision Making (IOM, 2010). Examples from that report are shown in Box 3-4.
BOX 3-4
Examples of Population-Based Obesity Prevention
Approaches
Policy and Legislative Approaches
Relevant approaches could include limiting the availability of sugar-sweetened beverages and high-calorie, energy-dense foods in certain settings (e.g., schools) or within programs (e.g., federal nutrition assistance programs); imposing taxes or price increases on sugar-sweetened beverages and high-calorie, energy-dense foods; or mandating a reduction in serving sizes for sugar-sweetened beverages and high-calorie, energy-dense foods.
Approaches Involving Changes in Organizational Policies, Environments, and Practices
Relevant programs or policies could include regulatory changes that affect an organization or voluntary changes that could be implemented by an organization itself (e.g., posting calorie content on menus; increasing the availability of fruits and vegetables in a worksite cafeteria; limiting the availability of sugar-sweetened beverages and high-calorie, energy-dense foods in a school).
As will become evident in Chapter 4, these examples help explain what is meant by population-based obesity prevention and are indicative of the types of actions— individual and combined—that often are recommended for obesity prevention.
A SUCCESSFUL MODEL OF COMPREHENSIVE CHANGE
To date, obesity prevention has not fully employed the complex thinking that is required to address the obesity epidemic. Applying the social change strategies described in this chapter to the community environment in order to encourage increased levels of physical activity, decreased sedentary behaviors, and healthful
Approaches Designed to Foster Changes in Communities and Neighborhoods
Strategies and actions could include advocating for zoning to limit fast-food establishments; facilitating the situating of supermarkets in underserved areas; increasing the availability of farmers’ markets; creating and supporting community gardens; supporting safe routes to school; creating and maintaining a walking school bus; increasing the number of bike paths and parks; and enhancing walking infrastructure.
Health Communication and Social Marketing Approaches
Strategies and actions to prevent obesity can be enhanced through communication, marketing, and promotion and new technologies.
Interventions in Health Care Settings
Interventions could include annual screening for obesity, counseling about physical activity and diet, and expanded insurance coverage for behavioral and nutritional counseling.
SOURCE: Based on the “Spectrum of Prevention” in IOM, 2010.
eating is emerging as a practical way to address obesity on a large scale (de Silva-Sanigorski and Economos, 2010). Community-based obesity interventions (targeting policy and environmental changes) require an understanding of how social systems operate, how change occurs within and among systems, and how community changes influence individual behavior and health. Box 3-5 describes a working framework for such a whole-system approach to public health problems.
Shape Up Somerville (SUS): Eat Smart, Play Hard, conducted in Somerville, Massachusetts, illustrates the potential of a whole-system approach. Informed by previous social change models, this initiative was one of the first community-based
BOX 3-5
Features of a Whole-System Approach to Public Health Problems
1. Explicit recognition of the public health problem(s) as a system: recognition of interacting and evolving elements; self-regulation; and synergy and emergent properties associated with complex adaptive systems.
2. Capacity building: capacity building within communities and organizations stated as an explicit goal. This could take the form of increasing understanding about obesity as a problem in the community and in potential partner organizations, training for those in positions addressing obesity, more dedicated staff addressing obesity, etc.
3. Local creativity: local creativity and/or innovation were encouraged to address obesity prevention. This might be evidenced by mechanisms for local people to design locally relevant activities and solutions, while rigid requirements for activities imposed from outside the area would suggest that this was not present.
4. Relationships: clear methods were used to develop and maintain working relationships, within and between organizations.
5. Engagement: clear methods were used for engaging community members in program development and delivery. This engagement should be with diverse people, organizations and sectors.
6. Communication: clear methods were used for enhancing communication between actors and organizations within the system. This would not mean communication of health promoting messages to the people living in a community as part of a specific intervention.
efforts designed to change the environment to prevent obesity in early elementary school-aged children (Economos et al., 2009). The SUS intervention, as described by de Silva-Sangorski and Economos (2010, p. 59), is:
focused on creating multilevel environmental change to support behavioral action and its maintenance and to prevent excessive weight gain among early elementary school-aged children through community participation. For example, specific changes within
7. Focus on the embeddedness of action and policies for obesity prevention in organizations and systems. Examples of this might include the visibility of obesity as an explicit policy goal or concern for non-health organizations, ongoing strategic commitment to obesity as a local concern, etc.
8. Focus on the robustness and sustainability of the system to tackle obesity. Ongoing strategies for resourcing existing and new projects and staff might be an indicator of this feature.
9. Facilitative leadership. This is leadership which is not necessarily located at any particular level or organization and is likely to encourage bottom up solutions and activities while providing strong strategic support where needed as well as appropriate resourcing.
10. Well articulated methods for ongoing monitoring and evaluation of activities, the results of which feed back into the system and drive change to enhance appropriateness and effectiveness. This relates to notions of the adaptability and learning capabilities of the systems/networks/partnerships established.
SOURCE: Quoted from NICE, 2011, pp. 14-15.
the before-, during-, and after-school environments provided a variety of increased opportunities for physical activity. The availability of less energy-dense foods, with an emphasis on fruits, vegetables, whole grains, and low-fat dairy products, was increased; foods high in fat and sugar were discouraged. Additional changes within the home and the community reinforced opportunities for increased physical activity and improved access to healthier food. To achieve this level of change, many groups and individuals within the community (including children, parents, teachers, school food service providers, city departments, policy makers, health care providers, before- and after-school programs, restaurants, and the media) were engaged in the intervention.
These changes were successful in bringing the community’s overall energy equation into balance and were designed to be replicated as a cost-effective community-based action plan (de Silva-Sanigorski and Economos, 2010; Economos and Irish-Hauser, 2007).
Other large-scale, multilevel, community-based childhood obesity prevention initiatives in the United States, including Healthy Eating Active Communities1 and Healthy Eating Active Living,2 offer additional lessons for conducting this type of initiative through their resources and publications. These initiatives, begun in 2005-2006 by the California Endowment and Kaiser Permanente, respectively, have funded communities across the state of California (and now spreading across the country) to develop and implement a broad set of interventions focused on improving the physical activity and food environments for children in schools; health care facilities; after-school programs; neighborhoods; marketing and advertising venues; and other places where families live, learn, work, and play.
Similarly, acknowledgment of the responsibility to address obesity in the private and public sectors has been demonstrated globally. As reviewed in 2007, a number of countries and regions have been developing and implementing strategic plans to promote physical activity and healthful eating and to prevent obesity (IOM, 2007). Many of these plans and initiatives continue to evolve, and include the use of multiple types of actions; the development of partnerships, including private and public agreements; and the use of multiple settings, various sectors, and multiple levels of government (WHO, 2007).
An example is EPODE (Together Let’s Prevent Childhood Obesity), a multistakeholder prevention program that focuses on facilitating the adoption of healthier lifestyles (Borys et al., 2011). Programs developed using the EPODE framework focus on long-term environmental and behavior change without stigmatizing culture, food habits, or overweight and obesity. EPODE began in France in 2003 and has since expanded to cover millions of people in Australia, Belgium, Canada, France, Greece, and Spain.
In 2008, the United Kingdom released a cross-government strategy titled Healthy Weight, Healthy Lives, designed to support people in maintaining a healthy weight. The marketing component of the United Kingdom’s government response (called Change4Life3), begun in 2009, aims to change behaviors that lead to childhood obesity through a multistakeholder campaign. In 2010, the United
![]()
1 Healthy Eating Active Communities. http://www.partnershipph.org/projects/heac (accessed November 14, 2011).
2 Healthy Eating Active Living. http://www.convergencepartnership.org (accessed November 14, 2011).
3 Change4Life. http://www.nhs.uk/Change4Life/Pages/change-for4ife.aspx (accessed January 3, 2012).
Kingdom released a broader public health strategy entitled Healthy Lives, Healthy People, which sets out the national government’s “long-term vision” for the future of public health in England: to provide support to and for local governments as leaders and those responsible for their communities’ wellness.
As a final example, in 2008 Switzerland introduced its National Programme on Diet and Physical Activity.4 This program “defines long-term goals and national priorities and provides a basis for collaboration between the various institutions and organizations working in the field.”
PRACTICAL AND POLICY CONSIDERATIONS
This section highlights what the committee views as major practical and policy considerations requiring close attention during the planning of strategies to accelerate obesity prevention. Experience to date provides many examples of issues that can impede progress or lead to unintended adverse consequences. The committee’s vision takes into account the need for strategies to be realistic, as well as consistent with fundamental values and principles. At the same time, however, having a diversity of values and priorities among them is itself a principle of U.S. society. Potentially competing values and principles must be reconciled, for example, in considering protections needed for individuals versus the community at large or for the public versus the private sector. Vigilance regarding unintended adverse effects of changes undertaken to address the obesity epidemic also is needed.
Raising awareness of obesity, drawing attention to the associated economic and health care costs, passing new laws or regulations, and implementing community action strategies to mobilize change all require resources, political will, and public support from those whose lives or livelihoods could be affected. Support for changes in living environments or the policies that govern them will vary according to the perception that those changes are needed and sensible, as well as what may be sacrificed if the changes are implemented. The potential for variation in political and public support is illustrated by results of an analysis of variables associated with the passage of state laws designed to reduce obesity prevalence between 2003 and 2005, a period when the number of such laws increased (Cawley and Liu, 2008). The probability of states enacting bills related to physical education, school nutrition, BMI screening, or health education differed according to adult obesity prevalence, the difference between self-reported and ideal weights
![]()
4 National Programme on Diet and Physical Activity. http://www.bag.admin.ch/themen/ernaehrung_bewegung/05141/05142/index.html?lang=en (accessed January 3, 2012).
of adults in the state, the percentage of adults with a bachelor’s degree or higher, income level, the percentage of the population living below the poverty line, the percentage employed in agricultural occupations, the percentage of blacks in the population, and the political party of the governor. The prevailing economic environment also has an impact. As this report goes to press, the United States continues to wrestle with a major economic crisis that influences the availability of public resources at the national, state, and local levels, as well as private and personal resources (Brown and Lundblad, 2009).
Realities of the Way Americans Live
Perhaps the most prominent and overarching of the practical realities associated with preventing obesity is that Americans are now accustomed to the very societal influences that predispose the average person to gain excess weight. “Obesogenic” environmental forces have been observed not only in the United States but also worldwide, driven by powerful economic and social forces that cannot easily be redirected and for which changes have interconnected and far-reaching effects that must be taken into account (Swinburn et al., 2011; WHO, 2000). Modern, technologically sophisticated lifestyles characterized by dependence on cars; jobs that require limited physical effort; labor-saving devices at home; sedentary entertainment; and the widespread availability of good-tasting, high-calorie foods and beverages are the cultural norm. Americans are steeped in a consumer culture in which many of the rewards of daily life, including food-related pleasures, are increasingly shaped by marketers and in which electronic media are a major source of information, social communication, and recreation for many people (Rideout et al., 2010).
If Americans are in equilibrium with or aspiring to obesity-promoting, modern lifestyles, what—short of a major shock—will it take to motivate and effect changes in the social fabric of the level and scope needed to create routine environments that foster healthy weight? Policy makers and other influential people must be convinced that the adverse health and societal consequences of current lifestyles outweigh the positives. They must then identify and support strategies and actions that will be acceptable with respect to gains and losses. They must resist strong counterpressures from those who see themselves as socially or economically disadvantaged by the changes that are contemplated. Public- and private-sector support and advocacy may be needed for policy adoption. Or, when policies are instituted without the need for public consultation or are not contro-
versial, public- and private-sector support may be critical for implementation and eventual uptake and adoption.
The following example of the types of trade-offs involved is useful in visualizing what might have to happen to effect a major change in the proportion of the population engaging in active transportation such as walking or cycling. Using one’s car less is inconvenient but may be acceptable if the cost savings (e.g., low public transportation fares and avoidance of fuel costs and parking fees), convenience (e.g., public transportation routes to necessary or popular destinations), social and aesthetic value (e.g., inviting destinations and pleasant scenery along the way), and safety (e.g., sidewalks along the entire route) of using alternative modes of transportation can be made attractive. Disincentives can also be used to equalize options (e.g., raising parking fees or tolls to discourage bringing cars into urban areas) but would presumably generate much more public opposition than incentive-oriented strategies. Trade-offs also must be balanced to avoid opposition from the automobile industry—including companies that produce and sell cars and the people and communities for whom this industry is a key part of the economy. At the level of social norms and consumer culture, ways to replace the use of cars as a status symbol also may be needed.
Environmental and Policy-Level Intervention Versus Freedom of Choice
Concern that intervening to change environments will inappropriately and unfairly constrain individual freedom of choice is a continuing part of the debate about how to address the obesity epidemic (Kersh, 2009). Such concerns often relate to public policy (i.e., government interventions related to schools and public places), but they may also apply to interventions to change policies or environments at places of employment within private-sector worksites. The importance of protecting individual freedoms has a level of political and public support in the United States that may be unparalleled in other democratic societies. Those who raise concern about the potential loss of individual freedom assert that what people eat (or what their children eat) or whether people walk or use their car or drive their children to school are personal choices, and that government should not intervene to limit these choices. Closely related to this perspective is the argument that obesity results primarily from a failure of personal responsibility to control food intake or, in the case of parents, of the responsibility to feed their children appropriately. This perspective may be waning somewhat given that such “failures”—if signified by overweight and obesity—now affect a majority of
adults in the U.S. population and a substantial proportion of the child and adolescent population, but it may still be perpetuated by prevailing biases and negative stereotypes about obese people (Andreyeva et al., 2008; Washington, 2011). Several, related counterarguments to the concern that environmental interventions are inappropriate or unjustified are reviewed below. People differ in the extent to which they are convinced by these counterarguments.
The Context for the Exercise of Free Choice Must Be Improved
Evidence suggests that the current range of choices related to physical activity and food intake is limited and biased toward the unhealthy end of the continuum such that policies are needed to improve the environment for free choice. Commonly cited examples are communities where streets and roads are designed in ways that do not permit pedestrian access, and food outlets or vending machines where all of the choices are relatively unhealthy (Rahman et al., 2011; Sallis and Glanz, 2006). In addition, high-calorie, low-nutrient packaged foods or certain items at fast-food restaurants may be the cheapest ways to obtain calories. Food prices may, therefore, indirectly constrain the range of choices if costs matter. The cost of healthier foods may be higher in terms of price, time needed to shop for healthier foods that are attractive and affordable, time taken away from other pursuits to spend in preparing food, or all of these.
Many Apparent Choices Reflect Habitual or Natural Responses to Environmental Cues
Theory and empirical data from the field of behavioral economics suggest that the majority of physical activity and eating behaviors are routine rather than choices made after deliberation about a set of options (Just and Payne, 2009; Just et al., 2008). In such cases, changing the environmental cues or “default choices” to routinely prompt healthier choices could cause favorable (from a public health perspective) shifts in population behavior (Angell et al., 2009; Frieden et al., 2010).
Individuals’ Innate Regulatory Systems Are Overwhelmed
An evolutionary argument is related to the observation that human physiological responses to foods containing fat and sugar still are geared primarily to avoiding hunger and conserving energy, with no innate mechanisms to ensure maintenance of energy balance when such foods are available in high quantities and the demand or opportunity for caloric expenditure is low (WHO, 2000). In
this scenario, even conscious efforts to prevent excess weight gain are likely to be ineffective.
Government Has a Responsibility to Protect Health
Ethical principles, as well as numerous precedents, can be cited to support the concept that government has a responsibility to protect the health of the public and therefore the authority to intervene in relevant societal sectors and processes (Economos et al., 2001; IOM, 2005, Appendix A; Kersh and Morone, 2002; Kersh et al., 2011). Precedents include laws that require the use of seat belts in cars or helmets while cycling, restrict the use of certain drugs, make it illegal to drive a vehicle while under the influence of alcohol, or restrict tobacco smoking in public venues, as well as laws supporting water fluoridation or fortification of foods with folic acid. In these cases, governments have determined either that it is essential to ensure that the interventions in question reach the general public without requiring an active choice on the part of each individual (e.g., water and food), or that rules about personal behavior are needed to protect individuals (seat belts or helmets or drugs) or the society at large (driving under the influence, secondhand smoke). Ethical arguments are particularly salient with respect to the government’s responsibility to protect children and adolescents. Well-established precedents include child labor laws and policies that restrict the promotion and sale of tobacco and alcohol to children and adolescents (FDA/HHS, 2010; Miller, 2010; Toomey and Wagenaar, 1999).
Public schools, in particular, have an obligation to question and refute policies that do not benefit their students and their communities and a corresponding responsibility to protect students, for whom school attendance is mandated, from harm (Crawford et al., 2011). Children and adolescents spend up to half their waking hours in school, where they may consume as much as one-third to one-half of their daily calories. Therefore, the school food environment is a logical focus for efforts to encourage healthy dietary behaviors. Today, school food service includes two competing arms—the federally regulated reimbursable National School Lunch and School Breakfast programs and the competitive food and beverage marketplace, which has expanded substantially during recent decades. Competitive foods and beverages are those sold throughout schools in vending machines, school stores, and snack bars and at fundraisers. They are typically of low nutritional quality, such as sweetened beverages, chips and other salty snacks, and sweets such as cookies and pastries (Crawford et al., 2011; Fox et al., 2009; Wechsler et al., 2001). Efforts to encourage children to eat nutritionally sound
school meals are undermined by the provision of snacks and beverages that compete with healthier options (Crawford et al., 2011).
Students at schools providing nutritious food offerings still have access to a variety of food choices, along with the option of bringing foods from home. Their freedom of choice is not unjustly breached by limiting the availability of obesogenic foods on campus (Crawford et al., 2011).
Regulation of Food Marketing to Children and Adolescents
Aggressive marketing of high-calorie foods to children and adolescents has been identified as one of the major contributors to childhood obesity (IOM, 2006). The way in which products marketed as oriented to children and adolescents are made available and promoted has been shown to influence children and adolescents’ food preferences and selections (IOM, 2006; WHO, 2010). Marketing of non-nutritious foods and beverages on public school grounds (e.g., in classroom materials, on sporting equipment, by signage), a common school fundraising technique in recent decades, undermines attempts to provide nutrition education in the classroom. Frequent exposure to this marketing in schools in low-income areas where children and adolescents are at greater nutritional risk is at odds with fairness and social justice (Crawford et al., 2011).
How to protect children and adolescents from potential adverse effects of such marketing is a major public health policy issue, argued primarily on ethical grounds and, in schools, on economic grounds. Statutory regulation of food marketing to children and adolescents has been proposed, on the grounds that children and adolescents are a vulnerable population in this respect because of their inability to understand the commercial intent of advertising (Hawkes, 2007; Pomeranz, 2010; Swinburn et al., 2008). Attempts to pass laws to this effect have not been successful, however, based on a ruling in 1978 that to restrict advertising would violate the First Amendment of the U.S. Constitution, which guarantees the right to free speech and extends this protection to commercial entities. A prior IOM report on this issue recommends that the food industry voluntarily restrict advertising of unhealthy foods and beverages to children and adolescents (IOM, 2006). A recent evaluation concludes that food and beverage companies have made moderate progress in this respect, with only limited progress being seen in other subsectors of the food industry (Kraak et al., 2011). Public health experts continue to conclude that statutory regulation will be needed to address the problem. They base this conclusion on comparisons of what has been accomplished through voluntary measures and what is perceived as being needed, as
well as on increasing changes in advertising practices designed to circumvent the ability of children and adolescents to understand or defend against them (Goren et al., 2010; Harris et al., 2009). Current public- and private-sector efforts to standardize and strengthen ways of classifying foods as appropriate or inappropriate to advertise to children and adolescents could facilitate progress in regulating food marketing to children and adolescents through either voluntary or statutory means.
An important aspect of this challenge is the nature of the food industry—that is, the desirability of having a positive, cooperative relationship with the system that provides our food. Here the difference between the food and tobacco industries is paramount: tobacco products are intrinsically harmful and expendable whereas food is not, although the harm to health from current dietary patterns and excesses is clear. In the framework of Kersh and Morone (2002) regarding the type of climate that is sometimes necessary to generate public action on personal behavior, the tobacco industry can readily be demonized, but doing so is more difficult and less desirable with respect to the food industry. Nevertheless, there are noteworthy similarities in the public policy strategies proposed to change the behavior of the food industry and in the countering strategies used by the industry (Brownell and Warner, 2009), suggesting that strategies to address obesity cannot be naïve.
Effects on Children, Adolescents, and Adults Who Are Obese
Efforts to address the obesity epidemic must consider the potential impact of actions taken on those children, adolescents, and adults who are already obese. Environmental and policy changes that will make it easier to achieve and maintain energy balance should have positive effects across the continuum of body weight. However, the process needed to achieve these changes may inadvertently worsen the day-to-day lives of obese children, adolescents, and adults. The pervasive negative societal attitudes about obese people have been well documented, held by the general public; by employers; by schoolteachers and other professionals, including health professionals; and by children, adolescents, and adults who are obese (Andreyeva et al., 2008; Washington, 2011). Greater awareness of obesity may increase these negative perceptions and the bias and discrimination experienced by obese people. Emphasizing the costs of treating obesity may cause a backlash in which obese people are blamed for rising health care costs, including public expenditures for Medicaid and Medicare. Similarly, emphasizing effects of having a heavier population on infrastructure and other aspects of the economy may increase negative attitudes about obese people. Another potential adverse conse-
quence, of particular importance for children and adolescents, is the inadvertent generation or aggravation of poor body image, low self-esteem, preoccupation with dieting, or inappropriate weight concern, which can impair healthy growth and physical and psychosocial development (Griffiths et al., 2010).
Kersh and Morone (2002) point out the troubling reality that movements toward government action on personal behaviors sometimes take an oversimplified view that begins with public disapproval or demonization of the affected population—e.g., alcoholics, drug users—as weak or irresponsible. Given the prevailing attitudes about obesity and the fact that it is more prevalent in low-income and minority communities, the same effect could occur in the case of the obesity epidemic. Policies and practices to address obesity must take this potential for harm into account and incorporate appropriate safeguards, including the institution of measures to track such outcomes. The case for addressing the obesity epidemic cannot be made at the expense of obese people. Ethical arguments can be and have been made against measures that penalize obese people. For example, when airlines began requiring passengers who were unable to fit safely into one seat to pay full price for a second seat, many major airlines were sued for discrimination. The Canadian Supreme Court formally prohibited airlines from charging obese passengers for additional seats. Despite the opposition, however, some airlines have kept such policies in place.
Careful consideration of the terminology used when discussing the topic and images used to illustrate obesity is warranted to avoid reinforcing negative stereotypes. In addition, making an effective case for universal interventions—that is, environmental and policy-level changes that do not rely on screening and identification of children, adolescents, or adults who are at high risk of obesity or are already obese (IOM, 1995)—will help mitigate potential adverse effects on individuals.
Effects on Racial/Ethnic Minority and Low-Income Populations
The potential for negative stereotyping and social disapproval also applies at the group level. Similar to the considerations for individuals, this means that drawing attention to the high prevalence of obesity in racial/ethnic minority or low-income populations, as in Chapter 1 of this report, must be done not only carefully with respect to terminology and imagery but also accurately with respect to evidence about what is driving the higher obesity rates in these groups. Specifically, a coherent body of evidence implicates relatively greater exposure to the types of environmental contributors that predispose to low levels of physical
activity and excess energy intake in higher obesity rates among racial/ethnic minority and low-income populations (Kumanyika et al., 2008). For example, options for safe and affordable leisure-time physical activity are generally less common in racial/ethnic minority and low-income communities (Gordon-Larsen et al., 2006; Powell et al., 2006; Taylor et al., 2006). Likewise, food availability and promotion are less favorable to healthy eating patterns in such communities (e.g., fewer supermarkets selling a greater variety of foods; more fast-food restaurants; and more advertising of fast food and of high-calorie foods and beverages generally) (Grier and Kumanyika, 2008; Kumanyika and Grier, 2006; Taylor et al., 2006; Yancey et al., 2009). Black and Latino children and adolescents are particularly targeted by marketers of sugar-sweetened beverages and fast food, and their vulnerability to such advertising may be increased by their developmental characteristics, limitations on their ability to recognize when advertising is targeting them, and certain techniques used in multicultural marketing (Grier, 2009; Grier and Kumanyika, 2010; Powell et al., 2010; Tharp, 2001). It is unclear whether there are systematic neighborhood differences in the cost of healthy foods in racial/ethnic minority or low-income communities compared with other communities (Grier and Kumanyika, 2008; Krukowski et al., 2010). However, evidence indicates that the lowest-cost foods may be the least healthy (Drewnowski, 2009). Thus, households with limited resources may buy less healthy foods to stretch their dollars. It is worth noting that among immigrant populations, the prevalence of obesity tends to increase with duration of residence in the United States (Oza-Frank and Cunningham, 2010), a fact that also strongly implicates environmental factors in excess weight gain.
Sociocultural influences are part of the environment affecting physical activity and eating habits, and interact with other aspects of the environment (Swinburn et al., 1999). Characteristics of physical activity or food marketing environments and the high prevalence of obesity itself may influence social norms about physical activity and healthy eating, making higher weight, consumption of high-calorie foods and beverages, and sedentary behavior seem normal and appropriate. Body image norms that associate thinness with ill health and larger body sizes with good health and robustness may decrease recognition of clinically significant obesity and undercut motivation for weight control, particularly if large body size is normative in the community (Brown and Konner, 1987; Diaz et al., 2007; Kumanyika, 2008; Liburd et al., 1999). Ethnically targeted marketing, which incorporates cultural preferences, imagery, and traditions and relationship building with the targeted communities (Tharp, 2001), may reinforce cultural attitudes
and preferences that favor the consumption of high-fat or high-sugar foods if these are the types of foods marketed. Some cultural preferences are based on foods that may at one time have been difficult to obtain but may now be overabundant in racial/ethnic minority communities (Kumanyika, 2006, 2008). With respect to low-income or food-insecure populations, retail food promotions such as two-for-one deals, 99 cent menus, or large portion sizes, which are for relatively less healthful foods, may hold appeal (Power, 2005). Also, foods that are promoted as normative and desirable for the general population may be attractive to consumers in low-income populations as symbols of belonging or participating in mainstream lifestyles (Power, 2005).
TRACKING PROGRESS IN THE CHANGE PROCESS
Examples of outcomes of interest for tracking progress in the process of change include (1) the quality, scope, reach, and intensity of effects of obesity prevention policies and programs, to answer the questions of what is being done and whether enough of the appropriate types of interventions are occurring to expect success and (2) improvements in intermediate measures of progress toward goals, such as the indicators listed in Boxes 3-1 and 3-2. Assessments should include measures relevant to reaching high-risk populations. Ideally, assessments of progress through interim measures would be traceable to particular intervention approaches and also to obesity outcomes.
The committee that produced Progress in Preventing Childhood Obesity: How Do We Measure Up? (IOM, 2007) concluded that the infrastructure for assessing progress was severely underdeveloped and inadequately conceptualized. That report includes specific guidance on needed approaches and provides an evaluation framework to facilitate adoption of these approaches. Several advances have since been made in the development of concepts and tools for assessing the success of obesity prevention efforts. These include the aforementioned IOM report on a framework to inform decision making on obesity prevention (IOM, 2010), several ongoing efforts to compile evidence on promising programs (Appendix B in IOM, 2010), recommendations for improving the likelihood that ongoing policies and programs can be well evaluated (Leviton et al., 2010), and the development of a detailed framework and process for assessing the strength of evidence for various policy and environmental change strategies undertaken to prevent childhood obesity (Brennan et al., 2011). With respect to the ability to track progress on interim environmental and policy changes and behavioral trends, the National Collaborative on Childhood Obesity Research (NCCOR [http://www.nccor.org/css]) has developed publicly
available, interactive online databases to facilitate the identification of relevant resources—a catalogue of surveillance systems with data related to childhood obesity prevention and a registry of research measures for assessing physical activity and dietary intake (http://www.nccor.org/projects_registry_of_measures.html).
Although the obesity epidemic in the United States has been instrumental in bringing worldwide attention to the problem—as noted in Chapter 1 and illustrated by Figures 2-7 and 2-8 in Chapter 2, showing the increases in global as well as U.S. media attention to the problem—the epidemic extends across the globe. Extensive analyses and strategizing on how to approach the epidemic have taken and continue to take place in many countries, particularly in light of the implications of obesity for rising rates of cardiovascular diseases, diabetes, and other noncommunicable diseases globally (OECD, 2010; Swinburn et al., 2011; WHO, 2011). Among the most comprehensive efforts to understand the obesity epidemic, identify effective interventions, and formulate a national action plan was carried out by the Foresight Group in the United Kingdom (Foresight, 2007), which identified a broad range of factors that influence obesity and relationships among key factors in an effort to develop the most effective future responses to obesity for that country.
The consensus among stakeholders engaged in trying to address the obesity problem is that meaningful change on a societal level is needed if individuals’ attempts to change their physical activity and eating behaviors are to be effective (Foresight, 2007; White House Task Force on Childhood Obesity, 2010; WHO, 2000). The needed societal changes must be achieved through a public health approach that focuses on policy change and interventions in the environments in which people live, learn, work, and play. Complex realities associated with the obesity epidemic include practical and policy considerations, some of which may impede progress or lead to unintended adverse consequences that must be addressed during the design, implementation, and evaluation of measures to accelerate obesity prevention. These considerations include the nature of modern lifestyles, uncertainty or ambivalence about whether or how governments or other decision makers should use policy strategies to shift population physical activity and eating behaviors, the tensions associated with attempts to regulate food marketing to children and adolescents, and the potential adverse effects of obesity prevention efforts on individuals and population subgroups that are most affected by obesity.
The relevant causal pathways, settings, and sectors for intervention in other high-income countries (e.g., Australia, Canada, Europe, and New Zealand) bear many similarities to those in the United States. Analyses and experiences from these countries—for example, with respect to taxation; regulation of food advertising; and school, health care, or whole-community interventions—or modeling of cost-effectiveness may offer rich opportunities to inform U.S. strategies. The committee recognized the potential value of learning from this broader experience. However, experiences in other countries underscore the importance of tailoring and adapting strategies to policy mechanisms, environmental characteristics, health care systems and other institutional infrastructures, and sociocultural norms and values that apply nationally, regionally, and locally.
Anderson, L. M., T. A. Quinn, K. Glanz, G. Ramirez, L. C. Kahwati, D. B. Johnson, L. R. Buchanan, W. R. Archer, S. Chattopadhyay, G. P. Kalra, and D. L. Katz. 2009. The effectiveness of worksite nutrition and physical activity interventions for controlling employee overweight and obesity: A systematic review. American Journal of Preventive Medicine 37(4):340-357.
Andreyeva, T., R. M. Puhl, and K. D. Brownell. 2008. Changes in perceived weight discrimination among Americans, 1995-1996 through 2004-2006. Obesity (Silver Spring) 16(5):1129-1134.
Angell, S. Y., L. D. Silver, G. P. Goldstein, C. M. Johnson, D. R. Deitcher, T. R. Frieden, and M. T. Bassett. 2009. Cholesterol control beyond the clinic: New York City’s trans fat restriction. Annals of Internal Medicine 151(2):129-134.
Borys, J. M., Y. Le Bodo, S. A. Jebb, J. C. Seidell, C. Summerbell, D. Richard, S. De Henauw, L. A. Moreno, M. Romon, T. L. Visscher, S. Raffin, and B. Swinburn. 2011. EPODE approach for childhood obesity prevention: Methods, progress and international development. Obesity Reviews. Epub ahead of print.
Brennan, L., S. Castro, R. C. Brownson, J. Claus, and C. T. Orleans. 2011. Accelerating evidence reviews and broadening evidence standards to identify effective, promising, and emerging policy and environmental strategies for prevention of childhood obesity. Annual Review of Public Health 32:199-223.
Brown, G. W., and C. Lundblad. 2009. The U.S. economic crisis: Root causes and the road to recovery: Return to prosperity requires reversal of excessive consumption, low savings trends. http://www.journalofaccountancy.com/Issues/2009/Oct/20091781.htm (accessed November 9, 2011).
Brown, P. J., and M. Konner. 1987. An anthropological perspective on obesity. Annals of the New York Academy of Sciences 499:29-46.
Brownell, K. D., and K. E. Warner. 2009. The perils of ignoring history: Big tobacco played dirty and millions died. How similar is big food? Milbank Quarterly 87(1):259-294.
Cawley, J., and F. Liu. 2008. Correlates of state legislative action to prevent childhood obesity. Obesity (Silver Spring) 16(1):162-167.
Cohen, L., and S. Swift. 1999. The spectrum of prevention: Developing a comprehensive approach to injury prevention. Injury Prevention 5(3):203-207.
Crawford, P. B., W. Gosliner, and H. Kayman. 2011. The ethical basis for promoting nutritional health in public schools in the United States. Preventing Chronic Disease 8(5):A98.
Davison, K. K., C. N. Markey, and L. L. Birch. 2003. A longitudinal examination of patterns in girls’ weight concerns and body dissatisfaction from ages 5 to 9 years. International Journal of Eating Disorders 33(3):320-332.
de Silva-Sanigorski, A. M., and C. Economos. 2010. Evidence of multi-setting approaches for obesity prevention: Translation to best practice. In Preventing childhood obesity: Evidence, policy, and practice, edited by E. Waters, J. C. Seidell, B. A. Swinburn, and R. Uauy. Hoboken, NJ: Wiley-Blackwell. Pp. 57-63.
Diaz, V. A., A. G. Mainous, 3rd, and C. Pope. 2007. Cultural conflicts in the weight loss experience of overweight Latinos. International Journal of Obesity (London) 31(2):328-333.
Drewnowski, A. 2009. Obesity, diets, and social inequalities. Nutrition Reviews 67(Suppl. 1):S36-S39.
Economos, C. D., and S. Irish-Hauser. 2007. Community interventions: A brief overview and their application to the obesity epidemic. Journal of Law, Medicine and Ethics 35(1):131-137.
Economos, C. D., R. C. Brownson, M. A. DeAngelis, P. Novelli, S. B. Foerster, C. T. Foreman, J. Gregson, S. K. Kumanyika, and R. R. Pate. 2001. What lessons have been learned from other attempts to guide social change? Nutrition Reviews 59(3 Pt. 2):S40-S56; discussion S57-S65.
Economos, C. D., S. C. Folta, J. Goldberg, D. Hudson, J. Collins, Z. Baker, E. Lawson, and M. Nelson. 2009. A community-based restaurant initiative to increase availability of healthy menu options in Somerville, Massachusetts: Shape Up Somerville. Preventing Chronic Disease 6(3):A102.
Edelman. 2011. Health barometer 2011: Global findings. http://www.edelman.com/healthbarometer (accessed November 9, 2011).
FDA/HHS (U.S. Food and Drug Administration/U.S. Department of Health and Human Services). 2010. Regulations restricting the sale and distribution of cigarettes and smokeless tobacco to protect children and adolescents. Final rule. Federal Register 75(53):13225-13232.
Foresight. 2007. Tackling obesities: Future choice—Project report, 2nd edition. London, UK: Government Office for Science.
Fox, M. K., A. Gordon, R. Nogales, and A. Wilson. 2009. Availability and consumption of competitive foods in US public schools. Journal of the American Dietetic Association 109(Suppl. 2):S57-S66.
Frieden, T. R., W. Dietz, and J. Collins. 2010. Reducing childhood obesity through policy change: Acting now to prevent obesity. Health Affairs 29(3):357-363.
Gordon-Larsen, P., M. C. Nelson, P. Page, and B. M. Popkin. 2006. Inequality in the built environment underlies key health disparities in physical activity and obesity. Pediatrics 117(2):417-424.
Goren, A., J. L. Harris, M. B. Schwartz, and K. D. Brownell. 2010. Predicting support for restricting food marketing to youth. Health Affairs 29(3):419-424.
Grier, S. 2009. African American & Hispanic youth vulnerability to target marketing: Implications for understanding the effects of digital marketing. http://digitalads.org/reports.php (accessed November 11, 2011).
Grier, S. A., and S. K. Kumanyika. 2008. The context for choice: Health implications of targeted food and beverage marketing to African Americans. American Journal of Public Health 98(9):1616-1629.
Grier, S. A., and S. Kumanyika. 2010. Targeted marketing and public health. Annual Review of Public Health 31:349-369.
Griffiths, L. J., T. J. Parsons, and A. J. Hill. 2010. Self-esteem and quality of life in obese children and adolescents: A systematic review. International Journal of Pediatric Obesity 5(4):282-304.
Harris, J. L., J. L. Pomeranz, T. Lobstein, and K. D. Brownell. 2009. A crisis in the marketplace: How food marketing contributes to childhood obesity and what can be done. Annual Review of Public Health 30:211-225.
Hawkes, C. 2007. Marketing food to children: Changes in the global regulatory environment 2004-2006. Geneva, Switzerland: WHO.
Heinen, L., and H. Darling. 2009. Addressing obesity in the workplace: The role of employers. Milbank Quarterly 87(1):101-122.
Ikeda, J. P., P. B. Crawford, and G. Woodward-Lopez. 2006. BMI screening in schools: Helpful or harmful. Health Education Research 21(6):761-769.
IOM (Institute of Medicine). 1995. Weighing the options: Criteria for evaluating weight-management programs. Washington, DC: National Academy Press.
IOM. 2005. Preventing childhood obesity: Health in the balance. Washington, DC: The National Academies Press.
IOM. 2006. Food marketing to children and youth: Threat or opportunity? Washington, DC: The National Academies Press.
IOM. 2007. Progress in preventing childhood obesity: How do we measure up? Washington, DC: The National Academies Press.
IOM. 2009. Weight gain during pregnancy: Reexamining the guidelines. Washington, DC: The National Academies Press.
IOM. 2010. Bridging the evidence gap in obesity prevention: A framework to inform decision making. Washington, DC: The National Academies Press.
Just, D. R., and C. R. Payne. 2009. Obesity: Can behavioral economics help? Annals of Behavioral Medicine 38(Suppl. 1):S47-S55.
Just, D. R., B. Wansink, L. Mancino, and J. Guthrie. 2008. Behavioral economic concepts to encourage healthy eating in school cafeterias: Experiments and lessons from college students, ERR-68. Washington, DC: USDA.
Kersh, R. 2009. The politics of obesity: A current assessment and look ahead. Milbank Quarterly 87(1):295-316.
Kersh, R., and J. Morone. 2002. How the personal becomes political: Prohibitions, public health, and obesity. Studies in American Political Development 16(2):162-175.
Kersh, R., D. F. Stroup, and W. C. Taylor. 2011. Childhood obesity: A framework for policy approaches and ethical considerations. Preventing Chronic Disease 8(5):A93.
Kraak, V. I., M. Story, E. A. Wartella, and J. Ginter. 2011. Industry progress to market a healthful diet to American children and adolescents. American Journal of Preventive Medicine 41(3):322-333; quiz A324.
Krukowski, R. A., D. S. West, J. Harvey-Berino, and T. Elaine Prewitt. 2010. Neighborhood impact on healthy food availability and pricing in food stores. Journal of Community Health 35(3):315-320.
Kumanyika, S. K. 2006. Nutrition and chronic disease prevention: Priorities for US minority groups. Nutrition Reviews 64(2 Pt. 2):S9-S14.
Kumanyika, S. K. 2008. Environmental influences on childhood obesity: Ethnic and cultural influences in context. Physiology and Behavior 94(1):61-70.
Kumanyika, S. K., and S. Grier. 2006. Targeting interventions for ethnic minority and low-income populations. Future of Children 16(1):187-207.
Kumanyika, S. K., E. Obarzanek, N. Stettler, R. Bell, A. E. Field, S. P. Fortmann, B. A. Franklin, M. W. Gillman, C. E. Lewis, W. C. Poston, 2nd, J. Stevens, and Y. Hong. 2008. Population-based prevention of obesity: The need for comprehensive promotion of healthful eating, physical activity, and energy balance: A scientific statement from American Heart Association Council on Epidemiology and Prevention, Interdisciplinary Committee for Prevention (formerly the expert panel on population and prevention science). Circulation 118(4):428-464.
Leviton, L. C., L. K. Khan, D. Rog, N. Dawkins, and D. Cotton. 2010. Evaluability assessment to improve public health policies, programs, and practices. Annual Review of Public Health 31:213-233.
Lewis, C. E., D. R. Jacobs, Jr., H. McCreath, C. I. Kiefe, P. J. Schreiner, D. E. Smith, and O. D. Williams. 2000. Weight gain continues in the 1990s: 10-year trends in weight and overweight from the CARDIA study. Coronary artery risk development in young adults. American Journal of Epidemiology 151(12):1172-1181.
Liburd, L. C., L. A. Anderson, T. Edgar, and L. Jack, Jr. 1999. Body size and body shape: Perceptions of black women with diabetes. Diabetes Educator 25(3):382-388.
Miller, M. E. 2010. Child labor and protecting young workers around the world. An introduction to this issue. International Journal of Occupational and Environmental Health 16(2):103-112.
NICE (National Institute for Health and Clinical Excellence). 2011. Whole system approaches to obesity prevention: Review of cost-effectiveness evidence. http://www.nice.org.uk/nicemedia/live/12109/55093/55093.pdf (accessed November 9, 2011).
Norman, J. E., and R. Reynolds. 2011. The consequences of obesity and excess weight gain in pregnancy. Proceedings of the Nutrition Society 70(4):450-456.
OECD (Organisation for Economic Co-operation and Development). 2010. Obesity and the economics of prevention: Fit not fat. http://www.oecd.org/document/31/0,3746,en_2649_33929_45999775_1_1_1_1,00.html (accessed January 4, 2012).
Oza-Frank, R., and S. A. Cunningham. 2010. The weight of US residence among immigrants: A systematic review. Obesity Reviews 11(4):271-280.
Pomeranz, J. L. 2010. Television food marketing to children revisited: The Federal Trade Commission has the constitutional and statutory authority to regulate. Journal of Law, Medicine and Ethics 38(1):98-116.
Powell, L. M., S. Slater, F. J. Chaloupka, and D. Harper. 2006. Availability of physical activity-related facilities and neighborhood demographic and socioeconomic characteristics: A national study. American Journal of Public Health 96(9):1676-1680.
Powell, L. M., G. Szczypka, and F. J. Chaloupka. 2010. Trends in exposure to television food advertisements among children and adolescents in the United States. Archives of Pediatrics and Adolescent Medicine 164(9):794-802.
Power, E. M. 2005. Determinants of healthy eating among low-income Canadians. Canadian Journal of Public Health. Revue Canadienne de Sante Publique 96(Suppl. 3):S37-S42.
Rahman, T., R. A. Cushing, and R. J. Jackson. 2011. Contributions of built environment to childhood obesity. Mount Sinai Journal of Medicine 78(1):49-57.
Rideout, V. J., U. G. Foehr, and D. F. Roberts. 2010. Generation M2: Media in the lives of 8- to 18-year-olds. Menlo Park, CA: Henry J. Kaiser Family Foundation.
Sallis, J. F., and K. Glanz. 2006. The role of built environments in physical activity, eating, and obesity in childhood. Future of Children 16(1):89-108.
Seidell, J. C., A. J. Nooyens, and T. L. Visscher. 2005. Cost-effective measures to prevent obesity: Epidemiological basis and appropriate target groups. Proceedings of the Nutrition Society 64(1):1-5.
Swinburn, B., G. Egger, and F. Raza. 1999. Dissecting obesogenic environments: The development and application of a framework for identifying and prioritizing environmental interventions for obesity. Preventive Medicine 29(6 Pt. 1):563-570.
Swinburn, B., G. Sacks, T. Lobstein, N. Rigby, L. A. Baur, K. D. Brownell, T. Gill, J. Seidell, and S. Kumanyika. 2008. The “Sydney Principles” for reducing the commercial promotion of foods and beverages to children. Public Health Nutrition 11(9):881-886.
Swinburn, B. A., G. Sacks, K. D. Hall, K. McPherson, D. T. Finegood, M. L. Moodie, and S. L. Gortmaker. 2011. The global obesity pandemic: Shaped by global drivers and local environments. The Lancet 378(9793):804-814.
Taylor, W. C., W. S. C. Poston, L. Jones, and M. K. Kraft. 2006. Environmental justice: Obesity, physical activity, and healthy eating. Journal of Physical Activity and Health 3(Suppl. 1):S30-S54.
Tharp, M. 2001. Chapter 3, marketing in a multicultural environment. In Marketing and consumer identity in multicultural America. Thousand Oaks, CA: Sage. Pp. 57-90.
Toomey, T. L., and A. C. Wagenaar. 1999. Policy options for prevention: The case of alcohol. Journal of Public Health Policy 20(2):192-213.
USDA (U.S. Department of Agriculture)/HHS. 2010. Dietary Guidelines for Americans, 2010. 7th ed. Washington, DC: U.S. Government Printing Office.
Washington, R. L. 2011. Childhood obesity: Issues of weight bias. Preventing Chronic Disease 8(5):A94.
Wechsler, H., N. D. Brener, S. Kuester, and C. Miller. 2001. Food service and foods and beverages available at school: Results from the school health policies and programs study 2000. Journal of School Health 71(7):313-324.
White House Task Force on Childhood Obesity. 2010. Solving the problem of childhood obesity within a generation: White House Task Force on Childhood Obesity report to the President. Washington, DC: Executive Office of the President of the United States.
WHO (World Health Organization). 2000. Obesity: Preventing and managing the global epidemic. Report of a WHO consultation. World Health Organization Technical Report Series 894:i-xii, 1-253.
WHO. 2007. Nutrition, physical activity and the prevention of obesity: Policy developments in the WHO European region. www.euro.who.int/__data/assets/pdf_file/0013/111028/E90669.pdf (accessed January 4, 2012).
WHO. 2010. Set of recommendations on the marketing of foods and non-alcoholic beverages to children. Geneva, Switzerland: WHO Press.
WHO. 2011. Global status report on noncommunicable diseases 2010: Description of the global burden of NCDS, their risk factors and determinants. http://www.who.int/nmh/publications/ncd_report2010/en/ (accessed January 4, 2012).
Williamson, D. F., H. S. Kahn, P. L. Remington, and R. F. Anda. 1990. The 10-year incidence of overweight and major weight gain in US adults. Archives of Internal Medicine 150(3):665-672.
Yancey, A. K., B. L. Cole, R. Brown, J. D. Williams, A. Hillier, R. S. Kline, M. Ashe, S. A. Grier, D. Backman, and W. J. McCarthy. 2009. A cross-sectional prevalence study of ethnically targeted and general audience outdoor obesity-related advertising. Milbank Quarterly 87(1):155-184.




































