Crisis Standards of Care
A Systems Framework for Catastrophic Disaster Response
Volume 4: Hospital
Committee on Guidance for Establishing Standards of Care for Use in Disaster Situations
Board on Health Sciences Policy
Dan Hanfling, Bruce M. Altevogt, Kristin Viswanathan, and Lawrence O. Gostin, Editors
INSTITUTE OF MEDICINE
OF THE NATIONAL ACADEMIES
THE NATIONAL ACADEMIES PRESS
Washington, D.C.
|
THE NATIONAL ACADEMIES PRESS |
500 Fifth Street, NW |
Washington, DC 20001 |
NOTICE: The project that is the subject of this report was approved by the Governing Board of the National Research Council, whose members are drawn from the councils of the National Academy of Sciences, the National Academy of Engineering, and the Institute of Medicine. The members of the committee responsible for the report were chosen for their special competences and with regard for appropriate balance.
This study was supported by Contract No. HHSP23320042509XI between the National Academy of Sciences and the Department of Health and Human Services. Any opinions, findings, conclusions, or recommendations expressed in this publication are those of the author(s) and do not necessarily reflect the view of the organizations or agencies that provided support for this project.
Library of Congress Cataloging-in-Publication Data
Crisis standards of care : a systems framework for catastrophic disaster
response / Committee on Guidance for Establishing Standards of Care for Use in
Disaster Situations, Board on Health Sciences Policy ; Dan Hanfling … [et al.], editors.
p. ; cm.
Includes bibliographical references.
ISBN 978-0-309-25346-8 (hardcover) — ISBN 978-0-309-25347-5 (pdf) I. Hanfling, Dan.
II. Institute of Medicine (U.S.). Committee on Guidance
for Establishing Standards of Care for Use in Disaster Situations.
[DNLM: 1. Disaster Medicine—standards—United States. 2. Emergency
Medical Services—standards—United States. 3. Emergency Treatment—
standards—United States. WA 295]
363.34—dc23
2012016602
Additional copies of this report are available from the National Academies Press, 500 Fifth Street, NW, Keck 360, Washington, DC 20001; (800) 624-6242 or (202) 334-3313; http://www.nap.edu.
For more information about the Institute of Medicine, visit the IOM home page at: www.iom.edu.
Copyright 2012 by the National Academy of Sciences. All rights reserved.
Printed in the United States of America
The serpent has been a symbol of long life, healing, and knowledge among almost all cultures and religions since the beginning of recorded history. The serpent adopted as a logotype by the Institute of Medicine is a relief carving from ancient Greece, now held by the Staatliche Museen in Berlin.
Suggested citation: IOM (Institute of Medicine). 2012. Crisis Standards of Care: A Systems Framework for Catastrophic Disaster Response. Washington, DC: The National Academies Press.
THE NATIONAL ACADEMIES
Advisers to the Nation on Science, Engineering, and Medicine
The National Academy of Sciences is a private, nonprofit, self-perpetuating society of distinguished scholars engaged in scientific and engineering research, dedicated to the furtherance of science and technology and to their use for the general welfare. Upon the authority of the charter granted to it by the Congress in 1863, the Academy has a mandate that requires it to advise the federal government on scientific and technical matters. Dr. Ralph J. Cicerone is president of the National Academy of Sciences.
The National Academy of Engineering was established in 1964, under the charter of the National Academy of Sciences, as a parallel organization of outstanding engineers. It is autonomous in its administration and in the selection of its members, sharing with the National Academy of Sciences the responsibility for advising the federal government. The National Academy of Engineering also sponsors engineering programs aimed at meeting national needs, encourages education and research, and recognizes the superior achievements of engineers. Dr. Charles M. Vest is president of the National Academy of Engineering.
The Institute of Medicine was established in 1970 by the National Academy of Sciences to secure the services of eminent members of appropriate professions in the examination of policy matters pertaining to the health of the public. The Institute acts under the responsibility given to the National Academy of Sciences by its congressional charter to be an adviser to the federal government and, upon its own initiative, to identify issues of medical care, research, and education. Dr. Harvey V. Fineberg is president of the Institute of Medicine.
The National Research Council was organized by the National Academy of Sciences in 1916 to associate the broad community of science and technology with the Academy’s purposes of furthering knowledge and advising the federal government. Functioning in accordance with general policies determined by the Academy, the Council has become the principal operating agency of both the National Academy of Sciences and the National Academy of Engineering in providing services to the government, the public, and the scientific and engineering communities. The Council is administered jointly by both Academies and the Institute of Medicine. Dr. Ralph J. Cicerone and Dr. Charles M. Vest are chair and vice chair, respectively, of the National Research Council.
COMMITTEE ON GUIDANCE FOR ESTABLISHING STANDARDS OF CARE FOR USE IN DISASTER SITUATIONS
LAWRENCE O. GOSTIN (Chair), O’Neill Institute for National and Global Health Law, Georgetown University Law Center, Washington, DC
DAN HANFLING (Vice-Chair), Inova Health System, Falls Church, VA
DAMON T. ARNOLD, Illinois Department of Public Health, Chicago (retired)
STEPHEN V. CANTRILL, Denver Health Medical Center, CO
BROOKE COURTNEY, Food and Drug Administration, Bethesda, MD
ASHA DEVEREAUX, California Thoracic Society, San Francisco, CA
EDWARD J. GABRIEL,* The Walt Disney Company, Burbank, CA
JOHN L. HICK, Hennepin County Medical Center, Minneapolis, MN
JAMES G. HODGE, JR., Center for the Study of Law, Science, and Technology, Arizona State University, Tempe
DONNA E. LEVIN, Massachusetts Department of Public Health, Boston
MARIANNE MATZO, University of Oklahoma Health Sciences Center, Oklahoma City
CHERYL A. PETERSON, American Nurses Association, Silver Spring, MD
TIA POWELL, Montefiore-Einstein Center for Bioethics, Albert Einstein College of Medicine, New York, NY
MERRITT SCHREIBER, University of California, Irvine, School of Medicine
UMAIR A. SHAH, Harris County Public Health and Environmental Services, Houston, TX
JOLENE R. WHITNEY, Bureau of Emergency Medical Services (EMS) and Preparedness, Utah Department of Health, Salt Lake City
Study Staff
BRUCE M. ALTEVOGT, Study Director
ANDREW M. POPE, Director, Board on Health Sciences Policy
CLARE STROUD, Program Officer
LORA TAYLOR, Senior Project Assistant (until January 2012)
ELIZABETH THOMAS, Senior Project Assistant (since February 2012)
KRISTIN VISWANATHAN, Research Associate
RONA BRIER, Editor
BARBARA FAIN, Consultant for Public Engagement
_________________
* Resigned from the committee October 2011.
Reviewers
This report has been reviewed in draft form by individuals chosen for their diverse perspectives and technical expertise, in accordance with procedures approved by the National Research Council’s Report Review Committee. The purpose of this independent review is to provide candid and critical comments that will assist the institution in making its published report as sound as possible and to ensure that the report meets institutional standards for objectivity, evidence, and responsiveness to the study charge. The review comments and draft manuscript remain confidential to protect the integrity of the deliberative process. We wish to thank the following individuals for their review of this report:
Richard Alcorta, Maryland Institute for Emergency Medical Services Systems
Knox Andress, Louisiana Poison Center
Connie Boatright-Royster, MESH Coalition
Susan Cooper, Tennessee Department of Health
Lance Gable, Wayne State University Center for Law and the Public’s Health
Carol Jacobson, Ohio Hospital Association
Amy Kaji, Harbor-UCLA Medical Center
Jon Krohmer, Department of Homeland Security
Onora Lien, King County Healthcare Coalition
Suzet McKinney, The Tauri Group
Peter Pons, Denver Health Medical Center
Clifford Rees, University of New Mexico School of Law
Linda Scott, Michigan Department of Community Health
Robert Ursano, Uniformed Services University School of Medicine
Lann Wilder, San Francisco General Hospital and Trauma Center
Matthew Wynia, American Medical Association
Although the reviewers listed above have provided many constructive comments and suggestions, they were not asked to endorse the conclusions or recommendations nor did they see the final draft of the report before
its release. The review of this report was overseen by Dr. Georges Benjamin, American Public Health Association. Appointed by the Institute of Medicine, he was responsible for making certain that an independent examination of this report was carried out in accordance with institutional procedures and that all review comments were carefully considered. Responsibility for the final content of this report rests entirely with the authoring committee and the institution.
Contents
VOLUME 1: INTRODUCTION AND CSC FRAMEWORK
2 Catastrophic Disaster Response: Creating a Framework for Medical Care Delivery
4 Cross-Cutting Themes: Ethics, Palliative Care, and Mental Health
VOLUME 2: STATE AND LOCAL GOVERNMENT
6 Prehospital Care: Emergency Medical Services (EMS)
7 Hospitals and Acute Care Facilities
Roles and Responsibilities of Health Care Facilities
Template 7.1. Core Functions of Hospital Facilities and Providers in the Implementation of CSC Plans
|
ARDS |
acute respiratory distress syndrome |
|
ASPR |
Assistant Secretary for Preparedness and Response |
|
CDC |
Centers for Disease Control and Prevention |
|
CSC |
crisis standards of care |
|
DMAT |
disaster medical assistance team |
|
ECG |
electrocardiogram |
|
ECMO |
extracorporeal membrane oxygenation |
|
EMS |
emergency medical services |
|
EMTALA |
Emergency Medical Treatment and Active Labor Act |
|
EOC |
emergency operations center |
|
ESAR-VHP |
Emergency System for Advance Registration of Volunteer Health Professionals |
|
HICS |
hospital incident command system |
|
HIPAA |
Health Insurance Portability and Accountability Act |
|
ICS |
incident command system |
|
ICU |
intensive care unit |
|
IOM |
Institute of Medicine |
|
IVIG |
intravenous immune globulin |
|
JIC |
joint information center |
|
JIS |
joint information system |
|
MRC |
Medical Reserve Corps |
|
MSOFA |
Modified Sequential Organ Failure Assessment |
|
NIMS |
National Incident Management System |
|
PACU |
postanesthesia care unit |
|
PHEP |
Public Health Emergency Preparedness |
|
RDMAC |
regional disaster medical advisory committee |
|
SDMAC |
state disaster medical advisory committee |
|
SNS |
Strategic National Stockpile |
|
SOFA |
Sequential Organ Failure Assessment |
|
VA |
Department of Veterans Affairs |
|
VAMC |
VA Medical Center |
|
VHA |
Veterans Health Administration |
|
VISN |
Veterans Integrated Service Network |
Volume 4 7: Hospitals and Acute Care Facilities
Hospitals and acute care facilities providing acute medical care to the community have a “duty to plan” (Hodge and Brown, 2011)1 for mass casualty incidents, including planning for the expansion of clinical operations, commonly referred to as surge capacity (Barbera and MacIntyre, 2004; Barbisch and Koenig, 2006; Hick et al., 2004, 2008; Joint Commission, 2008; Kaji et al., 2006). Surge capacity occurs across a continuum that is based on resource availability and demand for health care services (see Chapter 2). One end of the continuum is defined by conventional responses—the maximal utilization of services usually provided in health care facilities; at the other end of the continuum is crisis care, when the care provided is the best possible given the very limited resources available. Along this continuum, significant changes are made in the methods and locations of care delivery, and the focus of decision making shifts from being primarily on individuals to being more population centered. Crisis care planning is a significant deficit in many emergency plans (GAO, 2008).2
An overview of the importance of planning for a tiered approach that utilizes many of the key components of crisis standards of care (CSC) is provided in Chapter 1. This chapter presents the roles and responsibilities of health care facilities in a disaster response and operational considerations entailed in carrying out those roles and responsibilities. It also includes a template detailing the core functions of hospitals and hospital providers in the implementation of CSC. While this chapter is not intended to provide a review of hospital disaster preparedness, there is some overlap because crisis care depends on good underlying plans. Although hospitals providing acute care to the community are the focus of this discussion, other health care facilities—such as free-standing surgery centers, urgent cares, ambulatory clinics, free-standing emergency departments, nursing homes, federally qualified health centers, and other facilities that can be adapted to provide acute or critical care—can play key roles in a surge response and should refer to this chapter, as well as the following chapter on out-of-hospital and alternate care systems.
_________________
1Preston v. Tenet Healthsystem Memorial Medical Center Inc., no. 05-11709-B-15 (La. Civ. Dist. Ct. settled March 23, 2011).
2 This report addresses resource deficits in the setting of disasters, although it should be acknowledged that daily capacity challenges in emergency departments and hospitals may risk patient complications due to capacity issues (Bernstein et al., 2009; IOM, 2006; Maa, 2011).
ROLES AND RESPONSIBILITIES OF HEALTH CARE FACILITIES
Hospitals may be individual facilities, part of a corporate chain, or part of a federal system (such as Department of Veterans Affairs [VA] medical centers or military hospitals). The committee recognizes that it may be very difficult to create policy across institutions located in disparate geographic areas that is consistent with local policy and incidents, as the impact, resources, and cultural or societal expectations associated with an incident may differ.
The committee believes that health system facilities, whether private or public, should be expected to provide care and resources commensurate with what is being provided in the community in which they are located. Thus, if the hospital system has resources in excess of those available in the community, it should allow patients into the system or commit resources to the community to allow equilibration of resource availability. For example, VA resources may be tasked to support the response to civilian disasters under the Stafford Act, or at the discretion of their medical center director may assist the community during a disaster. A VA medical center could potentially offer care to veterans’ families, other service-connected personnel, or the general public, depending on resources, or support community facilities with staff or pharmaceuticals.3The same should be expected of military and other governmental or private health system facilities. This expectation includes a commitment on the part of specialty hospitals (children’s, rehabilitation, women’s health, cardiac) to provide care or resources to patients outside their usual patient population if an incident otherwise results in underutilization of their facilities and services.
By contrast, if specific groups (e.g., pediatric patients) are disproportionately affected by a disaster, plans should be in place for triaging patients to those facilities most capable of providing specialty care. For example, a recommendation has been made that children’s hospitals provide care to those aged 5-8 and under who are most likely to benefit from pediatric specialty care (Christian et al., 2011; Nap et al., 2010). Regional management of access to pediatric intensive care units could have a significant beneficial effect on overall mortality in an incident affecting primarily children (Kanter, 2007). Similarly, regional burn plans in some areas concentrate the most severely burned patients at recognized burn centers, and include relocation of patients from those facilities to make room for burn patients.
For facilities in corporate or government health systems that cross regional planning areas or state borders, close coordination with the community medical advisory committees and the state is critical to ensure that system and local guidelines are as consistent as possible, since identical guidance is unrealistic unless provided at the federal level. Within health care systems, there may be a strong inclination to set incident-related policy at the corporate/national level. While this inclination is understandable, overly specific policies set at this level may conflict with attempts to provide local consistency among institutions. This balance should be considered by those in health system emergency management.
Regional Coordination
The regional resource management illustrated by the pediatric and burn hospital examples above requires active coordination of all disaster response stakeholders. In fact, a regionally coordinated response is impera-
_________________
3Department of Veterans Affairs Emergency Preparedness Act of 2002, Public Law 107-287, 107th Cong., 2d sess. (November 7, 2002), 38 U.S.C. § 1785.
BOX 7-1
Key Steps for Veterans Affairs Medical Center (VAMC) Emergency Management Planning
• designate an Emergency Preparedness Coordinator (EPC);
• establish the Emergency Management Committee (EMC);
• develop the all-hazard Emergency Operations Plan (EOP);
• conduct an HVA;
• develop incident specific planning guides;
• coordinate the Emergency Management Program (EMP) with external entities;
• train key staff;
• exercise the EOP; and
• conduct program review/evaluation and plan for improvements.
SOURCE: VA, 2010.
tive to facilitate a consistent standard of care within all affected communities after a disaster. Regional coordination allows the maximum use of available resources; facilitates obtaining and distributing resources; and provides a mechanism for policy development and situational awareness that is critical to avoiding crisis situations and, when a crisis does occur, ensuring fair and consistent use of resources to provide a uniform level of care across the region. Without such coordination, some facilities may be operating with crisis care in effect while others maintain conventional care; coordination can prevent such inconsistencies (Fisher et al., 2011). Box 7-1 highlights the steps that are taken across VA Medical Centers (VAMCs) under their comprehensive emergency management program to ensure that each facility is addressing the needs of emergency planning and response. Box 7-2 describes some of the specific functions by which the medical centers, which are organized regionally within the Veterans Integrated Service Network (VISN) will coordinate in the planning for implementation of crisis standards of care in a catastrophic disaster.4 More information on regional coordination and the state and regional roles therein can be found in Chapter 5.
Box 7-3 describes the health coalition model and the success it has had in coordinating regional disaster preparedness efforts (see also Figure 2-5 in Chapter 2). A regionally coordinated health care response effort includes
• coalition or other mutual-aid agreements among hospitals (Box 7-2);
• coordination with local public health, emergency management, and emergency medical services (EMS) to formulate an operational response plan and describe how that plan intersects with agencies and facilities in the surrounding regional area (may include plans for a health and medical coordination center or multiagency coordination center) (Burkle et al., 2007; Maldin et al., 2007);
• communication and information sharing mechanisms and agreements among the above entities; and
• a concept of operations for the allocation of scarce resources:
_________________
4 After initial distribution of the report, Boxes 7-1 and 7-2 were added to provide more specific information regarding the responsibilities of the VAMC and the VISN.
BOX 7-2
Key CSC Roles and Responsibilities for the Veterans Health Administration
|
Key Roles in the Veterans Health Administration (VHA) |
Responsibilities in CSC Planning |
|
VAMC |
|
|
Quadrad Leadership |
|
|
Medical Center Director |
Provide oversight of CSC planning, including specific administrative and clinical response plans; ensure that surge capacity and capability planning is expanded to include CSC principles |
|
Associate Director |
Support VAMC participation in local/ regional hospital coalition efforts |
|
Chief of Staff |
Implement specific medical care planning, including implementation of VHA guidance (see below); provide recommendations for Scarce Resource Allocation (SRA) Team members and Associate Director for Nursing Triage Team members |
|
Emergency Preparedness Coordinator |
Help to coordinate administrative support to CSC, including integrating logistics, Pharmacy, HR, Public Affairs, Engineering, Police and Quadrad; present CSC issues at appropriate committee meetings; participate in regional hospital coalition meetings |
|
Veterans Integrated Service Network (VISN) |
|
|
VISN Director |
Ensure consistency in VISN preparations for CSC planning; ensure Medical Center Directors are provided all necessary planning resources, including VHA and other Federal Guidance (IOM) |
|
Area Emergency Manager |
Develop CSC plans in context of VHA NDMS responsibilities, including patient reception function; serve as resource support to Medical Center planning efforts |
|
SOURCES: VA, 2006, 2012, n.d.; Veterans Health Administration, 2010. |
|
![]() How do local hospitals coordinate and prioritize resource requests?
How do local hospitals coordinate and prioritize resource requests?
![]() How is regional situational awareness maintained?
How is regional situational awareness maintained?
![]() Who makes allocation decisions if there are not enough supplies to fill the requests?
Who makes allocation decisions if there are not enough supplies to fill the requests?
![]() How is regional policy guidance developed for clinical care, and who is responsible?
How is regional policy guidance developed for clinical care, and who is responsible?
![]() Is there a provision for regional triage or appeals teams?
Is there a provision for regional triage or appeals teams?
The incident commander and planning section chief at each health care facility are responsible for ensuring that liaison exists with local public health and other health care facilities and regional coalitions to provide for regional situational awareness and consistency.
During ongoing incidents, hospitals should understand what communication structures are used in
BOX 7-3
Best Practices: Hospital Coalitions
Over the past decade, robust regional hospital and health care coalitions have developed that often started as mutual-aid agreements or simply meetings as part of hospital preparedness grant programs. Some are led by an executive director, with hospital administrators serving as the board of directors (Northern Virginia Hospital Alliance); others are led by a public health agency (e.g., King County, Washington) or a consortium of state public health and health departments (Southeastern Regional Pediatric Disaster Surge Network); and still others are led by elected members of the emergency preparedness group (e.g., Minneapolis/St. Paul). These coalitions have been extremely successfully in planning and exercising for disasters, as well as demonstrated operational response functions during actual incidents. Key features of strong coalitions are
• collaborative and invested leadership;
• written agreements specifying how and when the coalition is to be activated and what its delegated responsibilities are;
• a trusted agency or entity to represent the facilities to the emergency management and public health communities;
• collaborative work in concrete response areas (e.g., regional HAZMAT training and planning);
• linkages to cooperative agreements, grants, and programs such as the Hospital Preparedness Program, Metropolitan Medical Response System, Urban Area Security Initiative, and Centers for Disease Control and Prevention’s (CDC) Public Health Emergency Preparedness (PHEP) cooperative agreements (notably, the PHEP cooperative agreement has adopted the conventional/contingency/crisis framework for health care surge capacity);
• operational experience in representing or coordinating policy and resources during exercises and incidents; and
• multiagency collaboration and integration with other response partners, ensuring recognition of the coalition as a defined entity within the emergency response framework of the community.
SOURCES: CDC, 2011a; CIDRAP, 2011; County of Santa Clara, 2007; Courtney et al., 2009; King County Healthcare Coalition, 2011; O’Toole, 2009; Toner et al., 2009.
their area and how they receive and share information with the state disaster medical advisory committee (SDMAC) and (if operational) the regional disaster medical advisory committee (RDMAC) (IOM, 2009), both of which are expected to provide clinical guidance and policy support to hospitals and public health agencies. The SDMAC membership usually is weighted toward technical experts who can interpret epidemiologic and other incident information to provide clinical and triage guidelines for the hospitals in the state and coordinate with adjacent states to ensure consistency of approaches. The Minnesota Department of Health used its Science Advisory Team (the state’s SDMAC construct) to define a rationing strategy for N95 masks that could provide consistency across the state (Minnesota Department of Health, 2009).
In some areas, RDMACs are required where there are geographic areas with unique issues and concerns that require interpretation of state guidance for local issues or conditions, especially those that cut across state boundaries. This can be the case in very large urban areas in otherwise less populated states, multiple states with very few referral centers among them, or urban areas that are contiguous across state or jurisdictional borders.
As with the clinical care committee (discussed in detail below), the functions, authorities, and scope of operations of the RDMAC should be defined and exercised prior to an incident. This is usually part of a health care coalition agreement and should be reflected in the hospital’s scarce resource plans (Appendix B). The RDMAC should interface with a regional health and medical coordination center or multiagency coordination center, but its role is distinct from that of an actual emergency operations center (EOC) in that it provides medical guidance rather than operational or management support. The RDMAC may provide oversight and policy support for a regional triage team or regional management of specialty patient transfers.
Roles of the Clinical Care Committee
A group of technical experts (referred to as the clinical care committee), drawn from numerous disciplines within and sometimes outside the facility (e.g., toxicologists), should be convened to determine how the facility’s resources can best be utilized to meet community needs, and to develop clinical and other guidance or policies required to support the response to a disaster. This assessment should involve assessing the core responses of the facility and how its departments and service lines provide or support those responses. Membership of the clinical care committee will vary depending on the size of the institution, the type and duration of an incident, and the scope of the challenges entailed. Possible member disciplines include (AHRQ, 2007; Hick et al., 2007; IOM, 2009)
• administrative leadership,
• chief medical officer,
• facilities,
• nursing supervisor/manager,
• pharmacy,
• respiratory therapy,
• infection prevention and control/infectious diseases,
• critical care,
• emergency medicine,
• EMS,
• state EMS medical directors,
• ethics,
• law, and
• pediatrics or other affected specialties.
Possible members should be identified prior to an incident and should understand the analysis and action processes that will be followed. These members may work on an ongoing basis with the emergency management program at the facility to identify potential scarce resources (e.g., N95 masks, antiviral medications, ventilators, extracoporeal membrane oxygenation [ECMO] equipment) and potential coping strategies or caching recommendations.
In some areas (e.g., pediatrics, critical care, trauma, burn, toxicologic events), expertise itself will be a scarce resource. Since local specialists will be occupied with incident-related patients, it is optimal to plan with other geographic areas to provide telemedicine or hotline specialist support for clinicians at affected facilities (Xiong et al., 2010). Burn centers, trauma centers, academic hospitals, children’s hospitals, renal dialysis networks (Kopp et al., 2007), and poison control centers are likely partners in these efforts. Planning for this type of support should be done at the regional or state level, and activation and operational policies established prior to an incident. Some facilities may already use telemedicine for trauma or critical care, but may have to leverage expertise from outside the immediate area in a disaster.
Analysis of demands and possible coping strategies, both current and anticipated, may be based on usual surge capacity constructs (Table 7-1). Ideally, the hospital incident command system (HICS) planning section chief (EMSA, 2007) should request this sort of analysis for any prolonged or large-scale incident. This analysis can anticipate potential adaptations and drive resource and patient transfer requests that might help avoid or reduce the need to operate under CSC conditions. Those personnel who would play a role in incident analysis (e.g., the planning section chief) or clinical leadership (e.g., the medical director) should have disaster exercise experience, written plans, and resource materials to inform their decisions.
Preparedness Efforts
Scarce resource situations may affect an isolated medication or therapy, or they may affect multiple resource categories (staff, supplies, infrastructure, delivery), greatly increasing the complexity of decision making and the impact on providers and patients. Learning from systemwide exercises and real-world events can help prepare health care facilities and providers to implement CSC.
Hospitals should examine their hazard vulnerability analysis and ensure that they are as prepared as possible for the hazards affecting their community, including having the ability to operate as autonomously as possible for up to 96 hours (Joint Commission, 2008), or more, if the risk of isolation of the facility is high. The importance of exercising crisis situations from the provider to the incident command level cannot be overemphasized. Appendixes C and D detail specific resource deficits and situations that hospitals may wish to assess and for which they may wish to exercise their responses. It is difficult to simulate an overwhelming number of casualties in exercises, but through scenario-based learning and the posing of “extension” questions during smaller exercises or debriefs, providers can gain experience with the building blocks of manag-
TABLE 7-1
Implications of the Care Capacity Continuum for Resources
| Low Risk, Low Impact | Moderate Risk, Moderate impact | High Risk, High Impact | |||
|
Space |
• Expand hours and use procedural spaces for out-of-hospital care (e.g., surgery and procedure center recovery areas) (Chung et al., 2011; Scarfone et al., 2011) • Use postanesthesia care areas for inpatient capacity |
• Use operative spaces for inpatient care • Use alternate care sites to divert outpatients (e.g., “flu centers”) (Cruz et al., 2010) or provide basic nonambulatory care (hospital overflow) |
• Use cot-based care in flatspace areas • Make major changes to admission criteria (e.g., no admission for cardiac rule-outs if no electrocardiogram [ECG] changes and normal troponin) |
||
|
Staff |
• Change documentation requirements • Delegate nonclinical duties (e.g., meal serving) to administrative or other staff |
• Change staffing patterns, hours, or supervision • Change frequency of clinical assessments (e.g., vital signs based on clinical changes) |
• Provide just-in-time training to staff to allow them to provide lower-impact interventions and overall patient care (e.g.,inhaler administration, change of burn dressings) so specialty staff can concentrate on higher-impact interventions (e.g., ventilator management, burn debridements) |
||
|
Supplies |
• Implement conservation strategies (e.g., restrict oxygen use to those that have hypoxia) • Recommend substitute medication classes where possible |
• Adapt medications or supplies to the incident (e.g., use of BiPAP or selected anesthesia machines as ventilators) • Reuse otherwise disposable products that can easily be cleaned or disinfected (e.g., cervical collars, tourniquets) |
• Reuse products that require high-level disinfection or sterilization (e.g., central lines, ventilator circuits) • Reallocate medications or supplies to those who will derive the greatest benefit and/or make the least demand on resources (duration of use or amount used for outcome) |
ing a much larger incident. Triage teams can effectively gain experience through tabletop and other simulation experiences, as can incident command/hospital command center teams (DHS, 2007). Use of structured decision-making frameworks for routine scarce resource situations, such as medication shortages, may offer great benefit during a disaster incident (see Box 7-4).
CSC often involve triage decisions. The impact of triage on the primary goal of CSC—to provide the best outcomes for the largest number of patients—depends on the number of patients presenting, the duration for which they use specific resources, and their outcomes relative to other patients (Utley et al., 2011).
There are three basic types of triage (Hick et al., 2011; IOM, 2009; Iserson and Moskop, 2007):
• primary triage—performed at first assessment and prior to any interventions (e.g., triage upon entry to the emergency department or by EMS providers at a disaster scene) (Benson et al., 1996; Lerner et al., 2008; Sasser et al., 2009);
• secondary triage—performed after additional assessments and initial interventions (e.g., triage performed by surgery staff after administration of intravenous fluids and an initial CT scan); and
BOX 7-4
Hospital Pharmaceutical Shortages
Drug and supply shortages are increasingly common. A recent survey found that 240 common hospital supplies or pharmaceuticals were delayed or unavailable, representing a dramatic increase from prior years. Fully 89 percent of facilities responding indicated that a medication or clinical safety issue resulted from these shortages. In some cases, shortages have led to more uniform and considered use of therapies. For example, limited supplies of intravenous immune globulin (IVIG) led to national discussions, guidelines for use, and expert published opinions regarding the indications and efficacy of these agents for certain conditions. In other cases, institutional guidelines for conservation and adaptation have been developed. And sometimes, no guidance is circulated, leaving the physician to make decisions on a case-by-case basis.
Key points:
• Drug and supply shortages are common, and offer the opportunity to utilize the incident command system framework and the input of technical experts to resolve scarce resource issues in a nondisaster situation.
• Facility guidelines developed through these processes provide accountability and consistency and reduce ad hoc decision making that can lead to inconsistent use of scarce resources.
• Droactive approaches to drug shortages provide a model and support for other disaster response activities.
SOURCES: AHA, 2011; Fox and Tyler, 2004; Gurwitch et al., 1998; Hollak et al., 2010; Premier, Inc., 2011.
• tertiary triage—performed after or during the provision of definitive diagnostics and medical care (e.g., triage performed by critical care staff after intubation and mechanical ventilation with assessment of physiologic variables).
Primary and secondary triage are taught and performed routinely in mass casualty or other high-volume situations. For example, primary triage is used daily to determine who is seen next in the emergency department, and secondary triage often is used to determine who will be first to receive a CT scan or go to the operating room. However, most of these routine, and even mass casualty, decisions revolve around priority access and not absolute access to a resource, and thus they have minimal clinical consequences. Triage tools have been developed for use in predicting resource utilization (Challen et al., 2007; Talmor et al., 2007), and therefore the type of bed or unit to which a patient should be assigned. However, these decisions also are distinct from those that involve absolute access, which are much more difficult to make.
Reactive Resource Allocation
Primary and secondary triage generally are reactive, rather than proactive, in the early stages of an incident. This means providers are making resource allocation decisions individually and without structured guide-
lines, often without knowledge of the scope of the incident. Therefore, providers should gain experience in deciding when usual modes of care should be abandoned in favor of more limited interventions. When an overwhelming number of casualties present, for example, operative care should be deferred in favor of interventions that provide the greatest benefit for the least expenditure of time and resources (e.g., hemorrhage control or needle thoracostomy) (Casagrande et al., 2011; Hick et al., 2011; USAISR, 2009).
Decisions during this reactive phase rely on the best clinical judgment of providers based on their knowledge of the incident and patients’ conditions (usually trauma, burns, or chemical exposures). Triage decisions are influenced by rapidly changing patient volumes and often reflect the prior experience of the provider (e.g., previous military or mass casualty training). Experienced triage officers can potentially limit overtriage (which would commit more resources than necessary) and undertriage (which would risk a viable patient’s dying) (Frykberg, 2002). Providers likely to perform triage should understand their facility’s ethical and procedural grounding; otherwise they may make implicit value judgments that do not reflect institutional and community values (e.g., giving priority to children, among others with similar injuries, for surgical intervention).
The goal is to reach a point in the incident as early as possible when reactive triage is replaced by proactive triage strategies (see Boxes 2-1 and 2-2, respectively, in Chapter 2). Reactive triage is unavoidable in the early stages of an incident but should be limited to the time prior to situational awareness, and proactive strategies should be instituted as soon as possible, with a consistent process for decisions that are as evidence based as possible.
Tertiary triage seldom is practiced, but involves a decision about whether to initiate or continue certain therapies on the basis of a relatively complete knowledge of the patient’s diagnosis and prognosis so as to maximize the use of available resources to save more patients (Kanter, 2007). In many cases, allocation decisions do not critically impact survivability (e.g., the use of certain medications, appropriateness for discharge, diagnostic testing). In other cases, access to a life-saving intervention, such as mechanical ventilation or ECMO, may not be available to all patients who need it. These allocation decisions are extremely challenging, and require careful consideration, strong ethical grounding (O’Laughlin and Hick, 2008; Powell et al., 2008; Tabery and Mackett, 2008; University of Toronto, 2005; Vawter et al., 2010), and thoughtful transition to palliative care (see Chapter 4 for a detailed discussion of palliative care) (Eschun et al., 1999; Society of Critical Care Medicine Ethics Committee, 1994a). The dynamic nature of events requires that patients be reassessed in relation to their changing clinical condition as well as to changes in resource availability (both when resources grow scarcer and when they are replenished). During the Hurricane Katrina response, of the 50 patients initially assigned to the “expected to die—comfort care only” category at Louis Armstrong Airport by federal disaster medical assistance team (DMAT) members responsible for triaging thousands of patients, only 26 actually died. This was because patients were reassessed and reprioritized as additional resources became available or the patients’ conditions improved (Klein et al., 2008).
Structured reassessment of the strategies being used and the ability to make real-time adjustments to plans are important, as incidents are likely to encompass several supply and demand spikes involving different resources (e.g., operative and pharmacy supply issues today, staffing issues tomorrow). Incidents will not affect all health care facilities (or all areas of a single facility) at the same time in the same way. Thus, there is no standard approach to resource triage. This is why it is important that the ethical and procedural prin-
ciples of the facility be clearly stated (see the ethics section of Chapter 4 for further discussion). The same principles can then be applied consistently regardless of the allocation decision to be made (e.g., allocating limited N95 masks, reserving a stock of antivirals for staff, or making patient intervention decisions).
Surge Capacity and the Care Continuum
Each hospital should have concrete goals for expansion during a disaster, including outpatient, inpatient, and specialty unit capacity. However, the extent to which a hospital can surge will vary. Recommendations are not standardized; for example, Israeli hospitals are required by the government to be able to increase their capacity by 20 percent within hours (Peleg and Kellermann, 2009), while a U.S. critical care workgroup recommended surge capacity of 200 percent over usual intensive care capacity (Rubinson et al., 2008a), which would involve significant operational planning (Gomersall et al., 2006; Hota et al., 2010; Rubinson et al.,2005). The role of the institution in the community and its size contribute to this calculus. For example, it may be easier for a smaller hospital to surge to 200 percent of a small number of critical care beds, and a higher goal may be in order (as compared with a tertiary hospital). Similarly, a level 1 trauma hospital with an accredited burn unit will be expected to be prepared for a much larger number of operative and burn patients than a hospital that does not usually receive trauma cases. A consensus group has recommended that pediatric intensive care units be prepared to provide 100 percent surge capacity (doubled volume) for 10 days (Bohn et al., 2011). An example surge capacity template for a moderate-sized hospital is found in Table 7-2.
As noted earlier, mass casualty response in a health care facility spans a continuum from conventional to crisis care, depending on the incident demands (Box 7-5, presented also in Chapter 2) (Hick et al., 2009; IOM, 2009). The better prepared the institution and the more resources available, the longer a facility can stay in conventional and contingency mode before the shift to CSC becomes necessary, when the threat of morbidity and mortality to patients becomes significant as a result of the lack of resources. The ability to meet demand for hospital resources, especially during an incident involving infection or potential contamination (e.g., radiation), is highly dependent on capable out-of-hospital and alternate care systems, good risk communication, sound transport policies, and other community-based resources that can radically reduce (or increase) patient demand on hospitals during an incident. Table 7-2 presents a template for planning hospital inpatient surge capacity.
The goal of incident management in mass casualty situations or catastrophic critical infrastructure failure is to get the right resources to the right place at the right time. This may involve anticipating shortfalls, adapting responses (Table 7-3), partnering with other stakeholder agencies to provide alternate care sites for patient volumes that cannot be accommodated within the usual medical facilities, and other strategies.
Only when no alternatives are possible should the institution provide crisis care—when the focus shifts from patient-centered to population-centered care. Patients’ prognosis and the degree of resource commitment required should be considered, and patients and/or resources may have to be triaged. Planning for CSC should not be done in isolation, but should be incorporated into the facility emergency operations plan and mutual-aid agreements. A sample scarce resource annex for a facility emergency operations plan is provided in Appendix B.
TABLE 7-2
Template for Hospital Inpatient Surge Capacity
Accommodate incident demands within the time frame shown, progressing from conventional to contingency, then crisis strategies, and returning to conventional as soon as possible.
| Time (hours) | 0-2 | 2-4 | 4-12 | 12-24 | |
Major Incident |
Conventional Care |
• Fill available staffed beds. Cancel/hold elective surgeries if operative\ capacity needed or if expected to require admission. • Begin “surge discharge”: º Medicine on-call º Surgery on-call º Unit supervisors • Identify patients for “early” discharge, and begin to organize for move. |
• Provide staff for unstaffed but available beds through unit call-in. • Add in-storage beds to usual patient rooms (total X additional possible beds) on the following units, and contact leasing agencies if additional beds required; consider intensive care unit (ICU) bed needs (below): list units and beds here. • Move “surge discharge” patients to halls initially to open beds, and then to preidentified discharge holding area; ensure that physicians and nurses attend to the pharmacy, transport, and home care needs of these patients. |
• Obtain additional beds through leasing or from storage, and add to existing patient rooms; move patients from temporary areas (e.g., postanesthesia care unit [PACU]) to these beds as soon as available. |
• Cancellation of elective cases begins to have an impact (but does not open new beds). |
| Contingency Care (functionally equivalent care—most incidents will require this level of care for a short period of time/adjustment period) |
• Clear patients out of preinduction/phase 1 recovery areas, and fill available beds (total number) in: º Unit 1 (#) º Unit 2 (#) º PACU (#) º Preinduction (#) • Consider area for overflow of minor trauma cases from emergency department vs. overflow from clinics (list locations). |
• Preinduction and procedural areas fully available. Consider adding GI lab (#), pulmonary/ bronchitis lab (#), and (X) areas; Phase 2 recovery areas/ preinduction areas (#); and same-day admission/recovery areas (#). Reserve beds in recovery as needed for cases coming out of surgery. • Transfer patients from higheracuity care areas to loweracuity care areas (e.g., from ICU to monitored floor) to free ICU space (can shift from private to double ICU rooms, but limited in storage/lease bed availability. Bio has (#) contingency monitors). Transfer overflow ICU patients to (list stepdown units in order of preference). |
• Assess the situation—consider mechanisms for returning to conventional care, and contact regional health care coalition for necessary resources if unable to return to conventional status within following 8-12 hours. |
• If transfer possible and unable to return to conventional care status within 8-12 hours, initiate local or regional patient transfers. |
 |
|||||
|
|
|
• Consider “inpatient” care on rehab/observation units subject to availability/discharges (X beds). |
|
|
|
| Crisis Care (provide best care possible in the circumstances—rare situation) Evacuation* |
• Place patients in hallways or lobby areas (unit name(s)) on cots if floor beds are immediately lacking. Cots stored in: º Storage location 1 (#) º Storage location 2 (#) • Evaluate options for patient transfer to reduce demand. |
• Set up preplanned facility areas for austere inpatient care: º Area 1 (conference rooms or other flat space) º Area 2 º Area 3 • Contact regional hospital coalition—(XXX) XXX-XXXX—on call to advise of situation, and arrange resources/staff or local/interregional patient transfers sufficient to return to contingency care operations and/or activate alternate care sites. • Request that units identify patients for possible transfer, and prioritize patients for evacuation based on the situation. Create transfer patient lists for regional/federal use. Request units identify patients for possible transfer and prioritize patients for evacuation based on situation. Create transfer patient lists for regional/federal use. |
• Mobilize resources for alternate care sites if needed; coordinate with regional hospital coalition. • Prepare patient belongings and charting, and begin local/regional patient transfers. |
• Begin patient transfers to alternate care sites if activated. Federally facilitated (National Disaster Medical System) patient movement (if activated) begins at about 36 hours postincident. |
|
*If no evacuation of patients is possible and the crisis care situation is prolonged, the incident commander should convene the clinical care committee to prioritize resources/service delivery.
BOX 7-5
Conventional, Contingency, and Crisis Care Conventional Capacity:
The spaces, staff, and supplies used are consistent with daily practices within the institution. These spaces and practices are used during a major mass casualty incident that triggers activation of the facility emergency operations plan.
Contingency Capacity: The spaces, staff, and supplies used are not consistent with daily practices but provide care that is functionally equivalent to usual patient care. These spaces or practices may be used temporarily during a major mass casualty incident or on a more sustained basis during a disaster (when the demands of the incident exceed community resources).
Crisis capacity: Adaptive spaces, staff, and supplies are not consistent with usual standards of care, but provide sufficiency of care in the context of a disaster (i.e., provide the best possible care to patients given the circumstances and resources available). Crisis capacity activation constitutes a significant adjustment to standards of care.
SOURCE: Hick et al., 2009.
Principles of Crisis Care in Hospitals
Crisis care and triage may be required in the early phase of a no-notice incident, prior to the establishment of situational awareness or incident management. This is termed the reactive phase (discussed more fully in Chapter 2). Triage decisions are made by bedside providers in this phase, but the goal is to move toward a more proactive, incident-specific, structured, and reproducible decision-making process as rapidly as possible once reasonable situational awareness has been attained and an incident management structure is in place. This approach is consistent with a recommendation from the American College of Physicians that “resource allocation decisions are policy decisions that are most appropriately made at the system level, not at the bedside” (American College of Physicians, 2011). General prerequisites for making proactive resource triage decisions are as follows (IOM, 2009):
• Critically limited resource(s) and infrastructure are identified.
• Surge capacity is fully employed within health care facilities (and regionally) if capacity/space is the limited resource.
• Maximal efforts to conserve, substitute, adapt, and reuse are insufficient if supplies are the limited resource.
• Regional, state, and federal resources are insufficient or cannot meet demand.
• Patient transfer or resource importation is not possible or will occur too late for bridging therapies (such as bag-valve ventilation or other temporizing measures) to be considered.
• Necessary resources have been requested from local and regional health officials (as applicable).
• A state of emergency has been declared, or other health powers (as applicable) have been activated.
TABLE 7-3
Sample Strategies to Address Resource Shortfalls
|
|
Definition |
Example* |
|
Prepare |
Plan and train for responses and emergency patient care, anticipate potential resource shortfalls and likely adaptive strategies |
Cache equipment and common pharmaceuticals (e.g., narcotic analgesics, burn dressings, ventilators) (24), pre-incident mutual aid agreements with other facilities, and plans for staff and space adaptations in place |
|
Substitute |
Functionally equivalent device or supply used |
Benzodiazepines substituted for other sedation agents, alternate antibiotics when first-line unavailable |
|
Conserve |
Restrictions are placed on the use of therapies or interventions to preserve supply |
Oxygen is used only for patients with documented hypoxia |
|
Adapt |
Re-purpose a medical device |
Saturation monitors with rate alarms used in lieu of full-featured monitors, anesthesia machines used for temporary ventilators |
|
Reuse |
Re-use a device with appropriate cleaning, disinfection, or sterilization |
Re-use of cervical collars, nasogastric tubes, and other supplies |
|
Re-allocate |
Prioritization of therapy to those patients with the best chance of a good outcome, most likely to benefit, or with the least resource investment required |
Treatment of subset of patients with vaccine/antiviral treatments, prioritization of patients to receive mechanical ventilation |
*Note that these examples may be carried across the conventional/contingency/crisis continuum to reflect their impact on patient care. For more detailed information, see http://www.health.state.mn.us/oep/healthcare/standards.pdf.
SOURCE: IOM, 2009, p. 54.
Box 7-6 (repeated from Chapter 2) details the proactive plan components (familiar to those that utilize the “Planning P” in incident action planning) that will enable an institution to implement CSC, emphasizing integration with the incident command system.
Triage Decision Tools
The process and structure by which a facility moves from reactive to proactive triage decision making are what is critical, not the decision tools utilized; for example, burn triage, trauma triage, and influenza triage utilize different variables, but they should be used within a common facility concept of operations. Decision tools often change during an incident as more information becomes available about the disease-specific process, predicted demands, and resources that will become available or depleted. The clinical care committee should, as part of its work, identify relevant incident-specific prognostic indicators and share or obtain incident-specific information from other entities (e.g., RDMAC, state, CDC). During the 2009 H1N1 pandemic, for example, CDC circulated guidelines on high-risk patient characteristics and corresponding treatment recommendations (CDC, 2009a). These guidelines were widely used as a decision tool in allocating antiviral therapy to patients.
For therapies that are not binary—meaning they can be shared or titrated—consideration of minimum qualifications for survival may be relevant when the supply of that resource becomes scarce. The ceiling on resource use may be related to the patient’s prognosis and the resources available; it may not be an absolute
BOX 7-6
Implementation of the Surge Response Framework: Conventional, Contingency, and Crisis Response Cycle
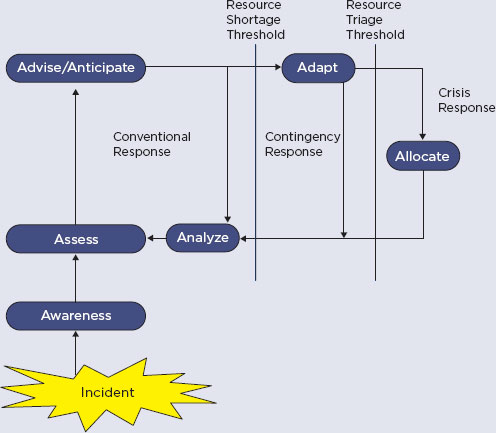
After an incident occurs, the first priority is to develop situational Awareness, and then to Assess the situation relative to the available resourcss. The incident commander, along with relevant technical experts and/or the clinical care committee (in a proactive response/longer-term incident) Advises on strategies and Anticipates any resource deficits (and recommends obtaining necessary supplies, staffing, etc.). If a resource is scarce, Adaptive strategies (such as conservation, substitution, adaptation, and reuse) should be implemented. In a crisis, a deliberate triage decision to Allocate/reallocate resources may be necessary. In all cases, the response and any strategies should be Analyzed at regular intervals as part of the disaster response planning cycle, and the elements repeated until the incident concludes. The terms in this figure can be further described as follows:
Awareness
• Incident commander recognizes current or anticipated resource shortfall(s) and assesses impact of current strategies.
Assess
• Technical experts are assigned to specific questions or areas of expertise.
• Clinical care committee performs assessment for more complex situations or when allocation of critical care resources is required during an ongoing incident.
• Logistics and liaison officers coordinate (across agencies) with suppliers, area public health and health care stakeholders, and emergency management as needed to obtain additional resources or assistance.
Advise/Anticipate
• Clinical care committee examines available resources, data, decision tools, and predictions of demand and determines possible adaptive actions. This analysis should also include what is happening within the region; the likely time frame for the crisis situation; and future impacts on demand, supplies, and staffing.
• Clinical care committee provides input to the planning section (or incident commander, depending on assignment) as to the specific adaptations necessary to accommodate ongoing demands and any recommended decision tools or policies. The committee also facilitates the transition back to conventional care as soon as possible.
• Public information and liaison officers coordinate with the planning section to ensure that the situation and adaptive strategies are included in risk communications provided to staff, patients, their families, and the community. A mechanism for addressing questions should also be available.
Adapt
• Clinical services are augmented or curtailed to allow the institution to focus on saving lives (e.g., subspecialty clinics may repurposed for outpatient acute care).
• Auxiliary equipment or spaces are utilized, including on-campus or off-campus alternate care sites, to support outpatient or inpatient overflow.
• Administrative changes involve little risk to patients and are usually the first adaptations.
• Changes are made in record-keeping and administrative duties.
• Ancillary personnel are used to provide basic hygiene and feeding services.
• Clinical changes involve escalating risk to patients and providers.
• Significant changes are made in shift lengths or number of patients supervised.
• Changes are made in criteria for evaluation (outpatient) and admission, as well as in criteria for admission to certain units (use of monitored units for critical care, for example).
• Changes are made in therapeutics, such as ventilation techniques and medication administration.
Allocate
• After approval of the incident commander, the plan is activated for the next operational period (during which the cycle begins again).
• Allocation policies are circulated (for example, use of medications or blood products).
• Reallocation decisions are made. A triage team is appointed if required for scarce critical care interventions, consisting of at least two specialists practicing and ex-
perienced in the clinical specialty affected (e.g., critical care, infectious disease, nephrology) (this team may be institutional, health system, or regional).
• Triage team utilizes decision tools to determine prognoses and, when a clear difference in prognosis exists, recommends treatment for patients with a predicted better outcome (first-come, first-served applies if there is no difference in prognosis substantial enough to justify reassignment).
• Triage team decisions are communicated to the medical branch director (or designated unit supervisor), who orders appropriate patient movement and actions to implement the team’s recommendations.
• Triage team decisions are documented in the medical record, as well as in the team’s daily activity log.
• Transition plans are in place to maintain the dignity and comfort of patients (and their families) who should have certain forms of care withdrawn or are receiving only palliative care.
Analyze
• Quality assurance is performed for ongoing allocation strategies: Is new information available? Are the policies and procedures appropriate for the situation being followed?
• Situational and resource information is updated, and the current strategies are analyzed, with feedback to the incident commander.
Resource Shortage Threshold
• The resource shortage threshold denotes the “indicators” (described in the committee’s letter report) (IOM, 2009) that demonstrate a point at which a potential or actual resource shortfall is recognized; however, substitution or other strategies may suffice to mitigate the problem.
Resource Triage Threshold
• The resource triage threshold denotes the “triggers” (described in the committee’s letter report) that demonstrate that specific resources are in short supply or are altogether unavailable. Therefore, an allocation schema must be implemented, and access to a specific care resource must be triaged because of demand. The triage decision involves an assessment of need, benefit, and duration of use.
limit, but at least prompts consideration of the impact of continued interventions (Beekley et al., 2007; Christian et al., 2010). This can be particularly useful with blood products and certain other medications to avoid committing the majority of an available resource to a minority of patients. In one series of military mass casualty patients, for example, each patient received an average of 3.5 units of packed red blood cells, but 4 of 24 patients (17 percent) consumed 43 percent of the blood products used (Propper et al., 2009).
Decision tools that predict patient prognosis are extremely helpful in the triage process, as they provide
• common criteria that can be applied in a relatively uniform fashion by multiple providers,
• objective indicators with which to determine prognosis (rather than gestalt),
• improved consistency of decisions across multiple providers and facilities,
• prognostic value that is evidence based, and
• a degree of protection from legal action if the provider is following published guidelines or facility plans in good faith.
The benefits and limitations of several commonly used triage tools are discussed in the following subsections.
Allocation of Life-Preserving Resources
Since the committee’s 2009 letter report was issued, incidents involving ventilator triage have occurred, most notably during the response to the Haiti earthquake (Burnweit and Stylianos, 2011; Ytzhak et al., 2012). The decision process considered organ system function, prognosis, and duration of resource use, consistent with prior Institute of Medicine (IOM) and other recommendations. While the process and criteria used were considered valuable, the experience in Haiti reinforced the reality that prognosis in disaster situations is rarely well defined; therefore, the reassessment of patients who did not receive intervention is an important part of the ongoing triage process (Ytzhak et al., 2012).
Recent additions to ventilator stockpiles at the federal (CDC, 2011b), state, regional, and local levels have decreased the chances that triaging of ventilators will be necessary in the United States, although it is still a real possibility during a major pandemic (notably, development of a universal influenza vaccine would render most ventilator triage scenarios moot). In some cases of mass respiratory failure (e.g., mass chemical exposure, burns, local epidemics, terrorist use of botulism), temporizing the use of bag-valve ventilation is reasonable when additional resources will become available in a timely manner and adequate personnel are on hand. Although some authors have advocated for mass use of bag-valve ventilation (Trotter, 2010), several factors argue against its use in an epidemic/pandemic situation except in isolated instances or as a temporizing measure. These difficult resource allocation decisions need to be made in the context of the incident by the facility and community (Box 7-7).
With growing interest in ECMO as salvage therapy for refractory hypoxemia comes a higher likelihood that access to this therapy may have to be triaged, even during severe seasonal influenza years, because of the small number of institutions providing it. Note that ECMO at present is not considered standard critical care for these situations, but evidence and practical experience in this regard are evolving (ANZ ECMO Investigators, 2009; Noah et al., 2011; Peek et al., 2009). The use of ECMO entails the following considerations:
• The total ECMO capacity within a community and region should be known prior to an incident, and staff providing ECMO should consider possible related surge needs, including catheters, oxygenators, and staff. Equipment requirements for ECMO continue to evolve, with simpler, smaller machines and catheters now available (Muller et al., 2011).
• In an epidemic, staffing, space, and supply constraints may require that ECMO (or other intensive care therapies) no longer be offered, as the resource commitment is unjustified compared with the
BOX 7-7
Considerations Regarding Bag-Valve Ventilation of Patients
• B ag-valve ventilation is appropriate, even for a large number of patients, while additional supplies or patient transfers are being awaited, in particular for chemical or inhalational (Darcy, 2003) incidents and power failures (Barkemeyer, 2006). In short-term situations, hospitals should be prepared to provide bagvalve ventilation to a large number of patients (usually constrained by oxygen delivery rates [see below]), as these devices are inexpensive and usually available in large quantities in major hospitals. If the patient is intubated, which should be the case for any prolonged intervention, the technique is easy to learn (Lin et al., 2009).
• B ag-valve ventilation consumes large volumes of oxygen with constant flow rates usually ranging from 10 to 15 liters/minute, compared with the small volumes used by ventilators. Hospital oxygen systems are not designed to operate with high flow rates being delivered to more than a fraction of non-intensive care rooms. Portable oxygen systems similarly are not designed to provide high flow rates of oxygen. Thus, significant pressure drops in the system may occur if multiple bag-valve units are in use.
• B he physical effort to provide bag-valve ventilation is substantial. Some members of the committee have had personal experience with this in austere settings for up to 48 hours, and can attest that these efforts require multiple persons, and providers can usually bag for no more than 1 hour at a time.
• B oom air ventilation without supplemental oxygen is extremely unlikely to benefit patients with pneumonitis from influenza, who usually have significant and sometimes refractory hypoxemia, although it may have limited application in muscular disorders such as botulism (or, historically, polio) (West, 2005).
• A irway resistance is usually high and ventilatory management can be difficult for patients with pneumonitis, and these conditions are unlikely to respond well to bag-valve ventilation or simple, pressure-cycled ventilation.
• I t is ethically inappropriate to allow patients to be ventilated by family members while others without family members do not receive the same support. The facility clinical care committee and ethics committee should determine how to handle these situations, as they are likely to arise and will require a thoughtful response. Additionally, individuals unable to keep up with the physical requirements of bagging may feel that they have contributed to the patient’s death.
life-saving potential those resources would have for a larger number of patients. The clinical care committee should be prepared to examine this possibility, especially when highly intensive therapies are being provided.
• Triage decisions in this setting may have to be made in the absence of any state declaration of emergency or activation of a full incident response by the facility. Critical care, cardiothoracic, and ethics committee members should have a plan for making decisions in these situations, including the process to be followed, documentation to be required, and any recommended decision tools.
Sequential Organ Failure Assessment Scores
The development of tertiary triage schemas has focused on the triage of mechanical ventilation (Christian et al., 2006), as this has been viewed as a life-saving resource with limited availability. The most commonly utilized decision tool in triaging of mechanical ventilators has been the Sequential Organ Failure Assessment (SOFA) score (Lemeshow et al., 1993; Moreno et al., 1999; Pettila et al., 2002; Vincent et al., 1996, 1998), as it relies on minimum clinical variables and is easier to calculate than other predictive models. Some authors have recommended use of a Modified SOFA (MSOFA) score (Grissom et al., 2010) that requires even fewer laboratory variables. Although MSOFA is promising, studies confirming its predictive value are as yet relatively small, and some of the assumptions MSOFA makes (including elimination of some categories of scoring) have not been examined carefully. MSOFA scores, if obtained, should not be compared directly with SOFA scores because of these differences (Rubinson et al., 2010). In limited studies, some authors have examined adding more factors to the SOFA score (Adeniji and Cusack, 2011). A simpler assessment tool or laboratory value capable of predicting mortality with accuracy across multiple underlying causes of organ system failure (e.g., infection, trauma) would be welcome, but at present no such tool or value is available.
While these scoring systems have the potential to standardize decisions on the allocation of scarce resources, they are subject to the following limitations:
• SOFA and other scores are predictive in retrospective cohorts, but their use in prospective systems has not been validated (Zygun, 2005). Thus, the difference of a few points among SOFA scores may be significant in a large retrospective cohort but of minimal significance when used in a prospective fashion. For example, a difference of 2 points on the SOFA scale may indicate a survival probability of 20 percent versus 35 percent, but predicting prospectively which 20 or 35 of 100 patients will survive is impossible; thus the difference of 15 percent is not significant (IOM, 2009).
• The mortality of the underlying disease process is critical in determining prognosis. This is why SOFA performs poorly in influenza patients, where the mortality of the underlying disease process is relatively low compared with that of septic shock. Thus if the SOFA sensitivity is 80 percent and the mortality of septic shock is 80 percent, the death rate will correlate well with the score; if influenza mortality is 20 percent, the death rate correlation will be poor (Khan et al., 2009; Rubinson et al., 2010). A recent study found that a SOFA score of 11, which has been used as an exclusion criterion in some triage schemes, was associated with a mortality range of26-67 percent, depending on the underlying pathology (Shahpori et al., 2011).
• Scoring systems do not account for disease- or condition-specific factors, which are critical. All workgroups and committees considering issues of critical care triage should ensure that disease-specific factors enter into their decision process.
• Failure of a score to improve over a selected period of time is generally a poor criterion. Static, very high scores may be a helpful predictor, but failure to improve is irrelevant when the scores are lower or when the underlying pathology predicts the need for a prolonged course of therapy (e.g., acute respiratory distress syndrome [ARDS]) (Khan et al., 2009).
Other Considerations for Triage Decisions
Numeric scores and disease-specific factors provide information about prognosis, but other factors may need to be weighed. The American Medical Association has published guidelines on transplant organ allocation that include and support these factors (AMA, 1995). The committee proposes that triage teams consider the following factors in their decision process:
• the prognosis of underlying diseases and any severe limitations on life span that this implies (e.g., severe underlying heart or liver disease);
• the resource commitment and duration (e.g., consideration of the duration of ventilator use for flash pulmonary edema versus ARDS or use of minimum qualifications for survival to determine ceilings for the commitment of blood product resources);
• ongoing resource needs—not likely to be relevant in the United States, but a consideration in certain situations (In Haiti after the earthquake, for example, the context of the resource scarcities at the country level led to the consideration of whether short-term interventions were likely futile in the long term because of the broader limitations of medical care [e.g., intensive treatment for high spinal cord injury.]) (Merin et al., 2010); and
• age, a medical factor in certain situations, such as burn or trauma, in which advanced age is a clear contributor to increased mortality (discussed below).
Although age clearly affects mortality in trauma and burn situations (Kuhne et al., 2005; Saffle et al., 2005) and can impact overall survival (Lieberman et al., 2009), there is substantial physiologic variability among elders of similar chronologic age (Society of Critical Care Medicine Ethics Committee, 1994b). The ethics section of Chapter 4 provides a more detailed discussion of age as a factor in triage decisions. It should be noted that there is no currently accepted scoring system for pediatric patients (Antommaria et al., 2010). Common scores (Pollack et al., 1996) require a significant number of laboratory values and are relatively complex. This is an area that requires additional research and policy work. A recent CDC workgroup on pediatric critical care in disaster situations did not recommend a pediatric-specific system (Christian et al., 2011). However, consistent with the ethical framework previously discussed, any scoring system must be fair and equitable.
A Schema for Making Triage Decisions
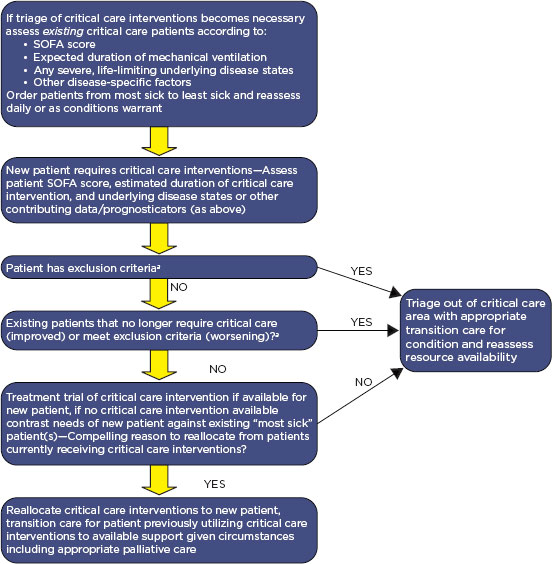
Having considered currently available decision tools, the committee continues to support the triage schema originally proposed by Devereaux and colleagues (2008) (and adopted or adapted by others [Christian et al., 2010]) when triage of life-saving, binary resources (e.g., ventilators that cannot be shared or titrated) is required (Figure 7-1). However, the committee does so with the following comments and caveats:
• Decision tools should not be used to exclude patients preemptively from use of life-saving resources when these resources are available. Even in an epidemic, available resources will vary among facilities, and if a resource is available (e.g., a ventilator), it should be provided to a patient in need unless the clinical care committee finds compelling reasons for not doing so—for example, if the demand
FIGURE 7-1
The basic triage process.
NOTE: SOFA = Sequential Organ Failure Assessment.
aExclusion criteria should be limited if utilized, and may include factors, such as age extremes or organ system failure with extreme life span limitations or severe, irreversible neurologic compromise, that the community agrees upon. SOURCE: Adapted from IOM, 2009, p. 87.
rate is so high that it is certain the patient will not have the resource for more than a few hours. It is notable, however, that even at the peak of a moderate pandemic, an average level 1 trauma center was calculated to receive a patient in respiratory failure only once every 1.3 days, based on CDC FluSurge predictions and local data.5 This decision to provide life-saving resources when they are
_________________
5 Hennepin County. Minnesota data used in the CDC FluSurge predictive model, available at: CDC (Centers for Disease Control and Prevention). 2009. FluSurge special edition. Atlanta, GA: CDC, http://www.cdc.gov/h1n1flu/tools/flusurge/ (accessed March 5, 2012).
available regardless of the patient’s prognosis was reinforced by experiences in Haiti, where the decision was made to provide resources that were available until there was competition for them (Ytzhak et al., 2012).
• Incident-driven decision tools may be developed to direct care (e.g., antiviral medications) to groups of patients who are in greatest need or who stand to benefit the most. However, these tools should emphasize the need for flexibility in the triage process and reinforce the idea that the process for decision making, not the decision tool, is the key component of crisis care planning.
• Disease-specific predictors of mortality should be the dominant factor in decision making when prognostic information is available (Singanayagam et al., 2011). This emphasizes the need for the SDMAC and RDMAC to tailor guidance to the incident, and for epidemiologic data to be gathered in a timely manner and incorporated as they become available.
• A specific SOFA score should not be used to exclude or differentiate among treatment/allocation groups because prospective correlation with mortality is not sufficiently accurate to be the sole driver of allocation decisions. SOFA scores may be used to compare prognoses among patients requiring a critical care therapy, with the limitations noted previously.
• Factors incorporated into decision tools should be validated and follow accepted ethical and community principles. Incorporation of invalidated variables is not recommended (e.g., the Glasgow Coma Score, which, despite its good predictive ability in certain head injury cases, is not accepted as a medical triage criterion).
It may be hoped that progress in the field of triage decision tools will lead to the identification of better predictors of mortality that will allow health care providers to determine patient outcomes accurately and prospectively. Until that time, however, resource allocation decisions will have to rely on measures and assessments that, while imperfect, at least prompt consideration of the key clinical factors in a structured process.
Implementation Issues for Crisis Standards of Care
A broad spectrum of responses and resource deficits is possible within crisis medical care. The scope of the guidance required from the clinical care committee may range from circulating general guidelines for the use of antivirals to ceasing all but emergency department operations and providing only basic emergent interventions (airway, wound, and comfort care) during a disaster. In some situations, radical changes to usual practice are required, but are appropriate for the situation (Lin et al., 2010). It is the responsibility of the clinical care committee and incident commander to ensure that transitions to crisis care are as graceful as possible, as more and more resources are committed to certain areas while other care activities (e.g., specialty clinics, outpatient and elective surgeries) are deferred. It is crucial that institutional support be provided for what otherwise might be controversial decisions in implementing CSC. As noted earlier, however, no-notice incidents can require immediate adaptations; therefore, key providers should be familiar with triage and surge plans for their area and be prepared to implement them without formal guidance.
Implementing CSC often is not an intuitive process, as daily medical care is extremely patient focused. Thus when faced with scarce resources, providers may be subject to “cognitive lock” (Aarts and Dijksterhuis,
2000) in which they default to the choices they usually make and with which they have experience. All personnel who may be in a position to make triage decisions or will be participating in a command or supervisory role during a response should understand the transition that occurs from considering the needs of individual patients to considering the needs of the community. Written prompts in response plans and job aids, as well as experience with exercising hospital CSC plans, can facilitate provider choices that balance a broader range of needs but also reflect an understanding of the facility’s core ethical goals.
This section describes the core functions and associated tasks of hospital facilities and hospital providers in CSC implementation that are included in Template 7.1 at the end of the chapter.
Hospital Facilities
Function 1. Alerting. The hospital should be able to receive a broad range of communications from public health agencies, other hospitals, EMS, poison control, emergency management, and other partners. Although notifications for a mass casualty or weather incident often are provided by web or radio systems that are monitored around the clock, the actions that are taken and each party’s responsibilities should be clear. More difficult is ensuring that the multiple health alert, email, and other updates are captured during longer-term incidents and incorporated into the incident management process; for example, a health alert or CDC bulletin sent by e-mail during a weekend may not reach a recipient in a timely fashion, or there may be no accountability for getting that information to the situation unit leader. Expectations for the monitoring and processing of information should be clear prior to an incident.
Activation of the CSC plan should begin with recognition by the incident commander that a scarce resource situation exists or may exist, and therefore requires proactive management beyond immediate requests for resources and assistance (thus, the incident is likely to be longer term). Activation may be based on triggers (Table 7-4) or on identified indicators that predict progression to crisis conditions (e.g., epidemiologic forecasts, demand on intensive care beds, or other community or facility indicators). Further discussion of indicators and triggers is found in Chapter 2 of this report.
Function 2. Notification. Hospitals should predetermine the groups that will be notified if a specific incident occurs, such as a mass casualty, HAZMAT, or epidemic incident. Hospital staff should understand how they will be contacted, what their responsibilities are, and where they are to report during an incident. Personnel expected to serve on a clinical care committee should be assigned to one of these groups if possible, with other technical experts being added according to the needs of the incident. All participating personnel, including any backup personnel, should clearly understand their responsibilities and exercise their roles prior to an incident. Provision of crisis care should prompt notification of other hospitals in the area, as well as local and state health or emergency management authorities, depending on local plans. This can be facilitated through the Tier 2 health care coalition role in situational awareness and supporting communications about resources.
Function 3. Command. Hospital personnel should be trained in a National Incident Management System (NIMS)-compatible incident management system (such as a hospital incident command system [HICS]) (EMSA, 2007; FEMA, 2011) according to their roles and responsibilities. Command staff, especially those who have responsibilities to interact with agencies outside of the hospital setting, ideally should be trained at the incident command system (ICS) 300/400 level (FEMA, 2007a,b), which emphasizes incident action planning, a key component of incident management during a prolonged incident.
The incident commander directs planning and logistics, in coordination with the operations section, to determine options for ameliorating a scarce resource situation. If it is clear that proactive approaches are required, and they are not self-evident to the incident commander and/or will be necessary over a prolonged period, the incident commander should task the clinical care committee to develop strategies for addressing resource shortfalls. In some cases, a single or few technical experts (e.g., in pharmacy) may be required to address the situation. In more complex cases, particularly if proactive triage of life-saving resources is required, the full clinical care committee is likely to be needed. Generally, if specific or intermittent input is required, the technical specialists directly inform the incident commander or operations section. When a technical unit (such as the clinical care committee) is required for ongoing analysis and input, it generally is located within the planning section (Figure 7-2) (FEMA, 2011).
An incident commander’s authorities are delegated to him or her, usually by the hospital administrator. The process for delegation and specification of scope of authorities should be outlined in writing prior to an incident, if possible. During a crisis, close communication and involvement with the administrator are required, as accountability for the strategies and tactics employed should belong, to the extent possible, to the institution as a whole rather than to individuals. Individual decisions made in crisis settings, particularly under severe emotional and physical strain or in unfamiliar areas of expertise, may place both patients and providers at risk (Fink, 2009).
TABLE 7-4
CSC Triggers by Category
|
Category |
Trigger |
|
Space/Structure |
Need to use non-patient care locations for patient care (e.g., cot-based care, care in lobby areas) to accommodate demand; specific space resources overwhelmed (operating rooms), and delay poses a significant risk of morbidity or mortality; disrupted or unsafe facility infrastructure (damage, systems failure) |
|
Staff |
Specialty staff unavailable to provide or adequately supervise care (pediatric, burn, surgery, critical care) in timely manner, even after call-back procedures have been implemented |
|
Supply |
Supplies absent or cannot be substituted for (e.g., absence of available ventilators, lack of specific antibiotics), leading to risk to patient of morbidity |
|
SOURCE: IOM, 2009, p. 64. |
|
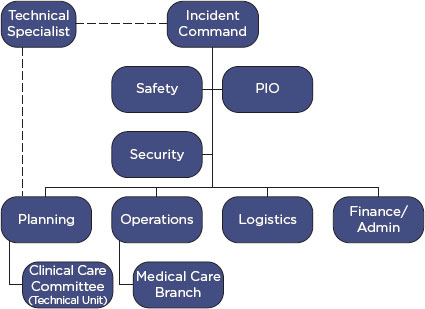
FIGURE 7-2
Usual location of technical specialist(s) and technical units within the incident command framework.
NOTE: PIO = public information officer.
Function 4. Control. Incident command training should be supplemented by facility- and department- specific training and exercises, as familiarity with incident management does not correlate with competency in initiating or supervising a departmental response. Staff at all levels should attain competency in facility protective actions (e.g., securing of entrances/exits, whom to contact to manage the ventilation system) and expansion or reassignment of their area’s resources to support the incident response. Some of these actions will be predetermined—such as central supply bringing a disaster cart to the emergency department in a mass casualty incident—while others will be implemented on an as-needed basis by the incident commander, often with input from the clinical care committee or technical experts. Job action sheets and response guides (Hick et al., 2008) should provide initial information to unit supervisors and command staff about how their units’ space and staffing will expand should there be a need to transition from conventional to contingency and even to crisis care.
Function 5. Communications. Internal communications to patients and staff, as well as to external staff and, optimally, patients’ families, are critical. Hotlines, the Internet, text messaging, e-mail, written letters, updates on social media (at a minimum Facebook and Twitter), and other means of communication may be used to provide incident information. It is helpful to provide updates both at scheduled times and when new information is available. The public information officer serves as the conduit for information to the internal and external stakeholders, including staff, visitors, families, and news media, as approved by the incident commander (California Emergency Medical Services Authority, 2006a). Following ICS principles, a process should be in place for rapidly vetting new information or status
changes from general staff and other command or technical specialists via the public information officer, as approved by the incident commander.
Function 6. Coordination. A large part of incident management for a hospital is working with EMS and public health/emergency management to manage, to the extent possible, the flow of victims to the facility. If a hospital is overwhelmed and other facilities have capacity, EMS and public information can help avoid further burden on the affected hospital and organize the transfer of patients or resources as needed to restore the facility to contingency and eventually to conventional footing. Accomplishing this involves coordination among command staff, the liaison officer, and the public information officer to assess the situation and make appropriate requests to the jurisdictional EOC or EMS agencies/media consistent with the community plan. The EOC, in turn, will need a liaison to speak for area hospitals and help coordinate information and a common operating picture for health care that will drive resource requests and actions from the EOC. Without coordination mechanisms, a hospital can easily become an “island,” as happened at Charity Hospital in New Orleans after Hurricane Katrina (Deboisblanc, 2005). If a regional health care coordination center or multiagency coordination center (FEMA and Emergency Management Institute, 2008) is activated, the hospital should understand the authorities, resources to support coordination, and purpose of and how to interface with this entity.
If proactive triage of resources is necessary, command staff should understand how the hospital can provide input into the deliberations of the state and/or regional disaster medical advisory committee and receive guidance on implementing guidelines and triage mechanisms. This coordination helps promote regional consistency. A regional system for coordinating patient transfers, if in use, potentially can affect mortality by “gatekeeping,” or triaging the transportation of patients with key underlying needs to regional centers (Kanter, 2007; Kirby, 2010; Noah et al., 2011).
Function 7. Public Information. Providing the public with clear messages about when and where to seek care is a priority in a stressed health care system. The bigger the incident, the more important this issue becomes. To get effective messages out in a timely manner, the hospital will need to coordinate with its usual media sources via the public information officer (FEMA, 2007c), but also work closely with any joint information system (JIS) (FEMA and Emergency Management Institute, 2010), usually managed at the jurisdictional or state EOC level. The JIS ensures consistency of messages and provision of these messages to the media. If public health, health care, and EMS lack consistency in their recommendations for when and where to seek care, when to use 911, and so on, the public will quickly become confused, and trust will be lost.
Managing expectations during an incident is extremely important because a clear understanding of resource limitations gained from the major media at least facilitates a “frame shift” for patients seeking care and health care providers. Messages should include what the institution is doing, why, what the priorities are for the hospital and its patients, and what is being done at other levels to address the problems.
Function 8. Operations. The operations section, including the triage team and clinical care providers under operations, is responsible for developing and implementing strategies and tactics needed to meet
incident action plan objectives as approved by the incident commander (see Figure 7-2 above for operations’ position on the abbreviated ICS organizational chart) (California Emergency Medical Services Authority, 2006b).
Especially in a no-notice incident, the operations section chief may be responsible for a wide variety of tasks, such as facility assessment and evacuation, patient triage and treatment, and the expansion of clinical care areas. The section chief should be well versed in gaining situational awareness and promoting communication with the clinical units, as well as with the command staff. Delegation is critical to ensure that strategies and tactics are properly implemented. Job aids can facilitate the process of situational assessment and guide initial actions. These aids may include job action sheets, initial action prompts or assessment tools, tables reflecting expansion or evacuation needs, and other resources (Hick et al., 2008).
Based on the situational assessment, the incident commander or appropriate section chief should decide how much to expand or “surge” clinical care (California Department of Public Health, 2008). Default actions may be taken when a disaster alert is called. In a mass casualty incident, for example, surgeries may be held and postanesthesia care and preinduction areas cleared for patient care. Conventional capacity can easily be maximized by summoning additional staff. Expansion to contingency and, if necessary, crisis capacity should be template driven and may involve space and supply adaptations in addition to staffing changes. During the 2009 H1N1 pandemic, for example, facilities had success remaining in conventional operations by implementing their surge plans (Meites et al., 2011). Table 7-2 provides an example of a template expansion plan. These templates should be supported by policy and other documents, and, while they may take many forms, are useful as a quick reference. If it is clear to the operations section chief that crisis capacity should be utilized, the incident commander and planning section chief should be made aware so that external assistance can be sought or plans made to cope with the demand. It is fundamentally important that a decision to implement CSC not be made independently, but jointly with other health care institutions in the region. In the HICS, the operations section’s infrastructure branch is responsible for maintaining hospital infrastructure, including power, water, HVAC (heating, ventilation, air-conditioning), medical gases, and environmental and food services. It will be important for the operations section to coordinate infrastructure with the planning and logistics sections in developing surge capacity during conventional, contingency, and crisis conditions (California Emergency Medical Services Authority, 2006b).
The medical care branch director implements the incident action plan for clinical care. He/she may be the first to recognize an impending shortfall of resources and alert the incident commander and operations section chief. In a crisis, they should oversee and be accountable for the actions taken at the unit level (e.g., emergency department, intensive care) and any triage processes. Their input to the clinical care committee is crucial to the committee’s understanding of the existing challenges and needs, as well as how the strategies and tactics in use are working or failing. The clinical care committee should work with the medical care branch director to determine what services the hospital can provide and how and where to provide them, and to recommend to the incident commander courses of action for coping with the scarce resource situation.
The clinical care committee also should determine crisis clinical policies for the hospital, which can include the surgeries that may be performed, what triage criteria the emergency department will use
BOX 7-8
Appeals
A process appeal is an appeal generated when an invested individual (family member or patient’s clinician) believes that a decision was arrived at unfairly or deviated substantially from guidelines without justification. This is a retrospective appeal, and requires that the clinical care committee examine documentation and discuss the case with the triage team members and additional technical experts. If there are findings of an unfair or unjust decision, a process should be in place for communicating this to the invested individual(s). Regionally, there may be an appeals committee that examines these cases if there is any initial finding of merit. Note that this is not a legal proceeding, but essentially an ethics opinion on whether triage personnel executed their duties in good faith.
A clinical appeal is an appeal generated when the patient’s clinician believes the clinical data used for the triage decision do not reflect recent improvements in the patient’s condition. This is an urgent appeal that, if the triage team reconsiders, may affect the clinical decision. Clinical staff should be aware of the mechanism and indications for initiating such an appeal.
based on volume, what patients may be seen in what clinics, and what adjunct spaces and equipment are to be used for critical care (Rubinson et al., 2008b). Recommendations on when and how to implement substitution, adaptation, conservation, or reuse/reallocation strategies for specific resources also may be required (Hanfling, 2006; IOM, 2009; Minnesota Department of Health, 2011; Peleg and Kellermann, 2009; Rubinson et al., 2008a,b). These recommendations should be developed in close collaboration with the clinical departments and the medical care branch director prior to adoption. The clinical care committee also should provide any required modifications to guidelines and triage tools that are available from other sources, including regional and state disaster medical advisory committees. Examples of how this process has been structured are available in the literature (Frolic et al., 2009; Kaposy et al., 2010).
Finally, the clinical care committee is responsible for quality assurance of allocation and triage decisions, including review of the decisions and related documentation and discussion with clinical staff and triage team members about pending process modifications that might aid their performance. The clinical care committee also should review any process appeals (that is, any challenge to a triage decision on the basis of faulty reasoning or malfeasance) and either address them or refer them to a regional appeals committee (if established) (Box 7-8). Process appeals are retrospective and do not change the allocation decision (Debruin et al., 2010).
A triage team is used when proactive triage decisions are made regarding the allocation of scarce, potentially life-saving interventions (for example, mechanical ventilation and ECMO). The team should comprise at least two physicians trained in critical care or with substantial expertise in critical care decision making (or in the specialty area within which the allocation decisions are being made) (Hick et al., 2007; IOM, 2009).6 These physicians may be supported by other technical or ethics personnel at the
_________________
6 It may be advantageous to have an odd number of individuals serve on the triage team.
facility’s discretion. They should review objective evidence for the patients requiring the intervention and determine who should receive the resources available. These decisions are then communicated to the medical care branch director or designated unit leader (e.g., critical care unit leader) for action.
Optimally, triage team members should understand their possible roles and have exercise experience in making such decisions prior to an incident to ensure their familiarity with the operational components involved (including, e.g., patient data, work flow, documentation). Note that it would be unusual for a facility triage team not to be available for other duties most of the time, as proactive triage decisions will be relatively infrequent; a mechanism for conference calls or other decision making should therefore be available. However, it is not ideal for the triage team members to be the clinical care providers for the patients they are considering, as it is difficult to remain a patient advocate and avoid bias due to knowledge of the full scope of the patient’s situation (Kirby, 2010).
The team should document its decisions in both the patient chart and a unit log. Clinical documentation for those not receiving resources should follow a template and reflect the current situation, the demands of the incident, and the data considered in the decision relative to those patient(s) who received the resources. Unit staff should document the transition of care and continued palliative or other ongoing care, as well as communications to the family and the patient if they are able to understand the situation. Reevaluation of these patients is important to ensure their continued consideration for resources as the incident and their conditions evolve (Klein et al., 2008). The legal and ethical implications of withdrawal of care are substantial, and should be examined with the assistance of legal counsel in advance of an incident in conjunction with analysis of applicable state laws (see Chapter 3) (Eastman et al., 2010).
Given the expertise involved, coalitions or health systems may elect to have centralized, regional, or even state-based triage teams to facilitate decision making at multiple sites, with the added benefit of maintaining situational awareness across multiple facilities. In these cases, a process for ensuring documentation of the decision process in the patient’s medical record is essential, whether in the form of a dictation, faxed or e-mailed template, or other mechanism.
If a resource is being assigned among persons not yet receiving it, it should be assigned to those patients with the better prognosis. An ethically fair triage process requires that physicians use the best available data and system to assess patient prognosis. Once this step is accomplished, some patients will have an essentially equal prognosis. When the medical prognosis is equal, any allocation scheme must ensure consistency in order to be fair. Community engagement strategies (see Chapter 9) may help solicit community values regarding prioritization of care schema, such as prioritizing patient age or using a first-come, first-served or lottery approach. If such engagement processes have not yet occurred, an allocation system should follow a consistent and fair approach, and the health care system should communicate that strategy broadly to the public. Close coordination among the health care institution and regional and state entities is thus required to prevent inconsistencies in triage when medical prognoses are equal, and the state ideally should define secondary processes to be followed, which should be understood by providers.
The threshold for withdrawal of a critical resource for reassignment to another patient should be much higher. The patient who is using the resource should, in the judgment of the triage team, have a substantially worse prognosis to justify withdrawal and reassignment of the resource. Therapies are
not assigned in this setting, but offered as therapeutic trials; the triage team should weigh whether the patient with the resource has had an adequate trial of the therapy with respect to prognosis and benefit. Patient condition and clinical data should be reexamined at least every 24 hours (although, as noted above, failure to improve over this period of time may be expected rather than indicate failure of treatment).
More triage decisions are likely to be required early in an incident when, using influenza management as an example, patients already on ventilators are likely to have more organ system failures and poor predicted survival compared with healthier patients with more isolated respiratory failure. As this cohort of patients is ventilated, it will be less and less likely that arriving patients will have a substantially better chance of a good outcome, and thus few reallocations of ventilators will occur.
The triage team may occasionally receive clinical appeals and may need to reconsider its decisions if there has been a substantial improvement in parameters and/or prognosis. The institution should have a process in place for requesting these appeals and communicating any appeals holds or changes in decisions to unit staff, as well as mechanisms for ensuring that timely data are supplied to the triage team.
Triage situations will have a profound emotional impact on patients, families, and providers. Mental health issues should be addressed in a proactive fashion by the incident command team (see Chapter 4 for detail on these issues).
Mental health under CSC will require specific competencies of mental health, social services, and health care staff. Efforts also will be required to enhance community resilience through “neighbor-to-neighbor, family-to-family” support systems (such as certain psychological first aid models created specifically for use by community members as needed). The resilience of the health care workforce is paramount to the success of the CSC strategy.
One-shot, one-size-fits-all approaches, such as some once-common stress debriefing, are no longer recommended and may result in exacerbating the mental health problems of those most affected by a disaster (Bisson et al., 1997, 2007; IASC, 2007; McNally et al., 2003; NIMH, 2002). The replacement for those outmoded approaches is more integrated efforts to enhance the resilience of the workforce specifically with respect to mass casualty events, including CSC, as part of CSC preparedness (Schreiber and Shields, 2012).
Hospital incident command operations need to encompass integrated mental health operations as part of ICS/EOC and medical/health operations. Recent models developed for Los Angeles County, Seattle/King County, the American Red Cross’s National Operations Center/Disaster Mental Health, and a new national prototype specifically for children utilize real-time situational awareness of triage/ mental health risk in patients/disaster victims and responders (including health care workers and their families) across varied disaster systems of care (e.g., hospitals, schools, shelters, public health settings) to guide actual mental health operations within the ICS (see Schreiber et al., in press). Other recommended features include a common operating picture of
• population-level mental health risks (traumatic loss, multiple traumatic losses) using a common rapid mental health triage system across disaster systems of care;
• mental health risks among health care workers; and
• mental health resources, including emerging national models of Internet-based intervention (Ruggiero et al., 2006).
Addressing the social and psychological challenges of CSC requires a triage-driven mental health incident management system and community resilience efforts through community engagement (see Chapter 9). Also required are basic “neighbor-to-neighbor, family-to-family” psychological first aid competencies that leverage the community, responders, and family members as the first line of psychosocial support (see the American Red Cross’s “Coping in Times of Crises” and the “Listen, Protect and Connect” psychological first aid models).
Palliative care focuses on the relief of suffering and distress (e.g., pain, nausea) during serious, lifethreatening illness to help patients and families have the best possible quality of life. The emphasis is on coping, comfort, and well-being. One goal of disaster response is to provide comfort to the most people possible. Therefore, efforts to plan for appropriate palliative care for all victims are a high priority, along with caching and adequate use of medications to provide comfort (Bogucki and Jubanyik, 2009; Matzo et al., 2009). During triage situations, planning for thoughtful care transitions if support and interventions are unavailable is critical to maintaining comfort and dignity. Multidisciplinary planning is helpful to identify processes and interventions that can be implemented at the hospital and support that can be offered to patients and their families. Planning in advance for these activities is as critical as planning for the triage process, yet often is overlooked; the result may be greatly increased suffering and emotional distress for all during an incident (Downar and Seccareccia, 2010). More in-depth discussion of palliative care planning and the needs of patients can be found in Chapter 4.
Function 9. Logistics. Logistical planning for scarce resource incidents begins with anticipating possible deficits (see Appendix C) based on
• hospital location (geographic risks of facility impact and isolation by natural, terrorist, or other incidents);
• hospital role in the community (e.g., trauma center, children’s hospital);
• fragility of vendor supplies and anticipated supply lines; and
• facility goals and resources.
Often, hospitals in a geographic area rely on the same vendors for supplies of medical equipment (such as hospital beds and ventilators), which can lead to rapid depletion of these items during an incident. Also, vendors may not be able to deliver items because of access problems. Hospitals should determine minimum amounts of equipment to be kept on hand. Durable medical equipment is expensive, but retaining monitors, ventilators, and hospital beds that have been removed from service may be a good strategy. Increasing par levels of medications and supplies can be difficult in times ofjust-in-time inventory management, but often there are no good substitutes for inexpensive caches of medications (e.g., narcotic analgesias) that are rotated through stock. Forecasting demand can reveal staggering supply needs, especially during a prolonged incident (Hota et al., 2010).
The logistics section provides for maintenance of the physical environment, providing human resources, materiel, and services to support the incident response activities. The logistics section should coordinate with the operations and planning sections to expand alternate care locations (California Emergency Medical Services Authority, 2006c). Space expansion plans should include planning for both inpatient and outpatient surge, and may require preincident or just-in-time modification of spaces, including creation of temporary walls, changes in room configurations, ventilation modifications, or other changes. Predictive and historical demand forecasting can yield helpful information about the likely impact on the institution (Sills et al., 2011). In addition to a surge of patients, accommodations may have to be made for the family members or pets of staff during an incident that severely damages community infrastructure.
The logistics section also is responsible for the labor pool and credentialing unit, a collection point for available hospital staff and volunteers that may be a resource for addressing staffing shortages (California Emergency Medical Services Authority, 2006d). Staffing patterns and shift lengths may be changed during an incident, although such changes should be balanced against the detrimental effects of fewer staff per patient, less experienced staff, and fatigue (Cheung et al., 2008; Clarke et al., 2002; Gershengorn et al., 2011; Needleman et al., 2002). Consistent with the Assistant Secretary for Preparedness and Response’s (ASPR’s) Emergency System for Advance Registration of Volunteer Health Professionals (ESAR-VHP), an adequate staff must be held in reserve, especially in no-notice incidents, when many staff may self-report and then be unable to supplement shifts later that day or night. Agreements for obtaining and integrating additional staff from the Medical Reserve Corps, federal teams, and local sources should be in place prior to an incident (ASPR, 2011; HHS, 2012). The logistics unit should make requests to the EOC or partner facilities and ensure adequate credentialing, check-in, privileging, orientation, and supervision. Use of supplemental personnel should conform to the hospital’s staffing bylaws and policies.
Special challenges during an incident may include the need for patient isolation, decontamination, or special equipment. Managing contaminated belongings and washwater, creating negative airflow or isolation areas, and ensuring that adequate equipment is available for pediatric or burn patients in advance of an incident, as well as identifying multiple vendors and sources for resupply, can greatly reduce the potential for scarce resource situations and prevent staff exposure to harmful agents.
Another challenge is providing for the nearly one-third of the U.S. population that qualifies in some manner as at-risk, whether by virtue of functional limitations, age, medical conditions, pregnancy, or mental health problems (among other factors). Hospital planning should focus on those factors that require specialized planning, training, or equipment, such as the following:
• Maternal health: Pregnant patients represent two lives to be saved, and they may be at higher risk of complications from influenza or other disease processes or trauma. Considerations for planning for a crisis with respect to maternal health include (Beigi, 2007; Rasmussen et al., 2008)
![]() Triage: Discussion should encompass whether pregnancy results in triage priority when other factors are relatively equal. A model for triage of pregnant patients has been proposed, but it does not address how such decisions are integrated with decisions about other patients being
Triage: Discussion should encompass whether pregnancy results in triage priority when other factors are relatively equal. A model for triage of pregnant patients has been proposed, but it does not address how such decisions are integrated with decisions about other patients being
triaged (Beigi et al., 2010). The committee believes triage processes should be inclusive of all patients requiring the same resource, although the prognostic predictors may vary depending on the underlying disease.
![]() Prioritization of maternal care: What is required and what may become optional for prenatal care and evaluation of symptoms (e.g., abdominal pain)?
Prioritization of maternal care: What is required and what may become optional for prenatal care and evaluation of symptoms (e.g., abdominal pain)?
![]() Infection: Is a separate area or process for pregnant patients required to prevent them from acquiring an illness in the health care environment (CDC, 2009b)? Do pregnant women access vaccine in the same way as the general population?
Infection: Is a separate area or process for pregnant patients required to prevent them from acquiring an illness in the health care environment (CDC, 2009b)? Do pregnant women access vaccine in the same way as the general population?
![]() Delivery: What deliveries may be accomplished more safely at home, particularly during an epidemic? Few providers are knowledgeable about the process of labor and delivery or management of common complications.
Delivery: What deliveries may be accomplished more safely at home, particularly during an epidemic? Few providers are knowledgeable about the process of labor and delivery or management of common complications.
![]() Information and consultation: Hotlines and other resources that do not require an actual provider visit are strongly preferred during an epidemic, and may reduce workload during other incidents (University of Minnesota, 2007).
Information and consultation: Hotlines and other resources that do not require an actual provider visit are strongly preferred during an epidemic, and may reduce workload during other incidents (University of Minnesota, 2007).
• Pediatrics: Children represent 24.3 percent of the U.S. population, and 6.9 percent of the U.S. population is under age 5 (U.S. Census Bureau, 2012). Children evoke emotional responses in most health care providers, which can complicate their care and lead to additional psychological stressors for providers, particularly if they are not accustomed to caring for children who are severely injured or ill. Community emergency departments see 90 percent of pediatric emergency cases (American Academy of Pediatrics et al., 2009), few of which involve critical injury or illness. The following are a few key tenets of pediatric care planning (see also Box 7-9):
![]() Age-appropriate equipment and sufficient volumes and types of supplies should be stocked for pediatric emergency use.
Age-appropriate equipment and sufficient volumes and types of supplies should be stocked for pediatric emergency use.
![]() Providers should have at least basic skills in pediatric resuscitation, including quick reference materials.
Providers should have at least basic skills in pediatric resuscitation, including quick reference materials.
![]() The facility should plan for unaccompanied minors and their physical and emotional support.
The facility should plan for unaccompanied minors and their physical and emotional support.
• Functional limitations: The institution’s usual resources (for example, wheelchairs or sign language interpreters) may be unavailable during a disaster, and contingency plans for those needing these resources should be developed.
• Medically dependent patients: Those on home oxygen and electrical devices may arrive at the hospital during blackouts and other community infrastructure losses for assistance. Outpatient dialysis systems usually have robust disaster plans, but local transportation and infrastructure may be too damaged to meet dialysis needs initially.
• Mental health: Disasters are extremely destabilizing for patients with mental health issues. Additionally, patients may run out of or become separated from their medications or be unable to fill prescriptions. Planning should account for the potential for disaster stocking of psychotropic and anxiolytic medication for both maintenance and acute use.
BOX 7-9
Pediatric Issues in the Tuscaloosa Tornado
On April 27, 2011, an EF-4 tornado struck Tuscaloosa, Alabama. DCH Regional Medical Center in Tuscaloosa treated 600-800 patients in the first 24 hours after the tornado, the vast majority in the first 14 hours. One hundred patients were admitted. DCH is not a usual receiving facility for pediatric trauma but received at least 50 pediatric victims, including three pediatric fatalities (all of whom were apparently dead on arrival and one of whom was unclaimed for days after the storm). After initial assessment, stabilization, and management, 30 patients were transferred to Children’s Hospital of Alabama for admission and further care, representing a high percentage of transferred and admitted patients. Although the area hospitals have outstanding referral criteria for pediatric patients and participate in the Southeastern Regional Pediatric Disaster Response Network (a multistate pediatrics preparedness network) to improve surge response, no just-in-time training, network support, or follow-on resources could substitute for the availability of pediatric-specific supplies and the response of emergency and pediatric providers to the local hospital. Additional supplies were brought to DCH Regional as the evening wore on, but initial stabilization efforts relied on supplies that were present at the institution. Many children presented without family members, and families often were separated as a result of transfers or admission to other facilities. These children required significant staff support. One staff member recalled being moved at the sight of a 6-year-old crying in the hospital hallway, injured, and knowing his parents were dead.
Key points:
• R egional plans for specialty patients (e.g., burn, pediatrics) are critical for ongoing care and referral. In overwhelming situations, concentrating those less than 5 years of age at children’s hospitals may offer the best outcomes when all patients cannot be admitted to specialty facilities. This requires regional coordination.
• Rtabilization care often will occur at the institution closest to the incident, requiring a commitment to stocking basic supplies and providing basic training and immediate reference materials.
• R lanning for unaccompanied minors and their support (including their safe disposition once medical care has been completed) often is underemphasized.
SOURCES: AAP, 2011; Branson, 2011; EMSC National Resource Center, 2010; Kanter and Cooper, 2009; National Commission on Children and Disasters, 2009; NYCDHMH, 2007.
Function 10. Planning. The planning section is responsible for gathering incident-related data, which encompass up-to-date incident information, analyses, and forecasts regarding operations and assigned resources, including the development of alternatives for tactical operations. The planning section conducts planning meetings and prepares the incident action plan. It also provides awareness through materiel and personnel tracking, and situational awareness through patient and bed tracking (California Emergency Medical Services Authority, 2006d). The planning section is responsible as well for working with command staff, technical specialists, and the operations section to identify objectives for the next operational period (usually 12-24 hours) (Plourde and Moats, 2006). In addition, the planning section
may be asked to activate, support, and facilitate interactions with technical specialists and the clinical care committee to obtain input on clinical care strategies for meeting excess demand or specialty consultation.
Personnel management includes ensuring that current staff can be contacted easily (with up-to-date information and processes) and that modifications to shift durations and other staffing changes are checked against current personnel policies and any union or other agreements. A range of options may be implemented, including changing staffing patterns and responsibilities, using administrative staff to provide basic patient care and feeding, adding supplemental staff if possible, and changing staffing ratios. Those changes that result in the least impact on patient care should be implemented first (AHRQ, 2007).
Additional training and orientation materials may need to be developed and provided to current staff either as a refresher or to introduce new concepts. The emphasis should be on reassigning personnel so that those with technical expertise can focus on those areas, and others can perform less technical (and less consequential) tasks. For example, respiratory therapists may concentrate on supervising ventilator use while other staff are delegated to administer inhaled medications (nebulizers and metered dose inhalers).
Function 11. Administration. The administrator of the facility should work with legal counsel and any corporate administrators to determine the institution’s authority and liability in crisis settings, and how declarations of emergency may change those rights and responsibilities. These issues should be understood before an incident occurs.
Regulations affecting patient care and information exchange (such as the Emergency Medical Treatment and Active Labor Act [EMTALA] and the Health Insurance Portability and Accountability Act [HIPAA]) (California Hospital Association, 2009; HHS, 2011) should be examined in advance of an incident; certain actions, such as suspension of selected federal requirements, may be requested and granted during disaster situations. Usually, exceptions to the regulations are made for emergencies, including permitting information sharing to allow family reunification and the exchange of public health and safety information. A crisis is not the time to scramble to research these issues. Administration and counsel should have a good understanding of applicable state laws and federal regulations (see also the detailed discussion of legal issues in Chapter 3).
It is important for hospitals and providers to understand their regulatory and legal protections and liabilities. Both can be held liable for their clinical and administrative decisions (Hodge and Brown, 2011).7 Clear documentation of actions and use of standard or community guidelines can mitigate that liability. Activation of emergency health powers may confer additional protections, depending on the state. Having a preplanned, systematic approach consistent with that of other facilities in the community contributes to protecting institutions and providers. Triage decisions may have to be made in the absence of a declaration of emergency (e.g., an isolated ECMO triage decision during a seasonal influenza epidemic, no other regional/community resources available). Thus, it is important to consider the process within or between institutions when there is no disaster situation. In most states, when an inci-
_________________
7Preston v. Tenet Healthsystem Memorial Medical Center Inc., No. 05-11709-B-15 (La. Civ. Dist. Ct. settled Mar. 23, 2011).
dent is large enough to warrant a declaration, early actions may be protected by dating the emergency orders to cover the entire incident timeline regardless of when the declaration was issued.
Providers should be familiar with their protections in daily operations, during disasters (when some state laws provide additional protections for clinical decisions), and during declared health emergencies. There often are significant differences in liability when care is provided in nonhospital versus hospital settings and in situations where reimbursement is not expected. Furthermore, there is significant state-to-state variability in protections, so providers responding to assist in other states who are not protected as federal or state employees should understand their obligations and liabilities.
Hospital Providers
It is important for providers to take an active interest in their facility’s disaster preparedness and response plan, with specific attention to its CSC indicators, triggers, and implementation protocols. This section of the template enumerates the functions and associated tasks of those providing health care during a disaster.
Function 1. Notification. Providers that have agreed to act as technical specialists or members of the clinical care committee or triage team should understand their responsibilities to those groups during a disaster. These duties may need to be reconciled with their other clinical responsibilities, especially if the duration of the response is lengthy. All providers should regularly update and ensure the accuracy of their contact information, as the facility will need to get in touch with staff to meet rapidly changing demand. It is important for all providers to participate actively in tests and exercises of the facility’s notification systems so they can gain insight into those systems prior to an incident, and so the facility has an opportunity to identify and rectify any issues.
Function 2. Command, Control, Communications, and Coordination. All providers should receive role-appropriate incident command training, including knowledge of how to access available resources to guide their actions as the standard of care progresses from conventional to crisis. In the reactive phase of triage, providers may not have an understanding of the scope and scale of the incident, so it is important that they know how to contact their facility’s command center to determine resource availability. Beyond their commitment to a particular facility, providers may have obligations that involve public-sector disaster response roles, including serving as a part of the Medical Reserve Corps or ESAR-VHP. For each of their roles, providers should be clear about whom to contact, where to report, and how to execute their responsibilities.
Function 3. Public Information. While facilities will be responsible for managing internal and external communications systems, individual providers should familiarize themselves with processes for inputting information into and extracting information from facility and public sources (likely electronic or telephone based).
Function 4. Operations. Providers should know their unit’s protocols for expanding care as demand overwhelms available resources. To operate effectively under CSC conditions, providers should thor-
oughly understand their triage roles (if any), as well as acceptable and unacceptable bases for triage decisions.
Function 5. Logistics (space, staff, supplies). While local and state governments and facilities bear responsibility for managing resources to avoid or mitigate scarcity on a regional level, individual providers will have to adapt to any deficits that occur in their unit. It is important that providers be well versed in how to expand their patient care space to accommodate a significant increase in patient volume. Providers themselves may become a scarce resource as patient volume increases; familiarity, through education and exercises, with the ways in which their own roles will change with shifts in the care continuum will enable maximal use of their time and energy. These changes can include an expansion or contraction of their traditional scope of practice, changes in documentation duties, and incorporation of external staff into the unit. Finally, providers should know where to access additional supplies and how guidance is to be received on substituting, conserving, adapting, and reusing those supplies.
Function 6. Operations (mental health). Changes to the clinical care environment during disaster response can take a toll on providers’ emotional health. For this reason, it is important that providers be able to recognize the signs and symptoms of abnormal (as opposed to normal) responses to stress and be clear on how to access employee mental health services. Greater detail on mental health care can be found in the mental health section of Chapter 4.
Function 7. Legal Issues. The legal implications of providing care during a disaster, especially one that requires the use of CSC, can be daunting. Providers should not wait until an incident has occurred to learn about their legal protections and liabilities in different disaster scenarios (e.g., in a declared versus a nondeclared emergency, as a public versus private care provider). Chapter 3 provides a detailed discussion of the legal issues associated with disaster response.
Function 1. Alerting
Notes and Resources
Triggers and indicators are consistent with regional and state plans as applicable.
Task 1
Health care facility is able to receive and manage alerts from emergency medical services (EMS), public safety, hospital partners, the department of public health (Health Alert Network), and the National Weather Service.
Task 2
Health care facility emergency response plan provides the triggers and process for incident command to activate the CSC plan and indicators (if applicable) to prompt consideration of activation.
Function 2. Notification
Notes and Resources
Institution tests notification systems at least annually and ensures that up-to-date contact information is available.
Task 1
Institution is able to alert staff within and external to the facility, including
• EMS and coalition/partner health care facilities;
• medical, administrative, and support staff;
• clinical care committee members; and
• technical experts, including those in toxicology, radiation safety, infectious disease, critical care, emergency medicine, trauma surgery, blood banking, dialysis, pediatrics, burn surgery, and mental health (those institutions without in-house expertise should identify other sources for consultation).
Notification mechanisms account for redundancy in case a disaster affects usual means of contact/consultation.
Task 2
Expectations of staff, including technical experts and those staffing the clinical care team, are understood prior to an incident, and appropriate activation/notification policies are in place.
Function 3. Command
Notes and Resources
See Appendix B for a sample hospital CSC plan.
See Table 7-2 in Chapter 7 for a sample surge capacity template.
Task 1
Hospital incident command system (HICS) (or other national incident management system [NIMS]) and community-compliant system is in place. Includes
• understanding where technical specialists, the clinical care committee, and the triage team fit into the incident management structure;
• training and exercising with key staff, including those on the clinical care committee and potential triage team members;
• command staff being trained and exercised (at least table-top) in activation of the full continuum of care, including use of crisis spaces and staffing;
• command staff understanding incident action planning and use of the planning section during longer-term events; and Notes and ResourcesSee Appendixes B, C, and D.
• appropriate resources (job aids) being available to guide capacity expansion.
Function 4. Control
Notes and Resources
See Appendixes B, C, and D.
Task 1
Command staff understand interfaces for resource requests and acquisition (as well as any existing plans for resource triage/allocation) with
• Local public health and emergency management,
• Local/regional hospital coalitions, and
• State resources (usually via local emergency management and/ or state public health).
Task 2
Command and other appropriate staff understand transfer and diversion policies in the area and their function during a disaster.
Task 3
Command staff understand the process for sheltering, relocation, and evacuation in response to threats to the facility.
Task 4
Command staff understand options for security/access controls and community law enforcement support during a disaster.
Task 5
Facility plan reflects a phased expansion of surge capacity/capabilities for conventional, contingency, and crisis situations.
Task 6
Command staff understand the process for rapid facility and incident
assessment in the immediate aftermath of an incident to gain situational awareness.
Task 7
Command staff understand the state public health department authorities and resource allocation/policy/plans for an epidemic or other public health crisis, including how the health care facility interfaces with local and state public health (this affects facility isolation, personal protective equipment, quarantine, vaccination, countermeasures, and other actions taken to contain an outbreak).
Function 5. Communications
Task 1
Facility has policies and procedures in place for sharing situational information with staff, patients, and other facilities and agencies within the region.
Task 2
Facility has redundant ability to communicate with
• local EMS,
• the local emergency operations center,
• the local/regional health and medical multiagency coordination center (as applicable), and
• other hospitals/facilities in the area.
Task 3
Facility has around-the-clock capability to receive health alerts and other local, state, and federal health communications and a process for rapidly analyzing those communications, and developing or modifying policy accordingly.
Function 6. Coordination
Task 1
Command staff understand the interface between the institution and local public health, emergency management, and local/regional hospital coalitions, as well as any multiagency coordination constructs.
Task 2
Facility understands the function of the state disaster medical advisory committee and any regional medical coordination center or regional disaster medical advisory committees, as well as the means by which information is received from or communicated to these bodies.
Task 3
If the facility is part of a health care system, plans document the responsibilities of the facility vs. the corporate response structure and the process by which corporate policy and other region- or communitydeveloped policies and processes are integrated.
Task 4
If facility has a limited patient population (Department of Veterans Affairs [VA] hospital, children’s hospital, military hospital, rehabilitation hospital), there is guidance/a plan for how that facility will contribute to the response when an incident affects either its usual target population or other groups disproportionately.
Function 7. Public Information
Task 1
Facility has a process in place to ensure the development of appropriate risk communications in conjunction with coalitions and/ or public agencies, as well as facility-specific means of dissemination (website, calling programs, e-mail, social media).
Task 2
Facility coordinates information with other agencies and facilities and participates in joint information system (JIS) and joint information center (JIC) activities when implemented by the jurisdiction, state, or coalition. This includes the ability to reach key cultural groups served by the facility.
Function 8. Operations
Notes and Resources
See Appendix B.
See Appendix C.
Conventional Care
Task 1
Command and unit staff are aware of actions to be taken to maximize the availability of staffed beds, including canceling elective admissions/ surgeries and invoking early patient discharge ("surge discharge") or movement.
Contingency Care
Task 1
Command and unit staff are aware of how to implement institutional plans for supply substitution, conservation, and adaption; staff responsibility extension; and patient care area repurposing (e.g., opening pre- and postanesthesia care units for general patient care).
Crisis Care
Task 1
This task is the same as Task 1 for contingency care, but options are expanded to include
• reuse and reallocation of supplies,
• changes in staff roles,
• use of cot-based care, and
• resource allocation and triage decisions and interface with the triage team (if activated).
Standards for patient care are adjusted according to circumstances (e.g., changed thresholds for intensive care unit or floor admission).
See Appendix B.
The mental health section of Chapter 4 provides more detailed discussion and examples.
Medical Care Branch, Clinical Care Committee, and Triage Team
Task 1
Facility has planned for crisis care by convening potential members of an institutional clinical care committee and triage team (for tertiary triage of inpatients, not for no-notice incidents) to identify specific risks to the facility and specific resources at risk.
Task 2
Facility emergency operations plan includes a crisis care annex that details the use of the clinical care committee and triage team, including
• membership,
• activation,
• roles and responsibilities,
• considerations prior to implementing triage strategies,
• documentation of decisions (medical records as well as incident documentation),
• the triage process and possible decision tools to be used (including the ability to incorporate incidents or community-specific modifications),
• an appeals process for triage decisions, and
• anticipated clinical and administrative strategies.
Mental Health
Task 1
Facility has non-mental health personnel trained in basic psychological first aid and psychological triage and assigns a role to mental health operations within its incident command system.
Task 2
CSC-specific coping information/resources are provided to patients, family members, and staff, including CSC-specific “neighbor-to-neighbor, family-to-family” psychological first aid.
Task 3
Facility has a plan for triage-driven management of psychological casualties, including participation in local/regional plans for mental health incident management.
Task 4
Facility participates in the development of risk communications that include a behavioral component related to “coping with CSC” for patients, their families, and health care workers.
Task 5
Facility has a personal resilience plan for health care workers that includes triage and referral to a continuum of evidence-based care.
Task 6
Facility participates in a local gap analysis and develops an action plan to build key local disaster mental health and spiritual care capacities.
Palliative care may be addressed in the CSC/scarce resources annex or elsewhere in the facility emergency operations plan.
The palliative care section of Chapter 4 provides a more detailed discussion.
Task 7
Facility has a plan to engage community faith-based and other support providers, as well as key cultural groups within the community, during crisis care operations to expand mental health care capacity, particularly in times of resource triage.
Palliative Care
Task 1
Facility has planned for adequate symptomatic management (analgesia, antiemetics, anxiolytics) for all patients (including those that will not receive other treatment modalities).
Task 2
Palliative care, including palliative care principles, triage tools, and any facility-specific procedures, is addressed in the emergency operations plan.
Task 3
Palliative care training (including just-in-time training) is developed and provided according to the facility plan.
Function 9. Logistics
Notes and Resources
For an example, see the Minnesota Department of Health’s Strategies for Scarce Resource Situations.
Supplies
Task 1
In conjunction with the clinical care committee, emergency management committee identifies key potential scarce resources based on different types of incidents and, to the extent possible, stockpiles or identifies alternative sources for these supplies.
Task 2
For highly vulnerable supplies, facility identifies strategies for appropriate substitution, conservation, adaptation, reuse, and reallocation.
Task 3
For local or state cached supplies (such as a local pharmaceutical cache) or Strategic National Stockpile (SNS) supplies, facility understands the process for requesting, receiving, and distributing these supplies.
Space
Task 1
Facility examines available beds, beds in storage, cots, beds for lease, and other potential sources and develops a plan for maximizing available patient care space and converting non-patient care areas to patient care as necessary.
Staffing
Task 1
Call-back criteria and policies are in place and include maintenance of current and accurate employee contact information.
All institutions should prepare to initially stabilize and treat all types of victims during a disaster.
Task 2
Facility assesses number of staff available for selected large-scale events, including those that limit access to the facility or result in provider illness. Consideration is given to the need for extended staffing requirements or for holding back adequate staff for future operational periods.
Task 3
Facility plans for on-site accommodation of staff and family members as appropriate.
Special Challenges
Task 1
Patient groups requiring special consideration are identified, and to the extent possible, equipment and supplies to address their needs are purchased and/or stockpiled in relation to the facility’s size and role in the community. These groups include (but are not limited to)
• pediatric patients,
• burn patients,
• patients requiring airborne isolation,
• patients requiring decontamination,
• patients with functional limitations (e.g., hearing or visually impaired), and
• patients requiring dialysis/renal replacement therapy.
Task 2
Facility understands regional/state plans or resources for specific groups (e.g., pediatric-specific disaster supplies, regional pediatric or dialysis networks) and how to access/activate them.
Function 10. Planning
Technical Specialists and Clinical Care Committee
Task 1
Clinical care committee understands its interface with incident command, and in particular the medical care branch director, planning section chief, and planning cycle, including its role in developing strategies for the next operational period.
Task 2
Technical specialists understand their interface with the command and planning sections.
Task 3
Clinical care committee reviews current response strategies, including any triage decisions made, and modifies strategies, tools, or processes based on evolving incident information as part of the incident planning cycle.
Personnel Management
Task 1
Hospital bylaws, credentialing policies and procedures account for disaster use of nonhospital staff (including use of local/regional staff in accordance with coalition agreements).
Task 2
Emergency operations plan includes anticipating orientation, mentoring, education, and clinical care policies for outside staff.
Task 3
Policies for altered staffing ratios, shift lengths, and staff roles are examined, and any collective bargaining issues are identified, if not addressed.
Task 4
As needed, emergency operations plan addresses the use of nontraditional assistance (family members, volunteers, Medical Reserve Corps [MRC] providers) to provide non-medical patient care.
Task 5
Hospital understands the process and supporting agreements (e.g., worker’s compensation, liability) for sharing staff with outside facilities in need, including staffing of alternate care systems.
Task 6
Hospital understands the need to attend to staff resilience and mental health risk to maintain the hospital’s continuity of operations.
Function 11. Administration
Notes and Resources
See Chapter 3 for a more detailed discussion.
Authority
Task 1
Administration (including corporate administration) has examined its disaster delegation of authority to incident commanders and made any changes necessary to ensure that crisis care decisions are supported (i.e., that the incident commander is acting with the authority of the institution). During a crisis, the administration may require additional communications and coordination with the incident commander.
Task 2
Administration understands relevant changes to agency/facility authorities and protections when the state declares an emergency/ public health emergency, including legal protections or obligations for medical providers (e.g., duty to serve).
Regulatory/Legal Issues
Task 1
Facility and/or corporate legal counsel are aware of CSC plans and implications for patient care.
Task 2
Legal department identifies state and local laws and regulations that would impact the institution’s ability to implement CSC plans and possible solutions (see Chapter 3 for a full list of functions).
Core Functions of Hospital Facilities and Providers in the Implementation of CSC Plans
Hospital Provider Functions
Function 1. Notification
Task 1
Providers understand their call-back responsibilities during an incident, including potential roles as technical specialists or clinical care committee/triage team members.
Task 2
Providers ensure up-to-date contact information and acknowledge receipt of exercise and incident messaging.
Function 2. Command, Control, Communications, and Coordination
Notes and Resources
If provider is a member of command staff, additional training is required; see Function 3 in “Hospital Facilities” section of this template.
Task 1
Providers receive information on community disaster roles, including the Medical Reserve Corps (MRC) and Emergency System for the Advance Registration of Volunteer Health Professionals (ESAR-VHP).
Task 2
Providers understand where they report, to whom they answer during a disaster, and how to execute their roles. (This may include private as well as public roles, e.g., MRC member.)
Task 3
Providers know how to contact hospital command center and request resources.
Task 4
Providers receive incident command training appropriate to their role in the command structure, including
• location of plans and actions taken to implement the continuum of care in their area, including use of conventional/crisis spaces and
• resources (job aids) or unit-based plans to guide capacity expansion.
Function 3. Public Information
Task 1
Providers understand key sources of facility/community information in disaster (web, Twitter, hospital hotline, etc.).
Function 4. Operations
Task 1
Providers understand unit-based actions during expansion of care from conventional to crisis (surge discharge, adapted care on unit, cot-based care, etc.).
Task 2
Providers are prepared to perform triage as it relates to their roles (may involve, e.g., triage for early discharge, triage for resources in emergency department/surgery/other units, participation in triage team).
Task 3
Providers likely to perform triage (both reactive and proactive) understand the criteria they may consider (as well as what not to consider) when making triage decisions.
Function 5. Logistics
Space
Task 1
Providers understand disaster space utilization on their units, including contingency/crisis expansion as applicable.
Staffing
Task 1
Providers understand how their unit staffing and hours may change during a disaster.
Task 2
Providers understand through education and other communications how their roles may be changed/expanded during a crisis (e.g., burn nurses may have responsibility only for burn/wound care as other nurses assume responsibility for overall patient care), including incorporation process for staff from outside the unit or facility as applicable.
Task 3
Providers understand how changes in record-keeping and other duties may occur in crisis situations (e.g., where to find and how to use paper forms).
Supplies
Task 1
Providers can access supplies from pharmacy/central/sterile supply and understands any existing contingency plans in case of shortage.
Function 6. Operations
Notes and Resources
See mental health section of Chapter 4 for a more detailed discussion.
Mental Health
Task 1
Providers understand employee resilience plan, including sources of employee mental health support.
Task 2
Providers are trained in anticipating normal stress reactions, developing a personalized “resilience plan” and identifying coping resources, as well as self-triage indicators of traumatic stress.
Function 7. Legal Issues
Notes and Resources
Chapter 3 provides more detailed discussion.
Task 1
Providers understand legal obligations and liabilities for practice both within and outside of their hospitals when
* a disaster or public health emergency has been declared;
* a disaster or public health emergency has not been declared; and
* when providing other disaster relief functions (for example, if serving as MRC or disaster medical assistance team\ member).
AAP (American Academy of Pediatrics). 2011. Children & disasters. Grove Village, IL: AAP, http://www.aap.org/disasters/hospitals.cfm (accessed November 29, 2011).
Aarts, H., and A. Dijksterhuis. 2000. Habits as knowledge structures: Automaticity in goal-directed behavior. Journal of Personality and Social Psychology 78(1):53-63.
Adeniji, K. A., and R. Cusack. 2011. The Simple Triage Scoring System (STSS) successfully predicts mortality and critical care resource utilization in H1N1 pandemic flu: A retrospective analysis. Critical Care 15(1):R39.
AHA (American Hospital Association). 2011. AHA survey on drug shortages. Chicago, IL: AHA, www.aha.org/aha/content/2011/pdf/drugshortagesurvey.pdf (accessed November 29, 2011).
AHRQ_(Agency for Healthcare Research and Quality). 2007. Providing mass medical care with scarce resources: A community planning guide, edited by Phillips, S. J., and A. Knebel. Publication no. 07-0001. Rockville, MD: AHRQ, http://archive.ahrq.gov/research/mce/mceguide.pdf (accessed February 27, 2012).
AMA (American Medical Association). 1995. Ethical considerations in the allocation of organs and other scarce medical resources among patients. Council on Ethical and Judicial Affairs, American Medical Association. Archives of Internal Medicine 155(1):29-40.
American Academy of Pediatrics, American College of Emergency Physicians, and Emergency Nurses Association. 2009. Joint policy statement—guidelines for care of children in the emergency department. Pediatrics 124(4):1233-1243. http://aappolicy.aappublications.org/cgi/reprint/pediatrics;124/4/1233.pdf (accessed February 27, 2012).
American College of Physicians. 2011. How can our nation conserve and distribute health care resources effectively and efficiently? Policy Paper. Philadelphia, PA: American College of Physicians, http://www.acponline.org/advocacy/where_we_stand/policy/health_care_resources.pdf (accessed February 27, 2012).
Antommaria, A. H., J. Sweney, and W. B. Poss. 2010. Critical appraisal of: Triaging pediatric critical care resources during a pandemic: Ethical and medical considerations. Pediatric Critical Care Medicine 11(3):396-400.
ANZ ECMO Investigators (The Australia and New Zealand Extracorporeal Membrane Oxygenation Influenza Investigators). 2009. Extracorporeal membrane oxygenation for 2009 influenza A(H1N1) acute respiratory distress syndrome. JAMA 302(7):1888-1895.
ASPR (Assistant Secretary for Preparedness and Response). 2012. National Disaster Medical System. Washington, DC: Department of Health and Human Services, http://www.phe.gov/preparedness/responders/ndms/Pages/default.aspx (accessed February 27, 2012).
Barbera, J. A., and A. G. MacIntyre. 2004. Medical surge capacity and capability: A management system for integrating medical and health resources during large-scale emergencies, 2nd ed. Washington, DC: HHS.
Barbisch, D. F., and K. L. Koenig. 2006. Understanding surge capacity: Essential elements. Academic Emergency Medicine 13(11):1098-1102.
Barkemeyer, B. M. 2006. Practicing neonatology in a blackout: The University Hospital NICU in the midst of Hurricane Katrina: Caring for children without power or water. Pediatrics 117(Supplement 4):S369-S374.
Beekley, A. C., B. W. Starnes, and J. A. Sebesta. 2007. Lessons learned from modern military surgery. Surgical Clinics of North America 87(1):157-184, vii.
Beigi, R. H. 2007. Pandemic influenza and pregnancy: A call for preparedness planning. Obstetrics and Gynecology 109(5):1193-1196.
Beigi, R. H., J. Hodges, M. Baldisseri, D. English; Magee-Womens Hospital Ethics Committee. 2010. Clinical review: Considerations for the triage of maternity care during an influenza pandemic—one institution’s approach. Critical Care 14(3):225.
Benson, M., K. L. Koenig, and C. H. Schultz. 1996. Disaster triage: START, then SAVE—a new method of dynamic triage for victims of a catastrophic earthquake. Prehospital and Disaster Medicine 11:117-124.
Bernstein, S. L., D. Aronsky, R. Duseja, S. Epstein, D. Handel, U. Hwang, M. McCarthy, K. John McConnell, J. M. Pines, N. Rathlev, R. Schafermeyer, F. Zwemer, M. Schull, B. R. Asplin; Society for Academic Emergency Medicine, Emergency Department Crowding Task Force. 2009. The effect of emergency department crowding on clinically-oriented outcomes. Academic Emergency Medicine 16:1-10.
Bisson, J. I., P. L. Jenkins, J. Alexander, and C. Bannister. 1997. Randomized controlled trial of psychological debriefing for victims of acute burn trauma. British Journal of Psychiatry 171:78-81.
Bisson, J. I., M. Brayne, F. M. Ochberg, and G. S. Everly. 2007. Early psychosocial intervention following traumatic events. American Journal of Psychiatry 164(7):1016-1019.
Bogucki, S., and K. Jubanyik. 2009. Triage, rationing, and palliative care in disaster planning. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 7(2): 221-224.
Bohn, D., R. K. Kanter, J. Burns, W. D. Barfield, and N. Kissoon. 2011. Supplies and equipment for pediatric emergency mass critical care. Pediatric Critical Care Medicine 12(Suppl.):S120-S127.
Branson, R. D. 2011. Disaster planning for pediatrics. Respiratory Care 56(9):1457-1463.
Burkle, F. M., Jr., E. B. Hsu, M. Loehr, M. D. Christian, D. Markenson, L. Rubinson, and F. L. Archer. 2007. Definition and functions of health unified command and emergency operations centers for largescale bioevent disasters within the existing ICS. Disaster Medicine and Public Health Preparedness 1(2):135-141.
Burnweit, C., and S. Stylianos. 2011. Disaster response in a pediatric field hospital: Lessons learned in Haiti. Journal of Pediatric Surgery 46(6):1131-1139.
California Department of Public Health. 2008. Standards and guidelines for healthcare surge during emergencies. http://bepreparedcalifornia.ca.gov/EPO/CDPHPrograms/PublicHealthPrograms/EmergencyPreparednessOffice/EPOProgramsServices/Surge/StandGuide/SSG1.htm (accessed February 25, 2011).
California Emergency Medical Services Authority. 2006a. Incident commander: Job action sheet. http://www.emsa.ca.gov/HICS/files/JAS_Command.pdf (accessed February 5, 2012).
California Emergency Medical Services Authority. 2006b. Operations section chief: Job action sheet. http://www.emsa.ca.gov/HICS/files/JAS_Ops.pdf (accessed February 5, 2012).
California Emergency Medical Services Authority. 2006c. Logistics section chief: Job action sheet. http://www.emsa.ca.gov/HICS/files/JAS_Logs.pdf (accessed February 5, 2012).
California Emergency Medical Services Authority. 2006d. Planning section chief: Job action sheet. http://www.emsa.ca.gov/HICS/files/JAS_Plan.pdf (accessed February 5, 2012).
California Hospital Association. 2009. EMTALA requirements and options for hospitals in a disaster. http://www.calhospitalprepare.org/node/675 (accessed February 27, 2012).
Casagrande, R., N. Wills, E. Kramer, M. Mussante, R. Kurinsky, P. McGhee, L. Katz, D. M. Weinstock, and C. N. Coleman. 2011. Using the Model of Resource and Time-based Triage (MORTT) to guide scarce resource allocation in the aftermath of a nuclear detonation. Disaster Medicine and Public Health Preparedness 5(Suppl. 1):S98-S110.
CDC (Centers for Disease Control and Prevention). 2009a. Updated interim recommendations for the use of antiviral medications in the treatment and prevention of influenza for the 2009-2010 season. http://www.cdc.gov/h1n1flu/recommendations.htm (accessed February 27, 2012).
CDC. 2009b. Interim guidance: Considerations regarding 2009 H1N1 influenza in intrapartum and postpartum hospital settings. http://www.cdc.gov/h1n1flu/guidance/obstetric.htm (accessed February 27, 2012).
CDC. 2011a. Public health emergency preparedness cooperative agreement. Funding Number CDC-RFA-TP11-1101CONT11. Atlanta, GA: CDC, http://www.cdc.gov/phpr/documents/PHEP_FY_2011.pdf (accessed November 29, 2011).
CDC. 2011b. Strategic National Stockpile (SNS). http://www.cdc.gov/phpr/stockpile/stockpile.htm (accessed February 27, 2012).
Challen, K., J. Bright, A. Bentley, and D. Walter. 2007. Physiologicalsocial score (PMEWS) vs. CURB-65 to triage pandemic influenza: A comparative validation study using community-acquired pneumonia as a proxy. BMC Health Services Research 7:33.
Cheung, L. Y. S., G. M. Joynt, C. D. Gomersall, and A. Lee. 2008. Is the nurse workload:staffing ratio associated with the outcome of critcally ill patients. Intensive Care Medicine 34:S8.
Christian, M. D., L. Hawryluck, R. S. Wax, T. Cook, N. M. Lazar, M. S. Herridge, M. P. Muller, D. R. Gowans, W. Fortier, and F. M. Burkle. 2006. Development of a triage protocol for critical care during an influenza pandemic. Canadian Medical Association Journal 175(11):1377-1381.
Christian, M. D., G. M. Joynt, J. L. Hick, J. Colvin, M. Danis, and C. L. Sprung. 2010. Chapter 7: Critical care triage. Intensive Care Medicine 36(Suppl. 1):S55-S64.
Christian, M. D., P. Toltzis, R. K. Kanter, F. M. Burkle, D. D. Vernon, and N. Kissoon. 2011. Treatment and triage recommendations for pediatric emergency mass critical care. Pediatric Critical Care Medicine 12(Suppl.):S109-S119.
Chung, S., S. Monteiro, T. Hogencamp, F. J. Damian, and A. Stack. 2011. Pediatric alternate site of care during the 2009 H1N1 pandemic. Pediatric Emergency Care 27(6):519-526.
CIDRAP (Center for Infectious Disease Research & Policy). 2011. Creating a regional pediatric disaster preparedness network: The importance of collaboration (AL, FL, LA, MS, TN). Public Health Practices: Enhancing Emergency Preparedness and Response. Minneapolis, MN: University of Minnesota. http://www.publichealthpractices.org/practice/creating-regional-pediatric-disaster-preparedness-network-importance-collaboration-al-fl—0 (accessed February 5, 2012).
Clarke, S. P., D. M. Sloane, and L. H. Aiken. 2002. Effects of hospital staffing and organizational climate on needlestick injuries to nurses. American Journal of Public Health 92(7):1115-1119.
County of Santa Clara. 2007. County of Santa Clara hospital mutual aid system memorandum of understanding. Santa Clara, CA: County of Santa Clara, http://www.sccgov.org/SCC/docs/SCC%20Public%20Portal/keyboard%20agenda/B0S%20Agenda/2007/February%2027,%202007/TMPKeyboard201832702.pdf (accessed September 8, 2009).
Courtney, B., E. Toner, R. Waldhorn, C. Franco, K. Rambhia, A. Norwood, T. V. Inglesby, and T. O’Toole. 2009. Healthcare coalitions: The new foundation for national healthcare preparedness and response for catastrophic health emergencies. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 7(2):153-163.
Cruz, A. T., B. Patel, M. C. DiStefano, C. R. Codispoti, J. E. Shook, G. J. Demmler-Harrison, and P. E. Sirbaugh. 2010. Outside the box and into thick air: Implementation of an exterior mobile pediatric emergency response team for North American H1N1 (swine) influenza virus in Houston, Texas. Annals of Emergency Medicine 55(1):23-31.
Darcy, M. J. 2003. Tragedy and response—the Rhode Island nightclub disaster. New England Journal of Medicine 349(21): 1990-1992.
Deboisblanc, B. P. 2005. Black hawk, please come down: Reflections on a hospital’s struggle to survive in the wake of Hurricane Katrina. American Journal of Respiratory and Critical Care Medicine 172:1239-1240.
Debruin, D. A., M. F. Marshall, E. Parilla, J. Liaschenko, J. P. Leider, D. J. Brunnquell, J. E. Garrett, and D. E. Vawter. 2010. Implementing ethical frameworks for rationing scarce health resources in Minnesota during severe influenza pandemic. Minneapolis, MN: Minnesota Department of Health, http://www.health.state.mn.us/divs/idepc/ethics/implement.pdf (accessed February 29, 2012).
Devereaux, A. V., J. R. Dichter, M. D. Christian, N. N. Dubler, C. E. Sandrock, J. L. Hick, T. Powell, J. A. Geiling, D. E. Amundson, T. E. Baudendistel, D. A. Braner, M. A. Klein, K. A. Berkowitz, J. R. Curtis, and L. Rubinson. 2008. Definitive care for the critically ill during a disaster: A framework for allocation of scarce resources in mass critical care. From a Task Force for Mass Critical Care summit meeting, January 26-27, 2007, Chicago, IL. Chest 133(Suppl. 5):S51-S66.
DHS (U.S. Department of Homeland Security). 2007. Homeland security exercise and evaluation program. Volume II: Exercise planning and conduct. https://hseep.dhs.gov/support/VolumeII.pdf (accessed February 27, 2012).
Downar, J., and D. Seccareccia. 2010. Educational fellows in care at the end of life. Palliating a pandemic: “All patients must be cared for." Journal of Pain and Symptom Management 39(2):291-295.
Eastman, N., B. Philips, and A. Rhodes. 2010. Triaging for adult critical care in the event of overwhelming need. Intensive Care Medicine 36(6):1076-1082.
EMSA (California Emergency Medical Services Authority). 2007. Disaster medical services division—Hospital Incident Command System (HICS). http://www.emsa.ca.gov/hics/ (accessed February 5, 2012). EMSC (Emergency Medical Services for Children) National Resource Center. 2010. Pediatric disaster preparedness. Silver Spring, MD: EMSC, http://www.childrensnational.org/EMSC/PubRes/OldToolboxPages/PDPreparedness.aspx (accessed November 29, 2011).
Eschun, G. M., E. Jacobsohn, D. Roberts, and B. Sneiderman. 1999. Ethical and practical considerations of withdrawal of treatment in the intensive care unit. Canadian Journal of Anaesthesia 46(5):497-504.
FEMA (Federal Emergency Management Agency). 2007a. Fact sheet: NIMSICS-400 training in FY2007: Who must take it, what it covers. http://www.fema.gov/pdf/emergency/nims/ics_400_fs.pdf (accessed February 27, 2012).
FEMA. 2007b. Fact sheet: NIMS ICS-300 training: Who must take it, what it covers. http://www.fema.gov/pdf/emergency/nims/ics_300_fs.pdf (accessed February 27, 2012).
FEMA. 2007c. National Incident Management System (NIMS) basic guidance for Public Information Officers (PIOs). http://www.fema.gov/library/viewRecord.do?id=3095 (accessed February 27, 2012).
FEMA. 2011. NIMS resource center. http://www.fema.gov/emergency/nims/ (accessed February 27, 2012).
FEMA and Emergency Management Institute. 2008. National Incident Management System independent study 701—Multi-Agency Coordination System (MACS) course. Emmitsburg, MD: FEMA. http://training.fema.gov/EMIWeb/IS/is701.asp (accessed July 31, 2008).
FEMA and Emergency Management Institute. 2010. IS-702.a National Incident Management System (NIMS) public information systems. http://training.fema.gov/EMIweb/IS/IS702a.asp (accessed February 27, 2012).
Fink, S. 2009. The deadly choices at memorial. ProPublica, August 27. http://www.propublica.org/topic/deadly-choices-memorial-medical-center-after-katrina/ (accessed May 5, 2011).
Fisher, D., D. S. Hui, Z. Gao, C. Lee, M. D. Oh, B. Cao, T. T. Hien, K. Patlovich, and J. Farrar. 2011. Pandemic response lessons from influenza H1N1 2009 in Asia. Respirology 16(6):876-882.
Fox, E. R., and L. S. Tyler. 2004. Measuring the impact of drug shortages. American Journal of Health-System Pharmacy 61(19):2009.
Frolic, A., A. Kata, and P. Kraus. 2009. Development of a critical care triage protocol for pandemic influenza: Integrating ethics, evidence and effectiveness. Healthcare Quarterly 12(4):54-62.
Frykberg, E. R. 2002. Medical management of disasters and mass casualties from terrorist bombings: How can we cope? Journal of Trauma 53:201-212.
GAO (U.S. Government Accountability Office). 2008. States are planning for medical surge, but could benefit from shared guidance for allocating scarce medical resources. GAO-08-668. Washington, DC: GAO.
Gershengorn, H. B., H. Wunsch, R. Wahab, D. Leaf, D. Brodie, G. Li, and P. Factor. 2011. Impact of nonphysician staffing on outcomes in a medical ICU. Chest 139(6):1347-1353.
Gomersall, D. C., D. Y. Tai, S. Loo, J. L. Derrick, M. S. Goh, T. A. Buckley, C. Chua, K. M. Ho, G. P. Raghavan, O. M. Ho, L. B. Lee, and G. M. Joynt. 2006. Expanding ICU facilities in an epidemic: Recommendations based on experience from the SARS epidemic in Hong Kong and Singapore. Intensive Care Medicine 30:381-387.
Grissom, C. K., S. M. Brown, K. G. Kuttler, J. P. Boltax, J. Jones, A. R. Jephson, and J. F. Orme, Jr. 2010. A modified sequential organ failure assessment score for critical care triage. Disaster Medicine and Public Health Preparedness 4(4):277-284.
Gurwitch, K. D., M. A. Goldwire, and C. J. Baker. 1998. Intravenous immune globulin shortage: Experience at a large children’s hospital. Pediatrics 102(3 Pt. 1):645-647.
Hanfling, D. 2006. Equipment, supplies, and pharmaceuticals: How much might it cost to achieve basic surge capacity? Academic Emergency Medicine 13(11):1232-1237.
HHS (Department of Health and Human Services). 2011. Emergency preparedness planning and response. http://www.hhs.gov/ocr/privacy/hipaa/understanding/special/emergency/index.html (accessed February 27, 2012).
HHS. 2012. Division of the Civilian Volunteer Medical Reserve Corps. Washington, DC: HHS, http://www.medicalreservecorps.gov/HomePage (accessed February 27, 2012).
Hick, J. L., D. Hanfling, J. Burstein, C. DeAtely, D. Barbisch, G. Bogdan, and S. Cantrill. 2004. Healthcare facility and community strategies for patient care surge capacity. Annals of Emergency Medicine 44:253-261.
Hick, J. L., L. Rubinson, D.T. O’Laughlin, and J. C. Farmer. 2007. Clinical review: Allocating ventilators during large-scale disasters—problems, planning, and process. Critical Care 11(3):217.
Hick, J. L., K. L. Koenig, D. Barbisch, and T. A. Bey. 2008. Surge capacity concepts for health care facilities: The CO-S-TR model for initial incident assessment. Disaster Medicine and Public Health Preparedness 2(Suppl. 1):S51-S57.
Hick, J. L., J. A. Barbera, and G. D. Kelen. 2009. Refining surge capacity: Conventional, contingency, and crisis capacity. Disaster Medicine and Public Health Preparedness 3(Suppl. 2):S59-S67.
Hick, J. L., D. Hanfling, and S. V. Cantrill. 2011. Allocating scarce resources in disasters: Emergency department principles. Annals of Emergency Medicine (e-published ahead of print).
Hodge, J. G., and E. F. Brown. 2011. Assessing liability for health care entities that insufficiently prepare for catastrophic emergencies. JAMA 306(3):308-309.
Hollak, C. E., S. vom Dahl, J. M. Aerts, N. Belmatoug, B. Bembi, Y. Cohen, T. Collin-Histed, P. Deegan, L. van Dussen, P. Giraldo, E. Mengel, H. Michelakakis, J. Manuel, M. Hrebicek, R. Parini, J. Reinke, M. di Rocco, M. Pocovi, M. C. Sa Miranda, A. Tylki-Szymanska, A. Zimran, and T. M. Cox. 2010. Force majeure: Therapeutic measures in response to restricted supply of imiglucerase (cerezyme) for patients with Gaucher disease. Blood Cells, Molecules & Diseases 44(1):41-47.
Hota, S., E. Fried, L. Burry, T. E. Stewart, and M. D. Christian. 2010. Preparing your intensive care unit for the second wave of H1N1 and future surges. Critical Care Medicine 38(Suppl. 4):e110-e119.
IASC (Inter-Agency Standing Committee). 2007. IASC guidelines on mental health and psychological support in emergency settings. Geneva, Switzerland: IASC.
IOM (Institute of Medicine). 2006. Hospital-based emergency care: At the breaking point. Washington, DC: The National Academies Press.
IOM. 2009. Guidance for establishing crisis standards of care for use in disaster situations: A letter report. Washington, DC: The National Academies Press.
Iserson, K. V., and J. C. Moskop. 2007. Triage in medicine, part I: Concept, history, and types. Annals of Emergency Medicine 49:275-281.
Joint Commission. 2008. Emergency management standards in compliance elements of performance. Chicago, IL: The Joint Commission.
Kaji, A., K. L. Koenig, and T. Bey. 2006. Surge capacity for healthcare systems: A conceptual framework. Academic Emergency Medicine 13(11):1157-1159.
Kanter, R. K. 2007. Strategies to improve pediatric disaster surge response: Potential mortality reduction and tradeoffs. Critical Care Medicine 35(12):2837-2842.
Kanter, R. K., and A. Cooper. 2009. Mass critical care: Pediatric considerations in extending and rationing care in public health emergencies. Disaster Medicine and Public Health Preparedness 3(Suppl. 2):S166-S171.
Kaposy, C., N. Bandrauk, D. Pullman, R. Singleton, and F. Brunger. 2010. Adapting the Hamilton Health Sciences critical care pandemic triage protocol. Healthcare Quarterly 13(2):60-63.
Khan, Z., J. Hulme, and N. Sherwood. 2009. An assessment of the validity of SOFA score based triage in H1N1 critically ill patients during an influenza pandemic. Anaesthesia 64(12):1283-1288.
King County Healthcare Coalition. 2011. Welcome to the coalition. http://www.kingcountyhealthcarecoalition.org/ (accessed November 29, 2011).
Kirby, J. 2010. Enhancing the fairness of pandemic critical care triage. Journal of Medical Ethics 36(12):758-761.
Klein, K. R., P. E. Pepe, F. M. Burkle, Jr., N. E. Nagel, and R. E. Swienton. 2008. Evolving need for alternative triage management in public health emergencies: A Hurricane Katrina case study. Disaster Medicine and Public Health Preparedness 2(Suppl. 1):S40-S44.
Kopp, J. B., L. K. Ball, A. Cohen, R. J. Kenney, K. D. Lempert, P. E. Miller, P. Muntner, N. Qureshi, and S. A. Yelton. 2007. Kidney patient care in disasters: Emergency planning for patients and dialysis facilities. Clinical Journal of the American Society of Nephrology 2(4):825-838.
Kuhne, C. A., S. Ruchholtz, G. M. Kaiser, and D. Nast-Kolb. 2005. Mortality in severely injured elderly trauma patients—when does age become a risk factor? World Journal of Surgery 29(11):1476-1482.
Lemeshow, S., D. Teres, J. Klar, J. S. Avrunin, S. H. Gehlbach, and J. Rapoport. 1993. Mortality probability models based on an international cohort of intensive care unit patients. Journal of the American Medical Association 270:2478-2486.
Lerner, E. B., R. B. Schwartz, P. L. Coule, E. S. Weinstein, D. C. Cone, R. C. Hunt, S. M. Sasser, J. M. Liu, N. G. Nudell, I. S. Wedmore, J. Hammond, E. M. Bulger, J. P. Salomone, T. L. Sanddal, D. Markenson, and R. E. O’Connor. 2008. Mass casualty triage: An evaluation of the data and development of a proposed national guideline. Disaster Medicine and Public Health Preparedness 2(Suppl. 1):S25-S34.
Lieberman, D., L. Nachshon, O. Miloslavsky, V. Dvorkin, A. Shimoni, and D. Lieberman. 2009. How do older ventilated patients fare? A survival/functional analysis of 641 ventilations. Journal of Critical Care 24(3):340-346.
Lin, G., H. Lavon, R. Gelfond, A. Abargel, and O. Merin. 2010. Hard times call for creative solutions: Medical improvisations at the Israel Defense Forces Field Hospital in Haiti. American Journal of Disaster Medicine 5(3):188-192.
Lin, J. Y., N. Bhalla, and R. A. King. 2009. Training medical students in bag-valve-mask technique as an alternative to mechanical ventilation in a disaster surge setting. Prehospital and Disaster Medicine 24(5):402-406.
Maa, J. 2011. The waits that matter. New England Journal of Medicine 364(24):2279-2281.
Maldin, B., C. Lam, C. Franco, D. Press, R. Waldhorn, E. Toner, T. O’Toole, and T. V. Inglesby. 2007. Regional approaches to hospital preparedness. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 5:43-53.
Matzo, M., A. Wilkinson, J. Lynn, M. Gatto, and S. J. Phillips. 2009. Palliative care considerations for mass casualty events with scarce resources. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 7(2):199-210.
McNally, R. J., R. A. Bryant, and A. Ehlers. 2003. Does early psychological intervention promote recovery from posttraumatic stress? Psychological Science in the Public Interest 4(2):45-79.
Meites, E., D. Farias, L. Raffo, R. Albalak, O. L. Carlino, L. C. McDonald, and M. A. Widdowson. 2011. Hospital capacity during an influenza pandemic—Buenos Aires, Argentina, 2009. Infection Control and Hospital Epidemiology 32(1):87-90.
Merin, O., N. Ash, G. Levy, M. J. Schwaber, and Y. Kreiss. 2010. The Israeli field hospital in Haiti: Ethical dilemmas in early disaster response. New England Journal of Medicine 362(11):e38.
Minnesota Department of Health. 2009. MDH Interim 2009 H1N1 Influenza Infection Prevention and Control Guidelines are posted. Minneapolis, MN: Minnesota Department of Health, http://www.health.state.mn.us/mls/LabAlerts/091109update5.pdf (accessed February 28, 2012).
Minnesota Department of Health. 2011. Patient care strategies for scarce resource situations. St. Paul Minneapolis, MN: Minnesota Department of Health, http://www.health.state.mn.us/oep/healthcare/standards.pdf (accessed February 1727, 2012).
Moreno, R., J. L. Vincent, R. Matos, A. Mendonca, F. Cantraine, L. Thijs, J. Takala, C. Sprung, M. Antonelli, H. Bruining, and S. Willatts. 1999. The use of maximum SOFA score to quantify organ dysfunction/failure in intensive care. Results of a prospective, multicentre study. Intensive Care Medicine 25(7):686-696.
Muller, T., A. Philipp, M. Lubnow, C. Weingart, M. Pfeifer, G. A. J. Riegger, and C. Schmid. 2011. First application of a new portable, miniaturized system for extracorporeal membrane oxygenation. Perfusion 26(4):284-288.
Nap, R. E., M. P. Andriessen, N. E. Meessen, M. J. Albers, and T. S. van der Werf. 2010. Pandemic influenza and pediatric intensive care. Pediatric Critical Care Medicine 11(2):185-198.
National Commission on Children and Disasters. 2009. National Commission on Children and Disasters homepage. http://www.childrenanddisasters.acf.hhs.gov (accessed November 29, 2011).
Needleman, J., P. Buerhaus, S. Mattke, M. Stewart, and K. Zelevinsky. 2002. Nurse-staffing levels and the quality of care in hospitals. New England Journal of Medicine 346(22):1715-1722.
NIMH (National Institute of Mental Health). 2002. Mental health and mass violence: Evidence-based early psychological intervention for victims/survivors of mass violence. A workshop to reach consensus on best practices. NIH publication no. 02-5138, Washington, DC: U.S. Government Printing Office.
Noah, M. A., G. J. Peek, S. J. Finney, M. J. Griffiths, D. A. Harrison, R. Grieve, M. Z. Sadique, J. S. Sekhon, D. F. McAuley, R. K. Firmin, C. Harvey, J. J. Cordingley, S. Price, A. Vuylsteke, D. P. Jenkins, D. W. Noble, R. Bloomfield, T. S. Walsh, G. D. Perkins, D. Menon, B. L. Taylor, and K. M. Rowan. 2011. Referral to an extracorporeal membrane oxygenation center and mortality among patients with severe 2009 influenza A(H1N1). JAMA 306(15):1659-1668.
NYCDHMH (New York City Department of Health and Mental Hygiene). 2007. Preparedness focus areas: Pediatric preparedness. New York: NYCDHMH, http://www.nyc.gov/html/doh/html/bhpp/bhpp-focus-ped-toolkit.shtml (accessed November 29, 2011).
O’Laughlin, D. T., and J. L. Hick. 2008. Ethical issues in resource triage. Respiratory Care 53(2):190-197; discussion 197-200.
Peek, G. J., M. Mugford, R. Tiruvoipati, A. Wilson, E. Allen, M. M. Thalanany, C. L. Hibbert, A. Truesdale, F. Clemens, N. Cooper, R. K. Firmin, and D. Elbourne. 2009. Efficacy and economic assessment of conventional ventilatory support versus extracorporeal membrane oxygenation for severe adult respiratory failure (CESAR): A multicentre randomised controlled trial. Lancet 374(9698):1351-1363.
Peleg, K., and A. L. Kellermann. 2009. Enhancing hospital surge capacity for mass casualty events. Journal of the American Medical Association 302:565-567.
Pettila, V., M. Pettila, S. Sarna, P. Voutilainen, and O. Takkunen. 2002. Comparison of multiple organ dysfunction scores in the prediction of hospital mortality in the critically ill. Critical Care Medicine 30(8):1705-1711.
Plourde, K. L., and J. Moats. 2006. The Incident Command System: A process to move our response stance from reactive to proactive. The Coast Guard Journal of Safety & Security at Sea 63:11-14, www.uscg.mil/proceedings (accessed February 27, 2012).
Pollack, M. M., K. M. Patel, and U. E. Ruttiman. 1996. PRISM III: An updated pediatric risk of mortality score. Critical Care Medicine 24:743-752.
Powell, T., K. C. Christ, and G. S. Birkhead. 2008. Allocation of ventilators in a public health disaster. Disaster Medicine and Public Health Preparedness 2(1):20-26.
Premier, Inc. 2011. Hospital drug shortages. Charlotte, NC: Premier, Inc, http://www.premierinc.com/about/advocacy/issues/11/Hospital-Drug-Shortages-Premier-Policy-Paper.pdf (accessed November 29, 2011).
Propper, B. W., T. E. Rasmussen, S. B. Davidson, S. L. Vandenberg, W., D. Clouse, G. E. Burkhardt, S. M. Gifford, and J. A. Johannigman. 2009. Surgical response to multiple casualty incidents following single explosive events. Annals of Surgery 250(2):311-315.
Rasmussen, S. A., D. J. Jamieson, and J. S. Bresee. 2008. Pandemic influenza and pregnant women. Emerging Infectious Diseases 14(1):95-100.
Rubinson, L., J. B. Nuzzo, D. S. Talmor, T. O’Toole, B. R. Kramer, and T. V. Inglesby. 2005. Augmentation of hospital critical care capacity after bioterrorist attacks or epidemics: Recommendations of the Working Group on Emergency Mass Critical Care. Critical Care Medicine 33(10):2393-2403.
Rubinson, L., J. L. Hick, D. Hanfling, A. V. Devereaux, J. R. Dichter, M. D. Christian, D. Talmor, J. Medina, J. R. Curtis, J. A. Geiling; Task Force for Mass Critical Care. 2008a. Definitive care for the critically ill during a disaster: A framework for optimizing critical care surge capacity. Chest 133(Suppl. 5):18S-31S.
Rubinson, L., J. L. Hick, J. R. Curtis, R. D. Branson, S. Burns, M. D. Christian, and A. V. Devereaux, J. R. Dichter, D. Talmor, B. Erstad, J. Medina, and J. A. Geiling; Task Force for Mass Critical Care. 2008b. Definitive care for the critically ill during a disaster: Medical resources for surge capacity. From a Task Force for Mass Critical Care summit meeting, January 26-27, 2007, Chicago, IL. Chest 133(Suppl. 5):32S-50S.
Rubinson, L., A. Knebel, and J. L. Hick. 2010. MSOFA: An important step forward, but are we spending too much time on the SOFA? Disaster Medicine and Public Health Preparedness 4(4):270-272.
Ruggiero, K. J., H. S. Resnick, R. Acierno, S. F. Coffey, M. J. Carpenter, A. M. Ruscio, R. S. Stephens, D. G. Kilpatrick, P. R. Stasiewicz, R. A. Roffman, M. Bucuvalas, and S. Galea. 2006. Internet-based intervention for mental health and substance use problems in disaster-affected populations: A pilot feasibility study. Behaviour Research and Therapy 37(2)190-205.
Saffle, J. R., N. Gibran, and M. Jordan. 2005. Defining the ratio of outcomes to resources for triage of burn patients in mass casualties. Journal of Burn Care & Rehabilitation 26(6):478-482.
Sasser, S. M., R. C. Hunt, E. E. Sullivent, M. M. Wald, J. Mitchko, G. J. Jurkovich, M. C. Henry, J. P. Salomone, S. C. Wang, R. L. Galli, A. Cooper, L. H. Brown, and R. W. Sattin. 2009. Guidelines for field triage of injured patients. Recommendations of the National Expert Panel on Field Triage. Morbidity and Mortality Weekly Report. Recommendations and Reports 58(RR-1):1-35.
Scarfone, R. J., S. Coffin, E. S. Fieldston, G. Falkowski, M. G. Cooney, and S. Grenfell. 2011. Hospital-based pandemic influenza preparedness and response: Strategies to increase surge capacity. Pediatric Emergency Care 27(6):565-572.
Schreiber, M., and S. Shields. 2012. Anticipate, Plan, and Deter: building resilience in emergency health responders. Presented at the 2012 NACCHO (National Association of City and County Health Officials) Public Health Preparedness Summit, Anaheim, California.
Schreiber, M., B. Pfefferbaum, L. Sayegh, and J. Coady. In press. The way forward: The national children’s disaster mental health concept of operations. Disaster Medicine and Public Health.
Shahpori, R., H. T. Stelfox, C. J. Doig, P. J. Boiteau, and D. A. Zygun. 2011. Sequential Organ Failure Assessment in H1N1 pandemic planning. Critical Care Medicine 39(4):827-832.
Sills, M. R., M. Hall, H. K. Simon, E. S. Fieldston, N. Walter, J. E. Levin, T. V. Brogan, P. D. Hain, D. M. Goodman, D. D. Fritch-Levens, D. B. Fagbuyi, M. B. Mundorff, A. M. Libby, H. O. Anderson, W. V. Padula, and S. S. Shah. 2011. Resource burden at children’s hospitals experiencing surge volumes during the spring 2009 H1N1 influenza pandemic. Academic Emergency Medicine 18(2):158-166.
Singanayagam, A., A. Singanayagam, V. Wood, and J. D. Chalmers. 2011. Factors associated with severe illness in pandemic 2009 influenza A (H1N1) infection: Implications for triage in primary and secondary care. Journal of Infection 63(4):243-251.
Society of Critical Care Medicine Ethics Committee. 1994a. Attitudes of critical care medicine professionals concerning distribution of intensive care resources. Critical Care Medicine 22:358-362.
Society of Critical Care Medicine Ethics Committee. 1994b. Consensus statement on the triage of critically ill patients. Journal of the American Medical Association 271:1200-1203.
Tabery, J., and C. W. Mackett, III. 2008. Ethics of triage in the event of an influenza pandemic. Disaster Medicine and Public Health Preparedness 2(2):114-118.
Talmor, D., A. E. Jones, L. Rubinson, M. D. Howell, and N. I. Shapiro. 2007. Simple triage scoring system predicting death and the need for critical care resources for use during epidemics. Critical Care Medicine 35(5):1251-1256.
Toner, E., R. Waldhorn, C. Franco, B. Courtney, K. Rambhia, A. Norwood, T. Inglesby, and T. O’Toole. 2009. Hospitals rising to the challenge: The first five years of the U.S. hospital preparedness program and priorities going forward. Baltimore, MD: Center for Biosecurity of UPMC.
Trotter, G. 2010. Sufficiency of care in disasters: Ventilation, ventilator triage, and the misconception of guideline-drive treatment. Journal of Clinical Ethics 21(4):294-307.
University of Minnesota. 2007. Caring for pregnant/birthing women and their newborns during disasters: An introduction to the issues. http://www.nursing.umn.edu/meret/MERET_Courses/moms_module.html (accessed February 27, 2012).
University of Toronto. 2005. Stand on guard for thee: Ethical considerations in preparedness planning for pandemic influenza. University of Toronto Joint Centre for Bioethics Pandemic Influenza Working Group. Toronto, Canada: University of Toronto.
U.S. Census Bureau. 2012. State & county QuickFacts. http://quickfacts.census.gov/qfd/states/00000.html (accessed February 27, 2012).
USAISR (U.S. Army Institute of Surgical Research). 2009. Tactical Combat Casualty Care guidelines. http://www.usaisr.amedd.army.mil/tccc/TCCC%20Guidelines%20091104.pdf (accessed February 25, 2011).
Utley, M., C. Pagel, M. J. Peters, A. Petros, and P. Lister. 2011. Does triage to critical care during a pandemic necessarily result in more survivors? Critical Care Medicine 39(1):179-183.
VA (Department of Veterans Affairs). 2006. Staff discussion forum materials: Ethical issues in pandemic influenza preparedness and response—material to guide staff discussions. Washington, DC: http://www.ethics.va.gov/docs/pandemicflu/VA_Pandemic_Flu_Forum_Guide_040507.pdf (accessed March 15, 2012).
VA. 2010. Emergency Management Program Guidebook. Washington, DC.
VA. 2012. Ethical issues in pandemic influenza preparedness. Washington, DC: Department of Veterans Affairs, http://www.ethics.va.gov/docs/pandemicflu/Meeting_the_Challenge_of_Pan_Flu-Ethical_Guidance_VHA_20100701.pdf (accessed March, 15, 2012).
VA. [no date]. VAfact sheet for health care staff: Meeting the ethical challenges of a severe pandemic influenza. Washington, DC: VA, http://www.ethics.va.gov/docs/pandemicflu/Ethics_and_Pandemic_Flu_Fact_Sheet_508_2010-09-30.pdf (accessed March 15, 2012).
Veterans Health Administration. 2010. Meeting the challenge of pandemic influenza: Ethical guidance for leaders and health care professionals in the Veterans Health Administration. Washington, DC: Veterans Health Administration, http://www.ethics.va.gov/activities/pandemic_influenza_preparedness.asp (accessed March 15, 2012).
Vawter, D. E., J. E. Garrett, K. G. Gervais, A. W. Prehn, D. A. DeBruin, C. A. Tauer, E. Parilla, J. Liaschenko, and M. F. Marshall. 2010. For the good of us all: Ethically rationing health resources in Minnesota in a severe influenza pandemic. St. Paul, MN: Minnesota Center for Health Care Ethics and University of Minnesota Center for Bioethics, http://www.health.state.mn.us/divs/idepc/ethics/ (accessed February 27, 2012).
Vincent, J. L., R. Moreno, J. Takala, S. Willatts, A. De Mendon?a, H. Bruining, C. K. Reinhart, P. M. Suter, and L. G. Thijs. 1996. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Medicine 22(7):707-710.
Vincent, J. L., A. de Mendonca, F. Cantraine, R. Moreno, J. Takala, P. M. Suter, C. L. Sprung, F. Colardyn, and S. Blecher. 1998. Use of the SOFA score to assess the incidence of organ dysfunction/failure in intensive care units: Results of a multicenter, prospective study. Working group on “Sepsis-related problems” of the European Society of Intensive Care Medicine. Critical Care Medicine 26(11):1793-1800.
West, J. B. 2005. The physiological challenges of the 1952 Copenhagen poliomyelitis epidemic and a renaissance in clinical respiratory physiology. Journal of Applied Physiology 99(2):424-432.
Xiong, W., A. Bair, C. Sandrock, S. Wang, J. Siddiqui, and N. Hupert. 2010. Implementing telemedicine in medical emergency response: Concept of operation for a regional telemedicine hub. Journal of Medical Systems (e-publication ahead of print).
Ytzhak, A., R. Sagi, T. Bader, A. Assa, A. Farfel, O. Merin, and Y. Kreiss. 2012. Pediatric ventilation in a disaster—clinical and ethical decision making. Critical Care Medicine 40(2):603-607.
Zygun, D. A. 2005. Limited ability of SOFA and MOD scores to discriminate outcome: A prospective evaluation in 1,436 patients. Canadian Journal of Anaesthesia 52(3):302-308.