Educating People with Epilepsy and Their Families
Accurate information for individuals with epilepsy and their families, education about the consequences of epilepsy, and skills development in self-management are essential components for helping individuals become better partners in patient-centered care. People with epilepsy and their families are often not educated about epilepsy’s risks, including injury and mortality. Parents of children with epilepsy need information about the disorder and available support resources. Children and youth with epilepsy, as they get older, need increasing information about the disorder and its implications for their future. Adults’ information priorities relate to employment, driving, and management of stress; and women need information about hormonal influences on the disorder and the potential effects of seizure medications on pregnancy. Older adults also may have specific information needs, given the likelihood they are taking medications for other chronic health conditions and have an increased risk of falls. People often rely on health care providers for this information, and a wealth of information is offered in written form and online. However, research suggests that both printed and online epilepsy information is written at too high a literacy level. Actions needed to improve education for people with epilepsy and their families include evaluating available educational resources, such as Internet resources and tools; expanding the reach and dissemination of available resources; engaging people with epilepsy and their families in developing and testing educational resources; evaluating, replicating, and expanding the use of self-management programs; and exploring new opportunities for improving education, such as a centralized web resource to connect people with epilepsy to reliable websites and a certification program for epilepsy health educators.
Our introduction to epilepsy came when we were abruptly woken to the sound of Savannah shaking and gagging. Doctors called her seizures attacks and spells, but never seizures…. [A]s a family living with these [epilepsy] statistics, what do we need? In the early years, we needed the facts—like the fact that approximately 33 percent of people with epilepsy don’t respond to treatment. We lost a great deal of trust in doctors because of their choice to censor.
–Tracy Dixon-Salazar
The diagnosis of epilepsy, although given to an individual, affects the entire family and its constellation of friendships and other relationships. At onset all are confronted with the immediate need to learn about the disorder and its management. Receiving helpful information and education1 in the diagnostic phase of a chronic health condition can facilitate coping, because early perceptions may affect long-term adjustment to the condition (Johnson, 2003). Living with epilepsy, its unpredictable seizures, and its comorbid conditions presents many challenges over time. Again, continued educational efforts can play a key role in helping people learn to live with and understand epilepsy and its effects over the life span. Thus, individuals and families need education and skills building throughout the course of the disorder, particularly during times of change, such as an increased frequency of seizures, changes in treatment (e.g., switching medications, starting a new treatment option, discontinuing a medication or other treatment option), and major life transitions (e.g., from youth to adulthood, from adulthood to older adulthood).
This chapter describes goals and priorities for educating people with epilepsy and their families, their knowledge acquisition needs across the life span, and methods through which individuals and families currently learn about epilepsy. It reviews different models, programs, and approaches to providing epilepsy education that have been developed and contrasts them with educational efforts in other chronic disease fields, in order to identify strategies for improvement.
_______________
1For this report, the committee conceptualized awareness, information, education, and skills building as representing a rough continuum of knowledge development regarding epilepsy. Awareness is often the first step in knowledge development (discussed further in Chapter 8) and can be targeted to reducing stigma. For some diseases and conditions, awareness suffices for people in the general public. Information is what the public, to be well informed, needs to know about epilepsy (or other common medical conditions). Information tends to be general but suffices for most people not involved in the care or supervision of individuals with epilepsy. Education is the goal of efforts to provide more in-depth knowledge that increases understanding, decision-making capacity, and preparedness for action among people with epilepsy, families, and caregivers. Skills-building efforts are aimed at helping people acquire the specific capacities to carry out certain tasks. In the context of epilepsy, skills-building is often aimed at improving self-management and care provided by family members or other caregivers and begins with education.
GOALS AND PRIORITIES FOR EDUCATION
In conceptualizing goals for patient and family education,2 the committee considered recommendations for health care from the Institute of Medicine in Crossing the Quality Chasm: A New Health System for the 21st Century. The report recommends that health care in the 21st century be patient centered, which involves health care providers’ partnering with patients and families so that the care provided “is respectful of and responsive to individual patient preferences, needs, and values and [ensures] that patient values guide all clinical decisions” (IOM, 2001, p. 6). As described in Chapter 4, patient-centered care is the committee’s foundation for an epilepsy care model. The medical literature supports the importance of a patient-centered approach and indicates that people prefer patient-centered care. It even suggests which aspects of patient-centered care are most important to them. For example, a study of UK patients found that three important components of a patient-centered approach were “communication, partnership, and health promotion” (Little et al., 2001, p. 468). For patient-centered care and physician-patient partnerships to work, consistent, relevant health education efforts for patients and families are required.
Cochrane (1995) emphasizes that epilepsy education helps people with epilepsy become self-confident, competent in self-management, aware of their needs, and able to access resources to meet their needs—in other words, it helps them become better partners in patient-centered care. Moreover, having accurate, in-depth information about epilepsy helps people better understand the disorder, prevents misconceptions, and reduces concerns about stigma. Finally, epilepsy education helps promote optimal well-being and quality of life. The committee’s vision is for all individuals with epilepsy and their families to have access to relevant and usable knowledge to meet their individual needs and allow them to participate effectively in patient-centered care, to be competent in the management of their epilepsy, and to attain the best possible physical and emotional well-being.
UNDERSTANDING INFORMATION NEEDS
In patient-centered care, the specific health and quality-of-life needs of people with epilepsy and their family members must be paramount in guiding the care provided by health professionals; similarly, the information,
_______________
2As noted in Chapter 1, terminology is a challenge for people with epilepsy and for the field in general. The committee was purposeful in the terms used throughout this report. The committee recognizes that people with epilepsy and their families should not always be identified as patients, and throughout the report individuals are usually referred to as patients only when there is a direct intersection with health care providers or the health care system. However, for the sake of brevity, the committee uses the phrase “patient and family education” or “patient and caregiver education” in this chapter.
knowledge, and skills-building needs of patients and families must guide educational efforts.
Lack of Knowledge and Familiarity with Epilepsy
At the time of epilepsy onset and diagnosis, most patients and families probably know as much about epilepsy as the general public does, and their knowledge does not always improve in the period following diagnosis (Elliott and Shneker, 2008). Literature reviews and U.S. surveys show that knowledge about epilepsy among the general public is low (Chapter 8):
• An analysis of the 2002 Porter Novelli HealthStyles Survey results concluded that only about one-fourth of respondents believed they were knowledgeable about epilepsy, and only about one-third thought they knew what to do in the event of a seizure (Kobau and Price, 2003).
• A large telephone survey of U.S. Spanish-speaking adults found a similar lack of information about epilepsy and many misperceptions about the causes of seizures, beliefs that people with epilepsy were dangerous, and the use of unconventional treatments such as vitamins, herbal remedies, and spiritual healing (Sirven et al., 2005).
• According to Paschal and colleagues (2005), lack of knowledge and misperceptions about epilepsy in the African American community increase the stigma burden on African Americans with epilepsy. Moreover, people with epilepsy reported they had to spend a substantial amount of time teaching family members about their disorder.
Research consistently demonstrates that people with epilepsy themselves do not have a solid understanding of basic information about the condition, including knowledge about their diagnosis, seizure precipitants or triggers, specific seizure type(s), the purpose and potential side effects of seizure medications, safety concerns, and the risks and potential consequences of seizures (Bishop and Allen, 2007). In one of the few U.S. studies that examined knowledge about epilepsy among people with the disorder, less than 60 percent of the questions were answered correctly (Long et al., 2000). Thirty percent of respondents believed that epilepsy is contagious or a type of mental disorder. Some of this misinformation had the potential to affect personal safety; for example, 41 percent of people with epilepsy believed that something should be put in the mouth of the person having a seizure, 25 percent thought that women should discontinue medication when they are pregnant, and 25 percent believed it is safe to drive if they
double their medication dose before driving, do not drive alone, or pull over when they feel a seizure coming on (Long et al., 2000).
When children lack knowledge about epilepsy, they are more likely to be worried and to have more negative attitudes about having epilepsy (Austin et al., 2006b). Moreover, when parents of children with epilepsy lack adequate knowledge or hold inaccurate beliefs about epilepsy, they may develop negative attitudes and reduced expectations for their children (Frank-Briggs and Alikor, 2011).
Knowledge Needs of All People with Epilepsy and Their Families
The literature indicates that all individuals with epilepsy and their families need to receive some level of education about the disorder, especially as it relates to each person’s specific diagnosis and treatment plan. It is especially important that individuals with epilepsy and their families be given, preferably in writing, specific information about their syndrome, seizure type, and treatment plan. A review of literature on health information for adults with epilepsy by Couldridge and colleagues (2001) identified specific information needs related to diagnosis and treatment options, medications and their side effects, seizures and seizure control, safety and injury prevention, and common social and psychological problems. Individuals with epilepsy and their families also need to be informed about the full range of comorbid conditions associated with the disorder, including mental health, cognitive, neurological, and somatic disorders (Chapter 3).
People with epilepsy and their family members may have many fears when the diagnosis is made. The onset of epilepsy during childhood can be particularly frightening (Oostrom et al., 2001), and seeing seizures may make parents believe their child’s condition is life-threatening (Besag et al., 2005). Children and adults with epilepsy likewise fear that mental health conditions, injury, or death may ensue (Austin, 2000). To manage these fears and prevent unnecessary anxiety, people with epilepsy and their families need complete and accurate information about the comorbidities and mortality risks associated with epilepsy, including sudden unexpected death in epilepsy (SUDEP), suicide, the risks of seizure-related injuries, and the risks of prolonged seizures such as status epilepticus (Ficker et al., 1998; Kwon et al., 2011; So et al., 2009). Patients and families need to be made aware of the risk for suicidal ideation associated with seizure medication, including symptoms of depression and mood changes that should be reported to health care providers (FDA, 2008).
My son, Tyler Joseph Stevenson, passed away on January 23, 2011, from a seizure in his sleep at the young age of 20. The more research we do and the interactions with families who have lost loved ones to SUDEP all share that they were never advised that their loved one could die from epilepsy
or a seizure. I knew in my previous research that people with epilepsy do not normally live as long as others but did not think that Tyler would die so young.
–Mark J. Stevenson
My son, Dallas, at the age of 5, passed away on January 12, 2011, of SUDEP. I and many other parents had never even heard of SUDEP until we lost our child. Physicians don’t want to scare parents, so they don’t discuss SUDEP, but the medical community has a responsibility to properly inform patients and parents of SUDEP risk factors. The risk factors may not always be controlled, but it is only fair to tell parents the risks that are involved.
–Mylissa Daniels
The majority of families first hear about [SUDEP] upon the loss of their loved one. Realization of a lack of prior knowledge can have a devastating emotional impact, not only for individuals bereaved by a death in their family but also for individuals who first learn of SUDEP after having lived with epilepsy for some time. Education and communication is paramount to prevent this.
–Tamzin Jeffs
During its public workshops, the committee heard testimony from several families who had lost loved ones due to SUDEP; all of the families reported that health professionals had not discussed SUDEP with them, and they advocated for SUDEP education and information for people with epilepsy and their families (see excerpts of testimony above). Additional work is necessary to determine if health professionals need more education and knowledge about SUDEP generally and if they need more education on how to discuss this and other sensitive topics related to risks and mortality with their patients. Hirsch and colleagues (2011) recommended the development of evidence-based guidelines to inform health professionals of “why, when, and how SUDEP should be discussed with people affected by epilepsy” (p. 1937) based on discussion at a 2008 SUDEP workshop hosted by the National Institute of Neurological Disorders and Stroke. Additionally, the efficacy and reach of existing SUDEP educational materials designed for health professionals and individuals with epilepsy and their families needs to be reviewed and additional materials may have to be developed.
Interviews with UK adults with epilepsy indicated a desire for more information about a broad range of disease-related topics, including mortality risks (Prinjha et al., 2005). A survey of UK neurologists indicated that only 30 percent discussed SUDEP with all or a majority of their patients, and one of the most common reasons for such a discussion was that the patients requested it (Morton et al., 2006). Similarly, a UK survey of pediatric neurologists and parents found that 91 percent of the parents desired information about SUDEP, but only 20 percent of the neurologists
consistently provided it to all patients (Gayatri et al., 2010). In this study, 61 percent of parents did not want their children to be told about SUDEP, while 21 percent did. Of those wanting their children to be told, almost half of the parents wanted to be the ones to tell them, and about one-third wanted the health professional to do so (Gayatri et al., 2010).
People with epilepsy and their families also need information about living a healthy lifestyle, not only because of the impact of epilepsy, but also because of the associated physical comorbidities (e.g., diabetes, heart disease, high blood pressure). A survey of adults showed that in addition to information about epilepsy and their treatment, they wanted information on self-management, available social and community resources, support groups, and counseling (Paschal et al., 2007). Box 7-1 provides an overview of these broad information needs. Having access to information about healthy lifestyles and community resources is essential for ensuring that people with epilepsy are able to achieve the best possible quality of life (see also Chapter 6).
In a survey conducted by Paschal and colleagues (2007), concerns about stigma were prominent, with 89 percent of respondents perceiving that the public lacks awareness of and knowledge about epilepsy, 65 percent experiencing stress because of this lack of awareness, and 42 percent reporting stigma in the general public. Feelings of secrecy, shame, and worry about stigma also were identified in a qualitative study of children and adolescents (Lewis and Parsons, 2008). As described in Chapter 6, stigma has been associated with diminished quality of life. Additional work is needed to examine the role that educational materials and programs, support groups, and counseling resources may play in helping individuals and their families successfully cope with stigma and related concerns, such as the fear of having a seizure in public.
Knowledge Needs of Children, Adolescents, and Youth Transitioning to Adulthood
Studies consistently indicate that children and adolescents with epilepsy need increasing knowledge about their condition over time, tailored to their growing ability to comprehend the information and its implications. Empirical evidence suggests that children’s information needs are not being met. For example, a prospective study indicated that these needs remained high even 2 years after seizure onset, with 64 percent of children continuing to have questions about epilepsy’s causes, 64 percent still wanting to talk to another child who has seizures, and 62 percent wanting more information about keeping safe during a seizure (Shore et al., 2009).
Children and adolescents want to understand and resolve their fears related to epilepsy, to understand how it might affect their future, and to
Box 7-1 EXAMPLES OF BROAD KNOWLEDGE AREAS FOR PEOPLE WITH EPILEPSY AND THEIR FAMILIES
Basic Educational Needs of All People with Epilepsy
- Epilepsy—seizure type, syndrome, causes
- Treatment and management—options, medications, devices, surgery, dietary modifications, side effects, treatment discontinuation, seizure triggers, risk for suicidal ideation associated with medications, other management strategies
- Safety risks—risk assessment, seizure first aid, injury prevention, equipment to prevent injury
- Mortality risks—sudden unexpected death in epilepsy, status epilepticus, seizure-related injury, suicide
- Healthy lifestyle—general health, sleep, fatigue, physical exercise
- Possible comorbidities
- Mental health (e.g., anxiety, depression, attention problems, behavior problems, psychosis, seizure-like events with a psychological basis)
- Cognitive (e.g., memory, information processing problems, learning problems)
- Neurological (e.g., stroke, autism spectrum disorders, migraine)
- Somatic (e.g., heart disease, bone health)
- Social concerns—engaging new friends, seizures in social settings, telling others, family burden, stigma
- Emotional response—coping, dealing with fears, stress management
- Available informational and community resources—websites, state and local Epilepsy Foundation affiliates, community agencies, health care providers
Specific Educational Needs for Population Subgroups
Children, adolescents, and youth transitioning to adulthood
- School—managing seizures at school, common learning problems, safety, participation in extracurricular activities
learn how to manage it in their daily lives, especially at school (McNelis et al., 1998). A UK study demonstrated that providing information about mortality, including SUDEP, is especially relevant for youth, because of the higher death rates in individuals under age 30 who have long-term epilepsy (Mohanraj et al., 2006). While reluctant to initiate a conversation about sensitive topics such as alcohol use and sexual activity, older adolescents participated in these discussions when health professionals began them (Lewis et al., 2010). However, the researchers found that young people believed health professionals were more interested in providing medical information than in helping with more practical aspects of daily living (Lewis et al., 2010).
Youth transitioning into adulthood need information and knowledge that will help them assume appropriate responsibility for managing their epilepsy and living a healthy lifestyle. However, few studies could be found
- Mental health—attention deficit hyperactivity disorder, autism spectrum disor-ders, social withdrawal
- Dealing with fears—future, death, mental health conditions, stigma
- Lifestyle management—establishing healthy habits
- Opportunity to discuss sensitive information, such as puberty, sexuality, drugs, and alcohol
- Career planning
- Transition to adulthood, such independence and driving
Adults
- Career and vocational concerns
- Discussions with employers
- Driving regulations and transportation concerns
- Sexual and gender-specific topics, such as reproductive health and family planning, hormonal changes and seizure frequency, effects of seizure medications on pregnancy
- Drug-alcohol interactions Impact on relationships Independent living
Older adults
- Medication side effects, adverse interactions, and adherence
- Drug-alcohol interactions Independent living
- Safety and injury risks
that focused on the needs of this “in-transition” group. Jurasek and colleagues (2010) believe these youth need to be knowledgeable about the following:
• Epilepsy management—Knowledge about their specific epilepsy condition (e.g., specific syndrome, seizure type and triggers) and treatment plans helps them make informed decisions about care.
• Topics that emerge during adolescence—Knowledge about topics such as sexuality, alcohol and drug use, and driving, in the context of living with epilepsy, helps to support informed decision making.
• Living independently—Skills that facilitate independent living are related to (1) education, career, and employment decisions; (2) living a healthy lifestyle, including managing stress and getting sufficient sleep; (3) self-management skills, such as knowing which
health care provider to contact, getting to appointments, knowing how to fill prescriptions, and medication adherence strategies; and (4) obtaining and paying for medications.
Knowledge Needs of Adults
In a large national survey, adults with epilepsy indicated that they have many fears related to seizures or dying during a seizure and that they face specific social challenges, including potential embarrassment about having a seizure in public (Fisher, 2000). Areas in which adults desired more information were related to employment (e.g., discussion of epilepsy with employers), the link between seizures and stress, dealing with cognitive problems, managing their emotions, and sleep and fatigue (Fraser et al., 2011). In another study, adults also needed more information about driving regulations (Couldridge et al., 2001) (see also Chapter 6).
Gender-Specific Needs
The predominant knowledge needs of women and men with epilepsy are summarized in Box 7-2.
Women The specific knowledge needed by women with epilepsy, which may vary by age, has generally received insufficient attention. Because sex hormones can affect seizure frequency, girls and women need information related to hormonal fluctuations and seizure frequency.3 Further, women of reproductive age need to understand how their epilepsy and its treatment could affect pregnancy. In a UK survey, adult women with epilepsy between the ages of 19 and 44 identified their most important information needs as relating to risks of epilepsy and medication affecting the fetus (87 percent), the effect of pregnancy on seizure control (49 percent), and the risk of their children developing epilepsy (42 percent) (Crawford and Hudson, 2003). For example, recent findings that show an increased risk for congenital malformations and impaired cognition in children of women treated during pregnancy with valproate, a commonly used seizure medication, suggest that all women of child-bearing age need to be kept apprised of the latest research in this area (Harden et al., 2009). Women with epilepsy also have been found to have higher-than-expected rates of sexual dysfunction (Pennell and Thompson, 2009). Among women over age 44, the most
_______________
3Studies have found higher-than-expected onset of seizures during the year of menarche; in girls with preexisting seizures, 29 percent experienced more frequent seizures during peri-menarche (Klein et al., 2003). Because of hormonal fluctuation, some women have a cyclic pattern of seizure frequency associated with their menses that often is unrecognized (Pennell and Thompson, 2009).
Box 7-2 EXAMPLES OF SPECIFIC KNOWLEDGE NEEDS FOR WOMEN AND MEN
• Pregnancy, effects of medications on the fetus, and breastfeeding (women)
• Bone health
• Hormonal states (e.g., sexual dysfunction; fertility rates; for women: menarche, monthly hormonal patterns, menopause, hormone replacement therapy)
• Sexual dysfunction
• Reproductive endocrine disorders (women)
• Driving and transportation
• Employment
• Cognitive problems—memory
• Social concerns
important information needs concerned epilepsy medication and osteoporosis (63 percent), seizure medications and aging (57 percent), and seizure changes during menopause (44 percent) (Crawford and Hudson, 2003).
Men One of the least studied subgroups of people with epilepsy is men. Studies show that men with epilepsy are less likely to be married, they have lower-than-expected fertility rates, and about one-fourth have problems with sexual dysfunction (Pennell and Thompson, 2009). In one of the few studies examining the perceptions and experiences of adult men with epilepsy, 18 percent rated themselves at the highest level of knowledge about the condition, but 25 percent said they have a low level of knowledge (Sare et al., 2007). In that study, the men’s most common concerns related to limitations on driving and employment. More than half of the men reported that their epilepsy affected them either “a lot” or “some” in other areas, such as memory problems, confidence, ambition and plans for the future, sense of self-esteem, overall health, social life, and quality of life. Finally, more than half indicated that they worried about the possibility that their children might inherit their epilepsy.
Knowledge Needs of Older Adults
The education needs of older adults with epilepsy, their family members, and other caregivers are poorly understood and underexplored (Martin et al., 2003). The committee found few studies that considered them. Likely areas for education were identified by extrapolating factors that are unique to older adults with epilepsy. For example, because older adults are especially vulnerable to the adverse effects of medication (Leppik, 2006), they need education about the side effects of seizure medications, particularly given the likely complications of aging-related factors, such as
memory impairment, complex multidrug regimens, and difficulty affording medications (Rowan, 2000).
An important concern among older adults is avoiding fall-related injuries, which may result in skeletal fractures. Risks for fractures are significantly higher in people with epilepsy than in the general population (Donald and Bulpitt, 1999; Gaitatzis et al., 2004; Tinetti and Williams, 1997) (Chapter 3). In addition to seizures, contributing risk factors for falls include female gender, polytherapy, side effects of seizure medications (including dizziness or ataxia), and coexisting neurological conditions and deficits (Fife et al., 2006; Mattson and Gidal, 2004). The high prevalence of osteoporosis among older adults increases the risk of injury when falls occur (Cohen et al., 1997; Pack and Morrell, 2001). In a recent community-based survey of older adults living with epilepsy, Martin and colleagues (2005) identified that driving and transportation and medication side effects were the most frequently cited concerns, followed by personal safety, medication costs, employment, social embarrassment, and memory loss. Information about independent living resources and housing modifications to enhance and increase personal safety at home was also indicated.
Additionally, consideration should be given to the educational needs of older adults who are newly diagnosed versus those of older adults who were diagnosed at an earlier age and who have lived with epilepsy for many years. Although few studies have been conducted to assess the knowledge needs of older adults, as mentioned above, individuals who have lived with epilepsy for a long time and who are transitioning from adulthood to older adulthood may need information on how aging could affect their epilepsy and treatment regimens (e.g., necessary dosage adjustments). Older individuals with new-onset epilepsy may need basic information about epilepsy, such as seizure type, treatment side effects, and safety. For example, if their seizures developed as a result of another condition, such as a stroke or Alzheimer’s disease, they also may require information about the interplay of their condition and epilepsy.
Education Needs of Parents and Other Caregivers
Research demonstrates that families of children with epilepsy function less well, experience more problems in parent-child relationships, and show more maternal stress and depression than families of children with other chronic conditions (Rodenburg et al., 2005). Studies show that parents of children with epilepsy experience high rates of stress, anxiety, and depression, particularly when the child has a comorbid condition such as a behavior disorder or intellectual disability (Buelow et al., 2006; Chiou and Hsieh, 2008; Ferro and Speechley, 2009; Lv et al., 2009; Mu, 2005; Wood et al., 2008). Children’s depression and learning disabilities can significantly
increase the stress of parenting (Cushner-Weinstein et al., 2008). Parents need information and strategies that can help them come to terms with having a child with epilepsy so that they, in turn, can help their children cope more effectively (Austin and Tooze, 2003). Families especially require reliable information about accessing services to meet their children’s needs (Mu, 2008; Nolan et al., 2008; Wagner et al., 2009; Wu et al., 2008), communicating with health professionals, interacting with school personnel, and finding support in the community (Buelow et al., 2006; Wagner et al., 2009). In focus groups, parents report needing information about how to coordinate health care among the numerous medical consultants and specialists with whom they interact (McNelis et al., 2007). Box 7-3 provides an overview of the educational needs of parents and other caregivers.
Few studies describe the educational needs of parents with infants or very young children with epilepsy or children with more severe forms of childhood-onset epilepsies, such as Lennox-Gastaut syndrome, infantile spasms (West syndrome), and severe myoclonic epilepsy of infancy (Dravet syndrome). Studies by Nolan and colleagues (2006, 2008) examined how families of children with Dravet syndrome coped across different stages of the disorder. These parents experienced such high levels of stress from the frequent seizures and behavioral problems that the integrity of the parental relationship and other social relationships was threatened. With regard to managing the syndrome, parents reported that they needed help with identifying social and community resources, such as respite care, and that they also needed specific information on developing a protocol for emergency management of seizures (Nolan et al., 2006). They reported that online support groups were helpful to connect them with other families whose children had Dravet syndrome and other severe syndromes (Nolan et al., 2008).
Educational needs of caregivers vary depending on their relationship to the person with epilepsy, their role in providing care, and their emotional needs. Kendall and colleagues (2004) conducted a study of families and
Box 7-3 EXAMPLES OF SPECIFIC EDUCATIONAL NEEDS OF PARENTS AND OTHER CAREGIVERS
• First aid for seizures
• Parenting concerns—overprotection, discipline, accessing needed services
• Emotional response
• Typical child cognitive and psychosocial development
• Sources of age-appropriate information for children
• Resources—respite care, support groups, equipment, assistance in navigating health care, school, and community services
• Advocacy skills
caregivers of older teens and adults with epilepsy and identified several themes related to educational needs. Barriers to receiving information included respondents’ lack of confidence in their ability to seek the needed information and health care providers’ not recognizing that caregivers have unique information needs. Some caregivers reported that they felt that health care providers did not care about their information needs (Kendall et al., 2004).
Needs of People with Seizure-Like Events
In many cases, seizure-like events include symptoms very similar to the seizures associated with epilepsy, but occur without the electrophysiological changes associated with epilepsy seizures (Carton et al., 2003). These events can be attributed to psychological causes and may occur in people who have a confirmed epilepsy diagnosis as well as those who do not. There is scant evidence of what constitutes appropriate management of seizure-like events that have been identified as not being epilepsy (Martlew et al., 2007), and little is known about the knowledge needs of people with seizure-like events. A study investigating response to diagnosis in patients with these types of events who had been misdiagnosed previously with epilepsy found that the most common reactions to the new diagnosis were confusion (38 percent), relief (21 percent), and anger (18 percent) (Carton et al., 2003). Factors associated with poor outcomes were persistent seizure-like events and responding to the diagnosis with either confusion or anger (Carton et al., 2003). Carton and colleagues recommend that people with seizurelike events that have a psychological basis receive understandable information about the new diagnosis, that their retention of information is checked later, and that they be referred to psychological resources. Box 7-4 includes examples of education needs for individuals with these types of events.
Closing Knowledge Gaps
In general, the committee found substantial evidence that people with epilepsy, their families, and caregivers want more information than they
Box 7-4 EXAMPLES OF SPECIFIC EDUCATIONAL NEEDS OF PEOPLE WITH SEIZURE-LIKE EVENTS
• Information about seizure-like events that are not epilepsy
• Information about treatment
• Emotional support—coping with a new diagnosis
• Resources—psychological counseling
currently receive and that they want to be educated in a manner that best meets their specific situations (see discussion below). Although all people with epilepsy and their families need certain basic information, beyond that, educational needs vary because of the wide diversity in the epilepsies (e.g., seizure type, severity, comorbidities), ages of onset, cognitive abilities, health literacy levels, and cultural and demographic considerations.
The quality and scope of the research literature exploring these knowledge gaps varies, and the committee identified persistent gaps in research to support patient and family education. Across the board, the current research base on the design and implementation of educational programs for people with epilepsy, regardless of demographic group, is insufficient. A number of groups have specific vulnerabilities that educational programs could take into account. For example, recent studies have tied racial and ethnic minority populations’ beliefs that epilepsy medications are harmful or only minimally helpful to lower medication adherence (Nakhutina et al., 2011), which may help explain African Americans’ lower epilepsy medication adherence in comparison with Caucasians (Bautista et al., 2011). Although more research is needed to clarify these topics, the gaps already identified need to be eliminated.
These gaps might be remediated, at least in part, through targeted patient and family education efforts. Moreover, people with persistent seizures, severe forms of epilepsy, or more severe comorbidities and their caregivers undoubtedly will have relatively greater needs for education. Much of the research conducted on education needs was based on international samples, and findings from these studies might not directly translate to the U.S. population, because of health system, cultural, and other differences.
WHERE, WHEN, AND HOW PEOPLE WITH EPILEPSY AND THEIR FAMILIES RECEIVE INFORMATION
Traditionally, people with epilepsy and their families received information and education about the disorder one-on-one from health care providers. Although many people still prefer to receive health education in this manner (Fraser et al., 2011; Kendall et al., 2004), it is not always practical for today’s clinicians to provide extensive education. Consultation times with neurologists and other health care providers are brief, and patients commonly report that provider visits are rushed (Escoffery et al., 2008; Gilliam et al., 2009; Prinjha et al., 2005). In a recent study by Gilliam and colleagues (2009), epilepsy patients’ clinical interviews with neurologists averaged slightly less than 12 minutes; Figure 7-1 depicts the proportion of time spent discussing a range of topics. Four percent of a 12-minute visit—
the amount of time spent on quality of life and daily living—amounts to less than half a minute.
Some settings, such as large health care systems and epilepsy centers, may employ nurses who specialize in epilepsy to help provide patient education (see also Chapter 4). However, such personnel are not generally available to people who receive care from primary care providers, general pediatricians, or neurologists in private practice.
The educational content of clinical encounters may be further limited by patient discomfort in asking questions or by other factors that impede effective communication (DiIorio et al., 2003; Swarztrauber, 2004). For these and a number of other reasons, individuals with epilepsy and their families increasingly seek information from sources outside the health care setting. In fact, many providers recommend that patients and families seek information from outside sources to complement their own educational efforts. It is important that health professionals who educate patients and their families in a clinical setting understand the specific information needs and preferences of patients and their families and take into consideration factors related to health literacy and culture, including cultural differences that may exist between them and their patients (Chapter 5).
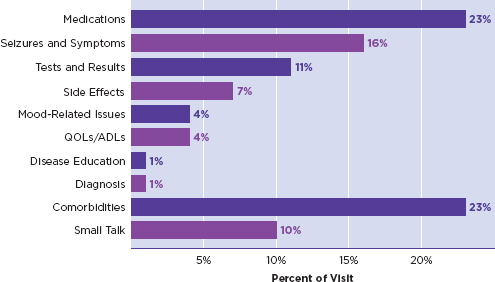
FIGURE 7-1
Topics discussed and percent visit spent on each.
NOTE: QOLs = quality of life; ADLs = activities of daily life.
SOURCE: Gilliam et al., 2009. Reprinted with permission from Elsevier.
Timing, Format, and Delivery of Epilepsy Education
Timing
Few studies have investigated how epilepsy information should be provided, and most such studies were conducted in the United Kingdom. Interviews and surveys provide some information related to appropriate timing, format, and delivery of epilepsy patient and caregiver education. The greatest agreement across studies relates to timing. Although information could be given when a person seeks care for the first seizure, as described below, there is general consensus that education about epilepsy is more effective when provided around the time of diagnosis, inclucing when waiting for diagnosis, at diagnosis, and after the reality of the diagnosis has set in.
Because receiving an epilepsy diagnosis is often upsetting, health professionals must be sensitive to whether the patient and family are sufficiently recovered to be receptive to an educational intervention (Kendall et al., 2004). Even in less stressful situations, patient-provider and family-provider communications can miss the mark, and many efforts have been made to improve them.4 When discussing epilepsy, clear communication is essential. For example, a recent study found a persistent pattern of seizure medication nonadherence in 58 percent of children with new-onset epilepsy during the first 6 months of therapy; the authors emphasized the importance of providing clear information and education that dispels misconceptions about drug treatment at the time the medication is prescribed (Modi et al., 2011). As discussed below, people with epilepsy also need education to build skills in self-management, which include medication management skills.
A consensus appears to be growing that information about SUDEP should be provided around the time of diagnosis and within the context of a discussion related to epilepsy’s risks, either around the time of diagnosis or in the presence of SUDEP risk factors (e.g., when seizures persist, when treatment is refused, when generalized tonic-clonic seizures occur) (Devinsky, 2011; Hitiris et al., 2007; Lewis et al., 2008; Mohanraj et al., 2006; Shorvon and Tomson, 2011; So et al., 2009). In the case of young children or people with intellectual disabilities, of course, such information would be provided to family and caregivers.
Research suggests that some information is most useful before it is actually needed; for example, women need information about the effect of epilepsy on pregnancy and the possible effects of seizure medications on the fetus before becoming pregnant (Crawford and Hudson, 2003).
The timing of epilepsy education for young people depends on the youth’s ability to understand it and interest in receiving it. Because youth
_______________
4As one example, the National Patient Safety Foundation’s Ask Me 3 campaign (http://www.npsf.org/for-healthcare-professionals/programs/ask-me-3).
are often diagnosed with epilepsy when they are quite young, it is usually parents who need and receive education around the time of diagnosis. Age 13 to 19, when youth are transitioning to adult care, is considered a critical period for them to be educated about epilepsy and to learn skills that help them become responsible for appropriate self-management (Lewis et al., 2010). Finally, there is agreement that education related to living with epilepsy is most helpful if offered repeatedly at regular intervals over time and as needed during changes or transitions, as shown in Box 7-5.
Format and Delivery
Little evidence is available on the best format for education, with the exception that educational materials and information need to be customized to meet individual needs and circumstances, regardless of whether they are presented orally or in writing (Couldridge et al., 2001). In their literature review. Couldridge and colleagues (2001) found that some studies support information being provided in written form, rather than orally, because remembering oral information can be a challenge for people with epilepsy who may also have memory impairment. However, as described below, written materials can also present challenges for the large number of U.S. residents with low literacy and poor health literacy.
People vary as to their preferred format for receiving information. For example, in a study of family caregivers of adults with epilepsy in
Box 7-5 EXAMPLES OF CRITICAL JUNCTURES FOR PATIENT AND FAMILY EDUCATION
• At diagnosis
• During first year
• When there is a change or new concerns develop
• Developmental status (beginning school, transitioning from pediatric to adult care, transitioning from adulthood to older adulthood, living independently)
• Seizures (breakthrough seizures, type, frequency)
• Treatment-related concerns (surgery, change in or discontinuation of medication or other treatment, dietary therapy, alternative therapy, side effects, nonadherence)
• When treatment fails (reevaluation of options)
• Health status changes (pregnancy, injuries, other health complications)
• Life stressors (moving, change in occupation, change in marital status, death or grief)
• Travel (new environments, time changes)
• Comorbidities (mental health, cognitive, neurological, somatic)
• Employment and vocational status
the United Kingdom, Kendall and colleagues (2004) found the majority believed they obtained the most benefit when they received information orally during personal contact with a physician, preferably a neurologist (66 percent). As noted in Chapter 4, telemedicine offers an innovative delivery mechanism for patient care, and its effectiveness in providing patient education warrants further exploration. Telemedicine opportunities may be especially valuable for connecting health professionals and health educators to patients and caregivers who live in rural and geographically isolated areas or to patients for whom travel is difficult.
In their literature review on delivery of information to young people, Lewis and colleagues (2010) found that this population wanted to receive information in an age-appropriate format and that, while the presence of parents can be supportive, their absence can also have a positive impact in that youth may feel more comfortable discussing sensitive topics, such as alcohol use and pregnancy. These young people also wanted to see the same health care provider at each visit, in order to become more comfortable talking with them. Finally, they preferred to receive information in a quiet room rather than during clinic visits, which can be too distracting to attend to the information or to learn skills related to self-management (Lewis et al., 2010). As noted in Chapter 8, electronic media formats (e.g., the Internet, social networking) are very popular among youth and young adults, and they may present an opportunity for educating young people with epilepsy about the disorder and self-management.
Health Literacy Considerations for Educational Resources
Written materials, which are often used to augment a clinical encounter, can be an effective, inexpensive, and easy-to-implement strategy to improve patient and family understanding of a condition or its treatment (Arhan et al., 2009). However, they fall short of their potential when, as is often the case in the United States, materials for adults are written at a ninth-grade reading level or higher, even though the average U.S. adult reads at the eighth-grade level and materials for children and adolescents are written above a fifth-grade level (that is, a level more appropriate for some adults) (Foster and Rhoney, 2002; Safeer and Keenan, 2005). Almost 20 years ago, testing showed that 68 to 73 percent of U.S. parents could read at less than a ninth-grade level, and 28 to 55 percent read at less than a seventh-grade level (Davis et al., 1994). Materials that pediatricians typically give these parents—for example, consent forms, take-home instructions, and medication guidelines—are frequently poorly understood. At that time, the authors noted the trend within the American Academy of Pediatrics and the public health community to create more low-literacy materials. Recent reviews of both print and online epilepsy educational materials indicate the problem
persists, and the reviewers found scant content appropriate for low-literacy individuals and their families (Elliott and Shneker, 2009; Elliott et al., 2007; Foster and Rhoney, 2002; Rajasundaram et al., 2006). One analysis found that materials from general Internet sources and university websites required the highest level of reading ability, while other Internet material from state epilepsy organizations required the lowest (seventh grade, approximately) (Foster and Rhoney, 2002). The authors suggested that the common measures of readability used in their analysis5 may underestimate the difficulty in understanding health and medical written materials, because such information often contains unfamiliar terms or concepts.6
In an effort to provide guidance for developing materials that are user friendly and understandable to broad audiences for all health conditions, the Centers for Medicare and Medicaid Services produced a Toolkit for Making Written Material Clear and Effective (CMS, 2011a). Use of the toolkit is intended to provide practical assistance, not strict guidelines. Rather than specifying a target grade level or readability standard, the toolkit urges users to “orient toward the subset of your readers for whom the potential barriers are the greatest, that is, the readers who are less attentive, less interested, less knowledgeable, and less skilled at reading. If you can make your material work well for these readers, it will work well for the rest of your readers, too” (CMS, 2011a). It provides information on assessing the readability of a text and guidance on establishing a robust user feedback program. Similarly, the Centers for Disease Control and Prevention (CDC) has developed an array of materials to help public health entities and other health professionals create clear communications about health topics (CDC, 2011), notably Simply Put: A Guide for Creating Easy-to-Understand Materials, which also includes information on how to test the readability of a text. Commercial health literacy testing products also are available, such as those marketed by Health Literacy Innovations or the tests and strategies described in Pfizer, Inc.’s Clear Health Communication Program (Health Literacy Innovations, 2012; Pfizer, 2012).
The National Action Plan to Improve Health Literacy recommends that developers of health educational content of any type (e.g., web, audio, video, print)
• adopt user-centered design (e.g., involve members of the target audience in product design and testing),
• target and tailor communications for specific groups of individuals, and
_______________
5The Flesch Reading Ease Score and the Flesch-Kincaid Grade Level Score.
6Centers for Medicare and Medicaid Services’ Toolkit for Making Written Material Clear and Effective (described later) includes a useful section on the limitations of using some of the common readability assessment tools in evaluating health education materials (CMS, 2011b).
• assess how well the health care organization is responding to the health literacy characteristics of its patients. (Tools to accomplish this have been developed for hospitals, health centers, and pharmacies.) (ODPHP, 2010)
In addition to having access to clearly written materials, individuals—especially those with low literacy skills—are also likely to benefit from the use of pictures in health communications (Houts et al., 2006). For example, research shows that picture-based communications improve understanding of how to take medications and decrease medication errors (ODPHP, 2010). Key factors to keep in mind when using pictures are to minimize distracting details, use simple language to link to and support the message of the picture, include people from the intended audience and health professionals in designing the pictures (rather than relying solely on artists), and evaluate the effectiveness of the materials, comparing those with pictures to those without (Houts et al., 2006).
The number of people in the United States who have poor health literacy is high; it is estimated that only 12 percent of adults have proficient health literacy skills (IOM, 2004; Kutner et al., 2006). Physicians may recognize the need to identify patients who cannot read and therefore may be unable to follow a complex regimen of seizure medications or other instructions. However, the extent of a patient’s health literacy is difficult to assess, and physicians have to be aware of and recognize the effects that low health literacy can have on patients’ ability to understand health information related to their diagnosis and treatment (e.g., specific syndrome, seizure type and triggers). Physicians also need to recognize the resulting impact that low health literacy may have on health outcomes.
Sources of Information for People with Epilepsy and Their Families
Most parents navigate [the care] process with very little information. There are costs for that, too, especially for the failure to provide resources and information to patients, families, and care providers.
-Joan Skluzacek
In addition to receiving education from health care providers, people with epilepsy and their families access a variety of other sources for information. Individuals and family members who are knowledgeable about epilepsy serve as important resources for others. Information sources identified in a Canadian study of families of children with epilepsy included health care providers, the Internet, television, radio, newspapers, books, family and friends, families whose members have epilepsy, and epilepsy organizations (Lu et al., 2005). In this study, the average family accessed 3.5 sources recommended to them by their health care provider as well as 4 additional
sources. In another study, Prinjha and colleagues (2005) found that patients received information from health care providers, epilepsy organizations, first aid training, leaflets, books, magazines, newspapers, videos, and the Internet. A UK survey of men with epilepsy that asked about preferences for receiving information found that the Internet was the third most preferred choice, after general practitioners and consultant neurologists (Sare et al., 2007). In this study, 84 percent were more likely to find information on their own, rather than ask health professionals. Sample and colleagues (2006) noted that word-of-mouth was frequently cited in addition to physicians, nurses, and the Internet as sources of information about medications and services.
Role of the Internet in Educating People with Epilepsy and Their Families
As Internet use becomes more widespread, it is an increasingly promising vehicle for delivering health education to people with epilepsy and their families, as well as general information about epilepsy to the public (Chapter 8). The Internet enables provision of information to many people with limited access to other information sources. Helpful information about epilepsy can be found on websites for health care systems and hospitals, on general health information sites such as WebMD, on government websites such as those maintained by the CDC and the National Institutes of Health, and on a host of epilepsy-specific websites run by epilepsy organizations and people with epilepsy and their families (see Box 7-6).7 A recent survey of individuals participating in an online epilepsy community indicated that participants believed that their online interactions with others provided a number of benefits, including gaining knowledge about epilepsy (e.g., increased understanding of seizures) (Wicks et al., 2012).
Gaps in Internet use are closing, but disparities still exist among people with lower incomes and racial/ethnic minorities. Surveys of Internet use indicate that, nationwide, 96 percent of adults with annual incomes of $75,000 or more use the Internet, compared with 63 percent of those with incomes less than $30,000 a year; additionally, 78 percent of English-speaking Hispanic adults and 79 percent of white, non-Hispanic adults use the Internet, compared with 67 percent of black non-Hispanic adults (Census Bureau, 2012). Population groups disproportionately affected by epilepsy (e.g., older adults, those who are less well educated) are less frequent Internet users: U.S. adults with the lowest Internet use are those 65 and older and those with less than a high school
_______________
7Box 7-6 contains a list of examples of existing epilepsy-related websites as of March 2012. Due to the dynamic nature of the Internet, websites and website content will change over time.
BOX 7-6 EXAMPLES OF WEB RESOURCES AVAILABLE FOR INFORMATION ABOUT THE EPILEPSIES
• American Epilepsy Society: www.aesnet.org
• Centers for Disease Control and Prevention: www.cdc.gov/epilepsy
• Citizens United for Research in Epilepsy: www.cureepilepsy.org
• Dravet.Org (formerly International Dravet Syndrome Epilepsy Action League): www.dravet.org
• Epilepsy Foundation: www.epilepsyfoundation.org
• Epilepsy Therapy Project: www.epilepsy.com
• Finding A Cure for Epilepsy and Seizures: www.nyufaces.org
• Health Resources and Services Administration’s Maternal and Child Health Bureau: www.mchb.hrsa.gov/programs/epilepsy
• The Hemispherectomy Foundation: www.hemifoundation.intuitwebsites.com
• Hope for Hypothalamic Hamartomas: www.hopeforhh.org International Bureau for Epilepsy: www.ibe-epilepsy.org International League Against Epilepsy: www.ilae-epilepsy.org
• Lennox-Gastaut Syndrome Foundation: www.lgsfoundation.org
• National Association of Epilepsy Centers: www.naec-epilepsy.org
• National Institute of Neurological Disorders and Stroke: www.ninds.nih.gov/disorders/epilepsy/epilepsyhtm
• National Library of Medicine Medline Plus: www.nlm.nih.gov/medlineplus/epilepsy.html
• Preventing Teen Tragedy: www.preventingteentragedy.net
• Rasmussen’s Encephalitis Children’s Project: www.rechildrens.org
• TalkAboutlt.org: www.talkaboutit.org
• Tuberous Sclerosis Alliance: www.tsalliance.org
• WebMD: www.webmd.com/epilepsy
education. Only 42 percent of adults in these two groups use the Internet (Census Bureau, 2012). Two recent epilepsy-specific studies suggest that Internet access among people with epilepsy varies and is on the lower end of general population ranges. For example, only 51 percent of veterans with epilepsy had Internet access (Pramuka et al., 2010), as did 62 percent of adults recruited from an epilepsy clinic (Escoffery et al., 2008).
Among the many websites devoted to epilepsy information in the United States, Escoffery and colleagues (2008) identified two sites as being the most comprehensive: that of the Epilepsy Foundation (www.epilepsyfoundation.org) and Epilepsy.com (www.epilepsy.com), the public website of the Epilepsy Therapy Project (ETP). Both sites have up-to-date information on epilepsy (e.g., seizures, treatments, medication side effects, pregnancy, school and education, safety precautions, resources), information on living with epilepsy for individuals and families across the life span, strategies for communicating with health professionals, answers to frequently asked questions, and opportunities for e-community programs. The Epilepsy Foundation has developed parts of its website to reach culturally
diverse population subgroups, including African Americans and Hispanics, and many of its pages are available in Spanish. Other websites, such as the International League Against Epilepsy (ILAE) site (www.ilae-epilepsy.org/), provide patient and family educational material in languages such as Spanish, Russian, Farsi, and Chinese. The Epilepsy Foundation’s website also includes links to its affiliate organizations as sources for state and local information and support for people with epilepsy and their families. In developing its content, Epilepsy.com provides information at varying levels of detail and complexity.
The Internet has an especially important role for families coping with the more severe epilepsy syndromes. For example, Dravet.org (formerly the International Dravet Syndrome Epilepsy Action [IDEA] League) provides advocacy and support for families with a child who has Dravet syndrome (Black and Baker, 2011). Because this syndrome is so rare, families often feel isolated and have problems obtaining specific information about it. The Dravet.org website includes a social networking function for families, which includes forums in four languages. In addition, the website provides comprehensive clinical information and links to resources (Black and Baker, 2011). As noted in Box 7-6, there are also websites specific to hypothalamic hamartoma, Lennox-Gastaut syndrome (LGS), and tuberous sclerosis complex that provide content on the complicated health needs and consequences of these disorders and support for families. More broadly, Wicks and colleagues (2012) demonstrated that online communities, such as PatientsLikeMe.com, can help connect people with epilepsy; 30 percent of participants did not know anyone else with epilepsy previously, but 63 percent of those participants identified at least one other person through the online community with whom they could openly discuss and share information. Although there are many websites devoted to epilepsy information in the United States, a central, reliable resource that provides a place to which professionals can easily refer patients and their families does not exist. A centralized resource could provide a venue for people with epilepsy and their families to learn about and navigate the wealth of available websites, which may be useful for them to learn more about epilepsy generally and about specific syndromes and seizure types.
To determine the types of information that people are looking for when it comes to the epilepsies, one study (Escoffery et al., 2008) concluded that information was sought in the following areas: general information (43 percent), medication (30 percent), epilepsy type (23 percent), different treatment options (20 percent), updated information (15 percent), social support (12 percent), and other (16 percent). Topics included in the “other” category related to lifestyle, daily living, sleep, diet, stress, pregnancy, and menopause. During the course of its work, the committee reached out to its sponsors and other epilepsy organizations, many of which maintain
websites (examples listed in Box 7-6) with the goal of informing people with epilepsy, their families, and the public about the epilepsies, to gain a better understanding of how their websites are being used. The following organizations generously shared web statistics for the committee’s consideration: the American Epilepsy Society, CDC, Citizens United for Research in Epilepsy, ETP, Finding A Cure for Epilepsy and Seizures, ILAE, LGS Foundation, National Institute of Neurological Disorders and Stroke, and Tuberous Sclerosis Alliance. Because of variations in methodologies used to capture statistics and the variation in site content and audiences of the websites, direct comparisons could not be made regarding the number of users and visits or pages viewed. However, in reviewing the available information the committee was able to determine the following:
• There is wide variation among the types of data that can be collected from websites, such as time spent on a page, bounce rate, number of pages per visit, and referral websites.
• Average visits per month to the various websites ranged from approximately 1,000 to more than 360,000, with the most-visited site being geared toward general information for a broad audience.
• Search engines are the largest source of traffic for many of the sites, in a number of cases representing approximately two-thirds of referrals.
• Websites that are able to track how many visitors they receive through social media and visitors using mobile devices noted an increase in traffic from these sources over time.
• Keyword searches and the most-viewed pages vary from one site to another depending on the site content and its audience, for example:
• General terms and page topics, such as epilepsy, seizure types, and treatment (e.g., medication, surgery, ketogenic diet) and frequently asked questions, were common across many of the websites.
• Topics related to quality of life, family and caregiving, and schools were popular for users of websites that target families of people with specific epilepsy syndromes.
• When available, patient-oriented tools and resources, such as seizure first aid, seizure diaries, seizure action plans, and medication information, were popular with users.
Although individuals and families may be trying to find and use health information online, the sites are not often geared to people with low health literacy. Content assessments of the basic consumer education por-
tions of the Epilepsy Foundation website and the Epilepsy.com website in 2007 and 2009, respectively, found that only between 3 and 6 percent of pages were written at a sixth-grade level or lower (31 to 46 percent of the Spanish-language pages on the Epilepsy Foundation website were at that level) (Elliott and Shneker, 2009; Elliott et al., 2007). On the Epilepsy.com website, only 15 percent of pages were at the eighth-grade level or below. In the long run, with additional focus on health literacy, comprehensive content testing with users, and optimization of content based on user feedback, online epilepsy educational resources could be important tools for all individuals and their families, including those with low health literacy. Online resources allow users to proceed at their own pace, and the technology enables written, visual, audio, and video learning experiences (Lewis, 2005). Someday, it may be possible to tailor web-based health information to the learning style and, potentially, language and literacy level of a specific user. Design guidelines specific to websites are evolving as use of the Internet for health care communications expands to ensure readability for populations with limited literacy (Eichner and Dullabh, 2007). Nevertheless, guidelines that do exist emphasize many of the same themes relevant to health communication in general:
• Keep it simple in design, content, and navigation.
• Highlight important information.
• Develop content that is culturally relevant.
• Take advantage of the Internet’s capacity to provide choices and additional information in various forms (e.g., audio transcription).
• Include a simplified search function (e.g., one that can recognize misspelled words).
• Use the most widely accessible formats (e.g., HTML) and be sure the website can be used on both old and new hardware.
• Engage in iterative testing. (Eichner and Dullabh, 2007; IOM, 2009)
There are downsides to health information obtained online, including varying quality of the information, complexity that may lead to misunderstanding, and its sheer volume (Lewis, 2005). To assess quality of Internet content for education about epilepsy in Canada, Burneo (2006) evaluated websites to determine compliance with the Health On the Net (HON) Foundation Code of Conduct.8 None of the sites evaluated followed all
_______________
8The HON Foundation, based in Switzerland, has developed the HON Code of Conduct (HONcode). HONcode defines principles for “quality, objective and transparent medical information tailored to the needs of the audience” (Health On the Net Foundation, 2011). Websites can be certified through the Health on the Net Foundation (http://www.hon.ch/HONcode/Conduct.html).
eight principles of the HON Code of Conduct, with average compliance at 3.3. The author of this study highlighted the potential value of the Internet in educating patients and families, which has the potential to help health care providers maximize their time with patients. Another Canadian study of families of children with epilepsy found that Internet sites were the most often used sources of information outside the clinic, and those recommended by a health care provider were judged by families to be the most accurate (Lu et al., 2005). In a review of the literature on how Internet users find, evaluate, and use websites for health information, Morahan-Martin (2004) found that many users are concerned about the quality of the information they retrieve, but their skills in evaluating the material are limited. The author recommended that health professionals specifically recommend sites and be proactive in helping patients and families become better at conducting searches and evaluating and using the information found. However, the committee questions the feasibility of this recommendation given the very short clinical encounters and lack of reimbursement for patient education.
The committee found limited research that would guide health professionals in making recommendations about specific Internet sites to patients and families. The committee has identified this as an opportunity for epilepsy organizations to fill an important gap in patient and family education. These organizations could collaborate on a common website (clearing house) linking to the spectrum of websites that include reliable, high-quality information. The common website could describe the content and types of information found on various websites, along with contact information for the organizations providing it. Information about the common website could be widely disseminated to the full range of professionals who work with people with epilepsy.
Based on its review of Internet sources of patient and family education, the committee concludes the following:
• There is a wealth of reliable and accurate information available online for individuals and their family about the epilepsies.
• Greater attention to health literacy and concepts of clear communications is needed when developing web content.
• Greater attention to the needs of target audiences is necessary to ensure they are able to find the information they want and need.
• Innovative strategies to convey information that is engaging, user friendly, and action oriented and that provides links to other epilepsy resources need to be explored and implemented.
• Epilepsy organizations can take advantage of communications opportunities offered by online communities, social networking, and the increasing use of mobile devices when possible.
Opportunities to Improve Information Delivery
The committee has identified the need for more research to guide the delivery of patient and family education in epilepsy. Individuals and families vary greatly in how they want to receive information, with some wanting it orally, some wanting written instructions, and some being comfortable using the Internet, which suggests that educational content will reach the greatest numbers of people if it is made available in multiple formats. Oral (face-to-face) education could be delivered to small groups, requiring less time from health care providers (Couldridge et al., 2001).
Delivery mechanisms need to take into consideration the age, health literacy level, and cultural background of the target audience. The lack of studies on racial/ethnic minorities’ preferences related to the delivery of epilepsy education suggests that research within these populations is especially needed to ensure that efforts are sensitive to potential cultural differences. Research is needed on the level of Internet access among different subpopulations of people with epilepsy (older adults, racial/ethnic minorities), as well as their preferences with regard to sources, format, and delivery of epilepsy education. Studies are needed on relationships between Internet use for education and various clinical or psychosocial outcomes. Epilepsy-specific websites need to be evaluated for their inclusion of information that reflects health literacy and cultural considerations. Knowing which websites are best suited to different population groups would aid health professionals in making recommendations to patients and families. The committee also noted that research on the use of social networking websites for information sharing and obtaining social support for people with epilepsy is needed.
In short, although today there are many more channels for delivering health education about epilepsy, what is not yet known is which channels are the most useful for which purposes. For example, social networking websites may be most effective in providing social support or helping families with practical problems encountered in daily living; epilepsy-specific websites may be most effective in helping individuals with epilepsy and their family understand drug regimens and side effects, because they can be visited repeatedly, or in identifying local resources; and a one-on-one visit with a clinician, in which follow-up questions can be asked, may be the most effective educational approach in initial conversations about diagnosis and in providing the motivation and reassurance to engage in self-management.
MODELS OF EPILEPSY EDUCATION AND SELF-MANAGEMENT
Self-Management: A Critical Goal of Epilepsy Education
Health professionals have been informally educating patients and families about epilepsy for many years using a variety of strategies and supporting materials; however, only in recent decades have formal education models and programs been developed that focus on self-management strategies to improve health outcomes, quality of life, and well-being. “Self-management” is a commonly used term that generally refers to the active involvement of individuals with chronic conditions in their health care (Clark et al., 2010; Lorig and Holman, 2003). Although by definition (“self-”) these terms refer to the individual with epilepsy, management is often carried out by family members (“family management”), such as the parent of a child with epilepsy or an adult caring for a parent or other older relative (Grey et al., 2006). Sometimes, a caregiver is not related to the individual at all. Many people with epilepsy may find full participation in self-management beyond their capabilities for any number of reasons— such as age, developmental status, extent of impairment and comorbidities, overwhelming personal situations, or low health literacy—which makes it difficult to understand, take necessary steps, or follow clinical recommendations. As a result, the committee adopted the concept of “optimal self-management,” recognizing that participating in health care represents a wide range of possibilities and that what is optimal for one person may be beyond the capacity of another.
The broad definition of self-management for chronic health conditions used by Lorig and Holman (2003) includes reference to both tasks and skills that can be introduced through education. The tasks focus on three areas: managing the medical aspects of the condition, adapting or creating new behavior and new roles that incorporate the condition into one’s life, and dealing with the emotional effects of having a chronic condition; and the five skills involve learning to solve problems, make decisions, use resources, develop partnerships with health care providers, and take action. It is important to note that learning self-management skills begins with education and that a critical goal for patient and family education is to help people acquire and master self-management skills. This section focuses on the educational factors and efforts that are necessary to facilitate and promote optimal self-management for people with epilepsy and their families. Over the last two decades, a number of self-management programs have been designed that include educational programs, behavioral and counseling programs, and mind-body techniques (DiIorio, 2011). A number of the efforts focused on education are described below. Chapter 4 includes discussion of PEARLS (Program to Encourage Active, Rewarding Lives for Seniors) and Project UPLIFT (Using Practice and Learning to Increase
Favorable Thoughts), self-management programs that incorporate behavioral, counseling, and mindfulness techniques and are designed to reduce depression among people with epilepsy.
Self-management for epilepsy includes the information and resources that people with epilepsy and their families need to develop skills and behaviors that enable them to actively participate in patient-centered care; it is “the sum total of steps a person takes to control seizures and to control the effects of having a seizure disorder” (DiIorio, 1997, p. 214). The identification of the core elements of self-management for individuals with epilepsy is an evolving process that has been informed by the Living Well Conferences and the work of the Managing Epilepsy Well (MEW) Network,9 an organization whose mission is to advance self-management in the epilepsy field (AES et al., 2004; Austin et al., 2006a; CDC et al., 1997; DiIorio et al., 2010). Core elements of self-management models often focus on the connections between knowledge, attitudes, skills, and behaviors and individuals’ ability to manage seizures, medications, safety considerations, communication, and healthy lifestyle choices (Buelow, 2001; DiIorio, 1997, 2011; Shope, 1980). Some models have been expanded to include skills and knowledge in the following areas: information management, general health status, self-advocacy, development of productive patient-provider partnerships, individuals’ ability to manage their lives within the context of having a chronic health condition, and competence and autonomy derived from self-determination theory10 (Buelow and Johnson, 2000; Clark et al., 2010; DiIorio et al., 2004; Shafer, 1998, 2009; Shafer and DiIorio, 2004, 2006). Many of these elements support the need for a patient-centered approach to education, provide individuals and their families with knowledge and skills that promote competency in optimal self-management, and apply to managing both epilepsy and its comorbidities.
Knowledge and skills necessary for optimal self-management can be divided into two broad categories—epilepsy-specific management and chronic care management. Epilepsy-specific self-management domains relate to managing seizures, medications and treatments, safety concerns, seizure triggers, and comorbidities. The epilepsy-specific knowledge needs of individuals and their family vary, depending the characteristics of seizures and the severity of comorbidities. Other information is useful for all people with epilepsy and their families. For example, they must understand the
_______________
9The MEW Network is a collaborative research network created through funding from the CDC’s Prevention Research Centers and Epilepsy Program. http://www.sph.emory.edu/ManagingEpilepsyWell/ http://www.sph.emory.edu/ManagingEpilepsyWell/about/at_a_glance.php.
10The self-determination theory is based on the premise that internal and external motivators exist and have varying roles in and influence on individual and social development (Deci and Ryan, 1985).
importance of medication adherence, because nonadherence is a common trigger for the development of status epilepticus (Neligan and Shorvon, 2010) and is associated with higher rates of emergency room visits, hospital admissions, auto accidents, fractures, and mortality in adults (Faught et al., 2008). Similarly, teaching all individuals and their caregivers to keep a record of seizures in a seizure diary or an online tool,11 such as “My Log” used in WebEase (Web Epilepsy Access, Support, and Education) (DiIorio et al., 2009a), can help identify seizure triggers.
Chronic care self-management education domains relate to knowledge and skills that are necessary for maintaining a healthy lifestyle, having an active partnership with the health care team, and living independently— broad domains that are important to all individuals living with a chronic condition regardless of the specific condition. Table 7-1 provides an overview of the knowledge and skills for epilepsy-specific management and chronic care self-management.
Development and Evaluation of Epilepsy Education Programs
The committee explored the literature on the development and evaluation of epilepsy education programs aimed at improving at least one aspect of knowledge, self-management, coping, or quality of life in either patients or their families and found that the research base lags behind that for other chronic conditions, such as arthritis (Nunez et al., 2009). There are signs of progress, however, with a number of innovative education programs that are now under development and being evaluated. This section describes what is known about the efficacy of several epilepsy-specific educational and self-management programs for children, families, and adults. These descriptions are followed by discussion of a program specific to seizure-like events with a psychological basis and a review of educational programs for people with low health literacy.
Programs for Children and Their Families
In its review of the literature, the committee determined that educational programs for children and their families were generally intended to increase knowledge about epilepsy; improve skills in self-management, communication about epilepsy to others, and developmental tasks (e.g., increasing independence); and optimize quality of life and psychological well-being (e.g., improving attitudes, coping, adjustment, self-esteem, behavior). Programs differed in length (from intensive 2-day programs to
_______________
11A variety of seizure diaries and tracking tools are available online and through epilepsy organizations.
TABLE 7-1
Areas of Self-Management Education for Epilepsy
| Epilepsy-Specific Management | Examples of Knowledge and Skills |
|
• Seizures |
• Knowledge—Specific seizure type, first aid response, recognition and treatment for seizure emergencies (seizure action plans) • Skills—Recognizing, recording, and tracking episodic events; identifying seizure triggers; keeping a seizure diary |
|
• Medications, Treatments |
• Knowledge—Medication name, dosage, possible medication interactions and side effects, consequences of missed or late doses, drug-alcohol interactions • Skills—Tracking medication intake, tracking medication dose and changes, managing refills, responding to allergic reactions or adverse effects |
|
• Safety |
• Knowledge—Risks for injury related to seizures and treatment, strategies for reducing injury, risks for mortality, including sudden unexpected death in epilepsy • Skills—Assessing risks in environment, modifying environment and lifestyle to reduce risks yet maintain quality of life |
|
• Comorbid conditions |
• Knowledge—Common comorbidities, symptoms, treatments, and management • Skills—Recognizing symptoms, knowing when to seek support and treatment, monitoring treatment |
| Chronic Care Management | Examples of Knowledge and Skills |
|
• Maintaining a healthy lifestyle ○ Physical activity ○ Adequate sleep ○ Pleasurable activities ○ Physical health ○ Emotional health |
• Knowledge—How seizures and everyday life interact, importance of a healthy lifestyle and behaviors, symptoms of an unhealthy lifestyle • Skills—Assessing the impact of seizures on daily life and making modifications; developing strategies for maintaining a healthy lifestyle, for seeking emotional support, and for coping with stressful situations |
|
• Active partnership with health care team |
• Knowledge—Need for active partnership with health care providers, effective communication strategies • Skills—Communicating, problem solving, decision making, self-advocating, goal setting, developing action plans |
|
• Independent living |
• Knowledge—Environmental support, resources, and services needed • Skills—Assessing and evaluating resources, developing action plans, handling emergencies |
weekly sessions over 1-2 months), intervention strategy (e.g., lecture, group sessions, role-playing, use of games, videoconferencing, film, workbooks), and target group (children and family separately or together). Although many education programs focused solely on epilepsy, others were geared toward families of children with epilepsy and cognitive comorbidities; Buelow
(2007), for example, taught parents of children with long-term epilepsy and learning difficulties skills related to problem solving, partnership development, and advocacy.
Epilepsy education programming for children and families has not been as thoroughly evaluated in the United States as in some other countries. Of four educational programs tested using randomized controlled trials (often referred to as the gold standard of research methodology) (Glueckauf et al., 2002; Lewis et al., 1990, 1991; Rau et al., 2006; Tieffenberg et al., 2000), only one was carried out in the United States (Glueckauf et al., 2002). A challenge for many U.S. evaluation studies has been recruitment of sufficient numbers of study participants (Mittan, 2009; Wagner and Smith, 2006).
Nevertheless, programs tested in randomized clinical trials and those with sound methodologies have achieved improvements in a number of outcome variables for both children and parents. In a review of epilepsy education programs for youth, Lewis and colleagues (2010) found these programs produced positive trends toward improvements in health-related knowledge and quality of life. The evaluation of a large, comprehensive educational program for children is highlighted in Box 7-7.
Other promising research may contribute to the field by overcoming recognized limitations in program and study design, such as the lack of a theoretical foundation for a program and limited study participation. For
Box 7-7 AN EDUCATIONAL MODEL TO PROMOTE SELF-MANAGEMENT IN CHILDREN
Tieffenberg and colleagues (2000) developed a program to enhance child autonomy and self-management and tested it in children, ages 6 to 15, with epilepsy. The program involved five weekly meetings of separate parent and child groups. Data were collected before the start of the program and at 6 and 12 months afterward, and clinical and school records were monitored. Children were taught to assume a leading role in managing their condition, and parents were taught to help their children take on this role. Trained teachers used a variety of activities, including games, drawing, storytelling, videos, and role playing to develop the children’s skills in observation (e.g., seizure triggers), communication, and decision making (e.g., working through decision trees). Outcomes measured health locus of control; parent and child knowledge, beliefs, attitudes, and behavior; family dynamics; patient-physician relationships; school attendance; and clinical variables (i.e., seizure frequency, physician visits, hospitalizations). Results showed significant improvement at both 6 and 12 months in the experimental group, compared to controls, on most parent outcomes, including knowledge, fear of child’s death, and disruptions in family life. Children also showed significant improvement in internal locus of control and child-physician relationship. Additional improvements were found for clinical and school variables, including reduction in seizure frequency, absenteeism, and emergency room visits.
example, despite a small sample size, Wagner and colleagues (2010) used empirically supported cognitive-behavioral treatment as the foundation for their COPE (Coping Openly and Personally with Epilepsy) program, which has the objective of improving skills related to self-management, self-efficacy, and coping. Other programs use communications technology to make education programs more available to families unable to travel long distances to participate. For example, Glueckauf and colleagues (2002) used videoconferencing to offer counseling to rural teenagers and their parents, and Austin and colleagues (2002) used telephone conferencing to deliver tailored educational materials for the Be Seizure Smart intervention.
Germany’s FLIP&FLAP program (Jantzen et al., 2009) has many attributes that might be considered in future U.S. programs for educating children and families. The curriculum was carefully developed based on needs identified in qualitative interviews and further evaluated in a pilot study. Researchers created a wide range of teaching materials, including a notebook, a film, rag dolls called FLIP&FLAP, a game about epilepsy, and a comic book, in order to accommodate different learning styles. Teaching methods also varied and included imagination techniques, role playing, and teaching problem-solving skills using an experience-based learning approach. The intervention was an intensive 2-day program delivered to parents and children separately; data were collected immediately before the program and 6 months later. Compared to a control group, children in the intervention group showed greater knowledge about epilepsy and improvement in parent-reported self-management and communication skills. Parents showed improvement in knowledge and fewer epilepsy-related worries.
Programs for Adults
Relatively few evaluations of epilepsy-specific educational programs for self-management were found for adults. Of the studies identified in literature reviews (Bradley and Lindsay, 2009; May and Pfäfflin, 2002; Mittan, 2009), only two were conducted in the United States. However, the committee found significant recent progress in the development and evaluation of self-management educational programs through the MEW Network (DiIorio et al., 2010). WebEase, one of the programs developed through the MEW Network, is described below.
One of the earliest adult programs, the Seizures and Epilepsy Education
(SEE) program,12 delivers health education and psychosocial therapy in a 2-day program. The program uses facts to resolve common fears of individuals with epilepsy and their families, provides information on medication management, and teaches strategies for living successfully with epilepsy. A small randomized clinical trial by Helgeson and colleagues (1990) tested the SEE program and demonstrated a significant decrease in participants’ fears and misinformation or misunderstandings, as well as a significant improvement in self-management and medication adherence, compared to the control group.
Another comprehensive self-management program, the Modular Service Package Epilepsy (MOSES) program (Ried et al., 2001) has nine educational modules: living with epilepsy, epidemiology, basic knowledge, diagnostics, therapy, self-control, prognosis, psychosocial aspects, and resources. The modules are designed to improve knowledge about epilepsy, its treatment, and its psychosocial effects; self-management; and independence (Ried et al., 2001). May and Pfäfflin (2002) examined the efficacy of the MOSES program when formatted as a 2-day course for adults with epilepsy. Participants reported significantly greater knowledge, improved coping with epilepsy, and improved seizure outcomes at the 6-month follow-up.
The committee found assessments of two self-management programs for adults with epilepsy who also had intellectual disabilities. Clark and colleagues (2001) evaluated a video-assisted program that involved three 1-hour group sessions, a 10-minute video that was viewed twice, participation in a discussion of epilepsy medication and safety, and learning about using seizure diaries. Pre- and post-assessments documented a 43-percent increase in knowledge about epilepsy, with increases particularly in understanding the purpose of an electroencephalograph (EEG) and the need to keep a seizure diary. A second program, the PEPE Program, was developed in Germany and replicated in the United Kingdom (Kushinga, 2007). This multimedia program, which used film clips, quizzes, and photographs, was led by two trained interviewers and was presented over eight 2-hour sessions. A pilot study showed high participant satisfaction with the program characters and the social interaction during the program, and an increase in participants’ knowledge about seizures and medication.
Educational programs developed for improving self-management via the Internet also are being tested. One of the first of these was WebEase, designed by DiIorio and colleagues (2009b), and it is one of the programs included in the CDC-sponsored MEW Network. The theoretical founda-
_______________
12Developed by R. J. Mittan and formerly known as the Sepulveda Epilepsy Education program. The SEE program has recently been revised for children with epilepsy and their families; a pilot study showed promising results (Shore et al., 2008).
tions for WebEase include social cognitive theory (Bandura, 1976), the transtheoretical model of behavioral change (Prochaska and DiClemente, 1982), and motivational interviewing (Miller and Rollnick, 2002). WebEase program modules encourage participants to learn about targeted concerns, explore readiness for change, and set goals. Participants have access to online tools that are used to track thoughts, concerns, actions, and progress. Modules focus on medication-taking practices, sleep, and stress management. The program was evaluated in a randomized controlled trial in adults with epilepsy and demonstrated improvements in medication adherence, perceived stress, knowledge, and self-management compared to a control group (DiIorio et al., 2011). This study also collected information from participants about their experience in using the online program that could be helpful in further program development (DiIorio et al., 2009a). Despite the advantages offered through online programs, some individuals prefer programs that consist of individual meetings or in-person group meetings that are led by a health professional or a peer (Fraser et al., 2011), and it is important that personal preferences and individual needs are taken into consideration in program design and dissemination.
Educational Programs for Seizure-Like Events
Although literature reviews show few assessments of educational interventions for seizure-like events that are determined to not be epilepsy (Martlew et al., 2007), there is some empirical support for the notion that educational interventions might be helpful in this population (Gaynor et al., 2009). One educational program that shows promise was developed by Hall-Patch and colleagues (2010) in the United Kingdom, based on the self-regulation model (Leventhal et al., 1992). In a study of the program’s effects, patients newly diagnosed with seizure-like events with a psychological basis were given an informational leaflet with 14 points covering patients’ representations of their health condition. There was also a guide for physicians with explanations for each of the points and advice for providing information to patients. Follow-up interviews indicated that 94 percent of patients found the leaflet easy to understand, and only 11 percent had questions that it did not answer. Although 86 percent of patients reported negative emotions during the consultation, 94 percent had their questions answered, and 90 percent felt their feelings had been heard. Moreover, only 14 percent were confused about the diagnosis, and only 4 percent were angered by it, a much lower rate than described in an earlier study (18 percent) among people who did not receive an educational intervention (Carton et al., 2003). Approximately 3 months later, 63 percent of the study participants had a greater than 50-percent reduction in seizure-like events, and 14 percent were event-free (Hall-Patch et al., 2010). In addition
to educational interventions, cognitive-behavioral therapy shows promise as an effective approach for reducing the frequency of seizure-like events and improving psychosocial outcomes for individuals who have seizure-like events with a psychological basis (Goldstein et al., 2010; LaFrance et al., 2009).
Health Literacy Considerations for Educational Programs
Clear communication about health-related topics not only helps those who have low health literacy, but can benefit everyone. As a result, the concept of “universal precautions” has been borrowed from the infectious disease field to convey the importance of making “clear communication … the basis for every health information exchange” (ODPHP, 2010, p. 11). This concept is an important consideration for the development and evaluation of epilepsy education programs.
Berkman and colleagues (2011) conducted a recent review of studies of programs for low-literacy populations, including those with diverse chronic diseases and conditions, not specifically epilepsy, but their findings regarding the impact of these programs are suggestive for this population. Findings from 42 studies of general interventions (i.e., non-epilepsy specific) to mitigate the effects of low health literacy were assessed in the review (Berkman et al., 2011). Although the overall strength of evidence supporting specific design features was low (in part because of the diversity of interventions), the following features seemed to improve the comprehension of low-literacy populations:
• presenting essential information by itself,
• presenting essential information first,
• presenting quality information so that higher numbers mean higher quality (e.g., a basketball score, not a golf score),
• using the same denominators to present baseline risk and treatment benefits,
• adding icons to numerical presentations of treatment benefit, and
• adding video to verbal narratives.
Berkman and colleagues concluded that intensive self-management and adherence interventions appeared to increase self-management and reduce disease severity, as well as reduce emergency department visits and hospitalizations.
Next Steps for Epilepsy Education Programs
Despite the paucity of epilepsy education program evaluations, the committee was encouraged that all of the programs that were tested documented significant improvements in at least one outcome. However, none of the programs appeared to have been tested in more than one study. Replication and assessment of existing programs, especially those tested in only a small number of individuals, are needed. Moreover, new programs should be developed and tested in populations that have been understudied, including older adults, parents and caregivers of infants and young children, and individuals with uncontrolled seizures, serious comorbidities, and cognitive limitations. Finally, educational programs that include all of the recommended content for epilepsy-specific knowledge and skills that are necessary for optimal self-management (described in Table 7-1) also are still needed.
The committee noted the need for greater attention to cultural diversity in the programs. Educational programs developed for diverse population groups in other clinical areas have achieved positive results and might provide a model for epilepsy. For example, one diabetes education program designed to respond to cultural barriers to diabetes self-management successfully managed cultural barriers, increased participants’ self-efficacy,13 and promoted engagement in healthier lifestyles (McCloskey and Flenniken, 2010).
The committee found that many programs currently being developed have the potential to make major contributions to the field of epilepsy self-management. Many are being guided by evidence-based principles of program design. For example, the WebEase self-management program, which is based on proven techniques of motivational interviewing and stages-of-change research (DiIorio et al., 2009b), has the potential to provide an effective comprehensive epilepsy self-management program via the Internet. Additional core modules could be developed for epilepsy-specific areas, such as comorbidities, safety, and risks including mortality, again using evidence-based methods.
Finally, the positive outcomes from the available educational programs, coupled with the promise of innovative programs being developed, led the committee to conclude that this is a propitious time for the CDC to continue its investment in educational and self-management programs for individuals with epilepsy. Existing MEW Network programs should be implemented using strategies that will ensure their sustainability and expanded use. The MEW Network could also work to develop additional
_______________
13In the context of epilepsy, self-efficacy theory stresses the importance of an individual’s belief that he or she can successfully manage the challenges of the condition, and it is an important underpinning for self-management programs that affects many aspects of how people think, feel, and act.
educational programs for people with epilepsy across the life span and across the epilepsy spectrum.
LESSONS FROM MODELS FOR OTHER HEALTH CONDITIONS
In selecting models from other health conditions that might suggest strategies to inform the development of educational programs for people with epilepsy and their families, the committee considered (1) the nature of the epilepsies, with their wide spectrum of characteristics and associated comorbidities; (2) the broad range of individual and family needs for information; and (3) the areas of knowledge and skill development identified in epilepsy self-management models. Therefore, the committee explored both condition-specific models and models for the management of chronic health conditions in general and selected one of each for further exploration below.
Diabetes Self-Management Education
Diabetes educators are a model for the provision of condition-specific health education by a health professional and are certified by the National Certification Board for Diabetes Educators. Diabetes educators come from a variety of health care disciplines (e.g., medicine, nursing, psychology, nutrition, social work) and provide patient education, commonly referred to as diabetes self-management education (DSME) (NCBDE, 2012).
Diabetes education programs are based on evidence-based standards and take into account the individual needs, goals, circumstances, and experiences of the patient. DSME is designed to increase knowledge, improve problem-solving skills, and develop skills for self-management. Patients learn informed decision making and how to establish effective partnerships with their health care team, which in turn can lead to improved clinical outcomes (e.g., lower blood glucose levels), health status, and quality of life (NCBDE, 2012). An Australian national consensus study on outcomes and indicators for diabetes education identified primary goals and optimal outcomes in three areas: living with diabetes, physical health, and cost-effectiveness (Colagiuri and Eigenmann, 2009). Because of the difficulty in linking diabetes education with clinical and cost outcomes, the desired outcomes identified by this group were knowledge, self-management, self-determination, and psychological adjustment. Outcomes such as these are clearly relevant to epilepsy education.
An international literature review of studies evaluating outcomes of DSME was carried out to explore theoretical foundations, outcomes, and the use of community partnerships (Jack, 2003). Of the eight studies selected for review, only two used a theory to underpin the education. Half
of the programs measured both short-term and intermediate outcomes. Results demonstrated that both short-term (e.g., fasting glucose, glycosylated hemoglobin, body mass index) and intermediate (e.g., exercise, diet, diabetes knowledge) outcomes can be improved with DSME. Many programs developed collaborative relationships among diabetes care providers, researchers, and community programs, including faith-based organizations, support groups, and health clubs and recreational facilities. These community partnerships were important to the success of all of the programs studied, by improving recruitment and continued participation (Jack, 2003).
Lessons from this review of DSME programs that are applicable for epilepsy education include (1) identification of the components (knowledge, self-management, self-determination, and psychological adjustment) that are relevant to optimal living with a chronic condition; (2) the importance of effective community partnerships in the delivery of educational programs; and (3) recognition of the importance of outcomes of educational programs over time. Additionally, the development of a cadre of well-trained, certified diabetes educators could serve as a model for an educator program specific to the epilepsies.
Chronic Disease Self-Management Program
The Chronic Disease Self-Management Program (CDSMP) is intended for adults with a range of chronic conditions. A major assumption underlying this generic approach to self-management is that many concerns, tasks, and skills are common to managing all chronic conditions (Lorig et al., 1999). In developing the CDSMP, two needs assessments were carried out. The first was a review of the literature on programs for chronic health conditions to identify components taught across conditions. The authors identified 12 of these components, including symptom monitoring and response, strategies for handling emergencies, maintaining a healthy lifestyle, and managing emotional responses to the health condition. The second needs assessment involved 11 focus groups of adults older than age 40. It asked participants to describe, for example, the impact (e.g., physical, social, psychological) of their condition on their lives, strategies they used to cope with their chronic health condition, and their thoughts about the future. Information from these two needs assessments shaped both the content and the delivery of the CDSMP program (Lorig et al., 1999).
The theoretical foundation for delivery of the program is self-efficacy theory, which suggests that people do better in managing a situation when they believe they can do so successfully (Bandura, 1997). There is empirical support for using self-efficacy concepts in self-management programs (Marks et al., 2005), and strategies consistent with this theory are used in CDSMP, such as modeling behaviors, action planning and feedback, and
participation in problem solving. The content is delivered in small groups of 10 to 15 adults with diverse chronic conditions and their family members. The group is facilitated by a volunteer lay leader, often someone who also has a chronic condition. The leader is trained and uses a teaching manual. The course is generally offered in weekly 2.5-hour sessions for 7 weeks (Lorig et al., 1999).
A test of CDSMP’s effectiveness, compared to a condition-specific self-management program (the Arthritis Self-Management Program [ASMP]), was conducted in adults with arthritis (Lorig et al., 2005). ASMP was also developed based on needs assessments of patients and their rheumatologists. The two programs were compared in a randomized controlled trial and followed for a year. Both programs showed improvements. However, short-term results indicated that individuals in the arthritis-specific self-management program had significantly greater improvement in distress, limitation of activity, and fatigue, compared to individuals in the generic program. Furthermore, there was a trend toward greater improvement in other outcomes, such as global health and pain. By the 1-year follow-up the gap in improvements between the groups had narrowed, and participants in both programs had significant improvements; however, overall improvement and self-reported ratings of global health and fatigue were still better for people who received the arthritis-specific program (Lorig et al., 2005).
These findings have relevance for epilepsy. Individuals with epilepsy might benefit from attending CDSMP programs, because some of the content (e.g., developing strategies for handling emergencies, living a healthy lifestyle) is directly relevant to epilepsy. Attending these programs might also reduce feelings of social isolation. The finding that people in the condition-specific program demonstrated both earlier and greater improvement than people in the generic program suggests epilepsy-specific self-management programs cannot be replaced with generic chronic health conditions education programs.
A VISION FOR OPTIMAL EPILEPSY EDUCATION
People who are informed, supported, and actively engaged in productive interactions with “prepared, proactive, practice teams” (Wagner et al., 2005, p. S-9) should be at the center of a health care system that is designed to provide access to high-quality epilepsy care (Chapter 4). To be consistent with this broad framework for the delivery of health care, appropriate educational programs and resources ought to be readily available to ensure that people with epilepsy (and their families and caregivers, as needed) are knowledgeable about their condition and have the requisite skills to engage in productive interactions with their health care
team. The committee conceptualized a combination of epilepsy-specific self-management—which would include epilepsy-specific knowledge and skills related to seizures, medication and treatments, safety, and comorbid conditions—with chronic care management, which would include knowledge and skills related to maintaining a healthy lifestyle and behaviors, actively partnering with a health care team, and living independently (see Table 7-1).
Educational Needs Across the Spectrum
The committee recognizes that because of the diverse nature of the epilepsies, some people with epilepsy will need more educational assistance than others. Figure 7-2 depicts how different severity levels of seizures and comorbidities could be linked to different levels of education and resources. Epilepsy-specific education may meet the needs of people with mild forms of epilepsy or those who are mildly compromised—people who may be seizure-free and have no associated comorbidities or those with occasional seizures or mild comorbidities. However, individuals who are seriously compromised—those with uncontrolled seizures and severe comorbidities— will have much greater resource and educational needs. These individuals and their families will need comprehensive education that would include both epilepsy-specific and chronic care self-management program elements.
Some moderately compromised adults also might benefit from both epilepsy-specific education and chronic care programs, such as the CDSMP. A possible benefit of this combined approach, which could be tested through research, is that some somatic comorbidities associated with epilepsy, such as cardiovascular disease, diabetes, and osteoporosis (Chapter 3), could be improved through participation in a generic chronic care program. The finding that online delivery of the CDSMP effectively improved health status (Lorig et al., 2006) suggests that online programs, both epilepsy-specific and generic for chronic conditions, could provide benefits for people with epilepsy who otherwise would not have access to them.
Optimal Educational Outcomes for People with Epilepsy and Their Families
The committee’s vision for optimal patient and family education and outcomes is depicted in Figure 7-3. The education side of the model includes three major domains—knowledge, self-management, and self-determination—and the corresponding indicator areas necessary for optimal patient and family education. The indicator areas define a combination of knowledge, perceptions, tasks, and skills that can be used to measure the efficacy of education programs.
Because there is not a direct cause and effect between the quality of patient education and health outcomes and because health outcomes can be affected by a complex array of factors, the committee concentrated on outcomes more directly related to education. Therefore, the outcomes side of the model focuses on those that can result from optimal education: access to and use of community resources, psychosocial adjustment, and patient-centered outcomes. Corresponding indicator areas define a range of desirable services and patient outcomes. For example, educational programs focusing on self-management and self-determination would prepare people to take advantage of community resources, such as support groups and educational services; similarly, educational programs focusing on increasing knowledge about treatment would help individuals set and monitor epilepsy management goals. Thus, the outcome indicators are important measures of the success of educational efforts.
Designing educational programs to achieve optimal outcomes requires consideration of the characteristics of program participants, such as health literacy, cultural diversity, age and developmental stage, cognitive ability, severity of disease, and gender.
Over the course of its work, the committee identified and reviewed the literature base documenting the general information needs of people with epilepsy and their families. However, the needs of many specific subgroups are understudied, including men, older adults, racial/ethnic minority populations, people with seizure-like events, caregivers of infants and young children, youth transitioning into adulthood, and individuals with the severest forms of epilepsy. In addition to these gaps in research, this chapter highlights several important points about education for people with epilepsy and their families:
• Education for people with epilepsy and their families is critical around the time of diagnosis; through the first year; whenever there is a change in the person’s condition, developmental status, or health status; and if new concerns or comorbidities develop. Few studies identify the most effective formats and delivery mechanisms for patient and family education, and evidence on educational preferences is lacking, especially across diverse populations.
• Relatively few epilepsy-specific self-management programs have been developed and tested, and none have been replicated. All of the programs have demonstrated some positive outcomes, and newer programs show much promise in improving options for the delivery of patient and family education. Studies comparing the
effectiveness of generic chronic care versus epilepsy-specific education programs individually and in combination are needed.
• The use of the Internet presents many potential opportunities to expand the reach and sophistication of epilepsy education programs, enabling them to respond to the needs of individual learners of different literacy levels, language proficiencies, cultural backgrounds, and learning styles. Increased availability of online educational information and the use of social networking websites provide new opportunities for sharing information about the epilepsies and providing interpersonal support.
• Individuals and their families need guidance to ensure that they are connected to the most accurate and reliable information resources and tools available, especially those available online.
• High-quality, validated epilepsy education programs can provide individuals, families, and caregivers with accurate information and education to build the skills needed to achieve optimal self-management. In order to be effective and to maximize reach, programs eventually will need to stratify and balance many dimensions—the severity of the disorders, the existence of comorbidities, the racial/ethnic and cultural background of users, language, the level of general literacy and health literacy, age and gender, and preferred learning styles.
Throughout this chapter, the committee has provided the basis for its research priorities and recommendations regarding improvements needed in education for people with epilepsy and their families, which are detailed in Chapter 9. In order to improve this education and build the necessary knowledge and skills of people with epilepsy and their families, additional research and time needs to be devoted to
• evaluating available educational resources and tools, including those available on the Internet;
• expanding the reach and dissemination of available resources;
• engaging people with epilepsy and their families in developing and testing educational resources;
• evaluating, replicating, and expanding the use of self-management programs; and
• exploring new opportunities for improving education, such as a centralized web resource to connect people with epilepsy to reliable websites and a certification program for epilepsy health educators.
AES (American Epilepsy Society), CDC (Centers for Disease Control and Prevention), Chronic Disease Directors, Epilepsy Foundation, and NAEC (National Association of Epilepsy Centers). 2004. Living Well with Epilepsy II: Report of the 2003 National Conference on Public Health and Epilepsy: Priorities for a public health agenda on epilepsy. http://www.cdc.gov/epilepsy/pdfs/living_well_2003.pdf (accessed February 2, 2012).
Arhan, E., A. Serdaroglu, S. Soysal, A. Ozcelik, K. Gucuyener, and E. Demir. 2009. Assessment of mothers’ knowledge and perceptions of electroencephalography and determination of the short-term effect of an informational leaflet. Epilepsy and Behavior 15(4):491-495.
Austin, J. 2000. Impact of epilepsy in children. Epilepsy and Behavior 1(1):S9-S11.
Austin, J. K., and J. Tooze. 2003. Parenting the daughter with epilepsy. In Women with epilepsy: A handbook of health and treatment issues, edited by M. J. Morrell and K. Flynn. Cambridge, UK: Cambridge University Press. Pp. 249-262.
Austin, J. K., A. M. McNelis, C. P. Shore, D. W. Dunn, and B. Musick. 2002. A feasibility study of a family seizure management program: Be Seizure Smart. Journal of Neuroscience Nursing 34(1):30-37.
Austin, J. K., D. A. Carr, and B. P. Hermann. 2006a. Living Well II: A review of progress since 2003. Epilepsy and Behavior 9(3):386-393.
Austin, J. K., D. W. Dunn, S. M. Perkins, and J. Shen. 2006b. Youth with epilepsy: Development of a model of children’s attitudes toward their condition. Children’s Health Care 35(2):123-140.
Bandura, A. 1976. Social learning theory. Upper Saddle River, NJ: Prentice Hall.
———. 1997. Self-efficacy: The exercise of control. New York: W.H. Freeman and Company.
Bautista, R. E., C. Graham, and S. Mukardamwala. 2011. Health disparities in medication adherence between African-Americans and Caucasians with epilepsy. Epilepsy and Behavior 22(3):495-498.
Berkman, N., S. Sheridan, K. Donahue, D. Halpern, A. Viera, K. Crotty, A. Holland, M. Brasure, K. Lohr, E. Harden, E. Tant, I. Wallace, and M. Viswanathan. 2011. Health literacy interventions and outcomes: An updated systematic review. Evidence report/technology assessment no. 199. Rockville, MD: Agency for Healthcare Research and Quality.
Besag, F M., A. Nomayo, and F Pool. 2005. The reactions of parents who think that a child is dying in a seizure—In their own words. Epilepsy and Behavior 7(3):517-523.
Bishop, M., and C. Allen. 2007. Coping with epilepsy: Research and intervention. In Coping with chronic illness and disability: Theoretical, empirical, and clinical aspects, edited by E. Martz and H. Livneh. New York: Springer Publishing Co. Pp. 241-266.
Black, A. P., and M. Baker. 2011. The impact of parent advocacy groups, the Internet, and social networking on rare diseases: The IDEA League and IDEA League United Kingdom example. Epilepsia 52(Suppl. 2):102-104.
Bradley, P. M., and B. Lindsay. 2009. Care delivery and self-management strategies for adults with epilepsy. Cochrane Database of Systematic Reviews 1:CD006244.
Buelow, J. M. 2001. Epilepsy management issues and techniques. Journal of Neuroscience Nursing 33(5):260-269.
———. 2007. An intervention for parents of children with epilepsy and significant learning problems: Lessons learned from a feasibility study. Journal of the American Psychiatric Nurses Association 13(3):146-152.
Buelow, J. M., and J. Johnson. 2000. Self-management of epilepsy: A review of the concept and its outcomes. Disease Management and Health Outcomes 8(6):327-336.
Buelow, J. M., A. McNelis, C. P. Shore, and J. K. Austin. 2006. Stressors of parents of children with epilepsy and intellectual disability. Journal of Neuroscience Nursing 38(3):147-154, 176.
Burneo, J. G. 2006. An evaluation of the quality of epilepsy education on the Canadian world wide web. Epilepsy and Behavior 8(1):299-302.
Carton, S., P. J. Thompson, and J. S. Duncan. 2003. Non-epileptic seizures: Patients’ understanding and reaction to the diagnosis and impact on outcome. Seizure 12(5):287-294.
CDC (Centers for Disease Control and Prevention). 2011. Health literacy: Guidance and standards. http://www.cdc.gov/healthliteracy/DevelopMaterials/GuidanceStandards.html (accessed August 24, 2011).
CDC, AES (American Epilepsy Society), Epilepsy Foundation, and NAEC (National Association of Epilepsy Centers). 1997. Living Well with epilepsy: Report of the 1997 National Conference on Public Health and Epilepsy. http://www.cdc.gov/epilepsy/pdfs/living_well_1997.pdf (accessed February 2, 2012).
Census Bureau. 2012. Adult computer and adult Internet users by selected characteristics: 2000 to 2011. http://www.census.gov/compendia/statab/2012/tables/12s1158.pdf (accessed February 22, 2012).
Chiou, H. H., and L. P. Hsieh. 2008. Parenting stress in parents of children with epilepsy and asthma. Journal of Child Neurology 23(3):301-306.
Clark, A. J., C. A. Espie, and A. Paul. 2001. Adults with learning disabilities and epilepsy: Knowledge about epilepsy before and after an educational package. Seizure 10(7): 492-499.
Clark, N. M., S. Stoll, E. J. Youatt, M. Sweetman, R. Derry, and A. Gorelick. 2010. Fostering epilepsy self management: The perspectives of professionals. Epilepsy and Behavior 19(3):255-263.
CMS (Centers for Medicare and Medicaid Services). 2011a. Toolkit for making written material clear and effective: Part 2. Using a reader-centered approach to develop and test written material. http://www.cms.gov/WrittenMaterialsToolkit/Downloads/ToolkitPart02.pdf (accessed August 25, 2011).
———. 2011b. Toolkit for making written material clear and effective: Part 7. Using readability formulas: A cautionary note. http://www.cms.gov/WrittenMaterialsToolkit/Downloads/ToolkitPart07.pdf (accessed Feb-ruary 22, 2012).
Cochrane, J. 1995. Patient education: Lessons from epilepsy. Patient Education and Counseling 26(1-3):25-31.
Cohen, A., M. Lancman, H. Mogul, S. Marks, and K. Smith. 1997. Strategies to protect bone mass in the older patient with epilepsy. Geriatrics 52(8):70, 75-78, 81.
Colagiuri, R., and C. A. Eigenmann. 2009. A national consensus on outcomes and indicators for diabetes patient education. Diabetic Medicine 26(4):442-446.
Couldridge, L., S. Kendall, and A. March. 2001. A systematic overview—A decade of research. The information and counselling needs of people with epilepsy. Seizure 10(8):605-614.
Crawford, P., and S. Hudson. 2003. Understanding the information needs of women with epilepsy at different lifestages: Results of the “Ideal World” survey. Seizure 12(7):502-507.
Cushner-Weinstein, S., K. Dassoulas, J. A. Salpekar, S. E. Henderson, P. L. Pearl, W. D. Gaillard, and S. L. Weinstein. 2008. Parenting stress and childhood epilepsy: The impact of depression, learning, and seizure-related factors. Epilepsy and Behavior 13(1):109-114.
Davis, T. C., E. J. Mayeaux, D. Fredrickson, J. A. Bocchini, Jr., R. H. Jackson, and P. W. Murphy. 1994. Reading ability of parents compared with reading level of pediatric patient education materials. Pediatrics 93(3):460-468.
Deci, E. L., and R. M. Ryan. 1985. Intrinsic motivation and self-determination in human behavior. New York: Plenum Press.
Devinsky, O. 2011. Sudden, unexpected death in epilepsy. New England Journal of Medicine 365(19):1801-1811.
DiIorio, C. 1997. Epilepsy self-management. In Handbook of health behavior research II: Provider determinants. New York: Plenum Press. Pp. 213-230.
———. 2011. Education for self-management. PowerPoint presented at the IOM Workshop on Public Health Dimensions of the Epilepsies, June 28. http//iom.edu/~/media/Files/Activity%20Files/Disease/Epilepsy/Panel%205%20DiIorio.pdf (accessed February 22, 2012).
DiIorio, C., P. Osborne Shafer, R. Letz, T. Henry, D. L. Schomer, and K. Yeager. 2003. The association of stigma with self-management and perceptions of health care among adults with epilepsy. Epilepsy and Behavior 4(3):259-267.
———. 2004. Project EASE: A study to test a psychosocial model of epilepsy medication managment. Epilepsy and Behavior 5(6):926-936.
DiIorio, C., C. Escoffery, F. McCarty, K. A. Yeager, T. R. Henry, A. Koganti, E. L. Reisinger, and B. Wexler. 2009a. Evaluation of WebEase: An epilepsy self-management web site. Health Education Research 24(2):185-197.
DiIorio, C., C. Escoffery, K. A. Yeager, F. McCarty, T. R. Henry, A. Koganti, E. Reisinger, E. Robinson, R. Kobau, and P. Price. 2009b. WebEase: Development of a web-based epilepsy self-management intervention. Preventing Chronic Disease 6(1):A28.
DiIorio, C. K., Y. A. Bamps, A. L. Edwards, C. Escoffery, N. J. Thompson, C. E. Begley, R. Shegog, N. M. Clark, L. Selwa, S. C. Stoll, R. T. Fraser, P. Ciechanowski, E. K. Johnson, R. Kobau, and P. H. Price. 2010. The Prevention Research Centers’ Managing Epilepsy Well Network. Epilepsy and Behavior 19(3):218-224.
DiIorio, C., Y. Bamps, E. R. Walker, and C. Escoffery. 2011. Results of a research study evaluating WebEase, an online epilepsy self-management program. Epilepsy and Behavior 22(3):469-474.
Donald, I. P., and C. J. Bulpitt. 1999. The prognosis of falls in elderly people living at home. Age and Ageing 28(2):121-125.
Eichner, J., and P. Dullabh. 2007. Accessible health information technology (IT) for populations with limited literacy: A guide for developers and purchasers of health IT. AHRQ Publication No. 08-0010-EF. Rockville, MD: National Resource Center for Health IT.
Elliott, J. O., and B. F. Shneker. 2008. Patient, caregiver, and health care practitioner knowledge of, beliefs about, and attitudes toward epilepsy. Epilepsy and Behavior 12(4):547-556.
———. 2009. A health literacy assessment of the epilepsy.com website. Seizure 18(6):434-439.
Elliott, J. O., C. Charyton, and L. Long. 2007. A health literacy assessment of the national Epilepsy Foundation web site. Epilepsy and Behavior 11(4):525-532.
Escoffery, C., C. Diiorio, K. A. Yeager, F. McCarty, E. Robinson, E. Reisinger, T. Henry, and A. Koganti. 2008. Use of computers and the Internet for health information by patients with epilepsy. Epilepsy and Behavior 12(1):109-114.
Faught, E., M. S. Duh, J. R. Weiner, A. Guerin, and M. C. Cunnington. 2008. Nonadherence to antiepileptic drugs and increased mortality: Findings from the RANSOM study. Neurology 71(20):1572-1578.
FDA (Food and Drug Administration). 2008. Information for healthcare professionals: Suicidal behavior and ideation and antiepileptic drugs. http://www.fda.gov/Drugs/Drugsafety/PostmarketDrugSafetyInformationforPatientsandProviders/ucm100192.htm (accessed January 5, 2012).
Ferro, M. A., and K. N. Speechley. 2009. Depressive symptoms among mothers of children with epilepsy: A review of prevalence, associated factors, and impact on children. Epilepsia 50(11):2344-2354.
Ficker, D. M., E. L. So, W. K. Shen, J. F. Annegers, P. C. O’Brien, G. D. Cascino, and P. G. Belau. 1998. Population-based study of the incidence of sudden unexplained death in epilepsy. Neurology 51(5):1270-1274.
Fife, T. D., D. Blum, and R. S. Fisher. 2006. Measuring the effects of antiepileptic medications on balance in older people. Epilepsy Research 70(2-3):103-109.
Fisher, R. S. 2000. Epilepsy from the patient’s perspective: Review of results of a community-based survey. Epilepsy and Behavior 1(4):S9-S14.
Foster, D. R., and D. H. Rhoney. 2002. Readability of printed patient information for epileptic patients. Annals of Pharmacotherapy 36(12):1856-1861.
Frank-Briggs, A. I., and E. A. Alikor. 2011. Knowledge and attitudes of parents toward children with epilepsy. Annals of African Medicine 10(3):238-242.
Fraser, R. T., E. K. Johnson, J. W. Miller, N. Temkin, J. Barber, L. Caylor, P. Ciechanowski, and N. Chaytor. 2011. Managing epilepsy well: Self-management needs assessment. Epilepsy and Behavior 20(2):291-298.
Gaitatzis, A., K. Carroll, A. Majeed, and J. W. Sander. 2004. The epidemiology of the comorbidity of epilepsy in the general population. Epilepsia 45(12):1613-1622.
Gayatri, N. A., M. C. Morrall, V. Jain, P. Kashyape, K. Pysden, and C. Ferrie. 2010. Parental and physician beliefs regarding the provision and content of written sudden unexpected death in epilepsy (SUDEP) information. Epilepsia 51(5):777-782.
Gaynor, D., H. Cock, and N. Agrawal. 2009. Psychological treatments for functional non-epileptic attacks: A systematic review. Acta Neuropsychiatrica 21(4):158-168.
Gilliam, F., P. E. Penovich, C. A. Eagan, J. M. Stern, D. M. Labiner, M. Onofrey, G. L. Holmes, E. Mathis, and J. Cramer. 2009. Conversations between community-based neurologists and patients with epilepsy: Results of an observational linguistic study. Epilepsy and Behavior 16(2):315-320.
Glueckauf, R. L., S. P. Fritz, E. P. Ecklund-Johnson, H. J. Liss, P. Dages, and P. Carney. 2002. Videoconferencing-based family counseling for rural teenagers with epilepsy: Phase 1 findings. Rehabilitation Psychology 47(1):49-72.
Goldstein, L. H., T. Chalder, C. Chigwedere, M. R. Khondoker, J. Moriarty, B. K. Toone, and J. D. C. Mellers. 2010. Cognitive-behavioral therapy for psychogenic nonepileptic seizures: A pilot RCT. Neurology 74(24):1986-1994.
Grey, M., K. Knafl, and R. McCorkle. 2006. A framework for the study of self- and family management of chronic conditions. Nursing Outlook 54(5):278-286.
Hall-Patch, L., R. Brown, A. House, S. Howlett, S. Kemp, G. Lawton, R. Mayor, P. Smith, and M. Reuber. 2010. Acceptability and effectiveness of a strategy for the communication of the diagnosis of psychogenic nonepileptic seizures. Epilepsia 51(1):70-78.
Harden, C. L., K. J. Meador, P. B. Pennell, W. A. Hauser, G. S. Gronseth, J. A. French, S. Wiebe, D. Thurman, B. S. Koppel, P. W. Kaplan, J. N. Robinson, J. Hopp, T. Y. Ting, B. Gidal, C. A. Hovinga, A. N. Wilner, B. Vazquez, L. Holmes, A. Krumholz, R. Finnell, D. Hirtz, C. Le Guen, the American Academy of Neurology, and the American Epilepsy Society. 2009. Management issues for women with epilepsy—Focus on pregnancy (an evidence-based review): II. Teratogenesis and perinatal outcomes: Report of the Quality Standards Subcommittee and Therapeutics and Technology Subcommittee of the American Academy of Neurology and the American Epilepsy Society. Epilepsia 50(5):1237-1246.
Health Literacy Innovations. 2012. Improving health communication one word at a time. http://www.healthliteracyinnovations.com/home (accessed February 22, 2012).
Health On the Net Foundation. 2011. The commitment to reliable health and medical information on the Internet. http://www.hon.ch/HONcode/Patients/Visitor/visitor.html (accessed January 26, 2012).
Helgeson, D. C., R. Mittan, S. Y. Tan, and S. Chayasirisobhon. 1990. Sepulveda Epilepsy Education: The efficacy of a psychoeducational treatment program in treating medical and psychosocial aspects of epilepsy. Epilepsia 31(1):75-82.
Hirsch, L. J., E. J. Donner, E. L. So, M. Jacobs, L. Nashef, J. L. Noebels, and J. R. Buchhalter. 2011. Abbreviated report of the NIH/NINDS Workshop on Sudden Unexpected Death in Epilepsy. Neurology 76(22):1932-1938.
Hitiris, N., S. Suratman, K. Kelly, L. J. Stephen, G. J. Sills, and M. J. Brodie. 2007. Sudden unexpected death in epilepsy: A search for risk factors. Epilepsy and Behavior 10(1):138-141.
Houts, P. S., C. C. Doak, L. G. Doak, and M. J. Loscalzo. 2006. The role of pictures in improving health communication: A review of research on attention, comprehension, recall, and adherence. Patient Education and Counseling 61(2):173-190.
IOM (Institute of Medicine). 2001. Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
———. 2004. Health literacy: A prescription to end confusion. Washington, DC: The National Academies Press.
———. 2009. Health literacy, eHealth, and communication: Putting the consumer first: Workshop summary. Washington, DC: The National Academies Press.
Jack, L. 2003. Diabetes self-management education research: An international review of intervention methods, theories, community partnerships and outcomes. Disease Management and Health Outcomes 11(7):415-428.
Jantzen, S., E. Muller-Godeffroy, T. Hallfahrt-Krisl, F. Aksu, B. Pust, B. Kohl, A. Redlich, J. Sperner, and U. Thyen. 2009. FLIP&FLAP: A training programme for children and adolescents with epilepsy, and their parents. Seizure 18(7):478-486.
Johnson, J. 2003. On receiving the diagnosis of multiple sclerosis: Managing the transition. Multiple Sclerosis 9(1):82-88.
Jurasek, L., L. Ray, and D. Quigley. 2010. Development and implementation of an adolescent epilepsy transition clinic. Journal of Neuroscience Nursing 42(4):181-189.
Kendall, S., D. Thompson, and L. Couldridge. 2004. The information needs of carers of adults diagnosed with epilepsy. Seizure 13(7):499-508.
Klein, P., L. M. van Passel-Clark, and J. C. Pezzullo. 2003. Onset of epilepsy at the time of menarche. Neurology 60(3):495-497.
Kobau, R., and P. Price. 2003. Knowledge of epilepsy and familiarity with this disorder in the U.S. population: Results from the 2002 HealthStyles Survey. Epilepsia 44(11):1449-1454.
Kushinga, K. 2007. Practice and research—The PEPE project—Katrina Kushinga describes how a German epilepsy education programme was adapted with the help of service users. Learning Disability Practice 10(5):10-13.
Kutner, M., E. Greenberg, Y. Jin, and C. Paulsen. 2006. The health literacy of America’s adults: Results from the 2003 National Assessment of Adult Literacy. Washington, DC: National Center for Education Statistics.
Kwon, C., M. Liu, H. Quan, V. Thoo, S. Wiebe, and N. Jetté. 2011. Motor vehicle accidents, suicides, and assaults in epilepsy: A population-based study. Neurology 76(9):801-806.
LaFrance, W. C., Jr., I. W. Miller, C. E. Ryan, A. S. Blum, D. A. Solomon, J. E. Kelley, and G. I. Keitner. 2009. Cognitive behavioral therapy for psychogenic nonepileptic seizures. Epilepsy and Behavior 14(4):591-596.
Leppik, I. E. 2006. Epilepsy in the elderly. Epilepsia 47(Suppl. 1):65-70.
Leventhal, H., M. Diefenbach, and E. A. Leventhal. 1992. Illness cognition: Using common sense to understand treatment adherence and affect cognition interactions. Cognitive Therapy and Research 16(2):143-163.
Lewis, A., and S. Parsons. 2008. Understanding of epilepsy by children and young people with epilepsy. European Journal of Special Needs Education 23(4):321-335.
Lewis, D. 2005. Delivery of online learning for healthcare consumers. In Consumer health informatics: Informing consumers and improving health care. Health Informatics Series, edited by D. Lewis, G. Eysenbach, R. Kukafka, Z. Stavri, and H. Jamison. New York: Springer. Pp. 71-84.
Lewis, M. A., I. Salas, A. de la Sota, N. Chiofalo, and B. Leake. 1990. Randomized trial of a program to enhance the competencies of children with epilepsy. Epilepsia 31(1):101-109.
Lewis, M. A., C. L. Hatton, I. Salas, B. Leake, and N. Chiofalo. 1991. Impact of the children’s epilepsy program on parents. Epilepsia 32(3):365-374.
Lewis, S., S. Higgins, and M. Goodwin. 2008. Informing patients about sudden unexpected death in epilepsy: A survey of specialist nurses. British Journal of Neuroscience Nursing 4(1):30-34.
Lewis, S. A., J. Noyes, and S. Mackereth. 2010. Knowledge and information needs of young people with epilepsy and their parents: Mixed-method systematic review. BMC Pediatrics 10:103.
Little, P., H. Everitt, I. Williamson, G. Warner, M. Moore, C. Gould, K. Ferrier, and S. Payne. 2001. Preferences of patients for patient centred approach to consultation in primary care: Observational study. BMJ 322(7284):468-472.
Long, L., A. L. Reeves, J. L. Moore, J. Roach, and C. T. Pickering. 2000. An assessment of epilepsy patients′ knowledge of their disorder. Epilepsia 41(6):727-731.
Lorig, K. R., and H. Holman. 2003. Self-management education: History, definition, outcomes, and mechanisms. Annals of Behavioral Medicine 26(1):1-7.
Lorig, K. R., D. S. Sobel, A. L. Stewart, B. W. Brown, Jr., A. Bandura, P. Ritter, V. M. Gonzalez, D. D. Laurent, and H. R. Holman. 1999. Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalization: A randomized trial. Medical Care 37(1):5-14.
Lorig, K., P. L. Ritter, and K. Plant. 2005. A disease-specific self-help program compared with a generalized chronic disease self-help program for arthritis patients. Arthritis and Rheumatism 53(6):950-957.
Lorig, K. R., P. L. Ritter, D. D. Laurent, and K. Plant. 2006. Internet-based chronic disease self-management: A randomized trial. Medical Care 44(11):964-971.
Lu, C., E. Wirrell, and M. Blackman. 2005. Where do families of children with epilepsy obtain their information? Journal of Child Neurology 20(11):905-910.
Lv, R., L. Wu, L. Jin, Q. Lu, M. Wang, Y. Qu, and H. Liu. 2009. Depression, anxiety and quality of life in parents of children with epilepsy. Acta Neurologica Scandinavica 120(5):335-341.
Marks, R., J. P. Allegrante, and K. Lorig. 2005. A review and synthesis of research evidence for self-efficacy-enhancing interventions for reducing chronic disability: Implications for health education practice (part II). Health Promotion Practice 6(2):148-156.
Martin, R., L. Vogtle, F. Gilliam, and E. Faught. 2003. Health-related quality of life in senior adults with epilepsy: What we know from randomized clinical trials and suggestions for future research. Epilepsy and Behavior 4(6):626-634.
———. 2005. What are the concerns of older adults living with epilepsy? Epilepsy and Behavior 7(2):297-300.
Martlew, J., A. Baker Gus, L. Goodfellow, N. Bodde, and A. Aldenkamp. 2007. Behavioural treatments for non-epileptic attack disorder. Cochrane Database of Systematic Reviews 1:CD006370.
Mattson, R. H., and B. E. Gidal. 2004. Fractures, epilepsy, and antiepileptic drugs. Epilepsy and Behavior 5(Suppl. 2):S36-S40.
May, T. W., and M. Pfäfflin. 2002. The efficacy of an educational treatment program for patients with epilepsy (MOSES): Results of a controlled, randomized study. Modular Service Package Epilepsy. Epilepsia 43(5):539-549.
McCloskey, J., and D. Flenniken. 2010. Overcoming cultural barriers to diabetes control: A qualitative study of southwestern New Mexico Hispanics. Journal of Cultural Diversity 17(3):110-115.
McNelis, A., B. Musick, J. Austin, D. Dunn, and K. Creasy. 1998. Psychosocial care needs of children with new-onset seizures. Journal of Neuroscience Nursing 30(3):161-165.
McNelis, A. M., J. Buelow, J. Myers, and E. A. Johnson. 2007. Concerns and needs of children with epilepsy and their parents. Clinical Nurse Specialist 21(4):195-202.
Miller, L., and S. Rollnick. 2002. Motivational interviewing. 2nd ed. New York: Guilford Press
Mittan, R. J. 2009. Psychosocial treatment programs in epilepsy: A review. Epilepsy and Behavior 16(3):371-380.
Modi, A. C., J. R. Rausch, and T. A. Glauser. 2011. Patterns of nonadherence to antiepileptic drug therapy in children with newly diagnosed epilepsy. JAMA 305(16):1669-1676.
Mohanraj, R., J. Norrie, L. J. Stephen, K. Kelly, N. Hitiris, and M. J. Brodie. 2006. Mortality in adults with newly diagnosed and chronic epilepsy: A retrospective comparative study. Lancet Neurology 5(6):481-487.
Morahan-Martin, J. M. 2004. How Internet users find, evaluate, and use online health information: A cross-cultural review. Cyberpsychology and Behavior 7(5):497-510.
Morton, B., A. Richardson, and S. Duncan. 2006. Sudden unexpected death in epilepsy (SUDEP): Don’t ask, don’t tell? Journal of Neurology, Neurosurgery and Psychiatry 77(2):199-202.
Mu, P. F. 2005. Paternal reactions to a child with epilepsy: Uncertainty, coping strategies, and depression. Journal of Advanced Nursing 49(4):367-376.
———. 2008. Transition experience of parents caring of children with epilepsy: A phenomenological study. International Journal or Nursing Studies 45(4):543-551.
Nakhutina, L., J. S. Gonzalez, S. A. Margolis, A. Spada, and A. Grant. 2011. Adherence to antiepileptic drugs and beliefs about medication among predominantly ethnic minority patients with epilepsy. Epilepsy and Behavior 22(3):584-586.
NCBDE (National Certification Board for Diabetes Educators). 2012. National Certification Board for Diabetes Educators. http://www.ncbde.org/index.cfm (accessed February 22, 2012).
Neligan, A., and S. D. Shorvon. 2010. Frequency and prognosis of convulsive status epilepticus of different causes: A systematic review. Archives of Neurology 67(8):931-940.
Nolan, K. J., C. S. Camfield, and P. R. Camfield. 2006. Coping with Dravet syndrome: Parental experiences with a catastrophic epilepsy. Developmental Medicine and Child Neurology 48(9):761-765.
———. 2008. Coping with a child with Dravet syndrome: Insights from families. Journal of Child Neurology 23(6):690-694.
Nunez, D. E., C. Keller, and C. D. Ananian. 2009. A review of the efficacy of the self-management model on health outcomes in community-residing older adults with arthritis. Worldviews on Evidence-Based Nursing 6(3):130-148.
ODPHP (Office of Disease Prevention and Health Promotion). 2010. National action plan to improve health literacy. Washington, DC: U.S. Department of Health and Human Services.
Oostrom, K. J., A. Schouten, C. L. Kruitwagen, A. C. Peters, and A. Jennekens-Schinkel. 2001. Parents’ perceptions of adversity introduced by upheaval and uncertainty at the onset of childhood epilepsy. Epilepsia 42(11):1452-1460.
Pack, A. M., and M. J. Morrell. 2001. Adverse effects of antiepileptic drugs on bone structure: Epidemiology, mechanisms and therapeutic implications. CNS Drugs 15(8):633-642.
Paschal, A. M., E. Ablah, R. Wetta-Hall, C. A. Molgaard, and K. Liow. 2005. Stigma and safe havens: A medical sociological perspective on African-American female epilepsy patients. Epilepsy and Behavior 7(1):106-115.
Paschal, A. M., S. R. Hawley, T. St Romain, K. Liow, C. A. Molgaard, J. Sly, and T. L. Sadler. 2007. Epilepsy patients’ perceptions about stigma, education, and awareness: Preliminary responses based on a community participatory approach. Epilepsy and Behavior 11(3):329-337.
Pennell, P. B., and P. Thompson. 2009. Gender-specific psychosocial impact of living with epilepsy. Epilepsy and Behavior 15(Suppl. 1):S20-S25.
Pfizer. 2012. The newest vital sign: A new health literacy assessment tool for health care providers. http://www.pfizerhealthliteracy.com/public-policy-researchers/NewestVitalSign.aspx (accessed February 22, 2012).
Pramuka, M., R. Hendrickson, and A. C. Van Cott. 2010. Survey results of Internet and computer usage in veterans with epilepsy. Epilepsy and Behavior 17(3):366-368.
Prinjha, S., A. Chapple, A. Herxheimer, and A. McPherson. 2005. Many people with epilepsy want to know more: A qualitative study. Family Practice 22(4):435-441.
Prochaska, J. O., and C. C. DiClemente. 1982. Transtheoretical therapy: Toward a more inte-grative model of change. Psychotherapy: Theory, Research and Practice 19(3):276-288.
Rajasundaram, R., S. Phillips, and N. R. Clay. 2006. Information leaflet used in out-patient clinics: A survey of attitude and understanding of the user. International Journal of Health Care Quality Assurance Incorporating Leadership in Health Services 19(6-7):575-579.
Rau, J., T. W. May, M. Pfäfflin, D. Heubrock, and F. Petermann. 2006. [Education of children with epilepsy and their parents by the modular education program epilepsy for families (FAMOSES)—Results of an evaluation study]. Rehabilitation (Stuttgart) 45(1):27-39.
Ried, S., U. Specht, R. Thorbecke, K. Goecke, and R. Wohlfarth. 2001. MOSES: An educational program for patients with epilepsy and their relatives. Epilepsia 42(Suppl. 3):76-80.
Rodenburg, R., A. M. Meijer, M. Dekovic, and A. P. Aldenkamp. 2005. Family factors and psychopathology in children with epilepsy: A literature review. Epilepsy and Behavior 6(4):488-503.
Rowan, A. J. 2000. Epilepsy and the elderly. Epilepsy and Behavior 1(1):S12-S14.
Safeer, R. S., and J. Keenan. 2005. Health literacy: The gap between physicians and patients. American Family Physician 72(3):463-468.
Sample, P. L., P. L. Ferguson, J. L. Wagner, E. Elisabeth Pickelsimer, and A. W. Selassie. 2006. Experiences of persons with epilepsy and their families as they look for medical and community care: A focus group study from South Carolina. Epilepsy and Behavior 9(4):649-662.
Sare, G., M. Rawnsley, A. Stoneman, and S. Duncan. 2007. Men with epilepsy—The lost tribe? Results of a nationwide survey of men with epilepsy living in the UK. Seizure 16(5):384-396.
Shafer, P. O. 1998. Counseling women with epilepsy. Epilepsia 39(Suppl. 8):S38-S44.
———. 2009. Epilepsy self-management in clinical practice: What we do and know. Paper read at AES Annual Meeting, Boston, MA: Hynes Conference Center.
Shafer, P. O., and C. DiIorio. 2004. Managing life issues in epilepsy. Continuum: Lifelong Learning in Neurology—Epilepsy 10(4):138-156.
———. 2006. Part one: Self-management in epilepsy care: Putting teen and families in the center. EP Magazine June:46-48, http://www.epilepsy.com/pdfs/Except_parents_art1.pdf (accessed January 5, 2011).
Shope, J. T. 1980. Intervention to improve compliance with pediatric anticonvulsant therapy. Patient Counselling and Health Education 2(3):135-141.
Shore, C. P., S. M. Perkins, and J. K. Austin. 2008. The Seizures and Epilepsy Education (SEE) program for families of children with epilepsy: A preliminary study. Epilepsy and Behavior 12(1):157-164.
Shore, C. P., J. M. Buelow, J. K. Austin, and C. S. Johnson. 2009. Continuing psychosocial care needs in children with new-onset epilepsy and their parents. Journal of Neuroscience Nursing 41(5):244-250.
Shorvon, S., and T. Tomson. 2011. Sudden unexpected death in epilepsy. Lancet 378(9808):2028-2038.
Sirven, J. I., R. A. Lopez, B. Vazquez, and P. Van Haverbeke. 2005. Qué es la epilepsia? Attitudes and knowledge of epilepsy by Spanish-speaking adults in the United States. Epilepsy and Behavior 7(2):259-265.
So, E. L., J. Bainbridge, J. R. Buchhalter, J. Donalty, E. J. Donner, A. Finucane, N. M. Graves, L. J. Hirsch, G. D. Montouris, N. R. Temkin, S. Wiebe, and T. L. Sierzant. 2009. Report of the American Epilepsy Society and the Epilepsy Foundation Joint Task Force on Sudden Unexplained Death in Epilepsy. Epilepsia 50(4):917-922.
Swarztrauber, K. 2004. Barriers to the management of patients with surgically remediable intractable epilepsy. CNS Spectrums 9(2):146-152.
Tieffenberg, J. A., E. I. Wood, A. Alonso, M. S. Tossutti, and M. F. Vicente. 2000. A randomized field trial of ACINDES: A child-centered training model for children with chronic illnesses (asthma and epilepsy). Journal of Urban Health 77(2):280-297.
Tinetti, M. E., and C. S. Williams. 1997. Falls, injuries due to falls, and the risk of admission to a nursing home. New England Journal of Medicine 337(18):1279-1284.
Wagner, E. H., S. M. Bennett, B. T. Austin, S. M. Greene, J. K. Schaefer, and M. Vonkorff. 2005. Finding common ground: Patient-centeredness and evidence-based chronic illness care. Journal of Alternative and Complementary Medicine 11(Suppl. 1):S7-S15.
Wagner, J. L., and G. Smith. 2006. Psychosocial intervention in pediatric epilepsy: A critique of the literature. Epilepsy and Behavior 8(1):39-49.
Wagner, J. L., P. L. Sample, P. L. Ferguson, E. E. Pickelsimer, G. M. Smith, and A. W. Selassie. 2009. Impact of pediatric epilepsy: Voices from a focus group and implications for public policy change. Epilepsy and Behavior 16(1):161-165.
Wagner, J. L., G. Smith, P. Ferguson, K. van Bakergem, and S. Hrisko. 2010. Pilot study of an integrated cognitive-behavioral and self-management intervention for youth with epilepsy and caregivers: Coping Openly and Personally with Epilepsy (COPE). Epilepsy and Behavior 18(3):280-285.
Wicks, P., D. L. Keininger, M. P. Massagli, C. D. la Loge, C. Brownstein, J. Isojarvi, and J. Heywood. 2012. Perceived benefits of sharing health data between people with epilepsy on an online platform. Epilepsy and Behavior 23(1):16-23.
Wood, L. J., E. M. Sherman, L. D. Hamiwka, M. A. Blackman, and E. C. Wirrell. 2008. Maternal depression: The cost of caring for a child with intractable epilepsy. Pediatric Neurology 39(6):418-422.
Wu, K. N., E. Lieber, P. Siddarth, K. Smith, R. Sankar, and R. Caplan. 2008. Dealing with epilepsy: Parents speak up. Epilepsy and Behavior 13(1):131-138.