2
What Progress in Reducing Health
Disparities Has Been Made?:
A Historical Perspective
William Vega noted that a decade has passed since several seminal reports on health disparities were released, including Surgeon General David Satcher’s series of reports showing dramatic racial and ethnic disparities in morbidity and mortality rates and in certain risk behaviors, such as tobacco use (HHS, 1998). He also noted that members of racial and ethnic minorities have access to a lower quality of health care services than majority group members.
At about the same time, the Institute of Medicine (IOM) published its routinely cited study focusing on health care quality, Crossing the Quality Chasm: A New Health System for the 21st Century (IOM, 2001). Furthermore, in 2000, the first federal legislation focusing on the reduction of health disparities was signed into law.
Taken together, these developments helped shine a light on the problem of health disparities. Even today, however, some dominating issues continue to perplex the field because they are not easy to disentangle. First, no agreed-upon definition of “health disparities” exists. To effectively monitor changes in health disparities, definitions that are widely accepted need to be available. Furthermore, although data indicate that some health indicators are improving for all racial and ethnic groups, the gap between groups remains constant.
Second is the issue of scale. When the promotion of healthy lifestyles across the life course is considered, the integration of large sectors and policies across sectors that have never before been integrated can seem daunting. Moreover, sectors such as housing, transportation, and energy are
not typically associated with health, which makes efforts to integrate these sectors into promotion of healthy lifestyles more complex.
Finally, the magnitude of the effort that is necessary to eliminate health disparities should be acknowledged. Because the problem of health disparities is so intransigent, an effort of a magnitude appropriate to the scale of the problem should be made.
BUILDING STRONGER COMMUNITIES FOR BETTER HEALTH: MOVING FROM SCIENCE TO POLICY AND PRACTICE
Brian Smedley is director of the Health Policy Institute at the Joint Center for Political and Economic Studies. His presentation focused on policy and programmatic trends that relate to health inequities and the progress that has been made in addressing these trends.
Challenges to Advancing the Health Equity Agenda
Advancing the health equity agenda has three major challenges, said Smedley. First, the effects of the current economic downturn cannot be underestimated. It is likely that over the next few years the data will show that health inequities have widened rather than narrowed.
Second, the perception among Americans that the United States is now in a postracial period is inaccurate, Smedley said. Because the country has an African American president and because many people of color are leading major corporations, some believe that U.S. society is now color-blind (e.g., Cho, 2009). The research shows, however, that structural inequalities and racial discrimination persist at significant levels.
One example of this line of research uses matched-pair testers. By this approach, two people—one white and one Latino or African American—are equally matched on levels of education, personality, clothing, and so on. The two people are then sent out into a community to apply for jobs, obtain rental housing, apply for a mortgage, or seek to purchase a home. Studies consistently show that the paired tester of color receives poorer treatment, on average (Turner et al., 2003).
In one study that was replicated in two different cities, Pager (2003) found that when the paired testers—one white member with a criminal background and one African American member with no criminal background—were sent out to seek employment, the white member of the pair had a better chance of being hired for a job than the African American member. These findings, Smedley explained, show the depth of the persistent discrimination experienced by people of color in the United States.
The third challenge is the value that American society places on the strong individual determinist ideal. Americans believe that their success is
determined by how hard they work and how hard they pull themselves up by their own bootstraps. The nation is oriented toward personal responsibility, said Smedley. This orientation means that people fail to pay attention to context or environmental factors, but the context in which a person is born affects the life opportunities available to that person.
One example of the tendency to ignore environmental influences on individual behavior can be found in research on local retail food environments. Low-income neighborhoods frequently lack decent grocery stores, and the source of food is often limited to convenience stores, carryout places, and fast-food restaurants. These characteristics of low-income neighborhoods make access to nutritious foods difficult (Powell et al., 2007; Ver Ploeg et al., 2009). Moreover, Smedley noted that systematic differences in the quality of retail food available in different communities exist by race and geography.
Developments from 2000 to 2010
Smedley indicated, however, that it is important to acknowledge that some major developments in both the governmental and private sectors to address health inequities occurred between 2000 and 2010. During that period, the increase in the levels of attention and awareness about health inequities by all levels of government and by the general public was dramatic.
The federal government, in particular, is making significant efforts to address health inequities. For example, the Patient Protection and Affordable Care Act (ACA) of 2010 will help improve access to care for many and will disproportionately improve access for low-income people and people of color. Smedley commented that more needs to be done in the area of community-based primary prevention. However, an important development is the elevation of the National Center on Minority Health and Health Disparities to an institute within the National Institutes of Health so that it is now the National Institute on Minority Health and Health Disparities.
The federal government also addressed health inequities through the stimulus funding provided through the American Recovery and Reinvestment Act of 2009, which led to the creation of the Communities Putting Prevention to Work initiative. Smedley stated that this initiative is critically important because it focuses on the importance of place and the need to create healthier conditions within communities.
The private sector has also provided important leadership in this area. In fact, earlier in the decade, Smedley said, private-sector leadership was critical in bringing attention to health inequities. For example, both the Robert Wood Johnson Foundation’s Commission to Build a Healthier America and the Kellogg Foundation’s ongoing focus on health inequities
and racial healing led to major efforts to reduce health inequities. Similarly, The California Endowment is emphasizing the importance of place and the need for investing in communities. Finally, initiatives of the Kaiser Family Foundation and the MacArthur Research Network on Socioeconomic Status and Health are taking significant steps to advance efforts to reduce health inequities.
Scientific advances have played a role in educating elected officials and the general public about the causes of health inequities. One example of such an advance is the debunking of the use of race as a biological construct. Race has no genetic or biological basis, explained Smedley, but rather is a social construct and should be studied as such. It is still essential to study race as a social construct because of its implications for health inequities and because in the United States race often structures opportunity in powerful ways. According to Smedley, “It is the lived experience of race in America that has biological and health consequences. So this is where our focus needs to be.”
Smedley believes that a greater appreciation of the social determinants of health exists today. Research findings accumulated over the past 20 years make it clear that social and economic inequalities shape many of the health disparities in the United States. In particular, the role of residential segregation in shaping health inequities cannot be underestimated.
Residential Segregation
Although much progress in the desegregation of communities was made in the aftermath of Jim Crow laws1 and other legal means of enforcing racial segregation, segregation persists at high levels in the United States, Smedley said. Describing patterns of residential segregation in the United States, Smedley explained that demographers use an index called the “dissimilarity index” (Massey and Denton, 1988), which is the percentage of people in a defined geographic area who would have to move to create integration in that area. Detroit, Michigan, for example, has a dissimilarity index of 85; in other words, 85 percent of white and African American Detroiters would have to move to create racial integration.
Residential segregation in many other U.S. cities is not far behind that in Detroit. Milwaukee, Wisconsin; New York City; Chicago, Illinois; and Newark, New Jersey, all have dissimilarity indexes of 80. In other words, four out of five residents of those cities would have to move to achieve integration in those cities.
An additional link can be drawn between residential segregation and
![]()
1 Jim Crow laws were enacted in southern states and localities after the Civil War in order to institutionally segregate African Americans and whites (Woodward, 1955).
the percentage of people of color who live in communities with highly concentrated poverty (defined as 30 percent or more of the population living below the federal poverty line). A large body of research shows that living in these communities is harmful to people’s health. This is because health-enhancing resources (access to physician care, for example) are generally harder to find in these communities. At the same time, conditions that present health risks (for example, environmental degradation, lack of access to healthy food, and lack of access to appropriate outdoor spaces that encourage physical activity) are generally more prevalent in these communities.
For example, no single major chain grocery store is located within the Detroit city limits. Therefore, a person living in Detroit has to go outside Detroit, to the suburbs, to purchase low-cost fresh fruit and vegetables. Furthermore, because little public transportation is available, a person living in Detroit without a car will find it nearly impossible to maintain a healthy diet.
Figure 2-1 shows that the percentage of poor families living in high-poverty neighborhoods declined from 1960 to 2000 (although in every decade, more African American families than families in other racial and ethnic groups still lived in high-poverty neighborhoods). In 1960, for example, about 64 percent of poor African American families and about 54 percent of poor Latino families lived in high-poverty neighborhoods.
However, Smedley noted that the decline was more rapid for poor
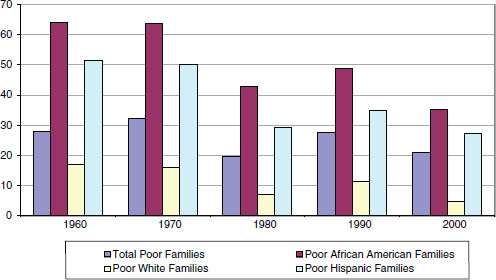
FIGURE 2-1 Percentage of poor families living in high-poverty neighborhoods (poverty rate of 30 percent or more), 1960 to 2000. SOURCE: The Opportunity Agenda (2006). Figure 2-1, color
white families than for African American or Latino families living in high-poverty neighborhoods (Figure 2-1). What, then, is the relative risk that families of color (relative to white families) live in neighborhoods of concentrated poverty? In 1960, the relative risk for African American families was 13 (that is, African American families were 13 times more likely than white families to live in high-poverty neighborhoods). By the year 2000, the relative risk had increased to 36: African American families were 36 times more likely to be living in a community with high concentrations of poverty. The same trend can be seen for Latino families (Figure 2-2).
A more specific look at poor families shows that poor African American families were almost six times as likely as poor white families to live in a high-poverty neighborhood in 1960. By 2000, that relative risk had increased to 11. Poor Latino families were four times as likely as poor white families to live in a high-poverty neighborhood in 1960; by 2000, the relative risk had increased to 6.7.
What does this information mean? Although the overall percentage of poor families living in concentrated-poverty neighborhoods (Figure 2-2) declined, many families of color were left behind. Smedley speculated that this might be due to white flight from high-poverty neighborhoods.
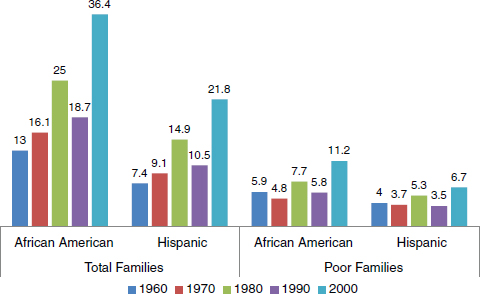
FIGURE 2-2 Relative risk of living in a neighborhood with concentrated poverty (40 percent or more). The relative risk for white families is 1.00. SOURCE: Smedley (2010).
Strategies for Addressing the Effects of Segregation on Health
Smedley concluded his comments by noting that two general strategies for addressing segregation and its relationship to health may be used. The first is a set of people-based strategies to increase housing mobility options. In this way, people would have the ability to move out of communities experiencing stress and disinvestment and into communities with greater investments.
The second set consists of place-based strategies, which are designed to increase investments in communities, thereby improving the conditions for better health in those communities. An example is the effort to provide incentives for large chain grocery stores to move into communities characterized as “food deserts.” Other place-based strategies include increases in investments in housing, transportation, and job creation. Dr. Smedley emphasized that these are the most important issues to be tackled to reduce health inequities.
WHERE DO HEALTH DISPARITIES STAND TODAY?
David Williams has an academic and research background in public health as well as in the social, cultural, and historical issues associated with the health of African Americans. His presentation focused on the status of health disparities in the United States today.
Persistence of Disparities Over Time
The first characteristic of health disparities that Williams pointed out is that racial and ethnic health disparities have persisted over time. For example, the rate of heart disease—the number one cause of death in the United States—has declined over time for both African Americans and whites. In 1950 (Figure 2-3), no disparity in rates of death from heart disease existed between African Americans and whites. However, even though rates of death from heart disease for both groups have steadily declined, since 1980, a gap in rates between whites and African Americans that was not present in 1950 has appeared.
A similar pattern exists for rates of death from cancer, which began increasing for both groups. In 1970, however, the rate for African Americans began to show a steeper increase than that for whites. Although by 1990 cancer death rates began to decline for both groups, a gap remains between African Americans and whites.
These gaps in death rates do not exist only between whites and African Americans. Data from the Indian Health Service (Figure 2-4) indicate that since the 1950s American Indians have consistently had higher rates of
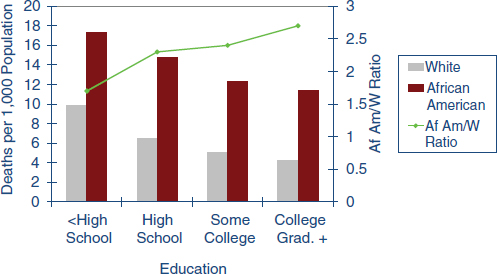
FIGURE 2-3 Rates of mortality from heart disease among African Americans (Af Am) and whites (W).
SOURCE: Miniño et al. (2007).
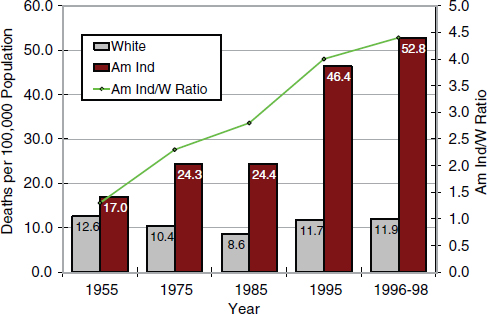
FIGURE 2-4 Rates of disparity in mortality from diabetes among American Indians (Am Ind) and whites (W), 1955 to 1998.
SOURCE: Indian Health Service (2001).
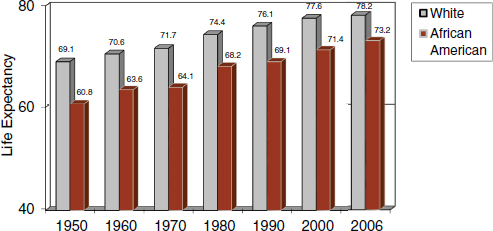
FIGURE 2-5 Life expectancy rates for African Americans and whites, 1950 to 2006.
SOURCE: Arias et al. (2010).
death from diabetes than whites. However, the rate has increased dramatically for American Indians and far outpaces that for whites.
Another way to document health disparities is to look at life expectancies for African Americans and whites (Figure 2-5), as life expectancy rates serve as a widely used indicator of health. In 1950, the life expectancy for whites was 69.1 years. However, it was not until 1990 that the life expectancy for African Americans reached 69.1 years, four decades later. In other words, it took African Americans 40 years to catch up to the life expectancy of white Americans in 1950.
Disparities Across the Life Span
A second characteristic of health disparities by race and ethnicity is that they exist across the life course. Beginning with the first part of life (under 24 years of age), ratios of the rates of mortality for minorities to rates for whites are the highest for infants and children from 1 to 4 years of age. For infants under 12 months, the mortality ratios are higher for African American and American Indian infants than white infants. For young children (ages 1 to 4 years), American Indians have the highest mortality compared to whites.
In midlife (ages 25 to 64 years), the mortality ratio for African Americans to whites is highest during every decade of life (25-34, 35-44, 45-54, and 55-64 years), followed by the mortality ratio for American Indians
to whites. The same pattern exists for ages 65 years and older, with the exception of the group age 85 years and older; although the mortality ratio for African Americans to whites is still the highest for that age group, the mortality ratio for Latinos to whites is higher than that for American Indians to whites.
In short, health disparities exist from the cradle to the grave, Williams said. Even since 1999, the data show elevated rates of mortality for African Americans and American Indians at all ages compared with those for whites. Moreover, mortality rates for African Americans are trending downward, while mortality rates for whites are trending upward. This is another disparity that exists over time and generations.
First and Worst
Having documented the higher death rates for minority groups than whites, Williams stated that not only are mortality rates higher for racial and ethnic minorities, but these groups must also contend with earlier disease onset and a greater severity of disease. Breast cancer is a good example of a disease with earlier onset for racial and ethnic minority groups and serves as a classic example of the need to look more closely at the data. Although white women have a higher overall incidence of breast cancer than African American women, this pattern is reversed for African American women under age 40 years.
Even worse, stated Williams, African American women are more likely than white women to be diagnosed with cancer when the cancer is at a more advanced stage, to have more aggressive forms of the cancer that are resistant to treatment, and to have what are called “triple-negative tumors” (tumors that grow more quickly, recur more quickly, and kill more frequently). African American women also have higher rates of mortality from breast cancer than white women. In short, although African American women have a lower overall incidence of breast cancer than white women, their health outcomes after breast cancer are worse for every indicator.
Major depression provides another example of “first and worst,” said Williams. National-level data indicate a lower overall prevalence of current and lifetime rates of major depression for African Americans than whites. However, those African Americans who are depressed are more likely than whites to be chronically depressed, to have higher levels of impairment, to have more severe symptoms, and to not receive treatment. Again, although the overall incidence of major depression is lower for African Americans than for whites, on every measure of severity, African Americans do more poorly.
One of the most striking examples of first and worst can be seen from the patterns of neonatal mortality for women having their first birth.
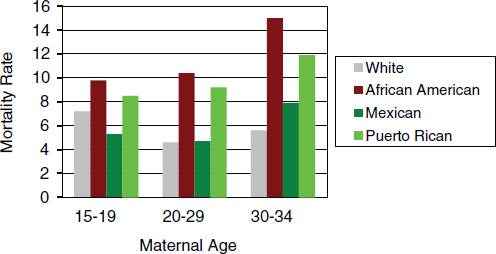
FIGURE 2-6 Neonatal mortality rates for first births in the United States.
SOURCE: Geronimus and Bound (1991) and CDC (1983).
For white women and Mexican American women (Figure 2-6), delaying childbirth until they are in their 20s or 30s results in lower mortality rates (Geronimus and Bound, 1990). In contrast, rates of neonatal mortality are higher when African American and Puerto Rican women delay their first births. The authors of the study explain this finding by suggesting that minorities living in disadvantaged circumstances and under adverse conditions have been physiologically compromised. Thus, their wait until later in life to have a child means that they have had greater exposure to adverse conditions at the time that they become pregnant. It should be noted, however, that as indicated by Figure 2-6, neonatal mortality rates are highest for African Americans across all three age groups, with Puerto Rican women the second highest across all age groups when compared to white and Mexican women.
Migration
Patterns of migration should be considered when health disparities are examined, Williams said, because migration has powerful influences on health. According to 2000 census data, almost 69 percent of Asians in the United States are foreign born and more than 40 percent of Latinos are foreign born. This is important because immigrants of all racial and ethnic groups have better health outcomes than their counterparts born in the United States. Across the board, Williams said, the data show this “healthy immigrant” effect.
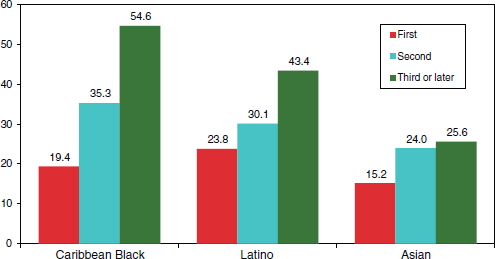
FIGURE 2-7 Lifetime prevalence of psychiatric disorders by race and generational status (in percent).
SOURCE: Alegria et al. (2007), Takeuchi et al. (2007), and Williams et al. (2007).
Unfortunately, the longer that an immigrant remains in the United States, the worse his or her health becomes. Similarly, declines in health outcomes are seen with an increase in generational status. That is, the longer that a family stays in the United States, the greater is the decline in health across a broad range of health indicators. Figure 2-7 shows an example of one worsening health outcome by generational status among three immigrant ethnic minority groups: lifetime prevalence of psychiatric disorder. What drives this pattern is not clear, said Williams, but it is critical to understand it and to consider what interventions can be implemented to reverse the trajectory of worsening health for immigrant populations over time.
Socioeconomic Disadvantage and Geographic Marginalization
For those populations that have lived in the United States for multiple generations (American Indians and African Americans), the data show a pattern that points to the roles of geographic isolation, residential segregation, and socioeconomic disadvantage in the creation and maintenance of health disparities. Williams noted that socioeconomic status, in particular, is one of the most powerful predictors of health status in virtually every society.
Census data from 2006 (Figure 2-8) demonstrate that although the
majority of people living in poverty in the United States are white, African Americans and Latinos are overrepresented in the population of poor Americans. African Americans make up 12.8 percent of the U.S. population but make up 23.1 percent of the people living in poverty. Similarly, Latinos make up 14.4 percent of the general population but represent almost 24 percent of the people living in poverty.
However, race/ethnicity and socioeconomic status are not interchangeable systems of inequality, said Williams. It is therefore essential to look at both of them together. Although socioeconomic status accounts for a large portion of health disparities, race/ethnicity is an added burden that is linked to poor health.
Data showing the relationship between the mother’s level of education (which is closely related to socioeconomic status) and infant mortality illustrate this linkage. Figure 2-9 shows that even white mothers who are high school dropouts have lower infant mortality rates than college-educated
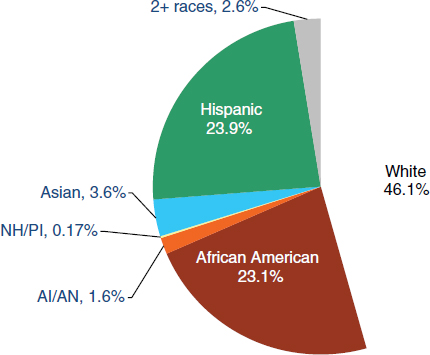
FIGURE 2-8 Racial/ethnic composition of people in poverty in the United States. AI/AN = American Indian/Alaska Native; NH/PI = Non-Hispanic/Pacific Islander.
SOURCE: DeNavas-Walt et al. (2007).
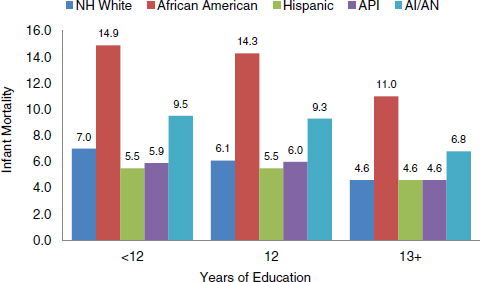
FIGURE 2-9 Infant mortality rate by mother’s education (infant death per 1,000 live births).
AI/AN = American Indian/Alaska Native; API = Asian/Pacific Islander; NH = Non-Hispanic.
SOURCE: CDC (2001).
African American mothers. The best-off African American mothers had worse health outcomes than all other racial/ethnic groups (with the exception of American Indian/Alaska Native high school dropouts).
Williams posed the question, Why does race matter so much? Three different lines of research evidence can help provide an answer. First, indicators of socioeconomic status are not equivalent across races/ethnicities. Compared with whites, African Americans with the same level of education earn less income. Compared with whites with the same income level, African Americans have less purchasing power because of the higher costs of goods and services in the places where African Americans live. The dismaying conclusion is that people of color have far fewer assets and a lower net worth than whites, even low-income whites. This is called the “wealth gap.”
Second, although current socioeconomic status has a major influence on health, exposure to social and economic adversity across the life course also influences health. For example, an African American woman who was herself born with a low birth weight is more likely to give birth to an infant with low birth weight. Clearly, early life adversities have long-term effects on health and on intergenerational health, said Williams.
Finally, Dr. Williams explained that personal experiences of discrimination and institutionalized racism affect the health of minority populations by multiple mechanisms. The effects of racism on health are not limited to the United States; data from Australia, South Africa, and New Zealand show the persistent health effects of exposure to discrimination and racism among people of color.
Residential segregation, too, has a disturbing effect on African Americans, Williams noted. Sampson and Wilson (1995) looked at the largest 171 cities in the United States. In none of those cities did African Americans and whites live under the same conditions and in the same circumstances. In fact, they found that the worst conditions for whites were better than the best conditions for African Americans. Residential segregation for the Latino population in the United States is also growing.
Access to Care
Not surprisingly, large differences in access to health care also exist between whites and people of color. Both Latinos and Native Americans have low levels of health insurance coverage. Among all people with some form of health insurance, Latinos, African Americans, and Native Americans are more likely to have some form of public health insurance, such as Medicaid, than private insurance.
Good health, however, is about more than just having access to care. It is critical to consider what happens before an individual needs to go to a doctor’s Office and to consider what is happening in the community where that individual lives. Where people live, work, worship, and play, said Williams, has a greater impact on health outcomes than having access to a physician. This means that it is essential to look at ways to reduce inequalities in the nonmedical social determinants of health. “We need to redefine health policy to include housing, employment, community development, income support, transportation, and environmental policies,” he said.
Williams offered an example illustrating this. Since 1970, the group experiencing the biggest gains in overall life expectancy is African American women, and in fact, African American women have a higher life expectancy than white men. What caused this increase in life expectancy rates? Williams speculated that this increase is largely due to the positive health effects arising from civil rights policies. For example, the civil rights movement narrowed the economic gap between whites and African Americans by offering access to more and better jobs. Additionally, the desegregation of hospitals in the South due to civil rights policies led to the survival beyond infancy of an additional 5,000 to 7,000 infants between 1965 and 1975 due to access to better health care (Almond et al., 2006).
Unfortunately, since 1978, the African American–white income gap
has again widened; the situation got worse in the 1980s, leading to a decline in life expectancy for African Americans. Worsening of economic conditions during the 1980s led to worsening of health outcomes, a finding that points to the strong link between social and economic conditions and overall health. Closing Comments
Williams concluded his comments with a list of resources for learning more about racial disparities in health and the role of social conditions in causing those disparities:
• The MacArthur Foundation Research Network on Socioeconomic Status and Health (www.macses.ucsf.edu)
• Unnatural Causes: Is Inequality Making Us Sick? (www.unnaturalcauses.org)
• Robert Wood Johnson Foundation’s Commission to Build a Healthier America (www.commissionhealth.org)
The Robert Wood Johnson Foundation’s Commission to Build a Healthier America also supports the establishment of national benchmarks for health. For example, the infant mortality rate serves as an indicator of overall health. The data show that even college-educated women of all races and ethnicities do not have a level of health that reaches the benchmark established by the commission. This finding can be interpreted to mean that the country as a whole is not enjoying the best health possible. Therefore, not only do the gaps in health need to be addressed, but also the health of Americans across all racial and ethnic groups must be dealt with, said Williams.
A recent report from the Joint Center for Political and Economic Studies documents the finding that these health disparities are quite costly (LaVeist et al., 2009). For example, health care costs, lost work productivity, and premature death are all significant costs, Dr. Williams explained. Furthermore, LaVeist and his coauthors concluded that the economy loses $390 billion per year because of health disparities.
W.E.B. DuBois wrote about African American health in the publication Philadelphia Negro, noting that “the most difficult social problem in the matter of Negro health is the peculiar attitude of the nation toward the well-being of the race. There have … been few other cases in the history of civilized peoples where human suffering has been viewed with such peculiar indifference” (DuBois and Easton, 1899). Dr. Williams emphasized that it is time to consider what investments need to be made now to give every American child, of any race, ethnicity, or socioeconomic status, the tools to
be healthy and to achieve the American dream. Doing nothing has a cost that the United States should not continue to bear.
MAGNITUDE AND CONSEQUENCES OF HEALTH DISPARITIES
Steven Woolf, professor of family medicine at Virginia Commonwealth University, began his presentation by noting that his remarks have recurring themes: historic trends in the patterns of health disparities, levels of education, and income.
The first recurring theme involves historic trends in the patterns of health disparities. In 1963, for example, President John F. Kennedy noted that African Americans had a life expectancy that was 7 years shorter than that for whites. This disparity in life expectancy has persisted over the decades, as depicted in Figure 2-10.
Woolf commented that “in the back of our minds, most people understand that disparities are not a good thing for health.” In the United States, a tension between two competing arguments about how to reduce disparities exists. The first argument focuses on efforts to increase the efficacy and effectiveness of medical treatments. A huge amount of money is invested in this enterprise, with the goal of creating more powerful treatments and thereby doing a better job of providing health care. The second argument is that the focus should be on increasing equity and on closing the gaps
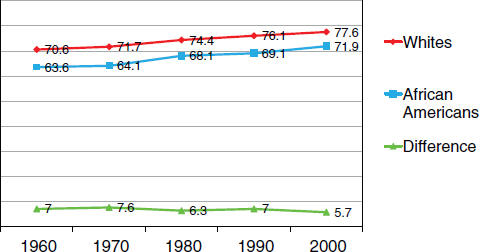
FIGURE 2-10 Life expectancy, 1960-2000.
SOURCE: Arias (2002).
in life expectancy between whites and people of color. Woolf argued that most people—including policy makers and members of the general public—believe that the first approach is going to achieve more substantial health improvements than the second one.
Describing an experiment he conducted to compare these two approaches (Woolf et al., 2004), Woolf and colleagues compared the number of lives saved by medical advances that resulted in a reduction of the number of deaths attributable to excess mortality among African Americans (176,663 deaths averted) with the number of lives saved when mortality rates between whites and African Americans are equalized (886,202 deaths averted). In other words, “achieving equity may do more for health than perfecting the technology of care” (Woolf et al., 2004, p. 2078). For each single life saved via biomedical advances, five would be saved by eliminating the discrepancy in mortality rates between African Americans and whites.
The second recurring theme involves levels of education. As discussed earlier in this chapter, it is clear that low levels of education mean worse health outcomes (Figure 2-11). It is also clear that stark disparities in
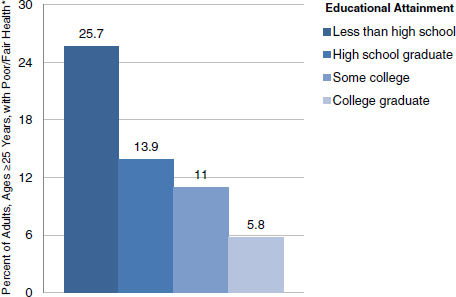
FIGURE 2-11 Less education is linked with worse health. Compared with college graduates, adults who have not finished high school are more than four times as likely to be in poor or fair health.
*Age-adjusted.
SOURCE: National Health Interview Survey, 2001-2005. Prepared for the Robert Wood Johnson Foundation by the Center on Social Disparities in Health at the University of California, San Francisco. © 2008 Robert Wood Johnson Foundation. www.commissiononhealth.org.
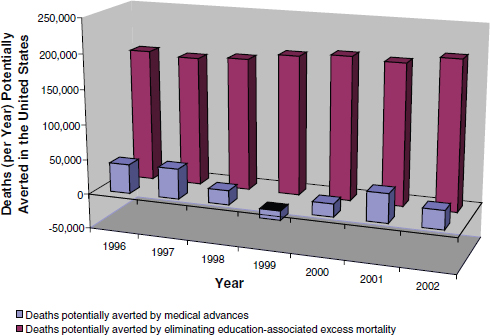
FIGURE 2-12 Deaths potentially averted by medical advances and elimination of education-associated excess mortality.
SOURCE: Woolf et al. (2007).
educational attainment exist among racial and ethnic groups. In a second study, Woolf and his colleagues (Woolf et al., 2007) again compared the number of potential lives saved by biomedical advances with the number of potential lives saved if every person over the age of 25 years had the mortality rate of people with some college education. They found that for each single life saved by biomedical advances, eight would be saved by addressing educational disparities, as seen in Figure 2-12.
The Robert Wood Johnson Foundation created a web-based interactive tool for the Commission to Build a Healthier America. The tool allows users to target a state or county of interest and then manipulate the educational attainment of the population in that state or county. The tool shows the user how many deaths could be averted if educational attainment was improved. (As of December 2009, the Robert Wood Johnson Foundation’s Commission came to a close; however, information may still be found at the following link:http://www.commissiononhealth.org/Education.aspx.)
Along with race/ethnicity and education level, income is a third recurring theme affecting health inequities. Over the past decade, the United States has seen a widening gap between the rich and the poor. Describing a recently published study of Virginia, Woolf compared the richest and
poorest counties. If the mortality rate of the richest counties was applied to everyone in the state, 25 percent of all deaths would not have occurred.
Woolf concluded his remarks by circling back to the issue of clinical care. As seen in Figure 2-13, health is more than health care, and health is more than just individual behavior choices. When disparities are discussed, much of the attention in the past has focused on how disparities in the way in which patients are treated and managed can be reduced or eliminated. Although vitally important, Woolf stated that efforts to reduce discrimination in clinical settings have a relatively marginal impact on the reduction of health disparities. Rather, the focus needs to be on the root causes of health disparities, including the living and working conditions in the communities where people live. These factors, said Woolf, play a much larger role in health disparities than anything that is a part of clinical care. Furthermore, the larger economic conditions—poverty, low educational attainment—have an even greater role in health disparities.
The movement toward a “health in all policies” approach to shaping public policy will improve health conditions for all. For example, promoting transportation policies that make it easier for people to walk and bike in their communities will affect health, as will the promotion of housing policies that support reduced exposure to lead and radon in the home. In short, Woolf concluded, it is time to begin thinking more broadly about
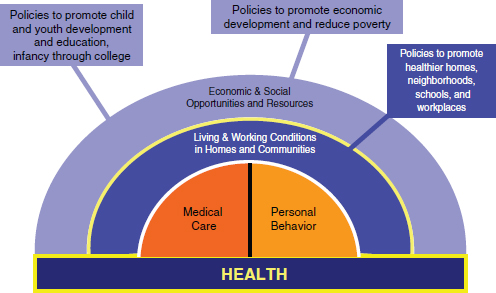
FIGURE 2-13 Importance of social factors.
SOURCE: Robert Wood Johnson Foundation, Commission to Build a Healthier America (2009).
public policy approaches to the elimination of health disparities. This will involve thinking about policy issues that are typically thought of as being outside the health arena.
Ruth Perot of the Summit Health Institute for Research and Education raised the issue of community engagement and the importance of connecting systems changes with the political process. David Williams commented that most Americans from all racial and ethnic groups are still unaware of the existence of health disparities. Although these issues have been discussed for years, even most African Americans are unaware of the disparities in rates of infant mortality and life expectancy between African Americans and whites. Thus, the issue of first raising awareness is critical. One powerful tool for raising awareness of health disparities at the community level is the Unnatural Causes television series, Williams pointed out.
Additionally, since the election of President Barack Obama, many Americans believe that race is less of an issue now than in the past. Because of this general feeling that race is less of an issue, people are less supportive of policies to address racial inequities in the United States, Williams noted.
Brian Smedley commented on the growing recognition that any effort to intervene in the reduction of health disparities needs to include the community as a partner. Some pragmatic solutions can be implemented at the local level, for example, solutions involving land use policies and zoning. However, these solutions cannot be put into place without meaningful community engagement.
Much of the action to address health inequities is taking place at the local levels, Smedley said. However, health disparities will not be completely solved until the broader issues of social and economic inequalities are addressed because stark differences in access to opportunity exist between people of color and whites in the United States.
Steven Woolf added that two large events that took place in the past 10 years have affected how Americans look at race and poverty: Hurricane Katrina and the ongoing recession and economic crisis. Hurricane Katrina brought brief attention to issues of poverty and race because of the television images of events in the lower Ninth Ward of New Orleans. Unfortunately, that attention did not last.
The ongoing economic crisis has also brought a brief focus on the issue of race and poverty, said Woolf. Because of the scope of the economic crisis, it has affected the middle class and more affluent groups in the United States, and now might be the time to try to build interest in addressing social issues, such as jobs and unemployment. They are no longer solely the problems of the lower classes.
Aida Giachello from the University of Illinois at Chicago described efforts under way in Brazil to improve health outcomes for all. First, the constitution was changed to include a statement that health care is a right and not a privilege. Second, policy makers in Brazil began to integrate health into all national policies, including housing, education, and commerce. Brazil recognizes that the health of a community cannot be improved without also improving the economic well-being of that community, and so health is an issue that cuts across all national policies.
With this background information, Giachello asked the panelists to again address the question of whether progress in the reduction of disparities in the United States has been made. Woolf responded that evidence of some positive trends can be seen; for example, educational attainment rates are increasing for all population groups in the United States. Positive trends from the health care sector are reductions in mortality rates and some increases in access to preventive services and other clinical services for disadvantaged populations. Unfortunately, the ongoing economic crisis does not bode well for the continuation of these positive trends.
Williams agreed that although some good news can be provided, the country nonetheless has a long way to go to reduce health disparities. However, he said, “The very fact that the IOM has a Roundtable on this topic is good news, and that is progress” because it means that these issues are being considered at the highest levels. Additionally, Howard Koh, assistant secretary for health of the U.S. Department of Health and Human Services, outlined the many prevention provisions in the health reform law (the ACA of 2010) that also mean good news, including additional resources for community health centers. The Obama administration also has a number of initiatives that address the social determinants of health in new ways. In short, Williams said, although much remains to be accomplished, these issues are receiving more attention than ever before.
Smedley concluded this conversation by commenting that he worries that the country is only “nibbling at the margins” rather than dealing with big policy questions. For example, public school systems across the United States are re-segregating to pre–Brown v. Board of Education levels. He believes that this is a disturbing trend because educational attainment is such a powerful predictor of health status. Wealth inequality between racial and ethnic groups is also increasing; along with the current economic downturn, this could lead to increasing—rather than decreasing—health inequities.
Chiquita Collins of the Altarum Institute raised a question about dismantling systemic institutional racism. Williams responded that a large body of scientific research documents the finding that exposure to racism at the individual level has pervasive adverse consequences on health status. Additionally, exposure to unfair treatment on the basis of race or ethnicity
adversely affects the health of all population groups, including whites. Therefore, he said, it is critical to treat racism as an important topic and to think about ways to achieve racial healing.
Alegria, M., N. Mulvaney-Day, M. Torres, A. Polo, Z. Cao, and G. Canino. 2007. Prevalence of psychiatric disorders across Latino subgroups in the United States. American Journal of Public Health 97:68-75.
Almond, D., K. Y. Chay, and M. Greenstone. 2006. Civil Rights, the War on Poverty, and Black-White Convergence in Infant Mortality in the Rural South and Mississippi. Working paper 07-04. Cambridge, MA: Department of Economics, Massachusetts Institute of Technology.
Arias, E. 2002. United States Life Tables, 2000. National vital statistics reports 51(3). Hyatts-ville, MD: National Center for Health Statistics.
Arias, E., B. L. Rostron, and B. Tejada-Vera. 2010. United States life tables, 2005. National Vital Statistics Reports 58(10). Hyattsville, MD: National Center for Health Statistics.
CDC (Centers for Disease Control and Prevention). 1983. Linked Birth and Infant Death Data. Atlanta, GA: Centers for Disease Control and Prevention.
CDC. 2001. Health, United States, 2001: Urban and Rural Health Chartbook. Atlanta, GA: Centers for Disease Control and Prevention.
Cho, S. 2009. Post-racialism. Iowa Law Review 94(5):1589-1649.
DeNavas-Walt, C., B. D. Proctor, and J. Smith. 2007. U.S. Census Bureau, Current Population Reports, P60-233, Income, Poverty, and Health Insurance Coverage in the United States: 2006. Washington, DC: U.S. Government Printing Office.
DuBois, W.E.B., and I. Easton. 1899. The Philadelphia Negro: A Social Study. Political Economy and Public Law. Philadelphia, PA: University of Philadelphia.
Geronimus, A. T., and J. Bound.1991. Black/White Infant Mortality Differentials in the United States: Towards More Theory Based Research. American Statistical Association Proceedings, pp. 228-237.
HHS (U.S. Department of Health and Human Services). 1998. Tobacco Use Among U.S. Racial/Ethic Minority Groups—African Americans, American Indians and Alaska Natives, Asian Americans and Pacific Islanders, and Hispanics: A Report of the Surgeon General. Atlanta, GA: Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention, U.S. Department of Health and Human Services.
Indian Health Service. 2001. Trends in Indian Health 2000-2001. Washington, DC: Indian Health Service.
IOM (Institute of Medicine). 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
LaVeist, T. A., D. J. Gaskin, and P. Richard. 2009. The Economic Burden of Health Inequalities in the United States. Washington, DC: Joint Center for Political and Economic Studies.
Massey, D. S., and N. A. Denton. 1988. The dimensions of residential segregation. Social Forces 67(2):281-315.
Miniño, A. M., M. P. Heron, S. L. Murphy, and K. D. Kochankek. 2007. Deaths: Final data for 2004. National Vital Statistics Reports 55(19). Hyattsville, MD: National Center for Health Statistics.
Murphy, S. L. 2000. Deaths: Final data for 1998. National Vital Statistics Reports 48(11). Hyattsville, MD: National Center for Health Statistics.
The Opportunity Agenda. 2006. The State of Opportunity Report 2006. New York: The Opportunity Agenda.
Pager, D. 2003. The mark of a criminal record. American Journal of Sociology 108(5):937-975.
Powell, L. M., C. Auld, F. J. Chaloupka, and P. M. O’Malley. 2007. Associations between access to food stores and adolescent body mass index. American Journal of Preventive Medicine 33(4S):S301-S307.
RWJF (Robert Wood Johnson Foundation), Commission to Build a Healthier America. 2009. Issue Brief 5: Race and Socioeconomic Factors. Princeton, NJ: Robert Wood Johnson Foundation.
Sampson, R. J., and W. J. Wilson. 1995. Toward a theory of race, crime, and urban inequality. In Crime and Inequality, edited by J. Hagan and R. D. Peterson. Stanford, CA: Stanford University Press, pp. 37-54.
Smedley, B. 2010. Building Stronger Communities for Better Health: Moving from Science to Policy and Practice. Presentation to the IOM Roundtable on the Promotion of Health Equity and the Elimination of Health Disparities, April 2010, Washington, DC.
Takeuchi D. T., N. Zane, S. Hong, D. H. Chae, F. Gong, G. C. Gee, E. Walton, S. Sue, and M. Alegria. 2007. Immigration-related factors and mental disorders among Asian Americans. American Journal of Public Health 97:84-90.
Turner, M. A., E. Godfrey, S. L. Ross, and R. R. Smith. 2003. Other things being equal: A paired testing study of discrimination in mortgage lending. Economics Working Papers, Paper 200309, digitalcommons.uconn.edu (accessed March 7, 2012).
Ver Ploeg, M., V. Breneman, T. Farrigan, K. Hamrick, D. Hopkins, P. Kaufman, B. H. Lin, M. Nord, T. Smith, R. Williams, K. Kinnson, C. Olander, A. Singh, and E. Tuckermanty. 2009. Access to Affordable Nutritious Food: Measuring and Understanding Food Deserts and Their Consequences. A Report to Congress. Washington, DC: U.S. Department of Agriculture.
Williams, D. R., H. M. Gonzalez, H. Neighbors, R. Nesse, J. M. Abelson, J. Sweetman, J. S. Jackson. 2007. Prevalence and distribution of major depressive disorder in African Americans, Caribbean blacks, and non-Hispanic whites: Results from the National Survey of American Life. Archives of General Psychiatry 64:305-315.
Woodward, C. V. 1955. The Strange Career of Jim Crow. New York: Oxford University Press.
Woolf, S. H., R. E. Johnson, G. E. Fryer, Jr., G. Rust, and D. Satcher. 2004. The health impact of resolving racial disparities: An analysis of U.S. mortality data. American Journal of Public Health 94:2078-2081.
Woolf, S. H., R. E. Johnson, R. L. Phillips, and M. Philipsen. 2007. Giving everyone the health of the educated: An examination of whether social change would save more lives than medical advances. American Journal of Public Health 97:679-683.
























