A panel of experts discussed the scope, applications, process, structure, and capacity issues faced in telehealth. This included an overview of the common challenges of telehealth, issues in licensure, the FCC Rural Health Care Support Programs, and issues with the misalignment of definitions of rural and how it is operationalized programmatically and financially within today’s health care system. The following sections reflect the individual speaker’s comments and reflections.
Jonathan Linkous, M.P.A.
American Telemedicine Association
When the ATA started in 1993, telemedicine largely consisted of hub and spoke networks based out of tertiary care or academic medical centers. Today it is a quite different picture. Every year in the United States, about 10 million patients receive telemedicine services. In most of those cases, the patients do not know that telemedicine is being used. This is a sign of success, but it is also a sign of how telemedicine has been absorbed into many health care networks. There are “seven deadly barriers” for telemedicine: money, regulations, hype, adoption, technology, evidence, and success. Some of these are shared with health care in general and some are new kinds of barriers that accompany the transformation of health care by telemedicine.
Money
Reimbursement is commonly cited as a major barrier for telemedicine. About 90 million people are in managed care systems, yet there is not much evidence about managed care organizations using telemedicine to control costs. Additionally, Medicare does not reimburse very much in the fee-for-service system, and that reimbursement is largely limited to nonmetropolitan areas, to certain institutions, and to certain current procedural terminology (CPT) codes. Many of these restrictions result from fears that telemedicine either will allow providers to abuse the health care system or will lead to overutilization and drive up costs. A lot of technology companies that are not fully informed about the health care market are getting involved in telemedicine because they see large financial opportunities. As a result, many technologies are being produced by people who are attracted to the potential market of health care without really understanding the applicability of telemedicine.
Regulations
Licensing was a minor issue when the ATA was formed, because most telemedicine systems operated within a single state. Today there are multistate systems with multistate practices. As most of the major health care providers move into a national system, licensure is becoming a bigger barrier. Practice regulations may be an even larger barrier than licensure, as many state medical boards require an in-person consultation before initiation of any telemedicine services. In fact, the American Medical Association recently proposed a resolution to the same effect, and federal legislation has also been proposed. Telemedicine also often encounters barriers with traditional regulatory agencies (e.g., the Food and Drug Administration [FDA], the FCC). Finally, another major barrier to the use of telemedicine is Section 1834(m) of the Social Security Act,1 which limits the use of telemedicine to certain providers.
Hype
We are victims of our own hype. We tend to talk about studies and all the wonderful things that telemedicine can do, but a lot of studies show that some applications of telemedicine do not work or cost too much. To move telemedicine forward, we have to be realistic about what works and what does not.
______________
1 Social Security Act, § 1834(m).
Adoption
Health care providers sometimes resist innovation in telemedicine because it creates competition. Individual providers may resist solutions to licensing barriers because they do not want competition from another state’s telemedicine network. This resistance is even greater with the development of nationwide networks.
Technology
Technology has been the focus of telemedicine for a long time. However, telemedicine is really about the services—where they can be provided and how they change people’s lives—and not about the uniqueness of the newest piece of technology. Additionally, the implementation of multiple technologies may create huge data flows that are not useful or easily maintained (e.g., continuous monitoring of temperature and blood pressure).
Evidence
Some applications of telemedicine show great progress, but other areas lack large studies, or require synthesis of existing studies to evaluate their value. For example, some large payers are ready to implement telemedicine, but more evidence is needed regarding cost savings.
Success
Telemedicine is becoming part of the business plan of many hospitals. Telemedicine is also moving into urban areas because that is where the people are. As a result, we need to think about what happens to the rural networks and rural populations. Telemedicine networks are expanding ICUs and capabilities for stroke care, but many of these are independent networks, and isolated from the traditional telemedicine networks. Are they competing or are they a part of it? Are independent teleradiology firms working with the hospital or are they competing? Finally, applications of mobile telehealth (mHealth) have a lot of potential, but may not be embraced by traditional health care providers.
Gary Capistrant, M.A.
American Telemedicine Association
Capistrant began with the premise that licensure should be more patient centered in order to address not just the mere license, but also some of the discrepancies and practice issues that vary from state to state. There are many issues related to professional licensure. First is that the population is incredibly mobile. Individuals travel across state lines on a daily basis, and telehealth facilitates the dissolution of the barriers of distance and geography.
Second is patient choice. Multistate health care systems let patients choose which providers they want to go to, no matter where they live. This is especially important for access to specialists. Twelve states have less than 2,000 specialists, and 11 states have less than 11 specialists per 10,000 population. Would it be right to limit individuals in those states just to the provider pools within their own states? Three states are on both of these lists: Idaho, Montana, and Wyoming. This is especially a problem for people with special needs, such as in the care of rare diseases (diseases that affect less than 200,000 Americans). What kind of access does somebody with one of those diseases have in rural or underserved areas? Where would you go if you needed a pediatric cardiologist who spoke Spanish or knew sign language?
A third issue is that the current system does not encourage provider productivity. In the short term, we cannot dramatically affect the number of health care providers, but we can do something about the productivity of their time and resources. Increasingly, multistate plans deliver health care, whether it is a managed care plan or an ACO, in order to provide more care options.
Licensure raises many other questions for telehealth. For state practice acts, is telemedicine sufficient to meet doctor-patient relationship requirements? When is a medical exam involved? What can you do with prescribing? Also, many Americans live along the 22,000 miles of state borders in this country, and the closest health care provider is in a different state. While many health care providers have multiple state licenses, this comes with a high cost. Reciprocity is one solution, but some states will not even allow for a physician to talk to another physician without being licensed in that other state. Some states have developed a telehealth license, but this is not a good long-term solution. Telehealth should not be separate; it is not a specialty of medicine.
Federal health care programs should not be hindered by state law in the same way the federal government has authority to deal with interstate com-
merce. The first article of the Constitution indicates that the states agreed to give Congress the power to regulate interstate commerce. Later, an amendment gave the states the authority to deal with intrastate commerce. This has been used to address exceptions for health care providers in federal agencies (e.g., DoD, VA) needing multiple state licenses. In December, Congress unanimously approved an expansion for the DoD that extends a license in one state to all other states (just as you need only one license to drive). That model is being used in another proposal for the VA, and could be used for other federal agencies, federal health programs (e.g., Medicare, Medicaid), and federally funded sites like community health centers.
Dale C. Alverson, M.D.
University of New Mexico
This country needs ubiquitous, adequate, affordable broadband to support telehealth and health information exchange in order to increase access to quality care for all individuals at the right place and the right time when it is needed. This can improve access to care, lead to better health outcomes, and reduce costs. Yet, significant gaps in access to broadband remain, particularly among rural and underserved populations. Access to broadband is also necessary for other community and individual needs in education and training, economic development, and government. Major public health issues impact rural communities and their economic development, in part due to a lack of access to health care services. Telehealth technologies play a major role in helping individuals and their health care providers to better manage health.
In 2010, the U.S. Government Accountability Office reported on the lack of good data on the impact of FCC programs (GAO, 2010). Millions of dollars have been invested in broadband, but its value needs to be demonstrated. The FCC has three rural health care programs that are managed by the Universal Services Administrative Company (USAC). First, the rural urban rate discount permits rural communities to only pay as much as the largest city in their area. Second is the Internet subsidy, which provides 25 percent of the cost of Internet. Third is the Rural Health Care Pilot Program (RHCPP) in which USAC provided coaches for the individually funded projects involved in the establishment of broadband health care networks.
In 2010, the FCC issued its National Broadband Plan (www.broadband.gov) that reviews the potential value of broadband-enabled health information technology (IT); provides an overview of the current health IT use in the United States; and issues recommendations such as better reimbursement, modern regulation, increased data capture and usage, and sufficient
connectivity. In July 2010, the FCC issued a notice of proposed rulemaking related to their rural health care programs. In July 2012, the FCC requested more input about how these programs might be improved.
Rural Health Care Pilot Program
The RHCPP was established by the FCC to help public and nonprofit health care providers deploy a state or regional dedicated broadband network, with the ultimate goal of creating a nationwide broadband network dedicated to health care. In 2007, the FCC initially announced 69 projects, for a total of $417 million, to be distributed over 3 years. To date, only 50 projects remain.
One such project, the Southwest Telehealth Access Grid, analyzed the strengths, weaknesses, opportunities, and threats of the RHCPP. Strengths include that it is a great idea to design, construct, and operate broadband to support telemedicine and health information exchange as a means to increase access to health care. Weaknesses mean the process did not work well—it was cumbersome, required two 1-year extensions, and several projects dropped out. Also, there is inadequate evaluation of the benefits, and there was poor coordination with other federal programs. Opportunities include the ability to improve and streamline the process to make it more user-friendly and timely. Finally, threats include incomplete implementation, persistent gaps in broadband coverage, inability to demonstrate the value of broadband, wasting of funds, and lack of sustainability.
Potential Next Steps
In order to advance broadband networks for health care, Alverson said that efforts in coordination, cooperation, and collaboration will be needed across multiple programs and initiatives. This includes federal programs, private initiatives, and international efforts. He suggested that one step in that direction could be the formation of a transdisciplinary advisory board that includes public- and private-sector representatives. In addition, he said, processes need to be streamlined and common network design is needed for state, regional, and national initiatives. Assessment is needed to determine and fill gaps in broadband connectivity. Finally, he asserted that the development and implementation of evaluation metrics is needed to promote the adoption and use of broadband, and to definitively demonstrate its value.
Steve Hirsch, M.S.L.S.
Health Resources and Services Administration
Many federal entities are involved in defining rural, including the U.S. Census Bureau, the Office of Management and Budget (OMB), the USDA’s Economic Research Service (ERS), and the Office of Rural Health within HRSA.
The Census Bureau
The U.S. Census Bureau has never defined rural; instead, it defines urban, and everything that is not urban is therefore rural. About a century ago, the U.S. Census Bureau defined urban as any incorporated place that had at least 2,500 people. Around 1950, recognizing that suburbs were growing up around cities, it expanded the definition to include suburbs, ignoring the borders of the incorporated places. The U.S. Census Bureau defines two kinds of urban areas: urbanized areas and urban clusters. Urbanized areas have a core population of at least 50,000 people, and urban clusters have a core population of 2,500 to 50,000 people. Generally, urbanized areas need a population density of at least 500 people per square mile, or fewer than one person per acre. However, this cutoff may therefore consider some suburban areas as non-urban, even though they are in close proximity to urban areas.
In 1900, the majority of the U.S. population lived in rural areas, but this has been steadily declining (see Figure 4-1). Census data show that between 2000 and 2010, most of the population growth in the United States was in urban areas. According to the 2010 Census, for the first time, less than 20 percent of the U.S. population resided in rural areas. The density of the entire U.S. population is about 87 people per square mile, but the density of the urban population is more than 2,500 people per square mile. More than 80 percent of the U.S. population lives on less than 5 percent of the total land area. However, about 60 million people still live in rural areas.
The Office of Management and Budget
The OMB defines core-based statistical areas based on the population of individual counties. Metropolitan statistical areas have a core urban area of at least 50,000 people, while micropolitan statistical areas have an urbanized core of at least 10,000 but fewer than 50,000 people. Like the U.S. Census Bureau, the OMB does not formally define rural. About 35 percent of U.S. counties are considered metropolitan, accounting for nearly 84 percent of the U.S. population. Ten percent of the U.S. population
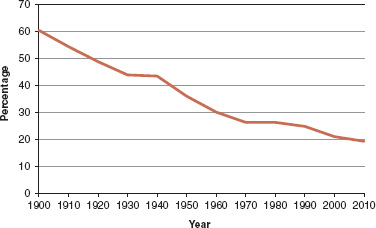
FIGURE 4-1 Rural percentage of U.S. population.
SOURCE: U.S. Census Bureau (2012).
resided in micropolitan counties, while just over 6 percent were in neither micropolitan nor metropolitan counties.
This consideration of whole counties facilitates distinction of metropolitan counties, micropolitan counties, and counties without an urbanized core. However, these definitions still create problems. For example, Coconino County in Arizona, which includes the Grand Canyon, is considered a metropolitan area because of the density of the population in the southern part of the county. Just as the U.S. Census Bureau’s definitions might lead to suburban areas being considered rural, OMB’s definitions include a lot of rural areas within the boundaries of a metropolitan county.
The Economic Research Service
To classify populations, ERS uses 9 Rural-Urban Continuum Codes (see Table 4-1) and 12 Urban Influence Codes (see Table 4-2) to divide both metropolitan and nonmetropolitan counties based on size or proximity to a metropolitan (metro) area.
Additionally, ORHP and ERS have worked together to develop rural-urban commuting area (RUCA) codes, which are based on subcounty units (see Table 4-3). This coding system takes functional relationships (e.g., commuting flows), population, and population density into account. A zip code approximation of these tracts was developed so that health care researchers can compare zip code data with its RUCA code to determine if that area is considered rural, micropolitan, or metropolitan.
TABLE 4-1 Rural-Urban Continuum Codes
|
|
|
| Code | Description |
|
|
|
| Metropolitan | Counties |
| 1 | Counties in metro areas of 1 million population or more |
| 2 | Counties in metro areas of 250,000 to 1 million population |
| 3 | Counties in metro areas of fewer than 250,000 population |
| Non-Metropolitan Counties | |
| 4 | Urban population of 20,000 or more, adjacent to a metro area |
| 5 | Urban population of 20,000 or more, not adjacent to a metro area |
| 6 | Urban population of 2,500 to 19,999, adjacent to a metro area |
| 7 | Urban population of 2,500 to 19,999, not adjacent to a metro area |
| 8 | Completely rural or less than 2,500 urban population, adjacent to a metro area |
| 9 | Completely rural or less than 2,500 urban population, not adjacent to a metro area |
|
|
|
| SOURCE: USDA (2012b). | |
TABLE 4-2 Urban Influence Codes
|
|
|
| Code | Description |
|
|
|
| Metropolitan Counties | |
| 1 | In large metro area of more than 1 million residents |
| 2 | In small metro area of less than 1 million residents |
| Non-Metropolitan Counties | |
| 3 | Micropolitan area adjacent to large metro area |
| 4 | Non-core adjacent to large metro area |
| 5 | Micropolitan area adjacent to small metro area |
| 6 | Non-core adjacent to small metro area and contains a town of at least 2,500 residents |
| 7 | Non-core adjacent to small metro area and does not contain a town of at least 2,500 residents |
| 8 | Micropolitan area not adjacent to a metro area |
| 9 | Non-core adjacent to micro area and contains a town of at least 2,500 residents |
| 10 | Non-core adjacent to micro area and does not contain a town of at least 2,500 residents |
| 11 | Non-core not adjacent to metro or micro area and contains a town of at least 2,500 residents |
| 12 | Non-core not adjacent to metro or micro area and does not contain a town of at least 2,500 residents |
|
|
|
| SOURCE: USDA (2012c). | |
TABLE 4-3 Rural-Urban Commuting Areas
|
|
||
| Code | Description | |
|
|
||
| 1 | Metropolitan area core: primary flow within an urbanized area | |
| 2 | Metropolitan area high commuting: primary flow 30% or more to an urbanized area | |
| 3 | Metropolitan area low commuting: primary flow 5% to 30% to an urbanized area | |
| 4 | Micropolitan area core: primary flow within a large urban cluster (10,000 to 49,999) | |
| 5 | Micropolitan high commuting: primary flow 30% or more to a large urban cluster | |
| 6 | Micropolitan low commuting: primary flow 10% to 30% to a large urban cluster | |
| 7 | Small town core: primary flow within a small urban cluster (2,500 to 9,999) | |
| 8 | Small town high commuting: primary flow 30% or more to a small urban cluster | |
| 9 | Small town low commuting: primary flow 10% to 29% to a small urban cluster | |
| 10 | Rural areas: primary flow to a tract outside an urbanized area or urban cluster | |
|
|
||
| SOURCE: USDA (2012a). | ||
Office of Rural Health Policy
ORHP defines all nonmetropolitan counties in the United States as rural. In addition, ORHP looks for RUCA tracts inside metropolitan counties. This adds up to about 60 million people being considered rural, which is near the U.S. Census Bureau’s estimation. ORHP also estimates that about 91 percent of the U.S. land area is rural; this is less than the estimation by the U.S. Census Bureau, and more than the estimation of the OMB. Finally, the ORHP has a new definition for frontier. Just like the RUCA codes, frontier has several categories, based on population and travel times to different sizes of urban areas.
Moderator: Spero M. Manson, Ph.D.
University of Colorado Denver
An open discussion followed the panelists’ presentations. Manson began the session by noting that we have invested in defining rural from a policy point of view, but that we might need to consider whether rural
may actually be a symbol for isolation. Thinking of food deserts2 within urban areas, he suggested thinking about isolated communities rather than rural versus urban. Next, he commented on the discontinuities among the different kinds of networks that have emerged nationally, regionally, and internationally, as well as the challenges of bringing them together. Finally, Manson noted that the idea of a driver’s license that works in every state is an interesting precedent for rethinking the notion of licensure at both the state and federal levels, adding that practice standards, scopes of practice, and other regulatory issues are increasingly polarizing stakeholders. Audience members were then able to give comments and ask questions of the panelists. The following sections summarize the discussion.
Defining Rural
One participant commented on the need to more accurately define rural, giving the example of San Bernardino County, which is 20,000 square miles and includes the Mojave Desert, yet is defined as metropolitan. Hirsch stated that rather than focusing on definitions of rural, more concentration should be placed on the broadband coverage necessary to serve all individuals. Hirsch added that no definition is perfect, and asserted that the ORHP’s current definition works well. He added that the new definition of frontier will be especially helpful for identifying areas that are truly isolated and need greater help in connecting to health care. The participant further remarked on the need to address limitations on reimbursement solely to rural areas, as it impedes the ability of telehealth to reach all underserved populations. Capistrant agreed that geographic location should be irrelevant in health care, and these provisions need to be removed in both Medicare and Medicaid. He further noted that limitations of coverage may prevent an area from having an adequate population base on which to create a sustainable telehealth network.
Alternative Providers
One participant mentioned that the ACA promotes the use of new and different types of health care providers that may be lower cost, more efficacious, and particularly amenable to telehealth. She further noted Section 2706, a nondiscrimination section of the law. Capistrant agreed this is one of many solutions to licensure and productivity issues.
______________
2 Food deserts are “low-income census tracts with a substantial number or share of residents with low levels of access to retail outlets selling healthy and affordable foods” (Ver Ploeg et al., 2011, p. 46).
The Potential of Telehealth
Alverson stated that telemedicine will have an important role navigating a combination of major issues: the ACA remains very controversial, there is an economic downturn, the current health care system is not sustainable, care demand is on the rise, the population is aging, and there is a significant shortage of health care providers of all kinds. Alverson also stated that telehealth will enable the integration of all types of health care, including behavioral health.
One participant commented that telemedicine will likely be driven by vendors or big businesses. Alverson commented that telehealth has to be driven by needs. He noted that his home state works collaboratively with communities (including health care providers) to address what the community itself sees as the most important health needs. He further described New Mexico’s Health Extension Rural Offices, patterned after the agricultural rural offices that help farmers understand best practices, to look at best local practices in health care.
Another participant asked about the use of Geospatial Informational Systems mapping to look at smaller communities. Alverson stated this will be important for a variety of public health issues (e.g., pandemic flu, seeing where patients with diabetes reside) in order to redirect resources. Linkous commented that as systems are consolidated and networks are broadened, the number of independent rural health providers will be likely to decline, and that technology will be critical to link in health care providers in rural areas to the other parts of the network.
Payment
Linkous suggested that some providers embrace telehealth because they can see more patients in the same amount of time, yet want to be paid at the same rate as in-person care. He said that because of these efficiencies, perhaps the payment rate should not be the same as in-person care, but noted the issue is extremely sensitive. Physician payment might be the most important challenge in telehealth, even more than licensure, Linkous asserted. Another participant mentioned that a recent IOM study on geographic payment adjustment for Medicare payment called for changes in payment policy on telehealth. She added that the committee saw the availability of telehealth as a matter of equity of access to care, and also that the committee made recommendations on scope of practice, seeing that as a matter of efficiency and access for Medicare beneficiaries.
Federal Communications Commission
One participant commented that the FCC Rural Health Pilot was “an absolute mess.” Another participant working for the FCC urged participants to file comments in line with the recent public notice. She added that when the notice of proposed rulemaking was issued in 2010, many of the pilot projects were not fully off the ground, and now have more questions. She further added that there is a strong commitment to reform of the programs. Alverson said that everyone needs to work collaboratively toward realistic solutions and shared goals, and that the FCC plays a huge role in achieving adequate broadband connectivity in this country.
Levels of Evidence
One participant related the story of a study that aimed to look at both clinical and the financial benefits of home telemonitoring for elderly congestive heart failure patients. She noted that the randomized controlled trial (RCT) was difficult because of delays in institutional review board approval. Furthermore, many patients would not enroll because they knew about home telemonitoring, and did not want to risk being in the control arm and not receive the technology. When she asked what level of evidence is necessary to speed up the adoption of telehealth technologies, Linkous recommended focusing on cost savings instead of patient satisfaction surveys.














