4
Individual, Household, and
Environmental Factors Affecting
Food Choices and Access
Chapter 3 presented the evidence on relationships between participation in the Supplemental Nutrition Assistance Program (SNAP) and the potential for participants to achieve the program goals of improving food security and access to a healthy diet. This chapter presents evidence on individual, household, and environmental factors that affect food purchasing and consumption decisions and their impact on food choices and access and ultimately on the adequacy of SNAP allotments for achieving those goals. First, however, the chapter describes household food production theory as a framework for the discussion of these factors. After a brief review of the data and analytical challenges to research designed to broaden understanding of the issues facing SNAP participants, the final section presents a summary of findings and conclusions.
It should be noted that, in evaluating the available evidence, the committee determined it would be most useful to examine research questions with a focus on observational studies. This is because randomized controlled trials are infrequent among the types of studies considered. Much of the observational evidence available was cross-sectional, and the findings from these studies were considered in the context of the total available evidence, including that from both observational and experimental studies. All studies reviewed were evaluated by content area, study design, and publication source. Although they were not given equal weight with peer-reviewed publications, some publications from nongovernmental organizations and stakeholder groups also were considered because of the additional insight they provided into the behavioral aspects of participation in nutrition assistance
programs. The committee’s literature search strategy is described in Appendix D.
HOUSEHOLD PRODUCTION THEORY AS
AN ORGANIZING FRAMEWORK
Consumers choose foods for consumption within the context of their own and their household’s preferences and available resources. According to basic economic theory, households purchase foods and other market goods to maximize utility, or well-being, based on their preferences and subject to the constraint that the cost of those goods is less than or equal to the sum of all sources of income. However, households are subject not only to an income constraint but also a time constraint. Thus, according to household production theory, households combine time and market goods to produce commodities for consumption in the household (Becker, 1965). In the context of food choices, food consumption requires not only money expenditures for purchasing food but also time expenditures for purchasing, preparing, and consuming food and for cleaning up after preparation and consumption. Therefore, the full price of consumption is the sum of the direct and indirect prices for food, where the direct price is the purchase cost, and the indirect price is the value of the time requirements (Becker, 1965). The Becker model and its extensions help identify the types of individual and household factors that may be relevant in defining the adequacy of SNAP allotments. Furthermore, in the context of SNAP, the allotment is another source of “income” to the household that can be used to purchase food and may free up resources for the purchase of other types of market goods.
A complication of household production theory as it applies to the production of commodities that require both market goods and time is that a household’s “technology” determines behavior in addition to its preferences (Pollak, 2011). A household’s technology could relate to human capital (e.g., food preparation knowledge) or physical capital (e.g., kitchen equipment). Furthermore, it could relate to the form of the production function transforming ingredients into foods for consumption, such as whether there are economies of scale in food production. Economies of scale relate to the fact that as household size increases, the incremental money and time expenditures for each individual are reduced because meals are prepared jointly, so the resources for acquiring, preparing, and serving are spread over more individuals. These economies of scale factor into the allocation of SNAP benefits based on household size.
Recent research has investigated the trade-off between money expenditure and time expenditure in food production. These studies have found that low-income individuals and households, like those at higher income
levels, are time-constrained for meal preparation. A household needs both sufficient money and sufficient time to prepare healthy meals (Davis and You, 2011). The amount of time individuals spend preparing food for consumption in the household is affected by household and individual factors such as earnings; labor force participation; the number of children in the household; and sociodemographic characteristics such as education, ethnicity, and gender (Mancino and Newman, 2007). Having multiple jobs, inflexible hours, and night work, for example, is associated with limited time for choosing and preparing healthy foods (Devine et al., 2003). In addition, environmental factors such as region of the country and whether an individual lives in a metropolitan area affect food consumption decisions (Mancino and Newman, 2007). Using data from the 2003-2004 American Time Use Survey (ATUS), which is administered by the Bureau of Labor Statistics, Mancino and Newman (2007) found that household time resources have a greater effect than an individual’s earnings or household income on how much time is allocated to preparing foods. As described further in the next section, households in which women work full-time or are the single head of household have fewer time resources.
In summary, multiple factors affect a household’s ability to transform foods available for purchase into foods that can be consumed. With the exception of foods purchased in prepared form, for example, one or more individuals within the household must have the necessary knowledge and physical ability to prepare foods from ingredients and sufficient time available for all the activities involved in food preparation; moreover, the household must have the necessary equipment to refrigerate, prepare, and cook foods. In addition, food knowledge and choices are strongly influenced by social and cultural preferences of individuals and households. Furthermore, environmental factors affect the types of foods available for purchase, the cost of those foods, and the means of transportation (a personal vehicle, a social network, or public transportation) that can be used to acquire the foods. Thus, the broader context of the theory of household production must address the various factors that influence the theory’s application to actual food choices.
INDIVIDUAL AND HOUSEHOLD FACTORS
This section describes individual and household factors affecting the adequacy of SNAP allotments: food choices; the time available for food purchasing and preparation; knowledge, skills, and abilities related to food preparation; and the availability of personal, nonpublic transportation for individuals and households. Implicitly, SNAP allotments are based on assumptions about these factors, and departures from these assumptions for individual participants may affect their ability to purchase healthy foods with their SNAP benefits.
Definition of the adequacy of SNAP allotments for achieving the program goals is closely linked to food choices. As illustrated by the Food Choice Process Model (Sobal and Bisogni, 2009), food choices are strongly influenced by events and experiences beginning early in life and continuing throughout the life course. The following discussion focuses on components of this model that are potentially related to the ability of SNAP participants to achieve the program goals: taste preferences, personal and social factors, employment status, acculturation, and access to personal transportation (which is also considered later in this section as a potential constraint on the access of SNAP participants to healthy foods).
Taste Preferences
Taste preferences often are cited as a primary motivator of individuals’ food choices (Drewnowski, 1997; Drewnowski and Levine, 2003; Drewnowski et al., 1999). While preferences for sweet and salty flavor appears to be innate, other preferences are clearly influenced by early exposure. Evidence reviewed by the committee included both social and environmental factors that can influence taste preferences. A review of research on taste preferences includes evidence that foods eaten by a woman during pregnancy and lactation can influence the infant’s early flavor experience (Birch, 1999). It is not clear, however, that such exposure has a lasting impact on the infant’s subsequent taste preferences, given the number of social and environmental factors that can influence the development of those preferences during infancy and childhood (Birch, 1999; Devine et al., 1999).
Personal and Social Factors
Food deprivation and irregular availability of food during childhood have been found to contribute to the development of poor eating behaviors (e.g., overeating and binging and having an emotional attachment to food), as well as to less healthful food choices in general. Olson and colleagues (2007) propose early food deprivation in childhood and associated attitudes and behaviors toward food as a possible mechanism for the association between childhood poverty and adult obesity.
Food choices also are influenced by personal and cultural ideals, constrained by resources and present contexts. Family structure, including single head of household versus married/partnered heads of household, the presence of children, the health of family members, and the roles of each family member in food choices all influence the household’s ability to be food secure and have access to a healthy diet (Devine et al., 1999; Evans
et al., 2011; Wiig and Smith, 2009; Wiig Dammann and Smith, 2009). For example, children and other family members may influence the food decisions of the individual(s) procuring and preparing food to the detriment of the bottom-line cost, as well as the nutritional quality of what is purchased. As financial resources and consequent food security decline, low-income populations increasingly focus on price and quantity instead of preference and quality (Dachner et al., 2010; Wiig Dammann and Smith, 2009). They make use of a variety of family and community resources (Mammen et al., 2009), even resorting to strategies such as attending events where food is offered (e.g., church events), selling or pawning items, and eating discarded and out-of-date foods (Kempson et al., 2003). Specific strategies that impact nutritional quality include giving priority to meat above other foods; limiting fruits and vegetables because of cost and the short shelf life of fresh produce, combined with poorer flavor acceptance of canned varieties; limiting milk because of cost; and consuming more filling starches (Wiig and Smith, 2009). On the other hand, several qualitative studies of low-income women have found that having children has a positive influence on the mothers’ consumption of a nutritious diet, such as consuming more fruits and vegetables (Dubowitz et al., 2007), and on their motivation to improve the nutritional quality of their families’ diets even though they are constrained by cost and family members’ preferences (Evans et al., 2011). Recently, however, Laroche and colleagues (2012) analyzed data from the Coronary Artery Risk Development in Young Adults study to examine whether the percentages of saturated fat and energy intake and the daily intake levels for fruits and vegetables changed when children were present in the home. This longitudinal study of more than 2,500 adults found no relationship between becoming a parent and changes in the household’s eating habits, regardless of employment status.
Employment Status
Work life can influence food choices in several different ways. Qualitative and quantitative research by Devine and colleagues (2003, 2009) examining the “spillover” of work into food choices among low- and moderate-wage workers revealed that long hours, inflexible schedules, shift work, and multiple jobs have an impact on the time and energy available for food procurement and preparation. Strategies used by workers for acquiring food under these conditions involved compromises viewed as unsatisfactory for maintaining a healthy diet, such as skipping meals, eating take-out meals, eating away from home, and limiting time to meet family needs and skipping family meals. Those who reported managing well had flexible work schedules, support from others for family responsibilities, and personal resources that included planning and cooking skills. The results
of these studies were confirmed in a much larger cross-sectional study of a population of more than 3,700 diverse parents of adolescents participating in Project F-Eat (Bauer et al., 2012). Full-time working mothers reported spending less time in meal preparation, preparing fewer family meals, and consuming fewer fruits and vegetables. When work-life stress was higher, the outcome was a less healthful food environment overall, exemplified by even fewer family meals and more frequent consumption of fast foods and sugar-sweetened beverages. These effects did not differ between mothers and fathers.
Acculturation
Acculturation among immigrant populations has been shown to be associated with changes in both diet quality and food security (Mazur et al., 2003). Most of this research has been in Latino populations, which have disproportionately high levels of food insecurity (Coleman-Jensen et al., 2012) and in which acculturation among youth appears in part to increase the negative effects of poverty on childrens’ diet quality (Mazur et al., 2003).
In a recent study of the impact of acculturation on food security, Dhokarh and colleagues (2011) retrospectively analyzed respondents to the 1998-1999 Acculturation and Nutrition Needs Assessment survey of low-income Puerto Rican households to examine the impact of acculturation and social capital indicators on nutrition and health outcomes. The analysis focused on a convenience sample of women (N = 200) with young children in the Hartford, Connecticut, area who were either SNAP participants or SNAP-eligible. Among study participants surveyed, 76 percent were found to be food insecure. A bivariate analysis found positive associations between food insecurity and being unemployed, not owning a car, having older children, speaking Spanish only, planning to return to Puerto Rico, not attending Latino church or cultural events, receiving SNAP benefits that did not last the entire month, and accessing emergency food assistance. Likewise, a multivariate analysis showed positive associations between being unemployed, single, born in the United States, speaking Spanish only, planning to return to Puerto Rico, not attending Latino church or cultural events, and having SNAP benefits that did not last the entire month. These results illustrate the complexity of the relationship between acculturation and food insecurity in this Latino population. Another cross-sectional study, also in Hartford, examined the differences between low-income pregnant women who were Puerto Rican (N = 243) or non–Puerto Rican Latinas. The Puerto Rican women were more acculturated than the other Latinas and had diets that were higher in fat and sugar and lower in vegetables (Hromi-Fiedler et al., 2012). The presence of acculturation covaried with ethnicity so could not be assessed separately.
A qualitative focus-group study of Special Supplemental Nurition Program for Women, Infants, and Children (WIC)–eligible women who were mothers of infants and were either first-generation immigrants or U.S.-born found differences in attitudes related to food procurement and preparation (Dubowitz et al., 2007). Although there were similarities between the two groups, including time and money constraints on food choices, those born in the United States were more likely to buy prepared foods, including fast foods, and were less likely to travel to shop for foods they wanted. No difference was found in levels of food security, with both groups being marginally food insecure.
As with Latina populations, lack of acculturation was found to be related to food insecurity among mothers with young children who were refugees from Liberia in West Africa (Hadley et al., 2007). In a mixed methods study (15 qualitative interviews followed by a survey of 101 women), food insecurity was higher, at 73 percent, among those who had been in the United States only 1 year than among those who had resided in the United States for 3 years, at 33 percent. Food insecurity generally was negatively associated with measures of acculturation, including perceived difficulty in understanding the language and time in the United States (p < 0.05).
Access to Personal Transportation
One additional factor influencing food choice is the availability of personal, nonpublic transportation. Households without a personal vehicle or access to public transportation must rely on alternative means—walking or biking to a store close at hand or social networks (family, friends, neighbors) that provide reliable transport. People with disabilities are particularly at risk, often completely dependent on social networks for access to food. For example, an in-depth qualitative study of food access among 28 low-income rural, village, and inner-city families with disabled primary grocery shoppers found that they relied on social networks for assistance with food shopping (Webber et al., 2007). An unexpected finding in this study was that nearly half of the participants had a variety of health conditions and disabilities that limited their access to food, in particular, healthy, affordable food.
Time
Purchasing and preparing a healthy diet can be a time-intensive process for households that do not use commercially prepared foods. Producing healthy meals requires a number of activities, skills, and resources that include planning, transportation to and from a grocery store or other food outlet, shopping, preparation, and cleanup. Thus, time involving food preparation is particularly relevant to defining the adequacy of
SNAP allotments. The committee identified several studies that found a disconnect between the assumptions of the Thrifty Food Plan (TFP), which is used as the basis for the SNAP maximum benefit, and in turn for SNAP allotments, and resource constraints among low-income households. The TFP market baskets take into account the types and quantities of nutritious foods that can be purchased with the maximum SNAP benefit, but they do not consider time required for food preparation. Davis and You (2010, 2011) analyzed the money and time requirements associated with the TFP. They matched ATUS data with the Food Security Supplement to create a dataset providing total weekly food expenditures and daily time allocations, along with household composition information, for approximately 6,300 single-headed households. They found mean expenditures for food of $107.37 per week and a total amount of time involved in food production of about 4.41 hours per week. Applying a mean price of time of $10.48 per hour, the total mean money-time requirements can be estimated at an average of $178 per week. Thus while actual monetary expenditures are 35 percent greater than required to meet the TFP target, actual expenditures accounting for the cost of time are 40 percent less than the TFP target. Across households in the dataset, 62 percent spent enough to meet the TFP target when only money costs were considered, but just 13 percent did so when time costs were included in the cost calculation.
The TFP provides the potential for an adequate diet and makes allowance for including some commercially prepared foods (Carlson et al., 2007). However, using the Center for Nutrition Policy and Promotion (CNPP) publication Recipes and Tips for Healthy, Thrifty Meals (CNPP, 2000), which provides 2 weeks’ worth of meals with recipes and preparation times, the average estimated time requirement is 16.1 hours per week or 2.3 hours per day (Davis and You, 2010; Rose, 2007). In their study, Davis and You (2010) included a sensitivity analysis of 8 hours per week to account for different food choices and recipe combinations, consistent with the Economic Research Service (ERS) publication Who Has Time to Cook?, which reports that 13-16 hours per week is required for food preparation (Mancino and Newman, 2007).
Household factors also impact the time available for food preparation. Low-income households with either two adults or a single-parent head of household working less than 35 hours per week reported allocating enough time for food preparation to meet the TFP target. However, low-income women working full-time spent too little time in food preparation to meet the TFP’s implied requirement of at least 80 minutes per day (Mancino and Newman, 2007).
The time required for each step in the procurement and preparation of food is also affected by household factors and resources, such as the availability of public transportation or ownership of a vehicle; access to food
outlets carrying a variety of healthful foods; the availability of household equipment with which to store (e.g., refrigerator or freezer) and prepare (e.g., range and oven) food; and the knowledge and skills to plan, choose, and prepare foods that meet dietary needs within budgetary limits. While limited data exist on the time costs of this entire process, it is clear that a money-time trade-off is entailed in the preparation step, with convenience foods that are wholly or partially preprepared having a higher monetary cost than foods prepared largely from basic unprocessed ingredients—i.e., from “scratch,”—that require more preparation time (Mancino and Newman, 2007). Available time resources thus affect the choices between commercially prepared and home-prepared foods and potentially the nutritional quality of the diet as well (Beshara et al., 2010; Devine et al., 2003, 2009; Jabs and Devine, 2006). In addition to the general shift to more women in the workforce, Rose (2007) points to several government policies that have specifically promoted employment among low-income women over the last two decades, such as increases in the earned income tax credit. This trend, as well as the increasing number of single-parent households among SNAP participants, has altered the allocation of time resources, decreasing the amount available to spend on food preparation (Mancino and Newman, 2007).
Time use surveys conducted between 1965 and 2000 show a decrease in time spent in food preparation, with less time for working than nonworking women: 4.5 versus 7.9 hours per week, respectively. Nonworking women in food secure households responding to the 1996-1997 National Food Stamp Program Survey reported significantly greater time expenditures relative to this latter figure, an average of 13.9 hours per week (Rose, 2007). In the 2003-2004 ATUS, women working full-time in households at 130 percent or less of the federal poverty level reported 5.41 hours per week spent in food preparation and cleanup, compared with 8.2 hours per week for those not working (Mancino and Newman, 2007). Regression models pointed to certain individual and household characteristics that partially explained women’s time reported for food preparation and cleanup: having a partner, the number of children in the household, and age were positively associated, whereas having unhealthy adults in the household was negatively associated. Low-income men reported spending less time than women, and low-income men who were not working reported spending twice as much time as men working full-time—3.0 versus 1.5 hours per week, respectively. Having a household partner or a young child was positively associated with time men dedicated to food preparation. Estimating direct food costs and monetizing time costs using the USDA Food Security Supplement and the
____________________
1To compare across studies, Mancino and Newman (2007) used data in minutes per day that were then converted to hours per week (m/d × 7 d/60 m).
ATUS for 2004 and 2005, time was found to be more constraining than money, with time costs adding about 35 percent to total food costs (Davis and You, 2011). Thus, if labor costs are not included, the real cost of food for low-income households is severely underestimated.
Knowledge, Skills, and Abilities
According to the 2010 Dietary Guidelines for Americans (DGA), very few Americans consume diets that meet the DGA recommendations (USDA and HHS, 2010). The complexity of the food and information environments makes it difficult for all consumers to improve their dietary patterns. Contento (2007) makes the case that this complexity calls for nutrition education to give individuals the knowledge and skills necessary to navigate these environments in a way that results in healthful food choices. SNAP participants need to be especially skillful in making choices within the constraints of available resources so they can maximize the purchasing power of their SNAP benefits.
The committee found limited research directly documenting a lack of nutrition and resource management knowledge and skills among low-income populations generally, or among SNAP participants specifically. One cross-sectional study, by Gleason and colleagues (2000), investigated knowledge and attitudes, but not skills. This study, using data from the 1994-1996 Continuing Survey of Food Intakes by Individuals and the Diet and Health Knowledge Survey, found that among adults, factual knowledge about the health consequences of specific dietary practices and which practices are most healthful was lower among low-income (<130 percent of the poverty level) (N = 1,464) than higher-income (N = 4,194) respondents. In addition, no significant differences in knowledge were found between SNAP participants (N = 435) and nonparticipants (N = 1,029). Low-income participants believed that eating a healthy diet (rich in fruits and vegetables, limited in fat and cholesterol) was important, but this belief did not translate into confidence that they were making healthful choices, suggesting a possible lack of the skills needed to translate nutrition knowledge into practice. SNAP participants reported even lower confidence than low-income nonparticipants in the healthfulness of their choices. In regression analyses, knowledge and attitudes did not mediate the relationship between SNAP participation and dietary intake. The food resource management skills of planning, shopping, and preparation are recognized as necessary to translate knowledge into practice (Contento, 2007). However, the study by Gleason and colleagues (2000) did not investigate resource management knowledge and skills and how they would impact dietary intake and food security in the context of resource constraints. The authors do conclude that their study provides “circumstantial
evidence that there is a role for increasing nutrition education and promotion among participants” (p. 155).
In addition to knowledge, several studies point to the effect of perceptions of time pressure or self-efficacy as related to meal preparation, factors that are at least somewhat modifiable by nutrition education. For example, a random digit dial survey (N = 458) of meal preparers found a negative effect on diet quality of respondents’ perceptions of time pressure as related to meal preparation that was moderated by self-reported knowledge of nutrition, along with years of formal education and perceptions of health risk (Mothersbaugh et al., 1993). More recently, Beshara and colleagues (2010) investigated the effects of perceived time pressure and other related variables on the healthiness of meals served over a 7-day period to school-aged children in Australia. Among the 120 mothers surveyed, no significant relationship was found between perceived time pressure and healthiness of meals. The study did find, however, that mothers’ self-confidence in their ability to prepare healthy meals was predictive of dietary quality. The authors point to social cognitive theory (Contento, 2007), which provides a theoretical basis for much of the community-based nutrition education provided to low-income audiences.
Federally Funded Nutrition Education
USDA provides funding for several programs focused on improving nutrition knowledge and skills either as the sole purpose (e.g., the Expanded Food and Nutrition Education Program [EFNEP]) or in conjunction with nutrition assistance programs (e.g., SNAP-Education [SNAP-Ed]). Both of these educational initiatives (described in Box 4-1) aim to enhance participants’ ability to meet the recommendations of the DGA. Both use theory-guided interventions that take into account participants’ existing strengths and emphasize building skills for resource management through planning meals and shopping wisely so as to use both nutrition assistance program benefits and cash to make healthy food choices (FNS, 2012; NIFA, 2009a). Food preparation skills are included to teach participants how to provide food with less reliance on more expensive convenience and fast foods.
More evaluation studies have been done of EFNEP than of SNAP-Ed, partly because EFNEP is an older program, beginning nationally in 1969, 20 years before the establishment of SNAP-Ed. Studies evaluating the effectiveness of EFNEP can be applied to assessments of SNAP-Ed for several reasons: The target populations are similar; the objectives are similar; and EFNEP is delivered solely through the Land Grant University Cooperative Extension System, the same system that delivers the largest number of SNAP-Ed programs across the country, generally using the same curricula and approaches (NIFA, 2009b).
BOX 4-1
SNAP-Related Federally Sponsored
Nutrition Education Programs
Expanded Food and Nutrition Education Program
The Expanded Food and Nutrition Education Program (EFNEP), sponsored by U.S. Department of Agriculture and delivered through the Land Grant University Cooperative Extension System, is a program designed to help those with limited resources acquire the knowledge, skills, attitudes, and behaviors needed to develop and improve the diet and nutritional well-being of themselves and their families. As a component of the program, participants learn how to make food choices to improve the nutritional quality of the meals they serve; how to increase their ability to select and buy food that meets the nutritional needs of their family; how to gain new skills in food production, preparation, storage, safety, and sanitation; and how to better manage their food budgets and related resources.
SNAP-Ed
The Supplemental Nutrition Assistance Program-Education (SNAP-Ed) is a federal-state partnership program, sponsored by USDA, that supports nutrition education for SNAP participants. It provides educational programs and social marketing campaigns to increase the likelihood that participants will make healthier food choices within their budget constraints and will choose active lifestyle habits consistent with the recommendations of the Dietary Guidelines for Americans.
EFNEP has an evaluation system that has allowed for evaluation of the national program (NIFA, 2012) and has been recognized by the Government Accountability Office (GAO) for its ability to show how program goals are met (GAO, 2004). Outcome data resulting from ongoing evaluation, as well as research studies over time, have shown positive changes in nutrition practices and improvements in food security among graduates of EFNEP. Studies of the program’s effects include randomized controlled trials (e.g., Burney and Haughton, 2002; Cason and Logan, 2006; Townsend et al., 2006), quasi-experimental studies (e.g., Cason et al., 2005; Cox et al., 2003; Del Tredici et al., 1988) and observational studies (Arnold and Sobal, 2000; Bergman, 1997; Dickin et al., 2005; Dollahite et al., 2003, 2008). Researchers and educators also report positive changes as a result of participation in SNAP-Ed through randomized controlled trials (e.g., Eicher-Miller et al., 2009; Foster et al., 2008; Keihner et al., 2011), quasi-experimental studies (e.g., Backman et al., 2011; Gabor et al., 2012; Joy et al., 1999), and observational studies (Bell et al., 2006; Ellis et al., 2005; e.g., Hersey et al., 2001). Nevertheless, government reports have indicated that the process of evaluating SNAP-Ed needs improvement (GAO, 2004; Guthrie et al., 2006).
Nutrition education interventions, such as those delivered through SNAP-Ed, vary dramatically in terms of participants’ age, gender, and cultural background and the contextual factors that impact participants’ ability to both engage in and benefit from the interventions. In addition, interventions differ greatly in the specific behavioral objectives targeted, the educational dose administered, and the approach employed (e.g., direct education with and without changes in the surrounding food and activity environment; whether the intervention is delivered by professional nutritionists or trained paraprofessionals), thus making an overall assessment of the effectiveness of nutrition education challenging. Moreover, while each of the studies cited above reports at least some positive results of these interventions, each has weaknesses in study design and/or assessment of outcomes. For example, the intensity of interventions studied varies dramatically, and the committee found no studies assessing the educational dose needed to elicit positive outcomes.
Only one study (Arnold and Sobal, 2000) included longitudinal data to assess the retention of behavior change over time—in this case, 1 year postintervention—but this was an observational study with no control group, and data were collected by the staff providing the nutrition education. Only two studies included biological measures, with both showing significant improvements with education. The first was an intensive school-based intervention (kindergarten through eighth grade) that included 50 hours of classroom nutrition education plus changes in school food policy, social marketing, and parent outreach (Foster et al., 2008). At the end of 2 years, the incidence of overweight in children in the intervention schools was significantly lower than that in the control schools. A second study found a significantly lower incidence of low birth weight among the population receiving nutrition education, but outcomes were compared with the local population as a whole rather than with a control group (Bergman, 1997). All other studies assessed the impact of the interventions through self-reports, with few including measures of convergent validity, such as consistency between reported behavior and dietary recall data; among those that did report multiple outcome assessments, results were consistent in some (e.g., Burney and Haughton, 2002; Keihner et al., 2011) and inconsistent in others (e.g., Arnold and Sobal, 2000). In addition, mediators and moderators of behavior change have infrequently been reported.
The report of Wave 1 of a Food and Nutrition Service (FNS) independent impact evaluation of four SNAP-Ed demonstration projects—three focused on children and one on women—was recently released (Gabor et al., 2012). No statistically significant impacts were seen across the projects for the common primary outcome variable of increased average daily fruit and vegetable consumption, although one project resulted in significantly
increased at-home intakes of vegetables among children. In addition, a number of secondary outcomes that varied by project were significantly better with education; for example, children were more willing to try fruits and vegetables and more likely to initiate eating vegetables as snacks.
In summary, the available data indicate that nutrition education has some positive impacts on food choices and food security. However, the body of evidence has limitations and is missing key components for understanding what is necessary to provide cost-effective nutrition education.
Availability of Food Preparation and Storage Equipment
The committee reviewed evidence on the impact of having the food storage and preparation equipment and appliances needed to prepare a healthy diet that could be purchased with SNAP benefits, consistent with the assumptions of the TFP. The committee found a paucity of research studies measuring the impact of a lack of food storage and cooking equipment in homes on the ability to prepare healthy meals. In a study of housing quality among 186 Latino farm-worker families in six North Carolina counties, Gentry and colleagues (2007) found that many lacked functional appliances, including ovens (27 percent), refrigerators (8 percent), and stoves (5 percent). By contrast, in a study of SNAP applicants in three Oklahoma counties (rural, suburban, and urban), Landers and Shults (2008) found that more than 97 percent of homes surveyed had adequate equipment for cooking. One additional study examined the ability of homeless families living in temporary housing with limited or no cooking and storage equipment to prepare healthy meals (Landers and Shults, 2008). The study found that not having adequate food preparation equipment resulted in the families resorting to consuming more unhealthy foods, such as sweetened beverages, candy, cookies, and chips.
Access to Personal, Nonpublic Transportation
Access to transportation was discussed above as a factor to consider for its impact on individual food choice decisions. Personal transportation is considered here as an individual/household factor that could have an impact on the purchasing power of SNAP allotments by constraining the ability of SNAP participants to access healthy foods.
A 2009 report to Congress by USDA indicates that 23.5 million Americans were living in low-income areas that were also more than 1 mile from a supermarket or large grocery store (Ver Ploeg et al., 2009). Based on this evidence, the committee examined the impact of individuals’ or households’ access to a personal vehicle or to a reliable vehicle as a factor in the feasibility of defining the adequacy of SNAP allotments. The committee identified
a number of studies examining whether a lack of transportation is a significant barrier to access to supermarkets or large grocery stores that provide a range of healthy foods. The committee also examined evidence on whether access to personal transportation is modified by race/ethnicity, age, medical conditions, and other factors affecting low-income populations.
In one of the most comprehensive reviews of U.S. studies on neighborhood disparities in food access, Larson and colleagues (2009) found that neighborhood residents with better access to supermarkets and limited access to convenience stores tend to have healthier diets and reduced risk for obesity. On the other hand, those residing in “food deserts”2—especially those without transportation—may be limited to shopping at small neighborhood convenience and corner stores, where fresh produce, low-fat food items, and other healthy foods are often limited and of poor quality (Andreyeva et al., 2008). In a study of focus groups of low-income women in Minneapolis who were predominantly SNAP users, Wiig and Smith (2009) found that store accessibility was a major factor in shopping frequency because many households did not own a vehicle.
Feather (2003) assessed the impact of changes in store access policies on SNAP recipients. His modeling of price, selection, quality, and accessibility costs revealed that, depending on transportation and store proximity, increased access to a new grocery store resulted in a monthly gain of $2.78 to $7.76 per SNAP participant. Rose and Richards (2004) conducted a secondary analysis of a nationally representative sample of households participating in the Food Stamp Program using data from the 1996-1997 National Food Stamp Program Survey. The study analyzed distance to store, travel time to store, ownership of a car, and difficulty of supermarket access as variables associated with the household’s use of fruits and vegetables. Most households surveyed (76 percent) had easy access to a supermarket, even though the majority of households did not own a car. Among survey participants who lived more than 5 miles from their principal food store, however, fruit consumption was significantly below that of those who lived within a mile of their principal store.
Laraia and colleagues (2004) investigated the association between distance to the closest supermarket and a composite measure of diet among pregnant women. While they do not specifically mention study participants’ lack of personal transportation, their findings suggest that a woman’s food environment, as measured by distance to supermarkets, grocery stores, and
____________________
2The concept of a “food desert,” defined by USDA as “low-income urban areas that are more than one mile from a supermarket and low-income rural areas that are more than ten miles from a supermarket” (ERS, 2012), lacks a consistent definition in the broader literature. Some define it by the quality of available foods, while others define it as the quantity of available foods. There is no consensus on the best or most appropriate definition, nor is there agreement on the existence of food deserts (Bitler and Haider, 2011).
convenience stores, directly influences diet quality during pregnancy. Living more than 4 miles from the closest supermarket is most strongly associated with poor diet quality, even after controlling for individual socioeconomic characteristics and the availability of grocery and convenience stores.
In a study of Latino neighborhoods in upstate New York, Lopez-Class and Hosler (2010) found that the lack of supermarkets, fewer stores with access for those with physical disabilities, and the lack of public transportation left Latino residents without a vehicle and those with physical disabilities with few food shopping options. Those with physical disabilities or debilitating chronic illnesses were likely to encounter difficulties accessing food stores in their own community because of a lack of stores with disability access features. All supermarkets in the study were located outside the Latino neighborhood, well beyond pedestrian access. Residents in the Latino neighborhood experienced difficulties reaching a supermarket if they lacked personal transportation because public transportation was very limited. The end result was that the residents had to rely on small neighborhood stores with higher prices and fewer choices for some items.
Residents of rural areas must either own or have access to reliable transportation to access healthy food. The findings of Sharkey and Horel (2008) confirm that rural residents have overall low potential access to supermarkets, which is of particular concern given that greater distance from a supermarket has been associated with the lowest diet quality (Laraia et al., 2004; Powell et al., 2007). Spatial inequality experienced by rural low-income families may be exacerbated by mobility and time constraints—including time spent commuting to work, lack of or limited access to transportation, or not being able to afford the cost of transportation (Blanchard and Lyson, 2002; Clifton, 2004; Kaufman, 1999; Powell et al., 2007). Sharkey and colleagues (2010) combined data from the Brazos Valley Food Environment Project, which included identification and geocoding of all food stores (N = 185) in six rural counties in Texas, with 2000 U.S. census data for 101 census block groups to examine neighborhood access to fruits and vegetables. In contrast with other studies, such as those of Zenk and colleagues (2005) and Morland and colleagues (2007), they found that neighborhoods considered highly deprived had better spatial access to supermarkets, grocery stores, convenience stores, and discount stores than less deprived areas. This was the case both for distance to the nearest food source and number of opportunities to get there. Taken together, the evidence reviewed by the committee suggests that among low-income households, greater distances to major food outlets are more likely than shorter distances to be associated with limited food choices and fewer purchases of healthy foods.
The committee examined evidence for the impact of various environmental factors on the feasibility of defining the adequacy of SNAP allotments. The range of available evidence included specific environmental factors affecting food choices: food prices; access to food outlets offering a wide range of healthy foods; and disparities in access, particularly in transportation. The committee notes that relevant data collection is ongoing but the data are not yet available through the ERS National Household Food Acquisition and Purchase Survey. When completed, this survey will provide detailed information on household food purchases and acquisitions, including foods purchased for consumption at and away from home and foods acquired through public and private food and nutrition assistance programs. This dataset will be useful for a broad range of economic analyses of food choices and for understanding the implications of food choices for diet quality.
Food Prices
Access to food varies substantially across households because of the various factors affecting food prices. These factors include a number of environmental dimensions, such as geographic region of the country; urban versus rural setting; types of stores available (e.g., supermarkets, convenience stores, mass merchandisers, warehouse club stores); and types of foods available, such as healthier versus less healthy and degree of processing (e.g., raw ingredients, processed ingredients, processed foods, fully prepared foods). Over time, food prices are influenced by changes in costs, due largely to inflationary factors, for farm-level inputs and production, transportation at each stage of production, food processing, and food distribution, which may result in greater or lesser changes than in overall prices for all goods and services. Considering food prices as a component of the evidence needed to define the adequacy of SNAP allotments is important because the influence of food prices on the likelihood of food insecurity is both positive and significant; an increase of one standard deviation in the price of a food basket based on the TFP results in increases in food insecurity of 2.4 percentage points for adults and 3.7 percentage points for children (Gregory and Coleman-Jensen, 2011). In the following discussion, the committee describes the differences in food prices across several dimensions and changes in food prices over time in the context of how these patterns affect food access as a factor in defining the adequacy of SNAP allotments.
Geographic and Regional Variation in Food Prices
Food prices vary across geographic regions of the United States because of differences in the cost of living and other market conditions (Todd et al., 2010). The ERS Quarterly Food at Home Price Database is based on 2006 Nielsen Homescan data and can be used to examine differences in food prices across regions. It is preferred to the Bureau of Labor Statistics’ (BLS’s) Consumer Price Index (CPI) because the CPI is available only for a limited number of food items and four broad regional markets (Todd et al., 2010). Using 2006 Nielsen Homescan data from the ERS Quarterly Food at Home Price Database, Todd and colleagues (2010) show that the average prices per 100 grams across 50 food categories and 35 market regions differed by 125 percent to 217 percent in the highest-cost versus the lowest-cost region (see Table 4-1).3 The smallest price difference identified was for canned soups, sauces, and prepared foods, while the largest price difference was for low-fat cheese. In general, grain-based foods, prepared foods, snack foods, and carbonated beverages appeared to have smaller price differences than fruits and vegetables, dairy foods, and meat and poultry. For particular types of foods, the ratio of the average price to the national average varied substantially across market regions. For example, as shown in Table 4-2 for low-fat milk, the average price per 100 grams was 73 percent of the national average for the full sample in Salt Lake City but 129 percent of the national average in urban New York. For purchases made by low-income households in the Nielsen Homescan sample (income below 185 percent of the poverty level), the corresponding ratios ranged from 66 percent to 133 percent across the same market regions. Across the sample of other food categories examined in the report (canned fruit, packaged whole grains, eggs, and carbonated beverages), the lowest relative prices were generally 70 to 90 percent of the national average, while the highest relative prices were generally 120 percent to 140 percent of the national average. Overall, the ranges appeared to be similar for the full Homescan sample and the low-income portion of the sample, with generally similar rankings by market group. However, some of the differences in average prices across regions and across income levels could be due to differences in the level of quality of foods purchased.
Like Todd and colleagues (2010), Leibtag and Kumcu (2011), using Nielsen Homescan data, found substantial price variation by region of the country when examining more disaggregated data for fresh fruits and
____________________
3Homescan data for 2006 were used because this was the most recent year for which a portion of the Nielsen Homescan panel reported random-weight food purchases (which applies particularly to fruits, vegetables, meat, poultry, and fish) in addition to Universal Price Code (UPC) food purchases. Since 2007, the Homescan panel has recorded only UPC food purchases at the detailed level.
TABLE 4-1 Range in Market Group Prices for Selected Food Groups, First Quarter 2006
| Minimum Price | Maximum Price | Max. as % of Min. | |
| Food Group | $ per 100 grams | ||
| Fresh and frozen fruit | 0.229 | 0.422 | 184.1 |
| Canned fruit | 0.237 | 0.385 | 162.4 |
| Fruit juice | 0.146 | 0.223 | 152.3 |
| Fresh and frozen dark green vegetables | 0.259 | 0.399 | 154.0 |
| Fresh and frozen orange vegetables | 0.202 | 0.302 | 149.7 |
| Fresh and frozen starchy vegetables | 0.176 | 0.277 | 157.3 |
| Canned legumes | 0.116 | 0.208 | 178.7 |
| Whole grain bread, rolls, rice, pasta, and cereal | 0.429 | 0.540 | 125.8 |
| Refined grain bread, rolls, rice, pasta, and cereal | 0.335 | 0.467 | 139.7 |
| Low-fat milk | 0.067 | 0.124 | 185.9 |
| Low-fat cheese | 0.432 | 0.938 | 217.2 |
| Fresh and frozen regular-fat meat | 0.598 | 0.906 | 151.4 |
| Fresh and frozen poultry | 0.468 | 0.856 | 182.9 |
| Fresh and frozen fish | 0.891 | 1.506 | 169.1 |
| Eggs | 0.143 | 0.250 | 174.6 |
| Nonalcoholic carbonated beverages | 0.075 | 0.104 | 138.5 |
| Noncarbonated caloric beverages | 0.095 | 0.160 | 168.4 |
| Packaged sweets and bakery goods | 0.803 | 1.463 | 182.3 |
| Ready-to-eat bakery items | 0.399 | 0.652 | 163.3 |
| Frozen entrees and sides | 0.590 | 0.784 | 133.0 |
| Canned soups, sauces, and prepared foods | 0.226 | 0.283 | 125.4 |
| Packaged snacks | 0.709 | 1.025 | 144.5 |
SOURCE: Todd et al., 2010. ERS calculations using 2006 Quarterly Food-at-Home Price Database.
vegetables for 2004-2006. As shown in Table 4-3, the average prices for fruits and vegetables differed by 12 percent (green beans) to 140 percent (watermelons) between the lowest- and highest-cost regions. The minimum prices were at least 11 percent below the national average price, while the maximum prices were up to 47 percent above the national average price. Aggregated across the 20 categories of fresh fruits and vegetables, prices were lowest in the Metro South 2 region, comprising Nashville, Birmingham, Memphis, and Louisville, and highest in San Francisco (see Table 4-4). According to Leibtag and Kumcu’s (2011) analysis, these differences in prices across regions have substantial implications for the purchasing power of benefits provided by nutrition assistance programs.
TABLE 4-2 Price Variations Across Market Groups, Full Sample Versus Low-Income Sample, Low-Fat Milk (Food Group 23), 2006 Nielsen Homescan Data
| Full Sample | Low-Income Sample | ||
| Market Group | Price Relative to National Mean (%) | Market Group | Price Relative to National Mean (%) |
| Salt Lake City | 72.8 | Salt Lake City | 65.6 |
| Non-Metro East North Central | 80.3 | Metro Ohio | 81.8 |
| Metro Ohio | 81.5 | Non-Metro East North Central | 82.1 |
| Metro Midwest 1 | 82.4 | Metro Midwest 1 | 82.6 |
| Western New York/Pennsylvania | 83.4 | Metro Mountain | 84.0 |
| North Pacific | 86.7 | Non-Metro Pacific | 84.2 |
| Chicago | 87.3 | Western New York/Pennsylvania | 86.0 |
| Non-Metro West North Central | 88.2 | Chicago | 87.4 |
| Metro Mountain | 89.0 | North Pacific | 87.7 |
| Metro Midwest 2 | 89.2 | Non-Metro Mountain | 88.0 |
| Metro South 3 | 93.7 | Metro Midwest 2 | 90.7 |
| Non-Metro Pacific | 94.4 | Metro South 3 | 91.5 |
| Metro South 2 | 94.7 | Non-Metro West North Central | 92.5 |
| Non-Metro Middle Atlantic | 97.9 | Metro South 2 | 96.2 |
| Non-Metro Mountain | 98.0 | Boston | 100.9 |
| Philadelphia | 105.6 | Non-Metro West South Central | 104.5 |
| Non-Metro West South Central | 106.3 | Metro South 4 | 105.4 |
| Non-Metro South Atlantic | 106.3 | Non-Metro East South Central | 105.7 |
| Metro South 4 | 106.6 | Non-Metro New England | 105.7 |
| Boston | 107.1 | Philadelphia | 106.0 |
| Non-Metro New England | 107.6 | Other New York | 106.1 |
| Non-Metro East South Central | 108.5 | Washington, DC | 108.9 |
| Washington, DC | 110.6 | San Francisco | 110.6 |
| Baltimore | 111.4 | Hartford | 110.7 |
| Other New York | 111.4 | Metro California | 112.5 |
| San Antonio | 111.6 | Atlanta | 113.3 |
| Atlanta | 111.8 | North Florida | 113.9 |
| Metro California | 111.9 | Baltimore | 114.2 |
| Los Angeles | 112.9 | South Florida | 116.2 |
| North Florida | 113.6 | Non-Metro South Atlantic | 116.4 |
| San Francisco | 115.1 | Metro South 1 | 117.2 |
| Hartford | 115.5 | Los Angeles | 117.5 |
| South Florida | 116.8 | San Antonio | 118.8 |
| Metro South 1 | 117.7 | Non-Metro Middle Atlantic | 122.5 |
| Urban New York | 128.7 | Urban New York | 131.4 |
NOTES: National mean prices are weighted and calculated separately for each sample; low-income households have income below 185 percent of the federal poverty level.
SOURCE: Todd et al., 2010. ERS calculations using 2006 Quarterly Food-at-Home Price Database.
TABLE 4-3 Market Prices for the 20 Most Popular Fruits and Vegetables, with Deviation of Their Minimum and Maximum Prices from the National Average, 2004-2006
| Fruit/Vegetable | National Average of Market Prices per Pound | Minimum Market Price per Pound | Maximum Market Price per Pound | Difference from Minimum to Maximum | Difference from National Average to Minimum | Difference from National Average to Maximum |
| $ | % | |||||
| Tomatoes | 1.66 | 1.42 | 1.98 | 39 | –15 | 19 |
| Onions | 1.33 | 0.95 | 1.68 | 77 | –29 | 26 |
| Lettuce | 1.01 | 0.89 | 1.17 | 30 | –11 | 16 |
| Green beans | 0.96 | 0.59 | 1.31 | 12 | –38 | 36 |
| Corn | 0.89 | 0.74 | 1.11 | 50 | –17 | 25 |
| Carrots | 1.18 | 0.99 | 1.38 | 39 | –16 | 17 |
| Broccoli | 1.34 | 1.10 | 1.61 | 46 | –18 | 20 |
| Cucumbers | 1.02 | 0.81 | 1.33 | 64 | –21 | 30 |
| Peppers | 1.72 | 1.18 | 2.35 | 100 | –32 | 37 |
| Cabbage | 0.52 | 0.42 | 0.70 | 68 | –20 | 34 |
| Bananas | 0.49 | 0.40 | 0.62 | 55 | –19 | 26 |
| Apples | 1.10 | 0.98 | 1.24 | 27 | –12 | 12 |
| Watermelon | 0.87 | 0.49 | 1.19 | 140 | –43 | 37 |
| Oranges | 0.85 | 0.72 | 1.25 | 73 | –15 | 47 |
| Grapes | 1.51 | 1.31 | 1.70 | 30 | –14 | 12 |
| Strawberries | 2.41 | 2.15 | 2.86 | 33 | –11 | 19 |
| Peaches | 1.13 | 0.95 | 1.40 | 47 | –15 | 25 |
| Pineapples | 1.29 | 0.99 | 1.63 | 65 | –23 | 26 |
| Pears | 1.06 | 0.94 | 1.18 | 26 | –11 | 12 |
| Grapefruit | 0.98 | 0.78 | 1.24 | 60 | –21 | 27 |
SOURCE: Leibtag and Kumcu, 2011.
Urban Versus Rural Food Prices
The data in Table 4-2 also provide evidence of differences in prices by urban versus rural areas. Higher costs in urban areas may reflect the higher costs of operating retail establishments in those areas and the fact that urban communities are often served by smaller stores with higher prices (Stewart and Dong, 2011). For example, prices for low-fat milk in non-metropolitan East North Central (80.3 percent relative to the national mean) are lower than those in the corresponding metropolitan areas in the same region: metropolitan Ohio (81.5 percent); metropolitan Midwest comprising Indianapolis, Detroit, Milwaukee, and Grand Rapids (82.4 percent); and Chicago (87.3 percent). Prices for low-fat milk in non-metropolitan New England (107.6 percent relative to the national mean) are lower than those in the corresponding metropolitan area of Hartford (115.5 percent)
TABLE 4-4 Index Ranking of Markets from Lowest to Highest Prices for the 20 Fruits and Vegetables Most Frequently Purchased by U.S. Households, 2004-2006
|
Aggregate Market Group |
Index Ranking |
|
Metro South 2 |
90.8 |
|
Metro Ohio |
91.9 |
|
Salt Lake City |
92.2 |
|
Metro Mountain |
92.8 |
|
Metro South 3 |
93.8 |
|
San Antonio |
93.8 |
|
Metro Midwest 1 |
95.0 |
|
Chicago |
95.3 |
|
Metro South 4 |
95.4 |
|
Urban New York City |
96.3 |
|
Metro Midwest 2 |
96.4 |
|
Los Angeles |
97.4 |
|
Western New York/Pennsylvania |
98.1 |
|
Metro Northwest |
99.9 |
|
National average |
100.0 |
|
Atlanta |
101.1 |
|
Metro California |
101.7 |
|
Mid-Atlantic |
102.2 |
|
Other New York City |
103.4 |
|
Boston |
103.8 |
|
Philadelphia |
103.9 |
|
North Florida |
104.4 |
|
South Florida |
104.7 |
|
Baltimore |
108.8 |
|
Washington, DC |
110.9 |
|
Hartford-New Haven |
111.9 |
|
San Francisco |
113.9 |
SOURCE: Leibtag and Kumcu, 2011.
but similar to those in the metropolitan area of Boston (107.1 percent). Generally, patterns of lower prices in non-metropolitan areas were found across the other food categories examined (canned fruit, packaged whole grains, eggs, and carbonated beverages). Stewart and Dong (2011) found similar results using data from the Nielsen Homescan panel for 2006, which showed that prices paid by households in urban areas for fresh vegetables and salty snacks were significantly higher than those in non-urban areas.
Food Prices by Store Type
Households acquire food for use at home from a broad variety of stores and outlets (see Box 4-2), including traditional supermarkets and grocery
BOX 4-2
Types of Food Stores and Outlets
Supermarket: Encompasses establishments commonly known as supermarkets, food stores, and food warehouses engaged primarily in the retail sale of an extensive variety of grocery and other store merchandise. This type of store typically has 10 or more checkout lanes with registers, bar code scanners, and conveyor belts. Customers normally make large-volume purchases.
Grocery store: A store that carries a selection of all four staple food categories (i.e., fruits and vegetables; meat, poultry, or fish; bread and cereal; dairy products). This type of store may sell items ineligible for purchase with SNAP benefits as well, but its primary stock is food items. These stores can be categorized as large, medium, or small depending on the size of the selection of items in the four staple food categories.
Convenience store: A self-service store that offers a limited line of convenience items and is typically open for long hours to provide easy access for customers. This type of store is engaged primarily in the retail sale of a variety of canned goods, dairy products, prepackaged meats, and other grocery items in limited amounts. It usually sells a large variety of SNAP-ineligible products such as hot coffee, alcohol, or tobacco products.
Combination grocery/other: A store whose primary business is the sale of general merchandise but that also sells a variety of food products. Such stores include independent drugstores, dollar stores, and general stores.
Supercenter/chain store: A very large supermarket, “big box” store, super store, or food warehouse engaged primarily in the retail sale of a wide variety of grocery and other store merchandise. This category includes stores that are large food/drug combination stores and mass merchandisers under a single roof, as well as membership retail/wholesale hybrids offering a limited variety of products in a warehouse-type environment.
Farmers’ market: A single- or multistall market that sells agricultural products, particularly fresh fruits and vegetables, to the general public. This designation applies to any organization that operates a farmers’ market location.
Specialty food/gourmet store: A store that operates in a fixed or semipermanent location whose primary business is the sale of meat/poultry products, seafood, fruits and vegetables, or baked goods. It may sell nonfood items or other food items, but such products are incidental to the primary specialty food stock.
SOURCE: Personal communication, Benefit Redemption Division, USDA, September 12, 2012.
stores; convenience and combination grocery stores (e.g., drug stores), mass merchandisers or supercenters and warehouse club stores, farmers’ markets, and specialty and gourmet food stores. Over time, there has been a trend for a larger portion of food purchases to be made in stores other than traditional supermarkets (Leibtag, 2005).
Prices vary across types of stores, and thus the types of stores accessible to households affect their total food budgets and ability to acquire healthy foods. In particular, greater access to large grocery stores in suburban than in inner-city and rural areas may result in the poor paying higher prices for food (Andreyeva et al., 2008). In an extensive comparison of food prices at nontraditional discount stores4 and traditional food stores, Leibtag and colleagues (2010), using 2004-2006 Nielsen Homescan data, found that national average unit prices (total price divided by product weight) were significantly lower in nontraditional stores for 86 percent of food products at the broadest level of comparison. At the Universal Price Code (UPC) comparison level, 82 percent of products had significantly lower prices in nontraditional stores, with an average price discount of 7.5 percent. Meat products had the largest price discounts at nontraditional stores. Furthermore, all canned products had significantly lower prices in nontraditional stores on average. With respect to specific markets, those with more nontraditional stores had smaller differences in prices between those stores and traditional stores, which could be due to increased competition or the exit of traditional stores in markets with a large number of nontraditional stores (Leibtag et al., 2010).
In studies focused on specific areas, food prices were also found to differ substantially across store types. In a study of six neighborhoods in New Haven, Connecticut, Andreyeva and colleagues (2008) found that prices in 2007 were 51 percent higher on average in small neighborhood stores than in supermarkets across 622 food items. In another analysis, Andreyeva and colleagues (2008) constructed a representative basket of food items from 75 stores to compare prices across types of stores (convenience versus grocery, including small neighborhood grocery stores) and neighborhoods (low-income versus high-income). Results indicated that the average price of the market basket was about 4 percent higher in higher-income neighborhoods and also about 4 percent higher in convenience stores than in grocery stores; thus, the authors conclude that price differences across neighborhoods and store types are relatively modest. In a study of food prices in 77 stores in a rural South Carolina county, Liese and colleagues (2007) found that prices of selected foods were substantially higher in convenience stores than in supermarkets (greater than $2 million in annual sales) and grocery stores (less than $2 million in annual sales). The differences were statistically
____________________
4Defined as supercenters, mass merchandisers, wholesale club stores, and dollar stores.
significant for apples, packaged bacon, packaged smoked turkey, canned salmon, canned tuna, low-fiber breakfast cereals, whole milk, and low-fat/nonfat milk.
Prices of Healthy Versus Unhealthy Foods
Whether healthy foods are found to be more expensive than less healthy foods may depend on how both “healthy” and the units of measure are defined (Carlson and Frazao, 2012; Lipsky, 2009). Numerous studies have examined whether healthy foods are more or less expensive than less healthy foods, using either secondary data available across a broad range of foods or data collected from specific stores for a more limited set of foods. While some argue that nutritious diets of whole grains, lean meats, and fresh vegetables and fruits are affordable, others believe that energy-dense foods (i.e., with more calories per serving) are less expensive (Drewnowski, 2010; Drewnowski and Eichelsdoerfer, 2010; Drewnowski and Specter, 2004; Monsivais et al., 2010). For example, Monsivais and colleagues (2010) linked longitudinal retail price data for 378 foods and beverages in Seattle for 2004-2008 with energy density (kcal/g) and two measures of nutrient density—the Naturally Nutrient Rich (NNR) score, which is the sum of the percent Daily Values (DV) per 100 kcal for 16 nutrients, and the Nutrient Rich Food Index, which is based on the levels of nine positive and three negative nutrients relative to calories. They found that the mean cost of the most nutrient-dense foods (those with high positive nutrients and low negative nutrients relative to calories) were substantially higher and increasing more rapidly than the mean costs of the least nutrient-dense foods.
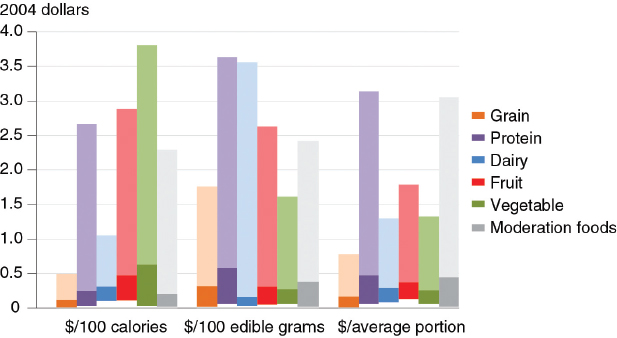
A recent analysis by Carlson and Frazao (2012) defines a healthy food as one that contains at least half the portion size defined by the 2010 DGA in at least one of the major food groups and has only a moderate amount of saturated fats, added sugars, and sodium. Their analysis examines the price per calorie, per edible gram, and per average portion consumed using the CNPP food prices database based on 2003-2004 Nielsen Homescan data as the source of prices. The authors found that foods high in calories tend to have a lower price per calorie than foods lower in calories. As shown in Figure 4-1, while vegetables have the highest price per 100 calories, they have the lowest price on the basis of price per 100 edible grams or per average portion. Dairy products have the lowest price per 100 calories but one of the highest prices on a 100 edible grams basis. “Moderation” foods, which are defined primarily as those high in sodium, added sugars (including sugar-sweetened beverages), or saturated fat, have a relatively low price per 100 calories but a relatively high price on an average portion basis. Thus, Figure 4-1 shows that comparisons of the costs of healthy versus unhealthy foods can be misleading if expressed on the basis of 100 calories
FIGURE 4-1 Prices of healthy versus less healthy foods vary with the measurement method.
NOTES: The dark areas of each bar represent the price range for the less expensive half of the foods in the category, while the lighter areas are the price ranges for the higher-cost foods. White space at the bottom of the bars represents the start of the price range. Moderation foods are foods that are high in sodium, added sugars, or saturated fat or that do not contain foods from a food group.
SOURCE: Carlson and Frazao, 2012.
(and 100 edible grams) because many healthy foods have fewer calories per serving (and per 100 grams) than unhealthy foods. Most important, on a per-serving basis, grains, dairy products, fruits, and vegetables, cost less than moderation foods.
Todd and colleagues (2011) examined differences in prices of a selected set of healthy foods relative to their less healthy counterparts by geographic region using the ERS Quarterly Food at Home Price Database for 1998 through 2006 and found mixed results by food type and region. For some foods, such as whole grains compared with refined grains and fresh and frozen dark green vegetables compared with starchy vegetables, the healthier version was more expensive in all geographic regions. For other foods, such as orange vegetables compared with starchy vegetables and skim and 1 percent milk compared with 2 percent and whole milk, the healthier version was less expensive than the less healthy version in some geographic areas. The magnitudes of the price differences for healthier versions of foods varied substantially across the country.
In addition to the studies discussed above, other studies have examined the prices of healthier food alternatives based on the prices of foods available
in stores in specific areas. For example, Jetter and Cassady (2006) collected price data from 25 stores in Los Angeles and Sacramento for September 2003 through June 2004 and calculated the average cost of a standard market basket based on the TFP versus the average cost of a healthier market basket. Because of the higher costs of healthier foods such as whole grains, lean ground beef, and skinless poultry, the average cost of the healthier market basket was $230, compared with $194 for the TFP market basket. Using similar data for a longer time period, Cassady and colleagues (2007) estimated that a low-income family would need to devote 43 percent to 70 percent of its food budget to fruits and vegetables to meet the 2005 DGA, thus indicating the high price of fruits and vegetables relative to other foods. Because of their relatively high costs, discounts on fruits and vegetables might result in fairly substantial increases in consumption (Dong and Lin, 2009). In a separate study of food prices in 77 stores in a rural South Carolina county in 2004, Liese and colleagues (2007) found that the prices of more healthful versions of foods were higher than those of the less healthful versions, with the exception of milk. For example, high-fiber bread was more expensive than low-fiber bread, low-fat beef was more expensive than high-fat beef, and chicken breasts were more expensive than chicken drumsticks in convenience stores and supermarkets. The results of these more narrowly focused price studies demonstrate that substantial differences in the prices of healthier foods can occur in specific geographic areas, although studies using larger secondary data sources show a broader pattern of mixed results depending on the level of aggregation of the data by food type and by geographic region.
Variation in Food Prices Over Time Due to Inflationary Factors
Food prices vary over time because of changes in the availability of supplies of raw commodities, changes in farm-level production costs, and changes in food processing costs (e.g., due to changes in land, capital, energy, and labor costs). In addition, some food prices, particularly for fresh fruits and vegetables, vary seasonally, being lower during the products’ harvest seasons.
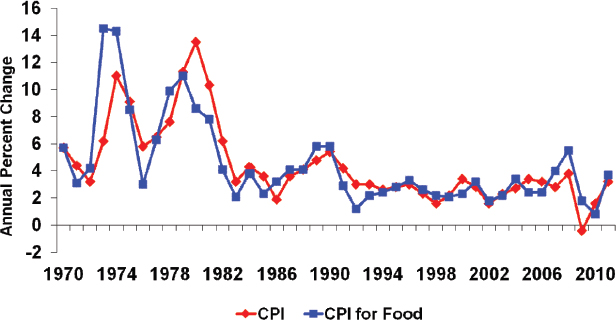
Rising food prices may reduce the purchasing power of benefits received through federal nutrition assistance programs, depending on how and whether the benefits are adjusted for inflation over time (Hanson and Andrews, 2008). As discussed in Chapter 2, there is a lag of up to 16 months between calculation of the TFP cost and adjustments to the maximum SNAP benefit to account for inflation. Food prices are particularly affected by changes in world supply and demand and may increase more or less than the overall price level. As shown in Figure 4-2, the percentage changes in the CPI for food generally track the changes in the CPI
FIGURE 4-2 Overall Consumer Price Index (CPI) and CPI for food, 1970-2011, based on Bureau of Labor Statistics data.
SOURCE: Leibtag, 2012.
for all products, but the timing and magnitude of the changes are not always aligned. After a relatively stable period during the 1990s and early 2000s, increases in the CPI for food exceeded the overall CPI over many of the past few years. However, Hausman and Leibtag (2007) show that the methodology used by BLS to calculate the CPI may overstate the price of food because it does not fully capture lower prices in supercenters and other nontraditional retail outlets that sell food.
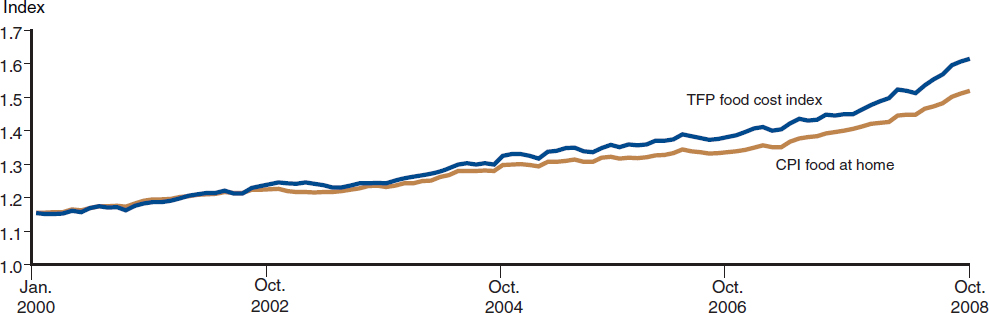
In addition to differences between changes in overall food price levels and changes in the price levels for all products, overall food price levels have been shown to differ from the price levels for the TFP (Hanson and Andrews, 2008). Figure 4-3 shows that the TFP price index, which is calculated using CNPP’s monthly updates of the costs of the TFP, is rising more rapidly than the CPI for food consumed at home. The differences are likely due to larger shares of fresh fruits and vegetables and eggs, which have the most volatile prices, in the TFP price index than in the CPI for food consumed at home (Hanson and Andrews, 2008). Because SNAP benefits are adjusted annually in October using the prior year TFP price index, the food purchasing power of the benefits may decline to the extent that the adjustments do not fully account for the potential monthly rise in the cost of the TFP. However, because the TFP is a theoretical construct, actual food purchase patterns likely differ from the foods represented in the TFP. Thus, the extent to which the difference between the TFP price index and the CPI represents true higher costs to SNAP recipients is uncertain. The 16-month lag in adjusting the
FIGURE 4-3 Thrifty Food Plan (TFP) food cost index compared with the Consumer Price Index (CPI) for food consumed at home.
NOTES: Monthly data. The TFP is for the reference family of four with children aged 6-8 and 9-10.
SOURCE: Hanson and Andrews, 2008. Data from USDA, ERS.
maximum benefit according to the CPI is a more certain contributor to a larger discrepancy between SNAP benefits and the actual cost of the TFP. The temporary increase in SNAP benefits under the American Recovery and Reinvestment Act of 20095 likely reduced this discrepancy, but the extent of reduction is currently unknown.
Access to Food Outlets
As described above, choosing foods that make up a diet consistent with the recommendations of the 2010 DGA, such as increased consumption of fruits and vegetables and whole-grain-rich foods and decreased consumption of solid fats and added sugars (USDA and HHS, 2010), can be challenging for populations with limited resources as a result of factors affecting food prices both regionally and locally. In light of this evidence, the committee examined additional evidence for an impact of the ability of low-income populations to access affordable healthy foods on the purchasing power of SNAP allotments under the assumptions of the TFP.
Access to Food Outlets and Purchasing Behavior
The committee identified a number of observational studies showing correlations between various means of access to food outlets and purchasing behavior. Personal transportation was previously discussed as an individual
____________________
5American Recovery and Reinvestment Act of 2009, Public Law 111-5, 111th Congress (February 17, 2009).
factor. The following discussion focuses on other barriers to access to healthy foods.
Urban or rural locale In a survey of the availability of fruits and vegetables in urban and rural areas of upstate New York, Hosler and colleagues (2008) identified one urban minority neighborhood among those surveyed that, in this respect, was the most disadvantaged site within an urban locale, as measured by the population density of stores selling these products. This community was found to be lacking not in the number of food stores but in an accessible high-impact super produce store. By contrast, such stores were available in a higher-income urban mixed neighborhood in the same locale, illustrating that disparity in access to fresh produce was associated with a single disadvantaged area within a larger locale.
A recent example of associations between access to healthy food and consumption is a cross-sectional community survey, conducted in 2002-2003, which was used as a data source for analyzing associations between neighborhood availability and consumption of dark green and orange vegetables in an ethnically diverse low- to moderate-income population in Detroit (Izumi et al., 2011). Data derived from the survey included the frequency of consumption of these vegetables and their availability in all food stores in the communities studied. The mean intake of dark green and orange vegetables among all participants was found to be 0.61 servings per day. The lowest intake was among participants living in neighborhoods where no store carried five or more varieties of such vegetables; residents in those neighborhoods consumed 0.17 fewer servings per day than those in neighborhoods where at least two stores provided more variety. The results of this study suggest a direct relationship between the availability of vegetables and consumption patterns within a locale.
Fisher and Strogatz (1999) conducted a telephone survey to (1) determine whether there is an association between the availability and consumption of low-fat milk, and (2) assess whether the availability of low-fat milk is associated with household income and racial composition. The study was carried out in three different geographic settings in New York: large metropolitan, midsize urban, and rural. Household interviews were conducted in each setting to determine the type of milk consumed. In each store surveyed within a corresponding zip code, containers of whole, 2 percent, 1 percent, and skim milk were counted for each container size (quart, half gallon, and gallon). The percentage of low-fat milk in the store and the average percentage across all stores in a zip code were then determined. A direct correlation was found among the percentage of low-fat milk in stores, consumption of low-fat milk in the household, and income level by zip code. In particular, low-fat milk tended to be less common in the stores located in rural or low-income areas and areas in which the majority
of the population was nonwhite. The authors note, however, that only 51 percent of survey respondents reported usually purchasing milk within their residential zip code.
Cheadle and colleagues (1991) conducted a similar study using a survey of healthful food choices in different grocery store environments to assess the relationship between individual dietary choices and the grocery store environment. They carried out a telephone survey in 12 different communities, including the corresponding larger zip code area, to obtain self-reported dietary intake data on low-fat and high-fiber foods, as well as the availability of health information in the community stores. They found a significant correlation between the availability of healthful foods in the community and zip code area stores and the self-reported healthfulness of participants’ diets. In a review of cross-sectional studies on associations between food environment and consumption, Rose and colleagues (2010) identified a number of studies that combined in-store measures with mapping of store location and found significant direct associations between neighborhood food environment and measures of consumption.
These studies are important because they suggest a link between purchasing power and access to food. A general conclusion that can be drawn from this work is that although associated with income, access to food outlets and healthy foods needs to be considered in the context of how certain factors within the food environment affect the cost of healthier food options. Overall, the evidence suggests that limited access to healthy food may influence food shopping and spending behavior by reducing choices.
Farm-to-consumer venues Farm-to-consumer venues show promise in improving dietary intake among all people in the United States, including low-income groups (Blanck et al., 2011). However there are few such venues, especially in low-income communities (FNS, 2011). In addition, many farmers’ markets do not accept SNAP. Although USDA figures indicate that the number of farmers’ markets accepting SNAP has increased by 16 percent since 2010, more needs to be done to increase the number of these venues authorized as retailers by the program (FNS, 2011). The lack of awareness of farm-to-consumer venues, the lack of farmers’ markets and farm stands close to home, the lack of transportation to these venues, inconvenient hours, and affordability concerns are additional barriers to use of farm-to-consumer venues among those receiving federal food assistance (Briggs et al., 2010).
Disparities in Access and Geographic Proximity to Food Outlets
According to a 2009 USDA report, 23.5 million people lack access to a supermarket within a mile of their home (Ver Ploeg et al., 2009). Limited
access to food stores is not unique to urban areas; about 20 percent of rural counties across the United States (418 counties) also have been identified as areas where half the population lives more than 10 miles from a large food store (Morton and Blanchard, 2007). The disparate distribution of grocery stores and supermarkets in low-income neighborhoods or geographic areas is especially notable in light of the distribution of racial/ethnic groups within these tracts. For example, Mantovani and Welsh (1996) found that “a large majority of low-income households are in close proximity to a full-line grocery store or supermarket” (p. iv), but minority households in rural areas live farther from these types of food stores than nonminority households.
Disparities in Access by Type of Food Outlet
Apart from the question of distance from a food store is that of where SNAP participants are more likely to shop. Ohls (1999) analyzed data from the National Food Stamp Program Survey, conducted between June 1996 and January 1997. The analysis examined the food shopping opportunities of low-income households, including SNAP participants and eligible nonparticipants. The study found that most low-income households shopped at supermarkets but tended to supplement their purchases by shopping at neighborhood grocery stores, convenience stores, bakeries, and produce markets. They also engaged in “careful” shopping practices, including making bargain purchases, taking advantage of special offers, and using shopping lists to extend their food dollars. Olander and colleagues (2006) and Castner and Henke (2011) also found that most SNAP participants redeemed their benefits at supermarkets, and their purchase patterns were similar to those identified by Cole (1997).
As noted by Mantovani and Welsh (1996), minority low-income groups may experience disparities in access that are not seen across the low-income population as a whole. In a study examining associations between local food environments and neighborhood racial/ethnic and socioeconomic composition, Moore and Diez Roux (2006) analyzed census tract demographics as well as food store characteristics in selected study areas in Maryland, New York, and North Carolina. Their comparison across study areas and across racial/ethnic composition revealed that the predominantly minority and racially mixed areas had at least twice as many grocery stores but fewer than half the number of supermarkets compared with predominantly white areas. The low-income and nonwhite areas also had fewer fruit and vegetable markets, bakeries, specialty stores, and natural food stores.
A cross-sectional survey in Michigan (Zenk et al., 2005) assessed the availability, quality, and price of fresh produce in various types of stores—large and small grocery stores, “mom and pop” stores, and convenience
and specialty stores—in three Detroit communities and an adjacent suburb. The communities surveyed varied in racial/ethnic composition and socioeconomic characteristics and exhibited different health profiles for diet and obesity-related diseases. Among the findings was that produce quality was lower in low-income African American communities than in more affluent or racially mixed neighborhoods. Moreover, the low-income African American communities had more than four times more liquor stores and fewer grocery stores per 100,000 residents compared with the racially mixed communities.
Overall, this body of evidence suggests that supermarket access is poorer among low-income and minority populations, and that individuals without ready access to supermarkets have more difficulty finding fruits and vegetables in their neighborhood. In addition, individuals with supermarkets in their neighborhood are more likely than those lacking nearby supermarkets to eat more fruits and vegetables.
Disparities in the Quality of Food Available for Purchase
In a cross-sectional study of 25 stores in South San Diego County, California, Emond and colleagues (2012) examined associations between the availability, quality, and cost of healthy and unhealthy food items and store location—specifically, non-ethnically based supermarkets and Latino grocery stores (tiendas) in low-income areas. They found no difference in the availability of fresh produce by store type and quality differences for only one fruit item. Further, the price per pound for fresh produce was lower in the tiendas than in the supermarkets. However, the cost of skim milk was significantly higher in the tiendas and lean ground beef was significantly less available than in the supermarkets surveyed. Similarly, Andreyeva and colleagues (2008), conducted two studies examining changes in price differences between large grocery stores and small neighborhood markets over the past 35 years (study 1), and price and nutritional quality as a function of income and neighborhood (study 2) in New Haven, Connecticut. In assessing the results of both studies, they concluded that the availability of many healthful food items was lower and produce quality was worse in lower-income than in higher-income areas even though average prices were not significantly different between the two types of neighborhoods. In Baltimore, Maryland, Franco and colleagues (2007) conducted a small observational study to determine the availability and price of food in 240 stores in area neighborhoods. In the neighborhoods surveyed, 94.4 percent of residents were African American; 64.4 percent of family households were female headed; the unemployment rate of residents was 23.5 percent, with a median household income of $15,493; and only 53.6 percent of adults had completed high school. Of the 187 food stores located within the city,
17 were classified as supermarkets, 136 as grocery stores, and 34 as convenience stores. No fresh fruits or vegetables, whole-wheat bread, or skim milk was found in the city’s grocery stores; other food items, such as whole milk, soda, chips, and canned foods, were typically available. Further, the price of whole milk, cereal, and white bread at a representative store was 20 percent higher than in the closest supermarket, 0.9 miles away. Overall, food outlets in lower-income and minority neighborhoods tend to stock lower-quality items than food outlets in predominantly higher-income, white neighborhoods.
Disparities in Access to and Availability of Public Transportation
Residents in many urban areas have few transportation options to reach supermarkets. To examine whether access to transportation plays a role in risk factors for food insecurity and access to food outlets, Bjorn and colleagues (2008) developed and mapped a number of food insecurity index values, including income, ethnicity, employment, and education. Analysis of the indices identified a number of high-risk areas lacking food access in Seattle, King County, Washington. Many of the high-risk lower-income neighborhoods assessed were racially and ethnically diverse. For some of these areas, transportation access was a major barrier to food security. Households in the areas at risk of food insecurity were more vulnerable to economic and social as well as geographic barriers that may have made them dependent on local convenience stores and/or required long trips to distant grocery stores.
Inadequate transportation can also be a major challenge for rural residents, given the long distances to stores. Sharkey and colleagues (2009) examined associations between neighborhood needs, as measured by socioeconomic deprivation and vehicle availability, and two criteria for food environment access: distance to the nearest food store and fast-food restaurant, and number of food stores and fast-food restaurants within a specified network distance of neighborhood areas. The authors analyzed data from the 2006-2007 Colonias Food Environment Project and the decennial 2000 U.S. Census Summary File 3. They found that the rural neighborhoods studied had better access to convenience stores and fast-food restaurants in terms of both distance and shopping opportunity compared with access to supermarkets. Supermarkets provided greater proximity and coverage than traditional grocery stores, but when neighborhood deprivation was taken into account, the neighborhoods with higher deprivation had the least access to supermarkets and grocery stores but the greatest access to convenience stores. When transportation access was considered, limited availability of a vehicle was correlated with greater proximity to a supermarket as well as other store types, but higher deprivation was associated with greater
distance to supermarkets as well as other store types. Collectively, these results indicate an association between high-deprivation neighborhoods and both low access and limited transportation to supermarkets in a rural area.
In response to a request from Congress, USDA conducted a comprehensive 1-year study to assess the impact of limited access to food on local populations and outline recommendations for addressing the problem (Ver Ploeg et al., 2009). The study included two conferences on food deserts and a set of commissioned studies carried out in cooperation with the National Poverty Center at the University of Michigan, as well as reviews of the existing literature, a national-level assessment of access to supermarkets and large grocery stores, analysis of the economic and public health effects of limited access, and a discussion of existing policy interventions. Table 4-5 shows the study findings on access to supermarkets according to individual factors of low-income and underserved population groups in the United States. Data in the table indicate that the median distance to a supermarket for low-income, minority, and elderly populations is comparable to that for higher-income populations. However, as data in Table 4-6 indicate, the percentage of households without a vehicle is higher in low-income areas. For example, 2.5 to 3.3 percent of urban and 7.4 percent of rural low-income households live more than a mile from a supermarket and lack access to a vehicle. Research has shown that inadequate transportation is a significant barrier to access to supermarkets for residents of economically disadvantaged African American neighborhoods (Zenk et al., 2005).
Impact of Disparities in Access on Health Outcomes
The committee identified a number of studies examining associations between disparities in access to healthy foods and food insecurity, obesity, and obesity-related chronic disease. On the whole, the evidence supports a positive relationship between food insecurity and risk for obesity that is strongest among women (Dinour et al., 2007; Frongillo et al., 1997; Jilcott et al., 2011; Jones and Frongillo, 2006; Larson and Story, 2011; Velasquez-Melendez et al., 2011) and stronger among African American and Hispanic groups than whites (Fitzgerald et al., 2011; Sharkey and Schoenberg, 2005). The evidence reviewed was inconsistent as to significant associations between food insecurity and obesity in children (IOM, 2011).
A review of 54 studies examining associations between neighborhood differences in access to healthy food and risk for obesity identified an association between better access to convenience stores and higher risk for obesity (Larson et al., 2009). An observational study that analyzed data collected from a telephone survey found increased odds of obesity associated with distance to a supermarket in metropolitan but not in nonmetropolitan areas (Michimi and Wimberly, 2010). In contrast, another analysis of data
TABLE 4-5 Supermarket Access by Household Income, Race/Ethnicity, Age, and Vehicle Access
| Distance to Nearest Supermarket (miles) | |||||
| High Access (.0.5 mi) | Medium Access (0.5–1.0 mi) | Low Access (>1.0 mi) | |||
| Number (millions) | Mediana (miles) | Number in millions (percent) | |||
| Incomeb | |||||
| Low-income | 79.3 (28.8) | 0.76 | 22.6 (28.5) | 26.4 (33.3) | 30.2 (38.1) |
| Higher-income | 196.1 (71.2) | 0.87 | 43.8 (22.3) | 66.3 (33.8) | 86.1 (43.9) |
| All income levels | 275.5 (100) | 0.84 | 66.5 (24.1) | 92.7 (33.7) | 116.3 (42.2) |
| Race/Ethnicity | |||||
| Nonwhite | 85.7 (30.7) | 0.63 | 31.4 (36.6) | 31.5 (36.8) | 22.8 (26.6) |
| White | 193.9 (69.3) | 0.96 | 39.1 (20.2) | 61.3 (31.6) | 93.4 (48.2) |
| All races/ethnicities | 279.6 (100) | 0.86 | 70.5 (25.2) | 92.8 (33.2) | 116.3 (41.6) |
| Age | |||||
| ≥65 years | 34.8 (12.4) | 0.81 | 8.9 (25.7) | 11.8 (33.9) | 14.4 (40.4) |
| 65 years | 244.8 (87.6) | 0.82 | 61.6 (25.2) | 81.0 (33.1) | 102.2 (41.8) |
| All ages | 279.6 (100) | 0.82 | 70.6 (25.2) | 92.7 (33.2) | 116.3 (41.6) |
| Vehicle access | |||||
| Households without a vehicle | 10.8 (10.3) | 0.55 | 5.0 (46.2) | 3.4 (31.7) | 2.4 (22.1) |
| Households with a vehicle | 94.1 (89.7) | 0.84 | 22.2 (23.6) | 31.7 (33.7) | 40.2 (42.7) |
| All households | 104.9 (100) | 0.81 | 25.9 (25.9) | 35.1 (33.5) | 42.5 (40.6) |
aMedians are weighted by population of each square kilometer grid area.
bLow-income households are those with income less than or equal to 200 percent of the federal poverty level for family size.
SOURCE: Ver Ploeg et al., 2009. Economic Research Service(ERS) analysis based on data from Census of Population, 2000, and the ERS-compiled supermarket directory for the contiguous United States in 2006.
TABLE 4-6 Household Vehicle Access and Supermarket Access
| Household Without Access to a Vehicle | |||||
| 0.5–1 Mile from a Supermarket | >1 Mile from a Supermarket | ||||
| Total Households*(millions) | Number (millions) | Percent | Number (millions) | Percent | |
| Total U.S. | 104.9 | 3.4 | 3.2 | 2.4 | 2.3 |
| Low-income areas | 25.1 | 1.6 | 6.4 | 0.9 | 3.8 |
| Urban areas | 69.9 | 2.9 | 4.1 | 1.1 | 1.5 |
| Low-income areas | 15.6 | 1.3 | 8.3 | 0.4 | 2.5 |
| Urban clusters | 9.7 | 0.4 | 4.1 | 0.2 | 2.5 |
| Low-income areas | 3.6 | 0.2 | 5.6 | 0.1 | 3.3 |
| Rural areas | 25.3 | 0.2 | 0.8 | 1.1 | 4.4 |
| Low-income areas | 5.9 | 0.1 | 1.7 | 0.4 | 7.4 |
*This column shows the total number of households regardless of vehicle access.
SOURCE: Ver Ploeg et al., 2009. ERS analysis based on data from Census of Population, 2000, and the ERS-compiled supermarket directory for the contiguous United States in 2006.
collected on more than 21,000 Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) participants in Kansas failed to find an association between the availability of grocery stores and supermarkets within a census tract and body mass index (BMI) (Ford and Dzewaltowski, 2011). A recent ERS report (Ver Ploeg et al., 2009) suggests that access to a supermarket or large grocery store is a problem for a small percentage of households.
Other observational evidence supports a reduced risk for obesity and related conditions associated with better access to healthy foods. Morland and colleagues (2006) analyzed cross-sectional data collected from men and women participating in the third visit (1993-1995) of the Atherosclerosis Risk in Communities Study to determine whether characteristics of the local food environment were associated with the prevalence of cardiovascular disease risk factors. They found that people with access only to supermarkets or to supermarkets and grocery stores had the lowest rates of obesity and overweight, while those with access only to convenience stores had the highest rates. However, associations for diabetes, high serum cholesterol, and hypertension were not consistently observed.
To examine the association of retail food environments with obesity and diabetes, the California Center for Public Health Advocacy, PolicyLink, and the University of California, Los Angeles, Center for Health Policy Research combined individual-level demographic and health outcome data
from the 2005 California Health Interview Survey (CHIS, 2007) with the locations of retail food outlets. Geographic information system software was used to calculate a Retail Food Environment Index for each adult CHIS respondent within a given radius around his/her home address. It was found that in California, rates of obesity and diabetes were 20 percent higher for those living in the least healthy food environments after controlling for household income, race/ethnicity, age, gender, and physical activity levels (Babey et al., 2008).
Evidence that access to food has a direct impact on pregnancy outcomes is limited. In a study examining associations between diet quality, measured by a Diet Quality Index, among pregnant women and distance from a supermarket, Laraia and colleagues (2004) found that women living more than 4 miles from a supermarket had a twofold increased risk for being in the lowest quartile of the DQI. In another study on access to food and birth outcomes, Lane and colleagues (2008) found that women living in food deserts without access to healthy foods had significantly more low-birth-weight infants than women who had access to supermarkets and a variety of foods.
Although diet is integral to the treatment of diabetes and maintenance of glycemic control, evidence now exists that foods recommended as part of a healthy diabetic diet are in short supply in low-income, nonwhite neighborhoods. To illustrate, Horowitz and colleagues (2004) documented and compared the availability and cost of foods recommended for people with diabetes in East Harlem and the adjacent more affluent and predominantly white Upper East Side neighborhood. They found that the East Harlem neighborhood had a shortage of food markets, and some stores did not carry foods needed for a healthy diabetic diet. Additionally, the neighborhood had few large stores with a variety of foods and fewer stores that carried recommended food items. Further, East Harlem had many more undesirable stores than the more affluent Upper East Side neighborhood. These disparities in availability of healthy foods many be a barrier to diabetes self-management for East Harlem residents.
As described above, limited access to healthy food can influence purchasing behavior. Therefore, it is possible that the availability of food outlets and costs of food items may impact the purchasing power of SNAP allotments for healthy foods under the assumptions of the TFP, which in turn may affect diet-related health outcomes for SNAP participants.
Effectiveness of Addressing Environmental Challenges to Food Access
Environmental interventions to address challenges to food access show some promise. A recent study evaluating the impact of the first full-service supermarket to locate in Harlem in New York City found that the store allocated the same amount of space to fresh fruits, vegetables, fish, and
meat as a typical suburban market, at similar prices (Lavin, 2005). The Pennsylvania Fresh Food Financing Initiative—a statewide financing program designed to increase supermarket development in underserved areas—has funded 78 fresh-food outlets in Pennsylvania, which have increased food access for 500,000 children and adults (Karpyn et al., 2010). More research is need to understand what changes might improve access to food outlets. Approaches at the environmental level might include transportation policies that address both affordability and routes, and incentive/financing programs to increase the number of and quality of supermarkets in low-income, minority communities.
DATA AND ANALYTICAL CHALLENGES
While the evidence is clear that a number of factors create barriers to purchasing healthy foods under the assumptions of the TFP, the relative importance of these factors to determining the feasibility of defining the adequacy of SNAP allotments is uncertain. For example, is geographic proximity to food outlets more or less important than the the quality of food available for purchase? Is the type of food outlet available more or less important than access to public transportation? Understanding these issues is complicated by the following measurement challenges:
• Evidence on time requirements for SNAP participants to prepare healthy meals consistent with the assumptions of the TFP is lacking. Additional research is needed to evaluate the time used to prepare a healthy meal compared with that used for preprepared processed foods.
• Multiple dimensions have an impact on prices paid for food consumed at home by SNAP households. Additional evidence is needed to examine regional differences in the cost of foods purchased by SNAP participants.
• Existing studies consider access to stores almost exclusively from a consumer’s home, not from work, church, or other activities, and therefore may not fully account for the range of access constraints experienced by SNAP participants. Thus further research is needed on the possible impact of limited access to certain food outlets (e.g., supermarkets) on the ability of some SNAP participants to purchase a variety of healthy foods at reasonable cost. Evaluation and assessment of barriers to access should include the degree to which, and for whom, limitations in access to food outlets constrain the SNAP allotment.
• The availability of food stores within a given locale is the most frequently used measure of the food environment. However, identifying
stores can be difficult as information from some sources (e.g., proprietary databases of stores by category, size, and other attributes) may not always be up-to-date and thus may be inconsistent with information from federal sources such as USDA-FNS. Moreover, efforts to improve food access often are designed to solve local problems, which may vary considerably, leading to issues of generalizability.
• For purposes of assessing the adequacy of SNAP allotments, it is necessary to understand
—how prices paid by SNAP recipients vary relative to those paid by other populations;
—what types of foods are purchased by SNAP recipients using their benefits; and
—how benefits received from other federal nutrition assistance programs are used by individual SNAP participants.
Data gaps exist for prices, quantities, and types of foods purchased by SNAP participants using SNAP benefits or other resources by type of food outlet. If these data could be linked to information on basic household factors such as ages of SNAP recipients, numbers of children, region of the country, and rural or urban setting, analyses could be carried out to assess which individual, household, and environmental factors are most important in defining the adequacy of SNAP allotments.
SUMMARY OF FINDINGS AND CONCLUSIONS
The evidence reviewed in this chapter reveals a number of individual, household, and environmental factors that can influence the adequacy of SNAP allotments. The committee’s findings based on this evidence take into account the robustness of the evidence and the likely impact of a given factor on the feasibility of an evidence-based definition of allotment adequacy. Although the committee acknowledges that most of the observational studies evaluated are cross-sectional, the findings considered collectively and in the context of the totality of the available evidence suggest that the factors with the greatest influence on the adequacy of SNAP allotments are availability of time to purchase and prepare meals, geographic variation in prices, and access to food outlets (at the environmental level). Consideration of these factors can inform the development of a definition of the adequacy of SNAP allotments and transform implicit assumptions underlying the determination of SNAP benefits into explicit statements that can be evaluated for SNAP participants. Factors for which the evidence is not strong enough to warrant their consideration in analyses to support an evidence-based assessment of the adequacy of SNAP allotments include nutrition
knowledge, skills, and abilities, and transportation (at the individual/household level). The committee notes, however, that some factors, such as access to personal transportation, may be beyond the scope of USDA-FNS to use in an assessment of allotment adequacy.
Availability of Time to Purchase and Prepare Meals
The committee’s review of evidence on the amount of time needed by most households, in particular those with a working head of household, to purchase and prepare food for healthy meals is inconsistent with the assumptions of the TFP. In addition, the resource constraints experienced by many low-income households, such as reduced transportation access to food outlets, widen the disconnect between the time needed to prepare meals consistent with the TFP and the reality of the amount of time available to these households. Further, evidence from analyses of household food expenditures suggests that the result of failing to account for labor costs is severe underestimation of the real cost of food for low-income households.
Geographic Variation in Prices
The evidence reviewed by the committee shows that food prices vary substantially across geographic regions of the country and between rural and urban areas. Yet the cost of the TFP, which serves as the basis for determining the maximum SNAP benefit, is not adjusted by geographic region, with the exception of Alaska and Hawaii. SNAP participants in locales with higher food prices would likely have greater difficulty than those in areas with lower food prices in purchasing the types and amounts of foods determined in the TFP as adequate to meet their needs for a healthy diet. The evidence points further to a lack of data on the magnitude of the impact of differences in food prices across locales on the ability of SNAP participants to purchase sufficient quantities of healthy foods based on household composition assumptions (Gundersen et al., 2011).
Access to Food Outlets
Overall, the evidence reviewed by the committee suggests that access to supermarkets is lower among low-income and minority populations than other population groups and that individuals without access to supermarkets experience greater disparity in availability of healthier foods, such as fresh fruits and vegetables, in their neighborhood food outlets. In addition, a lack of transportation infrastructure was found to be the most defining characteristic of limited food access for small-town and rural areas.
Nutrition Knowledge, Skills, and Abilities
The evidence reviewed by the committee suggests that evaluations of nutrition education programs for low-income participants that include skill-based education show change in behavioral outcomes. This finding lends credence to the theory that nutrition knowledge and skills are limited and that education is necessary to assist households in maximizing the purchasing power of their SNAP benefits. However, evidence on the influence of nutrition knowledge and skills on the ability of SNAP participants to purchase and prepare healthy foods consistent with the assumptions of the TFP is insufficient to support a conclusion about the relevance of these factors to an evidence-based definition of the adequacy of SNAP allotments. Assessing the nutrition skills of the SNAP population directly (i.e., through direct observation) would be difficult at the population level. However, several variables likely to be associated with skill level could be assessed—for example, skills normally used (e.g., using grocery store lists, planning meals, using recipes with raw ingredients), perceived level of these skills, and self-efficacy to perform the skills.
Andreyeva, T., D. M. Blumenthal, M. B. Schwartz, M. W. Long, and K. D. Brownell. 2008. MarketWatch: Availability and prices of foods across stores and neighborhoods: The case of New Haven, Connecticut. Health Affairs 27(5):1381-1388.
Andreyeva, T., F. J. Chaloupka, and K. O. Brownell. 2011. Estimating the potential of taxes on sugar-sweetened beverages to reduce consumption and generate revenue. Preventive Medicine 52:413-416.
Arnold, C. G., and J. Sobal. 2000. Food practices and nutrition knowledge after graduation from the Expanded Food and Nutrition Education Program (EFNEP). Journal of Nutrition Education and Behavior 32(3):130-138.
Atkinson, N. L., A. S. Billing, S. M. Desmond, R. S. Gold, and A. Tournas-Hardt. 2007. Assessment of the nutrition and physical activity education needs of low-income, rural mothers: Can technology play a role? Journal of Community Health 32(4):245-267.
Atkinson, N. L., S. M. Desmond, S. L. Saperstein, A. S. Billing, R. S. Gold, and A. Tournas-Hardt. 2010. Assets, challenges, and the potential of technology for nutrition education in rural communities. Journal of Nutrition Education and Behavior 42(6):410-416.
Babey, S. H., A. L. Diamant, T. A. Hastert, S. Harvey, H. Goldstein, R. Flourney, R. Banthia, V. Rubin, and S. Treuhaft. 2008. Designed for disease: The link between local food environments and obesity and diabetes. http://www.healthpolicy.ucla.edu/pubs/files/Designed_for_Disease_050108.pdf (accessed June 14, 2012).
Backman, D., V. Scruggs, A. A. Atiedu, S. Bowie, L. Bye, A. Dennis, M. Hall, A. Ossa, S. Wertlieb, and S. B. Foerster. 2011. Using a toolbox of tailored educational lessons to improve fruit, vegetable, and physical activity behaviors among African American women in California. Journal of Nutrition Education and Behavior 43(4 Suppl. 2):S75-S85.
Bauer, K. W., M. O. Hearst, K. Escoto, J. M. Berge, and D. Neumark-Sztainer. 2012. Parental employment and work-family stress: Associations with family food environments. Social Science and Medicine 75(3):496-504.
Becker, G. S. 1965. A theory of the allocation of time. Economic Journal 75(299):493-517.
Bell, L., F. Tao, J. Anthony, C. Logan, R. Ledsky, M. Ferreira, and A. Brown. 2006. Food stamp nutrition education systems review: Final report. Submitted by Abt Associates, Inc. to U.S. Department of Agriculture, Food and Nutrition Service, Alexandria, VA. http://www.fns.usda.gov/ora/menu/published/NutritionEducation/Files/FSNESystemsReview.pdf (accessed June 7, 2012).
Bergman, M. 1997. Improving birth outcomes with nutrition intervention. Topics in Clinical Nutrition 13(1):74-79.
Beshara, M., A. Hutchinson, and C. Wilson. 2010. Preparing meals under time stress. The experience of working mothers. Appetite 55(3):695-700.
Birch, L. L. 1999. Development of food preferences. Annual Review of Nutrition 19:41-62.
Bitler, M., and S. J. Haider. 2011. An economic view of food deserts in the United States. Journal of Policy Analysis and Management 30(1):153-176.
Bjorn, A., B. J. Lee, B. Born, P. Monsivais, S. Kantor, and R. Sayre. 2008. At the table with the Seattle-King County Acting Food Policy Council: Issue Paper No. 4: Mapping food insecurity and access in Seattle and King County. http://www.b-sustainable.org/builtenvironment/access-to-local-food-by-neighborhood/AFPCFoodAccessIssuePaperNo.4_000.pdf (accessed July 24, 2012).
Blanchard, T., and T. Lyson. 2002. Access to low cost groceries in nonmetropolitan counties: Large retailers and the creation of food deserts. http://srdc.msstate.edu/trainings/presentations_archive/2002/2002_blanchard.pdf (accessed June 7, 2012).
Blanck, H. M., O. M. Thompson, L. Nebeling, and A. L. Yaroch. 2011. Improving fruit and vegetable consumption: Use of farm-to-consumer venues among U.S. adults. Preventing Chronic Disease 8(2):A49.
Briggs, S., A. Fisher, M. Lott, S. Miller, and N. Tessman. 2010. Real food, real choice: Connecting SNAP recipients with farmers markets. Portland, OR: Community Food Security Coalition & Farmers Market Coalition. http://www.foodsecurity.org/pub/RealFoodRealChoice_SNAP_FarmersMarkets.pdf (accessed April 8, 2013).
Burney, J., and B. Haughton. 2002. EFNEP: A nutrition education program that demonstrates cost-benefit. Journal of the American Dietetic Association 102(1):39-45.
Carlson, A., and E. Frazao. 2012. Are healthy foods really more expensive? It depends on how you measure the price, EIB-96. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/eib-economic-information-bulletin/eib96.aspx (accessed July 5, 2012).
Carlson, A., M. Lino, W. Y. Juan, K. Hanson, and P. P. Basiotis. 2007. Thrifty Food Plan, 2006, CNPP-19. Washington, DC: USDA, CNPP. http://www.cnpp.usda.gov/Publications/FoodPlans/MiscPubs/TFP2006Report.pdf (accessed May 31, 2012).
Cason, K. L., and B. N. Logan. 2006. Educational intervention improves 4th-grade school-children’s nutrition and physical activity knowledge and behaviors. Topics in Clinical Nutrition 21(3):234-240.
Cason, K. L., T. R. Wenrich, and N. Lv. 2005. Nutrition Mission—A multimedia educational tool for youth grades 4-6. Journal of Extension 43(3). Published online at: http://www.joe.org/joe/2005june/tt5.php (accessed April 8, 2013).
Cassady, D., K. M. Jetter, and J. Culp. 2007. Is price a barrier to eating more fruits and vegetables for low-income families? Journal of the American Dietetic Association 107(11):1909-1915.
Castner, L., and J. Henke. 2011. Benefit redemption patterns in the Supplemental Nutrition Assistance Programs. Submitted by Mathematica Policy Research, Inc. to U.S. Department of Agriculture, Food and Nutrition Service, Alexandria, VA. http://www.fns.usda.gov/ora/menu/Published/snap/FILES/ProgramOperations/ARRASpendingPatterns.pdf (accessed June 7, 2012).
Cheadle, A., B. M. Psaty, S. Curry, E. Wagner, P. Diehr, T. Koepsell, and A. Kristal. 1991. Community-level comparisons between the grocery store environment and individual dietary practices. Preventive Medicine 20(2):250-261.
CHIS (California Health Interview Survey). 2007. CHIS 2005 adult public use file. Release 1 [computer file]. Los Angeles, CA: UCLA Center for Health Policy Research, January.
Clifton, K. J. 2004. Mobility strategies and food shopping for low-income families: A case study. Journal of Planning Education and Research 23(4):402-413.
CNPP (Center for Nutrition Policy and Promotion). 2000. Recipes and tips for healthy, thrifty meals. Washington, DC: USDA, CNPP. http://www.cnpp.usda.gov/publications/foodplans/miscpubs/foodplansrecipebook.pdf (accessed June 14, 2012).
Cole, N. 1997. Evaluation of the expanded EBT demonstration in Maryland. Patterns of food stamp and cash welfare benefit redemption. Submitted by Abt Associates, Inc., to the U.S. Department of Agriculture, Food and Consumer Service, Alexandria, VA.
Coleman-Jensen, A., M. Nord, M. Andrews, and S. Carlson. 2012. Household food security in the United States in 2011. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/err-economic-research-report/err141.aspx (accessed September 6, 2012).
Contento, I. R. 2007. Nutrition education: Linking research, theory, and practice. Sudbury, MA: Jones and Bartlett Publishers, Inc.
Cox, R. H., A. H. White, and C. K. Gaylord. 2003. A video lesson series is effective in changing the dietary intakes and food-related behaviors of low-income homemakers. Journal of the American Dietetic Association 103(11):1488-1493.
Dachner, N., L. Ricciuto, S. I. Kirkpatrick, and V. Tarasuk. 2010. Food purchasing and food insecurity among low-income families in Toronto. Canadian Journal of Dietetic Practice and Research 71(3):e50-e56.
Davis, G. C., and W. You. 2010. The Thrifty Food Plan is not thrifty when labor cost is considered. Journal of Nutrition 140(4):854-857.
Davis, G. C., and W. You. 2011. Not enough money or not enough time to satisfy the Thrifty Food Plan? A cost difference approach for estimating a money-time threshold. Food Policy 36(2):101-107.
Del Tredici, A. M., A. Block Joy, C. L. Omelich, and S. G. Laughlin. 1988. Evaluation study of the California expanded food and nutrition education program: 24-hour food recall data. Journal of the American Dietetic Association 88(2):185-190.
Devine, C. M., W. S. Wolfe, E. A. Frongillo Jr, and C. A. Bisogni. 1999. Life-course events and experiences: Association with fruit and vegetable consumption in 3 ethnic groups. Journal of the American Dietetic Association 99(3):309-314.
Devine, C. M., M. M. Connors, J. Sobal, and C. A. Bisogni. 2003. Sandwiching it in: Spillover of work onto food choices and family roles in low- and moderate-income urban households. Social Science and Medicine 56(3):617-630.
Devine, C. M., T. J. Farrell, C. E. Blake, M. Jastran, E. Wethington, and C. A. Bisogni. 2009. Work conditions and the food choice coping strategies of employed parents. Journal of Nutrition Education and Behavior 41(5):365-370.
Dhokarh, R., D. A. Himmelgreen, Y. K. Peng, S. Segura-Perez, A. Hromi-Fiedler, and R. Perez-Escamilla. 2011. Food insecurity is associated with acculturation and social networks in Puerto Rican households. Journal of Nutrition Education and Behavior 43(4):288-294.
Dickin, K. L., J. S. Dollahite, and J. P. Habicht. 2005. Nutrition behavior change among EFNEP participants is higher at sites that are well managed and whose front-line nutrition educators value the program. Journal of Nutrition 135(9):2199-2205.
Dinour, L. M., D. Bergen, and M.-C. Yeh. 2007. The food insecurity-obesity paradox: A review of the literature and the role food stamps may play. Journal of the American Dietetic Association 107(11):1952-1961.
Dollahite, J., C. Olson, and M. Scott-Pierce. 2003. The impact of nutrition education on food insecurity among low-income participants in EFNEP. Family and Consumer Sciences Research Journal 32(2):127-139.
Dollahite, J., D. Kenkel, and C. S. Thompson. 2008. An economic evaluation of the Expanded Food and Nutrition Education Program. Journal of Nutrition Education and Behavior 40(3):134-143.
Dong, D., and B. H. Lin. 2009. Fruit and vegetable consumption by low-income Americans: Would a price reduction make a difference?, ERR-70. Washington, DC: USDA, ERS.
Drewnowski, A. 1997. Taste preferences and food intake. Annual Review of Nutrition 17(1):237-253.
Drewnowski, A. 2010. The Nutrient Rich Foods Index helps to identify healthy, affordable foods. American Journal of Clinical Nutrition 91(4):1095S-1101S.
Drewnowski, A., and P. Eichelsdoerfer. 2010. Can low-income Americans afford a healthy diet? Nutrition Today 44(6):246-249.
Drewnowski, A., and A. S. Levine. 2003. Sugar and fat—From genes to culture. Journal of Nutrition 133(3):829S-830S.
Drewnowski, A., and S. E. Specter. 2004. Poverty and obesity: The role of energy density and energy costs. American Journal of Clinical Nutrition 79(1):6-16.
Drewnowski, A., S. A. Henderson, A. Levine, and C. Hann. 1999. Taste and food preferences as predictors of dietary practices in young women. Public Health Nutrition 2(4):513-519.
Dubowitz, T., D. Acevedo-Garcia, J. Salkeld, A. C. Lindsay, S. V. Subramanian, and K. E. Peterson. 2007. Lifecourse, immigrant status and acculturation in food purchasing and preparation among low-income mothers. Public Health Nutrition 10(4):396-404.
Eicher-Miller, H. A., A. C. Mason, A. R. Abbott, G. P. McCabe, and C. J. Boushey. 2009. The effect of Food Stamp nutrition education on the food insecurity of low-income women participants. Journal of Nutrition Education and Behavior 41(3):161-168.
Ellis, J., M. A. Johnson, J. G. Fischer, and J. L. Hargrove. 2005. Nutrition and health education intervention for whole grain foods in the Georgia older Americans nutrition programs. Journal of Nutrition for the Elderly 24(3):67-83.
Emond, J. A., H. N. Madanat, and G. X. Ayala. 2012. Do Latino and non-Latino grocery stores differ in the availability and affordability of healthy food items in a low-income, metropolitan region? Public Health Nutrition 15(2):360-369.
ERS (Economic Research Service). 2012. Food desert locator. http://www.ers.usda.gov/data/fooddesert/documentation.html (accessed June 14, 2012).
Evans, A., S. Chow, R. Jennings, J. Dave, K. Scoblick, K. R. Sterba, and J. Loyo. 2011. Traditional foods and practices of Spanish-speaking Latina mothers influence the home food environment: Implications for future interventions. Journal of the American Dietetic Association 111(7):1031-1038.
Feather, P. M. 2003. Valuing food store access: Policy implications for the food stamp program. American Journal of Agricultural Economics 84(1):162-172.
Fisher, B. D., and D. S. Strogatz. 1999. Community measures of low-fat milk consumption: Comparing store shelves with households. American Journal of Public Health 89(2):235-237.
Fitzgerald, N., A. Hromi-Fiedler, S. Segura-Perez, and R. Perez-Escamilla. 2011. Food insecurity is related to increased risk of type 2 diabetes among Latinas. Ethnicity & Disease 21(3):328-334.
FNS (Food and Nutrition Service). 2011. We welcome SNAP putting healthy food within reach: 2010 annual report. Alexandria, VA: USDA, FNS. http://www.fns.usda.gov/snap/retailers/pdfs/2010-annual-report.pdf (accessed August 28, 2012).
FNS. 2012. Supplemental Nutrition Assistance Program: Nutrition education. http://www.fns.usda.gov/snap/nutrition_education/default.htm (accessed June 14, 2012).
Ford, P. B., and D. A. Dzewaltowski. 2011. Neighborhood deprivation, supermarket availability, and BMI in low-income women: A multilevel analysis. Journal of Community Health 36(5):785-796.
Foster, G. D., S. Sherman, K. E. Borradaile, K. M. Grundy, S. S. Vander Veur, J. Nachmani, A. Karpyn, S. Kumanyika, and J. Shults. 2008. A policy-based school intervention to prevent overweight and obesity. Pediatrics 121(4):e794-e802.
Franco, M., A. Nandi, T. Glass, and A. Diez-Roux. 2007. Smoke before food: A tale of Baltimore city. American Journal of Public Health 97(7):1178.
Frongillo, E. A, Jr., C. M. Olson, B. S. Rauschenbach, and A. Kendall. 1997. Nutritional consequences of food insecurity in a rural New York state county. Submitted by the Division of Nutritional Sciences, Cornell University to the Institute for Research on Poverty, University of Wisconsin–Madison. http://irp.wisc.edu/publications/dps/pdfs/dp112097.pdf (accessed July 10, 2012).
Gabor, V., S. Cates, S. Gleason, V. Long, G. A. Clarke, J. Blitstein, P. Williams, L. Bell, J. Hersey, and M. Ball. 2012. SNAP Education and Evaluation Study (Wave 1): Final report. Submitted by Altarum Institute to U.S. Department of Agriculture, Food and Nutrition Service, Alexandria, VA. http://www.fns.usda.gov/ora/menu/Published/snap/FILES/Other/SNAPEdWaveI.pdf (accessed June 14, 2012).
GAO (Government Accountability Office). 2004. Nutrition education: USDA provides services through multiple programs, but stronger linkages among efforts are needed. Washington, DC: GAO. http://www.gao.gov/new.items/d04528.pdf (accessed June 14, 2012).
Gentry, A. L., J. G. Grzywacz, S. A. Quandt, S. W. Davis, and T. A. Arcury. 2007. Housing quality among North Carolina farmworker families. Journal of Agricultural Safety and Health 13(3):323-337.
Gleason, P., A. Rangarajan, and C. Olson. 2000. Dietary intake and dietary attitudes among food stamp participants and other low-income individuals. Submitted by Mathematica Policy Research, Inc. to U.S. Department of Agriculture, Food and Nutrition Service, Alexandria, VA. http://www.fns.usda.gov/ora/menu/published/NutritionEducation/Files/FSPDiet.pdf (accessed February 9, 2012).
Gregory, C. A., and A. Coleman-Jensen. 2011. Do food prices affect food security? Evidence from the CPS 2002-2006. Paper presented at the Agricultural and Applied Economics Association 2011 Annual Meeting, Pittsburgh, PA.
Gundersen, C., B. Kreider, and J. Pepper. 2011. The economics of food insecurity in the United States. Applied Economic Perspectives and Policy 33(3):281-303.
Guthrie, J. F., E. Stommes, and J. Voichick. 2006. Evaluating Food Stamp nutrition education: Issues and opportunities. Journal of Nutrition Education and Behavior 38(1):6-11.
Hadley, C., A. Zodhiates, and D. W. Sellen. 2007. Acculturation, economics and food insecurity among refugees resettled in the USA: A case study of West African refugees. Public Health Nutrition 10(4):405-412.
Hanson, K., and M. Andrews. 2008. Rising food prices take a bite out of food stamp benefits, EIB-41. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/eib-economic-information-bulletin/eib41.aspx (accessed July 5, 2012).
Hausman, J., and E. Leibtag. 2007. Consumer benefits from increased competition in shopping outlets: Measuring the effect of Wal-Mart. Journal of Applied Econometrics 22(7):1157-1177.
Hersey, J., J. Anliker, C. Miller, R. M. Mullis, S. Daugherty, S. Das, C. R. Bray, P. Dennee, M. Sigman-Grant, and H. O. Thomas. 2001. Food shopping practices are associated with dietary quality in low-income households. Journal of Nutrition Education and Behavior 33(Suppl.):S16-S26.
Horowitz, C. R., K. A. Colson, P. L. Hebert, and K. Lancaster. 2004. Barriers to buying healthy foods for people with diabetes: Evidence of environmental disparities. American Journal of Public Health 94(9):1549-1554.
Hosler, A. S., D. T. Rajulu, B. L. Fredrick, and A. E. Ronsani. 2008. Assessing retail fruit and vegetable availability in urban and rural underserved communities. Preventing Chronic Disease 5(4):A123.
Hromi-Fiedler, A., A. Bermúdez-Millán, S. Segura-Pérez, and R. Pérez-Escamilla. 2012. Nutrient and food intakes differ among Latina subgroups during pregnancy. Public Health Nutrition 15(2):341-351.
IOM (Institute of Medicine). 2011. Hunger and obesity: Understanding a food insecurity paradigm: Workshop summary. Washington, DC: The National Academies Press.
Izumi, B. T., S. N. Zenk, A. J. Schulz, G. B. Mentz, and C. Wilson. 2011. Associations between neighborhood availability and individual consumption of dark-green and orange vegetables among ethnically diverse adults in Detroit. Journal of the American Dietetic Association 111(2):274-279.
Jabs, J., and C. M. Devine. 2006. Time scarcity and food choices: An overview. Appetite 47(2):196-204.
Jetter, K. M., and D. L. Cassady. 2006. The availability and cost of healthier food alternatives. American Journal of Preventive Medicine 30(1):38-44.
Jilcott, S. B., E. D. Wall-Bassett, S. C. Burke, and J. B. Moore. 2011. Associations between food insecurity, Supplemental Nutrition Assistance Program (SNAP) benefits, and body mass index among adult females. Journal of the American Dietetic Association 111(11):1741-1745.
Jones, S. J., and E. A. Frongillo. 2006. The modifying effects of Food Stamp Program participation on the relation between food insecurity and weight change in women. Journal of Nutrition 136(4):1091-1094.
Joy, A. B., N. Feldman, M. L. Fujii, L. Garcia, M. Hudes, R. Mitchell, S. Bunch, and D. Metz. 1999. Food stamp recipients eat more vegetables after viewing nutrition videos. California Agriculture 53(5):24-28.
Karpyn, A., M. Manon, S. Treuhaft, T. Giang, C. Harries, and K. McCoubrey. 2010. Policy solutions to the “grocery gap.” Health Affairs 29(3):473-480.
Kaufman, P. 1999. Rural poor have less access to supermarkets, large grocery stores. Rural Development Perpectives 13(3):19-62, http://www.ers.usda.gov/publications/rdp/rdp1098/ (accessed June 14, 2012).
Keihner, A. J., R. Meigs, S. Sugerman, D. Backman, T. Garbolino, and P. Mitchell. 2011. The Power Play! Campaign’s school idea & resource kits improve determinants of fruit and vegetable intake and physical activity among fourth- and fifth-grade children. Journal of Nutrition Education and Behavior 43(4 Suppl. 2):S122-S129.
Kempson, K., D. P. Keenan, P. S. Sadani, and A. Adler. 2003. Maintaining food sufficiency: Coping strategies identified by limited-resource individuals versus nutrition educators. Journal of Nutrition Education and Behavior 35(4):179-188.
Landers, P., and C. Shults. 2008. Pots, pans, and kitchen equipment: Do low-income clients have adequate tools for cooking? Journal of Extension 46(1), http://www.joe.org/joe/2008february/rb4.php (accessed May 31, 2012).
Lane, S. D., R. H. Keefe, R. Rubinstein, B. A. Levandowski, N. Webster, D. A. Cibula, A. K. Boahene, O. Dele-Michael, D. Carter, T. Jones, M. Wojtowycz, and J. Brill. 2008. Structural violence, urban retail food markets, and low birth weight. Health and Place 14(3):415-423.
Laraia, B. A., A. M. Siega-Riz, J. S. Kaufman, and S. J. Jones. 2004. Proximity of supermarkets is positively associated with diet quality index for pregnancy. Preventive Medicine 39(5):869-875.
Laroche, H. H., R. B. Wallace, L. Snetselaar, S. L. Hillis, and L. M. Steffen. 2012. Changes in diet behavior when adults become parents. Journal of the Academy of Nutrition and Dietetics 112(6):832-839.
Larson, N. I., and M. T. Story. 2011. Food insecurity and weight status among U.S. children and families: A review of the literature. American Journal of Preventive Medicine 40(2):166-173.
Larson, N. I., M. T. Story, and M. C. Nelson. 2009. Neighborhood environments: Disparities in access to healthy foods in the U.S. American Journal of Preventive Medicine 36(1):74-81.
Lavin, M. 2005. Supermarket access and consumer well-being: The case of Pathmark in Harlem. International Journal of Retail and Distribution Management 33(5):388-398.
Leibtag, E. 2005. Where you shop matters: Store formats drive variation in retail food prices. Amber Waves, http://webarchives.cdlib.org/sw1vh5dg3r/http://www.ers.usda.gov/AmberWaves/November05/Features/WhereYouShop.htm (accessed July 5, 2012).
Leibtag, E. 2012. Tracking purchase behavior of low-income households: Assessment of data needs. Presented at the Institute of Medicine Workshop on Defining the Adequacy of Food Resources and SNAP Allotments. Washington, DC, March 28.
Leibtag, E., and A. Kumcu. 2011. The WIC fruit and vegetable cash voucher: Does regional price variation affect buying power? EIB-75. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/eib-economic-information-bulletin/eib75.aspx (accessed July 5, 2012).
Leibtag, E., C. Baker, and P. Dutko. 2010. How much lower are prices at discount stores? An examination of retail food prices. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/err-economic-research-report/err105.aspx (accessed July 5, 2012).
Liese, A. D., K. E. Weis, D. Pluto, E. Smith, and A. Lawson. 2007. Food store types, availability, and cost of foods in a rural environment. Journal of the American Dietetic Association 107(11):1916-1923.
Lipsky, L. M. 2009. Are energy-dense foods really cheaper? Reexamining the relation between food price and energy density. American Journal of Clinical Nutrition 90(5):1397-1401.
Lopez-Class, M., and A. S. Hosler. 2010. Assessment of community food resources: A Latino neighborhood study in upstate New York. Journal of Poverty 14(4):369-381.
Mammen, S., J. W. Bauer, and L. Richards. 2009. Understanding persistent food insecurity: A paradox of place and circumstance. Social Indicators Research 92(1):151-168.
Mancino, L., and C. Newman. 2007. Who has time to cook? How family resources influence food preparation, ERR-40. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/err-economic-research-report/err40.aspx (accessed July 5, 2012).
Mantovani, R. E., and J. Welsh. 1996. Authorized Food Retailer Characteristics Study. Technical Report III Geographic Analysis of Retailer Access. Submitted by Macro International, Inc. to U.S. Department of Agriculture, Food and Nutrition Service, Alexandria, VA.
Mazur, R. E., G. S. Marquis, and H. H. Jensen. 2003. Diet and food insufficiency among Hispanic youths: Acculturation and socioeconomic factors in the third National Health and Nutrition Examination Survey. American Journal of Clinical Nutrition 78(6):1120-1127.
Michimi, A., and M. C. Wimberly. 2010. Associations of supermarket accessibility with obesity and fruit and vegetable consumption in the coterminous United States. International Journal of Health Geographics 9:49. Published online at: http://www.ijhealthgeographics.com/content/pdf/1476-072X-9-49.pdf (accessed April 8, 2013).
Monsivais, P., J. McLain, and A. Drewnowski. 2010. The rising disparity in the price of healthful foods: 2004-2008. Food Policy 35(6):514-520.
Moore, L. V., and A. V. Diez Roux. 2006. Associations of neighborhood characteristics with the location and type of food stores. American Journal of Public Health 96(2):325-331.
Morland, K., and S. Filomena. 2007. Disparities in the availability of fruits and vegetables between racially segregated urban neighbourhoods. Public Health Nutrition 10(12):1481-1489.
Morland, K., A. V. Diez Roux, and S. Wing. 2006. Supermarkets, other food stores, and obesity: The Atherosclerosis Risk in Communities Study. American Journal of Preventive Medicine 30(4):333-339.
Morton, L. W., and T. C. Blanchard. 2007. Starved for access: Life in rural America’s food deserts. Rural Realities 1(4), http://www.ruralsociology.org/wp-content/uploads/2012/03/Rural-Realities-1-4.pdf (accessed June 14, 2012).
Mothersbaugh, D. L., R. O. Herrmann, and R. H. Warland. 1993. Perceived time pressure and recommended dietary practices: The moderating effect of knowledge of nutrition. Journal of Consumer Affairs 27(1):106-126.
NIFA (National Institute of Food and Agriculture). 2009a. About EFNEP. http://www.nifa.usda.gov/nea/food/efnep/about.html (accessed June 14, 2012).
NIFA. 2009b. About SNAP-Ed. http://www.nifa.usda.gov/nea/food/fsne/about.html (accessed July 26, 2012).
NIFA. 2012. EFNEP Nutrition Education Evaluation and Reporting System. http://www.csrees.usda.gov/nea/food/efnep/neers5/neers5.html (accessed June 14, 2012).
Ohls, J. C., M. Ponza, A. Moreno, A. Zambrowski, and R. Cohen. 1999. Food stamp participants’ access to food retailers. Submitted by Mathematica Policy Research, Inc., to the U.S. Department of Agriculture, Food and Nutrition Service, Alexandria, VA.
Olander, C., E. Jones, and S. Carlson. 2006. An analysis of food stamp redemption patterns. Office of Analysis, Nutrition, and Evaluation, Alexandria, VA.
Olson, C. M., C. F. Bove, and E. O. Miller. 2007. Growing up poor: Long-term implications for eating patterns and body weight. Appetite 49(1):198-207.
Pollak, R. A. 2011. Allocating time: Individuals’ technologies, household technology, perfect substitutions, and specialization, NBER Working Paper No. 17529. http://www.nber.org/papers/w17529 (accessed September 6, 2012).
Powell, L. M., S. Slater, D. Mirtcheva, Y. Bao, and F. J. Chaloupka. 2007. Food store availability and neighborhood characteristics in the United States. Preventive Medicine 44(3):189-195.
Rose, D. 2007. Food stamps, the Thrifty Food Plan, and meal preparation: The importance of the time dimension for U.S. nutrition policy. Journal of Nutrition Education and Behavior 39(4):226-232.
Rose, D., and R. Richards. 2004. Food store access and household fruit and vegetable use among participants in the U.S. Food Stamp Program. Public Health Nutrition 7(8):1081-1088.
Rose, D., J. N. Bodor, P. L. Hutchinson, and C. M. Swalm. 2010. The importance of a multidimensional approach for studying the links between food access and consumption. Journal of Nutrition 140(6):1170-1174.
Sharkey, J. R., and S. Horel. 2008. Neighborhood socioeconomic deprivation and minority composition are associated with better potential spatial access to the ground-truthed food environment in a large rural area. Journal of Nutrition 138(3):620-627.
Sharkey, J. R., and N. E. Schoenberg. 2005. Prospective study of black-white differences in food insufficiency among homebound elders. Journal of Aging and Health 17(4):507-527.
Sharkey, J. R., S. Horel, D. Han, and J. C. Huber Jr. 2009. Association between neighborhood need and spatial access to food stores and fast food restaurants in neighborhoods of Colonias. International Journal of Health Geographics 8(1):9. Published online at: http:///www.ij-healthgeographics.com/content/pdf/1476-072X-8-9.pdf (accessed April 8, 2013).
Sharkey, J. R., S. Horel, and W. R. Dean. 2010. Neighborhood deprivation, vehicle ownership, and potential spatial access to a variety of fruits and vegetables in a large rural area in Texas. International Journal of Health Geographics 9: Article no. 26.
Silk, K. J., J. Sherry, B. Winn, N. Keesecker, M. A. Horodynski, and A. Sayir. 2008. Increasing nutrition literacy: Testing the effectiveness of print, web site, and game modalities. Journal of Nutrition Education and Behavior 40(1):3-10.
Sobal, J., and C. A. Bisogni. 2009. Constructing food choice decisions. Annals of Behavioral Medicine 38(Suppl.):S37-S46.
Stewart, H., and D. Dong. 2011. Variation in retail costs for fresh vegetables and salty snacks across communities in the United States. Food Policy 36(2):128-135.
Todd, J. E., L. Mancino, E. Leibtag, and C. Tripodo. 2010. Methodology behind the quarterly food-at-home price database, Technical Bulletin No. 1926. Washington, DC: USDA, ERS. http://www.ers.usda.gov/Publications/TB1926 (accessed July 5, 2012).
Todd, J., E. Leibtag, and C. Penberthy. 2011. Geographic differences in the relative price of healthy foods, EIB-78. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/eib-economic-information-bulletin/eib78.aspx (accessed July 24, 2012).
Townsend, M. S., M. Johns, M. K. Shilts, and L. Farfan-Ramirez. 2006. Evaluation of a USDA nutrition education program for low-income youth. Journal of Nutrition Education and Behavior 38(1):30-41.
USDA and HHS (U.S. Department of Agriculture and U.S. Department of Health and Human Services). 2010. Dietary Guidelines for Americans, 2010. 7th ed. Washington, DC: Government Printing Office. http://www.health.gov/dietaryguidelines/2010.asp (accessed June 11, 2012).
Velásquez-Melendez, G., M. M. Schlüssel, A. S. Brito, A. A. M. Silva, J. D. Lopes-Filho, and G. Kac. 2011. Mild but not light or severe food insecurity is associated with obesity among Brazilian women. Journal of Nutrition 141(5):898-902.
Ver Ploeg, M., V. Breneman, T. Farrigan, K. Hamrick, D. Hopkins, P. Kaufman, B. H. Lin, M. Nord, T. A. Smith, R. Williams, K. Kinnison, C. Olander, A. Singh, and E. Tuckermanty. 2009. Access to affordable and nutritious food—Measuring and understanding food deserts and their consequences: Report to Congress. Washington, DC: USDA, ERS. http://www.ers.usda.gov/publications/ap-administrative-publication/ap-036.aspx (accessed June 14, 2012).
Webber, C. B., J. Sobal, and J. S. Dollahite. 2007. Physical disabilities and food access among limited resource households. Disability Studies Quarterly 27(3). http://dsq-sds.org/article/view/20/20 (accessed August 16, 2012).
Wiig, K., and C. Smith. 2009. The art of grocery shopping on a food stamp budget: Factors influencing the food choices of low-income women as they try to make ends meet. Public Health Nutrition 12(10):1726-1734.
Wiig Dammann, K., and C. Smith. 2009. Factors affecting low-income women’s food choices and the perceived impact of dietary intake and socioeconomic status on their health and weight. Journal of Nutrition Education and Behavior 41(4):242-253.
Zenk, S. N., A. J. Schulz, B. A. Israel, S. A. James, S. M. Bao, and M. L. Wilson. 2005. Neighborhood racial composition, neighborhood poverty, and the spatial accessibility of supermarkets in metropolitan Detroit. American Journal of Public Health 95(4):660-667.