![]()
This chapter begins with a discussion of what access to health care means. It then presents a discussion of how active-duty military and veterans access their health care through the Department of Defense (DOD) and the Department of Veterans Affairs (VA) health care systems with a focus on mental-health care. Mental-health issues are highlighted because of the large numbers of returning Operation Enduring Freedom (OEF) and Operation Iraqi Freedom (OIF) that have been diagnosed with posttraumatic stress disorder (PTSD) and other mental-health disorders (see Chapter 4). The chapter then presents a discussion of issues related to fragmentation of care and disparities in care, in particular, disparities based on gender and ethnicity. The chapter highlights many of the barriers to care and examines the DOD’s and VA’s programmatic responses to those barriers; finally, the committee provides its recommendations. Returning OEF and OIF military and veterans have been diagnosed with a host of physical- and mental-health outcomes (as documented in earlier chapters of this report). The DOD and VA health care systems have been struggling in certain health care areas to provide timely care to the over 2 million service members who have been deployed since 2001. While the DOD and VA have excelled in providing acute care and care to patients with polytrauma, areas such as mental-health care services have fallen behind.
As documented and discussed in several chapters of this report and other sources, OEF and OIF deployed service members are returning with high rates of mental-health disorders; concerns regarding the availability and adequacy of mental-health services have been highlighted in numerous reports (e.g., Tanielian and Jaycox, 2008). That is troubling as untreated mental-health disorders are strongly linked to numerous adverse outcomes (see Chapter 4).
A 2009 report of mental-health care for OEF and OIF veterans (Burnam et al., 2009) found that the mental-health workforce had insufficient capacity to address the mental-health needs of service members returning home. The study also found that the workforce lacked sufficient training in evidence-based practices and that there were inadequate organizational systems and tools to support mental-health quality improvements. Other concerns about VA health care have been highlighted and include perceptions that programs and service options are not adequate or uniform across different locations, facilities or providers, that services are not welcoming to certain groups (e.g., women and minorities) (GAO, 2011b), and that their availability differs across regions. For example, studies indicate that VA patients in rural areas have reduced access to health services and fewer alternatives to VA care (Weeks et al., 2004; West and Weeks, 2006).
This section begins with a definition of access to health care and provides information about how active-duty service members and veterans access care through the DOD’s Military Health System (MHS) and the VA’s Health Care System. Access to care has been defined as “the timely use of personal health services to achieve the best possible health outcomes” (IOM, 2001). A related concept is perceived access, defined as the individual’s subjective impression of his or her personal access to services. Perceived access is influenced by personal knowledge, actual experience in obtaining preferred services, and degree of satisfaction with those services. Satisfaction in turn is influenced by utilization, quality, and patient outcomes experience, all of which are influenced by the individual’s perceived need for care. Perceived access may be greater or less than actual access. For example, someone who is not attempting to obtain care may be unaware of impediments they would likely encounter; thus, their perceived access may be greater than actual access (Fortney et al., 2011).
TABLE 9.1 Patient, Community, Health System and Provider Determinants of Access
| Dimension of Access | Actual Access | Perceived Access | Examples of Measures |
| Geographic | Road travel distance and travel time to nearest provider or nearest facility with telemedicine equipment; number and choice of providers | Self-report of one's travel | Distance to nearest provider or telehealth provider |
| Temporal | Time delay between when services are needed and how long it actual takes to receive the service; length of time to get an appointment or to communicate digitally with the provider; time spent waiting in the reception area, receiving the treatment, and wait time for next appointment | Self-reported time burden and temporal convenience of receiving services | Appointment wait times |
| Financial | Eligibility and cost of utilizing the services, including insurance premiums, out-of-pocket costs, and opportunity costs, cost of digital connectivity, and other computer health applications. | Influenced by perceptions of eligibility and affordability | Copayments |
| Cultural | Whether language of the patient is offered, and whether service is discriminatory free | Patients trust and understanding of their provider; trust in their treatment plan; degree to which a patient internalizes any provider discrimination or public stigma | Linguistic match between provider and patient |
SOURCE: Fortney et al., 2011 (adapted).
Successfully achieving “access” requires that there be a unique fit among the above elements, the patient, and health care system (Fortney et al., 2011). Thus, the DOD and VA health systems must be flexible enough to adapt to the individual patient’s characteristics and specific needs as they relate to the domains above (see Table 9.1), both on the actual and perceived level. As noted in Fortney et al. (2011), policy makers are responsible for developing and implementing performance measures across the five dimensions as they relate to all components influencing access and barriers to care.
Below is a description of how active-duty service members, their families, and veterans access care through the DOD’s Military Health Care System and the VA’s Health Care System.
MILITARY HEALTH CARE SYSTEM
The DOD’s MHS provides the resources, health professionals, and direction necessary to promote the health of its beneficiary population. It is one of the largest health care organizations in the country, providing services to 9.6 million beneficiaries and employing 140,000 military, civilian, and contract personnel in the MHS setting who work with an additional 380,000 civilian providers in the United States and overseas (DOD, 2011b). The MHS provides direct care to most active-duty service members through military treatment facilities (MTFs) and clinics. The direct care is supplemented by care purchased from the civilian sector. Retirees and dependent family members of active-duty service members are also eligible to receive care at an MTF on a space-available basis; priority is given to those enrolled in TRICARE Prime (described below). Responsibility for delivering health care to garrisoned and deployed troops remains with the health departments of the individual services—Army, Navy,1 and Air Force—which have considerable autonomy in facility and personnel management (DOD, 2011a; IOM, 2010). In addition to providing health care to its beneficiaries, the health system funds education and training in accredited medical and graduate school programs and devotes approximately $600 million per year on research and development (Merlis, 2012).
_____________________
1 The medical department of the Navy oversees health care delivery for the Marine Corps.
TRICARE refers to the DOD’s collective medical programs, which provide care to all active-duty military, activated members of the National Guard and reserves, retired military personal, and their dependents who are eligible for coverage. Services may be provided through managed-care providers directly in DOD facilities,2 which includes 44 inpatient hospitals and medical centers, 291 ambulatory care clinics, 213 dental clinics in the United States, or through the purchased care system which includes 379,233 network individual providers (primary care, mental-health, and specialty care) and 3,146 TRICARE network acute care hospitals (DOD, 2011a; Merlis, 2012). There is also a fee-for-service option for care administered by civilian providers who are not part of the network (Deployment Health Clinical Center, 2012).
Eligibility and Enrollment
The total number of eligible beneficiaries stationed or residing in the United States at the end of fiscal year (FY) 2010 was 9.09 million (0.60 million were stationed or residing abroad). Retirees and their family members under the age of 65 constitute the largest percentage of the eligible population (3.07 million, 55%); followed by retirees and their family members over the age of 65 (1.88 million, 215); active-duty family members (1.91 million, 21%); active duty (1.28 million, 14%); and National Guard and reserve family members (0.58 million, 6%) (DOD, 2011a). Figure 9.1 shows the extent to which the MHS population has geographic access to direct care by providing a visual of the US distribution of the 9.09 million beneficiaries eligible for TRICARE coverage overlaid with the DOD MTFs (medical centers, community hospitals, and medical clinics).
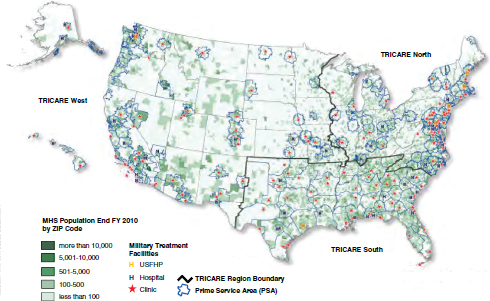
FIGURE 9.1 Military Health System population distribution in the United States relative to military treatment facilities in FY2010.
SOURCE: DOD, 2011a.
_____________________
2 Direct care treatment facilities are operated under one of the three service branches: Army, Navy, and Air Force.
To enroll in any TRICARE plan, service members, their families, and retirees must first establish eligibility through the Defense Enrollment Eligibility Reporting System (DEERS). Active-duty and retired service members, including National Guard and reserve members activated for at least 30 days, are automatically registered in DEERS, but individual service members are responsible for registering their family members, updating their status, and ensuring that their information is current and correct (TRICARE Management Activity, 2009). Activeduty service members, including members of the reserve components activated for at least 30 days, automatically enroll in TRICARE Prime3 at no cost. Eligible service members may also enroll their dependent family members in TRICARE Prime at no cost. Dependents, however, may also choose to pay extra to enroll in TRICARE Extra, an option within the TRICARE Standard program that functions similar to a preferred provider organization where participants may pay lower coinsurance if using a contracted network provider or seek coverage through a civilian health-insurance provider. There is no enrollment fee; however, an annual deductible must be met (Andrews et al., 2009; Military.com, 2012b).
In addition to active-duty members and their families, the following beneficiary groups are also eligible for coverage under TRICARE Prime: retired National Guard and reserve members (age 60 and receiving retired pay but not eligible for TRICARE for Life) and their families, survivors, Medal of Honor recipients and their families, and qualified former spouses. However, these individuals (non-active-duty members and their families) are also eligible for and may choose TRICARE Standard, a fee-for-service option that allows beneficiaries to obtain care from any TRICARE-authorized provider; there is a deductible, and coinsurance of 20–25% but no enrollment fee. About one-third of non-active-duty individuals eligible for TRICARE Prime (mostly retirees under the age of 65 and their families) live in areas without access to the Prime network and thus must choose TRICARE Standard (Military.com, 2012b).
Reserve component members and their eligible family members are covered by TRICARE up to 180 days prior to reporting to active duty (preactivation) and up to 180 days after deactivation through the Transitional Assistance Management Program (TAMP). When not in mobilized status, reservists may purchase TRICARE Select Reserve coverage, which is premium-based and offers comprehensive health care coverage similar to the TRICARE Standard and TRICARE Extra options (DOD, 2011a).
Access to Facilities
TRICARE Prime is available in the United States in areas known as Prime Service Areas. After enrolling in TRICARE Prime, a primary care manager (PCM) is assigned to the beneficiary at either an MTF or from the TRICARE network. The PCM will provide referral to care specialists when they are unable to provide the necessary care, coordinate with the regional contractor for authorization, find a specialist in the network, and file claims on the beneficiary’s behalf. Active-duty service members and their families pay no out-of-pocket costs for any type of care as long as it is received from the PCM or from another provider with a referral (DOD, 2012).
Military hospitals have historically been defined by two geographic boundaries: a 40-mile catchment area (59 catchment areas) for inpatient and referral care and a 20-mile Provider
_____________________
3 TRICARE Prime is a point-of-service health-maintenance organization that covers 100% of care at MTFs or any civilian provider that is a member of the TRICARE network.
Requirement Integrated Specialty Model (PRISM) (290 PRISM areas) for outpatient care. Standalone clinics or ambulatory care centers have only a PRISM area boundary.4 From FY 2004 to FY 2010 there was a downward trend (from 51 to 46%) in the proportion of beneficiaries living in catchment areas, due mostly to Base Realignment and Closure (BRAC) actions; the percentage living in PRISM has remained relatively constant at 64%.
Most active-duty members and their families (91%) live in MTF service areas. Ninety-six percent live in Prime Service Areas, which are geographic areas that in the least include catchment areas where the TRICARE Managed Care Support Contractors offer the TRICARE Prime benefits through an established network of providers. The percentage of Reserve Component members5 and families with access to MTF-PRIME (those living in a catchment or PRISM area) is 44.8%. TRICARE Prime is available at MTFs, in areas around most MTFs, and in some areas where an MTF was recently removed as a result of BRAC (DOD, 2011a). Note that non-active-duty beneficiaries that do not live in a catchment or a PRISM area have limited or no access to MTF-based Prime (DOD, 2011a). Figure 9.2 provides further information on beneficiaries and their geographic access to catchment and PRISM areas.
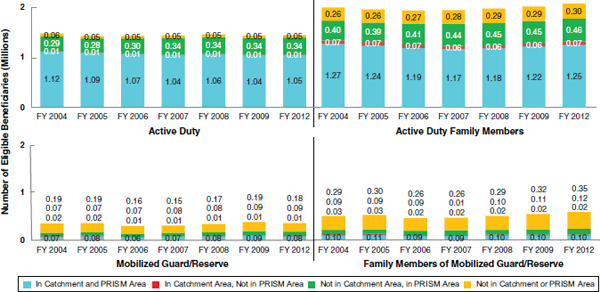
FIGURE 9.2 Trend in the number of eligible beneficiaries living in and out of MTF catchment and PRISM areas (year-end population).
NOTE: In Catchment and PRISM Area = within 20 miles of a military hospital (proximity to both inpatient and outpatient care); In Catchment, Not in PRISM Area = beyond 20 miles but within 40 miles of a military hospital (proximity to inpatient care); Not in Catchment Area, in PRISM Area = within 20 miles of a freestanding military clinic (no military hospital nearby; proximity to outpatient care only); Not in Catchment or PRISM Area = beyond 20 miles of a freestanding military clinic (lack of proximity to either inpatient or outpatient MTF-based care). SOURCE: DOD, 2011a.
_____________________
4 The distance-based catchment and PRISM area concepts have been superseded within MHS by a time-based geographic concept referred to as an MTF Enrollment Area. An MTF Enrollment Area is defined as the area within a 30-minute drive time of an MTF in which a commander may require TRICARE Prime beneficiaries to enroll with the MTF. However, because this is a relatively new concept, it has not yet been implemented within DEERS or in MHS administrative data and is consequently unavailable for use in this report.
5 Reserve component includes ready, standby, and retired reserve.
Since 2007, the population of beneficiaries has grown by about 400,000. However, the direct care system has decreased—70 hospitals in 2004 to 59 in 2009. To handle the increase in eligible beneficiaries while accounting for the decrease in direct care facilities, TRICARE must rely more heavily on civilian providers. Eligible beneficiaries are also choosing TRICARE Prime with more frequency, and, consequently, purchased care workload has grown (DOD, 2011b). In addition, mobilizations of National Guard and reserve contributed disproportionately to the number of beneficiaries living outside the catchment areas. Most members live in noncatchment areas when they are called to and leave for active duty; however, their families usually remain in the same location (DOD, 2011a). That may explain the shift in MHS workload from direct care to purchase care in the 2004–2010 period.
Mental-Health Care Within the MHS
The DOD provides mental-health services through military treatment facilities and clinics for active-duty service members and their families as well as eligible military retirees, eligible reserve-component members, and their respective families (Burnam et al., 2009). Some combat veterans have access to community-based networks of practitioners through TRICARE. TRICARE requires active-duty service members (ADSMs) to seek nonemergency mental-health care at MTFs, when available. If not available, ADSMs must obtain referrals from their MTFs or service points of contact before receiving civilian care. Non-active-duty service members do not need referrals or prior authorization for the first eight outpatient mental-health care visits per fiscal year to a network provider for a medically diagnosed and covered condition. Services provided include psychotherapy, psychoanalysis, psychologic testing, medical management, telemental-health program, acute inpatient psychiatric care, psychiatric partial hospitalization program, residential treatment center care, inpatient detoxification, rehabilitation, and outpatient substance abuse care.
Transitional Health Care Coverage
Separating active-duty members and their dependents are eligible for transitional TRICARE coverage for 180 days through TAMP if they were involuntarily separated under honorable conditions, separated following involuntary retention (stop-loss) in support of a contingency operation, separated following a voluntary agreement to stay on active duty in support of contingency operation, received a sole survivorship discharge, or separated and agreed to become a member of Selected Reserve. Deactivated National Guard and reserve members who were called to active duty for at least 30 days in support of a contingency operation and their dependents are also usually eligible to receive health care coverage for 180 days through TAMP (Military.com, 2012a).
If not eligible for TAMP or within 60 days of terminating TAMP coverage, active-duty members leaving the military under other than adverse conditions and their dependent family members can purchase a health plan similar to TRICARE Standard for up to 18 months of coverage through the Continued Health Care Benefit Program (CHCBP) if family coverage is selected. Children and spouses who were enrolled in TRICARE and lose eligibility can purchase CHCBP coverage for up to 36 months if individual coverage is selected (Military.com, 2012a).
VA is the second-largest cabinet-level department in the federal government, next to the DOD. Like other large government agencies, the VA administers its many programs through a number of subcabinet agencies, the primary ones being the Veterans Benefits Administration (VBA), the Veterans Health Administration (VHA), and the National Cemetery Administration (NCA). The VBA administers veteran’s compensation and pension, home loan, educational, life insurance, vocational rehabilitation, and other non–health care benefits; VHA administers the Veterans Health Care System; and the NCA oversees 136 national cemeteries and other memorials.
The VA Health Care System was established in the early 1900s to care for disabled and poor veterans. Expansion of the system was catalyzed first by the 2 million veterans returning home from World War I and second by the 12 million new veterans from World War II. The VA Health Care System grew rapidly after 1945. Today, it is the nation’s largest and only national direct care delivery system. Integral to its clinical services, the VA also provides transportation, housing, vocational rehabilitation, and other social support services rarely offered by private health plans (CBO, 2009; Panangala, 2010).
The VA began affiliating with academic health centers in 1947 (CBO, 2009). It operates the nation’s largest health care professions training program, providing training on a yearly basis for about 110,000 aspiring health care workers in more than 40 health care disciplines through affiliations with some 1,100 universities, colleges, and other institutions of higher education. VA funds more than 9,500 graduate medical education positions, and 85% of its medical centers are teaching hospitals, and almost one-third of all postgraduate physicians receive some portion of their training at a VA facility. Thus, the VA is the nation’s largest provider of training for nurses, pharmacists, optometrists, podiatrists, clinical psychologists, and other health care professions.
The VHA also conducts a broad portfolio of research on veterans. In FY2010, the VHA’s research program had a total budget of $1.8 billion, including intramural funding of $575 million and an additional indeterminate amount of medical care funds to support clinical research.
Embedding a biomedical, health services delivery and quality-improvement research program in a national health care delivery system and serving a stable population with an unusually high prevalence of chronic conditions, the VA has been very productive. Because veterans often have been a sentinel population for health conditions affecting the public at large, VA research about amputations and prosthetics, organ transplants, end-stage renal disease, traumatic brain injury, diabetes, geriatrics, mental-health, and quality improvement, among other areas, have materially benefitted all Americans. A description of VHA-funded studies that are currently in progress on the OEF, OIF, and OND population are provided in Appendix D.
Health Care Facilities
Since 1924, the VA has served as a national health care safety net for veterans (Kizer and Dudley, 2009; Koenig, 2003; Wilson and Kizer, 1997). Approximately 30% of VA enrollees have one or more mental-health conditions (Liu et al., 2005; Ralston et al., 2007; Seal et al., 2007), making VA the nation’s largest provider of mental-health services.
In federal FY 2010, the VA Health Care System had an operating budget of $45.1 billion, 8.3 million enrollees, and 222,551 full-time employees, including some 14,000 staff physicians
and more than 40,000 nurses (CBO, 2009; Panangala, 2010). Medical treatment facilities are located in all 50 states and essentially every major metropolitan area of the country, as well as in Puerto Rico, the US Virgin Islands, Guam, American Samoa, and the Philippines.
Health care is delivered through Veterans Affairs Medical Centers (VAMCs) that provide acute and long-term care delivery facilities through 152 hospitals; more than 800 ambulatory care clinics (CBOCs), 135 community living centers, 140 home-based primary care programs, 299 readjustment counseling centers, and 43 residential care facilities. VHA also co-funded 133 state-operated nursing facilities for elderly veterans in FY 2010 and managed 9 purchased care programs that bought more than $6 billion of services from private providers (Himmelstein et al., 2007; Koenig, 2003). The various components of the system provide a wide spectrum of medical services, including inpatient and outpatient care, mental-health care, rehabilitation, complex specialty care, and pharmaceutical benefits and distribution.
Finally, services may be provided to veterans in non-VA facilities and fall into two broad categories: contract care and noncontract care purchased on a fee-for-service basis. The use of non-VA care is justified if there is geographic inaccessibility, a lack of clinical capacity, if medical expertise or technology is not available at the local facility, or in an emergency situation.
Eligibility
With the enactment of the National Defense Authorization Act (PL 110-181), veterans who served in a combat theater (including National Guard and reserves) after November 11, 1998, and were discharged or released for reasons other than dishonorable on or after January 28, 2003, now have 5 years from their date of discharge to enroll in and obtain health care coverage from the VA. This includes all OEF and OIF veterans. Effective January 28, 2003, OEF and OIF veterans who enroll within the first 5 years after separating from the military are eligible for enhanced enrollment placement into priority group 6 (see Table 9.2) for 5 years after discharge. Injuries or conditions related to combat service are treated by the VA health care system free of charge (IOM, 2010). After the designated 5 years, enrolled veterans are placed in the appropriate priority group (see Table 9.2) on the basis of income and disability; placement determines the extent of coverage and copayment amounts. Each year, VA determines whether appropriations are adequate to cover all priority groups; if not, those in the lowest groups may lose coverage (Panangala, 2007).
In general, VHA does not provide health care services or coverage to spouses or dependents of veterans (IOM, 2009; VA, 2009). However, in accordance with the Veterans’ Mental-health and Other Care Improvements Act of 2008 (S. 2162, 110th Congress), if VA health care services for family members are necessary for the proper treatment of a veteran, then various family members also will have access. Previously, family members were only allowed to take part in such services if they were initiated during a veteran’s hospitalization and continued only if necessary for hospital discharge (IOM, 2010).
TABLE 9.2 Enrollment Priority Groups
| Priority Group |
Definition |
| 1 | Veterans with VA service-connected disabilities 50% or more disabling. Veterans assigned a total disability rating for compensation based on unemployability. |
SOURCE: Department of Veterans Affairs website:
http://www.va.gov/healthbenefits/resources/priority_groups.asp (accessed October 3, 2012).
All enrolled veterans are provided treatment and medications for service-connected illness of injury by the VA free of charge. Those who are in the higher-priority groups usually do not pay a copayment for services unrelated to their military service, while those veterans in the lower-priority groups usually pay $15 for a primary care visit and $50 for a specialist care visit (VA, 2012a). With the passage of the Veterans Millennium Health Care Act in 1999 (effective in FY 2002) the copayment for outpatient prescriptions increased from $2 to $7 per 30-day supply (Zeber et al., 2007). As of January 2006, the copayment for veterans in priority categories 2 through 6 increased to $8 per prescription with a maximum annual copayment of $960. Veterans with higher incomes (priority group 7 and 8) pay $9 per 30-day supply; there is no annual cap for this group (VA, 2012a). For those with very low income or a disability rating of 50% of higher, all copayments are waived (CBO, 2009; Stroupe et al., 2007). Thus, veteran’s health care is provided at no cost to veterans in high-priority groups and at low cost to veterans in other priority categories. Furthermore, in its attempt to reduce or eliminate costs for some treatments, the VA no longer requires a copayment for telehealth (discussed later in this chapter) (VA, 2012b).
VA Electronic Health Record
In an effort to improve access through communication between health care provider and patient, the website MyHealtheVet was introduced by the VHA in 2003. It is a Web-based personal health record that provides information on health conditions, benefits, and VA facility locations and contains a personalized patient health record, which allows patients to perform certain functions related to their health care, such as refilling prescriptions, making appointments, and viewing the results of certain laboratory tests (Jackson et al., 2011; Turvey et al., 2012). More broadly, it is intended to improve co-managed care and empower patients to play a more active role in their health care (Nazi et al., 2010).
In 2010, a survey was conducted using the American Customer Satisfaction Index. Veterans who had viewed at least four pages of MyHealtheVet were invited to participate in the survey regarding utilization of the website. The majority of the users were male (91%), between 51 and 70 years old (68%), and served during Vietnam (60%). Most rated their health in the “good” or “very good” category, one-third live 1 or more hours away from a VA facility, and 75% use the system to refill prescriptions (Nazi, 2010). Results also indicated that 40% of users printed out their information, 21% saved their information to their computers, 4% sent to other users, 18% shared their medication lists with VA providers, and 9.6% shared with non-VA providers. As of April 2011, the website had registered over 1.2 million users. While MyHealtheVet has the capacity to improve access through increased coordination of care, VHA will need to determine how to increase usage among veterans.
Mental-Health Care Within the VA
The VA offers acute inpatient care, intensive and regular outpatient care (e.g., psychotherapy, pharmacotherapy, and telemedicine), residential care, and supported work settings. Services include treatment for depression and anxiety, substance abuse, PTSD, severe mental illnesses (e.g., schizophrenia, schizoaffective disorder, and bipolar disorder), and special programs for veteran populations with special needs (e.g., suicide prevention services, sexual
trauma, services for women veterans, homeless veterans, older veterans, and veterans within the criminal justice system).
In 2004, when the VA adopted a new approach to mental-health care designed to focus on recovery, it integrated mental-health care into overall health care for veteran patients. The VA also developed a 5-year action plan that includes more than 200 initiatives, including initiatives aimed at raising awareness of the importance of mental-health, eliminating disparities in the availability and quality of mental-health services for veterans, and providing comprehensive mental-health care services to veterans with mental illness (VA, 2011b).
In 2008, the VA published a handbook specifying which mental-health and substance-use treatment services VA hospitals and clinics are required to offer veterans and their families; in 2011 a simplified version to help beneficiaries navigate services was published (VA, 2011a; VA and VHA, 2008).
FRAGMENTATION OF CARE
Fragmentation of care diminishes continuity and coordination, often resulting in higher use of emergency departments, increased hospitalization, duplication of tests, and increased costs. It has also been shown to increase the likelihood of adverse effects and medical errors. Persons with chronic conditions and mental-health diagnoses are especially vulnerable to these consequences, as are young adult males who are more likely to seek care from multiple providers (Kizer, 2011, 2012). Continuity of care is an essential element in health care service delivery and includes availability of patient information, clinician consistency and availability, coordination during transition events, and ongoing patient and provider communication (Donaldson, 2001). The transition between the DOD and the VA systems is a vulnerable period when continuity of care might be compromised.
Transitions Within the DOD and VA
Military service men and women experience frequent changes in geographic location related to their military service. Those changes necessitate changes in primary care and mental-health care, which can delay treatment (until new providers are identified and appointments secured) and change treatment protocols. Transfer of medical records within the military health system might not capture all medical information, particularly treatment for mental-health visits. Paper records for mental-health evaluations might not be available, and repeat examinations might occur as might treatments that had previously proved ineffective (Tanielian and Jaycox, 2008).
When active-duty members leave military service and return to civilian status, their health care coverage transitions from DOD to the VA health care system. That requires successful completion of several handoffs, from MTFs and TRICARE network providers to VA facilities. Critical handoffs include enrollment in the VA system, identification of and enrollment in programs, and the successful transfer of medical records. Additionally, some reserve members might receive care from both DOD and VA, and although both use electronic health records, the two systems are not yet compatible.
In general, transition points pose risks to access and quality of care, including disruption of relationships with care providers, treatment interruption, and handoff errors. Risks are increased for service members receiving mental-health care as they make the transition. Furthermore, the VA requires consent for medical records to be transferred from DOD to VA for reserve members, creating another potentially risky transition point.
Programs have been developed by both DOD and VA to bridge gaps in care and decrease fragmentation. For example, DOD utilizes the in Transition Program, which offers specialized assistance and coaching aimed at enhancing continuity for service members receiving mental-health care as they make any of the following transitions: relocating to another assignment, returning from deployment, transitioning from active duty to reserve or vice versa, and leaving military service (Office of the Assistant Secretary of Defense, 2010). The Federal Recovery Coordination Program (FRCP) was jointly developed by DOD and VA to coordinate care for severely wounded service members and veterans. It was designed to complement existing programs such as DOD’s Recovery Coordination Program, the Wounded Warrior Program operated by the individual military services,6 Army Warrior Transition Units, VA’s OEF and OIF Care Management Program, VA’s Spinal Cord Injury Disorders Program, and the VA Polytrauma System of Care. FRCP coordinators are assigned to link together multiple case managers, oversee their enrollment in programs, and serve as the single point of contact for the injured service member and their families (CBO, 2011; Yano et al., 2003).
A major limitation and concern of the FRCP is the inability to share information across DOD and VA and the general incompatibility among systems used by different programs. Service members are typically enrolled in multiple programs—in September 2010, 84% of FRCP enrollees were also enrolled in a military service wounded warrior program. That limits coordination of services, increases duplications of services, and may result in enrollee confusion. Accordingly, FRCP is making efforts to address those limitations and improve information sharing; however, as noted by the GAO (2011a), it appears that increased efforts to improve data exchange between the two systems and interdepartmental coordination are needed.
Electronic Health Records
Successful transfer of medical records is a necessary component of the DOD-to-VA transition and, more broadly, a way in which to decrease fragmentation of care resulting from movements between health systems and providers. Electronic health records have the potential to facilitate communication between patients and providers, especially from differing health care systems, to improve coordination and reduce redundant care, medication errors, and costs (Kaelber and Pan, 2008; Ralston et al., 2007; Ross et al., 2004; Schnipper et al., 2009; Zhou et al., 2007). Additionally, electronic health records should allow patients the ability to transfer their records to providers who are not in the system; for example, rural veterans who often receive both VA and non-VA care.
The DOD and the VA health systems currently employ electronic health records and the Federal Health Information Exchange (HIE) supports the transfer of electronic health information from the DOD to VA at time of separation. That one-way exchange of information
_____________________
6 The Wounded Warrior Program includes the Army Wounded Warrior Program, the Marine Wounded Warrior Regiment, Navy Safe Harbor, the Air Force Warrior and Survivors Care Program, and the Special Operations Command’s Care Coalition.
allows VA providers to view the clinical data record, and the deployment and postdeployment health assessments (DOD, 2011a). Additionally, there is a Bidirectional Health Information Exchange that provides bidirectional health care data transfers between VA and DOD health care facilities for shared patients. For example, the Clinical Health Data Repository (CHDR) provides, at a minimum, outpatient pharmacy and drug allergy records; and the Laboratory Data Sharing and Interoperability supports the sharing of secure encrypted laboratory orders and results between the two agencies. Despite those technologies, service members have indicated poor management throughout medical record transfer.
In an effort to address those problems, the DOD and the VA have announced that they are working to integrate their health records; currently the goal is to reach that milestone by 2017. The goal of the new system is to provide a seamless transition of care between the DOD and the VA. The development of the Integrated Electronic Health Record (iEHR) is to be tested in two sites by 2014 that offer DOD and VA care: San Antonio, Texas, and Hamptons Roads, Virginia (Pellerin and Marshall, 2012).
DISPARITIES IN HEALTH CARE
Providing uniform services within the DOD and VA health care systems across geographic locations, facilities, and providers should be a priority; as should providing quality care to women and ethnic minorities (GAO, 2011b). There is a paucity of information regarding disparities in health care in the OEF and OIF active duty and veteran populations. This section, however, highlights issues regarding health care in women, racial and ethnic minorities, and rural veterans. As discussed below, disparities in health might manifest in subtle ways; for example, the type of diagnoses received by women or different ethnic groups.
Women in the Military
As noted in Chapter 4, women comprise about 14% of all active-duty military, and 17.6% of National Guard and reserves; about 12% of women veterans served in OEF, OIF, or OND.7 Historically, the research on the health of veterans has focused on the health consequences of combat service in men with little scientific research or longitudinal study of the health consequences of military service for women. Research that has examined gender differences is generally mixed, and a recent review (Street et al., 2009) highlighted the need to conduct studies with larger samples of women to understand issues relevant specifically for women. Women in the military cope with some unique stressors that might amplify their risk for mental-health problems, such as military sexual trauma (MST); histories of premilitary trauma, pregnancy, and the multiple family roles (e.g., mother, spouse, caregiver).
Recent studies of OEF and OIF female veterans suggest that they exhibit higher need for mental-health care than that evidenced in previous conflicts, with reports that 17% are diagnosed with PTSD (compared to other eras, in which 8–9% of women veterans were diagnosed with current PTSD) and 23% are diagnosed with depression (Litz et al., 1997; Maguen et al., 2009; Schlenger et al., 1992). Recent data suggest that between half to a third of women veterans indicated that they needed counseling for depression (48%), relationship issues (38%), anxiety
_____________________
7 See http://www.womenshealth.va.gov/WOMENSHEALTH/facts.asp.
(36%), and anger management (30%) (Shekelle et al., 2011). In addition, a greater number of deployments seem to be associated with screening positive for mental-health problems (Bean-Mayberry et al., 2011).
MST appears to be an important risk factor for PTSD. Suris and Lind (2008) reviewed research on health consequences of MST and found higher rates of PTSD, depression, and substance abuse in female veterans with a history of sexual assault. In fact, female veterans with a history of MST were nine times more likely to develop PTSD than female veterans with no history of sexual trauma. Recent research on OEF and OIF veterans supports those findings. Kimerling et al. (2010) reviewed medical records of OEF and OIF veterans (17,580 women and 108,149 men) for diagnoses of mental-health disorders and found that those with a history of MST were significantly more likely to receive a diagnosis of PTSD, other anxiety disorders, depression, or substance-use disorders than those with no history of abuse. Odds ratios remained significant after adjusting for other significant associations, and effect sizes for women were substantially stronger than those for men.
Estimates of MST have been reported based on a universal screening program implemented by the VA. In 2003, shortly after implementation of VA screening, 21.5% of women and 1.1% of men reported experiencing MST (Kimerling et al., 2007). It has been noted that those estimates have remained fairly consistent, and as of 2008 those percentages translate into 48,106 women and 43,693 men screening positive for MST (Hyun et al., 2009). DOD estimates of MST report that the annual prevalence of sexual assault for women was 6.8% and 1.8% for men (Lipari et al., 2008). A study of reservists examined sexual harassment and assault during military service and found that sexual assault was reported by 13.1% of the women and 1.6% of the men (Street et al., 2008).
There are mixed findings regarding the relationship between women’s health care use and sexual assault. Kelly et al. (2008) found MST to be associated with greater use of VHA care but less satisfaction with VHA services. Other studies found that women with a positive history of any form of sexual assault were more likely to meet the criteria for PTSD but accessed fewer health care services (Suris et al., 2004). Women veterans who have experienced MST and access health care report significant anxiety if treated by a male provider, particularly if subjected to any invasive exam, a concern with regard to aggravating mental-health symptoms and accessing future health care (Bean-Mayberry et al., 2010).
Utilization
Utilization of mental-health services provides an interesting comparison between men and women serving in OEF and OIF. Differences in gender use of DOD or VA mental-health services might be linked to type of psychiatric condition, since some data seem to suggest that there are no disparities across gender groups when adjusting for differences in need. For example, Maguen et al. (2012) conducted a retrospective study to examine gender differences in VA health care use among a national sample of newly returning OEF and OIF veterans with PTSD seeking care from 2001–2010. The study population consisted of 159,705 OEF and OIF veterans (15,303 women, 144,402 men) who had at least one clinical VA facility visit from 2001 through 2010 and were diagnosed with PTSD. Mean number of visits for each type of use were similar for men and women with PTSD; both had a median of about 3 mental-health outpatient visits per year. Other research has shown, however, that 9 or more sessions of evidence-based treatment is needed to reduce PTSD severity (Foa et al., 2005).
There were a few small, statistically significant differences in the incidence rate ratio for those initiating care. Women with PTSD initiating care were more likely than male veterans with PTSD to have lower use of inpatient mental-health hospitalization, higher rates of outpatient mental-health service use, higher use of primary care visits, and higher use of emergency care visits. These findings are consistent with research of women in the general (nonmilitary) population that shows that women use primary care and emergency services at higher rates than men (Bertakis et al., 2000).
Men and women with comorbid PTSD and depression (respectively 57% and 72%) were more likely to use all categories of services more frequently than those with PTSD alone. For example, the rate of mental-health inpatient use by women with PTSD and depression was 12.5 imes greater than for those without depression, while that figure for men was only 6.7 times greater. Comorbid alcohol use disorders and PTSD was present in 8.2% of women and 29% of men. Again, both women and men in the comorbid group were more likely to have used all categories of VA services (Maguen et al., 2012).
Washington et al. (2006) conducted a study to determine why women do or do not use VA health care services. A telephone survey was conducted in 2004 among women veterans eligible for VA health care; the women lived in southern California and southern Nevada. The most often cited reasons for VA use included the following: affordability (67.9%), availability of a women’s health clinic (58.8%), quality of care (54.8%), and convenience (47.9%). Findings also indicated reasons for choosing non-VA care, such as having health insurance (71.0%), greater convenience of non-VA care (66.9%), lack of knowledge about VA eligibility and services (48.5%), and perceived better non-VA quality of care (34.5%). Thus, lack of information about VA health care, poor perceptions about quality, and inconvenience reduce utilization of VA health care.
The National Survey of Women Veterans, a national population-based telephone survey, was conducted in 2008–2009 to examine health care needs of women veterans. Of the 10,638 contacted households, 3,611 (33.9%) participants were eligible for and consented to enroll in the survey. Overall, 18.9% of the population delayed or went without needed health care in the prior 12 months, including 14.3% of insured and 54.6% of uninsured. Younger age was associated with a higher prevalence of delayed care or unmet need (35% of 18–34-year-olds). Women veterans with delayed care were more likely to be OEF and OIF veterans, a high-priority group for VA enrollment, and to have experienced MST. In the study, 4.8% (n = 173) of the overall population sampled were OEF and OIF veterans, of which more than a third (37.2%) experienced an unmet need for care. The most commonly cited reason for unmet need was not being able to afford medical care. The independent predictors of delayed or unmet need for OEF and OIF women veterans health care were the following: being uninsured (OR = 6.5; 95% CI: 3.0–14.0) followed by being in the under-35 age group (OR = 4.5; 95% CI 1.8–11.3). After controlling for potential confounders, other predictors of delayed care were the perception that VA providers are not gender sensitive (Shekelle et al., 2011) and having a history of MST.
Racial and Ethnic Minorities
There is a paucity of literature on disparities in health care in racial and ethnic minorities in the OEF and OIF populations. Therefore, the committee includes studies in this section on all
minority veterans, in particular African American, Latino, American Indian, and Alaskan Native veterans.
In 2007, the VA conducted a systematic review of racial and ethnic disparities in its health care system. Findings from several studies indicate that black and Hispanic patients were more frequently diagnosed and treated for psychotic disorders (e.g., schizophrenia), while white veterans were more frequently diagnosed and treated for affective disorders (e.g., bipolar disorder and depression). The difference in patterns of diagnosis and treatment are unclear. The review notes, however, that black veterans might benefit from having black clinicians (Saha et al., 2007).
A small study of Puerto Rican OEF and OIF veterans and family members following deployment examined unmet health needs. Hannold et al. (2011) found that Puerto Rican veterans tend to deny symptoms of stress and do not seek psychologic examinations. The authors also found that the families of these veterans experience emotional problems and expressed the need for family support groups. The veterans also indicated that they had physical problems and needed pain treatment. The authors concluded that there is a need for “veteran-centric” and family-focused health care.
The Native American Indian, Pacific Islander, native Hawaiian, and Alaska Native (AIAN) populations serve at the highest rate per capita in the Armed Forces (Holiday et al., 2006; Kramer et al., 2009). Nearly half of all Native veterans reside in rural locations on tribal or Alaska Native lands. According to the American Indian Vietnam Veterans Project, a community-based epidemiological study, Native veterans have high rates of combat-related mental-health disorders, 31% current and 59% lifetime, and alcohol abuse and dependence, 72% current, 84% lifetime. These figures are significantly higher than any other ethnic group (Beals et al., 2002). AIAN veterans have 1.9 higher odds of being uninsured compared with non-Latino white veterans (Johnson et al., 2010). They have a disproportionate amount of service-related military conditions, and they are more likely to use the Indian Health Service as opposed to the VA system (Johnson et al., 2010). The Indian Health Service, similar to the VA, struggles to find and retain physicians, especially those who have the necessary cultural awareness (Brod et al., 1982; Fannin and Barnes, 2007; Hostetter and Felsen, 1975; Johnson and Cameron, 2001).
The AIAN population, similar to other rural veterans as described below, experiences significant barriers in accessing care, such as underfunded resources (i.e., time, money, and transportation), lack of culturally appropriate care, inability to recruit and retain health care professionals, and geographic access issues (Kaufman et al., 2010). AIAN veterans are more likely than their white counterparts to report delays in care because of not getting a timely appointment, not being able to reach a contact by phone, or because of transportation problems. Despite the growing evidence on telehealth effectiveness, acceptance and implementation in the rural areas where these veterans reside remain a challenge (Barton et al., 2007; Grigsby et al., 2007; Spaulding et al., 2005). For example, one study examined the differences in administering a mental-health assessment, the SCID, by teleconference versus in person to AIAN veterans. Attitudes did not differ significantly between the groups; however, participants expressed lower ratings of satisfaction and comfort in the telehealth interviews (Shore et al., 2008).
There is a dearth of knowledge on disparities in mental-health care in the OEF and OIF veterans, and available studies show mixed findings on whether disparities exist. For example, one study found racial disparities in the granting of service connection for PTSD by the VA for black patients compared to non-Latino white patients. In the study of 20,284 veterans, black veterans were significantly less likely to have received services connected for PTSD (Murdoch et al., 2003) compared to their non-Latino white counterparts. Service-connected veterans receive priority for VA enrollment due to documented, compensative conditions related to or aggravated by military service. For many, service connection represents the difference between access to VA health care facilities and no access. Although black and Hawaiian/Pacific Islander veterans were as likely as non-Latino whites to receive psychotropic medications, they were less likely to receive at least four 1-month supplies of the medication (Murdoch et al., 2003). Similarly, the authors discuss that even among poor, homeless veterans who are eligible for VA care because of their low income, lack of service connection decreased their odds of using VA services. However, another study found no disparities in the use of intensive VA treatment programs for PTSD among black and Hispanic patients compared to white patients (Rosenheck and Fontana, 2002).
There are also mixed findings among the few studies conducted in OEF and OIF veterans on racial and ethnic disparities in mental-health care. One recent study found that ethnicity (i.e., Latino) was not a contributing factor to mental-health service use among veterans with a new diagnosis of PTSD, and that once engaged in mental-health services, all veterans were more likely to use counseling and complete at least eight counseling sessions of treatment (Spoont et al., 2009). However, veteran race (i.e., African American and Hawaiian/Pacific Islander) contributed to lower use (Spoont et al., 2009). Another recent study found that black veterans were less likely than white veterans to receive guideline concordant depression care at the VA and less likely to receive or adhere to pharmacotherapy (Chermack et al., 2008).
Black and Hispanic veterans are most significantly affected by racial and ethnic disparities in the VA (Saha et al., 2007). Race and ethnicity was related to the number of VA outpatient visits among veterans, with black and Latino veterans having more visits (reverse disparity) and Asian and Pacific Islanders having fewer visits (greater disparity) than non-Latino white veterans (Harada et al., 2002). Black, Latino, and Asian/Pacific Islander veterans were less likely than non-Latino white veterans to persist with health care services over a 12-month period, with ambulatory care varying by race/ethnicity (Washington et al., 2005). Black and Latino veterans were less likely to indicate having a primary care physician than whites. Despite these disparities, black and Latino veterans are more likely to use VA-only health services, with Asian/Pacific Islanders and non-Latino white veterans more likely to seek help outside the VA system (Washington et al., 2002).
Rural Veterans
Health disparities between rural and urban communities have been well documented (IOM, 2005). Health care in rural populations poses challenges such as limited specialized providers, limited options for assessment and treatment referrals, and the lack of providers’ cultural awareness of the community (Richardson et al., 2009). Rural veterans are less likely to access mental-health services because they are hindered by challenges such as greater distance
and travel time than their urban counterparts. According to VA’s Office of Rural Health, as of FY 2010, veterans living in rural areas make up 41% of those enrolled in the VA system (GAO, 2011b); 39% of enrolled OEF and OIF veterans are from rural areas (VA, 2012d). Although 11.8% of 18–24-year-old military recruits are from rural areas, that number decreases to 7.6% of 18–24-year-olds in the general population (Kane, 2006).
Studies have shown that VA patients in rural areas have more physical comorbidities and worse health-related quality of life than those residing in suburban or urban settings. In addition, they have reduced access to health services and fewer alternatives to VA care (Weeks et al., 2004; West and Weeks, 2006). Compared to urban and suburban veterans, rural veterans live further from private-sector and VA hospitals, have access to fewer mental-health and specialty services, and visit their providers less frequently, but they have more physical- and mental-health problems (Weeks et al., 2004). Among veterans seeking treatment for serious mental illness, travel distance was found to be the strongest predictor of poor service (McCarthy et al., 2006). Increasing travel distance also predicts poor retention for alcohol abuse treatment, especially among older and younger veterans (but less so among the middle-aged) (Fortney et al., 1995).
Outpatient service utilization trends were examined for rural veterans with PTSD compared to their urban counterparts. Data were obtained for 415,617 veterans with PTSD who received outpatient care at a VA facility. Results indicate that veterans from rural and highly rural areas had 19% (CI = 0.80–0.82) and 25% (CI = 0.72–0.79), respectively, fewer outpatient visits than those who lived in an urban setting. Results are similar for visits to specialized PTSD clinics with 22% (CI = 0.87–0.89) fewer visits for those in rural and 33% (CI = 0.64–0.71) fewer visits for those in highly rural areas compared to their counterparts in urban areas. Service use was contingent on proximity to services, with a larger effect seen for those requiring specialized mental-health care. There is concern that those living further distances from a facility might not receive optimal care (Brooks et al., 2012).
The effect of distance on access to care for rural veterans was assessed through surveys (n = 96 patients, 88 providers/staff), interviews (42 patient, 64 providers/staff), and focus groups (n = 7 consisting of providers and staff) at 15 VHA primary care clinics in the Midwest (VISN 23). “Distance to drive” was the most frequently selected barrier by patient and provider; other barriers included travel related challenges such as time, limited transportation, and cost or expense. Veterans indicated that the same travel distance was more burdensome when seeking care for routine services (e.g., laboratory, podiatry) as compared to specialty care (e.g., cardiology, neurology) (Buzza et al., 2011).
Numerous studies have noted an increased risk of suicide for those living in rural areas (Kapusta et al., 2008; Levin and Leyland, 2005; Middleton et al., 2003; Razvodovsky and Stickley, 2009; Singh and Siahpush, 2002). McCarthy et al. (2012) examined rural–urban differences in suicide rates in a population of veterans receiving services in the VA health system. Suicide mortality was assessed in two periods: FY 2004–FY 2005 and FY 2007–FY 2008; and suicide risks were assessed for two cohorts—those that had VA inpatient or outpatient encounters in those time periods. Median distance to the nearest VA mental-health provider was greater for patients in rural areas. In the two cohorts, residence in rural areas was associated with increased rates of suicide and increased suicide risk. Although previous studies have documented decreased service utilization and continuity of care with greater distances to health system providers, the McCarthy et al. (2012) study noted that distance measures were not necessarily
related to suicide risk. That finding suggested that elevated suicide risks observed among rural populations might have less to do with health system accessibility barriers and more to do with socioeconomic or sociocultural factors.
BARRIERS TO CARE
Barriers to care imply impediments that make it difficult for a service member or veteran to receive treatment. Numerous studies have detailed barriers to care. For example, Britt et al. (2008) and Hoge et al. (2008) highlight issues such as veterans not knowing where to go for treatment, not having enough leave time, long distances to travel to a facility, lengthy wait times, workforce shortages, and stigma. Furthermore, among military personnel who screened positive for a mental disorder, 55% stated it would be difficult to obtain time off from work, and 45% stated it would be difficult to schedule an appointment (Hoge et al., 2008). Similarly, a recent GAO report (2011b) notes logistical challenges for veterans in accessing mental-health care, including difficulty in scheduling and coordinating appointments, long distances to facilities and other transportation challenges, cost of services, challenges in arranging child care or spousal support, and other time constraints.
The section below begins with a discussion of stigma, a barrier that has been well documented in the military population as it relates to mental-health; additional barriers discussed include wait times, workforce capacity, and geographic accessibility.
Stigma, the Military Environment, and Attitudes About Treatment
In the military, stigma refers to the belief that treatment seeking might cause harm to one’s career, diminish the trust and confidence of fellow service members, or affect how a soldier will be perceived by his colleagues and superiors (Britt, 2000; Christensen et al., 2009; Greene-Shortridge et al., 2007; Hoge et al., 2008; Link and Phelan, 2001). Furthermore, stigma in military populations, as in the general population, has been found to have a negative impact on treatment seeking, treatment initiation, and adherence to treatment (Kim et al., 2011).
Research indicates that stigma deters individuals in the military from seeking help for mental illness because service members might interpret seeking such care as a weakness and that it is possible to “tough it out” (Dickstein et al., 2010). Stecker et al. (2007) notes that the most frequently reported barrier to mental-health care by soldiers and Marines deployed to Iraq was the belief that one “ought to handle it on my own.” Hoge et al. (2004) found that service members with mental-health disorders felt they “would be seen as weak” if they engaged in treatment.
Rae Olmsted et al. (2011) examined the differences in perceived stigma among soldiers in treatment for substance abuse (n = 12), for mental-health treatment (n = 388), for both substance use and mental-health (n = 70), and those not in treatment (n = 966). Soldiers were recruited from two Army installations between October 2009 and February 2010. Those reporting any treatment within the past 12 months indicated more stigma with regard to both substance abuse and mental-health treatment than those without treatment. Results of the study demonstrate that while all military personnel reported stigma related to treatment of mental-health and substance use, those in treatment reported increased perceptions of stigma regarding
mental-health treatment. The authors note that stigma may be a barrier to care and that it might result in treatment failure or dropout from treatment.
Seeking treatment is often at odds with several aspects of military culture. It has been noted that military culture promotes individual strength and selfless devotion to the nation and to one’s comrades. Soldiers fear loss of support from their unit as well as fear of career repercussions, as mental-health treatment will appear on medical records (Tanielian and Jaycox, 2008). Gorman et al. (2011) conducted a study of 332 National Guard troops who had been deployed to OEF and OIF, and their partners. Findings indicate that 49% of National Guard members and 34% of their partners met screening criteria for one or more mental-health symptoms. Although 53% of the National Guard soldiers who met screening criteria reported getting some type of care, concerns about treatment influencing career advancement among service members was a barrier for those not seeking care.
Gibbs et al. (2011) reported on results from 48 focus-group interviews conducted at six Army installations regarding the perception of treatment for substance abuse and mental-health in the military environment. Study participants varied in that some were currently in the Army Substance Abuse Program (n = 80), others in treatment for mental-health (n = 56), and others were not in any treatment program (n = 134). Those in treatment for alcohol abuse or mental-health issues were more likely to describe negative attitudes from command and peers. The negative perceptions of treatment for alcohol abuse were based on potential infractions, in addition to “social distancing” from peers that was felt by those in treatment. Ironically, high alcohol use prior to treatment was associated with bonding with peers and as a way to respond to stressors (similar results were reported by Ames et al., 2007).
Another frequent reason reported by service members for not seeking treatment was negative perceptions from leadership (Kim et al., 2011). Britt et al. (2012) studied perceived stigma and barriers to care for mental-health treatment. The authors examined leadership behaviors (in noncommissioned officers8 [NCOs] and officers) and the effect on stigma and practical barriers to seeking mental-health treatment in 1,455 soldiers following a 15-month deployment to Afghanistan. Positive and negative leadership by NCOs were more strongly correlated with stigma and practical barriers than officers. Only NCO behaviors were uniquely predictive of stigma over time, with higher ratings of negative behaviors and lower ratings of positive behaviors being associated with higher reports of stigma.
Wright et al. (2009) studied soldiers in combat support units (n = 680) 3 months postreturn from combat in Iraq. A relatively small but statistically significant relationship was found between factors such as officer leadership and unit cohesion as predictors of stigma and subsequent treatment seeking. Not only were both factors related independently to reduced stigma and greater use, but positive leader behavior in conjunction with unit cohesion enhanced access to care (Wright et al., 2009). This study supports other work indicating that leadership behaviors, along with unit cohesion, override the relationship between high symptom levels of mental-health issues and higher perceptions of stigma in terms of seeking treatment (Britt et al., 2012; Hoge et al., 2008; Kessler et al., 2001). In addition, a study of OEF and OIF National Guard and reservists found that lower unit support was related to higher perception of barriers in accessing care as well as perceived stigma (Pietrzak et al., 2009).
_____________________
8 Noncommissioned officers (NCOs) are the front-line supervisors of most military personnel and have a more direct daily impact on service members than commissioned officers.
Hoerster et al. (2012) examined the effect of perceived barriers on prospective mental-health care use among a sample 305 OEF and OIF veterans who sought care and presented with symptoms of depression (n = 273), PTSD (n = 231), or alcohol misuse (n = 91) at a VA postdeployment health clinic. Barriers related to stigma such as “it would harm my career, members of my unit might have less confidence in me, my unit leadership might treat me differently, and I would be seen as weak” were most commonly cited among the sample (n = 111; 37% endorsed at least one stigma-related barrier). Despite those stated barriers, they did not interfere with receipt of adequate treatment in this population of care-seeking veterans. The results may not accurately reflect those who have not sought or initiated care (Hoerster et al., 2012).
Finally, negative attitudes toward treatment, including perceived effectiveness of treatment and prior experiences with providers can also be barriers to seeking care. Positive experiences with mental-health providers improve the likelihood of seeking additional treatment. For example, studies have found that the use of mental-health services in National Guard troops was associated with previous mental-health care satisfaction and belief in treatment efficacy (Kehle et al., 2010; Pietrzak et al., 2009).
Kim et al. (2011) analyzed data from self-reported questionnaires on barriers to care, treatment utilization, and mental-health risk in 2,623 soldiers approximately 6 months postdeployment to OEF or OIF. Results indicate that those reporting a mental-health issue were significantly more likely to report barriers to accessing care and more likely to endorse negative attitudes toward treatment than those not reporting mental-health concerns. Negative perceptions from peers and leadership were a frequently reported concern with utilizing mental-health care. Controlling for age, gender, and education, negative attitudes toward treatment were also negatively associated with use of mental-health professionals and military facilities; those reporting negative attitudes were 42% less likely to utilize care in a military facility. Negative attitudes were identified as the only unique predictor of utilization and treatment seeking. It is, however, unclear whether those negative attitudes stem from the soldier’s belief that they could address their own problems or because of their negative perceptions on efficacy of the treatment itself.
Britt et al. (2011) conducted a cross-sectional survey in a sample of National Guard and reserve members from the Army, Marine Corps, and Air Force (n = 760) and members of the Pennsylvania National Guard (n = 334) who had been deployed in support of a military operation since 2003. Survey results indicated that 27.5% reported a “mild problem,” 11.7% reported a “moderate problem,” and 2.6% reported a “severe problem” when asked about current experience with a psychologic problem. Thirty-four percent of veterans (n = 120) reporting a mental-health problem had no interest in obtaining care. The most frequently cited reason for not obtaining care was that “the problem was not severe enough” (26.6%), followed by a lack of resources in being able to seek treatment, such as cost, time, and transportation (16.5%), followed by negative beliefs about the treatment itself (12%). Overall attitude and beliefs about psychologic problems was a unique predictor of whether one reported treatment seeking for mental-health. Those who had a positive attitude toward treatment and those not believing they could handle the problem on their own were more likely to seek care.
Excessive wait times are a frequent complaint expressed by both active-duty and veteran service members. The DOD’s MHS is supposed to meet statutory access standards9 for its TRICARE beneficiaries. For example, the wait time for an appointment must be less than 4 weeks for a well-patient visit or a specialty care referral, less than 1 week for a routine visit, and less than 24 hours for an urgent care visit. MTF enrollees see their assigned primary care manager about 40% of the time; if beneficiaries call for an acute care appointment, they should be offered at least three options within 24 hours about 50% of the time; that figure increases to 70% for routine appointments (DOD, 2011a, 2011b).
Evaluations of TRICARE reveal that active-duty service members and their families complain about delays in receiving TRICARE mental-health services primarily because of long wait times for appointments and difficulty in locating providers accepting TRICARE (Avery and MacDermid Wadsworth, 2011; Bagchi et al., 2007; National Council on Disability, 2009).
Problems with access to mental-health services have been highlighted (Tanielian and Jaycox, 2008) and include shortages of uniformed mental-health specialty providers, long wait times, and unfilled training slots. Numerous studies have shown such organizational barriers to seeking care (Britt et al., 2008; Wright et al., 2009). An earlier example is the study by Hoge et al. (2004). The authors examined mental-health problems and barriers to care in three Army units and one Marine unit before deployment to OEF or OIF and 3–4 months after deployment. Among military personnel who screened positive for a mental-health disorder, nearly half reported difficulty in scheduling an appointment (45%); other barriers included being seen as weak (65%), problems with leadership such as being blamed (51%) and being treated differently (63%), and harming ones career (50%).
Kim et al. (2011) collected data from 3,380 soldiers approximately 6 months postdeployment from OEF or OIF (with 2,623 reported being deployed at least once). Numerous barriers to care were examined. Specific to wait times, among respondents with mental-health problems, 32.5% of those receiving care indicated it was difficult to get an appointment vs 16.8% of those not receiving care.
VHA policy requires that first-time patients requesting mental-health care be seen within 24 hours for an initial evaluation with followup for a comprehensive exam within 14 days. However, a recent review of access to mental-health care in the VHA has been conducted and findings indicate that the VHA does not have a “reliable and accurate method” of determining whether they are meeting that standard (VA Office of the Inspector General, 2012). In addition to the finding above, the VA Office of the Inspector General (OIG) found that the VHA does not provide first-time patients with timely mental-health exams as patients often waited more than 14 days; VHA schedulers did not consistently follow procedures outlined in VHA directives; and vacancies in mental-health staffing might affect VHA’s timeliness goals.
Prior to the VA OIG report (noted above) in July 2011, the US Senate Committee on Veterans Affairs requested that the VA conduct a survey among mental-health professionals regarding whether their medical center had adequate staff to meet the veterans’ demands for treatment. Seventy-one percent indicated that their medical centers did not have adequate staffing to meet the needs. The VA OIG interviewed clinicians at four of the sites participating in
_____________________
9 CFR ° 199.17(p)(5)(ii).
the survey and found that three of the four sites had vacant positions in psychiatry. It was determined that a patient in need of a mental-health visit at one of those sites10 had to wait, on average, 86 days to see a psychiatrist (VHA, 2011).
In general, long wait times can compromise health due to delayed utilization, lead to poorer health outcomes, and decrease patient satisfaction (Pizer and Prentice, 2011). Several studies have examined the effects of wait times on health outcomes in the VA (Pizer and Prentice, 2011; Prentice and Pizer, 2007; Prentice et al., 2011) and found that there are statistically significant decreases in utilization particularly in the elderly and vulnerable veteran populations. In addition, long-term outcomes such as mortality and preventable hospitalizations are worse for veterans who seek care at facilities with longer waits compared to veterans at facilities with shorter wait periods.
Workforce Capacity
Poor availability and distribution of mental-health specialists in many parts of the United States presents a significant barrier for OEF and OIF veterans to access mental-health care. Many specialists are in urban areas, and even in those areas there are disparities in concentrations of psychiatrists. For example, according to Burnam et al. (2009) in the mid-Atlantic region there are 8.2 psychiatrists per 100,000 people. However, in New England, there are 53 psychiatrists per 100,000 people. In some rural areas, psychiatrists are entirely absent.
For active-duty service members, limited participating provider networks is a primary barrier for accessing mental-health care. In Indiana, for example, providers in markets with higher populations are more likely to accept the TRICARE plan than providers in rural, less populated areas (Avery and MacDermid Wadsworth, 2011). Additionally, provider lists for TRICARE consumers may be confusing and inaccurate; certain providers are listed in the TRICARE directory of providers but are no longer providing services to TRICARE.
A study by Avery and MacDermid Wadsworth (2011) examined access to mental-health services for active-duty service members and National Guard in Indiana. The authors found several discrepancies in the TRICARE outpatient network—of the 907 providers in the list, only 404 were distinct providers in 551 office locations. Of those, only 339 were nonredundant, listed with correct contact information, and answered telephones during office hours. Furthermore, only 235 (25%) of the listed providers were accepting TRICARE, and only 200 of these were accepting new patients. It was also noted that providers in areas with the greatest density of National Guard troops were more likely to report that they were no longer accepting TRICARE coverage.
With regard to veterans’ access to mental-health services, some states have established public–private collaborative programs so veterans can seek care in areas of poor availability of VHA mental-health services. The VA also has recently hired more than 3,500 mental-health professionals, increasing the mental-health staff to more than 21,000 (VHA, 2011). However, even with the increase in personnel, concerns remain with regard to maldistribution of providers.
Finally, the literature documents a lack of training in combat-related mental-health treatments in the civilian workforce, despite the need for such programs (Burnam et al., 2009). For example, self-reports of mental-health problems and barriers to care in 200 active-duty Air
_____________________
10 The Salisbury VA Medical Center.
Force members indicated that some service members expressed hesitation to seek care from civilian providers due mainly to the inability to relate to the deployment experience (Visco, 2009).
Geographic Accessibility
Most active-duty service members and families live within 20 miles of a medical treatment facility and within 40 miles of inpatient services; however, less than 50% of National Guard and reserve members live within those described areas (DOD, 2011b). Time to travel to a treatment facility has been highlighted as a barrier to seeking care (see discussion above), although, as noted in Fortney et al. (2011), long distance to travel to a treatment facility has less impact on those with high levels of perceived need for care (e.g., cardiac issues) as opposed to those with lower levels of perceived need (e.g., substance use disorders).
Veterans enrolled in a low-priority group (as described in Table 9.1) with long distances to travel to VHA facilities will likely be deterred from seeking treatment (Burnam et al., 2009). Seal et al. (2010) conducted a study examining VA mental-health service utilization in nearly 85,000 OEF and OIF veterans who had received a new mental-health diagnosis. The veterans had at least one followup mental-health visit during the first year of the diagnosis. One finding was that veterans living more than 25 miles from a VA facility were less likely to receive the recommended PTSD treatment compared to veterans living within 25 miles of their treatment.
RESPONSE TO BARRIERS
Earlier in the chapter, the committee noted that important barriers to care included stigma, the military environment, and attitudes about treatment; wait times; clinical capacity; and geographic accessibility. Telemedicine is one response to most of those barriers in accessing care.
Telemedicine
Telemedicine has been defined as “the use of electronic information and communication technologies to provide support in health care when distance separates the participants (IOM, 1996). Historically, that definition included a variety of modalities such as e-mail, the Internet, phone, Fax, still imaging, and video-conferencing (Antonacci et al., 2008). A more recent and broader interpretation defines “virtual health care” as the use of communication and information technologies to bridge geographic distance and to facilitate the interactions and relationships necessary for providing accessible, coordinated, and high-quality care (Kizer, 2011).
Telemedicine provides a mechanism by which many access barriers might be overcome, particularly with regard to wait time, cost of care, travel distance to a treatment facility, and stigma (Pietrzak et al., 2009; Wong et al., 2007). The VHA has been in the forefront of information technology, and telemedicine has been a focus for recent VHA funding (Hill et al., 2010). Initiatives have been employed to expand services into a national telemental-health clinical and technical infrastructure. In FY 2011, 55,000 patients and 140,000 telemental-health visits were provided from 146 VA hospitals to 531 CBOCs (Darkins, 2012). The VHA currently provides various types of telehealth services, including services linking clinical settings with each other and in-home telehealth delivered directly to the patient’s home, which eliminates the
need for travel (VA, 2012b). Resulting from those VA initiatives, there is a growing body of literature describing and evaluating telemedicine, including telemental-health services in the veteran population, with the majority of studies focused on the treatment of PTSD and depression.
Two studies by Detweiler et al. (2011, 2012) describe the clinical experience of a collaborative telepsychiatry clinic between the VA and the US Army Warrior Transition Clinic (WTC). There are 38 WTCs on US military bases nationally and internationally that were developed to treat soldiers with the most severe health problems. Telepsychiatry offers a mechanism for VA mental-health professionals to treat returning OEF and OIF veterans with one or more mental-health diagnosis, and other medical comorbidities, in areas where there is limited access to timely evaluation and treatment. The authors examined data from telepsychiatry encounters at the Womack WTC (North Carolina Womack Army Medical Center) between September 2008 and August 2009. During those 12 months, 120 active-duty soldiers were seen for a total of 394 clinic visits. Prior to the implementation of the telepsychiatry team, soldiers on average waited more than 30 days to see a psychiatrist; after, the wait decreased to 22 days with a range of 1–79 days. At the start, 10% of the WTC psychiatry caseload was managed by the VA team; at the end of the 12-month period, that figure increased to 47%. The two most frequent diagnoses at psychiatry intake and at the last psychiatry visit were anxiety and mood disorders. Findings indicate that there was an increase in the incidence of anxiety and mood disorders from the VA psychiatric intake (anxiety, 59.2%, and mood disorders, 45.8%) to the final 12-month VA psychiatry visit (anxiety, 65.0%, and mood disorders, 46.7%). The authors acknowledge that the mental-health profile of this group is not representative of the entire OEF and OIF population, as the WTC typically treats the most traumatized soldiers. This innovative approach demonstrates an opportunity for collaboration between the DOD and VA in addressing the potential shortage of US Army psychiatrists. However, considering that the VA is also experiencing issues related to capacity, understaffing, and delivery of timely care, this approach may not be feasibly deployed as a systematic nationwide effort, but rather implementation on a site-by-site basis might be further explored (Detweiler et al., 2011, 2012).
Godleski et al. (2012) reports on outcomes in 98,609 veterans newly enrolled in telemental-health services between 2006 and 2010. Findings indicate that the total number of hospital admissions among the telemental-health patients dropped from 3,948 before enrollment in the program to 2,994 after enrollment; the total days for hospitalization fell from 35,532 before enrollment to 26,080 after enrollment. Several smaller studies, for example, also found positive outcomes using telemental-health. Morland et al. (2010) conducted a randomized controlled study to compare the effectiveness of cognitive behavioral anger management treatment delivered via televideoconferencing vs traditional in-person service delivery for rural combat veterans with PTSD. The study included 125 male veterans: one group received televideoconferencing treatment (n = 61), and the other received in-person treatment (n = 64). There was a significant reduction of PTSD symptoms posttreatment for both videoconferencing and in-person treatment, and both groups reported positive outcomes with no statistically significant differences; there was, however, high group therapy alliance observed in the inperson treatment group. Mohr et al. (2011) conducted a randomized controlled trial in a group of veterans meeting the DSM-IV diagnosis of depression to compare the effectiveness of telephoneadministered cognitive behavioral therapy (T-CBT) vs treatment as usual (TAU). Results indicated no significant treatment effects for the 16-session course of T-CBT and no statistically significant difference between the T-CBT and TAU group.
Ruskin et al. (2004) conducted a study comparing treatment outcomes and satisfaction of patients receiving treatment for depression remotely vs in person. Veterans suffering from depression who were referred to VA mental-health clinics (n = 119) were randomized to receive treatment through telepsychiatry (n = 59) or in person (n = 60). Results indicate scores on the Hamilton Depression Rating Scale and the Beck Depression Inventory improved significantly over the study period, however, with no significant differences between the two treatment modalities. There was also no difference in dropout rates or medication adherence between the two groups. General patient satisfaction also did not differ; however, psychiatrist satisfaction was greater for patients who received in-person treatment.
Hill et al. (2010) conducted a systematic review of 19 VHA-sponsored telemedicine interventions published between 2000 and 2009. The studies included populations over the age of 60 with issues of chronic disease management for multiple morbidities. Studies with a mean population age under 60 targeted mental-health, including PTSD and clinical depression. Conclusions indicate that telehealth interventions had distinct advantages, such as enhanced patient access to treatments, a medium for patient–provider communication, access to electronic medical record information, and the facilitation of collaborative care. The studies demonstrated that frequent contact between patient and provider fostered a therapeutic alliance and may increase patient satisfaction and willingness to participate in collaborative care. The authors concluded that telemedicine was one method of addressing issues for veterans struggling with access to care or living in areas without adequate facilities.
Remote health services such as diagnosis, assessment, case management, and treatment are provided by a VA-credentialed psychiatric practitioner at a main facility in Denver to patients located at a CBOC or tribal facility in a rural reservation. From April 2002 through February 2011, there have been 3,845 total sessions (3,220 individual followups and 44 group sessions) and 4,610 patient contacts. Clinical feasibility of services was established (Shore and Manson, 2004a, 2004b, 2005), and a high degree of patient and provider satisfaction was documented (Shore et al., 2008). Diagnostic reliability of videoconferencing was supported by evidence from a randomized controlled trial (Shore et al., 2007). Longitudinal clinical data showed a significant increase in medical service utilization associated with the subset of the clinics (Shore et al., 2012).
Wilson et al. (2008) conducted a study in 352 active-duty soldiers regarding their attitudes on the use of technology such as computerized therapy, video teleconferencing, and virtual reality in mental-health care. The majority were willing to use technology-based approaches to treatment (84%). Notably, 33% of soldiers who were not willing to speak to a counselor in person were willing to use at least one type of technology for mental-health treatment.
The VA is in a unique position to conduct national studies on the outcomes of telehealth because of the size of the telemental-health network and because of access to patient data from the electronic medical record (Godleski et al., 2012). The VA also has the opportunity to transform itself into an exemplary model of continuous and coordinated health care wherein patients can exchange secure messages through MyHealtheVet, and have automated transmission of patient data from in-home devices (i.e., videoconferencing) (Hogan et al., 2011; IOM, 2001). Also, many returning OEF and OIF service members and veterans are comfortable with the use of technology.
Thus, telemedicine offers an alternative to traditional health care delivery. It addresses most of the issues related to barriers to care identified in this report. Although its acceptance among active-duty service members and veterans is mixed, it appears to be more positive than negative. Telemedicine offers rural veterans the opportunity to access health care that they might not otherwise obtain and reduces wait time and addresses workforce capacity issues. Continued study on the efficacy of telemedicine will be needed to determine the value of this approach.
VHA Strategies to Improve Geographic Accessibility
In the early 1990s, the VHA implemented a system of CBOCs, which were designed to provide primary care, mental-health services, pharmacy benefits, and the management of acute and chronic conditions for veterans (Panangala and Mendez, 2010). CBOCs are separate entities from their parent medical facility; they can be either VA-owned and staffed or contracted to an HMO. The VA currently has more than 812 CBOCs throughout the United States and its territories, with plans to open 13 new facilities in nine states; it is expected that they will be operational over the next 3 years (VA, 2012c).
In a recent review, Kehle and Greer (2011) describe four studies that examined the impact of CBOCs on access to care (Fortney et al., 2002, 2005a, 2005b; Rosenheck, 2000). Findings from that review indicate a positive impact on geographic accessibility for veterans: CBOCs attracted more new users to the VA than did VAMCs; there was a decrease in travel distance to the closest VA facility for those in the CBOC catchment areas; and there was a higher rate of accessing VA medical services in counties with a CBOC. It was also noted that decreases in travel distance significantly predicted an increase in number of primary care encounters; however, improvements in health outcomes were small and not clinically significant.
The Government Accountability Office (GAO) highlighted other efforts to remove barriers and improve access for veterans (GAO, 2011b). These include VA integration of mental-health care into primary care, increasing the number of Vet Centers to provide confidential and free mental-health counseling; increasing the use of VA call centers; increasing VA mental-health staff; and expanded use of VA telemental-health services (discussed above). Additionally, the GAO notes that more than 2 million unique veterans received mental-health care at the VA between FY 2006 and FY 2010, with each year seeing an increase in veterans. The OEF and OIF veteran population accounts for that increase. VA began requiring its primary care clinics to conduct mental-health screenings for PTSD, depression, substance-use disorders, and history of MST. Since 2008, the VA requires mental-health providers to be on-site in mental-health clinics that treat more than 1,500 veterans annually. Those measures have been associated with a doubling of the number of unique patients receiving mental-health care in primary care clinics from 2008 through 2010.
The VA has continued to increase the number of Vet Centers as a mechanism to overcome barriers such as stigma and geographic accessibility. These centers provide confidential and free mental-health counseling services. VA increased the number of its Vet Centers from 232 to 292, from FY 2008 through August 2011. The VA has also increased the availability Vet Centers through the use of about 70 mobile Vet Centers to provide counseling services, especially to rural veterans.
VA call centers connect veterans with telephone-based counseling services. The VA has expanded the use of such centers, which, like Vet Centers, are free and confidential. One of the
call centers is a Veterans Crisis Line that allows not only veterans, but their family members to call and receive counseling. According to the VA, since 2007 it has received more than 400,000 calls and has referred more than 55,000 veterans to suicide-prevention coordinators for same-day or next-day services. The VA has also implemented programs to assist veterans and their family members with mental-health care. The VA now needs to study the effectiveness of those efforts in improving veterans’ access to mental-health care and determine how well they eliminate barriers. This will enable the VA to expand policies and programs that are effective and eliminate those that are not attaining their stated goals.
DOD MENTAL-HEALTH PREVENTION PROGRAMS
In response to recommendations from the DOD Mental-health Task Force, DOD has taken steps to reduce stigma while building psychologic fitness and resilience in service members. Prevention programs aim to foster more robust mental-health, involve leadership, and increase cohesion among service members. There are numerous prevention programs for mental-health issues within the DOD, almost all of which are aimed at promoting resilience. Resilience in these programs is rarely and inconsistently defined, according to RAND, which catalogued 23 resilience programs (Meredith et al., 2011). Moreover, there are few studies of program effectiveness. Here the committee focuses on the most prominent prevention programs for which there is evidence of efficacy in alleviating the occurrence of psychiatric symptoms or disorders.11 Both the RAND report and a recent IOM report (IOM, 2012) comprehensively describe the wide-ranging prevention programs. Two of these programs are highlighted below.
Battlemind
Battlemind—now referred to as Resilience Training—is a training program originally developed by Army researchers to ease returning troops’ transition from combat to civilian life. Its explicit purpose is to promote resilience and prevent postcombat psychosocial problems. Battlemind is a group training intervention that draws on positive psychology and cognitive behavioral techniques to reframe combat experience into adaptive experiences at home, away from the front lines (Castro et al., 2006; Orsingher et al., 2008). The Army mandated Battlemind in 2007, and since then some of its components have been extended to different stages of deployment (Williams, 2008).
The term “Battlemind” is an acronym, each letter of which stands for a strength or skill to adapt from the combat mindset to that in civilian life. The “B” in Battlemind stands for “buddies,” and the intervention strives to teach that reliance on buddies, while essential to unit cohesiveness, can be detrimental at home, where service members need to make the shift from buddies to reliance on family and friends. A pervasive problem is that service members, upon return, tend to withdraw from family and friends because they feel that only their buddies can understand what they have experienced. Battlemind seeks to prevent withdrawal from families and friends through skill training. Similarly, the program teaches that hypervigilance, which is crucial during combat, is maladaptive at home; in fact, hypervigilance in civilian life is one of the hallmarks of PTSD.
_____________________
The concepts behind Battlemind have also been incorporated into a new variant of psychologic debriefing known as “Battlemind debriefing” (Adler et al., 2009a, 2009b). It is a group-level intervention run by a specially trained professional facilitator to resemble the more familiar critical incident debriefing or a military after-action review (Adler et al., 2009a). The goal is for the group to arrive at lessons learned after a traumatic event and to focus on reintegration through resilience. Participants are encouraged to recall traumatic events, but in a limited way to prevent their own retraumatization or prevent exposing others to trauma. Standard psychologic debriefing has been criticized for its heavy emphasis on the traumatic experience, which risks retraumatization and worsening of mental-health (McNally et al., 2003).
The efficacy of Battlemind has been measured in a few studies. Adler and colleagues compared Battlemind training and Battlemind debriefing in 2,297 Army active-duty service members returning from a 12-month deployment to Iraq (Adler et al., 2009a). Platoons were randomly assigned to Battlemind training, Battlemind debriefing, or the Army’s standard postdeployment stress education. A cluster randomization was conducted at the level of the platoon (rather than the individual). The study assessed symptoms of PTSD, depression, and sleep problems, once at the beginning of the 7-day reintegration period and then 4 months later (n = 1,060). Compared with stress education, the Battlemind debriefing was associated with fewer symptoms of PTSD, depression, and sleep problems, but only among those with high combat exposure. Battlemind training that was delivered in a small group (18–45 individuals), as compared to stress education, was associated with fewer PTSD and depression symptoms, again only among those highly exposed to combat. Battlemind training that was delivered in a large group setting (126–225 individuals) reported fewer symptoms of PTSD, fewer stigmatizing beliefs about mental-health, and, irrespective of combat exposure, fewer depression symptoms. The researchers concluded that both types of Battlemind programs were efficacious for service members with high combat exposure.
The findings propelled UK researchers to test an anglicized version of Battlemind in a cluster randomized controlled trial similar in design to that of Adler and colleagues. Mulligan et al. (2012) compared Battlemind to “standard care” by the UK military, i.e., a postdeployment standardized lecture on stress and homecoming. The most prominent change to Battlemind was an increased emphasis on alcohol, as alcohol problems are more prevalent in the United Kingdom than in the US military. Researchers assessed outcomes on the PTSD Checklist, the General Health Questionnaire, the Patient Health Questionnaire, and the Alcohol Use Disorders Identification Test (AUDIT). Six months after the program, the investigators found no improvement in mental-health or the overall AUDIT score, but those who received Battlemind were less likely to report binge drinking. The effect size, however, was small.
Comprehensive Soldier Fitness
Comprehensive Soldier Fitness (CSF) is an Army-wide resilience program introduced in 2009. Its broad goal is to prevent adverse consequences of combat through resilience and mental fitness. More specifically, the goals are to enhance soldiers’ ability to handle adversity, prevent depression and anxiety, prevent PTSD, and enhance overall well-being and performance (Reivich et al., 2011). The program was derived from an evidence-based civilian program, the Penn Resiliency Program (Brunwasser et al., 2009), which draws on cognitive-behavioral theories of depression. The CSF program has four components (Cornum et al., 2011):
1. Assessment. Psychologic fitness is assessed through a comprehensive questionnaire known as the Global Assessment Tool (GAT), which was expressly developed for the CSF. The GAT measures psychologic fitness in four domains: emotional, social, family, and spiritual fitness. Service members are expected to take the GAT at recruitment and then on an annual basis thereafter to monitor their own growth. The results are confidential, with the Army only monitoring aggregate data. The key point about the GAT is that measuring psychologic fitness is seen as important as measuring physical fitness (Peterson et al., 2011). A special GAT is available for family members.
2. Universal resilience training. This is accomplished by online training modules that focus on teaching specific resilience skills. Thus far there are 20 such modules focusing on each of the dimensions measured by the GAT (emotional, social, family, and spiritual fitness).
3. Individualized training. This component of the program tailors resilience training to domains that are needed according to performance on the GAT. It is not a one-size-fits-all approach, unlike universal resilience training (above).
4. Master Resilience Trainer Course (MRT). This is a train-the-trainer approach via a 10-day resilience training course for noncommissioned officers, primarily Staff Sergeants or Sergeants First Class. The MRT course is designed to train resilience skills to noncommissioned officers in a way that they in turn can teach these skills to their soldiers. The Army’s goal is to have MRT experts in every company for the purpose of monitoring CSF and its component domains (Reivich et al., 2011).
The efficacy of Comprehensive Soldier Fitness has not yet been formally evaluated, but its predecessor program, the Penn Resiliency Program, has been evaluated by at least 17 controlled studies. A meta-analysis of those studies found a modest effect of the Penn program in reducing depression symptoms 12 months after the program’s introduction (Brunwasser et al., 2009). The meta-analysis found no significant effect of the program in preventing diagnoses of depression.
Several research projects are planned or are currently in progress regarding the CSF program. One assessment will focus on whether the CSF program influences the rate of suicide, divorce, PTSD, crime, reenlistment, and promotion of rank (Lester et al., 2011). A longitudinal study is currently under way to determine if the Master Resilience Training program and the computer modules foster longstanding resilience. Another evaluation effort is designed to measure the empirical validity of the GAT (Peterson et al., 2011). A final study will be examining physiological and neurobiological correlates of psychologic resilience.
CONCLUSIONS
Access to heath care is defined as the timely use of service to achieve the best possible health care outcome. Active-duty military and veterans access their health care through the DOD’s military health system, TRICARE, and the VA’s health care system, respectively. Fragmentation of care in both those systems does occur. Electronic health records offer the promise of minimizing fragmentation of care, but the DOD and VA have not yet integrated their health records.
There are disparities in health care in the DOD and VA health care systems. In particular, women face some unique stressors, and more study is needed to understand issues relevant to them. Military sexual assault needs to be addressed both in the DOD and the VA. There are limited studies in racial and ethnic minorities; however, studies show patterns of diagnostic inconsistencies between different racial groups. Those variations might be due to provider insensitivity toward cultural behaviors regarding mental-health. Rural veterans face many challenges in gaining access to care, and those veterans typically have more physical comorbidities and worse health-related quality of life than veterans in more urban areas.
Barriers to health care access include stigma, the military culture, and attitudes about treatment; long wait times for care; limited workforce capacity; and geographic accessibility. There is a continued high prevalence of stigma associated with mental-health problems and their treatment. Many active-duty service members are concerned about possible adverse effects of mental-health diagnoses and treatment on career advancement. Service members are reluctant to seek care for mental-health problems due to concerns about the privacy of their health information. The DOD and the VA have initiated policies and procedures to address those barriers, but clearly more needs to be done. Telemedicine offers promise as a mechanism to address those barriers; however, continued evaluation should occur to determine its acceptance and efficacy. Finally, the DOD has implemented programs for prevention of mental-health and resiliency training; those programs should be evaluated.
RECOMMENDATIONS
Transitioning from the DOD health care system to the VA health care system presents challenges for OEF and OIF service men and women. There are numerous difficulties in navigating services because of the complexities of both systems. Although DOD and VA are making administrative changes to alleviate some of the problems, information sharing between the two agencies remains a problem.
The committee recommends improved coordination of care and services between the Department of Defense and the Department of Veterans Affairs medical treatment facilities, including the completion of an interoperable or single combined electronic health record for all care that begins with entry into military service and continues throughout care in the Department of Veterans Affairs system after transition.
Stigma is still a problem for military personnel in care or seeking care for mental-health or substance-abuse problems. Active-duty military fear that visits to a mental-health provider will jeopardize their careers because of the military’s long-standing policy of reporting mental-health and substance-abuse problems to the chain of command. Mixed messages about seeking treatment and concerns about health-information privacy remain disincentives to seeking care.
The committee recommends that the Department of Defense continue to promote an environment that reduces stigma and encourages treatment for mental-health and substance-use disorders. The committee recommends that the department undertake a systematic review of its policies regarding mental-health and substance-abuse treatment with regard to issues of confidentiality and the relation
between treatment-seeking and military advancement. The committee recommends that the department regularly issue reports describing actions taken with regard to its policies and procedures to determine progress in this area.
Excessive wait time is a complaint often expressed by both active-duty and veteran service members. Long wait times can compromise health because of delayed use and decreased patient satisfaction. In addition, adverse long-term outcomes, such as death and preventable hospitalizations, are more common for veterans who seek care at facilities that have longer wait times than for veterans at facilities that have shorter wait times.
Poor availability and misdistribution of mental-health specialists in many parts of the United States, especially in rural areas, present substantial barriers to OEF and OIF veterans’ access to mental-health care. For active-duty service members, inadequate participating provider networks present a challenge for accessing mental-health care.
The committee recommends that the Department of Defense and the Department of Veterans Affairs conduct a needs assessment to determine the numbers and types of providers needed to address the long-term health needs of Operation Enduring Freedom, Operation Iraqi Freedom, and Operation New Dawn activeduty service members and veterans. The Department of Defense and the Department of Veterans Affairs should determine the optimal team composition—for example, MDs, PhDs, RNs, master’s-trained professionals, and peer counselors—needed to ensure that providers function efficiently and perform at the upper level of their credentials and privileges.
There is evidence of cultural insensitivity to nonwhite service members, who might have different or more severe physical-health and mental-health problems than their white counterparts. For example, black personnel are less likely than white personnel to use mental-health services and quicker to drop out of treatment. Issues related to types of diagnoses and potential misdiagnoses have also been raised. Whether clinicians who have ethnic characteristics similar to those of their patients would alleviate those problems is unknown.
The committee recommends that the Department of Defense, the Department of Veterans Affairs, and other federal agencies fund research to determine whether culturally sensitive clinicians and treatment approaches improve retention in care and improve clinical outcomes.
Women now constitute 14% of deployed forces in the US military, and an unprecedented number of female soldiers are deployed to combat areas. Although all service members are exposed to high levels of workplace stress, women in the military face some unique stressors, such as MST, which may affect their mental-health and emotional well-being. Female veterans report a higher burden of medical illness and worse quality-of-life outcomes than do men who are exposed to the same levels of trauma. MST appears to be an important risk factor for the development of PTSD.
The committee recommends that the Department of Defense and the Department of Veterans Affairs consider ways to remove barriers and improve women’s access to and use of health care in their systems. The two departments should examine
issues related to women’s circumstances and stressors—such as military workplace stress, sexual harassment and assault, posttraumatic stress disorder, and premilitary trauma—in an effort to reduce disparities and to provide health care that is sensitive to their needs and preferences.
REFERENCES
Adler, A. B., P. D. Bliese, D. McGurk, C. W. Hoge, and C. A. Castro. 2009a. Battlemind debriefing and battlemind training as early interventions with soldiers returning from Iraq: Randomization by platoon. Journal of Consulting and Clinical Psychology 77(5):928-940.
Adler, A. B., C. A. Castro, and D. McGurk. 2009b. Time-driven battlemind psychological debriefing: A group-level early intervention in combat. Military Medicine 174(1):21-28.
Ames, G. M., C. B. Cunradi, R. S. Moore, and P. Stern. 2007. Military culture and drinking behavior among US Navy careerists. Journal of Studies on Alcohol and Drugs 68(3):336-344.
Andrews, K., K. Bencio, J. Brown, L. Conwell, C. Fahlman, and E. Schone. 2009. Health Care Survey of DOD Beneficiaries 2008 Annual Report. Washington, DC: Mathematica Policy Research, Inc.
Antonacci, D. J., R. M. Bloch, S. A. Saeed, Y. Yildirim, and J. Talley. 2008. Empirical evidence on the use and effectiveness of telepsychiatry via videoconferencing: Implications for forensic and correctional psychiatry. Behavioral Sciences and the Law 26(3):253-269.
Avery, G. H., and S. MacDermid Wadsworth. 2011. Access to mental-health services for active duty and National Guard TRICARE enrollees in Indiana. Military Medicine 176(3):261-264.
Bagchi, A., K. Bencio, J. Kim, M. Lee, and E. Schone. 2007. Health Care Survey of DOD Beneficiaries 2007 Annual Report. Washington, DC: Mathmatica Policy Research, Inc.
Barton, P. L., A. G. Brega, P. A. Devore, K. Mueller, M. J. Paulich, N. R. Floersch, G. K. Goodrich, S. G. Talkington, J. Bontrager, B. Grigsby, C. Hrincevich, S. Neal, J. L. Loker, T. M. Araya, R. E. Bennett, N. Krohn, and J. Grigsby. 2007. Specialist physicians’ knowledge and beliefs about telemedicine: A comparison of users and nonusers of the technology. Telemedicine Journal and E-Health 13(5):487-499.
Beals, J., S. M. Manson, J. H. Shore, M. Friedman, M. Ashcraft, J. A. Fairbank, and W. E. Schlenger. 2002. The prevalence of posttraumatic stress disorder among American Indian Vietnam veterans: Disparities and context. Journal of Traumatic Stress 15(2):89-97.
Bean-Mayberry, B., C. Huang, F. Batuman, C. Goldzweig, D. L. Washington, E. M. Yano, and I. M. Miake-Lye. 2010. Systematic Review of Women Veterans Health Research 2004-2008. Los Angeles, CA: Evidence-based Synthesis Program (ESP) Center.
Bean-Mayberry, B., E. M. Yano, D. L. Washington, C. Goldzweig, F. Batuman, C. Huang, I. Miake-Lye, and P. G. Shekelle. 2011. Systematic review of women veterans’ health: Update on successes and gaps. Womens Health Issues 21(4 Suppl):S84-S97.
Bertakis, K. D., R. Azari, L. J. Helms, E. J. Callahan, and J. A. Robbins. 2000. Gender differences in the utilization of health care services. Journal of Family Practice 49(2):147-152.
Britt, T. W. 2000. The stigma of psychological problems in a work environment: Evidence from the screening of service members returning from Bosnia. Journal of Applied Social Psychology 30(8):1599-1618.
Britt, T. W., T. M. Greene-Shortridge, S. Brink, Q. B. Nguyen, J. Rath, A. L. Cox, C. W. Hoge, and C. A. Castro. 2008. Perceived stigma and barriers to care for psychological treatment: Implications for reactions to stressors in different contexts. Journal of Social and Clinical Psychology 27:19.
Britt, T. W., E. A. Bennett, M. Crabtree, C. Haugh, K. Oliver, A. McFadden, and C. L. S. Pury. 2011. The theory of planned behavior and reserve component veteran treatment seeking. Military Psychology 23(1):82-96.
Britt, T. W., K. M. Wright, and D. Moore. 2012. Leadership as a predictor of stigma and practical barriers toward receiving mental-health treatment: A multilevel approach. Psychological Services 9(1):26-37.
Brod, R. L., P. A. May, and T. J. Stewart. 1982. Recruitment and retention of federal physicians on the Navajo reservation. Social Science Journal 19(4):47-66.
Brooks, E., D. K. Novins, D. Thomas, L. Jiang, H. T. Nagamoto, N. Dailey, B. Bair, and J. H. Shore. 2012. Personal characteristics affecting veterans’ use of services for posttraumatic stress disorder. Psychiatric Services 63(9):862-867.
Brunwasser, S. M., J. E. Gillham, and E. S. Kim. 2009. A meta-analytic review of the Penn Resiliency program’s effect on depressive symptoms. Journal of Consulting and Clinical Psychology 77(6):1042-1054.
Burnam, M. A., L. S. Meredith, T. Tanielian, and L. H. Jaycox. 2009. Mental-health care for Iraq and Afghanistan war veterans. Health Affairs 28(3):771-782.
Buzza, C., S. S. Ono, C. Turvey, S. Wittrock, M. Noble, G. Reddy, P. J. Kaboli, and H. S. Reisinger. 2011. Distance is relative: Unpacking a principal barrier in rural healthcare. Journal of General Internal Medicine 26(2 Suppl):648-654.
Castro, C. A., C. W. Hoge, C. W. Milliken, D. McGurk, and A. B. Adler. 2006. Battlemind Training: Transitioning Home from Combat. Silver Spring, MD: Walter Reed Army Institute of Research.
CBO (Congressional Budge Office). 2009. Quality Initiatives Undertaken by the Veterans Health Administration. Washington, DC: Congressional Budget Office.
———. 2011. CBO Testimony: Statement of Randall B. Williamson, Director, Health Care Federal Recovery Coordination Program: Enrollment, Staffing, and Care Coordination Pose Significant Challenges before Subcommittee on Health, Committee on Veterans’ Affairs, House of Representatives, May 13, 2011.
Chermack, S. T., K. Zivin, M. Valenstein, M. Ilgen, K. L. Austin, J. Wryobeck, and F. C. Blow. 2008. The prevalence and predictors of mental-health treatment services in a national sample of depressed veterans. Medical Care 46(8):813-820.
Christensen, E., P. Netzer, E. Schaefer, C. Hill, D. Farr, and J. McMahon. 2009. Economic Impact on Caregivers of the Seriously Wounded, Ill, and Injured. Alexandria, VA: Center for Naval Analyses.
Cornum, R., M. D. Matthews, and M. E. P. Seligman. 2011. Comprehensive soldier fitness building resilience in a challenging institutional context. American Psychologist 66(1):4-9.
Darkins, A. 2012. Experiences of the Department of Veterans Affairs and the Indian Health Services. Paper read at Workshop on the Role of Telehealth in an Evolving Health Care Environment, August 9, Washington, DC.
Deployment Health Clinical Center. 2012. DOD/VA/Federal Healthcare Services. http://www.pdhealth.mil/hss/healthcare_services.asp#mhs (accessed September 25, 2012).
Detweiler, M. B., S. Arif, J. Candelario, J. Altman, P. F. Murphy, M. H. Hailing, J. G. Detweiler, and S. Vasudeva. 2011. A telepsychiatry transition clinic: The first 12 months experience. Journal of Telemedicine and Telecare 17(6):293-297.
Detweiler, M. B., S. Arif, J. Candelario, J. Altman, P. F. Murphy, M. H. Halling, S. Vasudeva, and J. G. Detweiler. 2012. Salem VAMC-US Army Fort Bragg warrior transition clinic telepsychiatry collaboration: 12-month operation clinical perspective. Telemedicine Journal and E-Health 18(2):81-86
Dickstein, B. D., D. S. Vogt, S. Handa, and B. T. Litz. 2010. Targeting self-stigma in returning military personnel and veterans: A review of intervention strategies. Military Psychology 22(2):224-236.
DOD (Department of Defense). 2011a. Evaluation of the TRICARE Program. Washington, DC: DOD.
———. 2011b. MHS Stakeholder’s Report. Washington, DC: DOD.
———. 2012. TRICARE (webpage). http://www.tricare.mil/mybenefit/ProfileFilter.do;jsessionid=PQ2hM96Jx9ybGG8xnbhCwqnvK331Lxql3d5vQgcLjC1pNv21J2ND!349025571?puri=%2Fhome (accessed March 2, 2012).
Donaldson, M. S. 2001. Continuity of care: A reconceptualization. Medical Care Research and Review 58(3):255-290.
Fannin, J. M., and J. N. Barnes. 2007. Recruitment of physicians to rural America: A view through the lens of transaction cost theory. Journal of Rural Health 23(2):141-149.
Foa, E. B., E. A. Hembree, S. P. Cahill, S. A. Rauch, D. S. Riggs, N. C. Feeny, and E. Yadin. 2005. Randomized trial of prolonged exposure for posttraumatic stress disorder with and without cognitive restructuring: Outcome at academic and community clinics. Journal of Consulting and Clinical Psychology 73(5):953-964.
Fortney, J. C., B. M. Booth, F. C. Blow, and J. Y. Bunn. 1995. The effects of travel barriers and age on the utilization of alcoholism treatment aftercare. American Journal of Drug and Alcohol Abuse 21(3):391-406.
Fortney, J. C., S. J. Borowsky, A. N. Hedeen, M. L. Maciejewski, and M. K. Chapko. 2002. VA community-based outpatient clinics: Access and utilization performance measures. Medical Care 40(7):561-569.
Fortney, J. C., M. L. Maciejewski, J. J. Warren, and J. F. Burgess, Jr. 2005a. Does improving geographic access to VA primary care services impact patients’ patterns of utilization and costs? Inquiry 42(1):29-42.
Fortney, J. C., D. E. Steffick, J. F. Burgess, Jr., M. L. Maciejewski, and L. A. Petersen. 2005b. Are primary care services a substitute or complement for specialty and inpatient services? Health Services Research 40(5 Pt 1):1422-1442.
Fortney, J. C., J. F. Burgess, Jr., H. B. Bosworth, B. M. Booth, and P. J. Kaboli. 2011. A reconceptualization of access for 21st century healthcare. Journal of General Internal Medicine 26(2 Suppl):639-647.
GAO (Government Accountability Office). 2011a. DOD and VA Health Care: Federal Recovery Coordination Program Continues to Expand but Faces Significant Challenges. Washington, DC: GAO.
———. 2011b. VA Mental-health: Number of Veterans Receiving Care, Barriers Faced, and Efforts to Increase Access. Washington, DC: GAO.
Gibbs, D. A., K. L. Rae Olmsted, J. M. Brown, and A. Clinton-Sherrod. 2011. Dynamics of stigma for alcohol and mental-health treatment among army soldiers. Military Psychology 23(1):36-51.
Godleski, L., A. Darkins, and J. Peters. 2012. Outcomes of 98,609 US Department of Veterans Affairs patients enrolled in telemental-health services, 2006-2010. Psychiatric Services 63(4):383-385.
Gorman, L. A., A. J. Blow, B. D. Ames, and P. L. Reed. 2011. National Guard families after combat: Mental-health, use of mental-health services, and perceived treatment barriers. Psychiatric Services 62(1):28-34.
Greene-Shortridge, T. M., T. W. Britt, and C. A. Castro. 2007. The stigma of mental-health problems in the military. Military Medicine 172(2):157-161.
Grigsby, B., A. G. Brega, R. E. Bennett, P. A. Devore, M. J. Paulich, S. G. Talkington, N. R. Floersch, P. L. Barton, S. Neal, T. M. Araya, J. L. Loker, N. Krohn, and J. Grigsby. 2007. The slow pace of interactive video telemedicine adoption: The perspective of telemedicine program administrators on physician participation. Telemedicine Journal and E-Health 13(6):645-656.
Hannold, E. M., I. M. Freytes, and C. R. Uphold. 2011. Unmet health services needs experienced by Puerto Rican OEF/OIF veterans and families post deployment. Military Medicine 176(4):381-388.
Harada, N. D., J. Damron-Rodriguez, V. M. Villa, D. L. Washington, S. Dhanani, H. Shon, M. Chattopadhyay, H. Fishbein, M. Lee, T. Makinodan, and R. Andersen. 2002. Veteran identity and race/ethnicity: Influences on VA outpatient care utilization. Medical Care 40(1 Suppl):I117-I128.
Hill, R. D., M. K. Luptak, R. W. Rupper, B. Bair, C. Peterson, N. Dailey, and B. L. Hicken. 2010. Review of Veterans Health Administration telemedicine interventions. American Journal of Managed Care 16(12 Suppl):e302-e310.
Himmelstein, D. U., K. E. Lasser, D. McCormick, D. H. Bor, J. W. Boyd, and S. Woolhandler. 2007. Lack of health coverage among US veterans from 1987 to 2004. American Journal of Public Health 97(12):2199-2203.
Hoerster, K. D., C. A. Malte, Z. E. Imel, Z. Ahmad, S. C. Hunt, and M. Jakupcak. 2012. Association of perceived barriers with prospective use of VA mental-health care among Iraq and Afghanistan veterans. Psychiatric Services 63(4):380-382.
Hogan, T. P., B. Wakefield, K. M. Nazi, T. K. Houston, and F. M. Weaver. 2011. Promoting access through complementary ehealth technologies: Recommendations for VA’s home telehealth and personal health record programs. Journal of General Internal Medicine 26(2 Suppl):628-635.
Hoge, C. W., K. Wright, P. Bliese, A. Adler, and J. Thomas. 2004. Prevalence and Screening of Mental-Health Problems Among US Combat Soldiers Pre- and Post- Deployment. Silver Spring, MD: Walter Reed Army Institute of Research.
Hoge, C. W., C. A. Castro, S. C. Messer, D. McGurk, D. I. Cotting, and R. L. Koffman. 2008. Combat duty in Iraq and Afghanistan, mental-health problems and barriers to care. US Army Medical Department Journal:7-17.
Holiday, L. F., G. Bell, R. E. Klein, and M. R. Wells. 2006. American Indian and Alaska Native Veterans: Lasting Contributions. Washington, DC: Assistant Secretary for Policy, Planning, and Preparedness, Department of Veterans Affairs.
Hostetter, C. L., and J. D. Felsen. 1975. Multiple variable motivators involved in the recruitment of physicians for the Indian Health Service. Public Health Reports 90(4):319-324.
Hyun, J. K., J. Pavao, and R. Kimerling. 2009. Military sexual trauma. PTSD Research Quarterly 20(2).
IOM (Institute of Medicine). 1996. Telemedicine: A Guide to Assessing Telecommunications for Health Care. Washinton, DC: National Academy Press.
———. 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
———. 2005. Quality Through Collaboration: The Future of Rural Health Care. Washington, DC: The National Academies Press.
———. 2009. Combating Tobacco Use in Military and Veteran Populations. Washington, DC: The National Academies Press.
———. 2010. Returning Home from Iraq and Afghanistan: Preliminary Assessment of Readjustment Needs of Veterans, Service Members, and Their Families. Washington, DC: The National Academies Press.
———. 2012. Treatment for Posttraumatic Stress Disorder in Military and Veteran Populations: Initial Assessment. Washington, DC: The National Academies Press.
Jackson, G. L., S. L. Krein, D. C. Alverson, A. W. Darkins, W. Gunnar, N. D. Harada, C. D. Helfrich, T. K. Houston, T. F. Klobucar, K. M. Nazi, R. K. Poropatich, J. D. Ralston, and H. B. Bosworth. 2011. Defining core issues in utilizing information technology to improve access: Evaluation and research agenda. Journal of General Internal Medicine 26(2 Suppl):623-627.
Johnson, J. L., and M. C. Cameron. 2001. Barriers to providing effective mental-health services to American Indians. Mental-health Services Research 3(4):215-223.
Johnson, P. J., K. F. Carlson, and M. O. Hearst. 2010. Healthcare disparities for American Indian veterans in the United States: A population-based study. Medical Care 48(6):563-569.
Kaelber, D., and E. C. Pan. 2008. The value of personal health record (PHR) systems. AMIA Annual Symposium proceedings:343-347.
Kane, T. 2006. Who Are the Recruits? The Demographic Characteristics of US Military Enlistment, 2003-2005. Washington, DC: The Heritage Foundation.
Kapusta, N. D., A. Zorman, E. Etzersdorfer, E. Ponocny-Seliger, E. Jandl-Jager, and G. Sonneck. 2008. Rural-urban differences in austrian suicides. Social Psychiatry and Psychiatric Epidemiology 43(4):311-318.
Kaufman, C., E. Brooks, T. Noe, B. Bair, N. Dailey, and J. Shore. 2010. How Rural are American Indian and Alaska Native Veterans? Salt Lake City, UT: Veterans Rural Health Resource Center, Western Region Native Domain.
Kehle, S., and N. Greer. 2011. Interventions to Improve Veterans’ Access to Care: A Systematic Review of the Literature. Washington, DC: Department of Veterans Affairs, Evidence-Based Synthesis Program Center.
Kehle, S. M., M. A. Polusny, M. Murdoch, C. R. Erbes, P. A. Arbisi, P. Thuras, and L. A. Meis. 2010. Early mental-health treatment-seeking among US National Guard soldiers deployed to Iraq. Journal of Traumatic Stress 23(1):33-40.
Kelly, M. M., D. S. Vogt, E. M. Scheiderer, P. Ouimette, J. Daley, and J. Wolfe. 2008. Effects of military trauma exposure on women veterans’ use and perceptions of Veterans Health Administration care. Journal of General Internal Medicine 23(6):741-747.
Kessler, R. C., P. A. Berglund, M. L. Bruce, J. R. Koch, E. M. Laska, P. J. Leaf, R. W. Manderscheid, R. A. Rosenheck, E. E. Walters, and P. S. Wang. 2001. The prevalence and correlates of untreated serious mental illness. Health Services Research 36(6 Pt 1):987-1007.
Kim, P. Y., T. W. Britt, R. P. Klocko, L. A. Riviere, and A. B. Adler. 2011. Stigma, negative attitudes about treatment, and utilization of mental-health care among soldiers. Military Psychology 23(1):65-81.
Kimerling, R., K. Gima, M. W. Smith, A. Street, and S. Frayne. 2007. The Veterans Health Administration and military sexual trauma. American Journal of Public Health 97(12):2160-2166.
Kimerling, R., A. E. Street, J. Pavao, M. W. Smith, R. C. Cronkite, T. H. Holmes, and S. M. Frayne. 2010. Military-related sexual trauma among Veterans Health Administration patients returning from Afghanistan and Iraq. American Journal of Public Health 100(8):1409-1412.
Kizer, K. W. 2011. The emerging era of virtual healthcare. Paper read at VHA Visioning Summit on Virtual Health Care Delivery, October 13, 2010, Arlington, VA.
———. 2012. Veterans and the Affordable Care Act. Journal of the American Medical Association 307(8):789-790.
Kizer, K. W., and R. A. Dudley. 2009. Extreme makeover: Transformation of the veterans health care system. Annual Review of Public Health 30:313-339.
Koenig, K. L. 2003. Homeland security and public health: Role of the Department of Veterans Affairs, the US Department of Homeland Security, and implications for the public health community. Prehospital and Disaster Medicine 18(4):327-333.
Kramer, B. J., M. Wang, S. Jouldjian, M. L. Lee, B. Finke, and D. Saliba. 2009. Veterans Health Administration and Indian Health Service: Healthcare utilization by Indian Health Service enrollees. Medical Care 47(6):670-676.
Lester, P. B., S. McBride, P. D. Bliese, and A. B. Adler. 2011. Bringing science to bear an empirical assessment of the Comprehensive Soldier Fitness program. American Psychologist 66(1):77-81.
Levin, K. A., and A. H. Leyland. 2005. Urban/rural inequalities in suicide in Scotland, 1981–1999. Social Sciences and Medicine 60(12):2877-2890.
Link, B. G., and J. C. Phelan. 2001. Conceptualizing stigma. Annual Review of Sociology 27:363-385.
Lipari, R. N., P. J. Cook, L. M. Rock, and K. Matos. 2008. 2006 Gender Relations Survey of Active Duty Members. Arlington, VA: Defense Manpower Data Center.
Litz, B. T., S. M. Orsillo, M. Friedman, P. Ehlich, and A. Batres. 1997. Posttraumatic stress disorder associated with peacekeeping duty in Somalia for US military personnel. American Journal of Psychiatry 154(2):178-184.
Liu, C. F., M. L. Maciejewski, and A. E. Sales. 2005. Changes in characteristics of veterans using the VHA health care system between 1996 and 1999. Health Research Policy and Systems 3(1):5.
Maguen, S., T. J. Metzler, B. T. Litz, K. H. Seal, S. J. Knight, and C. R. Marmar. 2009. The impact of killing in war on mental-health symptoms and related functioning. Journal of Traumatic Stress 22(5):435-443.
Maguen, S., B. Cohen, G. Cohen, E. Madden, D. Bertenthal, and K. Seal. 2012. Gender differences in health service utilization among Iraq and Afghanistan veterans with posttraumatic stress disorder. Journal of Women’s Health 21(6):666-673.
McCarthy, J. F., J. D. Piette, J. C. Fortney, M. Valenstein, and F. C. Blow. 2006. Outpatient visit chaining among patients with serious mental illness. Medical Care 44(3):257-264.
McCarthy, J. F., F. C. Blow, R. V. Ignacio, M. A. Ilgen, K. L. Austin, and M. Valenstein. 2012. Suicide among patients in the Veterans Affairs health system: Rural–urban differences in rates, risks, and methods. American Journal of Public Health 102(S1):S111-S117.
McNally, R. J., R. A. Bryant, and A. Ehlers. 2003. Does early psychological intervention promote recovery from posttraumatic stress? Psychological Science in the Public Interest 4(2):45-79.
Meredith, M., C. D. Sherbourne, S. Gailot, L. Hansell, H. V. Ritschard, A. M. Parker, and G. Wrenn. 2011. Promoting Psychological Resilience in the US Military. Santa Monica, CA: RAND Corporation.
Merlis, M. 2012. The Future of Health Care for Military Personnel and Veterans. Washington, DC: Academy Health.
Middleton, N., D. Gunnell, S. Frankel, E. Whitley, and D. Dorling. 2003. Urban-rural differences in suicide trends in young adults: England and Wales, 1981-1998. Social Science and Medicine 57(7):1183-1194.
Military.com. 2012a. Transition Assistance Management Program.
http://www.military.com/benefits/tricare/transition-assistance-management-program.html (accessed November 8, 2012).
———. 2012b. TRICARE: Benefits. http://www.military.com/benefits/tricare (accessed September 25, 2012).
Mohr, D. C., T. Carmody, L. Erickson, L. Jin, and J. Leader. 2011. Telephone-administered cognitive behavioral therapy for veterans served by community-based outpatient clinics. Journal of Consulting and Clinical Psychology 79(2):261-265.
Morland, L. A., C. J. Greene, C. S. Rosen, D. Foy, P. Reilly, J. Shore, Q. He, and B. C. Frueh. 2010. Telemedicine for anger management therapy in a rural population of combat veterans with posttraumatic stress disorder: A randomized noninferiority trial. Journal of Clinical Psychiatry 71(7):855-863.
Mulligan, K., N. T. Fear, N. Jones, H. Alvarez, L. Hull, U. Naumann, S. Wessely, and N. Greenberg. 2012. Postdeployment Battlemind training for the U.K. Armed Forces: A cluster randomized controlled trial. Journal of Consulting and Clinical Psychology 80(3):331-341.
Murdoch, M., J. Hodges, D. Cowper, L. Fortier, and M. van Ryn. 2003. Racial disparities in VA service connection for posttraumatic stress disorder disability. Medical Care 41(4):536-549.
National Council on Disability. 2009. Invisible Wounds: Serving Service Members and Veterans with PTSD and TBI. Washington, DC: National Council on Disability.
Nazi, K. M. 2010. Veterans' voices: Use of the American Customer Satisfaction Index (ACSI) survey to identify My Healthevet personal health record users’ characteristics, needs, and preferences. Journal of the American Medical Informatics Association 17(2):203-211.
Nazi, K. M., T. P. Hogan, T. H. Wagner, D. K. McInnes, B. M. Smith, D. Haggstrom, N. R. Chumbler, A. L. Gifford, K. G. Charters, J. J. Saleem, K. R. Weingardt, L. F. Fischetti, and F. M. Weaver. 2010. Embracing a health services research perspective on personal health records: Lessons learned from the VA My Healthevet system. Journal of General Internal Medicine 25(1 Suppl):62-67.
Office of the Assistant Secretary of Defense. 2010. Department of Defense ‘In Transition’ Program. Washington, DC: Department of Defense.
Orsingher, J. M., A. T. Lopez, and M. E. Rinehart. 2008. Battlemind training system: Armor for your mind. US Army Medical Department Journal Jul-Sep:66-71.
Panangala, S. V. 2007. Veterans Health Care Issues. Washington, DC: Congressional Research Service.
———. 2010. Veterans Medical Care: FY2011 Appropriations. Washington, DC: Congressional Research Service.
Panangala, S. V., and B. H. P. Mendez. 2010. Veterans Health Administration: Community Based Outpatient Clinics. Washington, DC: Congressional Research Service.
Pellerin, C., and T. C. Marshall. 2012. DOD, VA Announce Joint Health Record Milestone. http://www.defense.gov/news/newsarticle.aspx?id=116437 (accessed October 6, 2012).
Peterson, C., N. Park, and C. A. Castro. 2011. Assessment for the US Army Comprehensive Soldier Fitness program the Global Assessment Tool. American Psychologist 66(1):10-18.
Pietrzak, R. H., D. C. Johnson, M. B. Goldstein, J. C. Malley, and S. M. Southwick. 2009. Perceived stigma and barriers to mental-health care utilization among OEF-OIF veterans. Psychiatric Services 60(8):1118-1122.
Pizer, S. D., and J. C. Prentice. 2011. What are the consequences of waiting for health care in the veteran population? Journal of General Internal Medicine 26 (2 Suppl):676-682.
Prentice, J. C., and S. D. Pizer. 2007. Delayed access to health care and mortality. Health Services Research 42(2):644-662.
Prentice, J. C., B. G. Fincke, D. R. Miller, and S. D. Pizer. 2011. Outpatient wait time and diabetes care quality improvement. American Journal of Managed Care 17(2):e43-e54.
Rae Olmsted, K. L., J. M. Brown, J. Vandermaas-Peeler, S. J. Tueller, R. E. Johnson, and D. A. Gibbs. 2011. Mental-health and substance abuse treatment stigma among soldiers. Military Psychology 23(1):52-64.
Ralston, J. D., D. Carrell, R. Reid, M. Anderson, M. Moran, and J. Hereford. 2007. Patient web services integrated with a shared medical record: Patient use and satisfaction. Journal of the American Medical Informatics Association 14(6):798-806.
Razvodovsky, Y., and A. Stickley. 2009. Suicide in urban and rural regions of Belarus, 1990-2005. Public Health 123(1):27-31.
Reivich, K. J., M. E. P. Seligman, and S. McBride. 2011. Master resilience training in the US Army. American Psychologist 66(1):25-34.
Richardson, L. K., B. C. Frueh, A. L. Grubaugh, L. Egede, and J. D. Elhai. 2009. Current directions in videoconferencing tele-mental-health research. Clinical Psychology 16(3):323-338.
Rosenheck, R. 2000. Primary care satellite clinics and improved access to general and mental-health services. Health Services Research 35(4):777-790.
Rosenheck, R., and A. Fontana. 2002. Black and hispanic veterans in intensive VA treatment programs for posttraumatic stress disorder. Medical Care 40(1 Suppl):I52-I61.
Ross, S. E., L. A. Moore, M. A. Earnest, L. Wittevrongel, and C. T. Lin. 2004. Providing a web-based online medical record with electronic communication capabilities to patients with congestive heart failure: Randomized trial. Journal of Medical Internet Research 6(2):e12.
Ruskin, P. E., M. Silver-Aylaian, M. A. Kling, S. A. Reed, D. D. Bradham, J. R. Hebel, D. Barrett, F. Knowles 3rd, and P. Hauser. 2004. Treatment outcomes in depression: Comparison of remote treatment through telepsychiatry to in-person treatment. American Journal of Psychiatry. 161(8):1471-1476.
Saha, S., M. Freeman, J. Toure, K. M. Tippens, C. Weeks, and S. Ibrahim. 2007. Racial and Ethnic Disparities in the VA Healthcare System: A Systematic Review. Washington, DC: Department of Veterans Affairs.
Schlenger, W. E., R. A. Kulka, J. A. Fairbank, R. L. Hough, B. Kathleen Jordan, C. R. Marmar, and D. S. Weiss. 1992. The prevalence of post-traumatic stress disorder in the Vietnam generation: A multimethod, multisource assessment of psychiatric disorder. Journal of Traumatic Stress 5(3):333-363.
Schnipper, J. L., C. Hamann, C. D. Ndumele, C. L. Liang, M. G. Carty, A. S. Karson, I. Bhan, C. M. Coley, E. Poon, A. Turchin, S. A. Labonville, E. K. Diedrichsen, S. Lipsitz, C. A. Broverman, P. McCarthy, and T. K. Gandhi. 2009. Effect of an electronic medication reconciliation application and process redesign on potential adverse drug events: A cluster-randomized trial. Archives of Internal Medicine 169(8):771-780.
Seal, K. H., D. Bertenthal, C. R. Miner, S. Sen, and C. Marmar. 2007. Bringing the war back home: Mental-health disorders among 103,788 US veterans returning from Iraq and Afghanistan seen at Department of Veterans Affairs facilities. Archives of Internal Medicine 167(5):476-482.
Seal, K. H., S. Maguen, B. Cohen, K. S. Gima, T. J. Metzler, L. Ren, D. Bertenthal, and C. R. Marmar. 2010. VA mental-health services utilization in Iraq and Afghanistan veterans in the first year of receiving new mental-health diagnoses. Journal of Traumatic Stress 23(1):5-16.
Shekelle, P. G., F. Batuman, B. Bean-Mayberry, C. Goldzweig, C. Huang, I. M. Miake-Lye, D. L. Washington, E. M. Yano, and L. C. Zephyrin. 2011. Health Effects of Military Service on Women Veterans. Washington, DC: VA Evidence-based Synthesis Program, Department of Veterans Affairs.
Shore, J. H., and S. M. Manson. 2004a. The American Indian veteran and posttraumatic stress disorder: A telehealth assessment and formulation. Culture, Medicine and Psychiatry 28(2):231-243.
———. 2004b. Telepsychiatric care of American Indian veterans with post-traumatic stress disorder: Bridging gaps in geography, organizations, and culture. Telemedicine Journal and E-Health 10(1 Suppl):S64-S69.
———. 2005. A developmental model for rural telepsychiatry. Psychiatric Services 56(8):976-980.
Shore, J. H., D. Savin, H. Orton, J. Beals, and S. M. Manson. 2007. Diagnostic reliability of telepsychiatry in American Indian veterans. American Journal of Psychiatry 164(1):115-118.
Shore, J. H., E. Brooks, D. Savin, H. Orton, J. Grigsby, and S. M. Manson. 2008. Acceptability of telepsychiatry in American Indians. Telemedicine and eHealth 14(5):461-466.
Shore, J. H., E. Brooks, H. Anderson, B. Bair, N. Dailey, L. J. Kaufmann, and S. Manson. 2012. Characteristics of telemental-health service use by American Indian veterans. Psychiatric Services 63(2):179-181.
Singh, G. K., and M. Siahpush. 2002. Increasing rural-urban gradients in US suicide mortality, 1970-1997. American Journal of Public Health 92(7):1161-1167.
Spaulding, R. J., T. Russo, D. J. Cook, and G. C. Doolittle. 2005. Diffusion theory and telemedicine adoption by Kansas health care providers: Critical factors in telemedicine adoption for improved patient access. Journal of Telemedicine and Telecare 11(1 Suppl):107-109.
Spoont, M. R., J. Hodges, M. Murdoch, and S. Nugent. 2009. Race and ethnicity as factors in mental-health service use among veterans with PTSD. Journal of Traumatic Stress 22(6):648-653.
Stecker, T., J. C. Fortney, F. Hamilton, and I. Ajzen. 2007. An assessment of beliefs about mental-health care among veterans who served in Iraq. Psychiatric Services 58(10):1358-1361.
Street, A. E., J. Stafford, C. M. Mahan, and A. Hendricks. 2008. Sexual harassment and assault experienced by reservists during military service: Prevalence and health correlates. Journal of Rehabilitation Research and Development 45(3):409-419.
Street, A. E., D. Vogt, and L. Dutra. 2009. A new generation of women veterans: Stressors faced by women deployed to Iraq and Afghanistan. Clinical Psychology Review 29(8):685-694.
Stroupe, K. T., B. M. Smith, T. A. Lee, E. Tarlov, R. Durazo-Arvizu, Z. Huo, T. Barnett, L. Cao, M. Burk, F. Cunningham, D. M. Hynes, and K. B. Weiss. 2007. Effect of increased copayments on pharmacy use in the Department of Veterans Affairs. Medical Care 45(11):1090-1097.
Suris, A., and L. Lind. 2008. Military sexual trauma: A review of prevalence and associated health consequences in veterans. Trauma, Violence, and Abuse 9(4):250-269.
Suris, A., L. Lind, T. M. Kashner, P. D. Borman, and F. Petty. 2004. Sexual assault in women veterans: An examination of PTSD risk, health care utilization, and cost of care. Psychosomatic Medicine 66(5):749-756.
Tanielian, T., and L. H. Jaycox. 2008. Invisible Wounds of War: Psychological and Cognitive Injuries, Their Consequences, and Services to Assist Recovery. Santa Monica, CA: RAND Corporation.
TRICARE Management Activity. 2009. DEERS.
http://tricare.mil/mybenefit/home/overview/Eligibility/DEERS (accessed July 6, 2009).
Turvey, C. L., D. M. Zulman, K. M. Nazi, B. J. Wakefield, S. S. Woods, T. P. Hogan, F. M. Weaver, and K. McInnes. 2012. Transfer of information from personal health records: A survey of veterans using My Healthevet. Telemedicine Journal and E-Health 18(2):109-114.
VA (Department of Veterans Affairs). 2009. Stats at a Glance: VA Benefits and Health Care Utilization, April 2009. http://www1.va.gov/vetdata (accessed July 9, 2009).
———. 2011a. Guide to VA Mental-health Services for Veterans and Families. Washington, DC: VA.
———. 2011b. Strategic Plan Refresh: Fiscal Year (FY) 2011-2015. Washington, DC: Office of the Secretary.
———. 2012a. Copays. http://www.va.gov/healthbenefits/cost/copay_rates.asp (accessed August 14, 2012).
———. 2012b. Exempting in-home video telehealth from copayments: Direct final rule. Federal Register 77(44):13195-13198.
———. 2012c. VA to Expand Health Care Service by Opening 13 New Community-based Outpatient Clinics. http://www.va.gov/opa/pressrel/pressrelease.cfm?id=2358 (accessed September 25, 2012).
———. 2012d. VHS Office of Rural Health. http://www.ruralhealth.va.gov (accessed March 1, 2012).
VA and VHA (Veterans Health Administration). 2008. VHA Handbook 1160.01: Uniform Mental-health Services in VA Medical Centers and Clinics. Washington, DC: Department of Veterans Affairs.
VA Office of the Inspector General. 2012. Veterans Health Administration: Review of Veterans’ Access to Mental-health Care. Washington, DC VA Office of Inspector General.
VHA (Veterans Health Administration). 2011. A Query of VA Mental-health Professionals: Executive Summary and Preliminary Analysis. Washington, DC: Veterans Health Administration.
Visco, R. 2009. Postdeployment, self-reporting of mental-health problems, and barriers to care. Perspectives in Psychiatric Care 45(4):240-253.
Washington, D. L., N. D. Harada, V. M. Villa, J. Damron-Rodriguez, S. Dhanani, H. Shon, and T. Makinodan. 2002. Racial variations in Department of Veterans Affairs ambulatory care use and unmet health care needs. Military Medicine 167(3):235-241.
Washington, D. L., V. Villa, A. Brown, J. Damron-Rodriguez, and N. Harada. 2005. Racial/ethnic variations in veterans’ ambulatory care use. American Journal of Public Health 95(12):2231-2237.
Washington, D. L., E. M. Yano, B. Simon, and S. Sun. 2006. To use or not to use. What influences why women veterans choose VA health care. Journal of General Internal Medicine 21(3 Suppl):S11-S18.
Weeks, W. B., L. E. Kazis, Y. Shen, Z. Cong, X. S. Ren, D. Miller, A. Lee, and J. B. Perlin. 2004. Differences in health-related quality of life in rural and urban veterans. American Journal of Public Health 94(10):1762-1767.
West, A., and W. B. Weeks. 2006. Physical and mental-health and access to care among nonmetropolitan Veterans Health Administration patients younger than 65 years. Journal of Rural Health 22(1):9-16.
Williams, J. 3rd. 2008. Army Expands Battlemind Training. http://www.army.mil/article/9548/army-expands-battlemind-training (accessed September 30, 2012).
Wilson, J. A., K. Onorati, M. Mishkind, M. A. Reger, and G. A. Gahm. 2008. Soldier attitudes about technology-based approaches to mental-health care. Cyberpsychology and Behavior 11(6):767-769.
Wilson, N. J., and K. W. Kizer. 1997. The VA health care system: An unrecognized national safety net. Health Affairs 16(4):200-204.
Wong, E. C., G. N. Marshall, V. Shetty, A. Zhou, H. Belzberg, and D. D. Yamashita. 2007. Survivors of violence-related facial injury: Psychiatric needs and barriers to mental-health care. General Hospital Psychiatry 29(2):117-122.
Wright, K. M., O. A. Cabrera, P. D. Bliese, A. B. Adler, C. W. Hoge, and C. A. Castro. 2009. Stigma and barriers to care in soldiers postcombat. Psychological Services 6(2):108-116.
Yano, E. M., D. L. Washington, C. Goldzweig, C. Caffrey, and C. Turner. 2003. The organization and delivery of women's health care in Department of Veterans Affairs Medical Center. Womens Health Issues 13(2):55-61.
Zeber, J. E., K. L. Grazier, M. Valenstein, F. C. Blow, and P. M. Lantz. 2007. Effect of a medication copayment increase in veterans with schizophrenia. American Journal of Managed Care 13(6 Pt 2):335-346.
Zhou, Y. Y., T. Garrido, H. L. Chin, A. M. Wiesenthal, and L. L. Liang. 2007. Patient access to an electronic health record with secure messaging: Impact on primary care utilization. American Journal of Managed Care 13(7):418-424.












































