![]()
This chapter explores long-term outcomes associated with diagnoses of mild traumatic brain injury (TBI), posttraumatic stress disorder (PTSD), or other mental-health disorders, such as depression, substance-use disorders (SUDs), and suicidal ideation. The committee focused on those outcomes as TBI and mental-health disorders were highlighted in the legislation directing its task. Not everyone who receives a diagnosis of any of those conditions will necessarily experience the sequelae discussed. Many active-duty personnel and veterans will return home and not have any adverse effects, however, others will suffer the consequences of deployment. Many of those who receive diagnoses of the outcomes discussed in this chapter will need support from family members and friends, treatment, and programs to assist them.
The committee has defined long-term outcomes as those lasting more than 6 months from the time of diagnosis. The committee did not conduct an exhaustive evidence-based review of the literature (see Chapter 2). It reviewed studies that focused on mild TBI, PTSD, and other mental-health disorders and possible outcomes in Operation Enduring Freedom (OEF) and Operation Iraqi Freedom (OIF) active-duty and veterans. If studies of OEF and OIF personnel were not available, studies of other combat veterans and civilians were included. The committee did not attempt to describe every study in detail but rather highlighted studies and reviews that demonstrated an outcome associated with the conditions of interest. The committee notes that there are difficulties in untangling long-term outcomes from preexisting disease, from diseases that have similar symptoms, and from various comorbid conditions that might occur with the conditions of interest. In its review of the literature, the committee also has summarized and included in this chapter relevant sections of recent Institute of Medicine (IOM) reports: Gulf War and Health, Volume 6: Physiologic, Psychologic, and Psychosocial Effects of Deployment-Related Stress (IOM, 2008a), Gulf War and Health, Volume 7: Long-Term Consequences of Traumatic Brain Injury (IOM, 2009), and Returning Home from Iraq and Afghanistan: Preliminary Assessment of Readjustment Needs of Veterans, Service Members, and Their Families (IOM, 2010).
Since the committee’s Phase 1 report, a large volume of government-sponsored research, statistics, reports, and peer-reviewed studies have been published and a significant portfolio of research has been funded. Despite the focused efforts of DOD and VA to increase understanding of the risk and resiliency factors, military occupational exposures, health consequences, and readjustment challenges of those who had wartime service in Iraq and Afghanistan, the committee finds that the efforts to date do not provide definitive answers sought nor do they adequately address the major concerns faced by combat veterans. Although the last decade has
seen much advancement in the empirical documentation of combat exposures and postwar outcomes in military service members, there is still a need for further elucidation of key research questions and improvement in study design. For example, Tanielian and Jaycox (2008) reviewed 22 epidemiologic studies of returnees from deployment to OEF and OIF and found that only one included clinical diagnostic assessment for PTSD and other psychiatric disorders. The other 21 studies identified “cases” solely on the basis of brief, self-report screening scales or from medical record reviews. Although screening scales and medical records are useful for many purposes, Tanielian and Jaycox note that using either as the sole basis of estimating the prevalence of PTSD and other psychiatric disorders is fraught with hazard—a finding echoed by an earlier IOM report (2006).
Our understanding of the health consequences of service in Iraq and Afghanistan remains incomplete; even simple questions such as prevalence rates of physical and psychologic morbidity after military service in Iraq or Afghanistan continue to lack precision. For example, the literature reviewed by the committee reported PTSD prevalence rates that ranged from approximately 1% to 30% in different studies. Those wide-ranging prevalence estimates have added to the public’s confusion, have not been informative for health care planning, and fail to assist in projecting long-term readjustment needs. As noted previously by the committee, these differences might be explained by variations in study design factors including, population sampling strategy (e.g., random versus nonrandom samples; deployed population versus individuals seeking health care); use of different screening instruments or the same instrument with different cutoff values; self-reports versus medical record reviews versus clinician examinations; levels of combat exposure; length, number, and time elapsed after deployment; demographic and service-related characteristics including military component (Reserve/National Guard versus active); military training and occupation (combat versus combat support); and Service (Air Force, Army, Marines versus Navy). Accounting for, understanding, and reconciling those differences to provide the insights and answers needed for effective public policy, prevention, treatment and readjustment purposes has proved difficult.
ORGANIZATION OF THE CHAPTER
This chapter is organized into six main sections: mild TBI, PTSD, depression, substanceuse disorders, suicide and suicidal ideation, and women’s health outcomes. The TBI section begins with a definition of TBI and how its severity is measured; discusses what we have learned about TBI (of all levels of severity) from previous wars and in civilian populations (primarily summarized from Gulf War and Health, Volume 7: Long-Term Consequences of Traumatic Brain Injury [IOM, 2009]); includes a rationale for the committee’s focus on mild TBI; presents the methodologic difficulties in studying mild TBI in the OEF and OIF populations; and discusses outcomes and conditions that are often comorbid with mild TBI. It also includes a subsection that focuses on the complexity in separating the effects of TBI from those due to comorbid conditions such as PTSD, depression, and other mental-health disorders.
The remaining sections of the chapter include a discussion of PTSD, associated outcomes, and comorbidities, followed by discussions of depression, substance-use disorders, and suicidal ideation and associated outcomes, comorbidities, and risk or protective factors. The final major section focuses on women’s health outcomes in active-duty and veteran populations.
The issue of comorbidity is a recurring theme in this chapter and adds complexity to a study of outcomes. The committee found that in many cases it was difficult or impossible to separate sequelae from comorbid conditions and often could not make the distinction accurately. In fact, the construct of comorbidity does not do justice to the complexity that clinicians and service members encounter when attempting to understand symptoms. From the perspective of an individual patient, an event that is experienced is coupled with the biopsychosocial response to the event and might lead to a constellation of symptoms that express the particular circumstances. Our diagnostic systems cannot capture that level of complexity adequately, so we apply multiple diagnoses (such as depression, PTSD, and TBI) in our attempts to capture what is observed in the individual patient. From the perspective of the population, we divide people who experience symptoms and signs of various classes (such as cognitive, mood, and anxiety) into discrete categories for a host of purposes (such as case counting and assignment to standard protocols of diagnosis and treatment); but the categorization does not do justice to the reality of the distribution of symptoms among individuals in the population.
TRAUMATIC BRAIN INJURY
TBI is a common injury of the wars in Iraq and Afghanistan. The Department of Defense (DOD) and Veterans Brain Injury Center estimate that brain injuries account for 22% of all OEF and OIF combat casualties, whereas in Vietnam only 12% of combat casualties were attributed to brain injuries (Summerall, 2012). Several organizations, such as the American Congress of Rehabilitation Medicine and the Brain Injury Association of America, and government agencies, such as the National Institutes of Health and the Centers for Disease Control and Prevention (CDC), have developed definitions of TBI, but the committee will focus on the definition developed by DOD and the Department of Veterans Affairs (VA) as it focuses on service members and veterans.
The DOD–VA common definition of TBI is
A traumatically induced structural injury and/or physiological disruption of brain function as a result of an external force that is indicated by new onset or worsening of at least one of the following clinical signs, immediately following the event (DOD, 2009a), such as
• Any period of loss of or a decreased level of consciousness;
• Any loss of memory for events immediately before or after the injury;
• Any alteration in mental state at the time of the injury (confusion, disorientation, slowed thinking, etc.);
• Neurological deficits (weakness, loss of balance, change in vision, praxis, paresis/plegia, sensory loss, aphasia, etc.) that may or may not be transient;
• Intracranial lesion.
The DOD–VA guidance notes that external forces may include any of the following events: the head being struck by an object, the head striking an object, the brain undergoing an acceleration/deceleration movement without direct external trauma to the head, a foreign body penetrating the brain, forces generated from events such as a blast or explosion, or other force yet to be defined. Not all individuals exposed to an external force will sustain a TBI.
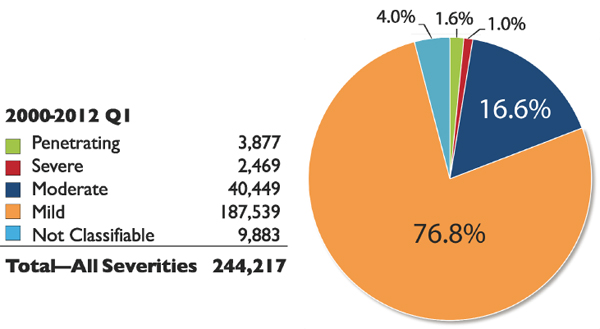
FIGURE 4.1 TBI by severity in all armed forces, 2000–2011, as of May 16, 2012.
SOURCE: DVBIC, 2012.
A TBI may be closed or penetrating. TBI is often classified according to severity: mild, moderate, or severe. A mild TBI is typically referred to as a concussion, and the two terms are often used interchangeably. In a review of TBI incidence by severity, the number of mild TBIs suffered by all the armed forces far exceeds the numbers of penetrating, severe, or moderate TBIs; in fact, mild TBI accounts for 76.8% of all brain injures (see Figure 4.1).
Severity
TBI, as noted above, is categorized as mild, moderate, or severe. TBIs can also be penetrating or closed head injuries. Severity is typically based on measures of loss of consciousness (LOC) and posttraumatic amnesia; alteration of consciousness and structural imaging are also used to determine acute severity (see Table 4.1).
TABLE 4.1 Criteria for Assessing Severity of TBI
| Measuring Severity | Mild | Moderate | Severe |
| Structural imaging | Normal | Normal or abnormal | Normal or abnormal |
| Loss of consciousness | Up to 30 minutes | 30 minutes–24 hours | Over 24 hours |
| Alteration of consciousness | Up to 24 hours | Over 24 hours | Over 24 hours |
| Posttraumatic amnesia | Up to 1 day | 1–7 days | Over 7 days |
| Glasgow Coma | 13–15 | 9–12 | 3–8 |
| Scale rating | |||
SOURCE: Adapted from VA and DOD, 2009.
| Type of Response and Score | Type of Response and Score | Type of Response and Score | |||
| Eye Opening: | Motor: | Verbal: | |||
| Spontaneous | 4 | Obeys commands | 6 | Alert and oriented | 5 |
| To speech | 3 | Localizes pain | 5 | Confused, yet coherent | 4 |
| To pain | 2 | Withdraws from pain | 5 | Inappropriate words | 3 |
| No eye-opening | 1 | Abnormal flexion | 4 | Incomprehensible sounds | 2 |
| Extensor response- | 3 | No sounds | 1 | ||
| No response | 2 | ||||
NOTE: Overall score is the sum of all scores.
SOURCE: Adapted from IOM, 2009; adapted from Teasdale and Jennett, 1974.
Although the above definitions, except the Glasgow Coma Scale (GCS), rely on length of impaired consciousness, depth of impaired consciousness as measured with the GCS is another method used to classify acute severity of the injury (see Table 4.2) (Teasdale and Jennett, 1974). The GCS is useful in diagnosing moderate and severe TBI, but most civilian and combat TBIs are in the mild range (GCS 13–15) with little differentiation in outcomes.
TRAUMATIC BRAIN INJURY OUTCOMES FROM PREVIOUS WARS AND THE CIVILIAN POPULATION
Traumatic Brain Injury and Cognition in Active-Duty Personnel and Veterans of Previous Wars and in Civilians
Over the last 30 years, much has been learned about the nature of impairments, disabilities, and participation problems that occur in the survivors of civilian closed TBI. Numerous neuropsychologic difficulties—such as problems with memory, attention, executive functions, and speed of information processing—are frequent consequences of TBI (Dikmen et al., 1990, 1995; Levin et al., 1990). Research has also determined that neuropsychologic outcome after TBI is significantly related to the severity of the brain injury (that is, whether it is penetrating or closed and whether it is mild, moderate, or severe). On the basis of review of available literature, a recent IOM report (2009) concluded that the presence, degree, and nature of cognitive impairments depend on the severity of the brain injury.
The results of research on the cognitive effects of penetrating brain injuries in military populations in previous wars clearly and consistently show a decline in cognitive functioning as a result of brain injury (Corkin et al., 1989; Grafman et al., 1986, 1988, 1990; Raymont et al., 2008; Salazar et al., 1986; Teuber and Weinstein, 1954; Weinstein and Teuber, 1957). Research also indicates that the decline is related to the volume of brain tissue lost (Grafman et al., 1988) and the affected region of the brain (Corkin et al., 1989). And there is evidence from long-term longitudinal studies that over many years intellectual ability continues to decline at a greater rate in veterans who have penetrating brain injuries than in veterans who do not (Corkin et al., 1989; Raymont et al., 2008).
Most studies of civilians who have mild TBI have found early neuropsychologic deficits that resolve by 1–3 months after injury in most cases (McCrea et al., 2009). Belanger et al.
(2005) performed a meta-analysis of 39 studies of 1,463 adults who had non-sports-related mild TBI and 1,191 control cases. They excluded sports-related injuries from their meta-analysis and included only those who sought medical attention for mild TBI. Their results indicate that the overall size of the effect of mild TBI on neuropsychologic functioning was moderate. However, the results varied by type of cognition affected, time since injury, patient characteristics, and sampling methods. Delayed memory and fluency were the types of cognition most affected by mild TBI when measured less than 3 months after injury. There were no neuropsychologic effects of mild TBI by 3 months after injury in unselected or representative, prospectively studied samples of subjects. However, clinic-based samples or groups involved in litigation showed greater cognitive sequelae of mild TBI at 3 months or more after injury. Moreover, litigation was associated with stable or worsening neuropsychologic performance. Belanger and Vanderploeg (2005) performed a separate meta-analysis of the neuropsychologic effects of sports-related concussion. They examined 21 studies that included 790 cases of sports-related concussion and 2,014 control cases. The results indicated that the overall effect size of concussion (d = 0.49) was similar to that found with mild TBI. Effect size was greater in studies that included subjects who had additional prior head injury than in studies that excluded subjects who had prior head injury. Neuropsychologic impairments were no longer found when testing occurred later than 7–10 days after injury. Such impairments are measured by psychometric testing and do not necessarily pertain to subjective neuropsychologic complaints.
On the basis of the literature, TBI clearly has an effect on cognitive functions with a clear dose–response relationship. However, the findings regarding mild TBI indicate that there is insufficient evidence that a single, mild civilian TBI has long-term effects on cognition (Dikmen et al., 2009; IOM, 2009). There may be differences between civilian and military exposures, including “blast” due to improvised explosive devises and other explosive munitions.
Traumatic Brain Injury and Postconcussive Symptoms in Active-Duty Personnel and Veterans of Previous Wars and in Civilians
IOM recently reviewed studies that evaluated the relationship between TBI and selfreported symptoms (2009). The results of studies of mild TBI (Gerber and Schraa, 1995; Heitger et al., 2007; Mickeviciene et al., 2002, 2004; Stulemeijer et al., 2006) varied, but the majority of evidence indicated that those who had mild TBI reported significantly more symptoms than those whose injuries did not involve the head. Dikmen et al. (2010) examined rates of new or worse symptoms 1 month and 1 year after civilian TBI in a large, representative series of cases and compared symptom reports with those of people whose injuries spared the head. The TBI group reported significantly more symptoms than the control group at 1 month and 1 year after injury. Symptom reports declined from 1 month to 1 year after injury, but 53% of the TBI group and 24% of the control group continued to report three or more symptoms at 1 year after injury. The most frequently reported symptoms at 1 year were problems with memory, concentration, fatigue, anxiety, and irritability. People who had severe TBI reported significantly more problems with memory, temper, and irritability and had three or more symptoms compared with controls at 1 year after injury. There were no significant differences between the most mildly injured TBI group and controls, possibly because the TBI group was small. However, those in the mild TBI group did endorse the majority of symptoms at least 50% more often than the controls at 1 year after injury. In fact, 44% of the mild TBI group reported three or more symptoms at 1 year after injury. Similar rates were reported in a very mild TBI sample 6 months
after injury (Bell et al., 2008) and in a nonhospitalized population-based sample of very mild TBI 3 months after injury (Lannsjo et al., 2009). The rates are much higher than the common belief that the occurrence of three or more symptoms for more than a month after a mild TBI is rare and occurs in less than 5% of the population (McCrea et al., 2009).
Traumatic Brain Injury and Depression in Active-Duty Personnel and Veterans of Previous Wars and in Civilians
The recent IOM review of this literature (2009) found strong evidence of an association between TBI and depression. Regardless of the severity of the TBI (mild, moderate, or severe), the rates of major depression 6 months or more after injury are higher than in control groups. The association could not be totally explained by depression before injury (Fann et al., 2004; Jorge et al., 2004; Vanderploeg et al., 2007). In addition, there is some evidence that prior mood disorder may predispose to TBI (Fann et al., 2002; Vassallo et al., 2007), and depression after TBI is more frequent in those who had depression before the injury than in those who did not (Bombardier et al., 2010; Fann et al., 2004). For instance, Bombardier et al. (2010) found that although about 70% of the cases with preinjury depression showed major depressive disorder by 1 year after injury, only 41% of the cases with no prior history did so.
The strong association between depression and TBI has also been reported in studies of World War II and Vietnam veterans. Holsinger et al. (2002) found that the odds of lifetime and current major depression were significantly higher in World War II veterans who had TBI than in controls. In addition, the odds of lifetime depression were highest in those who sustained severe TBI. The odds of depression also increased as the veterans aged. There is some evidence that depression is associated with mild TBI in veterans. A study of postdischarge Vietnam veterans found that those who reported mild TBI had a significantly higher frequency of depression than the control group (Vanderploeg et al., 2007).
Traumatic Brain Injury and Social Functioning in Active-Duty Personnel and Veterans of Previous Wars and in Civilians
A recent review by IOM (2009) concluded that TBI can have adverse effects on all aspects of social functioning, including employment, social relationships, independent living, functional status, and leisure activities. Research in civilians has shown that the severity of TBI decreases the probability of employment after injury and lengthens the time to return to work (Dikmen et al., 1993, 1994; Doctor et al., 2005; Oddy et al., 1978). There is evidence of an association between penetrating TBI and long-term unemployment in the military (Schwab et al., 1993), and return to work has been associated with computed-tomography findings in veterans who had penetrating head injury (Groswasser et al., 2002). For more comprehensive information about the effects of TBI on employment and other aspects of social functioning, see IOM (2009).
Traumatic Brain Injury in the Operation Enduring Freedom and Operation Iraqi Freedom Populations and the Committee’s Focus on Mild Traumatic Brain Injury
TBI is a common injury of the wars in Iraq (OIF) and Afghanistan (OEF). A recent report on US army soldiers deployed in 2001–2007 found that 0.14% (207 of 145,505) of those deployed to Afghanistan and 0.31% (2,241 of 722,474) of those deployed to Iraq had one or more TBI-related hospitalizations. Almost all those had moderate or severe brain injuries
(Wojcik et al., 2010). However, the estimated number of cases of mild TBI outweighs all the other types of brain injury. As noted early in this chapter, 76.8% of all brain injuries in OEF and OIF are considered mild TBI.
The committee decided to focus its attention on mild TBI because the vast majority of TBI in OEF and OIF is considered mild, it is difficult to identify and diagnose mild TBI, and long-term outcomes of mild TBI are much less understood than those of moderate and severe TBI (see IOM, 2009). In fact, many veterans returning from OEF and OIF have presented to the VA with symptoms of mild TBI, although they had not received the diagnosis while on active duty (Elder and Cristian, 2009). In an attempt at earlier diagnosis, DOD began screening all soldiers for mild TBI on their return from deployment by using the Post-Deployment Health Assessment (PDHA) and the Post-Deployment Health Reassessment (PDHRA).1 In addition, DOD began to assess soldiers with the Military Acute Concussion Evaluation while they were still on active duty, and VA began to screen all OEF and OIF veterans for mild TBI when they were seen by VA medical care providers.
The prevalence of mild TBI in the OEF- and OIF-deployed is based on a few large studies that have reported estimates of probable TBI of around 20%. For example, RAND conducted a telephone survey of 1,938 soldiers who had been deployed in OEF and OIF to determine probable TBI and other mental-health issues. Probable TBI was determined by the Brief Traumatic Brain Injury Screen, which was considered positive for probable TBI if a soldier reported being injured during deployment and experienced “being dazed, confused or seeing stars,” “not remembering the injury,” or “losing consciousness.” Results were weighted to improve the representativeness of the sample. The results of the study indicate that 19.5% had probable TBI (Tanielian and Jaycox, 2008).
Finally, all 3,973 members of a brigade combat team returning to Fort Carson from a 1-year deployment to Iraq were screened with the Warrior Administered Retrospective Casualty Assessment Tool (WARCAT). The WARCAT is a self-administered tool for ascertaining detailed information regarding injury; it enables soldiers to indicate whether they were injured through mechanisms commonly associated with TBI while deployed, whether any of their injuries resulted in an altered mental state, and whether symptoms often associated with mild TBI occurred after their injury. After completing the WARCAT, all soldiers were interviewed by a clinician, all available medical records were reviewed, and information was obtained from witnesses. The results indicate that 22.8% of the brigade had sustained a probable deploymentrelated mild TBI (Terrio et al., 2009).
A recent longitudinal study of a National Guard brigade combat team found much lower rates of mild TBI in theater than previous studies (Polusny et al., 2011). The authors administered an adapted version of the Defense and Veterans Brain Injury Center screening tool to determine probable mild TBI in a large group of soldiers still in Iraq who would be returning from deployment in about 1 month and then again 1 year after their return from deployment. Soldiers were determined to have a history of in-theater mild TBI if they endorsed an injury with altered mental status or loss of consciousness. The initial assessment, while the soldiers were still deployed, resulted in self-reporting of mild TBI in 9% of the cases. That percentage more than
__________________
1The PDHA is given immediately on return from deployment. The PDHRA, mandated by the assistant secretary of defense for health affairs, has been used since March 2005; it provides a second health assessment and is meant to be completed 90–180 days after return to home station from deployment.
doubled to 22% a year after return from deployment. It is not clear whether those results are due to recall bias, to soldiers’ minimizing their reports of mild TBI so that they might remain with their units, to soldiers’ wanting to ensure that health concerns did not delay their return home, to poor reliability of the questionnaire, or to other issues associated with attribution of current psychosocial difficulties to mild TBI.
Methodologic Problems in Studies of Mild Traumatic Brain Injury in Operation Enduring Freedom and Operation Iraqi Freedom Populations
Most epidemiologic studies have methodologic problems, but the outcomes being studied are often easier to identify or measure than those associated with mild TBI. The methodologic problems in the existing studies of mild TBI sustained during OEF and OIF conflicts add to the complexity of understanding the outcomes. The problems include the use of convenience samples of soldiers recently returned from deployment or convenience samples of soldiers receiving clinical care many months after sustaining mild TBI. The use of convenience samples makes it difficult to generalize study results to the entire military population engaged in OEF and OIF. Furthermore, many of the studies of mild TBI have involved small groups of subjects receiving clinical services typically in the VA health care system (Belanger et al., 2009; Campbell et al., 2009; Cooper et al., 2011). Many of the groups studied have substantially different demographic features, differ in the amount of time that has passed since the mild TBI, and often comprise people who had more complex outcomes; all those factors might affect the results of the studies.
In addition, many studies have low enrollment rates. For example, although Wilk et al. (2010b) studied outcomes in 3,952 soldiers after their return from Iraq, participants made up only 52% of the sample population surveyed. Similarly, the Hoge et al. (2008) study represented 59% of the sample, and Brenner et al. (2010b) approached 399 soldiers back from their second deployment to Iraq but had only a 12% enrollment rate. The effects of low enrollment rates are unknown, but one must seriously consider participation bias as having a potentially important effect on study results.
Many studies of mild TBI do not include a control group. A control group is essential to rule out the effect of other factors—such as physical, emotional, and preinjury characteristics—to determine whether an outcome is due to the TBI. Some studies have compared service members returning from OEF and OIF who have no injuries (control group) with those who selfreport a mild TBI and a subset of the mild-TBI group who also self-report postconcussion symptoms (Roebuck-Spencer et al., 2012) or with those who report injuries to the body but not to the head (Hoge et al., 2008). Those strategies attempt to compare people drawn from the same population (such as deployed service members), but it is unclear whether the groups are similar with respect to other relevant characteristics that might influence outcomes.
The determination of probable mild TBI in an active-duty soldier is by necessity through self-reporting with little or no acute-injury information from the field to accompany or substantiate the diagnosis. And a report of mild TBI is typically related to distant events that could have occurred at any time during deployment. Retrospective recall of events is likely to introduce bias. Another complicating factor is a determination of the number of possible TBIs and when they were sustained.
The questions used in screening subjects for mild TBI vary among researchers, and the psychometric properties of the measures are often unknown. Other methodologic problems include lack of information about baseline neuropsychologic functioning and other information about the individual, including demographic information and preexisting psychiatric or neurologic conditions or substance-use disorders; all these can complicate the effects of mild TBI on outcomes.
Traumatic Brain Injury Outcomes and Comorbidities in Operation Enduring Freedom and Operation Iraqi Freedom Populations
The presence of conditions that present as comorbid with mild TBI, such as PTSD or depression, makes it difficult to separate the outcomes related to mild TBI from the outcomes related to the comorbid conditions. This issue is the subject of current research. The subsections below discuss outcomes associated with mild TBI and outcomes of conditions that appear to be comorbid with mild TBI. The overall subject of comorbidities and the difficulties presented in diagnosis and treatment is discussed in detail in the section “Mild Traumatic Brain Injury, Comorbidities, and Complicated Issues of Causality in Operation Enduring Freedom and Operation Iraqi Freedom Populations.”
Mild Traumatic Brain Injury and Cognition in Operation Enduring Freedom and Operation Iraqi Freedom Populations
There has been a paucity of research on the cognitive effects of mild TBI sustained during the current conflicts and assessed with formal performance measures. Most studies suffer from the methodologic problems described above. There is some evidence that mild TBI has cognitive effects soon after injury. Luethcke et al. (2011) examined 82 active-duty military personnel and a few civilian contractors referred to an outpatient TBI clinic at a combat support hospital in Iraq within 72 hours of mild TBI; they were assessed on measures of cognitive performance with the Automated Neuropsychological Assessment Metrics (ANAM).2 Subjects were divided into those who had blast injuries and those who had nonblast injuries on the basis of clinical interviews. The authors examined the magnitude of change in ANAM from baseline (before deployment) to after injury in a subsample of 53 who completed the ANAM before deployment. The results indicated significantly worse reaction time from baseline to after injury. Differences were not found between those injured by blast and those injured who had nonblast injuries. Accuracy was also significantly related to duration of loss of consciousness rather than to type of injury.
Conflicting results with respect to the cognitive effects of mild TBI have been reported when cognition was evaluated months after mild TBI, that is, once the service members had returned from deployment. Brailey (2009) conducted a prospective and longitudinal study that examined the effects of mild TBI on postdeployment cognitive performance. The author examined 780 active-duty soldiers who had been deployed to Iraq before deployment (Time 1) and after deployment (Time 2) and collected data on cognitive measures by using a series of hierarchic regressions. The cognitive measures administered before and after deployment
__________________
2 The ANAM is a neurocognitive assessment tool designed to detect speed and accuracy of attention, memory, and thinking ability. It records a service member's performance through responses provided on a computer.
included several tests of neuropsychologic functioning, including the Trail Making Test, Wechsler Memory Scale Verbal Paired Associates and Visual Reproduction subtests (Wechsler, 2009), and the Neurobehavioral Evaluation System Continuous Performance Test (Letz, 1990) and measures from the ANAM (Reeves et al., 1992). The cognitive functions evaluated included attention, executive functioning, learning and memory, psychomotor problems, and self-reported health and cognitive problems. In the sample, 70 soldiers reported deployment-related TBI with LOC, and 87 soldiers screened positive for deployment-related PTSD. Predictors of postdeployment cognitive outcome were entered into the regression in steps starting with the relevant predeployment cognitive function; then demographics, mild TBI, and emotional status (such as PTSD or depression or deployment risk and resilience inventory); and finally interactions between mild TBI and emotional status. The results indicated that PTSD was a reliable predictor of postdeployment cognitive outcome. The pattern of results was similar when self-reported depression was substituted for PTSD. However, self-reported mild TBI was not a significant predictor of cognitive outcome.
Roebuck-Spencer et al. (2012) found cognitive decline in a sample of people who reported mild TBI as a result of their most recent deployment. The authors obtained deidentified data on 10,869 service members who were deployed to OIF and OEF and who had been evaluated with the ANAM version 4 TBI battery before and less than 1 week after return from deployment. The average test–retest interval was 398 days. The 1,609 service members who reported having sustained one or more TBIs in the 4 years before deployment were excluded. The remaining subjects were divided into four groups on the basis of their responses to the TBI questionnaire. Mild TBI was defined as an injury with alteration of consciousness. Those who reported no TBI or other important injury during their most recent deployment formed the control group of 8,002. A sample of 400 of the controls was randomly selected for use in the analysis. Those who reported one or more TBIs in their most recent deployment were divided into those reporting current symptoms (197) and those who had no current symptoms (305) at the postdeployment evaluation. A small fourth group (28) consisted of those who reported an injury but not TBI during their most recent deployment and who had current symptoms. Cognitive performance was evaluated by using a composite score that covered all the ANAM tests.
The results showed that there were no significant differences between the groups in predeployment ANAM performance. However, there were significant differences between the groups in postdeployment ANAM performance: the TBI group who had active symptoms performed significantly worse than controls (p < 0.0001) and worse than those who had TBI but no current symptoms (p < 0.0001). The control group and the TBI group who had no current symptoms were not significantly different in postdeployment ANAM performance. In addition, the control group showed significant predeployment–postdeployment improvement, the TBI group who had no current symptoms showed no predeployment–postdeployment change, and the TBI group who had current symptoms showed a significant predeployment–postdeployment decline in ANAM performance. Another analysis of the small group who were injured and had current symptoms but did not sustain TBI showed similar predeployment–postdeployment improvement in ANAM performance. In an analysis of reliable change using a 90% confidence interval (CI), 4.3% of the control group, 10.8% of the group who had TBI but no current symptoms, 10.7% of the non-TBI group, and 30.5% of the TBI group who had current symptoms had a clinically significant predeployment–postdeployment reduction in ANAM performance.
The authors note that 70% of those who reported TBI had no reduction in cognitive performance; this finding is consistent with the civilian literature. However, the authors did not have information on such comorbid conditions as PTSD, depression, or pain, so the results could not be taken into account as was possible in the study by Brailey (2009). Still, it is important to note that Brailey (2009) did not find a significant association between mild TBI and neuropsychologic performance even before adjusting for other factors, such as PTSD (Vasterling et al., 2012).3 The evidence in the best literature suggests cognitive decline within days of mild TBI, but the evidence is mixed with respect to longer-term outcomes and the factors (mild TBI vs PTSD) that might be responsible for the decline in cognition.
Mild Traumatic Brain Injury and Chronic Traumatic Encephalopathy in Operation Enduring Freedom and Operation Iraqi Freedom Populations
As study of the effects of a single mild TBI has been generating information about timelimited cognitive problems or inconsistent findings, the construct of chronic traumatic encephalopathy (CTE) has been drawing increased attention. CTE is a long-term consequence of repetitive mild trauma to the brain. It is marked by progressive decline of memory and cognition and is often accompanied by suicidal behavior, poor impulse control, parkinsonism, and, in advanced cases, dementia.
With current methods, the diagnosis of CTE can be confirmed only at autopsy on the basis of the pathologic appearance of neurodegeneration, inflammation, and staining for the protein tau found in insoluble deposits of two types—neurofibrillary tangles and neuritic threads (Saulle and Greenwald, 2012; Shively et al., 2012; Stern et al., 2011). Previously called dementia pugilistica, CTE was first diagnosed in the 1920s in boxers (Martland, 1928), but it is now recognized as possibly occurring in several contact sports in which repetitive mild head injuries occur, namely, soccer, field hockey, boxing, and football. More recently, the diagnosis has been extended to combat veterans.
CTE has been studied most intensively in boxers. Several studies revealed consistently poorer performance on neuropsychologic tests, according to a previous IOM report on TBI (IOM, 2009). Boxers were found to have deficits in memory, information processing and speed, finger-tapping speed, attention and concentration, sequencing, and other characteristics in a standard neuropsychologic test battery (Drew et al., 1986; Porter, 2003; Porter and Fricker, 1996). The largest pathology study involved 15 retired boxers. Their autopsies revealed cerebellar damage, cortical damage, substantia nigra degeneration, and neurofibrillary tangles in the cerebral cortex and temporal areas (Corsellis et al., 1973).
Those findings were extended to football players and other athletes in professional contact sports, such as soccer, wrestling, and field hockey. The first autopsy study appeared in 2005 and included findings in a professional football player 12 years after retirement. There was no cortical atrophy, but CTE was evident in sparse neurofibrillary tangles and neuritic threads in neocortical areas but not in the hippocampus or entorhinal cortex (Omalu et al., 2005). A year later, the same investigators reported on a second autopsy case of a football player (Omalu et al., 2006), and that was followed by larger case series that showed the hallmark pathologic evidence of CTE: neurofibrillary tangles and neuritic threads in the cerebral cortex, neurodegeneration,
__________________
3 Vasterling et al. (2012) used the same data as Brailey (2009).
and neuroinflammation (Omalu et al., 2010, 2011a). Pathologic findings were similar in two other case series of professional athletes (McKee et al., 2009, 2010).
The first postmortem case in blast-exposed veterans was reported in 2011 (Omalu et al., 2011b). The investigators reported degeneration characteristic of CTE: multifocal, neocortical, and subcortical neurofibrillary tangles and neuritic threads and mild fibrillary astrogliosis. The next published study was a controlled case series of four veterans who had a history of multiple blast or concussive injuries (Goldstein et al., 2012). The investigators had similar pathologic findings, including neurofibrillary and glial tangles in frontal, temporal, and parietal cortexes; tau immunoreactivity; myelinated axonopathy; and astrocytosis. The pathologic appearance in veterans was indistinguishable from that in four professional athletes who were studied as a comparator population. None of the features was seen in postmortem brains of age-matched normal subjects who had no history of blast or concussive injuries. The study also produced the first mouse model of blast injury, showing similar memory and cognitive deficits and CTE-like neurodegeneration, including tau immunoreactivity and astrocytosis, starting 2 weeks after a single blast exposure. Memory and cognitive deficits were prevented by head immobilization of the mice during blast exposure (Goldstein et al., 2012). The advent of this study and related studies indicates that this line of evidence is important for monitoring for repeated blast-exposed veterans and has generated increased interest in the neurobiologic basis of PTSD and TBI in combat veterans (Shively et al., 2012). No epidemiologic studies on OEF, OIF or OND active duty or veterans exist at present; the relevance of CTE to blast or concussive brain injuries remains to be studied.
Mild Traumatic Brain Injury and Postconcussive Symptoms in Operation Enduring Freedom and Operation Iraqi Freedom Populations
A variety of symptoms associated with mild TBI—including cognitive, somatic, and affective complaints—are collectively referred to as postconcussive symptoms (PCS). Research in service members who have returned from deployment to OEF and OIF has focused on whether mechanism of injury plays an important role in symptom reporting. There is some evidence that service members who report mild TBI with LOC from a blast have significantly higher rates of headaches and tinnitus after injury than those injured by a nonblast mechanism, although both groups report a variety of other posttraumatic symptoms. Wilk et al. (2010b) looked at self-reported concussion in US Army infantry soldiers 3–6 months after returning from a year-long deployment to Iraq. Of the 587 who met the criteria for concussion, 201 reported LOC and 373 reported an alteration of consciousness without LOC; 424 reported being in a blast, 150 did not experience a blast mechanism. Of those who experienced LOC, being in a blast was associated with headaches and tinnitus 3–6 months after deployment at a significantly higher rate than having been subject to a nonblast mechanism. However, in soldiers who had self-reported concussion and no LOC, blast was not associated more highly with physical or mental-health symptoms, absenteeism, or sick-call days than in those who reported a nonblast mechanism.
Studies that have examined other factors in relation to symptom reporting have concluded that symptom reporting is not specific to TBI alone and may be related to other co-occurring conditions or distressing experiences. For example, Hoge et al. (2008) used self-reported screening of 2,525 US Army infantry soldiers 3–4 months after their return from deployment to Iraq and found that 124 (4.9%) reported injuries with LOC, 260 (10.3%) reported injuries with altered mental state, and 435 (17.2%) reported other injuries during their deployment. Of those
who had LOC, 43.9% met the criteria for PTSD, 27.3% reported altered mental state, 16.2% reported other injuries, and 9.1% reported no injury. The researchers found that soldiers who had mild TBI and had experienced LOC were more likely to report poor general health, more sick days and doctor visits, and a higher number of symptom complaints, including PCS, than soldiers who had other injuries. However, after adjustment for PTSD and depression, mild TBI was not found to be associated with adverse outcomes, except headache. Wilk et al. (2012) reported that multiple mild TBIs with LOC increased the odds of headache compared with a single mild TBI (odds ratio [OR] = 4.0, CI = 2.4–6.8), although depression also increased the odds of headache (OR = 4.2, CI = 2.6–6.8).
Mental-Health Disorders Associated with Mild Traumatic Brain Injury
A recent review by IOM (2008a) concluded that service members deployed to a war zone have a greater prevalence of psychiatric disorders—especially PTSD, other anxiety disorders, and major depression—than veterans not deployed to a war zone. Another review notes that psychiatric disorders can contribute to disability in TBI and delay recovery (Silver et al., 2011). Rates of specific disorders in those who have TBI are presented below.
Depression and Mild Traumatic Brain Injury in Operation Enduring Freedom and Operation Iraqi Freedom Populations
Depression and symptoms of depression are often seen in those who have brain injury. In military populations, the prevalence of depression in OEF and OIF participants has been reported by RAND. Findings of a 2008 study indicate that 13.7% of OEF and OIF veterans who served through October 2007 had a diagnosis of depression (Tanielian and Jaycox, 2008). Of those who received a diagnosis of TBI, 31.8% suffered from major depression. A study by Hoge et al. (2008) evaluated major depression in US soldiers returning from OIF. Depression was associated with brain injury and LOC (22.9%) more than with other system injury. Of soldiers who had brain injury and altered mental state but no LOC, only 8.4% met the criteria for depression.
Substance-Use Disorders and Mild Traumatic Brain Injury
Whether survivors of mild TBI are at increased risk of substance-use disorders is unclear. Many studies have shown that drug and alcohol use often precede brain injury, but not many studies have examined whether sustaining a TBI, particularly a mild TBI, increases the likelihood of substance use in previous nonusing people. Studies based on civilian injuries that monitor substance use after head injury do not always indicate the severity of brain injury or include brain injury of all severity levels (e.g., Bombardier et al., 2003; Horner et al., 2005; Jorge et al., 2005). Most of the studies and reviews of the civilian population and one study of the military have indicated that there is an overall decline in substance use after TBI (Bombardier et al., 2003; Graham and Cardon, 2008; Heltemes et al., 2011), although a subset may continue heavy alcohol use (Bombardier et al., 2003). A 2009 IOM report on TBI concludes that there is limited but suggestive evidence of an association between TBI (of all severity levels) and decreased drug and alcohol use, relative to preinjury use, in the 1–3 years after the TBI. One civilian study of TBI found that the amount of drinking and reported problems with alcohol decreased, relative to the time before the injury, 1 month after injury but then increased at 1 year,
although not to preinjury levels (Dikmen et al., 1995). Those who had more severe TBI decreased alcohol use significantly more than those who had milder TBIs.
Suicidal Ideation and Mild Traumatic Brain Injury
Suicidal behavior is a serious consequence of mood disorders and may consist of suicidal ideation (thoughts), suicide attempts, or completed suicide. It is often associated with such psychologic conditions as depression or other mental disorders. In a Danish population-based study, Teasdale and Engberg (2001) compared the incidence of suicide in a group of patients who were admitted to a hospital from 1979 to 1993 with a concussion (n = 126,114), a cranial fracture (n = 7,560), or a cerebral contusion or traumatic intracranial hemorrhage (n = 11,766) with the incidence in the general population stratified by age and sex. The results demonstrated an increased incidence of suicide in the TBI groups compared with the general population (standardized mortality ratio = 3.0, 2.7, and 4.1, respectively). The diagnosis of substance misuse was associated with increased suicide rates in all three TBI groups. The authors concluded that concomitant risk factors (such as psychiatric illness and psychosocial disadvantage) might predispose to completed suicide in the mild-TBI group.
A recent study of active-duty soldiers was conducted by Skopp et al. (2012). The study was a retrospective case–control study, and the period of surveillance was 2001–2009. Those who died from suicide (n = 1,764) were compared with a control group (n = 7,018) matched by sex, race, age, service, date of entry into the active military component, and years of service. The two groups were similar regarding frequencies and types of TBI and number of deployments. Results of multivariate analyses demonstrated that there was an increased risk of suicide in those who had mood disorders, partner relationship problems, and family circumstance problems, but not in those who had mild TBI, alcohol dependence, or PTSD. In a separate analysis, an increased risk of suicide was found in those who had psychiatric comorbidities. The differences in results between the Skopp et al. study and that by Teasdale and Engberg (2001) were discussed as possibly reflecting differences between the populations and injury events. Civilian TBI tends to be associated with high-risk behaviors, and it is possible that preexisting personality characteristics increase the risk of suicide in civilians. In contrast, TBI in the military might often occur as the result of unpredictable incidents during training and combat.
Posttraumatic Stress Disorder and Mild Traumatic Brain Injury
An extensive literature review of brain injury and long-term outcomes (IOM, 2009) noted that there was limited or suggestive evidence of an association between mild TBI and PTSD in Gulf War military populations. The overlapping symptomatology between mild TBI, PCS, and PTSD complicates the issue. In 2009, VA published a systematic review of evidence on assessment of and treatment for TBI and PTSD. The findings show a wide range of prevalence of TBI and PTSD, depending on the population (military or civilian), the instruments used to diagnose TBI or PTSD (self-reports vs validated diagnostic instruments), and the size and representativeness of the population being studied. Another review of the literature on PTSD and TBI noted that studies varied considerably in their design and that there was not consistent evidence on the frequency of mild TBI and PTSD (Carlson et al., 2011b). There are important contextual distinctions between civilian and combat trauma that might influence the difference in prevalence of the comorbidity of PTSD and TBI.
Numerous studies have shown that OEF and OIF military veterans who had diagnoses of mild TBI had symptoms of PTSD (Carlson et al., 2010; Hill et al., 2009; Hoge et al., 2008; Kennedy et al., 2010; Schneiderman et al., 2008). For example, TBI and PTSD prevalence in OEF and OIF veterans has been reported in a RAND study of 1,965 OEF and OIF participants (Tanielian and Jaycox, 2008): 19.5% had probable TBI, and 13.8% had probable PTSD on the basis of the PTSD Checklist.4 However, in veterans who had TBI, the prevalence of PTSD was 33.8%. Hoge et al. (2008) examined soldiers 3–4 months after return from a year-long deployment in Iraq. The authors divided the soldiers into four groups: those who reported injury involving LOC, those who reported sustaining an injury with an altered mental state (for example, dazed, confused, “seeing stars,” or not remembering the injury) without LOC, those who had another type of injury that did not involve LOC or altered mental state, and those who reported no injury. The rates of PTSD were significantly and systematically different among the four groups: 44% in the group who reported injury with LOC, 27% in the group who reported injury with altered mental state, 16% in the group who had another type of injury, and 9% in the group who had no injury.
Mild Traumatic Brain Injury, Comorbidities, and Complicated Issues of Causality in Operation Enduring Freedom and Operation Iraqi Freedom Populations
Although estimates of PTSD, depression, PCS, and poor health are reported to be high in OEF and OIF active-duty personnel and veterans who have mild TBI, the relationships among those conditions are complicated and controversial. PTSD is often comorbid with several other mental-health disorders—such as depression, substance abuse, and suicidal behavior—and the conflicts in Iraq and Afghanistan have increased awareness of the relationship between mild TBI and PTSD, although it is confusing. Complicating the picture of PTSD that develops after a mild TBI is the issue of the overlapping symptomatology of mild TBI, PCS, and PTSD. In addition, it has been noted that PTSD can impede recovery from mild TBI and make clinical management difficult (Vasterling et al., 2009) and that the co-occurrence of TBI (of all severities) and PTSD increases the risk of self-reported cognitive impairment compared with that in civilians who do not have PTSD (Zatzick et al., 2010).
It is generally accepted that mild TBI, PTSD, and depression co-occur and that the rates of PTSD and depression are much higher after a mild TBI than are found in the general public or in non-TBI-injured soldiers. The controversy centers on whether symptoms and other adverse psychosocial outcomes reported by soldiers who have mild TBI and PTSD are due to the aftermath of the emotional trauma (possible PTSD) or to neurologic consequences of the mild TBI. Hoge et al. (2008) found that soldiers who reported injury with LOC were significantly more likely to report ill health, doctor visits, and missed workdays than soldiers who reported another type of injury that did not involve LOC or altered mental state. In addition, a significantly higher percentage of those reporting LOC also reported symptoms of irritability, sleep disturbance, fatigue, and other symptoms than the percentage of people who had a different type of injury. However, when the effects of PTSD and depression were covaried, all significant findings except headache disappeared. The authors concluded that the high rates of health
__________________
4 The PTSD Checklist (PCL) is a 17-item self-reporting measure of the 17 DSM-IV symptoms of PTSD. The PCL has a variety of purposes, including screening for and diagnosis of PTSD and monitoring of symptom change during and after treatment.
problems and symptoms reported by soldiers 3–4 months after return from deployment are associated largely with PTSD or depression rather than TBI.
Polusny et al. (2011) conducted a longitudinal study of National Guard soldiers deployed to Iraq. The soldiers completed a questionnaire evaluating probable mild TBI, PTSD, and depression about 1 month before return from a 16-month deployment to Iraq and again 1 year after return from deployment. The assessment at 1 year evaluated additional outcomes, including problematic drinking, social adjustment, and quality of life. The soldiers were divided into four groups on the basis of their mild TBI status as determined by their responses while they were still in Iraq and their PTSD status as determined by their responses after they returned from deployment. The groups consisted of those who had neither mild TBI nor PTSD (the control group), those who had mild TBI only, those who had PTSD only, and those who had both mild TBI and PTSD. The results showed that report of symptoms 1 year after return from Iraq was least frequent in the group who had neither mild TBI nor PTSD, more frequent in the group who had only mild TBI, and most frequent in the groups who had only PTSD or both mild TBI and PTSD. For example, irritability was reported by 64% of the group who had neither condition, 83% of the mild-TBI group, 99% of the PTSD group, and 100% of the group who had both mild TBI and PTSD. There were a number of significant differences in symptom reporting between the control group and the other groups, but after covarying the effects of PTSD symptoms in the mild-TBI-only group, the authors found no differences between the controls and the mild-TBI group in any outcome. Therefore, they concluded that mild TBI alone does not play a role in long-term impairments and suggested that their findings have policy implications for widespread screening for mild TBI in the military. They argued that the current screening policy may have unintended consequences of misattribution to mild TBI of symptoms that may be more properly attributable to PTSD, pain, sleep problems, or stress.
Other researchers have found different results in their investigation of TBI, PTSD, and PCS. Brenner et al. (2010a) examined separate groups of soldiers who had mild TBI alone, PTSD alone, and both conditions to look for relationships between those conditions and symptoms without trying to control for the effects of one of the conditions. Their focus was on whether having both PTSD and mild TBI resulted in a higher risk of symptoms than either condition alone. They performed a retrospective analysis of 1,247 injured members of a single Army brigade combat team who returned to Fort Carlson, Colorado, after a 1-year deployment to Iraq. The sample comprised the injured portion of the entire team previously reported on by Terrio et al. (2009). On return from Iraq, all members of the team were examined with the WARCAT, which included questions about injuries sustained in Iraq, symptoms experienced at the time of the incidents, and current symptoms. In addition to the questionnaire, each soldier was interviewed by a clinician, all available medical records were reviewed, and information from witnesses was gathered. Some 71% of the sample had at least one clinician-confirmed mild TBI, and the remainder reported an injury history not consistent with mild TBI. PTSD was diagnosed by using four questions from the PDHA, which assessed reexperiencing, numbing, avoidance, and hyperarousal dimensions of the disorder. Positive responses on any two of the four questions indicated PTSD. Symptoms experienced after return from Iraq included headaches, dizziness, memory difficulties, balance problems, and irritability. Symptoms were examined in four groups: mild TBI alone, PTSD alone, both mild TBI and PTSD, and neither condition. The analyses adjusted for age, education, sex, military rank, and military occupational specialty. The results showed that mild TBI alone (adjusted prevalence ratio = 4.03; CI = 2.67–6.07), PTSD alone (adjusted prevalence ratio = 2.74; CI = 1.58–4.74) and both conditions
together (adjusted prevalence ratio = 6.27; CI = 4.13–9.43) were significantly associated with having any symptom compared with absence of both mild TBI and PTSD. The combination of the two disorders was more strongly associated with a higher prevalence of each symptom than either condition alone. For example, the adjusted prevalence ratio for memory problems in those who had PTSD only was 4.00. The ratio increased to 6.22 in those who had mild TBI only and increased further to 12.70 in those who had both PTSD and mild TBI. The authors argued that their results support the additive effects of PTSD and mild TBI on symptoms and urged continued screening for both mild TBI and PTSD for early identification and treatment.
It is difficult to reconcile the contrasting results because of the many differences in study methods and design and in conceptualization of the problem. Statistical adjustment has been based on the assumptions that PTSD (or events that cause PTSD) confounds the relationship of mild TBI and that PTSD mimics the effects of mild TBI. In other words, PTSD is correlated with both mild TBI (independent variable) and outcomes (PCS and poor health) but has no causal relationship to mild TBI. That assumption might be questionable on the basis of findings that mild TBI might increase the likelihood of PTSD (Brenner et al., 2010a; Vasterling et al., 2009). If PTSD is indeed in the causal chain, statistical adjustments with covariance or other multivariate methods are inappropriate. What is not clear is whether the same event causes both and there is no causal link between them or whether they are causally related. The available evidence suggests that they are likely to be causally related.
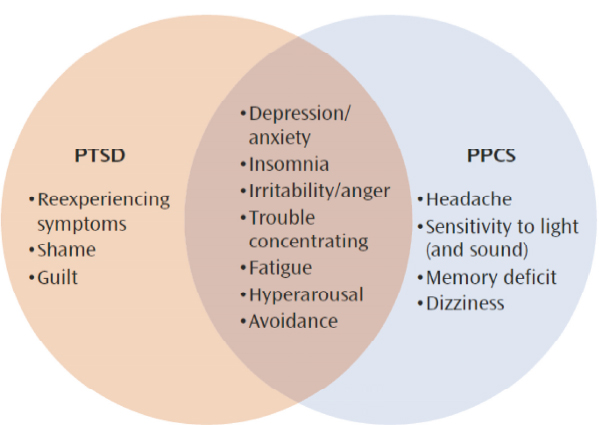
Several authors have tried to address the conceptual issues of comorbidities, the controversy, and the causes for the complexity of the problem (Kennedy et al., 2007; McAllister and Stein, 2010; Stein and McAllister, 2009; Vasterling and Dikmen, 2012). Mild TBI and PTSD are known or hypothesized to share a number of properties. They have common symptoms, hypothesized underlying biologic mechanisms, other comorbid conditions (such as depression and substance abuse), and premorbid risk and resilience factors. Given known and hypothesized common properties, it is difficult to reconcile whether psychologic or neurologic factors are responsible for the high morbidity observed in those who have both conditions. Overlapping symptoms, as seen in Figure 4.2, may include depression, anxiety, insomnia, irritability or anger, trouble in concentrating, fatigue, hyperarousal, avoidance, and others (Stein and McAllister, 2009).
Recent efforts are attempting to find the answer in biologic underpinnings although much of this approach is based on theory rather than empirical support. It is hypothesized that some areas of the brain—including the hippocampus, amygdala, and medial and prefrontal cortex—are typically damaged in TBI and implicated in the development of PTSD; this suggests a common origin of the overlapping symptom profile (Kennedy et al., 2007; Koenigs and Grafman, 2009; McAllister, 2011; McAllister and Stein, 2010; Stein and McAllister, 2009). PTSD and TBI may also have similar risk factors. For example, many studies have reported that lower IQ before trauma is associated with a higher risk of PTSD and other psychologic disorders (Breslau et al., 2006; Gale et al., 2008; Koenen et al., 2007; Kremen et al., 2007). If one considers IQ to be a proxy for cognitive reserve, lower cognitive reserve, either innate or acquired (for example, as a result of mild TBI), could increase the risk of psychologic health problems. Vasterling et al. (2009) suggest that mild TBI may interfere with the development of trauma memories because of cognitive impairment immediately after the TBI and thus influence the development of PTSD.
FIGURE 4.2 Interface of PTSD and persistent postconcussive symptoms following mTBI that involves biomechanical force to the brain with loss of consciousness, amnesia, and/or altered mental state. SOURCE: Stein and McAllister, 2009, reprinted with permission from the American Journal of Psychiatry.
Although the comorbidity of PTSD and TBI has become widely known in recent years as the result of OEF and OIF, the history of this issue dates back to World War I (Jones et al., 2007), and there has been no clear consensus. The same issues have long plagued the study of civilian mild TBI in attempts to explain the lack of recovery. In the current literature related to war injuries, some have concluded that there is sufficient evidence to attribute PCS to TBI. The suggestion is that the PCS might result from stress reactions after TBI rather than from the neurologic trauma itself (Bryant, 2011). Others have cautiously concluded that more research is needed—especially multidisciplinary research in psychiatry, neuropsychology, neurology, and other fields—to examine PTSD, TBI, and their interaction with the use of comprehensive definitions and language that spans different disciplines (Stein and McAllister, 2009).
Disentangling the outcomes related to mild TBI and PTSD is important for understanding the underlying reasons for the symptomatology so that prevention strategies and more precise treatment protocols might be developed.
Summary
Outcomes associated with TBI that occurred in previous wars and in the civilian population have been well described (IOM, 2008b, 2009), but outcomes associated with mild TBI that has occurred in the current conflicts (OEF and OIF) are not yet well understood. Although there is evidence to suggest cognitive impairment shortly after a mild TBI sustained during OEF and OIF, there is conflicting evidence on the longer-term cognitive outcomes and on the factors that might be associated with cognitive decline if it is observed. The study of chronic
traumatic encephalopathy related to repetitive blast exposure is an important new subject of research and has generated increased interest in the neurobiologic basis of TBI.
On the basis of available information on OIF and OEF injuries, it is generally accepted that mild TBI, PTSD, and depression co-occur and that rates of PTSD and depression after mild TBI are much higher than rates in the general public or in non-TBI-injured active duty personnel. The controversy centers on whether physical and emotional health-related symptoms and other adverse psychosocial outcomes reported by soldiers who have mild TBI and PTSD are due to the aftermath of the emotional trauma or to neurologic consequences of the mild TBI itself. Current scientific research has yielded insufficient evidence to answer that important diagnostic question. Better exposure data and objective diagnostic tests for or biomarkers of mild TBI and PTSD will improve our understanding of these highly comorbid conditions.
POSTTRAUMATIC STRESS DISORDER
PTSD is a psychiatric disorder that can develop after direct, personal experience or witnessing of an event that poses a perceived threat of death or serious injury. Symptoms that characterize PTSD arise in the aftermath of such an emotionally traumatic exposure and include reexperiencing the traumatic event through flashbacks and nightmares, avoidance of things associated with the trauma, and hyperarousal (exaggerated startle and difficulty in sleeping and in concentrating) (IOM, 2006). The Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV) recognizes that the onset of PTSD may be acute, beginning within 6 months of exposure to the traumatic event, or delayed, beginning more than 6 months after the event. Symptoms typically begin shortly after exposure—even on the same day (North et al., 1999). If the symptoms persist for 2 days to 4 weeks, the diagnosis is acute stress disorder; if the symptoms endure for more than 1 month, the diagnosis is PTSD. The time between exposure and development of enough symptoms to meet the diagnostic criteria (see Box 4.1) is variable and may be years (Bremner et al., 1996; Bryant and Harvey, 2002; Carty et al., 2006; Gray et al., 2004; Green et al., 1990; Op den Velde et al., 1996; Port et al., 2001; Ruzich et al., 2005). It is considered to be chronic PTSD by DSM-IV-Text Revision (DSM-IV-TR) criteria if symptoms persist for 3 months or longer. PTSD can be chronic and have no remission, or it can be recurrent and have periods of remission and recurrence (Friedman, 2003).
The DSM-IV criteria are undergoing revision currently with the upcoming publication of DSM-5. At the time of this report, the DSM-5 criteria for PTSD are not final. Draft criteria of DSM-5 vary from those of DSM-IV in that they are framed to increase the specificity of the diagnosis. Examples include the following: Criterion A (prior exposure to traumatic events) is more specifically stated, and evaluation of a person’s emotional response at the time is deleted; Criterion C focuses solely on avoidance of behaviors or of physical or temporal reminders of the traumatic experiences; and new Criterion D focuses on adverse alterations in cognition and mood associated with the traumatic events. Those changes should not adversely affect the case frequency of PTSD or the factors associated with the diagnosis substantially.
It should be noted that before the development of DSM-5 two interrelated issues have been raised (Rosen et al., 2008). First, some have suggested that, given the overlap of symptoms of PTSD with other diagnoses (such as major depression), mental-health workers have reflexively assumed that PTSD is the expected response to severe traumatic experiences (and some that are not so serious). Second, there are suggestions that the constellation of symptoms
that make up the diagnosis of PTSD may occur in the absence of trauma. Neither of those concerns appears to have gained a consensus in the overall scientific community, so in this report we state with confidence that the DSM-IV criteria for PTSD, on which the bulk of the reported studies are based, remain current and applicable.
The types of trauma exposure that are of high incidence in military personnel deployed to war zones are those known to be most likely to precipitate PTSD. Wojcik et al. (2009) evaluated data on soldiers deployed to OIF (2001–2004) and OEF (2002–2004) and found that PTSD explained 4.6 hospital admissions per 10,000 soldier-years and accounted for 35–45% of anxiety-disorder hospitalizations.
BOX 4.1
DSM-IV Criteria for Posttraumatic Stress Disorder (309.81)
A. The person has been exposed to a traumatic event in which both of the following have been present:
(1) the person experienced, witnessed, or was confronted with an event or events that involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others
(2) the person's response involved intense fear, helplessness, or horror. Note: In children, this may be expressed instead by disorganized or agitated behavior.
B. The traumatic event is persistently reexperienced in one (or more) of the following ways:
(1) recurrent and intrusive distressing recollections of the event, including images, thoughts, or perceptions. Note: In young children, repetitive play may occur in which themes or aspects of the trauma are expressed.
(2) recurrent distressing dreams of the event. Note: In children, there may be frightening dreams without recognizable content.
(3) acting or feeling as if the traumatic event were recurring (includes a sense of reliving the experience, illusions, hallucinations, and dissociative flashback episodes, including those that occur upon awakening or when intoxicated). Note: In young children, trauma-specific reenactment may occur.
(4) intense psychological distress at exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
(5) physiological reactivity on exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
C. Persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness (not present before the trauma), as indicated by three (or more) of the following:
(1) efforts to avoid thoughts, feelings, or conversations associated with the trauma
(2) efforts to avoid activities, places, or people that arouse recollections of the trauma
(3) inability to recall an important aspect of the trauma
(4) markedly diminished interest or participation in significant activities
(5) feeling of detachment or estrangement from others
(6) restricted range of affect (e.g., unable to have loving feelings)
(7) sense of a foreshortened future (e.g., does not expect to have a career, marriage, children, or a normal life span)
D. Persistent symptoms of increased arousal (not present before the trauma), as indicated by two (or more) of the following:
(1) difficulty falling or staying asleep
(2) irritability or outbursts of anger
(3) difficulty concentrating
(4) hypervigilance
(5) exaggerated startle response
E. Duration of the disturbance (symptoms in Criteria B, C, and D) is more than one month.
F. The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
SOURCE: Reprinted with permission from the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (Copyright 2000). American Psychiatric Association.
Prevalence
PTSD is one of the disorders most commonly diagnosed in US combat troops after their deployment to Afganistan and Iraq. A range of estimates have been reported for PTSD prevalence, and the estimates depend on when the evaluation is conducted and the diagnostic method (for example, self-reported symptoms vs diagnosis by a health care professional). The prevalence may also depend on whether the full criteria for PTSD are met as opposed to a positive screen for PTSD. A sample of studies is described below:
• Hoge et al. (2004a) reported the prevalence of PTSD 3–4 months after deployment as 6.2% and 12.9% in Army troops returning from Afghanistan and Iraq, respectively, and 12.2% in marines returning from Iraq. The prevalence of PTSD before deployment was 5.0% in all the military personnel screened with the PTSD Checklist (PCL), a self-reporting instrument.
• Hoge et al. (2007) later reported that 16.6% of US Army combat troops met the screening criteria (not DSM diagnosis) for PTSD a year after their return from Iraq.
• DOD conducted a mental-health survey of Army soldiers and marines deployed in Iraq in 2003, 2004, and 2006. In 2003, 16% of the soldiers and marines met the screening criteria for PTSD while deployed; in 2004, 14% met the criteria; and in 2006, 17% of soldiers and 14% of marines met the criteria (MHAT-III, 2006).
• Smith et al. (2008) conducted a prospective cohort analysis of 50,184 participants in the millennium cohort. PTSD was measured by self-reports using the PCL Civilian. New onset of self-reported PTSD was reported in 7.6-8.7% of deployers who reported combat exposures, 1.4–2.1% of deployers who did not report combat exposure, and 2.3–3% of nondeployers.
• Using the PCL, Booth-Kewley (2010) reported the prevalence of PTSD in OIF and OEF marines as 17.1%.
• Thomas et al. (2010) collected 18,305 mental-health surveys from members of four active components and two National Guard brigade combat teams at 3 and 12 months after deployment to Iraq; they analyzed 13,226 surveys. The prevalence of PTSD depended on how PTSD was defined (broad vs strict definition) and ranged from 14.7% to 21.5% at 3 months and from 16.6% to 30.5% at 12 months. Rates were significantly higher at 12 months in both groups; much larger increases were observed in National Guard participants.
• Thomas et al. (2010) also estimated prevalence on the basis of impairment and found that prevalence of PTSD with some functional impairment ranged from 12.6% (3 months) to
29.4% (12 months) and prevalence of PTSD with serious functional impairment ranged from 5.6% (3 months) to 12.4% (12 months).
A review of 22 studies (Tanielian and Jaycox, 2008) found that 5–15% experienced PTSD following deployment to war zones. The review also suggested that the prevalence of PTSD (and depression) increases with time after deployment (that is, in the readjustment period). A critical review by Richardson et al. (2010) yielded a similar result: estimated prevalence of combat-related PTSD of 4–17% in OIF veterans. The authors noted that PTSD prevalence in other Western countries is typically lower than in the United States, and they attributed that finding to differences in combat experience and in methods used to estimate prevalence and to sociopolitical and cultural factors. The difference in PTSD prevalence between the United States and other Western countries is supported by Fear et al. (2010), who estimated PTSD prevalence in UK armed forces who had been deployed to Iraq and Afghanistan at 4%.
Service members who experience combat exposure and are wounded appear to have higher prevalence of PTSD. Hoge et al. (2007) found that 31.8% of soldiers who had physical injuries had PTSD. In a more recent study of over 2,000 postdeployment active-duty service members, those who reported LOC had the highest rate of PTSD (43.9%) compared with those who had altered mental states (27.3%), those who had only physical injuries (16.2%), and those who reported no injury (9.1%) (Hoge et al., 2008). Gaylord et al. (2008) evaluated 76 service members who had sustained a burn and a blast injury for PTSD by using the PCL and excluded those who had moderate or severe TBI; the prevalence was 32%. However, Greiger et al. (2006) evaluated 613 soldiers who were seriously injured in combat in Iraq or Afghanistan for PTSD with the PCL 1, 4, and 7 months after their injury; 243 participated at all three times. At 1 month, 4.2% met the criteria for PTSD; at 4 and 7 months, about 12% met the criteria. The authors noted that 78.8% of people who received a diagnosis of PTSD or depression at 7 months were negative for the conditions at 1 month.
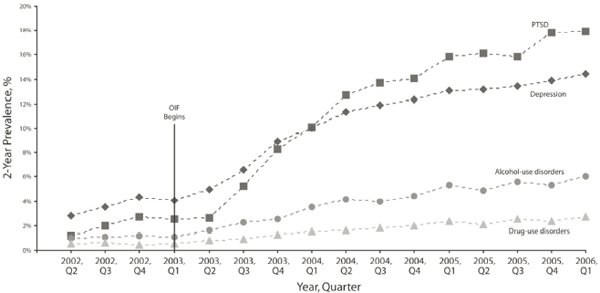
Seal et al. (2009) investigated new mental-health diagnoses in 289,328 OEF or OIF veterans who were new users of VA health care services from April 2002 to March 2008. Diagnoses were based on the International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) codes 290.0–319.0. Their investigation found that the 2-year cumulative prevalence increased from 6.4% in 2002 to 36.9% in 2008; PTSD diagnoses showed the greatest change, increasing from 0.2% to 21.8%. Figure 4.3 illustrates the increasing 2-year prevalence of PTSD and other mental-health disorders, particularly after the start of the Iraq War. It is consistent with the increasing trend noted by Seal et al. (2009) that Bagalman (2011) reported the PTSD prevalence in OEF and OIF veterans who used VA health care services in FY 2002–2010 as 27%.
FIGURE 4.3 Two-year prevalence of PTSD and other mental-health disorders among OEF and OIF veterans entering the Department of Veterans Affairs health care system.
SOURCE: From Seal et al., 2009, with permission.
The studies described above clearly indicate the variability in estimates of PTSD prevalence in the OEF and OIF military populations. Ramchand et al. (2010) reviewed 29 studies of OIF and OEF service members to characterize the variability in PTSD estimates and possible sources of the variability. They found that the studies could be divided into studies of military personnel who were seeking treatment and those who were not seeking treatment. Studies of non-treatment-seeking service members generally provided PTSD prevalence estimates of about 5–20%, and studies of treatment-seeking service members yielded estimates as high as 50% on the basis of screening, although rates were typically lower when actual diagnoses were made. Recent research indicates that 23% of those seeking treatment receive a PTSD diagnosis. The authors found that the variability in PTSD estimates was probably related to representativeness and case definitions. Most studies used convenience samples, which may not be representative of the entire population deployed to war zones, and the studies used different definitions of PTSD. Methodologic differences in outcome measurements in the studies may lead to substantial underestimation of the prevalence of PTSD (and depression) in the postdeployment samples (Tanielian and Jaycox, 2008). Those methodologic issues are similar to the issues discussed above in determining estimates of mild TBI. Regardless, using different definitions most likely contributes to much of the variability observed in the various studies and indicates the need to use a consistent set of criteria for PTSD and a standardized assessment for optimal estimation of prevalence.
Risk Factors
Demographic Factors
Many factors have been associated with an increased likelihood of PTSD, although the literature contains some conflicting findings. Age, sex, race or ethnicity, rank, marital status, and educational level have been associated with PTSD. Specifically, studies have shown that a young age (less than 25 years) is associated with increased odds of PTSD in OEF and OIF veterans (Seal et al., 2009), although National Guard and reserve veterans older than 30 years old had
significantly higher risks of PTSD than younger National Guard and reserve veterans. Wojcik et al. (2009) found that female soldiers had 3.3 times the risk of hospitalization for PTSD of male soldiers. Black soldiers had half the risk of PTSD hospitalization of white soldiers, and enlisted personnel had 6 times higher risk of PTSD than officers. Lapierre et al. (2007) and Phillips et al. (2010) also found that junior rank was associated with PTSD, but the absence of an association between sex and PTSD is consistent with results of other research (see discussion below in the section “Women’s Health Outcomes”).
Studies also have shown that being single or divorced is associated with increased risk of PTSD (Booth-Kewley et al., 2010; Lapierre et al., 2007). Higher educational status has been reported to be protective against PTSD (Booth-Kewley et al., 2010; Dedert et al., 2009), but some have found increased PTSD risks with higher educational level (Reger et al., 2009). In a small study of health care workers, Kolkow et al. (2007) found that the only demographic factor related to increased risk of PTSD was nonwhite race. Although Grieger et al. (2006) found some associations of demographic factors with PTSD at 1 month, they did not find any associations with demographic factors at later evaluation times.
Deployment-Related Stressors
Deployment and deployment-related stressors have been associated with increased risk of PTSD. Booth-Kewley et al. (2010) used the PCL to evaluate 1,569 marines deployed to Iraq or Afghanistan; multivariate analyses indicated that deployment-related stresses—such as concerns back home, lack of privacy, and problems with leadership—were significantly associated with PTSD. Vasterling et al. (2010) used the PCL to evaluate changes in PTSD symptom severity in 774 deployed and 309 nondeployed soldiers. Multiple regression analyses indicated that PTSD symptoms increased with deployment; the greatest positive increase was observed in those who had high combat exposure. Results could not be explained on the basis of preexisting symptoms.
Some investigations have indicated that National Guard soldiers suffer disproportionately from deployment (Milliken et al., 2007; Thomas et al., 2010). Riviere et al. (2011) reviewed selfreport data to determine risk factors for PTSD and depression in 4,034 National Guard soldiers who had been deployed to Iraq. Soldiers were evaluated at 3 or 12 months, and the factors evaluated were specific to National Guard soldiers who leave and then return to civilian employment. They included “financial hardship, job loss, [lack of] employer support, and the effect of deployment absence on co-workers.” The investigators found that PTSD was associated with all factors at one or both evaluation times. Depression was associated with financial hardship, job loss, and lack of employer support at 3 and 12 months. The authors noted that their results indicated that “National Guard soldiers have unique post-deployment social and material concerns that impair their mental health.”
Combat Exposure
As expected, combat exposure and PTSD are linked. Seal et al. (2009) reported higher combat exposure associated with increased PTSD risk in OEF and OIF veterans but not in National Guard or reserve veterans. Booth-Kewley et al. (2010) also reported a strong association between combat exposure and PTSD in marines deployed to Iraq and Afghanistan. MacGregor et al. (2009) compared mental-health diagnoses in 831 men serving in OIF who had sustained a battle injury with those in 1,137 who had sustained a nonbattle injury; men were evaluated at least 1 month after injury. Men who suffered battle injuries had significantly higher
rates of PTSD and other mental-health conditions than men who suffered nonbattle injuries, and mental-health diagnoses were significantly associated with severity of injury. Grieger et al. (2006), however, did not find combat exposure (or long deployments) to be predictive of PTSD at later evaluation points in the severely injured soldiers.
In a small study of 317 Gulf War veterans with the PCL, Maguen et al. (2011c) found that killing someone was a significant predictor of PTSD symptoms (and other mental-health outcomes) after control for other combat-related factors. In their review of 29 studies of OIF and OEF military personnel, Ramchand et al. (2010) found that the only factor that was consistently significantly associated with PTSD was combat exposure and that other factors that often appear to be associated with PTSD may simply be surrogates of combat exposure. For example, those who are younger and of lower rank may be exposed to more combat than those who are older and of higher rank. Assuming that combat exposure is an important risk factor for PTSD, Pietrzak et al. (2011b) evaluated survey data on 285 OIF and OEF National Guard or reserve veterans to identify specific combat experiences as predictors of PTSD. After adjustment for various factors, they found that two combat experiences—“personally witnessing someone from one’s unit or an ally unit being seriously wounded or killed” and experiencing “friendly” fire—were associated with PTSD symptom severity and were independent predictors of probable PTSD. Exposure to land mines or traps was also associated with PTSD symptom severity.
Another risk factor related to combat exposure is the threat of personal harm. Kolkow et al. (2007) used the PCL to survey 102 health care providers who had been deployed to a combat setting in Iraq or Afghanistan and found that PTSD was increased in those who experienced “direct and perceived threats of personal harm.” They did not observe an association between PTSD and exposure to the dead or wounded. Peterson et al. (2010) compared mental-health outcomes in 4,408 active-duty Air Force noncombatants returning from deployment to a combat zone in Iraq with those in 959 personnel returning from a noncombat zone in Qatar. They used the PDHA to evaluate PTSD and found that those deployed to Iraq were significantly more likely to report combat experiences, such as “feeling in great danger of being killed,” and to screen positive for PTSD. Phillips et al. (2010) evaluated self-report data on 706 male marines who had been deployed at least 30 days to Iraq or Afghanistan between baseline and followup assessments. They conducted multivariate logistic regression analyses and found that the most significant predictor of screening positive for PTSD was “feeling in great danger of death.” Other significant predictors were being shot or seriously injured and witnessing an injury or death.
Prior Traumatic Exposure
Veterans who have experienced prior traumatic stress appear to be more likely to develop PTSD than those who do not have such a history. In addition to the combat-related risk factors noted above, Phillips et al. (2010) found that two or more exposures to violence before entering the military also increased the likelihood of screening positive for PTSD. Dedert et al. (2009) evaluated 356 military veterans who served after September 11, 2001, using the Structured Clinical Interview for DSM-IV, and investigated the contribution of lifetime traumatic events5 to PTSD. Multiple traumatic events, including childhood assault and disasters or accidents, increased the likelihood of PTSD in veterans who had comorbid psychiatric conditions. The only
__________________
5 The author defined a traumatic stressor as a “life threatening event to which the person responded with fear, helplessness or horror.”
predictors of PTSD in veterans who did not have comorbid psychiatric conditions were combat exposure and adult physical assault.
Fritch et al. (2010) also found an association between childhood physical abuse and PTSD symptoms. They reviewed self-report data on 1,045 OIF and OEF National Guard or reserve veterans who had been referred to a behavioral-health clinic. Multiple regression analyses revealed a significant association between postdeployment psychiatric symptoms—those of PTSD, anxiety, and depression—and childhood physical abuse. An association between psychiatric symptoms and combat-related trauma was also noted. No interactive effects between child abuse and combat were observed.
Cabrera et al. (2007) investigated the relationship between adverse childhood experiences6 and rates and symptoms of mental-health disorders. They compared self-report data on 2,392 male active-duty soldiers who had recently returned from Iraq (surveyed 3 months after deployment) with data on 4,529 male active-duty soldiers who had not served in Iraq; about 43% of the latter had served in Afghanistan, but their rates of PTSD and depression were similar to those in soldiers who had not been previously deployed. The investigators found that soldiers who reported at least two categories of childhood adversity were significantly more likely to screen positive for PTSD and depression. More important, the authors stated that adverse childhood experiences “independently predicted higher depression and post-traumatic stress symptoms, beyond the expected contribution of combat exposure.” Similarly, Gahm et al. (2007) evaluated self-report data on 1,626 active-duty soldiers at an outpatient mental-health clinic and found that adverse childhood experiences were stronger predictors of PTSD and depression than were demographic characteristics. Combat experience was also associated with PTSD, but depression was not.
Military Sexual Trauma
Estimates of military sexual trauma (MST) have been reported on the basis of a universal screening program implemented by VA. In 2003, shortly after implementation of the VA program, it was reported that 21.5% of women and 1.1% of men reported MST (Kimerling et al., 2007). It has been noted that those estimates have remained fairly consistent; as of 2008, they translate to 48,106 women and 43,693 men screening positive for MST (Hyun et al., 2009). DOD estimates of MST indicate that the annual prevalence of sexual assault in women and men was 6.8% and 1.8% (Lipari et al., 2008). A study of reservists (Street et al., 2008) examined sexual harassment and assault during military service and found that sexual assault was reported by 13.1% of women and 1.6% of men.
MST appears to be an important risk factor for PTSD. Suris and Lind (2008) reviewed research on health consequences of MST and found higher rates of PTSD, depression, and substance abuse in female veterans who had a history of sexual assault. In fact, female veterans who had a history of MST were nine times more likely to develop PTSD compared to female veterans who had no history of sexual trauma. Recent research on OIF and OEF veterans supports that finding. Kimerling et al. (2010) reviewed medical records of OIF and OEF veterans (17,580 women and 108,149 men) for diagnoses of mental-health disorders and found that those who had a history of MST were significantly more likely to receive a diagnosis of PTSD, other
__________________
6 The authors defined adverse childhood experiences by using six categories: exposure to a mentally ill, alcoholic, or violent person in the home or exposure to physical, sexual, or psychologic abuse.
anxiety disorders, depression, or substance-use disorders than those who did not have a history of abuse. Odds ratios remained significant after adjustment for other significant associations, and effect sizes in women were substantially greater than those in men. The link between MST and PTSD is discussed further below in the section “Women’s Health Outcomes.”
History of Mental-Health Condition
Military personnel who have been previously diagnosed with a mental-health condition, particularly PTSD, are at greater risk for a repeat diagnosis in theater (Larson et al., 2011). Using self-report data, Sandweiss et al. (2011) assessed the relationship between postdeployment PTSD and predeployment (baseline) psychiatric conditions and injury severity among 22,630 military personnel who had been deployed to Iraq or Afghanistan. PTSD was significantly associated with baseline psychiatric conditions; service members who had one or more baseline psychiatric conditions were 2.52 times more likely to report PTSD symptoms than those who had no baseline psychiatric conditions.
Injury Severity and Neurologic Dysfunction
Although injury severity was significantly associated with PTSD symptoms, the observed association was weak. Grieger et al. (2006), however, evaluated seriously injured soldiers and found that severe physical problems were significantly associated with PTSD at all times of evaluation. As noted above, MacGregor et al. (2009) also observed a positive association between injury severity and PTSD and other mental-health diagnoses.
Subtle neurologic dysfunction may predispose people to PTSD. Gurvits et al. (2006) evaluated 25 male Vietnam veterans who had received a diagnosis of PTSD and 24 who had no PTSD diagnosis and compared them with each other and with their combat-unexposed identical twins. Combat veterans who had a diagnosis of PTSD had significantly higher scores on subtle neurologic dysfunction (neurologic soft signs) than combat veterans who did not have PTSD. However, the combat-unexposed twins of the combat veterans who had PTSD also had increased scores. The results suggest that the dysfunction is not a result of PTSD but rather might indicate a vulnerability to PTSD.
An earlier study by Gilbertson et al. (2002), using a case-control design, examined male monozygotic twin pairs in which one twin was a combat Vietnam veteran and the identical twin had no combat exposure. Hippocampal volume was measured in both twins. Because monozygotic twins are genetically identical, the authors interpreted differences in hippocampal volume to be due to environmental effects. The authors concluded that smaller hippocampal volume was found to constitute a risk factor for the development of PTSD.
Protective Factors
Some research has been conducted on factors that might protect soldiers from PTSD and other mental-health disorders. IOM (2008a) reviewed studies of veterans of such past conflicts as World War II, the Gulf War, and the Vietnam War and noted that psychologic resilience—often characterized by hardiness, personal control, and positive coping strategies—is inversely related to the risk of PTSD after traumatic or stressful events. Studies have indicated that strong social support is protective against the onset of PTSD. A recent study of OIF and OEF veterans
supports the past research on protective factors. Pietrzak et al. (2009b, 2009c) reviewed selfreport data on 272 OIF and OEF veterans; PTSD was assessed with the PCL. They found that the PTSD group had significantly lower total and individual resilience scores than those who did not have PTSD.7 The only exception was the individual score that measured spiritual influences. They also found that unit support and postdeployment support were inversely related to PTSD and depressive symptoms.
In results that were consistent with findings from Pietrzak and colleagues, Skopp et al. (2011) found that soldiers who had positive appraisals of military service were less likely to screen positive for PTSD after deployment, and Phillips et al. (2010) found that marines who had five or more close confidants were less likely to screen positive for PTSD. MacGregor et al. (2012) investigated the effect of dwell time on new diagnoses of PTSD and other mental-health disorders in male marines deployed to Iraq once (49,328) or twice (16,376).8 They reviewed military and medical records, conducted logistic regression analyses, and found that longer dwell times were associated with significantly lower odds of new diagnoses of PTSD and other mental-health disorders.
COMORBID CONDITIONS
PTSD is often comorbid with other psychiatric conditions and substance-use disorders. The 2008 IOM report Gulf War and Health, Volume 6: Physiologic, Psychologic, and Psychosocial Effects of Deployment-Related Stress noted that the temporal relationship between PTSD and these other conditions is complex. PTSD increases the likelihood of other psychiatric disorders, and the other disorders increase the likelihood of PTSD. The subsections that follow discuss PTSD and the comorbid conditions in veteran populations. The complex and most important association between PTSD and TBI is described above.
Depression and Other Psychiatric Disorders
IOM (2008a) reviewed the research on psychiatric disorders in veteran populations and concluded that PTSD is highly comorbid with other psychiatric conditions, especially generalized anxiety disorder (GAD) and major depressive disorder. For example, Kulka et al. (1990) found that 75% of male veterans who had PTSD had a lifetime diagnosis of alcohol abuse or dependence, 44% had GAD, and more than 20% had another psychiatric disorder.
Magruder et al. (2005) conducted clinical interviews via telephone with 746 randomly selected patients who had visited a VA hospital in FY 1999. They found that those who had a diagnosis of PTSD were significantly more likely to have a comorbid mental-health disorder than those who did not have PTSD (87% vs 21%). The most common comorbid psychiatric condition was major depression, which was followed by other anxiety disorders—such as GAD, panic disorder, and agoraphobia—and then substance-use disorders.
Recent studies have confirmed the common occurrence of psychiatric comorbidities in OIF and OEF veteran populations. As discussed above, Seal et al. (2009) investigated mental-health diagnoses in OIF and OEF veterans. They found that 29% of the 106,726 veterans who
__________________
7 Individual scores included measures of personal competence, tolerance of negative affect and stress-related growth, acceptance of changes, and personal control.
8The authors defined dwell time as time at home between deployments.
had mental-health diagnoses had two diagnoses and 33% had three or more. PTSD was the most common mental-health diagnosis (see Figure 4.3, from Seal et al., 2009).
The individual effects of the comorbid psychiatric conditions on mental or physical functioning or quality of life have also been examined. Rauch et al. (2010) evaluated the effects of depression and anxiety on health satisfaction in 249 combat veterans who had and did not have PTSD. PTSD was diagnosed by using clinical interviews. Average scores on self-report questionnaires indicated that the veterans had moderately high levels of anxiety, moderately severe levels of depression, and low levels of health satisfaction. Anxiety and depression were shown to have adverse effects on health satisfaction. However, when the study authors controlled for PTSD severity, combat exposure, and age and examined the conditions simultaneously in the model, only depression had a significant adverse effect on health satisfaction.
Similarly, Pittman et al. (2012) used a self-report questionnaire (SF-36) to evaluate the individual effects of PTSD and depression on mental and physical health-related quality of life in 220 OIF and OEF combat veterans. PTSD was diagnosed in 46% by using structured clinical interviews; all the veterans showed some level of depression, from minimal to severe. The investigators controlled for overlapping symptoms (anhedonia, difficulty concentrating, and insomnia) and found that PTSD and depression both had adverse effects on mental and physical health outcomes. However, the two conditions were significant independent predictors only of mental-health–related quality of life, not physical-health–related quality of life. Depression was the more significant contributor with respect to mental-health–related quality of life.
Substance-Use Disorders
IOM (2008a) noted that it is now well accepted that alcohol and drug use are often comorbid with PTSD in veteran populations. Several studies have shown that veterans who have PTSD are at increased risk for alcohol or drug abuse or dependence (O’Toole et al., 1998; Ouimette et al., 1996; Shipherd et al., 2005; Yarvis et al., 2005).
Recent studies support the correlation between PTSD and substance-use disorders. Jakupcak et al. (2010a) investigated the relationship of psychiatric disorders and alcohol misuse in 287 OIF and OEF veterans who had PTSD (37.3%), depression (37.3%), or alcohol misuse (28%). PTSD was identified by using the PCL; 76.6% of veterans who had PTSD screened positive for depression. Several significant independent predictors of alcohol misuse were identified, including PTSD and depression. Veterans who had PTSD or depression were twice as likely to abuse alcohol as those who had neither disorder. Investigation of the PTSD symptom clusters revealed that emotional numbing correlated most significantly with alcohol misuse. The authors suggested that the co-occurrence of these disorders indicates that veterans misuse alcohol to blunt the symptoms of PTSD or depression.
Stecker et al. (2010) reviewed VA data on 293,861 OIF and OEF veterans to determine common medical and psychiatric diagnoses. They found that alcohol misuse, sleep problems, and pain were common co-occurring conditions with PTSD or depression. They noted that pain was diagnosed in about 50% of the sample population. Similarly, Thomas et al. (2010) found that alcohol misuse or aggression was a common comorbidity with PTSD or depression in soldiers who had been deployed to Iraq; they concluded that “the significant overlap between alcohol misuse, aggressive behavior, and mental disorders highlights the high rate of comorbidity in this population.”
Health Outcomes Associated with Posttraumatic Stress Disorder
A variety of health outcomes have been associated with PTSD. The following sections briefly review several health outcomes that have been reported in studies of OIF and OEF veterans who have PTSD.
Cardiovascular Effects and Risk factors
IOM (2008a) reviewed the relationship between PTSD and cardiovascular effects. As stated in that report, there is strong evidence that resting heart rate is slightly increased in veterans who have PTSD but no clear indication that PTSD leads to hypertension (Buckley and Kaloupek, 2001). Such changes are potentially important for long-term development of heart disease because there is extensive evidence that increased heart rate is a risk factor for hypertension and cardiovascular events (Palatini and Julius, 1997). However, the findings on an association between PTSD and cardiovascular disease were mixed; a few studies indicated a positive association, and one found no association.
Andersen et al. (2010) reviewed medical records of 4,416 OIF and OEF veterans to determine whether there is an association between PTSD and various physical diseases. Enrolled study participants were followed from 2001 to 2007, and physical disease was diagnosed by primary care providers using ICD-9 codes. The authors adjusted for possible confounders and found that veterans who had a diagnosis of PTSD had significantly increased odds of developing several diseases, including circulatory and hypertensive diseases, compared with veterans who did not have PTSD. Not only was prevalence increased, but survival analyses indicated early onset of several diseases, including circulatory and hypertensive diseases, in veterans who had PTSD (see Figure 4.4).
Trief et al. (2006) investigated whether PTSD and other comorbid psychiatric conditions affect diabetes outcomes. They evaluated male veterans enrolled in a VA primary care database with diabetes and sorted them into four comparison groups: PTSD only (480), depression only (1,696), PTSD and depression (649), and neither PTSD nor depression (11,613). Outcomes evaluated were glycemic control, cholesterol, triglycerides, weight, and body mass index (BMI). The PTSD–depression group had significantly higher cholesterol, low-density lipoprotein, weight, and BMI than one or more of the other groups.
FIGURE 4.4 Hazard ratio of eight disease categories for veterans with PTSD compared to veterans without PTSD.
SOURCE: Andersen et al., 2010 (with permission).
Digestive System Disorders
IOM (2008a) evaluated the relationship between PTSD and gastrointestinal effects and found several studies that reported increased prevalence of gastrointestinal symptoms and disorders in veterans who had PTSD (Barrett et al., 2002; Boscarino, 1997; Dobie et al., 2004; Hoge et al., 2007; Irwin et al., 1996; Schnurr et al., 2000). However, the studies were limited by self-reporting and cross-sectional design. Furthermore, IOM (2008a) noted that the gastrointestinal symptoms are among many somatic symptoms reported by veterans who have PTSD, and this raises the likelihood that PTSD is like other stress-related conditions in which lower sensation thresholds lead to reporting of multiple symptoms.
As described above, Andersen et al. (2010) assessed OIF and OEF veterans for physical disease and found that veterans who had a diagnosis of PTSD had higher odds of developing digestive system diseases and experienced earlier onset of the diseases than veterans who did not have PTSD.
Endocrine Diseases
As reviewed in IOM (2008a), veterans who have PTSD do not appear to be at significantly greater risk for diabetes or thyroid disease than veterans who do not have PTSD (Boscarino, 1997; Dobie et al., 2004; Schnurr et al., 2000; Spiro et al., 2006), although one small study did find that Vietnam veterans who had PTSD had a greater risk of hypothyroidism
(Boscarino, 2004). Differences in some serum thyroid-hormone concentrations have been noted in a few small studies (Mason et al., 1994; Wang and Mason, 1999; Wang et al., 1995), but the results did not suggest hyperthyroidism or hypothyroidism. Andersen et al. (2010) did not find a significant association between PTSD and increased risk of endocrine, nutritional, or metabolic diseases, and this was consistent with the conclusions of IOM (2008a).
Neurocognitive and Neurobehavioral Effects
IOM (2008a) evaluated the relationship between PTSD and neurocognitive and neurobehavioral effects in veteran populations. (The association of PTSD and TBI is covered elsewhere.) Most of the relevant studies have focused on Vietnam veterans. Overall, no association was found between PTSD alone and deficits on tests of cognition in large, wellcontrolled studies, using overlapping populations (Barrett et al., 1996; Crowell et al., 2002; Zalewski et al., 1994). However, the studies did not appear to have included specific tests for memory, such as explicit memory. Other studies that compared veterans who had and did not have PTSD had inconsistent findings; however, when test results were positive, the most common findings were deficits in attention and memory (Gilbertson et al., 2001; Koso and Hansen, 2006; Uddo et al., 1993; Vasterling et al., 1998, 2000, 2002; Yehuda et al., 1995).
Samuelson et al. (2006) compared neuropsychologic functioning in veterans who had PTSD (37), who had PTSD and a history of alcohol abuse (30), who had a history of alcohol abuse (30), and who had neither PTSD nor a history of alcohol abuse (31). The study attempted to eliminate the confounding often caused by comorbid alcohol abuse. PTSD was diagnosed on the basis of structured interviews conducted by a clinical psychologist. The authors controlled for confounders—such as alcohol abuse, depression, education, and vocabulary—and found that PTSD was significantly associated with decreases in verbal memory, attention, and processing speed. They stated that “by controlling for alcohol and depression, the authors can more conclusively demonstrate that verbal memory and attention differences are associated with PTSD.”
Marx et al. (2009) evaluated neuropsychologic outcomes (verbal learning, visual memory, attention, and retention time) in 268 active-duty soldiers before and after deployment to Iraq. One group was tested a median of 42 days before deployment and a median of 404 days after deployment, and the other group was tested a median of 378 days before deployment and a median of 122 days after deployment. PTSD was assessed with the PCL. Soldiers assessed 1 year after deployment showed reduced attention with greater PTSD symptoms. At either postdeployment assessment, greater combat exposure was related to better reaction time. Depression was not associated with neuropsychologic outcomes.
Yaffe et al. (2010) investigated the relationship between PTSD and dementia in 181,093 veterans who were at least 55 years old and free of dementia in 1997–2000. Followup examinations occurred during 2000–2007, and diagnoses were made according to ICD-9-CM codes. Authors compared veterans who had a diagnosis of PTSD (53,155) with veterans who did not (127,938) and found that those who had PTSD had significantly higher rates of dementia. After adjusting for demographic factors and medical and neuropsychiatric comorbidities, the authors found that the veterans who had PTSD still had nearly twice the risk of dementia of veterans who did not have PTSD.
Afari et al. (2009) evaluated the relationship of PTSD, combat-related physical injuries, and headache in 308 OIF and OEF veterans with a battery of questionnaires. They found that PTSD and combat injuries independently predicted headaches. Veterans who had PTSD were 4 times more likely to report headaches than veterans who did not have PTSD or combat injuries. Furthermore, PTSD was significantly associated with tension and migraine headaches, whereas combat injuries were significantly associated only with migraine headaches.
Sexual Dysfunction
Few studies have examined the relationship of sexual dysfunction and PTSD. IOM (2008a) reviewed one small study of combat veterans (Cosgrove et al., 2002) that found that 85% of male veterans who had PTSD and only 25% of those who did not have PTSD had erectile dysfunction. PTSD severity was associated with the severity of erectile dysfunction. However, psychotropic drugs may have contributed to the findings, given that more than 50% of veterans who had PTSD used the medications compared with only 17% of veterans who did not have PTSD.
Hirsch (2009) evaluated sexual dysfunction in 53 male OIF and OEF veterans in a PTSDtreatment facility. Study participants were younger and had received a diagnosis of PTSD more recently than in earlier studies. Conditions reported were diminished libido (39), erectile dysfunction (26), and ejaculatory dysfunction (8). However, most participants were abusing alcohol, were depressed, and had suffered multiple TBIs, all of which were serious study limitations.
Nunnink et al. (2010) investigated which PTSD cluster might be associated with sexual dysfunction in 197 OIF and OEF veterans who completed a battery of questionnaires. Sexual problems were reported by 30.5% of veterans and were characterized as “diminished sexual desire/function” (36) or “impotence or other sexual problems” (32). They found that PTSD symptom severity was significantly higher in the veterans who reported sexual problems and that the numbing cluster9 was the only significant predictor of sexual function. A serious study limitation is that no information was collected on prescription medication, which could have caused or explained the results observed.
Sleep Disorders
Sleep disturbances are common complaints of veterans who have PTSD. In fact, nightmares and difficulty in falling or staying asleep are two of the diagnostic criteria for PTSD. Furthermore, as discussed above, PTSD is often comorbid with other psychiatric conditions that are associated with sleep disturbance, such as depression. IOM (2008a) reviewed the relationship between PTSD and sleep disturbances and noted several studies (Engel et al., 2000; Inman et al., 1990; Neylan et al., 1998) that indicated significantly more problems in veterans who had PTSD than in those who did not on the basis of self-reported information. Several small studies have used objective sleep measures to assess sleep quality, but the results have been inconsistent; some reported no differences (Dagan et al., 1991; Dow et al., 1996; Engdahl et al., 2000), and others reported more sleep disturbances in the PTSD groups (Mellman et al., 1995, 1997; Woodward et al., 2000). The IOM report concluded that objective sleep measures have not been
__________________
9The authors noted that the numbing cluster includes such symptoms as “detachment from others, loss of interest, and restricted range of affect.”
studied in veteran populations large enough to permit generalizations about the association between PTSD and sleep disturbances.
Recent research indicates that sleep disturbances are common generally in veterans and that other health factors contribute to the sleep disturbances observed. Lewis et al. (2009) evaluated 65 Australian Vietnam veterans who had probable PTSD and 87 who did not meet the PTSD criteria. PTSD was assessed with the PCL. The authors reviewed self-report data and found that significant sleep disturbances were reported by all those who had PTSD and by 90% of those who did not. The data indicated, however, that those who had PTSD had more severe sleep problems than those who did not.
Gellis et al. (2010a) investigated health factors that were associated with sleep disturbance in 201 OIF and OEF veterans who had experienced a psychologic trauma and had been referred for a behavioral assessment. The veterans were assessed with the PCL, and 120 were found to have symptom severity consistent with PTSD. Although waking PTSD-symptom severity was strongly associated with sleep disturbances, multivariate analysis that controlled for demographics and waking PTSD symptoms indicated that head injury with LOC was associated with moderate and severe nightmares, alcohol abuse or dependence was associated with moderate nightmares, and depression was associated with moderate and severe difficulties in initiating and maintaining sleep. The data indicate that other comorbid conditions play a role in the sleep disturbances reportedly associated with PTSD.
New research suggests that sleep disturbances might contribute to the development or maintenance of mental-health conditions, such as PTSD and depression. Picchioni et al. (2010) evaluated 567 Army veterans 3 months after their return from an Iraq deployment. PTSD was identified with the PCL. Having nightmares was evaluated as a possible mediator between combat stressors and PTSD, and insomnia was evaluated as a possible mediator between combat stressors and depression. Modeling results indicated that the sleep disturbances were partial mediators and thus could play a role in the development of the mental-health outcomes observed. Research by McLay et al. (2010) supports that hypothesis in that they found that active-duty military personnel who reported insomnia on return from deployment had significantly higher PTSD scores at a 3-month followup than those who did not report insomnia. Furthermore, Wright et al. (2011b) investigated the relationship between insomnia and mental-health disorders—specifically PTSD and depression—in 659 active-duty soldiers who had been deployed to Iraq. Study participants completed questionnaires at 4 and 12 months after deployment; PTSD was assessed with the PCL. They found that insomnia at 4 months significantly predicted PTSD and depression symptoms observed at 12 months, but not vice versa; that is, psychologic symptoms did not significantly predict insomnia. They concluded that their findings supported the idea that insomnia plays a role in the development of PTSD and depression. Wright et al. (2011a) assessed how insomnia affects the relationship between combat exposure and mental-health disorders, specifically PSTD and “alcohol problems.” Study participants—522 military personnel who had been deployed to Iraq—were screened at 12 months before and 3 months after their deployment; PTSD was assessed with the PCL. The authors observed a stronger association between combat exposure and mental-health disorders when insomnia symptoms were more severe than when they were not, and this supported the mediating role of insomnia in the development of these mental-health disorders.
General Symptoms and Health Status
Several investigators have examined the relationship between PTSD and general symptoms or health status. IOM (2008a) concluded that PTSD is associated with increased reports of symptoms, medical conditions, and poor physical health in male and female veterans regardless of whether physical health is determined through physical examinations or selfreports. In fact, PTSD appears to be an even stronger predictor of poor health than does combat exposure. Furthermore, veterans, including OIF and OEF veterans, who have PTSD report more nonspecific chronic pain—such as back pain, headaches, and joint pain—than veterans who do not. The co-occurrence of PTSD and pain appears to be equally common in men and women (Asmundson et al., 2004).
Evaluating the relationship of chronic pain and PTSD, Otis et al. (2010) reviewed data from self-report questionnaires on 149 veterans suffering from chronic pain. Almost half (49%) met the criteria for PTSD on the basis of the PCL. Controlling for age, sex, pain duration, and depressive symptom severity, they found that PTSD was a significant predictor of pain and that veterans who had PTSD and chronic pain scored significantly higher on measures of affective distress than veterans who had pain but not PTSD. Seal et al. (2012) evaluated data on 141,029 OIF and OEF veterans and found that veterans who had PTSD were significantly more likely to be prescribed opioids to treat pain than veterans who did not have PTSD or who had another mental-health diagnosis. The findings held for all PTSD groups, including veterans who had PTSD and a substance-use disorder. Furthermore, the opioids were prescribed at higher doses, in combination with other opioids, and more frequently in the veterans who had PTSD. Consequently, the veterans who had PTSD were at greater risk for adverse clinical outcomes.
Using a battery of questionnaires and medical history interviews, Spiro et al. (2006) compared the health status of veterans who had PTSD (456), depression only (351), and neither condition (1,455). Most of the veterans who had PTSD (83%) screened positive for depression. Health status was assessed by using scales related to physical functioning, bodily pain, general health perceptions, vitality, limitations in activities for various reasons, and mental health (SF-36 Health Survey). Veterans who had PTSD scored significantly lower on all measures than veterans who had depression or veterans who had neither condition, and they reported significantly more medical conditions. The authors concluded that PTSD substantially affects health and that the effects are equal to or greater than those of depression. Their results are consistent with those of an earlier study by Magruder et al. (2004) in which the mental and physical functioning of 513 VA patients was evaluated with the PCL and the SF-36 Health Survey. They controlled for potential confounding factors and found that PTSD symptom severity was significantly associated with decreased mental and physical functioning.
Ouimette et al. (2004) evaluated health status in 134 patients in the VA health care system. They reviewed medical records for physician-diagnosed illnesses and self-report questionnaires on quality of life. PTSD was diagnosed in 33 patients on the basis of structured clinical interviews. A variety of traumatic events were noted; only 12% were combat related. The authors controlled for potential confounders and found that PTSD diagnoses and symptoms were significantly associated with an increased risk of circulatory and musculoskeletal disorders. They observed a positive correlation between PTSD symptom severity and total number of medical conditions. PTSD diagnoses and symptoms also were associated with a poorer quality of life as indicated by lower scores on all measures of the questionnaire (physical function, role limitations due to physical health, energy or fatigue, pain, and general health). Similar results were obtained
after controlling for comorbid psychiatric conditions, such as depression, GAD, and panic attacks. The results are consistent with those reported by Andersen et al. (2010). In addition to the positive associations noted above, Andersen and co-workers found that PTSD was significantly associated with increased prevalence and onset of nervous system diseases, musculoskeletal diseases, and ill-defined signs and symptoms.
Nazarian et al. (2012) evaluated the relationship between medical comorbidities and PSTD (and substance-use disorders) in 62,496 male and 11,224 female OIF and OEF veterans who had at least two visits to a VA medical center over a 2-year period. They reviewed medical records and conducted separate analyses for men and women in 11 medical categories. Prevalences of PTSD, substance-use disorders, and both were 28.2%, 6.2%, and 3.8%, respectively, in women and 35.7%, 12.5%, and 8.1% in men. After adjusting for sociodemographic factors, they found that PTSD significantly increased the odds of a diagnosis in nine categories in men and women and that substance-use disorders significantly increased the odds of a diagnosis in two categories in women and three in men. The investigators did not observe a significant interaction between PTSD and substance-use disorders and concluded that PTSD was more strongly associated with medical comorbidities than were substance-use disorders.
Carlson et al. (2011a) investigated the relationship between postdeployment injuries and PTSD and other mental-health disorders in 742 OIF and OEF veterans using VA health care. They evaluated self-report data and found that about 50% of veterans reported an injury that had occurred after deployment. Results did not differ between men and women. Multivariate analysis indicated that probable PTSD, depression, and anger problems were significantly associated with increased odds of a postdeployment injury.
Psychosocial Effects
Many studies have shown an association between PTSD and a variety of psychosocial effects. IOM (2008a) reviewed the research on PTSD and marital and family conflict and noted several studies of Vietnam veterans that found that marital conflict and family adjustment problems were significantly higher in veterans who had combat-related PTSD than in veterans who did not have PTSD and that the problems persisted for years after the war. For example, Jordan et al. (1992) found that veterans who had PTSD reported significantly more marital and relationship problems, more parenting problems, and poorer family adjustment than veterans who did not. Their spouses or partners were significantly more likely to report lower levels of happiness and life satisfaction and to be more demoralized. Furthermore, children of veterans who had PTSD were substantially more likely to have a behavior problem than those of veterans who did not have PTSD.
Violence and Aggression
Closely related to the reports of marital and family conflict and adjustment problems are studies of intimate-partner violence. IOM (2008a) reviewed the research on this topic and noted an association between combat-related PTSD and increased intimate-partner violence and reports of hostility and violence toward other family members. Jordan et al. (1992), for example, found that family violence was significantly more prevalent in families of veterans who had PTSD. The mean numbers of violent acts committed or threatened over a year by veterans who had and did not have PTSD were 4.86 and 1.32, respectively, and the mean numbers of violent acts
committed or threatened by spouses or partners of veterans who had and did not have PTSD were 3.03 and 0.96. Furthermore, Glenn et al. (2002) found that PTSD symptoms were associated with reports of hostility and violence toward the children of veterans who had PTSD and that the veterans’ violent behavior correlated with their children’s violent behavior.
Reports on OIF and OEF veterans support the findings noted in IOM (2008a). Jakupcak et al. (2007) investigated the relationship between PTSD symptoms and measures of anger, hostility, and aggression by comparing responses in self-report questionnaires by OIF and OEF veterans who had PTSD (47), subthreshold PTSD (21), and no PTSD (49). PTSD was identified by using the PCL. After controlling for such factors as problem drinking and combat exposure, the authors found that veterans who had PTSD or subthreshold PTSD reported significantly greater anger, hostility, and aggression than veterans who had no PTSD; and veterans who had PTSD reported significantly greater anger and hostility than veterans who had subthreshold PTSD. No significant difference in aggression was found between veterans who had PTSD and those who had subthreshold PTSD.
Elbogen et al. (2010) evaluated anger and hostility in 676 Iraq and Afghanistan veterans who served since 2001. The outcome measures evaluated were “aggressive impulses or urges, difficulty managing anger, and perceived problems controlling violent behavior.” The Davidson Trauma Scale was used to assess PTSD symptoms; structural clinical interviews were conducted in a subset of study participants to verify the diagnostic accuracy of the survey. The authors found that PTSD hyperarousal symptoms were significantly associated with all three measures; other PTSD symptoms were less strongly or inconsistently associated with the measures.
Widome et al. (2011) investigated the relationship between PTSD and health-risk behaviors in 406 OIF and OEF veterans attending college. They evaluated self-report data and found that PTSD was significantly associated with a greater risk of physically fighting. They also found a marginally significant association between PTSD and high-risk drinking, which was defined as having at least five drinks at one time.
Taft et al. (2009) investigated intimate-partner aggression and general aggression in 236 male combat veterans at a PTSD clinic. The cohort comprised primarily Vietnam veterans (63%); only 5% and 1% were OIF and OEF veterans, respectively. The majority (68%) were involved in an intimate relationship in the preceding year. Structured clinical interviews were used to diagnose PTSD; 78% of veterans had diagnoses of PTSD. The data indicated that most veterans who had partners had engaged in some type of aggressive behavior in the preceding year; 33% reported physical aggression toward a partner, and 91% reported psychologic aggression toward a partner. Furthermore, veterans who had and did not have partners reported general physical aggression (32% partnered and 39% nonpartnered) and general psychologic aggression (81% partnered and 87% nonpartnered). The PTSD symptoms that best predicted aggressive behavior were those related to “arousal” and “lack of control.”
Teten et al. (2010) compared intimate-partner aggression in male OIF and OEF veterans who had PTSD (27) or did not have PTSD (31) and in Vietnam veterans who had PTSD (28). PTSD was identified at a routine diagnostic screening at a VA medical clinic. The results suggested that OIF and OEF veterans who had PTSD were more likely than the other groups to abuse a female partner but also that OIF and OEF veterans who had PTSD were more likely to sustain abuse by a female partner. In an earlier study of OIF, OEF, and Vietnam veterans, Teten et al. (2009) found that PTSD was not associated with sexual aggression.
Monson et al. (2009) reviewed the research on intimate-relationship problems and PTSD and found that veteran studies indicated that “PTSD is strongly associated with intimate relationship problems and a number of other indices of family adjustment difficulties.” Numbing or avoidance symptoms were most strongly associated with family-relationship problems, and hyperarousal symptoms were most strongly associated with physical and psychologic aggression. Furthermore, comorbid conditions appeared to contribute to the problems observed. The authors noted that few theories have been proposed to explain the association and concluded that “study of the connection between PTSD and intimate relationship functioning is sorely in need of theory development and testing to further understanding of these associations and ultimately advance prevention and treatments.”
Legal Problems
Producing results consistent with the association between PTSD and anger, hostility, and aggression, Highfill-McRoy et al. (2010) found that PTSD was associated with behavior problems in active-duty marines. They compared 77,998 marines deployed to Iraq, Afghanistan, or Kuwait (war-deployed marines) with 13,944 marines deployed elsewhere outside the United States (non-war-deployed marines) on the basis of information from military records that contained physician-diagnosed conditions. They found that war-deployed marines who had PTSD were more likely to receive demotions and punitive discharges than war-deployed marines who had no psychiatric diagnosis. Both groups of deployed marines who had PTSD were more likely to receive drug-related discharges than were marines who did not have a psychiatric diagnosis. The finding that most troubled the authors was that war-deployed marines who had PTSD were over 11 times more likely than their peers who had no psychiatric diagnosis to commit serious offenses that resulted in punitive discharges. Kulka et al. (1990) found an association between PTSD and arrest and incarceration: 45.7% of Vietnam veterans who had current PTSD had been arrested or jailed more than once in their lives compared with 11.6% of the veterans who did not have PTSD, and 11.5% of the veterans who had PTSD had been convicted of a felony.
Quality of Life
Several recent studies have investigated overall well-being among veterans and found that veterans who have PTSD have more psychosocial problems than veterans who do not. Pietrzak et al. (2009a) investigated the psychosocial effects of partial PTSD in 557 OEF and OIF veterans. PTSD was identified by using the PCL, and psychosocial effects were assessed by using a self-report questionnaire. Study authors found that 120 had full PTSD, 124 had partial PTSD, and 313 had no PTSD. Veterans who had partial PTSD exhibited significantly worse health and psychosocial difficulties than veterans who had no PTSD. A severity–response trend was observed; veterans who had full PTSD exhibited the most significant decrements in health and psychosocial scores.
Similarly, Gellis et al. (2010b) investigated the effects of partial PTSD on quality of life in OIF and OEF veterans who had experienced a traumatic event and were referred for behavioral assessment. All study participants were interviewed by telephone; PTSD was identified by using the PCL. Comparison groups were full PTSD (120), partial PTSD (37), and trauma only (44). The study authors found that veterans who had partial PTSD had significantly
worse mental-health functioning than the trauma-only group; however, when they controlled for “other psychiatric factors,” the two groups did not differ significantly. As in previous studies, those who had full PTSD had the most significant decrements. No differences in physical functioning were found among the groups. The study authors noted that the lack of significant differences between groups could be due to various study limitations, including misclassification (that is, veterans who had partial PTSD might have been assigned to the trauma-only group and those who had full PTSD might have been assigned to the partial-PTSD or trauma-only group).
In a longitudinal study, Shea et al. (2010) investigated the relationship between PTSD and impaired psychosocial functioning in 124 National Guard or reserve veterans who had been deployed to Iraq or Afghanistan. PTSD was diagnosed by using structured clinical interviews at about 6 months after deployment. Controlling for potential confounders, the authors found that PTSD diagnosis and symptoms were significantly associated with poor psychosocial functioning and distress. Numbing or avoidance symptoms adversely affected relationships and strongly predicted impaired interpersonal and social functioning. Hyperarousal symptoms strongly affected overall functioning and predicted overall severity and distress. The authors noted that the results are important because they show that poor function and distress can occur soon after exposure (that is, within months), not necessarily only years after exposure.
Overall, Kehle et al. (2011b) found a negative association between PTSD and social functioning and quality of life in a study of 348 OIF National Guard soldiers. The soldiers were surveyed 1 month before and 3 months after deployment. Structured clinical interviews were conducted 6–12 months after deployment, and self-report responses were collected on social functioning and quality of life. PTSD and subthreshold PTSD were diagnosed in 7% and 9% of the cohort, respectively. Other psychiatric diagnoses—including depression (15%), other anxiety disorders (13%), alcohol-use disorders (13%), and drug-use disorders (1%)—were noted. They found that soldiers who had PTSD or subthreshold PTSD were significantly more likely to have impaired social functioning and decreased quality of life than those who did not have such a diagnosis. Comorbid psychiatric diagnoses were associated with greater impairment in the soldiers who had PTSD. Those general findings are consistent with the adverse psychosocial effects that have been noted in military personnel or veterans who have PTSD.
Employment
One factor important for successful reintegration of veterans into civilian life is gainful employment. IOM (2008a) reviewed several studies (Jordan et al., 1992; Savoca and Rosenheck, 2000; Zatzick et al., 1997a, 1997b) that found that veterans who had PTSD were more likely to be unemployed and, if employed, likely to receive lower wages than their counterparts who did not have PTSD. Smith et al. (2005) investigated employment outcomes in 325 Vietnam veterans who had severe or very severe PTSD and found that veterans who had severe symptoms were more likely to be unemployed or to have only part-time employment. They, however, did not find a significant association between earnings and symptom severity in people who had comparable employment.
Adler et al. (2011) recently evaluated work-performance measures in 797 OIF and OEF veterans who were referred for behavioral-health assessment. They reviewed self-report data from standard questionnaires and surveys and found that psychiatric disorders—major depressive disorder, PTSD, and GAD or panic disorder—adversely affected multiple dimensions of work performance, including mental–interpersonal demands, time management, and output.
Substantial decrements in productivity were noted in those veterans compared with nonveteran employees who did not have psychiatric disorders. Similarly, Erbes et al. (2011) investigated the relationship between mental-health disorders and occupational functioning in 262 National Guard or reservists who had been deployed to Iraq. Mental-health disorders—PTSD, subthreshold PTSD, major depressive disorder, and alcohol-use disorder—were diagnosed by using structured clinical interviews about 6 months after deployment, and occupational functioning was assessed at the diagnostic interview and again 1 year later. A high prevalence of comorbidity was found, ranging from 46% in participants who had alcohol-use disorder to 85% for participants who had PTSD. The investigators found that employment status did not differ between those who had mental-health disorders and those who did not; however, “work role functioning” was lower in those who had mental-health disorders, and those who had PSTD had high rates of deterioration in work role functioning.
Homelessness
Homelessness is closely related to employment difficulties, but few studies have investigated the possible association between PTSD and homelessness in veteran populations. IOM (2008a) noted one study (Rosenheck and Fontana, 1994) that did not find a direct relationship between PTSD and homelessness but did find that combat exposure and other psychiatric illnesses were directly related to homelessness.
Effects on Caregivers
Veterans or military personnel who have PTSD are not the only ones to suffer adverse psychosocial effects; their caregivers also appear to be adversely affected. Calhoun et al. (2002) investigated perceived burden and psychologic distress in the partners of 71 Vietnam veterans seeking treatment for PTSD. PTSD was diagnosed by using structured clinical interviews; 51 received a diagnosis of PSTD. The investigators found that partners of those who had PTSD reported greater burden and had worse psychologic adjustment—such as more depression, hostility, and aggression—than partners of those who did not have PTSD. Greater severity of PTSD correlated with greater burden, and caregiver burden was strongly associated with the veterans’ psychologic adjustment.
Summary
Estimates of prevalence of PTSD in service members deployed to OEF and OIF range from 5% to 20%. Some risk factors for PTSD are low age in active duty (higher age in reservists); combat exposure; being single or divorced; prior traumatic exposure, especially childhood physical abuse and other adverse experiences; MST; and a history of mental-health diagnosis. PTSD is often comorbid with several other health and mental-health conditions, such as depression, anxiety disorders, and substance use (particularly alcohol abuse). Numerous psychosocial conditions have been found to be associated with PTSD, for example, violence and aggression, relationship problems, decreased quality of life, legal problems, and homelessness. Research demonstrates that PTSD can cause substantial distress and functional impairment. The various effects and the interconnections of PTSD with other physical, mental, and social outcomes can interfere with readjustment into one’s previous life.
MULTIPLE DEPLOYMENTS AND POSTTRAUMATIC STRESS DISORDER
Multiple Deployments, Deployment Location, and Dwell Time
Soldiers deployed to Iraq report long deployment as the foremost stressor in theater (MHAT-II, 2005). To study the mental-health impact of deployment length, most researchers measure the number of deployments. The mental-health outcome most commonly diagnosed is PTSD or PTSD in conjunction with other mental disorders, such as depression and anxiety, as measured by validated symptom checklists used for screening purposes. Many studies have found that multiple deployments place soldiers at increased risk for PTSD, but the evidence is more ambiguous with respect to other mental-health outcomes. A few studies, described below, have examined the mental-health impact of dwell time; the data are conflicting as to whether a longer dwell time increases or decreases the risk of mental-health problems.
Phillips and colleagues (2010) studied marines in the Recruitment Assessment Program, of whom 433 were deployed once and 273 twice. Using the PCL, they found that two deployments nearly doubled the risk of PTSD (adjusted OR = 1.91 [1.10–3.33]). However, the cumulative length of deployment was not a significant predictor of PTSD.
Reger and colleagues (2009) studied Army troops in the Soldier Wellness Program, an extension of a standard postdeployment screening program conducted throughout the Army and DOD. They screened 661 who had a single deployment and 661 who had two deployments. They found a higher risk of PTSD in those who had two deployments—an adjusted OR of 1.64 (p = 0.001) with a less conservative cutoff and an OR of 1.60 (p = 0.001) with a more conservative cutoff. They did not find an association between the number of deployments and major depression, panic, other anxiety, and hazardous alcohol consumption.
To determine the effects of multiple deployments, Kline et al. (2010) reviewed self-report data on 2,543 National Guard troops deployed to Iraq and found that those who had at least one previous deployment to Iraq or Afghanistan were three times more likely than those not previously deployed to screen positive for PTSD and major depression. Alcohol dependence, chronic pain, and worse physical function were also significantly more likely in previously deployed troops. Phillips et al. (2010) also found that multiple deployments significantly increased the odds of screening positive for PTSD in marines who had been deployed to Iraq or Afghanistan. Fear et al. (2010) evaluated the effect of deployment location and multiple deployments on the mental health of UK armed forces and found a significant association between deployment to Iraq or Afghanistan and probable PTSD in reservists (1,712) but not in “regular” armed forces (8,278); PTSD was assessed with a questionnaire. No association was found for multiple deployments, but PTSD was associated with combat exposure. The UK experience may not be comparable with US experience, and the difference may account for the apparently conflicting results that have been observed.
The largest study of multiple deployments was published in the Medical Surveillance Monthly Report (AFHSC, 2011). It studied medical records of all 1.35 million active-duty military in 2003–2010 who had served in OIF, OEF, or Operation New Dawn (OND). The study was large enough to enable examination of not only a second deployment but third through fifth deployments. A greater percentage of deployers received a diagnosis of PTSD after the second through fourth deployments than after the first. Anxiety-related disorders, depression, and adjustment reactions were significantly higher after the second or third than after the first
deployment; after the third deployment, there was a dropoff in rates of disorders, which was indicative of a “healthy-warrior” effect. Health care workers had the highest rates of disorders—even higher than those of combat troops. There was no association between multiple deployments and alcohol dependence or abuse or between multiples deployments and suicidal ideation or self-inflicted injury.
The same study investigated the effects of dwell time and found that as dwell time lengthened, most mental disorders were increased, including PTSD, major depression, anxietyrelated disorders, and suicidal ideation. But there was no association between dwell time and substance abuse. Those findings are at odds with those of MacGregor and colleagues (2012), who studied nearly 16,400 marines deployed to Iraq. Using medical records and deployment databases, they found significantly reduced rates of disorders when dwell time doubled.10 For PTSD only, the OR was 0.47 (0.32–0.70); for PTSD with other mental health disorders, the OR was 0.56 (0.33–0.94); and for “other mental health disorder,” the OR was 0.62 (0.51–0.75). Thus, this study found that longer dwell time had a protective effect.
The Millennium Cohort study is a large, population-based prospective DOD study of military personnel in all branches of service. One of the investigations spawned by this undertaking was a study of multiple vs single deployers in relation to PTSD (Bonanno et al., 2012). The sample contained nearly 3,400 single deployers and 4,400 multiple deployers screened for PTSD before deployment and at two times thereafter spaced 3 years apart. The study was focused on the trajectory of symptoms assessed with the PCL-Civilian. It found moderate to improving PTSD in 8% of single and 8.5% of multiple deployers and a worsening to chronic course in 6.7% of single and 4.5% of multiple deployers. The study concluded that the trajectories were similar. No information was given on the specific number of deployments, on the grounds that this information might influence the outcome, according to a separate study (AFHSC, 2011), which found that PTSD rates declined precipitously at fourth and fifth deployments.
In a program that began in 2003, DOD conducts annual or biennial detailed assessments of soldiers’ mental health during deployment in Iraq or Afghanistan. The teams carrying out the assessments are known as mental-health assessment teams. Dispatched by the Army surgeon general, they survey up to 2,300 personnel, typically combat units of the Army and, more recently, marines. They also conduct focus groups, but their data on multiple deployments are based on surveys. Their method varies somewhat from year to year, but the investigators are most likely to use the PCL and other validated surveys to assess mental health. Their reports use the term acute stress to denote PTSD symptoms in a combat zone (MHAT-IV, 2006).
Four reports over the last 6 years have analyzed the effects of multiple deployments. The first, of 1,320 service personnel in 2006 (MHAT-IV, 2006), compared one-time with two-time deployers and found that the latter were significantly more likely to screen positive for acute stress (24% vs 15%), depression (10% vs 8%), anxiety (12% vs 7%), and any mental-health problem (27% vs 17%).
The next report compared three groups: first-time, second-time, and third-time deployers. Of a total of 2,163 service members, third-time deployers (27.2%) and second-time deployers (18.5%) were significantly more likely to screen positive for any mental-health problem than
__________________
10They measured dwell time as the length of time between deployments divided by the length of the first deployment.
were first-time deployers (11.9%). There was no relationship between multiple deployments and individual disorders, suicidal ideation, or marital discord. But there was a significant relationship between multiple deployments and use of alcohol (MHAT-V, 2008). The report did not specify whether personnel screened positive for individual disorders.
The ensuing report, published in 2009, also looked at first-, second-, and third-time deployers. Of a total of 638 service personnel, third-time deployers (31%) and second-time deployers (18%) were significantly more likely to screen positive for any mental-health problem than were first-time deployers (13.6%). Regarding medications, third-time deployers (9.8%) were more likely than second-time deployers (4.5%) and first-time deployers (3.5%) to report taking “any mental health” medication. The study also found that the longer the deployment or the greater the number of deployments, the more likely were multiple deployers to report marital problems. The report did not specify whether personnel screened positive for individual disorders (MHAT-VI, 2009).
The most recently published report, published in 2011, found that third- or second-time deployers were more likely than first-time deployers to report any psychologic problem, any mental-health medication, and considering divorce or separation. The report did not specify findings on individual mental disorders (MHAT-VII, 2011) (see Figure 4.5 below).
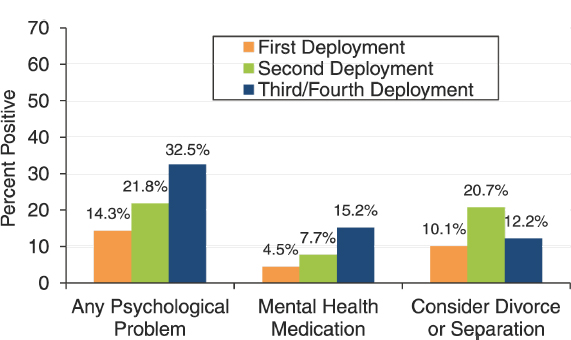
FIGURE 4.5 Number of deployments and selected outcomes.
SOURCE: MHAT-VII, 2011.
Shen et al. (2010) and Shen and Arkes (2009) examined the relationship between PTSD diagnosis and deployment location and duration in 678,227 active-duty enlisted personnel in all four branches of the armed services. They found that deployment to Iraq or Afghanistan significantly increased the odds of a PTSD diagnosis in all four services; the greatest effect was found in the Navy, and the smallest in the Air Force. Deployments longer than 180 days were associated with increased odds of a PTSD diagnosis. An analogous study of 95,873 officers in all four services yielded similar results, but the deployment effects were smaller and deployment duration appeared to be a risk factor only in Army and Navy officers (Shen and Arkes, 2009). Reger et al. (2009) reviewed routine mental-health screening of 1,322 regular, active-duty
soldiers who were evaluated 90–180 days after deployment to Iraq and reported increased odds of PTSD after two deployments.
MOOD DISORDERS
Mood disorders are signature conditions of the current conflicts. The present report focuses on TBI and PTSD, and depression is frequently comorbid with both. The centrality of depression has been emphasized in previous IOM reports on deployment and postdeployment health, so only a brief discussion of mood disorders, specifically depression, is provided below.
Mood disorders are a cluster of mental disorders that are characterized by mood swings or an abnormally depressed (low) mood or a manic mood or irritability. The most common mood disorder is depression, and the clinically most important form is major depression, which is characterized by persistent feelings of sadness accompanied by several symptoms related to changes in appetite or sleeping patterns, loss of interest in activities, fatigue, inability to concentrate, and hopelessness or suicidal thoughts. As described in DSM-IV (APA, 2000), major depressive disorder is characterized by the occurrence of at least one major depressive episode (see Box 4.2). It is the second-most common mental-health diagnosis in veterans after PTSD (Seal et al., 2009).
Like PTSD, depression may be defined by strict criteria, such as the DSM criteria for major depression, or by self-assessment of depression symptoms. The RAND (Tanielian and Jaycox, 2008) report reviewed 12 studies that assessed the prevalence of depression in service members who served in OEF or OIF. Estimates of prevalence in active-duty service members ranged from 5% (Hoge et al., 2006; Kolkow et al., 2007; MHAT-II, 2005) to 37% (Lapierre et al., 2007). Thomas et al. (2010), described above, also estimated the prevalence of depression in active-duty and National Guard troops at 3 and 12 months after deployment to Iraq. They used three case definitions of depression, each reflecting a level of functional impairment. At 3 months, the prevalence ranged from 16% (no functional impairment) to 8.3% (serious impairment) in active-duty soldiers and from 11.5% (no impairment) to 5.0% (serious impairment) in National Guard soldiers. At 12 months, the rates were similar to those at 3 months in active-duty soldiers but substantially increased in National Guard soldiers.
Prevalence varies by sex. For example, as in the general population, female veterans have higher rates of major depression and depressive symptoms, whereas male veterans typically have higher rates of substance use disorders. As noted above, a number of studies have documented that various aspects of deployment increase the risk of depression (Fritch et al., 2010; Kline et al., 2010; Riviere et al., 2011). For example, Wells et al. (2010) investigated the relationship between deployment and the risk of depression as defined by the Primary Care Patient Health Questionnaire. They evaluated data on over 30,000 men and 10,000 women in the Millennium Cohort Study who did not have depression at baseline and found that deployed service members who were exposed to combat in Iraq or Afghanistan had the highest rates of new-onset depression (men, 5.7%; women, 15.7%). Those who did not deploy had intermediate rates (men, 3.9%; women, 7.7%), and those who deployed and were not exposed to combat had the lowest rates (men, 2.3%; women, 5.1%).
BOX 4.2
Criteria for Major Depressive Episode
A. Five (or more) of the following symptoms have been present during the same 2-week period and represent a change from previous functioning; at least one of the symptoms is either (1) depressed mood or (2) loss of interest or pleasure.
Note: Do not include symptoms that are clearly due to a general medical condition, or moodincongruent delusions or hallucinations.
1. depressed mood most of the day, nearly every day, as indicated by either subjective report (e.g., feels sad or empty) or observation made by others (e.g., appears tearful). Note: In children and adolescents, can be irritable mood.
2. markedly diminished interest or pleasure in all, or almost all, activities most of the day, nearly every day (as indicated by either subjective account or observation made by others)
3. significant weight loss when not dieting or weight gain (e.g., a change of more than 5% of body weight in a month), or decrease or increase in appetite nearly every day. Note: In children, consider failure to make expected weight gains.
4. insomnia or hypersomnia nearly every day
5. psychomotor agitation or retardation nearly every day (observable by others, not merely subjective feelings of restlessness or being slowed down)
6. fatigue or loss of energy nearly every day
7. feelings of worthlessness or excessive or inappropriate guilt (which may be delusional) nearly every day (not merely self-reproach or guilt about being sick)
8. diminished ability to think or concentrate, or indecisiveness, nearly every day (either by subjective account or as observed by others)
9. recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan, or a suicide attempt or a specific plan for committing suicide
B. The symptoms do not meet criteria for a Mixed Episode (see DSM-IV-TR, 2000)
C. The symptoms cause clinically significant distress or impairment in social, occupational, or other important areas of functioning
D. The symptoms are not due to the direct physiological effects of a substance (e.g., a drug of abuse, a medication) or a general medical condition (e.g., hypothyroidism)
E. The symptoms are not better accounted for by Bereavement, i.e., after the loss of a loved one, the symptoms persist for longer than 2 months or are characterized by marked functional impairment, morbid preoccupation with worthlessness, suicidal ideation, psychotic symptoms, or psychomotor retardation
SOURCE: Reprinted with permission from the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (Copyright 2000). American Psychiatric Association.
Similarly, Shen et al. (2012) evaluated the relationship between deployment and major depression and substance-use disorders in 678,382 active-duty military personnel (Army, 333,548; Marines, 98,524; Navy, 134,015; and Air Force, 112,295). They reviewed military and medical records and found that deployment during Iraq and Afghanistan wars increased the likelihood of major depression and substance-use disorders; the greatest effect was observed in the Army and the Marine Corps. Deployment duration appeared to increase the odds of depression and substance-use disorders only in Army personnel. As noted in the section “Posttraumatic Stress Disorder,” other risk factors for depression include MST (Kimerling et al.,
2010; Suris and Lind, 2008), childhood physical abuse (Fritch et al., 2010), and adverse childhood experiences (Cabrera et al., 2007).
There have been no population-based studies of US service members deployed to war zones in which investigators used structured diagnostic interviews, which permit more direct estimation of major depression and have an advantage over the screening instruments that are commonly used in epidemiologic surveys. According to RAND (Tanielian and Jaycox, 2008), the extant studies may substantially underestimate the prevalence of depression in the postdeployment samples. Furthermore, most studies used convenience samples, which may not be representative of the entire population deployed to war zones.
Investigators have shown that depression is a major contributor to health dissatisfaction (Rauch et al., 2010) and to mental-health and physical-health outcomes (Pittman et al., 2012). In fact, Kinder et al. (2008) found a positive association between depression and all-causes mortality. They evaluated self-report data and administrative medical records on 35,715 patients of VA medical centers, who were assigned to four groups—those who had a history of depression (6,876), those who had a history of PTSD (748), those who had a history of depression and PTSD (3,762), and those who had no history of either condition (24,329). After adjusting for potential cofounders (age, demographic factors, alcohol and drug use, smoking status, and medical comorbidities), they found that those who had a history of depression were at higher risk for death over a 2-year period than those who had no history of depression or PTSD. Furthermore, those who had a history of depression and PTSD were not at greater risk than those who had only a history of depression; this is consistent with the finding that those who had a history of PTSD were not at greater risk of death. The authors noted that further analyses indicated that current depression symptoms might explain the observed relationship between death and history of depression. Regardless of a precise estimate of prevalence, depression in OIF and OEF veterans remains a serious problem that has increased since initiation of the Iraq War (see Figure 4.3).
SUBSTANCE-USE DISORDERS
Substance-use disorders include the abuse of and dependence on drugs (including illicit drugs, prescription drugs, alcohol, and other toxic agents). According to DSM-IV TR (APA, 2000), substance abuse is a “maladaptive pattern of substance use manifested by recurrent and significant adverse consequences related to the repeated use of substances,” whereas substance dependence is defined as “a cluster of cognitive, behavioral, and physiological symptoms indicating that the individual continues use of the substances despite significant substancerelated problems. There is a pattern of repeated self-administration that can result in tolerance, withdrawal, and compulsive drug-taking behavior” (APA, 2000).
Substance-Use Disorders in the General Population
Illicit Drugs
According to the results of the 2010 National Survey on Drug Use and Health (NSDUH) (SAMHSA, 2011), 8.9% of the general population of Americans 12 years old or older reported using illicit drugs in the month before the survey. That represents about 22.6 million people and was similar to the 2009 rate of 8.7% and higher than the 2008 rate of 8%. Illicit drugs included
marijuana and hashish, cocaine (including crack), heroin, hallucinogens, inhalants, and nonmedical use of prescription drugs.
Alcohol
With regard to alcohol abuse and dependence, 51.8% of Americans 12 years old or older, 131.3 million people, reported using alcohol, a rate that is similar to the 51.9% of 2009. Binge drinking (having five or more drinks per occasion on 1 day) was reported by 23.1% of the people 12 years old or older in the month before the survey, about 58.6 million people, a rate similar to the 23.7% of 2009.
Heavy drinking (defined as binge drinking on at least 5 days in the preceding 30 days) was reported by 6.7% of the population in 2010. However, among those 18–25 years old, the rate of binge drinking was 40.6% and the rate of heavy drinking 13.6%; both these rates were similar to the rates of 2009.
Prescription Drugs
According to the National Institute on Drug Abuse, the most commonly abused prescription drugs are opioids, which are often prescribed for pain relief; central nervous system depressants, such as barbiturates and benzodiazepine, often prescribed for anxiety or sleep problems; and stimulants, often prescribed for attention-deficit hyperactivity disorder, the sleep disorder narcolepsy, and obesity.
Abuse of prescription drugs has resulted in overdose deaths. According to CDC, 36,450 overdose deaths resulted from prescription drugs in 2008, and 73.8% of them involved opioid pain relievers (CDC, 2011b).
In 2010, the NSDUH found that about 9.0 million Americans 12 years old or older reported nonmedical use of prescription drugs, including 5.1 million users of pain relievers, 2.2 million users of tranquilizers, 1.1 million users of stimulants, and 374,000 users of sedatives (SAMHSA, 2011).
Substance Use Disorders in the Military
Illicit Drugs
The 2008 DOD Health Related Behavior Survey (Bray et al., 2009b), which is conducted in a random sample of active-duty military and questions them about drug use in the previous month, found the rate of illicit-drug use, excluding prescription drugs, to be about 2% and noted that the rate had been unchanged since 2002. However, in the Army, Marine Corps, and Air Force, rates of illicit-drug use (excluding prescription drugs) were significantly higher in personnel deployed to combat theaters other than OEF and OIF than in those deployed to OEF and OIF or those not deployed. Illicit-drug use, including prescription-drug use, increased from 5% in 2005 to 12% in 2008.
Status of Drug Use in the Department of Defense Personnel: Fiscal Year 2008 Drug Testing Statistical Report (DOD, 2009b) notes the rates of illicit-drug use in FY 2004–2008. That report indicates that illicit-drug use rates were below 2% in active-duty forces. Rates were also below 2% in reserve personnel not on active duty but exceeded 2% in National Guard
personnel not on active duty. Drugs tested included amphetamines, cocaine, ecstasy, marijuana, MDA (methylenedioxyamphetamine), opioids, and phencyclidine.
Alcohol
Milliken et al. (2007) found that rates of problem alcohol use—detected with a two-item screen on the PDHRA—in those screened by DOD after deployment ranged from 11.8% (active duty) to 15.0% (National Guard and reserve). They also noted that of the 56,350 active-duty soldiers who endorsed alcohol misuse (6,669, or 11.8%), only 134, or 0.2%, were referred to alcohol services and that only 29 of those referred were seen within 90 days.
The 2008 DOD HRBS (Bray et al., 2009b) found that military rates of alcohol use are higher than in civilians 18–35 years old but lower in those 46–64 years old. The 2008 survey noted that heavy drinking (five or more drinks per occasion at least once a week) remained at about the 2005 level (20% and 19%, respectively). The services that had the most pronounced increases were the Marine Corps, increasing from 25% in 2005 to 29% in 2008, and the Air Force, increasing from 10% in 2005 to 14% in 2008.
In a recent report that examined health and discipline in the Army (Department of the Army, 2012), findings indicated that incidents of drug and alcohol abuse in soldiers had increased from 28,740 offenses in 2006 to 34,586 in 2009 and then decreased by 9.1% to 31,617 offenses in 2010 and by 4% to 29,708 in 2011. Those recent decreases have been coupled with increased rates of referral for drug and alcohol treatment. In FY 2010, there were over 24,000 referrals of soldiers to the Army Substance Abuse Program; about 50% of those referred were enrolled. It has been found that 43% of active-duty Army personnel reported binge drinking within the preceding month. Although 12% of soldiers reported alcohol problems on the PDHRA, only 2% have been referred for further evaluation or treatment. The report also noted that alcohol abuse is associated with several risk factors related to combat service, such as exposure to the threat of death or injury and a diagnosis of PTSD.
Several earlier studies of military populations found similar problems with substance abuse and dependence, particularly alcohol abuse and dependence, when deployed service members returned from service in Iraq or Afghanistan (Hoge et al., 2004b; Jacobson et al., 2008; Lande et al., 2008; Stahre et al., 2009).
Prescription Drugs
The 2008 DOD HRBS (Bray et al., 2009b) found that in all services there was no significant difference in the rates of prescription-drug misuse in the preceding 12 months. Findings indicate that rates were significantly higher in combat personnel deployed to theaters other than OEF and OIF than in those deployed to OEF and OIF and those who had not been combat deployed (9% in combat deployed, 5% in OEF and OIF deployed, and 6% in nondeployed).
According to the Office of National Drug Control Policy, the number of active-duty military personnel reporting misuse of prescription drugs (12%) is more than twice that in the civilian population (4.4%) in those 18–65 years old. Similarly, 13.1% of women in the military report prescription-drug abuse compared with 3.2% of civilian women (Office of National Drug Control Policy, 2010).
A recent Army report, Army 2020 Generating Health and Discipline in the Force Ahead of the Strategic Reset (Department of the Army, 2012), notes that pain is a leading cause of disability and that 47% of soldiers returning from OEF and OIF report problems associated with pain. About 14% of US soldiers have been prescribed opiate pain medications, and about 25– 35% of wounded soldiers are addicted to prescription pain medications or illegal drugs. The report defines polypharmacy as the use of four or more prescription medications of which at least one is a psychotropic drug or a controlled substance, and it notes that the number of soldiers receiving polypharmacy increased in FY 2010–2011 from 141,199 to 160,175.
Substance-Use Disorders in Veterans: Drugs and Alcohol
Several studies have attempted to determine the prevalence of substance use in OEF and OIF veterans and in all veterans. The present committee has focused its attention on studies of OEF and OIF veterans, but it also presents one study that examined prevalence in all veterans.
Wagner et al. (2007) analyzed the NSDUH data from 2000 to 2003 to estimate the prevalence of substance use and abuse in all veterans. Findings indicated that 22.6% of veterans reported binge drinking, 7.5% heavy alcohol use, and 4.4% illicit-drug use in the preceding month. Veterans reported higher rates of any alcohol use and heavy alcohol use than did comparable nonveterans; binge drinking and illicit-drug use did not differ between veterans and nonveterans. In 2010, Hawkins et al. published findings on alcohol misuse in veterans whose records had been randomly selected from among those of VA outpatients for a standardized medical review for quality-monitoring purposes. Veterans were identified (12,092, including 2,009 women) and screened for alcohol misuse in FY 2007. Alcohol misuse had been assessed with the Alcohol Use Disorders Identification Test (AUDIT);11 findings indicated that the prevalence of alcohol misuse was 21.8% in OEF and OIF men, 10.5% in non-OEF and non-OIF men, 4.7% in OEF and OIF women, and 2.9% in non-OEF and non-OIF women.
Calhoun et al. (2008) conducted an analysis of data extracted from the VA outpatient Survey of Healthcare Experiences of Patients; the survey included a random sample of OEF and OIF veterans who were using VA clinics from October 1, 2004, to September 30, 2005. Findings indicated that 40% of the sample screened positive for hazardous alcohol use and 22% for possible alcohol-use disorder. The majority of the sample was white, male, and married; most were working or in school and had some college education. About 40% of the sample served in active-duty units, and the remaining 60% in the reserves or National Guard.
Eisen et al. (2012) examined alcohol and drug use in OEF and OIF veterans within a year of returning from deployment; PTSD and other mental-health conditions were also examined. A national sample of 596 OEF and OIF veterans were surveyed with validated screening instruments; surveys were mailed, and the authors allowed up to a year for the completed surveys to be returned. Findings indicated that 13.9% screened positive for probable PTSD, 39% for probable alcohol abuse, and 3% for probable drug abuse; men reported more alcohol and drug abuse than women. When examining health records of OEF and OIF veterans who were using VA health care services, Bagalman (2011) found the prevalence of drug abuse to be 4% and of dependence to be 3% during FY 2002–2010.
__________________
11 The Alcohol Use Disorders Identification Test screen is a 10-item instrument that is used to assess alcohol-related problems and hazardous drinking.
The VA produces a quarterly analysis of VA health care service use by OIF and OEF veterans (VA, 2012). The numbers include the 834,463 veterans who separated from active duty service and who obtained care at VA facilities since from FY 2002 to the third quarter of FY 2012. That analysis found that 52,672 veterans had alcohol-dependence syndrome and 28,218 were diagnosed with drug dependence.
A study of 4,270 veterans who were 18–30 years old and were seeking care at the VA Palo Alto Health Care System noted that the prevalence of opioid use had increased from 3% in 2003 to 4.5% in 2007 (Wu et al., 2010). The patients overwhelmingly were male (91%) and white (69.9%) and had a comorbid mental-health diagnosis (29.8% had a mood disorder, 26.8% PTSD, and 20.7% a substance-use disorder). The average veteran had prescriptions from three providers and was exposed to two opioids. The prescriptions were typically written by primarycare providers; less than 1% were written by pain specialists.
In another study of opioid use in OEF and OIF veterans, researchers conducted a retrospective review of VA administrative data (Macey et al., 2011). Findings indicated that prescription opioid use was fairly common in OEF and OIF veterans who had pain and diagnoses of particular medical conditions (for example, lower back pain, migraine headaches, and PTSD). Of the 763 OEF and OIF veterans who had chronic pain (not associated with cancer), about twothirds were prescribed opioids over a 1-year period, and at least one-third were prescribed opioids on a long-term basis.
Risk Factors for Substance-Use Disorders in Active-Duty Personnel
Two recent studies examined predictors of alcohol use in National Guard soldiers before deployment (Ferrier-Auerbach et al., 2009) and after deployment (Kehle et al., 2011a). Some 515 members of a National Guard unit completed questionnaires about alcohol use before deployment to OIF. Findings indicated that 2.7% had not consumed any alcohol in the preceding year, but 26.8% of the sample engaged in binge drinking at least once per week. Rates of probable PTSD were 7%, and 6% endorsed symptoms of depression. Being single was associated with drinking more total alcohol over the year and a greater frequency of binge drinking.
In the postdeployment group, 348 National Guard soldiers deployed to Iraq from March 2006 to July 2007 completed self-report measures a month before deployment and 3–6 months after deployment. About 13% had diagnoses of alcohol-use disorder; 38% of these had an alcohol-use disorder that developed after return from deployment and was predicted by higher levels of PTSD symptom severity.
Bray et al. (2009a) compared 2007 rates of substance use in civilians with 2008 rates in military personnel and found that after adjustment for sociodemographic differences, rates of heavy alcohol use were higher in military personnel than in civilians (20% vs 14%). Bray et al. (2010) examined stress, mental health, and substance use in 28,546 US military personnel who completed the 2008 DOD survey. Trends showed reductions in tobacco use and illicit-drug use but increases in prescription-drug misuse, heavy alcohol use, stress, PTSD, and suicide attempts. Deployment exacerbated some of those changes. Heavy alcohol use was higher in personnel who had been deployed to any operational theater than in the nondeployed. There were no differences by theater for any illicit-drug use, including prescription-drug misuse, in the preceding year. Perceived high work stress in the preceding 12 months was significantly higher in personnel in
any operational theater than in those who had not been deployed. Rates of experiencing high family stress in the preceding year were significantly higher in those deployed to Afghanistan or Iraq than in those deployed to other operational theaters.
Blume et al. (2010) assessed alcohol use in 876 US Army soldiers who mobilized and demobilized from Iraq during a 9-month period in 2003. HRBS questions were used to evaluate substance use and stress. The soldiers reported a moderate level of general stress at mobilization and demobilization, but only a minority reported substantial combat stress. Lower age, non-active-duty status before mobilization, and more general stress were associated with alcohol use in the 2 weeks before the demobilization evaluation. Male sex was associated with ingesting more drinks per drinking day. The results suggest that younger, non-active-duty men experiencing stress may be at risk for increased drinking after deployment.
Wilk et al. (2010a) found that a high rate of combat exposure involving threatening situations and witnessing of atrocities was associated with alcohol misuse. The authors anonymously surveyed 1,120 US Army infantry soldiers within 3–4 months after their return from deployment to Iraq regarding their experiences in combat and their physical and mental health. Soldiers who had higher rates of exposure to the threat of death or injury were significantly more likely to screen positive for alcohol misuse; exposure to atrocities predicted misuse of alcohol and alcohol-related behavioral problems.
Burnett-Ziegler et al. (2011) studied 585 members of recently returned Michigan National Guard members at a reintegration weekend. Some 36% of the National Guard members who participated met the AUDIT criteria for alcohol misuse. In the multivariate logistic regression analysis, service members who were male, were younger, and reported symptoms of depression and PTSD were at increased risk of meeting criteria for alcohol misuse. Of the National Guard members who met criteria for alcohol misuse, 31% reported receiving mental-health services in the preceding year, but only 2.5% reported receiving specific substance-abuse treatment. Those who reported misusing alcohol were most likely to report receiving services from a general physician at a military facility. National Guard members frequently identified stigma—particularly concerns related to their military career, commanding officers, and peers—as a barrier to treatment.
Spera et al. (2011) surveyed a stratified random sample of 56,137 active-duty Air Force members on 80 bases worldwide to determine the relationship between deployment and SUDs. Logistic regression analysis demonstrated that both higher frequency of deployment and greater cumulative time deployed since September 11, 2001, were associated with a greater likelihood of problem drinking. For each incremental increase in deployment frequency, the risk of being a problem drinker increased by 14%. Moreover, for each additional year that an Air Force member was deployed, the risk increased by 23%.
Army 2020 Generating Health and Discipline in the Force Ahead of the Strategic Reset (Department of the Army, 2012) notes that alcohol abuse is associated with several issues related to combat service, such as high rate of exposure to the threat of death or injury and a diagnosis of PTSD. A 2010 study by the Office of the Army Surgeon General (Office of the Army Surgeon General, 2010) identified numerous risk factors that may be associated with misuse of opioids, that is, being 45 years old or older, male sex, family history of prescription drugs, cigarettesmoking, substance disorder, preadolescent sexual abuse in women, major psychiatric disorder, prior legal problems, motor-vehicle accidents, and poor family support.
Risk Factors for Substance-Use Disorders in Veterans
Numerous studies have examined risk factors for substance-use disorders in veterans. Findings from the studies below indicate the following risk factors: childhood trauma, PTSD and depression, service in the Army or Marine Corps, deployment to OEF or OIF, and pain disorders.
In a study of 60 rural and urban OEF and OIF veterans enrolled at three VA sites in Nebraska, childhood trauma was associated with drug dependence, polysubstance dependence, and four or more attempts at treatment for SUDs (Nash et al., 2011). There were no significant differences in trauma exposure between the rural and urban veterans.
A sample of 287 OEF and OIF veterans assessed at a VA facility in Seattle from 2004 to 2007 were screened for PTSD, depression, and alcohol misuse with validated screening instruments. Findings indicate that 28% of the veterans screened positive for alcohol misuse, 37.3% for PTSD, and 37.3% for depression; 76.6% of the PTSD cases also screened positive for depression. There did not appear to be any significant difference in marital status, race, employment status, or family income as a function of alcohol misuse. However, veterans who screened positive for alcohol misuse were younger, more likely to have served in the Army or Marine Corps than in the Navy or Air Force, and more likely to have reported direct combat experience. Predictors of alcohol misuse included sex, branch of service, PTSD status, and depression; PTSD and depression were associated with a twofold increase in the likelihood of alcohol misuse (Jakupcak et al., 2010a).
A study by Hawkins et al. (2010) compared a national sample of OEF and OIF veterans with a sample of non-OEF and non-OIF veterans who were all seen in the VA health care system in FY 2007. Findings indicated that alcohol misuse was higher in OEF and OIF male veterans than non-OEF and non-OIF male veterans even after adjustment for recognized substance-use and mental-health disorders, such as PTSD. The highest-risk group was OEF- and OIF-deployed men under 30 years old.
Seal et al. (2012) note that opioid analgesic prescriptions have nearly doubled in the United States since 1994 with the recognition of pain treatment. OEF and OIF veterans who have pain and PTSD and are prescribed opioids might be at high risk for misuse of prescription opioid drugs. A national sample of OEF and OIF veterans were studied to look for risks and adverse clinical outcomes associated with prescription opioid use. A retrospective cohort of OEF and OIF veterans identified by using a VA database included veterans who received a new noncancer pain diagnosis within a year of entry into the VA health care system. A total of 141,029 veterans were identified and followed for a year beyond the pain diagnosis. The veterans were overwhelmingly male (88.5%), white (50.6%), and enlisted (93.3%), and most (64.3%) had served in the Army. Most (66%) of the veterans had received two or more pain diagnoses; 51% received at least one mental-health diagnosis—19% a diagnosis of excluding PTSD and the remaining 32% a PTSD diagnosis with or without other mental-health diagnoses.
The 141,029 veterans who received pain diagnoses included 15,676 (11%) who received prescription opioids for 20 or more consecutive days and were in most cases (77%) given prescriptions by VA primary care physicians. Patterns of high-risk opioid use were detected in the 15,676 if they also had a mental-health diagnosis other than PTSD or with PTSD. Compared with veterans who did not have a mental-health diagnosis, veterans who had PTSD were more likely to be in the highest quintile for dose (22.7% vs 15.9%), to receive more than one type of
opioid concurrently (19.8% vs 10.7%), to receive concurrent sedative hypnotics (40.7% vs 7.6%), and to obtain opioid refills (33.8% vs 20.4%). Thus, veterans who receive PTSD diagnoses were more likely than those who had other mental-health disorders to be prescribed opioids for longer periods and to receive sedative hypnotics in addition to opioids.
Veterans in all mental-health diagnostic categories who were prescribed opioid medications had a higher prevalence of adverse clinical outcomes than those who were not prescribed opioids (9.5% vs 4.15%). The types of adverse clinical outcomes, in an emergency setting or in inpatient admissions, included accidents resulting in wounds or injuries, opioidrelated accidents, overdoses, alcohol and nonopioid drug-related accidents and overdoses, selfinflicted injuries, and violence-related injuries. The absolute risk of all adverse clinical outcomes except wounds and injuries was highest in the PTSD group.
Substance-Use Disorders and Comorbid Conditions
Numerous studies have documented the epidemiology of the co-occurrence of substanceuse disorders and anxiety disorders (e.g., Flynn and Brown, 2008). A review article by Brady et al. (2009) examines comorbidity issues related to PTSD, SUDs, and TBI in veterans and notes that there is symptom overlap among those disorders in addition to a common neurobiology. It has been noted that veterans who have a diagnosis of depression and SUD at the time of entry into the VA system have an increased risk of greater disease burden that remains constant (Possemato et al., 2010). Several studies have examined the co-occurrence of PTSD and SUD in OEF and OIF veterans, and they are discussed briefly below.
Seal et al. (2008) conducted a study of 338 OEF and OIF veterans who participated in postdeployment screening at a VA medical center or associated VA community-based clinics from 2004 to 2006. Their results demonstrated that a substantial number of the veterans met the criteria for co-occurring mental-health outcomes. Of the 338, 69% (233) screened positive for one or more mental-health disorders, and 61% for comorbid mental-health symptoms. In a followup study, Seal et al. (2011), using the VA OEF/OIF Roster of veterans, examined diagnoses in veterans who used VA health care for the first time from October 16, 2001, through September 30, 2009. The study population included 456,502 veterans; 12% were female, median age of 28 years; 36% belonged to nonwhite ethnic minorities; 60% served in the Army; and 37% had multiple deployments. Alcohol-use disorder was found in 9% of the overall sample, and drug-abuse disorder was diagnosed in 4.5%. Substance-use disorder was found in 11%, and the prevalence was higher in male veterans than in female veterans. Veterans who had alcohol-use disorder, drug-use disorder, or both had at least one comorbid mental-health diagnosis (PTSD, depression, anxiety, adjustment disorder, or a combination of these).
Stecker et al. (2010) reviewed VA data on 293,861 OEF and OEF veterans to determine common medical and psychiatric diagnoses. They found that alcohol misuse, sleep problems, and pain commonly co-occurred with PTSD or depression, and they noted that pain was diagnosed in about 50% of the sample population. Similarly, Thomas et al. (2010) found that alcohol misuse or aggression was a common comorbidity with PTSD or depression in soldiers who had been deployed to Iraq.
McDevitt-Murphy et al. (2010) investigated relationships among PTSD, alcohol abuse, and health functioning—assessed with a self-report questionnaire (SF-36)—in 151 OEF and OIF veterans. PTSD was identified in 39.1% by using the PCL and a cutoff score of 50. Alcohol
abuse (or hazardous drinking) was identified in 26.5%, and PTSD and alcohol abuse in 15.9%. PTSD was negatively associated with all health measures. Mediation modeling, however, indicated that alcohol abuse was a mediator only for the association of PTSD and mental health, not physical health.
Nazarian et al. (2012) evaluated relationships among medical comorbidities, PSTD, and substance-use disorders in 62,496 male and 11,224 female OEF and OIF veterans who had at least two visits to a VA medical center over a 2-year period. They reviewed medical records and conducted separate analyses of men and women in 11 medical categories. Prevalences of PTSD, substance-use disorders, and comorbid PTSD and substance-use disorders were 28.2%, 6.2%, and 3.8%, respectively, in women and 35.7%, 12.5%, and 8.1% in men. After adjusting for sociodemographic factors, they found that PTSD significantly increased the odds of a diagnosis in nine categories in men and women and that substance-use disorders significantly increased the odds of a diagnosis in two categories in women and three categories for men. The investigators did not observe a significant interaction between PTSD and substance-use disorders and concluded that PTSD was more strongly associated with medical comorbidities than were substance-use disorders.
Shen et al. (2012) evaluated relationships among deployment, depression, and substanceuse disorders in 678,382 active-duty military personnel (Army, 333,548; Marines, 98,524; Navy, 134,015; and Air Force, 112,295). They reviewed military and medical records and found that deployment during Iraq and Afghanistan wars increased the likelihood of depression and substance-use disorders; the greatest effect was observed in the Army and Marine Corps. Deployment duration appeared to increase the odds of depression and substance-use disorders only in Army personnel.
OUTCOMES
The different outcomes associated with substances of abuse have been well documented; for example, cocaine use can precipitate heart attack, respiratory failure, strokes, seizures, abdominal pain, and nausea. Alcohol use has long been associated with damage to the liver and pancreas, fetal alcohol syndrome, changes in the brain, and effects on the heart. Alcohol has also been identified as posing a risk of several types of cancers, such as cancers of the mouth, esophagus, pharynx, larynx, liver, and breast (see http://www.drugabuse.gov; http://www.niaaa.nih.gov).
Studies in active-duty and veteran populations, not necessarily focused on OEF and OIF populations, have revealed additional outcomes associated with substances of abuse; most studies have concentrated on alcohol abuse. In active-duty personnel, the findings focus on spouse abuse, job performance, and alcohol-impaired driving. In veterans, sexual assault, suicide, and increased risk of homelessness have been noted.
Bell et al. (2006) found that alcohol abuse in heavy drinkers (defined as more than 14 drinks per week) and answering “yes” to two or more of six questions on alcohol-related problems was a predictor of domestic violence in whites and Hispanics but not blacks. In 2009, Stahre et al. examined results of the 2005 DOD HRBS (Stahre et al., 2009). Their findings indicated that binge drinkers (defined above) were more likely to report alcohol-related harms, such as poor job performance, alcohol-impaired driving, and criminal-justice problems than
nonbinge drinkers. Similarly, Mattiko et al. (2011) examined the 2008 HRBS and noted that there was a dose–response relationship between frequency of drinking and serious consequences and productivity. Heavy drinkers showed three times the rate of self-reported serious consequences and productivity loss. The types of serious consequences noted in binge drinkers include health consequences and injuries, poor academic performance, unsafe sex, drinking and driving, and a higher risk of sexual assault.
Finally, a study by Martin et al. (2010) examined data on soldiers who abused their spouses to determine the prevalence of substance use during abusive incidents. The authors examined the data in the Army Central Registry for 2000–2004 and noted that 1,873 of the 7,424 soldier spouse abuse offenders had been using substances at the time of the abusive incident. On examination of the records, it was found that 96% of the abusers were using alcohol only, 1% were using illicit drugs only, and 3% were using both alcohol and illicit drugs during abuse incidents. It was also found that 3% of the spouse abusers were women. The offenders using substances during a spouse-abuse incident were more likely to be male (97%) than female, and to be non-Hispanic white (51%) or non-Hispanic black (33%). The offenders were also more likely to be enlisted and in the lower pay grades (98%).
Suicides have been increasing in the military and among veterans; Ilgen et al. (2010) examined violent and nonviolent suicides in veterans who had substance-use disorders. Records of VA patients who had SUDs who were alive at the beginning of FY 2002 and died by suicide during FY 2002–2006 were examined (854) and compared with a random sample of SUD patients who did not die by suicide during that period (4,228). Data were obtained from VA medical records and the National Death Index. Findings indicated that 70% (600) of those who died of suicide used violent means. There was no association between the type of SUD and increased risk of violent suicide. The authors noted that psychiatric disorders are often comorbid with SUDs and increase the risk of suicide.
Cucciare et al. (2011) examined sexual assault and substance use in male veterans. Data were collected on male veterans who were receiving VA outpatient mental-health care. The authors found that 9.5% of the sample (880) reported a history of sexual assault and also reported increased alcohol consumption, increased alcohol-related consequences, and increased use of illicit substances (such as cannabis, cocaine, and opiates) in the preceding 90 days.
A study of substance use in veterans and VA service-connected disability benefits with risk of homelessness was conducted by Edens et al. (2011). The authors conducted a case– control study with VA administrative data from FY 2009 (1,120,424) and compared the data with those who had recently been homeless and those who had not been homeless. The authors used an ICD-10 diagnostic code indicating lack of housing to identify cases. The control group was a population of 1,011,368 veterans who did not receive VA homeless services or a code indicating homelessness. As a result of the analyses, with controlling for demographic and diagnostic factors, illicit-drug use remained the strongest predictor of homelessness, followed by pathologic gambling, alcohol-use disorders, personality disorders, being 40–49 years old, and being black.
Summary
Recent studies have confirmed evidence of an association between deployment to a war zone and alcohol and drug abuse and dependence. The risk of abuse and dependence increased
with greater number of deployments, length of deployment, rate of exposure to the threat of death or injury, and exposure to atrocities. Deployment to OEF or OIF also increased the likelihood of depression and substance-use disorders; the greatest effect was observed in the Army and Marine Corps.
Findings from the 2008 DOD HRBS (Bray et al., 2009b) indicated that military rates of alcohol use are higher than in civilians 18–35 years old but lower than in civilians 46–64 years old. Heavy alcohol use was higher in personnel who had been deployed to any operational theater than in nondeployed personnel. Younger members and members of the Air Force, Marine Corps, and National Guard higher rates of alcohol misuse. Trends show increases in prescriptiondrug misuse, heavy alcohol use, stress, PTSD, and suicide attempts; deployment exacerbated some of these behavior changes. Findings also indicated that the proportion of active-duty military personnel reporting misuse of prescription drugs (12%) is more than twice that in the civilian population (4.4%) 18–65 years old. Similarly, 13.1% of women in the military report prescription-drug abuse compared with 3.2% of civilian women (Office of National Drug Control Policy, 2010). Many active-duty personnel do not actively seek treatment for substanceuse disorders; barriers to reporting and treatment include stigma, concern about effects on military career, and the perceptions of commanders, units, and peers.
Studies of veterans reported higher rates of any alcohol use and heavy alcohol use than in comparable nonveterans. Recent studies of OEF and OIF veterans found that 13.9% screened positive for PTSD, 39% for probable alcohol abuse, and 3% for probable drug abuse (Eisen et al., 2012). Quarterly analysis of OEF and OIF veterans examined in VA health care facilities found that 6.2% had diagnoses of alcohol-dependence syndrome, 4.4% nondependent abuse of drugs, and 3.29% drug dependence.
Risk factors for alcohol abuse include lower age, deployment to OEF or OIF, non-activeduty status before deployment, more general stress, exposure to atrocities, exposure to the threat of death or injury, cumulative length of deployment, and high frequency of deployment.
Numerous studies have documented the epidemiology of comorbid SUDs and other mental-health conditions in OEF and OIF veterans. The comorbid conditions include anxiety disorders, PTSD (McDevitt-Murphy et al., 2010; Nazarian et al., 2012; Seal et al., 2008, 2011; Stecker et al., 2010), and depression (Seal et al., 2011; Shen et al., 2012; Stecker et al., 2010). Studies of suicide in veterans have found that mental-health disorders are often comorbid with SUDs and increase the risk of suicide. Studies of veterans who have used VA health care services have found that veterans who have alcohol-use disorder, drug-use disorder, or both also had at least one comorbid mental-health diagnosis (PTSD, depression, anxiety, or adjustment disorder). Other comorbidities reported were sleep problems and pain.
Alcohol abuse is a predictor of domestic violence (Bell et al., 2006). In Army populations, 96% of abusers were using alcohol during the violent events. Alcohol abuse was also associated with poor job performance, productivity loss, and criminal-justice problems (Stahre et al., 2009). Service members have experienced increased rates of acute anxiety disorders, PTSD, sleep disorders, depression, substance-abuse disorders, and chronic pain. Concerns have been raised about the safety and effectiveness of prescription-medication practices for those disorders. In recent studies, prescription-drug misuse has been identified as an important problem in military personnel and veterans who served in OEF or OIF.
The committee focused on suicidal ideation because it was directed to examine outcomes and treatments related to the mental health issues of concern. As there are no long-term outcomes of suicide (at least for the decedent) and no treatments for suicide, the committee examined the long-term outcomes and treatments (Chapter 5) for suicidal ideation.
Suicide is a lethal self-inflicted action, a suicide attempt is a nonfatal action, and suicidal ideation consists of suicidal thoughts, such as wishing to commit suicide (see Chapter 5). The suicide literature focuses primarily on studies of risk factors for suicide; long-term outcomes of suicide attempts or suicidal ideation have not been systematically studied. It is difficult to determine the percentage of people who have suicidal ideation that go on to attempt or complete suicide. However, a recent study of suicidal ideation and suicide attempts in a large number (52,780) of active-duty members of the US Air Force found that 3% of the male and 5.2% of the female study participants reported suicidal ideation in the previous year, and 8.7% of those who reported suicidal ideation also reported a recent suicide attempt (Snarr et al., 2010).
CDC has reported that in 2009, the rate of suicide in the general population was 16.25 per 100,000 in people 25–64 years old (CDC, 2012). That recent analysis indicates that there were about 36,500 suicides. In 2009, suicide was the tenth-leading cause of death in the US population. Prevalence estimates of suicidal thoughts and behaviors indicate that during 2008– 2009, an estimated 8.3 million adults in the United States reported having suicidal thoughts in the preceding year, and 2.9 million of them were 18–29 years old (CDC, 2011a).
At the beginning of the chapter, the committee notes numerous limitations of the studies it reviewed and makes a recommendation to address its concern. Although the committee has noted those limitations generally, it highlights some of them as they related to studies on suicide and suicidal ideation. Some findings are from studies of self-reported data (e.g., Jakupcak et al., 2010b, Snarr et al., 2010); others are based on VHA data, which only include veterans enrolled in VHA (McCarthy et al., 2012); the Kaplan et al. study (2012) is based on data extracted from the National Violent Death Reporting System (NVDRS). Currently only 16 states contribute data to NVDRS, which might not be representative of the veteran population.
Suicide Rates in the Military
Historically, suicide rates in the military have been lower than those in the civilian population. However, suicide in US military personnel has recently been of increasing concern. In 2009, the suicide rate in active-duty service members was 18.3 per 100,000, the highest rate since 2008. DOD confirmed about 2,000 suicides from 2003 to 2010, of which 300 occurred during deployment. In 2010, 50% of suicides occurred in active-duty personnel who had deployed to OEF or OIF; higher rates of suicide were found in the Army and Marine Corps than in other branches of the military (CBO, 2012). The Department of Defense Suicide Event Report (DCoE, 2011) summarized suicides and suicide attempts and relied on the Armed Forces Medical Examiner System (AFMES) for its data. In 2010, the AFMES provided data indicating that 295 service members committed suicide. Demographic data indicate that risk factors for suicide include being male, white, under the age of 25 years, junior enlisted or high-school educated, and divorced (the suicide rate in divorced service members was 55% higher than that in married service members). Active-duty service members had a 70% higher risk of suicide than
did deployed reserves and National Guard members. Firearms accounted for 62% of all suicides, and drug overdose was the most frequent method of suicide attempts (57%).
Some 57% of suicides were completed by persons who did not have a known history of suicide attempt or suicidal ideation, but 17% were known to have a mood disorder, specifically major depressive disorder (7%), 5% had an anxiety disorder (most frequently PTSD), and about 26% had a history of substance-use disorder (DCoE, 2011).
According to the Armed Forces Health Surveillance Center (AFHSC), suicide was the third-leading cause of death in US service members. The number of suicides in US military deployed to Iraq and Afghanistan has increased, and the estimated suicide rate in the Army almost doubled from 2004 to 2008 (from 10.8 to 20.2 per 100,000) and is now higher than that in the civilian population (Trofimovich et al., 2012). More recently, the AFHSC examined mortality data on 1998–2011 and found that since 2010 suicide has become the second-leading cause of death in service members. There were 2,990 suicides in 1998–2011 in active-duty members. The most common method of suicide in males and females was the use of firearms (AFHSC, 2012).
The AFHSC examined health care experiences that preceded suicide in US service members in January 2001–December 2010 (Trofimovich et al., 2012). Death and medical records maintained in the Defense Medical Surveillance System and the DOD Medical Mortality Registry (MMR) were used to indentify three retrospective cohorts: a suicide cohort, a selfinflicted injury cohort, and a likely self-harm cohort. During 2001–2010, 1,939 service members completed suicide, 19,955 had diagnoses of self-inflicted injuries, and 3,463 were hospitalized for likely self-harm. Among the three cohorts, the type of health care that was accessed in the month before the “event” was primary care. Specifically, 45% of those who died of suicide, 73% of those who had self-inflicted injuries, and 76% of the likely self-harm cohort had outpatient visits within 30 days before their cohort-defining events. The authors speculated that there might be “triggering” events that lead to seeking health care and that people might be screened for suicide risk in primary care (Trofimovich et al., 2012).
Risk Factors for Suicide in Active-Duty US Military Personnel
A study conducted by Bell et al. (2010) examined death, inpatient, and emergency-room records on 1,873 Army suicides and compared them with records on 5,619 matched controls. Their analysis revealed several risk factors for suicide, including being older, being male, being white, being single, having enlisted with a prior injury, having alcohol abuse, and having had a mental-health hospitalization. The authors noted that the risk was greatest after a mental-health diagnosis but remained high for 5 years or more.
In 2011, RAND completed a study of suicide prevention in the US military. A review of the scientific literature indicated that those at risk for suicide were in several broad categories: prior suicide attempt; mental-health disorders, specifically depression and anxiety disorders, including PTSD; known SUDs; TBI (concussion, cranial fractures, cerebral contusions, or traumatic intracranial hemorrhages); feelings of hopelessness, aggression, and impulsivity; and problem-solving deficits (Ramchand et al., 2011).
A study by Black et al. (2011) examined prevalence and risk factors associated with suicides in the US Army from 2001 to 2009. Data were selected from the Army Behavioral Health Integrated Data Environment, and 874 suicides in Army soldiers were examined. The
data included information on sociocultural and military risk factors, psychologic and environmental risk factors, and suicide-event characteristics. The data were compared with available data on Army personnel over the same period. Findings indicated that suicide rates doubled from 9.0 per 100,000 in 2001 to 22 per 100,000 in 2009 in all Army components (active duty, reserves, and National Guard). About 75% of suicides occurred in the United States, 20% occurred in the combat theater of operations, and the remainder occurred elsewhere. An overwhelming increase in suicide rates was observed from 2005 to 2009. The authors speculated that it might be associated with deployments to OEF and OIF. The most common method of suicide involved firearms (a finding common to all studies reviewed). Their findings are also consistent with those of other studies in that the relative risk of committing suicide is higher in men than in women, blacks are at lower risk for suicide than whites, junior enlisted committed suicide more often than senior enlisted and officers, and those deployed to OEF or OIF were at greater risk than those never deployed. In addition, 46% of those who committed suicide had a mental-health diagnosis, and 79% had personal stressors, most commonly involving relationship problems, military or work-related stress, and health issues (Black et al., 2011).
Having examined medical records, mental-health diagnoses, mental-health visits, prescriptions for anxiety and depression, and deployments to OEF and OIF, Hyman et al. (2012) determined risk factors for suicide in active-duty members during 2005 or 2007. The 2005 cohort consisted of 2,064,183, and the 2007 cohort 1,981,810. Study variables other than deployment and suicide were based on events that occurred in 2004 and 2005 for the 2005 cohort and in 2006 and 2007 for the 2007 cohort. The authors found that suicide rates increased in all services from the 2005 cohort to the 2007 cohort. Risk factors included mental-health diagnosis (especially PTSD and depression, previous suicide attempts, and suicidal ideation), prescriptions for selective serotonin reuptake inhibitors (commonly prescribed for depression or anxiety), use of sleep medications, reduction in rank, separation or divorce, and deployment to OEF or OIF. During deployments through 2005, suicide risk factors included being in the Army, particularly the National Guard and the Army reserves; in 2007, increases in suicide were experienced in all the services.
Skopp et al. (2012) conducted a study of active-duty members who served in the US military during 2001–2009. Suicide cases (1,764) according to the DOD MMR maintained by the Office of the Armed Forces Medical Examiner were included if they had been officially declared suicides. Controls (7,018) were randomly selected and matched by service, sex, age, race, entry into active component, and within 1 year of total active-duty service. The number of OEF or OIF deployment was studied as a potential risk factor. Military Health System records were reviewed (according to ICD-9-CM codes) for psychiatric diagnoses and partner-relationship and family problems. The standard DOD surveillance case definition was used to determine TBI status. With regard to demographic characteristics of the study population, 96% were male; about 43% were Army, 20% Air Force, and 17% Navy; and 72% were younger than 25 years old. The authors found suicide attempts were associated with mood disorders and partner and family problems. Psychiatric comorbidities were associated with increased risk for suicide.
Logan et al. (2012) obtained data on active-duty Army soldiers who committed suicide during 2005–2007. Using the CDC National Violent Death Reporting System and the DODSER, they were able to characterize the decedents. They found that the decedents were overwhelmingly male, white, less than 30 years old, married, and enlisted personnel. The circumstances preceding the suicides were health-related and stress-related and included
intimate-partner problems (45%) and military-related stress (41%), such as job problems and combat experiences. The decedents had shown symptoms of mental-health problems (32% were identified as having a depressed mood). Family members, friends, co-workers, and clinicians described the decedents as sad, depressed, or suicidal (36% had communicated their intent to harm themselves).
There is a great deal of agreement in the numerous studies of risk factors for suicide in the military, particularly in OEF and OIF active-duty personnel. As suicide rates have increased, many researchers have sought to provide information to identify those at risk for suicide so that treatments might be offered and prevention strategies developed.
Suicide Rates and Risks in Veteran Populations
A review in the Annals of the New York Academy of Sciences examined the available data on risk and rates of suicide in veterans served by VA. Although the review examined all veterans, the report noted that the data were most complete for OEF and OIF veterans. Findings indicated that there was a lower risk of all-causes mortality in veterans than in the general population, but OEF and OIF veterans and the general population were at equal risk for suicide, and the findings varied little with the branch of the military. The author highlighted risk factors for suicide in the OEF and OIF veteran population: higher age, prolonged combat or injury, and having a diagnosis of TBI or a psychiatric disorder, such as PTSD. The author noted that evidence in the reports reviewed suggested that OEF and OIF veterans might have fewer psychologic and social resources that might have served as protective factors (Bruce, 2010). An earlier review by Kang and Bullman (2009) examined suicides in veteran populations and found that being a former OEF or OIF active-duty veteran and having a select mental disorder resulted in a suicide risk higher than that in the general population.
It should be noted, however, that there is a paucity of data on the entire veteran population of the United States. The VA provides data for veterans enrolled in its health care and benefits systems. Those veterans are often older and sicker than the general US population; that is particularly true for veterans seen at the VA for psychosocial and mental-health problems.
Jakupcak et al. (2010b) examined PTSD as a moderating variable in the relationship between social support and suicide risk in treatment-seeking OEF and OIF veterans. Using a self-completed questionnaire, the authors assessed suicide risk in 431 OEF and OIF veterans referred for VA mental-health services. The veterans were mostly men (88.9%) and had an average age of 32.4 years; about 67% were white, and 55.5% were not married. The researchers found that PTSD was related to increased suicide risk and that married veterans and those satisfied with social networks were less likely than unmarried veterans to be at high risk for suicide. The authors noted that the presence of PTSD might diminish the protective effect of social networks.
Studies that included an examination of risk factors for suicide in all populations of veterans found that rural residence (McCarthy et al., 2012); poor mental health, substance abuse, adverse life events (related to financial matters, health, criminal problems, and so on) (Kaplan et al., 2012); and TBI (Brenner et al., 2011) were associated with greater suicide risk.
Risk Factors for Suicidal Ideation in Active-Duty and Veteran Populations
Several recent studies have evaluated risk factors for suicidal ideation in OEF and OIF active-duty or veteran populations.
Active-Duty Personnel
Suicidal ideation and suicide attempts were assessed in a sample of US Air Force activeduty members by Snarr et al. (2010). They assessed suicidality during the year before participation in the study at 82 US Air Force sites worldwide. It was not noted in the study whether or what percentage of the sample were deployed to OEF or OIF. The final sample included 52,780 participants who logged on to the survey and completed it. The 1-year prevalence of suicidal ideation in the sample was 3.3% in men and 5.5% in women (according to Substance Abuse and Mental Health Services Administration, comparable 2009 civilian rates were 3.4% in men and 3.9% in women). Risk factors for suicidal ideation in the sample of women included lower rank and being non-Christian; risk factors in men included not being married, being non-Christian, being junior enlisted, and an occupation of medical personnel. The authors noted that suicidal ideation and suicide attempts are more common than completed suicides in the Air Force. They suggested that identifying risk factors would assist public-health officials in targeting vulnerable groups with suicide-prevention programs.
Using the same sample as above, Langhinrichsen-Rohling et al. (2011) conducted a study of four factors and their association with suicidal ideation: individual, family, workplace, and community. Active-duty members sampled from 82 Air Force bases worldwide were invited to complete an anonymous survey, the 2006 Community Assessment. The analysis reveals that depression was the strongest predictor of suicidal ideation in both sexes. Additional risk factors in men were personal coping ability, physical well-being, alcohol problems, relationship satisfaction, interpersonal violence, dissatisfaction with the Air Force as a way of life, number of hours worked, community unity, and social support. Additional risk factors in women were financial stress, alcohol problems, relationship satisfaction, interpersonal violence, workplace satisfaction, hours worked, and social support. The authors suggested that the military develop prevention and early-intervention programs.
Using the DOD Survey of Health-Related Behaviors, which collects population-based data from reserve and active-duty forces, Lane et al. (2012) examined stress levels and mental-health status. People who participated in the survey included those who served in OEF or OIF, those who served in a different theater of operations (that is, not OEF or OIF), and those who did not served in theater. Data on the 2006 reserve component and the 2005 active-duty component of the surveys were analyzed and results revealed notable differences between reservists and active-duty personnel. For example, reservists who were deployed were more likely to report suicidal ideation and suicide attempts than those who were not deployed; active-duty personnel showed no differences in reports of suicidal ideation between deployed and nondeployed. Reservists deployed to OEF or OIF were more likely to report suicidal ideation and suicide attempts than reservists who served in other theaters or who were not deployed. Reservists reported mental-health issues related to deployment, especially more severe PTSD symptoms than the other groups, although all deployed personnel (reservists and active-duty) had higher rates of positive screening for PTSD. Deployment was also associated with perceived family and
work stress, particularly in active-duty personnel; a greater percentage of deployed active-duty personnel and reservists than of nondeployed personnel reported depression symptoms.
Veterans
Jakupcak et al. (2009) examined PTSD as a risk factor for suicidal ideation. A sample of 435 OEF and OIF veterans who were consecutively referred and assessed for mental-health services at a VA facility (VA Puget Sound Health Care System) in 2004–2007 were screened for PTSD symptoms and suicidal ideation with self-report screening methods. Veterans who had suicidal ideation (187) and veterans who did not (220) were compared on sociodemographic variables (such as sex, age, race or ethnicity, years of education, and marital status). PTSD was significantly associated with suicidal ideation (after accounting for age, depression, and substance abuse); in fact, veterans with who screened positive for PTSD were 4 times more likely than veterans who did not to report suicidal ideation, and the likelihood of suicidal ideation was 5.7 times greater in veterans who screened positive for PTSD and two or more comorbid disorders.
In a later study, Jakupcak et al. (2011) examined the association between PTSD symptoms and suicidal ideation in OEF and OIF veterans. Participants included 336 veterans who were assessed at the VA Puget Sound Health Clinic from May 3, 2004, to January 1, 2007. The final sample of 275 veterans was included in the study after removal of those who did not complete the self-report assessments or on whom information on key variables was missing. Analyses indicated that veterans who had subthreshold PTSD were more likely than veterans who did not have PTSD to express hopelessness or suicidal ideation. Those reporting hopelessness or suicidal ideation had poorer social support, higher levels of combat exposure, lower income, depression, and alcohol abuse. Depression, followed by PTSD, was the strongest correlate of hopelessness and suicidal ideation. The authors noted that people who had subthreshold PTSD might not be able to receive mental-health treatment, so there is a need to educate providers to address symptoms of PTSD to mitigate suicide risk.
Pietrzak et al. (2010) analyzed results of a survey of OEF and OIF veterans and found that those veterans contemplating suicide were more likely to screen positive for PTSD, depression, and an alcohol problem and scored lower on measures of resilience and social support. They also scored higher on measures of stigma, barriers to care, and psychosocial difficulties. The study identified 1,050 OEF and OIF veterans from Connecticut, but only 272 veterans returned the survey (a response rate of 26%).
Pietrzak et al. (2011a) studied suicidal ideation in treatment-seeking OEF and OIF veterans. Veterans were recruited from VA primary care and mental-health clinics; 80% of veterans who were approached completed the assessments on site. In all, 167 OEF and OIF veterans who were within a year of returning from their most recent deployment participated. The authors found that almost 22% of treatment-seeking OEF and OIF veterans contemplated suicide; compared with those who did not, those who contemplated suicide were older and more likely to screen positive for depression, PTSD, and deployment-related pain. They were also more likely to score low on measures of psychologic resilience and social support.
In 2011, Kline et al. (2011) examined suicidal ideation in National Guard troops deployed to OIF. Survey data for the study were obtained from 1,665 (of 1,723) New Jersey National Guard soldiers attending a 3-month postdeployment reintegration event after
deployment to Iraq in 2008–2009. The group had an average age of 31.3 years, were 89.5% male, and 45.9% white, 29.1% Hispanic, and 16.9% black. About 70% had some college experience; 52.5% had full-time employment, and 47.5% had part-time employment or were unemployed; 43.2% were married, 45.4% had never married, and 11.4% were separated, widowed, or divorced. Screening criteria were met in 5.6% for depression, in 10.8% for PTSD, 12.6% for alcohol dependence, and 13.2% for illicit-drug use. The group of respondents had low combat exposure—specifically, 33% reported no combat exposure, 47.7% low exposure, and 19.2% high exposure. The authors found that readjustment stressors correlated with psychiatric disorders and were more strongly associated with suicidal ideation than were the psychiatric disorders reported. After adjustment for the mental-health disorders, veterans who had readjustment problems were at 5.5 times greater risk for suicidal ideation than were those who did not.
Lemaire and Graham (2011) conducted a retrospective chart review of 1,740 veterans’ initial health screens after return from OEF or OIF to determine factors associated with suicidal ideation. The review highlighted 113 (6.5%) who reported suicidal ideation and identified a number of risk factors: physical- or sexual-abuse exposure, prior suicide attempts, female sex, and a diagnosis of a mental-health disorder, such as psychosis, depression, or PTSD. Comorbid PTSD and depression were associated with higher risk than PTSD or depression alone.
Maguen et al. (2011a) examined risk factors for suicidal ideation in 2,854 US soldiers returning from deployment in OIF. Data on the newly returning veterans were collected as part of a postdeployment screen at a large Army medical facility, and 2.8% of them reported suicidal ideation. It was noted that prior suicide attempts, prior psychiatric medication, and killing in combat were risk factors for suicidal ideation. Findings indicated that returning veterans who endorsed depression symptoms were at greatest risk.
Guerra and Calhoun (2011) examined the relationship between PTSD and suicidal ideation in a group of veterans who had been deployed to OEF or OIF. Participants included veterans who had served in the armed forces after September 11, 2001, and were recruited into a registry from June 2005 to August 2008. Participants (393) were administered structural clinical interviews for psychiatric disorders. They were primarily male (322) and were primarily white (186), and their average age was 38.3 years. Results showed that 36% of the sample (143) met the criteria for PTSD, 22% (88) met the criteria for major depressive disorder, 4% (17) met the criteria for alcohol-use disorder, and almost 9% (34) reported a prior suicide attempt. The authors found that prior suicide attempt was positively associated with suicidal ideation; PTSD was related to heightened suicidal ideation even in the absence of major depressive disorder or alcohol-use disorder. The authors advise clinicians treating patients who have PTSD to assess them regularly for suicidality.
Summary
Suicide in US military personnel is increasingly of concern, and suicidal ideation, suicide attempts, and suicide are increasingly associated with modern military service. In 2010, 50% of suicides in military personnel occurred in active-duty personnel who had been deployed to OEF or OIF; higher rates of suicide were found in the Army and Marine Corps than in other branches of the military (CBO, 2012). The AFHSC examined mortality data for 1998–2011 and found that since 2010 suicide has become the second-leading cause of death in service members. There
were 2,990 suicides during 1998–2011 in active-duty members. The most common method of suicide among males and females was through the use of firearms (AFHSC, 2012).
Demographic data highlight risk factors for suicide, including being male, being white, being under 25 years old, being junior enlisted or high-school educated, and being divorced (the suicide rate was 55% higher in divorced service members than in married service members). Active-duty service members had a 70% higher rate of suicide than did deployed reserve and National Guard personnel. Firearms accounted for 62% of all suicides, and drug overdose was the most frequent method for suicide attempts (57%).
Reservists who were deployed were more likely to report suicidal ideation and suicide attempts than those who were not deployed. Reservists deployed to OEF or OIF were more likely to report suicidal ideation and suicide attempts than were reservists who served in other theaters or who were not deployed.
Veterans who screened positive for PTSD were 4 times more likely to report suicidal ideation than veterans who did not, and the likelihood of suicidal ideation was 5.7 times greater in veterans who screened positive for PTSD and two or more comorbid disorders. Those reporting hopelessness or suicidal ideation had poorer social support and higher levels of combat exposure. Additionally, veterans with lower income, depression, and reported alcohol abuse were more likely to endorse feelings of hopelessness and suicidal ideation. Depression was the strongest correlate of hopelessness and suicidal ideation, followed by PTSD.
Some risk factors might be mitigated or prevented, but others, such as deployment and combat exposure, are difficult to prevent in a military population.
In the military population, 57% of the suicides occurred in people who had no known history of suicide attempts or suicidal ideation, but 17% of those who committed suicide were known to have had a mood disorder, specifically major depressive disorder (7%), 5% had an anxiety disorder (most frequently PTSD), and about 26% had a history of substance-use disorder (DCoE, 2011).
WOMEN’S HEALTH OUTCOMES
Women have served in operational support roles in every US military operation since the Revolutionary War. Mary Edwards Walker, a physician and surgeon, was denied a commission as a medical officer in the Civil War but volunteered and served as the first female surgeon in the US Army. She was the only woman to be awarded the Congressional Medal of Honor for military service. Today, women make up a rapidly growing segment of the military population.
They make up about 14% of all active-duty military and 17.6% of National Guard and reserve personnel, and about 12% of women veterans served in OEF, OIF, or OND.12 The recent military operations in Iraq and Afghanistan are the most sustained ground combat operations involving American forces since the Vietnam era, and although women are still barred from direct combat roles, they have served in those theaters in expanded roles and in greater numbers (Fontana and Rosenheck, 2008). Women in combat-support roles, like the men they serve beside, experience high-intensity asymmetric warfare and the constant threat of
__________________
12See http://www.womenshealth.va.gov/WOMENSHEALTH/facts.asp.
roadside bombs and other types of improvised explosive devices. For almost a decade, military personnel have been subject to repeated deployments and endured prolonged separation from families and loved ones and exposure to harsh wartime conditions, including witnessing or experiencing traumatic injuries and deaths of civilians and military forces. Asymmetric warfare produces combat exposures that result in continuous stress and a frontless war in which no location or military occupation can be considered without risk. Historically, research on the health of veterans has focused on the health consequences of combat service in men, and there has been little scientific research on or longitudinal study of the health consequences of military service in women who served. Research that has examined sex differences is generally mixed, and a recent review (Street et al., 2009) highlighted the need to conduct studies with larger samples of women to improve understanding of issues relevant specifically to women. This section highlights studies that have investigated sex differences or issues particularly relevant to women.
Women and Traumatic Brain Injury
TBI has important health implications for readjustment after deployment to Iraq or Afghanistan, but little information is available on whether the outcomes of patients suffering from TBI are affected by sex. One study suggested that sex differences may affect cognitive recovery after TBI. Ratcliff et al. (2007), in a multicenter civilian cohort study of 325 adult patients who had blunt TBI and were admitted to an acute-care facility, found that women performed significantly better than men on tests of attention or working memory and language. However, men outperformed women in visual analytic skills. Sex remained significantly associated with performance in those characteristics even after control for demographic variables, severity of injury, history of drug abuse, and length of acute hospitalization and of inpatient rehabilitation. The authors noted that further studies are needed to control for possible preinjury sex-related differences and to determine the long-term impact and health outcomes.
Slewa-Younan et al. (2008) conducted a systematic qualitative literature review and identified 13 human studies that examined sex differences in functional outcome measures after moderate to severe TBI. Contrary to findings in animal studies, results of human studies do not indicate that women do better than men after moderate to severe TBI. However, the authors noted that the studies examined functional outcomes 3–18 months after injury and that women may do better in the longer term in which psychosocial factors may play a role.
Iverson et al. (2011) investigated sex differences in psychiatric and neurobehavioral outcomes of deployment-related mild TBI in 11,951 male and 654 female OIF and OEF veterans who were using VA health care services. They reviewed records of VA’s standardized comprehensive TBI evaluation and found that men had significantly greater odds of receiving diagnoses of PTSD and SUDs but women had significantly greater odds of receiving diagnoses of depression (2 times greater), anxiety disorders other than PTSD (1.3 times greater), and comorbid PTSD and depression (1.5 times greater). Severity of neurobehavioral symptoms in several domains was significantly higher in women than in men; women were more likely to report “severe” or “very severe” cognitive, somatosensory, and vestibular symptoms. Significant sex differences in PTSD disappeared after controlling for blast exposure. Depression in female military personnel or veterans is discussed further below.
Women and Mental-Health Disorders
Retrospective research studies have indicated that women who serve in the military suffer more mental-health problems than their male counterparts. Rundell (2006) reviewed records of 1,264 military personnel who had been evacuated from Iraq or Afghanistan for psychiatric reasons and found that the evacuees were more likely to be female. Wojcik et al. (2009) reviewed records of 473,964 Army soldiers who had served in Iraq or Afghanistan and found that 1,948 of them were hospitalized for a primary psychiatric diagnosis. Their analysis indicated that women were at significantly higher risk for mental disorders—including mood, adjustment, and anxiety disorders—and that young women (less than 30 years old) made up a group at high risk for attempted suicide or self-inflicted injuries. Zouris et al. (2008) reviewed hospitalization records of OIF Marine Corps and Army personnel and found that a higher percentage of women than of men had diagnoses of mental-health disorders. Gibbons et al. (2012) evaluated data from the 2005 DOD Survey of Health Related Behaviors on 265 male and 180 female active-duty health care providers who had been deployed to OEF or OIF and found that female enlisted personnel and officers were more likely than their male counterparts to screen positive for serious psychologic distress, generalized anxiety disorder, depression, and harmful drinking habits. In a small study of female veterans who used VA health care services, Grubaugh et al. (2006) found that female veterans appeared to suffer worse mental (and physical) health than the general population. Overall, the research raises substantial concerns about the mental-health consequences of combat deployment of women.
The following subsections focus mainly on two mental-health outcomes, PTSD and depression, that are of particular concern for women who are on active duty and for female veterans.
Posttraumatic Stress Disorder
Regarding sex differences, three questions that are relevant to PTSD arise: Does prevalence differ between women and men? Do the type and frequency of risk factors differ between women and men? Do outcomes as a consequence of combat deployments differ between women and men? Studies of the general population have indicated that women have higher rates or greater prevalence of PTSD than men (Breslau, 2002; Holbrook et al., 2002; Pietrzak et al., 2012; Tolin and Foa, 2006). However, the findings are mixed in OEF and OIF military personnel or veterans. A telephone survey of 1,965 veterans who had been deployed to Iraq or Afghanistan found that female veterans had a significantly higher risk of self-reported PTSD (and depression) than male veterans (Tanielian and Jaycox, 2008). Luxton et al. (2010) evaluated screening data collected on 6,427 male and 516 female active-duty soldiers at a single large Army installation before and after deployment to OEF or OIF and found that women who reported higher levels of combat exposure were more likely to report PTSD (and depression) symptoms than men. The authors concluded that combat exposure was a strong predictor of PTSD and depression in women and that there were sex-based differences in risks.
In contrast, other research has not found that women have a higher risk of PTSD than men. Baker et al. (2009) reviewed self-report data on 302 male and 37 female OEF and OIF veterans or reservists who were enrolled in the VA health care system and did not find any significant relationship between PTSD and sex. Haskell et al. (2009) reviewed VA data on 134,731 male and 18,481 female OEF and OIF veterans to evaluate possible sex differences in
the prevalence and characteristics of pain. PTSD was more common in men than in women (11.3% vs 9.9%) whereas depression was more common in women (12.2% vs 7.5%). Later, Haskell et al. (2010) reviewed screening data from electronic medical records of 1,032 male and 197 female OEF and OIF veterans who used VA health care services and found that women were significantly less likely than men to screen positive for PTSD but significantly more likely to screen positive for depression. Maguen et al. (2010) reviewed VA administrative data on 288,348 male and 40,701 female OEF and OIF veterans who were seeking treatment and found that men were older than women and more often diagnosed with PTSD and alcohol abuse whereas women were more likely to be black and were more often diagnosed with depression than men. Women older than 30 years old were significantly more likely to receive diagnoses of PTSD than younger women; an opposite trend was observed in men, that is, younger men had a greater risk of PTSD than older men. Similar research on active-duty service members supports the study findings in the OEF and OIF veteran population. Maguen et al. (2011b) reviewed screening data on 6,697 male and 554 female active-duty soldiers collected before and after deployment to Iraq or Afghanistan. Men were more likely than women to report high-intensity combat exposure, but there were no sex differences in PTSD symptoms. However, the study did find that men were more likely than women to screen positive for alcohol abuse whereas women were more likely to screen positive for depression. Reviewing the literature, Zinzow et al. (2007) concluded that although the PTSD rates in the civilian population appear to be higher in women than in men, findings in the veteran population are mixed, and there is a general indication that the rates may be similar in men and women or higher in men than women.
Another question relevant to the development of PTSD in women is whether they suffered traumatic events before joining the military or have experienced MST, which would place them at higher risk for PTSD. Female military personnel and female veterans have high rates of sexual assault, particularly in comparison with men (Haskell et al., 2010; Maguen et al., 2011b; Murdoch et al., 2007). In a literature review, Zinzow et al. (2007) examined the nature and prevalence of trauma in female veterans, its effect on their physical and mental health, and their use of medical services. The authors found that over 50% of women who enter military service have already experienced physical or sexual abuse. A wide range of estimates of MST have been reported, but the authors estimated a range of 30–45%. The wide range of estimates was attributed to the various ways in which sexual assault was defined in the studies. For example, the authors estimated the lifetime rate of sexual assault as 38–64%, noted that nearly all female veterans report some type of trauma at some point in their lives (81–93% any type of trauma, 38–64% lifetime sexual assault, 27–49% child sexual abuse, 46–51% physical assault, 35% child physical abuse, and 18–19% domestic violence), and note that the rates are much higher in female veterans than in the civilian population.
The high rates of MST are particularly troubling given recent research that has shown strong correlations between MST and PTSD. Suris et al. (2004) conducted a retrospective evaluation of the effect of military, civilian adult, and childhood sexual trauma and the risk of PTSD in 270 female veterans who were using a single VA health care facility. The authors conducted structured interviews and reviewed medical records and found that veterans who reported MST were 9 times more likely than veterans who had no history of sexual assault to receive a diagnosis of PTSD, veterans who reported childhood sexual assault were 7 times more likely, and veterans who reported civilian sexual assault were 5 times more likely to receive a diagnosis of PTSD than veterans who did not have a history of sexual assault. The study suggests a worse PTSD outcome after MST than after civilian assault. Himmelfarb et al. (2006) reviewed
responses to questionnaires and interviews of 196 female veterans to evaluate the relationship between sexual trauma and PTSD. The authors found that MST was much more prevalent than sexual trauma before or after military service (41% vs 19% or 24%, respectively) and that women who reported MST had the greatest odds of receiving a diagnosis of PTSD.
As discussed earlier, Kimerling et al. (2010) reviewed electronic medical records of 108,149 male and 17,580 female OEF and OIF veterans who were using VA health care services to evaluate the relationship between MST and mental-health diagnoses.13 The authors adjusted for demographic factors and other potential confounders and found that victims of MST were significantly more likely to have received a PTSD diagnosis and to have other mental-health disorders, including depression, other anxiety disorders, and SUDs. Because the positive relationship between MST and PTSD was substantially greater in women than in men, the authors suggested that “military sexual trauma may be a particularly relevant gender-specific clinical issue in PTSD treatment settings.”
Maguen et al. (2011b) reviewed screening data on 6,697 male and 554 female active-duty soldiers collected before and after deployment to Iraq or Afghanistan and found that women reported MST more frequently than men (12% vs over 1%) and that MST was a significant predictor of PTSD (and depression) symptoms. Coincidentally, the authors also noted that women were experiencing higher rates of combat exposure than expected. In a later study, Maguen et al. (2012) assessed the effects of MST on comorbid mental-health disorders in 7,255 female and 67,238 male OEF and OIF veterans who had PTSD. They reviewed administrative data and medical records and found that MST increased odds of a PTSD diagnosis by 3 and 4 in men and women, respectively; that 31% of women and 1% of men who had PTSD reported MST; and that men and women who had PTSD and a history of MST had significantly more mental-health comorbidities than veterans who had PTSD and no history of MST. Female victims had significantly higher odds of having a diagnosis of depression, anxiety, or eating disorders than male counterparts, whereas male victims had significantly higher odds of SUDs than female counterparts.
Dutra et al. (2011) evaluated the effects of combat experiences and military sexual harassment on PTSD and depression. The authors reviewed screening data collected within 3 months after deployment to Iraq on 54 active-duty female military personnel and found that about 74% reported combat experiences, over 50% reported having experienced sexual harassment during deployment, and 11% screened positive for PTSD; regression analyses indicated that military sexual harassment was a unique predictor of PTSD symptoms. In fact, the authors concluded that MST might be more strongly associated with PTSD in women than combat exposure, a known risk factor for PTSD, and noted that their findings were consistent with those of previous studies that highlighted MST as a “factor of particular clinical importance for the female military population.”
The committee notes that although MST is much more common in women and therefore is particularly relevant for female military personnel and veterans, men appear to suffer similarly. Shipherd et al. (2009) investigated the relationship between MST and health and whether posttraumatic stress symptoms mediated the relationship. The authors reviewed self-report
__________________
13Kimerling et al. (2010) followed an earlier study (Kimerling et al., 2007) that evaluated the relationship between MST and mental and physical health in a large veteran population (134,894 women and 2,900,106 men) and that had results similar to those of the later study in the OEF and OIF veteran population.
data on 226 female and 91 male current or former marines who had reported MST in the previous 6 months and found that it was positively associated with increased posttraumatic stress symptoms in women and especially in men. Worse physical health was associated with higher levels of MST in men but with lower levels of MST in women.
Murdoch et al. (2007) reviewed cross-sectional survey questionnaire data on 487 male and 327 female active-duty military personnel to evaluate the relationship between sexual stressors and mental and physical functioning. Sexual stressors were defined as sexual-identity challenges (for example, accusations of homosexuality), sexual harassment, and sexual assault. The authors found that those who reported multiple stressors had more severe PTSD symptoms—and poorer physical, work, role, and social functioning; more sleep disorders; more severe depression; and more severe anxiety symptoms—than those who reported fewer or no stressors. Men and women in similar categories reported similar functioning and psychiatric symptoms.
As noted above, women have experienced higher levels of combat exposure than in previous conflicts (Dutra et al., 2011; Maguen et al., 2011b). That finding is troublesome because combat exposure is a known risk factor for PTSD and some have suggested that women may be more vulnerable to the effects of combat exposure than men. However, Vogt et al. (2011) reviewed survey and questionnaire data on 252 male and 340 female OEF and OIF veterans to determine whether there were significant sex differences in the effects of combat exposure and in mental-health outcomes, such as PTSD, depression, and substance abuse. As expected, men reported more exposure to combat-related stressors than women, and women reported more prior-life trauma and exposure to sexual harassment during deployment. Controlling for prior-life trauma and sexual harassment, the authors found only one statistically significant difference that suggested that men may be more likely to suffer substance abuse after exposure to combat. However, the effect was small and considered clinically insignificant. They concluded that the effects of combat-related stressors “may be more similar than different for female and male US service members” and that female OEF and OIF “service members may be as resilient to combat-related stress as men.” A study of UK military men and women (Woodhead et al., 2012) concluded similarly that their investigation showed “little evidence of gender differences in the impact of exposure to combat on mental health.”
Regardless of the similarity of response to combat exposure, the adverse effect on women is important to note. Hassija et al. (2012) investigated the differential effect of various types of trauma—combat exposure, childhood neglect and abuse, and adult sexual assault and noncombat physical violence—on mental-health disorders in 115 female veterans of the Persian Gulf, Iraq, and Afghanistan wars who had visited VA health clinics. The authors used regression analyses to evaluate questionnaire data and found that only combat exposure was significantly associated with more severe PTSD symptoms, depression-symptom severity, and alcohol misuse. The authors stated that they did not separate MST from the categories of adult traumatic events evaluated and noted that this distinction might be important given the particularly detrimental effects of MST that have been reported.
The burden of PTSD in women is of concern because, like men, women who have PTSD suffer worse physical and mental health and quality of life than those who do not have PTSD. For example, Frayne et al. (2004) evaluated the contribution of PTSD to poor physical health and functional status in female veterans who were using the VA health care system. They evaluated self-report data on 4,348 women who had PTSD, 7,580 women who had depression, and 18,937
women who had neither condition; 89% of the women who had PTSD also had depression. The authors found that women who had PTSD, regardless of age, had more medical conditions and worse functional status than women who had depression.
Because the research focus in the military setting has traditionally been on outcomes in men, the question arises whether women suffer different outcomes of PTSD than their male active-duty and veteran counterparts. Schnurr and Lunney (2008) evaluated possible sex differences in quality of life of veterans who had PTSD. The sample population consisted of 358 male Vietnam veterans and 203 female Vietnam veterans who were in group therapy or individual psychotherapy in a VA setting. PTSD was determined by using structured interviews, and quality of life was evaluated by using the Quality of Life Inventory, which assesses four domains (achievement, self-expression, relationships, and surroundings). As others had (Magruder et al., 2004; Suris et al., 2007), the authors found that veterans who had PTSD had poorer quality of life than those who did not, and they did not find clear differences between men and women who had PTSD. Although there were a few statistically significant differences, they were small and clinically insignificant. Frayne et al. (2011) investigated sex differences in the burden of medical illnesses by reviewing VA clinical and administrative data on 77,727 male and 12,831 female OEF and OIF veterans. They found that 27,083 men and 3,501 women had received diagnoses of PTSD and that women who had PTSD had a higher burden of diagnosed medical conditions than men. As expected, men and women who had PTSD had more medical conditions than their counterparts who did not. Lumbosacral spine disorders and lower extremity joint disorders were the most frequent conditions diagnosed in women and men who had PTSD. Headaches were also noted in women, and hearing problems in men. The results reported by Frayne et al. are consistent with those of a recent study of a civilian population (Galovski et al., 2011) that investigated sex differences in 45 men and 162 women who had PTSD that developed after sexual or physical assault. They found that men and women exhibited similar PTSD and depression symptoms and experienced similar guilt. However, women had significantly more health complaints, and men reported feeling more anger (as found with the anger-state scale of the State-Trait Anger Expression Inventory). The authors concluded that although civilian men and women may differ in the likelihood of developing PTSD after assaults, there are no differences in PTSD presentation once it is manifested.
Depression
Recent research appears to indicate that female OEF and OIF military personnel and veterans have a higher risk or greater prevalence of depression than their male counterparts. Many studies described above that investigated possible sex differences in PTSD also evaluated sex differences in depression. A study of 1,965 OEF and OIF veterans found that female veterans had a significantly higher risk of major depression than male veterans after control for confounding factors (Tanielian and Jaycox, 2008). Similarly, Seal et al. (2009), in their investigation of new mental-health diagnoses in 289,328 OEF and OIF veterans, found that women had a higher risk of depression than men. Haskell et al. (2009, 2010) consistently found that depression was more common in OEF and OIF female veterans than in their male counterparts. In their investigation of 6,943 active-duty soldiers who had been deployed to Iraq or Afghanistan, Luxton et al. (2010) found that women who had high combat exposure were more likely than men to report depression symptoms and concluded that there are sex-based differences in depression risks. Wells et al. (2010) found that women consistently had higher rates of new-onset depression than men in their investigation of the relationship between
deployment and the risk of depression. Carter-Visscher et al. (2010) found higher rates of depression in female National Guard soldiers than in their male counterparts on the basis of selfreport data collected before deployment to Iraq but did not find that sex moderated the relationship between various risk or resilience factors and baseline mental health. And Maguen et al. (2010, 2011b) found that female OEF and OIF active-duty soldiers and veterans were more likely than their male counterparts to receive a diagnosis of depression or to screen positive for depression. Thus, the evidence indicates that depression is a health issue that is particularly relevant to the female active-duty and veteran populations.
Depression is an especially relevant concern for women given the association of depression with MST and the high reported rates in female active-duty personnel and veterans. Hankin et al. (1999) reviewed questionnaire data on 3,632 female veterans and found that 23% reported military sexual assault. Furthermore, female victims of military sexual assault were significantly more likely than female veterans who had no history of such assault to screen positive for depression (60% vs 33%) and alcohol abuse (7% vs 4%). Suris et al. (2004) found that female veterans who had experienced military sexual assault had significantly higher rates of depressive-disorder diagnoses than veterans who had no history of such assault; the authors also noted that female veterans who had a history of civilian adult but not childhood sexual assault had significantly higher rates of depressive-disorder diagnoses than female veterans who had no history of such assault. Kimerling et al. (2010) found similar results specifically in OEF and OIF veterans; they reviewed electronic medical records of 108,149 male and 17,580 female OEF and OIF veterans and found that victims of MST were significantly more likely to have received diagnoses of depression.
Substance-Use Disorders
Few data are available for evaluating SUDs in female active-duty military personnel or veterans, and far fewer data are available specifically on the OEF and OIF female population. Where researchers have investigated sex differences, the results have appeared to indicate that women have significantly lower rates of alcohol abuse than their male counterparts. Bray et al. (1999) investigated the relationship between perceived stress and substance use during peacetime conditions by using questionnaire data on 16,193 active-duty military personnel obtained from the 1995 DOD Survey of Health Related Behaviors.14 They found that military men and women had similar rates of cigarette and illicit-drug use but that military men had significantly higher rates of heavy alcohol use. “Work” stress and “family” stress were significantly associated with substance use in men, but no such relationship was observed in women. The only significant relationship observed in women was between “stress associated with being a woman in the military” and cigarette and illicit-drug use. Brown et al. (2010) compared alcohol use in military men and women by using questionnaire data on 9,506 male and 3,250 female active-duty military personnel obtained from the 2002 DOD Survey of Health Related Behaviors. The investigators found that men had significantly higher rates of heavy or binge drinking and more alcohol-related problems than women. On the basis of their data, however, they concluded that women might experience alcohol-related problems at lower consumption levels. They appeared to base that conclusion on an analysis that indicated that female officers did not have statistically significant different rates of dependence symptoms, productivity loss, or serious consequences
__________________
14Substance use was defined as cigarette smoking, heavy alcohol use, or illicit-drug use.
from their male counterparts who had significantly higher rates of moderate, heavy, and binge drinking.
One issue to consider is whether risk factors for SUDs occur more commonly in women or have a greater effect on women. For example, Federman et al. (2000) investigated the relationship between peacetime deployment and substance use by using the 1995 DOD Survey of Health Related Behaviors. Regression analyses indicated a positive association between deployment and heavy alcohol use in both men and women, but a stronger association was observed in women; the authors noted that deployment was significantly associated with cigarette use, nonheavy alcohol use, and alcohol dependence in men but not in women.
As is the case with the other mental-health outcomes discussed above, the higher rate of military sexual abuse in women is relevant to SUDs. As noted earlier, Hankin et al. (1999) found that female victims of military sexual assault were significantly more likely to screen positive for alcohol abuse (7% vs 4%) than female veterans who had no such history. In their review of administrative data on 2,900,106 male and 134,894 female outpatients at VA health centers, Kimerling et al. (2007) found that alcohol disorders were much more common in women and men who reported MST than in those who did report MST and that the association was stronger in women. In a later study specifically on OEF and OIF veterans, Kimerling et al. (2010) found that MST was significantly associated with SUDs and that the effect again was stronger in women than in men. Booth et al. (2011) conducted a retrospective evaluation of the relationship between sexual assault and SUDs in 1,004 female veterans by using data collected in telephone interviews. The authors found that about 50% had been raped at some point in their lives (31% during childhood, 11% before military service, 25% during military service, and 11% after military service). A strong association between a rape history of any kind and a lifetime SUD was found.
Suicidal Ideation
Little information is available about sex differences in the prevalence of suicidal ideation. As in research on the general population, McCarthy et al. (2009) found in their review of data on 4,670,968 patients that female veterans using the VA health care system had a lower suicide rate than male veterans. However, female veterans 40–59 years old had significantly higher suicide rates than women of similar ages in the general population. The authors concluded that “female patients had particularly high relative risks.”
Although research indicates that suicide rates are lower in women than in men in the general and military populations, women tend to suffer higher rates of depression, which is a known risk factor for suicidal ideation. Zivin et al. (2007) evaluated demographic and clinical factors in 807,694 patients of the VA health care system who had diagnoses of depression and had been prescribed antidepressants, a group at high risk for suicide. The suicide rate was higher in male veterans than in female veterans, but the difference between the rates was smaller than the difference typically found in the general population (1:3 vs 1:4).
Summary
Although women are banned from combat, the reality of recent conflicts in OEF and OIF is that women serve in combat-support roles that expose them to high-intensity asymmetric warfare and combat trauma. For more than a decade, female military service members have been
subject to repeat deployments, have endured prolonged separation from family, have served side by side with men, and have been exposed to harsh wartime conditions, including witnessing death and destruction.
In contrast with results of animal research, there is little evidence of sex-based differences in TBI outcomes in women, but a study of neuropsychologic outcomes of mild TBI in female veterans did demonstrate that they had significantly higher rates of PTSD, other anxiety disorders, and depression than their male counterparts. Women were also more likely to report “severe” or “very severe” cognitive, somatosensory, and vestibular symptoms.
Research has raised substantial concerns about the mental-health consequences of OEF and OIF combat deployments in women. Women have been found to suffer more mental-health problems than men who served in Iraq or Afghanistan as evidenced by higher rates of medical evacuations and hospitalizations for primary psychiatric conditions. Women have higher rates of self-reported PTSD and depression symptoms in predeployment and postdeployment screenings and are more likely to received diagnoses of depression than their male counterparts. They also suffer from more comorbid mental-health conditions than men.
Exposure to MST has been associated with higher risks of poor mental health, physical health, and quality of life in women than in men. Trends in cross-sectional studies of VA health care user populations suggest that men more often screen positive for PTSD and women more often screen positive for depression. Studies have also identified persistently high rates of MST in OIF and OEF. Military sexual assault has been shown to convey a greater risk of PTSD and other mental-health conditions, such as depression and SUD, than either childhood or civilian adult sexual assault. MST is a stronger predictor of PTSD in women than in men.
Longitudinal studies of women who served in combat theaters and evaluations of the diagnosis of SUDs have not been performed, and far less research is available regarding those who served in Iraq or Afghanistan. Studies of veterans seeking care at VA facilities have not identified significant sex-based differences in PTSD risk. Well-designed longitudinal studies have not been completed to increase our understanding of those issues.
CONCLUSIONS
Being deployed to a war zone can result in numerous adverse outcomes. The committee focused on TBI, PTSD, depression, suicide and suicidal ideation, and SUDs in its review as specified in the legislation directing its work (see Appendix A). Any one of those outcomes can, in turn, have numerous sequelae and associated outcomes (comorbidities) that can have significant impacts on health, quality of life, functional impairment, and socioeconomic status. Emerging issues regarding multiple deployments, short dwell times, the relationship of multiple concussions to chronic traumatic encephalopathy, risk of suicide, and the importance of comorbidities with TBI, PTSD, and depression await study and clarification. With regard to suicide prevention, increased efforts are needed to train military personnel, health care providers, and family members in recognizing the signs of suicide risk. Increased emphasis on the importance of social networks and health care in reducing that risk is also needed, as is training to reduce the stigma associated with seeking care. It must be understood that occupational stressors associated with military service may continue long after troops leave the theater of
conflict. Finally, military sexual trauma continues to occur at high rates in OEF and OIF populations, and increased efforts to eliminate this violence are critically needed.
FUTURE RESEARCH DIRECTIONS
As the committee reviewed the literature and examined the range of federally funded research on TBI and mental health outcomes in OEF and OIF (Appendix D), it identified a number of unaddressed questions and areas for future study and research. The literature is incomplete and there remain significant challenges in determining the prevalence of physical and psychologic morbidity and comorbidities after military service in Iraq and Afghanistan.
Although the current reports and studies of OEF and OIF have progressively built upon knowledge gained from prior conflicts and have made valuable contributions to the growing understanding of the consequences associated with deployment to OEF and OIF, the have a set of common limitations. The committee noted in its Phase 1 report that most of the literature falls short of meeting the methodological standards it described. Additionally, many studies provide very broad ranges for prevalence estimates of various mental health outcomes making them difficult to use for policy makers. The committee reiterates its recommendation from Phase 1 regarding future studies and the need to be both scientifically sound and comprehensive (see Appendix B and Chapter 11).
Longitudinal studies are needed to answer many of the questions that are not answered by the literature and current studies. Such studies should strive to improve the recruitment and retention of subjects. Current studies might be the most appropriate platform for developing a strategy for long-term followup, such as the Millennium Cohort Study and the Longitudinal Health Study of Gulf War Era Veterans. Those can be augmented with supplementary samples of OEF and OIF veterans. Other characteristics that such studies should have include the ability to collect biologic specimens, oversampling of OEF and OIF female and minority-group populations, and planning for add-on studies to address newly identified needs. Specifically, what are the long-term outcomes of most conditions of concern? Do the outcomes vary by severity, comorbidity, ethnicity, or sex?
The committee provides areas for future research studies below.
• Longitudinal studies are needed to examine long-term outcomes of mild TBI using better exposure data, biological markers, and performance-based cognitive measures as well as measures of emotional health. Examine whether the results vary by number of mild TBIs, and various demographic factors including sex, race, and ethnicity. Do the results vary as a function of type and number of comorbidities?
• Longitudinal studies to examine evidence for accelerated aging and CTE in those with TBI. What are the risk factors for and protective factors against CTE?
• Studies to determine whether biologic markers can help in predicting outcomes?
• Studies with better exposure data, and objective diagnostic tests or biomarkers for mild TBI and PTSD are needed to improve our understanding of those highly comorbid conditions.
• Studies to elucidate how brain imaging can provide information about outcomes?
• Studies to determine if specific symptomatic markers predict the outcome of PTSD? The current array of PTSD symptoms might not be the most clinically relevant for tracking
outcome. For example, a focus on sleep disturbance coupled with troubling dreams as a specific symptom might be of more value.
• Studies to determine how the current distinction between diagnosis and symptoms might predict outcome? The line between a diagnosis of PTSD and PTSD symptoms is not well validated. Can longitudinal studies determine a threshold and a constellation of symptoms that point clearly to a diagnosis?
• Prospective studies of veterans, who present with first reports of suicidal ideation and have no previous mental-health diagnoses, to provide clarity in understanding risk factors for future suicide and future mental-health morbidity?
• Systematic studies on MST delineating where it occurs, the characteristics of perpetrators, the relationship between perpetrators and victims, and what types of sexual trauma are most common. A better understanding of those issues might be important in the design of initiatives to eliminate it.
RECOMMENDATIONS
The literature on the outcomes of military deployment has grown dramatically over the last two decades. Although discrepant findings do emerge, there is a clear consensus in the literature that the stressors of deployment, from exposure to combat to multiple deployments away from home and family, can lead to a number of adverse conditions. The committee concentrated on deployment-related outcomes—such as TBI, PTSD, depression, substance use, and suicidal ideation—but the list could be expanded to many additional psychiatric conditions and a host of physical conditions. The data on short-term outcomes (outcomes in 6 months or less) is extensive, but data on long-term outcomes (over years) less extensive and both can be challenged on methodologic grounds. To capture the true long-term outcomes of deployment to war zones and plan services to address them, more data will be essential.
The committee recommends that the Department of Defense and the Department of Veterans Affairs sponsor longitudinal studies to answer many of the questions regarding long-term effects of traumatic brain injury, posttraumatic stress disorder, and other mental-health disorders. Such studies should strive to improve the validity of exposure measurements, identification and use of biomarkers, and recruitment and retention of subjects. Attention should be paid to whether the outcomes of traumatic brain injuries depend on the severity and number of such injuries, on the presence of comorbid conditions, and on sex and ethnicity.
Current studies might be the most appropriate platform for developing a strategy for long-term followup, such as the Millennium Cohort Study and the Longitudinal Health Study of Gulf War Era Veterans. Those studies can be augmented with supplementary samples of OEF, OIF, and OND veterans. Other factors that should define such studies include the ability to collect biologic specimens, oversampling of OEF, OIF, and OND female and minority-group populations, and planning for add-on studies to address new needs as they are identified.
Many health consequences of service in OEF, OIF, and OND are related to the inherently dangerous nature of the wartime environment or resulting trauma. However, one major exposure, military sexual trauma (MST), is unrelated to war but rather is due to noncombat violent assault.
Studies show that MST has been occurring at high rates in the US military, including during OEF, OIF, and OND. Research demonstrates that MST is associated with poor readjustment and adverse mental-health and physical outcomes. The burden of physical and mental-health consequences for the victims and their family members is high. Increased efforts by DOD are necessary, and a zero-tolerance approach should be implemented.
The committee recommends that the Department of Defense develop policies to eliminate military sexual trauma as research demonstrates that it is associated with poor readjustment and mental-health and physical-health outcomes. The committee further recommends that the department reinforce existing policies on military sexual trauma by adding specific mandatory evaluation criteria regarding how well military leaders address the issue, for example, in the formal performance-appraisal and promotion systems.
The breadth and depth of the challenges faced by military service members and veterans who served in Iraq and Afghanistan result from the complex interaction of issues that must be addressed by primary prevention, diagnostics, treatment, rehabilitation, education and outreach, and community support programs if readjustment after combat service is to be successful.
REFERENCES
Adler, D. A., K. Possemato, S. Mavandadi, D. Lerner, H. Chang, J. Klaus, J. D. Tew, D. Barrett, E. Ingram, and D. W. Oslin. 2011. Psychiatric status and work performance of veterans of Operations Enduring Freedom and Iraqi Freedom. Psychiatric Services 62(1):39-46.
Afari, N., L. H. Harder, N. J. Madra, P. S. Heppner, T. Moeller-Bertram, C. King, and D. G. Baker. 2009. PTSD, combat injury, and headache in veterans returning from Iraq/Afghanistan. Headache: The Journal of Head and Face Pain 49(9):1267-1276.
AFHSC (Armed Forces Health Surveillance Center). 2011. Associations between repeated deployments to OEF/OIF/OND, October 2001-December 2010, and post-deployment illnesses and injuries, active component, US Armed Forces. Medical Surveillance Monthly Report 18(7):2-11.
AFHSC. 2012. Deaths by suicide while on active duty, active and reserve components, US Armed Forces, 1998-2011. Medical Surveillance Monthly Report 19(6):7-10.
Andersen, J., M. Wade, K. Possemato, and P. Ouimette. 2010. Association between posttraumatic stress disorder and primary care provider-diagnosed disease among Iraq and Afghanistan veterans. Psychosomatic Medicine 72(5):498-504.
APA (American Psychiatric Association). 2000. Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR), 4th ed. Washington, DC: American Psychiatric Association.
Asmundson, G. J. G., K. D. Wright, and M. B. Stein. 2004. Pain and PTSD symptoms in female veterans. European Journal of Pain 8(4):345-350.
Bagalman, E. 2011. Suicide, PTSD, and Substance Use Among OEF/OIF Veterans Using VA Health Care: Facts and Figures. Washington, DC: Congressional Research Service.
Baker, D. G., P. Heppner, N. Afari, S. Nunnink, M. Kilmer, A. Simmons, L. Harder, and B. Bosse. 2009. Trauma exposure, branch of service, and physical injury in relation to mental health among US veterans returning from Iraq and Afghanistan. Military Medicine 174(8):773-778.
Barrett, D. H., M. L. Green, R. Morris, W. H. Giles, and J. B. Croft. 1996. Cognitive functioning and posttraumatic stress disorder. American Journal of Psychiatry 153(11):1492-1494.
Barrett, D. H., G. C. Gray, B. N. Doebbeling, D. J. Clauw, and W. C. Reeves. 2002. Prevalence of symptoms and symptom-based conditions among Gulf War veterans: Current status of research findings. Epidemiologic Reviews 24(2):218-227.
Belanger, H. G., and R. D. Vanderploeg. 2005. The neuropsychological impact of sports-related concussion: A meta-analysis. Journal of the International Neuropsychological Society 11(4):345-357. Belanger, H. G., G. Curtiss, J. A. Demery, B. K. Lebowitz, and R. D. Vanderploeg. 2005. Factors moderating neuropsychological outcomes following mild traumatic brain injury: A meta-analysis. Journal of the International Neuropsychological Society 11(3):215-227.
Belanger, H. G., T. Kretzmer, R. Yoash-Gantz, T. Pickett, and L. A. Tupler. 2009. Cognitive sequelae of blast-related versus other mechanisms of brain trauma. Journal of the International Neuropsychological Society 15(1):1-8.
Belanger, H. G., and R. D. Vanderploeg. 2005. The neuropsychological impact of sports-related concussion: A meta-analysis. Journal of the International Neuropsychological Society 11(4):345-357.
Bell, K. R., J. M. Hoffman, N. R. Temkin, J. M. Powell, R. T. Fraser, P. C. Esselman, J. K. Barber, and S. Dikmen. 2008. The effect of telephone counselling on reducing post-traumatic symptoms after mild traumatic brain injury: A randomised trial. Journal of Neurology, Neurosurgery, and Psychiatry 79(11):1275-1281.
Bell, N. S., T. C. Harford, C. H. Fuchs, J. E. McCarroll, and C. E. Schwartz. 2006. Spouse abuse and alcohol problems among white, African American, and Hispanic US Army soldiers. Alcoholism: Clinical and Experimental Research 30(10):1721-1733.
Bell, N. S., T. C. Harford, P. J. Amoroso, I. E. Hollander, and A. B. Kay. 2010. Prior health care utilization patterns and suicide among US Army soldiers. Suicide and Life-Threatening Behavior 40(4):407-415.
Black, S. A., M. S. Gallaway, M. R. Bell, and E. C. Ritchie. 2011. Prevalence and risk factors associated with suicides of Army soldiers 2001–2009. Military Psychology 23(4):433-451.
Blume, A. W., K. B. Schmaling, and M. L. Russell. 2010. Stress and alcohol use among soldiers assessed at mobilization and demobilization. Military Medicine 175(6):400-404.
Bombardier, C. H., N. R. Temkin, J. Machamer, and S. S. Dikmen. 2003. The natural history of drinking and alcohol-related problems after traumatic brain injury. Archives of Physical Medicine and Rehabilitation 84(2):185-191.
Bombardier, C. H., J. R. Fann, N. R. Temkin, P. C. Esselman, J. Barber, and S. S. Dikmen. 2010. Rates of major depressive disorder and clinical outcomes following traumatic brain injury. Journal of the American Medical Association 303(19):1938-1945.
Bonanno, G. A., A. D. Mancini, J. L. Horton, T. M. Powell, C. A. Leardmann, E. J. Boyko, T. S. Wells, T. I. Hooper, G. D. Gackstetter, T. C. Smith, and Millennium Cohort Study Team. 2012. Trajectories of trauma symptoms and resilience in deployed US military service members: Prospective cohort study. British Journal of Psychiatry 200(4):317-323.
Booth, B. M., M. Mengeling, J. Torner, and A. G. Sadler. 2011. Rape, sex partnership, and substance use consequences in women veterans. Journal of Traumatic Stress 24(3):287-294.
Booth-Kewley, S., G. E. Larson, R. M. Highfill-McRoy, C. F. Garland, and T. A. Gaskin. 2010. Correlates of posttraumatic stress disorder symptoms in Marines back from war. Journal of Traumatic Stress 23(1):69-77.
Boscarino, J. A. 1997. Diseases among men 20 years after exposure to severe stress: Implications for clinical research and medical care. Psychosomatic Medicine 59(6):605-614.
———. 2004. Posttraumatic stress disorder and physical illness: Results from clinical and epidemiologic studies. Annals of the New York Academy of Sciences 1032:141-153.
Brady, K. T., P. Tuerk, S. E. Back, M. E. Saladin, A. E. Waldrop, and H. Myrick. 2009. Combat posttraumatic stress disorder, substance use disorders, and traumatic brain injury. Journal of Addiction Medicine 3(4):179-188.
Brailey, K. 2009. MTBI Effects on Emotion Symptoms, Neurocognitive Performance, and Functional Impairment: A Longitudinal Study of Deployed and Non-Deployed Army Soldiers. Fort Detrick, MD: Army Medical Research and Materiel Command.
Bray, R. M., J. A. Fairbank, and M. E. Marsden. 1999. Stress and substance use among military women and men. American Journal of Drug and Alcohol Abuse 25(2):239-256.
Bray, R. M., M. R. Pemberton, L. L. Hourani, M. Witt, K. L. Olmsted, J. M. Brown, B. Weimer, M. E. Lance, M. E. Marsden, and S. Scheffer. 2009a. 2008 Department of Defense Survey of Health Related Behaviors Among Active Duty Military Personnel. Research Triangle Park, NC: RTI International.
Bray, R. M., M. R. Pemberton, L. L. Hourani, M. Witt, K. L. Rae Olmsted, J. M. Brown, B. Weimer, M. E. Lane, M. E. Marsden, S. Scheffler, R. Vandermaas-Peeler, K. R. Aspinwall, E. Anderson, K. Spagnola, K. Close, J. L. Gratton, S. Calvin, and M. Bradshaw. 2009b. Department of Defense Survey of Health Related Behaviors Among Active Duty Military Personnel: A Component of the Defense Lifestyle Assessment Program (DLAP). Research Triangle Park, NC: RTI International.
Bray, R. M., M. R. Pemberton, M. E. Lane, L. L. Hourani, M. J. Mattiko, and L. A. Babeu. 2010. Substance use and mental health trends among US military active duty personnel: Key findings from the 2008 DOD Health Behavior Survey. Military Medicine 175(6):390-399.
Bremner, J. D., S. M. Southwick, A. Darnell, and D. S. Charney. 1996. Chronic PTSD in Vietnam combat veterans: Course of illness and substance abuse. American Journal of Psychiatry 153(3):369-375.
Brenner, L. A., B. J. Ivins, K. Schwab, D. Warden, L. A. Nelson, M. Jaffee, and H. Terrio. 2010a. Traumatic brain injury, posttraumatic stress disorder, and postconcussive symptom reporting among troops returning from Iraq. Journal of Head Trauma Rehabilitation 25(5):307-312.
Brenner, L. A., H. Terrio, B. Y. Homaifar, P. M. Gutierrez, P. J. Staves, J. E. Harwood, D. Reeves, L. E. Adler, B. J. Ivins, K. Helmick, and D. Warden. 2010b. Neuropsychological test performance in soldiers with blast-related mild TBI. Neuropsychology 24(2):160-167.
Brenner, L. A., R. V. Ignacio, and F. C. Blow. 2011. Suicide and traumatic brain injury among individuals seeking veterans health administration services. Journal of Head Trauma Rehabilitation 26(4):257-264.
Breslau, N. 2002. Gender differences in trauma and posttraumatic stress disorder. Journal of Genderspecific Medicine 5(1):34-40.
Breslau, N., V. C. Lucia, and G. F. Alvarado. 2006. Intelligence and other predisposing factors in exposure to trauma and posttraumatic stress disorder: A follow-up study at age 17 years. Archives of General Psychiatry 63(11):1238-1245.
Brown, J. M., R. M. Bray, and M. C. Hartzell. 2010. A comparison of alcohol use and related problems among women and men in the military. Military Medicine 175(2):101-107.
Bruce, M. L. 2010. Suicide risk and prevention in veteran populations. Annals of the New York Academy of Sciences 1208:98-103.
Bryant, R. 2011. Post-traumatic stress disorder vs traumatic brain injury. Dialogues in Clinical Neuroscience 13(3):251-262.
Bryant, R. A., and A. G. Harvey. 2002. Delayed-onset posttraumatic stress disorder: A prospective evaluation. Australian and New Zealand Journal of Psychiatry 36(2):205-209.
Buckley, T. C., and D. G. Kaloupek. 2001. A meta-analytic examination of basal cardiovascular activity in posttraumatic stress disorder. Psychosomatic Medicine 63(4):585-594.
Burnett-Zeigler, I., M. Ilgen, M. Valenstein, K. Zivin, L. Gorman, A. Blow, S. Duffy, and S. Chermack. 2011. Prevalence and correlates of alcohol misuse among returning Afghanistan and Iraq veterans. Addictive Behaviors 36(8):801-806.
Cabrera, O. A., C. W. Hoge, P. D. Bliese, C. A. Castro, and S. C. Messer. 2007. Childhood adversity and combat as predictors of depression and post-traumatic stress in deployed troops. American Journal of Preventive Medicine 33(2):77-82.
Calhoun, P. S., J. C. Beckham, and H. B. Bosworth. 2002. Caregiver burden and psychological distress in partners of veterans with chronic posttraumatic stress disorder. Journal of Traumatic Stress 15(3):205-212.
Calhoun, P. S., J. R. Elter, E. R. Jones, H. Kudler, and K. Straits-Troster. 2008. Hazardous alcohol use and receipt of risk-reduction counseling among US veterans of the wars in Iraq and Afghanistan. Journal of Clinical Psychiatry 69(11):1686-1693.
Campbell, T. A., L. A. Nelson, R. Lumpkin, R. E. Yoash-Gantz, T. C. Pickett, and C. L. McCormick. 2009. Neuropsychological measures of processing speed and executive functioning in combat veterans with PTSD, TBI, and comorbid TBI/PTSD. Psychiatric Annals 39(8):796-803.
Carlson, K. F., D. Nelson, R. J. Orazem, S. Nugent, D. X. Cifu, and N. A. Sayer. 2010. Psychiatric diagnoses among Iraq and Afghanistan war veterans screened for deployment-related traumatic brain injury. Journal of Traumatic Stress 23(1):17-24.
Carlson, K. F., A. A. Gravely, S. Noorbaloochi, A. B. Simon, A. K. Bangerter, and N. A. Sayer. 2011a. Post-deployment injury among new combat veterans enrolled in Veterans Affairs (VA) healthcare. Injury Prevention 17(5):343-347.
Carlson, K. F., S. M. Kehle, L. A. Meis, N. Greer, R. Macdonald, I. Rutks, N. A. Sayer, S. K. Dobscha, and T. J. Wilt. 2011b. Prevalence, assessment, and treatment of mild traumatic brain injury and posttraumatic stress disorder: A systematic review of the evidence. Journal of Head Trauma Rehabilitation 26(2):103-115.
Carter-Visscher, R., M. A. Polusny, M. Murdoch, P. Thuras, C. R. Erbes, and S. M. Kehle. 2010. Predeployment gender differences in stressors and mental health among US National Guard troops poised for Operation Iraqi Freedom deployment. Journal of Traumatic Stress 23(1):78-85.
Carty, J., M. L. O'Donnell, and M. Creamer. 2006. Delayed-onset PTSD: A prospective study of injury survivors. Journal of Affective Disorders 90(2-3):257-261.
CBO (Congressional Budget Office). 2012. The Veterans Health Administration's Treatment of PTSD and Traumatic Brain Injury Among Recent Combat Veterans. Washington, DC: Congressional Budget Office.
CDC (Centers for Disease Control and Prevention). 2011a. Suicidal thoughts and behaviors among adults aged .18 years—United States, 2008–2009. Morbidity and Mortality Weekly Report 60(s13):1-22.
———. 2011b. Vital signs: Overdoses of prescription opioid pain relievers—United States, 1999–2008. Morbidity and Mortality Weekly Report 60(43):1487-1492.
———. 2012. National suicide statistics at a glance. http://www.cdc.gov/ViolencePrevention/suicide/statistics/trends02.html (accessed April 13, 2012).
Cooper, D. B., J. E. Kennedy, M. A. Cullen, E. Critchfield, R. R. Amador, and A. O. Bowles. 2011. Association between combat stress and post-concussive symptom reporting in OEF/OIF service members with mild traumatic brain injuries. Brain Injury 25(1):1-7.
Corkin, S., T. J. Rosen, E. V. Sullivan, and R. A. Clegg. 1989. Penetrating head injury in young adulthood exacerbates cognitive decline in later years. Journal of Neuroscience 9(11):3876-3883.
Corsellis, J. A., C. J. Bruton, and D. Freeman-Browne. 1973. The aftermath of boxing. Psychological Medicine 3(3):270-303.
Cosgrove, D. J., Z. Gordon, J. E. Bernie, S. Hami, D. Montoya, M. B. Stein, and M. Monga. 2002. Sexual dysfunction in combat veterans with post-traumatic stress disorder. Urology 60(5):881-884.
Crowell, T. A., K. M. Kieffer, C. A. Siders, and R. D. Vanderploeg. 2002. Neuropsychological findings in combat-related posttraumatic stress disorder. Clinical Neuropsychologist 16(3):310-321.
Cucciare, M. A., S. Ghaus, K. R. Weingardt, and S. M. Frayne. 2011. Sexual assault and substance use in male veterans receiving a brief alcohol intervention. Journal of Studies on Alcohol and Drugs 72(5):693-700.
Dagan, Y., P. Lavie, and A. Bleich. 1991. Elevated awakening thresholds in sleep stage 3-4 in war-related post-traumatic stress disorder. Biological Psychiatry 30(6):618-622.
DCoE (Defense Centers For Excellence for Psychological Health and Traumatic Brain Injury). 2011. Department of Defense Suicide Event Report: Calendar Year 2010 Annual Report. Washington, DC: National Center for Telehealth and Technology, Defense Centers for Excellence for Psychological Health and Traumatic Brain Injury.
Dedert, E. A., K. T. Green, P. S. Calhoun, R. Yoash-Gantz, K. H. Taber, M. M. Mumford, L. A. Tupler, R. A. Morey, C. E. Marx, R. D. Weiner, and J. C. Beckham. 2009. Association of trauma exposure with psychiatric morbidity in military veterans who have served since September 11, 2001. Journal of Psychiatric Research 43(9):830-836.
Department of the Army. 2012. Army 2020: Generating Health and Discipline in the Force. Washington, DC: Department of Defense.
Dikmen, S., J. Machamer, N. Temkin, and A. McLean. 1990. Neuropsychological recovery in patients with moderate to severe head injury: 2 year follow-up. Journal of Clinical and Experimental Neuropsychology 12(4):507-519.
Dikmen, S., J. Machamer, and N. Temkin. 1993. Psychosocial outcome in patients with moderate to severe head injury: 2-year follow-up. Brain Injury 7(2):113-124.
Dikmen, S. S., N. R. Temkin, J. E. Machamer, A. L. Holubkov, R. T. Fraser, and H. R. Winn. 1994. Employment following traumatic head injuries. Archives of Neurology 51(2):177-186.
Dikmen, S. S., J. E. Machamer, H. Winn, and N. R. Temkin. 1995. Neuropsychological outcome at 1-year post head injury. Neuropsychology 9(1):80-90.
Dikmen, S. S., J. D. Corrigan, H. S. Levin, J. MacHamer, W. Stiers, and M. G. Weisskopf. 2009. Cognitive outcome following traumatic brain injury. Journal of Head Trauma Rehabilitation 24(6):430-438.
Dikmen, S., J. Machamer, J. R. Fann, and N. R. Temkin. 2010. Rates of symptom reporting following traumatic brain injury. Journal of the International Neuropsychological Society 16(3):401-411.
Dobie, D. J., D. R. Kivlahan, C. Maynard, K. R. Bush, T. M. Davis, and K. A. Bradley. 2004. Posttraumatic stress disorder in female veterans: Association with self-reported health problems and functional impairment. Archives of Internal Medicine 164(4):394-400.
Doctor, J. N., J. Castro, N. R. Temkin, R. T. Fraser, J. E. Machamer, and S. S. Dikmen. 2005. Workers' risk of unemployment after traumatic brain injury: A normed comparison. Journal of the International Neuropsychological Society 11(6):747-752.
DOD (Department of Defense). 2009a. DOD/VA Code Proposal Final. http://www.cdc.gov/nchs/data/icd9/Sep08TBI.pdf (accessed October 29, 2012).
———. 2009b. Status of Drug Use in Department of Defense Personnel: Fiscal Year 2008 Drug Testing Statistical Report. Falls Church, VA: Office of the Assistant Secretary of Defense for Health Affairs.
Dow, B. M., J. R. Kelsoe, Jr., and J. C. Gillin. 1996. Sleep and dreams in Vietnam PTSD and depression. Biological Psychiatry 39(1):42-50.
Drew, R. H., D. I. Templer, B. A. Schuyler, T. G. Newell, and W. G. Cannon. 1986. Neuropsychological deficits in active licensed professional boxers. Journal of Clinical Psychology 42(3):520-525.
Dutra, L., K. Grubbs, C. Greene, L. L. Trego, T. L. McCartin, K. Kloezeman, and L. Morland. 2011. Women at war: Implications for mental health. Journal of Trauma and Dissociation 12(1):25-37.
DVBIC (Defense and Veterans Brain Injury Center). 2012. DOD Numbers for Traumatic Brain Injury Worldwide — Totals. Silver Spring, MD: Department of Defense.
Edens, E. L., W. Kasprow, J. Tsai, and R. A. Rosenheck. 2011. Association of substance use and VA service-connected disability benefits with risk of homelessness among veterans. American Journal on Addictions 20(5):412-419.
Eisen, S. V., M. R. Schultz, D. Vogt, M. E. Glickman, A. R. Elwy, M. L. Drainoni, P. E. Osei-Bonsu, and J. Martin. 2012. Mental and physical health status and alcohol and drug use following return from deployment to Iraq or Afghanistan. American Journal of Public Health 102(S1):S66-S73.
Elbogen, E. B., H. Wagner, S. R. Fuller, P. S. Calhoun, P. M. Kinneer, and J. C. Beckham. 2010. Correlates of anger and hostility in Iraq and Afghanistan war veterans. American Journal of Psychiatry 167(9):1051-1058.
Elder, G. A., and A. Cristian. 2009. Blast-related mild traumatic brain injury: Mechanisms of injury and impact on clinical care. Mount Sinai Journal of Medicine 76(2):111-118.
Engdahl, B. E., R. E. Eberly, T. D. Hurwitz, M. W. Mahowald, and J. Blake. 2000. Sleep in a community sample of elderly war veterans with and without posttraumatic stress disorder. Biological Psychiatry 47(6):520-525.
Engel, C. C., Jr., X. Liu, B. D. McCarthy, R. F. Miller, and R. Ursano. 2000. Relationship of physical symptoms to posttraumatic stress disorder among veterans seeking care for gulf war-related health concerns. Psychosomatic Medicine 62(6):739-745.
Erbes, C. R., M. E. Kaler, T. Schult, M. A. Polusny, and P. A. Arbisi. 2011. Mental health diagnosis and occupational functioning in National Guard/reserve veterans returning from Iraq. Journal of Rehabilitation Research and Development 48(10):1159-1170.
Fann, J. R., A. Leonetti, K. Jaffe, W. J. Katon, P. Cummings, and R. S. Thompson. 2002. Psychiatric illness and subsequent traumatic brain injury: A case control study. Journal of Neurology, Neurosurgery, and Psychiatry 72(5):615-620.
Fann, J. R., B. Burington, A. Leonetti, K. Jaffe, W. J. Katon, and R. S. Thompson. 2004. Psychiatric illness following traumatic brain injury in an adult health maintenance organization population. Archives of General Psychiatry 61(1):53-61.
Fear, N. T., M. Jones, D. Murphy, L. Hull, A. C. Iversen, B. Coker, L. Machell, J. Sundin, C. Woodhead, N. Jones, N. Greenberg, S. Landau, C. Dandeker, R. J. Rona, M. Hotopf, and S. Wessely. 2010. What are the consequences of deployment to Iraq and Afghanistan on the mental health of the UK Armed Forces? A cohort study. Lancet 375(9728):1783-1797.
Federman, E. B., R. M. Bray, and L. A. Kroutil. 2000. Relationships between substance use and recent deployments among women and men in the military. Military Psychology 12(3):205-220.
Ferrier-Auerbach, A. G., S. M. Kehle, C. R. Erbes, P. A. Arbisi, P. Thuras, and M. A. Polusny. 2009. Predictors of alcohol use prior to deployment in National Guard soldiers. Addictive Behaviors 34(8):625-631.
Flynn, P. M., and B. S. Brown. 2008. Co-occurring disorders in substance abuse treatment: Issues and prospects. Journal of Substance Abuse and Treatment 34(1):36-47.
Fontana, A., and R. Rosenheck. 2008. Treatment-seeking veterans of Iraq and Afghanistan: Comparison with veterans of previous wars. Journal of Nervous and Mental Disease 196(7):513-521.
Frayne, S. M., M. R. Seaver, S. Loveland, C. L. Christiansen, A. Spiro, 3rd, V. A. Parker, and K. M. Skinner. 2004. Burden of medical illness in women with depression and posttraumatic stress disorder. Archives of Internal Medicine 164(12):1306-1312.
Frayne, S. M., V. Y. Chiu, S. Iqbal, E. A. Berg, K. J. Laungani, R. C. Cronkite, J. Pavao, and R. Kimerling. 2011. Medical care needs of returning veterans with PTSD: Their other burden. Journal of General Internal Medicine 26(1):33-39.
Friedman, M. 2003. Post Traumatic Stress Disorder. Kansas City, MO: Compact Clinicals.
Fritch, A. M., M. Mishkind, M. A. Reger, and G. A. Gahm. 2010. The impact of childhood abuse and combat-related trauma on postdeployment adjustment. Journal of Traumatic Stress 23(2):248-254.
Gahm, G. A., B. A. Lucenko, P. Retzlaff, and S. Fukuda. 2007. Relative impact of adverse events and screened symptoms of posttraumatic stress disorder and depression among active duty soldiers seeking mental health care. Journal of Clinical Psychology 63(3):199-211.
Gale, C. R., I. J. Deary, S. H. Boyle, J. Barefoot, L. H. Mortensen, and G. D. Batty. 2008. Cognitive ability in early adulthood and risk of 5 specific psychiatric disorders in middle age: The Vietnam Experience Study. Archives of General Psychiatry 65(12):1410-1418.
Galovski, T. E., J. Mott, Y. N. Young-Xu, and P. A. Resick. 2011. Gender differences in the clinical presentation of PTSD and its concomitants in survivors of interpersonal assault. Journal of Interpersonal Violence 26(4):789-806.
Gaylord, K. M., D. B. Cooper, J. M. Mercado, J. E. Kennedy, L. H. Yoder, and J. B. Holcomb. 2008. Incidence of posttraumatic stress disorder and mild traumatic brain injury in burned service members: Preliminary report. Journal of Trauma: Injury, Infection, and Critical Care 64(2):s200-s206.
Gellis, L. A., P. R. Gehrman, S. Mavandadi, and D. W. Oslin. 2010a. Predictors of sleep disturbances in Operation Iraqi Freedom/Operation Enduring Freedom veterans reporting a trauma. Military Medicine 175(8):567-573.
Gellis, L. A., S. Mavandadi, and D. W. Oslin. 2010b. Functional quality of life in full versus partial posttraumatic stress disorder among veterans returning from Iraq and Afghanistan. Primary Care Companion to the Journal of Clinical Psychiatry 12(3).
Gerber, D. J., and J. C. Schraa. 1995. Mild traumatic brain injury: Searching for the syndrome. Journal of Head Trauma Rehabilitation 10(4):28-40.
Gibbons, S. W., E. J. Hickling, S. D. Barnett, P. L. Herbig-Wall, and D. D. Watts. 2012. Gender differences in response to deployment among military healthcare providers in Afghanistan and Iraq. Journal of Women's Health 21(5):496-504.
Gilbertson, M. W., T. V. Gurvits, N. B. Lasko, S. P. Orr, and R. K. Pitman. 2001. Multivariate assessment of explicit memory function in combat veterans with posttraumatic stress disorder. Journal of Traumatic Stress 14(2):413-432.
Gilbertson, M. W., M. E. Shenton, A. Ciszewski, K. Kasai, N. B. Lasko, S. P. Orr, and R. K. Pitman. 2002. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nature Neuroscience 5(11):1242-1247.
Glenn, D. M., J. C. Beckham, M. E. Feldman, A. C. Kirby, M. A. Hertzberg, and S. D. Moore. 2002. Violence and hostility among families of Vietnam veterans with combat-related posttraumatic stress disorder. Violence and Victims 17(4):473-489.
Goldstein, L. E., A. M. Fisher, C. A. Tagge, X. L. Zhang, L. Velisek, J. A. Sullivan, C. Upreti, J. M. Kracht, M. Ericsson, M. W. Wojnarowicz, C. J. Goletiani, G. M. Maglakelidze, N. Casey, J. A. Moncaster, O. Minaeva, R. D. Moir, C. J. Nowinski, R. A. Stern, R. C. Cantu, J. Geiling, J. K. Blusztajn, B. L. Wolozin, T. Ikezu, T. D. Stein, A. E. Budson, N. W. Kowall, D. Chargin, A. Sharon, S. Saman, G. F. Hall, W. C. Moss, R. O. Cleveland, R. E. Tanzi, P. K. Stanton, and A. C. McKee. 2012. Chronic traumatic encephalopathy in blast-exposed military veterans and a blast neurotrauma mouse model. Science Translational Medicine 4(134):1-16.
Grafman, J., A. M. Salazar, H. Weingartner, and D. Amin. 1986. Face memory and discrimination: An analysis of the persistent effects of penetrating brain wounds. International Journal of Neuroscience 29(1-2):125-139.
Grafman, J., B. S. Jonas, A. Martin, A. M. Salazar, H. Weingartner, C. Ludlow, M. A. Smutok, and S. C.
Vance. 1988. Intellectual function following penetrating head injury in Vietnam veterans. Brain 111(Pt 1):169-184. Grafman, J., B. Jonas, and A. Salazar. 1990. Wisconsin card sorting test performance based on location and size of neuroanatomical lesion in Vietnam veterans with penetrating head injury. Perceptual and Motor Skills 71(3 Pt 2):1120-1122.
Graham, D. P., and A. L. Cardon. 2008. An update on substance use and treatment following traumatic brain injury. Annals of the New York Academy of Sciences 1141:148-162.
Gray, M. J., E. E. Bolton, and B. T. Litz. 2004. A longitudinal analysis of PTSD symptom course: Delayed-onset PTSD in Somalia peacekeepers. Journal of Consulting and Clinical Psychology 72(5):909-913.
Green, B. L., M. C. Grace, J. D. Lindy, and G. C. Gleser. 1990. War stressors and symptom persistence in posttraumatic stress disorder. Journal of Anxiety Disorders 4(1):31-39.
Grieger, T. A., S. J. Cozza, R. J. Ursano, C. W. Hoge, P. E. Martinez, C. C. Engel, and H. J. Wain. 2006. Posttraumatic stress disorder and depression in battle-injured soldiers. American Journal of Psychiatry 163(10):1777-1783.
Groswasser, Z., G. Reider, II, K. Schwab, A. K. Ommaya, A. Pridgen, H. R. Brown, R. Cole, and A. M. Salazar. 2002. Quantitative imaging in late TBI. Part II: Cognition and work after closed and penetrating head injury: A report of the Vietnam Head Injury study. Brain Injury 16(8):681-690.
Grubaugh, A. L., J. Monnier, K. M. Magruder, R. G. Knapp, and B. C. Frueh. 2006. Female veterans seeking medical care at Veterans Affairs primary care clinics: Psychiatric and medical illness burden and service use. Women and Health 43(3):41-62.
Guerra, V. S., and P. S. Calhoun. 2011. Examining the relation between posttraumatic stress disorder and suicidal ideation in an OEF/OIF veteran sample. Journal of Anxiety Disorders 25(1):12-18.
Gurvits, T. V., L. J. Metzger, N. B. Lasko, P. A. Cannistraro, A. S. Tarhan, M. W. Gilbertson, S. P. Orr, A. M. Charbonneau, M. M. B. S. Wedig, and R. K. M. D. Pitman. 2006. Subtle neurologic compromise as a vulnerability factor for combat-related posttraumatic stress disorder: Results of a twin study. Archives of General Psychiatry 63(5):571-576.
Hankin, C. S., K. M. Skinner, L. M. Sullivan, D. R. Miller, S. Frayne, and T. J. Tripp. 1999. Prevalence of depressive and alcohol abuse symptoms among women VA outpatients who report experiencing sexual assault while in the military. Journal of Traumatic Stress 12(4):601-612.
Haskell, S. G., C. A. Brandt, E. E. Krebs, M. Skanderson, R. D. Kerns, and J. L. Goulet. 2009. Pain among veterans of Operations Enduring Freedom and Iraqi Freedom: Do women and men differ? Pain Medicine 10(7):1167-1173.
Haskell, S. G., K. S. Gordon, K. Mattocks, M. Duggal, J. Erdos, A. Justice, and C. A. Brandt. 2010. Gender differences in rates of depression, PTSD, pain, obesity, and military sexual trauma among Connecticut war veterans of Iraq and Afghanistan. Journal of Women’s Health 19(2):267-271.
Hassija, C. M., M. Jakupcak, S. Maguen, and J. C. Shipherd. 2012. The influence of combat and interpersonal trauma on PTSD, depression, and alcohol misuse in US Gulf War and OEF/OIF women veterans. Journal of Traumatic Stress 25(2):216-219.
Hawkins, E. J., G. T. Lapham, D. R. Kivlahan, and K. A. Bradley. 2010. Recognition and management of alcohol misuse in OEF/OIF and other veterans in the VA: A cross-sectional study. Drug and Alcohol Dependence 109(1-3):147-153.
Heitger, M. H., R. D. Jones, C. M. Frampton, M. W. Ardagh, and T. J. Anderson. 2007. Recovery in the first year after mild head injury: Divergence of symptom status and self-perceived quality of life. Journal of Rehabilitation Medicine 39(8):612-621.
Heltemes, K. J., A. L. Dougherty, A. J. MacGregor, and M. R. Galarneau. 2011. Alcohol abuse disorders among US service members with mild traumatic brain injury. Military Medicine 176:147-150.
Highfill-McRoy, R. M., G. E. Larson, S. Booth-Kewley, and C. F. Garland. 2010. Psychiatric diagnoses and punishment for misconduct: The effects of PTSD in combat-deployed marines. BMC Psychiatry 10:88.
Hill, J. J., 3rd, B. H. Mobo, Jr., and M. R. Cullen. 2009. Separating deployment-related traumatic brain injury and posttraumatic stress disorder in veterans: Preliminary findings from the Veterans Affairs traumatic brain injury screening program. American Journal of Physical Medicine and Rehabilitation 88(8):605-614.
Himmelfarb, N., D. Yaeger, and J. Mintz. 2006. Posttraumatic stress disorder in female veterans with military and civilian sexual trauma. Journal of Traumatic Stress 19(6):837-846.
Hirsch, K. A. 2009. Sexual dysfunction in male Operation Enduring Freedom/Operation Iraqi Freedom patients with severe post-traumatic stress disorder. Military Medicine 174(5):520-522.
Hoge, C. W., C. A. Castro, S. C. Messer, D. McGurk, D. I. Cotting, and R. L. Koffman. 2004a. Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. New England Journal of Medicine 351(1):13-22.
Hoge, C. W., K. Wright, P. Bliese, A. Adler, and J. Thomas. 2004b. Prevalence and Screening of Mental Health Problems Among US Combat Soldiers Pre- and Post- Deployment. Silver Spring, MD: Walter Reed Army Institute of Research.
Hoge, C. W., J. L. Auchterlonie, and C. S. Milliken. 2006. Mental health problems, use of mental health services, and attrition from military service after returning from deployment to Iraq or Afghanistan. Journal of the American Medical Association 295(9):1023-1032.
Hoge, C. W., A. Terhakopian, C. A. Castro, S. C. Messer, and C. C. Engel. 2007. Association of posttraumatic stress disorder with somatic symptoms, health care visits, and absenteeism among Iraq war veterans. American Journal of Psychiatry 164(1):150-153.
Hoge, C. W., D. McGurk, J. Thomas, A. L. Cox, C. C. Engel, and C. A. Castro. 2008. Mild traumatic brain injury in US soldiers returning from Iraq. New England Journal of Medicine 358(5):453-463.
Holbrook, T. L., D. B. Hoyt, M. B. Stein, and W. J. Sieber. 2002. Gender differences in long-term posttraumatic stress disorder outcomes after major trauma: Women are at higher risk of adverse outcomes than men. Journal of Trauma—Injury, Infection and Critical Care 53(5):882-888.
Holsinger, T., D. C. Steffens, C. Phillips, M. J. Helms, R. J. Havlik, J. C. S. Breitner, J. M. Guralnik, and B. L. Plassman. 2002. Head injury in early adulthood and the lifetime risk of depression. Archives of General Psychiatry 59(1):17-22.
Horner, M. D., P. L. Ferguson, A. W. Selassie, L. A. Labbate, K. Kniele, and J. D. Corrigan. 2005. Patterns of alcohol use 1 year after traumatic brain injury: A population-based, epidemiological study. Journal of the International Neuropsychological Society 11(3):322-330.
Hyman, J., R. Ireland, L. Frost, and L. Cottrell. 2012. Suicide incidence and risk factors in an active duty US military population. American Journal of Public Health 102(1 Suppl):S138-S146.
Hyun, J. K., J. Pavao, and R. Kimerling. 2009. Military sexual trauma. PTSD Research Quarterly 20(2):1-8.
Ilgen, M. A., K. R. Conner, M. Valenstein, K. Austin, and F. C. Blow. 2010. Violent and nonviolent suicide in veterans with substance-use disorders. Journal of Studies on Alcohol and Drugs 71(4):473-479.
Inman, D. J., S. M. Silver, and K. Doghramji. 1990. Sleep disturbance in post-traumatic stress disorder: A comparison with non-PTSD insomnia. Journal of Traumatic Stress 3(3):429-437.
IOM (Institute of Medicine). 2006. Posttraumatic Stress Disorder: Diagnosis and Assessment. Washington, DC: The National Academies Press.
———. 2008a. Gulf War and Health, Volume 6: Physiologic, Psychologic, and Psychosocial Effects of Deployment-related Stress. Washington, DC: The National Academies Press.
———. 2008b. Treatment of Posttraumatic Stress Disorder: An Assessment of the Evidence. Washington, DC: The National Academies Press.
———. 2009. Gulf War and Health, Volume 7: Long-Term Consequences of Traumatic Brain Injury. Washington, DC: The National Academies Press.
———. 2010. Returning Home from Iraq and Afghanistan: Preliminary Assessment of Readjustment Needs of Veterans, Service Members, and their Families. Washington, DC: The National Academies Press.
Irwin, C., S. A. Falsetti, R. B. Lydiard, J. C. Ballenger, C. D. Brock, and W. Brener. 1996. Comorbidity of posttraumatic stress disorder and irritable bowel syndrome. Journal of Clinical Psychiatry 57(12):576-578.
Iverson, K. M., A. M. Hendricks, R. Kimerling, M. Krengel, M. Meterko, K. L. Stolzmann, E. Baker, T. K. Pogoda, J. J. Vasterling, and H. L. Lew. 2011. Psychiatric diagnoses and neurobehavioral symptom severity among OEF/OIF VA patients with deployment-related traumatic brain injury: A gender comparison. Women’s Health Issues 21(4 Suppl):S210-S217.
Jacobson, I. G., M. A. Ryan, T. J. Hooper, T. C. Smith, P. J. Amoroso, E. J. Boyko, G. D. Gackstetter, T. S. Wells, and N. S. Bell. 2008. Alcohol use and alcohol-related problems before and after military combat deployment. Journal of the American Medical Association 300(6):663-675.
Jakupcak, M., D. Conybeare, L. Phelps, S. Hunt, H. A. Holmes, B. Felker, M. Klevens, and M. E. McFall. 2007. Anger, hostility, and aggression among Iraq and Afghanistan war veterans reporting PTSD and subthreshold PTSD. Journal of Traumatic Stress 20(6):945-954.
Jakupcak, M., J. Cook, Z. Imel, A. Fontana, R. Rosenheck, and M. McFall. 2009. Posttraumatic stress disorder as a risk factor for suicidal ideation in Iraq and Afghanistan war veterans. Journal of Traumatic Stress 22(4):303-306.
Jakupcak, M., M. T. Tull, M. J. McDermott, D. Kaysen, S. Hunt, and T. Simpson. 2010a. PTSD symptom clusters in relationship to alcohol misuse among Iraq and Afghanistan war veterans seeking postdeployment VA health care. Addictive Behaviors 35(9):840-843.
Jakupcak, M., S. Vannoy, Z. Imel, J. W. Cook, A. Fontana, R. Rosenheck, and M. McFall. 2010b. Does PTSD moderate the relationship between social support and suicide risk in Iraq and Afghanistan war veterans seeking mental health treatment? Depression and Anxiety 27(11):1001-1005.
Jakupcak, M., K. D. Hoerster, A. Varra, S. Vannoy, B. Felker, and S. Hunt. 2011. Hopelessness and suicidal ideation in Iraq and Afghanistan war veterans reporting subthreshold and threshold posttraumatic stress disorder. Journal of Nervous and Mental Disease 199(4):272-275.
Jones, E., A. Thomas, and S. Ironside. 2007. Shell shock: An outcome study of a first world war “PIE” unit. Psychological Medicine 37(2):215-223.
Jordan, B. K., C. R. Marmar, J. A. Fairbank, W. E. Schlenger, R. A. Kulka, R. L. Hough, and D. S. Weiss. 1992. Problems in families of male Vietnam veterans with posttraumatic stress disorder. Journal of Consulting and Clinical Psychology 60(6):916-926.
Jorge, R. E., R. G. Robinson, D. Moser, A. Tateno, B. Crespo-Facorro, and S. Arndt. 2004. Major depression following traumatic brain injury. Archives of General Psychiatry 61(1):42-50.
Jorge, R. E., S. E. Starkstein, S. Arndt, D. Moser, B. Crespo-Facorro, and R. G. Robinson. 2005. Alcohol misuse and mood disorders following traumatic brain injury. Archives of General Psychiatry 62(7):742-749.
Kang, H. K., and T. A. Bullman. 2009. Is there an epidemic of suicides among current and former US military personnel? Annals of Epidemiology 19(10):757-760.
Kaplan, M. S., B. H. McFarland, N. Huguet, and M. Valenstein. 2012. Suicide risk and precipitating circumstances among young, middle-aged, and older male veterans. American Journal of Public Health 102(S1):S131-S137.
Kehle, S. M., A. G. Ferrier-Auerbach, L. A. Meis, P. A. Arbisi, C. R. Erbes, and M. A. Polusny. 2011a. Predictors of postdeployment alcohol use disorders in National Guard soldiers deployed to Operation Iraqi Freedom. Psychology of Addictive Behaviors 26(1):42-50.
Kehle, S. M., M. K. Reddy, A. G. Ferrier-Auerbach, C. R. Erbes, P. A. Arbisi, and M. A. Polusny. 2011b. Psychiatric diagnoses, comorbidity, and functioning in National Guard troops deployed to Iraq. Journal of Psychiatric Research 45(1):126-132.
Kennedy, J. E., M. S. Jaffee, G. A. Leskin, J. W. Stokes, F. O. Leal, and P. J. Fitzpatrick. 2007. Posttraumatic stress disorder and posttraumatic stress disorder-like symptoms and mild traumatic brain injury. Journal of Rehabilitation Research and Development 44(7):895-920.
Kennedy, J. E., F. O. Leal, J. D. Lewis, M. A. Cullen, and R. R. Amador. 2010. Posttraumatic stress symptoms in OIF/OEF service members with blast-related and non-blast-related mild TBI. NeuroRehabilitation 26(3):223-231.
Kimerling, R., K. Gima, M. W. Smith, A. Street, and S. Frayne. 2007. The Veterans Health Administration and military sexual trauma. American Journal of Public Health 97(12):2160-2166.
Kimerling, R., A. E. Street, J. Pavao, M. W. Smith, R. C. Cronkite, T. H. Holmes, and S. M. Frayne. 2010. Military-related sexual trauma among veterans health administration patients returning from Afghanistan and Iraq. American Journal of Public Health 100(8):1409-1412.
Kinder, L. S., K. A. Bradley, W. J. Katon, E. Ludman, M. B. McDonell, and C. L. Bryson. 2008. Depression, posttraumatic stress disorder, and mortality. Psychosomatic Medicine 70(1):20-26.
Kline, A., M. Falca-Dodson, B. Sussner, D. S. Ciccone, H. Chandler, L. Callahan, and M. Losonczy. 2010. Effects of repeated deployment to Iraq and Afghanistan on the health of New Jersey Army National Guard troops: Implications for military readiness. American Journal of Public Health 100(2):276-283.
Kline, A., D. S. Ciccone, M. Falca-Dodson, C. M. Black, and M. Losonczy. 2011. Suicidal ideation among National Guard troops deployed to Iraq: The association with postdeployment readjustment problems. Journal of Nervous and Mental Disease 199(12):914-920.
Koenen, K. C., T. E. Moffitt, R. Poulton, J. Martin, and A. Caspi. 2007. Early childhood factors associated with the development of post-traumatic stress disorder: Results from a longitudinal birth cohort. Psychological Medicine 37(2):181-192.
Koenigs, M., and J. Grafman. 2009. Posttraumatic stress disorder: The role of medial prefrontal cortex and amygdala. Neuroscientist 15(5):540-548.
Kolkow, T. T., J. L. Spira, J. S. Morse, and T. A. Grieger. 2007. Post-traumatic stress disorder and depression in health care providers returning from deployment to Iraq and Afghanistan. Military Medicine 172(5):451-455.
Koso, M., and S. Hansen. 2006. Executive function and memory in posttraumatic stress disorder: A study of Bosnian war veterans. European Psychiatry 21(3):167-173.
Kremen, W. S., K. C. Koenen, C. Boake, S. Purcell, S. A. Eisen, C. E. Franz, M. T. Tsuang, and M. J. Lyons. 2007. Pretrauma cognitive ability and risk for posttraumatic stress disorder: A twin study. Archives of General Psychiatry 64(3):361-368.
Kulka, R. A., W. E. Schlenger, J. A. Fairbank, R. L. Hough, B. K. Jordan, C. R. Marmar, D. S. Weiss, and D. A. Grady. 1990. Trauma and the Vietnam War Generation: Report of Findings from the National Vietnam Veterans Readjustment Study. New York: Routledge.
Lande, R. G., B. A. Marin, A. S. Chang, and G. R. Lande. 2008. Survey of alcohol use in the US Army. Journal of Addictive Diseases 27(3):115-121.
Lane, M. E., L. L. Hourani, R. M. Bray, and J. Williams. 2012. Prevalence of perceived stress and mental health indicators among reserve-component and active-duty military personnel. American Journal of Public Health 102(6):1213-1220.
Langhinrichsen-Rohling, J., J. D. Snarr, A. M. Slep, R. E. Heyman, and H. M. Foran. 2011. Risk for suicidal ideation in the US Air Force: An ecological perspective. Journal of Consulting and Clinical Psychology 79(5):600-612.
Lannsjo, M., J. L. af Geijerstam, U. Johansson, J. Bring, and J. Borg. 2009. Prevalence and structure of symptoms at 3 months after mild traumatic brain injury in a national cohort. Brain Injury 23(3):213-219.
Lapierre, C. B., A. F. Schwegler, and B. J. LaBauve. 2007. Posttraumatic stress and depression symptoms in soldiers returning from combat operations in Iraq and Afghanistan. Journal of Traumatic Stress 20(6):933-943.
Larson, G. E., P. S. Hammer, T. L. Conway, E. A. Schmied, M. R. Galarneau, P. Konoske, J. A. Webb-Murphy, K. J. Schmitz, N. Edwards, and D. C. Johnson. 2011. Predeployment and in-theater diagnoses of American military personnel serving in Iraq. Psychiatric Services 62(1):15-21.
Lemaire, C. M., and D. P. Graham. 2011. Factors associated with suicidal ideation in OEF/OIF veterans. Journal of Affective Disorders 130(1-2):231-238.
Letz, R. 1990. The Neurobehavioral Evaluation System (NES): An international effort. In Advances in Neurobehavioral Toxicology: Applications in Environmental and Occupational Health, edited by B. L. Johnson, W. K. Anger, A. Durao and C. Xintaras. Chelsea, MI: Lewis Publishers.
Levin, H. S., H. E. Gary, Jr., H. M. Eisenberg, R. M. Ruff, J. T. Barth, J. Kreutzer, W. M. High, Jr., S. Portman, M. A. Foulkes, J. A. Jane, A. Marmarou, and L. F. Marshall. 1990. Neurobehavioral outcome 1 year after severe head injury: Experience of the traumatic coma data bank. Journal of Neurosurgery 73:699-709.
Lewis, V., M. Creamer, and S. Failla. 2009. Is poor sleep in veterans a function of post-traumatic stress disorder? Military Medicine 174(9):948-951.
Lipari, R. N., P. J. Cook, L. M. Rock, and K. Matos. 2008. 2006 Gender Relations Survey of Active Duty Members. Arlington, VA: Defense Manpower Data Center.
Logan, J., N. A. Skopp, D. Karch, M. A. Reger, and G. A. Gahm. 2012. Characteristics of suicides among US Army active duty personnel in 17 US states from 2005 to 2007. American Journal of Public Health 102(S1):S40-S44.
Luethcke, C. A., C. J. Bryan, C. E. Morrow, and W. C. Isler. 2011. Comparison of concussive symptoms, cognitive performance, and psychological symptoms between acute blast-versus nonblast-induced mild traumatic brain injury. Journal of the International Neuropsychological Society 17(1):36-45.
Luxton, D. D., N. A. Skopp, and S. Maguen. 2010. Gender differences in depression and PTSD symptoms following combat exposure. Depression and Anxiety 27(11):1027-1033.
Macey, T. A., B. J. Morasco, J. P. Duckart, and S. K. Dobscha. 2011. Patterns and correlates of prescription opioid use in OEF/OIF veterans with chronic noncancer pain. Pain Medicine 12(10):1502-1509.
MacGregor, A. J., R. A. Shaffer, A. L. Dougherty, M. R. Galarneau, R. Raman, D. G. Baker, S. P. Lindsay, B. A. Golomb, and K. S. Corson. 2009. Psychological correlates of battle and nonbattle injury among Operation Iraqi Freedom veterans. Military Medicine 174(3):224-231.
MacGregor, A. J., P. P. Han, A. L. Dougherty, and M. R. Galarneau. 2012. Effect of dwell time on the mental health of US military personnel with multiple combat tours. American Journal of Public Health 102(1 Suppl):S55-S59.
Magruder, K. M., B. C. Frueh, R. G. Knapp, M. R. Johnson, J. A. Vaughan Iii, T. C. Carson, D. A. Powell, and R. Hebert. 2004. PTSD symptoms, demographic characteristics, and functional status among veterans treated in VA primary care clinics. Journal of Traumatic Stress 17(4):293-301.
Magruder, K. M., B. C. Frueh, R. G. Knapp, L. Davis, M. B. Hamner, R. H. Martin, P. B. Gold, and G. W. Arana. 2005. Prevalence of posttraumatic stress disorder in Veterans Affairs primary care clinics. General Hospital Psychiatry 27(3):169-179.
Maguen, S., L. Ren, J. O. Bosch, C. R. Marmar, and K. H. Seal. 2010. Gender differences in mental health diagnoses among Iraq and Afghanistan veterans enrolled in Veterans Affairs health care. American Journal of Public Health 100(12):2450-2456.
Maguen, S., D. D. Luxton, N. A. Skopp, G. A. Gahm, M. A. Reger, T. J. Metzler, and C. R. Marmar. 2011a. Killing in combat, mental health symptoms, and suicidal ideation in Iraq war veterans. Journal of Anxiety Disorders 25(4):563-567.
Maguen, S., D. D. Luxton, N. A. Skopp, and E. Madden. 2011b. Gender differences in traumatic experiences and mental health in active duty soldiers redeployed from Iraq and Afghanistan. Journal of Psychiatric Research 46(3):311-316 Maguen, S., D. S. Vogt, L. A. King, D. W. King, B. T. Litz, S. J. Knight, and C. R. Marmar. 2011c. The impact of killing on mental health symptoms in Gulf War veterans. Psychological Trauma: Theory, Research, Practice, and Policy 3(1):21-26.
Maguen, S., B. Cohen, L. Ren, J. Bosch, R. Kimerling, and K. Seal. 2012. Gender differences in military sexual trauma and mental health diagnoses among Iraq and Afghanistan veterans with posttraumatic stress disorder. Womens Health Issues 22(1):e61-e66.
Martin, S. L., D. A. Gibbs, R. E. Johnson, K. Sullivan, M. Clinton-Sherrod, J. L. Walters, and E. D. Rentz. 2010. Substance use by soldiers who abuse their spouses. Violence Against Women 16(11):1295-1310.
Martland, H. S. 1928. Punch drunk. Journal of the American Medical Association 91:1103-1107.
Marx, B. P., K. Brailey, S. P. Proctor, and E. al. 2009. Association of time since deployment, combat intensity, and posttraumatic stress symptoms with neuropsychological outcomes following Iraq war deployment. Archives of General Psychiatry 66(9):996-1004.
Mason, J., S. Southwick, R. Yehuda, S. Wang, S. Riney, D. Bremner, D. Johnson, H. Lubin, D. Blake, G. Zhou, et al. 1994. Elevation of serum free triiodothyronine, total triiodothyronine, thyroxine-binding globulin, and total thyroxine levels in combat-related posttraumatic stress disorder. Archives of General Psychiatry 51(8):629-641.
Mattiko, M. J., K. L. Olmsted, J. M. Brown, and R. M. Bray. 2011. Alcohol use and negative consequences among active duty military personnel. Addictive Behaviors 36(6):608-614.
McAllister, T. W. 2011. Neurobiological consequences of traumatic brain injury. Dialogues in Clinical Neuroscience 13(3):287-300.
McAllister, T. W., and M. B. Stein. 2010. Effects of psychological and biomechanical trauma on brain and behavior. Annals of the New York Academy of Sciences 1208:46-57.
McCarthy, J. F., M. Valenstein, H. M. Kim, M. Ilgen, K. Zivin, and F. C. Blow. 2009. Suicide mortality among patients receiving care in the Veterans Health Administration health system. American Journal of Epidemiology 169(8):1033-1038.
McCarthy, J. F., F. C. Blow, R. V. Ignacio, M. A. Ilgen, K. L. Austin, and M. Valenstein. 2012. Suicide among patients in the Veterans Affairs health system: Rural–urban differences in rates, risks, and methods. American Journal of Public Health 102(S1):S111-S117.
McCrea, M., G. L. Iverson, T. W. McAllister, T. A. Hammeke, M. R. Powell, W. B. Barr, and J. P. Kelly. 2009. An integrated review of recovery after mild traumatic brain injury (mTBI): Implications for clinical management. Clinical Neuropsychologist 23(8):1368-1390.
McDevitt-Murphy, M. E., J. L. Williams, K. L. Bracken, J. A. Fields, C. J. Monahan, and J. G. Murphy. 2010. PTSD symptoms, hazardous drinking, and health functioning among US OEF and OIF veterans presenting to primary care. Journal of Traumatic Stress 23(1):108-111.
McKee, A. C., R. C. Cantu, C. J. Nowinski, E. T. Hedley-Whyte, B. E. Gavett, A. E. Budson, V. E. Santini, H. S. Lee, C. A. Kubilus, and R. A. Stern. 2009. Chronic traumatic encephalopathy in athletes: Progressive tauopathy after repetitive head injury. Journal of Neuropathology and Experimental Neurology 68(7):709-735.
McKee, A. C., B. E. Gavett, R. A. Stern, C. J. Nowinski, R. C. Cantu, N. W. Kowall, D. P. Perl, E. T. Hedley-Whyte, B. Price, C. Sullivan, P. Morin, H. S. Lee, C. A. Kubilus, D. H. Daneshvar, M. Wulff, and A. E. Budson. 2010. TDP-43 proteinopathy and motor neuron disease in chronic traumatic encephalopathy. Journal of Neuropathology and Experimental Neurology 69(9):918-929.
McLay, R. N., W. P. Klam, and S. L. Volkert. 2010. Insomnia is the most commonly reported symptom and predicts other symptoms of post-traumatic stress disorder in US service members returning from military deployments. Military Medicine 175(10):759-762.
Mellman, T. A., R. Kulick-Bell, L. E. Ashlock, and B. Nolan. 1995. Sleep events among veterans with combat-related posttraumatic stress disorder. American Journal of Psychiatry 152(1):110-115.
Mellman, T. A., B. Nolan, J. Hebding, R. Kulick-Bell, and R. Dominguez. 1997. A polysomnographic comparison of veterans with combat-related PTSD, depressed men, and non-ill controls. Sleep 20(1):46-51.
MHAT-II. 2005. Mental Health Advisory Team (MHAT-II): Operation lraqi Freedom (01F-11) Washington, DC: Office of the Surgeon General, United States Army Medical Command, Office of the Surgeon Multinational Force-Iraq.
MHAT-III. 2006. Mental Health Advisory Team (MHAT III): Operation Iraqi Freedom 04-06. Washington, DC: Office of The Surgeon General, United States Army Medical Command, Office of the Surgeon Multinational Force-Iraq.
MHAT-IV. 2006. Mental Health Advisory Team (MHAT IV): Operation Iraqi Freedom 05-07 Final Report. Washington, DC: Office of the Surgeon General, United States Army Medical Command, Office of the Surgeon Multinational Force-Iraq.
MHAT-V. 2008. Mental Health Advisory Team (MHAT-V) Operation Iraqi Freedom 06-08: Iraq; Operation Enduring Freedom 8: Afghanistan. Washington, DC: Office of the Surgeon General, United States Army Medical Command, Office of the Surgeon Multinational Force-Iraq.
MHAT-VI. 2009. Operation Iraqi Freedom 07-09. Mental Health Advisory Team (MHAT-VI). Washington, DC: Office of The Surgeon General, US Army Medical Command, Office of the Surgeon Multinational Force-Iraq.
MHAT-VII. 2011. Joint Mental Health Advisory Team 7 (J-MHAT 7) Operation Enduring Freedom 2010. Washington, DC: Office of the Surgeon General, United States Army Medical Command, Office of the Command Surgeon HQ, USCENTCOM, Office of the Command Surgeon U.S. Forces Afghanistan.
Mickeviciene, D., H. Schrader, K. Nestvold, D. Surkiene, R. Kunickas, L. J. Stovner, and T. Sand. 2002. A controlled historical cohort study on the post-concussion syndrome. European Journal of Neurology 9(6):581-587.
Mickeviciene, D., H. Schrader, D. Obelieniene, D. Surkiene, R. Kunickas, L. J. Stovner, and T. Sand. 2004. A controlled prospective inception cohort study on the post-concussion syndrome outside the medicolegal context. European Journal of Neurology 11(6):411-419.
Milliken, C. S., J. L. Auchterlonie, and C. W. Hoge. 2007. Longitudinal assessment of mental health problems among active and reserve component soldiers returning from the Iraq war. Journal of the American Medical Association 298(18):2141-2148.
Monson, C. M., C. T. Taft, and S. J. Fredman. 2009. Military-related PTSD and intimate relationships: From description to theory-driven research and intervention development. Clinical Psychology Review 29(8):707-714.
Murdoch, M., J. B. Pryor, M. A. Polusny, and G. D. Gackstetter. 2007. Functioning and psychiatric symptoms among military men and women exposed to sexual stressors. Military Medicine 172(7):718-725.
Nash, D. L., J. Wilkinson, B. Paradis, S. Kelley, A. Naseem, and K. M. Grant. 2011. Trauma and substance use disorders in rural and urban veterans. Journal of Rural Health 27(2):151-158.
Nazarian, D., R. Kimerling, and S. M. Frayne. 2012. Posttraumatic stress disorder, substance use disorders, and medical comorbidity among returning US veterans. Journal of Traumatic Stress 25(2):220-225.
Neylan, T. C., C. R. Marmar, T. J. Metzler, D. S. Weiss, D. F. Zatzick, K. L. Delucchi, R. M. Wu, and F. B. Schoenfeld. 1998. Sleep disturbances in the Vietnam generation: Findings from a nationally representative sample of male Vietnam veterans. American Journal of Psychiatry 155(7):929-933.
North, C. S., S. J. Nixon, S. Shariat, S. Mallonee, J. C. McMillen, E. L. Spitznagel, and E. M. Smith. 1999. Psychiatric disorders among survivors of the Oklahoma City bombing. Journal of the American Medical Association 282(8):755-762.
Nunnink, S. E., G. Goldwaser, N. Afari, C. M. Nievergelt, and D. G. Baker. 2010. The role of emotional numbing in sexual functioning among veterans of the Iraq and Afghanistan wars. Military Medicine 175(6):424-428.
Oddy, M., M. Humphrey, and D. Uttley. 1978. Subjective impairment and social recovery after closed head injury. Journal of Neurology, Neurosurgery, and Psychiatry 41(7):611-616.
Office of National Drug Control Policy. 2010. Study shows increased misuse of prescription drugs in military. ONDCP Update 1(2):1-4.
Office of the Army Surgeon General. 2010. Pain Management Task Force: Final Report. Washington, DC: Department of Defense.
Omalu, B. I., S. T. DeKosky, R. L. Minster, M. I. Kamboh, R. L. Hamilton, and C. H. Wecht. 2005. Chronic traumatic encephalopathy in a National Football League player. Neurosurgery 57(1):128-134.
Omalu, B. I., S. T. DeKosky, R. L. Hamilton, R. L. Minster, M. I. Kamboh, A. M. Shakir, and C. H. Wecht. 2006. Chronic traumatic encephalopathy in a National Football League player: Part II. Neurosurgery 59(5):1086-1092.
Omalu, B. I., J. Bailes, J. L. Hammers, and R. P. Fitzsimmons. 2010. Chronic traumatic encephalopathy, suicides and parasuicides in professional american athletes: The role of the forensic pathologist. American Journal of Forensic Medicine and Pathology 31(2):130-132.
Omalu, B., J. Bailes, R. L. Hamilton, M. I. Kamboh, J. Hammers, M. Case, and R. Fitzsimmons. 2011a. Emerging histomorphologic phenotypes of chronic traumatic encephalopathy in American athletes. Neurosurgery 69(1):173-183.
Omalu, B., J. L. Hammers, J. Bailes, R. L. Hamilton, M. I. Kamboh, G. Webster, and R. P. Fitzsimmons. 2011b. Chronic traumatic encephalopathy in an Iraqi war veteran with posttraumatic stress disorder who committed suicide. Neurosurgical Focus 31(5):E3.
Op den Velde, W., J. E. Hovens, P. G. Aarts, E. Frey-Wouters, P. R. Falger, H. Van Duijn, and J. H. De Groen. 1996. Prevalence and course of posttraumatic stress disorder in dutch veterans of the civilian resistance during World War II: An overview. Psychological Reports 78(2):519-529.
Otis, J. D., K. Gregor, C. Hardway, J. Morrison, E. Scioli, and K. Sanderson. 2010. An examination of the co-morbidity between chronic pain and posttraumatic stress disorder on US veterans. Psychological Services 7(3):126-135.
O’Toole, B. I., R. P. Marshall, R. J. Schureck, and M. Dobson. 1998. Posttraumatic stress disorder and comorbidity in Australian Vietnam veterans: Risk factors, chronicity and combat. Australian and New Zealand Journal of Psychiatry 32(1):32-42.
Ouimette, P. C., J. Wolfe, and K. R. Chrestman. 1996. Characteristics of posttraumatic stress disorderalcohol abuse comorbidity in women. Journal of Substance Abuse 8(3):335-346.
Ouimette, P., R. Cronkite, B. R. Henson, A. Prins, K. Gima, and R. H. Moos. 2004. Posttraumatic stress disorder and health status among female and male medical patients. Journal of Traumatic Stress 17(1):1-9.
Palatini, P., and S. Julius. 1997. Heart rate and the cardiovascular risk. Journal of Hypertension 15(1):3-17.
Peterson, A. L., V. Wong, M. F. Haynes, A. C. Bush, and J. E. Schillerstrom. 2010. Documented combatrelated mental health problems in military noncombatants. Journal of Traumatic Stress 23(6):674-681.
Phillips, C. J., C. A. Leardmann, G. R. Gumbs, and B. Smith. 2010. Risk factors for posttraumatic stress disorder among deployed US male Marines. BMC Psychiatry 10:52.
Picchioni, D., O. A. Cabrera, D. McGurk, J. L. Thomas, C. A. Castro, T. J. Balkin, P. D. Bliese, and C. W. Hoge. 2010. Sleep symptoms as a partial mediator between combat stressors and other mental health symptoms in Iraq war veterans. Military Psychology 22(3):340-355.
Pietrzak, R. H., M. B. Goldstein, J. C. Malley, D. C. Johnson, and S. M. Southwick. 2009a. Subsyndromal posttraumatic stress disorder is associated with health and psychosocial difficulties in veterans of Operations Enduring Freedom and Iraqi Freedom. Depression and Anxiety 26(8):739-744.
Pietrzak, R. H., D. C. Johnson, M. B. Goldstein, J. C. Malley, A. J. Rivers, C. A. Morgan, and S. M. Southwick. 2009b. Psychosocial buffers of traumatic stress, depressive symptoms, and psychosocial difficulties in veterans of Operations Enduring Freedom and Iraqi Freedom: The role of resilience, unit support, and postdeployment social support. Journal of Affective Disorders 120(1-3).
Pietrzak, R. H., D. C. Johnson, M. B. Goldstein, J. C. Malley, and S. M. Southwick. 2009c. Psychological resilience and postdeployment social support protect against traumatic stress and depressive symptoms in soldiers returning from Operations Enduring Freedom and Iraqi Freedom. Depression and Anxiety 26(8):745-751.
Pietrzak, R. H., M. B. Goldstein, J. C. Malley, A. J. Rivers, D. C. Johnson, and S. M. Southwick. 2010. Risk and protective factors associated with suicidal ideation in veterans of Operations Enduring Freedom and Iraqi Freedom. Journal of Affective Disorders 123(1-3):102-107.
Pietrzak, R. H., A. R. Russo, Q. Ling, and S. M. Southwick. 2011a. Suicidal ideation in treatment-seeking veterans of Operations Enduring Freedom and Iraqi Freedom: The role of coping strategies, resilience, and social support. Journal of Psychiatric Research 45(6):720-726.
Pietrzak, R. H., J. M. Whealin, R. L. Stotzer, M. B. Goldstein, and S. M. Southwick. 2011b. An examination of the relation between combat experiences and combat-related posttraumatic stress disorder in a sample of connecticut OEF-OIF veterans. Journal of Psychiatric Research 45(12):1579-1584.
Pietrzak, R. H., R. B. Goldstein, S. M. Southwick, and B. F. Grant. 2012. Psychiatric comorbidity of full and partial posttraumatic stress disorder among older adults in the United States: Results from wave 2 of the National Epidemiologic Survey on alcohol and related conditions. American Journal of Geriatric Psychiatry 20(5):380-390.
Pittman, J. O., A. A. Goldsmith, J. A. Lemmer, M. T. Kilmer, and D. G. Baker. 2012. Post-traumatic stress disorder, depression, and health-related quality of life in OEF/OIF veterans. Quality of Life Research: An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation 21(1):99-103.
Polusny, M. A., S. M. Kehle, N. W. Nelson, C. R. Erbes, P. A. Arbisi, and P. Thuras. 2011. Longitudinal effects of mild traumatic brain injury and posttraumatic stress disorder comorbidity on postdeployment outcomes in National Guard soldiers deployed to Iraq. Archives of General Psychiatry 68(1):79-89.
Port, C. L., B. Engdahl, and P. Frazier. 2001. A longitudinal and retrospective study of PTSD among older prisoners of war. American Journal of Psychiatry 158(9):1474-1479.
Porter, M. D. 2003. A 9-year controlled prospective neuropsychologic assessment of amateur boxing. Clinical Journal of Sport Medicine 13(6):339-352.
Porter, M. D., and P. A. Fricker. 1996. Controlled prospective neuropsychological assessment of active experienced amateur boxers. Clinical Journal of Sport Medicine 6(2):90-96.
Possemato, K., M. Wade, J. Andersen, and P. Ouimette. 2010. The impact of PTSD, depression, and substance use disorders on disease burden and health care utilization among OEF/OIF veterans. Psychological Trauma: Theory, Research, Practice, and Policy 2(3):218-223.
Ramchand, R., T. L. Schell, B. R. Karney, K. C. Osilla, R. M. Burns, and L. B. Caldarone. 2010. Disparate prevalence estimates of PTSD among service members who served in Iraq and Afghanistan: Possible explanations. Journal of Traumatic Stress 23(1):59-68.
Ramchand, R., J. Acosta, R. M. Burns, L. H. Jaycox, and C. G. Pernin. 2011. The War Within: Preventing Suicide in the US Military. Santa Monica, CA: RAND Corporation.
Ratcliff, J. J., A. I. Greenspan, F. C. Goldstein, A. Y. Stringer, T. Bushnik, F. M. Hammond, T. A. Novack, J. Whyte, and D. W. Wright. 2007. Gender and traumatic brain injury: Do the sexes fare differently? Brain Injury 21(10):1023-1030.
Rauch, S. A., T. Favorite, N. Giardino, C. Porcari, E. Defever, and I. Liberzon. 2010. Relationship between anxiety, depression, and health satisfaction among veterans with PTSD. Journal of Affective Disorders 121(1-2):165-168.
Raymont, V., A. Greathouse, K. Reding, R. Lipsky, A. Salazar, and J. Grafman. 2008. Demographic, structural and genetic predictors of late cognitive decline after penetrating head injury. Brain 131(Pt 2):543-558.
Reeves, D. L., K. Winter, S. LaCour, K. Raynsford, G. Kay, and T. Elsmore. 1992. Automated Neuropsychological Assessment Metrics Documentation: Vol. I. Test Administration Guide. Silver Spring, MD: Office of Military Performance Assessment Technology.
Reger, M. A., G. A. Gahm, R. D. Swanson, and S. J. Duma. 2009. Association between number of deployments to Iraq and mental health screening outcomes in US Army soldiers. Journal of Clinical Psychiatry 70(9):1266-1275.
Richardson, L. K., B. C. Frueh, and R. Acierno. 2010. Prevalence estimates of combat-related posttraumatic stress disorder: Critical review. Australian and New Zealand Journal of Psychiatry 44(1):4-19.
Riviere, L. A., A. Kendall-Robbins, D. McGurk, C. A. Castro, and C. W. Hoge. 2011. Coming home may hurt: Risk factors for mental ill health in US reservists after deployment in Iraq. British Journal of Psychiatry 198:136-142.
Roebuck-Spencer, T. M., A. S. Vincent, D. A. Twillie, B. W. Logan, C. M. Lopez, C. K. Friedl, S. J. Grate, R. E. Schlegel, and K. Gilliland. 2012. Cognitive change associated with self-reported mild traumatic brain injury sustained during the OEF/OIF conflicts. Clinical Neuropsychologist 26(3):473-489.
Rosen, G. M., R. L. Spitzer, and P. R. McHugh. 2008. Problems with the post-traumatic stress disorder diagnosis and its future in DSM-V. British Journal of Psychiatry 192(1):3-4.
Rosenheck, R., and A. Fontana. 1994. A model of homelessness among male veterans of the Vietnam war generation. American Journal of Psychiatry 151(3):421-427.
Rundell, J. R. 2006. Demographics of and diagnoses in Operation Enduring Freedom and Operation Iraqi Freedom personnel who were psychiatrically evacuated from the theater of operations. General Hospital Psychiatry 28(4):352-356.
Ruzich, M. J., J. C. Looi, and M. D. Robertson. 2005. Delayed onset of posttraumatic stress disorder among male combat veterans: A case series. American Journal of Geriatric Psychiatry 13(5):424-427.
Salazar, A. M., J. Grafman, S. Schlesselman, S. C. Vance, J. P. Mohr, M. Carpenter, P. Pevsner, C. Ludlow, and H. Weingartner. 1986. Penetrating war injuries of the basal forebrain: Neurology and cognition. Neurology 36(4):459-465.
SAMHSA (Substance Abuse and Mental Health Services Administration). 2011. Results from the 2010 National Survey on Drug Use and Health: Summary of National Findings. Rockville, MD: Substance Abuse and Mental Health Services Administration.
Samuelson, K. W., T. C. Neylan, T. J. Metzler, M. Lenoci, J. Rothlind, C. Henn-Haase, G. Choucroun, M. W. Weiner, and C. R. Marmar. 2006. Neuropsychological functioning in posttraumatic stress disorder and alcohol abuse. Neuropsychology 20(6):716-726.
Sandweiss, D., D. Slymen, C. LeardMann, B. Smith, M. White, E. Boyko, T. Hooper, G. Gackstetter, P. Amoroso, and T. Smith. 2011. Preinjury psychiatric status, injury severity, and postdeployment posttraumatic stress disorder. Archives of General Psychiatry 68(5):496-504.
Saulle, M., and B. D. Greenwald. 2012. Chronic traumatic encephalopathy: A review. Rehabilitation Research and Practice 1-9.
Savoca, E., and R. Rosenheck. 2000. The civilian labor market experiences of Vietnam-era veterans: The influence of psychiatric disorders. Journal of Mental Health Policy and Economics 3(4):199-207.
Schneiderman, A. I., E. R. Braver, and H. K. Kang. 2008. Underdstanding sequelae of injury mechanisms and mild traumatic brain injury incurred during the conflicts in Iraq and Afghanistan: Persistent postconcussive symptoms and posttraumatic stress disorder. American Journal of Epidemiology 167(12):1446-1452.
Schnurr, P. P., and C. A. Lunney. 2008. Exploration of gender differences in how quality of life relates to posttraumatic stress disorder in male and female veterans. Journal of Rehabilitation Research and Development 45(3):383-393.
Schnurr, P. P., A. Spiro, 3rd, and A. H. Paris. 2000. Physician-diagnosed medical disorders in relation to PTSD symptoms in older male military veterans. Health Psychology 19(1):91-97.
Schwab, K., J. Grafman, A. M. Salazar, and J. Kraft. 1993. Residual impairments and work status 15 years after penetrating head injury: Report from the Vietnam Head Injury study. Neurology 43(1):95-103.
Seal, K. H., D. Bertenthal, S. Maguen, K. Gima, A. Chu, and C. R. Marmar. 2008. Getting beyond “Don't Ask; Don't Tell”: An evaluation of US Veterans Administration postdeployment mental health screening of veterans returning from Iraq and Afghanistan. American Journal of Public Health 98(4):714-720.
Seal, K. H., T. J. Metzler, K. S. Gima, D. Bertenthal, S. Maguen, and C. R. Marmar. 2009. Trends and risk factors for mental health diagnoses among Iraq and Afghanistan veterans using Department of Veterans Affairs health care, 2002-2008. American Journal of Public Health 99(9):1651-1658.
Seal, K. H., G. Cohen, A. Waldrop, B. E. Cohen, S. Maguen, and L. Ren. 2011. Substance use disorders in Iraq and Afghanistan veterans in VA healthcare, 2001-2010: Implications for screening, diagnosis and treatment. Drug and Alcohol Dependence 116(1-3):93-101.
Seal, K. H., Y. Shi, G. Cohen, B. E. Cohen, S. Maguen, E. E. Krebs, and T. C. Neylan. 2012. Association of mental health disorders with prescription opioids and high-risk opioid use in US veterans of Iraq and Afghanistan. Journal of the American Medical Association 307(9):940-947.
Shea, M. T., A. A. Vujanovic, A. K. Mansfield, E. Sevin, and F. Liu. 2010. Posttraumatic stress disorder symptoms and functional impairment among OEF and OIF National Guard and reserve veterans. Journal of Traumatic Stress 23(1):100-107.
Shen, Y., and J. Arkes. 2009. Effects of OEF/OIF Deployment Intensity on PTSD Diagnoses Among Still Active Population: Analysis of Enlisted and Officer Populations 2001-2006. Monterey, CA: Naval Postgraduate School.
Shen, Y.-C., J. Arkes, B. W. Kwan, L. Y. Tan, and T. V. Williams. 2010. Effects of Iraq/Afghanistan deployments on PTSD diagnoses for still active personnel in all four services. Military Medicine 175(10):763-769.
Shen, Y. C., J. Arkes, and T. V. Williams. 2012. Effects of Iraq/Afghanistan deployments on major depression and substance use disorder: Analysis of active duty personnel in the US military. American Journal of Public Health 102(1 Suppl):S80-S87.
Shipherd, J. C., J. Stafford, and L. R. Tanner. 2005. Predicting alcohol and drug abuse in Persian Gulf War veterans: What role do PTSD symptoms play? Addictive Behaviors 30(3):595-599.
Shipherd, J. C., S. L. Pineles, J. L. Gradus, and P. A. Resick. 2009. Sexual harassment in the marines, posttraumatic stress symptoms, and perceived health: Evidence for sex differences. Journal of Traumatic Stress 22(1):3-10.
Shively, S., A. I. Scher, D. P. Perl, and R. Diaz-Arrastia. 2012. Dementia resulting from traumatic brain injury: What is the pathology? Archives of Neurology 69(10):1245-1251.
Silver, J. M., T. W. McAllister, and S. C. Yudofsky. 2011. Textbook of Traumatic Brain Injury. 2nd ed. Arlington, VA: American Psychiatric Publishing, Inc.
Skopp, N. A., M. A. Reger, G. M. Reger, M. C. Mishkind, M. Raskind, and G. A. Gahm. 2011. The role of intimate relationships, appraisals of military service, and gender on the development of posttraumatic stress symptoms following Iraq deployment. Journal of Traumatic Stress 24(3):277-286.
Skopp, N. A., L. Troimovich, Col. J. Grimes, L. Oetjen-Gerdes, and G. A. Gahm. 2012. Relations between suicide and traumatic brain injury, psychiatric diagnoses, and relationship problems, active component, US Armed Forces, 2001-2009. Medical Surveillance Monthly Report 19(2):7-11.
Slewa-Younan, S., S. van den Berg, I. J. Baguley, M. Nott, and I. D. Cameron. 2008. Towards an understanding of sex differences in functional outcome following moderate to severe traumatic brain injury: A systematic review. Journal of Neurology, Neurosurgery, and Psychiatry 79(11):1197-1201.
Smith, M. W., P. P. Schnurr, and R. A. Rosenheck. 2005. Employment outcomes and PTSD symptom severity. Mental Health Services Research 7(2):89-101.
Smith, T. C., M. A. Ryan, D. L. Wingard, D. J. Slymen, J. F. Sallis, and D. Kritz-Silverstein. 2008. New onset and persistent symptoms of posttraumatic stress disorder self reported after deployment and combat exposures: Prospective population based US military cohort study. British Medical Journal 336(7640):366-371.
Snarr, J. D., R. E. Heyman, and A. M. Smith Slep. 2010. Recent suicidal ideation and suicide attempts in a large-scale survey of the US Air Force: Prevalences and demographic risk factors. Suicide and Life-Threatening Behavior 40(6):544-552.
Spera, C., R. K. Thomas, F. Barlas, R. Szoc, and M. H. Cambridge. 2011. Relationship of military deployment recency, frequency, duration, and combat exposure to alcohol use in the Air Force. Journal of Studies on Alcohol and Drugs 72(1):5-14.
Spiro, A., 3rd, C. S. Hankin, D. Mansell, and L. E. Kazis. 2006. Posttraumatic stress disorder and health status: The veterans health study. Journal of Ambulatory Care Management 29(1):71-86.
Stahre, M. A., R. D. Brewer, V. P. Fonseca, and T. S. Naimi. 2009. Binge drinking among US active-duty military personnel. American Journal of Preventive Medicine 36(3):208-217.
Stecker, T., J. Fortney, R. Owen, M. P. McGovern, and S. Williams. 2010. Co-occurring medical, psychiatric, and alcohol-related disorders among veterans returning from Iraq and Afghanistan. Psychosomatics: Journal of Consultation Liaison Psychiatry 51(6):503-507.
Stein, M. B., and T. W. McAllister. 2009. Exploring the convergence of posttraumatic stress disorder and mild traumatic brain injury. The American Journal of Psychiatry 166(7):768-776.
Stern, R. A., D. O. Riley, D. H. Daneshvar, C. J. Nowinski, R. C. Cantu, and A. C. McKee. 2011. Longterm consequences of repetitive brain trauma: Chronic traumatic encephalopathy. PM&R: The Journal of Injury, Function, and Rehabilitation 3(10 Suppl 2):S460-S467.
Street, A. E., J. Stafford, C. M. Mahan, and A. Hendricks. 2008. Sexual harassment and assault experienced by reservists during military service: Prevalence and health correlates. Journal of Rehabilitation Research and Development 45(3):409-419.
Street, A. E., D. Vogt, and L. Dutra. 2009. A new generation of women veterans: Stressors faced by women deployed to Iraq and Afghanistan. Clinical Psychology Review 29(8):685-694.
Stulemeijer, M., S. P. van der Werf, B. Jacobs, J. Biert, A. B. van Vugt, J. M. Brauer, and P. E. Vos. 2006. Impact of additional extracranial injuries on outcome after mild traumatic brain injury. Journal of Neurotrauma 23(10):1561-1569.
Summerall, E. L. 2012. Traumatic Brain Injury and PTSD. http://www.ptsd.va.gov/professional/pages/traumatic-brain-injury-ptsd.asp (accessed September 11, 2012).
Suris, A., and L. Lind. 2008. Military sexual trauma: A review of prevalence and associated health consequences in veterans. Trauma, Violence, and Abuse 9(4):250-269.
Suris, A., L. Lind, T. M. Kashner, P. D. Borman, and F. Petty. 2004. Sexual assault in women veterans: An examination of PTSD risk, health care utilization, and cost of care. Psychosomatic Medicine 66(5):749-756.
Suris, A., L. Lind, T. M. Kashner, and P. D. Borman. 2007. Mental health, quality of life, and health functioning in women veterans: Differential outcomes associated with military and civilian sexual assault. Journal of Interpersonal Violence 22(2):179-197.
Taft, C. T., R. P. Weatherill, H. E. Woodward, L. A. Pinto, L. E. Watkins, M. W. Miller, and R. Dekel. 2009. Intimate partner and general aggression perpetration among combat veterans presenting to a posttraumatic stress disorder clinic. American Journal of Orthopsychiatry 79(4):461-468.
Tanielian, T., and L. H. Jaycox. 2008. Invisible Wounds of War: Psychological and Cognitive Injuries, Their Consequences, and Services to Assist Recovery. Santa Monica, CA: RAND Corporation.
Teasdale, G., and B. Jennett. 1974. Assessment of coma and impaired consciousness. A practical scale. Lancet 2(7872):81-84.
Teasdale, T. W., and A. W. Engberg. 2001. Suicide after traumatic brain injury: A population study. Journal of Neurology, Neurosurgery, and Psychiatry 71(4):436-440.
Terrio, H., L. A. Brenner, B. J. Ivins, J. M. Cho, K. Helmick, K. Schwab, K. Scally, R. Bretthauer, and D. Warden. 2009. Traumatic brain injury screening: Preliminary findings in a US Army brigade combat team. Journal of Head Trauma Rehabilitation 24(1):14-23.
Teten, A. L., J. A. Schumacher, S. D. Bailey, and T. A. Kent. 2009. Male-to-female sexual aggression among Iraq, Afghanistan, and Vietnam veterans: Co-occurring substance abuse and intimate partner aggression. Journal of Traumatic Stress.
Teten, A. L., J. A. Schumacher, C. T. Taft, M. A. Stanley, T. A. Kent, S. D. Bailey, N. J. Dunn, and D. L. White. 2010. Intimate partner aggression perpetrated and sustained by male Afghanistan, Iraq, and Vietnam veterans with and without posttraumatic stress disorder. Journal of Interpersonal Violence 25(9):1612-1630.
Teuber, H. L., and S. Weinstein. 1954. Performance on a formboard-task after penetrating brain injury. Journal of Psychology 38:177-190.
Thomas, J. L., J. E. Wilk, L. A. Riviere, D. McGurk, C. A. Castro, and C. W. Hoge. 2010. Prevalence of mental health problems and functional impairment among active component and National Guard soldiers 3 and 12 months following combat in Iraq. Archives of General Psychiatry 67(6):614-623.
Tolin, D. F., and E. B. Foa. 2006. Sex differences in trauma and posttraumatic stress disorder: A quantitative review of 25 years of research. Psychological Bulletin 132(6):959-992.
Trief, P. M., P. Ouimette, M. Wade, P. Shanahan, and R. S. Weinstock. 2006. Post-traumatic stress disorder and diabetes: Co-morbidity and outcomes in a male veterans sample. Journal of Behavioral Medicine 29(5):411-418.
Trofimovich, L., N. A. Skopp, D. D. Luxton, and M. A. Reger. 2012. Health care experiences prior to suicide and self-inflicted injury, active component, US Armed Forces, 2001-2010. Medical Surveillance Monthly Report 19(2):2-6.
Uddo, M., J. J. Vasterling, K. Brailey, and P. B. Sutker. 1993. Memory and attention in combat-related post-traumatic stress disorder (PTSD). Journal of Psychopathology and Behavioral Assessment 15(1):43-52.
VA (Department of Veterans Affairs). 2012. Analysis of VA Health Care Utilization Among Operation Enduring Freedom (OEF), Operation Iraqi Freedom (OIF), and Operation New Dawn (OND) Veterans: Cumulative from 1st QTR FY 2002 through 3rd QTR FY 2012 (October 1, 2001–June 30, 2012). Washington, DC: Department of Veterans Affairs.
VA and DOD. 2009. VA/DOD Clinical Practice Guidelines for Management of Concussion/Mild Traumatic Brain Injury (mTBI). Washington, DC: Department of Veterans Affairs, Department of Defense.
Vanderploeg, R. D., G. Curtiss, C. A. Luis, and A. M. Salazar. 2007. Long-term morbidities following self-reported mild traumatic brain injury. Journal of Clinical and Experimental Neuropsychology 29(6):585-598.
Vassallo, J. L., Z. Proctor-Weber, B. K. Lebowitz, G. Curtiss, and R. D. Vanderploeg. 2007. Psychiatric risk factors for traumatic brain injury. Brain Injury 21(6):567-573.
Vasterling, J. J., and S. Dikmen. 2012. Mild traumatic brain injury and posttraumatic stress disorder: Clinical and conceptual complexities. Journal of the International Neuropsychological Society 18(3):390-393.
Vasterling, J. J., K. Brailey, J. I. Constans, and P. B. Sutker. 1998. Attention and memory dysfunction in posttraumatic stress disorder. Neuropsychology 12(1):125-133.
Vasterling, J. J., C. Rogers, and E. Kaplan. 2000. Qualitative block design analysis in posttraumatic stress disorder. Assessment 7(3):217-226.
Vasterling, J. J., L. M. Duke, K. Brailey, J. I. Constans, A. N. Allain, Jr., and P. B. Sutker. 2002. Attention, learning, and memory performances and intellectual resources in Vietnam veterans: PTSD and no disorder comparisons. Neuropsychology 16(1):5-14.
Vasterling, J. J., M. Verfaellie, and K. D. Sullivan. 2009. Mild traumatic brain injury and posttraumatic stress disorder in returning veterans: Perspectives from cognitive neuroscience. Clinical Psychology Review 29(8):674-684.
Vasterling, J. J., S. P. Proctor, M. J. Friedman, C. W. Hoge, T. Heeren, L. A. King, and D. W. King. 2010. PTSD symptom increases in Iraq-deployed soldiers: Comparison with nondeployed soldiers and associations with baseline symptoms, deployment experiences, and postdeployment stress. Journal of Traumatic Stress 23(1):41-51.
Vasterling, J. J., K. Brailey, S. P. Proctor, R. Kane, T. Heeren, and M. Franz. 2012. Neuropsychological outcomes of mild traumatic brain injury, post-traumatic stress disorder and depression in Iraqdeployed US Army soldiers. British Journal of Psychiatry 201(3):186-192.
Vogt, D., R. Vaughn, M. E. Glickman, M. Schultz, M. L. Drainoni, R. Elwy, and S. Eisen. 2011. Gender differences in combat-related stressors and their association with postdeployment mental health in a nationally representative sample of US OEF/OIF veterans. Journal of Abnormal Psychology 120(4):797-806.
Wagner, T. H., K. M. Harris, B. Federman, L. Dai, Y. Luna, and K. Humphreys. 2007. Prevalence of substance use disorders among veterans and comparable nonveterans from the national survey on drug use and health. Psychological Services 4(3):149-157.
Wang, S., and J. Mason. 1999. Elevations of serum T3 levels and their association with symptoms in World War II veterans with combat-related posttraumatic stress disorder: Replication of findings in Vietnam combat veterans. Psychosomatic Medicine 61(2):131-138.
Wang, S., J. Mason, S. Southwick, D. Johnson, H. Lubin, and D. Charney. 1995. Relationships between thyroid hormones and symptoms in combat-related posttraumatic stress disorder. Psychosomatic Medicine 57(4):398-402.
Wechsler, D. 2009. Wechsler Memory Scale—Fourth Edition (WMS-IV). San Antonio, TX: Pearson.
Weinstein, S., and H. L. Teuber. 1957. Effects of penetrating brain injury on intelligence test scores. Science 125(3256):1036-1037.
Wells, T. S., C. A. LeardMann, S. O. Fortuna, B. Smith, T. C. Smith, M. A. K. Ryan, E. J. Boyko, D. Blazer, and T. Millennium Cohort Study. 2010. A prospective study of depression following combat deployment in support of the wars in Iraq and Afghanistan. American Journal of Public Health 100(1):90-99.
Widome, R., S. M. Kehle, K. F. Carlson, M. N. Laska, A. Gulden, and K. Lust. 2011. Post-traumatic stress disorder and health risk behaviors among Afghanistan and Iraq war veterans attending college. American Journal of Health Behavior 35(4):387-392.
Wilk, J. E., P. D. Bliese, P. Y. Kim, J. L. Thomas, D. McGurk, and C. W. Hoge. 2010a. Relationship of combat experiences to alcohol misuse among US soldiers returning from the Iraq war. Drug and Alcohol Dependence 108(1-2):115-121.
Wilk, J. E., J. L. Thomas, D. M. McGurk, L. A. Riviere, C. A. Castro, and C. W. Hoge. 2010b. Mild traumatic brain injury (concussion) during combat: Lack of association of blast mechanism with persistent postconcussive symptoms. Journal of Head Trauma Rehabilitation 25(1):9-14.
Wilk, J. E., R. K. Herrell, G. H. Wynn, L. A. Riviere, and C. W. Hoge. 2012. Mild traumatic brain injury (concussion), posttraumatic stress disorder, and depression in US soldiers involved in combat deployments: Association with postdeployment symptoms. Psychosomatic Medicine 74(3):249-257.
Wojcik, B. E., F. Z. Akhtar, and L. H. Hassell. 2009. Hospital admissions related to mental disorders in US Army soldiers in Iraq and Afghanistan. Military Medicine 174(10):1010-1018.
Wojcik, B. E., C. R. Stein, K. Bagg, R. J. Humphrey, and J. Orosco. 2010. Traumatic brain injury hospitalizations of US Army soldiers deployed to Afghanistan and Iraq. American Journal of Preventive Medicine 38(1 Suppl):S108-S116.
Woodhead, C., S. Wessely, N. Jones, N. T. Fear, and S. L. Hatch. 2012. Impact of exposure to combat during deployment to Iraq and Afghanistan on mental health by gender. Psychological Medicine 42(9):1985-1996.
Woodward, S. H., M. M. Murburg, and D. L. Bliwise. 2000. PTSD-related hyperarousal assessed during sleep. Physiology and Behavior 70(1-2):197-203.
Wright, K. M., T. W. Britt, P. D. Bliese, and A. B. Adler. 2011a. Insomnia severity, combat exposure and mental health outcomes. Stress and Health: Journal of the International Society for the Investigation of Stress 27(4):325-333.
Wright, K. M., T. W. Britt, P. D. Bliese, A. B. Adler, D. Picchioni, and D. Moore. 2011b. Insomnia as predictor versus outcome of PTSD and depression among Iraq combat veterans. Journal of Clinical Psychology 67(12):1240-1258.
Wu, P. C., C. Lang, N. K. Hasson, S. H. Linder, and D. J. Clark. 2010. Opioid use in young veterans. Journal of Opioid Management 6(2):133-139.
Yaffe, K., E. Vittinghoff, K. Lindquist, D. Barnes, K. E. Covinsky, T. Neylan, M. Kluse, and C. Marmar. 2010. Posttraumatic stress disorder and risk of dementia among US veterans. Archives of General Psychiatry 67(6):608-613.
Yarvis, J. S., P. S. Bordnick, C. A. Spivey, and D. Pedlar. 2005. Subthreshold PTSD: A comparison of alcohol, depression, and health problems in Canadian peacekeepers with different levels of traumatic stress. Stress, Trauma, and Crisis 8(2-3):195-213.
Yehuda, R., R. S. Keefe, P. D. Harvey, R. A. Levengood, D. K. Gerber, J. Geni, and L. J. Siever. 1995. Learning and memory in combat veterans with posttraumatic stress disorder. American Journal of Psychiatry 152(1):137-139.
Zalewski, C., W. Thompson, and I. I. Gottesman. 1994. Comparison of neuropsychological test performance in PTSD, generalized anxiety disorder, and control Vietnam veterans. Assessment 1(2):133-142.
Zatzick, D. F., C. R. Marmar, D. S. Weiss, W. S. Browner, T. J. Metzler, J. M. Golding, A. Stewart, W. E. Schlenger, and K. B. Wells. 1997a. Posttraumatic stress disorder and functioning and quality of life outcomes in a nationally representative sample of male Vietnam veterans. American Journal of Psychiatry 154(12):1690-1695.
Zatzick, D. F., D. S. Weiss, C. R. Marmar, T. J. Metzler, K. Wells, J. M. Golding, A. Stewart, W. E. Schlenger, and W. S. Browner. 1997b. Post-traumatic stress disorder and functioning and quality of life outcomes in female Vietnam veterans. Military Medicine 162(10):661-665.
Zatzick, D. F., F. P. Rivara, G. J. Jurkovich, C. W. Hoge, J. Wang, M. Y. Fan, J. Russo, S. G. Trusz, A. Nathens, and E. J. Mackenzie. 2010. Multisite investigation of traumatic brain injuries, posttraumatic stress disorder, and self-reported health and cognitive impairments. Archives of General Psychiatry 67(12):1291-1300.
Zinzow, H. M., A. L. Grubaugh, J. Monnier, S. Suffoletta-Maierle, and B. C. Frueh. 2007. Trauma among female veterans: A critical review. Trauma Violence Abuse 8(4):384-400.
Zivin, K., H. M. Kim, J. F. McCarthy, K. L. Austin, K. J. Hoggatt, H. Walters, and M. Valenstein. 2007. Suicide mortality among individuals receiving treatment for depression in the Veterans Affairs Health System: Associations with patient and treatment setting characteristics. American Journal of Public Health 97(12):2193-2198.
Zouris, J. M., A. L. Wade, and C. P. Magno. 2008. Injury and illness casualty distributions among US Army and Marine Corps personnel during Operation Iraqi Freedom. Military Medicine 173(3):247-252.