Endothelial Effects From Contact Lens Wear
John P. Schoessler
Let me preface my remarks by saying that I too will address a risk associated with contact lens wear. It is a long-term risk and does not apply to an immediate concern for pilot performance during a mission. I consider those concerns to be the distracting and debilitating influences, such as unstable acuity, discomfort, and dislodging of the appliance. Putting contact lens risks into perspective, they are probably nothing like the risk of climbing into a high-tech aircraft and riding it multiple times the speed of sound.
I believe attitude in performance of any task counts for much. If there is a perceived advantage in the wearing of contact lenses versus spectacles when piloting an aircraft because of the “freedom” afforded the pilot in terms of not having spectacles “hanging on the face,” I guarantee that it will result in better performance—directly measurable or not.
Nevertheless, just as in the civilian community, military personnel about to be fitted with contact lenses must be apprised of the immediate and long-term risks of contact lens wear, so that wearers will not return saying: “I didn't know contact lenses might cause corneal ulcers” or “You didn't tell me about ‘Agent Contact Lens'.”
With this in mind, let me tell you about one long-term effect of contact lens wear.
An unexpected revelation in recent years has been that contact lens events at the anterior surface (or epithelial layer) of the cornea produce effects at the back surface (or endothelial layer). The endothelial cells line the back of the cornea as a single monolayer.
Because of the importance of the role of the corneal endothelium in controlling corneal hydration, there has been interest in studying the consequences of contact lens wear on this layer. There is a tendency for the
corneal stroma to swell and absorb water, but this is normally held in check by the front and back corneal barriers—the epithelium and endothelium. In addition, the endothelium is responsible for actively transporting water out of the stroma to maintain partial stroma dehydration. The importance of the endothelial layer is readily seen. Any major breakdown in its function as a barrier or pump will produce uncontrolled corneal swelling, loss of corneal transparency, and bullous kertopathy. The application of certain contact lens designs to the cornea places stress on the system, since the anterior hypoxic environment allows buildup of lactate in the stroma, which in turn draws water in from the aqueous. The corneal endothelium then must counteract this extra hydrating force.
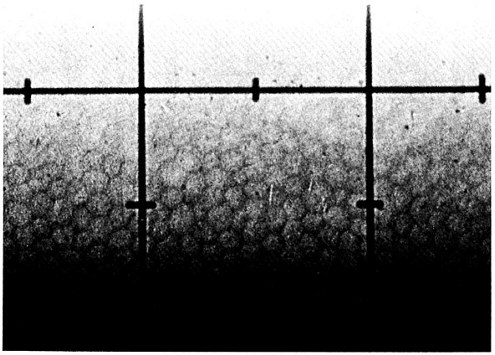
The normal corneal endothelium of a person who is a nonuser of contact lenses consists of a fairly regular mosaic pattern of cells. The majority are six-sided. The sizes of the cells are nearly the same, with larger cells tending to be about three to four times the area of the smallest cells for young adults. Figure 1 shows the normal endothelial cell pattern in a 24-year-old male who has never worn contact lenses.
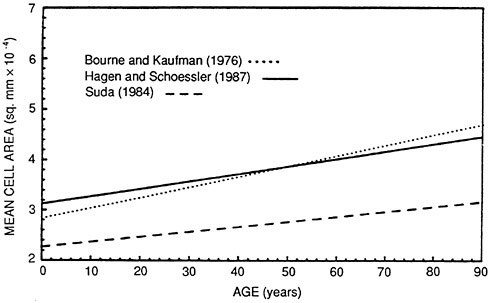
The endothelial cell density in the normal population has been extensively studied. The corneal endothelial cell density declines slowly over the life of an individual but never reaches a critical level of compromise. A cell density of about 2,800 cells per square millimeter is considered average. The cell density is apparently higher among persons of Japanese descent. These relationships are illustrated in Figure 2 in terms of mean cell area (1/ density).
Generally, corneal endothelial effects from contact lens wear can be divided into two categories: transient (or “blebs”) and long-term (or pleomorphic).
TRANSIENT ENDOTHELIAL CHANGES FROM CONTACT LENSES
Endothelial “blebs” were first described by Zantos and Holden (1977). These dark areas in the endothelial mosaic pattern are maximally observed 25–30 minutes after placing a hard or soft lens of low oxygen transmissibility on an eye previously unadapted to contact lens wear. The blebs gradually fade away as contact lens wear continues past 2 hours.
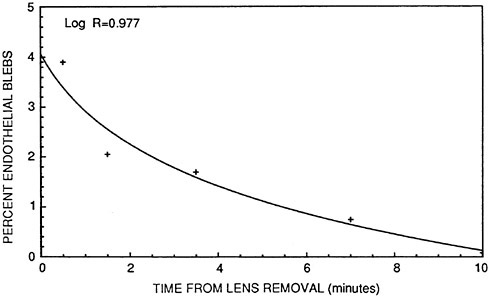
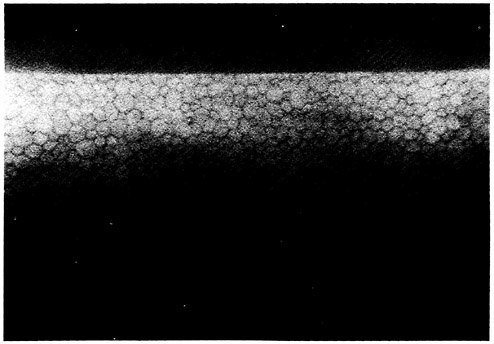
If the contact lens is removed at the peak of the bleb response, the mosaic returns to normal within minutes (Figure 3). Subjects vary markedly in the number of blebs produced.
The appearance of corneal endothelial blebs has been noted not only with contact lens wear but also with lid closure, nitrogen goggles, and carbon dioxide environment. The apparent cause for the dark areas is a bulging of the posterior cell membrane of certain endothelial cells, causing a disruption of the specularly reflected light.
This effect on the endothelium is said to be mediated by a pH change in the corneal tissue initiated by the corneal hypoxia. The significance of the bleb response and its wide quantitative variation among nonusers of contact lenses is not well understood. In any event, as this phenomenon is studied, it seems probable that the corneal endothelial bleb response to contact lenses will be found to bear some relationship to the viability of corneal endothelial cells.
LONG-TERM ENDOTHELIAL CHANGES FROM CONTACT LENSES
Endothelial changes over time are usually quantified not only by cell density but also by the amount of polymegethism and the percentage of hexagonal cells. Endothelial cell measures are (1) cell density (cells/square millimeter), (2) polymegethism (coefficient of variation of mean cell area), and (3) pleomorphism (percentage hexagonal cells).
Endothelial Cell Density
Contact lens wear apparently does not affect endothelial cell density. The literature overwhelmingly supports the view that there is no loss of endothelial cells even over long periods of wear.
Endothelial Polymegethism
Contact-lens-induced polymegethous corneal endothelial changes are characterized by marked endothelial cell size variation (Schoessler and Woloschak, 1981). Such cell size variation has been noted to occur gradually with age, but not to the extent or suddenness with which it appears in contact lens wearers. Examples of corneal endothelial polymegethism in long-term contact lens wearers are seen in Figure 4
Endothelial cell polymegethism is characterized by the development of many cells that are smaller than normal and by the development of cells much larger than normal.
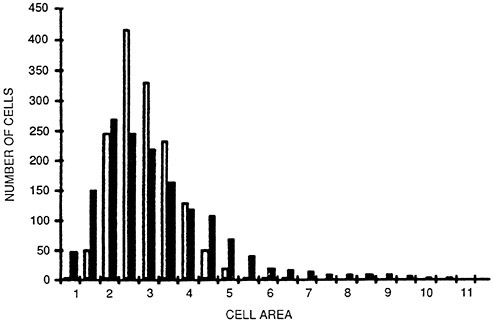
Corneal endothelial cell area distributions for long-term contact lens wearers differ from those of nonusers of contact lenses. A comparison of cell area distributions for contact wearers and a sex- and age-matched control group of nonwearers is shown in Figure 5
The coefficient of variation (standard deviation divided by the mean) of endothelial cell area is the generally accepted measure of endothelial polymegethism. For nonusers of contact lenses in the age range of 20–30, the coefficient of variation of endothelial cell area is generally about 24 per-
cent. For the same age range, contact lens wearers may show coefficients of variation for endothelial cell area that may approach 60 percent or greater.
Endothelial cell polymegethism has been noted with polymethylmethacrylate (PMMA) wear (Schoessler and Woloschak, 1981; Stocker and Schoessler, 1985), in hydrogel daily (MacRae et al., 1986) and extended wear (Schoessler, 1983), in rigid gas-permeable daily (Woloschak, 1983) and extended wear (Orsborn and Schoessler, 1988), and with continued eye closure (Schoessler and Orsborn, 1987). Endothelial cell polymegethism has not been found in persons wearing silicone elastomer for daily and extended wear (Schoessler et al., 1984).
Cell Pleomorphism
As endothelial cells become larger or smaller as a result of contact lens wear, they also tend to deviate from the normal hexagonal pattern. Larger cells tend to have more than six sides, while smaller cells are often pentagonal. The numbers of hexagonal cells are generally reduced to about 50–60 percent of the endothelial mosaic.
In addition, the endothelium of eyes exposed to long-term contact lens wear is often characterized by irregularly shaped cells. Examples of such cells are noted in Figure 6 Such extreme changes in cell morphology have generally not been described for the normally aging patient.
Endothelial cell photographs from contact lens wearers may also reveal cells that appear thick or “swollen.” These cells seem to project out of the mosaic pattern and are mostly noted in persons who have worn PMMA contact lenses for long periods of time. Examples of this phenomenon are seen in Figure 6
DISCUSSION
It is obvious that corneal endothelial cells respond both immediately and chronically to corneal hypoxia. Prolonged contact-lens-induced hypoxia causes: no change in endothelial cell density, increased endothelial polymegethism, decreased numbers of hexagonal cells, increased numbers of irregular cells, unevenness of endothelial mosaic pattern, and decreased cell functional capacity. The implications of these phenomena are not completely clear, although some trends are becoming evident.
The significance of polymegethous and pleomorphic cell changes lies in the notion that they are correlated with loss of endothelial cell function. It is not apparent whether the barrier function or pump mechanism of the endothelium, or both, is altered. Conner and Zagrod (1986) suggest several mechanisms by which the endothelial barrier and pump functions may be altered by contact lens wear. One suggestion is that ATP levels and altered
FIGURE 6 Endothelium of a long-term contact lens wearer. The mosaic demonstrates irregular and “swollen” cells.
calcium homeostasis may be responsible for contact-lens-induced endothelial polymegethism. In addition, other suggestions as to the actual agent involved in producing the cell changes include pH shift and lactate or carbon dioxide buildup. Some investigators postulate that the barrier function of the endothelial layer is faulty by reason of aberrated cells with altered interdigitations producing an ineffective barrier (Rao et al., 1984).
Rao and co-workers (1979, 1984) have shown that persons with corneal endothelial polymegethism are at greater risk for corneal swelling complications following surgery for (IOL) implantation. The implication is that contact lens wear may alter endothelial cells sufficiently to impair their ability to allow the cornea to regain normal deturgescence following severe corneal stress, such as that from IOL surgery. This conclusion reemphasizes the need for development of contact lens materials with high oxygen permeability. Lens design becomes a key factor also for providing maximum oxygen transmissibility. This would include the use of thinner rigid bitoric lenses for patients with moderate corneal astigmatism instead of rigid spherical back curve lenses designed with increased center thickness to prevent lens flexure. The development of endothelial polymegethism may also be responsible for the “corneal exhaustion syndrome,” whereby persons who have worn
PMMA lenses for many years suddenly find they are not able to tolerate them anymore.
Complete recovery from significant endothelial polymegethism is apparently not possible. Only slight recovery from contact-lens-induced endothelial polymegethism has been noted following cessation of contact lens wear or after switching to lenses of significantly higher oxygen transmissibility. The development of contact-lens-induced endothelial polymegethous cell changes is the indirect result of corneal hypoxia and is related to contact lens oxygen transmissibility, contact lens design, hours of contact lens wear, and type of wear (daily or extended).
It is certain that contact lens events at the front of the cornea affect the status of the important endothelial layer. For the majority of the present contact-lens-wearing population, this may mean an increased risk of corneal swelling complications or other problems following high corneal stress such as corneal surgery. One must be concerned not only with the reported results of cataract/IOL surgery but also with potential long-term problems associated with radial keratomy procedures on corneas with polymegethous endothelial cells.
Furthermore, a recent case study by Roth (1986) reports the observation of an apparent spontaneous bullous kertopathy resulting from pleomorphic endothelial changes induced by long-term PMMA and soft contact lens wear. This could possibly indicate that a contact lens environment alone is enough of a stress factor to cause corneal decompensation in some persons with abnormal endothelial cells. It is obvious that this topic will be the focus of much research for some time to come. At present, measures to reduce the probability of contact-lens-induced endothelial changes include using contact lens materials with the highest oxygen transmissibility and advising patients to use daily-wear lenses during waking hours only.
REFERENCES
Conner, C., and M. Zagrod 1986 Contact lens-induced corneal endothelial polymegethism: functional significance and possible mechanisms. American Journal of Optometry and Physiological Optics 63 : 539–544.
MacRae, S., M. Matsuda, S. Shellans, and L. Rich 1986 The effects of hard and soft contact lenses on the corneal endothelium American Journal of Ophthalmology 102 : 50–57.
Mandell, R. 1988 Contact Lens Practice . Springfield, Ill.: Charles C Thomas
Orsborn, G., and J. Schoessler 1988 Corneal endothelial polymegethism after the extended wear of rigid gas permeable lenses. American Journal of Optometry and Physiological Optics 65 : 84–90.
Rao, G., E. Shaw, E. Arthur, and J. Aquavella 1979 Endothelial cell morphology and corneal deturgescence. Annals of Ophthalmology 11:885–899.
Rao, G., J. Aquavella, S. Goldberg, and S. Berk 1984 Pseudophakic bullos keratopathy-relationship to preoperative corneal endothelial status. Ophthalmology 91:1135–1140.
Roth, H. 1986 Pseudo bullos keratopathy: a rare complication of contact lens wear. Contactologia (French) 8:116–117.
Schoessler, J. 1983 Corneal endothelial polymegethism associated with extended wear. International Contact Lens Clinic 10:148–155. 1988 Contact lens wear and the corneal endothelium. Journal of the American Optometric Association 58:804–810.
Schoessler, J., and M. Woloschak 1981 Corneal endothelium in veteran PMM A contact lenses wearers. International Contact Lens Clinic 8:19–25.
Schoessler, J., and G. Orsborn 1987 A theory of corneal endothelial polymegethism and aging. Current Eye Research 6:1–6.
Schoessler, J., et al. 1984 Corneal endothelial observations of silicone elastomer contact lens wearers. International Contact Lens Clinic 11:337–340.
Stocker, E., and J. Schoessler 1985 Corneal endothelial polymegethism induced by PMMA contact lens wear. Investigative Ophthalmology and Visual Science 26:857–863.
Woloschak, M. 1983 The Corneal Appearance of Unilateral Contact Lens Wearers. Master 's thesis, Ohio State University.
Zantos, S., and B. Holden 1977 Transient endothelial changes soon after wearing soft contact lenses. American Journal of Optometry and Physiological Optics 54:856–858.