KEY SPEAKER THEMES
Remington
- Rankings can be a useful tool for focusing the attention of community stakeholders and can motivate the larger public to become involved in efforts to improve health care.
- More work is needed to understand how to increase interest and engage people and create evidence-based programs and policies that can improve care delivery and other factors affecting health.
Gildemeister
- Metrics have played a key role in informing state health care reform efforts, with Minnesota serving as an example.
- It is important to establish clearly the purpose for creating metrics and to not have one measure that tries to accomplish everything.
- It is critical to align measures and to eliminate duplicate measures within states and across payers, including the federal government.
Romm
- Metrics cannot stand alone—it is necessary to have multiple levers operating in concert with the three-part aim in order to make progress in health care reform.
- A significant challenge is to align a state’s efforts with those of other payers and purchasers to minimize redundant efforts.
Once the best measures have been selected, there are multiple challenges to implementing measures in routine practice, particularly considering the wide range of populations and the multiple levels of the health system at which measurement needs to be useful. In this session, Patrick Remington, associate dean for public health at the University of Wisconsin School of Medicine and Public Health, spoke about how to measure the health status of the U.S. population on a county-by-county basis. Stefan Gildemeister, director of the Health Economics Program and state health economist in the Minnesota Department of Health, addressed the measurement issue from a state health reform perspective. Carole Romm, who led, in a consulting capacity, the accountability and quality efforts for the Oregon Health Authority’s Medicaid program, described a measurement framework for coordinated care in another state effort.
ANALYZING HEALTH STATUS ACROSS ALL COUNTIES
To begin his presentation, Patrick Remington described the simple logic model that informs his work on measuring health status. This logic model assumes that programs and policies impact health factors—what used to be called health determinants—and that changes in health factors, over the long run, impact health outcomes. Health outcomes are measured using measures of morbidity and mortality, while health factors consist of health behaviors, clinical care, social and economic factors, and the physical environment. Remington then described the metrics that he and his colleague David Kindig chose to measure each of these inputs and the weighting that each metric is given in the final calculation (see Figure 6-1). He noted that one of the keys to developing this model was deciding on a set of measures and acknowledging that the final list is not perfect but could be sufficient. He also remarked that an important factor in selecting metrics is that the data are readily accessible and preferably available at no cost from every one of the more than 3,000 counties in the nation. Remington commented that together, these metrics provide a good assessment of the three-part aim.
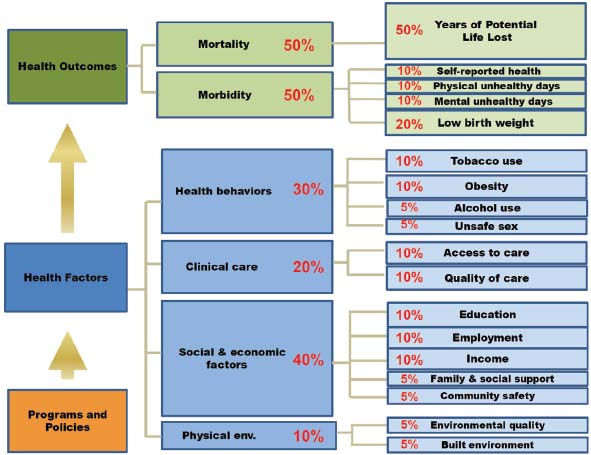
FIGURE 6-1 Metrics and weightings used to calculate health status on a county-by-county basis.
SOURCE: University of Wisconsin Population Health Institute and Robert Wood Johnson Foundation, 2013.
He showed some of the maps his group generated using the output from this model and explained how to use the maps to identify the healthiest and least healthy counties nationwide or within a state. He noted that counties are using these data, which are released annually in March, to take on the task of improving their ranking within their states. He remarked that the media are paying attention to the rankings, which appears to be forcing communities to form teams that can both talk about the rankings and move toward action based on the many measures in the model.
Remington concluded his talk with some of the lessons that he and his colleagues have learned from this project over the past decade. The first is that it is possible to collect the data needed for the model and to use the model to summarize health outcomes and health factors. Second, generating rankings gets the attention of the media, local health officers, the general public, and even physicians and others in the health care system within a community. In fact, he said, an integrator in a community could use this model of broad population health determinants to create
evidence-based programs and policies that would improve health. That realization leads to the third lesson, which is that more work is needed to understand how to move people from being interested and engaged to creating evidence-based programs and policies that can command the necessary resources to change the delivery system.
IMPLEMENTING STATEWIDE MEASUREMENTS ON ACCESS, COST, AND QUALITY
In Minnesota, Stefan Gildemeister said measurement activities have taken place in the context of a state in which the legislature has been active in health care reform efforts since the early 1990s and has enabled efforts to inform that process with empirical evidence. To increase the quantity of evidence, the legislature has provided funding to conduct research and population-based monitoring of access, utilization, quality, and health care costs. In addition, Minnesota benefits from having a dynamic and innovative private sector that has put the state in the lead on concepts of managed care and utilization management, and that is moving the state into the new area of shared savings through collaboration on generating evidence and best practices. In particular, the largely nonprofit plan and hospital environment in the state has given rise to organizations, such as the Institute for Clinical Systems Improvement and Minnesota Community Measurement, that are identifying what works and pointing the way to improvement.
More recently, in 2008, the state passed groundbreaking bipartisan health care reform legislation that aimed to improve population health through efforts targeting obesity and tobacco use, to enhance the patient experience by investing in health care homes and stressing patient-centered care, and to improve cost trends through transparency in cost and quality and through payment reform. To further the momentum generated by this legislation, the state is finalizing a roadmap for implementing reform efforts over the next few years as part of the governor’s health care reform task force. Gildemeister presented his office’s projections of annual spending for the next 10 years and noted that, without action, the state’s total health care spending will double (see Figure 6-2). He also discussed the data highlighting the current racial and ethnic disparities in health care that reform is also designed to address, noting that these data are indicative of how urgently reform is needed.
He then discussed some examples of the state’s activities and the progress that Minnesota is making in meeting the three-part aim. Data from the state’s measurement and reporting system on optimal diabetes care showed that the percentage of diabetics who received optimal care rose from 28.4 percent to 39.7 percent between 2009 and 2011 for patients regardless of the source of their health coverage. Medicare patients had
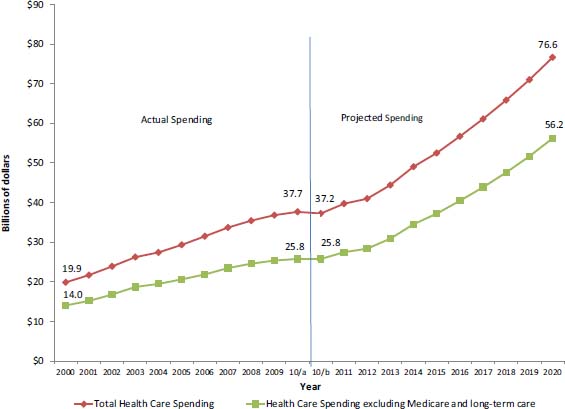
FIGURE 6-2 Estimates and projections of health care spending without the effects of Minnesota reforms.
SOURCE: MDH, 2012.
the biggest increase, jumping from 33.8 percent to 46.2 percent, while Medicaid and uninsured patients realized the smallest benefit, an increase from 17.5 percent to 26.3 percent. He also showed data using a total care risk-adjusted quality score that his office developed as part of Minnesota’s 2008 health reform law. This single measure, which looks at quality and cost as two dimensions and is based on confidentially reported data, is the result of early, high-level work that Gildemeister said could lead to a metric that could be drilled down to subpopulations. For example, the total care quality composite measure for hospitals summarizes care process measures and health outcomes using several currently reported data and adjusting for patient populations (MDH, 2013). This single risk-adjusted quality score plotted against risk-adjusted costs per discharge revealed a large disparity across the states hospitals in terms of quality versus cost.
Gildemeister noted that Minnesota’s health insurance exchange, established under the provisions of the ACA, will provide a wealth of data on a dramatically larger scale than is available today, creating new areas for measurements of affordability, provider innovation, and population health. He highlighted the potential this will create for better understanding of health care system performance, which will allow for better tracking of progress and for fine-tuned, regular adjustments to policies and programs
to ensure success. Based on Minnesota’s experiences, there are several factors that Gildemeister believes will be important for maximizing the use of this upcoming influx of data. First, it will be important to establish clearly the purpose for creating a specific metric and to not force one measure to accomplish the measurement needs for all potential applications, which can include regulation, evaluation, and public reporting. It is critical as well to align measures and to eliminate duplicate measures within states and across payers, including the federal government, and he noted the promising work that the Office of the National Coordinator for Health Information Technology (ONC) is engaged in with the Centers for Medicare & Medicaid Services (CMS) and other federal agencies.
Another area of emphasis going forward will be to resolve the tension between the need to accelerate the measurement development cycle while maintaining quality and incorporating community input and priorities. Gildemeister believes that more work is needed to make the business case for improved measures to policy makers. This effort should develop better approaches to tracking and communicating measurement results in a more organized fashion and not necessarily by datasets. It should also develop composites or indices that help policy makers and the public assess progress more easily.
A MEASUREMENT FRAMEWORK FOR COORDINATED CARE IN MEDICAID
Carole Romm then spoke about Oregon’s experience implementing the three-part aim and using metrics to assess progress in the state’s Medicaid program. Currently, Medicaid accounts for 11 percent of the total state budget and covers 16 percent of all Oregonians and 50 percent of all babies born in the state. Some 85 percent of Oregon’s health care providers participate in the state’s Medicaid program. She noted that, as in Minnesota, Oregon’s governor has been a strong proponent of health care reform efforts. She added that the state has set specific goals in achieving the three-part aim that include lowering cost increases by 2 percentage points over a 5-year demonstration period; ensuring that the quality of care is not degraded or improves; and ensuring that population health is not degraded or improves. Oregon, operating as a test bed, is working in close partnership with CMS to obtain a waiver that will enable it to move forward with its reform efforts.
Oregon realized that, to achieve the three-part aim, it would have to undertake a drastic revamping of its health care systems. This reinvention will start with what the state calls coordinated care organizations (CCOs) which will be responsible for a broad range of outcomes, including physical, mental, and oral health. These organizations will have a global budget,
be responsible for the health and well-being of all of the Medicaid population within their catchment areas, and reflect the core concept that responsibility for health care should reside at the local level. These organizations are mandated to work with community partners outside the health care system and are given the flexibility to deliver health care using approaches tailored to their specific populations. Furthermore, the state also developed a number of levers, such as alternative payment methodologies, to help advance the initiative.
To support the reform effort, Oregon is establishing a transformation center with innovator agents based on the model of the agricultural extension services suggested by Atul Gawande (2009). These innovator agents will be state employees embedded in individual coordinated care organizations and will serve as links between these organizations and the transformation center. In a sense, they will act as two-way conduits, informing the transformation center and the Oregon Health Authority of progress and challenges at the local level of the CCO, shaping the state’s efforts to create learning collaboratives to meet the needs of the CCOs, and then conveying information back to the care organizations. Romm noted that Oregon’s efforts will be focused on the patient-centered primary care home, reflecting the state’s belief that care is best provided in a coordinated and integrated way at the local level. In addition, Oregon believes that nontraditional or community health care workers are an essential part of the health care team. The state is supporting the growth of these workers by setting out criteria for certification and by working with the state’s community colleges to establish training programs.
In terms of metrics, Romm said the state used an open public process with stakeholder groups to create a list of principles for metrics selection. The coordinated care organizations will be required to collect these data as part of their contracts with the state. In conjunction with the development of these metrics, in 2012 the Oregon state legislature created a committee with nine members serving 2-year terms that used a public process to identify objective outcome and quality measures and associated benchmarks for disbursing funds from the state’s quality incentive pool. These metrics, which were being reviewed by CMS at the time of this workshop, covered six areas that the committee deemed critical for transformation: behavioral health, maternal child health, chronic conditions, access, patient experience of care, and electronic health record adoption.
Romm finished her remarks by describing some of the challenges this effort has faced and some of the lessons the state has learned. Perhaps the biggest challenge has been to align the state’s efforts with those of its purchasers and payers to minimize redundant efforts and to address the issue of parsimony. She acknowledged that the state is working hard to narrow the current list of measures to a reasonable set that covers critical aspects
of the three-part aim. It has been challenging to collect data at a reasonable cost, to establish a baseline for new metrics, and to avoid unintended consequences in the selection of metrics. It has been important, she said, to set attainable and meaningful performance goals and to accept that metrics cannot stand alone—that there need to be multiple levers operating in concert with the three-part aim in order to make progress. Stakeholder involvement, though difficult to achieve, has been critical to gaining acceptance in Oregon and to catalyzing the emergence of champions for this process. Finally, it was critical to align efforts around a single model, which in Oregon’s case was the coordinated care model.
A substantial portion of the discussion that followed the three presentations concerned the relationship of factors external to the health care system—smoking, diet, exercise, transportation policy, and the like—to internal factors that affect health. It was noted that establishing metrics for population health may be difficult given that these factors are sometimes beyond the direct control of the health care system. Diana Dooley, secretary of the California Health and Human Services Department, remarked that her state’s Let’s Get Healthy Task Force recognized that problem and decided to measure change across the state rather than by individual systems. In that way, the task force hoped to let local communities and health care organizations develop a wide range of initiatives and then see if the population health of the state changes. While this eliminates the ability to identify individual interventions, it does stimulate innovation that is not constrained by the need to measure. Gildemeister added that involving consumers in these community advisory councils can engage the broader community to take action beyond what a health care organization can do regarding the external factors that influence health.
During the discussion, Remington noted that his group’s county health rankings capture disparities across a state or between neighboring regions in different states. He said that in Wisconsin, there is more of a gap between the healthiest and least healthy counties within the state than across the country. Romm said that Oregon has recognized this gap and requires the coordinated care organizations to have a community advisory council and to perform a community health needs assessment as a way of dealing with health disparities across the state.
Gawande, A. 2009. Testing, testing. New Yorker 85(41):34–41.
MDH (Minnesota Department of Health). 2012. Minnesota Health Care Spending and Projections, 2010. http://www.health.state.mn.us/divs/hpsc/hep/publications/costs/healthspending2012.pdf (accessed February 26, 2013).
———. 2013. Provider Peer Grouping Metholodology: Hospital Total Care. http://www.health.state.mn.us/healthreform/peer/hospitalmethodology0313.pdf (accessed April 11, 2013).
University of Wisconsin Population Health Institute and Robert Wood Johnson Foundation. 2013. Data and Methods. http://www.countyhealthrankings.org/our-approach (accessed February 26, 2013).










