The Challenges and Opportunities for the BRICS Countries to Lead
Key Messagesa
• The BRICS countries are home to the majority of the global MDR TB patient population but are also engines of economic growth, funding a substantial portion of TB control worldwide.
• The BRICS countries could serve as sources of innovative ideas to develop and advance key areas of TB and MDR TB control.
• Poverty alleviation programs and free access to health care have helped Brazil keep MDR TB levels relatively low and focus on delivery system innovations such as community-based TB and MDR TB care.
• South Africa has made considerable progress in surveillance, infection control, better diagnosis methods, and the rollout of community-based MDR TB treatment, but challenges remain for effectively coordinating the currently siloed HIV and TB programs.
• India’s national TB control program has the goal of seeking to ensure universal access to quality TB care for its 1.3 billion people in 600 districts. The complexities of TB care coordination across India’s public and private sectors, poverty alleviation, active case finding, and treatment of latent TB are key challenges for the future.
• Russia has improved TB diagnostic capabilities, the availability of FLDs and SLDs, and infection control programs in recent years. Future steps to further improve the control of DR TB in Russia could include a shift in the TB care paradigm to more outpatient and community-
based services, as well as closer integration with the country’s HIV program.
• Major health care system reforms undertaken in China include reducing the cost of MDR TB treatment for patients and improving the national TB surveillance system to provide individual patients with care as early as possible while generating data to facilitate the management of the disease from a population-based perspective. Opportunities for the future include applying China’s strong scientific research capability to better understand the burden of disease and contribute to the development of new drugs to treat MDR TB.
__________________
a Identified by individual speakers.
As part of the final session of the workshop, several speakers provided reflections from the perspective of the BRICS countries. They were asked to discuss the leading role of the BRICS countries in the effort to combine science- and evidence-based policies with economic interventions to combat DR TB. After presenting an overview of the role of the BRICS countries overall in combating DR TB, this chapter summarizes remarks made by individual speakers concerning specific BRICS countries.
OVERALL ROLE OF THE BRICS COUNTRIES
Rifat Atun, Professor of International Health Management, and Head, Health Management Group, Imperial College London, noted that although the BRICS countries have been engines of economic growth, they also have been engines for the spread of MDR TB. Approximately 60 percent of the estimated 310,000 MDR TB cases among notified TB patients with pulmonary TB in 2011 were in China, India, and the Russian Federation, he observed (WHO, 2012).
The BRICS countries also provide a substantial portion of funding for TB control worldwide (Figure 2-1). Among 104 countries that account for almost 95 percent of TB cases globally, the BRICS countries have contributed an average of more than 60 percent of TB control funding since 2006. These countries also serve as a source for much of the funding for MDR TB. “Without the BRICS, global TB and MDR TB control efforts would collapse,” said Atun.
Atun identified four areas in which the BRICS countries can play an
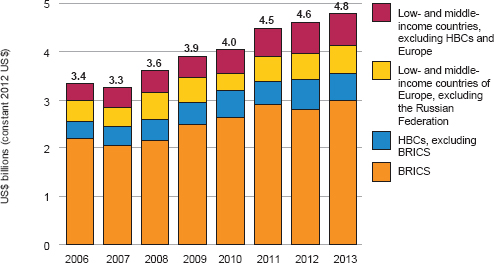
FIGURE 2-1 The BRICS countries provide the majority of funding for TB control in the 104 countries that account for 94 percent of global cases.
NOTE: BRICS, Brazil, Russia, India, China, and South Africa; HBC, high tuberculosis burden country.
SOURCE: WHO, 2012, Figure 5.1, p. 53. Reproduced with the permission of the publisher.
important role in combating TB and MDR TB. The first, he said, is filling the current gap in global leadership. Formation of the G20, for example, provides a new platform that could give a global campaign on TB control the visibility it urgently needs.
The sustained economic growth of the BRICS countries also provides an opportunity for new investment in TB control. For example, the percentage growth in gross domestic product of China’s economy remains several times that of the European Union or the United States. If the BRICS countries invested in TB control at the same rate at which their economies are growing, the results would be large investments in local as well as global TB control.
Third, the BRICS countries have the opportunity to build on their current experience and become a major source of innovation in six areas related to TB control: (1) molecular biology and genomics; (2) epidemiology; (3) diagnostic tools; (4) new treatments and regimens; (5) new delivery models, including community-based models; and (6) assessment and evaluation, including of the optimal delivery model.
Finally, noted Atun, the BRICS countries are well positioned to lead global technical cooperation in TB control. These countries could foster
south–south cooperation, and they could also facilitate south–north cooperation, in which the global north learns from the global south.
The BRICS countries are emerging as an important voice in global economic, political, and financial discourse. They are achieving rapid economic growth, they are agents of innovation, they have almost half the world’s population, in many sectors they are playing an important leadership role on the international stage, they have shown leadership in responding to HIV, they have been able to scale up TB control rapidly and successfully, and they have undertaken initiatives to achieve universal health care systems. “The BRICS countries can rise to the challenge of MDR TB treatment and control,” Atun said. “Not just that, but I think they have the capability to transform global health.”
Compared with the other BRICS countries, MDR TB levels have remained low in Brazil among both newly diagnosed and rediagnosed cases, for two major reasons. First, Brazil has had success in alleviating poverty through programs such as Bolsa Familia. Almost 40 million people were lifted out of poverty from 2003 to 2011 during the presidency of Luiz Inácio Lula da Silva. Second, in 1988, through enactment of the Federal Constitution, Brazil introduced free access to high-quality health care, and the Unified Health Care System has enabled a comprehensive response to the country’s health challenges. Relatedly, Brazil has emphasized innovation not only in the development of drugs and technologies for high-burden conditions but also in the delivery of health care services and the manufacturing of health care products.
Brazil’s family health program, which emphasizes primary health care that is delivered in the community, has been an important innovation. This community-based delivery system has been “the essence of the rapid achievements” in Brazil, said Atun. It is a proactive system that provides comprehensive care while fostering active outreach to communities and households, including those in congregate settings and difficult-to-access slums. The family health program is underpinned by a good information system, strong supply chains, and strong management. Atun characterized the program as being part of a community and civil society movement that has created an enabling platform for the treatment of TB and other conditions.
__________________
1 This section is based on the presentations by Rifat Atun, Professor of International Health Management, and Head, Health Management Group, Imperial College London; and Jarbas Barbosa da Silva, Jr., Vice Minister for Health Surveillance, Ministry of Health, Federative Republic of Brazil.
Participating in a telephone call from Brazil, the Vice Minister for Health Surveillance, Ministry of Health, Federative Republic of Brazil, Jarbas Barbosa da Silva, Jr., noted that access to no-cost drugs has been an important part of the country’s national TB program. At the same time, the drugs are not available for purchase in private drugstores, an approach that has helped prevent the development of MDR TB by reducing the injudicious use of drugs. Brazil also has made TB treatment a priority in primary health care delivery settings as a means of reaching the entire population.
The Delhi communiqué presents a concrete action plan in which each country serves as a nexus for different responsibilities, coordinating work in various areas—for example, Brazil in drug manufacturing, China in drug discovery and development, and Russia in medical technologies. At the next meeting of the ministers, in January 2014, the countries’ experiences will be shared and adjustments made. The communiqué is a very important statement, said Barbosa da Silva, Jr., because it is comprehensive and applies both on a national and international scale. Thus, he said, it can play a critical role not only for the BRICS countries but for all countries that need to improve their health systems and the health of their populations.
The incidence of TB in South Africa is worse than that in many other countries, including the other BRICS countries, observed Kristina Wallengren, Clinical Advisor, KwaZulu-Natal Research Institute for Tuberculosis and HIV (K-RITH), Nelson R. Mandela School of Medicine, University of KwaZulu-Natal; and Chief Executive Officer, Tuberculosis and HIV Investigative Network of KwaZulu-Natal (THINK). The official figure is about 900 per 100,000 population, compared with about 110 per 100,000 in India, 75 per 100,000 in China, and just 4 per 100,000 in the United States. In KwaZulu-Natal province, the incidence of TB is more than 1,200 per 100,000 population.
The official incidence of MDR TB (2.3 percent in KwaZulu-Natal) is lower in South Africa than in many other countries, such as Russia, where it is above 20 percent. But because of the very high incidence of TB in South Africa, the absolute number of MDR TB cases is still high. KwaZulu-Natal province has an estimated 3,000 MDR TB cases each year, which is equal to 30 MDR TB cases per 100,000 population. Among MDR TB cases, about
__________________
2 This section is based on the presentation by Kristina Wallengren, Clinical Advisor, KwaZulu-Natal Research Institute for Tuberculosis and HIV (K-RITH), Nelson R. Mandela School of Medicine, University of KwaZulu-Natal; and Chief Executive Officer, Tuberculosis and HIV Investigative Network of KwaZulu-Natal (THINK).
10 percent are XDR TB, and of the XDR TB cases, 88 percent are resistant to all 6 of the FLDs and SLDs that are tested routinely in KwaZulu-Natal.
Furthermore, the actual prevalence of MDR and XDR TB is likely to be substantially higher than currently measured. The observed level of MDR TB among the districts of KwaZulu-Natal province is proportional to the number of culture requests, which suggests that the actual rate of MDR TB in the province exceeds 100 per 100,000 (Wallengren et al., 2011). In addition, a postmortem study in a peri-urban public hospital in the province found that more than two-thirds of 240 deceased patients had TB, including 17 percent of patients in whom TB was not suspected (Cohen et al., 2010). The majority of the patients who were culture positive when they died, despite receiving TB treatment, were infected with drug-susceptible TB, suggesting that the diagnosis of TB was made too late to alter the course of their infection.
Wallengren described several areas in which some progress has been achieved, noting challenges that remain:
• Surveillance. Despite important progress, surveillance remains a major challenge in South Africa. The outbreak of XDR TB in Tugela Ferry detected in 2005, which demonstrated that XDR strains could readily be transmitted from person to person, was discovered “nearly by coincidence,” said Wallengren. In light of a number of TB patients failing to thrive despite being on antiretroviral treatment (ART), two medical students in need of a project were assigned the task of collecting samples from all the TB patients at the Church of Scotland Hospital in Tugela Ferry and sending them to the provincial laboratory to be cultured. That laboratory had an unusual policy in place that called for testing all six FLDs and SLDs, not just the drugs requested by a physician. And the laboratory manager, to prepare for a conference, noticed in looking at some recent laboratory results that a large number of people from the hospital in Tugela Ferry were resistant to all six drugs. South Africa now has a centralized TB data system that enables surveillance, although there are still “some kinks” in the system, according to Wallengren. Nevertheless, the current system has greatly improved surveillance in the country.
• Diagnosis. Diagnosis is a particular challenge in South Africa because of the high HIV burden in the country. In KwaZulu-Natal province, 39 percent of pregnant women are HIV positive, and 70 percent of all TB cases are HIV positive. About 40 percent of TB cases in KwaZulu-Natal are smear negative, often also culture
negative, and are diagnosed instead through chest X-rays and clinical symptoms. Because TB is so prevalent, said Wallengren, HIV patients are put on TB treatment despite the absence of a confirmative bacterial diagnosis. The rollout of GeneXpert in South Africa has improved diagnosis of MDR TB. In the past, many patients with MDR TB died within a few weeks of having their sputum collected for testing. Diagnosis is faster with GeneXpert, which improves the outcomes of treatment and reduces transmission in the community. Better diagnosis also has revealed the extent of the problem in South Africa.
• Treatment. Treatment of MDR TB is improving in South Africa. The country has piloted and is starting to roll out community-based MDR TB treatment, and the initial results are promising. In addition, increased use of antiretroviral therapy has improved the prospects for patients with MDR TB. Problematically, however, the HIV and TB programs in South Africa remain siloed. Documentation and evaluation of the programs occur separately and do not reinforce each other. To the extent that the programs have been coordinated, the result has so far been simply a third silo: a combined HIV-TB program that interrelates poorly with the preexisting programs.
• Infection control. Infection control also has improved dramatically in recent years, said Wallengren. At the time of the Tugela Ferry outbreak, few health care workers in the country knew what an N95 respirator was, but now they know that they should be wearing one routinely.
Finally, Wallengren described several important capacity-building initiatives in Africa. The Human Heredity and Health in Africa (H3 Africa) initiative is a consortium formed by the National Institutes of Health (NIH) and the Wellcome Trust to study genetic diversity in health and disease in Africa and develop the necessary expertise and networks among African investigators. K-RITH is an initiative undertaken by the Howard Hughes Medical Institute to conduct basic science research on TB and HIV and translate scientific findings into new tools for controlling these diseases. It is currently supporting investigations into a large variety of research questions, including the pharmacokinetics of TB treatment in children, new biomarkers and response to treatment, new diagnostic tools, assessment of drug resistance through whole genome sequencing, clinical trials of new treatment regimens, and investigation of the effects of anti-TB drugs on Mycobacterium tuberculosis (M.tb.).
India faces major challenges in diagnosing and treating MDR TB patients. It must reach 1.3 billion people in 600 districts, and each province has its own health care delivery system. The national TB control program has a small number of staff who must interact with a tremendously complex system. Nevertheless, said Salmaan Keshavjee, Harvard Medical School, “they have done a remarkable job.”
About 1.5 million cases of TB are notified each year in India, including about 65,000 cases of MDR TB. Given global case-finding statistics, these estimates are likely lower than the actual numbers, said Keshavjee, which would put the actual number of MDR TB cases at roughly 100,000 per year. Furthermore, these numbers are only from the public sector, and the private sector treats an estimated 70 to 80 percent of all patients.
India’s Revised National TB Control Program (RNTCP) has sought to ensure universal access to quality TB care throughout India. The RNTCP also has reached out to the private sector to promote the appropriate treatment of drug-susceptible TB. For example, it has become involved in medical college training, human resource development, and infection control to reduce the burden of both TB and MDR TB. The program has a goal of creating a nationwide network of more than 200 treatment sites that can enroll patients.
In the area of diagnosis, India has mounted a major effort since 2007 to modernize its testing of TB patients. It has established a network of culture and DST laboratories around the country, many of which are capable of line probe assays (LPAs). The goal for 2013 is to have 43 accredited public-sector laboratories and 22 private laboratories that are capable of undertaking drug-susceptibility testing for FLDs and SLDs and of diagnosing MDR and XDR TB. In addition, every province is to have at least one intermediate reference laboratory that can perform culture and DST and that has the associated infrastructure for getting samples to the laboratories and returning results to health care providers and patients.
Keshavjee listed several prominent challenges faced by India and other countries. Getting TB under control requires active case finding, not just waiting for very sick people to appear at TB facilities. Health care systems must look for contacts of patients and make sure that those contacts are treated. In addition, Keshavjee argued, given that patients with latent TB form a large part of the disease’s reservoir, treatment of the latent phase of TB must be addressed in order to see large reductions in the incidence of disease.
__________________
3 This section is based on the presentation by Salmaan Keshavjee, Director, Program in Infectious Disease and Social Change, Department of Global Health and Social Medicine, Harvard Medical School.
Keshavjee also argued that, because a large number of patients are treated outside of the public sector, private-sector health care in India needs to be mobilized and optimized. Doing so will require public–private partnerships that can, for example, modernize private-sector laboratories and reach patients who are using the private-sector system. Keshavjee cited as an example a recent project in Pakistan in which health workers screening private-sector patients increased case finding for TB by 400 percent, and this number was even higher for pediatric TB.
Finally, Keshavjee emphasized that improving the treatment of TB requires engaging with efforts to alleviate poverty. For example, Brazil’s recent success in reducing the incidence of TB is due at least in part to its economic performance and to targeted programs that pay poor families to keep their children in school. When poverty was reduced, TB rates fell. Keshavjee noted that India is about to embark on a poverty alleviation program that will affect hundreds of millions of people, and evaluations of the effects of this program on TB rates will be of interest.
In recent years, Russia has improved both the diagnostic capabilities of its health care system and the availability of FLDs and SLDs, said Grigory V. Volchenkov, Chief Doctor, Vladimir Oblast TB Dispensary, Center of Excellence for TB Infection Control. Russia’s efforts to address the transmission of DR TB have focused on health care settings, penitentiary settings, and other congregate settings. According to Volchenkov, a major program of infection control (discussed in Chapter 7) has brought the rate of occupational TB transmission in the Vladimir region to zero over the past 4 years. “We learned that we can make health care settings safer and less expensive,” said Volchenkov. These savings have in turn freed up resources for diagnostics and treatments.
Volchenkov listed what he considered the most important steps for Russia to take to control DR TB:
• introduction of rapid molecular diagnostics for TB case finding at the subregional level;
• improved quality assurance in TB laboratories;
• sustainable supplies of FLDs and SLDs;
• strict adherence to evidence-based treatment regimens and directly observed therapy;
__________________
4 This section is based on the presentation by Grigory V. Volchenkov, Chief Doctor, Vladimir Oblast TB Dispensary, Center of Excellence for TB Infection Control.
• a shift in the TB care paradigm from over-hospitalization to more outpatient services;
• closer integration with the HIV program; and
• the development and implementation of public health—oriented transborder TB control policies.
China has a great opportunity to provide leadership in addressing TB not only in China but around the world, said Yanlin Zhao, Vice Director, National Center for Disease Control and Prevention; and Director, National Tuberculosis Reference Laboratory, Chinese Center for Disease Control and Prevention (China CDC). But it also faces significant challenges posed by its high burden of MDR TB. Obtaining a fully accurate picture of the MDR TB burden in China remains difficult, particularly in vulnerable groups such as rural and migrant populations. Transmission control also remains a challenge, especially in facilities in remote areas that serve large numbers of patients. Yanlin Zhao said China is eager to learn from colleagues in other countries that have experience with community-based care and decentralized case management. In some provinces in which large numbers of men migrate to find work, rates of infection are high. Women may have lower rates of infection, but because of the persistent stigma associated with TB, they do not always get adequate care. And if care is not adequate, transmission of the disease is greater, which can lead to a higher prevalence of MDR TB.
To address these challenges, China recently enacted several major health care system reforms. MDR TB is now covered by medical insurance for all patients, with up to 70 percent of the cost of treatment being reimbursable, and this has significantly reduced the financial burden on MDR TB patients and their families. The health care system in China also has created a prevention network extending from the local to the national level to identify MDR TB patients and refer them to facilities where they can receive the proper treatment. This network is linked to a national TB surveillance system that provides patients with care as early as possible and also produces data for use in understanding the burden of MDR TB. These data, in turn, help with the management of diagnosis, treatment, infection control, health care worker training, and TB drug supplies.
__________________
5 This section is based on the presentation by Yanlin Zhao, Vice Director, National Center for Disease Control and Prevention; and Director, National Tuberculosis Reference Laboratory, Chinese Center for Disease Control and Prevention (China CDC). Zhao was the first author of the “milestone” epidemiological study published in the New England Journal ofMedicine in 2012, noted by Cassell earlier in the discussion (Zhao et al., 2012).
China has been acting both within the country and around the world to stop the spread of MDR TB and treat patients, Yanlin Zhao said. Although wealth alone cannot solve all problems, China’s innovative and dynamic economic expansion can bring both new and existing solutions to bear in addressing the problem. Improved surveillance is creating a better understanding of the problem and of potential solutions, new diagnostic capabilities are being implemented across the country, and MDR TB treatment is becoming more accessible and affordable.
The Chinese government has been investing in diagnostic technologies, such as a biochip designed to enable identification and treatment of patients as rapidly as possible. The country has a strong scientific research capability to contribute to the development of new drugs and drug regimens and to bring that knowledge to the pharmaceutical industry so that quality products can be produced for patients in China and other countries. Chinese scientists and specialists continue to conduct investigative studies to understand the burden of TB, the disease strains, the effectiveness of infection control measures, and means of assisting vulnerable populations and to explore novel drug therapies.
China combines a fast-paced and fast-growing manufacturing sector with high-technology modern information management systems that can report data on diagnosis, treatment delivery, and treatment adherence from the local to the national scale, Yanlin Zhao said. For example, cell phones have been used in a pilot study to alert or remind patients to take medicine and also to convey information about side effects of treatment to physicians.
China has a long and, some might say, “patient” view of history, Yanlin Zhao concluded. But China today is a fast-paced country undergoing rapid change. Addressing the enormous challenge of MDR TB requires both patience and resilience because the problems are complex and multifaceted and cannot be solved overnight. But it also requires acting with a sense of urgency to provide treatment to all those with MDR TB in China, and to reduce the burden of MDR TB in China and the rest of the world. China has the capability to act quickly, said Yanlin Zhao. “China will, together with you, harness our individual and collective resources to break down the walls that impede treatment and [address] this challenge that we all face together.”
This page intentionally left blank.












