Vulnerable Populations and Opportunities for Reducing Health Risks
Workshop participants identified many immediate opportunities and models for addressing health needs of those involved in the criminal justice system. Proposals addressed care and health interventions for a range of vulnerable populations, including not only inmates but also their families as well as those recently released. Many of these proposals involved changes to the workforce, such as retraining parole officers, educating judges, raising the skill of screeners, and hiring former inmates as community health workers. Throughout the discussion, workshop participants expressed awareness of the potential of many measures to perform a threefold function: prevent incarceration in the first place; treat the health needs of the currently incarcerated, their families, and the released; and prevent recidivism.
As a preliminary note, Newton Kendig reminded participants of the great range of inmates: “Incarcerated populations are extremely diverse, depending on geography, ethnicity, gender, and healthcare needs.” Correctional facilities are also very varied, from prisons holding inmates serving lengthy sentences to local jails with their “hyperdynamic population movement.” Finally, regional variations are also significant. For example, “in Appalachia, methamphetamine oral healthcare could be the number one issue at intake. In an inner city area, it could be HIV and Hepatitis C. On the border of Mexico it’s drug-resistant TB.” Thus, Kendig warned, it is likely not all proposals or priorities will apply across the correctional system.
The health needs of inmates with a history of mental illness or addic-
tion received considerable attention in the workshop, as did the health profile of older adults, women, and youth in prisons and jails, and families of those incarcerated, as well as individuals recently released from prisons or jails.
Overrepresentation
The overrepresentation of people with behavioral disorders in the correction systems was the focus of a workshop presentation by Fred Osher (Council of State Governments’ Justice Center). Osher explained that 5 percent of the general population are estimated to have a serious mental illness (Kessler et al., 1996); and while the rates are not directly comparable, other studies have shown that the rate is much higher among the incarcerated population, and especially so among women. In state prisons, 24 percent of women and 16 percent of men have a serious mental illness (Ditton, 1999). In jails, 31 percent of women and 15 percent of men have a serious mental illness (Steadman et al., 2009). Osher noted, “We don’t understand that exactly, but we’ve clearly got a big challenge with this gender disparity and responding in appropriate ways to the needs of women in correctional settings.”
Osher also offered estimates for substance abuse among prisoners, observing that while less than 20 percent of the general population suffer addiction, the figure in prisons and jails approaches 50 percent (Karberg and James, 2005; Mumola and Karberg, 2006). Co-occurring mental disorder and substance abuse is also very high. In the general population, about 25 percent of those with a serious mental illness have a co-occurring disorder, while in jails, more than 70 percent of those with a serious mental illness have a co-occurring disorder (Kessler et al., 1996; Ditton, 1999; James and Glaze, 2006; Steadman et al., 2009). Again, the rates are not directly comparable across different studies and time periods, but the potential differences are striking. The co-occurrence of mental disorder and substance abuse can complicate the detection of either, particularly when staff or diagnostic instruments are insufficiently sensitive, or where overcrowding and/or understaffing reduces the time spent on medical screening. Osher termed such co-occurrence a “critical issue” that needs to be addressed at points of both entry and exit from the correctional system.
While Osher’s figures highlighted those with serious mental illness (e.g., major affective disorders or schizophrenia), Fellner broadened attention to inmates whose mental health problems are less severe but might still lead to significant functional disabilities. This describes over half the incarcerated population. Fellner provided figures indicating that 56
percent of state prisoners have a mental health problem. Again, rates are substantially higher among women inmates, as 73 percent of women and 55 percent of men in state prisons have mental health problems (James and Glaze, 2006).
The overrepresentation of the mentally ill among the incarcerated is a prominent trend across the country though rates of mental illness vary somewhat across state and federal prisons and local jails. As Shannon Murphy (Montgomery County’s Prerelease and Reentry Center, Rockville, Maryland) observed, in the relative paucity of either mental health facilities or community support systems, prisons are now “the de facto chronic mental health system” in the United States. Craig Haney further suggested that the magnitude of the problem is undercounted and underestimated. In Haney’s view, the underestimate “creates a kind of ripple effect through the problem. If resources aren’t adequate to the task at hand then there is a way in which that unsolved problem tends to get greater rather than simply stay in its underestimated size.” Haney cited as an example the “so-called California overcrowding case” that culminated at the Supreme Court (Brown v. Plata), but which actually began as a mental health case. Litigation to ensure constitutionally adequate care for mentally ill prisoners brought attention to runaway overcrowding that exacerbated mental health and medical problems and caused the level of care to fall below constitutional standards.
Reflecting on the disproportionate numbers of people with untreated or undertreated mental health problems and addiction in the prison population, Allen noted that, given the lack of adequate care, “what we’re left with is a very large number of people with compelling health needs who are ultimately incarcerated in institutions whose mission is security and where [medical] treatment is an afterthought if it even occurs at all.” This theme of an inherent tension of attempting to provide therapeutic care within institutions organized for security recurred throughout the workshop (see further discussion below).
Treatment
Redonna Chandler (National Institute on Drug Abuse, National Institutes of Health) framed the value of addressing mental illness and addiction succinctly: “What are the health issues that if we addressed them could help to deal with some of the root causes of incarceration? Addiction and mental health are two of the primary health conditions. If those can be effectively addressed within the community, then you can lower the number of people who are incarcerated and the number of people who are re-incarcerated because of violating conditions of supervised release.”
Participants offered several proposals to address mental illness and addiction before, during, and after incarceration.
Osher offered a somewhat different perspective: “What I want to say as a main point here is that it’s just not as simple as we’d like it to be. Just treating mental illness or substance abuse disorders may not in and of itself be our solution to [reducing the prevalence of individuals with behavioral disorders in the criminal justice system].” Osher grounded this view in results of a study of inmates in Hawaii with schizophrenia spectrum disorder. The study suggested that for two-thirds of these inmates, factors other than mental illness or substance abuse had led to their initial incarceration or recidivism. Those factors, Osher emphasized, are the very same factors that explain why people without behavioral disorders become incarcerated. Osher identified these as the “central eight dynamic risk factors” that account for much of the variance in people becoming incarcerated: antisocial attitudes, antisocial friends and peers, antisocial personality patterns, substance abuse, family and marital factors, lack of education, poor employment history, and lack of pro-social leisure activities. Each of these risk factors, Osher emphasized, can be addressed through interventions. Osher further acknowledged that people with mental illness tend to have significantly more of the central eight dynamic risk factors.
To address these dynamic risk factors, Osher proposed adherence to the principles of the Risk-Needs-Responsivity Model (Andrews, 2006; Andrews and Bonta, 2006). The Risk Principle consists of screening an individual inmate’s risk of reoffending and matching the intervention to that level of risk. The Needs Principle consists of targeting the inmate’s criminogenic needs. According to Osher, the more criminogenic needs are targeted, the larger the effect of the intervention. The Responsivity Principle calls for tailoring the intervention to the learning style, motivation, culture, demographic, and abilities of the individual inmate. Osher clarified that while mental illness itself is not a criminogenic risk, and not one of the central eight dynamic risk factors, it can have a major impact on responsivity. Thus, “mental illness must be addressed so that the individual can fully engage in the interventions that are associated with reduced recidivism.”
Osher offered further advice on applying the Risk-Needs-Responsivity Model, particularly because of the potential to actually increase the rate of recidivism. According to Osher, “we know in fact that if you don’t attend to risk that you can actually do harm. We know that the largest impact on recidivism takes place when the focus is those individuals with [higher risk levels] and that one can actually increase recidivism if low risk individuals are the focus of treatment.” Osher referred to results from a study in Ohio to support this view (Latessa, 2012). He concluded
that “we should prioritize and use scarce resources most effectively to get the public health and public safety outcomes that we want.” That will involve developing the skillsets of those involved in providing the interventions, particularly interventions based in cognitive behavioral therapy. In Osher’s view, “there’s a large workforce development issue that we need to be mindful of.”
During discussion, Taxman highlighted the varying definitions of and perspectives on the concept of an antisocial personality, as well as the “diverse and inconsistent measurement of that particular domain.” Taxman also observed that it is a “very controversial issue in the field, whether or not mental illness is a criminogenic need or not, whether or not treating mental illness will reduce recidivism rates.” Her sense is that “over the last ten years I think the field has moved in a direction recognizing that [mental illness and criminogenic risk] are different entities.”
Taxman concurred with Osher regarding the imperative of developing the workforce to provide effective behavioral interventions. She particularly discussed retraining probation officers and parole officers to undertake roles as social workers and behavioral managers, rather than perform as agents of enforcement and security. “When probation officers and parole officers use behavioral management techniques,” Taxman declared, “it works.” In accordance with the Risk-Needs-Responsivity Model, Taxman suggested that correctional staff should identify the risks and needs of individuals, and then work with them to develop “problem-solving techniques.” An essential component of the process is instilling a sense of responsibility in the individual. According to Taxman, if the individual is to be compliant “for everything from [not] offending through [following through with] primary healthcare, then really the individual needs to have much more responsibility.” She therefore advocated less of a focus on any particular program for inmates, and greater effort to have probation and parole officers “help people make choices in their lives, how they are going to get through probation successfully.” Taxman saw great potential when supervising officers are trained less as agents of social control, and more as facilitators of behavioral change with an emphasis on helping individuals exercise responsibility and self-determination. According to Taxman, “If we don’t change the criminal justice policies … that focus just on monitoring conditions of release, then we’re not going to make progress toward a system so that people can take care of their own needs outside of the criminal justice system.” If this could be accomplished, Taxman argued, inmates could “find a way to become more contributing members of society and find value in their own lives.” Currently, however, “that’s not something the criminal justice system is invested in doing.”
Addressing substance abuse effectively was another priority
addressed in the workshop. Participants noted that there are many evidence-based treatments for substance abuse, both behavioral treatments and medication-assisted treatments. As Chandler lamented, however, “the capacity for delivering those treatments is limited and fragmented.” The delivery of evidence-based behavioral treatments is poor; the delivery of medication-assisted treatments is even worse. This is the case even though, explained Chandler, “we know that medication can help address opiate addiction, alcohol, as well as nicotine. It’s one of the most effective interventions we have. Yet when you look at the number of individuals that could potentially benefit, only a very small portion is being served.” Thus, expanding substance abuse treatment, including medication-assisted treatment, is critical.
Chandler dwelt further on the imperative of providing continuing treatment during re-entry. As she explained, “Study after study after study has shown that if you only provide treatment to an individual while they’re incarcerated and you don’t follow that up with ongoing care when they re-enter the community, you are not going to be able to significantly impact their drug use.” Two factors are closely linked to relapse. One is the cue-rich environments to which addicts return, cues that the underlying neurobiological mechanisms in their brains have associated with their drug use, triggering craving. The second is the incredibly stressful situation of re-entry itself, which also triggers neurobiological responses that lead to an increased risk of relapse.
Workforce issues also figured in the discussion of substance abuse treatment. “It’s really important,” Chandler affirmed, “to make sure that criminal justice actors, and especially leaders, understand the underlying and important health problems of this population.” Unfortunately, addiction is widely misunderstood. In her assessment, “very few people outside of the healthcare field—and even within the healthcare field— understand the underlying neurobiological principles of addictive disorders. If they don’t understand that they see it as moral failing, they blame the individual, and then they’re reticent to provide treatment or to be open to other types of models of care.” Because of her years of involvement in training judges, Chandler appreciates the value of such training. She described, “seeing the light bulb go off in their heads,” and their subsequent return to their jurisdictions to enact “radical changes in the way they deal with the problem of drug abuse because they understand the underlying biological processes that are occurring.” Chandler concluded, “Where there is ignorance I think we have the opportunity to shed some light, and that’s going to be really important if you want these partnerships and collaborations, and if you really want to be able to optimize outcomes.”
The proportion of older adults in the criminal justice system, and resultant healthcare concerns, have increased sharply (see Figure 2-1). In her presentation, Brie Williams (University of California, San Francisco) described the trend. From 1990 to 2012, the U.S. population age 55 or older increased by about 50 percent. In that same period, the U.S. prisoner population age 55 or older in the state and federal prison systems increased by some 550 percent as the prison population doubled. “This increasing number of older adults,” Williams declared, “really changes the entire health landscape of the correctional system.”
Williams explored several characteristics of the disease burden of older adult inmates. First, as in the general population, older inmates have the highest rates of typical chronic health conditions (congestive heart failure, diabetes, chronic obstructive pulmonary disease, etc.) and serious life-limiting illnesses. Second, older inmates also have very high rates of additional geriatric syndromes such as cognitive impairment or dementia, and disabilities or impaired ability to perform activities of daily living. Some of this disability is common to the general population, such
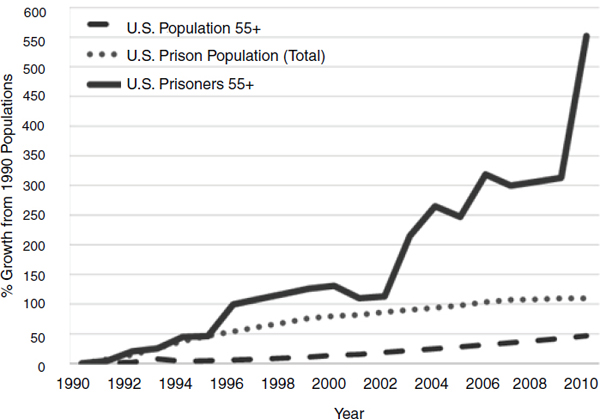
FIGURE 2-1 Rate of growth of older adults in the criminal justice system.
SOURCE: Williams et al. (2012a).
as impaired mobility or the need for assistance with eating or bathing. Other disabilities are unique to the prison environment, such as not being able to drop to the floor as instructed in response to an alarm or, worse, not being able to get back up again after the alarm is over, or difficulty climbing on or off one’s assigned bunk. Because of the unique challenges of a prison environment and the resulting disabilities, Williams explained, “In older adults, simply cataloguing chronic disease is insufficient.” Given aging trends of the incarcerated population and their associated health conditions, Williams observed that “correctional institutions are increasingly becoming a critical delivery site for long-term care or nursing home-level care, as well as palliative care or care for people with serious chronic illnesses.”
In confronting and meeting the needs of the rapidly increasing older adult inmate population, Williams underscored the importance of examining both health and nonhealth policies of the criminal justice system. Beginning with health-related policies, Williams advocated four immediate changes. First is to screen for and address cognitive impairment and dementia, and then incorporate these screening results into court proceedings, healthcare delivery, parole, probation, and release planning. This would have extensive repercussions for workforce training, as it would involve “everyone from police and judges and attorneys, through jail and prison clinicians, and then people responsible for probation and parole.”
A second imperative is to define and address disability, with attention to “what disability looks like in the correctional setting.” This would involve delineating the basic physical tasks that are necessary for a person to function with independence by housing unit, and then matching these physical tasks to prisoner abilities when housing is assigned. “This seems very basic,” Williams observed, “and [surprising] how infrequently it happens.” A re-screening schedule should then be implemented, especially because sentences have grown longer. Very often the only disability assessment is performed at intake, even if an individual is incarcerated for decades.
Williams’ third suggestion was to develop plans for long-term care and nursing home-level care, essentially a continuum of care across the spectrum of disability, with criteria for classification in different care levels. This would include enhanced palliative care or symptom-based chronic care management for people who are seriously ill. “I would love to see [the rate of incarceration decrease],” Williams remarked, “but until it does, I think we need to make these plans.”
Her fourth health-related policy proposal was to create a national medical release or so-called compassionate release guideline. These uniform guidelines would be based in scientific evidence from palliative and geriatric medicine and clinical medicine in general. Barriers that
prevent medically eligible persons from obtaining release would have to be addressed. Fellner concurred on the significance of compassionate release and noted that the Federal Bureau of Prisons and most states have provisions for releasing inmates in extraordinary and compelling circumstances, but that these are “greatly underutilized.” Fellner urged that healthcare providers “be involved in trying to make those [provisions] work.”
Williams expanded her suggestions to the nonhealth policies that have unanticipated health consequences on the growing older adult inmate population. “Good people can take different sides of each of these issues,” she acknowledged. “My point is not to say which [side] of these issues is correct or not correct, but to say that these points need to be debated given the changing demographic of the population.” Williams highlighted three such policies as meriting re-examination. First is sentencing decisions, as “three strikes [policies] and life without possibility of parole have really resulted in a higher concentration, very simply, of older and sicker persons across the nation in the correctional setting.” Second is facility policies, such as lockdowns and administrative segregation, because “evidence suggests that these may increase disability and deconditioning specifically for older prisoners or for those with chronic impairments.” Finally, a careful review of “well-meaning state-wide reorganization efforts that can be dramatic and really large in scope,” but may have unintended effects—such as shifting older adult inmates from prisons to jails, “which [often] have fewer healthcare resources, especially for chronic disease management.” In concluding, Williams affirmed the responsibility of the medical profession to “help with criminal justice policy, and be at the table to anticipate potential health consequences [of] both health policies [and] nonhealth policies.”
Although female inmates are only about 10 percent of the correctional population, they present higher rates of disease and additional reproductive health issues. As noted earlier, mental health disease burden is considerably higher for women than men. Very high rates of childhood sexual abuse and post-traumatic stress disorder are prevalent among female inmates. Given the disproportionate burden of mental illness borne by women inmates, the proposals for addressing the mental health needs, discussed above, are particularly applicable to this population.
Jennifer Clarke (Brown University Medical Center) addressed health issues of incarcerated women, particularly reproductive health. Clarke estimated that 5 to 6 percent of women coming into prisons or jails are pregnant. The data on birth outcomes vary, but in general, babies weigh
more the longer a woman is incarcerated. Reasons for better birth outcomes are likely better access to prenatal care, decrease in substance use, and, for some, stable housing and regular meals. Clarke hastened to note, “I always have to follow that by clarifying I am not advocating incarcerating pregnant women but rather underscoring the need for this population to have services in the community.”
Clarke also commented on the research finding that most of the women who enter incarceration pregnant had conceived within three months of leaving a prior incarceration. This emphasizes the need for correctional facilities to provide family planning services, as most so-called “pregnant women days” within prisons are from women who have been imprisoned previously where a more stable diet and less access to drugs may have improved fertility, and upon release, without family planning services, conceived promptly. The stress of an unplanned pregnancy could add to their difficulty of getting re-established in the community, and some are soon re-incarcerated. Clarke shared research that indicated that about 70 percent of women in the criminal justice system who are at risk for an unplanned pregnancy indicated they want to start a contraceptive method.
Sexually transmitted infections (tested on entry to prison or jail) are about 10 to 20 times higher in the incarcerated female population than the general population, and at least twice as high as that of the incarcerated male population. As health consequences of such infections for women are much greater than they are for men, Clarke affirmed the paramount importance of screening and treating women for such infections as they enter prisons and jails.
Clarke also offered observations on the rise in obesity. Women on average gain over a pound a week when incarcerated. A year’s incarceration thus results in over a 50-pound weight gain, with considerable consequences for both the physical and mental health of women inmates.
Clarke underscored the imperative of providing reproductive healthcare, with attention to continuing care after release. Recalling evidence that women expressed interest in starting a contraceptive method and also acknowledging that “there have been a lot of abuses in the past of reproductive freedom,” Clarke advocated the availability of reversible contraceptive methods.
Asked about the provision of nurseries in correctional facilities, Clarke noted “great outcomes,” including better bonding and more breastfeeding, when this is possible. Given the small size, limited resources, and security concerns of many facilities, however, Clarke acknowledged that nurseries are not universally feasible. She therefore concluded, “I think it’s in the best interest of correctional facilities to do the preventive healthcare to prevent needing a nursery later on.”
Youth were not a focus of presentations in the workshop. However, Chandler remarked on this lacuna, asserting “we’re missing a tremendous opportunity by not talking about adolescents and juvenile justice.” Taxman observed that there are more youths in the juvenile justice system than in foster care. Chandler provided figures indicating that approximately 1.5 million adolescents are involved in the juvenile justice system, either in community programs or detention centers. These youth have tremendous healthcare needs, including addiction, mental health problems, and infectious disease. If those needs are not addressed effectively, Chandler affirmed, there are two outcomes for these youth: premature violent death or involvement in the adult correctional system.
What initiatives could be undertaken to address the health needs of youths in the criminal justice system? According to Chandler, “This is the only population that we can name where we can safely say that all of the individuals in this population merit [screening for addiction and identifying] a drug abuse intervention.” She advocated “comprehensive screening for all adolescents in juvenile justice to determine the severity of their substance abuse problem,” to be followed by “either an indicated prevention intervention or a drug use treatment intervention.” Chandler estimated that half of youth in the juvenile justice system have a substance abuse problem severe enough to warrant a diagnosis; thus, “you’re going to be providing treatment to a large number of adolescents.”
The public health impacts of soaring incarceration rates are manifold. Relevant vulnerable populations include not only the incarcerated, but their family members as well. Christopher Wildeman (Yale University) offered several insights in his presentation on the effects of incarceration on the health of family members. Prisoners are embedded in social networks. Thus, Wildeman emphasized, for every individual inmate, a far greater number of family members may be affected. As the incarceration rate soars, so does the number of family members affected by incarceration. All of these people—the partners, children, and siblings of inmates—are drawn into the correctional system when a family member is incarcerated.
Considering the health of this population, Wildeman began by noting that they are exposed to the same risk factors for poor health as are the individuals who actually experience incarceration: the same socioeconomic status, education levels, and neighborhood exposures. This suggests a probable overlap in health problems, including mental health problems. In Wildeman’s view, this is “a tremendously vulnerable popu-
lation even if you assume having a family member incarcerated has no health impact on them.” Increasing evidence, however, suggests that incarceration does compromise the health of family members, amplifying the public health impact of increased rate of incarceration.
Wildeman considered the potential of using the criminal justice system to find ways to improve the health of this population, even though they are not directly involved in it. He particularly proposed that the process of prisoner release might be an opportunity to gather information about family members. This could facilitate enrolling them in social services, Medicaid, or other programs. In this way, indirect contact with the criminal justice system might have some benefit for this population, particularly as the bulk of this population is not now enrolled in any healthcare plan.
As explained in the background paper, the period immediately following release from prison or jail is especially risky (Rich, Dumont, and Allen, 2012). While mortality rates within prisons and jails are comparable to those of the general population for white males and lower than their nonincarcerated peers for black males, former prisoners are nearly 13 times more likely to die in the two weeks following release than the general population (Binswanger et al., 2007). In particular, former prisoners are 129 times more likely than the general population to die of an overdose during that period. This reflects both the challenges faced upon return to communities and the insufficient nature of substance abuse treatment during incarceration, during which prisoners may not realize their tolerance to opiates has declined. Despite efforts to improve the outcomes of prisoner re-entry through assistance with employment, housing, and other transitional needs that ultimately affect health, only about 10 percent of prisoners from state prisons in need of discharge planning actually receive it (Mellow and Greifinger, 2007). In general, mentally ill prisoners and those with HIV are more likely than others to receive discharge planning. Nonetheless, they are also more likely to be homeless and rely on extensive emergency department healthcare post-release. Although inmates with mental illnesses are generally given a supply of medications upon release, medication adherence falls off rapidly upon release.
Emily Wang (Yale University) addressed the health of the newly released based on her experience and research with the Transitions Clinic Network. This is a national network of programs currently operating in six states, the District of Columbia, and Puerto Rico, based in community health centers and providing primary care to individuals post-prison. Wang confirmed that the immediate aftermath of release is a particularly
risky period. She noted a worsening of chronic medical conditions and substance abuse, and a high risk of hospitalization and risk of death among the newly released. Based on her research among clients of the Transitions Clinic in San Francisco, Wang observed that many had not received any discharge planning, and had either short or no supply of medications. Among the clinic’s patients, 69 percent were uninsured. For those who had been enrolled, Medicaid or Medicare Part B had lapsed while they were incarcerated. Finally, drug felons faced additional barriers to meeting their basic needs and getting access to food stamps or housing assistance. Immediately post-release, 93 percent were homeless or at risk for being homeless. Wang also discovered that 39 percent of the clinic’s patients went a whole day without food.
An overriding priority in dealing with release is providing continuity of care, whatever care that might be, whether it is for treatment for addiction or mental illness, for reproductive care, or for management of chronic disease. The risks involved at the moment of re-entry, and the likelihood that healthcare would be interrupted, were reiterated several times during the workshop. Wang offered other insights from the focus groups that Transitions Clinic Network has conducted. Participants in these groups consistently express three preferences. They asked that primary care providers possess relevant cultural competence, and specifically that they have past experience caring for patients with a history of incarceration. They also requested community health workers with a history of incarceration to assist with patient navigation of the social service system and the healthcare system, as well as provide support in care management and chronic disease management. Their third request was access to primary care within the first two weeks after release.
Wang incorporated these preferences in developing suggestions for addressing the needs of inmates upon release. Her first proposal was that individuals with a past history of incarceration be involved in improving the healthcare of returning prisoners. This is an issue of workforce training and cultural competence, as well as providing former prisoners with a role in decision making or “having a seat at the table.” Addressing all these issues would entail “people with experience of incarceration coupled with proper training as a community health worker to help patients navigate the healthcare system following release, and really deal with all the social issues that might emerge in those days, weeks, months post-release.”
Wang’s second suggestion was to improve transitions from prison to community healthcare systems. Relevant evidence-based steps start with basic discharge planning, refilling medications, and ensuring availability of medical records. Several workshop participants mentioned the possibility that electronic medical records might ease this last task. Wang also
cited evidence-based methods for preparing community health centers to facilitate early access to care in the primary care setting.
As discussed more fully below in the context of the Patient Protection and Affordable Care Act, Wang’s third suggestion was to eliminate barriers to Medicaid enrollment and reinstatement. Her final suggestion was to eliminate full or partial food-stamp bans and barriers to housing and employment. Even where barriers are not formal or direct, regulations— such as the requirement of specific forms of identification—can block access to food aid or other services. “Time and time again, among the patients that I’m seeing, post-release, two weeks on,” Wang explained, “they’ve already come to the physician, they’re interested in their health, and the really crippling part is there are so many other needs there that they’re unable to attend to their health in the best possible way.” She cited evidence of access to food, “just the barebones importance of food,” as particularly crucial for this population.
Wildeman concurred, adding “if we just improve the medical care that [former inmates] receive but we don’t attend to their homelessness as a passive result of incarceration, or economic instability, or labor market outcomes, or family life,” then we miss much that has “a really profound effect on their health over the life course as well.”
A further set of suggestions emerged during workshop discussions. They dealt less with any particular inmate population, and more with how healthcare and criminal justice professionals approach the provision and context of care. Much of this involved education. For example, Williams advocated that healthcare professionals educate others about the health needs of aging inmates. She noted that as her team trains police, judges, public defenders, district attorneys, and correctional officers about dementia, “across the board people are [often] relieved to be finally getting healthcare information that [can] make their jobs both better, more rewarding, and less stressful.”
In response, Wang noted that healthcare providers need to be educated about many aspects of the criminal justice system. She lamented that primary care providers practicing in federally qualified health centers are seeing patients with a past history of incarceration, perhaps recently released, and yet have no idea of the type of care these patients have received during incarceration. Wang suggested that both criminal justice professionals and healthcare providers need to develop cultural competence when dealing with this population.
Steven Rosenberg (Community Oriented Correctional Health Services) pursued the theme of cultural competence, suggesting that health-
care providers should attempt to understand not only the conditions faced by inmates while incarcerated and upon release, but also the pressures faced by criminal justice professionals—thus becoming “cross culturally competent” so as to avoid possible conflict. Allen challenged this perspective, suggesting that no change of cultural frame would eliminate the innate conflict between providing care while simultaneously fulfilling a goal of security. Such conflicts cannot be navigated past: “They’re baked into the pie. There are two functions and they come into conflict.”
Yet Allen agreed on the imperative of mutual respect between corrections officers and healthcare providers: “It’s really important while we demand respect from custody [staff], that we’re also able to return it and learn to speak their language as much as we ask them to speak ours.” This is a matter of practical importance, “because you can talk all day about the ideals of medicine, but if you can’t translate it into how they can actually apply what you’re recommending in a way that they will still have their job at the end of the year, you’re just spinning your wheels.”
















