It was only after 2001 when Indonesia shifted from a highly centralized system of government to a decentralized one that governance became an issue of public debate. The public no longer remained a passive recipient of public sector development activities under the authoritarian regime; instead, it began to demand accountability from the executive and the legislature. These changes grew out of democratization and decentralization, but soon it became clear that these values themselves had become issues and even obstacles to the practice of good government.
This chapter looks at the impact of decentralization on public services in general, and on services related to maternal and neonatal health in particular, in the context of regional inequality and local politics in search of accountability. Although decentralization has allowed rapid expansion of the civil service, access to health services has not improved as expected. Indeed, public health services are even more difficult to access, forcing not just better-off but also poor mothers to turn to the private sector when giving birth. And thus the search for accountability has led the central government to develop guidelines for setting minimum service standards (MSS), which are supposed to be adjusted to local conditions by regional governments. However, the standards are outcome indicators for program evaluation without the meaningful measurements that would allow civil society and consumers of public health services and facilities to monitor and evaluate government responses to the needs and demands of its citizenry.
Decentralization
In 2001 Indonesia moved from a highly centralized government to a decentralized one; provinces, districts, and municipalities were extended the autonomy to choose and then plan their respective development paths. At the time, the demand for decentralization was widespread. It held the promise of hastening the development process, particularly for the poor, because of the greater proximity between policy makers and the people and the assumption that local governments know best the needs of their constituents (Conyers, 1984; Bird, 1993; Oates, 1999; Braun and Grote, 2000; Katsiaouni, 2003).
When implemented in 2001, the decentralization laws took effect nationwide, regardless of local conditions, the state of preparation of local institutions to deal with the responsibilities and consequences of the change, and the new public expectations of good governance practices. The “big bang” approach ignored not only the nation’s various levels of general development but also the differences in the quality of and access to public services (Hofman and Kaiser, 2002). Dissatisfaction with the initial results of decentralization led to amendments in 2004 to the original law that further extended authority to the provinces as extensions of the central government. For example, the Ministry of Health can earmark resources for specially designed programs for mothers and infants at the grassroots level through the mediation of the provincial and district/municipality health services offices.
Local Governments and Civil Servants
Decentralization applies not just to rights but also to responsibilities. Although rights are popular, the responsibilities for ensuring the well-being of constituents have not been embraced in all cases. The benefits
of decentralization have been enjoyed mostly by the local elites at both the province and the district/municipality levels,1 whereas general access to public services, including health services for mothers and infants, have not much improved.
Instead, implementation of the laws has resulted in extending to the local political elites the power and authority to recruit and hire civil servants2 and to allocate and spend more government funds locally. It did not take long for local governments to recognize and employ the power implicit in regional autonomy to ignore with impunity instructions from the central and provincial governments.
As a result, decentralization has been accompanied by the growth of public sector employment in the regions. In fact, most of the growth in the civil service can be attributed to the creation of new autonomous regions. Until 1998, when the centralized New Order government fell, there were 26 provinces and 299 districts and municipalities. Discontent with the central government and the promise of a better future under local government and governance fueled the drive to create new autonomous regions. Between 1999 and 2009, seven provinces and 198 new districts/municipalities were added (Direktorat Jenderal Otonomi Daerah, Kementerian Dalam Negeri, 2010), all requiring new offices with mostly new staff, recruited locally and often not qualified. In 2010 a moratorium was introduced to delay the formation of new autonomous regions and curtail growth in the size of the civil service. However, since the moratorium was lifted in late 2012 one province and at least seven new districts have been created, with more requests under consideration.
The new civil service positions are highly valued, particularly in those regions where formal sector jobs with regular salaries are few and hard to find. Moreover, the private sector in those regions remains less developed, operating mostly in the informal, peasant economy, which is still largely dependent on agriculture.
Since 2003, there has been a major transfer of civil service jobs to the districts, and the sharp increase in the size of the overall civil service has become a concern of the central government (Figure 6-1). Of the 3.5 million civil servants after decentralization in 2003, 2.7 million were employed at the regional level. Of this number, only 0.3 million were located at the provincial level, and the remaining 2.4 million were in the district and municipality governments. Between 2006 and 2010, the civil service grew from 3.7 million in 2006 to 4.1 million in 2007 to 4.5 million in 2009, with further slight growth to 4.6 million by 2010. In this period, central government employees expanded by only 0.1 million, to 0.9 million civil servants, and those at the provincial level remained relatively stable, at 0.3 million. By contrast, the civil service at the district and municipality levels increased by almost 1 million, from 2.6 million to 3.4 million local bureaucrats.
Unequal Access to Health Services
In spite of the rapid growth in the overall size of the civil service, public services, including health services, have little improved, and many Indonesians still cannot afford them. In many regions of the country, Indonesian women, especially poor ones, do not have access to the health services they need when giving birth. Health facilities and providers are largely concentrated in urban areas, and thus they are not easily accessible to the poor living in remote rural areas. As described in Chapter 5 (Figure 5-1), in 2010 only a very small percentage of births in Indonesia were attended by trained health staff (general practitioners or specialists). According to the 2010 Indonesian Basic Health Survey (Riskesdas), the majority were attended by nurses or trained midwives, and the rest by traditional birth attendants (TBAs) and others. On every count, Indonesia has been and continues to be characterized by significant regional variation, and the same is true for health services and providers. In some provinces, substantially higher pro-
1Maintaining the practice of “level skipping” embraced by the centralized New Order government of Indonesia (1966 1998), the decentralizing government extended autonomy to the district/city while bypassing the province.
2In most regions beyond the major urban centers, there are few salaried employment opportunities in the formal sector; civil servants hold tenured posts.
portions of births are attended by doctors than the national average. Most of these provinces are located in the western part of the country on the major islands of Java and Sumatra. They include the province of Yogyakarta, which is known as a center of higher education; the capital city of Jakarta; the dynamic industrial province of Riau Islands; and the global tourist destination of Bali. At the other end of the spectrum are the underserved provinces where relatively few births are attended by trained health services providers. These provinces are mostly located in Eastern Indonesia, where poverty is also more widespread and trained health staff are highly underrepresented. According to Table 6-1, in recent years women with limited education and those from poorer households have been much less likely to give birth in health facilities. Among those with less than a primary school education or from the lowest wealth quintile, more than three-quarters have given birth at home.
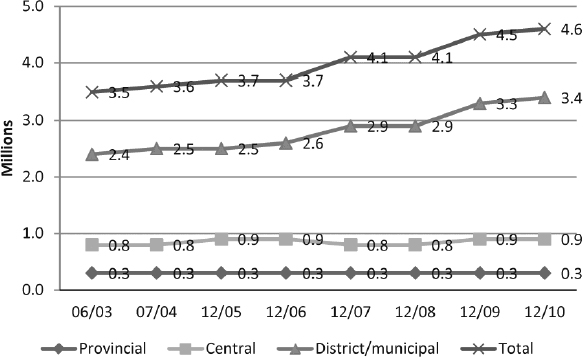
FIGURE 6-1 Number of Civil Servants by Level of Government: Indonesia, 2003 2010. SOURCE: Badan Pusat Statistik, Statistical Yearbook of Indonesia (various years).
| Education and Wealth Quintile | Health facility | Home | Other | Not specified | Sum | |
| Public | Private | |||||
| Education | ||||||
| No schooling | 5.9 | 9.5 | 81.4 | 1.4 | 1.8 | 100.0 |
| Less than primary school | 5.8 | 16.1 | 76.6 | 1.0 | 0.5 | 100.0 |
| Primary school | 7.1 | 23.8 | 67.2 | 0.9 | 0.9 | 100.0 |
| Less than secondary school | 9.6 | 39.1 | 50.2 | 0.5 | 0.7 | 100.0 |
| Secondary school + | 14.2 | 57.1 | 28.2 | 0.3 | 0.3 | 100.0 |
| Wealth quintile | ||||||
| Poorest Q | 5.2 | 8.4 | 84.8 | 0.9 | 0.7 | 100.0 |
| Q2 | 8.3 | 23.4 | 66.8 | 0.5 | 1.0 | 100.0 |
| Q3 | 11.4 | 36.5 | 51.1 | 0.6 | 0.4 | 100.0 |
| Q4 | 12.2 | 49.5 | 37.1 | 0.7 | 0.5 | 100.0 |
| Wealthiest Q | 12.3 | 71.0 | 15.5 | 0.6 | 0.6 | 100.0 |
| Total | 9 7 | 36 4 | 52 7 | 0 7 | 0 6 | 100 0 |
SOURCE: Badan Pusat Statistik and Macro International (2007: 138).
Local Politics
Before implementation of the decentralization laws that extended autonomy to regional governments, Indonesia’s great diversity was largely ignored in the government’s pursuit of a one-size-fits-all approach to programming and project design, despite clear differences among regions in environment, infrastructure, and natural and human resources. Public policies were determined nationally, and local governments—from the provinces and districts or municipalities to subdistricts and villages3—implemented decisions made in Jakarta.
Central-Regional Relations
Central-regional relations have changed dramatically under decentralization. In most sectors, including health, the vertical lines of authority from the central to local governments have been eliminated, and many of these local governments have wide discretion to prioritize services and determine local administrative organization. Certain services, however, including health services, are defined as obligatory functions, and local governments are required to have a common structure of facilities and to maintain separate health services offices (dinas kesehatan).4 Maternal and child health services are not mandatory, but, because of their importance, nearly all local health services have a unit for these services (Ministry of Health, 2008a). In an exceptional crisis such as an epidemic outbreak, the Ministry of Health can also mobilize the Health Crisis Center, a vertical organization under its authority that reaches down to the district or municipality level to offer human and monetary resources that have been earmarked for such use by the central government.
An exception to decentralization is international agreements; these are made only in the name of the central government. This situation applies to Millennium Development Goals (MDGs) 4 and 5, which are aimed at reducing maternal and child mortality. For such initiatives, the central government uses its own departmental funds to support the relevant programs and projects throughout the country, and funds are earmarked for particular activities for implementation by local governments. These earmarked resources, dekon, go first to the provincial governments and then for implementation to the district or municipality level.5 Another model is described in Box 6-1.
Besides these earmarked departmental funds, local governments also receive substantial support through general transfers known as DAU or dana alokasi umum (general allocated funds)6 as well as special earmarked sector-specific grants known as DAK or dana alokasi khusus (special allocated funds), one of which is for health. However, often the great bulk of DAU goes to cover PNS (pegawai negeri sipil) or civil servants’ salaries, which account for 70-80 percent of most regional budgets, leaving little available to carry out locally designed programs and projects. DAK is also limited to centrally defined activities, including the rehabilitation of facilities and selected operational expenses. Under these conditions, central government programs and projects are generally welcomed by local governments because they reduce the pressure to use their own funds for general purposes. This is particularly true of those lo-
3In Indonesia, the village is the lowest public administration unit.
4The availability and structure of the government for nonobligatory functions are determined by local governments. Some services are considered important by some governments but not by others, and some services are combined one way in one district and a different way in a neighboring district. For example, although the central government has a Ministry for Fishery, inland regions have no need for this service, or a municipality may consider forestry services unnecessary,
5In most cases, program or project content is vertically defined, whereas local governments have the discretion to decide exactly where implementation will take place.
6DAU has two major components: basic allocation and fiscal gap. The basic allocation mainly covers personnel and administration; the fiscal gap provides additional program funding for local needs and favors poorer regions with less local revenue-raising capacity.
cal governments with extremely limited locally derived revenues that constrain the availability and delivery of public services, including health services.
Consequences of Direct Elections
Regional diversity in the quality of public services and delivery is further exacerbated by another consequence of decentralization. Today, all heads of regions and officials down to the district and municipal levels are directly elected. Thus regents and mayors are responsible only to their constituents—or more likely to those close to them, including party members who were part of their successful election campaign teams—and so they are less answerable to their ”superiors” in government and able to exercise sanctions or withhold budget allocations.
As in other countries, the party winning a local election is often rewarded with government jobs for putting its candidate in office. As just described, a government position is a highly prized reward, especially in those regions where the private sector is weak and where salaried employment opportunities are few. Thus when new people are elected, the game “musical chairs” begins anew, resulting in frequent staff turnover.
Not surprising, local officials are often insufficiently informed of the conditions in their particular regions and the responsibilities of the positions they hold. Moreover, not just local governments but also local decision-making bodies are often uninformed of the commitments these bodies have to the needs of their citizens, including public social services, such as those related to maternal and neonatal health. Furthermore, the changing of the guard does not happen only once every five years when local heads are elected; rather, it happens far more frequently at the lower levels when those in power have to repay a favor. The result is that some local government officials are insufficiently informed about their jobs, having occupied their positions for only a short time.
So far, then, the promises of decentralization for improved access by the poor to better public services for mother and child health have not materialized. And the advantages attributed to proximity between local politicians and the needs of their constituents resulting in better needs assessments and services have not yet been borne out. Instead, a large proportion of those living in isolated rural areas, including the poor, often turn to private sector facilities for delivery, or they avoid facilities altogether (see Tables 6-1 and 6-2). Indeed, often there is no alternative because health service providers tend to concentrate in urban centers where there are better opportunities to receive monetary payments for services.
BOX 6-1 Decentralization and Argentina
Indonesia is not alone among countries dealing with decentralization and the MDGs at the same time. Argentina has faced a similar situation. A country with a history of authoritarian governments, it, like Indonesia, adopted a decentralized system of government upon the rise of a new democratic order. Political power moved to the provinces, some of which are in remote and hostile terrain. Despite high health expenditures nationwide during the first decade of the 21st century, one-third of the population had no access to health care, and the poor were excluded from health insurance. As a result, Argentina appeared unable to achieve the MDGs. In 2004 Argentina instituted a social insurance program, Plan Nacer, that provided women and children in the poorest provinces with basic health services (World Bank, 2009). It was based on an incentive mechanism between the Ministry of Health and the provinces, which were required to establish contracts containing quality of care provisions with local health care providers. The program was initially funded through a World Bank loan. In 2006 it was expanded to other provinces, and reached its program goals by 2009.
| Province | Health Facility | Home | Other | Not Specified | Total | No. of Births | |
| Public | Private | ||||||
| Aceh | 7.7 | 17.1 | 74.5 | — | 0.6 | 100.0 | 324 |
| North Sumatra | 5.1 | 29.9 | 64.4 | 0.4 | 0.2 | 100.0 | 1,197 |
| West Sumatra | 18.5 | 45.0 | 34.7 | 1.5 | 0.4 | 100.0 | 383 |
| Riau | 4.9 | 38.7 | 55.4 | 0.2 | 0.8 | 100.0 | 290 |
| Jambi | 5.6 | 20.5 | 72.9 | — | 0.1 | 100.0 | 186 |
| South Sumatra | 7.6 | 25.8 | 64.9 | 0.2 | 1.5 | 100.0 | 491 |
| Bengkulu | 6.3 | 5.8 | 87.9 | — | — | 100.0 | 111 |
| Lampung | 2.5 | 42.2 | 54.9 | — | 0.5 | 100.0 | 452 |
| Babel | 10.1 | 33.1 | 54.4 | 1.5 | 0.9 | 100.0 | 103 |
| Riau Islands | 11.0 | 65.3 | 23.1 | — | 0.6 | 100.0 | 93 |
| Jakarta | 14.8 | 73.7 | 11.2 | 0.2 | 0.2 | 100.0 | 741 |
| West Java | 6.0 | 38.6 | 54.5 | 0.1 | 0.8 | 100.0 | 2,600 |
| Central Java | 7.6 | 45.5 | 46.4 | 0.2 | 0.3 | 100.0 | 2,308 |
| Yogyakarta | 16.9 | 69.9 | 12.7 | 0.3 | 0.2 | 100.0 | 201 |
| East Java | 8.5 | 57.0 | 32.0 | 1.6 | 0.9 | 100.0 | 2,178 |
| Banten | 3.7 | 34.4 | 61.6 | 0.1 | 0.2 | 100.0 | 695 |
| Bali | 24.6 | 66.2 | 8.5 | — | 0.7 | 100.0 | 253 |
| West Nusa Tenggara | 25.9 | 6.3 | 58.4 | 8.9 | 0.6 | 100.0 | 412 |
| East Nusa Tenggara | 16.1 | 4.5 | 77.5 | 0.5 | 1.4 | 100.0 | 507 |
| West Kalimantan | 8.8 | 24.9 | 65.2 | 0.4 | 0.7 | 100.0 | 374 |
| Central Kalimantan | 5.2 | 8.9 | 84.9 | 0.4 | 0.6 | 100.0 | 160 |
| South Kalimantan | 8.8 | 10.5 | 79.8 | — | 0.8 | 100.0 | 289 |
| East Kalimantan | 21.2 | 24.6 | 53.5 | 0.4 | 0.2 | 100.0 | 262 |
| North Sulawesi | 26.6 | 28.4 | 43.0 | 0.5 | 1.5 | 100.0 | 191 |
| Central Sulawesi | 11.7 | 7.3 | 80.2 | 0.4 | 0.4 | 100.0 | 243 |
| South Sulawesi | 16.0 | 14.6 | 68.9 | — | 0.5 | 100.0 | 631 |
| Southeast Sulawesi | 6.3 | 2.0 | 90.5 | 0.6 | 0.5 | 100.0 | 192 |
| Gorontalo | 13.7 | 8.0 | 74.8 | 2.6 | 0.9 | 100.0 | 82 |
| West Sulawesi | 8.9 | 3.7 | 87.0 | — | 0.4 | 100.0 | 103 |
| Maluku | 8.4 | 4.0 | 87.1 | 0.2 | 0.2 | 100.0 | 143 |
| North Maluku | 10.7 | 7.3 | 80.5 | 0.4 | 1.0 | 100.0 | 93 |
| Papua | 18.9 | 7.4 | 70.8 | 1.2 | 1.7 | 100.0 | 152 |
| West Papua | 32.5 | 6.5 | 55.7 | 1.4 | 3.9 | 100.0 | 62 |
| Indonesia | 9.7 | 36.4 | 52.7 | 0.7 | 0.6 | 100.1 | 16,502 |
SOURCE: Badan Pusat Statistik and Macro International (2007: 289).
Although numerous programs and projects are aimed at improving the quality and accessibility of health services, including those for mothers and children, the perception that many of these services continue to be of poor quality remains. As shown in Table 6-3, this perception is reflected in the relatively low reliance on public health facilities, even among the poor. The causes of dissatisfaction are such things as administrative fees, slow or poor service delivery, ponderous bureaucratic procedures, and unskilled or,
even worse, unavailable service providers. It was in response to such challenges that the government introduced minimum service standards (MSS) in 2003. These standards were designed to serve as an instrument that would allow the central government to ensure that local governments were providing “affordable” basic standardized services to all who required them (Ismail Mohamad, n.d.).
In the health area, the standards have undergone an evolution. They initially encompassed some 54 output indicators for all available services (1458 Menkes/SK/X/2003). In 2008, however, a ministerial decree (741/Menkes/PER/ VII/2008 Tentang Standar Pelayanan Minimal Bidang Kesehatan di Kabupaten/Kota) reduced the number of covered services to 18, six of which refer directly to aspects of maternal and infant health (see Table 6-3). These services are presented in terms of target coverage rates (for 2010 or 2015) and include coverage of the following: visits by pregnant women to medical facilities, treatment of birth complications, birth attendance by trained personnel, postpartum services, and visits to medical facilities for infants from assisted births with neonatal complications.
| Type of service | 2010 | 2015 | ||
| a. | Basic health services | |||
| 1 | Coverage of four visits by pregnant women | 95 | ||
| 2 | Coverage of treatment of birth complications | 80 | ||
| 3 | Coverage of births attended by health staff with midwifery competence | 90 | ||
| 4 | Coverage of postpartum services | 90 | ||
| 5 | Coverage of assisted births with neonatal complications | 80 | ||
| 6 | Coverage of infant visits | 90 | ||
| 7 | Universal village coverage with child immunization | 100 | ||
| 8 | Coverage of under-5 services | 90 | ||
| 9 | Coverage of supplementary feeding for children 6 24 months of age in poor families | 100 | ||
| 10 | Coverage of care for children under age 5 suffering from malnutrition | 100 | ||
| 11 | Coverage of health of elementary school students | 100 | ||
| 12 | Coverage of active family planning participants | 100 | ||
| 13 | Coverage of finding and taking care of the sick | 70 | 100 | |
| 14 | Coverage of basic health services provision to the poor | 100 | ||
| b. | Referral health services | |||
| 1 | Coverage of poor patients’ health referral services | 100 | ||
| 2 | Coverage of first-level emergency assistance by district/municipality hospital facilities | 100 | ||
| c. | Epidemiological investigation and handling of extraordinary events | |||
| 1 | Coverage of epidemiological investigations in less than 24 hours in villages experiencing extraordinary events | 100 | ||
| d. | Health promotion and community empowerment | |||
| 1 | Covera e of active Alert Villa es | 80 | ||
SOURCE: Ministry of Health (2008b).
Although the notion of providing benchmarks and performance objectives is highly relevant to improving conditions, implementation of the MSS as they currently stand has been somewhat problematic. For example, the ministerial decree of 2008 includes detailed guidelines on data requirements, sources, and calculation of various indicators,7 but the system continues to rely on often incomplete records compiled by inadequately trained or motivated local personnel, and often it relies mainly on information provided by public health facilities (public hospitals or community health centers) that present only a partial picture of who is actually being served. In addition, base data on target populations are generally provided by sources—notably, the local offices of the national statistics agency (Badan Pusat Statistik, BPS)—that themselves lack reliable up-to-date information. This deficiency is particularly noticeable in local service areas where figures are usually estimates from surveys or projections. This problem, along with a general lack of attention at all levels to data quality control, frequently results in information with limited reliability or validity and thus of limited use for monitoring. Finally, and perhaps most critically, the existing standards also lack any locally meaningful monitoring measures such as those related to ease of access, availability of trained medical staff, and patient waiting times. Such measures would be designed to ensure the accountability of government entities in delivering quality health services that are relevant to the local people.
Conclusion
In Indonesia, regional inequities were further exacerbated by decentralization when the provision of public services became the responsibility of local governments in 2001. The resolution to achieve MDGs 4 and 5 was issued by the central government, but local governments have to shoulder the burden, and they are not prepared to do so. Some 70 80 percent of local government budgets are allocated to public sector wages and salaries, leaving little for locally designed social services. Just as before decentralization, many local governments continue to rely on the central government to provide social services. However, the central government can no longer place doctors in isolated areas on the basis of Law No. 8 (1961);8 today such placements are on a “voluntary” basis but are a requirement for doctors to earn their private practice license (SKTP). As recently as 2011, the central government placed on a voluntary basis 1,080 doctors for one year in remote and very isolated puskesmas (Pusat Komunikasi Publik, 2011). In a free market, doctors, nurses, and midwives tend to gravitate toward urban centers where earning opportunities in the private sector are greater.
At the local government level, local officials are often insufficiently informed about the conditions in their particular regions and about the responsibilities of the positions they hold. And local decision-making bodies are often uninformed about the commitments that they have to the needs of their citizens, including public social services, such as those related to maternal and neonatal health. Although the central government has introduced accountability measures to monitor service delivery, particularly through the introduction of minimum service standards, implementation has been inhibited by a lack of data and the inadequate human resource capacities of local governments. Outcome indicators produced under the MSS have little meaning to local government bureaucrats because no incentives are attached to any ”achievements,” and the indicators generally fail to deal with issues of service quality, which are at the core of customer dissatisfaction with public services.
7These include details on (1) definition, (2) operational definition, (3) formula calculation, (4) data source, (5) reference, (6) target, (7) activity steps, and (8) human resource requirements.
8Law No. 8 (1961), Wajib Kerja Sarjana, compelled university graduates to accept job placements in “isolated areas.” However, implementation of this law was considered discriminatory because it applied only to doctors and dentists, who therefore called for its elimination.
References
Badan Pusat Statistik (Statistics Indonesia). Various years. Statistical Yearbook of Indonesia. Jakarta: Badan Pusat Statistik.
Badan Pusat Statistik (Statistics Indonesia) and Macro International. 2007. 2007 Indonesian Demographic and Health Survey. Calverton, MD.
Bird, R. M. 1993. Threading the fiscal labyrinth: Some issues in fiscal decentralization. National Tax Journal 46(June):207 227.
Braun, Joachim von, and Ulrike Grote. 2000. Does Decentralization Serve the Poor? Paper presented at International Monetary Fund Conference on Fiscal Decentralization, Washington, DC, November 20 21.
Conyers, D. 1984. Decentralization and development: A review of the literature. Public Administration and Development 4(April June): 187 197.
Direktorat Jenderal Otonomi Daerah, Kementerian Dalam Negeri (Directorate General of Regional Autonomy, Ministry of Home Affairs). 2010. Potret 57 DOB, Sebuah Hasil Evaluasi Dini Perkembangan 57 Otonomi Daerah Baru (Profile of 57 New Autonomous Regions: An Evaluation of Current Developments of 57 New Autonomous Regions).
Hofman, Bert, and Kai Kaiser. 2002. The making of the Big Bang and its aftermath: A political economy perspective. Paper presented at conference Can Decentralization Help Rebuild Indonesia? A Conference Sponsored by the International Studies Program, Andrew Young School of Policy Studies, Georgia State University, Atlanta, May 1 3.
Katsiaouni, Olympios. 2003. Decentralization and poverty reduction: Does it work? Fifth Global Forum on Reinventing Government. Mexico City, November 3 7. Paper submitted to workshop on Linking Decentralized Governance and Human Development (UNDP, UNCDF, WBI, and UN-DESA). Interregional Adviser, UNDESA.
Ministry of Health. 2008a. MoH Decree No. 267/Menkes/SK/III/2008, Tentang Pedoman Teknis Pengorganisasian Dinas Kesehatan Daerah (Technical Guide on Organizing Regional Health Services). Jakarta.
______. 2008b. MoH Decree No. 741/Menkes/PER/ VII/2008, Tentang Standar Pelayanan Minimal Bidang Kesehatan Di Kabupaten/Kota. Jakarta.
Mohamad, Ismail. n.d. Service quality in public sector: An outcome-based approach. In Minimum Service Standard as Public Service Improvement Efforts: The Indonesian Experience. Draft.
Oates, Wallace E. 1999. An essay on fiscal federalism, Journal of Economic Literature 37(3):1120 1149.
Pusat Komunikasi Publik. 2011. Kemkes tempatkan 1,080 dokter PTT di daerah terpencil dan sangat terpencil (Ministry of Health places 1,080 temporary staff doctors in isolated and very isolated areas).
World Bank. 2009. En Breve. No. 150, December.










