Kathleen A. Cagney, Christopher R. Browning, Aubrey L. Jackson, and Brian Soller
The concept of community, both physical and social, has been central to social science inquiry on aging. Notions such as aging-in-place are predicated on the assumption that older adults would prefer to continue residing where they have established social ties and routines and where they have experienced seminal events over the life course. Research suggesting these preferences (Evans, Kantrowitz, and Eshelman, 2002; Rowles, Oswald, and Hunter, 2003), coupled with a burgeoning literature on neighborhood context effects across age groups (e.g., Sampson, Morenoff, and Gannon-Rowley, 2002), has led researchers on aging to examine the features of neighborhood context most salient for older adult well-being. In this chapter, we focus on the conceptualization and measurement of the social space that older adults inhabit, exploring implications for research on residential context. We approach this review broadly, incorporating research on social networks and institutional contexts that bear on the interpretation of “neighborhood effects.” Our initial aim is to illustrate that community can take many forms, and that networks, neighborhoods, and institutions, independent or interdependent, combine to shape the social environment in which older adults are embedded. Our subsequent aim is to argue that neighborhood effects research would benefit from alternative conceptualizations of the relevant spatial unit of analysis. We argue that residents, through their actions, define the activity space that they traverse and collectively constitute communities of routine interaction. This approach requires both new theory and new methods, which we elaborate on later in this chapter.
We begin by reviewing literature focused on the dyad or network in social interaction. We then shift to the neighborhood-level, describing select work that has been influential in the field and that brings insight to neighborhood-aging analyses. Next we review literature on the role of institutions and their import in understanding how networks and neighborhoods may be connected. This concludes our initial aim. We then turn to an overview of a multi-contextual theoretical perspective on the social context of aging anchored on the concept of “activity space” (that is, those places and spaces in which one engages in routine activities). We close with suggestions for future directions in context-related research in aging.
SOCIAL NETWORKS
Extant research suggests that the quality, extent, and type of social network ties are consequential for health. Reviews and theoretical expositions of this extensive literature can be found elsewhere (e.g., Berkman et al., 2000; Uchino, 2006) so we highlight the literature most relevant for older adults. Focusing first on the quality of social network ties, Thomas’s (2010) analysis of data from the Social Networks in Adult Life Survey indicates that receiving and providing social support are associated with better wellbeing among adults ages 50 and older, although these associations vary by the type of relationship to the alter (i.e., nominated network member) and the number of alters supported. Using longitudinal data from the Midlife in the U.S. Study, Seeman et al. (2010) find that frequency of social contact and social support are positively associated with cognitive function.
An expanding literature has emphasized patterns of change in network size as adults age and the implications of the extent or quantity of social ties for health and well-being. For instance, Cornwell, Laumann, and Schumm (2008), using data from the National Social Life, Health and Aging Project, find that older respondents report smaller networks and decreased closeness with network members. The volume of contact with network members also varies by age; contact volume tends to decrease with age until adults reach their mid-60s, at which point the association between age and contact flattens. Beginning in their mid-70s, however, the authors observe a positive association between contact volume and age. This U-shaped relationship may reflect changes in ties to social institutions—such as work—and an increased need for care late in life. Aartsen et al. (2004), based on a Dutch sample, find that as adults age, their networks increasingly consist of family members, although network size interacts with cognitive and physical decline to determine the network replacement of neighbors and friends with family members.
Finally, using longitudinal data from the Health Professionals Follow-up Study, Eng et al. (2002) find that over a 10-year period, older adult men
are at a greater risk of mortality across multiple causes of death if they have fewer social ties. They also find socially isolated men have an increased risk of fatal coronary heart disease. Differences in network size across the life course may have significant implications for health and well-being. Loneliness may be one manifestation of decreased social ties, and the concepts of loneliness and social isolation have received increasing attention in research on aging (e.g., Hawkley et al., 2008). A meta-analysis of research on adults’ loneliness suggests social contact, especially the quality of contact and contact with friends, is protective against loneliness (Pinquart and Sorensen, 2003). Cacioppo et al. (2006) find that loneliness is positively associated with subsequent depression net of initial depressive symptoms.
Recent research has also emphasized the type and structure of social networks within which older adults are embedded and their implications for health. Litwin and Shiovitz-Ezra (2006), for instance, find that the association between network type and mortality was important primarily to persons aged 70 and older; those in diverse, friend-focused, and, to a lesser extent, community-clan networks experienced lower risk of all-cause mortality. Cornwell (2009) examined patterns of network bridging among older adults (an individual acts as a “bridge” if he or she connects two otherwise disconnected individuals). Individuals who occupy bridge positions within their networks are hypothesized to benefit from improved access to diverse resources and better control over the exchange of information and resources between network members. Cornwell finds that older adults are more likely to serve as bridges if they exhibit good cognitive and functional health.
Research on networks and aging has also considered the potential downside of network embeddedness. Cornwell and Laumann (2011) find that the frequency of contact between a man’s female partner and his network members (i.e., partner betweenness) contributes to male sexual dysfunction, arguing that overlapping networks between heterosexual partners undermines a man’s independent control of social resources—contrary to traditional notions of masculinity. These findings are consistent with research emphasizing the potential for detrimental effects of social connections (Baum, 1999; Browning, Feinberg, and Dietz 2004; Lynch et al., 2000) and relates to a developing literature that emphasizes contingencies in the impact of social ties depending on features of the relationships and networks in which older adults are embedded.
NEIGHBORHOOD CONTEXT
Research in psychology suggests that attachments to place grow stronger with age (Zingmark, Norberg, and Sandman, 1995). The immediate neighborhood environment is typically understood to play an increasingly
important role in shaping daily life as retirement and mobility limitations diminish the radius of routine activity, although the claim that neighborhood exposures grow more relevant with age has not been directly tested (Cagney and York Cornwell, 2010). Older adults also experience comparatively lower rates of residential mobility. In 2000, only 4 percent of adults aged 65 and older changed residences in the past year compared to 15.6 percent of the younger population. As older adults age in place, the opportunities and constraints presented by their neighborhood environments become increasingly relevant to health and well-being (He et al., 2005). The findings below are consistent with the claim that neighborhoods are consequential for older adult health, with patterns of influence varying by individual-level factors such as stage in the life course, gender, and race. Drawing on key theoretical approaches that have been used to frame research on neighborhoods, we review health-related implications of neighborhood social structural and social process environments for older adults.
Research on the neighborhood context of health across the life course has drawn heavily from social disorganization theory—a long-standing theoretical approach with roots in the Chicago School of Sociology. Social disorganization theory proposes that neighborhood structural characteristics—concentrated economic disadvantage, racial/ethnic heterogeneity, and residential instability—influence the shared capacity of residents to achieve common goals and maintain effective social control (Sampson, 2003; Shaw and McKay, 1969). Poverty limits the availability of resources (including time and material) that can be deployed toward local ends; residential instability hampers the development of neighborhood social networks and weakens incentives to participate in voluntary organizations serving the community; and racial/ethnic heterogeneity may inhibit the development of ties across communities divided by language and customs—although typically not shared values regarding community functioning (e.g., norms regarding a crime-free environment). Although originally used to explain the differential distribution of crime and delinquency rates across urban areas, social disorganization theory has been enlisted to better understand the clustering of poor health outcomes, with increasing attention to older adult morbidity and mortality (Cagney, Browning, and Wen, 2005; Wen and Christakis, 2005).
Of the three structural factors emphasized in the social disorganization approach, research on the effects of concentrated economic disadvantage is most common in studies of health and older adult well-being (e.g., Freedman, Grafova, and Rogowski, 2011). Poverty and other indicators of socioeconomic disadvantage are associated with greater risks of mortality (Diez Roux et al., 2004) and morbidity (Merkin et al., 2007), as well as declines in mental health (Aneshensel et al., 2007), mobility (Lang et al., 2008), and self-rated health (Cagney, Browning, and Wen, 2005). Although
this research consistently finds detrimental effects of neighborhood structural disadvantage, Cagney et al. (2005) find that the prevalence of affluent residents exhibits more robust associations with self-rated health than does disadvantage. Regardless of the operationalization, a growing body of evidence suggests that neighborhood socioeconomic status (SES) matters for the health of older adults, with some research finding evidence that neighborhood SES explains older adult health disparities between race groups (Cagney, Browning, and Wen, 2005; Yao and Robert, 2008).
Increased attention to neighborhood context has led researchers to consider the conditions under which neighborhood structural factors exert more pronounced influence. For instance, research suggests that individual-level SES (Wen and Christakis, 2005) and race (Diez Roux, 2004) may moderate the relationship between neighborhood SES and older adult health outcomes. Yao and Robert (2008) find that neighborhood disadvantage explains baseline differences in self-rated health but not changes over time. Robert and Li (2001), however, find that neighborhood SES has the strongest effect on adult health at middle ages, its effect diminishing during early and late adulthood. Some research also suggests that neighborhood SES has little or no effect at older ages (Waitzman and Smith, 1998), perhaps due to selective mortality or study outcomes—such as mortality—that often are rare at younger ages (Glass and Balfour, 2003). Finally, LeClere, Rogers, and Peters (1997) find the changing influence of neighborhood SES across ages may vary by race.
Findings on the effects of racial/ethnic composition of neighborhoods have been equivocal. The Latino Paradox suggests that despite typically socioeconomically disadvantaged communities, Latinos tend to benefit from residence in highly immigrant or Latino-concentrated neighborhoods. Research suggests that such high concentrations may be protective against stroke, cancer, hip fracture, and mortality (Eschbach et al., 2004), as well as depressive symptoms (Ostir et al., 2003). Yet research also finds that the proportions of blacks and Hispanics in a neighborhood are positively associated with depressive symptoms (Aneshensel et al., 2007). Alternatively, some studies suggest that black concentration has no effect on depressive symptoms (Subramanian et al., 2006) or on self-rated health (Hybels et al., 2006; Kubzansky et al., 2005).
Residential instability generally has been shown to be detrimental to health, including outcomes such as self-rated health (Subramanian et al., 2006) and disability (Beard et al., 2009). Research also suggests that residential instability may influence perceived social environmental stress (Schulz et al., 2008). In contrast, Hybels et al. (2006) find no association between residential instability and depressive symptoms.
A fourth structural factor also has been considered in research motivated by the social disorganization framework—age (Cagney, 2006). Studies
show that older adults benefit from high concentrations of older adults in their neighborhoods. Elevated concentrations are associated with better self-rated health (Subramanian et al., 2006), mental health (Kubzansky et al., 2005), and are protective against older adult mortality during disasters (Browning et al., 2006). But as with residential instability, Hybels et al. (2006) find no effect of neighborhood age structure on depressive symptoms. A related finding suggests that for older widowed adults, aspects of neighborhood composition such as the proportion of widowers shape opportunities for interaction, social connectedness, and, ultimately, mortality (Subramanian, Elwert, and Christakis, 2008).
Finally, a related structural construct focuses on characteristics of the built environment, including physical features of the environment as well as the quality of local amenities. We include discussion of the built environment within the larger body of research on structural features because the type and quality of infrastructure can either facilitate or inhibit social interaction. Research suggests that heavy traffic, excessive noise, inadequate lighting, and poor sidewalks may discourage physical activity among older adults (Balfour and Kaplan, 2002; Gallagher et al., 2010; Giles-Corti and Donovan, 2002; Mendes de Leon et al., 2009; Strath, Isaacs, and Greenwald, 2007). Older adults may be particularly responsive to specific aspects of the built environment (e.g., walkable sidewalks, curb cuts) since physical limitations are more prevalent; mobility declines or inability to drive may mean that neighborhood conditions favorable to walking become more salient for older adults’ healthful living (Clarke, Ailshire, and Lantz, 2009). The press-competence model suggests that individual competencies interact with environmental conditions to influence health outcomes (Glass and Balfour, 2003).
Relatively few studies of neighborhood influences on aging-related outcomes have directly measured the social processes thought to mediate the influence of neighborhood structural characteristics on older adult health. An emerging literature, however, draws on recent data collection efforts that attempt to assess the social climate of (largely urban) neighborhoods in which older adults reside. Findings from this incipient literature suggest that features of the social environment such as characteristics of neighbor networks and “collective efficacy”—the level of mutual trust and willingness to intervene on behalf of shared local goals—may independently contribute to older adult well-being. Wen and Christakis (2005), for instance, find that a higher quality social environment—as measured by levels of collective efficacy, social support, participation in voluntary associations, and (lower levels of) perceived violence—prolongs survival following disease onset. Browning et al. (2006) find that collective efficacy protects against mortality among older adults, although this effect fails to persist under extreme conditions (i.e., during a heat wave). In contrast, however, Mendes de Leon
et al. (2009) find neighborhood-level social cohesion is not associated with walking after accounting for individual-level perceptions of social cohesion.
Some investigators have examined the extent to which social process measures and perceptions of them vary by key demographic indictors such as age. For instance, Galinsky, Cagney, and Browning (2012) compare two measures of collective efficacy, one originally developed through the Project on Human Development in Chicago Neighborhoods (PHDCN) and the other through the Neighborhood Organization, Aging and Health Study (NOAH). The measure developed for NOAH substituted some of the original collective efficacy items of the PHDCN related to informal monitoring of children with those believed to be more relevant for older adults (e.g., neighbors shovel snow, neighbors check on older adults during a heat wave, neighbors intervene to protect a threatened older adult). Both the original and older adult versions performed well, but item non-response was much improved with the measure tailored for older adults (suggesting that respondents were more interested in, or better able to answer, questions when the substance resonated with their experiences).
Research on the neighborhood context of older adult health remains incipient, but suggests the importance of neighborhood environments in shaping health outcomes. Neighborhoods may create opportunities for positive social network influences to take hold, as described earlier, and may foster the presence of institutions that promote older adult well-being. We now turn to a description of these institutions, highlighting the type and form that bear on the lives of older adults.
INSTITUTIONS
Institutional settings, both formal and informal, can be critical to older adult social integration and may have downstream effects for health. Sociological research like Slim’s Table (Duneier, 1994) illustrates the import of local gathering places, such as restaurants, for the maintenance of social connections. And Hochschild’s classic The Unexpected Community: Portrait of an Old Age Subculture (1973) intimates that community can be created through any number of institutional forms.
In this chapter, we consider institutions to be physical locations where some form of organized social activity takes place. Our focus is on institutional settings that promote social integration and social and physical contact. When initially considering institutional settings that may be important to aging, care arrangements such as formal long-term care facilities, home care services, and hospitals and other health services may come to mind. While we acknowledge that these institutional arrangements are critical for the well-being of older adults, their reason for being stems from health and long-term care service delivery. We choose instead to focus on the types of
institutions that might not readily be identified with older adults or care provision, but that serve to link older adults to one another, and to the community, and indirectly influence health and well-being.
The density and quality of the institutional environment may have important implications for older adult health and may also mediate the influence of residence in a disadvantaged neighborhood context on aging-related outcomes. We consider institutional involvement and access across a continuum from more formal organizations, to availability and quality of local businesses, to informal and unstructured but patterned interaction. For instance, older adults’ involvement in religious organizations has been the subject of extensive inquiry (e.g., Dupre, Franzese, and Parrado, 2006; Norton et al., 2008). However, a wide variety of institutions may be relevant to shaping the quality of daily life for older adults and providing access to ongoing sources of support (e.g., community-based senior centers) (Miner, Logan, and Spitze, 1993). Participation in voluntary organizations and even regular but informal gatherings in local restaurants, clubs, or recreational facilities may contribute to a richer social experience.
Increasing evidence suggests that organizational and institutional involvements have beneficial effects for older adults. York Cornwell and Waite (2009) find that social connectedness based on personal and group-oriented ties is positively associated with self-rated health and mental health. Shankar et al. (2011), with cross-sectional data from the second wave of the English Longitudinal Study of Ageing, find that increases in loneliness as well as increases in a combined measure of social isolation from family, friends, organizations, religious groups, and committees are associated with greater likelihood of inactivity, a heightened risk of smoking, and higher systolic and diastolic blood pressure. And, Eng et al. (2002) find religious service attendance and participation in social groups each is associated with a decreased risk of all-cause mortality.
Caveats in this body of research include cohort differences that are not examined and results related to age that are equivocal. Some research (e.g., Putnam’s Bowling Alone [2000]) suggests that successive cohorts will neither have the taste for organizational involvement nor the range of formal organizations to join. On age, Bukov, Maas, and Lampert (2002) examined social participation among adults aged 70 and older. They find that social participation is more likely among those with greater educational and occupational resources and that declines in participation are explained, in part, by aging and declines in health. In contrast, Cornwell et al. (2008) find that age is positively associated with religious service attendance and volunteering. Collecting more precise data from older adults on their specific institutional involvements could potentially contribute to an understanding of disparate findings related to age.
Evidence pointing to the role of institutional and organizational participation in older adult well-being highlights the need for a better understanding of the processes that shape access and opportunity. Critically, geographic isolation may limit access to beneficial health-related facilities, food outlets, recreational activities, and other amenities. Such isolation is pronounced in rural areas (Durazo et al., 2011), although differences within urban and suburban areas also exist. Pearce, Witten, and Bartie (2006) found substantial variation in proximity to health-related institutions—including shopping, education, and recreation—between rural and urban areas and within urban areas of New Zealand. In the United States, low SES neighborhoods are less likely to have recreational facilities (Moore et al., 2008) and free-for-use physical activity resources (Estabrooks, Lee, and Gyurcsik, 2003) than are higher SES neighborhoods. Research also suggests that residents in predominantly white neighborhoods are more likely to have better access to healthful food outlets, such as supermarkets, than those residing in predominantly black neighborhoods (Morland et al., 2002; Zenk et al., 2005). Finally, Yamashita and Kunkel (2011) assessed older adults’ access to healthful food outlets in Hamilton County, Ohio. They find older adults are concentrated in areas with lower densities of healthful food outlets and conclude that the majority of older adults in the county do not live within walking distance of such an outlet.
Institutional and organizational involvement appear consequential for older adult health, but differentially accessible by geographic location. Although individuals’ predispositions to avail themselves of local institutional opportunities clearly differ, teasing out the interrelationships between opportunity, inclination, and participation is difficult. The role of institutions, and the social network connections they provide, may be better understood with better data. For instance, more precise information could capture not only the institutions frequented but also their physical location, as well as the extent to which other social network members spend time there.
CHALLENGES
Despite the substantial promise of research on the social context of aging, this area of inquiry has faced a number of challenges. Although the criticisms directed at contextual research are not unique within the social sciences, addressing these issues has proved particularly vexing given the nature of the questions and the data typically involved. We focus on three major challenges to the literature: (1) the tendency for contextual research to be “silo’d” with respect to both theoretical formulation and empirical execution; (2) difficulties in establishing the causal impact of context on health; and (3) the substantial data and measurement shortfalls of existing resources. These challenges may apply to contextual research more
generally, but specific aspects are particularly consequential for research on aging and will be discussed in detail accordingly.
Silos in Contextual Research and Implications for Theoretical Integration
As suggested in our review of the extant literature on the social context of aging, the role of network, residential neighborhood, and institutional contexts in shaping aging-related processes cannot be easily disentangled. For example, theories of neighborhood effects on health often invoke the influence of local institutions and access to neighbor networks as key mechanisms (Sampson, Morenoff, and Gannon-Rowley, 2002). Institutional influences are difficult to understand in the absence of information on the local embeddedness of these organizations and their capacity to extend influence beyond the most formal aspects of organizational involvement through informal network processes. In addition, face-to-face social network interactions always occur in a geographic and more or less structured social setting. Understanding the emergence and quality of social networks as sources of support for older adults may require richer information on the settings that shape and sustain social networks.
These points highlight the inherent limitations of “uni-contextual” theoretical approaches to understanding social influences on health. Indeed, as Cook (2003) argues, the restricted scope of contextual studies leads to a number of potential concerns about the nature of extant findings. First, focusing on an arbitrarily limited set of contexts precludes assessment of the combined effects of multiple relevant contexts on aging-related outcomes. A joint contextual effect may be substantially greater than the effect of any given context in isolation. As noted, studies that simultaneously incorporate information on networks, neighborhoods, and institutions are exceedingly rare. Second, accounting for only a subset of older adult exposures may lead to biased contextual effects (i.e., if effects of measured contexts on individual outcomes are confounded with omitted characteristics of unmeasured contexts). Third, simultaneous assessment of multiple contexts allows insight into inter-context mediational processes that more limited-scope approaches cannot detect. Fourth, research designs that incorporate a limited number of contexts restrict the capacity to assess the influence of inter-context interactions on older adult outcomes (e.g., the negative impact of a disadvantaged neighborhood may be buffered by participation in highly supportive institutions such as churches or community centers). These concerns point to the need for theoretical approaches and data collection efforts that explicitly consider the multiple contexts relevant to older adults
Although our review highlighted emerging areas of research that attempt to combine contextual influences, these efforts remain the exception. In some instances, this may be due to a tendency to underemphasize
theoretical motivation. For instance, although some neighborhood research has drawn on theory to combine an emphasis on the effects of social structural characteristics on older adult health with attention to the mechanisms—such as social cohesion—that may explain structural effects, this literature remains incipient. Indeed, some have argued that neighborhood research on older adult populations has tended to neglect theory (Macintyre and Ellaway, 2003). In their comprehensive review of articles published between 1997 and 2007, Yen, Michael, and Perdue (2009) identified 33 articles on neighborhoods and older adult health. Only three of these publications explicitly mention a theoretical model.
Incorporating theory in contextual research more generally will help better elucidate the processes that link contexts with health for older adults and draw attention to the inherently interconnected nature of social contexts as they shape older adult outcomes. Substantial advances in this area, however, will require more complex theoretical models that explicitly acknowledge the multifaceted nature of social contextual influence. Extant theoretical models point toward this insight, but few efforts to understand the simultaneous and interactive effects of social network, geographic, and institutional influences have been attempted.
Causality and Selection
A second challenge relates to the seemingly intractable problem of establishing causality in studies of social context effects on health. Such studies face the inevitable criticism that individuals who select into disadvantaged contexts may be at high risk for poor health outcomes at the onset. One could argue that selection is an even more intractable problem for research on older adults because it could be compounded by time and residential history in ways we cannot address with available data (e.g., Li and Ferraro, 2005). In the neighborhood literature, for instance, substantial attention has been devoted to determining whether observed effects of neighborhood variables are compositional or contextual in nature. Compositional effects are attributable not to the context itself, but to the aggregation of similar individuals who consequently have comparable health outcomes. If only compositional effects exist, then relocation to a new context would not produce different health outcomes as individual-level traits persist. Compositional effects may be observed because individual traits that influence health also help determine where people live either through selective migration or through constraints on mobility. Furthermore, selection or constraint criteria may change over the life course. Compared to younger adults, older adults benefit less from services such as public schooling, and they likely have less flexible budgets if retired. It is therefore not surprising that low property taxes, for example, help determine whether
and to where older adults move (Duncombe, Robbins, and Wolf, 2001; Sabia, 2008). Neighborhood residence also may be determined by an individual’s health. Relocation or the expectation of moving is associated with changes in physical limitations, self-rated health, cognitive impairment, and proximity to a child (Sabia, 2008; Silverstein and Angelelli, 1998).
Unlike compositional effects, contextual effects are not attributable to aggregated features of individuals; hence, similar people may experience different health outcomes depending on their contextual exposures (Curtis and Jones, 1998; Macintyre and Ellaway, 2003). Multilevel modeling techniques enable researchers to better distinguish compositional from contextual effects. These analytic strategies allow context- and individual-level effects to be modeled simultaneously, thereby allowing researchers to distinguish variance in individual outcomes attributable to neighborhood versus individual characteristics (Diez Roux, 2004).
Yet, multilevel models are no panacea in the absence of adequate control for the individual-level factors associated with selection into neighborhoods. Unfortunately, the perennial challenge of estimating unbiased contextual effects is extremely difficult to overcome with standard research designs. Studies such as the Moving to Opportunity (MTO) Demonstration have attempted to approximate an experimental design in an effort to understand the “treatment” effect of moving from a high- to a low-poverty neighborhood among younger populations. The capacity of these approaches to isolate the treatment effect of interest has been questioned (Sampson, 2008). A major concern in the case of the MTO study surrounds the extent to which the residential move from a high- to a low-poverty neighborhood actually resulted in sustained differences in the routine exposures of study participants (Clampett-Lundquist and Massey, 2008). As we describe below, targeted data collection efforts motivated by multicontextual theoretical approaches offer some promise for improved estimation of contextual effects.
Data and Measures
Theory cannot be adequately tested, nor can efforts to address problems of selection and causation, in the absence of high-quality data collection efforts. An obvious advance would be to incorporate social contextual measures into ongoing, longitudinal investigations of older adult well-being. Despite the advantages of over-time data, Yen, Michael, and Perdue (2009) identified only eight longitudinal studies of neighborhoods and older adult health. Typically, longitudinal investigations of aging populations focus on individual-level characteristics. Thus, changes in neighborhood characteristics are unobserved and their potential influence impossible to assess.
Effective measurement of social context is a significant challenge. Boundary specification problems are endemic to this research, often resulting in arbitrary or convenience-based decisions regarding the operationalization of the context of interest. For instance, neighborhood research faces the ongoing challenge of defining the “neighborhood.” Neighborhoods have been defined by individual perceptions, administrative boundaries, and sociogeographic landscape. Although theory and the specific research question should inform the size of the relevant boundary (Raudenbush, 2003), available data usually restrict researchers to using predefined boundaries, such as the census tract, and consider only residential location.
Research also is limited by the relative lack of data on whole (as opposed to ego-centered) networks. Many studies rely on ego-centric networks that bound networks based on first-degree connections. Such studies often use measures of perceived levels of support or weight network ties based on the level of intimacy. But as Granovetter’s (1973) work suggests, weak ties may have important consequences as well. Smith and Christakis (2008) argue that health research should consider characteristics of the whole network. For example, Christakis and Fowler (2007) identified obesity clusters using over-time whole network data. They find that direct connections to obese alters (i.e., friends), as well as connections to individuals separated by up to three degrees, influence the ego’s likelihood of becoming obese. Although this research has been criticized on methodological grounds (Lyons, 2011), findings from these studies have sparked substantial interest in the health effects of embeddedness in network structures and raise important questions regarding the appropriate measurement of networks to capture health influence.
Finally, research has not fully explored the intersection of geographic location and global (or complete) networks, and their effects on health. As we discuss later in this chapter, individual-level reports of sociospatial ties can be combined to identify aggregate patterns of interaction. The interrelationship between social ties and social interaction, and the exact location in which ties are maintained, could potentially inform neighborhood-based interventions for older adults. If it is known, for instance, that certain neighborhood institutions create consistent opportunities for interaction, and that ties formed there are of some consequence, then efforts can focus on protecting or sustaining those institutions. The frame to describe institutions may also be extended; perhaps they need not exist in a formal sense or even under a roof. For instance, Chicago’s Hyde Park neighborhood is able to sustain more than one location (generally, a park) where older adults gather on a regular basis to play chess. The ability to efficiently identify this form of activity may be possible with newly designed social survey and tracking methods—we turn to a description of these below.
NEW DIRECTIONS
Despite the substantial challenges facing investigation of social context effects on aging, emerging directions in conceptualization and measurement hold the promise to significantly advance research in this area. Specifically, we focus on the concept of activity space as an integrative approach to capturing older adult spatial, social, and institutional exposures. Activity spaces may be understood to encompass all of the locations that individuals come into contact with as a result of their routine activities (Golledge and Stimson, 1997). Below we describe how incorporating activity space exposures into theoretical models and data collection efforts may aid in addressing the challenges facing contextual research on aging.
Reorienting Theory
First, theoretical approaches that emphasize the effects of one or another set of contexts on aging-related outcomes would benefit from conceptualizing individual exposures through the concept of activity space. For instance, research on neighborhoods, aging, and health largely has focused on the residential location. But individuals travel outside of their residential neighborhoods as they carry out routine activities, such as work, grocery shopping, health and dental care, and recreation. It is plausible that these nonhome contexts also influence individual outcomes (Kwan, 2009). Moreover, the degree of exposure to these contexts varies. Thus, research should consider characteristics of residential and nonresidential environments as well as the time spent, activities performed, and social interactions occurring at these locations. This approach is explicitly multicontextual, acknowledging the potential for substantial inter-individual variability in daily routines.
Consideration of activity space may help explain differential effects of neighborhood characteristics across individuals. For example, the protective effects of high immigrant concentration within the residential neighborhood may be attenuated if individuals spend considerable time outside their neighborhoods. Conversely, the harmful effects of concentrated disadvantage might be alleviated when individuals are routinely exposed to more affluent or pro-social contexts. Although advanced age and disability may limit the potential to travel beyond the residential neighborhood, as noted earlier, the assumption of age-constricted routine activity spaces has not been investigated empirically (Cagney and York Cornwell, 2010). Although it is likely true that, on average, the circumference of turf declines in size with age, inter-individual variability in this process may be substantial (and life course theory suggests that we might expect even greater heterogeneity at later ages [Elder, 1975]). Research thus should consider how
individuals’ activity spaces change as they age, and whether these changes shape the influence of traditionally emphasized contexts such as residential neighborhoods.
Attention to Institutional Interactions
As with neighborhood contexts, consideration of activity spaces could help improve understanding of older adults’ interactions with various institutions. By collecting data that directly assess older adults’ exposures to institutional contexts, the impact of such exposures can be more precisely estimated. Activity space data also may provide information on the specific venue where an individual spends time, offering the opportunity to capitalize on rapidly expanding publicly available data on institutions and public space (e.g., Google Maps, Street View, etc.). An emphasis on activity space data marks an important shift from the dominant survey-based approach to understanding institutional participation that relies on abstract categories of institutional participation (e.g., church attendance or membership in clubs and voluntary organizations, broadly construed) without observing actual social and spatial exposures. These methods do not replace survey-based approaches, which are still critical to gleaning perceptions, but suggest that surveys can be combined with Global Positioning System (GPS) technology and other space-time tracking systems to situate older adults in their social and geographic space.
Moreover, activity space information allows for assessment of the geographic proximity of institutions with which individuals are actually involved. Do residential neighborhoods provide institutional exposures or do older adults travel outside their immediate neighborhood contexts for some institutional involvements? The typical approach to estimating the impact of neighborhood institutional environments is to simply enumerate the presence of relevant organizations, businesses, and local facilities in a neighborhood and estimate the impact of institutional density on aging-related outcomes. Although this approach may tap potential opportunities or the community’s orientation toward pro-social organizations, it does not assess actual participation in local institutions by older adult residents and therefore cannot accurately measure the impact of institutional participation.
Activity space measures also allow researchers to disentangle the primary and secondary benefits of institutional presence. For instance, institutions may exert beneficial influence on participants directly, but also may indirectly influence the outcomes of other neighborhood residents through second- and third-order network ties (e.g., information passed through informal gatherings at a local coffee shop is passed on through neighbor networks), social psychological influences (e.g., a successful local youth organization engenders trust and a sense of security among older adults),
or ecological processes (e.g., a new store brings conventional activity and “eyes on the street” to the surrounding area, promoting monitoring and informal social control [Browning et al., 2011; Jacobs, 1961]). By incorporating direct exposure to geographically identified institutions into theoretical models of social context effects, researchers will be encouraged to think about the complex influences of institutions through participation, social networks, and proximate spatial processes.
Multicontextual Analysis Opportunities
In addition, a multicontextual approach to social network influences on aging would allow for detailed assessment of network partner characteristics while simultaneously capturing the embeddedness of network interactions in geographic, institutional, and social settings. The characteristics of settings in which network partnerships are enacted (e.g., local, public, accessible) may have important implications for the extent to which network interactions translate into actual and perceived social support (Small, 2009). Moreover, the availability of public or casual social ties—e.g., those ties that are routinely available through local public venues, such as restaurants, coffee shops, and parks—may provide a source of security and informal network-based monitoring that more intimate but less regularized family ties may not offer. The pioneering work of Jane Jacobs (1961) highlighted the critical role of overlapping routines and casual contact among neighborhood residents in developing public trust. In the absence of activity space information, the potential for such contact characterizing a given residential area is difficult to observe. To our knowledge, research on the social context of aging has not sought to integrate network information with data collected in real time on activity space and routine activities.
Framing theoretical approaches and analyses using the activity space concept may also help develop research designs that are better equipped to infer causal effects of social contexts. Clearly, the challenge of establishing causal effects of social contextual variables is one that social scientists will not easily overcome. However, activity space data provide a means of improving on standard approaches. Precise exposure data offer the opportunity to determine whether a specific “treatment” has occurred and the duration of exposure, where relevant. For instance, hypotheses regarding the role of institutions in the lives of older adults might capitalize on exogenous changes in the institutional environment to determine whether and how such changes influence older adult well-being. The impact of opening a recreation center with older adult programming on the activity patterns of local elderly is an obvious example, but other institutional changes could matter as well. For instance, a new elementary school in the neighborhood could renew life on the street and encourage older adults to leave their
homes more often. Research questions examining the impact of time spent with social network partners in fostering older adult well-being (along a variety of dimensions) could benefit from more accurate assessment of network dynamics through space-time data on social network interactions. Although the challenges associated with inferring causation from analyses of social context effects are exceedingly difficult to surmount, activity space data will offer an opportunity to, at a minimum, assess theoretically relevant characteristics of a contextual treatment with greater accuracy.
Promising Technological Advances
Finally, the data collection and measurement requirements of precise activity space information clearly extend beyond the traditional survey interview but are becoming increasingly feasible with new technologies. GPS technology is now a standard feature of cellular telephones, and most smartphone operation systems can accommodate applications to collect relatively precise location data. Smartphones also are increasingly used to collect real-time information from respondents on settings, social interactions, mood, and other phenomena using Ecological Momentary Assessment (EMA) (Cain et al., 2009). EMA uses smartphones to directly contact respondents with questions that can be answered, in the moment, using the device, limiting problems associated with recall of events and locations (potentially more effective if short-term memory is compromised). Question content can be crafted such that respondents are queried not only about what they are doing, whom they are with, and how they feel in the moment—three typical foci of EMA-based data collection efforts (Shiffman et al., 2008)—but also about the nature of the social exchange and the quality of it (Stafford et al., 2011). Moreover, the content of exchanges, personal or material, is rarely collected in traditional survey-based approaches because detailed recall of activity and context would be too onerous. Although older adult populations are less familiar with smartphone technology, a number of studies have successfully used these devices to collect EMA data (Cain et al., 2009). Moreover, the rapid spread of mobile phone technology ensures that each new cohort of older adults will experience fewer burdens associated with smartphone-based data collection. Apart from technological familiarity, EMA and GPS tracking may be less invasive (particularly the passive tracking of respondent movements) so may be well suited for older adults who lack the comfort or stamina to interact with interviewers and recount interactions and locations.
Sampling activity spaces in a geographically contained population also may allow investigators to measure the extent to which neighborhood residents share activity locations within a given boundary or more generally. Consistent with Jacobs’ (1961) approach, patterns of residential
interconnection through shared activity locations may capture important features of the social organization of a neighborhood. For instance, the pattern of these actor-location ties or “co-location networks” may have consequences for neighborhood processes such as social network formation and sustainability, the emergence of trust and neighborhood attachments, and shared expectations for informal social control and action on behalf of the local community (Browning et al., 2011). These factors have been linked with older adult health and well-being in the extant literature (e.g., Cagney, Browning, and Wen, 2005), but the social and ecological dynamics that tend to promote these features of neighborhood social organization have remained elusive. Moreover, by measuring the co-location network more precisely, researchers may be able to leverage social network analysis techniques to characterize routine activity patterns using sophisticated global network measures and identify an individual’s location in the network (e.g., through various measures of centrality) (Browning et al., 2011). We include a stylized example of just such potential. The network diagram (see Figure 8-1) illustrates how individuals (the circles) interact with places (the squares) in a hypothetical community. The sizes of the circles and squares suggest the network centrality of the person or the place. We could imagine that the larger squares could be churches, parks, or shopping centers—places that are central to routine activity. Graphically representing where people go, and how they may co-locate, could indicate both places that are successful at bringing together disparate groups and potentially identify shared tastes and norms. Rich measures of activity space may help uncover the social structure of community embeddedness that older adults experience.
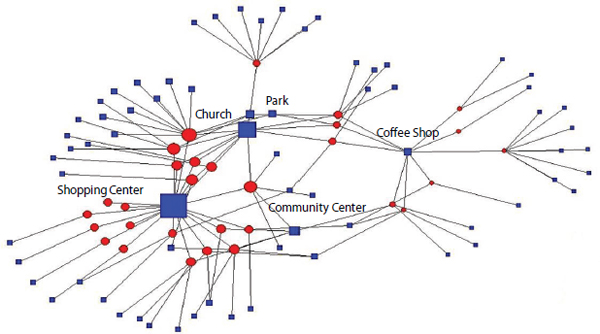
FIGURE 8-1 Affiliation network of older adults and neighborhood places.
These advances represent the frontier, but they also come with unforeseen challenges. The sheer volume of data points that will be available from data collection processes such as GPS tracking is one example of the emerging challenges of “big data” (Nyerges, Couclelis, and McMaster, 2011). Investigators could benefit from establishing “best practices” for how to manage, store, and clean these data so they are useful for analytic purposes. Another area that deserves attention is that of human subjects, how to protect their data and how to ensure their confidence in researchers’ ability to do so. Older adult participation in activity space research will be contingent on the field’s grasp of these sensitive issues.
CONCLUSIONS
We have spent a significant portion of this chapter building a case for activity space approaches in contextual research on aging. These approaches hold promise because they release us from predetermined boundaries of influence and allow respondents to reveal where they go and how they share their social spaces. We believe this is the next “turning point” in neighborhood effects research and that aging-related scholarship will particularly benefit. We think this is so because relatively little is known about older adults’ routine activities and the extent to which they are altered with life course transitions and changes in health.
Research on the social context of aging faces a variety of challenges and opportunities in the coming years. Significant advances have characterized research on specific social contexts, demonstrating the role of social networks, neighborhoods, and institutions in shaping trajectories of older adult health and well-being. Nevertheless, capitalizing on these advances will require increasingly integrated, multicontextual theoretical and methodological approaches and concomitant data resources. We suggest that studies incorporating the concept and measurement of older adult activity space hold substantial promise for advancing contextual research on older adults and will benefit from ongoing rapid innovation in technologies for the collection of real-time data on spatial and social exposures.
REFERENCES
Aartsen, M.J., van Tilburg, T., Smits, C.H.M., and Knipscheer, K.C.P.M. (2004). A longitudinal study of the impact of physical and cognitive decline on the personal network in old age. Journal of Social and Personal Relationships, 21(2), 249-266.
Aneshensel, C.S., Wight, R.G., Miller-Martinez, D., Botticello, A.L., Karlamangla, A.S., and Seeman, T.E. (2007). Urban neighborhoods and depressive symptoms among older adults. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 62(1), S52-S59.
Balfour, J.L., and Kaplan, G.J. (2002). Neighborhood environment and loss of physical function in older adults: Evidence from the Alameda County Study. American Journal of Epidemiology, 155(6), 507-515.
Baum, F. (1999). Social capital: Is it good for your health? Issues for a public health agenda. Journal of Epidemiology and Community Health, 53(4), 195-196.
Beard, J.R., Blaney, S., Cerda, M., Frye, V., Lovasi, G.S., Ompad, D., and Vlahov, D. (2009). Neighborhood characteristics and disability in older adults. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 64(2), 252-257.
Berkman, L.F., Glass, T., Brissette, I., and Seeman, T.E. (2000). From social integration to health: Durkheim in the new millennium. Social Science and Medicine, 51, 843-857.
Browning, C.R., Feinberg, S.L., and Dietz, R.D. (2004). The paradox of social organization: Networks, collective efficacy, and violent crime in urban neighborhoods. Social Forces, 83(2), 503-534.
Browning, C.R., Feinberg, S.L., Wallace, D., and Cagney, K.A. (2006). Neighborhood social processes, physical conditions, and disaster-related mortality: The case of the 1995 Chicago heat wave. American Sociological Review, 71(4), 661-678.
Browning, C.R., Jackson, A., Soller, B., Krivo, L.J., and Peterson, R.D. (2011). Ecological Community and Neighborhood Social Organization. Paper presented at the American Society of Criminology, Washington, DC.
Bukov, A., Maas, I., and Lampert, T. (2002). Social participation in very old age: Cross-sectional and longitudinal findings from base. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 57(6), 510-517.
Cacioppo, J.T., Hughes, M.E., Waite, L.J., Hawkley, L.C., and Thisted, R.A. (2006). Loneliness as a specific risk factor for depressive symptoms: Cross-sectional and longitudinal analyses. Psychology and Aging, 21(1), 140-151.
Cagney, K.A. (2006). Neighborhood age structure and its implications for health. Journal of Urban Health, 83(5), 827-834.
Cagney, K.A., and York Cornwell, E. (2010). Neighborhoods and health in later life: The intersection of biology and community. Annual Review of Gerontology and Geriatrics, 30(1), 323-348.
Cagney, K.A., Browning, C.R., and Wen, M. (2005). Racial disparities in self-rated health at older ages: What difference does the neighborhood make? The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 60(4), S181-S190.
Cain, A.E., Depp, C.A., and Jeste, D.V. (2009). Ecological momentary assessment in aging research: A critical review. Journal of Psychiatric Research, 43(11), 987-996.
Christakis, N.A., and Fowler, J.H. (2007). The spread of obesity in a large social network over 32 years. New England Journal of Medicine, 357(4), 370-379.
Clampet-Lundquist, S., and Massey, D.S. (2008). Neighborhood effects on economic self-sufficiency: A reconsideration of the Moving to Opportunity experiment. American Journal of Sociology, 114(1), 107-143.
Clarke, P., Ailshire, J.A., and Lantz, P. (2009). Urban built environments and trajectories of mobility disability: Findings from a national sample of community-dwelling American adults (1986-2001). Social Science and Medicine, 69(6), 964-970.
Cook, T.D. (2003). The case for studying multiple contexts simultaneously. Addiction, 98(Supplement 1), 151-155.
Cornwell, B. (2009). Network bridging potential in later life life-course experiences and social network position. Journal of Aging and Health, 21(1), 129-154.
Cornwell, B., and Laumann, E.O. (2011). Network position and sexual dysfunction: Implications of partner betweenness for men. American Journal of Sociology, 117(1), 172-208.
Cornwell, B., Laumann, E.O., and Schumm, L.P. (2008). The social connectedness of older adults: A national profile. American Sociological Review, 73(2), 185-203.
Curtis, S., and Jones, I.R. (1998). Is there a place for geography in the analysis of health inequality? Sociology of Health and Illness, 20(5), 645-672.
Diez Roux, A.V. (2004). The study of group-level factors in epidemiology: Rethinking variables, study designs, and analytical approaches. Epidemiologic Reviews, 26, 104-111.
Diez Roux, A.V., Borrell, L.N., Haan, M., Jackson, S.A., and Schultz, R. (2004). Neighborhood environments and mortality in an elderly cohort: Results from the cardiovascular health study. Journal of Epidemiology and Community Health, 58(11), 917-923.
Duncombe, W., Robbins, M., and Wolf, D.A. (2001). Retire to where? A discrete choice model of residential location. International Journal of Population Geography, 7(4), 281-293.
Duneier, M. (1994). Slim’s Table: Race, Respectability, and Masculinity. Chicago: University of Chicago Press.
Dupre, M.E., Franzese, A.T., and Parrado, E.A. (2006). Religious attendance and mortality: Implications for the black-white mortality crossover. Demography, 43(1), 141-164.
Durazo, E., Jones, M., Wallace, S., Van Arsdale, J., Aydin, M., and Stewart, C. (2011). The Health Status and Unique Health Challenges of Rural Older Adults in California. Health Policy Brief. Los Angeles: Center for Health Policy Research, University of California.
Elder, G.H. (1975). Age differentiation and the life course. Annual Review of Sociology, 1, 165-190.
Eng, P.M., Rimm, E.B., Fitzmaurice, G., and Kawachi, I. (2002). Social ties and change in social ties in relation to subsequent total and cause-specific mortality and coronary heart disease incidence in men. American Journal of Epidemiology, 155(8), 700-709.
Eschbach, K., Ostir, G.V., Patel, K.V., Markides, K.S., and Goodwin, J.S. (2004). Neighborhood context and mortality among older Mexican Americans: Is there a barrio advantage? American Journal of Public Health, 94(10), 1,807-1,812.
Estabrooks, P.A., Lee, R.E., and Gyurcsik, N.C. (2003). Resources for physical activity participation: Does availability and accessibility differ by neighborhood socioeconomic status? Annals of Behavioral Medicine, 25(2), 100-104.
Evans, G.W., Kantrowitz, E., and Eshelman, P. (2002). Housing quality and psychological well-being among the elderly population. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 57(4), 381-383.
Freedman, V.A., Grafova, I.B., and Rogowski, J. (2011). Neighborhoods and chronic disease onset in later life. American Journal of Public Health, 101(1), 79-86.
Galinsky, A.M., Cagney, K.A., and Browning, C.R. (2012). Is collective efficacy age graded? The development and evaluation of a new measure of collective efficacy for older adults. Journal of Aging Research, Article ID 360254. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3270404 [September 12, 2012].
Gallagher, N.A., Gretebeck, K.A., Robinson, J.C., Torres, E.R., Murphy, S.L., and Martyn, K.K. (2010). Neighborhood factors relevant for walking in older, urban, African American adults. Journal of Aging and Physical Activity, 18(1), 99-115.
Giles-Corti, B., and Donovan, R.J. (2002). Socioeconomic status differences in recreational physical activity levels and real and perceived access to a supportive physical environment. Preventive Medicine, 35(6), 601-611.
Glass, T.A., and Balfour, J.L. (2003). Neighborhoods, aging, and functional limitations. In I. Kawachi and L.F. Berkman (Eds.), Neighborhoods and Health (pp. 303-334). New York: Oxford University Press.
Golledge, R.G., and Stimson, R.J. (1997). Spatial Behavior: A Geographic Perspective. New York: Guilford Press.
Granovetter, M.S. (1973). The strength of weak ties. American Journal of Sociology, 78(6), 1,360-1,380.
Hawkley, L.C., Hughes, M.E., Waite, L.J., Masi, C.M., Thisted, R.A., and Cacioppo, J.T. (2008). From social structural factors to perceptions of relationship quality and loneliness: The Chicago Health, Aging, and Social Relations Study. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 63(6), 375-384.
He, W., Sengupta, M., Velkoff, V.A., and DeBarros, K.A. (2005). 65+ in the United States: 2005. Washington, DC: Department of Commerce, and Economics and Statistics Administration, U.S. Census Bureau.
Hochschild, A.R. (1978). The Unexpected Community: Portrait of an Old Age Subculture (rev. ed.). Berkeley: University of California Press.
Hybels, C.F., Blazer, D.G., Pieper, C.F., Burchett, B.M., Hays, J.C., Fillenbaum, G.G., Kubzansky, L.D., and Berkman, L.F. (2006). Sociodemographic characteristics of the neighborhood and depressive symptoms in older adults: Using multilevel modeling in geriatric psychiatry. American Journal of Geriatric Psychiatry, 14(6), 498-506.
Jacobs, J. (1961). The Death and Life of Great American Cities. New York: Random House.
Kubzansky, L.D., Subramanian, S.V., Kawachi, I., Fay, M.E., Soobader, M.J., and Berkman, L.F. (2005). Neighborhood contextual influences on depressive symptoms in the elderly. American Journal of Epidemiology, 162(3), 253-260.
Kwan, M.P. (2009). From place-based to people-based exposure measures. Social Science and Medicine, 69(9), 1,311-1,313.
Lang, I.A., Llewellyn D.J., Langa K.M., Wallace R.B., and Melzer D. (2008). Neighbourhood deprivation and incident mobility disability in older adults. Age and Ageing, 37(4), 403-410.
LeClere, F.B., Rogers, R.G., and Peters, K.D. (1997). Ethnicity and mortality in the United States: Individual and community correlates. Social Forces, 76(1), 169-198.
Li, Y., and Ferraro, K.F. (2005). Volunteering and depression in later life: Social benefit or selection processes? Journal of Health and Social Behavior, 46(1), 68-84.
Litwin, H., and Shiovitz-Ezra, S. (2006). Network type and mortality risk in later life. Gerontologist, 46(6), 735-743.
Lynch, J., Due, P., Muntaner, C., and Smith, G.D. (2000). Social capital: Is it a good investment strategy for public health? Journal of Epidemiology and Community Health, 54(6), 404-408.
Lyons, R. (2011). The spread of evidence-poor medicine via flawed social-network analysis. Statistics, Politics, and Policy, 2(1), 1.
Macintyre, S., and Ellaway, A. (2003). Neighborhoods and health: An overview. In I. Kawachi and L.F. Berkman (Eds.), Neighborhoods and Health (pp. 20-44). New York: Oxford University Press.
Mendes De Leon, C.F., Cagney, K.A., Bienias, J.L., Barnes, L.L., Skarupski, K.A., Scherr, P.A., and Evans, D.A. (2009). Neighborhood social cohesion and disorder in relation to walking in community-dwelling older adults: A multilevel analysis. Journal of Aging and Health, 21(1), 155-171.
Merkin, S.S., Diez Roux, A.V., Coresh, J., Fried, L.F., Jackson, S.A., and Powe, N.R. (2007). Individual and neighborhood socioeconomic status and progressive chronic kidney disease in an elderly population: The Cardiovascular Health Study. Social Science and Medicine, 65(4), 809-821.
Miner, S., Logan, J.R., and Spitze, G. (1993). Predicting the frequency of senior center attendance. Gerontologist, 33(5), 650-657.
Moore, L.V., Diez Roux, A.V., Evenson, K.R., McGinn, A.P., and Brines, S.J. (2008). Availability of recreational resources in minority and low socioeconomic status areas. American Journal of Preventive Medicine, 34(1), 16-22.
Morland, K., Wing, S., Diez Roux, A., and Poole, C. (2002). Neighborhood characteristics associated with the location of food stores and food service places. American Journal of Preventive Medicine, 22(1), 23-29.
Norton, M.C., Singh, A., Skoog, I., Corcoran, C., Tschanz, J.T., Zandi, P.P., Breitner, J.C.S., Welsh-Bohmer, K.A., and Steffens, D.C. (2008). Church attendance and new episodes of major depression in a community study of older adults: The Cache County Study. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 63(3), 129-137.
Nyerges, T., Couclelis, H., and McMaster, R. (2011). The Sage Handbook of GIS and Society. London: Sage.
Ostir, G.V., Eschbach, K., Markides, K.S., and Goodwin, J.S. (2003). Neighborhood composition and depressive symptoms among older Mexican Americans. Journal of Epidemiology and Community Health, 57(12), 987-992.
Pearce, J., Witten, K., and Bartie, P. (2006). Neighbourhoods and health: A GIS approach to measuring community resource accessibility. Journal of Epidemiology and Community Health, 60(5), 389-395.
Pinquart, M., and Sorensen, S. (2003). Associations of stressors and uplifts of caregiving with caregiver burden and depressive mood: A meta-analysis. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 58(2), P112-P128.
Putnam, R.D. (2000). Bowling Alone: The Collapse and Revival of the American Community. New York: Simon & Schuster.
Raudenbush, S.W. (2003). The quantitative assessment of neighborhood social environments. In I. Kawachi and L.F. Berkman (Eds.), Neighborhoods and Health (pp. 112-131). New York: Oxford University Press.
Robert, S.A., and Li, L.W. (2001). Age variation in the relationship between community socioeconomic status and adult health. Research on Aging, 23(2), 233-258.
Rowles, G.D., Oswald, F., and Hunter, E.G. (2003). Interior living environments in old age. Annual Review of Gerontology and Geriatrics, 23, 167-194.
Sabia, J.J. (2008). There’s no place like home: A hazard-model analysis of aging in place among older homeowners in the PSID. Research on Aging, 30(1), 3-35.
Sampson, R.J. (2003). Neighborhood-level context and health: Lessons from sociology. In I. Kawachi and L.F. Berkman (Eds.), Neighborhoods and Health (pp. 132-146). New York: Oxford University Press.
Sampson, R.J. (2008). Moving to inequality: Neighborhood effects and experiments meet social structure. American Journal of Sociology, 114(1), 189-231.
Sampson, R.J., Morenoff, J.D., and Gannon-Rowley, T. (2002). Assessing “neighborhood effects”: Social processes and new directions in research. Annual Review of Sociology, 28(1), 443-478.
Schulz, A., Zenk, S., Israel, B., Mentz, G., Stokes, C., and Galea, S. (2008). Do neighborhood economic characteristics, racial composition, and residential stability predict perceptions of stress associated with the physical and social environment? Findings from a multilevel analysis in Detroit. Journal of Urban Health, 85(5), 642-661.
Seeman, T.E., Miller-Martinez, D.M., Merkin, S.S., Lachman, M.E., Tun, P.A., and Karlamangla, A.S. (2011). Histories of social engagement and adult cognition: Midlife in the U.S. Study. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 66(Supplement), 141-152.
Shankar, A., McMunn, A., Banks, J., and Steptoe, A. (2011). Loneliness, social isolation, and behavioral and biological health indicators in older adults. Health Psychology, 30(4), 377-385.
Shaw, C.R., and McKay, H.D. (1969). Juvenile Delinquency and Urban Areas: A Study of Rates of Delinquency in Relation to Differential Characteristics of Local Communities in American Cities (rev. ed.). Chicago: University of Chicago Press.
Shiffman, S., Stone, A.A., and Hufford, M.R. (2008). Ecological momentary assessment. Annual Review of Clinical Psychology, 4, 1-32.
Silverstein, M., and Angelelli, J.J. (1998). Older parents‘ expectations of moving closer to their children. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 53(3), S153-S163.
Small, M.L. (2009). Unanticipated Gains: Origins of Network Inequality in Everyday Life. New York: Oxford University Press.
Smith, K.P., and Christakis, N.A. (2008). Social networks and health. Annual Review of Sociology, 34, 405-429.
Stafford, M., McMunn, A., Zaninotto, P. and Nazroo, J. (2011). Positive and negative exchanges in social relationships as predictors of depression: Evidence from the English Longitudinal Study of Ageing. Journal of Aging and Health, 23(4), 607-628.
Strath, S., Isaacs, R., and Greenwald, M.J. (2007). Operationalizing environmental indicators for physical activity in older adults. Journal of Aging and Physical Activity, 15(4), 412-424.
Subramanian, S.V., Kubzansky, L., Berkman, L., Fay, M., and Kawachi, I. (2006). Neighborhood effects on the self-rated health of elders: Uncovering the relative importance of structural and service-related neighborhood environments. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 61(3), S153-S160.
Subramanian, S.V., Elwert, F., and Christakis, N. (2008). Widowhood and mortality among the elderly: The modifying role of neighborhood concentration of widowed individuals. Social Science and Medicine, 66(4), 873-884.
Thomas, P.A. (2010). Is it better to give or to receive? Social support and the well-being of older adults. The Journals of Gerontology: Series B Psychological Sciences and Social Sciences, 65(3), 351-357.
Uchino, B. (2006). Social support and health: A review of physiological processes potentially underlying links to disease outcomes. Journal of Behavioral Medicine, 29(4), 377-387.
Waitzman, N.J., and Smith, K.R. (1998). Phantom of the area: Poverty-area residence and mortality in the United States. American Journal of Public Health, 88(6), 973-976.
Wen, M., and Christakis, N.A. (2005). Neighborhood effects on posthospitalization mortality: A population-based cohort study of the elderly in Chicago. Health Services Research, 40(4), 1108-1127.
Yamashita, T., and Kunkel, S.R. (2011). Geographic access to healthy and unhealthy foods for the older population in a U.S. metropolitan area. Journal of Applied Gerontology, 31(3), 287-313.
Yao, L., and Robert, S.A. (2008). The contributions of race, individual socioeconomic status, and neighborhood socioeconomic context on the self-rated health trajectories and mortality of older adults. Research on Aging, 30(2), 251-273.
Yen, I.H., Michael, Y.L., and Perdue, L. (2009). Neighborhood environment in studies of health of older adults: A systematic review. American Journal of Preventive Medicine, 37(5), 455-463.
York Cornwell, E., and Waite, L.J. (2009). Social disconnectedness, perceived isolation, and health among older adults. Journal of Health and Social Behavior, 50(1), 31-48.
Zenk, S.N., Schulz, A.J., Israel, B.A., James, S.A., Bao, S., and Wilson, M.L. (2005). Neighborhood racial composition, neighborhood poverty, and the spatial accessibility of supermarkets in metropolitan Detroit. American Journal of Public Health, 95(4), 660-667.
Zingmark, K., Norberg, A., and Sandman, P.O. (1995). The experience of being at home throughout the life span. Investigation of persons aged from 2 to 102. International Journal of Aging and Human Development, 41(1), 47-62.
























