Important Points Made by the Speakers
- The Patient-Centered Outcomes Research Institute (PCORI) has been designed to support research that gives people the information they need to make health care decisions that reflect their desired health outcomes, in part by continuously seeking input from patients and from a broad range of stakeholders. (Beal)
- Increasing the number of states that are willing to expand Medicaid is essential to realizing the potential of the ACA. (Miller)
- Community organizers need to identify unmet needs, the obstacles that must be overcome to meet those needs, and strategies to overcome those obstacles. (Lash)
- Grassroots activism is critical for policies made at the top levels to have an effect at the community and individual levels. (Kingwood-Small)
As noted in the first chapter of this workshop summary, consumer engagement will be critical to the ACA’s success. This final chapter of the summary provides four perspectives on consumer engagement ranging from the national to the local level.
THE PCORI APPROACH TO PATIENT AND STAKEHOLDER ENGAGEMENT
PCORI was created by the ACA as a 501(c)(1) independent nonprofit research organization, only about 30 of which exist in the United States. It was created and funded by Congress but is entirely separate from the federal government and has a private board. Its primary purpose is to fund comparative effectiveness research, which means that the institute “should be in a position to help answer questions commonly faced by patients and those who care for them in real-world settings,” said its chief officer for engagement, Anne Beal. The answers to those questions will affect people’s health by giving people the information they need to make informed choices. PCORI’s independence was designed to make sure that there is no bias in the research that it supports.
PCORI is also unusual in that its budget has been appropriated through 2019, with most of its resources coming from fees on Medicare, private health insurance, and self-insured plans. Its budget was approximately $150 million in 2012, and that amount will grow to a projected $500 million annually from 2014 through 2019. Twenty percent of its funding goes to the U.S. Department of Health and Human Services (HHS) to support dissemination, training, and other research capacity-building efforts. Nevertheless, said Beal, “we have the resources to support a robust portfolio of quality research proposals, and 10 percent of that research funding will be dedicated to address health disparities.”
“PCORI takes the ‘P’ in its name very seriously,” Beal said. Its board has spent considerable time defining patient-centered outcomes research, and it has emphasized that the work that PCORI does needs to be meaningful to patients. To do that, PCORI plans to ensure that it continuously seeks input from patients and from a broad range of stakeholders.
The mission of PCORI is to help people make informed health care decisions and improve health care delivery and outcomes by producing and promoting high-integrity, evidence-based information that comes from research guided by patients, caregivers, and the broader health care community. “The bottom line,” said Beal, “is that the institute wants to support research that gives people the information that they need to make health care decisions that reflect their desired health outcomes.”
Beal told the story of her 83-year-old aunt who had lung cancer. “I, as a physician, had very key ideas as to what I wanted in terms of her outcomes. She, as an 83-year-old woman, said, ‘I have to die of something. What I want is to not be in pain, and I don’t want to lose my hair,’” said Beal. “The philosophy behind PCORI,” she said, “would be to respect her views.”
PCORI’s core duties are to
- Establish national research priorities,
- Establish and carry out a research agenda,
- Develop and update methodological standards, and
- Disseminate research findings.
The PCORI board has also established a set of national priorities for research, and these are outlined below.
Assessment of Prevention, Diagnosis, and Treatment Options
- Comparing alternative clinical options to support personalized decision making and self-care
- Identifying differences in patients’ responses to therapy
- Studying patients’ preferences for various outcomes
- Improving support of patient self-management
- Focusing on coordination of care for complex conditions and improving access to care
- Comparing alternative strategies for workforce deployment
Communication and Dissemination Research
- Understanding and enhancing shared decision making
- Using alternative strategies for dissemination of evidence
- Exploring opportunities to improve patient health literacy
- Understanding differences in effectiveness across groups
- Understanding differences in preferences across groups
- Reducing disparities through the use of findings from patient-centered outcomes research
Accelerating Patient-Centered Outcomes Research and Methodological Research
- Improving study designs and analytical methods in patient-centered outcomes research
- Building and improving clinical data networks
- Establishing methods for training researchers and patients to participate in patient-centered outcomes research
- Establishing a methodology for the study of rare diseases
PCORI is a clinical comparative effectiveness research institute, Beal emphasized, so it is going to focus on comparing options to eliminate disparities rather than supporting studies to describe disparities. Also, in establishing its national priorities for research, PCORI chose not to mention specific diseases, to allow researchers and others broad latitude when they submit their best ideas.
Beal grouped the first category of research priorities—assessment of prevention, diagnosis, and treatment options—with classic comparative effectiveness research and noted that this category represents about 40 percent of PCORI’s budget. However, PCORI is also interested in ways to get the results of such research into practice quickly, because patients need answers right away. About 20 percent of its research budget focuses on communication and dissemination research that is focused on reaching different populations. For example, young people are now more likely to communicate through texts than through emails. “The way that you get to different populations needs to be done and approached in a thoughtful manner,” Beal explained.
PCORI is especially emphasizing patient and stakeholder engagement (see Figure 6-1). First, it is asking patients and stakeholders what PCORI should study. “What is the type of research that we should be doing? What are the challenges that you face?” said Beal. For example, shortly before the workshop, PCORI held a roundtable with a group of Latinas, because women are often the arbiters of health care decisions for families and their communities. The group helped identify opportunities to study different
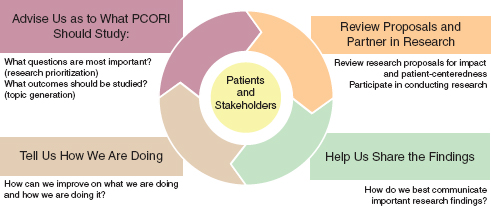
FIGURE 6-1 Patient-Centered Outcomes Research Institute (PCORI) is seeking multiple ways to engage patients and stakeholders.
SOURCE: Beal workshop presentation, April 22, 2013. From PCORI.
models of community outreach, such as contact by telephone versus door-to-door visits by community health workers. Other meetings with targeted groups are identifying other challenges that can inform the research agenda.
PCORI has advisory panels that met for the first time just a few days before the workshop. The initial set of advisory panels focused on four areas:
- Addressing disparities;
- Assessing prevention, diagnosis, and treatment options;
- Improving health care systems; and
- Patient engagement.
The panels, for which more than 1,000 people applied for 84 positions, are helping to identify and prioritize research questions. Panelists also represent a wide range of professions, geographic areas, and groups to provide a diverse set of perspectives.
PCORI has an open webpage through which anyone can submit a research question, and it has already accepted about 850 questions and topics. Furthermore, the questions come not just from health services researchers but, for example, from mothers who are having difficulty managing a child’s condition. In addition, PCORI has reached out to the public for help in reviewing proposals. It has determined that at least one-third of all the reviewers on study sections need to be either patients or other non-researcher stakeholders. Again, said Beal, many more people have applied to work with the institute than it has been able to accommodate, adding that “we take a lot of pride in making sure that the perspective of the entire health care community is reflected.”
Every research project supported by PCORI must have a patient and stakeholder partner. The engagement of patients and stakeholders should include participation in the formulation of research questions; definition of the essential characteristics of study participants, comparators, and outcomes; monitoring of study conduct and progress; and dissemination of research results. “It’s not just a check-off box,” said Beal. “We want to see their time and effort reflected in the research.”
PCORI’s inaugural funding cycle had the budget to distribute 50 awards, but it made only 25 because it was looking for projects of higher quality and with more patient involvement. “Our standards for including patients and other stakeholders in research are unique, and we are working with the research community to ensure that they are fluent in our criteria. Already we are seeing that work pay off in the recently submitted applications,” she said.
PCORI’s funding rate has increased in subsequent cycles, as the research community’s understanding of its requirements has improved. PCORI made 71 funding awards totaling more than $114 million in its third funding
cycle. The rate of applications approved doubled from the inaugural funding cycle to its third.
Finally, Beal discussed PCORI’s framework for dissemination and implementation, even though it has just started funding research and does not yet have much to disseminate. The framework has been designed to
- Guide the organization in disseminating the research findings of funded research conducted in the national program areas,
- Enhance implementation by actively facilitating how PCORI’s research findings can be used by health care decision makers, and
- Evaluate how the effect of the dissemination of such findings reduces practice variation and disparities in health care.
As an example of putting results into practice, Beal cited two findings: that mothers should have their babies sleep on their back to reduce crib death, and that doctors should use checklists to reduce central line infections for patients in an intensive care unit. Those are very different results aimed at very different populations, and different mechanisms should be used to disseminate and implement those findings. Important considerations include speeding the implementation and use of patient-centered outcomes research; becoming a trusted source of information; and engaging stakeholders across the health care community to include PCORI research in training, practice, and standards. Most researchers do not have much experience with the dissemination and implementation of their research results, but PCORI is asking them to develop partnerships and take other steps to get the word out and ensure that research results have an impact.
“One of the things that I’ve personally learned is there are a lot of moms and patient bloggers and listservs and tweeters out there,” said Beal. “Those are the kinds of folks we would want to have actively involved and engaged and anticipating the results of our work so that when it comes out they can help to share and spread the word,” she said.
Patient involvement tends to be an afterthought in the traditional research model, Beal noted, yet patients will have many new responsibilities in the work of PCORI. Patients will have to be involved for the research to have an impact and be successful and for health care reform to succeed.
“There are a lot of moms and patient bloggers and listservs and tweeters out there. Those are the kinds of folks we would want to have actively involved and engaged and anticipating the results of our work so that when it comes out they can help to share and spread the word.”
—Anne Beal
THE ROLE FOR CONSUMER ENGAGEMENT
Community Catalyst is a national nonprofit health advocacy organization that has been working to ensure that everyone has equal access to high-quality, affordable health care, said its director of strategic policy, Michael Miller. It collaborates with national, state, and local consumer organizations, policy makers, and foundations and has built and supported consumer advocacy networks in more than 40 states. In particular, it works to advance state health policy solutions and to bring state and local voices into the national health care debate.
Miller focused on three provisions related to community engagement that Community Catalyst sees to be critical to realizing the potential of the ACA: coverage expansion, delivery reform, and community benefits. Together, these three provisions can create a “new ecology” for reducing disparities, he said.
As an example of what can be achieved in expanding coverage, Miller cited the state of Massachusetts. Disparities have not been eradicated in Massachusetts, but significant progress in rates of coverage as well as access to care has been made (see Figure 6-2). Even uninsured individuals in Massachusetts are experiencing improved access to care, Miller noted, perhaps because the safety net is under less stress.
The ACA probably will not produce results as good as those that have been achieved in Massachusetts, partly because of the number of states that either will not participate or are leaning toward not participating in the expansion of Medicare (see Figure 6-3). This lack of state participation paints a “very disturbing picture with regard to racial and ethnic health disparities,” Miller said. “If you look at what percentage of people would be eligible for Medicaid in the states that are not taking up the Medicaid expansion or have not yet decided to take up the Medicaid expansion, it is twice the national average. . . . If we are going to realize the health equity potential of the Affordable Care Act, it starts with getting states to take up the Medicaid expansion,” he said.
Increasing the number of states that will expand Medicaid requires a robust grassroots effort, including active involvement of the affected communities. Toward that end, Community Catalyst has identified three major barriers to engaging communities of color in advocacy efforts. First, people have not yet grasped the magnitude of the opportunity. Second, resources to support such an effort are lacking. Third, greater trust is needed between state-based advocacy organizations and community-based organizations working on issues related to the health of their communities.
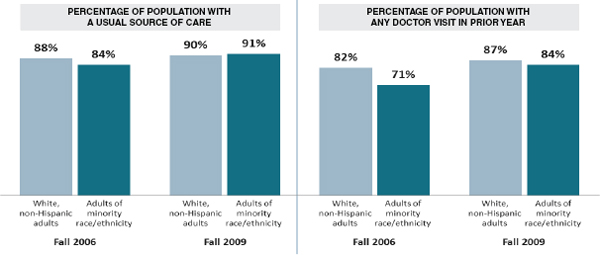
FIGURE 6-2 Massachusetts racial and ethnic disparities.
SOURCE: Miller workshop presentation, April 22, 2013. From Urban Institute, Massachusetts Health Reform Survey, 2010.
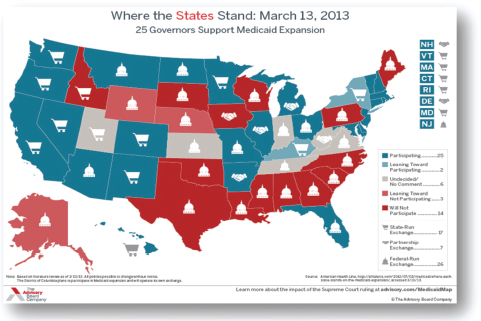
FIGURE 6-3 Governors supporting the expansion of Medicaid as of March 13, 2013.
SOURCE: Miller workshop presentation, April 22, 2013.
Miller presented a set of recommendations to remove these barriers:
- Build and strengthen community-based organizations.
- Encourage groups striving to provide access to health care statewide to prioritize work on achieving equity.
- Build strong partnerships between state and local organizations.
- Demystify the policy-making process and provide opportunities for local activists.
- Develop a disparities reduction and health equity policy agenda.
- Hold meetings in target communities to increase understanding and participation.
“It starts with embracing a vision of health equity as an organizational priority,” said Miller. State partners need “a plan for how they are going to engage with local communities of color,” he added.
The establishment of exchanges will also be a critical aspect of coverage expansion, because the people who will be covered through the exchanges are more likely to be from communities of color. These exchanges need to implement six principles, Miller said:
- Diverse inputs,
- Language access,
- Robust outreach,
- Simplified enrollment and protections for privacy and confidentiality,
- Robust networks of safety net providers, and
- A disparities-reduction plan as part of an overall strategy to achieve quality health care.
Exchanges will create a structural opportunity for diverse communities to influence coverage in their states. The extent to which they are able to increase coverage depends on the extent to which state and local groups are at the table helping to shape what the exchanges do. Whether an exchange targets disparity reduction as a key goal and whether the quality improvement strategy incorporates that goal will be critical elements of realizing this potential.
Only $50 million has been allocated to the outreach effort for the 30 states that are going to be operating under federally facilitated exchanges. “That money is not going to go very far, unfortunately, and that’s obviously a big concern,” said Miller, noting that “just because you build, it does not mean they will come.”
Populations eligible for Medicaid need to be a specific target of outreach and enrollment. Miller explained that “there are some real opportunities with the Medicaid population that we don’t have as much with the exchange population.” Large numbers of people who are eligible for the Supplemental Nutrition Assistance Program, who are currently receiving financial assistance through hospitals, or who are patients at health centers, can be moved quickly from not being covered to being covered. Also, the outreach workforce needs to look like the communities being targeted.
Turning from coverage to care, Miller flagged an important structural opportunity. People who are eligible for both Medicare and Medicaid are much more likely to be people of color. Creating organized delivery systems for this population also creates new opportunities for patient engagement.
Experiences in Massachusetts and elsewhere have shown that patient empowerment and engagement are associated with better health outcomes and lower costs, yet patients at lower socioeconomic levels tend to be less engaged. Experiments in places like New Jersey and Oregon have shown that health care reform can do much more to engage the community. In Oregon, for example, patients serve on the boards of coordinated care organizations as a means of increasing patient engagement. Patient involvement at the level of system oversight is another way to create patient-centered systems. “The motto of the disability community—nothing about us without us—in my mind applies very well to all of this work,” he said.
Finally, Miller briefly discussed the community health needs assessments. The community benefit provisions in the ACA provide an opportunity to integrate financial assistance and health promotion for patients. To take advantage of that opportunity, however, communities need to be involved in the development of community health needs assessments. Are communities of color at the table, and are they helping to shape the planning for assessments? As hospitals move away from a fee-for-service payment system toward more integrated systems and a greater emphasis on population health, Miller noted that “there is real opportunity to integrate the community benefits program with the clinical programs of hospitals.” This transition even provides an opportunity to think about the social determinants of health, economic development, and the hospital’s footprint in the community. “It’s somewhat like turning a battleship,” said Miller, but “we know that these things have as much or more to do with the health of the population as access to medical care.”
Miller provided 10 tips for engaging people of color:
- Practice basic etiquette.
- Engage beyond education.
- Support meaningful engagement in policy change.
- Do not ignore or forget to address racism.
- Make a commitment.
- Find the right messenger.
- Communicate effectively.
- Practice team building.
- Provide financial support.
- Celebrate wins.
The ACA provides many tools to address disparities, Miller concluded, “but tools don’t build houses; people do.” Fulfilling the potential of the ACA will depend on the extent to which people take advantage of the opportunities that it presents.
“If we are going to realize the health equity potential of the Affordable Care Act, it starts with getting states to take up the Medicaid expansion.”
—Michael Miller
CHALLENGES FOR EXCHANGES IN REACHING DIVERSE COMMUNITIES
The health care system is like a three-legged stool, said Alta Lash, executive director of United Connecticut Action for Neighborhoods. One leg consists of health care providers, who are very well organized. A second leg consists of health care payers, who also are very well organized. The third leg consists of the consumers of health care, “who interact with this system while sitting in a medical examining room on an examining table in a paper gown waiting to get your blood pressure taken and knowing inevitably they’re going to put you on the scale,” she said.
The ACA offers the promise of an entirely different model in which people actively participate in health care, said Lash. Realization of this promise, however, means reaching out to people who are not necessarily prepared to participate.
The group that Lash leads has been working with the community in Hartford, Connecticut, to prepare them for the new world of health care. The first task that the group faced was figuring out how to reach the people who it is targeting. That meant dealing not with just one community but with many: the hearing-impaired community, Latinas who are Puerto Rican versus Latinas who are Dominican, West Indian communities, African American communities, and so on. She noted that “we have to strategize about how to tailor the message for particular communities.”
Community organizers use a technique called a “power analysis” to identify the communities that they need to reach, the obstacles to be overcome, and the strategies that will maximize strengths and minimize weaknesses. In the context of health care, that will mean dealing largely with people who are uninsured, said Lash. For the most part, these are working people who are sometimes working two or three jobs. They are probably paid by the hour and are not paid when they cannot get to work, which means that if they are sick, they may not have enough money for groceries by the end of the month. “This is the target constituency for the exchange, and we have to figure out what is the best way to reach that constituency,” she commented.
Simply hiring a public relations firm will not get the job done, Lash said, explaining that “we’ve got to think much more creatively and outside of the box if we are going to be able to talk to the waitress, the hairdresser, the person who has a construction job 1 week and the next month he’s not working.” One organization that has done a good job of reaching these communities, said Lash, is H&R Block. H&R Block offices are easy to find. They advertise on buses and on media that many people use, like Univisión, Telemundo, and local radio stations. People carry their paperwork to the H&R Block office, and they get their taxes done at a reasonable rate. “If
H&R Block can reach them, we should be able to reach them, too, with the exchange message,” she noted. Another good model is the public library system, said Lash, which can help spread the message about health care reform.
If people are going to participate in the exchanges, the product that the exchanges are providing has to be good. For the communities where Lash works, this means that the product needs to be affordable. Not everyone in those communities will qualify for subsidies, and the insurance that they purchase is going to have to provide them with value for the money that they spend. “I can’t wait until I spend $5,000 of my own money in order to see the first dollar from the exchange. That just isn’t going to cut it,” Lash explained.
Finally, the people who are selling the product need to be good communicators. Complex ideas will need to be translated into concrete language that people can understand. For example, Lash said that “we use the term ‘exchange’ all the time. It took me weeks to figure out what exactly is an exchange.” Assistants are going to need to sit down at a computer with the people buying insurance and walk them through the process. “This is the one that scares me,” said Lash. “It has to be someone who knows and understands the community. But it also has to be someone who knows insurance and can explain insurance terminology to a group of people who don’t know what a copay is, what a deductible is, what is cost-sharing, what is silver metal tier.” Things that other people take for granted are not taken for granted in these communities, Lash said, adding that “when the person sits down with an individual to explain this, I think it’s going to be much more labor intensive than we anticipate, because people don’t have a clue of what they’re buying. . . . Getting the word out is the easy part. Getting people to actually understand what they’re paying their hard-earned dollars for is a whole other ball of wax.”
Perhaps a useful analogy is car insurance, Lash continued, since everyone is supposed to have car insurance, but health insurance is still more complicated than car insurance. And people will not react calmly when something that they think is covered is not covered.
“We’ve got to think much more creatively and outside of the box if we are going to be able to talk to the waitress, the hairdresser, the person who has a construction job 1 week and the next month, he’s not working.”
—Alta Lash
“We have to think through some of these challenges,” Lash concluded. “Old strategies won’t work.” At the same time, she emphasized the contin-
ued importance of political activism. Policies made at the top levels have momentous effects on people’s lives, and the people who are affected by those policies need to monitor what policy makers are doing and hold them accountable. She ended her comments by adding that “people need to realize that their voice matters.”
The Ashe Faith Project is a grassroots initiative of the Mount Aery Development Corporation whose goal is to close the health disparities gap in the Bridgeport, Connecticut, area by strengthening the partnerships between community and faith organizations and using knowledge, experience, and passion to maximize local synergies, collaboration, and service integration. “All that basically means,” said Reverend Nancy Kingwood-Small, project director at the Ashe Faith Project, “is we are the little engine that could.”
The Ashe Faith Project, which has been funded by the Connecticut Health Foundation and the Substance Abuse and Mental Health Services Administration, has been presented to Congress as a model program that can be replicated throughout the country. A volunteer initiative, it offers client-level services, including health screenings and support groups. Beginning with an initiative that addressed HIV and substance abuse about 3.5 years ago, it has established a network of more than 40 faith organizations and has expanded the infrastructure used to address health disparities. It has strengthened partnerships, gained the trust of community residents, held focus groups to learn about the needs of the community, and become an information hub for the community.
The Ashe Faith Project came out of an earlier initiative that Kingwood-Small started in her home about 7 years ago. A group of women came together on a weekly basis to look at the rate of HIV infection among women in the black community. Kingwood-Small wrote a 5-week training curriculum, and the group started engaging volunteers from the community. To date, more than 100 people have gone through the curriculum and have received their certificates of completion. Of that group, 27 women have received their trainer certificates, and 14 have gone on to full-time jobs working in the field of prevention.
One of the project’s initiatives is a monthly support group for women of color called Sacred Women, which offers women a safe environment for them to share and receive support and information. Sacred Women also offers an array of services, including addressing trauma-related experiences and substance abuse.
Another initiative is the Power Source Leadership Academy, which is designed for black men to feel comfortable and share their experiences.
Beginning as a monthly group, Power Source now meets weekly and has established partnerships with the Aspen Institute and the Connecticut Health Foundation. It offers workshops and roundtables and seeks to initiate men into responsible adulthood and fatherhood. Power Source also offers training on the ACA and on health disparities among black men. Similarly, the Ashe Faith Project offers advocacy training for women of color to help them become better advocates for themselves and their families.
Two years ago the Ashe Faith Project entered into a partnership with the University of Bridgeport Naturopathic Medicine Clinic to offer free naturopathic services. It has also partnered with Optimus Health Care and established a referral system that ensures that patients seeking an appointment will be seen within 48 hours. In addition, Kingwood-Small works as deputy director of the Greater Bridgeport Adolescent Prevention Program, which offers screening for sexually transmitted infections as well as pregnancy testing.
Turning to the ACA, Kingwood-Small quoted Steven Covey: “Seek first to understand, then to be understood.” The ACA is a paradigm shift in health care, but it requires that communities be brought through the transition. The Ashe Faith Project is helping in this process by providing help with applications, referrals, and even transportation. “We must learn to meet people where they are,” she said.
The ACA has the potential to create a disconnect between the policy and the people, said Kingwood-Small. Policies made at the top level often do not trickle down to the grassroots level, she said, noting that “we need to keep these people in mind, because there for the grace of God it could be you or I. I know at one time in my life it was me.”
The ACA can look like “a mess” in local communities, said Kingwood-Small, adding that “we need someone to help us educate, someone to raise awareness, someone to empower the community.” For example, the Ashe Faith Project has been involved in the convening of community meetings with the health exchange and partner agencies to identify strategies around engagement, recruitment, and enrollment. Such meetings help agencies and community organizations cooperate rather than compete. “Collectively, we can do the work,” she said.
“Eventually that window is going to lift and blessings will come down.”
—Nancy Kingwood-Small
The faith community is involved and engaged, but it needs resources and people. The Ashe Faith Project now has a waiting list of churches and faith projects that want to partner with it. “We are on the front lines, and we
continue to do the work with money or without money because we consider it a ministry. We know that eventually that window is going to lift and blessings will come down,” she concluded.
A participant who is doing a fellowship at the Aetna Foundation commented that she would like to know how to reach out and partner with media people. Lash replied that virtually all women’s magazines publish health pieces.
Participant Rebecca Skye from New Hampshire observed that she has concerns that states cannot effectively do community engagement with the limited funds available. Miller agreed that there is not adequate funding to support robust outreach and education efforts regarding enrollment. Kingwood-Small noted that this makes working together in partnerships with the agencies involved critical to identify strategies around engagement, recruitment, and enrollment.
Roundtable member Winston Wong asked if community engagement and mobilization is an extension of patient centeredness. Beal commented that we do not know the answer to that yet.
Amos Smith of the Community Action Agency of New Haven asked if the funding was weighted to spend more at the top and middle ends of the economic spectrum, rather than at the bottom end where the most vulnerable people are. This vulnerable population has literacy issues as well. Miller replied that there is progress being made in this area.
















