2
CONCEPTUAL FRAMEWORKS FOR REVIEWING EVIDENCE-BASED PREVENTION IN PSYCHOLOGICAL HEALTH
This chapter presents the conceptual frameworks that the committee used to approach its task of assessing resilience, reintegration, and prevention programs used to enhance psychological health and prevent psychological health disorders in service members and their families. These conceptual frameworks also guided the evaluation of the evidence base for maintaining service personnel in good psychological health. The chapter covers (1) the terminology used the report, (2) a definition of optimal psychological health for military members and their families, (3) the selection of a conceptual approach to preventive strategies in general and to evidence-based preventive activities, (4) a social ecological model for considering the determinants of good psychological health, (5) a framework for categorizing interventions to prevent psychological disorders and promote psychological health, (6) a framework for the phases of military experience and how prevention activities in psychological health work in the military, and (7) a model with which to organize concepts related to the prevention program development and measurement discussed in this chapter.
In the health field the terms “behavioral health,” “mental health,” and “psychological health” are often used interchangeably. Distinguishing among these terms is challenging, as there is little in the way of a shared language or clear definitions that are used consistently across systems and professional fields. There is a growing emphasis on the behavioral aspects of health promotion and illness prevention that had coincided with the increasing use of an interdisciplinary approach to health care delivery, one that maximizes the use of both medical and behavioral interventions (APA, 2013). This recognition of the importance of behavioral health promotion on good mental health is exemplified by the broad and inclusive definition of behavioral health used by the Substance Abuse and Mental Health Services Administration (SAMHSA) in its National Behavioral Health Framework (SAMHSA, 2013a):
By behavioral health, SAMHSA refers to a state of mental/emotional wellbeing and/or actions that affect wellness. Behavioral health problems include substance use disorders; alcohol and drug addiction; and serious psychological distress, suicide, and mental disorders. This includes a range of problems from unhealthy stress or subclinical conditions to diagnosable and treatable diseases like serious
mental illnesses and substance use disorders, which are often chronic in nature but from which people can and do recover with the help of a variety of interventions from medical and psychosocial treatments to self-help and mutual aid. The term is also used to describe the service systems encompassing prevention and the promotion of emotional health; the prevention of mental and substance use disorders, substance use, and related problems; treatments and services for mental and substance use disorders; and recovery support.
The committee deliberated about the use of the term “behavioral health” versus “psychological health” for this report. There was agreement that both terms are acceptable, but that both have drawbacks. The committee ultimately chose to use, in most cases, the term “psychological health,” because, as discussed below, the committee views psychological health as the foundation for health and wellness in general and because psychological health is protective against the development of mental illness and substance use disorders. Furthermore, the committee was concerned that the broad use of the term “behavioral health” might seem to imply that the various problems under discussion result solely from individual behavior, and the committee was also mindful of the practical consideration that research studies and other documents cited in this report often use the term “behavioral health” to refer specifically to alcohol and drug abuse. The committee notes that the effort to destigmatize mental health issues is one of the biggest factors driving the evolving use of terminology in the military health system and the health care field in general.
Prevention strategies designed to reduce the onset and severity of posttraumatic stress disorder (PTSD), depression, substance abuse, suicide, and interpersonal violence and to enhance responses to stress and trauma exposure as well as to promote reintegration with minimal challenges have the ultimate goal of creating good psychological health among military personnel and their families. Good psychological health is not simply the absence of diagnosable psychological health problems, although maintaining a state of good psychological health is likely to help protect against the development of many such problems. The committee holds the view that prevention should address both risk reduction and health promotion. Risk reduction targets specific outcomes or risk factors and health promotion focuses on increasing levels of health rather than preventing any particular disease (Nash and Watson, 2012). Health promotion is the process of enabling people to increase control over their health and its determinants and to thereby improve their health (Participants at the 6th Global Conference on Health Promotion, 2005). Prevention efforts aligned with health promotion emphasize fostering well-being among individuals with a goal of helping those individuals lead healthy, thriving lives. In the view of those who take this approach, the goal is not simply to prevent psychological health problems but also to promote positive psychological health, defined as a state of well-being in which persons can realize their abilities, cope with life’s stresses, and work regularly and productively (Jahoda, 1958). The notion of positive psychological health underpins the military notion of “Total Force Fitness,” which lies at the core of the Department of Defense (DOD) approach to building and maintaining health, readiness, and performance. According to the total force fitness approach, individuals should engage in choices and practices that will build psychological strength, just as
boot camp and physical exercise build physical fitness, because optimal performance requires one to be healthy both in mind and in body (Jonas et al., 2010).
Total Force Fitness involves targeting all domains of health: spiritual, psychological, behavioral, social, physical, nutritional, medical, and environmental (Bates et al., 2010). As mind, body, and spirit are intertwined, good psychological health is synergistic with the other domains of health. Thus, preventive strategies in one domain, such as those directed at depression, are likely to have benefits in other domains of health—such as social health—and strategies such as healthy nutrition, sleep, and exercise routines may be necessary for achieving optimal psychological health under conditions of high stress. Furthermore, this framework’s emphasis on the importance of social relationships indicates that service members’ families should be taken into consideration.
Background
Prevention is a set of strategies, complementary to the role of treatment, that is aimed at achieving a state of good psychological health, particularly in the context of population mental health (WHO, 2002). Broadly speaking, prevention is an approach in which either the general population or a specific group of people identified as being at risk for a disorder is targeted by policies, changes in the environmental, or the provision of group or individual services with the expectation that some future disorder in that group will be ameliorated, either by reducing its severity, delaying its onset, or decreasing the number of people affected (IOM, 2009). The definition and classification of prevention have evolved over time. In the well-known, original framework for public health prevention, prevention was classified into three levels: primary, secondary, and tertiary (Caplan, 1964).
The goal of primary prevention, as it was defined by Caplan and further refined by Cowen (1977, 1980), is to use risk reduction strategies to prevent the onset of specific diseases before any symptoms arise. Primary prevention efforts target either the entire population or subgroups with known vulnerabilities (e.g., raising alcohol prices on military bases so that they are equal to the prevailing price in the community). Secondary prevention efforts are designed to identify symptoms of disorders early in order to reduce their duration (e.g., screening and intervention for depression) or their sequelae (e.g., screening and intervention for suicidal risk). Tertiary prevention is designed to prevent long-term disability and rehabilitate individuals with a disorder and to return them to their productive capacity as quickly as possible (e.g., a pain management program aimed at preventing the sorts of disability that prevent a return to duty). Critics of Caplan’s classification argue that it may be difficult to differentiate between primary, secondary, and tertiary prevention in the field of psychological health because of the complex etiology and interconnected nature of psychological health problems (Hage and Romano, 2013).
Gordon (1983) provided an alternative conceptualization of prevention that focuses on the characteristics of the intended audience; it complements the classical conception based on risk factors and their sequelae. The three levels of prevention in Gordon’s framework are defined by the intended audience and are universal, selective, and indicated. Universal prevention strategies are offered to the entire population, with the goal of the intervention being to reduce the probability of the undesired outcome. Selective prevention strategies are targeted to
subpopulations identified as being at elevated risk for a disorder, for example, those being deployed to a war zone. Indicated prevention strategies are those targeted to individuals who have been identified as having increased vulnerability or risk for a disorder based on individual screening (but who are not currently symptomatic). In Gordon’s classification, Caplan’s “tertiary” prevention is viewed as a treatment (Gordon, 1983).
There is growing recognition that the next stage of improving health and preventing disease will involve renewed emphasis on population-level, non-clinical strategies (IOM, 2012). Population health is defined as “the health outcomes of a group of individuals, including the distribution of such outcomes within the group” (Kindig and Stoddart, 2003, p. 381). Population health is a function not only of health care, but also of health behaviors, social and economic factors, the physical environment, and other influences (Kindig, 2011). In the context of this report, population health refers to service members and their families and the various influences that are determinants of their health.
Committee’s Prevention Model
Consistent with two previous IOM committees (IOM, 1994, 2009), this committee has adopted a version of Gordon’s model (universal, selective, indicated). An assessment of treatment interventions is outside the scope of this committee’s charge, so it was important to the committee to distinguish prevention from treatment. Following Gordon, it defined indicated prevention interventions as those targeting high-risk individuals who do not meet the diagnostic criteria for a disorder but who do have detectable markers that indicate onset is likely. However, interventions targeting individuals with existing disorders are distinct from—although complementary to—prevention efforts and should be considered treatment. This committee is in agreement with the conclusions made by prior committees that for individuals with full-blown disorders, treatment should include prevention elements to lower the likelihood of relapse as well as associated negative outcomes; for example, treatment for individuals diagnosed with depression should include suicide prevention strategies. It should be noted, however, that individuals’ psychological health conditions will affect the psychological health of their families; thus, treatments that include an ecological framework may include preventive approaches for those at risk due to the illness of a family member (e.g., there are preventive opportunities for family members of service members with PTSD or traumatic brain injury; see Tanielian et al., 2013).
Evidence-Based Prevention
As mentioned above, prevention includes strategies to reduce the prevalence or severity of negative health outcomes and promote health. Throughout this report the committee emphasizes that prevention interventions should rest on sound conceptual and empirical foundations and should be rigorously designed and evaluated. An evidence-based intervention for one condition may not be effective for another condition.
The strength of evidence of tested approaches will fall somewhere along a continuum from weak to strong. Evidence becomes “stronger” with replication and field testing in various circumstances. Even evidence from multiple studies may be judged insufficient to resolve all doubts about the likely effectiveness of an approach designed for a different population or situation (SAMHSA, 2009). This is relevant in the military context where many interventions
have been developed and tested with civilian populations but not adapted or tested in military populations (IOM, 2013b; Lester and Flake, 2013).
SAMHSA formulated its Strategic Prevention Framework to guide the selection, implementation, and evaluation of evidence-based, culturally appropriate, sustainable prevention activities. In this framework, the strength of evidence is assessed using established scientific standards and criteria for applying those standards and comprises four major elements (SAMHSA, 2009):
1. Rigor of the evaluation design (e.g., use of appropriate intervention and control or other comparison groups, group assignment strategy, control of dosage and contextual factors that can provide an alternative explanation of the results or findings).
2. Rigor and appropriateness of the methods used to collect and analyze the data (e.g., use of appropriate data collection designs, use of measures that match outcomes targeted by the intervention, data collection without bias, and use of appropriate statistical tests).
3. The magnitude and consistency of the effects of the intervention on targeted outcomes.
4. The extent to which findings can be generalized to similar populations and settings.
Box 2-1 summarizes SAMHSA’s criteria for defining “evidence-based” as well as a set of guidelines for identifying and selecting evidence-based interventions (SAMHSA, 2009).
BOX 2-1
SAMHSA Criteria
A prevention intervention that is evidence-based meets at least one of the following three definitions:
1. Inclusion in federal registries of evidence-based interventions
2. Reported (with positive effects on the primary targeted outcome) in peer-reviewed journals
3. Documented effectiveness supported by other sources of information and the consensus judgment of informed experts, as described in the following guidelines, all of which must be met:
• Guideline 1: The intervention is based on a theory of change that is documented in a clear logic or conceptual model; and
• Guideline 2: The intervention is similar in content and structure to interventions that appear in registries and/or the peer-reviewed literature; and
• Guideline 3: The intervention is supported by documentation that it has been effectively implemented in the past, and multiple times, in a manner attentive to scientific standards of evidence and with results that show a consistent pattern of credible and positive effects; and
• Guideline 4: The intervention is reviewed and deemed appropriate by a panel of informed prevention experts that includes: well-qualified prevention researchers who are experienced in evaluating prevention interventions similar to those under review; local prevention practitioners; and key community leaders as appropriate, e.g., officials from law enforcement and education sectors or elders within indigenous cultures.
SOURCE: SAMHSA, 2009.
There are other generally accepted standards of evidence for effective prevention programs. In 2005, the Society for Prevention Research published a set of standards for identifying evidence-based programs (Flay et al., 2005). There are a total of 47 standards that are organized into 3 categories: efficacy, effectiveness, and dissemination.
Effective prevention services and programs, including those in the military, should be culturally competent by taking into account sociocultural factors, including aspects of military culture; racial, ethnic, and linguistic diversity; gender and sexual orientations; and health disabilities. Moreover, interventions should be developmentally appropriate and should reflect the life stage of the targeted population. Taking into account cultural and developmental considerations will improve the effectiveness of programs, policies, and practices selected for targeted populations (IOM, 2013c; SAMHSA, 2009).
In addition, effective prevention programs use varied methods of imparting knowledge and achieving behavior change. Active role playing or modeling, in which participants practice specific skills related to the prevention goal (e.g., communication skills for resisting drug use), is more likely to lead to behavior change than are passive learning methods. Furthermore, successful prevention programs are more likely to involve a sufficient intensity of activities (e.g., number, length, and duration of sessions). For a prevention program to be successful, these activities should be grounded in sound theory so that the outcomes are predictable, given the issues being addressed. A final characteristic of effective prevention programs is that they have a strong focus on fostering positive relationships, which serve as a powerful protective factor against psychological health problems (Nation et al., 2003).
There are a number of resources that are available to assist in the identification of evidence-based prevention programs; for example, the National Registry of Evidence-Based Programs and Practices (NREPP), a database maintained by SAMHSA of evidence-based mental health and substance abuse interventions. All programs in the publicly available database meet minimum requirements for review and have been independently assessed for quality of research and readiness for dissemination (SAMHSA, 2013b). Another resource is the National Institutes of Health and its work on prevention and implementation in mental health, which includes the National Institute of Mental Health’s Dissemination and Implementation research program, and the National Institute on Drug Abuse’s Prevention Research Branch (which has funded several military prevention studies).
It should be emphasized that if evidence-based interventions are to be broadly disseminated, they must be standardized, publicly available, and feasible to implement for target populations. Not all programs are equally ready for broad dissemination. The evolution from evidence generation to dissemination and implementation can take years. Examples of implementation frameworks and models to speed the development of evidence-based interventions and their ultimate transition into practice include the Research to Practice model and the Interactive Systems Framework developed by Centers for Disease Control and Prevention (Collins et al., 2012) and the pipeline framework of the Department of Veterans Affairs’ Quality Enhancement Research Initiative (Stetler et al., 2008).
As discussed further in Chapter 5, effective prevention programs must, in addition to being ready for dissemination, pay attention to organizational and community engagement, provide for regular evaluations of program quality and fidelity, and have a strategy in place for maintaining sustainability.
MULTI-LEVEL PREVENTION AND THE SOCIAL ECOLOGICAL MODEL
To be effective at addressing psychological health outcomes, prevention strategies need to be sufficiently comprehensive. The best approaches consider risk and protective factors across multiple determinants of health (Conyne, 2013). The central role of the family and community in the promotion and protection of good psychological health suggests that a multilevel conceptualization of determinants is appropriate. Based on Bronfenbrenner’s ecological systems theory (Bronfenbrenner, 1979), the ecological model (see Figure 2-1) recognizes multiple levels of influence, including the individual, interpersonal, institutional, community, and society, and therefore promotes targeting multiple levels to prevent negative outcomes. This model is particularly appropriate when considering military prevention programs because of the highly structured work and social life of military personnel and their families. Both active-duty military personnel and reserve component members who are activated live and work in tight social groups with many shared norms and values, with clear regulations governing behavior, and with clearly defined junior and senior leaders.
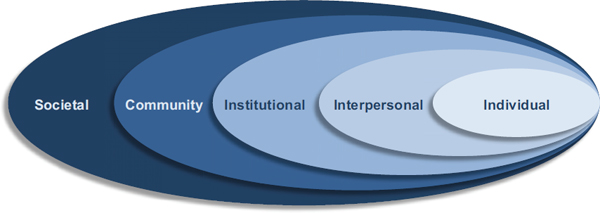
FIGURE 2-1 The ecological model.
In this context individual level influences are personal risk or protective factors that increase or decrease the likelihood of military personnel encountering psychological health problems. Examples include practices conducive of positive mental health attitudes and beliefs (e.g., look out for your buddy) or a personal history of witnessing or experiencing family violence. Prevention effects at the individual level aim to change individual-level risk factors. Mentoring would be one example of a specific individual approach.
Interpersonal- or relationship-level influences are factors that increase risk or are protective and that can be attributed to interactions with family, partners, and peers. Prevention strategies that address these influences include the promotion of good communication skills in marital relationships and learning to reflect on one’s own experiences and how they influence parenting practices. The social circle of active-duty military personnel can be considered to include members of one’s family, neighborhood, platoon, and company.
Institutional-level influences are factors that increase risk or protect based on formal and informal organizations or social environments. The institutional level for military personnel would include a service member’s junior and senior leaders, the battalion, the brigade, and the individual service (e.g., Army) or, in the case of National Guard members, the state, which issues specific instructions, policies, and regulations. The military unit is a social unit (composed of peers and friends) and also provides an institutional climate that can support healthy
relationships based on mutual support and trust or that can increase risks to personal safety if there is lack of discipline or a climate of harassment, hazing, bullying, or permissiveness toward sexual assault.
Community-level influences are factors that can increase risk through social norms that do not promote good health (such as the acceptance or encouragement of heavy drinking or other risky behavior). The community level can be defined geographically (such as a neighborhood) or by membership in a group. The community level for military personnel would include the individual service, one’s membership in the group of enlisted personnel or officers, and groups defined by other distinguishing aspects of military culture. Community features and norms concerning where service members and their families live or return to can shape the risk and protective factors that affect individual behaviors and outcomes. General population studies have previously examined the role of the community in psychological health (see, for example, Gottlieb et al., 2011; Holder et al., 2000; Pronyk et al., 2006; and Trickett, 2009).
Societal-level influences are the large, macro-level factors that influence psychological health, such as gender inequality, societal norms, policies, and regulations. A no-tolerance policy for sexual violence or assault would be one example of a societal influence.
APPLICATION OF PREVENTION FRAMEWORK TO PSYCHOLOGICAL HEALTH FOR MILITARY MEMBERS AND THEIR FAMILIES
This section discusses the committee’s prevention model defined above and how it applies to psychological health in the military. Nash (2011) recognized that psychological health protection, including combat and operational stress control,1 can be considered one approach to psychological health protection. For example, the overlap between PTSD and mild traumatic brain injury is high (Kennedy et al., 2007) and argues for adopting similar approaches to recognizing and managing these two separate but related health problems. Nash and colleagues (2010) adopted a framework for defining the scope of stress outcomes and for promoting military mental health prevention based on the IOM model for classifying the spectrum of interventions for psychological disorders, which is summarized in the IOM “protractor” (IOM, 1994) shown in Figure 2-2.
____________________
1 Programs developed and actions taken by military leadership to prevent, identify, and manage adverse combat and operational stress reactions in units; to enhance mission performance; to increase individual and unit resilience; to conserve fighting strength; to prevent or minimize the adverse effects of combat stress on members’ physical, psychological, behavioral, and social health; and to return the unit or service member to duty.
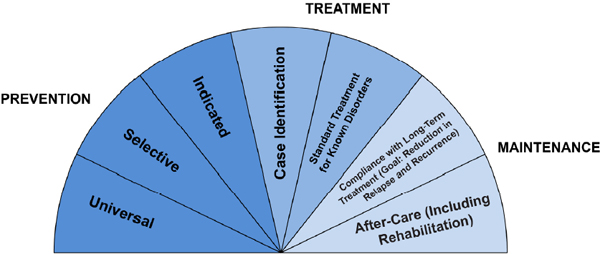
FIGURE 2-2 Intervention spectrum for psychological disorders.
SOURCE: IOM, 1994.
This model, which reflects Gordon’s prevention model, described previously, and is directly relevant for promoting psychological health in the military, follows from an examination of the relationship and boundaries between the promotion of psychological health and clinical treatment. The model recognizes that prevention is part of a continuum, along with treatment and rehabilitation interventions, and it recommends reserving the term “prevention” for interventions that occur before the onset of a full clinical disorder, or “case identification.” Central to this approach is a focus on preventive strategies that support the early identification of risk and the inclusion of targeted and indicated preventive interventions. For example, the recognition of increased depressive or posttraumatic stress symptoms2 through embedded primary care screening or leadership training can facilitate the timely delivery of indicated preventive interventions in order to reduce the onset of psychological disorders. Notably, preventive interventions may also be relevant to the continuum of treatment and rehabilitation interventions when addressing individuals or systems at risk due to the presence of illness or injury, such as children or spouses of service members or veterans with PTSD or physical injuries.
As discussed in Nash et al. (2010), the IOM prevention nomenclature discriminates between selective interventions offered to at-risk persons regardless of symptom status, such as battlemind debriefing3 for a company recently exposed to a potentially traumatic event such as mines and sniper fire, and indicated interventions offered only to persons identified as significantly symptomatic and therefore at increased risk. A review of theoretic constructs and empirical data informing efforts to prevent PTSD concluded that the most promising prevention interventions were those that were indicated based on identified symptom burden rather than merely selective based on stressors (Feldner et al., 2007).
The IOM model suggests that the military can promote more effective prevention interventions by defining the early subclinical states that confer the greatest risk for either failure of role performance or future psychological health disorders and by identifying the moderators
____________________
2 Acute stress reaction and acute stress disorder are subthreshold or preclinical posttraumatic states that are targets for early intervention to prevent the onset of PTSD. See Nash and Watson (2012) for a discussion about the spectrum of posttraumatic stress states. See the section on PTSD in Chapter 4, for a summary of research on interventions designed prevent PTSD.
3 Unlike other types of psychological debriefing, battlemind debriefing minimizes the degree to which traumatic events are recounted in order to avoid re-traumatization (Adler et al., 2009). For more on battlemind debriefing, see Chapter 4.
and mediators that can best be manipulated to reduce that risk. A significant obstacle to applying this standard to operational stress research and surveillance is the lack, in our present state of knowledge, of well-defined and validated categories, dimensions, and instruments to identify preclinical operational stress cases (Nash et al., 2010). The IOM model, taken together with the report of the Defense Health Board Mental Health Task Force (DOD, 2007), suggests the following aims of operational stress research and surveillance, in the service of which concepts should be developed and metrics defined:
• To promote the identification of at-risk populations based on stressor exposures as well as on other preexisting or concurrent factors, so that selective interventions can appropriately be offered to them.
• To promote the identification of persons with preclinical symptoms and/or concurrent elevated risk factors (e.g., a history of prior PTSD in a combat exposed service member) for whom indicated prevention interventions might most usefully be offered.
• To define “cases” of preclinical operational stress based on sound conceptual reasoning and empirical support.
• To identify biological, psychological, and behavioral markers of cases of preclinical operational stress.
• To better understand the natural history of operational stress outcome trajectories, ranging from preclinical distress or dysfunction in the immediate aftermath of a highintensity event to entrenched clinical mental disorders months or years later.
• To better understand the risk and resilience factors that mediate between stress exposures and outcomes at every point in individual stress trajectories over time.
• To evaluate outcomes of conceptually sound indicated biopsycho-social-spiritual interventions for preclinical operational stress based on uniformly applied case definition exposure regardless of symptoms.
PREVENTION WITHIN THE PHASES OF MILITARY EXPERIENCE
Different service branches use different terminology for the various phases of military life or have a different number of phases, or both, but regardless of the specific terminology, every service member goes through the same general process. Figure 2-3 illustrates the major phases of the military experience. The phases of the cycle are similar for National Guard and reserve service members, but some differences exist, such as the mobilization and demobilization processes that occur in, respectively, the pre-deployment and the post-deployment phases.
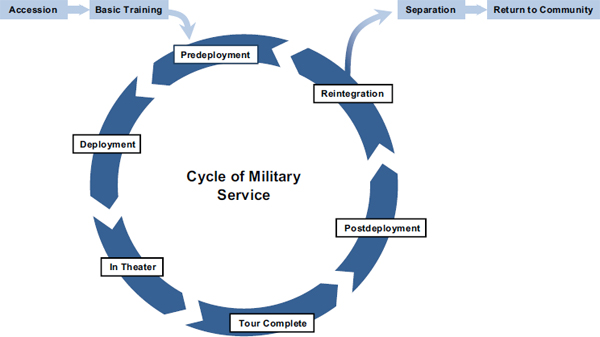
FIGURE 2-3 Phases of the military experience.
With the increased deployments and shorter dwell times that have characterized the wars in Iraq and Afghanistan, many service members experience the phases of pre-deployment, deployment, post-deployment, and reintegration multiple times. As discussed throughout this report, these phases in military life each present opportunities for identifying individuals at risk and for providing various individual- and system-level interventions.
MEASUREMENT OF PREVENTION PROGRAMS
Measurement is essential to any organizational efforts that aim to improve health, wellbeing, and resilience. Measurement implies the tracking of data that are essential for running a program effectively (IOM, 2013a). The committee was asked to identify the best performance measures for evaluating DOD resilience and prevention programs addressing psychological health. In its deliberations, the committee concluded that an organizing framework would help provide a structure for decision making about what is important to measure in a systematic assessment of resilience and prevention programs. Such a framework can guide DOD assessment of existing programs and the development of future prevention strategies for military populations and their families.
The committee’s model incorporates three frameworks relevant to effective measurement of prevention programs in the area of psychological health: the Donabedian paradigm for assessing quality of care, the National Behavioral Health Quality Framework, and the National Quality Forum criteria. The committee also considered the utility of the Porter model, as directed by the statement of task.
The Donabedian Paradigm
Donabedian’s (2005) classic paradigm for assessing the quality of care is based on a three-component approach focusing on structure, process, and outcome (see Figure 2-4). Donabedian’s model proposes that each component has a direct influence on the next, as represented by the arrows in the following schematic (Donabedian, 2005).

FIGURE 2-4 Donabedian paradigm.
“Structure” refers to the attributes of the settings in which providers deliver care or services, including material resources (e.g., electronic health records), human resources (e.g., staff expertise), and organizational structure (e.g., hospitals versus clinics). The premise is that the setting can be a strong determinant of care quality and that given the proper system, good care will follow. For example, one would expect care to be of higher quality when providers and staff are trained in applying evidence-based prevention interventions and competencies are assessed.
“Process” refers to the care and services that are delivered and received. This can include anything that is done as part of the encounter between an individual and the delivery system, including interpersonal processes such as providing information and emotional support as well as involving individuals in decisions in a way that is consistent with their preferences. Process measures assess the care and service that an individual received and the fidelity with which it was delivered.
“Outcome” refers to how an individual’s health status is affected by contact with an intervention (e.g., reduced problem drinking following exposure to an alcohol education intervention). There are both proximal outcomes (i.e., short-term consequences) and distal outcomes (long-term consequences); an example would be an individual quitting abusive drinking (a proximal outcome), which could eventually translate into less spouse and child abuse and possibly a longer life (distal outcomes).
National Behavioral Health Quality Framework4
The National Behavioral Health Quality Framework (NBHQF), which was developed by SAMHSA, is a guiding framework for the identification and implementation of key psychological health quality measures. The NBHQF provides a mechanism to examine and prioritize quality prevention, treatment, and recovery elements at various levels of the health system (i.e., payer/system/plan, provider/practitioner, and patient/population levels). The NBHQF defines the six goals as follows (SAMHSA, 2013a):
1. Effective—Promote the most effective prevention, treatment, and recovery practices for behavioral health disorders
2. Person centered—Ensure that behavioral health care is person, family, and community centered
3. Coordinated—Encourage effective coordination within behavioral health care and between behavioral health care and community-based primary care providers and other health care, recovery, and social support services
4. Healthy living—Assist communities to use best practices to enable healthy living
____________________
4 By behavioral health, SAMHSA refers to a state of mental/emotional well-being and/or actions that affect wellness. Behavioral health problems include substance use disorders; alcohol and drug addiction; and serious psychological distress, suicide, and mental disorders. See the previous section on terminology for more details on SAMSHSA’s definition and the use of related terms in this report.
5. Safe—Make behavioral health care safer by reducing harm caused in the delivery of care
6. Affordable/accessible—Foster affordable high-quality behavioral health care for individuals, families, employers, and governments by developing and advancing new and recovery-oriented delivery models
In the NBHQF, prevention and wellness are often captured as population-level measures. The NBHQF is aligned with the three aims of the National Quality Strategy5 developed by the Department of Health and Human Services (HHS): better care for individuals, better health for populations, and reduced expenditures. Similarly, DOD has its version of a strategic framework for improving the military health system (MHS) called the Quadruple Aim, which includes a component addressing readiness. The MHS Quadruple Aim is as follows (DOD, 2013):
1. Increased readiness—Ensuring that the total military force is medically ready to deploy and that the medical force is ready to deliver health care anytime, anywhere in support of the full range of military operations, including humanitarian missions.
2. Better health—Reducing the generators of ill health by encouraging healthy behaviors and decreasing the likelihood of illness through focused prevention and the development of increased resilience.
3. Better care—Providing a care experience that is patient and family centered, compassionate, convenient, equitable, safe, and always of the highest quality.
4. Lower cost—Creating value by focusing on quality, eliminating waste, and reducing unwarranted variation; considering the total cost of care over time, not just the cost of an individual health care activity.
Population health is the focus of the initiatives and metrics associated with the better health aim.
National Quality Forum
The committee was asked to use the National Quality Forum (NQF) framework to identify the best metrics for evaluating DOD prevention and resilience efforts. NQF is a private, nonprofit organization that endorses performance measures designed to evaluate the quality of health care in the United States.6 The evaluation framework refers to a set of standardized criteria that NQF uses to determine whether a measure is suitable for endorsement. For a particular performance measure to be endorsed by NQF, it must meet all five criteria that NQF has established:
1. Importance to measure and report: the extent to which the specific performance measure is evidence-based and is important to making concrete gains in the quality of health care and to improving health outcomes for high-impact aspects of health care.
2. Scientific acceptability of measure properties: the extent to which the performance measure produces consistent (reliable) and credible (valid) results about the quality of care
____________________
5 The National Quality Strategy is an element of the Affordable Care Act and offers a roadmap for improving the delivery of health care services, patient health outcomes, and population health.
6 NQF’s membership consists of a wide variety of stakeholders, including consumer organizations, public and private purchasers, physicians, nurses, hospitals, accrediting and certifying bodies, supporting industries, and health care research and quality-improvement organizations.
3. Feasibility: data elements that are readily available or can be collected without undue burden.
4. Usability and use: the extent to which potential audiences (e.g., consumers, purchasers, providers, or policy makers) are using or could use performance results for both accountability and performance improvement.
5. Comparison to related or competing measures: where a measure meets the above criteria and there are related measures or competing measures, the measures are compared to address harmonization or selection of the best measure.
Although NQF-endorsed performance measures are widely used in public-reporting, quality-improvement, and payment programs, the committee determined that the endorsed measures have significant limitations when it comes to assessing psychological health prevention and resilience programs. The NQF model of measurement is based on standards of clinical care that are promulgated by clinical guidelines. Therefore, the endorsed measures are clinically focused and primarily designed to improve the quality of care delivered to patients as part of a health care system or in inpatient or ambulatory settings. They do not address non-clinical prevention interventions such as campaigns, mentoring programs, or educational workshops. In addition, of the more than 700 measures that NQF has endorsed, only a small proportion—approximately 45—are measures related to psychological health (NQF, 2013). Few if any address the areas of child psychological health, family adaptive functioning, coping (individual and family), and individual positive functioning. Chapter 5 presents the committee’s review of NQF-endorsed measures.
The Porter Model
In addition to identifying the best metrics for resilience and prevention programs, the committee was asked to consider the potential utility of the Porter model and the psychological outpatient clinical pathway for PTSD among service members. The Porter model (Kaplan and Porter, 2011) is an approach for measuring value in health care developed by Michael Porter and his colleagues. The model measures health care costs at the level of the individual patient with a given medical condition over a full cycle of care and compares those costs to outcomes. On the basis of its review of the literature about Porter’s value model (Kaplan and Porter, 2011; Porter, 2008, 2010; Porter et al., 2013), the committee concluded that the framework is applicable to the treatment pathways; however, it is not an appropriate model for assessing the value of prevention interventions. Furthermore, the feasibility of this task is impeded by the lack of sufficient evidence surrounding current PTSD- and resilience-related programs and the outcomes on psychological health. For those reasons, the committee did not include the Porter model in its recommendations.
A previous IOM committee examined frameworks for assessing the value of communitybased, non-clinical interventions reaching individuals at all risk levels. For the assessment of value, that committee recommended a framework that proposes comprehensive consideration of benefits and harms in the context of health, community well-being, and community process as well as an inclusive and comprehensive consideration of the resources used (IOM, 2012). That model is consistent with this committee’s emphasis on the importance of social determinants of health.
MODEL FOR PREVENTION PROGRAM DEVELOPMENT AND MEASUREMENT
Figure 2-5 shows a model that the committee developed to organize the various concepts related to prevention program development and measurement that have been discussed in this chapter, including evidence-based prevention, types of prevention interventions, the socioecological model, and performance measures. The model is not intended to capture all of the complex pathways that characterize program development and measurement. Instead, the model serves as a general guide for thinking about the complex process of identifying the best metrics for assessing DOD prevention programs. In Chapter 5 the committee refers to this model when it considers what DOD should measure in assessing its resilience and prevention programs.
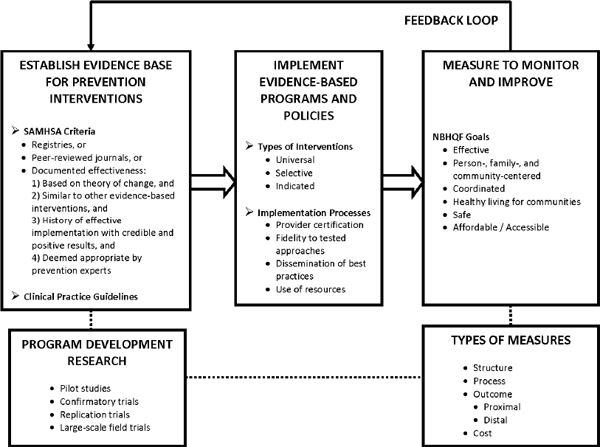
FIGURE 2-5 Model for prevention program development and measurement.
NOTE: SAMHSA is the Substance Abuse and Mental Health Services Administration.
The box in the figure labeled “Establish Evidence Base for Prevention Interventions” indicates that empirical evidence for the intervention of interest is foundational to implementation. Recommendations for the identification and selection of evidence-based prevention interventions are embodied in the SAMHSA criteria (see Box 2-1 for details) as well as in clinical practice guidelines, which serve as a standard for identifying clinically-based practices, such as screening. A dotted line leads from this box to the “Program Development Research” box, which identifies the types of research studies for evaluating the intervention and collecting the evidence necessary to demonstrate the efficacy and effectiveness of interventions. As illustrated by the box labeled “Types of Measures,” evaluation measures can include a mix of structure, process, outcome, and cost measures.
The box labeled “Implement Evidence-Based Programs and Policies” represents the process of using evidence to implement various types of prevention strategies—universal, selective, and indicated—that focus on the characteristics of the intended audience. Translating
evidence into a successful prevention program requires paying attention to myriad implementation processes that ensure the integrity, fidelity, and cost-effectiveness of the program; see Chapter 5 for a discussion of implementation processes.
The box labeled “Measure to Monitor and Improve” lists opportunities to measure various dimensions of program performance. The committee chose the six domains of SAMHSA’s NBHQF as a starting point because the framework specifically addresses psychological health and is consistent with the measurement priorities set by other federal agencies (e.g., HHS and DOD), research entities (e.g., IOM), and influential professional organizations (e.g., Institute for Health Improvement). The NBHQF domains for measurement emphasize prevention that is effective (based on evidence); that is person, family, and community centered; coordinated; that enables healthy living; that is safe (reduces harm caused in the delivery of care); and that uses affordable and accessible delivery models. As illustrated by the dotted line leading to “Types of Measures,” program performance can be assessed using structure, process, outcome, and cost measures. Robust measures meet methodological standards to ensure valid and reliable measurement, such as the criteria defined by NQF that are discussed above.
The feedback loop in the diagram represents the cycle of using measurement results to continuously inform the evidence base and to improve program implementation.
This chapter lays the groundwork for concepts discussed in later chapters of the report. Believing that prevention should address both risk reduction and health promotion, the committee sees “psychological health” as serving as the foundation for overall health and wellness and as being protective against the development of mental illness and substance use disorders. Prevention is a set of strategies, complementary to treatment, aimed at achieving a state of good psychological health, particularly in the context of population mental health. The committee has adopted a conceptual approach that emphasizes that these risk and protective factors may exert influence at multiple levels (individual, family, community, institution) and also may have influence across the boundaries of specific conditions, essentially at the preclinical level.
Prevention interventions should rest on sound conceptual and empirical foundations and should be rigorously designed and evaluated. To be effective at addressing psychological health outcomes, prevention strategies need to be sufficiently comprehensive. The best approaches consider risk and protective factors across multiple determinants of health. There are many distinct phases of military life, and these phases present opportunities for identifying individuals at risk and for providing various individual- and system-level interventions.
On the basis of its review of various models for assessing the effectiveness and performance of prevention programs, the committee found that Porter’s value model is applicable to the treatment pathways; however, it is not an appropriate model for assessing the value of prevention interventions. The committee concluded that an organizing framework would help provide a structure for decision making about what is important to measure in a systematic assessment of resilience and prevention programs. Such a framework can guide DOD’s
assessment of existing programs and the development of future prevention strategies for military populations and their families.
Adler, A. B., P. D. Bliese, D. McGurk, C. W. Hoge, and C. A. Castro. 2009. Battlemind debriefing and battlemind training as early interventions with soldiers returning from Iraq: Randomization by platoon. Journal of Consulting and Clinical Psychology 77(5):928–940.
APA (American Psychological Association). 2013. Psychology is a Behavioral and Mental Health Profession. http://www.apa.org/about/gr/issues/health-care/profession.aspx (accessed December 17, 2013).
Bates, M. J., S. Bowles, J. Hammermeister, C. Stokes, E. Pinder, M. Moore, M. Fritts, M. Vythilingam, T. Yosick, J. Rhodes, C. Myatt, R. Westphal, D. Fautua, P. Hammer, and G. Burbelo. 2010. Psychological fitness. Military Medicine 175(8):21–38.
Bronfenbrenner, U. 1979. The Ecology of Human Development: Experiments by Nature and Design. Cambridge, MA: Harvard University Press.
Caplan, G. 1964. Principles of Preventive Psychiatry. Oxford, England: Basic Books.
Collins, C. B., Jr., A. E. Edwards, P. L. Jones, L. Kay, P. J. Cox, and R. W. Puddy. 2012. A comparison of the Interactive Systems Framework (ISF) for Dissemination and Implementation and the CDC Division of HIV/AIDS prevention’s Research-to-Practice model for behavioral interventions. American Journal of Community Psychology 50(3-4):518–529.
Conyne, R. K. 2013. Program Development and Evaluation in Prevention. Los Angeles: Sage.
Cowen, E. L. 1977. Baby-steps toward primary prevention. American Journal of Community Psychology 5(1):1–22.
———. 1980. The wooing of primary prevention. American Journal of Community Psychology 8(3):258–284.
DOD (Department of Defense). 2007. An Achievable Vision: Report of the Department of Defense Task Force on Mental Health. Falls Church, VA: Defense Health Board Task Force on Mental Health.
———. 2013. Evaluation of the TRICARE Program: Access, Cost, and Quality. Fiscal Year 2013 Report to Congress. Washington, DC: Department of Defense.
Donabedian, A. 2005. Evaluating the quality of medical care. 1966. Milbank Quarterly 83(4):691–729.
Feldner, M. T., C. M. Monson, and M. J. Friedman. 2007. A critical analysis of approaches to targeted PTSD prevention: Current status and theoretically derived future directions. Behavior Modification 31(1):80–116.
Gordon, R. S., Jr. 1983. An operational classification of disease prevention. Public Health Reports 98(2):107–109.
Gottlieb, L., H. Waitzkin, and J. Miranda. 2011. Depressive symptoms and their social contexts: A qualitative systematic literature review of contextual interventions. International Journal of Social Psychiatry 57(4):402–417.
Hage, S., and J. L. Romano. 2013. Best Practices in Prevention. Thousand Oaks, CA: Sage Publishing.
Holder, H. D., P. J. Gruenewald, W. R. Ponicki, A. J. Treno, J. W. Grube, R. F. Saltz, R. B. Voas, R. Reynolds, J. Davis, L. Sanchez, G. Gaumont, and P. Roeper. 2000. Effect of community-based interventions on high-risk drinking and alcohol-related injuries. JAMA 284(18):2341–2347.
IOM (Institute of Medicine). 1994. Reducing Risks for Mental Disorders: Frontiers for Preventive Intervention Research. Washington, DC: National Academy Press.
———. 2009. Preventing Mental, Emotional, and Behavioral Disorders Among Young People: Progress and Possibilities. Washington, DC: The National Academies Press.
———. 2012. An Integrated Framework for Assessing the Value of Community-Based Prevention. Washington, DC: The National Academies Press.
———. 2013a. A Ready and Resilient Workforce for the Department of Homeland Security: Protecting America’s Front Line. Washington, DC: The National Academies Press.
———. 2013b. Returning Home from Iraq and Afghanistan: Assessment of Readjustment Needs of Veterans, Service Members, and Their Families. Washington, DC: The National Academies Press.
———. 2013c. Substance Use Disorders in the U.S. Armed Forces. Washington, DC: The National Academies Press.
Jahoda, M. 1958. Current Concepts of Positive Mental Health. New York: Basic Books.
Jonas, W. B., F. G. O’Connor, P. Deuster, J. Peck, C. Shake, and S. S. Frost. 2010. Why total force fitness? Military Medicine 175(8):6–13.
Kaplan, R. S., and M. E. Porter. 2011. The big idea: How to solve the cost crisis in health care. Harvard Business Review 89(9).
Kennedy, J. E., M. S. Jaffee, G. A. Leskin, J. W. Stokes, F. O. Leal, and P. J. Fitzpatrick. 2007. Posttraumatic stress disorder and posttraumatic stress disorder-like symptoms and mild traumatic brain injury. Journal of Rehabilitation Research and Development 44(7):895–920.
Kindig, D. A. 2011. Unpacking the Triple Aim Model. http://www.improvingpopulationhealth.org/blog/2011/01/unpacking_triple_aim.html (accessed November 12, 2013).
Kindig, D., and G. Stoddart. 2003. What is population health? American Journal of Public Health 93(3):380–383.
Lester, P., and L. C. E. Flake. 2013. How wartime military service affects children and families. The Future of Children 23(2):121–141.
Nash, W. P. 2011. U.S. Marine Corps and Navy combat and operational stress continuum model: A tool for leaders. In Combat and Operational Behavioral Health, edited by E. C. Ritchie. Washington, DC: Department of the Army. Pp. 107–120.
Nash, W. P., and P. J. Watson. 2012. Review of VA/DOD clinical practice guideline on management of acute stress and interventions to prevent posttraumatic stress disorder. Journal of Rehabilitative Research and Development 49(5):637–648.
Nash, W. P., J. Vasterling, L. Ewing-Cobbs, S. Horn, T. Gaskin, J. Golden, W. T. Riley, S. V. Bowles, J. Favret, P. Lester, R. Koffman, L. C. Farnsworth, and D. G. Baker. 2010. Consensus recommendations for common data elements for operational stress research and surveillance: Report of a federal interagency working group. Archives of Physical Medicine and Rehabilitation 91(11):1673–1683.
Nation, M., C. Crusto, A. Wandersman, K. L. Kumpfer, D. Seybolt, E. Morrissey-Kane, and K. Davino. 2003. What works in prevention. Principles of effective prevention programs. American Psychologist 58(6–7):449–456.
NQF (National Quality Forum). 2013. Behavioral Health Measures, Phases I and II. http://www.qualityforum.org/Projects/Behavioral_Health_Phase_1_and_2.aspx (accessed November 13, 2013).
Participants at the 6th Global Conference on Health Promotion. 2005. The Bangkok Charter for Health Promotion in a Globalized World. Geneva: World Health Organization.
Porter, M. E. 2008. Value-based health care delivery. Annals of Surgery 248(4):503–509.
———. 2010. What is value in health care? New England Journal of Medicine 363(26):2477–2481.
Porter, M. E., E. A. Pabo, and T. H. Lee. 2013. Redesigning primary care: A strategic vision to improve value by organizing around patients’ needs. Health Affairs 32(3):516–525.
Pronyk, P. M., J. R. Hargreaves, J. C. Kim, L. A. Morison, G. Phetla, C. Watts, J. Busza, and J. D. Porter. 2006. Effect of a structural intervention for the prevention of intimate-partner violence and HIV in rural South Africa: A cluster randomised trial. Lancet 368(9551):1973–1983.
SAMHSA (Substance Abuse and Mental Health Services Administration). 2009. Identifying and Selecting Evidence-Based Interventions. Rockville, MD: U.S. Department of Health and Human Services.
———. 2013a. National Behavioral Health Quality Framework (Draft). Rockville, MD: SAMHSA.
———. 2013b. SAMHSA’s National Registry of Evidence-Based Programs and Practices. http://nrepp.samhsa.gov/Index.aspx (accessed October 18, 2013).
Stetler, C. B., B. S. Mittman, and J. Francis. 2008. Overview of the VA Quality Enhancement Research Initiative (QUERI) and QUERI theme articles: QUERI series. Implementation Science 3:8.
Tanielian, T., R. Ramchand, M. P. Fisher, and C. S. Sims. 2013. Military Caregivers: Cornerstones of Support for Our Nation’s Wounded, Ill, and Injured Veterans. Santa Monica, CA: RAND Corporation.
Trickett, E. J. 2009. Community psychology: Individuals and interventions in community context. Annual Review of Psychology 60:395–419.
WHO (World Health Organization). 2002. Prevention and Promotion in Mental Health. Geneva: World Health Organization.
This page intentionally left blank.




















