1
Introduction, Background, and Overview of the Workshop1
Being able to communicate is a cornerstone of healthy aging. People need to make themselves understood and to understand others to remain cognitively and socially engaged with families, friends, and other individuals. When they are unable to communicate, people with hearing impairments can become socially isolated, and social isolation can be an important driver of morbidity and mortality in older adults (Cacioppo et al., 2011).
Despite the critical importance of communication, many older adults have hearing loss that interferes with their social interactions and enjoyment of life. This hearing loss is often subtle (Lin, 2012). People may turn up the volume on their televisions or stereos, miss words in a conversation, go to fewer public places where it is difficult to hear, or worry about missing an alarm or notification. In other cases, hearing loss is much more severe, and people may retreat into a hard-to-reach shell. Yet fewer than one in seven older Americans with hearing loss use hearing aids, despite rapidly advancing technologies and innovative approaches to hearing health care (Chien and Lin, 2012). In addition, there may not be an adequate number of professionals trained to address the growing need for hearing health care for older adults. Further, Medicare does not cover “routine hearing exams,
____________________
1 The planning committee’s role was limited to planning the workshop, and the workshop summary has been prepared by the workshop rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants, and are not necessarily endorsed or verified by the Institute of Medicine or the National Research Council, and they should not be construed as reflecting any group consensus.
BOX 1-1
Statement of Task
An ad hoc planning committee will plan and conduct a 2-day public workshop to examine the ways in which age-related hearing loss affects healthy aging, and how the spectrum of public and private stakeholders can work together to address hearing loss in older adults as a public health issue. The workshop will feature invited presentations and discussions that will:
- Describe and characterize the public health significance of hearing loss and the relationship between hearing loss and healthy aging (e.g., medical comorbidities);
- Examine and explore current and future areas of research on hearing loss and healthy aging;
- Discuss comprehensive hearing rehabilitative strategies, including innovative models of care;
- Explore innovative hearing technologies, as well as barriers to their development and use; and
- Consider and discuss short- and long-term collaborative strategies, including public-private partnerships, for approaching age-related hearing loss as a public health priority, for example, developing preventive intervention strategies; improving public awareness; and enhancing professional education.
hearing aids, or exams for fitting hearing aids” (CMS, 2014), which can be prohibitively expensive for many older adults.
The Forum on Aging, Disability, and Independence2 was created by the Institute of Medicine (IOM) in collaboration with the National Research Council (NRC) in 2012 to provide an ongoing, neutral venue where stakeholders in government, academia, industry, foundations, and consumer groups can come together to discuss issues at the intersection of aging and disability. On January 13–14, 2014, the forum held a workshop on age-related hearing loss that brought together more than one hundred researchers, advocates, policy makers, entrepreneurs, regulators, and others to discuss this pressing social and public health issue. The statement of task for the workshop is listed in Box 1-1. A webcast of the workshop is also available.3
____________________
2 See www.iom.edu/ADIForum (accessed February 24, 2014).
3 See http://www.iom.edu/Activities/PublicHealth/HearingLossAging/2014-JAN-13.aspx (accessed February 25, 2014).
Frank R. Lin Johns Hopkins University
In the initial session of the workshop, workshop planning committee co-chair Frank Lin, assistant professor of otolaryngology, geriatric medicine, mental health, and epidemiology at the Johns Hopkins University School of Medicine and the Bloomberg School of Public Health, provided background information on age-related hearing loss in the United States and around the world. The prevalence of hearing loss essentially doubles with each decade of age (see Figure 1-1). As a result, nearly two of three Americans ages 70 and above have a clinically meaningful hearing impairment.
The use of hearing aids, in contrast, is “phenomenally low,” said Lin (see Figure 1-2). Only about 15 percent of people with a hearing impairment in the United States use a hearing aid. Lin noted that the rate is only a little higher in England and Wales (about 17 percent) even though hearing aids are fully covered by national health insurance there. Furthermore, the prevalence of hearing aid use has not changed substantially for decades in the United States or around the world, Lin said.
A fundamental paradox surrounds hearing loss and the use of hearing
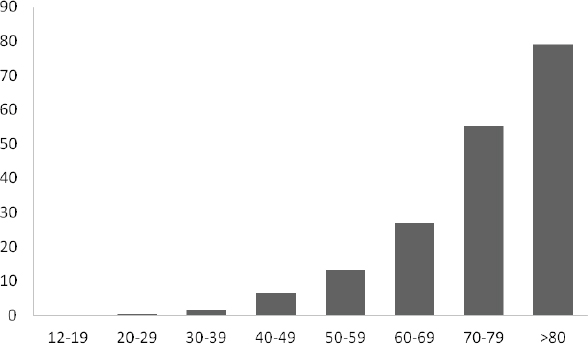
FIGURE 1-1 Prevalence percentage of bilateral hearing loss in the United States by age.
SOURCE: Data from Lin et al., 2011a.
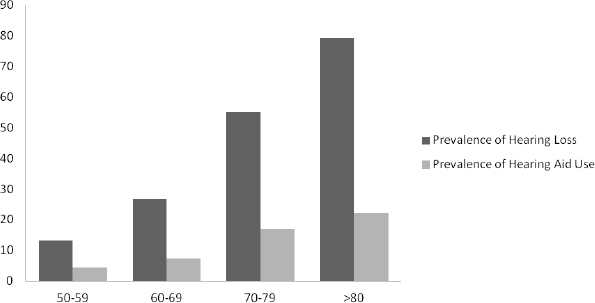
FIGURE 1-2 Prevalence percentage of hearing loss and hearing aid use in the United States by age.
SOURCE: Data from Chien and Lin, 2012.
aids, Lin pointed out. A hearing impairment that would be treated as a serious health issue in a 12-year-old boy is typically met with a shrug in a 72-year-old man. Yet both have a need to communicate with friends, family members, and others to function well in society.
Hearing depends on two basic processes: the peripheral transduction of sound by the cochlea and the central processing or decoding of sound by the brain. Auditory functioning can be measured at multiple levels and in multiple ways, including otoacoustic emissions testing; pure tone audiometry; speech discrimination scores; central auditory measures such as speech in noise and dichotic listening; and subjective hearing and communicative function. These different measures depend both on peripheral inputs or bottom-up processing and on central processing or top-down processing.
Hearing loss often reflects impairments in cochlear functioning that can be assessed with audiometry. For example, an audiogram can be used to calculate the pure-tone average hearing level in decibels (dB) at mid-level frequencies. The cochlea is made up of many cells that cannot regenerate and over time can be damaged by aging, noise, medicines, or other factors. Damage to the cochlea can lead not only to decreased hearing sensitivity but also to poor frequency and temporal encoding of sound. Instead of sending a crisply encoded signal to the brain, the cochlea produces a garbled signal. As Lin described it, people tend to say, “It isn’t that I can’t hear you. It’s that I can’t understand you. It sounds like you are mumbling at me all the time.” People can still hear what someone is saying if they make an effort, but they have to concentrate much harder to make out what is being said.
Hearing deficits can be associated with other forms of physical and cognitive decline, Lin observed. A fundamental question that remains unanswered is whether and how hearing loss is related to these other negative health outcomes. Do they have common causes in pathological processes, or is hearing loss a modifiable risk factor of declines in physical and cognitive functioning?
Over the course of the workshop, Lin identified several prominent themes that emerged from the presentations of individual speakers. These themes should not be seen as the conclusions or recommendations of the workshop, but they are presented here to introduce the wide range of topics discussed during the meeting as observed by Lin.
The Links to Healthy Aging
Hearing loss is often treated as an unavoidable and relatively unimportant consequence of aging, yet it clearly contributes to a variety of physical, cognitive, and psychosocial problems. Presently, age-related hearing loss is poorly understood and often stigmatized, not only among patients and consumers but also among the research community and providers, said Lin. Technology and models of care are not meeting the needs of many individuals.
Deficits in Hearing Health Care
According to Lin, hearing health care is fragmented, expensive, and often inadequate. The hearing health care workforce includes not just physicians but also audiologists, hearing aid dispensers, community health workers, and others. Although united by the underlying problem of hearing loss, each group has its own interests and approaches. In addition, third-party reimbursement in the United States for hearing products and services is generally spotty or nonexistent.
The Rapidly Changing State of Hearing Technologies
Although hearing aids, cochlear implants, assistive listening devices, and other technologies have made great advances in recent years, Lin noted, they still fail to meet the needs of many older adults with hearing loss, such as extracting a voice from a noisy environment. At the same time, technology is continuing to advance rapidly, and newer devices, such as hearing
loops in public spaces and hearing applications built into smartphones, have tremendous potential to help people hear better.
The Potential for Innovative Approaches
New ways of delivering care and raising awareness of age-related hearing loss could yield major steps forward, stated Lin. Higher levels of screening, enhanced education and counseling, rehabilitation strategies, greater use of community health workers, and outreach campaigns to both the hearing-impaired and general populations could greatly expand the visibility of the issue and the efforts being made to counter hearing loss.
Research Gaps
Lin concluded that much remains unknown about age-related hearing loss, including the relationship between hearing loss and other physical and cognitive deficits, the best ways to deliver hearing health care, and the effects of reimbursement on the use of hearing technologies. Several speakers at the workshop commented on the value that could be derived from a large-scale randomized controlled trial of the association between better hearing health care and healthy aging.
The workshop was designed to catalyze changes that are already ongoing, Lin observed. The aging of the baby boomers, rapid technological advances, changes in the health care system, and recognition of the problems caused by hearing loss are coming together to produce a unique opportunity. As Lin said, the workshop represented “the first time in history that we have had a meeting like this with this many stakeholders at the table.” Continued interdisciplinary efforts to address age-related hearing loss could improve the lives of many millions of peoples.
ORGANIZATION OF THE WORKSHOP SUMMARY
This workshop summary is limited to describing the presentations given and general topics discussed during the workshop itself. Overall, each speaker’s presentation is captured in a section attributed to that individual. All of the workshop discussions with the audience have also been captured in a variety of ways. For the most part, topics raised and responses given during the discussion periods were incorporated into the individual section for the speaker whose presentation was directly related to the given topic or question. In some cases, where a new topic or line of discussion arose, a separate section was introduced to reflect that new topic. Presentations are also not necessarily organized in the same order as the actual workshop,
but have been rearranged to provide a better flow for the readers of this workshop summary.
Following this introductory chapter, Chapter 2 presents the personal experiences of two people with moderate to severe hearing loss who have found ways to overcome these losses and remain healthy and active. Chapter 3 explores the link between hearing and those domains that characterize healthy aging, including physical, cognitive, and psychosocial functioning. Chapter 4 looks at current approaches to hearing health care delivery, both in the United States and abroad. Chapter 5 considers the wealth of rapidly advancing technologies available to counter hearing loss and maintain healthy aging. Chapter 6 describes innovative models to hearing health care, and Chapter 7 looks at some of the most prominent current issues in hearing health care. Finally, Chapter 8 describes collaborative strategies for moving forward, first from the perspectives of several representatives of large organizations and then from the perspectives of individual workshop participants.








