Abstract: This chapter presents the objectives, scope, and context for this report and describes the approach that the Institute of Medicine Committee on the Governance and Financing of Graduate Medical Education (GME) used to undertake the study. The committee’s charge was to examine the GME landscape and to recommend policies regarding GME governance and financing. The committee’s deliberations were based on the central premise that a good system of GME is one that supports the nation’s health and health care goals, as articulated in the “triple aim” of improving the individual experience of care, improving the health of populations, and reducing per capita costs of health care.
Becoming a physician in the United States is a long and costly process. American taxpayers have helped support physician education for generations. With that support, the nation’s teaching hospitals have been integral to the production of a physician workforce well prepared to enter clinical practice. Today, newly trained physicians enter practice with strong scientific underpinnings in the biological and physical sciences as well as supervised practical experience in delivering care and applying the knowledge and principles they have learned.
The federal government began funding residency training—graduate medical education (GME)—when it enacted the GI Bill through the Servicemen’s Readjustment Act of 1944 (Ludmerer, 2012). In 1965, with the creation of the Medicare program, federal funding of GME became a statutory mandate. Today, annual federal spending on GME exceeds
$15 billion (Henderson, 2013; HRSA, 2013b). Many observers believe this investment should be more strategic and more effective (ACP, 2011; MedPAC, 2010; Spero et al., 2013; Weinstein, 2011).
For decades, blue ribbon panels, public- and private-sector commissions, provider groups, and Institute of Medicine (IOM) committees have been assembled to assess the GME system and to propose policies to facilitate its improvement (AAMC, 2012a; AMA Citizens Commission on Graduate Medical Education, 1966; Bipartisan Policy Center Health Project, 2013a; Coggeshall, 1965; COGME, 2007, 2010, 2013; Commonwealth Fund Commission on a High Performance Health System, 2006; IOM, 1989, 2003a,b, 2004, 2010; Ludmerer, 2012; Macy Study Group on Graduate Medical Education, 1980; MedPAC, 2010; Weinstein, 2011). The reports generated by these efforts have highlighted a range of problems: lack of accountability and transparency (Johns, 2010; MedPAC, 2010); a mismatch between the health care needs of the population and the increasing number of physician specialists (Cassel and Reuben, 2011; Detsky et al., 2012); persistent geographic maldistribution of physicians; the growing burden of medical school debt (GAO, 2009; Youngclaus and Fresne, 2012); the significant differences in the racial and ethnic makeup of the physician population compared to the patient population (Reschovsky and Boukus, 2010; Saha et al., 2008; Sullivan and Suez Mittman, 2010); and the gap between new physicians’ knowledge, skills, and professional values and the competencies required for current medical practice (Cronenwett and Dzau, 2010; Crosson et al., 2011; IOM, 2003b, 2004; Weiss et al., 2013).
The impetus for this assessment of GME was two conferences sponsored by the Josiah Macy Jr. Foundation in 2010-2011, the first of which was jointly sponsored by the Association of Academic Health Centers (Johns, 2010; Weinstein, 2011). The conferences were designed to identify needed reforms to GME and suggest approaches for achieving them. The final conference proceedings included a recommendation that the IOM (or a similar body) conduct an independent external review of the goals, governance, and financing of the GME system (Weinstein, 2011). Subsequently, the Macy Foundation entered into a contract with the IOM for the review. Additional support to do this assessment came from 11 U.S. senators who expressed support in letters to the IOM.1
The initial and substantial financial support of the Macy Foundation catalyzed additional support for the IOM study from a wide range of sponsors from across the country. Ultimately, 12 private foundations, the Health
________________
1 The signatories to the letters were Senators Michael Bennet (D-CO), Mike Crapo (R-ID), Charles Grassley (R-IA), Bill Nelson (D-FL), Jack Reed (D-RI), Charles E. Schumer (D-NY), Mark Udall (D-CO), and Thomas Udall (D-NM) and former Senators Jeff Bingaman (D-NM), John Kerry (D-MA), and Jon Kyl (R-AZ). See Appendix B.
ABIM Foundation
Aetna Foundation
California Endowment
California HealthCare Foundation
The Commonwealth Fund
East Bay Community Foundation
Health Resources and Services Administration
Jewish Healthcare Foundation
Josiah Macy Jr. Foundation
Kaiser Permanente Institute for Health Policy
The Missouri Foundation for Health
Robert Wood Johnson Foundation
UnitedHealth Group Foundation
U.S. Department of Veterans Affairs
Resources and Services Administration (HRSA), and the U.S. Department of Veterans Affairs (VA) came forward to sponsor the study. Study sponsors are listed in Box 1-1.
This chapter provides background for the study, describes the scope of the inquiry, and presents the committee’s conceptual framework and goals for this report.
The IOM Committee on the Governance and Financing of Graduate Medical Education was appointed in the summer of 2012 to conduct the study and prepare this report. The 21-member committee included experts in GME financing; residency training of allopathic and osteopathic physicians; undergraduate medical education; nursing and physician assistant education; management of health care systems; physician training in a variety of settings, including teaching hospitals, large academic medical centers, Veterans Health Administration (VHA) facilities, rural areas, safety net institutions, and teaching health centers; the Medicare and Medicaid programs; health and labor economics; and accreditation, licensure, and other regulation of physician training and practice. The committee also included a consumer representative and a recent graduate of residency training. Brief biographies of committee members are provided in Appendix D.
The charge to the committee is presented in Box 1-2. Ideally, GME policy should be considered in the context of the trainees’ progress from undergraduate medical education through residency training and continu-
BOX 1–2
Charge to the IOM Committee on the Governance and Financing of Graduate Medical Education
An ad hoc Institute of Medicine committee will develop a report with recommendations for policies to improve graduate medical education (GME), with an emphasis on the training of physicians. Specific attention will be given to increasing the capacity of the nation’s clinical workforce that can deliver efficient and high-quality health care that will meet the needs of our diverse population. To that aim, in developing its recommendations the committee will consider the current financing and governance structures of GME; the residency pipeline; the geographic distribution of generalist and specialist clinicians; types of training sites; relevant federal statutes and regulations; and the respective roles of safety net providers, community health/teaching health centers, and academic health centers.
ing medical education after entry into practice. Although a comprehensive review of the full continuum of medical education is needed, it is beyond the scope of this study. As the committee considered its approach to the study, the group discussed whether this report should focus on not only graduate training of physicians but also other health professionals, such as dentists, podiatrists, advanced practice registered nurses, and physician assistants. The committee decided to focus on the former. The statutory definition of GME does not include other clinicians except for podiatrists and dentists.2 Podiatry and dentistry are outside the scope of the study.
This section provides a brief background on residency training and GME financing and governance. The subsequent chapters will review these topics in depth. See Table 1-1 for selected statistics on the GME pipeline, federal GME funding, and related data.
Continuum of Physician Education
The continuum of formal physician education begins with undergraduate medical education in an allopathic or osteopathic medical school (see Figure 1-1). U.S. medical schools confer the M.D. or D.O. degree. U.S. graduates with these degrees combine with some of the graduates of non-U.S. medical schools in competing for positions in U.S. GME, the period
________________
2 Consolidated Omnibus Budget Reconciliation Act of 1985, Public Law 99-272, 100 Stat. 82 (April 7, 1986).
TABLE 1-1 Selected GME Statistics
| Number | ||
| Pipeline to GME (2013) | ||
| Allopathic and osteopathic medical schools | 171 | |
| Allopathic and osteopathic medical school graduates | 20,164 | |
| Available ACGME residency positions | 29,171 | |
| Applicants for ACGME residency positions | 34,355 | |
|
5,095 | |
|
7,568 | |
| Available AOA residency positions | 2,900 | |
| ACGME-accredited training programs (2013) | 9,265 | |
| Initial residency period | 4,084 | |
| Subspecialties | 5,181 | |
| Number of AOA-accredited training programs (2012) | 1,015 | |
| Internships | 132 | |
| Residencies | 883 | |
| Residents in ACGME programs (2013) | 117,717 | |
| Initial residency period | 97,155 | |
| Subspecialties | 20,562 | |
| Residents in AOA programs (2012) | 11,020 | |
| Internships | 1,279 | |
| Residencies | 9,741 | |
| Principal federal GME funders | ||
| Medicare (2012) | $9.7 billion | |
| Medicaid (2012) | $3.9 billion | |
| Health Resources and Services Administration | $0.5 billion | |
| Veterans Health Administration (VHA) (2012) | $1.4 billion | |
| Trends in use of hospital services | 1980 | 2010 |
| Hospital days per 10,000 population | 13,027.0 | 5,369.2 |
| Hospital discharges per 10,000 population | 1,744.5 | 1,125.1 |
NOTES: Medicare estimates provided via e-mail by Marc Hartstein, Director, Hospital and Ambulatory Policy Group, Center for Medicare, Centers for Medicare & Medicaid Services, September 4, 2013. VA estimates provided via e-mail by Barbara K. Chang, Director of Medical and Dental Education, VHA Office of Academic Affiliations, July 15, 2013. The 2010 hospital statistics are drawn from pooled 2009-2010 data. ACGME and AOA data include dually accredited programs.
SOURCE: AACOM, 2013; AAMC, 2012b; ACGME, 2013; Brotherton and Etzel, 2012; Henderson, 2013; National Center for Health Statistics, 2013; National Resident Matching Program, 2013.
called residency training. GME has evolved from an apprenticeship model to a curriculum-based education program—though learning is still predominantly based on resident participation in patient care, under supervision, with increasing independence through the course of training.
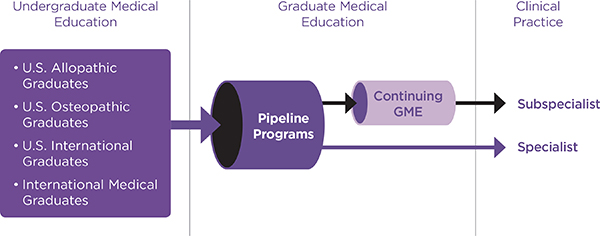
SOURCE: ACGME, 2013.
Most residency programs are sponsored by and take place in large teaching hospitals and academic health centers. However, as health care services are increasingly provided in ambulatory and community-based settings, residency training is beginning to expand to non-hospital sites (University of Texas System and Lieberman, 2012). Based on the rapid evolution under way in health system delivery involving an increasing emphasis on non-hospital-based care, many experts recommend an acceleration of this transition (Fuchs, 2011).
Every state requires at least a year of residency training in the United States to receive an unrestricted license to practice medicine (FSMB, 2013), and some require 2 or 3 years. However, most physicians train beyond the minimum licensure requirement in order to become board certified in a “pipeline” specialty (i.e., those that lead to initial board certification) (see Box 1-3) (ACGME, 2013; AOA, 2013). The number of pipeline training positions determines the total number of physicians that the entire continuum can produce. For many years, the number of U.S. residency slots has been larger than the number of U.S. medical graduates, so residency programs were filled in part by graduates of non-U.S. medical schools (including both U.S. and non-U.S. citizens). Now, with growth in the number and size of medical schools, the number of U.S. medical graduates is beginning to more closely approximate the current number of residency slots (AAMC, 2013; COGME, 2013). In a recent survey conducted by the Association of American Medical Colleges (AAMC), 122 of 130 responding medical school deans reported some concern about the number of clinical training opportunities for their graduates (AAMC, 2013).
Anesthesiology
Dermatology
Emergency medicine
Family medicine
Internal medicine
Internal medicine/pediatrics
Medical genetics
Neurological surgery
Neurology
Nuclear medicine
Obstetrics and gynecology
Ophthalmology
Orthopaedic surgery
Otolaryngology
Pathology—anatomic and clinical
Pediatrics
Physical medicine and rehabilitation
Plastic surgery
Plastic surgery—integrated
Preventive medicine
Psychiatry
Radiation oncology
Radiology—diagnostic
Surgery
Thoracic surgery—integrated
Urology
Vascular surgery—integrated
SOURCE: Adapted from ACGME, 2011.
Board certification in a pipeline specialty is increasingly required for credentialing3 and typically takes 3 to 7 years. A substantial and increasing proportion of physicians choose to go on to subspecialty training after their initial board certification, in a variety of fields, such as cardiology or gastroenterology (subspecialties of internal medicine and pediatrics) (Brotherton and Etzel, 2012). In 2012, more than 117,000 residents were on duty in 9,265 allopathic residency programs across the country (ACGME, 2013). Of these, more than 20,500 (17.5 percent) were in subspecialty fellowships.
A Note on Terminology
In this report, the term “GME” is used to describe the period of residency and fellowship training that is provided to physicians after they receive an allopathic or osteopathic medical degree. The committee distinguishes among GME, the educational enterprise, and GME funding, the financing of GME, largely through the Medicare and Medicaid programs. This report uses the term “residency” to refer to the initial period of residency training required for board eligibility and fellowship training that may occur afterward. “Fellows” and “subspecialty residents” are physicians who have completed the requirements for eligibility for first board certification and are training in a related subspecialty. Unless otherwise
________________
3 Credentialing is a process used by third-party payers and health care organizations to evaluate the qualifications and practice history of a doctor.
specified, our discussion of GME and comments about physicians refer jointly to osteopathic and allopathic physicians.
As Box 1-4 describes, the term “primary care” is often used to include a variety of specialties, depending on the context.
BOX 1–4
Primary Care Specialties
The Institute of Medicine defines primary care not as a collection of specialties but as:
the provision of integrated, accessible health care services by clinicians who are accountable for addressing a large majority of personal health care needs, developing a sustained partnership with patients, and practicing in the context of family and community.
However, in the context of graduate medical education, the term “primary care” typically refers to medical specialties. Federal agencies, for example, often describe primary care specialities as including family medicine, general internal medicine, and general pediatrics, as noted below. Sometimes obstetrics and gynecology (OB/GYN), psychiatry, and geriatrics are also considered (or formally designated) to be primary care specialties.
| Family Medicine | Internal Medicine (General)* | Pediatrics (General) | OB/GYN | Psychiatry (General) | Geriatrics | |
| Government Accountability Office | X | X | X | |||
| American Medical Association | X | X | X | X | ||
| National Health Service Corps | X | X | X | X | X | X |
| Medicare GME | X | X | X | ** | ** | X |
| Affordable Care Act | X | X | X | X | X | X |
*Internal medicine also includes internal medicine/family medicine and internal medicine/pediatrics.
**OB/GYN and psychiatry are considered primary care specialties by the Medicare graduate medical education program when the resident is the primary caregiver and the faculty physician sees the patient only in a consultative role.
SOURCES: GAO, 2009; HRSA, 2012; IOM, 1996.
GME Financing
Medicare is the single largest explicit contributor to GME ($9.7 billion in 2012), followed by Medicaid ($3.9 billion in 2012) (Henderson, 2013).4 The VHA and HRSA are also important funders of GME, contributing an estimated $1.4 billion and $0.5 billion respectively (HRSA, 2013a). States, private insurers, and industry also provide support.
GME Governance
There is no single public or private entity that provides oversight of GME. Standards and program requirements—across the continuum of physician education—are the responsibility of a wide array of private organizations and government licensing agencies with sometimes overlapping interests and jurisdiction. These include the AAMC, Accreditation Council for Graduate Medical Education (ACGME), American Board of Medical Specialties, American Medical Association, American Osteopathic Association, Commission on Dental Accreditation, Council of Medical Specialty Societies, Council on Osteopathic Postgraduate Training, Council on Podiatric Education, Educational Commission for Foreign Medical Graduates, Residency Review Committees (delegated authority via ACGME), and state medical boards.
This is a time of tremendous change and uncertainty in U.S. health care. Key provisions of the Patient Protection and Affordable Care Act (ACA)5 are not yet implemented. Many health providers and policy makers worry that the Act’s expansion of health insurance coverage to millions of Americans—combined with the aging of the population—will overwhelm the workforce we have. Some analysts have projected dramatic workforce shortages—especially for physicians—that could prevent many people from getting needed health services (AAMC, 2011, 2012a; Kirch et al., 2012; Petterson et al., 2012; Sheldon, 2010). There are also widespread concerns that the nation is not training the right specialty mix of physicians to meet society’s needs (ACP, 2011; Bipartisan Policy Center Health Project, 2013b; MedPAC, 2010), and that these physicians are not geographically well distributed (Iglehart, 2011). At the same time, current economic pressures
________________
4 Medicare estimate provided via personal communication with Marc Hartstein, Director, Hospital and Ambulatory Policy Group, Center for Medicare, Centers for Medicare & Medicaid Services, September 12, 2013.
5 Public Law 111-148.
place every federal program under intense scrutiny—including the funding of GME.
Workforce planning in today’s environment is a complex and daunting challenge. The United States has never established a data infrastructure to support an assessment of the health care workforce or the educational system that produces it.6 Although some suggest that covering the uninsured and the aging of the population will increase the need for physicians (COGME, 2013; Grover and Niecko-Najjum, 2013; Kirch et al., 2012), others suggest that new deployments of technology and other types of clinicians will reduce our reliance on physicians (Auerbach et al., 2013; Bodenheimer and Smith, 2013; Bodenheimer et al., 2009; Fuchs, 2013; Ghorob and Bodenheimer, 2012; Green et al., 2013; Reinhardt, 2013).
In this period of rapid change, there is also substantial concern that medical education is not preparing physicians to practice in contemporary America (Crosson et al., 2011; Johns, 2010; MedPAC, 2010; Skochelak, 2010; Weinstein, 2011). A variety of surveys indicate that recently trained physicians in some specialties cannot perform simple procedures often required in office-based practice and lack sufficient training and experience in care coordination, team-based care, and quality improvement (Cordasco et al., 2009; Crosson et al., 2011; MedPAC, 2010). They are often ill prepared to care for an increasingly diverse and aging population (IOM, 2008, 2012; Weissman et al., 2005).
CONCEPTUAL APPROACH TO THE STUDY
This report is based on the central premise that a good system of GME is one that supports the nation’s health and health care goals, and those goals are well represented by the “triple aim” of improving the individual experience of care, improving the health of populations, and reducing per-capita costs of health care (Berwick et al., 2008). A focus on the individual experience of care requires attention to six dimensions of health care quality: safety, effectiveness, patient-centeredness, timeliness, efficiency, and equity (IOM, 2001). Prioritizing the health of populations requires that the health care workforce has skills not only in the treatment of acute conditions, but also in managing chronic disease and multiple conditions, and in disease prevention and health promotion. Targeting the reduction of per capita costs requires that providers practice cost-effective care with appropriate use of resources and that financial management incorporates accountability and transparency.
________________
6 Although the ACA authorized the creation of a National Health Care Workforce Commission to assume some of these responsibilities, the funds have not been appropriated for its operations.
The committee examined the assumptions that underlie current GME governance and financing arrangements—including the fundamental question of whether public funds should be used for this enterprise. The committee debated—at great length—the justification and rationale for federal funding of GME either through Medicare or other sources, given the lack of comparable federal financing for undergraduate medical education, other health care professionals, or other areas important to society and in shortage. The committee also considered the economist’s perspective that residents, not teaching sites, bear the cost of their training by accepting low salaries that reflect (on average) the difference between the value of the services they provide and the cost of the training they receive (Becker, 1964; Chandra et al., 2014; Newhouse and Wilensky, 2001).
Improving the governance and financing of GME cannot, on its own, produce a high-value, high-performance health care system. Other factors, such as the way in which we pay for health care services, are surely more significant determinants of how physicians select specialties and geographic areas and how well the health care system functions more generally. Nevertheless, the GME system is a powerful influence over the makeup, skills, and knowledge of the physician workforce. The most important way to judge the governance and financing of GME is by the degree to which it helps the nation achieve the triple aim—objectives long advocated by the IOM. The committee, therefore, agreed that continued public funding of GME is warranted only if it is reformed to help produce a physician workforce better able to support a high-value, high-performing health care system.
Thus, this report examines the current landscape with an eye toward identifying opportunities to maximize the leverage of federal support and to minimize barriers to progress.
With the above principles in mind, the committee developed the following six goals to guide its research, analysis, and eventual recommendations for the future of GME:
- Encourage production of a physician workforce better prepared to work in, to help lead, and to continually improve an evolving health care delivery system that can provide better individual care, better population health, and lower cost.
- Encourage innovation in the structures, locations, and designs of graduate medical education programs, to better achieve Goal #1.
- Provide transparency and accountability of GME programs, with respect to the stewardship of public funds and the achievement of GME goals.
- Clarify and strengthen public policy planning and oversight of GME with respect to the use of public funds and the achievement of goals for the investment of those funds.
- Ensure rational, efficient, and effective use of public funds for GME in order to maximize the value of this public investment.
- Mitigate unwanted and unintended negative effects of transition from the current GME funding system to a future one.
The committee deliberated over six in-person meetings and numerous teleconferences between September 2012 and January 2014. It began the study by reviewing past reports and recommendations regarding GME policy dating back several decades. These included all the relevant reports of the Council on Graduate Medical Education (COGME) and the Medicare Payment Advisory Commission (MedPAC), as well as policy recommendations from the American College of Physicians, American College of Surgeons, American Medical Association, American Osteopathic Association, Association of American Medical Colleges, Bipartisan Policy Center, Government Accountability Office, Josiah Macy Jr. Foundation, previous IOM committees, and others. Many of the reports included recommendations regarding accountability and transparency of GME funding; the sufficiency of the numbers of Medicare-supported residency slots; GME performance outcomes, methods and sources of funding; and the site and content of training, innovation, and research (AAMC, 2012a; ACP, 2011; AMA Citizens Commission on Graduate Medical Education, 1966; Bipartisan Policy Center Health Project, 2013a; Buser and Hahn, 2013; Coggeshall, 1965; COGME, 2005a,b, 2007, 2010, 2013; IOM, 1989, 2003a,b, 2004, 2008, 2010, 2012; Johns, 2010; Kirch, 2012; Macy Study Group, 1980; MedPAC, 2001, 2003, 2009, 2010; Office of Academic Affiliations, Veterans Health Administration, 2009; Shannon et al., 2013; Weinstein, 2011).
Several committee workgroups were formed to examine the reports in depth and to assess the quality of the available evidence on key topics such as physician workforce supply, GME costs and financing, governance and accountability, and residency program outcomes. To address the lack of generalizable GME cost data, a workgroup of the committee explored what it could learn about GME financing by interviewing and collecting GME cost and revenue data from several academic medical centers. Further details of this review are in Chapter 3.
The committee actively sought input from a broad spectrum of GME stakeholders. At the first meeting in September 2012, the committee heard invited testimony on GME policy concerns from senior legislative staff; federal representatives from the Medicare and Medicaid programs; HRSA; VA;
the Department of Defense; and congressional staff to the Senate Health, Education, Labor, and Pensions Committee; the Senate Finance Committee; the House Committee on Energy and Commerce and the Health Subcommittee on Health of the House Committee on Ways and Means. The committee held a second public forum in December 2012. This day-and-a-half event featured a wide range of perspectives, including academic medical centers, current and recent trainees, accreditation and certification organizations, allopathic and osteopathic colleges of medicine, physician specialty organizations, state and regional health workforce organizations, private insurers, teaching hospitals, teaching health centers and other community-based training sites, workforce and health services and policy research. The event was organized in a series of panels on national and regional workforce planning; determining the sufficiency of the workforce; challenges in developing community-based training; perspectives from current residency trainees; innovations in health care and medical education; ensuring accountability; and understanding the costs and financing of GME. Appendix C contains the agendas for the two public meetings, including a complete list of all speakers and their affiliations. The speakers’ presentations and audio recordings from the December meeting are available on the study website: http://iom.edu/Activities/Workforce/GMEGovFinance.aspx.
ORIENTATION TO THE ORGANIZATION OF THIS REPORT
This introductory chapter has described the background, scope, methods, context, and conceptual approach to this report.
Chapter 2, Background on the Pipeline to the Physician Workforce, provides a snapshot of recent trends in the “production” of the physician workforce. It describes the characteristics of GME trainees and considers whether the GME system is producing the types of physicians that the nation requires. The focus is on specialty distribution, geographic location, the ability to care for diverse patient populations, and physicians’ overall readiness to practice medicine.
Chapter 3, GME Financing, gives an overview of the principal sources and payment methods of GME funding. It then describes current Medicare rules governing the distribution of these funds, reviews what is known about the true costs and revenues associated with residency training, and concludes with a discussion of the implications of the current system for funding GME.
Chapter 4, Governance, describes the organizations that have a role in GME oversight and reviews the use of accountability mechanisms in Medicare and other federal GME programs. The primary focus is on Medicare GME because it provides most of the public funding.
Chapter 5, Recommendations for the Reform of GME Financing and Governance, presents the committee’s conclusions and recommendations.
AACOM (American Association of Colleges of Osteopathic Medicine). 2013. U.S. colleges of osteopathic medicine. http://www.aacom.org/about/colleges/Pages/default.aspx (accessed September 19, 2013).
AAMC (Association of American Medical Colleges). 2011. Recent studies and reports on physician shortages in the U.S. Washington, DC: AAMC.
AAMC. 2012a. AAMC physician workforce policy recommendations. Washington, DC: AAMC.
AAMC. 2012b. Table 27: Total graduates by U.S. medical school and sex, 2008-2012. https://www.aamc.org/download/321532/data/2012factstable27-2.pdf (accessed September 19, 2013).
AAMC. 2013. Results of the 2012 Medical School Enrollment Survey. https://members.aamc.org/eweb/upload/12-237%20EnrollmSurvey2013.pdf (accessed October 7, 2013).
ACGME (Accreditation Council for Graduate Medical Education). 2011. Glossary of terms and common acronyms in GME. Chicago, IL: ACGME.
ACGME. 2013. Data resource book: Academic year 2012-2013. Chicago, IL: ACGME.
ACP (American College of Physicians). 2011. Aligning GME policy with the nation’s health care workforce needs: A position paper. Philadelphia, PA: ACP.
AMA (American Medical Association) Citizens Commission on Graduate Medical Education. 1966. The graduate education of physicians. Chicago, IL: AMA.
AOA (American Osteopathic Association). 2013. 2013 osteopathic medicine profession report. http://www.osteopathic.org/inside-aoa/about/aoa-annual-statistics/Documents/2013OMP-report.pdf (accessed February 27, 2014).
Auerbach, D. I., P. G. Chen, M. W. Friedberg, R. O. Reid, C. Lau, and A. Mehrotra. 2013. New approaches for delivering primary care could reduce predicted physician shortage. Santa Monica, CA. http://www.rand.org/pubs/research_briefs/RB9752 (accessed February 21, 2014).
Becker, G. S. 1964. Human capital: A theoretical and empirical analysis, with special reference to education. New York: National Bureau of Economic Research (distributed by Columbia University Press).
Berwick, D. M., T. W. Nolan, and J. Whittington. 2008. The triple aim: Care, health, and cost. Health Affairs 27(3):759-769.
Bipartisan Policy Center Health Project. 2013a. A bipartisan Rx for patient-centered care and system-wide cost containment (accessed April 22, 2013).
Bipartisan Policy Center Health Project. 2013b. The complexities of national health care workforce planning: A review of current data and methodologies and recommendations for future studies. http://bipartisanpolicy.org/sites/default/files/BPC%20DCHS%20Workforce%20Supply%20Paper%20Feb%202013%20final.pdf (accessed April 16, 2013).
Bodenheimer, T. S., and M. D. Smith. 2013. Primary care: Proposed solutions to the physician shortage without training more physicians. Health Affairs 32(11):1881-1886.
Bodenheimer, T., E. Chen, and H. D. Bennett. 2009. Confronting the growing burden of chronic disease: Can the U.S. health care workforce do the job? Health Affairs 28(1):64-74.
Brotherton, S. E., and S. I. Etzel. 2012. Graduate medical education, 2011-2012. JAMA 308(21):2264-2279.
Buser, B. R., and M. B. Hahn. 2013. Building the future: Educating the 21st century physician. http://mededsummit.net/uploads/BRC_Building_the_Future__Educating_the_21st_Century_Physician__Final_Report.pdf (accessed October 20, 2013).
Cassel, C. K., and D. B. Reuben. 2011. Specialization, subspecialization, and subsubspecialization in internal medicine. New England Journal of Medicine 364(12):1169-1173.
Chandra, A., D. Khullar, and G. R. Wilensky. 2014. The economics of graduate medical education. New England Journal of Medicine 379:2357-2360.
Coggeshall, L. T. 1965. Planning for medical progress through education. Evanston, IL: AAMC.
COGME (Council of Graduate Medical Education). 2005a. Sixteenth Report: Physician workforce policy guidelines for the United States. Rockville, MD: HRSA.
COGME. 2005b. Seventeenth Report: Minorities in medicine: An ethnic and cultural challenge for physician training: An update. Rockville, MD: HRSA.
COGME. 2007. Nineteenth report: Enhancing flexibility in graduate medical education. Rockville, MD: HRSA.
COGME. 2010. Twentieth report: Advancing primary care. Rockville, MD: HRSA.
COGME. 2013. Twenty-first report: Improving value in graduate medical education. http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/twentyfirstreport.pdf (accessed October 7, 2013).
Commonwealth Fund Commission on a High Performance Health System. 2006. Framework for a high performance health system for the United States. http://www.commonwealthfund.org/~/media/Files/Publications/Fund%20Report/2006/Aug/Framework%20for%20a%20High%20Performance%20Health%20System%20for%20the%20United%20States/Commission_framework_high_performance_943%20pdf.pdf (accessed September 30, 2012).
Cordasco, K. M., M. Horta, N. Lurie, C. E. Bird, and B. O. Wynn. 2009. How Are Residency Programs Preparing Our 21st Century Internists? A study conducted by staff from RAND Health for the Medicare Payment Advisory Commission. http://www.medpac.gov/documents/Jul09_ResidencyPrograms_CONTRACTOR_CB.pdf (accessed April 2, 2013).
Cronenwett, L., and V. J. Dzau, editors. 2010. Who will provide primary care and how will they be trained? Proceedings of a conference sponsored by the Josiah Macy Jr. Foundation, Durham, NC, January 8-11.
Crosson, F. J., J. Leu, B. M. Roemer, and M. N. Ross. 2011. Gaps in residency training should be addressed to better prepare doctors for a twenty-first–century delivery system. Health Affairs 30(11):2142-2148.
Detsky, A., S. R. Gauthier, and V. R. Fuchs. 2012. Specialization in medicine: How much is appropriate? JAMA 307(5):463-464.
FSMB (Federation of State Medical Boards). 2013. State-specific requirements for initial medical licensure. http://www.fsmb.org/usmle_eliinitial.html (accessed January 9, 2014)
Fuchs, V. R. 2011. The structure of medical education—it’s time for a change. Alan Greg Lecture, Denver, CO, November 6.
Fuchs, V. R. 2013. Current challenges to academic health centers. JAMA 310(10):1021-1022
GAO (Government Accountability Office). 2009. Graduate medical education: Trends in training and student debt. Washington, DC: GAO.
Ghorob, A., and T. Bodenheimer. 2012. Sharing the care to improve access to primary care. New England Journal of Medicine 366(21):1955-1957.
Green, L. V., S. Savin, and Y. Lu. 2013. Primary care physician shortages could be eliminated through use of teams, nonphysicians, and electronic communication. Health Affairs 32(1):11-19.
Grover, A., and L. M. Niecko-Najjum. 2013. Building a health care workforce for the future: More physicians, professional reforms, and technological advances. Health Affairs 32(11):1922-1927.
Henderson, T. M. 2013. Medicaid graduate medical education payments: A 50-state survey. https://members.aamc.org/eweb/upload/Medicaid%20Graduate%20Medical%20Education%20Payments%20A%2050-State%20Survey.pdfitat (accessed June 22, 2013).
HRSA (Health Resources and Services Administration). 2012. Students to service loan repayment pilot program. FY 2013 application and program guidance. http://nhsc.hrsa.gov/loanrepayment/studentstoserviceprogram/applicationguidance.pdf (accessed August 6, 2013).
HRSA. 2013a. Active grants for HRSA programs: Affordable Care Act Teaching Health Center (THC) Graduate Medical Education (GME) Payment Program (T91). http://ersrs.hrsa.gov/ReportServer/Pages/ReportViewer.aspx?/HGDW_Reports/FindGrants/GRANT_FIND&ACTIVITY=T91&rs:Format=HTML4.0 (accessed August 16, 2013).
HRSA. 2013b. HRSA Sequestration Operating Plan for FY 2013. http://www.hrsa.gov/about/budget/operatingplan2013.pdf (accessed June 25, 2013).
Iglehart, J. K. 2011. The uncertain future of Medicare and graduate medical education. New England Journal of Medicine 365(14):1340-1345.
IOM (Institute of Medicine). 1989. Primary care physicians: Financing their graduate medical education in ambulatory settings. Washington, DC: National Academy Press.
IOM. 1996. Primary care: America’s health in a new era. Washington, DC: National Academy Press.
IOM. 2001. Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
IOM. 2003a. Academic health centers: Leading change in the 21st century. Washington, DC: The National Academies Press.
IOM. 2003b. Health professions education: A bridge to quality. Washington, DC: The National Academies Press.
IOM. 2004. In the nation’s compelling interest. Washington, DC: The National Academies Press.
IOM. 2008. Retooling for an aging America: Building the health care workforce. Washington, DC: The National Academies Press.
IOM. 2010. Redesigning continuing education in the health professions. Washington, DC: The National Academies Press.
IOM. 2012. The mental health and substance use workforce for older adults: In whose hands? Washington, DC: The National Academies Press.
Johns, M. M. E.. 2010. Ensuring an effective physician workforce for America. Proceedings of a conference sponsored by the Josiah Macy Jr. Foundation, Atlanta, GA, October 24-25.
Kirch, D. G., M. K. Henderson, and M. J. Dill. 2012. Physician workforce projections in an era of health care reform. Annual Review of Medicine 63:435-445.
Ludmerer, K. M. 2012. The history of calls for reform in graduate medical education and why we are still waiting for the right kind of change. Academic Medicine 87:34-40.
Macy Study Group on Graduate Medical Education. 1980. Graduate medical education present and prospective: A call for action. New York: Josiah Macy Jr. Foundation.
MedPAC (Medicare Payment Advisory Commission). 2001. Chapter 10—Treatment of the initial residency period in Medicare’s direct graduate medical education payments. Washington, DC: MedPAC.
MedPAC. 2003. Impact of the resident caps on the supply of geriatricians. Washington, DC: MedPAC.
MedPAC. 2009. Report to Congress: Improving incentives in the Medicare program. Washington, DC: MedPAC.
MedPAC. 2010. Graduate medical education financing: Focusing on educational priorities. In Report to Congress: Aligning incentives in Medicare. Washington, DC. Pp. 103-126. http://www.medpac.gov/chapters/jun10_ch04.pdf (accessed September 30, 2012).
NCHS (National Center for Health Statistics). 2013. Health, United States, 2012: With special feature on emergency care. Hyattsville, MD: NCHS.
National Resident Matching Program. 2013. Results and data: 2013 main residency match. http://b83c73bcf0e7ca356c80-e8560f466940e4ec38ed51af32994bc6.r6.cf1.rackcdn.com/wp-content/uploads/2013/08/resultsanddata2013.pdf (accessed September 13, 2013).
Newhouse, J. P., and G. R. Wilensky. 2001. Paying for graduate medical education: The debate goes on. Health Affairs 20(2):136-247.
Office of Academic Affiliations, Veterans Health Administration. 2009. The report of the Blue Ribbon Panel on VA-Medical School Affiliations. Transforming an historic partnership for the 21st century. http://www.va.gov/oaa/archive/BRP-final-report.pdf (accessed June 26, 2013).
Petterson, S. M., W. R. Liaw, R. L. Phillips, D. L. Rabin, D. S. Meyers, and A. W. Bazemore. 2012. Projecting US primary care physician workforce needs: 2010-2025. Annals of Family Medicine. November/December 10(6):503-509.
Reinhardt, U. 2013. Testimony before the U.S. Senate Committee on Health Labor, Education & Pensions Subcommittee on Primary Health and Aging. Hearing on 30 million new patients and 11 months to go: Who will provide their primary care? http://www.help.senate.gov/imo/media/doc/Reinhardt.pdf (accessed November 26, 2013).
Reschovsky, J. D., and E. R. Boukus. 2010. Modest and uneven: Physician efforts to reduce racial and ethnic disparities. http://www.hschange.com/CONTENT/1113/1113.pdf (accessed October 7, 2013).
Saha, S., G. Guiton, P. F. Wimmers, and L. Wilkerson. 2008. Student body racial and ethnic composition and diversity-related outcomes in U.S. medical schools. JAMA 300(10): 1135-1145.
Shannon, S. C., B. R. Buser, M. B. Hahn, J. B. Crosby, T. Cymet, J. S. Mintz, and K. J. Nichols. 2013. A new pathway for medical education. Health Affairs 32(11):1899-1905.
Sheldon, G. F. 2010. The surgeon shortage: Constructive participation during health reform. Journal of the American College of Surgeons 210(6):887-894.
Skochelak, S. E. 2010. A decade of reports calling for change in medical education: What do they say? Academic Medicine 85(9):S26.
Spero, J. C., E. P. Fraher, T. C. Ricketts, and P. H. Rockey. 2013. GME in the United States: A review of state initiatives. http://www.shepscenter.unc.edu/wp-content/uploads/2013/09/GMEstateReview_Sept2013.pdf?utm_source=GME+in+the+United+States%3A+A+Review+of+State+Initiatives+&utm_campaign=GME+in+the+US%3A++A+Review+of+State+Initiatives&utm_medium=email (accessed February 20, 2014).
Sullivan, L. W., and I. Suez Mittman. 2010. The state of diversity in the health professions a century after Flexner. Academic Medicine 85(2):246-253.
University of Texas System and S. Lieberman. 2012. Transformation in medical education. http://www.utsystem.edu/initiatives/time/homepage/htm (accessed July 18, 2012).
Weinstein, D. 2011. Ensuring an effective physician workforce for the United States. Recommendations for graduate medical education to meet the needs of the public. Proceedings of a conference sponsored by the Josiah Macy Jr. Foundation, Atlanta, GA, May 16-19. New York: Josiah Macy Jr. Foundation.
Weiss, K. B., J. P. Bagian, and T. J. Nasca. 2013. The clinical learning environment: The foundation of graduate medical education. JAMA 309(16):1687-1688.
Weissman, J. S., J. Betancourt, E. G. Campbell, E. R. Park, M. Kim, B. Clarridge, D. Blumenthal, K. C. Lee, and A. W. Maina. 2005. Resident physicians’ preparedness to provide cross-cultural care. JAMA 294(9):1058-1067.
Youngclaus, J., and J. Fresne. 2012. Trends in cost and debt at U.S. medical schools using a new measure of medical school cost of attendance. AAMC Analysis in Brief 12(2). http://www.aamc.org/download/296002/data/aibroll2_no2.pdf (accessed September 12, 2012).


















