4
Review of the Evidence on Major ME/CFS Symptoms and Manifestations
This review of the evidence on major ME/CFS symptoms and manifestations begins with a discussion of the limitations of the research base in this area. The chapter then examines in turn the evidence on fatigue, post-exertional malaise (PEM), sleep-related symptoms, neurocognitive manifestations, and orthostatic intolerance and autonomic dysfunction in ME/CFS.
LIMITATIONS OF THE RESEARCH BASE
One of the most significant challenges to achieving a better understanding of ME/CFS results from the methodological limitations of the current research base. Issues related to external and internal validity and to reliability frequently have led to inconsistent results across studies, as well as other shortcomings. Despite these limitations, however, the committee was able to glean evidence of symptoms, signs, and objective measures for ME/CFS. The evidence with respect to major symptoms and manifestations is presented in this chapter, while that related to other symptoms and manifestations and to pediatric ME/CFS is reviewed in Chapters 5 and 6, respectively. This review of the evidence serves as the basis for the committee’s proposed diagnostic criteria for ME/CFS, which are presented in Chapter 7.
External Validity
Studies on ME/CFS used different inclusion criteria and different sources of ME/CFS patients and control participants. The end result is het-
erogeneity in both patient and control cohorts, creating an unclear picture of the symptoms and signs of the disorder and its outcomes. Findings are based on samples with a large majority of middle-aged women (late 40s to early 50s) who are Caucasian and of higher educational status, perhaps limiting the generalizability of the studies. Very few studies focused on other population subsets, such as pediatric or geriatric patients, or included ethnic and racial minority patients. Some studies recruited patients from specialized ME/CFS treatment centers, while others used community-based samples. These different sampling methods may result in patient groups that differ in demographic characteristics and symptom type and severity. Furthermore, those most severely affected by ME/CFS may be bedridden or homebound and may not have been included in any of these studies (Wiborg et al., 2010). Thus, there are selection biases in the studies’ sample composition.
Some limitations also stem from issues regarding the case definitions or diagnostic criteria used in the studies (see Chapter 3 for a review). Although a strong majority of studies used the Fukuda definition, a small number used various other definitions, thus complicating comparisons of the results. A major limitation of the Fukuda and other ME/CFS case definitions is their polythetic diagnostic criteria. Thus, two patients could have very little symptom overlap yet both be diagnosed with ME/CFS. Therefore, there is potential heterogeneity within and across patient samples in the literature that cannot be assessed because of the lack of reporting of symptom prevalence in most studies (Jason et al., 2012b). This problem is inherent in the study of any illness with polythetic diagnostic criteria. Finally, because most studies used the Fukuda definition to select cases, it is not possible to fully assess the evidence for the other diagnostic criteria for ME/CFS.
Internal Validity
In many cases, studies lacked properly matched controls to account for confounders. The majority of published studies compared a small number of ME/CFS patients with healthy controls. Control groups including people with other illnesses, sedentary individuals, or people who meet different case definitions of ME/CFS have not commonly been used. Because almost all controls were healthy and most were physically active, the findings from those studies do not shed light on which symptoms and signs distinguish ME/CFS from other disorders with some overlapping symptoms.
Some contradictory findings may also be due to the use of various scales, instruments, and measures for symptoms, some of which are imprecise, not comprehensive, or not validated. ME/CFS symptoms were derived mainly from patient self-reports, which raises questions about the internal validity of the study results. Moreover, relatively few studies were
longitudinal, so little light has been shed on the natural history of ME/CFS (Jason et al., 2011b). There also were few studies of the early stages of the illness. This is understandable given that the diagnosis can be made only after 6 months of symptoms (see Chapter 3 and below), but nevertheless is a barrier to understanding the natural history of the illness.
Reliability
A lack of replication and validation in many studies limits the ability to assess the study findings critically. Few attempts have been made to follow up on or replicate intriguing findings in the literature to date.
FATIGUE AND ITS IMPACT ON FUNCTION
The dictionary definition of fatigue as a noun is “weariness from bodily or mental exertion.” Fatigue is not typically considered a disease but is commonly used in medicine to represent a broad spectrum of tiredness, from the physical, cognitive, or emotional feeling at the end of a long day to the emotional or physical toll of acute, chronic, or terminal illness (Gambert, 2005).
Fatigue is one of the most common and nonspecific presenting complaints in primary care. Unfortunately, the word “fatigue” does not convey information about the cause, severity, or chronicity of fatigue or its impact on functionality. Although fatigue is a common experience, it has no unique physiological explanations or objective markers. A broad range of physical, medical, and mental health conditions and stressors may result in the complaint of fatigue (Matthews et al., 1991). Aging alone is associated with a gradual increase in fatigue and reduction in functional capacity for a variety of reasons (National Institute on Aging, 2007). Although overlap exists, fatigue usually can be distinguished from somnolence (also called drowsiness or sleepiness), which often is attributed to deprivation of sleep, primary sleep disorders, or sedating medications (Hossain et al., 2005). Thus, clinicians are challenged to integrate the subjective and objective evidence that can help identify the neurologic, malignant, infectious, inflammatory, cardiopulmonary, metabolic, endocrinologic, physical deconditioning, pharmacologic, or mental health factors that may underlie the presenting complaint of fatigue. (Note that a complete discussion of the differential diagnosis of fatigue is beyond the scope of this report.)
Description of Fatigue in ME/CFS
Patients with ME/CFS almost always suffer from fatigue, and the importance of the symptom is illustrated by its central role in most of the
case criteria developed to date (see Chapter 3). Regardless of what criteria are used, however, ME/CFS patients often have a level of fatigue that is more profound, more devastating, and longer lasting than that observed in patients with other fatiguing disorders. In addition, fatigue in ME/CFS is not the result of ongoing exertion, not lifelong, and not particularly responsive to rest (Jason and Taylor, 2002). Patients describe their fatigue as “exhaustion, weakness, a lack of energy, feeling drained, an inability to stand for even a few minutes, an inability to walk even a few blocks without exhaustion, and an inability to sustain an activity for any significant length of time” (FDA, 2013, p. 7). Some of the more extreme examples include “too exhausted to change clothes more than every 7-10 days”; “exhaustion to the point that speaking is not possible”; and “exertion of daily toileting, particularly bowel movements, sends me back to bed struggling for breath and feeling like I just climbed a mountain.” A few patients describe a “tired but wired” feeling (FDA, 2013, p. 14). Numerous efforts have been made to measure the nature and extent of fatigue in this population (Furst, 1999; Whitehead, 2009). Some patients improve, but most continue to experience some level of fatigue, physical and/or mental, ranging from mild to profound (Wilson et al., 1994).
Jason and colleagues (2009) found that those with ME/CFS frequently report the occurrence of several distinct fatigue states that may diverge from commonplace perceptions of fatigue among the general population. They examined dimensions of fatigue in ME/CFS using a unique 22-item ME/CFS Fatigue Types Questionnaire administered to 130 patients and 251 healthy controls. Factor analysis demonstrated a five-factor structure of fatigue for ME/CFS patients and a one-factor solution for controls. The five types of fatigue that differentiated ME/CFS patients from controls were postexertional, wired, brain fog, energy, and flu-like fatigue (Jason et al., 2009, 2010a), clearly showing the complex nature of fatigue in ME/CFS. Earlier efforts to assess fatigue were made (Jason et al., 2011a), among others, by Chalder and colleagues (1993), who developed the Fatigue Scale; by Ray and colleagues (1992), who created the Profile of Fatigue-Related Symptoms; by Smets and colleagues (1995), who developed the Multidimensional Fatigue Inventory (MFI-20); and by Krupp and colleagues (1989), who developed the Fatigue Severity Scale.
Regarding the duration of fatigue, the Fukuda definition and the Canadian Consensus Criteria (CCC) require 6 months for a diagnosis of ME/CFS. This 6-month requirement is supported by Nisenbaum and colleagues (1998), who showed that unexplained fatigue lasting for more than 6 months was related to symptoms included in the ME/CFS case definitions and that most other causes of similar fatigue do not last beyond 6 months.
In their review of 39 measures of fatigue, Whitehead and colleagues (2009) found that although some measures were better than others, none
were ideal. Most measures have insufficient sensitivity and specificity to encompass all of the various and important aspects of fatigue in ME/CFS (Jason et al., 2011a). In addition, health care providers should note that a single assessment of fatigue severity may not provide a full understanding of the patterns of fatigue presenting over 1 day in ME/CFS patients (Jason and Brown, 2013).
Impact of Fatigue on Function
Fatigue may be most relevant when assessed relative to its impact on function. However, disability caused by fatigue may not reflect the levels of fatigue a patient is experiencing. For instance, despite feeling extremely fatigued, a person may continue working to survive economically and stop only when functionally impaired (Jason and Brown, 2013). Appendix C provides additional examples and rates of functional impairment due to ME/CFS symptoms. In general, patients with ME/CFS experience a marked decrease in function across an array of domains, frequently attributed, at least in part, to their fatigue (Komaroff et al., 1996a).
Efforts have been made to assess the impact of the disease on patients’ function, but most such efforts have been research based. One of the more commonly used tools in medical research as well as in ME/CFS studies is the Short Form 36-Item Questionnaire (SF-36) of the Medical Outcomes Study (MOS) (McHorney et al., 1993; Ware, 2002), a standardized and validated 36-item patient-report questionnaire with eight principal components or subscales used to determine the impact of illness on functionality. Early studies used this tool to distinguish ME/CFS from major depression, multiple sclerosis, acute infectious mononucleosis, hypertension, congestive heart failure, type II diabetes mellitus, acute myocardial infarction, unexplained chronic fatigue, and healthy controls (Buchwald et al., 1996; Komaroff et al., 1996a).
The VT (vitality) subscale of the MOS SF-36, for example, a questionnaire used to assess function, is thought to reflect both mental and physical function (McHorney et al., 1993) and includes the sum of four questions about having a lot of energy, being full of life/pep, feeling worn out, or feeling tired, with higher scores reflecting greater vitality (Ware, 2002). VT scores are consistently much lower in ME/CFS patients with and without comorbidities than in healthy controls and patients with other chronic illnesses, including fibromyalgia. Examples of mean VT scores on the MOS SF-36 from various published studies for the general population and those with ME/CFS and other chronic fatiguing illnesses are summarized in Table 4-1 to demonstrate the profoundly low scores for ME/CFS compared with the other conditions. Several of the studies in the table do not specify the scoring algorithm (raw versus normalized t score) for the MOS SF-36,
TABLE 4-1 Mean VT Score on the MOS SF-36 for ME/CFS Versus Other Fatigue Conditions
| HC | CHF NYHA III | HD | HepC | MD | SSc | |
| Score | 60-70 | 29 | 49 | 48 | 40 | 45 |
| Reference | Buchwald et al., 1996; Komaroff et al., 1996a | Juenger et al., 2002 | Merkus et al., 1997 | Foster et al., 1998 | Komaroff et al., 1996a | Harel et al., 2012 |
NOTES: CHF NYHA III = congestive heart failure New York Heart Association Class III; FM = fibromyalgia; HC = healthy control; HD = hemodialysis; HepC = chronic hepatitis C (without cirrhosis); MCS = multiple chemical sensitivity; MD = major depression; MSD 4+ = at least 4 musculoskeletal diseases; RA = rheumatoid arthritis; SSc = scleroderma/systemic sclerosis; VT = vitality subscale of the MOS SF-36.
so that bias may exist in comparing VT scores across the studies. However, this bias is unlikely to explain the clear differences seen between the ME/CFS and non-ME/CFS groups in Table 4-1.
While Jason and Brown (2013) demonstrated that the VT scores of ME/CFS patients ranged from 15 to 25 depending on subtyping strategies, other domains often are affected as well. Nacul and colleagues (2011a) found that scores on the role-physical (RP)1 subscale of the SF-36 were even more affected than scores on the VT subscale (version 2) but that all domains were impaired, with mental health being the best preserved. Jason and colleagues (2011c) found that impairments in VT, social functioning, and RP had the greatest sensitivity and specificity in identifying patients who met the Fukuda definition of ME/CFS. In one early study, all eight subscores of the SF-36 were lower in ME/CFS patients than in the general population and other disease comparison controls, with the exception of the mental health and role-emotional subscales in the controls with major depression (Komaroff et al., 1996a).
It should be noted that, while widely used in research, the SF-36 may not be well suited to general clinical use because of user fees and the gen-
____________________
1 The RP subscale combines the scores of four questions related to physical activity.
| MSD 4+ | RA | FM | ME/CFS | ME/CFS + FM | ME/CFS + MCS | ME/CFS + FM + MCS |
| 48 | 43-52 | 39-40 | 15-25 | 20 | 15 | 11 |
| Picavet and Hoeymans, 2004 | Picavet and Hoeymans, 2004; Salaffi et al., 2009 | Picavet and Hoeymans, 2004; Salaffi et al., 2009 | Brown and Jason, 2007; Buchwald et al., 1996; Jason and Brown, 2013; Komaroff et al., 1996a | Brown and Jason, 2007 | Brown and Jason, 2007 | Brown and Jason, 2007 |
eral process of having to submit test results to the sponsor for scoring. The RAND-36 is an alternative version that is freely accessible, but it has a complex scoring algorithm (RAND, 1984).
Summary
Fatigue, chronic fatigue, and particularly the impact of fatigue on function should be assessed in making a diagnosis of ME/CFS. Health care providers may use a range of questions and instruments to evaluate fatigue and its impact on function in these patients (see Chapter 7, Table 7-1). However, ME/CFS should not be considered merely a point on the fatigue spectrum or as being simply about fatigue. Experienced clinicians and researchers, as well as patients and their supporters, have emphasized for years that this complex illness presentation entails much more than the chronic presence of fatigue. Other factors, such as orthostatic intolerance, widespread pain, unrefreshing sleep, cognitive dysfunction, and immune dysregulation, along with secondary anxiety and depression, contribute to the burden imposed by fatigue in this illness. The challenge in understanding this acquired chronic debility, unfortunately named “chronic fatigue syndrome” for more than two decades, will be to unravel those complexities.
Conclusion: There is sufficient evidence that fatigue in ME/CFS is profound, not the result of ongoing excessive exertion, and not substantially alleviated by rest. This fatigue results in a substantial reduction or impairment in the ability to engage in pre-illness levels of occupational, educational, social, or personal activities and persists for more than 6 months.
Description of PEM in ME/CFS
PEM is an exacerbation of some or all of an individual’s ME/CFS symptoms that occurs after physical or cognitive exertion and leads to a reduction in functional ability (Carruthers et al., 2003). As described by patients and supported by research, PEM is more than fatigue following a stressor. Patients may describe it as a post-exertional “crash,” “exhaustion,” “flare-up,” “collapse,” “debility,” or “setback.”2 PEM exacerbates a patient’s baseline symptoms and, in addition to fatigue and functional impairment (Peterson et al., 1994), may result in flu-like symptoms (e.g., sore throat, tender lymph nodes, feverishness) (VanNess et al., 2010); pain (e.g., headaches, generalized muscle/joint aches) (Meeus et al., 2014; Van Oosterwijck et al., 2010); cognitive dysfunction (e.g., difficulty with comprehension, impaired short-term memory, prolonged processing time) (LaManca et al., 1998; Ocon et al., 2012; VanNess et al., 2010); nausea/gastrointestinal discomfort; weakness/instability; lightheadedness/vertigo; sensory changes (e.g., tingling skin, increased sensitivity to noise) (VanNess et al., 2010); depression/anxiety; sleep disturbances (e.g., trouble falling or staying asleep, hypersomnia, unrefreshing sleep) (Davenport et al., 2011a); and difficulty recovering capacity after physical exertion (Davenport et al., 2011a,b). In some cases, patients experience new symptoms as part of the PEM response. The following quote reflects the breadth and severity of symptoms associated with PEM in these patients:
when I do any activity that goes beyond what I can do—I literally collapse—my body is in major pain, it hurts to lay in bed, it hurts to think, I can’t hardly talk—I can’t find the words, I feel my insides are at war. My autonomic system is so out of whack! I can’t see farsighted and glasses won’t help—only rest. My GI system is so messed up. Any food hurts it. I tried everything from elimination diets to all the GI meds. Nothing is working. My body jerks. The list goes on. There are days that I just want to cry because I can’t take care of myself—I need help. But, I have no help
____________________
2 Personal communication; public comments submitted to the IOM Committee on the Diagnostic Criteria for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome for meeting 1, 2014.
because of the term CFS and not understanding PEM. I am sorry that I am not dying in the short-term, but I am living life waiting to die because no one takes this disease seriously.3
The types and thresholds of triggers of PEM, its onset, and its duration may vary among individuals and over the course of illness.
Triggers
PEM may occur after physical (Bazelmans et al., 2005; Davenport et al., 2011b; Nijs et al., 2010) or cognitive exertion (Arroll et al., 2014; Cockshell and Mathias, 2014; Smith et al., 1999). Patients also have described other potential triggers, such as emotional distress (Davenport et al., 2011a), physical trauma, decreased sleep quantity/quality, infection, and standing or sitting up for an extended period (FDA, 2013; Ocon et al., 2012). The type, severity, and duration of symptoms may be unexpected or seem out of proportion to the initiating trigger, which may be as mild as talking on the phone or being at the computer (Spotila, 2010). Patients report that PEM can be severe enough to render them bedridden (FDA, 2013).
Onset
Although PEM may begin immediately following a trigger, patients report that symptom exacerbation often may develop hours or days after the trigger has ceased or resolved.4 Likewise, some studies have shown that PEM may occur quickly, within 30 minutes of exertion (Blackwood et al., 1998), while others have found that patients may experience a worsening of symptoms 1 to 7 days after exertion (Nijs et al., 2010; Sorensen et al., 2003; Van Oosterwijck et al., 2010; White et al., 2010; Yoshiuchi et al., 2007). The delayed onset and functional impairment associated with PEM also is supported by actigraphy data. ME/CFS participants enrolled in a walking program designed to increase their steps by about 30 percent daily were able to reach this goal initially, but after 4 to 10 days their steps decreased precipitously (Black and McCully, 2005).
Duration
PEM is unpredictable in duration, potentially lasting hours, days, weeks, and even months (FDA, 2013; Nijs et al., 2010). After maximal exercise
____________________
3 Personal communication; public comments submitted to the IOM Committee on the Diagnostic Criteria for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome for meeting 3, 2014.
4 Ibid.
tests, ME/CFS patients experience greater fatigue compared with healthy controls (Bazelmans et al., 2005; LaManca et al., 1999b), and their fatigue and other symptoms last much longer relative to healthy active (Bazelmans et al., 2005) and sedentary controls (Davenport et al., 2011a,b; LaManca et al., 1999b; VanNess et al., 2010). In several studies, healthy controls declared themselves recovered within 24 to 48 hours after physical or cognitive exertion, whereas fewer than 31 percent of ME/CFS subjects had returned to their prestressor baseline state by this time, and as many as 60 percent were still experiencing multiple symptoms after 1 week (Cockshell and Mathias, 2014; Davenport et al., 2011b; VanNess et al., 2010).
Prevalence of PEM in ME/CFS Patients
The prevalence of PEM among ME/CFS patients as diagnosed by existing criteria varies from 69 to 100 percent (Chu et al., 2013; De Becker et al., 2001; Jason et al., 2011b; Kerr et al., 2010; Nacul et al., 2011b; Vermeulen and Scholte, 2003; Zhang et al., 2010). In a longitudinal study that followed a random, community-based sample for 10 years, 100 percent of participants fulfilling the Fukuda definition reported PEM as a symptom at some point during their illness (Jason et al., 2011b), even though the Fukuda definition does not require PEM for diagnosis. Prevalence estimates of PEM vary for two major reasons: (1) some studies use ME/CFS case definitions that require PEM, while others list it as an optional symptom; and (2) the way PEM is defined, operationalized, or queried for can affect how patients interpret the concept of PEM and whether they endorse it (Jason et al., 1999, 2004, 2014).
The prevalence of PEM in healthy control subjects is considerably lower than in ME/CFS patients, ranging from 4 to 8 percent (Hawk et al., 2006b; Jason et al., 2011b; Kerr et al., 2010; Komaroff et al., 1996b; Zhang et al., 2010). Jason and colleagues (2013b) found that a greater percentage of ME/CFS patients than healthy controls experienced PEM symptoms (see Figure 4-1). After moderate thresholds for frequency and severity were applied, the percentage of controls who endorsed PEM decreased further, from 7 to 19 percent to 2 to 7 percent.5 Thus, applying increased severity or frequency thresholds for PEM may assist in identifying patients with ME/CFS (Hawk et al., 2006b).
A few studies that compared ME/CFS with other diseases found that, although PEM was experienced by 19 to 20 percent of subjects with major
____________________
5 Jason and colleagues (2013b) compared 236 ME/CFS patients with 86 healthy controls who completed the DePaul Symptom Questionnaire, rating the frequency and severity of 54 symptoms. Patient data were obtained from the SolveCFS BioBank, which includes patients diagnosed by a licensed physician using either the Fukuda definition or the CCC.
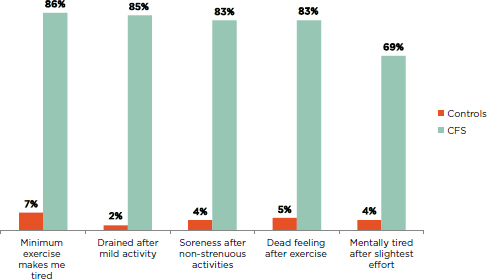
FIGURE 4-1 Percentage of ME/CFS patients and healthy controls reporting PEM symptoms of at least moderate severity that occurred at least half of the time during the past 6 months.
NOTE: All patients fulfilled the Fukuda definition for CFS.
SOURCE: Jason et al., 2013b.
depressive disorder (Hawk et al., 2006a; Komaroff et al., 1996b) and 52 percent of patients with multiple sclerosis (Komaroff et al., 1996b), it was still much more common in ME/CFS patients than in comparison groups. One study found that 64 percent of patients with major depressive disorder experienced PEM, but the authors did not describe how PEM was assessed (Zhang et al., 2010). As mentioned earlier, these prevalence estimates may vary depending on how PEM was defined and queried for, and thus they need to be interpreted with caution.
Assessment of PEM in ME/CFS
PEM can be assessed subjectively by clinical history. It also can be assessed by standardized symptom questionnaires specific to ME/CFS and by comparison of self-reported symptoms and objective measures (such as functional impairment) before and after exertion or other types of stressors. Instruments and tools for individually assessing various symptoms exacerbated by PEM triggers are discussed in other sections of this chapter. This section is focused on questionnaires and objective tests used to determine whether a patient experiences PEM. Self-report questionnaires currently
are the more readily available way to assess whether a patient experiences PEM. Objective testing for PEM generally is costly and not easily accessible, and it may worsen the patient’s condition (Diamond, 2007; Nijs et al., 2010).
Self-Report Measures of PEM
Standardized symptom questionnaires with self-report items used to assess PEM include the CFS Medical Questionnaire (Komaroff et al., 1996c), CFS Screening Questionnaire (Jason et al., 1997), Centers for Disease Control and Prevention (CDC) Symptom Inventory (SI) (CDC, 2005), ME/CFS Fatigue Types Questionnaire (MFTQ) (Jason et al., 2009), and DePaul Symptom Questionnaire (DePaul Research Team, 2010). These questionnaires, which include items designed to measure the presence, duration, frequency, or severity of PEM, were developed from patient input to query specifically about PEM, and some were tested for psychometric properties (Hawk et al., 2006b; Wagner et al., 2005). However, they have been used primarily for subject recruitment in research, for comparison of diagnoses in research protocols, or for epidemiological assessments.
Use of a standardized instrument is critical to measuring PEM accurately because slight differences in wording on various self-report items have been shown to change the prevalence of PEM in the same group of patients (Jason et al., in press); thus, how one asks about PEM can influence the responses. As indicated earlier in this chapter, individual experiences of PEM may vary widely in terms of triggers, onset, duration, severity, impairment, and symptoms that are exacerbated. For example, patients for whom normal daily activities, such as unloading the dishwasher, trigger PEM may not engage in exercise. Thus, an item that asks about fatigue after exercise will not capture these patients’ experiences with PEM. Similarly, responses to this item will not indicate PEM in patients who experience symptom exacerbation after cognitive exertion (Jason et al., in press). Thus, development of a sufficiently inclusive but probing clinical instrument is essential.
Objective Measures of PEM
Emerging evidence for objective indicators that may help us understand the presentation of PEM in ME/CFS patients centers on the two commonly reported domains in the PEM complex: recovery after physical exertion and cognitive function. Objective assessment of cognitive function is discussed in the section on neurocognitive manifestations later in this chapter.
One common characteristic of PEM is delayed ability to return to prior levels of physical capacity after physical exertion. One way to have them demonstrate this delayed lack of recovery in patients with ME/CFS is to
have them perform two cardiopulmonary exercise tests (CPETs) separated by 24 hours—the first to assess current level of function and elicit illness relapse (CPET 1) and the second to measure changes in exercise capacity due to the challenge (CPET 2) (Keller et al., 2014; Snell et al., 2013; Vermeulen et al., 2010). However, the committee emphasizes that the CPET is not required to diagnose patients with ME/CFS. Further, this test carries substantial risk for these patients as it may worsen their condition (Nijs et al., 2010; VanNess et al., 2010).
The CPET is used clinically to assess exercise capacity (maximal oxygen consumption or VO2max) and predict outcomes in cardiac patients. VO2max measured during repeated CPETs is both reliable (test-retest difference < 7 percent) (Katch et al., 1982; Taylor et al., 1955; Weltman et al., 1990) and reproducible (r > 0.95-0.99) (Balady et al., 2010; Bruce et al., 1973; Taylor et al., 1955). Several studies have found that, despite meeting objective indicators of maximal effort during both CPETs, ME/CFS patients have significantly lower results on CPET 2 than on CPET 1 on one or more of the following parameters: VO2max (Keller et al., 2014; VanNess et al., 2007; Vermeulen et al., 2010), VO2 at ventilatory threshold (Keller et al., 2014), and maximal workload or workload at ventilatory threshold (Keller et al., 2014; Snell et al., 2013). These findings support the 2-day CPET protocol as an objective indicator that physical exertion may decrease subsequent function in some ME/CFS patients.
By contrast, a single CPET may be insufficient to document the abnormal response of ME/CFS patients to exercise (Keller et al., 2014; Snell et al., 2013). Although some ME/CFS subjects show very low VO2max results on a single CPET, others may show results similar to or only slightly lower than those of healthy sedentary controls (Cook et al., 2012; De Becker et al., 2000; Farquhar et al., 2002; Inbar et al., 2001; Sargent et al., 2002; VanNess et al., 2007). Thus, the functional capacity of a patient may be erroneously overestimated and decreased values attributed only to deconditioning. Repeating the CPET will guard against such misperceptions given that deconditioned but healthy persons are able to replicate their results, even if low, on the second CPET.
Evidence for PEM in ME/CFS
The committee conducted a targeted literature search to identify research comparing self-reported or objectively assessed PEM in ME/CFS subjects and in those without the illness. The methodology used is described in Chapter 1. The findings from the literature are described below, but there are several limitations to consider when interpreting the evidence base, as described at the beginning of this chapter.
Exacerbation of Fatigue Following Exertion
Many studies found that fatigue increased and was prolonged after a physical stressor to a greater extent in ME/CFS patients than in healthy or sedentary controls. Findings of increased fatigue were consistent across different types of physical stressors, including subsequent maximal exercise tests (Davenport et al., 2011a,b), single maximal exercise tests (Bazelmans et al., 2005; Kishi et al., 2013; LaManca et al., 1998, 1999b, 2001; Meyer et al., 2013; Togo et al., 2010; VanNess et al., 2010), and other physical stressors (Black et al., 2005; Gibson et al., 1993; Nijs et al., 2010). When studies differentiated between mental and physical fatigue, both were found to have worsened in ME/CFS patients (Light et al., 2009, 2012; White et al., 2010, 2012).
As noted earlier, cognitive exertion also may trigger increased mental and physical fatigue in ME/CFS patients (Arroll et al., 2014; Cockshell and Mathias, 2014). Mental fatigue tracks closely with physical fatigue (Light et al., 2009, 2012; Meyer et al., 2013; White et al., 2012). Subjected to a 3-hour standardized neuropsychological battery, healthy subjects experienced mental fatigue during and up to 3 hours after testing but recovered full mental energy, on average, by 7 hours posttest. In contrast, at 24 hours posttest, ME/CFS subjects continued to experience significant mental fatigue and did not return to their pretest mental energy levels for an average of 57 hours (Cockshell and Mathias, 2014).
Exacerbation of Cognitive Symptoms Following Exertion or Orthostatic Challenge
Although cognitive problems are common in ME/CFS patients, few studies have examined the effect of exertion on cognitive function. Some studies have demonstrated that a physical or orthostatic stressor may cause exacerbation of cognitive symptoms, including difficulty with concentration (Nijs et al., 2010); deficits in the speed of information processing (LaManca et al., 1998); and other self-reported cognitive problems (Meyer et al., 2013; VanNess et al., 2010). Studies also have shown decreased cognitive performance, such as on tests of focused and sustained attention, the Symbol Digit Modalities Test, the Stroop test, and the N-back task (Blackwood et al., 1998; LaManca et al., 2001; Ocon et al., 2012). Findings of other studies, however, suggest that cognitive problems do not worsen after physical exertion (Claypoole et al., 2001; Cook et al., 2005; Yoshiuchi et al., 2007).
Cognitive exertion also may trigger cognitive symptoms (Capuron et al., 2006; Ocon et al., 2012). For example, one study asked ME/CFS subjects and healthy controls to complete computerized tests of memory, at-
tention, and psychomotor function and found that as the tests progressed, the performance of the ME/CFS subjects worsened significantly more than that of controls (Smith et al., 1999). On the other hand, the findings of some studies suggest that cognitive exertion alone may not necessarily trigger cognitive problems (LaManca et al., 1998; Marshall et al., 1997). These inconsistent results may be attributable to variations in subject selection, exercise testing procedures, and cognitive testing, which inhibit direct comparisons among studies.
Exacerbation of Pain Following Exertion
Many studies have demonstrated that pain is increased and prolonged after a physical stressor in ME/CFS subjects compared with healthy or sedentary controls. Similar to the evidence base for fatigue, reports of increased pain among ME/CFS subjects are consistent across maximal exercise tests (Davenport et al., 2011a,b; VanNess et al., 2010) and other physical stressors (Black et al., 2005; Nijs et al., 2010). In at least two studies, though, the increase in pain after exertion among ME/CFS subjects was not statistically significant compared with controls (Bazelmans et al., 2005; Kishi et al., 2013).
Effect of Exertion on Other Outcomes
In addition to the strong evidence demonstrating post-exertional effects on fatigue status, cognitive function, and pain, evidence is mounting for other symptoms and outcomes, albeit from a lesser number of studies to date. After an exercise stressor, ME/CFS patients compared with healthy controls demonstrated delayed recovery of muscle function and pH (Jones et al., 2010, 2012; Paul et al., 1999), increased depression or mood disturbances (Arroll et al., 2014; Meyer et al., 2013), inappropriate autonomic responses (Cordero et al., 1996; LaManca et al., 2001), and amplification of problems with sleep (Davenport et al., 2011a,b; Kishi et al., 2013; Togo et al., 2010). Further studies confirming the different expression of genes (Light et al., 2009, 2012; Meyer et al., 2013; White et al., 2012) and immune biomarkers (Maes et al., 2012; Nijs et al., 2010, 2014; Sorensen et al., 2003; White et al., 2010) in patients with ME/CFS in response to physical exertion may help us to better understanding the pathophysiology of PEM.
PEM as a Characteristic Symptom of ME/CFS
The existence of PEM can help physicians confirm a diagnosis of ME/CFS earlier rather than only after extensive exclusion of other conditions. Several studies have found that PEM best distinguishes ME/CFS from idio-
pathic chronic fatigue (Baraniuk et al., 2013; Jason et al., 2002a) and may help distinguish it from other fatiguing conditions with a lower frequency of PEM, such as multiple sclerosis and major depressive disorder (Hawk et al., 2006a; Komaroff et al., 1996b). Further, PEM may be an important prognostic indicator because its continued presence or increased duration predicts a poorer outcome for ME/CFS patients (Taylor et al., 2002).
Summary
PEM is a worsening of a patient’s symptoms and function after exposure to physical or cognitive stressors that were normally tolerated before disease onset. Subjective reports of PEM and prolonged recovery are supported by objective evidence, including failure to normally reproduce exercise test results (2-day CPET) and impaired cognitive function. These objective indices track strongly with the presence, severity, and duration of PEM.
Patients’ experience of PEM varies, and some patients may have adapted their lifestyle and activity level to avoid triggering symptoms. As a result, health care providers should ask a range of questions (see Chapter 7, Table 7-1) to determine whether PEM is present. Minimally, patients should be asked to describe baseline symptoms, the effects of physical or cognitive exertion, the time needed to recover to the pre-exertion state, and how they have limited their activities to avoid these effects. If the patient is unable to answer these questions clearly, health care providers may also ask the patient to track symptoms, activities, and rest in a diary—for example, in order to identify PEM patterns.
Conclusion: There is sufficient evidence that PEM is a primary feature that helps distinguish ME/CFS from other conditions.
Description of Sleep-Related Symptoms in ME/CFS
Patients with ME/CFS frequently experience sleep-related problems such as insomnia, sleep disturbances, unrefreshing sleep, and nonrestorative sleep (FDA, 2013; Fossey et al., 2004). These symptoms are included in all existing ME/CFS case definitions and diagnostic criteria (see Chapter 3). Unrefreshing sleep, or feeling as tired upon waking as before going to bed, is among the most common symptoms reported by ME/CFS patients, and only a small percentage of patients diagnosed with ME/CFS fail to report some type of sleep dysfunction (Carruthers et al., 2003; IACFS/ME, 2014; Jason et al., 2013b). This section summarizes the evidence on sleep-related signs and symptoms in ME/CFS reviewed by the committee to determine
whether such symptoms should be a component of its recommended diagnostic criteria for ME/CFS.
ME/CFS patients are more likely than healthy controls to experience sleep-related symptoms occurring at least half of the time and of at least moderate severity (see Figure 4-2) (Jason et al., 2013b). Although sleep-related symptoms also are reported by healthy persons and by chronically fatigued persons who do not fulfill ME/CFS criteria, a greater percentage of people fulfilling ME/CFS criteria report unrefreshing sleep, sleep disturbances, and difficulties falling asleep or waking up early in the morning (Komaroff et al., 1996a; Krupp et al., 1993; Nisenbaum et al., 2004) relative to these other groups.
Sleep-related complaints may change throughout the course of the illness. For example, one study found that in the first few months of the illness, ME/CFS patients complain of hypersomnia, but as the disease progresses, they have trouble staying asleep (Morriss et al., 1997). A cross-sectional study of randomly selected patients found that sleep-related symptoms may become less frequent over the course of the illness (Nisenbaum et al.,
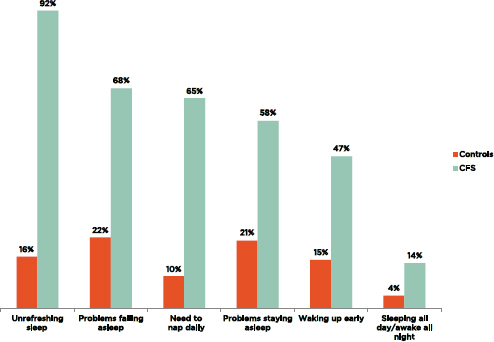
FIGURE 4-2 Percentage of ME/CFS patients and healthy controls reporting sleep-related symptoms of at least moderate severity that occurred at least half of the time during the past 6 months.
NOTE: All patients fulfilled the Fukuda definition for CFS.
SOURCE: Jason et al., 2013b.
2003); however, this may be due to behavioral adaptation or changes in sleep medication.
Sleep-related symptoms are listed differently in the various diagnostic criteria for ME/CFS (see Box 4-1), and there is conflicting evidence on whether ME/CFS patients fulfilling different diagnostic criteria experience sleep-related symptoms differently. Those fulfilling the CCC reported significantly worse (in terms of frequency and severity, p < 0.05) unrefreshing sleep (Jason et al., 2012a, 2013a) and more difficulty falling asleep (Jason et al., 2012a) relative to those fulfilling the Fukuda definition. Similarly, another
BOX 4-1
Sleep-Related Symptoms in Case Definitions and Diagnostic Criteria for ME/CFS
1994 Fukuda Case Definition of CFS (Fukuda et al., 1994)
- Unrefreshing sleep is a minor criterion (not required).
- Sleep apnea and narcolepsy are exclusionary conditions (as they are conditions that explain chronic fatigue).
Canadian Consensus Criteria for ME/CFS (Carruthers et al., 2003, p. 16)
- Sleep dysfunction, including unrefreshing sleep or sleep quantity or rhythm disturbances such as reversed or chaotic diurnal sleep rhythms, is a required criterion for diagnosis. “Loss of the deeper phases of sleep is especially characteristic, with frequent awakenings, and loss of restorative feelings in the morning. Restless leg syndrome and periodic limb movement disorder often accompany sleep disturbance.”
- “It is important to rule out treatable sleep disorders such as upper airway resistance syndrome, obstructive and central sleep apnea and restless leg syndrome.”
2011 International Consensus Criteria for ME (Carruthers et al., 2011, p. 330)
- Sleep disturbance is a minor criterion (not required), which includes
- – disturbed sleep patterns, such as insomnia, prolonged sleep including naps, sleeping most of the day and being awake most of the night, frequent awakenings, awaking much earlier than before illness onset, and vivid dreams/nightmares; and
- – unrefreshing sleep, such as awakening feeling exhausted regardless of duration of sleep and daytime sleepiness.
- “Sleep disturbances are typically expressed by prolonged sleep, sometimes extreme, in the acute phase and often evolve into marked sleep reversal in the chronic stage.”
study found that patients fulfilling the International Consensus Criteria for ME (ME-ICC) reported significantly worse symptom scores for unrefreshing sleep, need to nap during each day, difficulty falling asleep, and difficulty staying asleep relative to those fulfilling the Fukuda definition (Brown et al., 2013). In contrast to these results, however, are those from two other studies. One study found that more patients fulfilling the Fukuda definition reported greater difficulty staying asleep than those fulfilling the CCC (Jason et al., 2004), while a second study reported no significant differences in sleep-related symptom scores between patients fulfilling the Fukuda definition and those fulfilling the ME-ICC (Jason et al., 2014). Regardless, it is clear that all the major diagnostic criteria include sleep-related symptoms.
Chronic fatigue may be caused by sleep disorders; thus, most diagnostic criteria for ME/CFS require ruling out primary or treatable sleep disorders before a diagnosis of ME/CFS can be made (see Box 4-1). Sleep apnea—whether obstructive, central, or undefined—is an exclusionary condition in several criteria, but there is less consistency regarding whether other sleep disorders, such as narcolepsy or the spectrum of obstructive or central sleep disorders, truly exclude ME/CFS (Carruthers et al., 2003; Fukuda et al., 1994; Jason et al., 2010b; NICE, 2007). Some researchers have noted that the inclusion of unrefreshing or nonrestorative sleep as a case-defining symptom, combined with listing sleep disorders as exclusionary conditions, may confuse the diagnosis and management of ME/CFS (Mariman et al., 2012; Unger et al., 2004).
Assessment of Sleep-Related Symptoms in ME/CFS
Taking a careful history of sleep complaints can help a clinician identify whether objective testing of patients with such complaints is indicated. As noted above, sleep-related symptoms may change over time in ME/CFS patients, and it is possible for sleep disorders to develop over the course of the illness (Morriss et al., 1997; Nisenbaum et al., 2003; Reeves et al., 2006). Furthermore, it is plausible that the development of other symptoms, such as pain or headache, over time may cause or contribute to sleep disorders, or that the development of a primary sleep disorder leads to widespread pain. Also, many ME/CFS patients are prescribed medications that may improve or worsen sleep-related symptoms (Armitage, 1999; Foral et al., 2011; Kierlin and Littner, 2011; Trivedi et al., 1999).
Patients reporting symptoms of primary sleep disorders should be thoroughly evaluated to identify or rule out these conditions, as diagnosis and treatment of primary sleep disorders may be effective in reducing or relieving such symptoms (Qanneta, 2013; Reeves et al., 2006). Identifying insomnia in some patients may be useful therapeutically because techniques known to alleviate insomnia have been shown to be effective in fibromy-
algia, a comorbid condition occurring in some ME/CFS patients (Edinger et al., 2005).
Several questionnaires exist with which to capture patient-reported sleep symptoms and assess the subjective quality of sleep or sleep-related symptoms, although readily accessible clinical tools are not easy to find. The DePaul Symptom Questionnaire includes several items that can be used to assess the frequency and severity of symptoms that indicate sleep dysfunction in ME/CFS patients (DePaul Research Team, 2010). The Sleep Assessment Questionnaire© also has been found to describe sleep abnormalities experienced by ME/CFS patients (Unger et al., 2004). And although not developed specifically for ME/CFS, the Pittsburgh Sleep Quality Index (PSQI) is a validated tool for assessing subjective sleep quality (Buysse et al., 1989).
It is important to consider frequency and severity thresholds when assessing subjective sleep complaints. In a study using the DePaul Symptom Questionnaire, for example, 65 percent of healthy controls reported unrefreshing sleep that occurred with mild severity at least a little of the time, yet only 16 percent of healthy controls reported unrefreshing sleep that occurred with moderate severity at least half of the time (Jason et al., 2013b). The percentages of ME/CFS patients reporting unrefreshing sleep at the same thresholds were 99 and 92 percent, respectively.
Complaints of sleepiness or fatigue so severe as to result in a substantial decrease in activity often lead to referral to a sleep laboratory for evaluation of underlying sleep pathology. Polysomnography (PSG), the continuous monitoring of variables that define sleep states and stages, is a type of sleep study used to diagnose sleep disorders such as sleep apnea and narcolepsy (Kasper et al., 2005; Kushida et al., 2005). Sleepiness usually is the driving symptom for referral for PSG, yet many ME/CFS patients do not undergo sleep studies because they report being fatigued rather than being sleepy (Spitzer and Broadman, 2010a). And although PSG can be useful for diagnosing primary sleep disorders that are often comorbid with ME/CFS, many ME/CFS patients have normal sleep studies despite complaining of nonrestorative sleep (Reeves et al., 2006).
Recently, new ways of assessing sleep quality have emerged and have been applied to assess these abnormalities in ME/CFS patients. The classic method for assessing sleep is to record the electroencephalogram (EEG) of a patient every 30 seconds to determine the stage of sleep (Kushida et al., 2005). In contrast, one new method uses the actual waveform of the EEG and determines power at different frequencies (Armitage et al., 2007; Duffy et al., 2011). Another new approach assesses transitions between sleep stages and determines the probability of occurrence of each transition (Kishi et al., 2008).
PSG requires spending the night in a sleep laboratory, which limits its
use to those who are willing and able to travel to the laboratory for testing. PSG also may be less accessible in nonurban areas or too costly to include in a routine assessment (Oliveira et al., 2014; Rosen et al., 2012). However, home-based recording is a possibility. Moreover, the development of ambulatory monitoring methods, such as wrist actigraphy, may increase access to these diagnostic tests (Blackman et al., 2010; Corral-Penafiel et al., 2013; Libman et al., 2009). However, this method has been normed only for healthy people (Marino et al., 2013), and its use in people with sleep problems still needs to be validated. And, of course, wrist actigraphy cannot be used to evaluate patients for conditions such as sleep apnea (Morgenthaler et al., 2007).
Evidence for Sleep-Related Symptoms in ME/CFS
The committee conducted a targeted literature search to identify research comparing self-reported or objectively assessed sleep-related symptoms and signs in ME/CFS subjects and in those without the illness. Details of the search methodology are described in Chapter 1. The findings from the literature are described below, but there are several limitations to consider when interpreting the evidence base, in addition to those discussed earlier.
In general, the design and implementation of these studies was highly heterogeneous. Most articles document case-control studies in which symptoms or signs were compared in groups of subjects with and without ME/CFS. Most studies used healthy controls as a comparison group, and several compared twin pairs in which one twin was diagnosed with ME/CFS and the other was healthy. Fewer studies used controls affected by other illnesses. The studies assessed varied outcomes of interest. Self-reported symptoms were assessed with many different questionnaires and scales. Several studies used PSG, but many used different testing protocols or diagnostic thresholds for sleep disorders.
As with other literature on ME/CFS, the use of different diagnostic criteria for patient selection limits comparisons across studies. In particular, because of the variations in diagnostic criteria for ME/CFS, some studies excluded patients with primary sleep disorders, while others included them. The following subsections describe in turn the evidence for primary sleep disorders in patients with ME/CFS and the evidence for sleep abnormalities in patients with ME/CFS that do not have primary sleep disorders. Note that for many studies, it was unclear whether ME/CFS patients with sleep disorders were included or excluded; these studies are not discussed below.
Sleep Disorders in ME/CFS Patients
Many of the sleep-related symptoms reported by ME/CFS patients—difficulty falling asleep, frequent or sustained awakenings, early-morning awakenings, and nonrestorative or unrefreshing sleep (persistent sleepiness despite sleep of adequate duration)—are types of insomnia (Kasper et al., 2005; Watson et al., 2003). Insomnia can have many causes, including other sleep disorders, such as sensory motor disorders (restless leg syndrome and periodic limb movement disorder), narcolepsy, and sleep disordered breathing (SDB). SDB constitutes a spectrum of breathing problems during sleep that range from subtle changes in the pattern of breathing to more severe snoring and obstructive sleep apnea. These disorders may result in multiple arousals during sleep, which can produce the daytime symptoms of sleepiness or fatigue (Cowan et al., 2014).
Primary sleep disorders are fairly common in ME/CFS patients, with prevalence ranging from 19 to 69 percent (Creti et al., 2010; Gotts et al., 2013; Le Bon et al., 2000; Reeves et al., 2006). Studies have found sleep apnea/hypopnea syndrome to be present in 13 to 65 percent of patients, followed by periodic limb movement disorder (4 to 25 percent), narcolepsy (5 to 7 percent), and restless leg syndrome (4 percent) (Creti et al., 2010; Gotts et al., 2013; Le Bon et al., 2000; Reeves et al., 2006). Effective treatments are available for many of these sleep disorders, but there is little evidence on the effectiveness of these interventions in reducing the sleep-related symptoms of ME/CFS aside from those caused by the sleep disorder. Continuous positive airway pressure (CPAP) is a common treatment for SDB, and while it has been shown to reduce fatigue and sleepiness in people with obstructive sleep apnea (Tomfohr et al., 2011), reports of its improving ME/CFS symptoms are limited (Qanneta, 2014). One study of CPAP treatment in ME/CFS patients with sleep apnea/hypopnea syndrome (SAHS), a condition within the spectrum of SDB, found no difference in sleep-related symptoms between patients who were and were not compliant with the CPAP treatment. Further, there were no significant differences in symptoms, quality of life, or activity levels between ME/CFS patients with and without SAHS (Libman et al., 2009).
One inference from these few studies is that sleep disorders can be considered an exclusionary diagnosis for ME/CFS only if treatment of the sleep disorder cures the ME/CFS symptoms. Some researchers have suggested that sleep disorders should be considered comorbid conditions rather than exclusionary criteria for a diagnosis of ME/CFS (Jackson and Bruck, 2012; Libman et al., 2009). Studies comparing clinical presentation in ME/CFS patients with and without sleep disorders have found no differences between the two groups (Le Bon et al., 2000; Libman et al., 2009),
but greater functional impairment has been reported in ME/CFS patients with some sleep disorders (Morriss et al., 1993).
Studies that included ME/CFS patients with sleep disorders have found other objective abnormalities during sleep studies. One study found mean sleep latency to be greater in ME/CFS patients than in healthy controls (Bailes et al., 2006). Another found that ME/CFS patients spent less total time than controls in rapid eye movement (REM) sleep (Whelton et al., 1992). And in another study, ME/CFS patients compared with controls experienced significantly lower sleep efficiency—the ratio between sleep time and total recording time—and significantly more time awake after falling asleep (Morriss et al., 1993); these results have been replicated (Togo et al., 2008).
ME/CFS Patients Without Sleep Disorders
The studies described below excluded ME/CFS subjects that had previously been diagnosed with a sleep disorder. The authors of most of these studies explicitly describe their exclusion criteria, but studies also are included below if they selected participants that fulfilled the Fukuda definition for CFS, because sleep apnea and narcolepsy are exclusionary conditions. The selection criteria also may have differed in other ways (e.g., medication status), and the study designs (e.g., the type of control group) may have varied as well.
Subjective evidence Most of these studies found that ME/CFS patients without sleep disorders reported significantly more subjective sleep complaints than controls, but as described later, many failed to find major differences in objective measures of sleep (Majer et al., 2007; Reeves et al., 2006; Watson et al., 2004). More ME/CFS patients than controls reported unrefreshing sleep (Majer et al., 2007; Reeves et al., 2006) and problems sleeping (Majer et al., 2007). Self-reported sleep quality was significantly worse in ME/CFS patients than in healthy controls as measured by the PSQI (Le Bon et al., 2012; Neu et al., 2007, 2011; Rahman et al., 2011) and other questionnaires (Majer et al., 2007; Watson et al., 2004). PSQI sleep quality scores, however, were not associated with objective measures of sleep quality (Neu et al., 2007). ME/CFS patients also reported significantly more fatigue and sleepiness than healthy controls (Le Bon et al., 2012).
Objective evidence A number of studies have compared sleep parameters measured through PSG in ME/CFS patients and healthy controls; however, comparisons across studies are difficult to make because of the use of various case definitions and methods of measurement. One study examined pairs of twins in which one twin had ME/CFS and the other was healthy.
Compared with the healthy twins, the twins with ME/CFS reported more subjective complaints of insomnia, but objective measures of sleep were “remarkably similar” (Watson et al., 2003). Other studies generally have found only minor objective differences between ME/CFS patients and suitable comparison groups (Armitage et al., 2009; Majer et al., 2007; Neu et al., 2007; Reeves et al., 2006) or differences that were not statistically significant (Ball et al., 2004; Le Bon et al., 2007; Sharpley et al., 1997). These studies found that ME/CFS patients had decreased total sleep time, resulting in decreased sleep efficiency and less time spent in deep sleep, with some evidence for disturbed sleep in the form of more arousals and longer periods of being awake after sleep onset.
There is growing evidence that ME/CFS patients experience abnormal sleep continuation compared with healthy controls. In one study, ME/CFS patients had higher levels of microarousal, despite the study’s exclusion of sleep disorders normally associated with microarousals (Neu et al., 2008). A study of sleep transitions also found that ME/CFS patients were more likely than normal controls to awaken during sleep, especially during the later hours of sleep (Kishi et al., 2008).
The use of stratification strategies may help. One study stratified on sleep latency and sleep time to propose different sleep phenotypes (Gotts et al., 2013). Another stratified patients according to whether they felt more or less sleepy the morning after versus the night before the sleep study (Togo et al., 2008). The patients who reported feeling less sleepy had normal PSG, while those who reported feeling more sleepy showed evidence of more disrupted sleep. Also, in a follow-up study conducted after subjects had performed a stress test, patients who reported being less sleepy after a night of sleep had normal PSG, while those who reported feeling more sleepy were the group with sleep disruption (Togo et al., 2010).
Multiple sleep latency tests (MSLTs) may be used to measure objective daytime sleepiness, which is characteristic of narcolepsy. Subjects are asked to nap, and the time it takes them to fall asleep—latency to nap—is measured several times during the day and averaged to determine a mean sleep latency for naps (Johns, 2000). A shortened latency to nap is indicative of increased sleepiness. One group of researchers found shortened latency to nap in ME/CFS patients compared with healthy controls (Neu et al., 2008; Watson et al., 2004), while others have failed to find significant differences (Majer et al., 2007; Reeves et al., 2006). The results of these studies suggest that narcolepsy is not a significant factor in ME/CFS. Supporting that conclusion is one study reporting an opposite result after a night of sleep deprivation. While one would expect this manipulation to result in short sleep latencies, the researchers found that one-third of the patients had difficulty falling asleep (Nakamura et al., 2010b). Such an outcome is consistent with the idea that the sleep disruption of some ME/CFS patients may reflect
a problem with sleep initiation and maintenance. It is important to note that MSLT can be used reliably to diagnose narcolepsy only when patients are in a stable state off potentially sedating medications (Thorpy, 1992).
Subsets
To study more homogeneous groups of patients, some researchers have examined sleep characteristics in different subgroups of ME/CFS patients. As an example, ME/CFS patients who also had postural orthostatic tachycardia syndrome (POTS) were found to have reduced daytime hypersomnolence compared with those without POTS (Lewis et al., 2013).
Chronic pain is a common factor in sleep disorders resulting from a medical condition (Fishbain et al., 2010). A frequent cause of chronic widespread pain is fibromyalgia (FM)—a diagnosis that has substantial overlap with ME/CFS (Ciccone and Natelson, 2003). Several studies have compared evidence in ME/CFS patients with FM (CFS+FM) and those without FM (CFS only). In one study, FM was less frequent among ME/CFS patients with objective sleepiness as measured by short MSLT (< 10 minutes) (Le Bon et al., 2000). Some studies have found no differences in sleep parameters as measured through PSG between CFS+FM and CFS-only patients (Fischler et al., 1997; Spitzer and Broadman, 2010a,b).6 A study examining sleep-stage dynamics found differences between CFS+FM and CFS-only groups in transition probabilities and rates among sleep stages (Kishi et al., 2011). In CFS-only patients, the probability of transition from REM sleep to awake was significantly greater than in healthy controls. CFS+FM patients experienced significantly greater probabilities and rates of transition from waking, REM sleep, and S1 to S2, as well as greater probabilities and rates of transition from slow wave sleep (SWS) to waking and S1. Thus, CFS-only patients differed from those with CFS+FM. Another study found evidence of increased IL-10, an anti-inflammatory cytokine that may contribute to disrupted sleep, during the sleep of CFS-only but not CFS+FM patients (Nakamura et al., 2010a); however, the magnitude of the difference was small. The role of cytokines in regulating sleep in ME/CFS remains a research question.
Summary
Standard sleep studies are not substantially abnormal in people with ME/CFS. Several studies have found differences in sleep architecture in subsets of people with ME/CFS and in people with ME/CFS compared with healthy controls (Whelton et al., 1992), yet the current evidence base is not
____________________
6 Fischler and colleagues (1997) did not exclude sleep disorders.
strong enough to identify ME/CFS-specific sleep pathology. It is clear, however, that people with ME/CFS universally report experiencing unrefreshing sleep, and further research will be important to determine whether there is a specific sleep abnormality common to ME/CFS patients or a heterogeneity of abnormalities that may define subsets of ME/CFS patients.
In several case definitions and diagnostic criteria for ME/CFS, primary treatable sleep disorders such as sleep apnea and narcolepsy are listed as exclusionary criteria for an ME/CFS diagnosis. However, there is evidence to suggest that primary sleep disorders should be considered important comorbid conditions in the differential diagnosis and that sleep complaints are complex. Further, there is little evidence that treatment of primary sleep disorders improves ME/CFS symptoms rather than simply reduces symptoms of the comorbid disorder.
Conclusion: Despite the absence of an objective alteration in sleep architecture, the data are strong that the complaint of unrefreshing sleep is universal among patients with ME/CFS when questions about sleep specifically address this issue. While PSG is not required to diagnose ME/CFS, its use to screen for treatable sleep disorders when indicated is appropriate. Diagnosis of a primary sleep disorder does not rule out a diagnosis of ME/CFS.
Description of Neurocognitive Manifestations in ME/CFS
Impairments in cognitive functioning are one of the most frequently reported symptoms of ME/CFS. Patients describe these symptoms as debilitating and as affecting function as much as the physical symptoms that accompany this disease. During a survey of ME/CFS patients, descriptions of neurocognitive manifestations included, among others, “brain fog,” “confusion,” disorientation,” “hard to concentrate, can’t focus,” “inability to process information,” “inability to multitask,” and “short-term memory loss” (FDA, 2013). The short-term memory problems of ME/CFS patients include difficulty remembering something they just read. Patients usually report slowed information processing and impaired psychomotor functioning in more general terms as overall mental fatigue or slowed thinking (Constant et al., 2011; Larun and Malterud, 2007). In more severe cases, patients have difficulty completing tasks that require sustained attention and report problems performing even relatively simple activities such as watching television (FDA, 2013). Studies of the exact nature of neurocognitive deficits reported by patients with ME/CFS have shown that some patients meeting various current criteria for ME/CFS have different or
more severe impairments than others, but also that self-reported severity of impairments is not always associated with severity based on objective measures (Cockshell and Mathias, 2013).
Prevalence of Neurocognitive Manifestations in ME/CFS Patients
Estimates of the prevalence of neurocognitive manifestations in ME/CFS patients vary as a result of the different definitions used in research and the assessment of these manifestations using patient reports. The 2003 CCC, 2010 Revised CCC, and 2011 ME-ICC require the presence of neurological/cognitive manifestations for a diagnosis of ME/CFS, while the 1994 Fukuda definition and 2007 British National Institute for Health and Clinical Excellence (NICE) Clinical Guidelines do not. Moreover, these various case definitions and diagnostic criteria are inconsistent in the manifestations or symptoms listed for this category. For instance, the Fukuda definition includes only “impaired memory or concentration” as one optional criterion, while the CCC requires the presence of two or more difficulties from a more extensive list of cognitive (confusion, impairment of concentration and short-term memory consolidation, disorientation, difficulty with information processing) or neurologic (perceptual and sensory disturbances, ataxia, muscle weakness, and fasciculations) manifestations.
A study conducted in Belgium in a population of patients with chronic fatigue found a prevalence of 93 percent for attention deficit, 85.6 percent for memory disturbance, and 75.5 percent for difficulties with words for those fulfilling the Fukuda definition (De Becker et al., 2001). When applying frequency and severity scores of at least 2, Jason and colleagues (2013b) found that a greater percentage of ME/CFS patients than healthy controls reported neurocognitive symptoms of at least moderate severity that occurred at least half of the time (see Figure 4-3).
Assessment of Neurocognitive Manifestations in ME/CFS
Measurement of cognitive functioning is a challenge for researchers. While theoretical distinctions often are made among areas of cognition, such as memory, attention, and motor functioning, there presently are no “pure” measures that can directly test different areas of cognition individually rather than in the aggregate. Thus, while results of a specific neuropsychological test may be interpreted as evidence of a particular cognitive deficit, such as poor working memory, it is likely that any given test is actually measuring multiple aspects of cognitive function simultaneously.
Additionally, an important distinction must be made between objective measures of cognitive deficits, which measure participants’ performance on cognitively demanding tasks, and subjective measures of cognitive func-
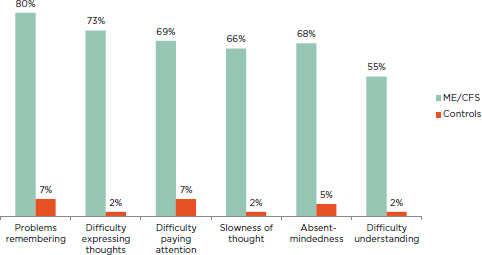
FIGURE 4-3 Percentage of ME/CFS patients and healthy controls reporting neurocognitive manifestations of at least moderate severity that occurred at least half of the time during the past 6 months.
NOTE: All patients fulfilled the Fukuda definition for CFS.
SOURCE: Jason et al., 2013b.
tioning that ask individuals to report cognitive difficulties they encounter in their daily lives. Both objective and subjective measures are important in understanding ME/CFS, but in the following discussion of evidence on the neurocognitive characteristics of ME/CFS, the committee has chosen to focus primarily on objective tests that may provide some indication of the cognitive processes and possible causal mechanisms involved in ME/CFS. It is worth noting, however, that from the clinical perspective, neuropsychological testing has shown significant overlap between ME/CFS and control populations, and that self-report of cognitive issues offers a more reliable means of discriminating between these two groups (Cockshell and Mathias, 2010).
Most studies focused on memory impairments test patients’ working memory (the ability to retain and make use of information in the short term) as measured by a range of neuropsychological tests. Researchers also divide memory tasks into various categories based on whether a task requires immediate (also related to working memory), short-term, or long-term memory; remembering something that has already happened (retrospective memory); or remembering to do something in the future (prospective memory). Tasks are divided as well by the type of content that is recalled (verbal or visual memory) (Attree et al., 2014; DeLuca et
al., 1995). Subjective measures used for memory testing include a range of different assessments, such as the Prospective and Retrospective Memory Questionnaire, the Cognitive Failures Questionnaire, or self-observation using a structured diary (Attree et al., 2014; Knoop et al., 2007). A meta-analysis of studies of cognitive functioning by Cockshell and Mathias (2010) found that the majority of objective tests used to assess memory function in ME/CFS asked participants to remember either verbal or written word lists, while some tested visual memory by having participants reproduce a complex figure from memory or remember visual patterns. Examples of verbal tests reported in the meta-analysis include the Selective Reminding Test, the Wechsler Memory Scale-Revised (WMS-R), and the California Verbal Learning Test. Tests of visual memory reviewed included, among others, the Rey Osterrieth Complex Figure and the Pattern Recognition Test. Some tests included both verbal and visual components and fell in both categories.
In addition, researchers use the n-back procedure to investigate the neurologic substrates of the working memory processes. The n-back task is a continuous performance measure whereby the subject is presented with stimulus sequences (i.e., visual, auditory, and olfactory) and is required to indicate when the current stimulus matches the one presented in “n” trials previously. This task requires the subject to maintain, update, and manipulate information and therefore is considered a demanding task. The n usually varies from 1 to 3. The responses of the n-back task can be correlated with neuroimaging reports of the activation of several brain regions (Owen et al., 2005).
In the neuropsychological literature, attempts are made to distinguish between information processing speed (as measured by reaction time) and motor speed (movement time or tests of fine motor speed [e.g., finger tapping test]). Recent studies assessing psychomotor functioning in ME/CFS have separated these components, but together these tests evaluate reaction time as part of the motor component (Schrijvers et al., 2009; Van Den Eede et al., 2011). The Paced Auditory Serial Addition Test (PASAT), the Attention Network Test (ANT), the Cambridge Neuropsychological Test Automated Battery (CANTAB), and similar measures or testing batteries are used to assess attention deficits and reaction times. Reaction times on these tests frequently are used to judge information processing speed independent of motor speed (Majer et al., 2008; Michiels and Cluydts, 2001). Impairment in psychomotor functioning is demonstrated by both increased simple reaction time, in which subjects respond to a verbal or visual stimulus, and choice reaction time, which measures length of time responding to a stimulus involving multiple potential options (Den Eede et al., 2011). The PASAT and ANT can additionally be used to assess slowed information processing (Davis and Claypoole, 1997; Togo et al., 2013).
Evidence for Neurocognitive Manifestations in ME/CFS
The committee conducted a targeted literature search to identify research papers comparing the presence of neurocognitive manifestations in ME/CFS cases versus controls. The researchers assessed presentation of neurocognitive impairments either by self-report questionnaires or by objective testing using neurocognitive test batteries. The committee’s targeted search was limited to the past 10 years because of the large number of results but considered older research that was reviewed and cited in the introduction or discussion of more recent literature. The approach the committee used to review the literature is described in Chapter 1. The findings of the targeted literature review are presented below, with the caveats regarding the research base described at the beginning of this chapter.
The literature shows with some consistency that neurocognitive problems such as memory impairment, slowed information processing, attention deficits, and impaired psychomotor function are highly prevalent in ME/CFS patients, as discussed in this section. Slowed information processing is the neurocognitive symptom of ME/CFS most consistently reported in objective neuropsychological testing, with evidence from twin studies showing that individuals with ME/CFS tend to process information more slowly than healthy individuals with similar intellectual abilities (Claypoole et al., 2007; Mahurin et al., 2004; Togo et al., 2013). Numerous papers both support and refute the existence of memory impairment in individuals with ME/CFS. Studies that do report impairment show a wide range in the measured severity of memory problems, with small to moderate and significant deficits in memory having been found for a range of cognitive tests, but not all (Cockshell and Mathias, 2010; Constant et al., 2011; Dickson et al., 2009; Majer et al., 2008). A large number of studies also have found impaired attention (Capuron et al., 2006; Cockshell and Mathias, 2010; Constant et al., 2011; Dickson et al., 2009; Hou et al., 2008, 2014; Hutchinson and Badham, 2013) and slowed reaction and movement times in people with ME/CFS (Den Eede et al., 2011; Majer et al., 2008; Schrijvers et al., 2009). Comparisons with other illnesses, such as sleep apnea and depression, suggest that psychomotor impairment in ME/CFS may be less severe than in those other illnesses (Neu et al., 2011; Schrijvers et al., 2009).
Memory Impairment
In objective neuropsychological testing, individuals meeting criteria for ME/CFS have displayed deficits in working memory compared with healthy controls. These patients have been found to be impaired on tests that assess working memory over a sustained period of time (Cockshell and Mathias, 2010; DeLuca et al., 2004b). Attree and colleagues (2009) found
that ME/CFS patients rated themselves as more forgetful than controls on both prospective and retrospective memory. However, objective memory impairment was limited to retrospective not prospective memory in these patients. Michiels and colleagues (1996) found that reduced verbal and visual memory was the most consistent finding in individuals with ME/CFS compared with normal controls.
With regard to verbal memory, moderate to large deficits were found on tests of list learning, including immediate recall, delayed recall, and recognition, while nonverbal memory for complex figures and spatial location was not impaired (Cockshell and Mathias, 2010). Numerous studies provide evidence that verbal memory impairment (often measured using the California Verbal Learning Test) likely is associated with ME/CFS (Cockshell and Mathias, 2010). However, because of the methodological weaknesses in much ME/CFS research, particularly the comparison of mean scores on neuropsychological tests rather than reporting of the number of impaired individuals, it is difficult to determine whether this impairment is characteristic of the illness or present only in a subset of patients (Vercoulen et al., 1998).
ME/CFS patients compared with controls perform significantly worse on free-recall retrospective memory. Research findings offer some support for the deficient acquisition hypothesis, which proposes that retrospective memory deficits in ME/CFS patients are attributable to difficulties with encoding information due to slower information processing (impaired delayed recall) (Attree et al., 2009). This interpretation appears to be supported by findings that the verbal memory problems of these patients stem from delayed acquisition of information rather than inaccuracy in recall (DeLuca et al., 2004a). Furthermore, in studies of working memory, researchers have found that difficulties emerge only when ME/CFS subjects are required to perform time-dependent tasks (DeLuca et al., 2004a; Togo et al., 2013), implying that ME/CFS patients’ cognitive processes may be slower than but not otherwise different from those of healthy control patients.
Memory impairment does appear to distinguish ME/CFS from such psychiatric disorders as depression and anxiety. The majority of studies examining severity of cognitive impairment, including memory problems, failed to find a relationship between such impairment and depression, even though ME/CFS patients have high rates of depression (Busichio et al., 2004; DeLuca et al., 1995; Short et al., 2002). In studies that divided ME/CFS patients according to whether they had a comorbid psychiatric condition, those without such a comorbidity showed more severe memory impairment (DeLuca et al., 2004b; Tiersky et al., 2003).
It is less clear whether memory impairment may distinguish ME/CFS from other fatiguing illnesses. However, mental fatigue is an important correlate of working memory in ME/CFS patients, with a population-based sample of these patients showing a clear association between subjec-
tive complaints of mental fatigue and objective measurements of memory (Capuron et al., 2006). Patients with ME/CFS who specifically reported mental fatigue were found to show significant impairment of working memory in the task of sustained attention/vigilance (a spatial working memory task of the CANTAB), suggesting higher cognitive fatigability (Capuron et al., 2006). Cognitive impairment in ME/CFS patients with mental fatigue was not attributable to mood disorders or psychotropic medication (Capuron et al., 2006).
Slowed Information Processing
Slowed information processing appears to be one of the most easily distinguishable features of ME/CFS (Cockshell and Mathias, 2010, 2013; Michiels and Cluydts, 2001; Tiersky et al., 1997). Despite some contradictory evidence, a large number of papers have emerged supporting the idea that individuals with ME/CFS often display slowed information processing (Claypoole et al., 2007; DeLuca et al., 2004a; Togo et al., 2013).
Positive evidence is provided by twin-control studies in which individuals with ME/CFS were compared with their twins who did not have the illness. These studies frequently revealed similar premorbid intellectual functioning (Claypoole et al., 2007; Mahurin et al., 2004) and no differences in content-dependent untimed testing, but significant differences in time-dependent tasks (Mahurin et al., 2004). Multiple studies have found that individuals with ME/CFS perform poorly compared with controls only in time-dependent tasks, with ME/CFS subjects showing no impairment in accuracy of information processing when given as much time as necessary to complete a task (DeLuca et al., 2004a; Mahurin et al., 2004). Also, in a meta-analysis of research studies, measures of both simple (reaction time task) and complex (PASAT) information processing speed showed moderate to large significant impairments in persons with ME/CFS compared with healthy controls (Cockshell and Mathias, 2010).
As with memory impairment, ME/CFS patients without psychiatric comorbidity show greater delays in information processing. Moreover, some evidence suggests that slower information processing is not related to reduced effort, depression, anxiety, fatigue, or sleep problems, nor is it dependent on slowed motor functioning, psychological status, number or severity of ME/CFS symptoms, or overall functioning (Cockshell and Mathias, 2012, 2013). Researchers in the field consider this symptom to be a possible cause of other neurocognitive impairments, including difficulties with attention and memory (DeLuca et al., 2004a; Togo et al., 2013). For that reason, it may be useful to compare ME/CFS patients with this symptom with other control groups (e.g., besides those with depression), as slowed information processing speed has also been identified in other
clinical groups, such as patients with multiple sclerosis and traumatic brain injury (DeLuca and Kalmar, 2008).
Attention Deficits
Considerable evidence shows that reduced attention is associated with ME/CFS (Cockshell and Mathias, 2010; Constant et al., 2011; Hou et al., 2014), although some research indicates that attentional deficits may be due to reduced information processing speed (Cockshell and Mathias, 2013). Cognition has been found to be weaker among patients with ME/CFS, who demonstrated an impaired ability to maintain attention and alertness (Constant et al., 2011). Several studies also have shown impairments in executive attention relative to healthy controls, with ME/CFS patients demonstrating greater difficulty concentrating on a particular element when confronted with potential distractions (Hou et al., 2014; Hutchinson and Badham, 2013). Some studies have confirmed the presence of objective impairments of attention in patients with ME/CFS compared with controls (Cockshell and Mathias, 2010; Hou et al., 2014). Differences have remained after patients showing low effort have been removed, suggesting that the differences cannot be explained by lack of effort (Constant et al., 2011).
Some studies have demonstrated that ME/CFS patients display greater attentional bias toward linguistic and pictorial health-related threat stimuli (i.e., any factor that represents a danger to one’s health) (Hou et al., 2008, 2014). Other studies have failed to find attentional bias but have found greater mood volatility with rumination (Martin and Alexeeva, 2010), suggesting variability in the ability of ME/CFS patients to control and sustain attention.
It is unclear whether this symptom can be used to distinguish ME/CFS from other disorders. Doing so would be difficult given that depression and anxiety can cause similar problems with attention (Moffoot et al., 1994) and have high comorbidity with ME/CFS (Attree et al., 2014). However, executive attention may be an option for distinguishing among subsets of the ME/CFS population, given some evidence of variability of this symptom in people with the illness (Hou et al., 2014). Studies of executive attention in children have shown that changes in the surface area of the anterior cingulate cortex account for a significant proportion of the variance in functioning on a test of cognitive control, suggesting that structural differences in this region of the brain could be a biomarker of conditions such as ME/CFS (Fjell et al., 2012). Deficits in patients may lead to poor activation or reduced connectivity of the anterior cingulate cortex. Exploring this possibility could further the effort to identify biomarkers of the disorder. More research comparing attentional deficits in fatiguing disorders and psychiatric conditions is necessary for this question to be answered.
Impaired Psychomotor Function
The literature offers conflicting evidence for the presence of impaired psychomotor function in ME/CFS patients. Some studies have found no difference in motor coordination and motor speed between ME/CFS patients and controls (reaction time test) (Cockshell and Mathias, 2013). Moreover, a meta-analysis found that fine motor speed was not impaired in subjects with ME/CFS (Cockshell and Mathias, 2010). However, there are significant differences in the movement time of reaction time tests between people with ME/CFS and healthy controls (Cockshell and Mathias, 2010). These findings suggest that information processing deficits contributed to the noted deficits in the movement time of reaction time tasks, which reportedly are not pure measures of motor speed (Smith and Carew, 1987; Vercoulen et al., 1998). Moreover, because fine motor speed was not found to be impaired in persons with ME/CFS, motor functioning is unlikely to be the primary cause of slower reaction times. This conclusion is consistent with the findings of more recent studies previously mentioned (Schrijvers et al., 2009; Van Den Eede et al., 2011) that reaction time but not movement time was impaired in ME/CFS patients.
On the other hand, considerable evidence that this symptom is associated with ME/CFS has been published (Davey et al., 2001; Lawrie et al., 2000; Marshall et al., 1997; Michiels et al., 1996). Results from a population-based study confirm and quantify alterations in motor speed in ME/CFS patients that are independent of psychiatric disorders or medication usage (Majer et al., 2008). In this study, ME/CFS patients recruited from the general population presented motor slowing after the researchers controlled for level of depressive symptoms. ME/CFS subjects also exhibited decreased motor speed, demonstrated by slower response times on the movement component of simple and choice reaction time tasks, a finding suggesting that these are primary features of cognitive changes in ME/CFS patients. The consistency of these results may provide clues to the involvement of neural circuits (i.e., basal ganglia) in ME/CFS. Further evidence of slowed psychomotor functioning is provided by twin-control studies in which individuals with ME/CFS were compared with their twins who did not have the illness (Claypoole et al., 2007; Mahurin et al., 2004).
Brain Studies
Studies of the brain in relation to ME/CFS have been performed for two purposes: to document any possible objective finding in ME/CFS and to develop diagnostic criteria for the disease. While in general these studies have been small (most with fewer than 20 patients with ME/CFS, usually fulfilling the Fukuda definition), most have shown statistically significant differ-
ences between patients with the condition and controls using a wide range of technologies and in a variety of brain regions. One study found that ME/CFS patients had 8 percent less gray matter relative to healthy controls, and that this difference was correlated with lower levels of physical activity (De Lange et al., 2005). Puri and colleagues (2012) found similar losses of both white and gray matter in patients with ME/CFS. Another study found that cognitive-behavioral therapy for ME/CFS patients increased prefrontal cortical volume after 16 sessions, suggesting that changes in brain volume and structure associated with the illness may be reversible with treatment (De Lange et al., 2008). However, the authors do not indicate whether such changes cause or result from neurocognitive symptoms of ME/CFS.
Recently, Nakatomi and colleagues (2014) found evidence of neuroinflammation in a small group of ME/CFS patients. While this was a small study (patients = 9, healthy controls = 10), it showed a significant increase in activated microglia or astrocytes using positron emission tomography (PET) in patients compared with controls. This study also found a positive correlation between activated microglia or astrocytes in the amygdala, thalamus, and midbrain and the cognitive impairment score of these subjects. The involvement of microglia could point to connectivity issues similar to those proposed with respect to the role of the anterior cingulate in maintaining attention. Spin-echo magnetic resonance imaging (MRI) revealed midbrain white matter and gray matter volume changes in these patients at fatigue onset, which the authors found to be consistent with an insult to the midbrain affecting multiple feedback control loops (Barnden et al., 2011).
In other brain studies, Yamamoto and colleagues (2003) used PET scanning to show that serotonin transporters were significantly reduced in the rostral subdivision of the anterior cingulate in ME/CFS patients. Functional MRI (fMRI) has been used to show an association between the subjective feeling of mental fatigue and brain responses during fatiguing cognition (Cook et al., 2007); reduced basal ganglia activation (caudate and globus pallidus) also may contribute to fatigue (Unger et al., 2012). Murrough and colleagues (2010) found increased ventricular lactate in ME/CFS patients based on proton magnetic resonance spectroscopy (MRS) imaging. The same group later found further evidence that increased oxidative stress may play a role in ME/CFS pathophysiology (Shungu et al., 2012). In another study, ME/CFS patients who were not medicated were reliably differentiated from healthy controls and those with depression using EEG spectral coherence (Duffy et al., 2011).
Some studies have found reduced activity in ME/CFS patients in regions of the brain associated with working memory during completion of a working memory task (Caseras et al., 2006), while others have found that individuals with ME/CFS appear to use more of their brain during working memory tasks (Lange et al., 2005). In addition, increased activation
has been seen by fMRI in ME/CFS patients in the occipito-parietal cortex, posterior cingulate gyrus, and parahippocampal gyrus, with decreased activation seen in the dorsolateral and dorsomedial prefrontal cortices (Caseras et al., 2008).
Findings suggest that ME/CFS patients require additional neural resources (more activation) to achieve the same level of behavioral performance as controls on the PASAT and other neuropsychological tests (Cook et al., 2007; Schmaling et al., 2003). During high-demand tasks, ME/CFS patients showed reduced activation in dorsolateral prefrontal and parietal cortices, showing differences only at the neurophysiological level. ME/CFS patients activated a large cluster in the right inferior/medial temporal cortex while undergoing 3-back condition testing—probably a compensatory strategy when working memory is dysfunctional or saturated as a result of ME/CFS (Caseras et al., 2006). Results are similar to those found in sleep-deprived healthy adults, so these findings could also be the consequence of sleep deprivation in ME/CFS patients (Caseras et al., 2006).
These objective findings based on multiple technologies support the concept that ME/CFS patients, at least those meeting Fukuda definition, have objective brain differences from healthy controls. However, the varying locations of these findings make insights into etiology and possible treatments less clear, and subsets of patients have not yet been defined.
Exacerbation of Cognitive Symptoms Following Exertion
Evidence on the effect of exertion on cognitive function was provided earlier in the section on PEM.
Summary
Collectively, the studies reviewed here support the notion that ME/CFS patients present with neurocognitive impairment. Slowed information processing, demonstrated by objective neuropsychological testing and potentially related to problems with white matter integrity, is one of the strongest neurocognitive indicators in support of a diagnosis of ME/CFS, particularly if there is evidence of normal functioning on untimed tests and impaired functioning on time-dependent tasks.
The greater severity of memory and other neurocognitive deficits in ME/CFS patients without psychiatric comorbidity suggests that these deficits may be a distinguishing feature of the disease, or at the very least a means of defining subgroups within the ME/CFS population. Confirming the presence of this symptom using objective neuropsychological testing would support diagnosis of ME/CFS and possibly support diagnosis of a specific subset of ME/CFS patients, but it is not necessary for the diagnosis.
The presence of attention deficits or impaired psychomotor function could support diagnosis of ME/CFS or potentially a subset of the ME/CFS population, but only in combination with other neurocognitive impairments.
Conclusion: There is sufficient evidence that slowed information processing is common in patients with ME/CFS, and a growing body of evidence shows that it may play a central role in overall neurocognitive impairment associated with the disease. Such a deficit may be responsible for the disability that results in loss of employment and loss of functional capacity in social environments.
ORTHOSTATIC INTOLERANCE AND AUTONOMIC DYSFUNCTION
Description of Orthostatic Intolerance in ME/CFS
Orthostatic intolerance is defined as a clinical condition in which symptoms worsen upon assuming and maintaining upright posture and are ameliorated (although not necessarily abolished) by recumbency (Gerrity et al., 2002; Low et al., 2009). Symptoms in orthostatic intolerance syndromes are those caused primarily by (1) cerebral underperfusion (such as lightheadedness, near-syncope or syncope, impaired concentration, headaches, and dimming or blurring of vision), or (2) sympathetic nervous system activation (such as forceful beating of the heart, palpitations, tremulousness, and chest pain) (Low et al., 2009). Other common signs and symptoms of orthostatic intolerance are fatigue, a feeling of weakness, intolerance of low-impact exercise, nausea, abdominal pain, facial pallor, nervousness, and shortness of breath (Kanjwal et al., 2003; Legge et al., 2008; Raj, 2013).
Orthostatic intolerance can occur as an isolated syndrome or in association with a variety of other comorbid disorders, including ME/CFS (Benarroch, 2012). The most prevalent forms of orthostatic intolerance in the general population, as well as among those with ME/CFS, are POTS and neurally mediated hypotension (NMH), with delayed variants of orthostatic hypotension and orthostatic tachycardia also being seen. Some individuals simply have low tolerance for upright posture without evidence of these objective circulatory changes (Bush et al., 2000; Rowe and Calkins, 1998).
Symptoms that occur upon assuming or maintaining upright posture are among the most commonly reported clinical features of ME/CFS. In surveys of ME/CFS patients, along with dizziness, a drop in blood pressure, spatial disorientation, and fainting, many participants “reported an inability to stand for even a few minutes” (FDA, 2013, p. 7). Some indi-
viduals described to the committee having difficulty standing, eating, and showering.7 Orthostatic symptoms also are a component of PEM: “[A crash is] not just the physical pain or it’s not just the head pain, it’s also more cognitive impairment, more orthostatic intolerance, more neurological issues … they’re very interrelated” (FDA, 2013, p. 8) (see the earlier section on PEM for more detail).
The symptoms and triggers for orthostatic intolerance syndromes are similar regardless of the associated diagnoses, although severity typically is greater in those with ME/CFS and POTS than in those with POTS alone (Okamoto et al., 2012a; Stewart et al., 1999). Orthostatic intolerance can begin acutely following a viral illness (Freeman and Komaroff, 1997), other infections (Kanjwal et al., 2011), pregnancy, or trauma, or it can have an insidious onset (Raj, 2013). It is made worse by deconditioning (Parsaik et al., 2012). Symptoms of orthostatic intolerance often are exacerbated by prolonged periods of upright posture; low-impact exercise; exposure to warm environments; and, less commonly, meals. Circumstances in daily life that can act as triggers include standing in line, shopping, hot showers or baths, hot weather, overheated rooms, and even prolonged quiet sitting (Raj, 2013; Schondorf et al., 1999). Some patients with orthostatic intolerance feel somewhat better and more energized while exercising, but they often are much worse afterward, especially if they are standing in the “cool-down” period (Calkins et al., 1995). Women with orthostatic intolerance can have worse symptoms during their menstrual periods (Low et al., 2009).
Prevalence of Orthostatic Intolerance and Autonomic Dysfunction in ME/CFS Patients
The committee’s literature review identified six research articles in which orthostatic and autonomic symptoms are reported. The prevalence of orthostatic symptoms in ME/CFS varies widely in these publications, but in all of them is higher in ME/CFS subjects than in controls (Bou-Holaigah et al., 1995; Miwa, 2014; Newton et al., 2007; Poole et al., 2000; Soetekouw et al., 1999; Timmers et al., 2002).
The study by Bou-Holaigah and colleagues (1995) included 23 U.S. adolescents and adults with ME/CFS, 96 percent of whom reported lightheadedness, 96 percent nausea, 83 percent diaphoresis, 78 percent abdominal discomfort, 78 percent blurred vision, and 43 percent prior syncope. Orthostatic stresses reported as exacerbating fatigue included a hot shower (78 percent), prolonged standing (78 percent), a warm environment (74 percent), and episodes of lightheadedness (43 percent). Autonomic symp-
____________________
7 Personal communication; public comments submitted to the IOM Committee on the Diagnostic Criteria for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome for meeting 3, 2014.
toms were assessed in 37 adult ME/CFS patients from the Netherlands compared with 38 controls of similar age and sex (Soetekouw et al., 1999). Those with ME/CFS had significantly higher rates of increased perspiration (57 percent versus 13 percent), decreased salivation (24 percent versus 3 percent), dysphagia (24 percent versus 0 percent), and constipation (22 percent versus 3 percent). Poole and colleagues (2000) evaluated 21 monozygotic twins discordant for CFS. Symptoms of orthostatic intolerance in the week before head-up tilt testing were graded on a 0 (none) to 5 (severe) scale. The CFS twins had significantly more severe dizziness (1.4 versus 0), lightheadedness (1.4 versus 0.3), nausea (0.6 versus 0), abdominal discomfort (0.7 versus 0.3), sweating (1.3 versus 0.4), chest pain (0.7 versus 0.3), and shortness of breath (0.8 versus 0.2). In a study of 36 Dutch adults with ME/CFS and 36 healthy controls, 28 percent of ME/CFS adults but no controls reported symptoms related to or avoidance of prolonged standing (Timmers et al., 2002). Newton and colleagues (2007) examined autonomic symptoms as measured by the detailed Composite Autonomic Symptom Score (COMPASS) questionnaire in 40 British adults with ME/CFS and 40 controls. The ME/CFS adults had significantly higher scores on domains assessing orthostatic tolerance, vasomotor, secretomotor, gastrointestinal, pupillomotor, and sleep problems, as well as higher total scores (mean [standard deviation] score 43.7 [16.6] versus 12.1 [10.2]; p < 0.0001). Finally, among 40 Japanese adults with ME/CFS, 28 (70 percent) reported symptoms of orthostatic intolerance, defined as the following symptoms while standing: disabling fatigue, dizziness, diminished concentration, tremulousness, sweating, lightheadedness, visual disturbances, palpitations, and nausea (Miwa, 2014).
The above variability in symptom reporting is related in part to the methods and comprehensiveness of the ascertainment for orthostatic intolerance, but also to temporal changes. While some older studies refer to autonomic and circulatory abnormalities in those with neuromyasthenia (MacLean et al., 1944), papers drawing attention to orthostatic intolerance in ME/CFS did not appear until 1995 (Bou-Holaigah et al., 1995; Rowe et al., 1995), the year after the Fukuda definition was published. As an example of the temporal changes in reporting, in a summary of clinical experience, Komaroff and Buchwald (1991) estimated that dizziness was present in 30-50 percent of patients. In a study published a decade later, Jason and colleagues (2002b) reported dizziness after standing in 47 percent of adults with ME/CFS, 21 percent of those with depression, and 9 percent of nonfatigued participants. And Nacul and colleagues (2011b) reported a prevalence of “intolerance to be on your feet” of 61 percent among 265 ME/CFS subjects in England.
A second source of variability in prevalence reports is the way in which orthostatic intolerance symptoms are classified. In the non-ME/CFS litera-
ture on orthostatic intolerance, symptoms of cerebral underperfusion (e.g., cognitive symptoms such as difficulty concentrating) were attributed to the circulatory dysfunction (Low et al., 2009). In the ME/CFS literature, those problems often are reported as independent symptoms. While orthostatic stress was reported to cause worse fatigue and cognitive function in those with ME/CFS as compared with those without ME/CFS (Stewart et al., 2012; Streeten and Anderson, 1992), it is impossible to determine which component of the overall ME/CFS symptom complex is due to the circulatory disorder or to some other aspect of ME/CFS physiology. Few studies specified the postures in which people reported triggering of their ME/CFS symptoms, and few distinguished orthostatic headaches or orthostatic cognitive difficulties from general causes of these symptoms. The dilemma is illustrated by the prevalence of symptoms documented by Nacul and colleagues (2011b): 61 percent of British adult ME/CFS patients reported intolerance of being on their feet, but 94 percent also reported memory or concentration problems, 82 percent difficulty thinking, 72 percent intolerance to exercise, 66 percent sweatiness/cold hands and feet, and 65 percent headaches. How many of these other symptoms were related to orthostatic stress is impossible to discern from the paper.
The Fukuda definition of CFS includes no mention of disorders in the regulation of heart rate and blood pressure in the differential diagnosis or management of ME/CFS symptoms (Fukuda et al., 1994). In the 2003 CCC, the diagnosis of ME/CFS can be made if—in addition to an illness of at least 6 months’ duration characterized by fatigue, PEM, sleep dysfunction, pain, and neurologic or cognitive manifestations—the individual also has one symptom from two of three of the following categories: autonomic manifestations, neuroendocrine manifestations, and immune manifestations. These categories are not mutually exclusive, but autonomic manifestations include the following: orthostatic intolerance, NMH, POTS, delayed postural hypotension, lightheadedness, extreme pallor, nausea and irritable bowel syndrome, urinary frequency and bladder dysfunction, palpitations with or without cardiac arrhythmias, and exertional dyspnea (Carruthers et al., 2003). In contrast, the NICE guidelines devote very little attention to circulatory dysfunction either in the differential diagnosis of fatigue as a symptom of ME/CFS or as a comorbid condition. The NICE guidelines recommend against performing a tilt table test routinely to aid in making a diagnosis of ME/CFS, but they do not comment on the potential utility of head-up tilt or standing tests for diagnosing comorbid orthostatic intolerance (NICE, 2007). The 2011 ME-ICC criteria list orthostatic intolerance as one of several qualifying abnormalities under the rubric of energy production/transportation impairments (Carruthers et al., 2011).
Assessment of Orthostatic Intolerance and Autonomic Dysfunction in ME/CFS
Clinical History
When querying for orthostatic intolerance, clinicians should pose questions about the frequency and severity of lightheadedness, near-fainting (presyncope), syncope, sweating, palpitations, chest pain, orthostatic dyspnea, and related symptoms when individuals are sitting or standing for prolonged periods of time. Chronic fatigue, difficulty concentrating, exercise intolerance, nausea, and tremulousness are common across a variety of forms of orthostatic intolerance. Not all individuals report lightheadedness; some simply report feeling unwell when upright and they avoid these situations. Questions with a high yield include asking how individuals feel in the following circumstances: while waiting in line, at receptions, in choir, while shopping or at the mall, while sitting still for long periods, and when exposed to warm/stressful circumstances (e.g., summer weather; after hot showers, baths, and saunas; after episodes of fear, pain, or exposure to blood) (Grubb, 2005; Raj, 2013; Thieben et al., 2007).
Formal Questionnaires
Several questionnaires are validated for use in adults with autonomic dysfunction or orthostatic intolerance syndromes, but they have not been evaluated specifically among those with ME/CFS. They include the Orthostatic Grading Scale (OGS) (Schrezenmaier et al., 2005); the Orthostatic Hypotension Questionnaire (OHQ) (Kaufmann et al., 2012); and a series of questionnaires developed at the Mayo Clinic, beginning with the 169-item Autonomic Symptom Profile (ASP) (Suarez et al., 1999), followed by the 84-question COMPASS. The COMPASS has been further abbreviated to a 31-item questionnaire (COMPASS 31) (Sletten et al., 2012).
Objective Measures
Orthostatic vital signs—measured by taking heart rate and blood pressure in supine, sitting, and standing positions—often are measured within 2 minutes or less, and thus are insufficient to identify most forms of chronic orthostatic intolerance. Prolonged testing of at least 10 minutes usually is needed for a sufficient orthostatic challenge. Two forms of prolonged orthostatic testing (standing test and upright tilt test) are commonly employed (see Box 4-2). The recommended duration of upright posture for detecting POTS is 10 minutes (Raj, 2013). Although neurally mediated hypotension can occur within the first 10 minutes of upright posture, an orthostatic
BOX 4-2
Prolonged Orthostatic Testing
Standing Test (Rowe et al., 1999)
This test can be performed in any clinic. The individual lies supine for 5 minutes to yield a steady baseline, then stands quietly, leaning against a wall, for 10 minutes. The individual is instructed to avoid moving, shifting his or her weight, or engaging in leg and other muscle contraction maneuvers. Symptoms such as fatigue, lightheadedness, nausea, warmth, shortness of breath, headache, pain, and impaired concentration/mental fogginess are recorded on a 0-10 scale while the individual is supine and every 1-2 minutes while he/she is standing. Individuals also are encouraged to report changes in symptoms as they occur. Heart rate and blood pressure recordings are made every 1-2 minutes. The test must be observed because of the potential for syncope and injury. The standing test, while helpful in some cases, is not a substitute for prolonged head-up tilt testing, and has limited ability to identify those with neurally mediated hypotension, most of whom develop hypotension beyond the 10-minute duration of a typical standing test.
Upright Tilt Tests (Bou-Holaigah et al., 1995)
The head-up tilt table test requires specialized equipment. The individual lies supine on the tilt table for 5-15 minutes. The table is then brought upright, usually to 70 degrees, for 10 to 60 minutes (usually 45 minutes if the goal is to evaluate for neurally mediated hypotension). Patient movement is discouraged. Heart rate is monitored continuously, and blood pressure is measured either continuously, using beat-to-beat measurements, or every 1-2 minutes for the first 10 minutes upright and every 5 minutes thereafter. Symptom reports usually are elicited every 2 minutes for the first 10 minutes upright and every 5 minutes thereafter, and recorded whenever major changes are reported by the individual. Passive tilt testing provokes a larger heart rate change in those with postural orthostatic tachycardia syndrome (POTS) than does active standing beyond 5 minutes of upright posture (Plash et al., 2013). During prolonged head-up tilt, a variety of pharmacological agents, including isoproterenol and nitroglycerine, are employed to provoke syncope. However, these challenges can lead to abnormal tests in some healthy individuals, so they must be interpreted with caution, as is described elsewhere (Moya et al., 2009). Moreover, head-up tilt testing is no longer thought to be necessary to diagnose all forms of neurally mediated syncope (Moya et al., 2009).
stress of more than 10 minutes of upright posture more commonly is required (Benditt et al., 1991). The median time to develop hypotension among adults with ME/CFS is 30 minutes in some studies (Bou-Holaigah et al., 1995). Among those with ME/CFS, orthostatic symptoms during
tilt testing emerge within minutes, long before hemodynamic changes are documented (Razumovsky et al., 2003).
Some investigators prefer to simulate orthostatic stress using lower-body negative pressure (LBNP), but these methods are used mainly in research settings (Wyller et al., 2008). Other methods used to capture physiological changes during upright tilt include transcranial Doppler ultrasound to measure cerebral blood flow velocity, capnography to measure expired CO2, and near infrared spectroscopy to measure changes in cerebral tissue oxygenation (Naschitz et al., 2000; Ocon et al., 2012; Tanaka et al., 2002).
Clinicians who evaluate those with orthostatic intolerance recognize that individuals with ME/CFS can develop an exacerbation of their typical symptoms not just during the head-up tilt test but for several days afterward. The committee’s literature search did not identify any publications describing this observation more formally, although administration of 1 liter of normal saline following the tilt test to reverse the post-tilt test exacerbation in symptoms is part of the tilt testing protocol in some centers (Rowe et al., 2001). Intravenous saline has been shown to improve orthostatic tolerance and to modify autonomic tone in those with neurally mediated syncope (Burklow et al., 1999) and after experimental prolonged bed rest (Takenaka et al., 2002).
Evidence for Orthostatic Intolerance and Autonomic Abnormalities in ME/CFS
This section examines the evidence for orthostatic intolerance and autonomic abnormalities in adults with ME/CFS. The methodology used for the committee’s literature review is described in Chapter 1. A full search for all forms of autonomic dysfunction (e.g., bladder dysfunction, gastrointestinal motility disorders) was not conducted. Instead, the committee elected to focus on circulatory abnormalities, as these are the most frequently reported autonomic abnormalities in ME/CFS. The most common forms of orthostatic intolerance are described in Box 4-3. Several studies reviewed were conducted by the same group of investigators. When it was not possible to ascertain from the description of the study methods whether the data were for independent study populations or some of the same patients on more than one occasion, the committee chose to select the most representative (or largest) of the studies for each group.
The studies reviewed vary widely on several methodological variables, notably in the following categories:
- patient characteristics (age, duration of ME/CFS, severity of ME/CFS, the ME/CFS case definition used, whether subjects were selected based on autonomic symptoms, referral biases, whether
-
the testing was performed on patients seeking clinical care or those participating in a research study);
- preparation for the test (medications allowed, prior sodium intake, duration of pretest fast);
- the type of orthostatic testing (active standing, standing while leaning against a wall, head-up tilt table) and, with tilt testing, the protocol used (e.g., angle of the tilt table, time of day for the study, ambient room temperature, degree of movement permitted);
- duration of the orthostatic stress; and
- criteria for abnormal response to orthostatic stress (earlier studies tended to report only rates of NMH, without reporting rates of
BOX 4-3
Common Orthostatic Intolerance Syndromes
Postural orthostatic tachycardia syndrome (POTS)
POTS is defined by a heart rate increase between the supine position and 10 minutes of standing of more than 30 beats per minute (bpm) for adults or 40 bpm for adolescents, or a heart rate that reaches 120 bpm or higher over the first 10 minutes of upright posture in the absence of orthostatic hypotension. A diagnosis of POTS requires that the change in heart rate also be accompanied by characteristic orthostatic symptoms that include lightheadedness, blurred vision, headaches, difficulty concentrating, diaphoresis, nausea, palpitations, chest pain, and shortness of breath (Freeman et al., 2011).
Neurally mediated hypotension (NMH)
NMH refers to a reflex drop in blood pressure that occurs during upright posture, and is defined as a drop in systolic blood pressure of 25 mm Hg (compared with supine blood pressure) during standing or upright tilt table testing. It usually is preceded by orthostatic symptoms of lightheadedness, nausea, pallor, and warmth and accompanied at the time of hypotension by a slowing of the heart rate (Bou-Holaigah et al., 1995). NMH sometimes is termed “neurocardiogenic syncope,” “vasodepressor syncope,” or “vaso-vagal syncope” (Bou-Holaigah et al., 1995).
Orthostatic hypotension (OH)
OH involves an immediate and sustained drop of at least 20 mm Hg in systolic or 10 mm Hg in diastolic blood pressure in the first 3 minutes of standing or upright tilt (Freeman et al., 2011). This is uncommon in ME/CFS, but a delayed form of OH has been recognized in ME/CFS patients, in which blood pressure changes occur after 3 minutes upright (Moya et al., 2009; Streeten and Anderson, 1992).
POTS, and studies employing less than 10 minutes of orthostatic stress reported rates of POTS, as these tests were not sufficiently prolonged to be able to exclude NMH).
These methodological factors contributed to the variability in rates of orthostatic intolerance reported in the various studies.
Orthostatic Testing
Prolonged orthostatic testing (> 10 minutes) The literature search identified 14 studies of prolonged orthostatic testing in which adults with ME/CFS were compared with healthy controls (Bou-Holaigah et al., 1995; De Lorenzo et al., 1997; Duprez et al., 1998; Hollingsworth et al., 2010; Jones et al., 2005; LaManca et al., 1999a; Naschitz et al., 2000, 2002; Poole et al., 2000; Razumovsky et al., 2003; Schondorf et al., 1999; Streeten et al., 2000; Timmers et al., 2002; Yataco et al., 1997), as well as three studies of subjects with ME/CFS without controls (Freeman and Komaroff, 1997; Reynolds et al., 2013; Rowe et al., 2001). None of the studies with controls and only one of the three studies without controls (Freeman and Komaroff, 1997) recruited participants based on the presence of autonomic symptoms.
Of the 14 studies with healthy controls in which orthostatic testing lasted longer than 10 minutes, only 2 did not report a higher prevalence of either POTS or NMH among those with ME/CFS compared with controls (Duprez et al., 1998; Jones et al., 2005). The rates of reported abnormalities ranged from 0 percent (Duprez et al., 1998) to 96 percent (Bou-Holaigah et al., 1995). The median proportion with hemodynamic abnormalities during the first 30-45 minutes upright in these studies was 37 percent in ME/CFS versus 7.5 percent in controls. In the three additional studies without controls, the reported rates of orthostatic intolerance ranged from 11 to 66 percent of adults with ME/CFS. This number needs to be interpreted with caution given the varying durations of orthostatic stress (ranging from 20 to 60 minutes) and other methodological differences in testing.
Brief orthostatic testing (< 10 minutes) The literature search identified seven studies with brief durations of orthostatic stress (2-10 minutes) (De Becker et al., 1998; Freeman and Komaroff, 1997; Hoad et al., 2008; Miwa, 2014; Natelson et al., 2007; Soetekouw et al., 1999; Winkler et al., 2004). The samples sizes ranged from 20 to 62 subjects with ME/CFS (median N = 37). Two studies used head-up tilt testing and five active standing as the orthostatic stressor. The prevalence of orthostatic intolerance was not documented in two studies in which the main focus was formal autonomic testing (De Becker et al., 1998; Soetekouw et al., 1999). In all of the remaining studies, the prevalence of POTS was numerically higher in adults
with ME/CFS than in controls (Freeman and Komaroff, 1997; Hoad et al., 2008; Miwa, 2014; Natelson et al., 2007; Winkler et al., 2004). Combining the data from these studies, the overall prevalence of POTS was 27 percent in adults with ME/CFS and 4.2 percent in healthy controls. The range of overall orthostatic abnormalities (including POTS, hypotension, and hypocapnia) in these studies with brief orthostatic testing varied widely—from 14 to 67 percent—in individual studies, reflecting differences in study measures, subject selection, and duration of orthostatic stress.
Symptoms reported during orthostatic testing The literature review identified five studies reporting orthostatic or ME/CFS symptoms following standing or tilt table testing. Upright posture was associated with provocation of fatigue symptoms and higher rates of lightheadedness, nausea, and warmth in 55-100 percent of subjects with ME/CFS (Bou-Holaigah et al., 1995; Hollingsworth et al., 2010; Naschitz et al., 2000; Streeten et al., 2000). For example, during the first 45 minutes of head-up tilt, 100 percent of 23 ME/CFS participants reported worse fatigue, 91 percent lightheadedness, 91 percent increased warmth, 73 percent nausea, and 18 percent diaphoresis. Controls made no reports of similar symptoms (Bou-Holaigah et al., 1995). One small study found a normalization of heart rate and blood pressure changes and improvement in ME/CFS symptoms after the acute application of a 45-mm Hg external compression device while subjects continued to stand (Streeten et al., 2000). In a study of 64 British adults with ME/CFS, 6 participants were unable to tolerate head-up tilt because of weakness. Of the remaining 58 with ME/CFS, 32 (55 percent) were symptomatic during the test, compared with 17/64 (27 percent) healthy controls. The types of symptoms were not specified (Hollingsworth et al., 2010). Research also has shown that the severity of orthostatic symptoms may predict the functional status of those with ME/CFS (Costigan et al., 2010).
Treatment of orthostatic intolerance Open (nonblinded) treatment studies of ME/CFS subjects found improvement in function after increased sodium intake or pharmacological treatment of orthostatic intolerance (Bou-Holaigah et al., 1995; De Lorenzo et al., 1997; Kawamura et al., 2003; Naschitz et al., 2004). However, randomized trials of fludrocortisone failed to confirm the efficacy of this treatment in adults as monotherapy or combined with hydrocortisone (Blockmans et al., 2003; Peterson et al., 1998; Rowe et al., 2001).
Autonomic Testing
More formal autonomic testing—using such measures as the cold pressor test, heart rate responses to deep breathing, handgrip tests, the Valsalva
maneuver, and quantitative sudomotor axon reflex tests—has not been conducted as extensively as have tests of the heart rate and blood pressure response to orthostatic stress. The majority of studies reporting the Valsalva ratio found no differences between ME/CFS and control groups (De Becker et al., 1998; Schondorf et al., 1999; Soetekouw et al., 1999; Winkler et al., 2004). Measures of heart rate variability have been used to examine the effects of autonomic tone on the heart noninvasively. ME/CFS is associated with enhanced sympathetic nervous system tone and reduced parasympathetic tone at baseline (Freeman and Komaroff, 1997; Frith et al., 2012; Sisto et al., 1995), in response to cognitive and orthostatic challenges (Beaumont et al., 2012; Yamamoto et al., 2003; Yataco et al., 1997), after walking (Cordero et al., 1996), and during sleep (Boneva et al., 2007; Rahman et al., 2011; Togo and Natelson, 2013; Yamaguti et al., 2013).
Ambulatory blood pressure measurements in subjects with ME/CFS have had conflicting results. One study found significantly lower systolic, diastolic, and mean arterial pressure in ME/CFS patients compared with controls, and a second found nighttime hypotension in ME/CFS patients (Newton et al., 2009; Van de Luit et al., 1998). Duprez and colleagues (1998), however, found no differences in daytime or nighttime blood pressure in ME/CFS patients. Of interest, although blood pressure did not differ in that study, there were significant differences in heart rate between ME/CFS cases and healthy controls throughout the 24-hour period.
Blood Volume and Cardiac Function Testing
Studies measuring blood volume have found lower values in ME/CFS subjects than in controls. Hurwitz and colleagues (2010) found a total blood volume deficit of 15.1 percent in ME/CFS patients compared with controls. Streeten and Bell (1998) identified low red blood cell mass in 16 of 19 patients with ME/CFS and an overall total lower blood volume in 63 percent of ME/CFS patients. Okamoto and colleagues (2012b) identified a 10.4 percent lower total blood volume in subjects with ME/CFS and POTS compared with controls studied at the same center.
Hurwitz and colleagues (2010) confirmed a lower cardiac index in ME/CFS patients (due to a 10.2 percent lower stroke index compared with sedentary and nonsedentary controls) and a cardiac contractility deficit of 25.1 percent. In a series of studies possibly involving some of the same patients, a high prevalence of orthostatic intolerance, associated with smaller heart on cardiothoracic ratios, was found in ME/CFS patients (Miwa, 2014; Miwa and Fujita, 2008, 2009, 2011). Hollingsworth and colleagues (2010) found a greater left ventricular work index with standing in ME/CFS patients compared with controls, suggesting that when the patients were standing, their hearts were working harder. These findings were associated
with the presentation of symptoms with standing in 95 percent of ME/CFS patients.
Orthostatic Hypocapnia
Three studies examined orthostatic hypocapnia in subjects with CFS. Naschitz and colleagues (2000) found that end-tidal CO2 was similar for ME/CFS patients and controls when supine, consistent with the absence of hyperventilation at baseline, but end-tidal CO2 was lower for the ME/CFS subjects during upright tilt testing. These results were confirmed by Razumovsky and colleagues (2003) during prolonged head-up tilt testing and by Natelson and colleagues (2007) during 8 minutes of active standing.
Microcirculatory Flow
Three studies examined abnormalities in peripheral blood flow in ME/CFS patients using different physiologic or pharmacologic challenges. ME/CFS patients had abnormally prolonged vasodilation in response to transdermally applied acetylcholine (Khan et al., 2003), reduced oxygen delivery to muscles after exercise and after cuff ischemia (McCully and Natelson, 1999), and a strikingly increased venous contractile sensitivity to infused epinephrine (Streeten, 2001). These studies have yet to be replicated.
Overlap of ME/CFS with Other Conditions Associated with Orthostatic Intolerance
A small number of studies have examined the prevalence of ME/CFS symptoms in those diagnosed with POTS (Okamoto et al., 2012b) or vasovagal syncope (Kenny and Graham, 2001; Legge et al., 2008). Okamoto and colleagues (2012b) examined the prevalence of the ME/CFS symptoms of the Fukuda definition among those with POTS who did not satisfy the criteria for ME/CFS, comparing this group with those who had POTS together with ME/CFS. Those with POTS alone often reported an elevated prevalence of severe fatigue, unrefreshing sleep, impaired memory or concentration, muscle pain, and post-exertional fatigue, although they did not have a sufficient number of symptoms to satisfy the Fukuda definition. By definition, the prevalence of Fukuda symptoms was higher in ME/CFS subjects who also had POTS than in those with POTS alone, but the pattern of symptoms was similar between the two groups (Okamoto et al., 2012b).
A high prevalence of hypotension and tachycardia is seen in FM, which, as noted earlier, is a clinical condition often comorbid with ME/CFS. Sym-
pathetic predominance of heart rate variability also is seen in FM studies (Martinez-Lavin, 2007; Martinez-Martinez et al., 2014).
The prevalence of Ehlers-Danlos syndrome and joint hypermobility is higher in ME/CFS patients than in healthy controls (Barron et al., 2002; Rowe et al., 1999). Studies also confirm high rates of fatigue as well as orthostatic and autonomic symptoms in those with hypermobility (Gazit et al., 2003) and the hypermobile form of Ehlers-Danlos syndrome (De Wandele et al., 2014a,b).
Summary
There is consistent evidence that upright posture is associated with a worsening of ME/CFS symptoms, as well as the onset of other symptoms such as lightheadedness, nausea, and palpitations. While there is variability in the reported prevalence of orthostatic intolerance in ME/CFS, heart rate and blood pressure abnormalities during standing or head-up tilt testing are more common in those with ME/CFS than in those without ME/CFS. Heart rate variability analyses demonstrate a sympathetic predominance of autonomic tone in those with ME/CFS, including during sleep.
Conclusion: Sufficient evidence indicates a high prevalence of orthostatic intolerance in ME/CFS, as measured by objective heart rate and blood pressure abnormalities during standing or head-up tilt testing or by patient-reported exacerbation of orthostatic symptoms with standing in day-to-day life. These findings indicate that orthostatic intolerance is a common and clinically important finding in ME/CFS.
Armitage, R. 1999. The effects of nefazodone on sleep in depressed patients and healthy controls. International Journal of Psychiatry in Clinical Practice 3(2):73-79.
Armitage, R., C. Landis, R. Hoffmann, M. Lentz, N. F. Watson, J. Goldberg, and D. Buchwald. 2007. The impact of a 4-hour sleep delay on slow wave activity in twins discordant for chronic fatigue syndrome. Sleep 30(5):657-662.
Armitage, R., C. Landis, R. Hoffmann, M. Lentz, N. Watson, J. Goldberg, and D. Buchwald. 2009. Power spectral analysis of sleep EEG in twins discordant for chronic fatigue syndrome. Journal of Psychosomatic Research 66(1):51-57.
Arroll, M. A., E. A. Attree, J. M. O’Leary, and C. P. Dancey. 2014. The delayed fatigue effect in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). Fatigue: Biomedicine, Health & Behavior 2(2):57-63.
Attree, E. A., C. P. Dancey, and A. L. Pope. 2009. An assessment of prospective memory retrieval in women with chronic fatigue syndrome using a virtual-reality environment: An initial study. Cyberpsychology and Behavior 12(4):379-385.
Attree, E. A., M. A. Arroll, C. P. Dancey, C. Griffith, and A. S. Bansal. 2014. Psychosocial factors involved in memory and cognitive failures in people with myalgic encephalomyelitis/chronic fatigue syndrome. Psychology Research and Behavior Management 7:67-76.
Bailes, S., E. Libman, M. Baltzan, R. Amsel, R. Schondorf, and C. S. Fichten. 2006. Brief and distinct empirical sleepiness and fatigue scales. Journal of Psychosomatic Research 60(6):605-613.
Balady, G. J., R. Arena, K. Sietsema, J. Myers, L. Coke, G. F. Fletcher, D. Forman, B. Franklin, M. Guazzi, M. Gulati, S. J. Keteyian, C. J. Lavie, R. Macko, D. Mancini, and R. V. Milani. 2010. Clinician’s guide to cardiopulmonary exercise testing in adults: A scientific statement from the American Heart Association. Circulation 122(2):191-225.
Ball, N., D. S. Buchwald, D. Schmidt, J. Goldberg, S. Ashton, and R. Armitage. 2004. Mono-zygotic twins discordant for chronic fatigue syndrome: Objective measures of sleep. Journal of Psychosomatic Research 56(2):207-212.
Baraniuk, J. N., O. Adewuyi, S. J. Merck, M. Ali, M. K. Ravindran, C. R. Timbol, R. Ray-Han, Y. Zheng, U. Le, R. Esteitie, and K. N. Petrie. 2013. A chronic fatigue syndrome (CFS) severity score based on case designation criteria. American Journal of Translational Research 5(1):53-68.
Barnden, L. R., B. Crouch, R. Kwiatek, R. Burnet, A. Mernone, S. Chryssidis, G. Scroop, and P. del Fante. 2011. A brain MRI study of chronic fatigue syndrome: Evidence of brainstem dysfunction and altered homeostasis. NMR in Biomedicine 24(10):1302-1312.
Barron, D. F., B. A. Cohen, M. T. Geraghty, R. Violand, and P. C. Rowe. 2002. Joint hypermobility is more common in children with chronic fatigue syndrome than in healthy controls. Journal of Pediatrics 141(3):421-425.
Bazelmans, E., G. Bleijenberg, M. J. M. Voeten, J. W. M. van der Meer, and H. Folgering. 2005. Impact of a maximal exercise test on symptoms and activity in chronic fatigue syndrome. Journal of Psychosomatic Research 59(4):201-208.
Beaumont, A., A. R. Burton, J. Lemon, B. K. Bennett, A. Lloyd, and U. Vollmer-Conna. 2012. Reduced cardiac vagal modulation impacts on cognitive performance in chronic fatigue syndrome. PLoS ONE 7(11):e49518.
Benarroch, E. E. 2012. Postural tachycardia syndrome: A heterogeneous and multifactorial disorder. Mayo Clinic Proceedings 87(12):1214-1225.
Benditt, D. G., S. Remole, S. Bailin, A. N. N. Dunnigan, A. Asso, and S. Milstein. 1991. Tilt table testing for evaluation of neurally-mediated (cardioneurogenic) syncope: Rationale and proposed protocols. PACE Pacing and Clinical Electrophysiology 14(10):1528-1537.
Black, C. D., and K. K. McCully. 2005. Time course of exercise induced alterations in daily activity in chronic fatigue syndrome. Dynamic Medicine 4(10).
Black, C. D., P. J. O’Connor, and K. K. McCully. 2005. Increased daily physical activity and fatigue symptoms in chronic fatigue syndrome. Dynamic Medicine 4(3).
Blackman, A., C. McGregor, R. Dales, H. S. Driver, I. Dumov, J. Fleming, K. Fraser, C. George, A. Khullar, J. Mink, M. Moffat, G. E. Sullivan, J. A. Fleetham, N. Ayas, T. D. Bradley, M. Fitzpatrick, J. Kimoff, D. Morrison, F. Ryan, R. Skomro, F. Series, and W. Tsai. 2010. Canadian Sleep Society/Canadian Thoracic Society position paper on the use of portable monitoring for the diagnosis of obstructive sleep apnea/hypopnea in adults. Canadian Respiratory Journal 17(5):229-232.
Blackwood, S. K., S. M. MacHale, M. J. Power, G. M. Goodwin, and S. M. Lawrie. 1998. Effects of exercise on cognitive and motor function in chronic fatigue syndrome and depression. Journal of Neurology Neurosurgery and Psychiatry 65(4):541-546.
Blockmans, D., P. Persoons, B. Van Houdenhove, M. Lejeune, and H. Bobbaers. 2003. Combination therapy with hydrocortisone and fludrocortisone does not improve symptoms in chronic fatigue syndrome: A randomized, placebo-controlled, double-blind, crossover study. American Journal of Medicine 114(9):736-741.
Boneva, R. S., M. J. Decker, E. M. Maloney, J. M. Lin, J. F. Jones, H. G. Helgason, C. M. Heim, D. B. Rye, and W. C. Reeves. 2007. Higher heart rate and reduced heart rate variability persist during sleep in chronic fatigue syndrome: A population-based study. Autonomic Neuroscience: Basic and Clinical 137(1-2):94-101.
Bou-Holaigah, I., P. C. Rowe, J. Kan, and H. Calkins. 1995. The relationship between neurally mediated hypotension and the chronic fatigue syndrome. Journal of the American Medical Association 274(12):961-967.
Brown, A. A., L. A. Jason, M. A. Evans, and S. Flores. 2013. Contrasting case definitions: The ME international consensus criteria vs. the Fukuda et al. CFS criteria. North American Journal of Psychology 15(1):103-120.
Brown, M. M., and L. A. Jason. 2007. Functioning in individuals with chronic fatigue syndrome: Increased impairment with co-occurring multiple chemical sensitivity and fibromyalgia. Dynamic Medicine 6(6).
Bruce, R. A., F. Kusumi, and D. Hosmer. 1973. Maximal oxygen intake and nomographic assessment of functional aerobic impairment in cardiovascular disease. American Heart Journal 85(4):546-562.
Buchwald, D., T. Pearlman, J. Umali, K. Schmaling, and W. Katon. 1996. Functional status in patients with chronic fatigue syndrome, other fatiguing illnesses, and healthy individuals. American Journal of Medicine 101(4):364-370.
Burklow, T. R., J. P. Moak, J. J. Bailey, and F. T. Makhlouf. 1999. Neurally mediated cardiac syncope: Autonomic modulation after normal saline infusion. Journal of the American College of Cardiology 33(7):2059-2066.
Bush, V. E., V. L. Wight, C. M. Brown, and R. Hainsworth. 2000. Vascular responses to orthostatic stress in patients with Postural Orthostatic Tachycardia Syndrome (POTS), in patients with low orthostatic tolerance, and in asymptomatic controls. Clinical Autonomic Research 10(5):279-284.
Busichio, K., L. A. Tiersky, J. DeLuca, and B. H. Natelson. 2004. Neuropsychological deficits in patients with chronic fatigue syndrome. Journal of the International Neuropsychological Society 10(2):278-285.
Buysse, D. J., C. F. Reynolds III, T. H. Monk, S. R. Berman, and D. J. Kupfer. 1989. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Research 28(2):193-213.
Calkins, H., M. Seifert, and F. Morady. 1995. Clinical presentation and long-term followup of athletes with exercise-induced vasodepressor syncope. American Heart Journal 129(6):1159-1164.
Capuron, L., L. Welberg, C. Heim, D. Wagner, L. Solomon, D. A. Papanicolaou, R. C. Craddock, A. H. Miller, and W. C. Reeves. 2006. Cognitive dysfunction relates to subjective report of mental fatigue in patients with chronic fatigue syndrome. Neuropsychopharmacology 31(8):1777-1784.
Carruthers, B. M., A. K. Jain, K. L. De Meirleir, D. L. Peterson, N. G. Klimas, A. M. Lemer, A. C. Bested, P. Flor-Henry, P. Joshi, A. C. P. Powles, J. A. Sherkey, and M. I. van de Sande. 2003. Myalgic encephalomyelitis/chronic fatigue syndrome: Clinical working case definition, diagnostic and treatment protocols (Canadian case definition). Journal of Chronic Fatigue Syndrome 11(1):7-115.
Carruthers, B. M., M. I. van de Sande, K. L. De Meirleir, N. G. Klimas, G. Broderick, T. Mitchell, D. Staines, A. C. P. Powles, N. Speight, R. Vallings, L. Bateman, B. Baumgarten-Austrheim, D. S. Bell, N. Carlo-Stella, J. Chia, A. Darragh, D. Jo, D. Lewis, A. R. Light, S. Marshall-Gradisbik, I. Mena, J. A. Mikovits, K. Miwa, M. Murovska, M. L. Pall, and S. Stevens. 2011. Myalgic encephalomyelitis: International consensus criteria. Journal of Internal Medicine 270(4):327-338.
Caseras, X., D. Mataix-Cols, V. Giampietro, K. A. Rimes, M. Brammer, F. Zelaya, T. Chalder, and E. L. Godfrey. 2006. Probing the working memory system in chronic fatigue syndrome: A functional magnetic resonance imaging study using the n-back task. Psychosomatic Medicine 68(6):947-955.
Caseras, X., D. Mataix-Cols, K. A. Rimes, V. Giampietro, M. Brammer, F. Zelaya, T. Chalder, and E. Godfrey. 2008. The neural correlates of fatigue: An exploratory imaginal fatigue provocation study in chronic fatigue syndrome. Psychological Medicine 38(7):941-951.
CDC (Centers for Disease Control and Prevention). 2005. CDC symptom inventory. http://www.institutferran.org/documentos/cdc_full_symptom_inventory.pdf (accessed January 12, 2015).
Chalder, T., G. Berelowitz, T. Pawlikowska, L. Watts, S. Wessely, D. Wright, and E. P. Wallace. 1993. Development of a fatigue scale. Journal of Psychosomatic Research 37(2):147-153.
Chu, L., M. Sunnquist, S. So, and L. A. Jason. 2013. Patient survey results for FDA drug development meeting for ME and CFS, April 25-26. http://www.iacfsme.org/LinkClick.aspx?fileticket=E8i8MVWh%2bX0%3d&tabid=119 (accessed August 19, 2014).
Ciccone, D. S., and B. H. Natelson. 2003. Comorbid illness in women with chronic fatigue syndrome: A test of the single syndrome hypothesis. Psychosomatic Medicine 65(2):268-275.
Claypoole, K., R. Mahurin, M. E. Fischer, J. Goldberg, K. B. Schmaling, R. B. Schoene, S. Ashton, and D. Buchwald. 2001. Cognitive compromise following exercise in monozygotic twins discordant for chronic fatigue syndrome: Fact or artifact? Applied Neuropsychology 8(1):31-40.
Claypoole, K. H., C. Noonan, R. K. Mahurin, J. Goldberg, T. Erickson, and D. Buchwald. 2007. A twin study of cognitive function in chronic fatigue syndrome: The effects of sudden illness onset. Neuropsychology 21(4):507-513.
Cockshell, S. J., and J. L. Mathias. 2010. Cognitive functioning in chronic fatigue syndrome: A meta-analysis. Psychological Medicine 40(8):1253-1267.
Cockshell, S. J., and J. L. Mathias. 2012. Test effort in persons with chronic fatigue syndrome when assessed using the validity indicator profile. Journal of Clinical and Experimental Neuropsychology 34(7):679-687.
Cockshell, S. J., and J. L. Mathias. 2013. Cognitive deficits in chronic fatigue syndrome and their relationship to psychological status, symptomatology, and everyday functioning. Neuropsychology 27(2):230-242.
Cockshell, S. J., and J. L. Mathias. 2014. Cognitive functioning in people with chronic fatigue syndrome: A comparison between subjective and objective measures. Neuropsychology 28(3):394-405.
Constant, E. L., S. Adam, B. Gillain, M. Lambert, E. Masquelier, and X. Seron. 2011. Cognitive deficits in patients with chronic fatigue syndrome compared to those with major depressive disorder and healthy controls. Clinical Neurology & Neurosurgery 113(4):295-302.
Cook, D. B., P. R. Nagelkirk, A. Peckerman, A. Poluri, J. Mores, and B. H. Natelson. 2005. Exercise and cognitive performance in chronic fatigue syndrome. Medicine & Science in Sports & Exercise 37(9):1460-1467.
Cook, D. B., P. J. O’Connor, G. Lange, and J. Steffener. 2007. Functional neuroimaging correlates of mental fatigue induced by cognition among chronic fatigue syndrome patients and controls. Neuroimage 36(1):108-122.
Cook, D. B., A. J. Stegner, P. R. Nagelkirk, J. D. Meyer, F. Togo, and B. H. Natelson. 2012. Responses to exercise differ for chronic fatigue syndrome patients with fibromyalgia. Medicine and Science in Sports and Exercise 44(6):1186-1193.
Cordero, D. L., S. A. Sisto, W. N. Tapp, J. J. LaManca, J. G. Pareja, and B. H. Natelson. 1996. Decreased vagal power during treadmill walking in patients with chronic fatigue syndrome. Clinical Autonomic Research 6(6):329-333.
Corral-Penafiel, J., J. L. Pepin, and F. Barbe. 2013. Ambulatory monitoring in the diagnosis and management of obstructive sleep apnoea syndrome. European Respiratory Review 22(129):312-324.
Costigan, A., C. Elliott, C. McDonald, and J. L. Newton. 2010. Orthostatic symptoms predict functional capacity in chronic fatigue syndrome: Implications for management. QJM: Monthly Journal of the Association of Physicians 103(8):589-595.
Cowan, D. C., G. Allardice, D. Macfarlane, D. Ramsay, H. Ambler, S. Banham, E. Livingston, and C. Carlin. 2014. Predicting sleep disordered breathing in outpatients with suspected OSA. BMJ Open 4(4):e004519.
Creti, L., E. Libman, M. Baltzan, D. Rizzo, S. Bailes, and C. S. Fichten. 2010. Impaired sleep in chronic fatigue syndrome: How is it best measured? Journal of Health Psychology 15(4):596-607.
Davenport, T. E., S. R. Stevens, K. Baroni, J. M. Van Ness, and C. R. Snell. 2011a. Reliability and validity of Short Form 36 version 2 to measure health perceptions in a sub-group of individuals with fatigue. Disability & Rehabilitation 33(25-26):2596-2604.
Davenport, T. E., S. R. Stevens, K. Baroni, M. Van Ness, and C. R. Snell. 2011b. Diagnostic accuracy of symptoms characterising chronic fatigue syndrome. Disability & Rehabilitation 33(19-20):1768-1775.
Davey, N. J., B. K. Puri, A. V. Nowicky, J. Main, and R. Zaman. 2001. Voluntary motor function in patients with chronic fatigue syndrome. Journal of Psychosomatic Research 50(1):17-20.
Davis, J. M., and K. H. Claypoole. 1997. Neuropsychological functioning in a pre-screened sample of chronic fatigue syndrome patients. Archives of Clinical Neuropsychology 12(4):306.
De Becker, P., P. Dendale, K. De Meirleir, I. Campine, K. Vandenborne, and Y. Hagers. 1998. Autonomic testing in patients with chronic fatigue syndrome. American Journal of Medicine 105(3A):22S-26S.
De Becker, P., J. Roeykens, M. Reynders, N. McGregor, and K. De Meirleir. 2000. Exercise capacity in chronic fatigue syndrome. Archives of Internal Medicine 160(21):3270-3277.
De Becker, P., N. McGregor, and K. De Meirleir. 2001. A definition-based analysis of symptoms in a large cohort of patients with chronic fatigue syndrome. Journal of Internal Medicine 250(3):234-240.
De Lange, F. P., J. S. Kalkman, G. Bleijenberg, P. Hagoort, J. W. M. van der Meer, and I. Toni. 2005. Gray matter volume reduction in the chronic fatigue syndrome. Neuroimage 26(3):777-781.
De Lange, F. P., A. Koers, J. S. Kalkman, G. Bleijenberg, P. Hagoort, J. W. M. van der Meer, and I. Toni. 2008. Increase in prefrontal cortical volume following cognitive behavioural therapy in patients with chronic fatigue syndrome. Brain 131(8):2172-2180.
De Lorenzo, F., J. Hargreaves, and V. V. Kakkar. 1997. Pathogenesis and management of delayed orthostatic hypotension in patients with chronic fatigue syndrome. Clinical Autonomic Research 7(4):185-190.
De Wandele, I., P. Calders, W. Peersman, S. Rimbaut, T. De Backer, F. Malfait, A. De Paepe, and L. Rombaut. 2014a. Autonomic symptom burden in the hypermobility type of Ehlers-Danlos syndrome: A comparative study with two other EDS types, fibromyalgia, and healthy controls. Seminars in Arthritis and Rheumatism 44(3):353-361.
De Wandele, I., L. Rombaut, L. Leybaert, P. Van de Borne, T. De Backer, F. Malfait, A. De Paepe, and P. Calders. 2014b. Dysautonomia and its underlying mechanisms in the hypermobility type of Ehlers-Danlos syndrome. Seminars in Arthritis and Rheumatism 44(1):93-100.
DeLuca, J., and J. H. Kalmar. 2008. Information processing speed in clinical populations. New York: Taylor & Francis.
DeLuca, J., S. K. Johnson, D. Beldowicz, and B. H. Natelson. 1995. Neuropsychological impairments in chronic fatigue syndrome, multiple sclerosis, and depression. Journal of Neurology, Neurosurgery & Psychiatry 58(1):38-43.
DeLuca, J., C. Christodoulou, B. J. Diamond, E. D. Rosenstein, N. Kramer, and B. H. Natelson. 2004a. Working memory deficits in chronic fatigue syndrome: Differentiating between speed and accuracy of information processing. Journal of the International Neuropsychological Society 10(1):101-109.
DeLuca, J., C. Christodoulou, B. J. Diamond, E. D. Rosenstein, N. Kramer, J. H. Ricker, and B. H. Natelson. 2004b. The nature of memory impairment in chronic fatigue syndrome. Rehabilitation Psychology 49(1):62-70.
Den Eede, F. V., G. Moorkens, W. Hulstijn, Y. Maas, D. Schrijvers, S. R. Stevens, P. Cosyns, S. J. Claes, and B. G. C. Sabbe. 2011. Psychomotor function and response inhibition in chronic fatigue syndrome. Psychiatry Research 186(2-3):367-372.
DePaul Research Team. 2010. Depaul symptom questionnaire. http://condor.depaul.edu/ljason/cfs/measures.html (accessed August 20, 2014).
Diamond, E. 2007. Developing a cardiopulmonary exercise testing laboratory. Chest 132(6): 2000-2007.
Dickson, A., A. Toft, and R. E. O’Carroll. 2009. Neuropsychological functioning, illness perception, mood and quality of life in chronic fatigue syndrome, autoimmune thyroid disease and healthy participants. Psychological Medicine 39(9):1567-1576.
Duffy, F. H., G. B. McAnulty, M. C. McCreary, G. J. Cuchural, and A. L. Komaroff. 2011. EEG spectral coherence data distinguish chronic fatigue syndrome patients from healthy controls and depressed patients: A case control study. BMC Neurology 11.
Duprez, D. A., M. L. De Buyzere, B. Drieghe, F. Vanhaverbeke, Y. Taes, W. Michielsen, and D. L. Clement. 1998. Long- and short-term blood pressure and RR-interval variability and psychosomatic distress in chronic fatigue syndrome. Clinical Science 94(1):57-63.
Edinger, J. D., W. K. Wohlgemuth, A. D. Krystal, and J. R. Rice. 2005. Behavioral insomnia therapy for fibromyalgia patients: A randomized clinical trial. Archives of Internal Medicine 165(21):2527-2535.
Farquhar, W. B., B. E. Hunt, J. A. Taylor, S. E. Darling, and R. Freeman. 2002. Blood volume and its relation to peak O(2) consumption and physical activity in patients with chronic fatigue. American Journal of Physiology. Heart and Circulatory Physiology 282(1):H66-H71.
FDA (Food and Drug Administration). 2013. The voice of the patient: Chronic fatigue syndrome and myalgic encephalomyelitis. Bethesda, MD: Center for Drug Evaluation and Research (CDER), FDA.
Fischler, B., O. LeBon, G. Hoffmann, R. Cluydts, L. Kaufman, and K. DeMeirleir. 1997. Sleep anomalies in the chronic fatigue syndrome: A comorbidity study. Neuropsychobiology 35(3):115-122.
Fishbain, D. A., B. Cole, J. E. Lewis, and J. Gao. 2010. What is the evidence for chronic pain being etiologically associated with the DSM-IV category of sleep disorder due to a general medical condition? A structured evidence-based review. Pain Medicine 11:158-179.
Fjell, A. M., K. B. Walhovd, T. T. Brown, J. M. Kuperman, Y. Chung, D. J. Hagler, Jr., V. Venkatraman, J. C. Roddey, M. Erhart, C. McCabe, N. Akshoomoff, D. G. Amaral, C. S. Bloss, O. Libiger, B. F. Darst, N. J. Schork, B. J. Casey, L. Chang, T. M. Ernst, J. R. Gruen, W. E. Kaufmann, T. Kenet, J. Frazier, S. S. Murray, E. R. Sowell, P. van Zijl, S. Mostofsky, T. L. Jernigan, and A. M. Dale. 2012. Multimodal imaging of the self-regulating developing brain. Proceedings of the National Academy of Sciences of the United States of America 109(48):19620-19625.
Foral, P., J. Knezevich, N. Dewan, and M. Malesker. 2011. Medication-induced sleep disturbances. The Consultant Pharmacist 26(6):414-425.
Fossey, M., E. Libman, S. Bailes, M. Baltzan, R. Schondorf, R. Amsel, and C. S. Fichten. 2004. Sleep quality and psychological adjustment in chronic fatigue syndrome. Journal of Behavioral Medicine 27(6):581-605.
Foster, G. R., R. D. Goldin, and H. C. Thomas. 1998. Chronic hepatitis C virus infection causes a significant reduction in quality of life in the absence of cirrhosis. Hepatology 27(1):209-212.
Freeman, R., and A. L. Komaroff. 1997. Does the chronic fatigue syndrome involve the autonomic nervous system? American Journal of Medicine 102(4):357-364.
Freeman, R., W. Wieling, F. B. Axelrod, D. G. Benditt, E. Benarroch, I. Biaggioni, W. P. Cheshire, T. Chelimsky, P. Cortelli, C. H. Gibbons, D. S. Goldstein, R. Hainsworth, M. J. Hilz, G. Jacob, H. Kaufmann, J. Jordan, L. A. Lipsitz, B. D. Levine, P. A. Low, C. Mathias, S. R. Raj, D. Robertson, P. Sandroni, I. J. Schatz, R. Schondorf, J. M. Stewart, and J. G. van Dijk. 2011. Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Autonomic Neuroscience 161(1-2):46-48.
Frith, J., P. Zalewski, J. J. Klawe, J. Pairman, A. Bitner, M. Tafil-Klawe, and J. L. Newton. 2012. Impaired blood pressure variability in chronic fatigue syndrome: A potential biomarker. QJM: Monthly Journal of the Association of Physicians 105(9):831-838.
Fukuda, K., S. E. Straus, I. Hickie, M. C. Sharpe, J. G. Dobbins, A. Komaroff, A. Schluederberg, J. F. Jones, A. R. Lloyd, S. Wessely, N. M. Gantz, G. P. Holmes, D. Buchwald, S. Abbey, J. Rest, J. A. Levy, H. Jolson, D. L. Peterson, J. Vercoulen, U. Tirelli, B. Evengård, B. H. Natelson, L. Steele, M. Reyes, and W. C. Reeves. 1994. The chronic fatigue syndrome: A comprehensive approach to its definition and study. Annals of Internal Medicine 121(12):953-959.
Furst, G. 1999. Measuring fatigue in chronic fatigue syndrome why and how. Journal of Chronic Fatigue Syndrome 5(3-4):55-59.
Gambert, S. R. 2005. Fatigue: Finding the cause of a common complaint. Clinical Geriatrics 13(10):6-8.
Gazit, Y., A. M. Nahir, R. Grahame, and G. Jacob. 2003. Dysautonomia in the joint hypermobility syndrome. American Journal of Medicine 115(1):33-40.
Gerrity, T. R., J. Bates, D. S. Bell, G. Chrousos, G. Furst, T. Hedrick, B. Hurwitz, R. W. Kula, S. M. Levine, R. C. Moore, and R. Schondorf. 2002. Chronic fatigue syndrome: What role does the autonomic nervous system play in the pathophysiology of this complex illness? Neuroimmunomodulation 10(3):134-141.
Gibson, H., N. Carroll, J. E. Clague, and R. H. Edwards. 1993. Exercise performance and fatiguability in patients with chronic fatigue syndrome. Journal of Neurology, Neurosurgery & Psychiatry 56(9):993-998.
Gotts, Z. M., V. Deary, J. Newton, D. Van der Dussen, P. De Roy, and J. G. Ellis. 2013. Are there sleep-specific phenotypes in patients with chronic fatigue syndrome? A cross-sectional polysomnography analysis. BMJ Open 3(6):e002999.
Grubb, B. P. 2005. Clinical practice. Neurocardiogenic syncope. New England Journal of Medicine 352(10):1004-1010.
Harel, D., B. D. Thombs, M. Hudson, M. Baron, and R. Steele. 2012. Measuring fatigue in SSC: A comparison of the Short Form-36 Vitality Subscale and Functional Assessment of Chronic Illness Therapy-Fatigue Scale. Rheumatology (Oxford) 51(12):2177-2185.
Hawk, C., L. A. Jason, and S. Torres-Harding. 2006a. Differential diagnosis of chronic fatigue syndrome and major depressive disorder. International Journal of Behavioral Medicine 13(3):244-251.
Hawk, C., L. A. Jason, and S. Torres-Harding. 2006b. Reliability of a chronic fatigue syndrome questionnaire. Journal of Chronic Fatigue Syndrome 13(4):41-66.
Hoad, A., G. Spickett, J. Elliott, and J. Newton. 2008. Postural orthostatic tachycardia syndrome is an under-recognized condition in chronic fatigue syndrome. QJM: Monthly Journal of the Association of Physicians 101(12):961-965.
Hollingsworth, K. G., D. E. Jones, R. Taylor, A. M. Blamire, and J. L. Newton. 2010. Impaired cardiovascular response to standing in chronic fatigue syndrome. European Journal of Clinical Investigation 40(7):608-615.
Hossain, J. L., P. Ahmad, L. W. Reinish, L. Kayumov, N. K. Hossain, and C. M. Shapiro. 2005. Subjective fatigue and subjective sleepiness: Two independent consequences of sleep disorders? Journal of Sleep Research 14(3):245-253.
Hou, R., R. Moss-Morris, B. Bradley, R. Peveler, and K. Mogg. 2008. Attentional bias towards health-threat information in chronic fatigue syndrome. European Neuropsychopharmacology 18(Suppl. 4):S278.
Hou, R., R. Moss-Morris, A. Risdale, J. Lynch, P. Jeevaratnam, B. P. Bradley, and K. Mogg. 2014. Attention processes in chronic fatigue syndrome: Attentional bias for health-related threat and the role of attentional control. Behaviour Research and Therapy 52:9-16.
Hurwitz, B. E., V. T. Coryell, M. Parker, P. Martin, A. Laperriere, N. G. Klimas, G. N. Sfakianakis, and M. S. Bilsker. 2010. Chronic fatigue syndrome: Illness severity, sedentary lifestyle, blood volume and evidence of diminished cardiac function. Clinical Science 118(2):125-135.
Hutchinson, C. V., and S. P. Badham. 2013. Patterns of abnormal visual attention in myalgic encephalomyelitis. Optometry and Vision Science 90(6):607-614.
IACFS/ME (International Association for Chronic Fatigue Syndrome/Myalgic Encephalomyelitis). 2014. ME/CFS: Primer for clinical practitioners. Chicago, IL: IACFS/ME.
Inbar, O., R. Dlin, A. Rotstein, and B. J. Whipp. 2001. Physiological responses to incremental exercise in patients with chronic fatigue syndrome. Medicine & Science in Sports & Exercise 33(9):1463-1470.
Jackson, M. L., and D. Bruck. 2012. Sleep abnormalities in chronic fatigue syndrome/myalgic encephalomyelitis: A review. Journal of Clinical Sleep Medicine 8(6):719-728.
Jason, L. A., and M. M. Brown. 2013. Sub-typing daily fatigue progression in chronic fatigue syndrome. Journal of Mental Health 22(1):4-11.
Jason, L. A., and R. R. Taylor. 2002. Applying cluster analysis to define a typology of chronic fatigue syndrome in a medically-evaluated, random community sample. Psychology and Health 17(3):323-337.
Jason, L. A., M. T. Ropacki, N. B. Santoro, J. A. Richman, W. Heatherly, R. Taylor, J. R. Ferrari, T. M. Haney-Davis, A. Rademaker, J. Dupuis, J. Golding, A. V. Plioplys, and S. Plioplys. 1997. A screening instrument for chronic fatigue syndrome: Reliability and validity. Journal of Chronic Fatigue Syndrome 3(1):39-59.
Jason, L. A., C. P. King, E. L. Frankenberry, K. M. Jordan, W. W. Tryon, F. Rademaker, and C. F. Huang. 1999. Chronic fatigue syndrome: Assessing symptoms and activity level. Journal of Clinical Psychology 55(4):411-424.
Jason, L. A., R. R. Taylor, C. L. Kennedy, K. Jordan, C. F. Huang, S. Torres-Harding, S. Song, and D. Johnson. 2002a. A factor analysis of chronic fatigue symptoms in a community-based sample. Social Psychiatry & Psychiatric Epidemiology 37(4):183-189.
Jason, L. A., S. R. Torres-Harding, A. W. Carrico, and R. R. Taylor. 2002b. Symptom occurrence in persons with chronic fatigue syndrome. Biological Psychology 59(1):15-27.
Jason, L. A., S. R. Torres-Harding, A. Jurgens, and J. Helgerson. 2004. Comparing the Fukuda et al. criteria and the Canadian case definition for chronic fatigue syndrome. Journal of Chronic Fatigue Syndrome 12(1):37-52.
Jason, L. A., T. Jessen, N. Porter, A. Boulton, M. G. Njoku, and G. Friedberg. 2009. Examining types of fatigue among individuals with ME/CFS. Disability Studies Quaterly 29(3).
Jason, L. A., A. Boulton, N. S. Porter, T. Jessen, M. G. Njoku, and F. Friedberg. 2010a. Classification of myalgic encephalomyelitis/chronic fatigue syndrome by types of fatigue. Behavioral Medicine 36(1):24-31.
Jason, L. A., M. Evans, N. Porter, M. Brown, A. Brown, J. Hunnell, V. Anderson, A. Lerch, K. De Meirleir, and F. Friedberg. 2010b. The development of a revised Canadian myalgic encephalomyelitis chronic fatigue syndrome case definition. American Journal of Biochemistry and Biotechnology 6(2):120-135.
Jason, L. A., M. Evans, M. Brown, N. Porter, A. Brown, J. Hunnell, V. Anderson, and A. Lerch. 2011a. Fatigue scales and chronic fatigue syndrome: Issues of sensitivity and specificity. Disability Studies Quarterly: DSQ 31(1).
Jason, L. A., N. Porter, J. Hunnell, A. Brown, A. Rademaker, and J. A. Richman. 2011b. A natural history study of chronic fatigue syndrome. Rehabilitation Psychology 56(1):32-42.
Jason, L. A., M. Brown, M. Evans, V. Anderson, A. Lerch, A. Brown, J. Hunnell, and N. Porter. 2011c. Measuring substantial reductions in functioning in patients with chronic fatigue syndrome. Disability and Rehabilitation 33(7):589-598.
Jason, L. A., A. Brown, E. Clyne, L. Bartgis, M. Evans, and M. Brown. 2012a. Contrasting case definitions for chronic fatigue syndrome, myalgic encephalomyelitis/chronic fatigue syndrome and myalgic encephalomyelitis. Evaluation and the Health Professions 35(3):280-304.
Jason, L. A., E. R. Unger, J. D. Dimitrakoff, A. P. Fagin, M. Houghton, D. B. Cook, G. D. Marshall, N. Klimas, and C. Snell. 2012b. Minimum data elements for research reports on CFS. Brain, Behavior, and Immunity 26(3):401-406.
Jason, L. A., A. Brown, M. Evans, M. Sunnquist, and J. L. Newton. 2013a. Contrasting chronic fatigue syndrome versus myalgic encephalomyelitis/chronic fatigue syndrome. Fatigue 1(3):168-183.
Jason, L. A., M. Sunnquist, A. Brown, M. Evans, S. Vernon, J. Furst, and V. Simonis. 2013b. Examining case definition criteria for chronic fatigue syndrome and myalgic encephalomyelitis. Fatigue: Biomedicine, Health & Behavior 2(1).
Jason, L. A., M. Sunnquist, A. Brown, M. Evans, and J. L. Newton. 2014. Are myalgic encephalomyelitis and chronic fatigue syndrome different illnesses? A preliminary analysis. Journal of Health Psychology [Epub ahead of print].
Jason, L., M. Evans, S. So, J. Scott, and A. Brown. In press. Problems in defining postexertional malaise. Journal of Prevention and Intervention in the Community.
Johns, M. W. 2000. Sensitivity and specificity of the multiple sleep latency test (MSLT), the maintenance of wakefulness test and the epworth sleepiness scale: Failure of the MSLT as a gold standard. Journal of Sleep Research 9(1):5-11.
Jones, D. E., K. G. Hollingsworth, R. Taylor, A. M. Blamire, and J. L. Newton. 2010. Abnormalities in ph handling by peripheral muscle and potential regulation by the autonomic nervous system in chronic fatigue syndrome. Journal of Internal Medicine 267(4):394-401.
Jones, D. E., K. G. Hollingsworth, D. G. Jakovljevic, G. Fattakhova, J. Pairman, A. M. Blamire, M. I. Trenell, and J. L. Newton. 2012. Loss of capacity to recover from acidosis on repeat exercise in chronic fatigue syndrome: A case-control study. European Journal of Clinical Investigation 42(2):186-194.
Jones, J. F., A. Nicholson, R. Nisenbaum, D. A. Papanicolaou, L. Solomon, R. Boneva, C. Heim, and W. C. Reeves. 2005. Orthostatic instability in a population-based study of chronic fatigue syndrome. American Journal of Medicine 118(12):1415.
Juenger, J., D. Schellberg, S. Kraemer, A. Haunstetter, C. Zugck, W. Herzog, and M. Haass. 2002. Health related quality of life in patients with congestive heart failure: Comparison with other chronic diseases and relation to functional variables. Heart 87(3):235-241.
Kanjwal, K., B. Karabin, Y. Kanjwal, and B. P. Grubb. 2011. Postural orthostatic tachycardia syndrome following Lyme disease. Cardiology Journal 18(1):63-66.
Kanjwal, Y., D. A. N. Kosinski, and B. P. Grubb. 2003. The postural orthostatic tachycardia syndrome. Pacing and Clinical Electrophysiology 26(8):1747-1757.
Kasper, D. L., E. Braunwalkd, A. S. Fauci, S. L. Hauser, D. L. Longo, and J. L. Jameson, eds. 2005. Harrison’s principles of internal medicine, 16th ed., Vol. 2. New York: McGraw-Hill.
Katch, V. L., S. S. Sady, and P. Freedson. 1982. Biological variability in maximum aerobic power. Medicine & Science in Sports & Exercise 14(1):21-25.
Kaufmann, H., R. Malamut, L. Norcliffe-Kaufmann, K. Rosa, and R. Freeman. 2012. The Orthostatic Hypotension Questionnaire (OHQ): Validation of a novel symptom assessment scale. Clinical Autonomic Research 22(2):79-90.
Kawamura, Y., M. Kihara, K. Nishimoto, and M. Taki. 2003. Efficacy of a half dose of oral pyridostigmine in the treatment of chronic fatigue syndrome: Three case reports. Pathophysiology 9(3):189-194.
Keller, B. A., J. L. Pryor, and L. Giloteaux. 2014. Inability of myalgic encephalomyelitis/chronic fatigue syndrome patients to reproduce VO2 peak indicates functional impairment. Journal of Translational Medicine 12(1):104.
Kenny, R. A., and L. A. Graham. 2001. Chronic fatigue syndrome symptoms common in patients with vasovagal syncope. American Journal of Medicine 110(3):242-243.
Kerr, J. R., J. Gough, S. C. Richards, J. Main, D. Enlander, M. McCreary, A. L. Komaroff, and J. K. Chia. 2010. Antibody to parvovirus B19 nonstructural protein is associated with chronic arthralgia in patients with chronic fatigue syndrome/myalgic encephalomyelitis. Journal of General Virology 91(Pt. 4):893-897.
Khan, F., V. Spence, G. Kennedy, and J. J. Belch. 2003. Prolonged acetylcholine-induced vasodilatation in the peripheral microcirculation of patients with chronic fatigue syndrome. Clinical Physiology & Functional Imaging 23(5):282-285.
Kierlin, L., and M. R. Littner. 2011. Parasomnias and antidepressant therapy: A review of the literature. Front Psychiatry 2:71.
Kishi, A., Z. R. Struzik, B. H. Natelson, F. Togo, and Y. Yamamoto. 2008. Dynamics of sleep stage transitions in healthy humans and patients with chronic fatigue syndrome. American Journal of Physiology—Regulatory Integrative & Comparative Physiology 294(6):R1980-R1987.
Kishi, A., B. H. Natelson, F. Togo, Z. R. Struzik, D. M. Rapoport, and Y. Yamamoto. 2011. Sleep-stage dynamics in patients with chronic fatigue syndrome with or without fibromyalgia. Sleep 34(11):1551-1560.
Kishi, A., F. Togo, D. B. Cook, M. Klapholz, Y. Yamamoto, D. M. Rapoport, and B. H. Natelson. 2013. The effects of exercise on dynamic sleep morphology in healthy controls and patients with chronic fatigue syndrome. Physiological Reports 1(6):e00152.
Knoop, H., J. B. Prins, M. Stulemeijer, J. W. M. van der Meer, and G. Bleijenberg. 2007. The effect of cognitive behaviour therapy for chronic fatigue syndrome on self-reported cognitive impairments and neuropsychological test performance. Journal of Neurology, Neurosurgery & Psychiatry 78(4):434-436.
Komaroff, A. L., and D. Buchwald. 1991. Symptoms and signs of chronic fatigue syndrome. Reviews of Infectious Diseases 13(Suppl. 1):S8-S11.
Komaroff, A. L., L. R. Fagioli, T. H. Doolittle, B. Gandek, M. A. Gleit, R. T. Guerriero, I. R. J. Kornish, N. C. Ware, J. E. Ware, Jr., and D. W. Bates. 1996a. Health status in patients with chronic fatigue syndrome and in general population and disease comparison groups. American Journal of Medicine 101(3):281-290.
Komaroff, A. L., L. R. Fagioli, A. M. Geiger, T. H. Doolittle, J. Lee, J. Kornish, M. A. Gleit, and R. T. Guerriero. 1996b. An examination of the working case definition of chronic fatigue syndrome. American Journal of Medicine 100(1):56-64.
Komaroff, A. L., L. R. Fagioli, T. H. Doolittle, B. Gandek, M. A. Gleit, R. T. Guerriero, R. J. Kornish II, N. C. Ware, J. E. Ware, Jr., and D. W. Bates. 1996c. Chronic fatigue syndrome questionnaire. In Health status in patients with chronic fatigue syndrome and in general population and disease comparison groups. American Journal of Medicine 101(3):281-290.
Krupp, L. B., N. G. LaRocca, J. Muir-Nash, and A. D. Steinberg. 1989. The fatigue severity scale. Application to patients with multiple sclerosis and systemic lupus erythematosus. Archives of Neurology 46(10):1121-1123.
Krupp, L. B., L. Jandorf, P. K. Coyle, and W. B. Mendelson. 1993. Sleep disturbance in chronic fatigue syndrome. Journal of Psychosomatic Research 37(4):325-331.
Kushida, C. A., M. R. Littner, T. Morgenthaler, C. A. Alessi, D. Bailey, J. Coleman, Jr., L. Friedman, M. Hirshkowitz, S. Kapen, M. Kramer, T. Lee-Chiong, D. L. Loube, J. Owens, J. P. Pancer, and M. Wise. 2005. Practice parameters for the indications for polysomnography and related procedures: An update for 2005. Sleep 28(4):499-521.
LaManca, J. J., S. A. Sisto, J. DeLuca, S. K. Johnson, G. Lange, J. Pareja, S. Cook, and B. H. Natelson. 1998. Influence of exhaustive treadmill exercise on cognitive functioning in chronic fatigue syndrome. American Journal of Medicine 105(3A):59S-65S.
LaManca, J. J., A. Peckerman, J. Walker, W. Kesil, S. Cook, A. Taylor, and B. H. Natelson. 1999a. Cardiovascular response during head-up tilt in chronic fatigue syndrome. Clinical Physiology 19(2):111-120.
LaManca, J. J., S. A. Sisto, X. Zhou, J. E. Ottenweller, S. Cook, A. Peckerman, Q. W. Zhang, T. N. Denny, W. C. Gause, and B. H. Natelson. 1999b. Immunological response in chronic fatigue syndrome following a graded exercise test to exhaustion. Journal of Clinical Immunology 19(2):135-142.
LaManca, J. J., A. Peckerman, S. A. Sisto, J. DeLuca, S. Cook, and B. H. Natelson. 2001. Cardiovascular responses of women with chronic fatigue syndrome to stressful cognitive testing before and after strenuous exercise. Psychosomatic Medicine 63(5):756-764.
Lange, G., J. Steffener, D. B. Cook, B. M. Bly, C. Christodoulou, W. C. Liu, J. DeLuca, and B. H. Natelson. 2005. Objective evidence of cognitive complaints in chronic fatigue syndrome: A BOLD fMRI study of verbal working memory. Neuroimage 26(2):513-524.
Larun, L., and K. Malterud. 2007. Identity and coping experiences in chronic fatigue syndrome: A synthesis of qualitative studies. Patient Education and Counseling 69(1-3):20-28.
Lawrie, S. M., S. M. MacHale, J. T. O. Cavanagh, R. E. O’Carroll, and G. M. Goodwin. 2000. The difference in patterns of motor and cognitive function in chronic fatigue syndrome and severe depressive illness. Psychological Medicine 30(2):433-442.
Le Bon, O., B. Fischler, G. Hoffmann, J. R. Murphy, K. De Meirleir, R. Cluydts, and I. Pelc. 2000. How significant are primary sleep disorders and sleepiness in the chronic fatigue syndrome? Sleep Research Online 3(2):43-48.
Le Bon, O., D. Neu, F. Valente, and P. Linkowski. 2007. Paradoxical nrems distribution in “pure” chronic fatigue patients a comparison with sleep apnea-hypopnea patients and healthy control subjects. Journal of Chronic Fatigue Syndrome 14(2):45-59.
Le Bon, O., D. Neu, Y. Berquin, J.-P. Lanquart, R. Hoffmann, O. Mairesse, and R. Armitage. 2012. Ultra-slow delta power in chronic fatigue syndrome. Psychiatry Research 200(2-3): 742-747.
Legge, H., M. Norton, and J. Newton. 2008. Fatigue is significant in vasovagal syncope and is associated with autonomic symptoms. Europace 10(9):1095-1101.
Lewis, I., J. Pairman, G. Spickett, and J. L. Newton. 2013. Clinical characteristics of a novel subgroup of chronic fatigue syndrome patients with postural orthostatic tachycardia syndrome. Journal of Internal Medicine 273(5):501-510.
Libman, E., L. Creti, M. Baltzan, D. Rizzo, C. S. Fichten, and S. Bailes. 2009. Sleep apnea and psychological functioning in chronic fatigue syndrome. Journal of Health Psychology 14(8):1251-1267.
Light, A. R., A. T. White, R. W. Hughen, and K. C. Light. 2009. Moderate exercise increases expression for sensory, adrenergic, and immune genes in chronic fatigue syndrome patients but not in normal subjects. The Journal of Pain 10(10):1099-1112.
Light, A. R., L. Bateman, D. Jo, R. W. Hughen, T. A. Vanhaitsma, A. T. White, and K. C. Light. 2012. Gene expression alterations at baseline and following moderate exercise in patients with chronic fatigue syndrome and fibromyalgia syndrome. Journal of Internal Medicine 271(1):64-81.
Low, P. A., P. Sandroni, M. Joyner, and W. Shen. 2009. Postural tachycardia syndrome. Journal of Cardiovascular Electrophysiology 20(3):352-358.
MacLean, A., E. Allen, and T. Magath. 1944. Orthostatic tachycardia and orthostatic hypotension: Defects in the return of venous blood to the heart. American Heart Journal 27(2):145-163.
Maes, M., F. N. M. Twisk, and C. Johnson. 2012. Myalgic encephalomyelitis (ME), chronic fatigue syndrome (CFS), and chronic fatigue (CF) are distinguished accurately: Results of supervised learning techniques applied on clinical and inflammatory data. Psychiatry Research 200(2-3):754-760.
Mahurin, R. K., J. H. Goldberg, K. H. Claypoole, L. Arguelles, S. Ashton, and D. Buchwald. 2004. Cognitive processing in monozygotic twins discordant for chronic fatigue syndrome. Neuropsychology 18(2):232-239.
Majer, M., J. F. Jones, E. R. Unger, L. S. Youngblood, M. J. Decker, B. Gurbaxani, C. Heim, and W. C. Reeves. 2007. Perception versus polysomnographic assessment of sleep in CFS and non-fatigued control subjects: Results from a population-based study. BMC Neurology 7.
Majer, M., L. A. M. Welberg, L. Capuron, A. H. Miller, G. Pagnoni, and W. C. Reeves. 2008. Neuropsychological performance in persons with chronic fatigue syndrome: Results from a population-based study. Psychosomatic Medicine 70(7):829-836.
Mariman, A., D. Vogelaers, I. Hanoulle, L. Delesie, and D. Pevernagie. 2012. Subjective sleep quality and daytime sleepiness in a large sample of patients with chronic fatigue syndrome (CFS). Acta Clinica Belgica 67(1):19-24.
Marino, M., Y. Li, M. N. Rueschman, J. W. Winkelman, J. M. Ellenbogen, J. M. Solet, H. Dulin, L. F. Berkman, and O. M. Buxton. 2013. Measuring sleep: Accuracy, sensitivity, and specificity of wrist actigraphy compared to polysomnography. Sleep 36(11):1747-1755.
Marshall, P. S., M. Forstot, A. Callies, P. K. Peterson, and C. H. Schenck. 1997. Cognitive slowing and working memory difficulties in chronic fatigue syndrome. Psychosomatic Medicine 59(1):58-66.
Martin, M., and I. Alexeeva. 2010. Mood volatility with rumination but neither attentional nor interpretation biases in chronic fatigue syndrome. British Journal of Health Psychology 15(4):779-796.
Martinez-Lavin, M. 2007. Biology and therapy of fibromyalgia. Stress, the stress response system, and fibromyalgia. Arthritis Research & Therapy 9(4):216.
Martinez-Martinez, L. A., T. Mora, A. Vargas, M. Fuentes-Iniestra, and M. Martinez-Lavin. 2014. Sympathetic nervous system dysfunction in fibromyalgia, chronic fatigue syndrome, irritable bowel syndrome, and interstitial cystitis: A review of case-control studies. Journal of Clinical Rheumatology 20(3):146-150.
Matthews, D. A., P. Manu, and T. J. Lane. 1991. Evaluation and management of patients with chronic fatigue. American Journal of the Medical Sciences 302(5):269-277.
McCully, K. K., and B. H. Natelson. 1999. Impaired oxygen delivery to muscle in chronic fatigue syndrome. Clinical Science 97(5):603-608; discussion 611-613.
McHorney, C. A., J. E. Ware, Jr., and A. E. Raczek. 1993. The MOS 36-item Short-Form Health Survey (SF-36): II. Psychometric and clinical tests of validity in measuring physical and mental health constructs. Medical Care 31(3):247-263.
Meeus, M., L. Hermans, K. Ickmans, F. Struyf, D. Van Cauwenbergh, L. Bronckaerts, L. S. De Clerck, G. Moorken, G. Hans, S. Grosemans, and J. Nijs. 2014. Endogenous pain modulation in response to exercise in patients with rheumatoid arthritis, patients with chronic fatigue syndrome and comorbid fibromyalgia, and healthy controls: A double-blind randomized controlled trial. Pain Practice. http://onlinelibrary.wiley.com/doi/10.1111/papr.12181/pdf (accessed January 14, 2015).
Merkus, M. P., K. J. Jager, F. W. Dekker, E. W. Boeschoten, P. Stevens, and R. T. Krediet. 1997. Quality of life in patients on chronic dialysis: Self-assessment 3 months after the start of treatment. The Necosad Study Group. American Journal of Kidney Diseases 29(4):584-592.
Meyer, J. D., A. R. Light, S. K. Shukla, D. Clevidence, S. Yale, A. J. Stegner, and D. B. Cook. 2013. Post-exertion malaise in chronic fatigue syndrome: Symptoms and gene expression. Fatigue: Biomedicine, Health & Behavior 1(4):190-209.
Michiels, V., and R. Cluydts. 2001. Neuropsychological functioning in chronic fatigue syndrome: A review. Acta Psychiatrica Scandinavica 103(2):84-93.
Michiels, V., R. Cluydts, B. Fischler, G. Hoffmann, O. Le Bon, and K. De Meirleir. 1996. Cognitive functioning in patients with chronic fatigue syndrome. Journal of Clinical & Experimental Neuropsychology: Official Journal of the International Neuropsychological Society 18(5):666-677.
Miwa, K. 2014. Cardiac dysfunction and orthostatic intolerance in patients with myalgic encephalomyelitis and a small left ventricle. Heart Vessels 1-6.
Miwa, K., and M. Fujita. 2008. Small heart syndrome in patients with chronic fatigue syndrome. Clinical Cardiology 31(7):328-333.
Miwa, K., and M. Fujita. 2009. Cardiovascular dysfunction with low cardiac output due to a small heart in patients with chronic fatigue syndrome. Internal Medicine 48(21): 1849-1854.
Miwa, K., and M. Fujita. 2011. Small heart with low cardiac output for orthostatic intolerance in patients with chronic fatigue syndrome. Clinical Cardiology 34(12):782-786.
Moffoot, A. P., R. E. O’Carroll, J. Bennie, S. Carroll, H. Dick, K. P. Ebmeier, and G. M. Goodwin. 1994. Diurnal variation of mood and neuropsychological function in major depression with melancholia. Journal of Affective Disorders 32(4):257-269.
Morgenthaler, T., C. Alessi, L. Friedman, J. Owens, V. Kapur, B. Boehlecke, T. Brown, A. Chesson, Jr., J. Coleman, T. Lee-Chiong, J. Pancer, and T. J. Swick. 2007. Practice parameters for the use of actigraphy in the assessment of sleep and sleep disorders: An update for 2007. Sleep 30(4):519-529.
Morriss, R., M. Sharpe, A. L. Sharpley, P. J. Cown, K. Hawton, and J. Morris. 1993. Abnormalities of sleep in patients with the chronic fatigue syndrome. British Medical Journal 306(6886):1161-1164.
Morriss, R. K., A. J. Wearden, and L. Battersby. 1997. The relation of sleep difficulties to fatigue, mood and disability in chronic fatigue syndrome. Journal of Psychosomatic Research 42(6):597-605.
Moya, A., R. Sutton, F. Ammirati, J. J. Blanc, M. Brignole, J. B. Dahm, J. C. Deharo, J. Gajek, K. Gjesdal, A. Krahn, M. Massin, M. Pepi, T. Pezawas, R. Ruiz Granell, F. Sarasin, A. Ungar, J. G. van Dijk, E. P. Walma, and W. Wieling. 2009. Guidelines for the diagnosis and management of syncope (version 2009). European Heart Journal 30(21):2631-2671.
Murrough, J. W., X. Mao, K. A. Collins, C. Kelly, G. Andrade, P. Nestadt, S. M. Levine, S. J. Mathew, and D. C. Shungu. 2010. Increased ventricular lactate in chronic fatigue syndrome measured by 1H MRS imaging at 3.0 T. II: Comparison with major depressive disorder. NMR in Biomedicine 23(6):643-650.
Nacul, L. C., E. M. Lacerda, P. Campion, D. Pheby, M. D. Drachler, J. C. Leite, F. Poland, A. Howe, S. Fayyaz, and M. Molokhia. 2011a. The functional status and well being of people with myalgic encephalomyelitis/chronic fatigue syndrome and their carers. BMC Public Health 11.
Nacul, L. C., E. M. Lacerda, D. Pheby, P. Campion, M. Molokhia, S. Fayyaz, J. C. Leite, F. Poland, A. Howe, and M. L. Drachler. 2011b. Prevalence of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) in three regions of England: A repeated cross-sectional study in primary care. BMC Medicine 9:91.
Nakamura, T., S. K. Schwander, R. Donnelly, F. Ortega, F. Togo, G. Broderick, Y. Yamamoto, N. S. Cherniack, D. Rapoport, and B. H. Natelson. 2010a. Cytokines across the night in chronic fatigue syndrome with and without fibromyalgia. Clinical and Vaccine Immunology 17(4):582-587.
Nakamura, T., F. Togo, N. S. Cherniack, D. Rapoport, and B. H. Natelson. 2010b. A subgroup of patients with chronic fatigue syndrome may have a disorder of arousal. The Open Sleep Journal 3:6-11.
Nakatomi, Y., K. Mizuno, A. Ishii, Y. Wada, M. Tanaka, S. Tazawa, K. Onoe, S. Fukuda, J. Kawabe, K. Takahashi, Y. Kataoka, S. Shiomi, K. Yamaguti, M. Inaba, H. Kuratsune, and Y. Watanabe. 2014. Neuroinflammation in patients with chronic fatigue syndrome/myalgic encephalomyelitis: An 11C-(R)-PK11195 PET study. Journal of Nuclear Medicine 55(6):945-950.
Naschitz, J. E., I. Rosner, M. Rozenbaum, L. Gaitini, I. Bistritzki, E. Zuckerman, E. Sabo, and D. Yeshurun. 2000. The capnography head-up tilt test for evaluation of chronic fatigue syndrome. Seminars in Arthritis & Rheumatism 30(2):79-86.
Naschitz, J. E., E. Sabo, S. Naschitz, I. Rosner, M. Rozenbaum, M. Fields, H. Isseroff, R. M. Priselac, L. Gaitini, S. Eldar, E. Zukerman, and D. Yeshurun. 2002. Hemodynamics instability score in chronic fatigue syndrome and in non-chronic fatigue syndrome. Seminars in Arthritis & Rheumatism 32(3):141-148.
Naschitz, J., D. Dreyfuss, D. Yeshurun, and I. Rosner. 2004. Midodrine treatment for chronic fatigue syndrome. Postgraduate Medical Journal 80(942):230-232.
Natelson, B. H., R. Intriligator, N. S. Cherniack, H. K. Chandler, and J. M. Stewart. 2007. Hypocapnia is a biological marker for orthostatic intolerance in some patients with chronic fatigue syndrome. Dynamic Medicine 6.
National Institute on Aging. 2007. Unexplained fatigue in the elderly—workshop summary. http://www.nia.nih.gov/print/about/events/2011/unexplained-fatigue-elderly (accessed January 12, 2015).
Neu, D., O. Mairesse, G. Hoffmann, A. Dris, L. J. Lambrecht, P. Linkowski, P. Verbanck, and L. B. Olivier. 2007. Sleep quality perception in the chronic fatigue syndrome: Correlations with sleep efficiency, affective symptoms and intensity of fatigue. Neuropsychobiology 56(1):40-46.
Neu, D., G. Hoffmann, R. Moutrier, P. Verbanck, P. Linkowski, and O. Le Bon. 2008. Are patients with chronic fatigue syndrome just “tired” or also “sleepy”? Journal of Sleep Research 17(4):427-431.
Neu, D., H. Kajosch, P. Peigneux, P. Verbanck, P. Linkowski, and O. Le Bon. 2011. Cognitive impairment in fatigue and sleepiness associated conditions. Psychiatry Research 189(1):128-134.
Newton, J. L., O. Okonkwo, K. Sutcliffe, A. Seth, J. Shin, and D. E. J. Jones. 2007. Symptoms of autonomic dysfunction in chronic fatigue syndrome. QJM: Monthly Journal of the Association of Physicians 100(8):519-526.
Newton, J. L., A. Sheth, J. Shin, J. Pairman, K. Wilton, J. A. Burt, and D. E. Jones. 2009. Lower ambulatory blood pressure in chronic fatigue syndrome. Psychosomatic Medicine 71(3):361-365.
NICE (National Institute for Health and Clinical Excellence). 2007. Chronic fatigue syndrome/myalgic encephalomyelitis (or encephalopathy): Diagnosis and management of CFS/ME in adults and children. London, UK: NICE.
Nijs, J., J. Van Oosterwijck, M. Meeus, L. Lambrecht, K. Metzger, M. Fremont, and L. Paul. 2010. Unravelling the nature of postexertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome: The role of elastase, complement C4a and interleukin-1beta. Journal of Internal Medicine 267(4):418-435.
Nijs, J., A. Nees, L. Paul, M. De Kooning, K. Ickmans, M. Meeus, and J. Van Oosterwijck. 2014. Altered immune response to exercise in patients with chronic fatigue syndrome/myalgic encephalomyelitis: A systematic literature review. Exercise Immunology Review 20:94-116.
Nisenbaum, R., M. Reyes, A. C. Mawle, and W. C. Reeves. 1998. Factor analysis of unexplained severe fatigue and interrelated symptoms: Overlap with criteria for chronic fatigue syndrome. American Journal of Epidemiology 148(1):72-77.
Nisenbaum, R., J. F. Jones, E. R. Unger, M. Reyes, and W. C. Reeves. 2003. A population-based study of the clinical course of chronic fatigue syndrome. Health & Quality of Life Outcomes 1:49.
Nisenbaum, R., M. Reyes, E. R. Unger, and W. C. Reeves. 2004. Factor analysis of symptoms among subjects with unexplained chronic fatigue: What can we learn about chronic fatigue syndrome? Journal of Psychosomatic Research 56(2):171-178.
Ocon, A. J., Z. R. Messer, M. S. Medow, and J. M. Stewart. 2012. Increasing orthostatic stress impairs neurocognitive functioning in chronic fatigue syndrome with postural tachycardia syndrome. Clinical Science 122(5):227-238.
Okamoto, L. E., S. R. Raj, and I. Biaggioni. 2012a. Chronic fatigue syndrome and the autonomic nervous system. In Primer on the Autonomic Nervous System, 3rd ed., edited by D. Robertson, I. Biaggioni, G. Burnstock, P. A. Low, and J. F. R. Paton. Oxford: Academic Press. Pp. 531-534.
Okamoto, L. E., S. R. Raj, A. Peltier, A. Gamboa, C. Shibao, A. Diedrich, B. K. Black, D. Robertson, and I. Biaggioni. 2012b. Neurohumoral and haemodynamic profile in postural tachycardia and chronic fatigue syndromes. Clinical Science 122(4):183-192.
Oliveira, M. G., S. Garbuio, E. C. Treptow, J. F. Polese, S. Tufik, L. E. Nery, and L. Bittencourt. 2014. The use of portable monitoring for sleep apnea diagnosis in adults. Expert Review of Respiratory Medicine 8(1):123-132.
Owen, A. M., K. M. McMillan, A. R. Laird, and E. Bullmore. 2005. N-back working memory paradigm: A meta-analysis of normative functional neuroimaging studies. Human Brain Mapping 25(1):46-59.
Parsaik, A., T. G. Allison, W. Singer, D. M. Sletten, M. J. Joyner, E. E. Benarroch, P. A. Low, and P. Sandroni. 2012. Deconditioning in patients with orthostatic intolerance. Neurology 79(14):1435-1439.
Paul, L., L. Wood, W. M. H. Behan, and W. M. Maclaren. 1999. Demonstration of delayed recovery from fatiguing exercise in chronic fatigue syndrome. European Journal of Neurology 6(1):63-69.
Peterson, P. K., S. A. Sirr, F. C. Grammith, C. H. Schenck, A. M. Pheley, S. Hu, and C. C. Chao. 1994. Effects of mild exercise on cytokines and cerebral blood flow in chronic fatigue syndrome patients. Clinical and Diagnostic Laboratory Immunology 1(2):222-226.
Peterson, P. K., A. Pheley, J. Schroeppel, C. Schenck, P. Marshall, A. Kind, J. M. Haugland, L. J. Lambrecht, S. Swan, and S. Goldsmith. 1998. A preliminary placebo-controlled crossover trial of fludrocortisone for chronic fatigue syndrome. Archives of Internal Medicine 158(8):908-914.
Picavet, H. S., and N. Hoeymans. 2004. Health related quality of life in multiple musculoskeletal diseases: SF-36 and EQ-5d in the DMC3 study. Annals of the Rheumatic Diseases 63(6):723-729.
Plash, W. B., A. Diedrich, I. Biaggioni, E. M. Garland, S. Y. Paranjape, B. K. Black, W. D. Dupont, and S. R. Raj. 2013. Diagnosing postural tachycardia syndrome: Comparison of tilt testing compared with standing haemodynamics. Clinical Science (London) 124(2):109-114.
Poole, J., R. Herrell, S. Ashton, J. Goldberg, and D. Buchwald. 2000. Results of isoproterenol tilt table testing in monozygotic twins discordant for chronic fatigue syndrome. Archives of Internal Medicine 160(22):3461-3468.
Puri, B. K., P. M. Jakeman, M. Agour, K. D. Gunatilake, K. A. Fernando, A. I. Gurusinghe, I. H. Treasaden, A. D. Waldman, and P. Gishen. 2012. Regional grey and white matter volumetric changes in myalgic encephalomyelitis (chronic fatigue syndrome): A voxelbased morphometry 3 T MRI study. British Journal of Radiology 85(1015):e270-e273.
Qanneta, R. 2013. Obstructive sleep apnea syndrome manifested as a subset of chronic fatigue syndrome: A comorbidity or an exclusion criterion? Rheumatology International 1-2.
Qanneta, R. 2014. Obstructive sleep apnea syndrome manifested as a subset of chronic fatigue syndrome: A comorbidity or an exclusion criterion? Rheumatology International 34(3):441-442.
Rahman, K., A. Burton, S. Galbraith, A. Lloyd, and U. Vollmer-Conna. 2011. Sleep-wake behavior in chronic fatigue syndrome. Sleep: Journal of Sleep and Sleep Disorders Research 34(5):671-678.
Raj, S. R. 2013. Postural Orthostatic Tachycardia Syndrome (POTS). Circulation 127(23): 2336-2342.
RAND. 1984. RAND 36-Item Health Survey. http://www.rand.org/health/surveys_tools/mos/mos_core_36item_survey.html (accessed January 14, 2015).
Ray, C., W. R. C. Weir, S. Phillips, and S. Cullen. 1992. Development of a measure of symptoms in chronic fatigue syndrome: The Profile of Fatigue-Related Symptoms (PFRS). Psychology & Health 7(1):27-43.
Razumovsky, A. Y., K. DeBusk, H. Calkins, S. Snader, K. E. Lucas, P. Vyas, D. F. Hanley, and P. C. Rowe. 2003. Cerebral and systemic hemodynamics changes during upright tilt in chronic fatigue syndrome. Journal of Neuroimaging 13(1):57-67.
Reeves, W. C., C. Heim, E. M. Maloney, L. S. Youngblood, E. R. Unger, M. J. Decker, J. F. Jones, and D. B. Rye. 2006. Sleep characteristics of persons with chronic fatigue syndrome and non-fatigued controls: Results from a population-based study. BMC Neurology 6.
Reynolds, G. K., D. P. Lewis, A. M. Richardson, and B. A. Lidbury. 2013. Comorbidity of postural orthostatic tachycardia syndrome and chronic fatigue syndrome in an Australian cohort. Journal of Internal Medicine 275(4):409-417.
Rosen, C. L., D. Auckley, R. Benca, N. Foldvary-Schaefer, C. Iber, V. Kapur, M. Rueschman, P. Zee, and S. Redline. 2012. A multisite randomized trial of portable sleep studies and positive airway pressure autotitration versus laboratory-based polysomnography for the diagnosis and treatment of obstructive sleep apnea: The homepap study. Sleep 35(6):757-767.
Rowe, P. C., and H. Calkins. 1998. Neurally mediated hypotension and chronic fatigue syndrome. American Journal of Medicine 105(3A):15S-21S.
Rowe, P. C., I. Bou-Holaigah, J. S. Kan, and H. Calkins. 1995. Is neurally mediated hypotension an unrecognised cause of chronic fatigue? Lancet 345(8950):623-624.
Rowe, P. C., D. F. Barron, H. Calkins, I. H. Maumenee, P. Y. Tong, and M. T. Geraghty. 1999. Orthostatic intolerance and chronic fatigue syndrome associated with Ehlers-Danlos syndrome. Journal of Pediatrics 135(4):494-499.
Rowe, P. C., H. Calkins, K. DeBusk, R. McKenzie, R. Anand, G. Sharma, B. A. Cuccherini, N. Soto, P. Hohman, S. Snader, K. E. Lucas, M. Wolff, and S. E. Straus. 2001. Fludrocortisone acetate to treat neurally mediated hypotension in chronic fatigue syndrome: A randomized controlled trial. Journal of the American Medical Association 285(1):52-59.
Salaffi, F., P. Sarzi-Puttini, R. Girolimetti, F. Atzeni, S. Gasparini, and W. Grassi. 2009. Health-related quality of life in fibromyalgia patients: A comparison with rheumatoid arthritis patients and the general population using the SF-36 Health Survey. Clinical and Experimental Rheumatology 27(5, Suppl. 56):S67-S74.
Sargent, C., G. C. Scroop, P. M. Nemeth, R. B. Burnet, and J. D. Buckley. 2002. Maximal oxygen uptake and lactate metabolism are normal in chronic fatigue syndrome. Medicine & Science in Sports & Exercise 34(1):51-56.
Schmaling, K. B., D. H. Lewis, J. I. Fiedelak, R. Mahurin, and D. S. Buchwald. 2003. Single-photon emission computerized tomography and neurocognitive function in patients with chronic fatigue syndrome. Psychosomatic Medicine 65(1):129-136.
Schondorf, R., J. Benoit, T. Wein, and D. Phaneuf. 1999. Orthostatic intolerance in the chronic fatigue syndrome. Journal of the Autonomic Nervous System 75(2-3):192-201.
Schrezenmaier, C., J. A. Gehrking, S. M. Hines, P. A. Low, L. M. Benrud-Larson, and P. Sandroni. 2005. Evaluation of orthostatic hypotension: Relationship of a new self-report instrument to laboratory-based measures. Mayo Clinic Proceedings 80(3):330-334.
Schrijvers, D., F. Van Den Eede, Y. Maas, P. Cosyns, W. Hulstijn, and B. G. C. Sabbe. 2009. Psychomotor functioning in chronic fatigue syndrome and major depressive disorder: A comparative study. Journal of Affective Disorders 115(1-2):46-53.
Sharpley, A., A. Clements, K. Hawton, and M. Sharpe. 1997. Do patients with “pure” chronic fatigue syndrome (neurasthenia) have abnormal sleep? Psychosomatic Medicine 59(6):592-596.
Short, K., M. McCabe, and G. Tooley. 2002. Cognitive functioning in chronic fatigue syndrome and the role of depression, anxiety, and fatigue. Journal of Psychosomatic Research 52(6):475-483.
Shungu, D. C., N. Weiduschat, J. W. Murrough, X. Mao, S. Pillemer, J. P. Dyke, M. S. Medow, B. H. Natelson, J. M. Stewart, and S. J. Mathew. 2012. Increased ventricular lactate in chronic fatigue syndrome. III. Relationships to cortical glutathione and clinical symptoms implicate oxidative stress in disorder pathophysiology. NMR in Biomedicine 25(9):1073-1087.
Sisto, S. A., W. Tapp, S. Drastal, M. Bergen, I. DeMasi, D. Cordero, and B. Natelson. 1995. Vagal tone is reduced during paced breathing in patients with the chronic fatigue syndrome. Clinical Autonomic Research 5(3):139-143.
Sletten, D. M., G. A. Suarez, P. A. Low, J. Mandrekar, and W. Singer. 2012. COMPASS 31: A refined and abbreviated Composite Autonomic Symptom Score. Mayo Clinic Proceedings 87(12):1196-1201.
Smets, E. M., B. Garssen, B. Bonke, and J. C. De Haes. 1995. The Multidimensional Fatigue Inventory (MFI) psychometric qualities of an instrument to assess fatigue. Journal of Psychosomatic Research 39(3):315-325.
Smith, A. P., L. Borysiewicz, J. Pollock, M. Thomas, K. Perry, and M. Llewelyn. 1999. Acute fatigue in chronic fatigue syndrome patients. Psychological Medicine 29(2):283-290.
Smith, G. A., and M. Carew. 1987. Decision time unmasked: Individuals adopt different strategies. Australian Journal of Psychology 39(3):339-351.
Snell, C. R., S. R. Stevens, T. E. Davenport, and J. M. Van Ness. 2013. Discriminative validity of metabolic and workload measurements for identifying people with chronic fatigue syndrome. Physical Therapy 93(11):1484-1492.
Soetekouw, P., J. W. M. Lenders, G. Bleijenberg, T. Thien, and J. W. M. van der Meer. 1999. Autonomic function in patients with chronic fatigue syndrome. Clinical Autonomic Research 9(6):334-340.
Sorensen, B., J. E. Streib, M. Strand, B. Make, P. C. Giclas, M. Fleshner, and J. F. Jones. 2003. Complement activation in a model of chronic fatigue syndrome. Journal of Allergy & Clinical Immunology 112(2):397-403.
Spitzer, A. R., and M. Broadman. 2010a. A retrospective review of the sleep characteristics in patients with chronic fatigue syndrome and fibromyalgia. Pain Practice 10(4):294-300.
Spitzer, A. R., and M. Broadman. 2010b. Treatment of the narcoleptiform sleep disorder in chronic fatigue syndrome and fibromyalgia with sodium oxybate. Pain Practice 10(1): 54-59.
Spotila, J. 2010. Post-exertional malaise in chronic fatigue syndrome. Charlotte, NC: CFIDS Association of America.
Stewart, J. M., M. H. Gewitz, A. Weldon, and J. Munoz. 1999. Patterns of orthostatic intolerance: The orthostatic tachycardia syndrome and adolescent chronic fatigue. Journal of Pediatrics 135(2, Pt. 1):218-225.
Stewart, J. M., M. S. Medow, Z. R. Messer, I. L. Baugham, C. Terilli, and A. J. Ocon. 2012. Postural neurocognitive and neuronal activated cerebral blood flow deficits in young chronic fatigue syndrome patients with postural tachycardia syndrome. American Journal of Physiology—Heart & Circulatory Physiology 302(5):H1185-H1194.
Streeten, D. H. P. 2001. Role of impaired lower-limb venous innervation in the pathogenesis of the chronic fatigue syndrome. American Journal of the Medical Sciences 321(3):163-167.
Streeten, D. H., and G. H. Anderson, Jr. 1992. Delayed orthostatic intolerance. Archives of Internal Medicine 152(5):1066-1072.
Streeten, D. H. P., and D. S. Bell. 1998. Circulating blood volume in chronic fatigue syndrome. Journal of Chronic Fatigue Syndrome 4(1):3-11.
Streeten, D. H. P., D. Thomas, and D. S. Bell. 2000. The roles of orthostatic hypotension, orthostatic tachycardia, and subnormal erythrocyte volume in the pathogenesis of the chronic fatigue syndrome. American Journal of the Medical Sciences 320(1):1-8.
Suarez, G. A., T. L. Opfer-Gehrking, K. P. Offord, E. J. Atkinson, P. C. O’Brien, and P. A. Low. 1999. The autonomic symptom profile: A new instrument to assess autonomic symptoms. Neurology 52(3):523-528.
Takenaka, K., Y. Suzuki, K. Uno, M. Sato, T. Komuro, Y. Haruna, H. Kobayashi, K. Kawakubo, M. Sonoda, M. Asakawa, K. Nakahara, and A. Gunji. 2002. Effects of rapid saline infusion on orthostatic intolerance and autonomic tone after 20 days bed rest. American Journal of Cardiology 89(5):557-561.
Tanaka, H., R. Matsushima, H. Tamai, and Y. Kajimoto. 2002. Impaired postural cerebral hemodynamics in young patients with chronic fatigue with and without orthostatic intolerance. Journal of Pediatrics 140(4):412-417.
Taylor, H. L., E. Buskirk, and A. Henschel. 1955. Maximal oxygen intake as an objective measure of cardio-respiratory performance. Journal of Applied Physiology 8(1):73-80.
Taylor, R. R., L. A. Jason, and C. J. Curie. 2002. Prognosis of chronic fatigue in a community-based sample. Psychosomatic Medicine 64(2):319-327.
Thieben, M. J., P. Sandroni, D. M. Sletten, L. M. Benrud-Larson, R. D. Fealey, S. Vernino, V. A. Lennon, W. K. Shen, and P. A. Low. 2007. Postural orthostatic tachycardia syndrome: The Mayo Clinic experience. Mayo Clinic Proceedings 82(3):308-313.
Thorpy, M. J. 1992. The clinical use of the multiple sleep latency test. The standards of practice committee of the American sleep disorders association. Sleep 15(3):268-276.
Tiersky, L. A., S. K. Johnson, G. Lange, B. H. Natelson, and J. DeLuca. 1997. Neuropsychology of chronic fatigue syndrome: A critical review. Journal of Clinical and Experimental Neuropsychology 19(4):560-586.
Tiersky, L. A., R. J. Matheis, J. DeLuca, G. Lange, and B. H. Natelson. 2003. Functional status, neuropsychological functioning, and mood in chronic fatigue syndrome (CFS): Relationship to psychiatric disorder. Journal of Nervous and Mental Disease 191(5):324-331.
Timmers, H. J., W. Wieling, P. M. Soetekouw, G. Bleijenberg, J. W. van der Meer, and J. W. Lenders. 2002. Hemodynamic and neurohumoral responses to head-up tilt in patients with chronic fatigue syndrome. Clinical Autonomic Research 12(4):273-280.
Togo, F., and B. H. Natelson. 2013. Heart rate variability during sleep and subsequent sleepiness in patients with chronic fatigue syndrome. Autonomic Neuroscience: Basic and Clinical 176(1-2):85-90.
Togo, F., B. H. Natelson, N. S. Cherniack, J. FitzGibbons, C. Garcon, and D. M. Rapoport. 2008. Sleep structure and sleepiness in chronic fatigue syndrome with or without coexisting fibromyalgia. Arthritis Research & Therapy 10(3):R56.
Togo, F., B. H. Natelson, N. S. Cherniack, M. Klapholz, D. M. Rapoport, and D. B. Cook. 2010. Sleep is not disrupted by exercise in patients with chronic fatigue syndromes. Medicine & Science in Sports & Exercise 42(1):16-22.
Togo, F., G. Lange, B. H. Natelson, and K. S. Quigley. 2013. Attention network test: Assessment of cognitive function in chronic fatigue syndrome. Journal of Neuropsychology. http://onlinelibrary.wiley.com/doi/10.1111/jnp.12030/pdf (accessed January 14, 2015).
Tomfohr, L. M., S. Ancoli-Israel, J. S. Loredo, and J. E. Dimsdale. 2011. Effects of continuous positive airway pressure on fatigue and sleepiness in patients with obstructive sleep apnea: Data from a randomized controlled trial. Sleep 34(1):121-126.
Trivedi, M. H., A. J. Rush, R. Armitage, C. M. Gullion, B. D. Grannemann, P. J. Orsulak, and H. P. Roffwarg. 1999. Effects of fluoxetine on the polysomnogram in outpatients with major depression. Neuropsychopharmacology 20(5):447-459.
Unger, E. R., R. Nisenbaum, H. Moldofsky, A. Cesta, C. Sammut, M. Reyes, and W. C. Reeves. 2004. Sleep assessment in a population-based study of chronic fatigue syndrome. BMC Neurology 4.
Unger, E. R., A. H. Miller, J. F. Jones, D. F. Drake, H. Tian, and G. Pagnoni. 2012. Decreased basal ganglia activation in chronic fatigue syndrome subjects is associated with increased fatigue. The FASEB Journal 26.
Van de Luit, L., J. Van der Meulen, T. J. M. Cleophas, and A. H. Zwinderman. 1998. Amplified amplitudes of circadian rhythms and night time hypotension in patients with chronic fatigue syndrome; improvement by inopamil but not by melatonin. European Journal of Internal Medicine 9(2):99-103.
Van Den Eede, F., G. Moorkens, W. Hulstijn, Y. Maas, D. Schrijvers, S. R. Stevens, P. Cosyns, S. J. Claes, and B. G. C. Sabbe. 2011. Psychomotor function and response inhibition in chronic fatigue syndrome. Psychiatry Research 186(2-3):367-372.
Van Oosterwijck, J., J. Nijs, M. Meeus, I. Lefever, L. Huybrechts, L. Lambrecht, and L. Paul. 2010. Pain inhibition and postexertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome: An experimental study. Journal of Internal Medicine 268(3):265-278.
VanNess, J. M., C. R. Snell, and S. R. Stevens. 2007. Diminished cardiopulmonary capacity during post-exertional malaise. Journal of Chronic Fatigue Syndrome 14:77-85.
VanNess, J. M., S. R. Stevens, L. Bateman, T. L. Stiles, and C. R. Snell. 2010. Postexertional malaise in women with chronic fatigue syndrome. Journal of Women’s Health 19(2):239-244.
Vercoulen, J. H. M. M., E. Bazelmans, C. M. A. Swanink, J. M. D. Galama, J. F. M. Fennis, J. W. M. van der Meer, and G. Bleijenberg. 1998. Evaluating neuropsychological impairment in chronic fatigue syndrome. Journal of Clinical and Experimental Neuropsychology 20(2):144-156.
Vermeulen, R. C., and H. R. Scholte. 2003. Rupture of silicone gel breast implants and symptoms of pain and fatigue. Journal of Rheumatology 30(10):2263-2267.
Vermeulen, R. C. W., R. M. Kurk, F. C. Visser, W. Sluiter, and H. R. Scholte. 2010. Patients with chronic fatigue syndrome performed worse than controls in a controlled repeated exercise study despite a normal oxidative phosphorylation capacity. Journal of Translational Medicine 8(93).
Wagner, D., R. Nisenbaum, C. Heim, J. F. Jones, E. R. Unger, and W. C. Reeves. 2005. Psychometric properties of the CDC symptom inventory for assessment of chronic fatigue syndrome. Population Health Metrics 3:8.
Ware, J. E. 2002. SF-36 Health Survey. In Chronic fatigue and chronic fatigue syndrome: A co-twin control study of functional status. Quality of Life Research 11:463-471.
Watson, N. F., V. Kapur, L. M. Arguelles, J. Goldberg, D. F. Schmidt, R. Armitage, and D. Buchwald. 2003. Comparison of subjective and objective measures of insomnia in monozygotic twins discordant for chronic fatigue syndrome. Sleep 26(3):324-328.
Watson, N. F., C. Jacobsen, J. Goldberg, V. Kapur, and D. Buchwald. 2004. Subjective and objective sleepiness in monozygotic twins discordant for chronic fatigue syndrome. Sleep 27(5):973-977.
Weltman, A., D. Snead, P. Stein, R. Seip, R. Schurrer, R. Rutt, and J. Weltman. 1990. Reliability and validity of a continuous incremental treadmill protocol for the determination of lactate threshold, fixed blood lactate concentrations, and VO2max. International Journal of Sports Medicine 11(1):26-32.
Whelton, C. L., I. Salit, and H. Moldofsky. 1992. Sleep, Epstein-Barr virus infection, musculoskeletal pain, and depressive symptoms in chronic fatigue syndrome. Journal of Rheumatology 19(6):939-943.
White, A. T., A. R. Light, R. W. Hughen, L. Bateman, T. B. Martins, H. R. Hill, and K. C. Light. 2010. Severity of symptom flare after moderate exercise is linked to cytokine activity in chronic fatigue syndrome. Psychophysiology 47(4):615-624.
White, A. T., A. R. Light, R. W. Hughen, T. A. VanHaitsma, and K. C. Light. 2012. Differences in metabolite-detecting, adrenergic, and immune gene expression after moderate exercise in patients with chronic fatigue syndrome, patients with multiple sclerosis, and healthy controls. Psychosomatic Medicine 74(1):46-54.
Whitehead, L. 2009. The measurement of fatigue in chronic illness: A systematic review of unidimensional and multidimensional fatigue measures. Journal of Pain and Symptom Management 37(1):107-128.
Wiborg, J. F., S. van der Werf, J. B. Prins, and G. Bleijenberg. 2010. Being homebound with chronic fatigue syndrome: A multidimensional comparison with outpatients. Psychiatry Research 177(1-2):246-249.
Wilson, A., I. Hickie, A. Lloyd, D. Hadzi-Pavlovic, C. Boughton, J. Dwyer, and D. Wakefield. 1994. Longitudinal study of outcome of chronic fatigue syndrome. British Medical Journal 308(6931):756-759.
Winkler, A. S., D. Blair, J. T. Marsden, T. J. Peters, S. Wessely, and A. J. Cleare. 2004. Autonomic function and serum erythropoietin levels in chronic fatigue syndrome. Journal of Psychosomatic Research 56(2):179-183.
Wyller, V. B., R. Barbieri, E. Thaulow, and J. P. Saul. 2008. Enhanced vagal withdrawal during mild orthostatic stress in adolescents with chronic fatigue. Annals of Noninvasive Electrocardiology 13(1):67-73.
Yamaguti, K., S. Tajima, and H. Kuratsune. 2013. Autonomic dysfunction in chronic fatigue syndrome. Advances in Neuroimmune Biology 4(4):281-289.
Yamamoto, Y., J. J. LaManca, and B. H. Natelson. 2003. A measure of heart rate variability is sensitive to orthostatic challenge in women with chronic fatigue syndrome. Experimental Biology & Medicine 228(2):167-174.
Yataco, A., H. Talo, P. Rowe, D. A. Kass, R. D. Berger, and H. Calkin. 1997. Comparison of heart rate variability in patients with chronic fatigue syndrome and controls. Clinical Autonomic Research 7(6):293-297.
Yoshiuchi, K., D. B. Cook, K. Ohashi, H. Kumano, T. Kuboki, Y. Yamamoto, and B. H. Natelson. 2007. A real-time assessment of the effect of exercise in chronic fatigue syndrome. Physiology & Behavior 92(5):963-968.
Zhang, L., J. Gough, D. Christmas, D. L. Mattey, S. C. Richards, J. Main, D. Enlander, D. Honeybourne, J. G. Ayres, D. J. Nutt, and J. R. Kerr. 2010. Microbial infections in eight genomic subtypes of chronic fatigue syndrome/myalgic encephalomyelitis. Journal of Clinical Pathology 63(2):156-164.
This page intentionally left blank.






































































