ABSTRACT
Approximately 20 percent of Americans are affected by mental health and substance use disorders, which are associated with significant morbidity and mortality. While the evidence base for the effectiveness of interventions to treat these disorders is sizable, a considerable gap exists between what is known to be effective and interventions that are actually delivered in clinical care. Addressing this quality chasm in mental health and substance use care is particularly critical given the recent passage of the Patient Protection and Affordable Care Act (ACA) and the Mental Health Parity and Addiction Equity Act, which are changing the delivery of care and access to treatments for mental health and substance use disorders. Increasing emphasis on accountability and performance measurement, moreover, will require strategies to promote and measure the quality of psychosocial interventions.
In this report, the study committee develops a framework that can be used to chart a path toward the ultimate goal of improving the outcomes of psychosocial interventions for those with mental health and substance use disorders. This framework identifies the key steps entailed in successfully bringing an evidence-based psychosocial intervention into clinical practice. It highlights the need
_____________
1 This summary does not include references. Citations for the discussion presented in the summary appear in the subsequent report chapters.
to (1) support research to strengthen the evidence base on the efficacy and effectiveness of psychosocial interventions; (2) based on this evidence, identify the key elements that drive an intervention’s effect; (3) conduct systematic reviews to inform clinical guidelines that incorporate these key elements; (4) using the findings of these systematic reviews, develop quality measures—measures of the structure, process, and outcomes of interventions; and (5) establish methods for successfully implementing and sustaining these interventions in regular practice, including the training of providers of these interventions. The committee intends for this framework to be an iterative one, with the results of the process being fed back into the evidence base and the cycle beginning anew. Central to the framework is the importance of using the consumer perspective to inform the process.
The recommendations offered in this report are intended to assist policy makers, health care organizations, and payers that are organizing and overseeing the provision of care for mental health and substance use disorders while navigating a new health care landscape. The recommendations also target providers, professional societies, funding agencies, consumers, and researchers, all of whom have a stake in ensuring that evidence-based, high-quality care is provided to individuals receiving mental health and substance use services.
Mental health and substance use disorders affect approximately 20 percent of Americans and are associated with significant morbidity and mortality. Although the current evidence base for the effects of psychosocial interventions is sizable, subsequent steps in the process of bringing a psychosocial intervention into routine clinical care are less well defined. The data from research supporting these interventions have not been well synthesized, and it can be difficult for consumers, providers, and payers to know what treatments are effective. This report details the reasons for the gap between what is known to be effective and current practice and offers recommendations for how best to address this gap by applying a framework that can be used to establish standards for psychosocial interventions.
Addressing the need for standards in mental health and substance use care is particularly critical given the recent passage of the Patient Protection and Affordable Care Act (ACA) and the Mental Health Parity and Addiction Equity Act. The ACA is aimed at reforming how care is delivered, with an emphasis on accountability and performance measurement, while the Mental Health Parity and Addiction Equity Act is intended to address
limits on access to behavioral health care services. Without accepted and endorsed quality standards for psychosocial care, however, there may still be reluctance to promote appropriate use of these treatments. To counter pressures to limit access to psychosocial care, it is critical to promote the use of effective psychosocial interventions and to develop strategies for monitoring the quality of interventions provided.
In this context, the Institute of Medicine (IOM) convened an ad hoc committee to create a framework for establishing the evidence base for psychosocial interventions, and to describe the elements of effective interventions and the characteristics of effective service delivery systems.
STUDY CHARGE AND APPROACH
The American Psychiatric Association, American Psychological Association, Association for Behavioral Health and Wellness, National Association of Social Workers, National Institutes of Health, the Office of the Assistant Secretary for Planning and Evaluation within the U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, U.S. Department of Veterans Affairs, asked the IOM to convene a committee to develop a framework for establishing standards for psychosocial interventions used to treat mental health and substance use disorders (see Box S-1 for the committee’s full statement of task). Reflecting the complexity of this task, the 16-member committee comprised experts in a variety of disciplines, including psychiatry, psychology, social work, nursing, primary care, public health, and health policy. Members’ areas of expertise encompassed clinical practice, quality and performance measurement, intervention development and evaluation, operation of health systems, implementation science, and professional education, as well as the perspectives of individuals who have been affected by mental health disorders. The scope of this study encompasses the full range of mental health and substance use disorders, age and demographic groups, and psychosocial interventions.
To complete its work, the committee convened for 5 meetings over the course of 12 months. It held public workshops in conjunction with two of these meetings to obtain additional information on specific aspects of the study charge (see Appendix A for further information).
KEY FINDINGS, CONCLUSIONS, AND RECOMMENDATIONS
The recommendations offered in this report are intended to assist policy makers, health care organizations, and payers that are organizing and overseeing the provision of care for mental health and substance use disorders while navigating a new health care landscape. The recommendations
The Institute of Medicine will establish an ad hoc committee that will develop a framework to establish efficacy standards for psychosocial interventions used to treat mental disorders. The committee will explore strategies that different stakeholders might take to help establish these standards for psychosocial treatments. Specifically, the committee will:
- Characterize the types of scientific evidence and processes needed to establish the effectiveness of psychosocial interventions.
- – Define levels of scientific evidence based on their rigor.
- – Define the types of studies needed to develop quality measures for monitoring quality of psychosocial therapies and their effectiveness.
- – Define the evidence needed to determine active treatment elements as well as their dose and duration.
- Using the best available evidence, identify the elements of psychosocial treatments that are most likely to improve a patient’s mental health and can be tracked using quality measures. In addition, identify features of health care delivery systems involving psychosocial therapies that are most indicative of high-quality care that can be practically tracked as part of a system of quality measures. The following approaches to quality measurement should be considered:
- – Measures to determine if providers implement treatment in a manner that is consistent with evidence-based standards;
- – Measures that encourage continuity of treatment;
- – Measures that assess whether providers have the structures and processes in place to support effective psychotherapy;
- – Consumer-reported experiences of evidence-based psychosocial care; and
- – Consumer-reported outcomes using a measurement-based care approach.
also target providers, professional societies, funding agencies, consumers, and researchers, all of whom have a stake in ensuring that evidence-based, high-quality care is provided to individuals receiving mental health and substance use services. The committee’s conclusions and recommendations are based on its review of the scientific evidence, information gathered in its public workshops, and the expert judgment of its members.2 The commit-
_____________
2 The committee’s recommendations are numbered according to the chapter of the report in which they appear. Thus, for example, recommendation 2-1 is the first recommendation in Chapter 2. For purposes of clarity, some recommendations are presented in this summary in a different sequence from that in which they appear in the full report; however, their numeric designation remains the same.
tee offers recommendations for each component of its framework, which collectively offer a roadmap for implementing evidence-based psychosocial interventions.
Need for a Framework to Establish and Apply Efficacy Standards for Psychosocial Interventions
Mental health disorders encompass a range of conditions, including, for example, neurodevelopmental, anxiety, trauma, depressive, eating, personality, and psychotic disorders. Substance use disorders entail recurrent use of alcohol and legal or illegal drugs (e.g., cannabis, stimulants, hallucinogens, opioids) that cause significant impairment.
Mental health and substance use disorders are prevalent, affecting approximately 20 percent of the U.S. population. Moreover, the two categories of disorders are often comorbid, occurring together. The rate of comorbidity of mental, substance use, and physical disorders also is high. Approximately 18 percent of cancer patients, for example, have a comorbid mental health disorder. Comorbidity of any type leads to reduced compliance with medication, greater disability, and poorer chance of recovery. People with comorbid mental health, substance use, and physical disorders also are at increased risk of premature mortality from a variety of causes.
For purposes of this study, the committee defines psychosocial interventions for mental health and substance use disorders as interpersonal or informational activities, techniques, or strategies that target biological, behavioral, cognitive, emotional, interpersonal, social, or environmental factors with the aim of reducing symptoms of these disorders and improving functioning or well-being. These interventions include psychotherapies (e.g., psychodynamic therapy, cognitive-behavioral therapy, interpersonal psychotherapy, problem solving therapy), community-based treatments (e.g., assertive community treatment, first episode psychosis interventions), vocational rehabilitation, peer support services, and integrated care interventions. Interventions can be delivered in a variety of settings (e.g., outpatient clinics, individual provider offices, primary care clinics, schools, hospitals, community settings, and virtual settings such as telephone and video conferencing). Interventions occur in different formats (such as individual, family, group, computer-based) and can be administered by a variety of providers, from social workers, psychiatrists, and psychologists to religious leaders and peer providers. Psychosocial interventions can be stand-alone treatments or can be combined with other interventions, such as medication, for a range of disorders or problems. In addition, interventions can address psychosocial problems that negatively impact adherence to medical treatments or can deal with the interpersonal and social challenges present during recovery from a mental health or substance use problem. Sometimes multiple psychosocial interventions are employed.
The efficacy of a broad range of psychosocial interventions has been established through hundreds of randomized controlled clinical trials and numerous meta-analyses (described below). However, the quality of care that is actually delivered is less than ideal. Evidence-based psychosocial interventions often are not taught in programs training mental health and substance use providers and often are not available as part of routine clinical care for mental health and substance use disorders. This gap between what is known to be effective and the actual delivery of care is due to problems of access, insurance coverage, and fragmentation of care (different systems of providers, separation of primary and specialty care, different entities sponsoring and paying for care, and poor coordination of care, as well as variability in the training of numerous types of providers and the lack of requirements that evidence-based interventions be taught in training programs).
Over the course of its early meetings, it became clear to the committee that the development of the framework called for in its statement of task would be critical to charting a path toward the ultimate goal of improving the outcomes of psychosocial interventions for those with mental health and substance use disorders. In the context of developing this framework, the committee did not conduct a comprehensive literature review of efficacious interventions or systematically identify the evidence-based elements of interventions, but rather used the best of what is known about the establishment of an evidence-based intervention to build a framework that would make it possible to fully realize the high-quality implementation of evidence-based interventions in everyday care.
While this report addresses the types of studies needed to build an evidence base and the best methods for each phase of intervention development, testing, and dissemination, it does not create a compendium of study types and their respective rigor. Instead, it emphasizes via the framework the iterative nature of intervention science and the evolving methodologies that will be required to meet the psychosocial needs of individuals with mental health and substance use disorders. In this light, the committee does not define levels of scientific rigor in establishing an intervention as evidence based or specify the many interventions that have crossed the threshold for being identified as evidence based. Rather, the committee emphasizes an iterative framework that should guide the process of establishing the evidence base for psychosocial interventions and for the systems in which the interventions are delivered.
Key Findings
The information gathered for this study led to the following key findings concerning mental health and substance use disorders and the interventions developed to treat them:
- Mental health and substance use disorders are a serious public health problem.
- A wide variety of psychosocial interventions play a major role in the treatment of mental health and substance use disorders.
- Psychosocial interventions that have been demonstrated to be effective in research settings are not used routinely in clinical practice or taught in educational programs training mental health professionals who deliver psychosocial interventions.
- No standard system is in place to ensure that the psychosocial interventions delivered to patients/consumers are effective.
A Proposed Framework for Improving the Quality and Delivery of Psychosocial Interventions
Figure S-1 depicts the committee’s framework, which identifies the key steps in successfully bringing an evidence-based psychosocial intervention into clinical practice. This framework highlights the need to
- support research to strengthen the evidence base on the efficacy and effectiveness of psychosocial interventions;
- based on this evidence, identify the key elements that drive the effects of an intervention;
- conduct systematic reviews to inform clinical guidelines that incorporate these key elements;
- using the findings of these systematic reviews, develop quality measures—measures of the structure, process, and outcomes of interventions; and
- establish methods for successfully implementing and sustaining these interventions in regular practice.
Central to this framework is the consumer perspective in informing the process. Evidence shows that consumers bring important perspectives and knowledge of mental health and substance use disorders. As applied to this framework, consumer involvement is important in identifying and formulating research questions for systematic review, helping to develop guideline recommendations, informing the development of quality measures, and monitoring the implementation of interventions. Consumer participation
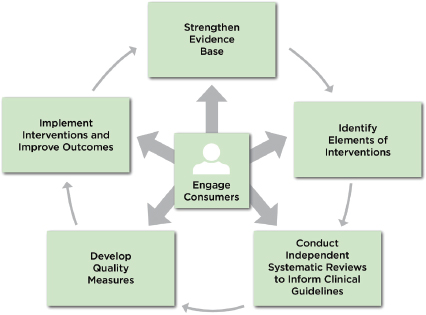
FIGURE S-1 Framework for developing standards for psychosocial interventions.
of this nature can lead to the development of interventions that address outcomes of importance to consumers, which in turn can lead to their increased participation in the interventions.
Importantly, the committee intends for the framework to be an iterative one, with the results of the process being fed back into the evidence base and the cycle beginning anew. Much has been done to establish the current evidence base for psychosocial interventions, but much more needs to be done to improve the quality of that evidence base; create new evidence-based interventions; engage consumers in this process; train the providers of psychosocial interventions; and ultimately streamline the process of developing, testing, implementing, and disseminating interventions that address the psychosocial needs of those with mental health and substance use problems.
The committee drew the following conclusions about the need for a framework:
The mental health and substance use care delivery system needs a framework for applying strategies to improve the evidence base for and increase the uptake of high-quality evidence-based interventions in the delivery of care.
Broad stakeholder involvement is necessary to develop effective interventions that will lead to improved outcomes for individuals with mental health and substance use disorders.
Recommendation 2-1. Use the committee’s framework for improving patient outcomes through psychosocial interventions to strengthen the evidence base. The U.S. Department of Health and Human Services should adopt the committee’s framework to guide efforts to support policy, research, and implementation strategies designed to promote the use of evidence-based psychosocial interventions. Steps in this iterative process should focus on
- strengthening the evidence base for interventions,
- identifying key elements of interventions,
- conducting independent systematic reviews to inform clinical guidelines,
- developing quality measures for interventions, and
- implementing interventions and improving outcomes.
This is a complex process, and the framework is intended to be used to guide a continuous progression. At each step in the process, systematic research and evaluation approaches should be applied to iteratively expand the knowledge base for the development of new and improved standards for psychosocial interventions that will improve patient outcomes.
Recommendation 2-2. Require consumer engagement. The U.S. Department of Health and Human Services and other public and private funding agencies should ensure that consumers are active participants in the development of practice guidelines, quality measures, policies, and implementation strategies for, as well as research on, psychosocial interventions for people with mental health and substance use disorders, and provide appropriate incentives to that end. In addition, family members of consumers should be provided with opportunities to participate in such activities.
Strengthen the Evidence Base
The framework’s cycle begins with strengthening the evidence base for identifying effective psychosocial interventions and their key elements. The data on these interventions are compelling. A number of meta-analyses have established the effects of psychosocial interventions on mental health and substance use disorders. Psychotherapies in particular have been subject to
numerous meta-analyses. Few meta-analyses exist for other types of psychosocial interventions, such as suicide prevention programs, vocational rehabilitation, and clinical case management. However, these interventions have been subjected to randomized clinical trials and have been shown to have positive effects on the intended intervention target. Although meta-analyses support the use of psychosocial interventions in the treatment of mental health and substance use problems, additional studies are needed to further determine the utility of these interventions in different populations and settings, as well as to determine who is most capable of delivering the interventions, what the interventions’ limitations are, and how best to implement them. Finally, there is a need to develop and test new interventions that are more effective and address currently unmet needs.
Identify Key Elements of Interventions
Once the evidence base for psychosocial interventions has been expanded, the next step is to identify the key elements that drive the effects of the interventions. Most evidence-based psychosocial interventions are standardized, and these standards are detailed in treatment manuals. Most if not all evidence-based, manualized psychosocial interventions are packages of multiple elements. An element is a therapeutic activity, technique, or strategy that is categorized as either “nonspecific”—fundamental, and occurring in most if not all psychosocial interventions (e.g., a trusting relationship with a therapist)—or “specific”—unique to a particular theoretical orientation and approach (e.g., systematic exposure to feared objects, a specific element of cognitive-behavioral therapy for anxiety). The application of effective interventions involves assembling combinations of elements that, based on evidence, are targeted to particular disorders and other patient characteristics The elements that make up evidence-based psychosocial interventions are clearly specified in measures of fidelity, which are used to ascertain whether a given intervention is implemented as intended in research studies, and to ensure that practitioners in training and practice are demonstrating competency in an intervention.
Furthermore, some elements identified as being specific are actually shared among certain manualized psychosocial interventions, although not always referred to with the same terminology, whereas others are unique. Recognition of the elements of evidence-based psychosocial interventions highlights their similarities as well as their true differences. However, this process of discovery is somewhat hampered by the lack of a common language for describing elements across different theoretical models and interventions. Examination of fidelity measures from different theoretical models indicates that different terms are used to describe the same element. For example, “using thought records” in cognitive-behavioral therapy is
likely to represent the same element as “using mood ratings” in interpersonal psychotherapy. The field would benefit from a common terminology for identifying and classifying the elements across all evidence-based psychosocial interventions.
A common terminology for specific and nonspecific elements could offer several advantages for evidence-based psychosocial interventions. It would permit researchers to use the same terms so that data could be pooled from different research groups, resulting in a much larger database than can be achieved from independent studies of manualized interventions comprising multiple elements described using different terms. This database could be used to establish the optimal sequencing and dosing of elements and for whom a given element, or set of elements, is most effective. In addition, it might be possible to connect elements more precisely to purported mechanisms of change than is the case with an entire complex psychosocial intervention. In the future, an elements framework could advance training in and implementation of evidence-based psychosocial interventions, as practitioners would learn strategies and techniques that can be applied across target problems, disorders, or contexts.
Conduct Independent Systematic Reviews to Inform Clinical Guidelines
No national, standardized, and coordinated process exists in the United States for compiling, conducting, and disseminating systematic reviews, guidelines, and implementation materials for use by providers and by those formulating guidance for implementation and for insurance coverage. Since as far back as 1982, some in the field of mental health have suggested that a regulatory body be formed to conduct high-quality systematic reviews for psychosocial interventions, much as the U.S. Food and Drug Administration regulates all medications and most medical devices. It is this approval process that informs decisions on which medications and devices can be included for coverage by health plans and should be used by providers as effective interventions. While the concept of having a single entity oversee and approve the use of psychosocial interventions has practical appeal, it has not gained traction in the field and has not been supported by Congress. In an attempt to address this gap, professional organizations, health care organizations, federal entities, nonfederal organizations, and various researchers have independently reviewed the literature on psychosocial interventions. However, the result has been sets of guidelines that often are at odds with one another, and clinicians, consumers, providers, educators, and health care organizations seeking information are given little direction as to which reviews are accurate and which guidelines should be employed.
An important challenge in creating a standardized process for reviewing evidence is the fact that systematic reviews as currently conducted are
laborious and costly, and rarely keep pace with advances in the field. To avoid the cost and timeliness problems inherent in systematic reviews, an entity charged with overseeing the reviews and their products could explore the potential for technology (e.g., the use of machine learning to augment and streamline the systematic review process) and clinical and research networks and learning environments to expedite the process and the development of updates to recommendations. In 2011, the IOM offered a set of recommendations for conducting high-quality systematic reviews. The guidelines broadly identify evidence-based treatments and approaches but generally are not designed to provide the level of detail needed to inform clinicians in the delivery of treatments to ensure reproducibility and a consistent level of quality outcomes. As a result, these guidelines would need to be modified to be more specific and ensure that information beyond intervention impact is available.
Having a process for systematically reviewing evidence is particularly important given the changes introduced under the ACA and the Mental Health Parity and Addiction Equity Act. Now more than ever, a standardized evaluation process is needed to enable the generation of reliable information to form the basis for policy and coverage decisions, curriculum development and training of clinicians, and other efforts to improve the quality of psychosocial care. Absent such a standardized process, the quality of care will continue to vary considerably. Systematic reviews need to address intervention efficacy, effectiveness, and implementation needs. Equally important is identifying the best information with which to answer these questions.
Two examples of the benefits of having a standardized, coordinated process for determining which interventions are evidence based are the National Institute for Health Care and Excellence (NICE) in the United Kingdom and the U.S. Department of Veterans Affairs’ (VA’s) Evidence-Based Synthesis Program (ESP). Both employ a coordinated process for conducting systematic reviews and creating guidelines based on internationally agreed-upon standards, and both have a process for evaluating the impact of guidelines on practice and outcomes. Based on the successes of NICE and the ESP, it is possible to develop a process for conducting systematic reviews and creating guidelines and implementation materials for psychosocial interventions, as well as a process for evaluating the impact of these tools, by leveraging existing resources.
The committee envisions a process that involves input from consumers and clinicians at every step. A potential direction is for the U.S. Department of Health and Human Services, in partnership with professional and consumer organizations, to develop a coordinated process for conducting systematic reviews of the evidence for psychosocial interventions and creating guidelines and implementation materials in accordance with the IOM
standards for guideline development. Dissemination of practice guidelines and implementation tools resulting from the reviews could be conducted by the National Registry of Evidence-based Programs and Practices (NREPP) and professional organizations.
The committee drew the following conclusion about synthesizing evidence:
Approaches applied in other areas of health care (as recommended in previous IOM reports) can be applied in compiling and synthesizing evidence to guide care for mental health and substance use disorders.
Recommendation 4-1. Expand and enhance processes for coordinating and conducting systematic reviews of psychosocial interventions and their elements. The U.S. Department of Health and Human Services, in partnership with professional and consumer organizations, should expand and enhance existing efforts to support a coordinated process for conducting systematic reviews of psychosocial interventions and their elements based on the Institute of Medicine’s recommendations for conducting high-quality systematic reviews. Research is needed to expedite the systematic review process through the use of machine learning and natural-language processing technologies to search databases for new developments.
Recommendation 4-2. Develop a process for compiling and disseminating the results of systematic reviews along with guidelines and dissemination tools. With input from the process outlined in Recommendation 4-1, the National Registry of Evidence-based Programs and Practices (NREPP) and professional organizations should disseminate guidelines, implementation tools, and methods for evaluating the impact of guidelines on practice and patient outcomes. This process should be informed by the models developed by the National Institute for Health Care and Excellence (NICE) in the United Kingdom and the U.S. Department of Veterans Affairs, and should be faithful to the Institute of Medicine standards for creating guidelines.
Develop Quality Measures
New care delivery systems and payment reforms being instituted under the ACA require measures for tracking the performance of the health care system. Quality measures are among the critical tools for health care providers and organizations during the process of transformation and improvement. To date, quality measures are lacking for key areas of mental
health and substance use treatment. Of the 31 nationally endorsed measures related to these disorders, only 2 address a psychosocial intervention (screening and brief intervention for unhealthy alcohol use). This lack of measures reflects both limitations in the evidence base for determining what treatments are effective at achieving improvements in patient outcomes and challenges faced in obtaining from existing clinical data the detailed information necessary to support quality measurement.
To guide the consideration of opportunities to develop quality measures for psychosocial interventions, the committee built on prior work to offer an approach for the development of quality measures—structure, process, and outcome measures—for psychosocial interventions.
Structure measures are necessary to ensure that key elements of care can actually be implemented in a way that conforms to the evidence base linking those elements to key outcomes. Structure measures can be used to assess providers’ training and capacity to offer evidence-based psychosocial interventions. They provide guidance on infrastructure development and best practices. They support credentialing and payment, thereby allowing purchasers and health plans both to select clinics or provider organizations that are equipped to furnish evidence-based psychosocial interventions and to provide incentives for the delivery of high-quality psychosocial care. They can support consumers in selecting providers with expertise in interventions specific to their condition or adapted to their cultural expectations. Finally, they can incorporate the capacity for the collection of outcome data.
Process measures are selected in areas where evidence from randomized controlled trials or observational studies has established an association between the provision of particular services in particular ways and the probability of achieving desired outcomes. The committee sees important opportunities to develop and apply process measures as part of a systematic, comprehensive, and balanced strategy for enhancing the quality of psychosocial interventions. While defining the processes of care associated with evidence-based psychosocial interventions is complicated, effective and efficient process measures provide important opportunities for the targeting and application of improvement strategies.
Of all quality measures, outcome measures have the greatest potential value for patients, families, clinicians, and payers because they indicate whether patients have improved or reached their highest level of function and whether full symptom or disease remission has been achieved. Importantly, outcome measures can be used to identify patients who are not responding to treatment or may require treatment modifications, to gauge individual provider and system performance, and to identify opportunities for quality improvement. Patient-reported outcomes are integral to measurement-based care, which is predicated on the use of brief, standard-
ized, and specific assessment measures for target symptoms or behaviors that guide a patient-centered action plan.
Despite the diverse players in the quality field, there is a lack of strategic leadership and responsibility for the development and testing of quality measures for mental health and substance use care in general and for psychosocial interventions in particular. Furthermore, consumers have limited involvement in the development and implementation of quality measures in this arena. Systems for accountability and improvement need to focus on improving outcomes for individuals regardless of modality of treatment. However, the infrastructure for measurement and improvement of psychosocial interventions is lacking, both at the national level for measure development and at the local level for measure implementation and reporting. Current quality measures are insufficient to drive improvement in psychosocial interventions. While there is enthusiasm for incorporating performance measures based on patient-reported outcomes, there is no consensus on which outcomes should have priority and what tools are practical and feasible for use in guiding ongoing clinical care. In addition, risk adjustment methodologies need to be developed to ensure effective use of these measures for monitoring the performance of the health care system with respect to treatment for mental health and substance use disorders.
The committee drew the following conclusion about quality measurement for psychosocial interventions:
Approaches applied in other areas of health care can be applied in care for mental health and substance use disorders to develop reliable, valid, and feasible quality measures for both improvement and accountability purposes.
Recommendation 5-2. Develop and continuously update a portfolio of measures with which to assess the structure, process, and outcomes of care. The U.S. Department of Health and Human Services (HHS) should designate a locus of responsibility and leadership for the development of quality measures related to mental health and substance use disorders, with particular emphasis on filling the gaps in measures that address psychosocial interventions. HHS should support and promote the development of a balanced portfolio of measures for assessing the structure, process, and outcomes of care, giving priority to measuring access and outcomes and establishing structures that support the monitoring and improvement of access and outcomes.
Recommendation 5-3. Support the use of health information technology for quality measurement and improvement of psychosocial interventions. Federal, state, and private payers should support investments
in the development of new and the improvement of existing data and coding systems to support quality measurement and improvement of psychosocial interventions. Specific efforts are needed to encourage broader use of health information technology and the development of data systems for tracking individuals’ care and its outcomes over time and across settings. Registries used in other specialty care, such as bariatric treatment, could serve as a model. In addition, the U.S. Department of Health and Human Services should lead efforts involving organizations responsible for coding systems to improve standard code sets for electronic and administrative data (such as Current Procedural Terminology [CPT] and Systematized Nomenclature of Medicine [SNOMED]) to allow the capture of process and outcome data needed to evaluate mental health/substance use care in general and psychosocial interventions in particular. This effort will be facilitated by the identification of the elements of psychosocial interventions and development of a common terminology as proposed under Recommendation 3-1. Electronic and administrative data should include methods for coding disorder severity and other confounding and mitigating factors to enable the development and application of risk adjustment approaches, as well as methods for documenting the use of evidence-based treatment approaches.
Implement Interventions and Improve Outcomes
A comprehensive quality framework needs to consider properties beyond interventions themselves—in particular, the context in which interventions are delivered. This context includes characteristics of the consumer, the qualifications of the provider, the clinic or specific setting in which care is rendered, characteristics of the health system or organization in which the setting is embedded, and the regulatory and financial conditions under which the system or organization operates. Stakeholders in each of these areas can manipulate various levers that can shape the quality of the psychosocial interventions delivered to patients. Stakeholders and examples of levers as their disposal include
- consumers—meaningful participation in governance, in organizational leadership positions, and as board members;
- providers—quality measurement and reporting, such as tracking outcomes for practices and for populations served;
- provider organizations—electronic data systems with which to share medical records across disciplines and sites of service;
- health plans and purchasers—benefit design, such as pay-for-performance systems; and
- regulators—accreditation and licensure to help ensure the implementation of evidence-based practices.
Ignoring the context of an intervention and shortfalls in the manipulation of available levers can render a highly efficacious intervention unhelpful or even harmful. Growing evidence suggests that multifaceted implementation strategies targeting multiple levels of service provision—consumers, providers, organizations, payers, and regulators—are most effective. Much of the evidence surrounding the use of these levers to improve quality (in health care generally) is weak but promising, and should be augmented with further research.
The committee drew the following conclusion about improving the quality of psychosocial interventions:
Multiple stakeholders should apply levers, incentives, and other means to create learning health systems that continually progress toward higher quality (as recommended in previous IOM Quality Chasm reports).
Recommendation 6-1. Adopt a system for quality improvement. Purchasers, plans, and providers should adopt systems for measuring, monitoring, and improving quality for psychosocial interventions. These systems should be aligned across multiple levels. They should include structure, process, and outcome measures and a combination of financial and nonfinancial incentives to ensure accountability and encourage continuous quality improvement for providers and the organizations in which they practice. Quality improvement systems also should include measures of clinician core competencies in the delivery of evidence-based psychosocial interventions. Public reporting systems, provider profiling, pay-for-performance, and other accountability approaches that include outcome measures should account for differences in patient case mix (e.g., using risk adjustment methods) to counteract incentives for selection behavior on the part of clinicians and provider organizations, especially those operating under risk-based payment.
Recommendation 6-2. Support quality improvement at multiple levels using multiple levers. Purchasers, health care insurers, providers, consumers, and professional organizations should pursue strategies designed to support the implementation and continuous quality improvement of evidence-based psychosocial interventions at the provider, clinical organization, and health system levels.
- The infrastructure to support high-quality treatment includes ongoing provider training, consumer and family education, supervision, consultation, and leadership to enhance organizational culture and foster a climate for continuously learning health care systems. Other core aspects of infrastructure for the implementation and quality improvement of evidence-based psychosocial interventions include the use of registries, electronic health records, and computer-based decision support systems for providers and consumers, as well as technology-supported technical assistance and training.
- This infrastructure could be fostered by a nonprofit organization, supported and funded through a public–private partnership (e.g., the Institute for Healthcare Improvement), that would provide technical assistance to support provider organizations and clinicians in quality improvement efforts.
A Research Agenda
Additional research is needed to expand the evidence base on the effectiveness of psychosocial interventions, validate strategies for applying elements approaches, develop and test quality measures, and design and evaluate implementation strategies and policies. The committee offers the following recommendations as a research agenda to further progress in each phase of the framework.
Recommendation 3-1. Conduct research to identify and validate elements of psychosocial interventions. Public and private organizations should conduct research aimed at identifying and validating the elements of evidence-based psychosocial interventions across different populations (e.g., disorder/problem area, age, sex, race/ethnicity). The development and implementation of a research agenda is needed for
- developing a common terminology for describing and classifying the elements of evidence-based psychosocial interventions;
- evaluating the sequencing, dosing, moderators, mediators, and mechanisms of action of the elements of evidence-based psychosocial interventions; and
- continually updating the evidence base for elements and their efficacy.
Recommendation 4-3. Conduct research to expand the evidence base for the effectiveness of psychosocial interventions. The National Institutes of Health should coordinate research investments among federal,
state, and private research funders, payers, and purchasers to develop and promote the adoption of evidence-based psychosocial interventions. This research should include
- randomized controlled trials to establish efficacy, complemented by other approaches encompassing field trials, observational studies, comparative effectiveness studies, data from learning environments and registries, and private-sector data;
- trials to establish the effectiveness of interventions and their elements in generalizable practice settings; and
- practice-based research networks that will provide “big data” to continuously inform the improvement and efficiency of interventions.
Recommendation 5-1. Conduct research to contribute to the development, validation, and application of quality measures. Federal, state, and private research funders and payers should establish a coordinated effort to invest in research to develop measures for assessing the structure, process, and outcomes of care, giving priority to
- measurement of access and outcomes;
- development and testing of quality measures, encompassing patient-reported outcomes in combination with clinical decision support and clinical workflow improvements;
- evaluation and improvement of the reliability and validity of measures;
- processes to capture key data that could be used for risk stratification or adjustment (e.g., severity, social support, housing);
- attention to documentation of treatment adjustment (e.g., what steps are taken when patients are not improving); and
- establishment of structures that support monitoring and improvement.
Recommendation 6-3. Conduct research to design and evaluate strategies that can influence the quality of psychosocial interventions. Research is needed to inform the design and evaluation of policies, organizational levers, and implementation/dissemination strategies that can improve the quality of psychosocial interventions and health outcomes. Potential supporters of this research include federal, state, and private entities.
- Policies should be assessed at the patient, provider, clinical organization/system, payer, purchaser, and population levels.
- Examples might include research to develop and assess the impact of benefit design changes and utilization management tools, new models of payment and delivery, systems for public reporting of quality information, and new approaches for training in psychosocial interventions.
CONCLUSION
The prevalence of mental health and substance use disorders and the impacts of these disorders on morbidity and mortality are well documented. The gap between what interventions are known to be effective and the care that is delivered, together with the changing landscape in health care, demands fundamental changes in processes used to ensure the availability and delivery of high-quality evidence-based psychosocial interventions. Determining the best ways to strengthen the evidence base, identify elements that underpin interventions, conduct systematic reviews to inform clinical guidelines, develop quality measures to track the effectiveness of interventions, and implement quality interventions to improve patient outcomes has been remarkably challenging for the field of mental health. The process of moving through each step of the committee’s framework is complex, requires evidence, and should be iterative. The committee believes that its framework and its recommendations for action can help achieve the goal of improved outcomes from psychosocial interventions for individuals suffering from mental health and substance use disorders.




















