Executive Summary
ABSTRACT Americans spend almost all of their time indoors in environments that are increasingly airtight and that often contain sources of allergens—such as dust mites, fungi, house pets, rodents, cockroaches, and certain chemicals. An increased incidence, prevalence, and severity of asthma and other allergic diseases are associated with exposure to these agents and constitute major components of the public health problems related to indoor air quality in the United States.
Methods for detecting and characterizing specific allergic diseases include taking a thorough medical history and performing skin tests, in vitro antibody tests, and pulmonary function tests. Environmental testing and exposure assessment can identify contaminants and their sources, environmental exposure media, routes of entry into the body, intensity and frequency of contact, and spatial and temporal concentration patterns. Using published data, a first-ever risk assessment in this field shows a positive relationship between cumulative exposure to mite allergen and the risk of sensitization.
Proper education of allergy sufferers and medical personnel, coupled with appropriate building design, construction, management, and engineering, can prevent many of the problems associated with indoor allergens and alleviate those that remain. Continued vigorous investigation of the problems related to indoor allergens is essential to improved public health. Recommendations focus on the need for improved education and expanded research.
INTRODUCTION
People have always considered the indoor environment a refuge from the dangers of the outdoors, offering protection from weather, wild animals, and, in the late nineteenth and twentieth centuries, air pollution—long viewed as primarily an outdoor phenomenon. In recent years, however, questions have been raised about potential health problems arising from indoor air pollution. The resultant concerns are related to modern lifestyles and the fact that most Americans spend more than 90 percent of their time inside a building of one kind or another. Indeed, if hours in transit between locations are considered, most Americans are indoors nearly 24 hours a day (Figure 1). In addition, there is a trend in newer construction toward energy-efficient, relatively airtight, structures. These factors taken together have raised increasing concern about the potential adverse health effects of indoor air quality.
Motivated by this concern, several agencies of the federal government asked the Institute of Medicine (IOM) to undertake an assessment of the public health significance of indoor allergens. The IOM responded by assembling a committee of experts in such fields as allergy and immunology, epidemiology, mycology, engineering, industrial health, pulmonology, education, and public policy. The study undertaken by the committee had three primary objectives: (1) to identify airborne biological and chemical agents found indoors that can be directly linked to allergic diseases; (2) to assess
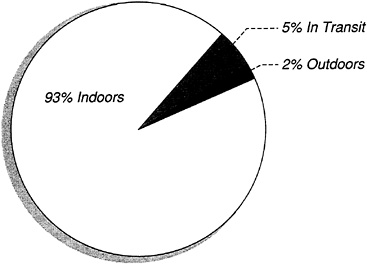
FIGURE 1
Amount of time spent indoors, outdoors, and in transit by most Americans.
Sources: NRC, 1981; Spengler and Sexton, 1983.
the health impacts of these allergens; and (3) to determine the adequacy of the knowledge base that is currently available on this topic.
This Executive Summary presents an overview of the committee's findings, followed by a section that presents all of the committee's recommendations and research agenda items from throughout the report.
The Allergic Reaction
An allergen is a biological or chemical substance that causes an allergic reaction. An allergy, in turn, is the immune-mediated state of hypersensitivity that results from exposure to an allergen. The symptoms commonly associated with allergy and allergic reactions are conjunctivitis (red, irritated eyes), rhinitis (a stuffy, runny nose, or ''hay fever"), and bronchitis (cough and congestion). Allergic reactions are classified and described in many ways, including: on the basis of the allergenic substance that causes them (such as cat dander, or pollen); according to the specific immunologic reactants (such as the types of antibodies or immune system cells involved in the reaction); or on the basis of the resulting disease (such as allergic asthma or hypersensitivity pneumonitis).
The most common allergic reaction is mediated by the immunoglobulin E (IgE) antibodies of the immune system. Mast cells, which contain histamine and other chemicals involved in the inflammatory response, also play a key role. After an initial exposure to a particular allergen, an individual who develops an allergy becomes "sensitized" to that allergen. In biological terms, sensitization occurs when IgE antibody specific for that allergen attaches to the surface of the individual's mast cells—making the individual "sensitive" (or "hypersensitive") to additional exposures. Subsequent exposure of the sensitized individual to the same allergen causes the mast cells to respond by releasing histamine and other inflammatory-response agents. These agents, in turn, interact with the surrounding tissues, causing an allergic reaction and the symptoms that we commonly associate with allergies (see Figure 2).
Everyone produces some IgE, but people with genetic predispositions to allergy (a condition called atopy) produce significantly greater quantities of it. In addition, the production of IgE antibody can continue for years after an encounter with an allergen. Thus, for example, someone who had an allergic reaction to penicillin as a child could still be allergic to the drug as an adult.
The reason why some people develop allergies and others do not is unclear. We do know, however, that genetic factors have a major influence on whether an individual develops allergy-related medical problems. For example, if one parent has allergies and the other does not, the chances are one in three that each of their children will have allergies. If both parents
have allergies, it is very likely (seven in ten) that their children will exhibit some allergic symptoms.
Another illustration of the process of developing allergic disease is presented in Figure 3. This figure shows the series of steps, beginning with the sensitization of a genetically predisposed or susceptible individual, and the potential interaction with other, nonallergenic agents (e.g., environmental tobacco smoke). Additional exposure to the sensitizing allergen then leads to a mild, moderate, or severe allergic reaction, depending on the amount of exposure. Exposure to nonallergens that irritate the respiratory tract (e.g., environmental tobacco smoke) can promote the development of allergic reactions and disease.
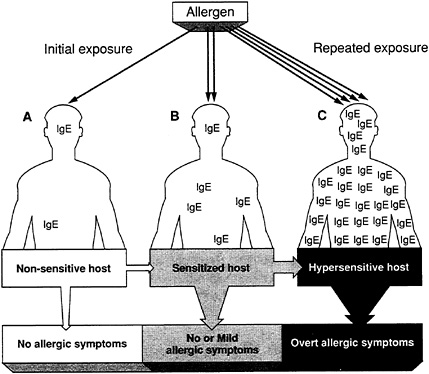
FIGURE 2 Hypersensitivity and IgE-mediated allergy. (A) Upon initial exposure to an allergen, there will be no overt manifestations of allergic disease because the patient is nonsensitized. However, this allergen will initiate an immune response that results in the synthesis of IgE and sensitization of the susceptible (atopic) host. (B) Upon subsequent, repeated exposures, this sensitized individual will synthesize increased amounts of IgE, thus becoming hypersensitive, although mild allergic symptoms may or may not be present. (C) From this point onward, reexposure to this specific allergen will provoke the overt manifestations of allergic disease.
Source: Fireman and Slavin, 1991.
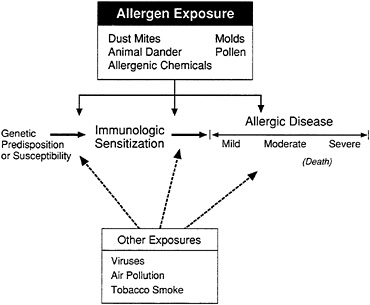
FIGURE 3 Development of allergic disease, illustrated schematically. A genetically susceptible individual is exposed to an allergen and becomes immunologically sensitized. At this stage the person is asymptomatic, but the sensitization may be detected by skin tests or laboratory tests. Over time, a proportion of sensitized individuals will develop one of a group of allergic diseases. Exposure to allergen is understood to be a major factor at each stage of the pathogenesis of these diseases.
MAGNITUDE OF THE PROBLEM
The most common allergic diseases caused by indoor allergens are allergic rhinitis, sinusitis, asthma, and allergic skin diseases (dermatitis). Figure 4 shows the generally accepted ranges of prevalence for these conditions in the United States. Based on these and other data, we can predict that one out of five Americans will experience allergy-related illness at some point during their lives and that indoor allergens will be responsible for a significant share of these cases. As such, indoor allergens are a major public health problem in the United States.
Some interesting facts about allergies and the indoor environment follow:
-
More than 50 million Americans—one out of five—suffer from allergic rhinitis (hay fever) and other allergic diseases, many of which are related to exposure to allergens in indoor environments
-
Allergic rhinitis is the single most common chronic disease experienced by humans.
-
The level of allergen exposure in the home relates to the risk of
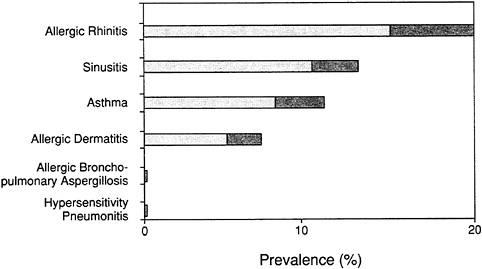
FIGURE 4 Estimated range of prevalence of diseases in total U.S. population that are commonly, although not invariably, related to allergy. Darker screen indicates the range in published data.
Source: NHLBI, 1991.
-
becoming sensitized to indoor allergens, the risk of developing an allergic disease, and the severity of the allergic disease.
-
Population-based and case-control studies suggest that indoor allergens are a major reason for trips to hospital emergency rooms.
-
Effective environmental control reduces disease severity.
Allergy also plays a key but sometimes unrecognized role in triggering asthma, a disease that deserves special public health attention because of its prevalence, documented cost, and potential severity. The following information provides perspective on the magnitude and cost of asthma:
-
An estimated 20 million to 30 million Americans—8 to 12 percent of the American population—have asthma.
-
Among chronic diseases, asthma is the leading cause of school absenteeism.
-
Asthma kills approximately 4,000 people per year (an increase of 33 percent in the past decade); in 1988, 4,580 people died from asthma in the United States.
-
Asthma mortality rates among African Americans are 2–3 times greater than among Caucasions; 5 times greater among children.
-
In 1985, an estimated 1.8 million people required emergency room services for asthma, 48% of these were children under 18 years of age.
-
In 1990, the estimated cost of asthma-related illness was $6.2 billion.
-
Some cases of asthma that require emergency care can be traced to poor control of home allergens.
-
With proper medical care and education, asthma can be controlled in the great majority of cases.
Figures 5, 6, and 7 show recent trends in asthma prevalence, mortality, and hospitalization rates, respectively.
Other allergic diseases related to indoor exposures, such as allergic bronchopulmonary aspergillosis and hypersensitivity pneumonitis, occur less frequently than allergic rhinitis and asthma, but are often severe and difficult to control. A role for indoor allergens has also been suggested in chronic sinusitis and bronchitis, sick building syndrome, and other nonspecific syndromes, as well as in acute respiratory illness.
The economic and social impacts of allergic disease in the United States are significant. The persistence of allergy-related symptoms and the occurrence of complications, such as otitis media and sinusitis, result in an overall increase in the number of physician visits and the use of medications.
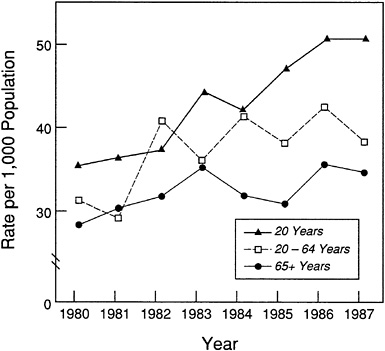
FIGURE 5 Trends in Asthma Prevalence. Source: NHLBI, 1991.
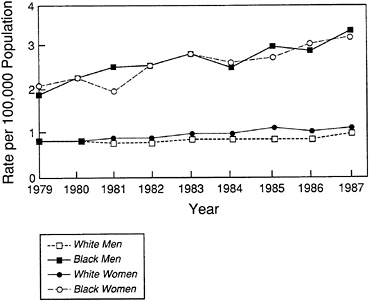
FIGURE 6 Trends in asthma mortality, U.S. age-adjusted death rates, 1979–1987.
Source: NHLBI, 1991.
Work and school absenteeism as a result of allergic reactions of the upper airway contributes to the economic burden posed by indoor allergens.
Although complete data are lacking, sufficient information exists to conclude that indoor allergens constitute a substantial public health problem. Given the amount of time most Americans spend indoors, expanded efforts to assess, prevent, and control the health threats posed by indoor allergens are warranted.
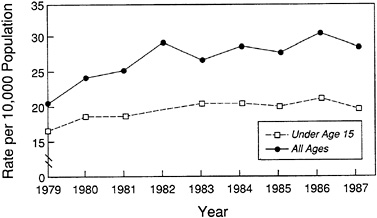
FIGURE 7 Trends in asthma hospitalization rates.
Source: NHLBI, 1991.
AGENTS, SOURCES, AND SOURCE CONTROLS
The major sources of indoor allergens in the United States are house dust mites, fungi and other microorganisms, domestic pets (cats and dogs), and cockroaches. The allergens produced by these organisms become airborne and can cause the allergic diseases mentioned previously, such as hay fever, asthma, and hypersensitivity pneumonitis.
The dust mite, a microscopic organism that lives primarily in carpeting and on mattresses and upholstery, produces several of the most common residential allergens. Although there are regional and local differences in dust mite concentrations, they are thought to be one of the most important allergenic causes of childhood asthma. Dust mite allergens, which have been purified and characterized, are contained in fecal balls that accumulate in bedding and on other surfaces.
Fungi release allergen-containing spores and other products indoors and outdoors. Although there are thousands of different fungi that can contaminate indoor air, purified allergens have been recovered from only a few; none has been completely characterized. Fungus spore allergens are known to cause hay fever, asthma, and hypersensitivity pneumonitis; other fungal products can be irritating or toxic, possibly exacerbating allergic conditions.
Allergens released by house pets have been purified and characterized and are an important cause of allergic rhinitis and asthma. Research has shown that cat allergens become airborne on very small particles and remain in buildings long after the cat has departed.
Cockroach allergen (which has also been purified and characterized) is derived from the insect's body parts and feces. In many inner-city areas, cockroach allergens probably play a significant role in the development of allergic rhinitis and asthma.
In addition to allergens derived from biological sources, some reactive allergenic chemicals can cause allergic disease. In general, these chemicals are more prevalent in the industrial workplace than the home. However, a limited number of household products may contain immunogenic agents (e.g., isocyanates in bathtub refinishing products).
The best way to prevent and/or control allergen-caused disease is to prevent exposure to the allergenic agent. Avoidance of specific allergens can lessen the probability of initial sensitization and, for individuals with known sensitivity, it can improve their condition dramatically by reducing the cascade of symptoms.
The bedroom is one area where steps to reduce exposure to allergens can have a beneficial effect on health. In the case of dust mite allergen, for example, covering mattresses and pillows with impermeable materials is an effective way to limit exposure (Box 1). Such avoidance measures are important tools for managing allergic disease and asthma caused by dust mite allergen.
|
BOX 1 Avoidance Measures for Mite Allergen
|
Drugs such as antihistamines, cromolyn, and topical steroids can be used to suppress allergic symptoms. Immunotherapy ("allergy shots") stimulates the production of protective antibodies and is especially effective for certain well-defined allergens.
MECHANISMS OF IMMUNE FUNCTION
The immunologic nature of allergic reactions was recognized early in this century, but many of the specific types of antibodies and cellular mechanisms involved in such reactions have only recently been defined. Research on the immune mechanisms of allergic disease has led to the hope that the immune responses that occur in allergic diseases can be interrupted at the molecular level. In addition, modern research techniques have allowed scientists to define the protein sequences of many allergens, providing a focus for studies into new methods for detecting and quantifying specific allergenic agents in the environment.
MEDICAL TESTING METHODS
There are several types of medical tests available for the detection and diagnosis of allergic disease. These include skin tests, in vitro antibody tests, and pulmonary function tests. In allergy practice, however, the medical
history is the primary diagnostic tool. Laboratory studies, including skin and in vitro tests for specific antibodies, have relevance only when correlated with the patient's medical history. Thus, although confirmation of a diagnosis of allergy generally requires an immunologic (laboratory) test to help identify a specific allergenic agent, an immunologic response is not sufficient to diagnose allergic disease; it means only that a prior sensitizing exposure has occurred. Treatment should always be directed toward current symptomatology, not merely toward the results of specific immunologic laboratory tests.
Medical History
Allergists use a variety of methods to obtain a history. These include open-ended, nondirected question-and-answer sessions, a series of questions ordered according to a formal protocol to ensure completeness, a structured questionnaire history completed by the physician, and a structured questionnaire history completed by the patient. Many allergists use a combination of these methods.
Despite universal agreement about the primary importance of a patient's allergy history, medical textbooks devote little or no space to this topic, and research on the subject seems to be nonexistent.
Skin Tests
The most common in vivo allergy test is the skin test. It is used both diagnostically for individual patients and by epidemiologists to develop estimates of disease incidence and prevalence in a population. Skin testing should be conducted with appropriate positive and negative controls. And for safety reasons, appropriately trained personnel and adequate equipment need to be available to treat any adverse systemic reactions resulting from the test.
One of the major problems with performing allergen skin tests is the lack of well-characterized, standardized reagents. Certain indoor allergenic extracts (e.g., dust mite and cat) now contain standardized amounts of major allergens, but others, such as fungi, are crude preparations of arbitrarily chosen fungi.
In Vitro Tests
There are several in vitro allergy tests used for diagnosis and in clinical research. The radioallergosorbent test (RAST) and the enzyme-linked immunosorbent assay (ELISA) can be used to evaluate levels of IgE or IgG directed against an allergen. Precipitin assays such as the double-immuno-diffusion
method of Ouchterlony, are often used to detect high levels of specific IgG, as can occur in patients with hypersensitivity pneumonitis. Specific cell-mediated immunity can be assessed by several methods, including the lymphocyte transformation assay and assays involving the production of mediators or cytokines. These tests are generally regarded strictly as research assays, however, and are not usually used to evaluate patients or populations.
As with skin tests, the accuracy of any immunodiagnostic test depends on the characteristics of the test reagents, and in particular on the allergen reagent. Standardization and characterization of allergen reagents used for immunodiagnostic tests are imperative. Similarly, the existence and characterization of control antibody, whether polyclonal or monoclonal, would be valuable for standardization and quality control of immunodiagnostic tests. Ideally, minimal standards for quality control should be devised for labs reporting results of tests to detect specific immunologic responses to indoor allergens.
Pulmonary Function Tests
Diseases such as asthma and hypersensitivity pneumonitis are characterized by decrements in lung function that vary over time. Pulmonary function tests, which measure these decrements and any improvements that may occur, have many applications in clinical medicine and research related to indoor allergens. These tests include spirometry (the most reliable pulmonary function test), peak-flow measurement, lung-volume measurement using gas dilution or body plethysmography, diffusing-capacity testing, exercise studies, and rhinomanometry. The choice of the appropriate pulmonary function test depends on the requirements of the specific application.
One drawback of many pulmonary function tests is that they must be administered by medical personnel or trained technicians. Peak-flow measuring devices are the exception. These devices are less reliable than some other technologies, but they are easily portable and can be self-administered—making them useful in the diagnosis and management of asthma.
ASSESSING EXPOSURE AND RISK
The process of assessing exposure to indoor allergens is complex. The relevant contaminants, contaminant sources, and environmental exposure media must be identified. The manner in which allergens are transported through each medium and how the contaminants are chemically and physically transformed must be determined. In addition, the allergen's routes of entry into the body, the intensity and frequency of contact between the
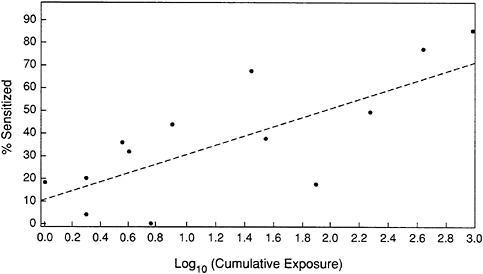
FIGURE 8 An exposure-response analysis of dust mite allergens.
allergen and the affected individuals, and the allergen's spatial and temporal concentration must be assessed.
A determination of the relationship between exposure and the development of allergic disease can be used to estimate the level of risk for developing allergic disease within a population. This relationship could be expressed as the number of new allergy cases expected at a given exposure level or the distribution of expected change in severity of symptoms with changing exposure levels. In an example using published data on dust mite allergy, this committee reports a positive relationship between cumulative exposure to dust mite allergen and the risk of allergic sensitization (see Figure 8). This is a finding that has long been suspected to exist, but has not been previously demonstrated. The residual sensitization predicted by these calculations would occur irrespective of exposure to dust mite allergen, and is consistent with the knowledge that other factors may also result in sensitization.
ENGINEERING CONTROL STRATEGIES
An in-depth understanding of how building systems and structures operate and perform is essential for assessing and controlling indoor air quality problems. The reduction and/or elimination of human exposure is probably best achieved by simultaneously controlling allergen sources and improving building ventilation, i.e., the design, operation, and maintenance of heating, ventilation, and air-conditioning (HVAC) systems.
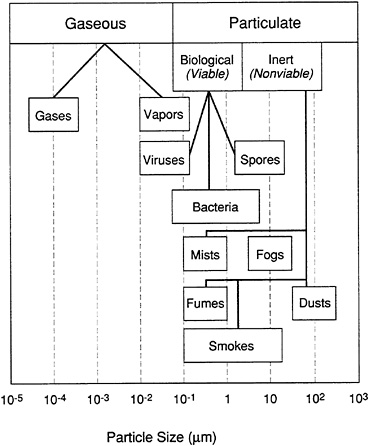
FIGURE 9 Dimensional continuum of potential contaminants.
Source: Adapted from Woods, 1982.
Most HVAC systems have dry, panel-type barrier filters, which are installed primarily to protect the system's mechanical air-handling equipment. Such filters remove few if any particles smaller than 1 to 2 μm (see Figure 9). Most pollens, many fungus spores, and dust mite fecal particles are larger than this. However, some allergens, such as cat dander and fragments of fungi, travel on particles less than 1 μm in size. Therefore, for optimal allergen control, it may be reasonable to upgrade these central filters and to use high-efficiency portable air cleaners in closed, confined, clean areas (e.g., the bedrooms of allergic patients).
The improved design, maintenance, and operation of residences and other buildings should reduce the incidence, prevalence, and severity of allergic disease. A recent report by the Environmental Protection Agency (Building Air Quality: A Guide for Building Owners and Facility Managers, 1991a) is an excellent source of practical information.
THE ROLE OF EDUCATION
Improved education is essential to the prevention and control of indoor allergic disease. This is true both for common allergic conditions of low-to-moderate severity and for less common diseases that are more severe and/or potentially fatal. Medical education at all levels (medical schools, postgraduate training programs, and continuing medical education programs for practicing physicians) should emphasize the importance of recognizing and properly managing these diseases. Nurses, physician assistants, and other nonphysician health care providers require similar education and training. In addition, patients and the general public should be made aware of when and where to seek medical help for allergy-related health problems.
One recent publication, the National Asthma Education Program's Guidelines for the Diagnosis and Management of Asthma (NHLBI, 1991), presents detailed recommendations for diagnosing and managing asthma. It also emphasizes the importance of education and of identifying causative agents, such as indoor allergens, that may initiate and exacerbate asthma symptoms. An evaluation of the impact of these guidelines awaits their wide dissemination and acceptance. Meanwhile, efforts to improve what is already known about preventing and controlling allergic diseases should continue. This knowledge should be disseminated to health care providers, allergy patients, and the public at large.
RECOMMENDATIONS AND RESEARCH AGENDA
This report describes what is known about the adverse effects on human health caused by indoor allergens, the magnitude of the problem nationally, the specific causative agents and their sources, the testing methods currently used for identifying allergens and diagnosing related diseases, and finally the need for increased knowledge and awareness of indoor allergens among primary care physicians, patients, and others. In describing these issues, the committee identified and developed a list of research agenda items and 15 priority recommendations. The recommendations focus primarily on the need to improve awareness and education, and as such are also relatively inexpensive and easy to implement compared to the research agenda items. The research agenda focuses on the longer term, more expensive, and more technical aspects of fundamental research and data collection.
Although cost-benefit analyses were beyond the scope of the committee's charge in conducting this study the committee's findings have been separated into recommendations and research agenda items, as described above, based on relative ease of implementation and estimations of associated costs. Policy development and further priority setting, however, should be based
on investigations of the probable costs and benefits of the various strategies for prevention and control. The cost analyses should include both direct and indirect costs (i.e., medical costs as well as lost work), and benefits should include a full assessment of the effects on improving the quality of life, as well as on reducing morbidity and mortality.
All of the committee's recommendations and research agenda items are presented below with brief introductions. The recommendations are presented first, followed by the research agenda.
Recommendations
AGENTS, SOURCES, SOURCE CONTROLS, AND DISEASES
Dust Mite, Cockroach, and Other Arthropoda
With most Americans spending the great majority of their time indoors—and much of that in their own homes—it is not surprising that the bulk of inhaled foreign protein is associated with indoor air. The evidence shows that a large proportion of asthmatics are allergic to indoor allergens and that several changes in the way we live indoors may have affected the levels of these allergens. These changes include increased mean temperatures, reduced ventilation (with consequent increased humidity), fitted carpets, and cool-wash detergents which have led to water temperatures for washing bedding that do not kill dust mites.
Once identified, reducing exposure to allergenic ''trigger factors" has been a standard part of the treatment of allergic disease for many years. Since approximately half of existing cases of asthma have been attributed to allergenic factors, it is reasonable to expect that asthmatics who require more than occasional treatment might also have allergies that induce their asthma.
Recommendation: Conduct appropriate allergy evaluations of asthmatics who require more than occasional treatment. Where allergic factors are present, ensure that these patients are given specific, practical information about how to reduce their exposure to arthropod and other allergens.
MEDICAL TESTING METHODS
Skin Tests
Despite some relatively minor shortcomings, the value of skin testing has been well established over the past century. When correlated with an appropriate clinical history, skin prick tests often are a useful way of screening for the presence of allergic disease. Using appropriate positive and negative
controls, intradermal testing can be used to demonstrate low levels of sensitization when allergy is clinically suspected. However, studies are necessary to determine the optimal concentrations and methods for skin testing and to address the relationship between defined skin test reactions and disease.
With respect to the specificity and sensitivity of skin tests within a population, more research is needed to determine the predictive values of both prick and intradermal tests. Moreover, the doses and criteria for positive skin tests used for such studies need further definition, together with criteria to define the relationship of a positive skin prick test to the wheal area or erythema that appears.
Recommendation: Encourage the development and use of improved standardized methods for performing and interpreting skin tests.
Pulmonary Function Tests
There are simple, reliable measures of lung function that may be used for studying diseases caused by indoor allergens. Indeed, objective measures of respiratory function should be a part of protocols to determine the efficacy of therapeutic strategies for these diseases. Predicted values for pulmonary function fall along a normal distribution curve with 95 percent confidence intervals for FEV1 and FVC of approximately 80–120 percent. The lower limit of variation in population studies for the midlevel expiratory flow rate (FEF25–75) is approximately 60 percent.
Spirometry is limited in its ability to detect impairment of ventilatory function in asymptomatic individuals because of the wide range of normal values, even with predicted levels that control for age, sex, and height. Significant inaccuracy can result from errors in spirometry performance, almost all of which lead to underestimation of the true respiratory function. These tests can, however, help to evaluate the effects on an individual of sensitization to specific allergens. They can also help to diagnose respiratory diseases that may be caused or worsened by indoor allergens and to assess disease severity, which is often critically important in clinical decisionmaking. Serial pulmonary function testing in the home or workplace can demonstrate causal relationships between the indoor environment and respiratory illness. Serial pulmonary function testing coupled with bronchoprovocation can demonstrate the causal relationship between specific allergens and respiratory responses.
In epidemiological studies, measures of environmental factors and of pulmonary function can be evaluated for associations that suggest causal relationships. Pulmonary function tests may also be used to assess the efficacy of therapy, determine response to treatment, or determine the effect of environmental modification. Such tests are required when physicians are
asked to determine impairment resulting from a respiratory disease for insurance or benefit systems such as workers' compensation and social security disability. Finally, estimates of disease incidence or prevalence often result from epidemiological studies in which pulmonary function tests are used to ascertain disease.
Recommendation: Include pulmonary function tests in epidemiological studies to help improve estimates of disease incidence and prevalence. Because they are portable and can be self-administered, tests that utilize peak-flow measurements are most desirable for this purpose.
One drawback of many pulmonary function tests is that they must be administered by technicians. Peak flow measurements are less reliable but are highly portable, can be self-administered, and are therefore often more sensitive in the diagnosis of asthma.
Recommendation: Include objective measures of respiratory function in experimental protocols designed to determine the efficacy of therapeutic strategies (e.g., pharmacotherapy, environmental modification, avoidance) used to treat respiratory diseases caused by indoor allergens.
ASSESSING EXPOSURE AND RISK
Methods for determining the effects of indoor allergens can be divided into two general categories: patient testing and environmental testing. Data from both kinds of testing can be useful to the physician in directing the treatment, control, and prevention of allergic disease. There are, however, no effective means currently available to physicians or other medical professionals for obtaining quantitative information on environmental exposures.
Recommendation: Establish effective mechanisms for medical professionals to acquire assessments of potential exposure to indoor allergens in residential environments.
ENGINEERING CONTROL STRATEGIES
The fundamental objectives of environmental control are to prevent or minimize occupant exposures that can be deleterious and to provide for the comfort and well-being of the occupants. Well-designed and maintained HVAC systems will exclude most aeroallergens (e.g., pollen, fungal spores) from interior spaces. Poorly designed or maintained systems, however, can provide for amplification and/or infiltration and dissemination of allergens.
Inappropriate control strategies have been associated with nearly all problem buildings.
Recommendation: Improve the design, installation, use, and maintenance of residential and commercial HVAC equipment, for both new and existing construction, in order to minimize allergen reservoirs and amplifiers. These improvements should be based on recommendations developed by the American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE).
Carpeting can provide niches for both the accumulation and production of allergens, and has been characterized by some as a "cultivation medium" for microorganisms when wetted. Carpeting can also serve as a reservoir for pollen and pollen fragments. The magnitude of the potential significance of carpeting as a source and reservoir of indoor allergens indicates that it should be given consideration as a serious problem.
Recommendation: Expand the scope of the Carpet Policy Dialogue Group of the Environmental Protection Agency to consider the serious problem of carpets as a source and reservoir of indoor allergens.
Standards have been established by the American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE) for acceptable temperature, humidity, and ventilation as they relate to human comfort. However, little attention is given in these standards to the protection of buildings, furnishings, and construction materials from water damage, and the potential for subsequent adverse health effects.
Recommendation: Develop consensus standard recommendations for controlling moisture in naturally and mechanically ventilated buildings. These recommendations, designed to help control microbial and arthropod aeroallergens and allergen reservoirs, should be developed by ASHRAE and be included in their Standard Series 55 (thermal environmental conditions for human occupancy) and Standard Series 62 (ventilation for acceptable indoor air quality).
THE ROLE OF EDUCATION
Education is an important component in the prevention and control of allergen-induced diseases. Considering that a large percentage of hospital admissions for asthma can be prevented by educating physicians and patients in the proper control measures, the need for emphasis on education becomes obvious. By disseminating information to patients, to health care providers, and to building design, construction and operations professionals, prevention of diseases associated with indoor allergens becomes not only realistic, but may offer a cost-effective means of reducing morbidity.
Patients
In developing and implementing educational interventions for patients, consideration should be given to identifying populations such as those with severe asthma who are more motivated and more likely to benefit from intervention.
Recommendation: Identify population groups most likely to benefit from educational and allergen-avoidance interventions. This effort should be based on an understanding of what allergens serve as risk factors for different individuals.
Socioeconomic, educational, and ethnic characteristics are important variables that should be considered in developing effective educational intervention programs. Programs that focus on these factors in tailoring self-management programs should greatly enhance both the acquisition and the performance of self-management competencies.
Recommendation: Develop focused educational programs for allergic populations with different socioeconomic and educational characteristics. Such programs should help patients:
-
understand allergic-disease risk factors;
-
predict the occurrence of such risk factors;
-
adopt behaviors required to avoid or control these factors; and
-
develop self-management skills to translate and use the knowledge they acquire to control allergic risk factors in different contexts.
A relapse prevention component should be included in these programs as well as follow-up studies to assess patient acquisition of allergy-related knowledge and the need for additional educational efforts.
Health Care Providers
Curricula vary in medical schools, often with little focus given to the topic of allergy diagnosis, prevention, and control—an unfortunate situation that should be corrected, especially considering the relationship of allergy to asthma. In addition, improved medical education is important because the majority of health care of the allergic patient is delivered by primary care providers, and the primary care provider is often the patient's main source of information about allergy control.
Recommendation: Incorporate the diagnosis and management of allergic diseases in the curricula and training materials for medical school students, residents in primary care practice, and subspecialists
who will subsequently care for patients with allergen-based allergic disease. Nurses, physician assistants, and other non-physician health care providers should receive similar education and training.
Allergic disease should receive additional emphasis at all levels of medical education, across specialties, and in clinical practice. One mechanism to help promote this concept would be to enlist the support and interest of scientific and medical societies.
Recommendation: Encourage scientific and medical societies with expertise in allergy, pulmonary medicine, public health, and occupational and environmental medicine to continue to assess and promote the development of prevention strategies for allergic disease.
Engineers, Architects, and Building Maintenance Personnel
Concerns about the design and operation of heating, ventilation, and air conditioning systems have focussed traditionally on the comfort of the building occupants and the efficiency of the operation of the equipment. It is important that those with responsibility for the design, construction, and maintenance of buildings also have an understanding of the potential adverse health effects associated with indoor environments, and the impact that design and operation of the systems can have on those effects.
Recommendation: Educate those with responsibilities for the design and maintenance of indoor environments about the magnitude and severity of diseases caused by indoor allergens.
Engineers, architects, contractors, and building maintenance personnel receive limited if any education about the health implications of the design, construction, and maintenance of buildings. Improved education in these areas is important to reducing the incidence, prevalence, and severity of adverse health effects associated with indoor environmental exposures.
Recommendation: Develop educational processes and accountability procedures for architects, engineers, contractors, and building maintenance personnel with respect to the health implications of the design, construction, and operation of buildings.
An interdisciplinary approach to the prevention and control on the adverse health effects associated with indoor exposures, including indoor allergens, is important. Such an approach should improve education in all areas of expertise and result in reduced health risks for building occupants.
Recommendation: Develop interdisciplinary educational programs for health care and building design, construction, and operations professionals.
Research Agenda
MAGNITUDE AND DIMENSIONS OF SENSITIZATION AND DISEASE
As outlined in this report, allergic disease constitutes a substantial public health problem in the United States. Data on its exact magnitude and dimensions, however, are incomplete, or lacking, in many cases. Better data regarding the incidence, prevalence, attributable fraction, and cost of allergic diseases are essential to the development and implementation of effective programs of prevention and control. Accurate determinations of the magnitude and dimensions of sensitization and disease caused by regional and local indoor allergens would be useful in this regard.
Research Agenda Item: Determine prevalence rates of sensitization, allergic diseases, and respiratory morbidity caused by regionally and locally relevant indoor allergens and assess the contributions of different allergens to these conditions.
Socioeconomic status seems to contribute to asthma prevalence rates and to indices of disease severity. Similarly, several studies have reported racial differences in the prevalence and severity of asthma in the United States, but such results are inconsistent. In order that these differentials can be translated into effectively targeted public health interventions, additional research is needed to clarify these relationships.
Research Agenda Item: Conduct studies to clarify the relationships that exist between socioeconomic status, race, and cultural environment and the incidence, prevalence, severity, and mortality associated with allergic disease including asthma.
The annual costs (direct and indirect) associated with asthma have been estimated at more than $6.2 billion—an increase of 39 percent since 1985. The size of these costs and the trend towards even greater costs argue for careful attention not only to the effects of allergy in causing asthma but also to the litany of other conditions that are more commonly thought to be associated with "allergies." Accurate assessments of the costs associated with asthma and other allergic diseases would be useful in the development of health policy initiatives and the implementation of appropriate and cost effective interventions.
Research Agenda Item: Determine the economic impact of asthma and other allergic diseases.
Allergic disease occurs when a genetically predisposed or susceptible individual is exposed to an allergen and becomes immunologically sensitized. In the early stages of sensitization, people who are sensitized have
not developed symptoms of disease. The magnitude of this group within the population is of interest, however, because it reflects the proportion of the population at greatest risk of developing allergic disease. Additional exposure to the sensitizing allergen leads to the development of an allergic reaction (disease) that can be mild, moderate, or severe, depending on the amount of exposure.
The relationship between exposure, sensitization, and disease, and the potential for a threshold level of exposure below which the risk of sensitization is reduced, is of critical importance in the prevention and control of allergic disease. Epidemiological data would be useful in determining these relationships and in developing and evaluating public health and medical intervention strategies.
Research Agenda Item: Conduct appropriate epidemiological studies of exposure-response relationships of important defined indoor allergens that induce sensitization in humans. Such studies should include a focus on identifying threshold exposures.
Indoor allergens are associated with a wide variety of particles in a broad size range, only some of which are microscopically identifiable, culturable, or detectable with existing immunoassays. Evaluation of indoor allergens requires both air and source sampling, and several different analytical techniques (including microscopy, culture, and immunoassays) must be used to characterize even the well-known allergens. Because of the complexity of the assessment problem, indoor allergens, with a few exceptions, have not been identified and studied.
Research Agenda Item: Encourage and conduct additional research to identify and characterize indoor allergens. The new information should be used to advise patients about avoiding specific allergenic agents.
AGENTS, SOURCES, SOURCE CONTROLS, AND DISEASES
Dust Mite, Cockroach, and Other Arthropoda
Although most studies investigate asthma (because it is common and can be measured objectively), sensitivity to indoor allergens is also very common among patients with other allergic conditions such as chronic rhinitis and atopic dermatitis. Because the important cause of inflammation that is common for all of these diseases is exposure to allergens, avoidance of the exposure should be the primary anti-inflammatory treatment. Developing realistic avoidance protocols for routine use is a challenge that must not take second place to pharmaceutical treatment.
Research Agenda Item: Conduct detailed studies of physical factors, such as sources and emission rates, that influence the levels of exposure to arthropod and other indoor allergens. These studies should include the effects of (a) protocols for reducing exposure and (b) devices advertised as reducing indoor allergen concentrations. More specifically, test the effectiveness of allergen avoidance protocols on the management of allergic asthma and other allergic diseases using protocols that have been demonstrated to reduce exposure by 90 percent or more. Such protocols should be tested under field conditions and should encompass the socioeconomic, cultural, ethnic, and geographic diversity of these problems in the United States.
The more important question now is the effectiveness of avoidance measures for reducing the development of disease (i.e., sensitization) related to arthropod allergen exposure. Specific measures include the use of polished wooden floors and no upholstered furniture in bedrooms and possibly in schoolrooms, keeping pillows and mattresses covered, and using bedding that can be washed regularly in hot water. Other measures, which require further evaluation, include air filtration, chemical treatment of carpets, and dehumidification.
Research Agenda Item: Develop allergen-free products to help reduce the incidence of allergic disease in the general public. The initial objective of this initiative, which should be carried out by the industrial/business sector, would be to provide an aesthetically appealing bedroom with reduced allergen exposure for children under the age of five.
There is considerable evidence that allergen avoidance is an effective means of reducing allergy symptoms. Practical measures to control exposure to mite and other allergens in the house can reduce both the symptoms and the underlying bronchial reactivity. For example, controlled studies of the effects of avoidance measures conducted in the homes of patients who were allergic to dust mites have shown significant improvement in both asthma and bronchial reactivity. The effects of avoidance measures on an individual's quality of life, however, remain to be determined.
Research Agenda Item: Conduct longitudinal studies to determine whether long-term allergen avoidance has a positive effect on quality of life.
Mammals and Birds
One of the difficulties in producing good epidemiological data on allergy is the lack of well-characterized, standardized allergenic extracts for
diagnostic purposes. Cat allergens have been well studied, although the role of serum albumin and its overall importance in allergic reactions to cats have yet to be determined. Allergenic extracts that are standardized for the content of Fel d I have appeared only recently. Well-characterized, standardized extracts of dog allergen preparations with known concentrations of Can f I are not available and should be developed. Similarly, there is a limited understanding of the identity and characteristics of many other mammalian and avian allergens. The lack of standardized extracts is partially responsible for the lack of development of immunochemical assays such as monoclonal antibody-based assays for many mammalian and avian allergens. Methods for measuring airborne allergen concentrations are critical for devising and evaluating control measures.
Research Agenda Item: Characterize important allergens from indoor animal sources (e.g., cats, dogs, birds, rodents) more precisely in order to develop standardized allergenic extracts for diagnostic purposes and immunoassays suitable for monitoring exposure.
Despite an increasing body of knowledge regarding the role of indoor allergen exposure, particularly to mammals, as a cause of asthma, much remains to be learned. The relationship between exposure to indoor pets and the increasing morbidity and mortality of asthma requires further clarification.
Research Agenda Item: Determine the relationship between exposure to indoor pets and the incidence, prevalence, and severity of asthma.
In addition, rodents that infest inner-city dwellings need to be examined as potential risk factors for asthma among individuals exposed to these potent allergens.
Research Agenda Item: Explore the possibility that exposure to rodent populations in inner-city areas may be a risk factor for asthma.
For many allergens, the size of airborne particles and their distribution in the air have not been elucidated and should be studied. Reservoirs of animal and avian allergen exposure and their dissemination through ventilation systems of offices, apartments, and other large buildings likewise require investigation.
Research Agenda Item: Investigate the potential role of mammalian- and avian-allergen- contaminated ventilation systems in the development of allergic disease among inhabitants of apartments, offices, and other large buildings.
Although control measures may reduce airborne concentrations of mammalian and avian allergens, the ability of these approaches to influence symptoms in sensitized patients or to prevent the sensitization of naive individuals requires clarification and study. The use of personal monitoring systems should be useful in making these determinations.
Research Agenda Item: Evaluate the effectiveness of environmental control measures on patient symptoms. This should include assessments of preventing sensitization in the naive individual as well as symptom reduction in those already sensitized.
The epidemiology, diagnostic techniques, and even pathogenesis of hypersensitivity pneumonitis from avian proteins are poorly characterized and require further elucidation. In addition, the risk factors and natural history of the disease are poorly understood and the effects of allergen avoidance remain controversial in the ultimate prognosis of the disease. All of these issues require clarification through further research.
Microbial Allergens
Overall, the fungus-associated allergies have been the least well-studied. Little data is available on the distribution of airborne fungal products, dynamics of human exposure, nature of the allergens, factors influencing the quality of skin test and immunotherapy materials, and the nature of fungus-related allergic disease.
Research Agenda Item: Initiate and conduct studies to determine the relative etiologic importance, geographic distribution, and concentrations of airborne fungus material associated with indoor allergy.
Fungi grow indoors in damp environments such as basements, window sills, shower stall surfaces, and in dust. Fungal spores and other effluents become airborne indoors when disturbed by air movement and normal human activities. The composition of aerosols of fungus-derived particles depends on the abundance and strength of sources as well as dissemination factors, mixing, dilution, and particle removal.
Research Agenda Item: Investigate the dynamics of fungal colonization of indoor reservoirs and emission of allergens from these sources. The results of such research should permit the risks associated with indoor fungal growth to be evaluated.
Exposure to fungal spores (and possibly other fungal antigen-carrying particles) can produce both IgE-mediated disease (e.g., asthma) and hypersensitivity pneumonitis while other allergens (e.g., dust mite, pollen) produce
only the IgE-mediated diseases. It is not clear why or under what conditions fungal particles can have this dual effect.
Research Agenda Item: Study the differences between fungal and other allergen-carrying particles that control the development of hypersensitivity pneumonitis as opposed to IgE-mediated asthma.
Chemicals
Many of the protein allergens have long been recognized, but a lengthening list of newly recognized allergenic chemicals is developing. Allergic diseases caused by these chemicals can differ from those caused by protein allergens in terms of symptoms, mechanisms of action, and appropriate treatment. The diseases can differ also in terms of etiology and exposure, i.e., often occurring at the work site. A better understanding of these differences will assist in the formulation of improved measures of prevention and treatment.
Research Agenda Item: Determine the types of allergic diseases caused by reactive allergenic chemicals, their prevalence rates, and the mechanisms responsible for the resulting airway reactions.
A body of knowledge about chemical allergens is available, but many areas have not been well studied. Other chemicals besides those already reported to cause allergic reactions may provoke responses. Thus, as new chemicals are introduced, the list of agents that elicit allergic reactions is likely to grow.
Research Agenda Item: Identify the risk factors, such as a specific immunologic response, that are predictive of the development of chemically induced sensitization or allergic disease, and as soon as possible after their introduction, determine the sensitizing potential of new chemical entities. This knowledge will facilitate the development of primary and secondary preventive strategies.
The allergic rhinitis, conjunctivitis, and asthma that arise from exposure to chemicals appear to be due to classic immunologic reactions. However, late respiratory systemic syndrome (LRSS) and immunologic hemorrhagic pneumonitis occur only in response to chemical exposures and are not the result of response to the usual protein allergens; the mechanisms of immunologic damage in these two cases are not entirely known. The mechanism of non-IgE-mediated isocyanate asthma is also unclear.
Research Agenda Item: Determine the disease mechanisms of chemically induced LRSS, of immunologic hemorrhagic pneumonitis, and of non-IgE-mediated isocyanate asthma. Appropriate in vitro or in vivo models should also be developed.
Low molecular weight reactive allergenic chemicals can cause immunologic sensitization and consequent allergic reactions. At a minimum, hundreds of thousands of U.S. workers are exposed to such chemicals that can form haptens with airway proteins and induce allergic diseases. The goal of reducing the incidence and severity of allergic disease caused by chemical exposure is achievable, although it may not be possible to prevent all such disease.
Research Agenda Item: Determine the number of workers exposed to allergenic chemicals in various industrial and non-industrial settings and the prevalence of allergic disease resulting from such exposure. Populations in close contact with reactive allergenic chemicals and highly potent sensitizers would be logical candidates for study.
For those individuals who develop allergic disease from exposure to chemicals, it is important to determine their long-term prognosis. In particular, if immune responses that are predictive of allergic disease can be identified, and reduced exposure can be shown to result in resolution of disease (and disappearance of immunologic sensitization), then reduced exposure may represent the most practical approach for preventing allergic disease arising from chemical exposure.
Research Agenda Item: Conduct dose-response studies in humans to determine both the relationship between allergen concentration and immunologic response, and a threshold environmental exposure concentration for sensitization.
PLANTS AND PLANT PRODUCTS
Indoor plants are commonly found in offices, schools, and the home. Although most indoor plants do not produce aerosols of allergen-containing particles, as more plants are used indoors, especially in large numbers in office settings, the risk of exposure to plant allergens increases.
Research Agenda Item: Assess the significance of workplace exposures to indoor plants, including the contribution to the overall magnitude of indoor allergic disease.
Latex allergy has recently received substantial attention because of an increasing number of reports of its occurrence and its potential, in certain individuals, to produce life-threatening anaphylactic reactions. In addition to health care workers and manufacturers, children with spina bifida are at increased risk for latex allergy.
Research Agenda Item: Conduct research to further characterize the immune response to natural rubber. This effort should include studies of the incidence and prevalence of natural-rubber-related allergic disease.
MECHANISMS OF IMMUNE FUNCTION
Evidence suggests that the adjuvant effects associated with macrophage activation are related to endotoxin. Additional research is necessary, however, to clarify this phenomenon.
Research Agenda Item: Determine whether bacterial products (such as endotoxin) or fungal products may act as adjuvants in the immune responses to indoor allergens.
The magnitude of allergen exposure appears to be related to the risk of sensitization. Allergen exposure is also related to the risk of developing asthma and the age at which asthma develops. However, genetic and other local host factors are also important in atopy and asthma. Understanding the relative importance of these individual factors and their interaction with each other is essential to understanding the mechanisms of immune function.
Research Agenda Item: Conduct research to identify risk factors other than exposure, and clarify their potential significance relative to indoor allergy. This effort should include an evaluation of the role of genetic and local host factors in allergen sensitization.
MEDICAL TESTING METHODS
Medical History and Diagnosis
In spite of universal agreement on the primary importance of a patient's allergy history, very little space in medical textbooks is devoted to the topic, and no standard exists for collecting appropriate information. A standardized, validated allergy-history questionnaire would be useful in both clinical and research settings.
Research Agenda Item: Develop, test, and validate a standardized allergy-history questionnaire for use in multi-center studies.
Skin Tests
A major unknown in skin testing is the identity of the more prevalent allergens involved in many indoor exposures. Studies to characterize these allergens are important for the development of reliable diagnostic reagents.
Additional research is needed to identify, characterize, and standardize indoor allergenic extracts used for diagnostic testing.
Research Agenda Item: Develop standardized, well-defined indoor-allergen reagents for skin tests that can be used in clinical diagnosis and research studies.
In Vitro Tests
The accuracy of any immunodiagnostic test is highly dependent on the characteristics of the test reagents, in particular, the allergen reagent. Standardization and characterization of allergen reagents used for immunodiagnostic tests are imperative. There are a variety of characterization methods and unitages that could be used. Similarly, the existence and characterization of control antibody, whether polyclonal or monoclonal, would be valuable for standardization and quality control of immunodiagnostic tests. Ideally, minimal standards for quality control should be devised for labs reporting results of tests to detect specific immunologic responses to indoor allergens.
Once the above are instituted, the specificity, sensitivity, and positive predictive value of immunodiagnostic tests could be determined for use in major epidemiological studies or to determine specific immunologic responses of individuals to indoor allergens. In addition, the degree of cross-reactivity of antibody developed in response to a given allergen could be determined by cross-inhibition with other allergens. It would be important to assess these factors prior to embarking on any large epidemiological studies. There are also several unclear aspects of the immunopathogenesis of allergic disease that need elucidation in order to define the role of various tests (e.g., tests of specific cell-mediated immunity in asthma). Further immunopathogenic studies of non-IgE-mediated asthma and cellular studies in all types of immunologic asthma will be required to clarify these issues.
Future studies in the development of in vitro diagnostic tests should include the following:
Research Agenda Item: Identify selected allergens of potential research usefulness, and prepare pure reference standards for the development of immunoassays, including those that can be used in large scale epidemiological studies.
Research Agenda Item: Develop and assess immunoassays for new allergens, including low molecular weight allergenic chemicals, that can be used for research and for the diagnosis of allergic disease.
Pulmonary Function
Bronchial hyperreactivity is a feature of asthma that correlates with clinical severity and does not require repeated measurement. It is unclear,
however, whether bronchial hyperreactivity can be correlated with exposure to indoor allergens.
Research Agenda Item: Determine whether changes in bronchial hyperreactivity can be correlated with exposure to indoor allergens. If such a correlation exists, determine how reducing the level of allergens affects bronchial hyperreactivity.
ASSESSING EXPOSURE AND RISK
Some of the issues to be considered when undertaking a risk assessment for aeroallergens have been discussed and an example has been given by using data from the literature on dust mite exposure and the development of sensitization. The data can be described by a linear model and indicates that there is a positive relationship between cumulative exposure to dust mite allergen and the risk of sensitization.
Some residual sensitization (i.e., approximately 10 percent in this example) will occur irrespective of exposure to dust mite allergen according to these estimates. This finding is consistent with the knowledge that other factors may also result in sensitization. For this reason, information on cross-reactivity of allergenic agents in study subjects is desirable, and important to the analysis of potential mechanisms of sensitization.
Research Agenda Item: Determine whether a practical method could be developed to measure concentrations of dust mite allergens that are capable of sensitizing humans.
Variability in the methods used in the multiple study protocols reported to date is high. More uniformity in the collection of exposure data would be useful in the risk assessment process. Although reservoir sampling has yielded meaningful results that assist in remediating exposure, further development of standardized air sampling collection and analytical methods is needed.
Research Agenda Item: Standardize methods of collecting and analyzing indoor allergen samples to facilitate comparative and collaborative studies.
Improved, standardized methods of collecting and analyzing indoor allergen samples would be particularly valuable in establishing the relationship between reservoir samples, personal exposure measures, levels of activity, and the potential for airborne exposure of sufficient magnitude to induce negative health outcomes.
Research Agenda Item: Quantitate the relationship of allergens in reservoirs (and on surfaces) to aerosols and develop monitoring methods
for quantitating airborne-allergen concentrations in personal breathing zones.
Assessment of exposure is a rapidly advancing, complex, and multistep process that entails numerous variables and estimations. Most monitoring, for example, is often based on sampling for indicators rather than the actual allergen. There is a need for developing improved methods for estimating environmental concentrations of aeroallergens and the resultant individual exposures.
Research Agenda Item: Develop appropriate exposure metrics for specific indoor allergens that are analogous to time-weighted averages and permissible-exposure limits for industrial chemicals.
ENGINEERING CONTROL STRATEGIES
Dry vacuum cleaning is traditionally used to remove dirt and debris from the fibrous pile of carpets. Little information is available, however, on the effectiveness of this cleaning method in removing the various types of particles, including specific allergens that may adhere to pile fibers, carpet backing, and other furnishings. In addition, the physical cleaning process itself may be sufficient to disperse fine allergenic particles.
Research Agenda Item: Develop standardized tests for rating the effectiveness of vacuum cleaners in removing allergen-containing particles of known size from carpets, upholstery, drapes, and other materials. The tests should take into account the possible dispersion of particles from carpet caused by the cleaning process itself.
The effectiveness of air cleaning devices and practices depends on variables such as the volume of air that passes through the filter, the particle size of the air contaminant to be removed, and the source emission rate. If the air flow rate through an air cleaning device is low, for example, and the emission rate of the allergen is high, then the beneficial effect of the air cleaner is likely to be nonsignificant.
Research Agenda Item: Develop standardized test procedures for rating the effectiveness of air cleaning devices and other methodologies for removal of known size classes of particles containing allergens. The tests should address the capability of the device or methodology in removing airborne particulates from entire rooms or zones of buildings.
Restricted airflow and dissemination of particulates into occupied spaces are valid reasons for cleaning air supply ducts. Protocols for cleaning air
conveyance systems are currently in development by the National Air Duct Cleaners Association. However, the effectiveness of duct cleaning in controlling allergic disease is yet to be determined.
Research Agenda Item: Evaluate the role of duct cleaning in controlling allergic diseases.
As described throughout this report, ambient relative humidity is often considered a major controlling factor for indoor allergens. Control of relative humidity, or water vapor pressure in occupied space and in the HVAC system is an important part of allergen control in both residential and commercial buildings.
Research Agenda Item: Develop a public-use guideline on moisture and allergen control in buildings. The guideline should describe the proper use of vapor retarders and other techniques for moisture control in both naturally and mechanically ventilated buildings.
There are approximately 4 million commercial and 84 million detached residential buildings in the United States. About 75–85 percent of the buildings that will exist in the year 2000 have already been built. Maintenance, operation, renovation, and housekeeping practices affect the useful life span of a building and the quality of the indoor air. Cost effective strategies for source and exposure control are needed to address the problems associated with normal degradation of the HVAC performance that occurs as a building ages.
Research Agenda Item: Determine the relative efficacy of currently recommended environmental control strategies and develop cost-effective strategies for controlling aeroallergens throughout the lifetimes of residences and other buildings.

































