4
Responding to Work-Related Health Needs of Informal Sector Workers
This chapter includes presentations describing institutional efforts to protect and promote the working capacity of informal sector workers and to provide protection from occupational health and safety hazards in the work environment.
PRIMARY-CARE BASED INTERVENTIONS FOR INFORMAL SECTOR WORKERS
Ivan Ivanov, World Health Organization
Ivan Ivanov from the World Health Organization (WHO) discussed efforts by the WHO and its partners to enhance the abilities of primary care organizations to address work-related health needs. Primary care is the most widely available option that informal sector workers have for accessing health services, and thus enhancing capacities within primary care is one way to effectively reach that population.
The health impacts and global burden of occupational risks are significant; occupational risks are among the 10 leading risks for disease and disability worldwide (Institute for Health Metrics and Evaluation, 2010). In 2007 the World Health Assembly (WHA) adopted a global plan of action on workers’ health which sets forth a 10-year agenda for the worldwide health sector to respond to the specific health needs of workers. As part of the resolution, the member states of the WHO committed themselves to work toward full coverage for workers, including those
in the informal economy, in small and medium-sized enterprises, and in agriculture and also migrant and contractual workers; this full coverage would include essential interventions and basic health services for primary prevention of occupational and work-related diseases and injuries. In a continuation of this commitment, the draft agenda of the post-2015 United Nations Sustainable Development Goals includes targets that are well aligned with the vision of the global plan of action for workers’ health. Even before these recent commitments to workers’ health, Ivanov said, occupational health was seen as a human right for everyone, not only for formal sector workers, as set forth in the Universal Declaration on Human Rights and the International Covenant on Economic, Social and Cultural Rights. Ivanov stated that globally the provision of employment injury benefits is greatly unequal and, overall, quite low.
Ivanov showed an adaptation of the WHO’s universal health care cube to the world of work (see Figure 4-1). In occupational health, cost sharing has important implications for employers, the public sector, and the workers. Ivanov suggested that, rather than society at large, it should be
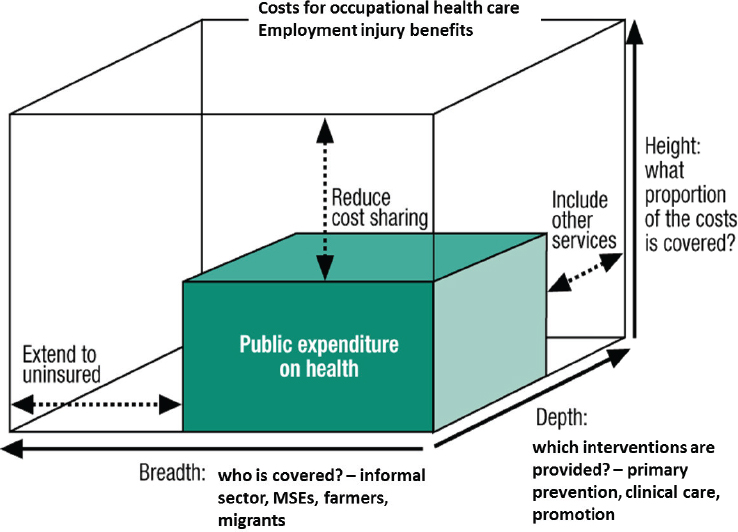
NOTE: MSE = micro and small scale enterprise.
SOURCES: Ivan Ivanov presentation to workshop, July 30, 2014; adapted from WHO, 2015b.
the entities that profit from economic activity that bear the consequences of exposure to occupational hazards. Furthermore, workers who become ill or injured as a result of their work should have social protection that is independent of whether they have a formal or informal employment contract.
Ivanov said that in the universal health care discussions at the WHO, the working poor and the informal sector are the target populations. These groups include about 1 billion workers who are below the global poverty line of US$2 per day. Globally, the informal sector constitutes up to 50 percent of the labor force, and in some countries the informal sector is nearly 90 percent of the labor force. The health of informal sector workers is directly linked to their earning potential. Informal sector workers sometimes are the only breadwinners in their families, and if an informal worker becomes sick or injured, his or her whole family can become trapped by persistent poverty. Protecting the health of informal sector workers and extending occupational health and safety services is part of the WHO’s poverty alleviation agenda.
The WHO currently is working with countries to scale up primary care–based interventions for the informal sector workforce. In 2011, the WHO held a meeting between occupational health providers, primary health care providers, and general practitioners to discuss the connections between health and labor at the primary care level within the health system. Ivanov said that the WHO meeting resulted in a recommendation for three groups of interventions that can be and should be provided at the primary care level: advice for workplace improvements, the control of work-related and occupational diseases and injuries, and health surveillance.
Following this meeting, the WHO reviewed the literature on the types of interventions for workers’ health that are being delivered at the primary care level. The literature review found that a group of environmental interventions and behavioral interventions for the primary prevention of occupational work-related diseases and injuries are delivered in countries where the primary care system has the responsibility for a defined area. Such interventions are not in primary care systems that are based on liberal medicine and free choice of provider (WHO, 2013). A second group of interventions delivered in many countries consists of interventions for the case management of occupational and work-related diseases, including taking work history, reporting occupational diseases, the followup of cases, and medical surveillance. The review found such interventions in both developing and developed countries (WHO, 2013). Several barriers to the delivery of interventions were identified by the review:
- Accessing workplaces in the informal sector
- No mandate to enter private enterprises
- Rapidly changing work practices
- No occupational health training program for primary care
- Shortage of health workforce
- Lack of knowledge of occupational health hazards among providers
- No time to visit workplace
- Lack of knowledge about occupational diseases and their causes
- Complex diagnostic and exposure criteria
- Difficulties with identifying occupational exposures and communicating with employers and occupational health services
- Fear of repression from employers
- No relationship with occupational physicians and no referral pathways
- Need extra time
- Long waiting time for specialists
- Inappropriate denial of workers’ compensation
- Refusal of workers to have their case notified
Following the literature review, the WHO conducted field studies and interviewed primary care providers in six countries. Ivanov said that the studies were conducted with the support of national collaborating centers for occupational health, and one country per region was picked based on feasibility and established networks. The selected countries were Colombia, Iran, Italy, Philippines, Thailand, and South Africa. The results of the field studies are summarized in Table 4-1.
Based on the results of the studies, Ivanov said, the WHO is encouraged that the delivery of certain interventions for improving the health of workers and keeping them on the job through primary care is possible, and the WHO is working toward scaling up effective models. The WHO is working to enable the primary care sector to address workers’ health by working with ministries of health to include work-related tasks and activities in the terms of reference of the primary care providers so that they can establish referral pathways to occupational health services. The WHO can set up programs for the training and retraining of primary care providers, ideally as part of continuous medical education. Additionally, the WHO is working to strengthen occupational health services, increase their numbers, improve their quality and effectiveness of delivery, and ensure that the occupational health services are connected to primary care. Furthermore, the WHO is working with ministries of health to provide financial protection for all workers, including workers in the informal sector, through social health insurance and noncontributory coverage for the poor, and by scaling up coverage of employment injury benefits.
Ivanov suggested that informal work should be considered as a social
TABLE 4-1 Results of the WHO Field Studies, 2012–2014
| Intervention | COL | ITA | IRA | PHL | THA | ZAF |
| 1. Primary prevention at the workplace level | ||||||
|
Yes | Yes | Yes | Yes | Yes | |
|
Yes | Yes | Yes | Yes | ||
| 2. Detection and case management of occupational and work-related ill health | ||||||
|
Yes | Yes | Yes | Yes | Yes | Yes |
|
Yes | Yes | Yes | Yes | Yes | Yes |
|
Yes | Yes | Yes | Yes | Yes | Yes |
|
Yes | Yes | Yes | Yes | ||
|
Yes | Yes | Yes | Yes | Yes | |
|
Yes | Yes | ||||
|
Yes | |||||
| 3. Fitness for work and health surveillance | ||||||
|
Yes | Yes | ||||
|
Yes | Yes | Yes | |||
|
Yes | |||||
|
Yes | Yes | ||||
NOTE: COL = Colombia; IRA = Iran; ITA = Italy; PHL = Philippines; THA = Thailand; ZAF = South Africa.
SOURCES: Ivan Ivanov presentation to workshop, July 30, 2014; data from the WHO Field Studies 2012–2014.
determinant of health. If informal work is classified as a social determinant, it would facilitate achieving a better understanding of risks and needs and their effects on income; removing the financial, structural, and cultural barriers to access to health services; and promoting social protections. Ivanov also suggested that informal work should be considered an environmental determinant and that the health sector should address it by mapping health risk (occupational, environmental, and behavioral) in typical informal settings; by identifying cost-effective interventions for health protection and promotion; by promoting policy options for delivery channels for informal sector workers; by developing resources for workers’ health; and by detecting and reporting occupational disease and injuries.
Ivanov said that the next steps for the WHO in the area of primary care–based interventions for informal sector workers will be developing
- definitions of essential interventions, target population, and channels and competencies for delivery;
- methodology for measuring workers’ health coverage;
- software for costing and planning scale-up scenarios (International OneHealth Costing Tool);
- standard modules for training of primary care providers;
- practical tools for delivery of interventions in low-resourced settings;
- support to countries to develop national road maps for scaling up workers’ health coverage; and
- special action on the health of the informal sector workforce—social determinants, occupational health, and health financing.
RESPONDING TO THE WORK-RELATED NEEDS OF INFORMAL SECTOR WORKERS IN LATIN AMERICA
Julietta Rodriguez-Guzman, Pan American Health Organization
Julietta Rodriguez-Guzman from the Pan American Health Organization (PAHO) described PAHO’s milestones in addressing workers’ health and the tools that PAHO uses to promote it in Latin America.
In 1984 PAHO hired the first regional advisor on workers’ health, and it has maintained the post continuously since then. In 1994 the Global Strategy for Occupational Health for All was issued and approved by the 3rd WHO Global Collaborating Centers Meeting held in Beijing, and was later endorsed by the WHA in 1996. Based on this strategy, PAHO developed a regional action plan for worker’s health that was approved by the Directive Council in 1999. The action plan originally had four strategic
lines of action, Rodriguez-Guzman said: policy and legislation, improving working environments, workers’ health promotion, and comprehensive workers’ health care services. Many activities and projects were carried out aiming to support member states. A strategy on workers’ health promotion in workplaces of Latin America and the Caribbean was launched in 2000. Campaigns to strengthen comprehensive health services delivery and capacity building in Members States through primary health care was also done. In 2006 the results of the first evaluation of the regional action plan led to prioritizing actions that could tackle needs of more Member States. Some initiatives are protecting the health of health care workers, preventing occupational disease (eliminating of silicosis, asbestos-related diseases, occupational cancer, etc.), and preventing emerging diseases (such as H1N1). In 2012 additional adjustments were made to include the protection of critical occupational sectors (including the informal sector), to strengthen the prevention of occupational disease and noncommunicable disease, and comprehensive OHS services in primary health care. To pursue in these actions strengthening of occupational health sciences was strongly needed. These adjustments also considered the dynamic changes of the theoretical framework of workers’ health during the past 20 years. The approach evolved from the heath and work relationship, to the new concept of work and labor as social and environmental determinants of health.
Rodriguez-Guzman listed PAHO’s current principles for global and regional action in workers’ health:
- The highest attainable standard of physical and mental health should be set.
- Workplaces should promote and protect health (and not be detrimental to health).
- Primary prevention should be made a priority.
- The workplace should be used as a setting for health interventions for adult working populations.
- The health system should use coordinated responses to address particular settings and economic sectors.
- There should be a focus on reducing inequities in workers’ health.
- Actions should be taken with the active participation of workers and employers.
- Coverage of basic occupational health services should be expanded to all workers.
Rodriguez-Guzman stressed that tackling the needs of workers in the informal sector will require advocacy, policies, education, training, surveillance, and research. In Latin America, she said, there are approxi-
mately 250 million people in precarious work and poverty (ILO, 2013). She said that child labor is also a significant problem in the region, often found and hidden in domestic or agricultural settings. Rodriguez-Guzman also pointed to several other hidden populations within the informal sector, including rural agricultural workers, immigrants and forced laborers.
In addressing the health and safety needs of informal sector workers in Latin America, Rodriguez-Guzman said, there are a number of challenges including defining, quantifying, and characterizing categories; the diversity of characteristics in and within countries, which makes it difficult to implement general interventions; and the payments or co-payments for social benefits are out of reach because of extreme poverty.
To implement the regional action plan on workers’ health, PAHO works with 21 WHO Collaborating Centers in the Americas. To address the needs of informal sector workers, several research alternatives have been assessed, aiming to identify who makes part of the sector, where they are located, and how they can be reached. PAHO has concluded that there is no “one-size-fits-all” solution for improving working conditions in the informal sector; but rather, that the solutions rise from bottom-up, with active participation of the communities involved in the problem. They are often vulnerable and poor populations, mainly composed by women, children, indigenous, immigrants and elderly people. PAHO is also committed to identifying interventions and best practices for reaching and helping these informal sector groups.
THE INTERNATIONAL LABOUR ORGANIZATION’S APPROACH AND GOOD PRACTICES FOR OCCUPATIONAL SAFETY AND HEALTH FOR INFORMAL WORKERS
Yuka Ujita, International Labour Organization
Yuka Ujita from the International Labour Organization (ILO) provided an overview of ILO’s tools for occupational safety and health. Ujita said that the occupational safety and health unit within ILO is merged with the labor administration. She also noted that ILO uses the term “occupational safety and health,” not occupational health and safety. For ILO, safety and prevention are seen as primary factors, and health is viewed as an outcome.
There are nearly 200 international labor standards, and Ujita said that 60 to 70 percent of the standards are related to safety and health. ILO has a two-dimensional approach to safety and health. The first dimension is advisory support at the national level using the International Labour Standards, and the second is technical support at the workplace level. Based on the experiences of ILO, Ujita said, several best practices have
been identified for successful occupational safety and health programs at the workplace level:
- Realistic goal setting in achieving “good practice”
- Self-help stepwise action aimed at low-cost solutions
- Link to increase of productivity
- Measures to ensure sustainability
When implementing occupational safety and health (OSH) programs at the workplace level, ILO applies a participatory, action-oriented training, or PAOT, methodology. As presented by Ujita, the flowchart of the PAOT methodology contains four steps: learn local good practices, check multiple areas jointly, implement simple improvements, and confirm benefits and follow up. The PAOT model typically follows a 2- to 3-day program. The program starts with a very short orientation, and then all participants visit a selected workplace nearby with the action checklist. When the participants return to the classroom, they are divided into small groups, and, through discussion, they identify three good characteristics of the visited workplace, three good examples of improvement on safety and health, and three points to be improved in terms of safety and health. Then the trainer presents principles of safety and health and good practices collected from the other regions. Following the trainer presentation, the small group discussions are repeated across different typical areas. In the last session, each participant developed action plans for his or her own workplace. One to six months later, the trainer visits the participants’ workplaces to see if they have implemented their action plans.
Ujita provided examples of ILO OSH programs that apply PAOT methodology. They are presented in Table 4-2.
TABLE 4-2 ILO OSH Programs Applying PAOT
| Program | Target |
| WISE: Work Improvement in Small Enterprises | Small enterprises |
| WIND: Work Improvement in Neighborhood Development | Small-scale farmers |
| WISH: Work Improvement in Safe Home | Home-based workers |
| WISCON: Work Improvement in Small Construction Sites | Small construction site workers |
| WARM: Work Adjustment for Recycling and Managing Waste | Waste recycling workers |
SOURCES: Yuka Ujita presentation to workshop, July 30, 2014; data from Khai et al., 2011.
Ujita said that the ILO does not provide any money to make OSH improvements through the PAOT programs. Instead, to promote sustainable changes, the improvements are made using available materials at the cost to the local organizations or workers. The idea is to shift the ownership for the improvement, and typically very low cost or free improvements are developed.
However, to ensure sustainability, Ujita said, support is needed from the national authority in terms of policies, and it is through coordination at the national and workplace levels that the best outcomes for OSH improvements will be achieved. For example, in Kazakhstan and Vietnam successful implementation of Work Improvement in Neighborhood Development (WIND) programs at the village and district levels led to the adoption at the government level of WIND as the national strategy for every worker in small-scale farming.
A PERSPECTIVE FROM THE UNITED STATES
John Howard, U.S. National Institute for Occupational Safety and Health
John Howard from the U.S. National Institute of Occupational Safety and Health (NIOSH) provided some brief remarks on the response to work-related health needs of informal sector workers in the United States. He noted that it is a topic that is not often discussed. However, it is a pertinent issue because low-wage jobs represent nearly one-half of all new jobs that are created in the United States, and evidence from research shows that workers in low-wage jobs are at an increased risk of work-related injuries and illnesses. There are some channels for accessing federally funded OHS services. Federally qualified health centers administered by the Health Resources and Services Administration sponsor community and migrant health centers that provide services to individuals who are frequently employed in the informal sector in the United States. The Patient Protection and Affordable Care Act, which was passed in 2010, provides a special fund over the first 5 years to support the expansion of these clinical centers and their services to increase the number of patients served by this population. Howard said that NIOSH is assisting these centers by helping provide preventive health services, but in the crush of providing rescue medicine, it is often very difficult to add preventive occupational health services despite a recognition of their value. NIOSH is working in several different areas to improve the diagnosis and management of and patient education concerning occupational health in the health centers.










