C.1
TRAINING FOR HEALTH EQUITY NETWORK: PAVING THE WAY
FOR RESULTS-ORIENTED HEALTH WORKFORCE EDUCATION
Björg Pálsdóttir, M.P.A.; and André-Jacques Neusy, M.D.
Training for Health Equity Network (THEnet)
Background
According to the seminal report of the Global Independent Commission on Education of Health Professionals for the 21st Century (Frenk et al., 2010), current models of health workforce education are not producing the people, research, and services needed to meet the changing needs of the 21st century. These challenges require a more fundamental shift in approach: it calls for the integration of health and education systems and for institutions that are equipped to address changing needs, to measure their impact, and collaborate to train health care teams with the necessary competencies and desire to address priority needs. The 2013 World Health Organization (WHO) guidelines for transforming and scaling up health professionals’ education calls for “promotion of social accountability (SA) and of close collaboration with communities” in its vision of the future (WHO, 2013, p. 12). SA is defined as schools having “the obligation to direct their education, research, and service activities toward addressing the priority health concerns of the community, the region, and/or the nation they have a mandate to serve” (Boelen and Heck, 1995, p. 3). SA serves as a useful mechanism to support institutional reform and evaluate schools’ impact on health services and health equity. It can also help determine the research agenda for evidence-based institutional reform.
The Training for Health Equity Network (THEnet) is a collaborative of trailblazing SA health professional education institutions from six continents. Working with and in underserved communities, THEnet schools define success through the lens of impact on health and equity and by how well schools meet the needs of the populations they serve. Data from THEnet’s schools—operating in highly diverse contexts in high- and low-income countries, urban and rural settings—show positive results in increasing the number and quality of health professionals and health outcomes in deprived areas (Cristobal and Worley, 2012; Kaufman et al., 2010; Larkins et al., 2015; Strasser, 2010; Tayag, 2011). Their common strategies include training embedded in primary, secondary, and tertiary levels of the health system; targeted recruitment; community-engagement; distributed learning; competencies defined by needs; and integration of population health with clinical and social sciences.
Built on the successful approaches of its members, THEnet developed
an institutional social accountability framework (Larkins et al., 2013; Ross et al., 2014). The framework identifies key factors that affect a school’s ability to positively influence health outcomes and health systems performance and proposes ways to measure them across institutions and contexts. THEnet is working with WHO to align the framework to WHO’s institutional assessment tools and with universal health coverage indicators. THEnet is conducting research and evaluations to build a solid evidence base for what works, how, and in which context. Research includes
- Graduate Outcomes Study: The ongoing study explores to what extent SA health professional education institutions are likely to train graduates that meet local workforce and health system needs, and identify factors that contribute to them doing so. It includes a longitudinal study (examining changes in students’ values and intentions throughout training and tracking graduates up to 10 years into practice).
- Philippines Impact Study: This ongoing study assesses how SA health professional education affects health care and health outcomes in rural and remote communities in the Philippines. The research includes case studies and a common impact study at the two participating schools (Ateneo de Zamboanga School of Medicine and University of the Philippines Manila School of Health Sciences).
- Return on Investment (RoI) Study: The first phase of this study aims to assess what social capital SA health professions education builds in the communities and population it works with. Later phases include focus on health and economic impact.
- Quality of Graduates: This study aims to assess the knowledge, skills, and attributes of first-year graduates of SA health professional education institutions compared to that of graduates from “traditional” programs. This will be done in both hospital and community settings, and will consist of a survey of supervisors and close collaborators of first-year graduates from socially accountable schools and comparison schools.
C.2
SPECIALTY TRAINING IN HEALTH PROFESSIONAL
EDUCATION: TIME FOR A PARADIGM SHIFT?
Jan De Maeseneer, M.D., Ph.D.1; and Paul Worley, MBBS, Ph.D.2
1Ghent University (Belgium); 2Flinders University (Australia)
Background
Worldwide there is a huge variation in the way postgraduate specialty training in health professional education is designed. When it comes to specialty training of physicians, for example, many countries have adopted the “UK-model,” where a specific (royal) college is in charge of the development of the training program and the assessment of the candidates. Often, organizations based on disciplines (family physicians, internists, surgeons, and others) are in charge of the recruitment, training, qualification, and license to practice for a certain specialty in a discipline. Mostly they are organized as strong bodies, with an important degree of independence, and apart from their training duties, they also act as representative bodies for that discipline, participating in societal and political health policy debates. In general, they are not accountable to the Minister of Education, but to the Minister of Health. In the United States, there is in essence a hybrid system where the universities do the training to college specifications within discipline-specific departments.
There are other models, such as in Europe, where the universities are responsible for the development of specialty training in the framework of a “Master-after-Master” program. We want to reflect on the question: “Is there a need for a paradigm shift for specialty training in health professional education in order to respond better to the changing health (care) needs?”
Analysis
Currently, societies are confronted with important new challenges: the demographic and epidemiologic transition, with a shift toward more chronic care and multimorbidity; the scientific and technological evolutions; the socioeconomic developments, especially the increasing social gradient in health in many countries; the cultural developments, in particular the fundamental change in the position of the patient as an active “consumer” of care; and globalization. How can the postgraduate educational systems be responsive?
The following reflections may be relevant: the availability of information through the Internet raises the chance that integrative models of medical practitioners and “new generalism” are now more possible; the debate
on the role of “physician assistants” and “technicians” has significant ramifications for the current income models of subspecialists who rely on procedural monopoly; there is a need to develop an evidence base around maintenance of expertise that is not developed by those who have the most to protect; status as a profession should be seen as a gift from society and requires “social accountability.”
Conclusion
The changing societal needs require appropriate training for specialties in the context of health professional education. We hypothesize that traditional colleges are probably not the best solution, due to the demonstrated conflicts of interest and lack of integrative capability of the college system, and that universities, especially if they are public universities, are better placed to serve society in postgraduate training. This hypothesis needs immediate investigation, exploring the ability of universities to experiment with different models and shifting the paradigm from “focus on subspecialization” toward “comprehensive integrative approaches.”
C.3
INTRODUCING EDUCATIONAL GAMING TO
ADVANCE INTERPROFESSIONAL EDUCATION
John R. Ressler, Ed.D.; Lucinda L. Maine, Ph.D., B.Pharm.; and
Ruth E. Nemire, Ed.D., Pharm.D., B.Pharm.
American Association of Colleges of Pharmacy and Professions Quest
Health professions educators worldwide have acknowledged that the graduates of our programs must enter practice equipped to participate in patient-centered teams to improve patient outcomes. The Interprofessional Education Collaborative (IPEC) released core competency statements for interprofessional learning in May 2011, and these have been widely embraced as a common framework for integrating interprofessional education (IPE) across the curricula of colleges and schools of the health professions. Despite this commitment, most educators acknowledge that logistical, cultural, and other barriers make it very difficult to achieve the goals of graduating “team-ready” clinicians.
Serious educational video gaming is increasingly recognized as a tool for learning and engaging students. The term serious games covers a broad range of applications from two-dimensional education games to totally immersive and code-driven three-dimensional environments where users interface with large volumes of data through sophisticated and interactive digital interfaces. This shift toward immersive world applications being
used to support education, health, and training activities and mobile applications mark the beginning of new challenges that offer real scope for collaborative and multidisciplinary research solutions, and real opportunities for innovative development.
The American Association of Colleges of Pharmacy has established Professions Quest to produce serious educational games for teaching and learning the IPEC core competencies. This interactive learning platform uses video game technology to bring multiple students from different health care professions together to solve real-world scenarios. The scenarios, called “Quests,” demand players work collaboratively to communicate, plan, exchange ideas, and develop options for solving the kind of challenges they will one day face in real life. Not only does MIMYCX provide students with a fun and engaging vehicle to help master the established IPEC core competencies, it also has the potential to improve knowledge exchange throughout the health care industry.
Additional information about the role of games in health professions education and how the quests released in the Professions Quest game called MIMYCX can enable and expand opportunities for collaborative learning in the health professions will be presented.
C.4
THE NEED FOR INTERPROFESSIONAL COLLABORATIVE-
READY NUTRITION AND DIETETICS PRACTITIONERS
Kathrin A. Eliot, Ph.D., R.D.; and Kathryn M. Kolasa, Ph.D., R.D.
Academy of Nutrition and Dietetics
Registered Dietitian Nutritionists (RDNs) are integral members of many health care and health prevention teams. As such, graduates of nutrition and dietetics education programs need opportunities to develop the soft skills required to become effective members of these teams. Currently there are no formal guidelines for incorporating IPE components into dietetics education programs in the United States, and the standards for core knowledge and competencies from the Accreditation Council for Education in Nutrition and Dietetics (ACEND) only generally refer to concepts that are related to IPE.
The benefit of IPE in health care education has been well studied across the professions though few studies mention specifically how dietetics has been involved. A review of literature, food, and nutrition conference abstracts and personal communication with dietetics education program directors revealed that dietetics education programs are minimally participating in IPE activities. The programs that are incorporating elements of IPE into their curricula cite benefits for both students and faculty. As a
result of IPE, students develop an increased understanding and awareness of professionalism, and improve their confidence in working as part of a team. Students also report that engaging in IPE is enjoyable, and they appear to recognize benefits to their futures as professionals.
Experiential learning is a critical component of IPE. While dietetic students and interns are often engaged in community-based education, most do not appear to have the opportunity to learn interprofessionally. As was suggested at the spring 2014 Institute of Medicine (IOM) Global Forum on Innovation in Health Professional Education meeting, participating in student-run clinics may be one way dietetic students could work collaboratively with other health professions. Some of the best examples have been seen in the interactions among dental and dietetic students and faculty. A review of abstracts on www.studentrunfreeclinics.org identified several dietetics education programs with various levels of participation in these clinics. Where these volunteer clinics operate successfully, students comment that they experience real interprofessional practice (IPP) and help them become “team ready.”
The Academy of Nutrition and Dietetics and ACEND are supporting efforts to involve the profession in the IPE movement. The academy currently sponsors membership in the Forum and recently renewed for an additional 3-year term. There is also an IPE task force within the dietetics education practice group that has been charged with devising a plan to distribute information about and promote opportunities for engaging in IPE. In February 2015, ACEND released a proposed new model for dietetics education that included a discussion of the need to train future dietitians interprofessionally. Ultimately, the IPE movement is rich with opportunities for nutrition and dietetics to become further involved in both the inpatient and outpatient settings. Dietetians have been members of multidisciplinary teams but now need to take advantage of opportunities for IPE and IPP. Educators and governing agencies need to respond to the challenges.
C.5
THE UNIVERSITY OF ARIZONA’S NATIONAL CENTER
FOR INTEGRATIVE PRIMARY HEALTHCARE (NCIPH):
CHANGING PRIMARY CARE HEALTH PROFESSIONALS’
EDUCATION TO INCORPORATE AN INTERPROFESSIONAL
INTEGRATIVE HEALTH APPROACH
Elizabeth A. Goldblatt, Ph.D., M.P.A./H.A.
NCIPH Leadership Team
The University of Arizona Center for Integrative Medicine, in collaboration with the Consortium of Academic Health Centers for Integrative
Medicine received a grant from the Health Resources and Services Administration to establish the National Center for Integrative Primary Healthcare (NCIPH). The NCIPH supports the incorporation of competency- and evidence-based integrative health care (IH) curricula into educational programs in a movement toward integrative interprofessional patient care. The NCIPH will develop competencies, curricula, and best practices taking into consideration the determinants of health including physical and social environment, individual health behaviors, and health services as they relate to the practice of IH to affect health outcomes. The center goals are
- Establish an interprofessional leadership team;
- Develop a coordinated set of competencies in IH across primary care professions;
- Develop a 45-hour interprofesssional IH curriculum for primary care;
- Create an accessible and interactive online infrastructure to house IH curriculum, best practices, and resources; and
- Develop patient education materials and facilitate access to IH practitioners working with the underserved.
First-year activities included developing IH meta-competencies and curriculum development planning. Experts representing primary care residency training programs, nursing, public health, dentists, pharmacy, behavioral health, and the complementary and integrative health professions of chiropractic, naturopathic, and traditional Chinese medicines convened to create a set of meta-competencies in integrative primary health care. A needs assessment was sent to primary care educational programs to assess interest and identify curriculum priorities, common content areas, core IH competencies, and implementation barriers to design a 45-hour IH online course. Curriculum content areas were identified based on the meta-competencies and needs assessment results. This presentation will include an overview of the project and a discussion of the 10 meta-competencies as well as the main subjects that will be included in the curriculum.
C.6
UNIVERSITY OF BRIDGEPORT INTEGRATED
CLINICS—INTERPROFESSIONAL EDUCATION
Jennifer Brett, N.D., L.Ac.
University of Bridgeport
The rise of interprofessional education/clinics (IPE/Cs) coincides with the era of the rise of the idea of health care teams in medical education and
delivery. U.S. patients increasingly self-choose services of a team of community complementary and alternative medicine (CAM) and conventional medical providers as their choice for care. Hospitals and health centers are adding CAM professionals to teams.
Dr. Brett describes the University of Bridgeport (UB) Integrated Clinics model of delivering interdisciplinary patient-centered care. The presenter will explore how a unique integration of interns of acupuncture, chiropractic, naturopathy, and dental hygiene at UB’s teaching clinic helps interns learn to work together for optimal patient care; and will discuss examples of strategies for interprofessional clinical collaboration in teaching clinics.
Critical teaching competencies that have been identified in the UB integrated team patient assessment clinic include
- Shared responsibility in patient care
- Communication skills for interns working together from different health care backgrounds
- Commitment to team-based care and team-building skills
- Understanding patient-centered care
- Time management
- Effective active listening and active communication skills
Critical patient care competencies identified in the UB integrated team patient assessment clinic include
- Incorporating assessment survey information (e.g., Short Form (36) Health Survey) with physical exam and subjective findings
- Identifying how to prioritize diagnoses and treatments in complex cases
- Identifying the type of care that is appropriate taking into account patient preferences
- Incorporating referral to specialists outside of and within the team
- Use of evidence-informed practices in an effective and timely manner
The presenter will identify issues that arose in setting up this model of care: level of training in patient assessment for each team member; understanding the strengths and weaknesses for each type of practice and practitioner; clinicians’ high level of commitment to own program/field; the relationship of integrated practice model to overall educational goals; faculty expectations and work load; and funding. Dr. Brett also shares the expected and unexpected benefits of this integrated model: student intern team building; improved intern and supervisor communication; patient assessment and organized care for complicated case presentations; and su-
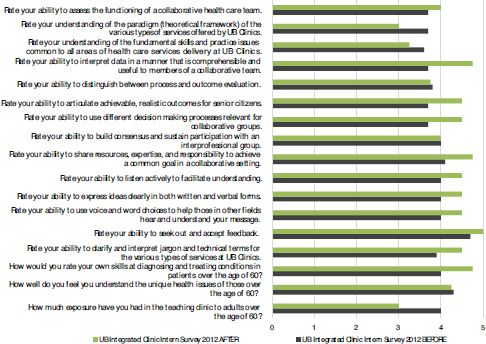
FIGURE C-1 University of Bridgeport (UB) integrated clinic intern survey 2012.
NOTES: Scale of 0–5 with 1 meaning poor/unsatisfactory and 5 meaning excellent. UB Integrated Clinic interns complete this survey before starting the shift and again and the conclusion of the semester.
SOURCE: Brett, 2015.
pervisor interprofessional respect and understanding. Figure C-1 shows the UB Integrated Clinic intern outcomes, as indicated by the interns.
REFERENCES
Boelen, C., and J. E. Heck. 1995. Defining and measuring the social accountability of medical schools. Geneva, Switzerland: WHO.
Brett, J. 2015. Strategies for interprofessional clinical collaboration in the U.S. based on ACCAHC competencies for optimal integration. Presented at the IOM workshop: Envisioning the Future of Health Professional Education. Washington, DC, April 24.
Cristobal, F., and P. Worley. 2012. Can medical education in poor rural areas be cost-effective and sustainable: The case of the Ateneo de Zamboanga University School of Medicine. Rural Remote Health 12:1835.
Frenk, J., L. Chen, Z. A. Bhutta, J. Cohen, N. Crisp, T. Evans, H. Fineberg, P. Garcia, Y. Ke, P. Kelley, B. Kistnasamy, A. Meleis, D. Naylor, A. Pablos-Mendez, S. Reddy, S. Scrimshaw, J. Sepulveda, D. Serwadda, and H. Zurayk. 2010. Health professionals for a new century: Transforming education to strengthen health systems in an interdependent world. Lancet 376(9756):1923-1958.
Kaufman, A., W. Powell, C. Alfero, M. Pacheco, H. Silverblatt, J. Anastasoff, F. Ronquillo, K. Lucero, E. Corriveau, B. Vanleit, D. Alverson, and A. Scott. 2010. Health extension in New Mexico: An academic health center and the social determinants of disease. Annals of Family Medicine 8(1):73-81.
Larkins, S. L., R. Preston, M. C. Matte, I. C. Lindemann, R. Samson, F. D. Tandinco, D. Buso, S. J. Ross, B. Palsdottir, and A. J. Neusy. 2013. Measuring social accountability in health professional education: Development and international pilot testing of an evaluation framework. Medical Teacher 35(1):32-45.
Larkins, S., K. Michielsen, J. Iputo, S. Elsanousi, M. Mammen, L. Graves, S. Willems, F. L. Cristobal, R. Samson, R. Ellaway, S. Ross, K. Johnston, A. Derese, and A. J. Neusy. 2015. Impact of selection strategies on representation of underserved populations and intention to practise: International findings. Medical Education 49(1):60-72.
Ross, S. J., R. Preston, I. C. Lindemann, M. C. Matte, R. Samson, F. D. Tandinco, S. L. Larkins, B. Palsdottir, and A. J. Neusy. 2014. The training for health equity network evaluation framework: A pilot study at five health professional schools. Education for Health 27(2):116-126.
Strasser, R. P. 2010. Community engagement: A key to successful rural clinical education. Rural Remote Health 10(3):1543.
Tayag, J. G. 2011. The service leaves of current medical students. In Bringing health to rural communities: Innovations of the U.P. Manila School of Health Sciences, edited by J. G. Tayag and L. L. Clavel. Manila: University of the Philippines Manila. Pp. 146-148.
WHO (World Health Organization). 2013. Transforming and scaling up health professionals’ education and training: World Health Organization guidelines 2013. Geneva, Switzerland: WHO.












