5
The Role of Public Health and Partnerships to Promote Eye and Vision Health in Communities
Health has been defined as “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity” (WHO, 1948). A population health approach involves multiple actors who work separately and cooperatively “on the interrelated conditions and factors that influence the health of populations over the life course, . . . systematic variations in their patterns of occurrence, and . . . the resulting knowledge to develop and implement policies and actions to improve the health and well-being of those populations” (Kindig and Stoddart, 2003, p. 380). Health is affected by multiple determinants, including
- innate individual traits (e.g., age, sex, race, genetics);
- individual behaviors;
- social, family, and community networks;
- living and working conditions (e.g., psychosocial factors, employment status and occupational factors, socioeconomic status, health care services); and
- broad social, economic, cultural, health, and environmental conditions and policies at the global, national, state, and local levels (e.g., economic inequality, urbanization, mobility, cultural values) (IOM, 2003).
Greater understanding of the determinants of health supports engaging the entire community in efforts to improve population health—hence the emergence of the concept of health in all policies (see, e.g., Wernham and Teutsch, 2015). Eye and vision health is no different. Although there are
specific system-related considerations that affect eye and vision outcomes, including the access to and quality of a complex health system (see Chapters 6 and 7), there are also societal-level factors that influence whether certain practices, policies, and conditions are available to reduce the risk of vision loss and decrease related health inequities. Good eye and vision health can reduce health disparities, but promoting optimal conditions for eye and vision health can also positively influence many other social ills, including poverty, other health inequities, increasing health care costs, and avoidable mortality and morbidity (Christ et al., 2014; Rahi et al., 2009; Rein, 2013).
The role of governmental public health is to ensure “the conditions in which people can be healthy” (IOM, 1988, p. 16). In contrast to medical care, which focuses on treating individual patients, the governmental public health departments (PHDs)1 concentrate on the risks to the population’s health and on improving health equity. As described in Chapter 1 when discussing the committee’s approach to its statement of task, the committee distilled the fundamental aspects of governmental public health work into three core public health functions: assessment, policy development, and assurance. These functions include 10 essential public health services: (1) monitoring health; (2) diagnosing and investigating; (3) informing, educating, and empowering; (4) mobilizing community partnerships; (5) developing policies; (6) enforcing laws; (7) linking to and providing care; (8) assuring a competent workforce; (9) evaluating; and (10) conducting research (CDC, 2014b). To this end, governmental PHDs provide a wide range of services to protect (preventing diseases, chronic conditions, and injuries), promote (educating and changing behavior), monitor (carrying out surveillance), and improve the population’s health.
The responsibility for improving population health, however, has never been the sole province of the governmental PHDs. Governmental PHDs work with and through other stakeholders, including other government agencies, the clinical care system, employers and businesses, media, nonprofit organizations, the education sector, and the community (IOM, 2003, 2011c) (see Figure 5-1). Within these categories are stakeholders such as religious organizations, sports organizations, clinical and public health associations, community living centers, nursing homes, assisted living facilities, and others. Successful health promotion in eye and vision health will require innovative partnerships engaged in a variety of activities that advance different objectives within population health. A key role for the governmental PHDs is to act as a convener of the different stakeholders who then develop and implement action plans that may complement national initiatives and that reflect a community’s needs and goals.
___________________
1 Governmental PHDs in this chapter encompasses federal, state, and local public health agencies.
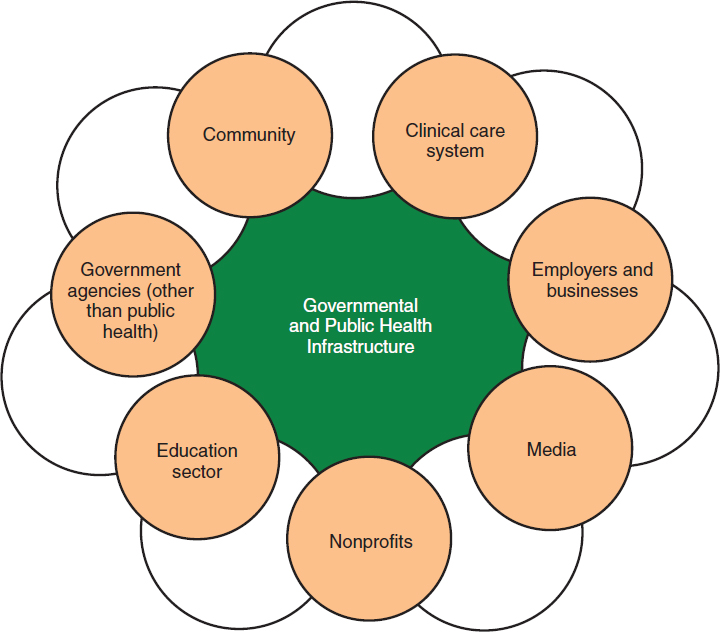
NOTES: This figure includes an additional circle for nonprofit organizations, which are also an important partner to advance population health objectives. The term “public health infrastructure” refers to the array of public entities charged with keeping the public healthy (e.g., agencies, laboratories, and partners) and to their operational capacity (IOM, 2003).
SOURCE: Adapted from IOM, 2011b.
The central issue we address in this chapter is the governmental PHD’s capacity to improve and promote eye and vision health and how partnerships between actors in the population health system can enhance this capacity. Programs to address the risk factors for vision loss, such as diabetes, tobacco use, and injury are common. But public health strategies to promote vision health are rarely supported as a categorical focus or even as part of chronic disease programs in state and local health departments (LHDs) because of resource limitations and competing priorities. Although eye and vision health is not a current public health priority, this chapter demonstrates the ways in which the governmental PHDs, working
in conjunction with the private sector, can transform eye and vision health into a public health imperative.
This chapter begins with a general overview of the governmental PHDs. In subsequent sections, we elaborate on the key governmental PHD functions as applied to eye and vision health. The second section introduces strategies for building capacities. The third section considers a variety of opportunities for governmental PHDs and other community stakeholders to incorporate eye and vision health into public health platforms. The final section concludes with a discussion of accountability, which includes priority setting and the evaluation of impact within governmental PHDs.
OVERVIEW OF THE GOVERNMENTAL PUBLIC HEALTH SYSTEM
Advancing eye and vision health as a population health priority will require more than simply asking governmental public health agencies and departments to place greater emphasis on the issue. Governmental public health professionals are responsible for a wide range of federal, state, and local activities and programs that are faced with dwindling resources and, simultaneously, increasing demand. Different levels of emphasis, resources, and staffing are required at each locus of government. In the absence of either increased funding overall or increased support for expanding programmatic focus, it will be difficult to rely on governmental PHDs to continue to provide current support or expand their footprints related to eye and vision health independently from other stakeholders.
This section provides an overview of the general responsibilities, structure, and current capacity constraints of federal, state, and local public health agencies to better understand the roles they could play to improve eye and vision health. In particular, it is important to understand the resource limitations of these systems as well as to recognize the heterogeneity among state and local PHDs because these factors underscore the need to embrace diverse partnerships and a wide range of strategies and programmatic emphases in order to adequately address the pressing public health needs related to eye and vision health and to vision impairment.
Federal Agencies and Organizations
Public health officials can use an array of legal and public health interventions to promote the population’s health, such as issuing and then enforcing regulations. At the federal level, there are numerous agencies, institutes, and centers whose work affects eye health and the impact of vision impairment on populations (see Appendix D). Current federal activities influence eye and vision health and the response to vision impairment
through various mechanisms, including (1) programs and funding that directly target the promotion of eye and vision health and are aimed at slowing the progression of vision impairment within defined populations; (2) tracking possible outcomes of poor eye and vision health, including activities to promote functionality following vision impairment; (3) promoting health more generally by addressing the underlying determinants of health that can also affect the risk of vision impairment; (4) establishing and enforcing policies related to the safety and functionality of occupational settings and built environments (i.e., the physical environment constructed by human activity), discrimination, and disability; (5) conducting research to advance scientific, medical, and public health knowledge; and (6) facilitating the delivery of services to promote access to the broader population.
The U.S. Department of Health and Human Services (HHS) supports a number of federal programs and institutes, such as the Centers for Disease Control and Prevention’s (CDC’s) Vision Health Initiative and the National Institutes of Health’s National Eye Institute (NEI) and National Eye Health Education Program (NEHEP), both of which focus on vision loss and the funding of various activities targeting at-risk populations (CDC, 2015a; NEI/NIH, 2015b). The Health Resources and Services Administraion (HRSA) funds grants and innovative projects to support its programmatic activities and delivers educational material on eye and vision health (HRSA, n.d.). Various federal and private grants are used to support HHS’s Healthy People 2020 objectives, which include eight goals that specifically address eye and vision conditions and emphasize early detection, timely treatment, and rehabilitation (ODPHP, 2016e).2 For eye health and safety, the Occupational Safety and Health Administration (OSHA) within the U.S. Department of Labor sets workplace safety standards. For example, employers must ensure that employees use appropriate eye or face protection when exposed to eye or face hazards. Other federal agencies involved with vision and eye health include the U.S. Department of Agriculture, the U.S. Department of Defense, the U.S. Department of Veterans Affairs, the U.S. Environmental Protection Agency, and the U.S. Food and Drug Administration, among others (see Appendix D).
Despite these activities, eye and vision health are insufficiently represented as a programmatic focus in federal government programs overall,
___________________
2 These goals include (1) increase the proportion of preschool children ages 5 years and under who receive vision screening, (2) reduce blindness and visual impairment in children and adolescents aged 17 years, (3) reduce occupational eye injuries, (4) increase the proportion of adults who have a comprehensive eye examination including dilation, within the past 2 years, (5) reduce visual impairment, (6) increase the use of personal protective eyewear in recreational activities and hazardous situations around the home, (7) increase vision rehabilitation, and (8) (developmental) increase the proportion of federally qualified health centers that provide comprehensive vision health services (ODPHP, 2016e).
and existing programs lack coordination within and across federal agencies and institutes. Support for more traditional public health activities has also been waning, which has affected the support available for grants that may target eye and vision health. For example, during fiscal year 2015, Iowa was the only state that used funds from a Preventive Health and Health Services federal block grant for any vision-related programming (CDC, 2015f). The funding for this grant program was eliminated in fiscal year 2016.
As described later in this chapter, chronic vision impairment is notably absent from government lists of priority chronic diseases, which means that eye and vision health are passively excluded from many federal programs and initiatives aimed at reducing the burden of chronic disease. Moreover, as described in Chapter 4, vision and eye health surveillance efforts have received only modest attention and support from federal agencies. Eye-related activities are not specifically listed as an area for funding or as an emphasis in the federal budget, unlike, for instance, oral health, and funding for the NEI has remained relatively stagnant over the past 5 years (NEI/NIH, 2016).
The Organization of State Health Departments
State health departments could provide substantial contributions to national eye and vision health efforts. First, their involvement in the planning process helps in the development of feasible action plans and ensures that the appropriate high-risk populations are targeted. Second, state health departments provide an important link between federal and community programs into incorporating eye and vision health strategies that are consistent with local needs and resources. State health departments offer grant opportunities that can be used to support specific eye and vision activities in LHDs or as part of a more comprehensive strategy in partnership with other groups. Third, as described more fully below, state health departments are expected to ensure that needed programs, regulations, and practices are monitored and improved.
The organizational model adopted for the state health department within each state offers insight into the roles they may play in relation to statewide and local public health services and priorities. There are four primary organizational models: a decentralized or home rule arrangement, under which local public health agencies operate independently of the state and report to local government; a centralized model in which there are no local public health agencies, though the state agency may have regional offices; a shared authority model; and a mixed authority model. In shared or mixed models, LHDs are generally responsible to both the state public health agency and to local government, but the details vary from state to state (NACCHO, 1998; Novick et al., 2005). As of 2012, 27 states had
decentralized governance, 14 states and the District of Columbia have centralized (or state) governance, and 10 had shared or mixed (state and local) governance (ASTHO, 2012).
In most states, public health is a component of a broader health department, which might be combined with other functions, such as Medicaid, mental health, substance abuse, environmental health, and human services programs (ASTHO, 2014). Moreover, public health responsibilities at the state level generally reside in multiple agencies. For instance, most states have a separate environmental agency. All states have public health codes that provide the agencies with the authority to conduct public health activities and permit them to promulgate regulations and take action. These codes are based on the police powers that the states have as sovereign governments under the U.S. Constitution, to safeguard their populations’ health, safety, and welfare (Lopez and Frieden, 2007). States may delegate this power to local governments, especially for public health activities. Surveillance and required disease reporting are exercises of state police powers.
Boards of Health provide additional oversight of governmental public health activities. The Institute of Medicine’s (IOM’s) report For the Public’s Health: Revitalizing Law and Policy to Meet New Challenges (2011b, p. 30) sums up the responsibilities that boards of health at different levels of governance have across the country:
Boards of health are [one] historical mechanism for public health governance at the state and local level, but their roles have evolved over time, and some have dismantled entirely (Nicola, 2005). Eighty percent of local public health agencies have an associated local board of health (NACCHO, 2009a), and 23 states have a state board of health (Hughes et al., 2011). Some local boards are advisory, and others play a role in governance and policymaking. Their functions may include adopting public health regulations, setting and imposing fees, approving the agency budget, hiring or firing the top agency administrator, and requesting a public health levy (Beitsch et al., 2010; Leahy and Fallon, 2005). State boards play varying roles as well, including agency oversight, appointing the health officer, a quasi-legislative function (i.e., adopting/rejecting rules) and a quasi-judicial function (i.e., enforcing rules) (Hughes et al., 2011).
The Organization of Local Health Departments
Except in states that use a centralized model, LHDs have broad authority to take actions necessary to protect and promote the public’s health. LHDs can use the full range of legal and policy initiatives as provided under the state’s and local public health code to achieve these objectives. For instance, LHDs can directly and indirectly use their regulatory authority
to require an industry to make certain changes to their products, and they have the authority to require individuals to operate within certain limits (e.g., using seatbelts). LHDs may also use their bully pulpit to motivate shifts in how private-sector entities operate with regard to its products, often working with industry to develop voluntary standards instead of governmental regulation (see, e.g., Mello et al., 2008). In the case of eye and vision health, for example, businesses could voluntarily adopt initiatives to improve worker safety (i.e., requiring and paying for safety glasses and monitoring their use).
For the most part, public health activities are conducted at the local level through approximately 2,800 regional or LHDs (Salinsky, 2010). Many LHDs are small agencies with limited resources and capabilities in certain areas, such as legal and policy analysis. Sixty-four percent of LHDs serve populations of 50,000 or less, often in rural areas (Salinsky, 2010). Some LHDs are regional (combining several smaller counties into one LHD), but most are countywide, stand-alone agencies (Salinsky, 2010). Because LHD workforces are not standardized across the United States, general statements about the nature of positions and tasks performed are difficult to make at a national level. Not surprisingly, smaller LHDs are likely to have fewer resources and less capacity to meet their obligations than larger departments (usually located in metropolitan areas) (Mays et al., 2006). Health departments are also dealing with an aging workforce and the imminent retirements of key staff (Hearne et al., 2015). From 2008 to 2010, the LHD workforce declined by 19 percent (NACCHO, 2011).
LHD capabilities and human resources are important in the context of eye and vision health because numerous LHDs are already struggling to provide their mandated services, which currently have higher priority than eye and vision health. Information regarding the distribution and trends of optometrists or ophthalmologists in LHDs is limited. A 2000 report from HRSA, which remains the most current and comprehensive report of the U.S. public health workforce, identified only five federal and four LHD public health optometrists (Gebbie, 2000). Nonetheless, many LHDs employ professionals such as physicians, behavioral health specialists, health educators, nurses, nutritionists, and epidemiologists (NACCHO, 2009b) whose educational background and training could make them valuable allies in promoting eye and vision health. Similarly, policy development and policy analysis capabilities are crucial elements lacking in many smaller health departments. This poses additional barriers to changing or adapting a programmatic emphasis within communities to include eye and vision health.
BUILDING CAPACITY AND STRATEGIES TO PROMOTE EYE AND VISION HEALTH
A fundamental challenge confronting state and local public health agencies is the availability of dedicated funding and staff resources to identify and respond to eye and vision health needs and to sustain a focus on efforts to improve vision health over time. Providing the full range of expected public health services requires significant capacity (i.e., financial resources, adequate staffing, and an adequately trained staff) that even large health departments struggle to meet. Unabated public demand for services and new legislative mandates exacerbate an already challenging environment. PHDs currently face “declining public investment, sustained attacks from opponents (including affected industries and anti-government political groups), limited political power, and competitors encroaching on its responsibilities” (Jacobson et al., 2015, p. S318). Moreover, flexibility in how state and local governments use federal grant funds varies (e.g., block grants provide broad parameters for spending decisions, whereas state and local governments generally do not have as much latitude for categorical focus grants) (CBO, 2013).
The result for this situation is that other more traditional public health activities, such as surveillance, health promotion, and policy development (including tracking underlying social and environmental conditions as well as eye and vision health) do not receive adequate attention or the necessary resources to address the growing need (Brooks et al., 2009; Honoré and Schlechte, 2007; Jacobson et al., 2015). Some studies suggest that a large, disproportionate percentage of public health funds is dedicated to linking and assuring access to health care services, to the detriment of agencies’ ability to adequately attend to other essential services (Brooks et al., 2009; Honoré and Schlechte, 2007). Programmatic emphasis may be narrowed and may reflect national public health priority lists, which do not typically include eye and vision health. For example, in its 2015 Prevention Status Reports, the CDC identified 10 top priority public health problems: motor vehicle injuries, obesity and nutrition, food safety, alcohol-related harms, health care–acquired infections, heart disease and stroke, HIV, prescription drug overdose, teen pregnancy, and tobacco use (CDC, 2015e). In the absence of federal directives and programs to advance eye and vision health, state and local PHDs are hard pressed to incorporate reduction of vision impairment as a categorical programmatic focus. Nor is eye and vision health well integrated into related programs, such as chronic disease and health education programs, although the risk of vision impairment is associated with a number of current public health issues, such as smoking rates. This opportunity is discussed later in this chapter.
An assessment of state-level activities for preventing eye disease and blindness found that the efforts of vision health stakeholders were generally uncoordinated and recommended the mobilization of partnerships to improve collaboration among public- and private-sector organizations (NACDD, 2004).
Public–Private Partnerships to Build Capacity
One response to the capacity constraints is for governmental PHDs to develop robust public–private partnerships, understood as arrangements in which public agencies formally or informally partner with private or nonprofit entities to provide or improve public services (The National Council for Public-Private Partnerships, 2016; Nishtar, 2004). Such partnerships can improve population health by advancing public health strategies and policies, improving public health education and advocacy, fostering trust and collaboration among sectors and stakeholders, and improving access to health care (Nishtar, 2004). For example, community and religious organizations involved with health promotion campaigns can increase knowledge about and awareness of disease, encourage screening, and help reduce risky behaviors (DeHaven et al., 2004). These partnerships have the potential to fill gaps in expertise and provide services that would not otherwise be supported through government hiring. They also may allow health departments to focus on meeting other core and essential services.
Eye and vision health can become an important component of public–private collaborations with effective leadership and sustained commitment and funding to track meaningful measures of eye and vision health as a population health outcome and risk factor for other social determinants of health. For example, health departments can serve as navigators between medical care and the community (e.g., arranging transportation, working with providers to use community health workers in coordinating eye health in the community). For example, the National Association of Chronic Disease Directors, with input from the CDC and Prevent Blindness America, recommended that states designate an integration specialist to take responsibility for coordinating vision services within the state department of health and among external actors and that they form a community-based coalition of actors led by a public health coordinator to provide basic vision services (PBA/NACDD, 2005). Similarly, a well-functioning medical care system can expand access to appropriate eye and vision care services, allowing public health agencies to focus on preventive policies and action and assurance. A well-functioning medical care system could hire navigators within their own organization or through contractual relationships with governmental public health systems or nonprofit organizations to assure coordinated eye and vision care and population-wide improvements in, and reduction
in inequalities associated with, eye and vision health. This includes linking people to needed care, assessing care quality, and promoting community support, policies, and environmental conditions that maximize health (IOM, 2003). Likewise, health care providers can collaborate with health departments to identify and refer individuals previously undiagnosed and to work with diagnosed individuals to secure needed services. The best collaborations should build on the unique strengths of partners to create a systemic effect that is greater than any single partner can produce.
At the same time, partnerships have limitations and may incur risks. The obligations of government to provide public services may conflict with the profit motives of for-profit private businesses or the political, economic, and social agendas of nonprofit organizations. Particular risks include the degradation of social safety nets, inappropriate reorientation of governmental health policy, fragmentation of health care systems, undesirable power imbalances among partner organizations, and unsustainable program operations (Nishtar, 2004). Most importantly, the failure to carefully select private-sector partners or to adequately delineate the partnership terms can erode traditional public-sector values such as accountability, transparency, responsibility, and quality (Reynaers, 2014).
Regionalization and Cross-Jurisdictional Sharing
Public health capacity can be expanded by consolidating smaller LHDs into a larger agency (also called regionalization) or at least by the cross-jurisdictional sharing of staff and services, two strategies that have been used most prominently in the context of emergency preparedness (Koh et al., 2008). Among others, Koh et al. (2008) and Stoto and Morse (2008) have argued that the benefits of regionalization and cross-jurisdictional sharing include improving LHD capacity, making more efficient use of funds, achieving economies of scale, and optimizing coordination—for example, in managing problems that are not bounded by municipal borders.
Consolidation offers several potential opportunities to elevate eye and vision health on the public health agenda. First, anything that expands staff capacity will enable an LHD to develop new initiatives or broaden current activities. As discussed below in the section Public Health Interventions to Promote Eye and Vision Health, the committee identified numerous opportunities for LHDs to improve eye and vision health if they have adequate staff and resources. Second, consolidation increases the number of people in the service area who might have vision impairment, making it more likely to detect changes in eye and vision health in response to specific interventions and initiatives. Third, consolidation improves the likelihood that LHDs will be active participants in the community health needs assessment process (discussed later in
this chapter), which could then support public–private collaborations to improve eye and vision health. Finally, for smaller LHDs, “combining resources and operations, sharing different types of capacities (e.g., legal guidance and policy analysis), and specialized positions (e.g., epidemiologists) could help smaller agencies meet [accreditation] standards (Konkle, 2009; Libbey and Miyahara, 2011; Mays et al., 2006)” (IOM, 2011b, p. 43). This can generate new opportunities to discuss the insertion of eye and vision health metrics into public health debates related to health care quality and access. However, this approach could also lead to a loss of local identity and responsiveness, particularly those related to local needs and priorities.
OPPORTUNITIES TO INCORPORATE EYE AND VISION HEALTH: THE PUBLIC HEALTH AGENDA
A public health agenda represents informed decisions and prioritizations about specific health threats based on the nature of those threats and the ability to influence the occurrence or impact on the overall health and well-being of populations. The agenda should represent thoughtful consideration within a community about what health threats command attention, the availability and application of resources across health and non-health sector domains to successfully address these priorities, agreed upon metrics to measure impact and correct course where applicable, and the appropriate community oversight to hold stakeholders accountable for short- and long-term successes and failures.
Establishing public health priorities requires an informed public. Simply put, “public health depends on laypeople’s ability to understand the health-related choices that they and their societies face” (Fischhoff et al., 2009, p. 940). To make such decisions wisely, individuals need to understand the risks and the benefits associated with alternative courses of action (Fischhoff et al., 1993). Health promotion and education are important components of any governmental PHDs population health approach to reducing the eye and vision health burden on society. Health promotion is “the process of enabling people to increase control over, and to improve, their health. It moves beyond a focus on individual behavior towards a wide range of social and environmental interventions” (WHO, n.d.b.). Therefore, health promotion activities include not only the communication of information to encourage changes in individual behaviors, but also larger policies and practices intended to promote social, economic, and structural environments that are more conducive to health. The related concept of health education includes strategies to promote optimal eye health, prevent vision impairment, and provide people with the skills and ability they need to manage vision impairment and rehabilitation, if necessary. This includes
interventions to promote public awareness, change behaviors, and build community environments that promote eye health. Another goal of health education is also to give people the skills they need (e.g., health literacy) and the wherewithal to use them (e.g., an equitable health system). Strategies to promote and protect vision and eye health that are available to governmental PHDs include
- Altering the informational environment (e.g., promoting eye and vision health);
- Altering the built/physical environment (e.g., removing barriers to mobility);
- Directly regulating and monitoring (e.g., requiring eye protections and reporting for sports-related activities and safer work environments);
- Self-regulating (e.g., promoting voluntary employer initiatives to provide accommodations for vision-impaired employees);
- Developing robust state-level surveillance strategies (e.g., incorporating eye health into community health needs assessments and health impact assessments) to collect and analyze data regarding eye health status;
- Monitoring access to vision care services;
- Assuring access to clinical services, especially for undiagnosed and low-income populations at risk of eye disease;
- Incorporating vision care as a strategic planning priority and in conducting health impact assessments;
- Incorporating vision care as an integral component of “health in all policies” programs; and
- Facilitating community engagement in order to promote eye health and obtain community collaboration in implementing policies and programs.
The remainder of this chapter explores some of these strategies in more detail, including efforts to improve public awareness and education, expand access to vision care services and appropriate follow-up care, develop policies to encourage eye healthy environments, promote eye and vision health as part of formal population health programs, and enhance accountability for activities (or lack thereof) related to eye and vision health.
Improving Public Awareness and Education
Understanding that a problem exists and what can be done to ameliorate that problem is the first step to combating any public health threat. Although rarely adequate by themselves, public awareness campaigns can
be an effective way to improve knowledge about key messages related to health within populations (Bray et al., 2015; Oto et al., 2011) and are one essential part of an effective population health strategy. In fact, the CDC has stated that public health strategies, which include efforts “to enhance awareness, to promote education, and to increase access to successful prevention, treatment, and rehabilitation services among populations at risk for poor vision outcomes[,] can improve vision health in the United States and globally” (Zambelli-Weiner et al., 2012, p. S23).
Knowledge About the Major Causes of Vision Loss
It is important to understand what the different causes of vision loss are because the types and scopes of applicable interventions vary based on the etiology of vision impairment. According to a recent online poll to examine the importance of eye and vision health among the U.S. population, 88 percent of the 2,044 respondents surveyed identified good vision as vital to maintaining overall health, and 47 percent rated losing their vision compared to loss of limb, memory, hearing, or speech as “potentially having the greatest effect on their day-to-day life” (Scott et al., 2016, p. E3). This same poll found that blindness ranked either first or second among African Americans, Asians, Hispanics, and whites as the worse disease or ailment.3 Yet a lack of awareness around vision and eye health issues is “a major public health concern,” especially for linking patients into care and attempting to make population-level changes in behavior and health practice (Bailey et al., 2006; Zhang et al., 2012).
Unfortunately, the peer-reviewed literature contains remarkably little comprehensive data from the past decade about eye and vision health knowledge and the impact of public awareness and health promotion in the United States nationally. In 2005 the NEI and the Lions Club International Foundation (LCIF) conducted a telephone survey of more than 3,000 English- and Spanish-speaking adults in the United States about public knowledge, attitudes, and practices related to eye health and disease. The study found that public awareness of glaucoma, age-related macular degeneration (AMD), diabetic eye disease, and low vision varied substantially by disease4 (see Figure 5-2). While the majority of people who were aware of glaucoma (90 percent) or diabetic eye disease (51 percent) knew that
___________________
3 Asians, Hispanics, and whites ranked blindness behind cancer and Alzheimer’s disease, respectively (Scott et al., 2016).
4 Low vision was defined as a visual impairment not correctable by standard eyeglasses, contact lenses, medication, or refractive surgery that interferes with the ability to perform everyday activities (NEI/LCIF, 2008).
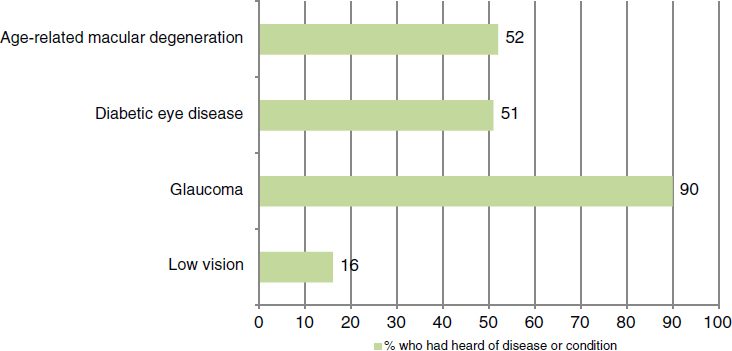
SOURCE: NEI/LCIF, 2008.
these conditions could be treated, the vast majority of these individuals did not know that glaucoma (92 percent) or diabetic retinopathy (89 percent) could present clinically with no early warning signs (NEI/LCIF, 2008). The most current, national data on vision loss awareness indicate that public knowledge about specific eye diseases and available treatment varies substantially.
Some improvements in knowledge over time have been observed. From 1991 to 2005, for instance, the percentage of adults who had heard of diabetic eye disease increased from 39 percent to 51 percent. The percentage of adults who had heard of glaucoma remained high (91 compared to 90 percent) during the same 14-year period (NEI/LCIF, 2008). The survey has not been updated since 2005, so there are no more recent statistics on public awareness of the major causes of eye disease. However, in its Five-Year Agenda for 2012–2017, NEHEP stated that “trends in the public’s knowledge, attitude, and practices will be examined through updates of the Knowledge, Attitude, and Practices (KAP) Survey” (NEHEP, 2011, p. 22). The committee supports this endeavor and encourages federal support for updating data on the public’s perception of and familiarity with eye health behaviors, risk factors, the relationship between eye and vision health and other measures of health, and available interventions, including the use of protective lenses, the utilization of health care, and the detection of uncorrected and correctable refractive error.
Awareness of Relevant Risk Factors for Vision Loss and Impairment
Knowing that a health threat exists is not the same as knowing what to do to avert that threat. Various factors are associated with an individual’s level of knowledge about eye and vision health. The NEI-LCIF KAP survey analyzed data by age, household income, and educational attainment. Although the findings varied by condition, individuals with higher income levels and educational attainment were generally found to have a greater awareness of eye health (NEI/LCIF, 2008; see also Jaggernath et al., 2014). An awareness of eye health and disease has also been shown to be positively correlated with age (NEI/LCIF, 2008). Hispanic Americans are less likely to have knowledge of eye health and disease than Caucasians, African Americans, and Asian Americans (NEI/LCIF, 2008; Zhang et al., 2012). Studies outside of the United States found similar results. For example, a study in Canada about cataract, glaucoma, and macular degeneration found that both non-European ancestry and low educational attainment were associated with a poor knowledge of eye diseases, suggesting “that innovative education programs in primary and secondary schools and in non-English languages are needed to improve knowledge, attitudes, and practices” (Noertjojo et al., 2006, p. 617).
Not surprisingly, the evidence about public awareness is more robust when one examines risk factors that overlap with major public awareness initiatives. For example, two studies have analyzed the public’s knowledge of smoking as a risk factor for AMD; these found, that 68 percent and 54 percent of the adults surveyed did not know that smoking was associated with specific types of vision impairment (AMD Alliance International, 2005; Caban-Martinez et al., 2011). A 2011 study investigating awareness of the relationship between smoking and vision impairment among smokers in the United States found that only 9.5 percent of smokers believed that smoking caused blindness, with those with a lower education level significantly more likely to doubt the association (Kennedy et al., 2011).
Even people who know that they have an eye disease or condition may not understand how that should affect their behavior. A primary reason that those who would benefit from an examination give for not seeing an eye care professional, even when they have an existing visual impairment and eye disease risk factors such as diabetes, is that “no need” exists (Bailey et al., 2006; Chou et al., 2014; McGwin et al., 2010; Varano et al., 2015). Substantial variation exists by state, and older populations are more likely to cite “no need” as a reason for not having their eyes examined (Chou et al., 2012, 2014). Patients are significantly more likely to receive annual eye examinations if they understand that examinations can detect eye disease (Sheppler et al., 2014). A 2008 American Optometric Association survey
found that, although 81 percent of Americans use some form of vision correction, 32 percent were unaware that chronic and systemic diseases can be detected during an eye exam (AOA, 2008). A more recent survey found that, although African American participants with diabetes knew that they needed to have their eyes checked, they did not know why (NEHEP, 2014). A lack of awareness is also a barrier to accessing rehabilitation services among people who have uncorrectable impaired vision (Lam and Leat, 2015). The NEI-LCIF KAP survey revealed that only 31 percent of individuals with low vision had been told to see a low vision specialist (NEI/LCIF, 2008). These findings suggest that many eye care providers may not be providing sufficient education to their patients about low vision and the resources available to help them face the challenges associated with it—a topic that is explored further in Chapter 8.
In the absence of more robust data on public awareness about eye and vision health in general, it is reasonable to assume that members of the public know less about risk factors and appropriate actions to reduce the risk for specific eye diseases or conditions than about the existence of those diseases or conditions. The combination of a lack of awareness and the asymptomatic nature of much of early treatable disease leads to delayed diagnoses and treatment, which in turn leads to a greater risk of developing blindness (Alexander et al., 2008; Sloan et al., 2005). This suggests a need for additional public education activities and policies that encourage health care providers and public health practitioners to actively promote eye and vision health.
Efforts to Improve National Public Awareness of Eye and Vision Health
Enhancing public knowledge about a health threat is a fundamental first step in informing discussions that promote behavior change across multiple determinants of health and aligning health policies with general public health interests. Having reliable, consistent, evidence-based information that is available and accessible by a variety of stakeholders can help increase overall knowledge and lead individuals to behave in ways that promote good eye and vision health or seek appropriate care to slow progression of a vision-threatening disease or condition or to improve function when vision impairment is irreversible.
Public awareness campaigns—generally in combination with other public health strategies—have been used extensively and successfully in population health for decades. These campaigns often focus on behavior change that reduces the risk of poor health (e.g., smoking cessation, improved nutrition and exercise, increased cancer screenings) or the risk of injury (e.g., seatbelt use, reducing drunk driving and drug use, water safety). For example, campaigns targeting population tobacco use in adults have been
identified as an important component in comprehensive tobacco control programs intended to affect knowledge, behaviors, and agenda setting (Bala et al., 2013; Chang et al., 2011; Durkin et al., 2012; Fosson et al., 2014; Hershey et al., 2005; Niederdeppe et al., 2004). Public education mass media campaigns in the United States and Australia have also been shown to be effective at reducing morbidity, mortality, and the economic costs due to skin cancer (Doran et al., 2016; Kyle et al., 2008; Shih et al., 2009). Public awareness campaigns also serve to raise the visibility of an issue among the national electorate, which can lead to changes in laws, regulations, and policies at the federal, state, and local levels that are intended to support and enforce individual behavior change (e.g., legislation to increase seatbelt use or increase the drinking age) or increase the resources and programmatic focus for specific diseases or conditions (e.g., breast cancer or HIV/AIDS).
Current national activities A number of national and state programs are designed to advance public awareness about eye issues. Many of these programs target particular threats to vision, especially among the most at-risk populations. For example, NEHEP partners with more than 60 professional, civic, and voluntary organizations and government agencies concerned with eye health in order to increase public awareness through culturally appropriate, health-literate, and evidence-based health information about the importance of early detection and timely treatment of eye disease and the use of vision rehabilitation services among health care professionals and the public (NEI/NIH, 2015b). Specifically, NEHEP includes five vision education programs focusing on (1) people living in Hispanic/Latino communities, (2) people at risk for glaucoma, (3) diabetic eye disease, (4) age-related conditions, and (5) people living with low vision. NEHEP’s printable cards, pamphlets, and infographics are geared toward use by a community health organizer. NEHEP partners with local governments to create culturally appropriate educational materials (NEHEP, 2011). The Lions Eye Health Program is a community-based education program that promotes healthy vision and raises awareness of the causes of preventable vision loss (Lions Club, 2016).
Various organizations design websites and related promotional materials to support national awareness months for specific eye diseases and conditions. For example, the NEI identifies January as Glaucoma Awareness Month (NEI/NIH, n.d.). Prevent Blindness has declared February to be National AMD and Low Vision Awareness Month and June to be Cataract Awareness Month (Prevent Blindness, 2016b). These types of activities provide valuable information about vision loss, but they fail to create a
cohesive message that can advance eye and vision health as a larger public health priority among the general public.
Data on the impact of public awareness campaigns related to eye and vision health have largely been limited to data on exposure—e.g., the number of imprints, webpage views, or followers on social media websites—rather than on specific measures of health outcomes or on such determinants as attitudes and beliefs. There are no data to assess whether NEHEP activities have had an impact on health outcomes, behavioral change, or even general public awareness because the focus is not on behavior change and no funds are available to formally evaluate the program.5,6 Moreover, there is no recent information about the number of Americans exposed to health education initiatives that are vision centric. In the future, large-scale public awareness campaigns will need to explicitly include resources to assess impact at different stages of the campaign.
Targeted education programs There are various smaller-scale, more conservative efforts to improve consumer education, and advocacy, professional, and patient organizations and other stakeholders can play an important role in their coordination. Smaller-scale health education initiatives have been shown to be effective at increasing the numbers of people receiving vision care and improving patient outcomes (Livingston et al., 1998). In the United States, for example, multiple health education interventions to promote screening for diabetic retinopathy have proven effective at increasing the rates of dilated fundus examinations (Jones et al., 2010; Walker et al., 2008; Weiss et al., 2015). After implementing a major vision health education campaign targeted to populations at higher risk for developing eye disease, Australia saw significant increases in the use of eye services and decreases in the prevalence of behaviors that are associated with increased risk to vision health (Müller et al., 2007). Similar findings emerged from a Norwegian study among diabetics (Sundling et al., 2008). A 2005 study of metal-ware factories in Italy found that the use of educational materials to prevent work-related eye injuries could be effective when it was coupled with increases in official inspections to promote compliance with workplace regulations (Mancini et al., 2005). More generally, health education has been shown to improve perceived security, quality of life, and functionality among patients with irreversible vision impairment (Dahlin Ivanoff et al., 2002; Eklund et al., 2004, 2005, 2008). Simple educational interventions
___________________
5 It is important to note that NEHEP is not a behavioral change campaign per se and does not conduct general public outreach about eye health.
6 Personal communication, N. Ammary-Risch, National Eye Health Education Program, 2016.
with patients can improve adherence to prescribed therapies and treatment schedules (Ellish et al., 2011; Weiss et al., 2015).
Examples of local public awareness campaigns include the Marshall B. Ketchum University’s Children’s Vision Initiative in California, the Day with the Doctor Intervention in Indiana, the Eye Exams in Putnam City Schools project in Oklahoma, the See to Read Vision Awareness Program in Tennessee, and the All The Kids project in Mississippi (AOA, 2014). Again, data on the impact of these types of programs vary and need to be linked to patient health outcomes, in addition to monitoring health care utilization rates.
The role of the media Mass and social media play a central role in shaping the lives and priorities of societies and individual communities. The media is an important public health tool for shaping public sentiment and political poignancy and their downstream effects on community attention and political priorities, respectively (Convissor et al., 1990; McCombs and Shaw, 1972). Furthermore, how the media portrays a particular health concern, such as visual impairment, may also be able to reduce the stigma or negative public perception related to that condition (e.g., IOM, 2012b; NASEM, 2016). For example, in the case of drug policy research, one study found that the media influences audiences by “setting the agenda and defining public interest; framing issues through selection and salience; indirectly shaping individual and community attitudes towards risk; and feeding into political debate and decision making” (Lancaster et al., 2011, p. 397). In its 2003 report The Future of the Public’s Health in the 21st Century, the IOM cited media coverage of AIDS as a good example of how the media can enhance the visibility of important health topics among the general public (IOM, 2003). This knowledge can then serve as a catalyst to promote changes at the federal, state, local and community levels.
Little academic research exists on the role of the media in promoting eye and vision health in the United States. Some of the more common topics in the literature are various causes of eye injury (e.g., party foam–induced, work-related eye injuries, fireworks), although many of these studies call for additional awareness campaigns rather than evaluating the effectiveness of existing campaigns (Abulafia et al., 2013; Glazier et al., 2011; Korchak et al., 2012; Zohar et al., 2004). However, the Community Preventive Services Task Force has found strong evidence supporting the effectiveness of those health communication campaigns designed to influence behaviors “that use multiple channels, one of which must be mass media (e.g., television, radio, and billboards) but can also include small media, social media, and interpersonal communication, combined with the distribution of free or reduced-price health-related products” (ODPHP,
2010). The media’s significance will continue to grow as more traditional news outlets (e.g., television, radio, and newspapers) are being replaced with ever-evolving communication technologies (e.g., smartphones, tablet computers) and social media outlets. The ubiquity of social media continues to expand opportunities to engage and educate the public about the importance of maintaining eye and vision health, and social media can serve as a valuable resource to connect visually impaired people to needed services and advocacy platforms. The effective use of social media platforms in health promotion intervention programs, in general, remains a fluid topic of discussion (Chou et al., 2009, 2013; Korda and Itani, 2013; Lefebvre and Bornkessel, 2013; Moorhead et al., 2013; Neiger et al., 2012). The use and efficacy of social media to educate the public and increase awareness concerning eye and vision health warrants additional research and consideration.
A national public awareness campaign to promote eye and vision health Large-scale public awareness campaigns for eye and vision health will require substantial resources, which will necessitate a federal presence and collaboration with a variety of stakeholders in the public and private sectors. The most effective public awareness campaigns are usually large scale and multifaceted, involving a range of outreach activities, stakeholders and sponsors, educational materials, messaging, and media platforms. For example, to influence ultraviolet (UV) radiation-protective behaviors, a systematic review by the Community Preventive Services Task Force recommends “combinations of individual-directed strategies, mass media campaigns, and environmental and policy changes across multiple settings within a defined geographic area (city, state, province, or country)” (CPSTF, 2014).
Likewise, a comprehensive public awareness campaign for eye and vision health would need to be one component of a larger, long-term effort to change attitudes, knowledge, behavior, and practice across the lifespan. For example, the Partnership for a Healthier America and the Let’s Move! initiative have raised the visibility of childhood obesity as a public health priority using a variety of media platforms to increase awareness (e.g., Chanel One News in schools, websites, mass marketing campaigns with industry, agreements with Sesame Street) (Spinweber and Honeysett, 2013). The media messaging is part of a larger effort to engage a wide range of public and private partners in diverse activities in order to catalyze large-scale changes in behaviors, interventions, and education around childhood obesity. Some of the other activities include increasing access to healthier, quality, affordable meals, maintaining and creating safe places for children to play, offering more opportunities for kids to get involved in active play, and educating parents on ways to increase healthy eating habits and active play (The White House, 2010).
Given the current and projected number of individuals with varying degrees and types of vision impairment in the United States (see Chapter 2), it will be necessary for advocacy organizations, government agencies, health care professionals, public health practitioners, researchers, and private industry to collaborate in order to amplify messaging from public health entities within and across the federal government, governmental PHDs, and population health systems. A large-scale public awareness campaign will need to be centered around concise and concrete goals and to consider a combination of individual-directed strategies, mass media campaigns, and environmental and policy changes across multiple settings within defined geographic areas (e.g., city, state, province, or country). Ascertaining the impact of specific campaigns and the elements most closely predictive of success will require careful evaluation. As with anti-smoking campaigns, the intensity and duration of mass vision health media campaigns may influence effectiveness, but the population characteristics, length of followup, and concurrent secular trends and events will also be important to monitor (Doyle et al., 2008). Necessary outcomes should include, but not be limited to
- changes in knowledge about high prevalence conditions, diseases, and events;
- risk and protective factors that account for multiple determinants of health;
- behavior changes (e.g., access to and use of eye health services, and adherence to risk reduction practices); and
- health outcomes, including more downstream effects from vision impairment.
Federal support for the infrastructure and engagement in public awareness campaigns, and large-scale public health initiatives, is “more likely when a field has a united front of advocates to communicate the urgency of a problem, why that problem should be addressed now, and how best to solve the problem” (IOM, 2015, p. 346). This will require the eye and vision field to establish a common platform from which to advance messages to improve eye and vision health that extend beyond the delivery of health care services. Moreover, because a lack of knowledge about vision loss and the possible prevention or treatment of subsequent vision impairment requires increased knowledge among vulnerable populations and practitioners, public awareness campaigns hold promise as a tactic to mitigate these deficits, when included as one component of a larger population health strategy. Assessing the impact of specific campaigns will require carefully designed evaluations, to not only provide some evidence of return
on investment, but also provide the foundation from which to generate sustained support for ongoing efforts in future years.
EXPANDING ACCESS TO COMMUNITY-BASED VISION SCREENING SERVICES AND FOLLOW-UP CARE
Ensuring that at-risk populations are linked to appropriate clinical care is a public health function. Vision screening can be a critical connection between the clinical vision services system, the larger public health system, and the populations they serve. It is a means of strengthening clinical vision service actions in community settings and an opportunity for refocusing the clinical vision services system and its providers on the public health objectives of preventing and treating vision loss and approaches to accomplishing those objectives. In the absence of adequate resources to provide comprehensive eye examinations to every person in accordance with evidence-based guidelines, vision screenings may be performed by both optometrists and ophthalmologists, as well as by other properly trained individuals in order to expand entry into appropriate eye and vision care systems, as well as into the overarching health care system.
Vision screenings allow for the identification—but not diagnosis—of eye disease. In this report, unless otherwise stated, the term “vision screening” is used to refer to any of a set of general eye health assessments that can be used to identify potential problems with visual functioning or symptoms suggestive of an eye disease or condition. Screenings cannot diagnose the cause of vision problems, but they can be used to expand entry to the health care system and access to appropriate follow-up care for more vulnerable populations. Mobile screening and imaging units can improve access to vision care, promote follow-up care, optimize the capacity of a limited workforce, and promote multidisciplinary collaborations (Beynat et al., 2009; Boucher et al., 2008; Griffith et al., 2016; Hautala et al., 2009; Kodjebacheva et al., 2011). Vision screenings are generally less expensive and less time-consuming than comprehensive eye examinations, but there are also concerns about the sensitivity and specificity of vision screenings. These concerns and more technical aspects of screenings and comprehensive eye examinations are described in Chapter 7.
In the United States, emerging diagnostic technologies and innovative screening programs have extended the services of the vision care system to schools in remote and medically underserved areas. For example, photoscreening and remote autorefraction have been shown to be effective at screening schoolchildren for amblyopia and vision disorders in urban and rural Alaska (Arnold et al., 2008; Lang et al., 2007). Screening high-risk populations such as children for refractive error and amblyopia and then assuring access to proper treatment, including eye examinations
for clinical diagnosis and corrective lenses, are key actions that can be advanced through a variety of population health partnerships and strategies.
Vision Screening for Children and Other At-Risk Populations
As in adults, refractive error is a major cause of preventable vision impairment in children and young adults (Tarczy-Hornoch et al., 2013; Vitale et al., 2008). For example, the Collaborative Longitudinal Evaluation of Ethnicity and Refractive Error Study evaluated more than 2,500 children ages 5 through 17 and found “overall, 9.2 percent of the children were myopic, 12.8 percent were hyperopic, and 28.4 were astigmatic,” with pronounced differences between the four ethnic/racial groups studied (Kleinstein et al., 2003, p. 1141). Undiagnosed vision impairment in children can have substantial effects on social development and health, with the potential to negatively impact social, physical, educational, and professional activities (Davidson and Quinn, 2011; Kulp et al., 2016). Uncorrected refractive error can have significant effects on educational performance and is a risk factor for amblyopia (Tarczy-Hornoch et al., 2013). Glewwe and colleagues explore disparities in vision care utilization by low-income and minority children, noting that they “have a greater than average risk of under-diagnosis and under-treatment . . . [and] Title 1 students are two to three times more likely than non-Title 1 students to have undetected or untreated vision problems” (Glewwe et al., 2014, p. 1).
Mobile clinics and school-based vision screenings that are provided at no cost offer a means of addressing demonstrated financial, social, and political barriers to accessing eye care for children and other at-risk populations (Castanes, 2003). One school-based screening program in the United Kingdom achieved a screening acceptance rate of greater than 95 percent among 3,721 children; of the 11.14 percent of students referred who were for follow-up care, more than half had refractive errors correctable by eyeglasses (Toufeeq and Oram, 2014). In a screening program in North Carolina, school nurses evaluated 2,726 elementary school children during the 2009–2010 school year and identified 3 cases needing intervention out of every 100 evaluations (Kemper et al., 2012). Mobile clinics have been used to provide vision screenings for pre-kindergarten, kindergarten, and first-grade public school children, with one program performing more than 63,000 evaluations, representing 55 percent of the eligible population during a 12-year period (Griffith et al., 2016). Similarly, the University of California, Los Angeles (UCLA) Mobile Eye Clinic identified 906 out of 11,302 first-graders as having decreased visual acuity and found that eyeglasses would correct vision in 94.7 percent of those cases, although
the investigation did not record rates of follow-up care after screening (Kodjebacheva et al., 2011).
Independent scholars have similarly recommended that policy makers implement vision programs that bring vision services to children, including screening, into classroom environments (Ethan and Basch, 2008). Head Start and Early Head Start programs are required, in collaboration with parents, to “obtain linguistically and age appropriate screenings to identify concerns regarding a child’s developmental, sensory (visual and auditory), behavioral, motor, language, social, cognitive, perceptual, and emotional skills” within 45 calendar days of the child’s entry into the program and facilitate implementation of follow-up plans and treatment.7 The American Academy of Ophthalmology, the American Academy of Pediatric Ophthalmologists and Strabismus, and the American Academy of Pediatrics have recommended that vision screening be included in routine school-based vision checks because it can maximize the rate of early detection of amblyopia, strabismus, refractive error, and other eye conditions in children, among other benefits (AAO, 2013). Many states have imposed vision screening requirements for school-age children to help identify students in need of eye care (see, AAPOS, 2011, for a current list of state-by-state school screening requirements). Box 5-1 details the example of how the state of Michigan has promoted vision screening programs for children. However, specific requirements and screening practices vary among and even within states, with implications for the percentage of students with visual impairments that are identified as requiring eye care (AAPOS, 2011; Marshall et al., 2010). Some states—including Arizona, Hawaii, Idaho, New Hampshire, North Dakota, South Carolina, and South Dakota—have no pediatric vision screening policies at all, though the governments of New Hampshire and South Carolina do recommend screenings (AAPOS, 2011).
Promoting Follow-Up Care After Screenings
Screening programs cannot lead to reduced vision impairment if the process does not include a mechanism to assure appropriate follow-up care. One demonstration project that provided vision screening of preschool-age children at two primary care practices and two community-based centers achieved monocular visual acuity and stereopsis screening rates between 70 and 93 percent and 88 and 98 percent for 3- and 4-year-olds, respectively. However, the rates of follow-up varied widely—from 29 to 100 percent and from 41 to 100 percent for the 3- and 4-year-olds, respectively (Hartmann et al., 2006). A quality improvement project to enhance the rate of pediatric vision screenings at 13 clinics in North Carolina saw significant
___________________
7 45 C.F.R. 1304.20 (italic added).
improvements in the rate of screening among children ages 3 to 5 years over a 6-month period; vision distance testing increased from 92 to 97 percent, and stereopsis screening rates increased from 80 percent to 89 percent. Yet, follow-up rescreening for initially untestable children was infrequently documented, and referral rates for abnormal screens remained low at 48 percent (Kemper et al., 2011). Other studies have also found that the rates of appropriate referral and follow-up care can be sub-optimal (Hered and Wood, 2013).
Simple logic dictates that programs that provide eyeglasses following screenings or eye examinations will improve the sight of more people with correctable refractive error than screenings or examinations alone. A number of programs available through various philanthropic and charitable
organizations, professional organizations, and industry provide free eyecare screenings, examinations, and eyeglasses for children and other vulnerable populations to better ensure the detection of potential vision problems and improve eyesight. Box 5-2 provides some examples. Many of these programs are designed to link children and low-income individuals to available eye and vision services, including in some cases, provision of eyeglasses. Only a few recent peer-reviewed articles on population-level impact are available for these programs. A 2015 study on 689 students at 28 different schools served by the Philadelphia Eagles Eye Mobile found that false-positive rates of school nurse screening averaged 16.11 percent (range 0 to 44 percent), suggesting the need for better training to reduce false-positive screenings. The same study found that the use of prescribed glasses was 71 percent at 12 months, but only 53 percent of children followed through with their pediatric ophthalmology referral (Alvi et al., 2015).
Recently, Vision To Learn partnered with Johns Hopkins University, the Baltimore City Health Department, and the Baltimore City Public School System to launch a citywide initiative, Vision for Baltimore, which will provide vision screenings and free eyeglasses for pre-kindergarteners to eighth-graders in all 50 Baltimore City public schools (Naron and Mendes,
2016). The Baltimore City Health Department will administer initial screenings, with the support of the Anne E. Casey Foundation, the Abell Foundation, and Vision To Learn, the latter of which has mobile eye clinics for onsite services. Warby Parker, a New York City–based online eyewear retailer, has agreed to provide eyeglasses (Naron and Mendes, 2016). Staff from the School of Education and the Wilmer Eye Institute will work with the schools to train school staff and maximize the use of prescribed eyeglasses. A formal evaluation of the program’s impact is planned. Results documenting the impact on student achievement and eyewear compliance have been submitted for publication (Naron and Mendes, 2016). A similar initiative exists in New York City, where the Community Schools Initiative will expand its vision screening program to all 130 Community Schools (including elementary, middle, and high schools) through a partnership with Warby Parker to provide free eyeglasses to every student in need (City of New York, 2016). Evaluations of the impacts of these programs will be essential to establishing better evidentiary support for investment in similar programs. As indicated by even the short list of activities provided in Box 5-2, a wide range of partners is already committed to improving the eye and vision health of the nation. It will be important to follow the impact of these programs and evaluate critical success and failure factors when considering whether similar initiatives will work in other communities and on larger scales. Policy makers could collaborate with PHDs, school administrators, and other stakeholders on a national effort to standardize state requirements for vision screening in schools.
Medicaid and the Children’s Health Insurance Program are public health programs that can also provide eye and vision care coverage for certain low-income and disabled people and families (Kaiser Family Foundation, 2013; Medicaid, 2016b). All plans that cover children and adolescents must provide basic eye care services as an essential health benefit (Healthcare.gov, 2016). Optional eye and vision benefits under Medicaid are determined by individual states and so vary from state to state, but they may include the provision of eyeglasses and optometric, diagnostic, screening, preventive, and rehabilitative services, as well as prescription drugs, dental care, physical and occupational therapy, and podiatric services, among others (Medicaid, 2016a). Efforts to expand the benefits of these programs are considered in Chapter 6.
ENCOURAGING ENVIRONMENTS THAT SUPPORT EYE HEALTH AND VISUAL FUNCTION: POLICY DEVELOPMENT AND ENFORCEMENT
Health departments can play an important role in influencing the built environment, i.e., the physical environment constructed by human activity,
although “exact [legal] mechanisms vary by state and locality” (see, e.g., Perdue et al., 2003, p. 1392). The built environment includes all the physical parts of where we live, including homes, buildings, worksites, transportation systems, civic infrastructure, and public places (Dannenberg et al., 2011). State and LHDs have the legal authority and capacity to work across sectors to improve the environmental conditions that impede eye and vision health; these environmental conditions include both the built and social determinants of eye and vision health. Two of the more obvious issues related to the built environment are accessibility and injury prevention, although building design regulations may now explicitly address vision-related conditions, such as eyestrain. Accessibility barriers can range from poorly designed pavement to inadequate pedestrian crossings. Poorly designed physical spaces (such as difficult-to-navigate subway platforms and poorly lighted building interiors) can cause injuries to people with low vision (Imrie and Kumar, 1998). These are important elements to consider when developing a comprehensive population health approach to address eye and vision health. Indeed, based on a variety of factors, health departments may take a leading role in recommending changes to the built environment. Arguably, for example, Frieden’s (2010) Health Impact Pyramid places greater reliance on changing the environment (the context in the pyramid) than on medical care as the basis for health department interventions at the population level.
Ensuring Equal Access to Facilities and Services
The Americans with Disabilities Act (ADA) of 1990 (42 U.S.C. 12181),8 including changes by the ADA Amendments Act of 2008,9 prohibits discrimination on the basis of disability by state and local governments, places of public accommodation (e.g., hotels, shopping centers, pharmacies, doctor’s offices, hospitals, libraries, private schools, health spas), commercial facilities, and private entities. The Rehabilitation Act of 1973 provides similar protections in relation to programs operated or funded by the federal government, as well as requiring equal employment opportunity within the federal government.10 The ADA’s definition of disability includes “blindness” (defined as meaning having less than 20/200 visual acuity even with corrective lenses or a visual field that is 20 degrees or less, regardless of acuity).11 People with “low vision” (eyesight that is better than 20/200 or a visual field that is greater than 20 degrees but that includes a significant
___________________
8 P.L. 101-336, enacted July 26, 1990.
9 P.L. 110-325, enacted January 1, 2009.
10 P.L. 93-112, enacted September 26, 1973.
11 Social Security Act § 216(i)(1)(B).
vision impairment that substantially limits the ability to see well under different circumstances) may also require accommodations.
Entities subject to regulations must
follow accessibility standards when constructing or altering facilities; remove architectural or structural communication barriers in existing facilities where it is readily achievable to do so; make reasonable modifications in policies and procedures (e.g., allow person to be accompanied by service animal or guide dog, even if a hotel has a “no pets” policy); eliminate discriminatory eligibility criteria (e.g., allow a guest to use alternative state ID to substitute for driver’s license at check-in); and provide auxiliary aids and services leading to effective communication if it is not an undue burden and does not fundamentally alter the nature of the goods or services provided (e.g., provide alternate format materials such as Braille, large print, and audio tape when a guest cannot read standard print materials due to a disability). (DOJ, n.d.)
The facilities and services covered by the ADA includes, but are not limited to, transportation services; academic, medical, and recreational facilities; and government programs, activities, and services. For example, mass transit systems should design their facilities and equipment to be accessible to disabled individuals (AFB, 2016a). Airlines could offer additional services such as pre-boarding, a guided tour of the aircraft, and providing menus and evacuation information in Braille (SATH, 2013). Similarly, libraries, museums, shopping malls, community health clinics, courthouses, and city sidewalks should all be accessible to individuals with disabilities, including those who are legally blind. The ADA also requires that regulated entities promote effective communication with people who have disabilities that can affect different communication capabilities (DOJ, 2015). The U.S. Department of Justice has offered guidance on the types of services and practices that can be considered to better accommodate people with vision impairment under the ADA (see Box 5-3).
The Equal Employment Opportunity Commission, the agency responsible for enforcing the ADA, has also issued regulations regarding vision needs under the ADA Amendments Act of 2008. The statute, at 42 U.S.C. 12102(4)(c)(ii), states, inter alia, that mitigating measures include lowvision devices (excluding ordinary eyeglasses or contact lenses), the use of assistive technology, and reasonable accommodations or auxiliary aids or services. With regard to eyeglasses, the regulations state,
The ameliorative effects of the mitigating measures of ordinary eyeglasses or contact lenses shall be considered in determining whether an impairment substantially limits a major life activity. The term “ordinary eyeglasses or contact lenses” means lenses that are intended to fully correct visual acuity
or eliminate refractive error; and the term “low-vision devices” means devices that magnify, enhance, or otherwise augment a visual image.
Likewise, adaptive behaviors to compensate for low vision (such as side-to-side movement for someone with monocular vision) are included. Problems associated with the affordability of eyeglasses are discussed in Chapter 6.
Ensuring and enforcing equal access under the ADA will require collaboration among federal, state, and local governments, architects and engineers, city planners, disability rights advocates, and others.
Coordinating these actions to derive maximum value and efficiency from individual efforts is the difficult but necessary task of stakeholders in all sectors. Governmental PHDs can help facilitate these efforts by convening and working with local employers, regulators, and low-vision community advocates to create a long-term strategy to continue to improve ADA compliance.
Building Design and the Consideration of Light Sources
Appropriate architectural design can promote and maintain good eye and vision health as well as the functionality of individuals with vision impairment, especially in home-like settings. According to the Low Vision Design Committee of the National Institute of Building Sciences (NIBS), “while treatment of low vision and other visual disorders are medical issues, assuring optimal access to the built environment for persons with visual impairments is a design issue” (NIBS, 2015, p. 5). The NIBS committee recently published guidelines to help those planning and designing building sites to create building access, interior spaces with appropriate visual cues, and lighting design that optimizes the functioning of people with chronic visual impairments. For example, the implementation and manipulation of lighting design is an effective means to compensate for aging eyes and diminished abilities (Gordon, 2003; Krusen, 2010). Low-level lighting can contribute to falls (Paul and Liu, 2012). Creating office spaces and public open spaces with appropriate visual cues can help individuals with visual impairment navigate these spaces. Using high contrast colors can help make signing, light switches, or stairs more visible, and the use of matte paint can reduce glare. Tactile flooring and variations in ceiling height can reflect sound in ways that create cues for the visually impaired (Anderson, 2014). Using uniform lighting in hallways and stairwells can eliminate confusing shadows that may mimic changes in elevation (AFB, 2016b). Currently, it is not known whether these guidelines are widely observed (Sawyer and Kaup, 2014).
As the population ages and more people experience the vision loss typically associated with the aging process, it will become increasingly important to ensure that retirement communities, assisted living and nursing facilities, and general rehabilitation facilities are designed or furnished to enhance visual function in order to reduce the potential negative downstream consequences of vision impairment. Similar considerations are useful in individual homes and should be incorporated into public awareness campaigns targeting older populations.
Maintaining Eye Health: Going Green and Eyestrain
Eyestrain is a common condition that occurs when eyes become tired from continuous use, but it usually does not have serious or long-term consequences. In some cases, eyestrain can be suggestive of an underlying eye condition (e.g., accommodation insufficiency or convergence insufficiency) necessitating treatment (Chase et al., 2009). The causes of eyestrain may include reading without resting one’s eyes if underlying factors are present; driving long distances and performing other activities involving extended focus; being exposed to bright light or glare; working with insufficient light; having an underlying eye problem such as dry eyes, uncorrected refractive error, eye teaming disorder, or accommodative or binocular vision disorders; being stressed or fatigued; and exposure to conditions that may contribute to dry eyes (Barnhardt et al., 2012; Gowrisankaran and Sheedy, 2015). The phenomenon of computer vision syndrome, which is “a group of visual symptoms experienced in relation to the use of computers,” is relatively new and is associated with reduced productivity at work and reduced quality of life (Ranasinghe et al., 2016). Visual symptoms may include eyestrain, eye fatigue, headaches, ocular discomfort, dry eye, photophobia, diplopia, and blurred vision (Rosenfield, 2011; Sheedy et al., 2003).
Appropriate architectural design can help reduce eyestrain. Proper lighting, anti-glare filters, the ergonomic positioning of computer monitors, physical breaks away from screens, lubricating eye drops, and special computer glasses all may help improve visual comfort (Blehm et al., 2005). In recent decades, there have been efforts to promote the concept of “green buildings,” which are meant to ensure the healthiest possible environment while representing the most efficient and least disruptive use of land, water, energy, and resources (EPA, 2015). Many of these new buildings reduce energy consumption by incorporating large windows or exteriors, allowing daylight to reach more space (EPA, 2015). Daylighting, “the practice of placing windows or other openings and reflective surfaces so that during the day natural light provides effective internal lighting,” creates new challenges related to eye comfort (Spellman and Bieber, 2012, p. 256). Existing guiding principles for new construction require that facilities achieve a minimum daylight factor while providing appropriate lighting controls and glare control to minimize eyestrain (GSA, 2014). Such lighting controls can include building maintenance to keep windows free from glare, installing screen-type shading devices that are automatically controlled according to the seasons and the time, veiling reflections on monitors to reduce visual display terminal glare, and providing artificial lighting (Hwang and Kim, 2011). These controls protect occupants’ eyes and also contribute to improved psychological health and productivity (Hwang and Kim, 2011). The committee believes that policies encouraging these practices
are advisable and can encourage a broader range of stakeholders, including architects and human resource professionals, to think about their roles in promoting eye and vision health. As the use of computers and digital electronic devices for both vocational and non-vocational activities continues to expand in terms of the length of time as well as of the type of digital electronic screen available, it will become increasingly important to monitor how this environmental exposure affects eye health and development, especially in younger populations.
Improving Eye Injury Protection
Occupational and sports-related eye injuries occur frequently. Goldstein and Wee (2011) estimate that approximately 40,000 to 600,000 sports-related eye injuries alone occur annually. Many instances of eye injury can be avoided by using protective eyewear. The CDC, professional societies, and others recommend wearing eye protection during specific high-risk activities to reduce the risk of occupational eye injury and the associated potential for vision loss (AAO, 2016a; CDC, 2013a; OSHA, 2003; Prevent Blindness, 2016a). To reduce eye injuries, OSHA requires employers to use three eye safety strategies, as appropriate, in workplaces. These include (1) using engineering controls (i.e., the best strategy) such as machine guards that prevent the escape of particles or welding curtains for arc flash protection; (2) using administrative controls such as making certain that areas designated as “off limits” are visited only by those assigned to work there; and (3) providing for and enforcing the use of proper protective eyewear (CDC, 2013b). Employers must ensure that eye and face protection, which meets specified safety standards, is provided whenever necessary to protect workers from occupational hazards, and that all workers required to wear eye and face protection receive proper training and, when appropriate, fittings (OSHA, 2009, 2016).
Unfortunately, factors such as uncomfortable fit, the lack of available protection, and the lack of a culture of workplace safety may contribute to poor adherence rates (Lombardi et al., 2009). To improve compliance among workers, state agencies have produced simple materials for posting or distribution that seek to educate employees about the risks of injury and the benefits of eye protection (CDPH, 2008; TDI, 2007). The National Institute for Occupational Safety and Health and eye health safety and advocacy organizations have produced similar materials, available online, and OSHA has made an e-tool available to assist employers and employees with understanding the requirements for eye protection in their specific industries or occupations (CDC, 2013b; CPWR, 2014; OSHA, 2016; Prevent Blindness, 2016c). There are also concerns about certain under-regulated (and culturally distinct) agricultural worker communities,
but more research is needed to demonstrate the effectiveness of community-based participatory models of education on the state-level enforcement of federal OSHA standards (Earle-Richardson et al., 2014; Tovar-Aguilar et al., 2014; Verma et al., 2011).
Nationally representative surveys have found that the rates of appropriate use of recreational eye protection in adults and children are low (approximately 30 percent and 15 percent, respectively) (Forrest et al., 2008; Matter et al., 2007). Estimates suggest that more than 90 percent of sports-related eye injuries could be prevented by using appropriate eye protection (Prevent Blindness, 2016c). The American Academy of Ophthalmology, the American Academy of Pediatrics, the American Association for Pediatric Ophthalmology and Strabismus, and the American Public Health Association, and the American Academy of Optometry all recommend protective eyewear for children in sports that pose a risk of eye injury (AAP, 2011; AOA, 2016). Appendix F shows examples of recommended eye protection for different sports (NEI/NIH, 2015a). Ordinary prescription glasses, contact lenses, and sunglasses do not protect against eye injuries (CDC, 2013b). In fact, regular eye glasses do not mitigate the risk of more serious injury and may shatter on impact (Goldstein and Wee, 2011).
The committee considers the use of protective eyewear in recreational and hazardous environments (e.g., home settings or around hazardous materials) to be amenable to change through policy implementation and education campaigns. Interventions targeted at multiple, engaged stakeholders can result in players more likely to change their behavior as a result (Eime et al., 2004, 2005). A 2009 systematic review (looking at both occupational and recreational eye protection) concluded that current research “[does] not provide reliable evidence that educational interventions are effective in preventing eye injuries,” primarily due to the low quality of existing research and significant variation in study design (Shah et al., 2009, p. 11). However, Healthy People 2020 recommends such campaigns that could be combined with relevant policies and the provision of protective eyewear—to increase the use of protective eyewear in sports (CPSTF, 2010; ODPHP, 2016e). Surveillance systems monitor injuries, but more is needed to ensure compliance with occupational safety standards and to have more widespread adoption of protective eyewear in high-risk sports. Public awareness accompanied by policies, monitoring, and the provision of appropriate protective gear is essential so that athletes, parents, coaches, trainers, referees, and health care providers can help decrease morbidity from eye injuries (CDC, 2012; Goldstein and Wee, 2011; NEI/NIH, 2015a,b). Most importantly, school and organized sports programs can establish policies that promote and enforce the use of protective devices in particularly high-risk activities. Governmental PHDs can work with local communities to help develop and adopt regulations and policies that
support the use of protective eyewear in both workplace and sports settings. Future research in this area should focus on the factors affecting policy adoption and compliance with established policies.
Promote Infection Control and Immunization
Poor hygiene, infrequent replacement of contact lens storage cases, and overnight contact lens wear are avoidable risk factors for microbial keratitis, contact lens–related inflammation, and other ophthalmic complications affecting eye health (Collier et al., 2014; Keay et al., 2007; Radford et al., 2009; Stapleton et al., 2008, 2012; Szczotka-Flynn et al., 2010). The CDC issued recommendations for keeping eyes healthy in contact lens wearers, but a recent review of the literature on past and recent trends found that the incidence of serious contact lens–related eye infections (e.g., microbial keratitis), which can lead to vision impairment, is rising (CDC, 2015g; Yildiz et al., 2012). This suggests that the public may not be adhering to published recommendations for various reasons.
The primary obstacle to eliminating contact lens–related infection and associated vision loss is not a lack of clarity on best practices, but rather improving patient education, awareness, and adherence. The CDC reported in 2015 that 99 percent of surveyed contact lens wearers engage in at least one risk behavior (including sleeping in their contact lenses, swimming or showering with them, rinsing/storing them in water, and failure to follow replacement schedules) (Cope et al., 2015). The impact of increased health promotion or education activities (e.g., at each eye care professional follow-up appointments) on contact lens–related infections and associated vision loss, while potentially helpful, remains ambiguous (Donshik et al., 2007; Kuzman et al., 2014; Robertson and Cavanagh, 2011). The degree to which industry-wide solutions (e.g., improved contact lens materials or case design) could ameliorate case-related infection rates is unclear (Wu et al., 2015b).
Beyond infections stemming from improper use and maintenance of prescription contact lenses, infectious keratitis, corneal abrasions, and other types of eye damage have also been documented as results of wearing decorative contact lenses (Steinemann et al., 2005). These lenses are classified by the U.S. Food and Drug Administration (FDA) as “medical devices” and should be obtained only with a prescription (FDA, 2006). Nonetheless, one study found that approximately 54 percent of patients attained these lenses from an unlicensed optical shop without a prescription (Singh et al., 2012). A previous study found similar results, with 51 percent of the patients surveyed reporting they obtained their decorative lenses from an unlicensed provider (Steinemann et al., 2005). The same study found that none of the patients had ever worn contact lenses, predisposing them to unhygienic lens
handling techniques. The FDA and the CDC provide information directed at consumers, eye care professionals, and the industry regarding the policies, regulations, and health risks associated with unlicensed decorative contact lenses (FDA, 2006). The American Academy of Ophthalmology has also published articles in multiple languages warning against the purchase of such lenses (AAO, 2015). Large-scale public awareness campaigns may include messages related to the threat to eye health from non-prescription decorative lenses. Moreover, working with industry and the FDA, governmental PHDs can assist in enforcing laws intended to stop the sale and purchase of such lenses.
Infection control and immunization have had great success in stemming the transmission of infectious agents that can have a profound effect on sight (Rao, 2015). For example, interventions to prevent transmission in pre- and peri-natal circumstances and to maintain high immunization rates have helped eliminate rubella (ODPHP, 2016b). Shingles affects approximately one third of the population and is associated with conjunctivitis, keratitis, uveitis, and optic neuritis (Opstelten and Zaal, 2005). Improving the vaccination rates for the herpes zoster virus may help reduce related vision loss. Similarly, sexually transmitted disease (STD) programs should take into account the effect that a particular disease can have on sight.
Governmental PHDs are traditionally on the frontline for many issues related to infection control and prevention and can serve as a logical and informed point of contact for providers, industry, and consumer groups to help organize responses and emphasize the threat to eye and vision health when applicable. Similarly, there is an opportunity for eye care professionals and other health care providers to help one another reiterate the role that eye and vision health can play in improving overall health through broader public health initiatives.
Promotion of Eye and Vision Health as a Programmatic Focus: Provision of Technical Expertise and Resources
Federal agencies charged with a wide range of responsibilities in the promotion of public health are uniquely situated to provide the needed resources and expertise that will allow state and LHDs to incorporate eye and vision health as a programmatic focus. The Vision Health Initiative (VHI) is a multilevel collaboration between the CDC’s Division of Diabetes Translation and state and national partners, designed to promote vision health and quality of life for all populations, throughout all life stages, by preventing and controlling eye disease, eye injury, and vision loss resulting in disability. VHI has the unique role of collaborating with state and national partners to strengthen science and develop interventions to improve eye health, reduce vision loss and blindness, and promote the
health of people with vision loss (CDC, 2015a). In addition to its leadership role in VHI, the CDC also
- Provides technical assistance to national, state, and local organizations oriented to preserving, protecting, and enhancing vision;
- Offers scientific bases for collaboration among provider groups, financing systems, and policy makers so that health care systems can respond effectively to vision and eye health as a major public health concern;
- Aids in translating science into programs, services, and policies and in coordinating service activities with partners in the public, private, and voluntary sectors; and
- Addresses issues related to the cost of vision loss, vision disability, eye disease, and quality of life (CDC, 2015a).
VHI provides a number of examples of how federal support and involvement in eye and vision health can translate into information and practices at the state level (see Box 5-4). Many of these examples are specific to eye and vision health, including specific eye diseases, but the supported partnerships have also been extended to chronic conditions more broadly. For example, in 2003, the CDC entered into a partnership with Prevent Blindness America to build capacity in states to address vision and eye health, which led to the active engagement of the National Association of Chronic Disease Directors, an organization that represents the leaders of state health department chronic disease programs (NACDD, n.d.).
In 2016, the CDC implemented a vision grant program in partnership with state-based chronic disease programs and other clinical and nonclinical stakeholders “to engage in strategic initiatives or activities designed to improve vision and eye health” (NACDD, 2016, p. 1). The current grant program will award three states an average of $25,000 toward the development of activities that (1) “achieve the overall goal of advancing vision loss and eye health as public health priorities”; (2) “implement a vision and eye health intervention that focuses on [characterizing the burden of eye disease or vision loss, promote systems change, or implement interventions related to eye and vision health]”; and . . . (3) “focus on sustainability . . . beyond the initial funding period” (NACDD, 2016, p. 4). This is an important step in the right direction, but more extensive resources will be needed to allow each state the opportunity to invest resources in the eye and vision health of its population.
Similarly, the NEI provides funding opportunities and resources that have helped to increase understanding about eye and vision health problems. The NEI reports awarding approximately 1,600 research grants and training awards related to vision research, in addition to laboratory and
patient-oriented research at its own facilities, and it supports NEHEP, as described earlier in this chapter (NEI/NIH, 2015c). A review of the major advances reported by the NEI on its website suggests a heavy focus on the development and evaluation of effective treatments for specific eye diseases and conditions. Moreover, a review of the NEI’s pioneering new advances to prevent and treat vision loss indicates that much research focused on
stem cell research, gene therapy, the genetics of complex diseases, and the regeneration of the retina and connections to the brain (NEI/NIH, 2015c). Again, this is valuable information, but this programmatic emphasis needs to balance the need for novel scientific discoveries against the need for research that focuses on diseases and conditions that affect a larger proportion of the public. Regardless, clinical advances should be evaluated in terms of their clinical effectiveness as well as improved population health.
Despite the CDC’s and the National Institutes of Health’s (NIH’s) current commitment to improving the population’s eye and vision health, doing so is not a prominent line item in either’s budget (see Chapter 4). Furthermore, no part of the federal government has the statutory responsibility to ensure an adequately funded population health vision care agenda. At the state and local levels, vision care remains subordinate to other public health mandates and competing priorities. In short, to elevate eye and vision health as a population health issue, more coordination is needed within the federal government to expand the number and scope of opportunities to enhance state and local capacities.
Integration of Eye and Vision Health into Other Health Initiatives and Programs
The link between chronic diseases and the various determinants of health has been of interest to public health professionals for several decades (Ford et al., 2013). The risk of vision loss may be a direct consequence of an uncontrolled chronic disease, such as diabetes. Conversely, vision loss may put an individual at greater risk for poor health by affecting that person’s ability to engage in health-promoting activities such as physical activity, by affecting treatment adherence (e.g., taking medications), or by increasing the risk of falls or injuries (see Chapter 3). High priority public health problems, such as population smoking rates, can be a direct risk factor for vision loss. The obvious overlap between eye and vision health and other aspects of health priorities provides a unique opportunity to improve surveillance and research that can reduce vision impairment and improve health equity. In fact, the CDC has suggested that public service announcements that tie chronic vision impairment to specific unhealthy behaviors (e.g., smoking) and other chronic conditions (e.g., diabetes) may improve public awareness of eye disease (CDC, 2015d).
The following subsections provide examples of existing programs that could be integrated with eye and vision health. These do not represent the full spectrum of programs that are available and amenable to these efforts. Rather they are intended to provide helpful illustrations that public health officials and other stakeholders can use to interpret their own programmatic work in the context of eye and vision health.
Anti-Tobacco and Smoking Cessation Programs
In 2014, the Surgeon General released a 50-year follow-up report about the health consequences of smoking, which highlighted new evidence about the causal relationship between cigarette smoking and AMD, as well as possible links to other smoking-related ocular morbidities, such as diabetic retinopathy or dry eye (U.S. Surgeon General, 2014). Several studies have linked smoking to various common and severe eye diseases, such as cataract, glaucoma, AMD, and inflammation (Chakravarthy et al., 2010; DeAngelis et al., 2007; Delcourt et al., 2011; Edwards et al., 2008; Evans et al., 2005; Galor and Lee, 2011; Khan et al., 2006; Klein et al., 2010; Lechanteur et al., 2015; Lindblad et al., 2014; Thornton et al., 2005; Zhang et al., 2011). Smoking may have a more pronounced impact on the vision health of some patients, such as older adults, genetically at-risk populations, and those with certain chronic health conditions and behaviors, than on others (Coleman et al., 2010; Liang et al., 2014; Schaumberg et al., 2007; Schmidt et al., 2006; Wu et al., 2015a). Even non-smokers exposed to secondhand smoke have an increased risk of AMD (Khan et al., 2006). Smoking may also decrease the effectiveness of AMD treatments (Lee et al., 2013a), and studies have found that the risk of AMD is higher among current smokers than among former smokers.
Smoking cessation programs have been implemented in community and clinical settings, targeted to both specific populations and diverse communities, and have employed varying methods and technologies using multiple types of care providers (Asvat et al., 2014; Chen et al., 2012; Gao et al., 2013; Kim et al., 2015; Lee et al., 2013b; Lin et al., 2013; Mussener et al., 2016; Omana-Cepeda et al., 2016; Papadakis et al., 2013; Sarna et al., 2014; Simpson and Nonnemaker, 2013; Stanczyk et al., 2014). These programs have been moderately successful at decreasing the prevalence of smoking among targeted populations, and programs that are effective at reducing smoking in the general population may also accomplish the same outcomes in patients with AMD. A meta-analysis of observational studies concluded that the beneficial impact of smoking cessation increased over time (Cong et al., 2008; Myers et al., 2014; Neuner et al., 2009).
Vision loss has already been incorporated into some public health activities related to smoking. The Vision Integration and Preservation Program, a collaboration between the New York State Department of Health and Prevent Blindness Tri-State, integrated vision health “preservation strategies into existing programs and functions within [the] state health department to promote public health strategies among community-based organizations and vision partners” (VHIPP, 2012, p. 2). The program produced vision health education resources on sports-related eye injuries and the impact of smoking, diabetes, and diet on vision health (Prevent Blindness, 2012).
Three programs were evaluated in terms of their efforts to integrate vision into existing program, and the results showed that sustained programming was feasible when vision fit into the existing deliverables and that it could be achieved with minimal effort and “very good” or “excellent” value (VHIPP, 2012). The New York State Department of Health also developed a “Smoking Causes Blindness” awareness campaign based on ads that had previously proved successful in increasing rates of smoking cessation in Australia (Asfar et al., 2015). The $2.5 million campaign ran on the radio and television and appeared on internet ads from December 2009 to February 2010 (NYSDOH, 2009). A 9 percent increase in calls to the state tobacco quit line was attributed to this public campaign, but rates to the call line decreased after the campaign’s end (Asfar et al., 2015). Despite such successes, questions remain about the effectiveness of smoking cessation programs, especially in the context of specific eye diseases, such as cataracts (Lindblad et al., 2005, 2014; Weintraub et al., 2002).
Incorporating eye and vision health into anti-smoking initiatives may have other benefits, which may affect ongoing and future collaborations between eye care professionals and other health care providers. A recent survey found that optometrists and ophthalmologists may not routinely advise patients to quit smoking (Caban-Martinez et al., 2011). Asfar and colleagues suggested that eye care professionals can “integrate smoking cessation treatment in the standard care of patients’ management” and can “serve as powerful public advocates against tobacco use, thereby significantly enhancing public awareness about the link between smoking and eye disease” and reducing vision loss in the long term (Asfar et al., 2015, p. 1120). This highlights a new role for eye care professionals in combating other high-priority health problems in at-risk populations, although more research is needed on systems-level strategies that include tobacco control in eye care settings (Asfar et al., 2015; Loo et al., 2009).
Skin Cancer and UV Exposure
UV radiation, both from natural sunlight and from artificial UV rays, can damage both the surface tissues (i.e., cornea) and the internal structures (i.e., lens and retina) of the eye (Behar-Cohen et al., 2014; Sliney, 2001). Because most UV radiation comes from the sun, outdoor behavior can significantly influence the risk of subsequent and cumulative eye damage. Multiple studies have documented an increased risk of UV-caused damage to the eyes among pilots (Chorley et al., 2011, 2015, 2016). Sun shields, hats, and contact lenses can provide some protection again UV damage, but sunglasses (and even non-tinted plastic spectacles) worn close to the head can reduce most UV back reflection and transmission (Citek, 2008; Krutmann et al., 2014). The back reflection of radiation from lenses to the
eye is also a concern, and antireflective coatings can considerably increase UV radiation back reflection (Citek, 2008). Better assessment and comparison of the UV-protective properties of lenses in actual use is needed (Behar-Cohen et al., 2014).
Recommendations for reducing the risk of skin cancer often focus on avoiding UV exposure to eyes and surrounding areas by wearing sunglasses (Glanz et al., 2002). For example, in Australia, “SunSmart” policies encourage school children to wear hats, especially broad-brimmed hats, during outdoor activities to reduce the risk of cancer from the sun, which can also benefit eye health (Gies et al., 2006). Similar policies in the United States encourage use of hats and sunwear in schools and in specific occupations (especially for workers who are often outside, such as migrant workers), although concerns about dress codes for reasons unrelated to eye health can present barriers (Hammond et al., 2009; Wright et al., 2007). Longitudinal studies that are designed to track the incidence of skin cancer (including on the skin around the eyes) in relation to UV exposure and the use of protective equipment could include eye health as another related health outcome.
Obesity and Physical Activity
A number of eye diseases and conditions may have risk factors that are associated, directly or indirectly, with obesity and exercise levels. For example, diabetic retinopathy may result from diabetes, and type 2 diabetes can be a consequence of obesity. Thus, understanding the risk factors for developing diabetes may also provide data relevant to the risk of developing diabetic retinopathy.
Increased exercise, including outdoor activity, is encouraged to reduce childhood and adult obesity (IOM, 2011a; U.S. Surgeon General, 2016). Outdoor activity has also been inversely associated with the likelihood of myopia in school children (Guo et al., 2013; Parssinen et al., 2014; Rose et al., 2008), although the exact mechanism is unknown. Recent increases in myopia among Chinese students (almost 82 percent of 16- to 18-year-olds were diagnosed with myopia) have highlighted the need for more information about the duration and characteristics of near-work activity and the risk of myopia in school children (Dolgin, 2015; Guggenheim et al., 2012). Another recent Chinese study found that watching television and playing on the computer, among other factors, was associated with increased prevalence of myopia (Zhou et al., 2016). The degree to which screen time exposure alone affects the development or progression of refractive error remains unknown. Screen time and other sedentary activities are already tracked as a contributor to the obesity epidemic in the United States (Boone et al., 2007; Council on Communications and Media, 2011; Rey-Lopez et al., 2008). Including measures of eye and vision health (such as
myopia) in studies on obesity and physical activity, especially those tracking physiological metrics, could provide valuable information about shared risk factors and related physiological mechanisms, maximizing efficiencies, resources, and overall impact on health. Furthermore, incorporating dilated eye examinations could provide another mechanism by which to identify other comorbid conditions (e.g., diabetes, multiple sclerosis) (CDC, 2016b; Frohman et al., 2008).
The committee concluded that governmental PHDs and other stakeholders should consider including eye and vision health measures and metrics into existing programs to better understand the risk and protective factors for vision impairment and the relationship that exists between eye and vision health and other chronic diseases. The committee recognized that incorporating other measures and metrics into existing programs will increase the scope and expense of such trials and studies. However, establishing partnerships between the eye and vision research communities and the cancer research communities, to the extent that they do not sufficiently exist within specific areas, could help improve efficiency and increase the impact of limited resources, requiring less horse trading to advance both eye and vision health and other governmental PHD duties.
Vision Impairment as a Chronic Condition
The designation of a health condition as a chronic condition is important because HHS
administers a large number of federal programs directed toward preventing and managing chronic conditions, including, for example, financing health care services (Centers for Medicare & Medicaid Services); delivering care and services to persons with chronic conditions (Administration on Aging, Health Resources and Services Administration, and Indian Health Service); conducting basic, interventional, and systems research (Agency for Healthcare Research and Quality, National Institutes of Health); implementing programs to prevent and manage chronic disease (Centers for Disease Control and Prevention, and Substance Abuse and Mental Health Services Administration); promoting the economic and social well-being of families, children, individuals, and communities (Administration for Children and Families); and overseeing development of safe and effective drug therapies (Food and Drug Administration). (HHS, 2010a, p. 4)
HHS has released a framework on multiple chronic conditions, with one of the overarching goals being to “foster health care and public health system changes to improve the health of individuals with multiple chronic conditions” (HHS, 2010a, p. 6). Under this framework, HHS encourages payment reform and incentives to reduce and avoid health outcomes that
negatively affect both the individual and the health care system, such as hospital readmissions. The framework also promotes preventive interventions to mitigate the progression and exacerbation of existing chronic conditions (HHS, 2010a).
Chronic vision impairment qualifies as a general chronic condition under the Assistant Secretary of Health’s definition. In Chapter 1, the committee defined chronic vision impairment as “a vision impairment that is present and must be managed over the lifespan to maintain the activities of daily living.” An analysis of legally blind adults included in National Health Interview Survey data found that 46 percent of blind adults reported a limited ability to perform personal care activities, and 52 percent reported problems with at least one instrumental activity of daily living12 (Zuckerman, 2004). Vision-threatening eye diseases and conditions (such as glaucoma, AMD, and diabetic retinopathy) cannot be cured, but permanent damage to the eye can be mitigated or their progression slowed through continuous medical management. In the case of refractive error, prescriptions must be monitored with some frequency (usually less so in mid-life), and new eyeglasses must be acquired if needed. Without these services and items, vision impairment can affect the performance of daily activities or even, in the case of amblyopia and strabismus in children, lead to permanent vision impairment. Even in the case of cataract, the progression and monitoring of the condition may occur over many years before surgery is necessary. Following surgery, examinations may be necessary to check for complications or to monitor the development of other eye conditions for which cataract surgery is a known risk factor.
The Centers for Medicare & Medicaid Services (CMS) have identified certain eye diseases and conditions as chronic conditions. Cataracts and glaucoma comprise the “eye disease” category. Medicare/Medicaid beneficiaries with cataracts and glaucoma equaled, respectively, 15.4 percent and 8.6 percent of all enrollees in 2008 (CMS, 2014). A CMS analysis grouped clinical and chronic conditions into categorical condition groups (CCGs), of which glaucoma and cataracts comprised the aggregate CCG “Eye Disease.” The total expenditure for possessing two CCGs at the per-member/per-month rate of $1,628 totaled more than $1.47 billion in 2008 (CMS, 2014). Analysis of comorbidity CCG pairs among enrollees with a diagnosed condition in the “Eye Disease” CCG found co-occurring CCG diagnoses in lung disease (26 percent), anemia (39 percent), mental health conditions (39 percent), diabetes (43 percent), musculoskeletal disorders (48 percent), and heart conditions (86 percent) (CMS, 2014).
___________________
12 Instrumental activities of daily living defined here as using telephones, shopping, preparing meals, managing money, and doing housework.
Nonetheless, vision impairment is generally excluded as a categorical focus for multiple chronic condition improvement. In 2013, Goodman and colleagues published an article that outlined a conceptual model for “improving understanding of and standardizing approaches to defining, identifying, and using information about chronic conditions in the United States” (Goodman et al., 2013, p. 1). As part of this exercise, the article included an appendix of 20 conditions13 that were chronic, prevalent, and “potentially amenable to public health or clinical interventions or both,” as well as being identifiable through International Classification of Diseases (ICD) codes (Goodman et al., 2013, p. 1). When this definition was applied to sources from CMS, the Agency for Healthcare Research and Quality, and the Robert Wood Johnson Foundation (RWJF) to identify a “manageable number” of conditions, eye disease was overlooked despite its prevalence across the lifespan as well as the fact that it was addressed as a chronic condition in both the RWJF and CMS sources (Anderson, 2010; CMS, 2016). The article itself does note that “visual impairment” is a chronic condition stemming from permanent or long-standing anatomical problems. Although this article serves as an example of how to approach the identification and prioritization of chronic conditions for various clinical and public health initiatives, it was not meant to dictate a formal list of the conditions to be included in these initiatives and programs—although it has been interpreted as such in many cases (Bayliss et al., 2014).
Although the visibility of other chronic conditions certainly does and should affect the prioritization of eye disease and vision impairment, chronic vision impairment also affects the prevalence and health outcomes associated with other chronic conditions (see Chapter 2). To the extent that data and evidence-based guidelines are available to assess the impact of, and care processes for, vision impairment as a chronic condition, vision impairment should be considered for inclusion in any framework targeting multiple chronic conditions. Some existing programs designed to combat the costs and negative outcomes of comorbid conditions should, given the high-prevalence of co-occurring diagnoses, incorporate eye and vision health This is already being studied in the United Kingdom, with eye care services being reciprocally incorporated into depression treatment and screening for hearing loss (Court et al., 2014). It is important for government agencies to consider reevaluating the status of eye and vision health.
___________________
13 These conditions include hypertension, congestive heart failure, coronary artery disease, cardiac arrhythmias, hyperlipidemia, stroke, arthritis, asthma, autism spectrum disorder, cancer, chronic kidney disease, chronic obstructive pulmonary disease, dementia, depression, diabetes, hepatitis, human immunodeficiency virus, osteoporosis, schizophrenia, and substance abuse disorders (Goodman et al., 2013, p. 1).
Upstream Determinants of Health
An elevated risk of vision impairment is often associated with other inequities associated with broader social, economic, and political conditions that either passively permit or inadvertently contribute to unhealthy conditions affecting a population, especially those already at-risk for poor health outcomes (see Chapters 1 and 2). The result is disparities in both the prevalence of vision-threatening eye diseases and conditions and also the severity of vision impairment among various race or ethnicity groups and genders and across geographic locations.
The World Health Organization’s Commission on Social Determinants of Health called on national governments and organizations to achieve greater health equity by addressing important social determinants of health (WHO, n.d.a.). Healthy People 2020, which is led by the Office of Disease Prevention and Health Promotion in HHS,14 has identified the creation of “social and physical environments that promote good health for all” as one of the four overarching goals for 2020 (ODPHP, 2016c). To this end, Healthy People 2020 includes measure such as “proportion of children ages 0 to 17 living with at least one parent,” “employed year round, full time,” “proportion of persons living in poverty,” and “proportion of all households that spend more than 50 percent of income on housing” (ODPHP, 2016d). The sense of sight is critically important to an individual’s communication, physical health, independence and mobility, social engagement, educational and employment opportunities, socioeconomic status, and performance of daily activities, such as reading, driving a car, and caring for family members (Alberti et al., 2014; Bowers et al., 2009; Bronstad et al., 2013; Davidson and Quinn, 2011; Rahi et al., 2009; Sengupta et al., 2015; Whitson and Lin, 2014; Whitson et al., 2007; Wood et al., 2012). Thus, part of the equation to maximize health equity will be to prevent vision loss and to adequately respond to the burden of vision impairment, including providing eyeglasses, treatments, and rehabilitation services.
Building Determinants of Health into Existing Programs
Intersectoral collaborative efforts to improve health and its determinants span various federal agencies. Some examples include First Lady Michelle Obama’s Let’s Move! campaign with its attention to the availability, accessibility, and promotion of nutrition; the Interagency Partnership for Sustainable Communities of the U.S. Department of Housing and Urban
___________________
14 Other departments include the U.S. Department of Agriculture, U.S. Department of Education, U.S. Department of Housing and Urban Development, U.S. Department of Justice, U.S. Department of the Interior, U.S. Department of Transportation, U.S. Department of Veterans Affairs, and the U.S. Environmental Protection Agency.
Development, the U.S. Department of Transportation, and the U.S. Environmental Protection Agency; and the new RWJF’s vision for a culture of health, which promotes healthy and safe environments, equal opportunity, and health care coverage as some of the elements necessary for people to lead healthier lives now and in the future (National Center for Appropriate Technology, 2014; RWJF, 2014; White House Task Force on Childhood Obesity, 2010). Other countries are also making strides in this area. For example, the Public Health Agency of Canada funded its national collaborating centers in 2005, which include a National Collaborating Centre for Determinants of Health, which focuses on advancing social determinants of health and health equity through public health practice and policy—engaging in many of the same broad categories of programmatic focus as the CDC’s VHI.
The CDC is well positioned to incorporate into its programs many of these upstream determinants of eye and vision health, which may fall outside the scope of more traditional clinical, research, and public health endeavors to improve health. The CDC has several programs indirectly related to eye and vision health targeting social determinants of health, which could be used as templates to build eye- and vision-specific programs addressing social determinants. For example, the National Program to Eliminate Diabetes-Related Disparities in Vulnerable Populations provides funding to organizations to “help plan, develop, implement, and evaluate multi-sector community-based interventions to work on social, cultural, economic, and environmental issues that influence health disparities associated with diabetes” (CDC, 2016a). This is led by the Division of Diabetes Translation within the National Center for Chronic Disease Prevention and Health Promotion, and it calls attention to increased rates of mortality and “serious health complications, including heart disease, blindness, kidney failure, and lower-extremity amputation” (CDC, 2014a) [emphasis added]. The CDC also provides a toolbox to help partnerships develop initiatives that address the social determinants of health in communities (Ramirez et al., 2008). In the context of eye and vision health, VHI acknowledges primary prevention and how health is shaped by many factors (e.g., family, community, social network, cultural, beliefs, healthy literacy, economics and environment), but these factors are typically couched in terms of improving “the use, acceptance, and accessibility of quality vision care” rather than in terms of reducing the risk factors that contribute to poor health (CDC, 2007, p. 16). VHI is an example of a program that could be expanded to provide a more comprehensive focus on the upstream factors that affect eye and vision health.
More is needed to ensure that greater improvements in population eye health outcomes can be achieved by addressing both the social determinants of health and individual-level risk factors for vision impairment. Because
social and environmental conditions contribute to almost all of the conditions that the CDC addresses, a more integrated focus may be needed across programs to address the upstream conditions of health. The committee encourages efforts to expand this focus on the broader determinants that affect all health conditions, with special attention placed on the role of eye and vision health as both an outcome and an intervening variable.
The Example of Health Literacy
Health literacy has been defined as the degree to which individuals have the capacity to obtain, process, and understand basic health information and the services needed to make appropriate health decisions (IOM, 2004, p. 2). Low health literacy is associated with less use of preventive services (e.g., mammograms, Pap smears, and flu shots), more use of health care services (i.e., emergency room visits and hospitalizations), higher health care costs, and a higher risk of death and poor treatment outcome (Al Sayah et al., 2015; Baker et al., 1997, 2002; Bennett et al., 1998; Cimasi et al., 2013; Glassman, 2013; Haun et al., 2015; McNaughton et al., 2015; Sentell et al., 2015). In glaucoma patients, several studies have shown that poor health literacy is associated with noncompliance to treatment, nonadherence to medications, worse disease understanding, greater disease progression, and poor visual outcomes (Freedman et al., 2012; Juzych et al., 2008; Muir et al., 2006, 2013). In addition, patients with poor health literacy have greater visual field loss on initial presentation than those with adequate health literacy (Juzych et al., 2008).
In 2003, both the IOM and the U.S. Surgeon General identified improving health literacy as critical to advancing the health of the nation (Carmona, 2003; IOM, 2003). In 2010, HHS introduced a National Action Plan to Improve Health Literacy, which highlights the need to develop and disseminate health and safety information, promote changes in the health care system to facilitate consumer decision making, incorporate appropriate curricula into educational settings, support local efforts to provide age-appropriate and culturally sensitive information, build partnerships to change policies, increase basic research and the evaluation of health literacy interventions, and increase the use of evidence-based practice (HHS, 2010b). The committee notes that the accompanying Health Literate Care Model does not specifically highlight any particular disease or condition, including eye and vision health (Koh et al., 2013). However, the proposed toolkit can be used by eye care professionals and public health practitioners together to design interventions that improve eye and vision health literacy, including raising awareness, communicating clearly, accounting for culture and other considerations, using health education materials effectively, and working with other health and literacy resources in the community. Available resources address
health care organization, health information systems, self-management support, links to supportive systems, engagement of individuals as partners in care and improvement efforts, and activated patients and families (ODPHP, 2016a). These are useful resources for the eye and vision care community. Moreover, efforts to evaluate the impact of general health literacy initiatives should take into account the interdependent relationships that exist among vision, overall health, and other social determinants of health.
ENHANCING ACCOUNTABILITY
Accountability refers to “the principle that individuals, organizations and the community are responsible for their actions and may be required to explain them to others” (Benjamin et al., 2006, p. 78). A core governmental PHDs function is providing assurance that appropriate institutions are protecting the public’s health, rather than a specific subset of the population (e.g., patients within a health care system). This is an essential accountability mechanism that only the governmental PHDs can provide for the population’s eye and vision health. In any population health initiative, accountability is important because it forces partners and collaborators to measure and communicate a program’s expectations and the magnitude of its impact to inform and influence the public and elected officials.
In 2011, the IOM released the report For the Public’s Health: The Role of Measurement in Action and Accountability, which chronicled different types of measures and assessments for characterizing the public health system’s impact and how decision makers can use these tools to inform policies and practices (IOM, 2011c). The report proposed that “assessing and measuring accountability at any level (local, state, or national) and holding organizations accountable require the following four foundational elements:
- An identified body with a clear charge to accomplish particular steps toward health goals.
- Ensuring that the body has the capacity to undertake the required activities.
- Measuring what is accomplished against the identified body’s clear charge.
- The availability of tools to assess and improve effectiveness and quality (such as a feedback loop as part of a learning system, incentives, and technical assistance).” (IOM, 2011c, p. 113)
This will require a process for priority setting and for evaluating the impact of specific programs to maintain accountability to the public, partners, and policy makers.
Prioritizing Eye and Vision Health
Population health priorities should be driven by more than simple mortality rates and should account for the potential quality of adjusted life years, the economic impact of the particular problem across the lifespan, and the ability to prevent or eliminate a potential burden for a large proportion of the affected individuals. As discussed in Chapter 2, the burden of eye diseases and vision impairment affects individuals across the lifespan to varying degrees of severity. To begin to diminish this public health burden, state and LHDs can explicitly make eye and vision health a priority as part of their strategic planning and program implementation. To establish nationwide consistency, the CDC and other federal bodies would also need to prioritize eye and vision health within their official strategic plans. As noted earlier in the chapter, neither state nor LHDs will be able to give, or support, emphasis in the eye and vision health area without some consistent source of financial and staffing support. Thus, additional congressional funding specific to eye and vision health initiatives beyond current levels would also be necessary.
The CDC has recognized five definitional features of a public health problem: (1) the problem affects a large number of people; (2) the problem imposes large morbidity, quality-of-life, and cost burdens; (3) the severity of the problem is increasing and is predicted to continue increasing; (4) the public perceives the problem to be a threat; and (5) community- or public health-level interventions to the problem are feasible (CDC, 2009). As described in earlier chapters, eye and vision health meet this definition. There are many diseases, conditions, and injuries that meet this definition, however, so governmental PHDs and other community stakeholders must decide whether the promotion of eye and vision health is indeed a priority.
Priority setting helps balance the most pressing needs with the finite budget. A number of tools are available to help governmental PHDs and other population health stakeholders determine what will constitute health priorities within their communities. Box 5-5 describes the broad suggestions of the National Association of County and City Health Officials for prioritizing community health issues. For example, the Department of Public Health for the County of Los Angeles identifies four categories of criteria that could be used by decision makers: (1) a quantitative assessment of the magnitude of the issue, (2) a qualitative assessment of the importance of the issue, (3) the effectiveness of interventions, and (4) the feasibility of implementing interventions (Department of Public Health County of Los Angeles, 2010). For evaluating eye and vision disorders, these criteria may accurately depict the preventable and correctable burden that could potentially be alleviated through public health measures. Studies evaluating the use of these criteria for eye and vision health in the health department
priority-setting processes would be particularly useful to serve as a model for implementation across the country.
In 2006 the National Association of Chronic Disease Directors with the support of the CDC’s National Center for Chronic Disease Prevention and Health Promotion, convened a workshop on chronic disease program integration because of its growing interest in state public health agencies. Participants developed a list of eight principles for state health agencies to use as a guide for supporting chronic disease program integration initiatives. These principles can be instructive in the context of vision impairment:
- Engage state health agency leadership,
- Develop crosscutting epidemiology and surveillance programs,
- Leverage the use of information technology,
- Build state and local partnerships,
- Develop integrated state plans,
- Engage management and administration,
- Implement integrated interventions, and
- Evaluate integration activities. (Slonim et al., 2007)
The strategic alignment of resources includes combining programs or activities that currently focus on a particular topic, but it also includes the integration of new yet complementary topics into existing programs. This integration affords the opportunity to address upstream determinants of health that span health conditions beyond eye and vision health across the spectrum, yet are seldom the primary purview of any single program. When evaluating whether eye and vision health rises to the level of a “top priority” within a given community, the committee encourages governmental PHDs, policy makers, private industry, nonprofit organizations, the media, the public, and other stakeholders to carefully consider the scope of the problems associated with vision impairment, the availability of treatments to effectively and relatively easily correct or reverse vision impairment for millions of people, the lack of knowledge about relatively simple behaviors that can reduce the risk of vision loss, and the wide range of strategies available to ensure that eye and vision health are present within formal programmatic designs.
Strategies to Improve Accountability for Eye and Vision Health
Holding organizations accountable for specific eye and vision health outcomes will be difficult for several reasons. First, there are numerous problems related to basic surveillance of the prevalence and impact of vision impairment from an epidemiological perspective, as described in Chapter 4. Second, because vision impairment can both contribute to and result from other chronic conditions, it can be difficult to eliminate the effects of confounding variables and ascertain the effects of specific variables on eye and vision health metrics. Third, all health outcomes in a community naturally shift and change over time, regardless of whether a public health intervention has been implemented. Fourth, there is a lack of evidence-based research documenting the characteristics and long-term impact of known community-based interventions across representative populations. For example, the Healthy People 2020 website lists systematic reviews for interventions that are strongly supported in the literature to accomplish goals related to eye and vision health (ODPHP, 2016f). Only three resources are listed, and two of them apply to clinical services.15 The community-based intervention pertains to health communication and social marketing
___________________
15 The website discloses that “evidence-based resources ha[ve] been rated and classified according to a set of selection criteria based, in part, on publication status, publication type, and number of studies. This classification scheme does not necessarily consider all dimensions of quality, such as statistical significance, effect size (e.g., magnitude of effect), meaningfulness of effect, additional effect over control, and study design (e.g., sample size, power, internal validity, external validity, generalizability, potential biases, potential confounders)” (ODPHP, 2016f).
in general. The same problems are not as prevalent for clinical interventions in the context of eye and vision health. Fifth, because there is little research available about the effect of specific interventions, there is even less information about how and whether to scale those interventions to benefit different populations in different geographic locations. Sixth, because vision loss and impairment can be the cumulative effect of multiple exposures over the lifespan, it can take decades to determine whether a particular public health intervention has had an impact. Finally, there are other challenges associated with aligning the missions of diverse population-health partnerships, which may affect the outcomes most relevant to particular groups.
Despite these challenges, strategies are available to enhance accountability for population-health activities intended to advance eye and vision health. For instance, public health agencies and departments can support collaborative efforts by collecting, analyzing, and disseminating data related to the targeted public health problem. Public health agencies could track and report progress related to the 10 essential public health services (see Chapter 1), across a variety of actors. As discussed in Chapter 4, this may involve combining eye-specific databases and those that track other chronic conditions or health determinants. Vision impairment should be added to chronic disease surveillance systems. Government public health agencies “can also serve as managers or facilitators of incentives that both reward and serve as a tool for holding stakeholders accountable (i.e., driving other sectors to demonstrate accountability on contributions to health improvement) in some cases on behalf of the community in general or a community group” (IOM, 2011c, p. 123).
To improve the quality, effectiveness, and consistency of public health services, the IOM and other organizations have identified national accreditation as a mechanism by which to improve accountability (see, e.g., IOM, 2012c). The expansion of the Public Health Accreditation Board (PHAB) process for quality standards and measurement has the potential to assure accountability, improve public health service delivery, and offer a better understanding of which public health programs are working and which need to be improved (PHAB, n.d.). The committee recognizes that the national accreditation effort is not mature, continues to evolve, and must remain dynamic and responsive to a changing system. Moreover, as described above, although some states have maintained their own accreditation process, there are significant variations across states regarding the process. As the accreditation standards for required public health services and measures evolve, there may be an opportunity to mandate components related to vision impairment, such as the number of at-risk people who receive an eye examination, which could address disparities in access to care. In the absence of a specific vision components, there are also opportunities to incorporate eye and vision health metrics into health impact
assessments and community health assessments and improvement plans, which are required elements for accreditation.
Health impact assessments Efforts to examine the ramifications of policy decisions on health outcomes are becoming possible through the use of tools, such as health-impact assessments, as part of the “health-in-all-policies” movement (CDC, 2015b; Koivusalo, 2010). The National Research Council defines a health impact assessment (HIA) as “a systematic process that uses an array of data sources and analytic methods and considers input from stakeholders to determine the potential effects of a proposed policy, plan, program, or project on the health of the population” (NRC, 2011, p. 5). As part of the requirements for public health accreditation, many state and LHDs conduct a systematic HIA on a regular basis. Through the HIA process, LHDs systematically collect and analyze data to identify the community’s health needs, establish priorities for programs and investments, devise metrics for ongoing evaluation and quality assurance (PHAB, 2013), and monitor progress toward meeting health improvement objectives (i.e., developing and implementing a health improvement plan) (ASTHO, 2016; Rubin et al., 2015). Eye and vision health, however, is not commonly part of these assessments and plans (Shin and Finnegan, 2009) (see Chapter 4). PHBA could develop an eye and vision HIA module and offer appropriate guidance for data collection and analysis.
Community health assessments and planning A community health assessment and community health improvement plan are required for accreditation. Additionally, changes in the health care environment, particularly the Patient Protection and Affordable Care Act (ACA), offer specific opportunities for health departments to be significant actors and partners in vision and eye health. First, under the ACA, nonprofit hospitals and health systems must conduct a community health needs assessment (CHNA) in conjunction with the LHD in their catchment area at least once every 3 years and implement a community health improvement plan to address the identified priorities. The CHNA process is a convenient mechanism for identifying those with visual impairment who are likely to need educational accommodation, along with income and other social supports. Second, vision is an element of the Healthy People 2020 objectives. According to the Office of Disease Prevention and Health Promotion,
The Healthy People 2020 Vision objectives focus on evidence-based interventions to preserve sight and prevent blindness. Objectives address screening and examinations for children and adults, early detection and timely treatment of eye diseases and conditions, injury prevention, and the use of vision rehabilitation services. (ODPHP, 2016e)
Third, the ACA created the National Prevention, Health Promotion, and Public Health Council with a process to set a national prevention strategy. The national prevention strategy could be a mechanism for promoting eye health, especially in the context of uncorrected refractive error.
Valuing community-based prevention Beyond current actionable items, there is also interest in establishing effective frameworks and models to assess the value of community-based prevention services and different types of partnerships. Although this area is still in the early stages, frameworks have been developed by the IOM and other organizations to guide communities, PHDs, and policy makers, among others, in thinking about quantifying the relationship between benefits and harms in terms of community health, well-being, and process and resource utilization (IOM, 2012a). Evaluating the impact of public–private partnerships will also be difficult. Partnerships vary in the scope, objectives, stakeholders involved, and the inclusion of multifaceted interventions to resolve complex health problems. As a result, improvements in public health outcomes cannot
always be reliably attributed to the actions of a partnership. In addition, partnership goals may be ambiguous or may shift over time, making it difficult to even define program success (Smith et al., 2009). Research into the effectiveness of public–private partnerships is generally limited, and many existing analyses conclude that further research is needed (Pedersen et al., 2015; Vrangbaek, 2008). Arthur Himmelman has suggested a matrix of strategies for working together, which includes networking, coordinating, cooperating, and collaborating, which may be good starting points from which to develop specific evaluation metrics (Himmelman, 2002). Population health research agendas would benefit from increased attention and support related to the systematic evaluation and valuation of the types of activities explored in this chapter. Evidence of their effectiveness would likely drive greater attention and provide more information on how best to target limited resources in order to best benefit population eye and vision health in various communities.
To better assist with the evaluation of the impact of specific interventions and programs and increase the accountability of specific governmental PHDs related to eye and vision health, it will be important to have additional information available to both establish a baseline for improvement and determine whether improvements in population eye and vision health have occurred. To this end, Box 5-6 provides a list of key research gaps that have been mentioned throughout this chapter.
CONCLUSION
Governmental PHDs are a critical lynchpin to advancing eye and vision health, but they are constrained by the current level of resources available and the overall emphasis of public health on communicable diseases and emergency preparedness. Governmental PHDs provide a range of services to promote population health, but capacity to provide these services is contingent on adequate and sustained resources (e.g., funding, personnel, and expertise) to meet increasing demands. It will be difficult to achieve better eye and vision health at a national level given current funding levels.
Because the role of governmental PHDs varies from the federal to the state and to the local level, and also by the specific organizational structure and resources of LHDs, advancing eye and vision health requires a broad range of activities that varies by jurisdiction based on available infrastructure, resource, and need. Short- and long-term population health strategies should address the broad determinants of health, including policies that influence individual behaviors, healthy environments, and social conditions, because of their potential impact on eye and vision health. Enhancing public awareness of the etiology, causes, and risk factors related to eye and vision health, as well as the behaviors that effectively reduce the risk of vision loss,
is an important and essential first step to establishing eye and vision health as a public health priority. However, public awareness and education alone will not be sufficient. Eye and vision health promotion will require varied strategies to influence both individuals and to create social and physical environments that support those behaviors. This may include policies and regulations that encourage the use of protective eyewear in hazardous work environments and during some recreational activities; that expand access to essential eye and vision screenings, examinations, and treatments; and that encourage eye-friendly building design. It may also require governmental PHDs and other critical stakeholders to integrate eye and vision health as a complementary element within existing public health programs, especially those related to chronic diseases. Public health can facilitate the development of clinical care systems that assure the organized delivery of care to everyone in their jurisdiction (see Chapters 7 and 8).
Establishing a wide range of partnerships can help expand governmental PHDs capacity by either providing additional resources to expand services related to eye and vision health or by providing necessary clinical services in community environments, which could allow governmental PHDs to focus on other essential public health services in eye and vision health such as coordination of clinical care systems and community-based efforts. Partnerships should include a variety of stakeholders from the community, clinical care systems, employers and businesses, the media, nonprofit organizations, the education sector, and government agencies—including those that have already made substantial contributions to the field, as well as stakeholders for whom optimal eye and vision health may be a non-explicit but nevertheless mission-specific objective. These partnerships can complement existing federal, state, and local funding and activities and future efforts to integrate eye and vision health into public health messaging, research, policy and practice, as well as across agencies, departments, and institutes in order to maximize efficiencies and enhance public health capacities.
Improving the accountability of governmental PHDs and health care systems will be important to increasing the visibility of community eye and vision health. This will require formal responsibility to incorporate objectives related to eye and vision health into existing public health and health care initiatives, to measure the impact of specific interventions, and to evaluate the availability of resources necessary to scale effective interventions that benefit the most at-risk populations. Establishing eye and vision health as public health priorities will not be easy due to limitations in public health capacities, surveillance challenges, limited evidence-based research, among other challenges. However, the chronic nature of many vision impairments and their impact on other chronic diseases and health determinants require federal, state, and local governments and other diverse yet critical stakeholders to carefully and collaboratively consider the potential benefits
and available opportunities to increase the prominence of eye and vision health among current population health priorities. Preventing disability and poor quality of life from preventable, modifiable, or correctable vision impairment is a health imperative in its own right. It is time to meet that challenge head on.
REFERENCES
AAO (American Academy of Ophthalmology). 2013. Vision screening for infants and children—2013. http://www.aao.org/clinical-statement/vision-screening-infants-children--2013 (accessed April 7, 2016).
———. 2015. Halloween warning from ophthalmologists: Over-the-counter contact lenses could contain dangerous chemicals. http://www.aao.org/newsroom/news-releases/detail/halloween-warning-from-ophthalmologists-over-count (accessed July 12, 2016).
———. 2016a. Eye injuries at work. http://www.aao.org/eye-health/tips-prevention/injuries-work (accessed April 6, 2016).
———. 2016b. Online referral center. https://secure.eyecareamerica.org/onlinematch/default.aspx?lang=en-US&refresh=1 (accessed July 11, 2016).
AAP (American Academy of Pediatrics). 2011. AAP publications reaffirmed and retired. Pediatrics 128(3):e748 (referencing Committee on Sports Medicine & Fitness. 2004. Protective eyewear for young athletes. Pediatrics 113(3):619–622).
AAPOS (American Association for Pediatric Ophthalmology and Strabismus). 2011. State-by-state vision screening requirements. http://www.aapos.org/resources/state_by_state_vision_screening_requirements/ (accessed April 7, 2016).
Abulafia, A., F. Segev, E. Platner, and G. J. Ben Simon. 2013. Party foam-induced eye injuries and the power of media intervention. Cornea 32(6):826–829.
AFB (American Foundation for the Blind). 2016a. Accessible mass transit. http://www.afb.org/info/living-with-vision-loss/getting-around/accessible-mass-transit/235 (accessed April 7, 2016).
———. 2016b. Creating a comfortable environment for people with low vision. http://www.afb.org/info/low-vision/living-with-low-vision/creating-a-comfortable-environment-forpeople-with-low-vision/235 (accessed April 7, 2016).
Al Sayah, F., S. R. Majumdar, L. E. Egede, and J. A. Johnson. 2015. Associations between health literacy and health outcomes in a predominantly low-income African American population with type 2 diabetes. Journal of Health Communication 20(5):581–588.
Alberti, C. F., E. Peli, and A. R. Bowers. 2014. Driving with hemianopia: III. Detection of stationary and approaching pedestrians in a simulator. Investigative Ophthalmology & Visual Science 55(1):368–374.
Alexander, R. L., N. A. Miller, M. F. Cotch, and R. Janiszewski. 2008. Factors that influence the receipt of eye care. American Journal of Health Behavior 32(5):547–556.
Alvi, R. A., L. Justason, C. Liotta, S. Martinez-Helfman, K. Dennis, S. P. Croker, B. E. Leiby, and A. V. Levin. 2015. The Eagles Eye mobile: Assessing its ability to deliver eye care in a high-risk community. Journal of Pediatric Ophthalmology and Strabismus 52(2):98–105.
AMD (Age-related Macular Degeneration) Alliance International. 2005. Awareness of age-related macular degeneration and associated risk factors. Toronto, Ontario: AMD Alliance International.
Anderson, G. 2010. Chronic care: Making the case for ongoing care. Princeton, NJ: Robert Wood Johnson Foundation.
Anderson, L. 2014. How a San Francisco architect reframes design for the blind. http://www.curbed.com/2014/8/6/10064320/how-a-san-francisco-architect-reframed-design-for-the-blind (accessed April 6, 2016).
AOA (American Optometric Association). 2008. Third annual American Optometric Association American Eye-Q survey. http://texas.aoa.org/documents/2008-Eye-Q-ExecutiveSummary.pdf (accessed July 25, 2016).
———. 2012. Infantsee®. http://www.infantsee.org (accessed July 11, 2016).
———. 2014. 2014 HEHP projects. http://www.aoafoundation.org/hehp/hehp-projects/2014-hehp-projects (accessed February 4, 2016).
———. 2016. School-aged vision: 6 to 18 years of age. http://www.aoa.org/patients-andpublic/good-vision-throughout-life/childrens-vision/school-aged-vision-6-to-18-years-ofage?sso=y (accessed July 11, 2016).
AOA Foundation. 2016. How the program operates. http://www.aoafoundation.org/visionusa/how-the-program-operates (accessed July 11, 2016).
Arnold, R. W., L. Stark, R. Leman, K. K. Arnold, and M. D. Armitage. 2008. Tent photoscreening and patched HOTV visual acuity by school nurses: Validation of the ASD–ABCD protocol. (Anchorage School District–Alaska Blind Child Discovery Program). Binocular Vision & Strabismus Quarterly 23(2):83–94.
Asfar, T., B. L. Lam, and D. J. Lee. 2015. Smoking causes blindness: Time for eye care professionals to join the fight against tobacco. Investigative Ophthalmology & Visual Science 56(2):1120–1121.
ASTHO (Association of State and Territorial Health Officials). 2012. State and local health department governance classification system. http://www.astho.org/Research/Data-andAnalysis/State-and-Local-Governance-Classification-Tree (accessed July 7, 2016).
———. 2014. ASTHO profile of state public health, volume three. Arlington, VA: ASTHO.
———. 2016. Community health needs assessments. http://www.astho.org/Programs/Access/Community-Health-Needs-Assessments (accessed April 6, 2016).
Asvat, Y., D. Cao, J. J. Africk, A. Matthews, and A. King. 2014. Feasibility and effectiveness of a community-based smoking cessation intervention in a racially diverse, urban smoker cohort. American Journal of Public Health 104(Suppl 4):S620–S627.
Bailey, R. N., R. W. Indian, X. Zhang, L. S. Geiss, M. R. Duenas, and J. B. Saaddine. 2006. Visual impairment and eye care among older adults—Five states, 2005. Morbidity and Mortality Weekly Report 55(49):1321–1325.
Baker, D. W., R. M. Parker, M. V. Williams, W. S. Clark, and J. Nurss. 1997. The relationship of patient reading ability to self-reported health and use of health services. American Journal of Public Health 87(6):1027–1030.
Baker, D. W., J. A. Gazmararian, M. V. Williams, T. Scott, R. M. Parker, D. Green, J. Ren, and J. Peel. 2002. Functional health literacy and the risk of hospital admission among Medicare managed care enrollees. American Journal of Public Health 92(8): 1278–1283.
Bala, M. M., L. Strzeszynski, R. Topor-Madry, and K. Cahill. 2013. Mass media interventions for smoking cessation in adults. Cochrane Database of Systematic Reviews 6:Cd004704.
Barnhardt, C., S. A. Cotter, G. L. Mitchell, M. Scheiman, M. T., Kulp, CITT Study Group. 2012. Symptoms in children with convergence insufficiency: Before and after treatment. Optometry & Vision Science 89(10):1512–1520.
Bayliss, E. A., D. E. Bonds, C. M. Boyd, M. M. Davis, B. Finke, M. H. Fox, R. E. Glasgow, R. A. Goodman, S. Heurtin-Roberts, S. Lachenmayr, C. Lind, E. A. Madigan, D. S. Meyers, S. Mintz, W. J. Nilsen, S. Okun, S. Ruiz, M. E. Salive, and K. C. Stange. 2014. Understanding the context of health for persons with multiple chronic conditions: Moving from what is the matter to what matters. Annals of Family Medicine 12(3): 260–269.
Behar-Cohen, F., G. Baillet, T. de Ayguavives, P. O. Garcia, J. Krutmann, P. Pena-Garcia, C. Reme, and J. S. Wolffsohn. 2014. Ultraviolet damage to the eye revisited: Eye-sun protection factor (E-SPF (R)), a new ultraviolet protection label for eyewear. Journal of Clinical Ophthalmology 8:87–104.
Beitsch, L. M., C. Leep, G. Shah, R. G. Brooks, and R. M. Pestronk. 2010. Quality improvement in local health departments: Results of the NACCHO 2008 survey. Journal of Public Health Management and Practice 16(1):49–54.
Benjamin, G., M. Fallon, P. E. Jarris, and P. Libbey. 2006. Final recommendations for a voluntary national accreditation program for state and local public health departments. Alexandria, VA: Public Health Accreditation Board.
Bennett, C. L., M. R. Ferreira, T. C. Davis, J. Kaplan, M. Weinberger, T. Kuzel, M. A. Seday, and O. Sartor. 1998. Relation between literacy, race, and stage of presentation among low-income patients with prostate cancer. Journal of Clinical Oncology 16(9):3101–3104.
Beynat, J., A. Charles, K. Astruc, P. Metral, L. Chirpaz, A. M. Bron, and C. Creuzot-Garcher. 2009. Screening for diabetic retinopathy in a rural French population with a mobile non-mydriatic camera. Diabetes & Metabolism 35(1):49–56.
Blehm, C., S. Vishnu, A. Khattak, S. Mitra, and R. W. Yee. 2005. Computer vision syndrome: A review. Survey of Ophthalmology 50(3):253–262.
Boone, J. E., P. Gordon-Larsen, L. S. Adair, and B. M. Popkin. 2007. Screen time and physical activity during adolescence: Longitudinal effects on obesity in young adulthood. The International Journal of Behavioral Nutrition and Physical Activity 4:26.
Boucher, M. C., G. Desroches, R. Garcia-Salinas, A. Kherani, D. Maberley, S. Olivier, M. Oh, and F. Stockl. 2008. Teleophthalmology screening for diabetic retinopathy through mobile imaging units within Canada. Canadian Journal of Ophthalmology 43(6):658–668.
Bowers, A. R., A. J. Mandel, R. B. Goldstein, and E. Peli. 2009. Driving with hemianopia, I: Detection performance in a driving simulator. Investigative Ophthalmology & Visual Science 50(11):5137–5147.
Bray, J. E., L. Straney, B. Barger, and J. Finn. 2015. Effect of public awareness campaigns on calls to ambulance across Australia. Stroke 46(5):1377–1380.
Bronstad, P. M., A. R. Bowers, A. Albu, R. Goldstein, and E. Peli. 2013. Driving with central field loss I: Effect of central scotomas on responses to hazards. JAMA Ophthalmology 131(3):303–309.
Brooks, R. G., L. M. Beitsch, P. Street, and A. Chukmaitov. 2009. Aligning public health financing with essential public health service functions and national public health performance standards. Journal of Public Health Management and Practice 15(4): 299–306.
Caban-Martinez, A. J., E. P. Davila, B. L. Lam, S. R. Dubovy, K. E. McCollister, L. E. Fleming, D. D. Zheng, and D. J. Lee. 2011. Age-related macular degeneration and smoking cessation advice by eye care providers: A pilot study. Preventing Chronic Disease 8(6):A147.
Carmona, R. H. 2003. Health literacy: Key to improving American’s health. http://www.surgeongeneral.gov/news/speeches/healthlit09192003.html (accessed April 6, 2016).
Castanes, M. S. 2003. Major review: The underutilization of vision screening (for amblyopia, optical anomalies and strabismus) among preschool age children. Binocular Vision & Strabismus Quarterly 18(4):217–232.
CBO (Congressional Budget Office). 2013. Federal grants to state and local governments. Washington, DC: CBO.
CDC (Centers for Disease Control and Prevention). 2007. Improving the nation’s vision health: A coordinated public health approach. Atlanta, GA: CDC.
———. 2009. Why is vision loss a public health problem? http://www.cdc.gov/visionhealth/basic_information/vision_loss.htm (accessed October 7, 2015).
———. 2012. Eye health tips. http://www.cdc.gov/visionhealth/basic_information/eye_health_tips.htm (accessed September 17, 2015).
———. 2013a. Eye safety. http://www.cdc.gov/niosh/topics/eye/eyechecklist.html (accessed April 6, 2016).
———. 2013b. Eye safety tool box talk—Instructor’s guide. http://www.cdc.gov/niosh/topics/eye/pdfs/instructor.pdf (accessed September 11, 2015).
———. 2014a. The National Program to Eliminate Diabetes-Related Disparities in Vulnerable Populations. http://www.cdc.gov/diabetes/prevention/pdf/vulnerablepopulationsfactsheet.pdf (accessed April 6, 2016).
———. 2014b. The public health system and the 10 essential public health services. http://www.cdc.gov/nphpsp/essentialservices.html (accessed March, 2016).
———. 2015a. About us. http://www.cdc.gov/visionhealth/about/index.htm (accessed April 6, 2016).
———. 2015b. Health in all policies. http://www.cdc.gov/policy/hiap/ (accessed April 6, 2016).
———. 2015c. NIOSH programs. http://www.cdc.gov/niosh/programs.html (accessed April 6, 2016).
———. 2015d. Powerful new “tips from former smokers” ads focus on living with vision loss and colorectal cancer. http://www.cdc.gov/media/releases/2015/p0326-tips.html (accessed June 13, 2016).
———. 2015e. Prevention status reports. Atlanta, GA: CDC.
———. 2015f. PHHS block grant. http://www.cdc.gov/phhsblockgrant/statehpprior.htm#i (accessed April 6, 2016).
———. 2015g. Protect your eyes. http://www.cdc.gov/contactlenses/protect-your-eyes.html (accessed April 6, 2016).
———. 2016a. CDC programs addressing social determinants of health. http://www.cdc.gov/socialdeterminants/cdcprograms/index.htm (accessed April 6, 2016).
———. 2016b. Keep an eye on vision health. http://www.cdc.gov/features/healthyvision (accessed July 12, 2016).
CDPH (Connecticut Department of Public Health). 2008. Health alert! Keeping an eye on eye protection. Hartford: CDPH.
Chakravarthy, U., T. Y. Wong, A. Fletcher, E. Piault, C. Evans, G. Zlateva, R. Buggage, A. Pleil, and P. Mitchell. 2010. Clinical risk factors for age-related macular degeneration: A systematic review and meta-analysis. BMC Ophthalmology 10:31.
Chang, F. C., C. H. Chung, Y. C. Chuang, T. W. Hu, P. T. Yu, K. Y. Chao, and M. L. Hsiao. 2011. Effect of media campaigns and smoke-free ordinance on public awareness and secondhand smoke exposure in Taiwan. Journal of Health Communication 16(4):343–358.
Chase, C., C. Tosha, E. Borsting, and W. H. Ridder, 3rd. 2009. Visual discomfort and objective measures of static accommodation. Optometry & Vision Science 86(7):883–889.
Chen, Y. F., J. Madan, N. Welton, I. Yahaya, P. Aveyard, L. Bauld, D. Wang, A. Fry-Smith, and M. R. Munafo. 2012. Effectiveness and cost-effectiveness of computer and other electronic aids for smoking cessation: A systematic review and network meta-analysis. Health Technology Assessment 16(38).
Chorley, A. C., B. J. Evans, and M. J. Benwell. 2011. Civilian pilot exposure to ultraviolet and blue light and pilot use of sunglasses. Aviation, Space, and Environmental Medicine 82(9):895–900.
———. 2015. Solar eye protection practices of civilian aircrew. Aerospace Medicine and Human Performance 86(11):953–961.
Chorley, A. C., K. A. Baczynska, M. J. Benwell, B. J. Evans, M. P. Higlett, M. Khazova, and J. B. O’Hagan. 2016. Occupational ocular UV exposure in civilian aircrew. Aerospace Medicine and Human Performance 87(1):32–39.
Chou, C. F., L. E. Barker, J. E. Crews, S. A. Primo, X. Zhang, A. F. Elliott, K. McKeever Bullard, L. S. Geiss, and J. B. Saaddine. 2012. Disparities in eye care utilization among the United States adults with visual impairment: Findings from the Behavioral Risk Factor Surveillance System 2006–2009. American Journal of Ophthalmology 154 (6 Suppl):S45–S52, e41.
Chou, C. F., C. E. Sherrod, X. Zhang, L. E. Barker, K. M. Bullard, J. E. Crews, and J. B. Saaddine. 2014. Barriers to eye care among people aged 40 years and older with diagnosed diabetes, 2006–2010. Diabetes Care 37(1):180–188.
Chou, W.-Y. S., Y. M. Hunt, E. B. Beckjord, R. P. Moser, and B. W. Hesse. 2009. Social media use in the United States: Implications for health communication. Journal of Medical Internet Research 11(4):e48.
Chou, W.-Y. S., A. Prestin, C. Lyons, and K. Y. Wen. 2013. Web 2.0 for health promotion: Reviewing the current evidence. American Journal of Public Health 103(1):e9–e18.
Christ, S. L., D. D. Zheng, B. K. Swenor, B. L. Lam, S. K. West, S. L. Tannenbaum, B. E. Muñoz, and D. J. Lee. 2014. Longitudinal relationships among visual acuity, daily functional status, and mortality: The Salisbury Eye Evaluation Study. JAMA Ophthalmology 132(12):1400–1406.
Cimasi, R. J., A. R. Sharamitaro, and R. L. Seiler. 2013. The association between health literacy and preventable hospitalizations in Missouri: Implications in an era of reform. Journal of Health Care Finance 40(2):1–16.
Citek, K. 2008. Anti-reflective coatings reflect ultraviolet radiation. Optometry 79(3):143–148.
City of New York. 2016. Partnership with Warby Parker. http://www1.nyc.gov/site/communityschools/schools-and-partners/partnership-with-warby-parker.page (accessed July 11, 2016).
CMS (Centers for Medicare & Medicaid Services). 2014. Physical and mental health condition prevalence and comorbidity among fee-for-service Medicare-Medicaid enrollees. Washington, DC: CMS.
———. 2016. Condition categories. https://www.ccwdata.org/web/guest/condition-categories (accessed March 18, 2016).
Coleman, A. L., R. L. Seitzman, S. R. Cummings, F. Yu, J. A. Cauley, K. E. Ensrud, K. L. Stone, M. C. Hochberg, K. L. Pedula, E. Thomas, C. M. Mangione, and the Study of Osteoporotic Fractures Research Group. 2010. The association of smoking and alcohol use with age-related macular degeneration in the oldest old: The Study of Osteoporotic Fractures. American Journal of Ophthalmology 149(1):160–169.
Collier, S. A., M. P. Gronostaj, A. K. MacGurn, J. R. Cope, K. L. Awsumb, J. S. Yoder, and M. J. Beach. 2014. Estimated burden of keratitis—United States, 2010. Morbidity and Mortality Weekly Report 63(45):1027–1030.
Cong, R., B. Zhou, Q. Sun, H. Gu, N. Tang, and B. Wang. 2008. Smoking and the risk of age-related macular degeneration: A meta-analysis. Annals of Epidemiology 18(8):647–656.
Convissor, R. B., R. E. Vollinger, Jr., and P. Wilbur. 1990. Using national news events to stimulate local awareness of public policy issues. Public Health Reports 105(3):257–260.
Cope, J. R., S. A. Collier, M. M. Rao, R. Chalmers, G. L. Mitchell, K. Richdale, H. Wagner, B. T. Kinoshita, D. Y. Lam, L. Sorbara, A. Zimmerman, J. S. Yoder, and M. J. Beach. 2015. Contact lens wearer demographics and risk behaviors for contact lens–related eye infections—United States, 2014. Morbidity and Mortality Weekly Report 64(32):865–870.
Council on Communications and Media. 2011. Children, adolescents, obesity, and the media. Pediatrics 128(1):201–208.
Court, H., G. McLean, B. Guthrie, S. W. Mercer, and D. J. Smith. 2014. Visual impairment is associated with physical and mental comorbidities in older adults: A cross-sectional study. BMC Medicine 12:181.
CPSTF (Community Preventive Services Task Force). 2010. Health communication and social marketing: Health communication campaigns that include mass media and health-related product distribution. Guide to Community Preventive Services. http://www.thecommunityguide.org/healthcommunication/campaigns.html (accessed June 10, 2016).
———. 2014. Preventing skin cancer: Multicomponent community-wide interventions. Guide to Community Preventive Services. http://www.thecommunityguide.org/cancer/skin/community-wide/multicomponent.html (accessed June 1, 2016).
CPWR (Center for Protection of Workers’ Rights). 2014. Eye protection. http://www.cpwr.com/sites/default/files/publications/CPWR_Eye_Protection_2.pdf (accessed April 6, 2016).
Dahlin Ivanoff, S., U. Sonn, and E. Svensson. 2002. A health education program for elderly persons with visual impairments and perceived security in the performance of daily occupations: A randomized study. American Journal of Occupational Therapy 56(3): 322–330.
Dannenberg, A. L., H. Frumkin, and R. J. Jackson. 2011. Making healthy places: Designing and building for health, well-being, and sustainability. Washington, DC: Island Press.
Davidson, S., and G. E. Quinn. 2011. The impact of pediatric vision disorders in adulthood. Pediatrics 127(2):334–339.
DeAngelis, M. M., F. Ji, I. K. Kim, S. Adams, A. Capone, Jr., J. Ott, J. W. Miller, and T. P. Dryja. 2007. Cigarette smoking, CFH, APOE, ELOV14, and risk of neovascular age-related macular degeneration. Archives of Ophthalmology 125(1):49–54.
DeHaven, M. J., I. B. Hunter, L. Wilder, J. W. Walton, and J. Berry. 2004. Health programs in faith-based organizations: Are they effective? American Journal of Public Health 94(6):1030–1036.
Delcourt, C., M. N. Delyfer, M. B. Rougier, P. Amouyel, J. Colin, M. Le Goff, F. Malet, J. F. Dartigues, J. C. Lambert, and J. F. Korobelnik. 2011. Associations of complement factor H and smoking with early age-related macular degeneration: The alienor study. Investigative Ophthalmology & Visual Science 52(8):5955–5962.
Department of Public Health County of Los Angeles. 2010. Priority-setting in public health. Los Angeles, CA: Quality Improvement Division.
DOJ (U.S. Department of Justice). 2001. Americans with Disabilities Act: Guide for place of lodging: Serving guests who are blind or who have low vision. https://www.ada.gov/lodblind.htm (accessed August 14, 2016).
———. 2015. ADA update: A primer for state and local governments. Washington, DC: DOJ.
———. n.d. Americans with Disabilities Act: Guide for places of lodging: Serving guests who are blind or who have low vision. https://www.ada.gov/reachingout/lodblind(lesson2).html (accessed July 11, 2016).
Dolgin, E. 2015. The myopia boom. Nature 519(7543):276–278.
Donshik, P. C., W. H. Ehlers, L. D. Anderson, and J. K. Suchecki. 2007. Strategies to better engage, educate, and empower patient compliance and safe lens wear: Compliance: What we know, what we do not know, and what we need to know. Eye & Contact Lens 33 (6 Pt 2):430–433; discussion 434.
Doran, C. M., R. Ling, J. Byrnes, M. Crane, A. P. Shakeshaft, A. Searles, and D. Perez. 2016. Benefit cost analysis of three skin cancer public education mass-media campaigns implemented in New South Wales, Australia. PLoS ONE 11(1):e0147665.
Doyle, J., R. Armstrong, and E. Waters. 2008. Issues raised in systematic reviews of complex multisectoral and community based interventions. Journal of Public Health (Oxford) 30(2):213–215.
Durkin, S., E. Brennan, and M. Wakefield. 2012. Mass media campaigns to promote smoking cessation among adults: An integrative review. Tobacco Control 21(2):127–138.
Earle-Richardson, G., L. Wyckoff, M. Carrasquillo, M. Scribani, P. Jenkins, and J. May. 2014. Evaluation of a community-based participatory farmworker eye health intervention in the “black dirt” region of New York State. American Journal of Industrial Medicine 57(9):1053–1063.
Edwards, R., J. Thornton, R. Ajit, R. A. Harrison, and S. P. Kelly. 2008. Cigarette smoking and primary open angle glaucoma: A systematic review. Journal of Glaucoma 17(7):558–566.
Eime, R., N. Owen, and C. Finch. 2004. Protective eyewear promotion: Applying principles of behaviour change in the design of a squash injury prevention programme. The American Journal of Sports Medicine 34(10):629–638.
Eime, R., C. Finch, R. Wolfe, N. Owen, and C. McCarty. 2005. The effectiveness of a squash eyewear promotion strategy. British Journal of Sports Medicine 39(9):681–685.
Eklund, K., U. Sonn, and S. Dahlin Ivanoff. 2004. Long-term evaluation of a health education programme for elderly persons with visual impairment. A randomized study. Disability and Rehabilitation 26(7):401–409.
Eklund, K., U. Sonn, P. Nystedt, and S. Dahlin Ivanoff. 2005. A cost-effectiveness analysis of a health education programme for elderly persons with age-related macular degeneration: A longitudinal study. Disability and Rehabilitation 27(20):1203–1212.
Eklund, K., J. Sjöstrand, and S. Dahlin Ivanoff. 2008. A randomized controlled trial of a health-promotion programme and its effect on ADL dependence and self-reported health problems for the elderly visually impaired. Scandinavian Journal of Occupational Therapy 15(2):68–74.
Ellish, N. J., R. Royak-Schaler, and E. J. Higginbotham. 2011. Tailored and targeted interventions to encourage dilated fundus examinations in older African Americans. Archives of Ophthalmology 129(12):1592–1598.
EPA (U.S. Environmental Protection Agency). 2015. What is green infrastructure? https://www.epa.gov/green-infrastructure/what-green-infrastructure (accessed April 7, 2016).
Ethan, D., and C. E. Basch. 2008. Promoting healthy vision in students: Progress and challenges in policy, programs, and research. Journal of School Health 78(8):411–416.
Evans, J. R., A. E. Fletcher, and R. P. Wormald. 2005. 28,000 cases of age related macular degeneration causing visual loss in people aged 75 years and above in the United Kingdom may be attributable to smoking. British Journal of Ophthalmology 89(5):550–553.
FDA (U.S. Food and Drug Administration). 2006. Decorative, non-corrective contact lenses. http://www.fda.gov/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/ucm071572.htm (accessed April 6, 2016).
Fischhoff, B., A. Bostrom, and M. J. Quadrel. 1993. Risk perception and communication. Annual Reviews of Public Health 14:183–203.
Fischhoff, B., R. Detels, R. Beaglehole, M. Lansing, and M. Gulliford. 2009. Risk perception and communication. Oxford Textbook of Public Health, Volume 2: The methods of public health (Ed. 5):940–953.
Ford, E. S., J. B. Croft, S. F. Posner, R. A. Goodman, and W. H. Giles. 2013. Co-occurrence of leading lifestyle-related chronic conditions among adults in the United States, 2002–2009. Preventing Chronic Disease 10:E60.
Forrest, K. Y., J. M. Cali, and W. J. Cavill. 2008. Use of protective eyewear in U.S. adults: Results from the 2002 National Health Interview Survey. Ophthalmic Epidemiology 15(1):37–41.
Fosson, G. H., D. M. McCallum, and M. B. Conaway. 2014. Antismoking mass media campaigns and support for smoke-free environments, Mobile County, Alabama, 2011–2012. Preventing Chronic Disease 11:E150.
Freedman, R. B., S. K. Jones, A. Lin, A. L. Robin, and K. W. Muir. 2012. Influence of parental health literacy and dosing responsibility on pediatric glaucoma medication adherence. Archives of Ophthalmology 130(3):306–311.
Frieden, T. R. 2010. A framework for public health action: The health impact pyramid. American Journal of Public Health 100(4):590–595.
Frohman, E. M., J. G. Fujimoto, T. C. Frohman, P. A. Calabresi, G. Cutter, and L. J. Balcer. 2008. Optical coherence tomography: A window into the mechanisms of multiple sclerosis. Nature clinical practice. Neurology 4(12):664–675.
Galor, A., and D. J. Lee. 2011. Effects of smoking on ocular health. Current Opinions in Ophthalmology 22(6):477–482.
Gao, K., M. D. Wiederhold, L. Kong, and B. K. Wiederhold. 2013. Clinical experiment to assess effectiveness of virtual reality teen smoking cessation program. Studies in Health Technology and Informatics 191:58–62.
Gebbie, K. M. 2000. The public health workforce: Enumeration 2000. Washington, DC: Health Resources and Services Administration.
Gies, P., J. Javorniczky, C. Roy, and S. Henderson. 2006. Measurements of the UVR protection provided by hats used at school. Photochemistry & Photobiology 82(3): 750–754.
Glanz, K., M. Saraiya, and H. Wechsler. 2002. Guidelines for school programs to prevent skin cancer. Morbidity and Mortality Weekly Report 51(RR04):1–16.
Glassman, P. 2013. Health literacy. https://nnlm.gov/outreach/consumer/hlthlit.html (accessed April 6, 2016).
Glazier, R., M. Slade, and H. Mayer. 2011. The depiction of protective eyewear use in popular television programs. Journal of Trauma and Acute Care Surgery 70(4):965–969.
Glewwe, P., K. West, and J. Lee. 2014. The impact of providing vision screening and free eyeglasses on academic outcomes: Evidence from a randomized trial in Title 1 elementary schools. Minneapolis: University of Minnesota.
Goldstein, M. H., and D. Wee. 2011. Sports injuries: An ounce of prevention and a pound of cure. Eye & Contact Lens 37(3):160–163.
Goodman, R. A., S. F. Posner, E. S. Huang, A. K. Parekh, and H. K. Koh. 2013. Defining and measuring chronic conditions: Imperatives for research, policy, program, and practice. Preventing Chronic Disease 10:E66.
Gordon, G. 2003. Interior lighting for designers. New York: Wiley.
Gowrisankaran, S., and J. E. Sheedy. 2015. Computer vision syndrome: A review. Work 52(2):303–314.
Griffith, J. F., R. Wilson, H. C. Cimino, M. Patthoff, D. F. Martin, and E. I. Traboulsi. 2016. The use of a mobile van for school vision screening: Results of 63,841 evaluations. American Journal of Ophthalmology 163:108–114.e1.
GSA (U.S. General Services Administration). 2014. Green building certification system. Washington, DC: GSA.
Guggenheim, J. A., K. Northstone, G. McMahon, A. R. Ness, K. Deere, C. Mattocks, B. S. Pourcain, and C. Williams. 2012. Time outdoors and physical activity as predictors of incident myopia in childhood: A prospective cohort study. Investigative Ophthalmology & Visual Science 53(6):2856–2865.
Guo, Y., L. J. Liu, L. Xu, P. Tang, Y. Y. Lv, Y. Feng, M. Meng, and J. B. Jonas. 2013. Myopic shift and outdoor activity among primary school children: One-year follow-up study in Beijing. PLoS One 8(9):e75260.
Hammond, V., A. I. Reeder, and A. Gray. 2009. Patterns of real-time occupational ultraviolet radiation exposure among a sample of outdoor workers in New Zealand. Public Health 123(2):182–187.
Hartmann, E. E., G. E. Bradford, P. K. Chaplin, T. Johnson, A. R. Kemper, S. Kim, and W. Marsh-Tootle. 2006. Project universal preschool vision screening: A demonstration project. Pediatrics 117(2):e226–e237.
Haun, J. N., N. R. Patel, D. D. French, R. R. Campbell, D. D. Bradham, and W. A. Lapcevic. 2015. Association between health literacy and medical care costs in an integrated healthcare system: A regional population based study. BMC Health Services Research 15(1):1–11.
Hautala, N., P. Hyytinen, V. Saarela, P. Hagg, A. Kurikka, M. Runtti, and A. Tuulonen. 2009. A mobile eye unit for screening of diabetic retinopathy and follow-up of glaucoma in remote locations in northern Finland. Acta Ophthalmologica 87(8):912–913.
Healthcare.gov. 2016. Preventive health services. https://www.healthcare.gov/coverage/preventive-care-benefits (accessed May 18, 2016).
Hearne, S., B. C. Castrucci, J. P. Leider, E. K. Rhoades, P. Russo, and V. Bass. 2015. The future of urban health: Needs, barriers, opportunities, and policy advancement at large urban health departments. Journal of Public Health Management and Practice 21(Suppl 1):S4–S13.
Hered, R. W., and D. L. Wood. 2013. Preschool vision screening in primary care pediatric practice. Public Health Reports 128(3):189–197.
Hershey, J. C., J. Niederdeppe, W. D. Evans, J. Nonnemaker, S. Blahut, D. Holden, P. Messeri, and M. L. Haviland. 2005. The theory of “truth”: How counterindustry campaigns affect smoking behavior among teens. Health Psychology 24(1):22–31.
HHS (U.S. Department of Health and Human Services). 2010a. Multiple chronic conditions—A strategic framework: Optimum health and quality of life for individuals with multiple chronic conditions. Washington, DC: HHS.
———. 2010b. National action plan to improve health literacy. Washington, DC: HHS.
Himmelman, A. 2002. Collaboration for a change: Definitions, descision-making models, roles, and collaboration process guide. Minneapolis, MN: Himmelman Consulting.
Honoré, P. A., and T. Schlechte. 2007. State public health agency expenditures: Categorizing and comparing to performance levels. Journal of Public Health Management and Practice 13(2):156–162.
HRSA (Health Resources and Services Administration). n.d. Vision screening. http://www.mchb.hrsa.gov/programs/visionscreening/index.html (accessed July 7, 2016).
Hughes, R., K. Ramdhanie, T. Wassermann, and C. Moscetti. 2011. State boards of health: Governance and politics. The Journal of Law, Medicine & Ethics 39:37–41.
Hwang, T., and J. T. Kim. 2011. Effects of indoor lighting on occupants’ visual comfort and eye health in a green building. Indoor and Built Environment 20(1):75–90.
Imrie, R., and M. Kumar. 1998. Focusing on disability and access in the built environment. Disability & Society 13(3):357–374.
IOM (Institute of Medicine). 1988. The future of public health. Washington, DC: National Academy Press.
———. 2003. The future of the public’s health in the 21st century. Washington, DC: The National Academies Press.
———. 2004. Health literacy: A prescription to end confusion. Washington, DC: The National Academies Press.
———. 2011a. Early childhood obesity prevention policies. Washington, DC: The National Academies Press.
———. 2011b. For the public’s health: Revitalizing law and policy to meet new challenges. Washington, DC: The National Academies Press.
———. 2011c. For the public’s health: The role of measurement in action and accountability. Washington, DC: The National Academies Press.
———. 2012a. For the public’s health: Investing in a healthier future. Washington, DC: The National Academies Press.
———. 2012b. An integrated framework for assessing the value of community-based prevention. Washington, DC: The National Academies Press.
———. 2012. Epilepsy across the spectrum: Promoting health and understanding. Washington, DC: The National Academies Press.
———. 2015. Strategies to improve cardiac arrest survival: A time to act. Washington, DC: The National Academies Press.
Jacobson, P. D., J. Wasserman, H. W. Wu, and J. R. Lauer. 2015. Assessing enrepreneurship in governmental public health. American Journal of Public Health 105(S2):S318–S322.
Jaggernath, J., L. Verland, P. Ramson, V. Kovai, V. F. Chan, and K. S. Naidoo. 2014. Poverty and eye health. Health 6(14):1849–1860.
Jones, H. L., E. A. Walker, C. B. Schechter, and E. Blanco. 2010. Vision is precious: A successful behavioral intervention to increase the rate of screening for diabetic retinopathy for inner-city adults. Diabetes Educator 36(1):118–126.
Juzych, M. S., S. Randhawa, A. Shukairy, P. Kaushal, A. Gupta, and N. Shalauta. 2008. Functional health literacy in patients with glaucoma in urban settings. Archives of Ophthalmology 126(5):718–724.
Kaiser Family Foundation. 2013. Medicaid: A primer. Menlo Park, CA: The Henry J. Kaiser Family Foundation.
Keay, L., F. Stapleton, and O. Schein. 2007. Epidemiology of contact lens-related inflammation and microbial keratitis: A 20-year perspective. Eye & Contact Lens 33(6 Pt 2):346–353, discussion 362–363.
Kemper, A. R., A. Helfrich, J. Talbot, N. Patel, and J. E. Crews. 2011. Improving the rate of preschool vision screening: An interrupted time-series analysis. Pediatrics 128(5):e1279–e1284.
Kemper, A. R., A. Helfrich, J. Talbot, and N. Patel. 2012. Outcomes of an elementary school-based vision screening program in North Carolina. Journal of School Nursing 28(1):24–30.
Kennedy, R. D., M. M. Spafford, C. M. Parkinson, and G. T. Fong. 2011. Knowledge about the relationship between smoking and blindness in Canada, the United States, the United Kingdom, and Australia: Results from the International Tobacco Control Four-Country Project. Optometry 82(5):310–317.
Khan, J. C., D. A. Thurlby, H. Shahid, D. G. Clayton, J. R. Yates, M. Bradley, A. T. Moore, and A. C. Bird. 2006. Smoking and age related macular degeneration: The number of pack years of cigarette smoking is a major determinant of risk for both geographic atrophy and choroidal neovascularisation. British Journal of Ophthalmology 90(1):75–80.
Kim, S. S., S. H. Kim, H. Fang, S. Kwon, D. Shelley, and D. Ziedonis. 2015. A culturally adapted smoking cessation intervention for Korean Americans: A mediating effect of perceived family norm toward quitting. Journal of Immigrant and Minority Health 17(4):1120–1129.
Kindig, D., and G. Stoddart. 2003. What is population health? American Journal of Public Health 93(3):380–383.
Klein, R., K. J. Cruickshanks, S. D. Nash, E. M. Krantz, F. J. Nieto, G. H. Huang, J. S. Pankow, and B. E. K. Klein. 2010. The prevalence of age-related macular degeneration and associated risk factors: The Beaver Dam Offspring Study. Archives of Ophthalmology 128(6):750–758.
Kleinstein, R. N., L. A. Jones, S. Hullett, S. Kwon, R. J. Friedman, R. E. Manny, D. O. Mutti, J. A. Yu, K. Zudnik, and Collaborative Longitudinal Evaluation of Ethnicity and Refractive Error Study Group. 2003. Refractive error and ethnicity in children. Archives of Ophthalmology 121(8):1141–1147.
Kodjebacheva, G., E. R. Brown, L. Estrada, F. Yu, and A. L. Coleman. 2011. Uncorrected refractive error among first-grade students of different racial/ethnic groups in Southern California: Results a year after school-mandated vision screening. Journal of Public Health Management and Practice 17(6):499–505.
Koh, H. K., L. J. Elqura, C. M. Judge, and M. A. Stoto. 2008. Regionalization of local public health systems in the era of preparedness. Annual Reviews of Public Health 29:205–218.
Koh, H. K., C. Brach, L. M. Harris, and M. L. Parchman. 2013. A proposed “health literate care model” would constitute a systems approach to improving patients’ engagement in care. Health Affairs (Millwood) 32(2):357–367.
Koivusalo, M. 2010. The state of health in all policies (HIAP) in the European Union: Potential and pitfalls. Journal of Epidemiology and Community Health 64(6):500–503.
Konkle, K. M. 2009. Exploring shared services collaboration in Wisconsin local public health agencies: A review of the literature. Madison: Institute for Wisconsin’s Health Inc.
Korchak, M. E., R. U. Glazier, R. S. Slack, M. W. Plankey, and H. R. Mayer. 2012. Protective eyewear use as depicted in children’s television programs. Journal of Pediatric Ophthalmology and Strabismus 50(2):118–123.
Korda, H., and Z. Itani. 2013. Harnessing social media for health promotion and behavior change. Health Promotion Practice 14(1):15–23.
Krusen, N. 2010. Home lighting: Understanding what, where and how much. OT Practice 15(19):8–9.
Krutmann, J., F. Behar-Cohen, G. Baillet, T. de Ayguavives, P. Ortega Garcia, P. Pena-Garcia, C. Reme, and J. Wolffsohn. 2014. Towards standardization of UV eye protection: What can be learned from photodermatology? Photodermatology, Photoimmunology, & Photo-medicine 30(2–3):128–136.
Kulp, M. T., E. Ciner, M. Maguire, B. Moore, J. Pentimonti, M. Pistilli, L. Cyert, T. R. Candy, G. Quinn, G. S., Ying, for the VIP HIP Study Group. Uncorrected hyperopia and preschool early literacy: Results of the Vision in Preschoolers-Hyperopia in Preschoolers (VIP-HIP) Study. Ophthalmology 123(4):681–689.
Kuzman, T., M. B. Kutija, S. Masnec, S. Jandrokovic, D. Mrazovac, D. Jurisic, I. Skegro, M. Kalauz, and R. Kordic. 2014. Compliance among soft contact lens wearers. Collegium Antropologicum 38(4):1217–1221.
Kyle, J. W., J. K. Hammitt, H. W. Lim, A. C. Geller, L. H. Hall-Jordan, E. W. Maibach, E. C. De Fabo, and M. C. Wagner. 2008. Economic evaluation of the US Environmental Protection Agency’s SunWise Program: Sun protection education for young children. Pediatrics 121(5):e1074–e1084.
Lam, N., and S. J. Leat. 2015. Reprint of: Barriers to accessing low-vision care: The patient’s perspective. Canadian Journal of Ophthalmology 50(Suppl 1):S34–S39.
Lancaster, K., C. E. Hughes, B. Spicer, F. Matthew-Simmons, and P. Dillon. 2011. Illicit drugs and the media: Models of media effects for use in drug policy research. Drug and Alcohol Review 30(4):397–402.
Lang, D., R. Leman, A. W. Arnold, and R. W. Arnold. 2007. Validated portable pediatric vision screening in the Alaska bush. A VIPS-like study in the Koyukon. Alaska Medicine 49(1):2–15.
Leahy, E., and M. Fallon. 2005. Boards of health: Extinction or evolution? Transformations in Public Health 6(3):1–4.
Lechanteur, Y. T., P. L. van de Camp, D. Smailhodzic, J. P. van de Ven, G. H. Buitendijk, C. C. Klaver, J. M. Groenewoud, A. I. den Hollander, C. B. Hoyng, and B. J. Klevering. 2015. Association of smoking and CFH and ARMS2 risk variants with younger age at onset of neovascular age-related macular degeneration. JAMA Ophthalmology 133(5):533–541.
Lee, S., S. J. Song, and H. G. Yu. 2013a. Current smoking is associated with a poor visual acuity improvement after intravitreal ranibizumab therapy in patients with exudative age-related macular degeneration. Journal of Korean Medical Science 28(5):769–774.
Lee, S. M., J. Landry, P. M. Jones, O. Buhrmann, and P. Morley-Forster. 2013b. The effectiveness of a perioperative smoking cessation program: A randomized clinical trial. Anesthesia & Analgesia 117(3):605–613.
Lefebvre, R. C., and A. S. Bornkessel. 2013. Digital social networks and health. Circulation 127(17):1829–1836.
Liang, X. Y., L. J. Chen, T. K. Ng, J. Tuo, J. L. Gao, P. O. Tam, T. Y. Lai, C. C. Chan, and C. P. Pang. 2014. FPR1 interacts with CFH, HTRA1 and smoking in exudative age-related macular degeneration and polypoidal choroidal vasculopathy. Eye (London) 28(12):1502–1510.
Libbey, P., and B. Miyahara. 2011. Cross-jurisdictional relationship in local public health: Preliminary summary of an environmental scan. Princeton, NJ: Robert Wood Johnson Foundation.
Lin, P. R., Z. W. Zhao, K. K. Cheng, and T. H. Lam. 2013. The effect of physician’s 30 s smoking cessation intervention for male medical outpatients: A pilot randomized controlled trial. Journal of Public Health (Oxford) 35(3):375–383.
Lindblad, B. E., N. Håkansson, H. Svensson, B. Philipson, and A. Wolk. 2005. Intensity of smoking and smoking cessation in relation to risk of cataract extraction: A prospective study of women. American Journal of Epidemiology 162(1):73–79.
Lindblad, B. E., N. Håkansson, and A. Wolk. 2014. Smoking cessation and the risk of cataract: A prospective cohort study of cataract extraction among men. JAMA Ophthalmology 132(3):253–257.
Lions Club. 2016. Lions eye health program. http://members.lionsclubs.org/EN/serve/sight/eye-health (accessed July 10, 2016).
Livingston, P. M., C. A. McCarty, and H. R. Taylor. 1998. Knowledge, attitudes, and self care practices associated with age related eye disease in Australia. British Journal of Ophthalmology 82(7):780–785.
Lombardi, D. A., S. K. Verma, M. J. Brennan, and M. J. Perry. 2009. Factors influencing worker use of personal protective eyewear. Accident Analysis & Prevention 41(4):755–762.
Loo, D. L., D. H. Ng, W. Tang, and K. G. Au Eong. 2009. Raising awareness of blindness as another smoking-related condition: A public health role for optometrists? Clinical and Experimental Optometry 92(1):42–44.
Lopez, W., and T. R. Frieden. 2007. Legal counsel to public health practitioners. In Law in public health practice, edited by R. A. Goodman, R. E. Hoffman, W. Lopez, G. W. Matthews, M. A. Rothstein and K. L. Foster. New York: Oxford University Press.
Mancini, G., A. Baldasseroni, G. Laffi, S. Curti, S. Mattioli, and F. S. Violante. 2005. Prevention of work related eye injuries: Long term assessment of the effectiveness of a multicomponent intervention among metal workers. Occupational and Environmental Medicine 62(12):830–835.
Marshall, E. C., R. E. Meetz, and L. L. Harmon. 2010. Through our children’s eyes—The public health impact of the vision screening requirements for Indiana school children. Optometry 81(2):71–82.
Matter, K. C., S. A. Sinclair, and H. Xiang. 2007. Use of protective eyewear in U.S. children: Results from the National Health Interview Survey. Ophthalmic Epidemiology 14(1):37–43.
Mays, G. P., M. C. McHugh, K. Shim, N. Perry, D. Lenaway, P. K. Halverson, and R. Moonesinghe. 2006. Institutional and economic determinants of public health system performance. American Journal of Public Health 96(3):523–531.
McCombs, M., and D. Shaw. 1972. The agenda-setting function of mass media. Public Opinion Quarterly 36(2):176–187.
McGwin, G., R. Khoury, J. Cross, and C. Owsley. 2010. Vision impairment and eye care utilization among Americans 50 and older. Current Eye Research 35(6):451–458.
McNaughton, C. D., C. Cawthon, S. Kripalani, D. Liu, A. B. Storrow, and C. L. Roumie. 2015. Health literacy and mortality: A cohort study of patients hospitalized for acute heart failure. Journal of the American Heart Association 4(5).
MDHHS (Michigan Department of Health and Human Services). 2016a. Vision screening. http://www.michigan.gov/mdhhs/0,5885,7–339-73971_4911_4912_6238_76134---,00.html (accessed May 18, 2016).
———. 2016b. Vision screening and reporting for kindergarten. https://www.mcir.org/wpcontent/uploads/2014/09/SS_Vision.pdf (accessed May 18, 2016).
Medicaid. 2016a. Benefits. https://www.medicaid.gov/medicaid-chip-program-information/by-topics/benefits/medicaid-benefits.html (accessed October 20, 2015).
———. 2016b. Eligibility. https://www.medicaid.gov/medicaid-chip-program-information/bytopics/eligibility/eligibility.html (accessed October 20, 2015).
Mello, M. M., J. Pomeranz, and P. Moran. 2008. The interplay of public health law and industry self-regulation: The case of sugar-sweetened bevarage sales in schools. American Journal of Public Health 98(4):595–604.
Moorhead, S. A., D. E. Hazlett, L. Harrison, J. K. Carroll, A. Irwin, and C. Hoving. 2013. A new dimension of health care: Systematic review of the uses, benefits, and limitations of social media for health communication. Journal of Medical Internet Research 15(4):e85.
Muir, K. W., C. Santiago-Turla, S. S. Stinnett, L. W. Herndon, R. R. Allingham, P. Challa, and P. P. Lee. 2006. Health literacy and adherence to glaucoma therapy. American Journal of Ophthalmology 142(2):223–226.
Muir, K. W., L. Christensen, and H. B. Bosworth. 2013. Health literacy and glaucoma. Current Opinion in Ophthalmology 24(2):119–124.
Müller, A., J. E. Keeffe, and H. R. Taylor. 2007. Changes in eye care utilization following an eye health promotion campaign. Clinical & Experimental Ophthalmology 35(4):305–309.
Mussener, U., M. Bendtsen, N. Karlsson, I. R. White, J. McCambridge, and P. Bendtsen. 2016. Effectiveness of short message service text-based smoking cessation intervention among university students: A randomized clinical trial. JAMA Internal Medicine 176(3):321–328.
Myers, C. E., B. E. K. Klein, R. Gangnon, T. A. Sivakumaran, S. K. Iyengar, and R. Klein. 2014. Cigarette smoking and the natural history of age-related macular degeneration: The Beaver Dam Eye Study. Ophthalmology 121(10):1949–1955.
NACCHO (National Association of County and City Health Officials). 1998. NACCHO survey examines state/local health department relationships. Washington, DC: NACCHO.
———. 2009a. 2008 national profile of local health departments. Washington, DC: NACCHO.
———. 2009b. The local health department workforce: Findings from the 2008 national profile of local health departments. Washington, DC: NACCHO.
———. 2011. Local health department job losses and program cuts: Findings from January 2011 survey and 2010 national profile study. Washington, DC: NACCHO.
———. 2016. Tip sheet: Prioritizing issues in a community health improvement process. Washington, DC: NACCHO. http://archived.naccho.org/topics/infrastructure/CHAIP/upload/Final-Issue-Prioritization-Resource-Sheet.pdf (accessed August 15, 2015).
NACDD (National Association of Chronic Disease Directors). 2004. Vision problems in the United States: Recommendations for a state public health response. Chicago, IL: Prevent Blindness.
———. 2016. Vision and eye health initiative funding opportunity announcement (FOA #VIi2015a). http://c.ymcdn.com/sites/www.chronicdisease.org/resource/resmgr/Healthy_Aging/RFA_for_Vision_and_Eye_Healt.pdf (accessed November 29, 2016).
———. n.d. About NACDD. http://www.chronicdisease.org/?page=AboutUs (accessed April 5, 2016).
Naron, S., and M. Mendes. 2016. Baltimore City announces new citywide initiative to provide free universal vision screening and glasses to students. Baltimore, MD: City of Baltimore.
NASEM (The National Academies of Sciences, Engineering, and Medicine). 2016. Hearing health care for adults: Priorities for improving access and affordability. Washington, DC: The National Academies Press.
National Center for Appropriate Technology. 2014. Partnership for sustainable communities: Five years of learning from communities and coordinating federal investments. https://www.sustainablecommunities.gov/sites/sustainablecommunities.gov/files/docs/partnership-accomplishments-report-2014-reduced-size.pdf (accessed July 22, 2016).
The National Council for Public-Private Partnerships. 2016. 7 keys to success. http://www.ncppp.org/ppp-basics/7-keys (accessed April 6, 2016).
NEHEP (National Eye Health Education Program). 2011. National Eye Health Education Progam five-year agenda 2012–2017. Bethesda, MD: National Eye Institute.
———. 2014. Diabetes focus group findings. Bethesda, MD: National Eye Institute.
———. n.d. Glaucoma awareness month. https://nei.nih.gov/nehep/gam (accessed July 10, 2016).
NEI/LCIF (National Eye Institute/Lions Club International Foundation). 2008. 2005 survey of public knowledge, attitudes, and practices related to eye health and disease. https://nei.nih.gov/sites/default/files/nei-pdfs/2005KAPFinalRpt.pdf (accessed April 6, 2016).
NEI/NIH (National Eye Institute/National Institutes of Health). 2015a. Eye health tips. https://nei.nih.gov/healthyeyes/eyehealthtips (accessed April 6, 2016).
———. 2015b. Finding the right eye protection. https://nei.nih.gov/sports/findingprotection (accessed September 23, 2015).
———. 2015c. National Eye Health Education Program (NEHEP). https://nei.nih.gov/nehep/about (accessed June 12, 2016).
———. 2015d. NEI’s research progress. https://nei.nih.gov/about/mission (accessed April 6, 2016).
———. 2016. Budget and Congress. https://nei.nih.gov/news/congress (accessed April 7, 2016).
Neiger, B. L., R. Thackeray, S. H. Burton, C. G. Giraud-Carrier, and M. C. Fagen. 2012. Evaluating social media’s capacity to develop engaged audiences in health promotion settings: Use of Twitter metrics as a case study. Health Promotion Practice 14(2):157–162.
Neuner, B., A. Komm, J. Wellmann, M. Dietzel, D. Pauleikhoff, J. Walter, M. Busch, and H. W. Hense. 2009. Smoking history and the incidence of age-related macular degeneration—results from the Muenster Aging and Retina Study (MARS) cohort and systematic review and meta-analysis of observational longitudinal studies. Addictive Behaviors 34(11):938–947.
New Eyes. n.d. U.S. voucher program. http://www.new-eyes.org/us-voucher-program-1 (accessed July 11, 2016).
NIBS (National Institute of Building Sciences). 2015. Design guidelines for the visual environment. Washington, DC: NIBS.
Nicola, R. M. 2005. Boards of health give citizens a voice. Transformations in Public Health 5(3):2–7.
Niederdeppe, J., M. C. Farrelly, and M. L. Haviland. 2004. Confirming “truth”: More evidence of a successful tobacco countermarketing campaign in Florida. American Journal of Public Health 94(2):255–257.
Nishtar, S. 2004. Public–private “partnerships” in health—A global call to action. Health Research Policy and Systems 2:5–5.
Noertjojo, K., D. Maberley, K. Bassett, and P. Courtright. 2006. Awareness of eye diseases and risk factors: Identifying needs for health education and promotion in Canada. Canadian Journal of Ophthalmology 41(5):617–623.
Novick, L. F., G. P. Mays, and G. Benjamin. 2005. Public health administration: Principles for population-based management. Burlington, MA: Jones and Bartlett.
NRC (National Research Council). 2011. Improving health in the United States: The role of health impact assessment. Washington, DC: The National Academies Press.
NYSDOH (New York State Department of Health). 2009. Graphic ad campaign warns smokers of stroke and eye damage from cigarettes: TV, radio, internet ads promote free NYS quitline services to kick addiction. Albany: NYSDOH.
ODPHP (Office of Disease Prevention and Health Promotion). 2010. Health communication and social marketing: Health communication campaigns that include mass media and health-related product distribution (community guide recommendation). https://www.healthypeople.gov/2020/tools-resources/evidence-based-resource/health-communication-and-social-marketing-health-0 (accessed April 6, 2016).
———. 2016a. Health literate care model. http://health.gov/communication/interactiveHLCM/resources.asp (accessed June 1, 2016).
———. 2016b. Immunization and infectious diseases. https://www.healthypeople.gov/2020/topics-objectives/topic/immunization-and-infectious-diseases/objectives (accessed April 6, 2016).
———. 2016c. Social determinants of health. https://www.healthypeople.gov/2020/topicsobjectives/topic/social-determinants-of-health (accessed April 13, 2016).
———. 2016d. Social determinants of health: Objectives. https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-of-health/objectives (accessed April 13, 2016).
———. 2016e. Vision. https://www.healthypeople.gov/2020/topics-objectives/topic/vision/objectives (accessed April 6, 2016).
———. 2016f. Vision interventions & resources. https://www.healthypeople.gov/2020/topicsobjectives/topic/vision/ebrs (accessed April 6, 2016).
Omana-Cepeda, C., E. Jane-Salas, A. Estrugo-Devesa, E. Chimenos-Kustner, and J. Lopez-Lopez. 2016. Effectiveness of dentist’s intervention in smoking cessation: A review. Journal of Clinical and Experimental Dentistry 8(1):e78–e83.
OneSight. 2016. FAQs. https://onesight.org/faqs (accessed July 11, 2016).
Opstelten, W., and M. J. W. Zaal. 2005. Managing ophthalmic herpes zoster in primary care. British Medical Journal 331(7509):147–151.
OSHA (Occupational Safety and Health Administration). 2003. Eye and face protection. https://www.osha.gov/Publications/osha3151.html#eyeandface (accessed April 6, 2016).
———. 2009. Regulations (Standards—29 CFR): Table of contents. https://www.osha.gov/pls/oshaweb/owadisp.show_document?p_table=STANDARDS&p_id=9778 (accessed April 6, 2016).
———. 2016. Eye and face protection eTool. https://www.osha.gov/SLTC/etools/eyeandface/employer/requirements.html (accessed April 6, 2016).
Oto, M. A., O. Ergene, L. Tokgozoglu, Z. Ongen, O. Kozan, M. Sahin, M. K. Erol, T. Tezel, and M. Ozkan. 2011. Impact of a mass media campaign to increase public awareness of hypertension. Turk Kardiyoloji Dernegi Ars 39(5):355–364.
Papadakis, S., P. W. McDonald, A. L. Pipe, S. T. Letherdale, R. D. Reid, and K. S. Brown. 2013. Effectiveness of telephone-based follow-up support delivered in combination with a multi-component smoking cessation intervention in family practice: A cluster-randomized trial. Preventive Medicine 56(6):390–397.
Parssinen, O., M. Kauppinen, and A. Viljanen. 2014. The progression of myopia from its onset at age 8–12 to adulthood and the influence of heredity and external factors on myopic progression: A 23-year follow-up study. Acta Ophthalmologica 92(8):730–739.
Paul, S., and Y. Liu. 2012. Inadequate light levels and their effect on falls and daily activities of community dwelling older adults: A review of literature. New Zealand Journal of Occupational Therapy 59(2):39–42.
PBA/NACDD (Prevent Blindness America/National Association of Chronic Disease Directors). 2005. A plan for the development of state based vision preservation programs: Summary of a retreat on public health vision preservation. Rensselaerville, NY: National Association of Chronic Disease Directors.
Pedersen, E. R., N. K. Eberhart, K. M. Williams, T. Tanielian, C. Epley, and D. M. Scharf. 2015. Public–private partnerships for providing behavioral health care to veterans and their families: What do we know, what do we need to learn, and what do we need to do? Santa Monica, CA: RAND Corporation.
Perdue, W. C., L. A. Stone, and L. O. Gostin. 2003. The built environment and its relationship to the public’s health: The legal framework. American Journal of Public Health 93(9):1390–1394.
PHAB (Public Health Accreditation Board). 2013. Getting started. http://www.phaboard.org/accreditation-overview/getting-started (accessed April 11, 2016).
———. n.d. What is public health accreditation. http://www.phaboard.org/accreditationoverview/what-is-accreditation (accessed July 15, 2016).
Phildelphia Eagles. 2016. Eagles charitable foundation: Vision care. http://www.philadelphiaeagles.com/community/org-vision.html (accessed July 11, 2016).
Prevent Blindness. 2012. The vision connection: Integrating vision into state health programs. Chicago, IL: Prevent Blindness America.
———. 2016a. Eye safety at work. http://www.preventblindness.org/eye-safety-work (accessed April 6, 2016).
———. 2016b. Prevent Blindness eye health and safety observance calendar. http://www.preventblindness.org/prevent-blindness-eye-health-and-safety-observance-calendar (accessed July 10, 2016).
———. 2016c. Preventing eye injuries. http://www.preventblindness.org/preventing-eye-injuries (accessed April 6, 2016).
Radford, C. F., D. Minassian, J. K. Dart, F. Stapleton, and S. Verma. 2009. Risk factors for nonulcerative contact lens complications in an ophthalmic accident and emergency department: A case-control study. Ophthalmology 116(3):385–392.
Rahi, J. S., P. M. Cumberland, and C. S. Peckham. 2009. Visual function in working-age adults: Early life influences and associations with health and social outcomes. Ophthalmology 116(10):1866–1871.
Ramirez, L. B., E. Baker, and M. Metzler. 2008. Promoting health equity: A resource to help communities address social determinants of health. Atlanta, GA: CDC.
Ranasinghe, P., W. S. Wathurapatha, Y. S. Perera, D. A. Lamabadusuriya, S. Kulatunga, N. Jayawardana, and P. Katulanda. 2016. Computer vision syndrome among computer office workers in a developing country: An evaluation of prevalence and risk factors. BMC Research Notes 9(1):150.
Rao, G. 2015. The Barrie Jones lecture—Eye care for the neglected population: Challenges and solutions. Eye 29(1):30–45.
Rein, D. B. 2013. Vision problems are a leading source of modifiable health expenditures. Investigative Ophthalmology & Visual Science 54(14):ORSF18–ORSF22.
Rey-Lopez, J. P., G. Vicente-Rodriguez, M. Biosca, and L. A. Moreno. 2008. Sedentary behaviour and obesity development in children and adolescents. Nutrition, Metabolism and Cardiovascular Diseases 18(3):242–251.
Reynaers, A.-M. 2014. Public values in public–private partnerships. Public Administration Review 74(1):41–50.
Robertson, D. M., and H. D. Cavanagh. 2011. Non-compliance with contact lens wear and care practices: A comparative analysis. Optometry & Vision Science 88(12):1402–1408.
Rose, K. A., I. G. Morgan, J. Ip, A. Kifley, S. Huynh, W. Smith, and P. Mitchell. 2008. Outdoor activity reduces the prevalence of myopia in children. Ophthalmology 115(8):1279–1285.
Rosenfield, M. 2011. Computer vision syndrome: A review of ocular causes and potential treatments. Ophthalmic and Physiologic Optics 31(5):502–515.
Rubin, D. B., S. R. Singh, and G. J. Young. 2015. Tax-exempt hospitals and community benefit: New directions in policy and practice. Annual Review of Public Health 36(1):545–557.
RWJF (Robert Wood Johnson Foundation). 2014. Building a culture of health. Princeton, NJ: RWJF.
Salinsky, E. 2010. Governmental public health: An overview of state and local public health agencies. Washington, DC: National Health Policy Forum.
Sarna, L. P., S. A. Bialous, E. Kralikova, A. Kmetova, V. Felbrova, S. Kulovana, K. Mala, E. Roubickova, M. J. Wells, and J. K. Brook. 2014. Impact of a smoking cessation educational program on nurses’ interventions. Journal of Nursing Scholarship 46(5):314–321.
SATH (Society for Accessible Travel & Hospitality). 2013. How to travel with a sight impairment or blindness. http://sath.org/how-to-travel-with-a-sight-impairment-or-blindness (accessed April 7, 2016).
Sawyer, J., and M. L. Kaup. 2014. Lighting, vision, and aging in place: The impact of living with low vision in independent living facilities. Undergraduate Research Journal for the Human Sciences 13.
Schaumberg, D. A., S. E. Hankinson, Q. Guo, E. Rimm, and D. J. Hunter. 2007. A prospective study of 2 major age-related macular degeneration susceptibility alleles and interactions with modifiable risk factors. Archives of Ophthalmology 125(1):55–62.
Schmidt, S., M. A. Hauser, W. K. Scott, E. A. Postel, A. Agarwal, P. Gallins, F. Wong, Y. S. Chen, K. Spencer, N. Schnetz-Boutaud, J. L. Haines, and M. A. Pericak-Vance. 2006. Cigarette smoking strongly modifies the association of LOC387715 and age-related macular degeneration. American Journal of Human Genetics 78(5):852–864.
Scott, A. W., N. M. Bressler, S. Ffolkes, J. S. Wittenborn, J. Jorkavsky. 2016. Public attitudes about eye and vision health. JAMA Ophthalmology 134(10):1111–1118.
Sengupta, S., A. M. Nguyen, S. W. van Landingham, S. D. Solomon, D. V. Do, L. Ferrucci, D. S. Friedman, and P. Y. Ramulu. 2015. Evaluation of real-world mobility in age-related macular degeneration. BMC Ophthalmology 15(1):1–11.
Sentell, T., K. L. Braun, J. Davis, and T. Davis. 2015. Health literacy and meeting breast and cervical cancer screening guidelines among Asians and Whites in California. SpringerPlus 4:432.
Shah, A., K. Blackhall, K. Ker, and D. Patel. 2009. Educational interventions for the prevention of eye injuries. Cochrane Database of Systematic Reviews (4):Cd006527.
Sheedy, J. E., J. N. Hayes, and J. Engle. 2003. Is all asthenopia the same? Optometry & Vision Science 80(11):732–739.
Sheppler, C. R., W. E. Lambert, S. K. Gardiner, T. M. Becker, and S. L. Mansberger. 2014. Predicting adherence to diabetic eye examinations: Development of the compliance with annual diabetic eye exams survey. Ophthalmology 121(6):1212–1219.
Shih, S. T., R. Carter, C. Sinclair, C. Mihalopoulos, and T. Vos. 2009. Economic evaluation of skin cancer prevention in Australia. Preventive Medicine 49(5):449–453.
Shin, P., and B. Finnegan. 2009. Assessing the need for on-site eye care professionals in community health centers. George Washington University Center for Health Services Research and Policy 1–23.
Simpson, S. A., and J. M. Nonnemaker. 2013. New York tobacco control program cessation assistance: Costs, benefits, and effectiveness. International Journal of Environmental Research and Public Health 10(3):1037–1047.
Singh, S., D. Satani, A. Patel, and R. Vhankade. 2012. Colored cosmetic contact lenses: An unsafe trend in the younger generation. Cornea 31(7):777–779.
Sliney, D. H. 2001. Photoprotection of the eye—UV radiation and sunglasses. Journal of Photochemistry and Photobiology B 64(2–3):166–175.
Sloan, F. A., G. Picone, D. S. Brown, and P. P. Lee. 2005. Longitudinal analysis of the relationship between regular eye examinations and changes in visual and functional status. Journal of the American Geriatrics Society 53(11):1867–1874.
Slonim, A. B., C. Callaghan, L. Daily, B. A. Leonard, F. C. Wheeler, C. W. Gollmar, and W. F. Young. 2007. Recommendations for integration of chronic disease programs: Are your programs linked? Preventing Chronic Disease 4(2):A34.
Smith, K. E., C. Bambra, K. E. Joyce, N. Perkins, D. J. Hunter, and E. A. Blenkinsopp. 2009. Partners in health? A systematic review of the impact of organizational partnerships on public health outcomes in England between 1997 and 2008. Journal of Public Health 31(2):210–221.
Spellman, F. R., and R. M. Bieber. 2012. Environmental health and science desk reference. Lanham, MD: Government Institutes.
Spinweber, E., and A. Honeysett. 2013. Partnership for a healthier America and Channel One News to bring healthy messages into the classroom. Washington, DC: Channel One News.
Stanczyk, N. E., E. S. Smit, D. N. Schulz, H. de Vries, C. Bolman, J. W. Muris, and S. M. Evers. 2014. An economic evaluation of a video- and text-based computer-tailored intervention for smoking cessation: A cost-effectiveness and cost-utility analysis of a randomized controlled trial. PLoS ONE 9(10):e110117.
Stapleton, F., L. Keay, K. Edwards, T. Naduvilath, J. K. Dart, G. Brian, and B. A. Holden. 2008. The incidence of contact lens–related microbial keratitis in australia. Ophthalmology 115(10):1655–1662.
Stapleton, F., K. Edwards, L. Keay, T. Naduvilath, J. K. Dart, G. Brian, and B. Holden. 2012. Risk factors for moderate and severe microbial keratitis in daily wear contact lens users. Ophthalmology 119(8):1516–1521.
State of Michigan. 2016. Michigan’s public health hearing & vision screening programs: Information for healthcare providers. https://www.michigan.gov/documents/mdch/physicans_flyer_361187_7.pdf (accessed June 10, 2016).
Steinemann, T. L., M. Fletcher, A. E. Bonny, R. A. Harvey, D. Hamlin, P. Zloty, M. Besson, K. Walter, and M. Gagnon. 2005. Over-the-counter decorative contact lenses: Cosmetic or medical devices? A case series. Eye & Contact Lens 31(5):194–200.
Stoto, M. A., and L. Morse. 2008. Regionalization in local public health systems: Public health preparedness in the Washington Metropolitan area. Public Health Reports 123(4):461–473.
Sundling, V., P. Gulbrandsen, J. Jervell, and J. Straand. 2008. Care of vision and ocular health in diabetic members of a national diabetes organization: A cross-sectional study. BMC Health Services Research 8(1):1–8.
Szczotka-Flynn, L. B., E. Pearlman, and M. Ghannoum. 2010. Microbial contamination of contact lenses, lens care solutions, and their accessories: A literature review. Eye & Contact Lens 36(2):116–129.
Tarczy-Hornoch, K., S. A. Cotter, M. Borchert, R. McKean-Cowdin, J. Lin, G. Wen, J. Kim and R. Varma. 2013. Prevalence and causes of visual impairment in Asian and non-Hispanic white preschool children: Multi-Ethnic Pediatric Eye Disease Study. Ophthalmology 120(6):1220–1226.
TDI (Texas Department of Insurance). 2007. Eye injury prevention factsheet. Austin: TDI.
Thornton, J., R. Edwards, P. Mitchell, R. A. Harrison, I. Buchan, and S. P. Kelly. 2005. Smoking and age-related macular degeneration: A review of association. Eye (London) 19(9):935–944.
Toufeeq, A., and A. J. Oram. 2014. School-entry vision screening in the United Kingdom: Practical aspects and outcomes. Ophthalmic Epidemiology 21(4):210–216.
Tovar-Aguilar, J. A., P. F. Monaghan, C. A. Bryant, A. Esposito, M. Wade, O. Ruiz, and R. J. McDermott. 2014. Improving eye safety in citrus harvest crews through the acceptance of personal protective equipment, community-based participatory research, social marketing, and community health workers. Journal of Agromedicine 19(2):107–116.
U.S. Surgeon General. 2014. The health consequences of smoking—50 years of progress: A report from the Surgeon General. Rockville, MD: U.S. Department of Health and Human Services.
———. 2016. Active living. http://www.surgeongeneral.gov/priorities/prevention/strategy/active-living.html (accessed August 4, 2016).
Varano, M., N. Eter, S. Winyard, K. U. Wittrup-Jensen, R. Navarro, and J. Heraghty. 2015. Current barriers to treatment for wet age-related macular degeneration (WAMD): Findings from the WAMD patient and caregiver survey. Journal of Clinical Ophthalmology 9:2243–2250.
Verma, A., M. R. Schulz, S. A. Quandt, E. N. Robinson, J. G. Grzywacz, H. Chen, and T. A. Arcury. 2011. Eye health and safety among Latino farmworkers. Journal of Agromedicine 16(2):143–152.
VHIPP (Vision Health Integration and Preservation Program). 2012. Centers for Disease Control & Prevention component 2a: Vision integration. Albany, NY: VHIPP.
Vision To Learn. 2016. Annual report 2015. Los Angeles, CA: Vision To Learn.
Vitale, S., L. Ellwein, M. F. Cotch, F. L. Ferris, 3rd, and R. Sperduto. 2008. Prevalence of refractive error in the United States, 1999–2004. Archives of Ophthalmology 126(8):1111–1119.
Vrangbaek, K. 2008. Public–private partnerships in the health sector: The Danish experience. Health Economics, Policy and Law 3(02):141–163.
VSP (Vision Service Plan). 2016. Gift certificates. https://vspglobal.com/cms/vspglobal-outreach/gift-certificates.html (accessed July 11, 2016).
———. n.d. Become a partner. https://vspglobal.com/cms/vspglobal-outreach/giftcertificatesnationalpartner.html (accessed August 31, 2106).
Walker, E. A., C. B. Schechter, A. Caban, and C. E. Basch. 2008. Telephone intervention to promote diabetic retinopathy screening among the urban poor. American Journal of Preventive Medicine 34(3):185–191.
Weintraub, J. M., W. C. Willett, B. Rosner, G. A. Colditz, J. M. Seddon, and S. E. Hankinson. 2002. Smoking cessation and risk of cataract extraction among US women and men. American Journal of Epidemiology 155(1):72–79.
Weiss, D. M., R. J. Casten, B. E. Leiby, L. A. Hark, A. P. Murchison, D. Johnson, S. Stratford, J. Henderer, B. W. Rovner, and J. A. Haller. 2015. Effect of behavioral intervention on dilated fundus examination rates in older African American individuals with diabetes mellitus: A randomized clinical trial. JAMA Ophthalmology 133(9):1005–1012.
Wernham, A., and S. M. Teutsch. 2015. Health in all policies for big cities. Journal of Public Health Management and Practice 21(Suppl 1):S56–S65.
The White House. 2010. First Lady Michelle Obama launches Let’s Move: America’s move to raise a healthier generation of kids. Washington, DC: The White House, Office of the First Lady.
White House Task Force on Childhood Obesity. 2010. Solving the problem of childhood obesity within a generation. Washington, DC: The White House.
Whitson, H. E., and F. R. Lin. 2014. Hearing and vision care for older adults: Sensing a need to update Medicare policy. JAMA 312(17):1739–1740.
Whitson, H. E., S. W. Cousins, B. M. Burchett, C. F. Hybels, C. F. Pieper, and H. J. Cohen. 2007. The combined effect of visual impairment and cognitive impairment on disability in older people. Journal of the American Geriatric Society 55(6):885–891.
WHO (World Health Organization). 1948. Preamble to the Constitution of the World Health Organization as adopted by the International Health Conference, New York, 19–22 June, 1946; signed on 22 July 1946 by the representatives of 61 States. Official Records of the World Health Organization 2:100.
______. n.d.a. Commission on Social Determinants of Health, 2005–2008. http://www.who.int/social_determinants/thecommission/en (accessed August 14, 2016).
______. n.d.b. Health promotion. http://www.who.int/topics/health_promotion/en (accessed August 14, 2016).
Wittenborn, J., and D. Rein. 2016. The potential costs and benefits of treatment for undiagnosed eye disorders. Paper prepared for the Committee on Public Health Approaches to Reduce Vision Impairment and Promote Eye Health. http://www.nationalacademies.org/hmd/~/media/Files/Report%20Files/2016/UndiagnosedEyeDisordersCommissionedPaper.pdf (accessed September 15, 2016).
Wood, J. M., A. Chaparro, P. Lacherez, and L. Hickson. 2012. Useful field of view predicts driving in the presence of distracters. Optometry & Vision Science 89(4):373–381.
Wright, C. Y., A. I. Reeder, G. E. Bodeker, A. Gray, and B. Cox. 2007. Solar UVR exposure, concurrent activities and sun-protective practices among primary schoolchildren. Photochemistry and Photobiology 83(3):749–758.
Wu, Y., L. Tian, and Y. Huang. 2015a. Correlation between the interactions of ABCA4 polymorphisms and smoking with the susceptibility to age-related macular degeneration. International Journal of Clinical and Experimental Pathology 8(6):7403–7408.
Wu, Y. T., M. Willcox, H. Zhu, and F. Stapleton. 2015b. Contact lens hygiene compliance and lens case contamination: A review. Contact Lens Anterior Eye 38(5):307–316.
Yazar, S., A. W. Hewitt, L. J. Black, C. M. McKnight, J. A. Mountain, J. C. Sherwin, W. H. Oddy, M. T. Coroneo, R. M. Lucas, and D. A. Mackey. 2014. Myopia is associated with lower vitamin D status in young adults’ myopia and vitamin D status. Investigative Ophthalmology & Visual Science 55(7):4552–4559.
Yildiz, E. H., S. Airiani, K. M. Hammersmith, C. J. Rapuano, P. R. Laibson, A. S. Virdi, T. Hongyok, and E. J. Cohen. 2012. Trends in contact lens–related corneal ulcers at a tertiary referral center. Cornea 31(10):1097–1102.
Zambelli-Weiner, A., J. E. Crews, and D. S. Friedman. 2012. Disparities in adult vision health in the United States. American Journal of Ophthalmology 154(6 Suppl):S23–S30, e21.
Zhang, X., J. Kahende, A. Z. Fan, L. Barker, T. J. Thompson, A. H. Mokdad, Y. Li, and J. B. Saaddine. 2011. Smoking and visual impairment among older adults with age-related eye diseases. Preventing Chronic Disease 8(4):A84.
Zhang, X., M. F. Cotch, A. Ryskulova, S. A. Primo, P. Nair, C.-F. Chou, L. S. Geiss, L. Barker, A. F. Elliott, J. E. Crews, and J. B. Saaddine. 2012. Vision health disparities in the United States by race/ethnicity, education, and economic status: Findings from two nationally representative surveys. American Journal of Ophthalmology 154(60): S53–S62, e51.
Zhou, J., Y. H. Ma, J. Ma, Z. Y. Zou, X. K. Meng, F. B. Tao, C. Y. Luo, J. Jing, D. H. Pan, J. Y. Luo, X. Zhang, H. Wang, and H. P. Zhao. 2016. Prevalence of myopia and influencing factors among primary and middle school students in 6 provinces of China. Zhonghua Liu Xing Bing Xue Za Zhi 37(1):29–34.
Zohar, Z., I. Waksman, J. Stolero, G. Volpin, E. Sacagiu, and A. Eytan. 2004. Injury from fireworks and firecrackers during holidays. Harefuah 143(10):698–701, 768.
Zuckerman, D. M. 2004. Blind adults in America: Their lives and challenges. Washington, DC: National Research Center for Women & Families.
This page intentionally left blank.
















































































