1
Introduction and Background1
BACKGROUND AND CHARGE TO THE COMMITTEE
Older adults are a growing demographic group in the United States, and a range of physical, social, financial, and cultural factors affect their nutritional status. Metabolic and physiologic changes that accompany normal aging modify the nutritional requirements of older adults. An examination of evidence is needed to better understand how nutritional status is associated with aging and risk of mortality or chronic disease among older adults. Underpinning many, if not most, nutritional problems in older adults is socioeconomic status. Therefore, understanding access challenges to healthy food, including geographic, financial, and transportation barriers, also is needed to better understand how to meet the nutritional needs of older adults.
On October 28-29, 2015, the Food and Nutrition Board convened a workshop, Meeting the Dietary Needs of Older Adults, in Washington, DC. The workshop was designed to examine factors in the physical, social, and cultural environment that affect the ability of older adults to meet their daily dietary needs.
The workshop planning committee highlighted several areas of focus
___________________
1 The planning committee’s role was limited to planning the workshop, and the workshop summary has been prepared by the workshop rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants, and are not necessarily endorsed or verified by the National Academies of Sciences, Engineering, and Medicine, and they should not be construed as reflecting any group consensus.
for the workshop: (1) describe the rapid increase in older adult populations and the need for new paradigms to meet their needs and examine new understandings of the meaning of “healthy aging”; (2) describe emerging insights into the changing physiology of aging and how that affects nutrient needs; (3) describe ecological insights about factors that influence food choices and nutritional status of older adults; (4) review national programs designed to address dietary and nutrition needs of older adults; (5) explore how community, retail, and nonprofit organizations are instituting programs and projects to meet older adults’ nutrition needs; and (6) examine research priorities and gaps. This document summarizes the presentations and discussions from the workshop, focusing on each session and highlighting issues raised by presenters and attendees.
Gordon Jensen, Senior Associate Dean for Research, Professor of Medicine and Nutrition, University of Vermont, and Chair of the Planning Committee on Meeting the Dietary Needs of Older Adults, opened the workshop. Jensen explained that the current workshop was built on two previous initiatives of the Food and Nutrition Board on nutrition and aging, and that he had participated in both initiatives. The first was a January 2000 report titled The Role of Nutrition in Maintaining Health in the Nation’s Elderly: Evaluating Coverage of Nutrition Services for the Medicare Population (IOM, 2000). The report addressed issues related to nutrition interventions for Medicare beneficiaries, provided recommendations for nutrition services for the elderly, and considered how Medicare’s coverage policy should be considered and implemented.
The second initiative was a March 2012 Workshop Summary titled Nutrition and Healthy Aging in the Community (IOM, 2012). The workshop addressed community-based delivery of nutrition services for older adults and identified nutrition interventions and model programs that support the transition to home care as well as healthy and independent living in the community.
PERSPECTIVES FROM THE AARP FOUNDATION
Lisa Marsh Ryerson, President of the AARP Foundation, noted that the AARP Foundation has worked very closely with the National Academies of Sciences, Engineering, and Medicine over the years on a number of issues. She expressed her pleasure that this partnership was now extending to a new issue—nutrition and the older adult.
Ryerson stated that this workshop will deepen the knowledge base concerning the dietary needs of the rapidly growing older population and will help to broaden the base of individuals and organizations working to meet those dietary needs.
The AARP Foundation and Low-Income Older Adults
Ryerson went on to explain that the AARP Foundation addresses the needs of low-income adults ages 50 and older by investing in and advancing effective solutions that attack the root causes of the many challenges they face: the need for adequate and nutritious food, for functional and affordable housing, for steady income, and for strong and sustaining bonds to family, friends, and community. The AARP Foundation emphasizes and builds upon the links among the four core issues of hunger, housing, income, and social isolation. For example, the AARP Foundation tries to ensure that vulnerable older adults have the information they need about proper nutrition. It also is working to promote efficient distribution systems that will reduce cost and increase availability and access to healthy and nutritious foods. Ryerson suggested that this will strengthen food knowledge to enhance buying power, purchasing habits, and cooking skills that result in healthy, nutritious, and age-appropriate meals.
More than 10 million Americans ages 50 and older are at risk of hunger every day. Ryerson noted that the scope of the problem and other ill effects affecting so many vulnerable low-income older adults is recognized and that a real sense of optimism is beginning to emerge because the 50+ demographic is finally starting to be understood by corporations, by nonprofits, by government, and others. Older adults are not only the fastest-growing segment of our population, but also one that warrants much greater attention as health care costs and chronic disease rates continue to rise.
Ryerson noted a growing awareness that a new model, with new strategies and tactics, is needed to combat hunger and food insecurity among older adults. She then described a new organization, the Root Cause Coalition, launched by the AARP Foundation. The Coalition is a nonprofit that brings together health care providers, insurers, the food and agriculture sectors, and other nonprofits to establish a national framework for programs, policies, and research to address the problem of hunger as a health issue in a proactive and systematic way. This means creating sustainable business models, promoting education, providing incentives for healthy eating and carrying out cutting-edge research. Ryerson added that charity can also play an indispensable, life-saving role in fighting hunger.
Time for a New Paradigm
But, she stated, it is time for a new paradigm that not only embraces a charitable response but that puts science in the forefront of the effort to meet the nutritional needs of older adults. Understanding what constitutes good nutrition for older adults is essential to this approach. This workshop is important, she explained, because it connects an informed understanding
of the elements of good nutrition with programs and initiatives designed to meet these dietary needs. It also helps to identify gaps in knowledge that require further study. This new paradigm will need a greater focus on the nutrition needs of older adults in the development of food products, in the retail setting, in federal assistance programs and nutrition guidance, and in community initiatives. For example, the AARP Foundation is working on a food insecurity nutrition incentive program in Mississippi and Tennessee. With a grant from the U.S. Department of Agriculture (USDA) and additional support from United Healthcare, Supplemental Nutrition Assistance Program (SNAP) beneficiaries in those states can go to participating grocery stores and farmers’ markets. They can spend up to $10 buying fruits and vegetables with their SNAP benefits card and receive deep discounts on future purchases of fruits and vegetables. The AARP Foundation also is exploring food by prescription through partnerships, pilots, research, and collaboration with the health care community. The Affordable Care Act’s (ACA’s) emphasis on prevention and keeping people healthy at home rather than in medical or institutional settings provides a strong impetus for these efforts.
Ryerson continued by saying that new collaborations between nutritionists, nurses, food producers, and family caregivers also would be helpful to make sure vulnerable people have access to healthy foods and health care. Particular attention is needed for two overlapping population groups who face an equally acute food insecurity problem. One group is people between the ages of 50 and 64. They are too young for Medicare but they are not too young to have chronic diseases that can severely impair their health and undermine their finances and therefore undermine their futures. The other group is multigenerational households. These households are almost three times as likely to be food insecure as households without grandparents.
CONSUMER BEHAVIOR
David Donnan is a partner at A.T. Kearney, a global management consulting firm that works across all industries, including food manufacturers, retailers, and restaurants chains. In its work with food industries, A.T. Kearney collaborates with a variety of nongovernmental organizations to find sustainable business models for hunger relief that can continue into the future and adapt to many of the major trends and changes that are occurring in the world.
The “Age Quake”
Donnan explained that the world is facing what is often called an “age quake.” This “age quake” is characterized by two major trends. The first is that even though the world’s overall population is increasing from 7.2 billion people today to 9 billion people in 2050, the birthrate is slowing in every country, including China and India. As a result, fewer young people are being added to populations. The second trend is that through advances in medicine and nutrition, people are living longer. This means the world has a growing older population that is living longer and a shrinking number of young people available to help support the aging population. In 2014, four countries—Germany, Greece, Italy, and Japan—had populations in which those older than age 65 represented more than 20 percent of the total population. In 2020, nine countries will join that list. By 2030, 34 countries, including the United States, will have at least 20 percent of their population older than age 65 (Johnson, 2014). Moreover, the fastest growing age cohort in the United States currently is people age 100 or older. By 2025, 119,000 consumers will be age 100 or older. By the year 2050, more than 1 million people will be age 100 or older (Baum, 1999). Donnan then noted that these 1 million people turned age 65 in 2015. They are alive today, and the challenge is ensuring that they are healthy and vibrant and living decent lives as they age.
Today, advertising and media focus to a large extent on the Millennial generation, but as Donnan explained, significant spending power rests with the Baby Boomers and older adult groups. He noted that the age 50 and older population is expected to spend close to 50 percent of the dollars spent on consumer packaged goods, yet less than 5 percent of advertising is aimed toward this group. In the United States, $3 trillion is spent annually by consumers older than age 60; globally it is $15 trillion. He further explained that simultaneously, the United States is facing an economic challenge in that 29 percent of older adults have no defined benefit plan or retirement savings.
Understanding the Consumer Preferences of Older Adults
Donnan then described an A.T. Kearney Global Maturing Consumer Study where more than 3,000 consumers ages 60 and older were interviewed in person in seven countries that represent 60 percent of the world population. The survey asked them about their perceptions on consumer shopping, products, and related issues. Donnan noted that these consumers have distinct characteristics that are different from those of younger groups (and will be different than the million people age 100 who will be shopping by 2050).
- They buy different product categories and enjoy shopping more.
- They shop often in smaller stores close to home.
- They are more loyal and demanding when it comes to quality.
- They watch for promotions but do not find them adapted to their needs and desires as much as they could be.
- Their priorities also change as they age. A person age 60 is different than one age 70, who is different than one age 80.
Donnan summarized the three main themes that emerged from the survey: (1) older adults are not being served well by retailers, customer service, or the products, (2) navigation in shops can be a real challenge and the supercenter shops that are increasingly common are not designed well for older adults, and (3) product packaging is still a big problem, as older adults have difficulty opening, reading, and using packages.
Survey findings revealed other differences between older adults and other age groups:
- Mature consumers spend less of their income on clothing and transportation. Older adults use cars less and public transportation more.
- They spend more of their income on food, beverages, and health care.
- They enjoy shopping and often shop as part of their daily routine. But not all are mobile enough to go out and shop, and meeting the needs of these consumers is a challenge for retailers.
- Though they do not necessarily always shop in smaller stores that are closer to home, they express a preference for doing so because of perceived easier navigation in the store, better customer service, and ability to walk to the store.
Donnan stated that these findings present both challenges and opportunities for retailers and service providers. For example, businesses have opportunities in providing transportation alternatives, such as Uber and Zip Car, to older adults who do not drive or in providing connectivity technology through mobile devices. Millennials who are already comfortable with technology will come to expect it as they age. Many existing approaches are based on old technologies and old conceptions about behaviors.
A.T. Kearney has conducted research in collaboration with the AARP Foundation on senior nutrition and meeting the needs of economically disadvantaged seniors. This research has shown that efforts to reach the mature consumer should take into account affordability, participation in nutrition assistance programs, new sources of food (such as drug stores), the availability and understandability of food and nutrition information,
and new approaches for delivering nutritious food. Donnan also stated that it will be difficult to depend on government for funding and other types of assistance in the future so it will be necessary to find ways of working on sustainable ways to use the vast amount of available expertise and help those in need. There is a way to achieve the “three bottom lines,” he said: be sustainable, be socially responsible, and be profitable.
Meeting the Needs of Older Adults in Innovative Ways
Using its knowledge of the older adult consumer, Donnan described ways in which industry should look at ways to leverage existing approaches and technologies to build a new and innovative model of outreach in three areas: food sourcing, food preparation, and food to consumer. For food sourcing, he asked whether there is a way to leverage the collective food purchases of older adults to buy produce less expensively. Could organizations such as Feeding America®2 work with AARP, Meals on Wheels™, and other groups to consolidate their purchases? For-profit companies use this approach, noted Donnan. He suggested that establishing a central kitchen that could prepare baskets of nutritious food and have them delivered to people who are economically disadvantaged could also be a new approach to food preparation for older adults. An innovative food to consumer approach might leverage the existing U.S. Postal Service (USPS) network to deliver nutritious food.
Donnan concluded his remarks by noting that with the coming “age quake,” older consumers will need help accessing healthy food. In concert with traditional approaches to food distribution, such as industry donations from distributors and wholesalers, community food drives, and food purchased using donated money, innovative ideas about how to deliver food to older adults in need will be significant (see Figure 1-1). Partnerships between for-profit companies and nonprofit organizations could provide an opportunity for generating innovative ideas.
Question and Answer Session
Following Donnan’s presentation, the floor was opened for questions. In response to one participant’s question about a role for government at different levels, Donnan responded that government definitely has a role to play. He noted that the AARP’s recent Hunger Summit included representatives from the USDA in addition to food manufacturers, agricultural
___________________
2 Feeding America® is a nonprofit, nationwide network of food banks that provides more than 3.6 billion meals to virtually every community in the United States through food pantries and meal programs.

SOURCE: Presented by David Donnan on October 28, 2015 (A.T. Kearney).
companies, food retailers, and nonprofit groups, such as Feeding America® and Ella’s Kitchen™.3 All these groups worked together to generate ideas for ways to address hunger. One idea that emerged was to work with a local nonprofit to use SNAP benefits to support infrastructure for a company like Peapod4 to enter an inner city market. A major cost for home food delivery is the route stops. Therefore, this infrastructure support would give the company enough fixed cost coverage to allow them to increase their business beyond areas that already can pay for delivery. This example demonstrates one way in which government, industry, and a nonprofit could partner on an initiative that all parties would benefit from.
A second question for Donnan dealt with the perception that food manufacturers tend to market more to the millennials than to older consumers. Donnan replied that this is true, but that this is beginning to shift because of changing understanding around assumptions about brand loyalty. The traditional assumption is that once a brand loyalty is established, people tend to stick with that brand. Manufacturers focus on millennials because their brand loyalties are still being molded. Donnan stated that this traditional assumption is being challenged now because manufacturers are finding that many older consumers may change their brand preferences. He noted that so many new products are coming out, there are so many different ways of being introduced to a product, and people are now more willing to experiment with new taste and flavors and types of foods.
WHAT IS HEALTHY AGING?
Simin Meydani, Director of the Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University, opened her presentation by
___________________
3 Ella’s Kitchen™ is a company that makes organic baby and toddler food that is sold in supermarkets internationally.
4 Peapod is an online grocery delivery service.
reiterating that with the population getting older it becomes important to develop a strategy that can enhance the health of older adults and help them live longer and healthier lives.
Meydani noted that to develop a strategy, two concepts that are fundamental to the concept of successful aging and that have evolved over the years must be considered:
- The first concept is that aging and age-associated diseases cannot be completely separated from each other.
- The second concept is that age-associated disabilities are an inevitable part of the aging process and controlled mainly by genetic factors. However, current research indicates that genetics might not have as important a role in aging as lifestyle and other environmental factors. This is good news in terms of being able to intervene and change the course and the trajectory of aging.
Definitions of Successful Aging
Meydani explained that gerontologists and geriatricians have not yet come to a consensus on what components are essential in successful aging. Early definitions of successful aging were focused on a lack of disease or an absence of negative attributes. The current understanding is that healthy aging is not really the opposite of aging with disease or of functional impairment. Rather, Rowe and Kahn (1987) one of the first research teams to describe successful aging, suggested that it involved freedom from disability, high cognitive and physical functioning, and social and productive engagement. They later added resilience, the ability to adapt to, and recover from, unpredictable events, such as the loss of a loved one or an accident, to this definition. Rowe and Kahn identified modifiable factors that could influence successful aging, including osteoporosis, cognitive function, psychosocial factors, and bereavement and relocation. Later, other groups, such as the National Institute on Aging (NIA), the White House Conference on Aging, and the World Health Organization (WHO), also emphasized that healthy aging goes beyond the absence of disease and disability. More recently, the Canadian government went even further in their definition, describing healthy aging in holistic terms as “a lifelong process of optimizing opportunities for improving and preserving health and physical, social, and mental wellness, independence, quality of life, and enhancing successful life-course transitions” (Health Canada, 2002). Meydani went on to show how others have defined successful aging as the degree to which older adults “adapt to age-associated changes,” “view themselves as successfully aging,” and “are morbidity-free until the latest time point before death” (Baltes, 1997;
Bowling and Dieppe, 2005; Fries, 2002; Schulz and Heckhausen, 1996; von Faber et al., 2001).
Factors That Contribute to Successful Aging
Meydani explained that researchers have subsequently attempted to identify factors that contribute to successful aging. A 2014 study looked at determinants of successful aging together with an assessment of dietary habits in relation to the use of health care facilities by older populations living in Mediterranean areas (Tyrovolas et al., 2014). They examined three domains: (1) low probability of diseases and disability, (2) high cognitive and physical capability, and (3) active participation in social activities. The investigators developed a 10-point index of successful aging that included education, financial status, participation in social activities with friends, social activities with family, number of yearly excursions, body mass index (BMI), number of cardiovascular disease risk factors, depression, adherence to the Mediterranean diet, and frequency of physical activity.
The results of their analysis showed that higher scores on these attributes combined were associated with less use of health care services. Specifically, a 1/10-unit increase in the successful aging index was associated with 0.8 fewer health care service visits or consultations within a 1-year period (Tyrovolas et al., 2014). A closer examination of these attributes shows that the lifestyle characteristics were the main contributors to successful aging, accounting for 48 percent of the variability. Clinical factors accounted for 38 percent of the variability and psychosocial factors accounted for 23 percent. Meydani pointed out that high scores on measures of healthy diet and daily physical activity both ranked high in terms of factors that contributed to successful aging.
Meydani went on to summarize findings from a literature review of 29 studies of community-dwelling older adults, which assessed the percentage of “successful agers” (Depp and Jeste, 2006). The percent of successful agers identified in these different studies were quite varied, but the authors noted that a major source of the variability in results was the differences across studies in the definition of successful aging and its components. Other factors, including the criteria for assigning subjects to the comparison “unsuccessful” group and a bias toward negative outcomes, also contributed to some of the low successful aging rates reported. That study found that factors strongly supportive of successful aging were absence of arthritis, absence of hearing problems, better activities of daily living, and not smoking. Moderate supporters were higher amount of exercise, better self-related health, and lower systolic blood pressure. Factors that had limited support for healthy aging included higher income, greater education, current marriage, and white ethnicity.
Other studies also have looked at the literature in an attempt to identify factors that contribute to successful aging. Peel et al. (2005) found that definitions of health or successful aging ranged from the primarily biological, such as survival to old age with absence of disability, to the comprehensive, such as sustained well-being using a bio-psychosocial model. Despite the wide range of definitions used, Peel et al. (2005) found that the majority of the studies emphasized maintenance of functional independence, measured as the ability to perform basic and/or instrumental activities of daily living. Factors such as high functioning in tests of physical performance, cognitive ability, and absence of disease and psychiatric morbidity appeared less frequently. The indicators used within the domains to measure outcomes, and the way they were aggregated into summary scores influenced the resulting percentages of healthy older adults in the populations. Several behavioral determinants were associated with healthy aging: normal weight, physical activity, not smoking, moderate alcohol consumption, absence of depression, and robust social contact.
Meydani then presented findings from Young et al. (2009), who took the definition further by incorporating a person’s own assessment of his or her health into determining successful aging. These researchers identified three domains that overlap and contain both physical as well as psychosocial elements (see Figure 1-2).
Meydani highlighted one particularly interesting finding, namely that social connectedness was important in determining how cognitively functional an older adult remained. Compared to people with the lowest levels
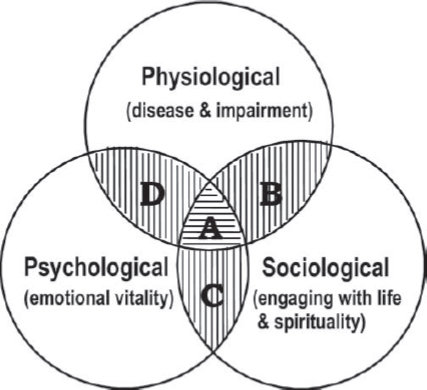
SOURCES: Presented by Simin Meydani on October 28, 2015; Young et al., 2009. Reprinted with permission.
of social integration, general cognitive decline was reduced by 39 percent among older adults with the highest number of social networks, and memory decline was halved over a period of 5 to 6 years (Haslam et al., 2014).
Meeting the Criteria for Successful Aging
Meydani noted that one challenge researchers and health care practitioners currently face is how best to use these findings to optimize cognitive health as people age. She went on to note that another way of looking at this is to break the domains of successful aging into objective definitions and subjective definitions. Researchers are finding that most older people do not meet objective criteria for successful aging while a majority of them will meet subjective criteria for successful aging. Data from Jeste et al. (2010) show that, for example, only 15 percent of people would meet the criterion of “absence of diseases,” but 84 percent would meet the criterion of “life satisfaction” and 90 percent would meet the criterion of “self-rated successful aging.”
Meydani summarized by stating that the criteria used are important in how successful aging is defined and in how the effectiveness of interventions will be judged. She added that a large gulf exists between how older adults identify successful aging and how researchers and physicians define it. Researchers and physicians define successful aging with more objective measures and in terms of lack of disease, whereas for older people, issues such as adaptation, meaningfulness, and connection are really important.
The question then, asked Meydani, is who should define successful aging? Should health care providers and researchers define it? Should older people define it? Or, should all of us together define successful aging? Longitudinal studies on the reliability and validity of definitions of successful aging are needed, she concluded. Another need, she noted, was for good measures of the contributions of nutrition to successful aging.
In concluding her presentation, Meydani stated that even with the different approaches to defining successful aging, some commonalities, such as high levels of physical activity and high cognitive and social engagement, emerge repeatedly. However, good ways to measure and objectively define social function and engagement are still lacking, as are ways to incorporate these measures in interventions. To move forward, Meydani urged close collaboration between biomedical scientists and psychosocial scientists, with the involvement of older adults, to develop a workable definition of successful aging and its components. She also suggested that good measures of nutritional status are lacking in many of the studies that have looked at successful aging, and this is a gap that needs to be filled. She expressed a hope that the workshop would help fill this gap by contributing to a bet-
ter understanding of nutritional factors in successful aging and ideas for including good nutrition measures in studies of aging.
REFERENCES
Baltes, P. B. 1997. On the incomplete architecture of human ontogeny. Selection, optimization, and compensation as foundation of developmental theory. American Psycholology 52(4):366-380.
Baum, R. M. 1999. Putting the new millennium in perspective. Chemical & Engineering News 77(49):45-47.
Bowling, A., and P. Dieppe. 2005. What is successful ageing and who should define it? BMJ 331(7531):1548-1551.
Depp, C. A., and D. V. Jeste. 2006. Definitions and predictors of successful aging: A comprehensive review of larger quantitative studies. American Journal of Geriatric Psychiatry 14(1):6-20.
Fries, J. F. 2002. Successful aging—an emerging paradigm of gerontology. Clinical Geriatric Medicine 18(3):371-382.
Haslam, C., T. Cruwys, and S. A. Haslam. 2014. “The we’s have it”: Evidence for the distinctive benefits of group engagement in enhancing cognitive health in aging. Social Science Medicine 120:57-66.
Health Canada. 2002. Workshop on healthy aging. Ottawa, Ontario: Division of Aging and Seniors, Health Canada. http://publications.gc.ca/collections/Collection/H39-6122002-1E.pdf (accessed February 8, 2016).
IOM (Institute of Medicine). 2000. The role of nutrition in maintaining health in the nation’s elderly: Evaluating coverage of nutrition services for the Medicare population. Washington, DC: National Academy Press.
IOM. 2012. Nutrition and healthy aging in the community: Workshop summary. Washington, DC: The National Academies Press.
Jeste, D. V., C. A. Depp, and I. V. Vahia. 2010. Successful cognitive and emotional aging. World Psychiatry 9(2):78-84.
Johnson, S. 2014. “Super-Agers” are coming fast. Mail Tribune. http://www.mailtribune.com/article/20140831/NEWS/140839997/101093/LIFE (accessed April 4, 2016).
Peel, N. M., R. J. McClure, and H. P. Bartlett. 2005. Behavioral determinants of healthy aging. American Journal of Preventative Medicine 28(3):298-304.
Rowe, J. W., and R. L. Kahn. 1987. Human aging: Usual and successful. Science 237(4811): 143-149.
Schulz, R., and J. Heckhausen. 1996. A life span model of successful aging. American Psychology 51(7):702-714.
Tyrovolas, S., J. M. Haro, A. Mariolis, S. Piscopo, G. Valacchi, N. Tsakountakis, A. Zeimbekis, D. Tyrovola, V. Bountziouka, E. Gotsis, G. Metallinos, J. A. Tur, A. L. Matalas, C. Lionis, E. Polychronopoulos, and D. Panagiotakos. 2014. Successful aging, dietary habits and health status of elderly individuals: A k-dimensional approach within the multi-national MEDIS study. Experimental Gerontology 60:57-63.
von Faber, M., A. Bootsma-van der Wiel, E. van Exel, J. Gussekloo, A. M. Lagaay, E. van Dongen, D. L. Knook, S. van der Geest, and R. G. Westendorp. 2001. Successful aging in the oldest old: Who can be characterized as successfully aged? Archives of Internal Medicine 161(22):2694-2700.
Young, Y., K. D. Frick, and E. A. Phelan. 2009. Can successful aging and chronic illness coexist in the same individual? A multidimensional concept of successful aging. Journal of the American Medical Directors Association 10(2):87-92.
This page intentionally left blank.














